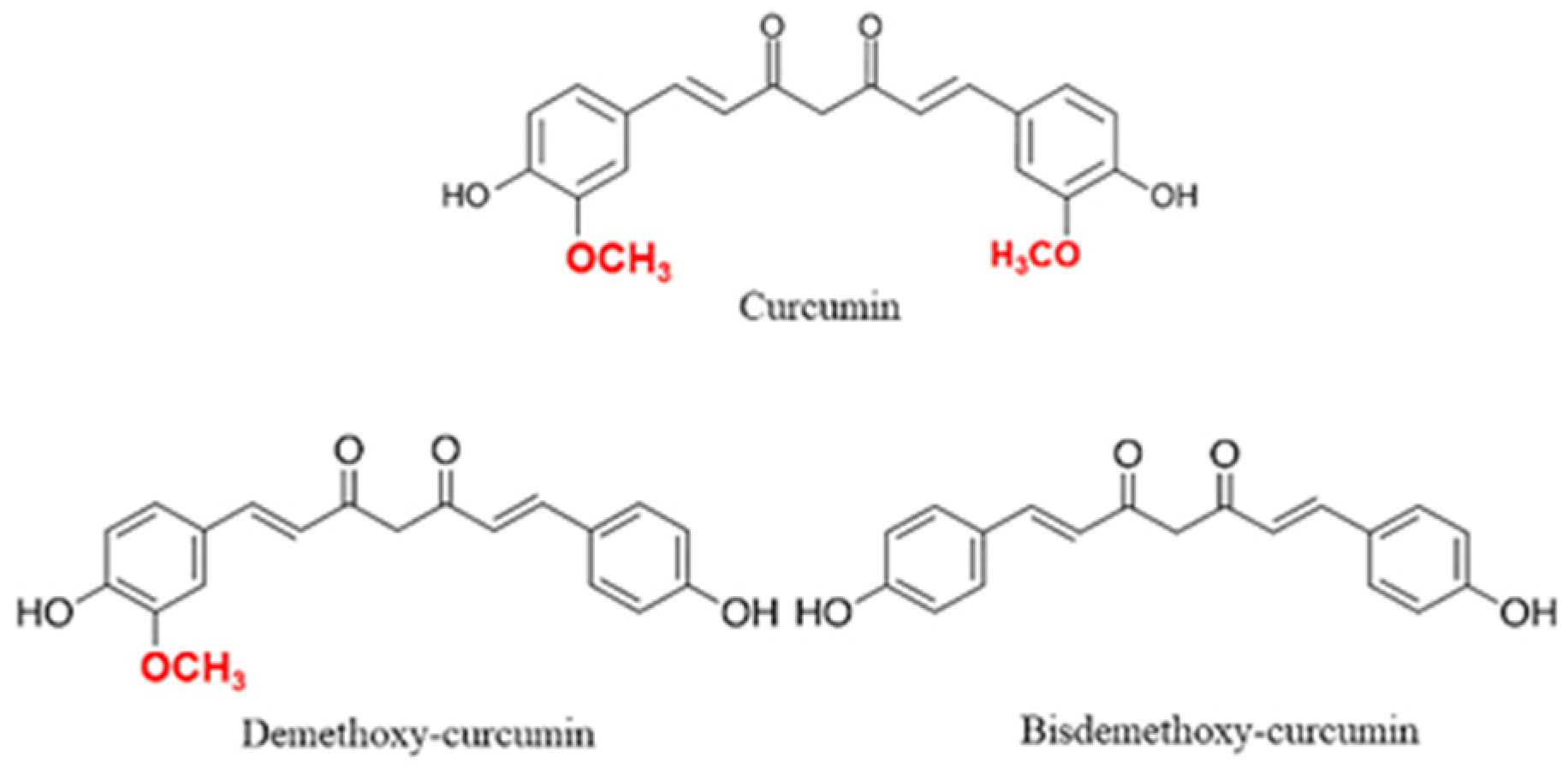
The Multifaced Actions of Curcumin in Pregnancy Outcome
Abstract
1. Introduction
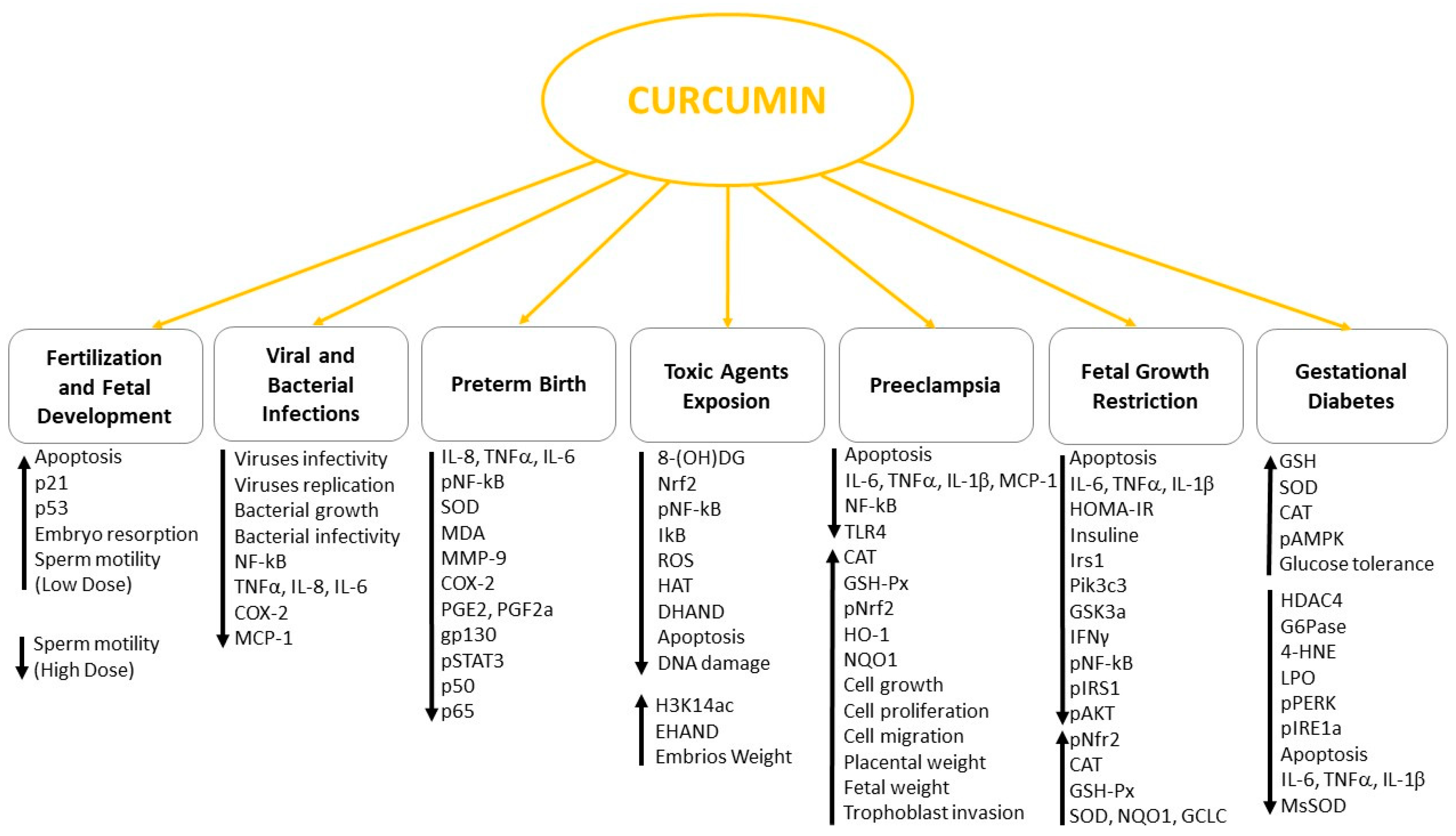
2. Curcumin Effects on Fertilization and Fetal Development
3. Curcumin as Protector of Cytotoxic and Teratogenic Agents
4. Curcumin as Potential Treatment of Viral and Bacterial Infections
5. Curcumin in Gestational Diabetes Mellitus (GDM)
6. Curcumin in Preeclampsia (PE)
7. Curcumin in Fetal Growth Restriction (FGR)
8. Curcumin in Preterm Birth
9. Conclusions and Further Research
Author Contributions
Funding
Conflicts of Interest
References
- Amalraj, A.; Pius, A.; Gopi, S.; Gopi, S. Biological activities of curcuminoids, other biomolecules from turmeric and their derivatives—A review. J. Tradit. Complement. Med. 2017, 7, 205–233. [Google Scholar] [CrossRef] [PubMed]
- Soleimani, V.; Sahebkar, A.; Hosseinzadeh, H. Turmeric (Curcuma longa) and its major constituent (curcumin) as nontoxic and safe substances: Review. Phytother. Res. 2018, 32, 985–995. [Google Scholar] [CrossRef] [PubMed]
- Kotha, R.R.; Luthria, D.L. Curcumin: Biological, Pharmaceutical, Nutraceutical, and Analytical Aspects. Molecules 2019, 24, 2930. [Google Scholar] [CrossRef] [PubMed]
- Best, L.; Elliott, A.C.; Brown, P.D. Curcumin induces electrical activity in rat pancreatic beta-cells by activating the volume-regulated anion channel. Biochem. Pharmacol. 2007, 73, 1768–1775. [Google Scholar] [CrossRef]
- Jamilian, M.; Foroozanfard, F.; Kavossian, E.; Aghadavod, E.; Shafabakhsh, R.; Hoseini, A.; Asemi, Z. Effects of curcumin on body weight, glycemic control and serum lipids in women with polycystic ovary syndrome: A randomized, double-blind, placebo-controlled trial. Clin. Nutr. ESPEN 2020, 36, 128–133. [Google Scholar] [CrossRef]
- Den Hartogh, D.J.; Gabriel, A.; Tsiani, E. Antidiabetic Properties of Curcumin I: Evidence from In Vitro Studies. Nutrients 2020, 12, 118. [Google Scholar] [CrossRef]
- Saberi-Karimian, M.; Keshvari, M.; Ghayour-Mobarhan, M.; Salehizadeh, L.; Rahmani, S.; Behnam, B.; Jamialahmadi, T.; Asgary, S.; Sahebkar, A. Effects of curcuminoids on inflammatory status in patients with non-alcoholic fatty liver disease: A randomized controlled trial. Complement. Ther. Med. 2020, 49, 102322. [Google Scholar] [CrossRef]
- Zhan, Y.; Chen, Y.; Liu, R.; Zhang, H.; Zhang, Y. Potentiation of paclitaxel activity by curcumin in human breast cancer cell by modulating apoptosis and inhibiting EGFR signaling. Arch. Pharm. Res. 2014, 37, 1086–1095. [Google Scholar] [CrossRef]
- Khazaei Koohpar, Z.; Entezari, M.; Movafagh, A.; Hashemi, M. Anticancer Activity of Curcumin on Human Breast Adenocarcinoma: Role of Mcl-1 Gene. Iran. J. Cancer Prev. 2015, 8, e2331. [Google Scholar] [CrossRef]
- Wang, J.; Zhang, J.; Zhang, C.J.; Wong, Y.K.; Lim, T.K.; Hua, Z.C.; Liu, B.; Tannenbaum, S.R.; Shen, H.M.; Lin, Q. In situ Proteomic Profiling of Curcumin Targets in HCT116 Colon Cancer Cell Line. Sci. Rep. 2016, 6, 22146. [Google Scholar] [CrossRef]
- Man, S.; Zhang, L.; Cui, J.; Yang, L.; Ma, L.; Gao, W. Curcumin enhances the anti-cancer effects of Paris Saponin II in lung cancer cells. Cell Prolif. 2018, 51, e12458. [Google Scholar] [CrossRef] [PubMed]
- Zhang, X.; Zhang, C.; Ren, Z.; Zhang, F.; Xu, J.; Zhang, X.; Zheng, H. Curcumin Affects Gastric Cancer Cell Migration, Invasion and Cytoskeletal Remodeling Through Gli1-beta-Catenin. Cancer Manag. Res. 2020, 12, 3795–3806. [Google Scholar] [CrossRef] [PubMed]
- Deng, Y.I.; Verron, E.; Rohanizadeh, R. Molecular Mechanisms of Anti-metastatic Activity of Curcumin. Anticancer Res. 2016, 36, 5639–5647. [Google Scholar] [CrossRef] [PubMed]
- Kolivand, S.; Amini, P.; Saffar, H.; Rezapoor, S.; Motevaseli, E.; Najafi, M.; Nouruzi, F.; Shabeeb, D.; Musa, A.E. Evaluating the Radioprotective Effect of Curcumin on Rat’s Heart Tissues. Curr. Radiopharm. 2019, 12, 23–28. [Google Scholar] [CrossRef] [PubMed]
- Nguyen, M.H.; Pham, N.D.; Dong, B.; Nguyen, T.H.; Bui, C.B.; Hadinoto, K. Radioprotective activity of curcumin-encapsulated liposomes against genotoxicity caused by Gamma Cobalt-60 irradiation in human blood cells. Int. J. Radiat. Biol. 2017, 93, 1267–1273. [Google Scholar] [CrossRef] [PubMed]
- Jayarajan, J.; Angandoor, S.; Vedulla, S.H.; Sritharan, S.; Ganesan, K.; War, A.R.; Sivalingam, N. Curcumin induces chemosensitization to doxorubicin in Duke’s type B coloadenocarcinoma cell line. Mol. Biol. Rep. 2020, 47, 7883–7892. [Google Scholar] [CrossRef]
- Najafi, M.; Mortezaee, K.; Rahimifard, M.; Farhood, B.; Haghi-Aminjan, H. The role of curcumin/curcuminoids during gastric cancer chemotherapy: A systematic review of non-clinical study. Life Sci. 2020, 257, 118051. [Google Scholar] [CrossRef]
- Davatgaran-Taghipour, Y.; Masoomzadeh, S.; Farzaei, M.H.; Bahramsoltani, R.; Karimi-Soureh, Z.; Rahimi, R.; Abdollahi, M. Polyphenol nanoformulations for cancer therapy: Experimental evidence and clinical perspective. Int. J. Nanomed. 2017, 12, 2689–2702. [Google Scholar] [CrossRef]
- Tossetta, G.; Avellini, C.; Licini, C.; Giannubilo, S.R.; Castellucci, M.; Marzioni, D. High temperature requirement A1 and fibronectin: Two possible players in placental tissue remodelling. Eur. J. Histochem. 2016, 60, 2724. [Google Scholar] [CrossRef]
- Huppertz, B. The anatomy of the normal placenta. J. Clin. Pathol. 2008, 61, 1296–1302. [Google Scholar] [CrossRef]
- Aplin, J.D.; Myers, J.E.; Timms, K.; Westwood, M. Tracking placental development in health and disease. Nat. Rev. Endocrinol. 2020, 16, 479–494. [Google Scholar] [CrossRef] [PubMed]
- Costa, M.A. The endocrine function of human placenta: An overview. Reprod. Biomed. Online 2016, 32, 14–43. [Google Scholar] [CrossRef] [PubMed]
- Carter, A.M.; Enders, A.C. Placentation in mammals: Definitive placenta, yolk sac, and paraplacenta. Theriogenology 2016, 86, 278–287. [Google Scholar] [CrossRef] [PubMed]
- Fantone, S.; Mazzucchelli, R.; Giannubilo, S.R.; Ciavattini, A.; Marzioni, D.; Tossetta, G. AT-rich interactive domain 1A protein expression in normal and pathological pregnancies complicated by preeclampsia. Histochem. Cell Biol. 2020, 154, 339–346. [Google Scholar] [CrossRef] [PubMed]
- Gesuita, R.; Licini, C.; Picchiassi, E.; Tarquini, F.; Coata, G.; Fantone, S.; Tossetta, G.; Ciavattini, A.; Castellucci, M.; Di Renzo, G.C.; et al. Association between first trimester plasma htra1 level and subsequent preeclampsia: A possible early marker? Pregnancy Hypertens 2019, 18, 58–62. [Google Scholar] [CrossRef] [PubMed]
- Tossetta, G.; Fantone, S.; Giannubilo, S.R.; Marinelli Busilacchi, E.; Ciavattini, A.; Castellucci, M.; Di Simone, N.; Mattioli-Belmonte, M.; Marzioni, D. Pre-eclampsia onset and SPARC: A possible involvement in placenta development. J. Cell Physiol. 2019, 234, 6091–6098. [Google Scholar] [CrossRef]
- Huppertz, B. The Critical Role of Abnormal Trophoblast Development in the Etiology of Preeclampsia. Curr. Pharm. Biotechnol. 2018, 19, 771–780. [Google Scholar] [CrossRef]
- Tsai, K.Y.F.; Tullis, B.; Mejia, J.; Reynolds, P.R.; Arroyo, J.A. Regulation of trophoblast cell invasion by Pyruvate Kinase isozyme M2 (PKM2). Placenta 2020, 103, 24–32. [Google Scholar] [CrossRef]
- Marzioni, D.; Lorenzi, T.; Altobelli, E.; Giannubilo, S.R.; Paolinelli, F.; Tersigni, C.; Crescimanno, C.; Monsurro, V.; Tranquilli, A.L.; Di Simone, N.; et al. Alterations of maternal plasma HTRA1 level in preeclampsia complicated by IUGR. Placenta 2012, 33, 1036–1038. [Google Scholar] [CrossRef]
- Niu, Y.; He, J.; Zhao, Y.; Shen, M.; Zhang, L.; Zhong, X.; Wang, C.; Wang, T. Effect of Curcumin on Growth Performance, Inflammation, Insulin level, and Lipid Metabolism in Weaned Piglets with IUGR. Animals 2019, 9, 1098. [Google Scholar] [CrossRef]
- Ustundag, B.; Yilmaz, E.; Dogan, Y.; Akarsu, S.; Canatan, H.; Halifeoglu, I.; Cikim, G.; Aygun, A.D. Levels of cytokines (IL-1beta, IL-2, IL-6, IL-8, TNF-alpha) and trace elements (Zn, Cu) in breast milk from mothers of preterm and term infants. Mediators Inflamm. 2005, 2005, 331–336. [Google Scholar] [CrossRef] [PubMed]
- Falsaperla, R.; Lombardo, F.; Filosco, F.; Romano, C.; Saporito, M.A.N.; Puglisi, F.; Piro, E.; Ruggieri, M.; Pavone, P. Oxidative Stress in Preterm Infants: Overview of Current Evidence and Future Prospects. Pharmaceuticals 2020, 13, 145. [Google Scholar] [CrossRef] [PubMed]
- Giannubilo, S.R.; Licini, C.; Picchiassi, E.; Tarquini, F.; Coata, G.; Fantone, S.; Tossetta, G.; Ciavattini, A.; Castellucci, M.; Giardina, I.; et al. First trimester HtrA1 maternal plasma level and spontaneous preterm birth. J. Matern. Fetal Neonatal Med. 2020, 1–5. [Google Scholar] [CrossRef] [PubMed]
- Jarrett, R.J. Reflections on gestational diabetes mellitus. Lancet 1981, 2, 1220–1221. [Google Scholar] [CrossRef]
- Yogev, Y.; Xenakis, E.M.; Langer, O. The association between preeclampsia and the severity of gestational diabetes: The impact of glycemic control. Am. J. Obstet. Gynecol. 2004, 191, 1655–1660. [Google Scholar] [CrossRef]
- Ali, S.; Majid, S.; Ali, M.N.; Taing, S.; Rehman, M.U.; Arafah, A. Cytokine imbalance at materno-embryonic interface as a potential immune mechanism for recurrent pregnancy loss. Int. Immunopharmacol. 2020, 107118. [Google Scholar] [CrossRef]
- Arefieva, A.; Nikolaeva, M.; Stepanova, E.; Krechetova, L.; Golubeva, E.; Tetruashvili, N.; Sukhikh, G. Association of CD200 expression in paternal lymphocytes with female Th1/Th2 balance and pregnancy establishment at immunotherapy of recurrent spontaneous abortion. Am. J. Reprod. Immunol. 2020, e13355. [Google Scholar] [CrossRef]
- Guerrero, B.; Hassouneh, F.; Delgado, E.; Casado, J.G.; Tarazona, R. Natural killer cells in recurrent miscarriage: An overview. J. Reprod. Immunol. 2020, 142, 103209. [Google Scholar] [CrossRef]
- Marzioni, D.; Quaranta, A.; Lorenzi, T.; Morroni, M.; Crescimanno, C.; De Nictolis, M.; Toti, P.; Muzzonigro, G.; Baldi, A.; De Luca, A.; et al. Expression pattern alterations of the serine protease HtrA1 in normal human placental tissues and in gestational trophoblastic diseases. Histol. Histopathol. 2009, 24, 1213–1222. [Google Scholar]
- Licini, C.; Tossetta, G.; Avellini, C.; Ciarmela, P.; Lorenzi, T.; Toti, P.; Gesuita, R.; Voltolini, C.; Petraglia, F.; Castellucci, M.; et al. Analysis of cell-cell junctions in human amnion and chorionic plate affected by chorioamnionitis. Histol. Histopathol. 2016, 31, 759–767. [Google Scholar]
- Tossetta, G.; Paolinelli, F.; Avellini, C.; Salvolini, E.; Ciarmela, P.; Lorenzi, T.; Emanuelli, M.; Toti, P.; Giuliante, R.; Gesuita, R.; et al. IL-1beta and TGF-beta weaken the placental barrier through destruction of tight junctions: An in vivo and in vitro study. Placenta 2014, 35, 509–516. [Google Scholar] [CrossRef] [PubMed]
- Racicot, K.; Mor, G. Risks associated with viral infections during pregnancy. J. Clin. Investig. 2017, 127, 1591–1599. [Google Scholar] [PubMed]
- Burdet, J.; Rubio, A.P.; Salazar, A.I.; Ribeiro, M.L.; Ibarra, C.; Franchi, A.M. Inflammation, infection and preterm birth. Curr. Pharm. Des. 2014, 20, 4741–4748. [Google Scholar] [CrossRef] [PubMed]
- Barandeh, B.; Amini Mahabadi, J.; Azadbakht, M.; Gheibi Hayat, S.M.; Amini, A. The protective effects of curcumin on cytotoxic and teratogenic activity of retinoic acid in mouse embryonic liver. J. Cell Biochem. 2019, 120, 19371–19376. [Google Scholar] [CrossRef]
- Ran, Z.; Zhang, Y.; Wen, X.; Ma, J. Curcumin inhibits high glucoseinduced inflammatory injury in human retinal pigment epithelial cells through the ROSPI3K/AKT/mTOR signaling pathway. Mol. Med. Rep. 2019, 19, 1024–1031. [Google Scholar]
- Hsuuw, Y.D.; Chang, C.K.; Chan, W.H.; Yu, J.S. Curcumin prevents methylglyoxal-induced oxidative stress and apoptosis in mouse embryonic stem cells and blastocysts. J. Cell Physiol. 2005, 205, 379–386. [Google Scholar]
- Basak, S.; Srinivas, V.; Mallepogu, A.; Duttaroy, A.K. Curcumin stimulates angiogenesis through VEGF and expression of HLA-G in first-trimester human placental trophoblasts. Cell Biol. Int. 2020, 44, 1237–1251. [Google Scholar] [CrossRef]
- Ghaneifar, Z.; Yousefi, Z.; Tajik, F.; Nikfar, B.; Ghalibafan, F.; Abdollahi, E.; Momtazi-Borojeni, A.A. The potential therapeutic effects of curcumin on pregnancy complications: Novel insights into reproductive medicine. IUBMB Life 2020, 72, 2572–2583. [Google Scholar]
- Filardi, T.; Vari, R.; Ferretti, E.; Zicari, A.; Morano, S.; Santangelo, C. Curcumin: Could This Compound Be Useful in Pregnancy and Pregnancy-Related Complications? Nutrients 2020, 12, 3179. [Google Scholar]
- Chan, W.H. Impact of genistein on maturation of mouse oocytes, fertilization, and fetal development. Reprod. Toxicol. 2009, 28, 52–58. [Google Scholar] [CrossRef]
- Chen, C.C.; Hsieh, M.S.; Hsuuw, Y.D.; Huang, F.J.; Chan, W.H. Hazardous effects of curcumin on mouse embryonic development through a mitochondria-dependent apoptotic signaling pathway. Int. J. Mol. Sci. 2010, 11, 2839–2855. [Google Scholar] [CrossRef] [PubMed]
- Huang, F.J.; Lan, K.C.; Kang, H.Y.; Liu, Y.C.; Hsuuw, Y.D.; Chan, W.H.; Huang, K.E. Effect of curcumin on in vitro early post-implantation stages of mouse embryo development. Eur. J. Obstet. Gynecol. Reprod. Biol. 2013, 166, 47–51. [Google Scholar] [CrossRef]
- Chen, C.C.; Chan, W.H. Injurious effects of curcumin on maturation of mouse oocytes, fertilization and fetal development via apoptosis. Int. J. Mol. Sci. 2012, 13, 4655–4672. [Google Scholar] [CrossRef] [PubMed]
- Ganiger, S.; Malleshappa, H.N.; Krishnappa, H.; Rajashekhar, G.; Ramakrishna Rao, V.; Sullivan, F. A two generation reproductive toxicity study with curcumin, turmeric yellow, in Wistar rats. Food Chem. Toxicol. 2007, 45, 64–69. [Google Scholar] [CrossRef]
- Vijayalaxmi. Genetic effects of turmeric and curcumin in mice and rats. Mutat. Res. 1980, 79, 125–132. [Google Scholar] [CrossRef]
- Zhou, Q.; Wu, X.; Liu, Y.; Wang, X.; Ling, X.; Ge, H.; Zhang, J. Curcumin improves asthenozoospermia by inhibiting reactive oxygen species reproduction through nuclear factor erythroid 2-related factor 2 activation. Andrologia 2020, 52, e13491. [Google Scholar] [CrossRef] [PubMed]
- Naz, R.K. Can curcumin provide an ideal contraceptive? Mol. Reprod. Dev. 2011, 78, 116–123. [Google Scholar] [CrossRef]
- Mondal, D.; Shenoy, S.R.; Mishra, S. Retinoic Acid Embryopathy. Int. J. Appl. Basic Med. Res. 2017, 7, 264–265. [Google Scholar] [CrossRef]
- Gad, A.; Abu Hamed, S.; Khalifa, M.; Amin, A.; El-Sayed, A.; Swiefy, S.A.; El-Assal, S. Retinoic acid improves maturation rate and upregulates the expression of antioxidant-related genes in in vitro matured buffalo (Bubalus bubalis) oocytes. Int. J. Vet. Sci. Med. 2018, 6, 279–285. [Google Scholar] [CrossRef]
- Zhao, Z. Reevaluation of Antioxidative Strategies for Birth Defect Prevention in Diabetic Pregnancies. J. Biomol. Res. Ther. 2016, 5, 145. [Google Scholar] [CrossRef]
- Bosetti, C.; Negri, E.; Fattore, E.; La Vecchia, C. Occupational exposure to polychlorinated biphenyls and cancer risk. Eur. J. Cancer Prev. 2003, 12, 251–255. [Google Scholar] [CrossRef] [PubMed]
- Ward, M.H.; Colt, J.S.; Metayer, C.; Gunier, R.B.; Lubin, J.; Crouse, V.; Nishioka, M.G.; Reynolds, P.; Buffler, P.A. Residential exposure to polychlorinated biphenyls and organochlorine pesticides and risk of childhood leukemia. Environ. Health Perspect. 2009, 117, 1007–1013. [Google Scholar] [CrossRef] [PubMed]
- Yao, M.; Hu, T.; Wang, Y.; Du, Y.; Hu, C.; Wu, R. Polychlorinated biphenyls and its potential role in endometriosis. Environ. Pollut. 2017, 229, 837–845. [Google Scholar] [CrossRef] [PubMed]
- Dickerson, A.S.; Ransome, Y.; Karlsson, O. Human prenatal exposure to polychlorinated biphenyls (PCBs) and risk behaviors in adolescence. Environ. Int. 2019, 129, 247–255. [Google Scholar] [CrossRef]
- Schantz, S.L.; Widholm, J.J.; Rice, D.C. Effects of PCB exposure on neuropsychological function in children. Environ. Health Perspect. 2003, 111, 357–576. [Google Scholar] [CrossRef]
- Aliyu, M.H.; Alio, A.P.; Salihu, H.M. To breastfeed or not to breastfeed: A review of the impact of lactational exposure to polychlorinated biphenyls (PCBs) on infants. J. Environ. Health 2010, 73, 8–14. [Google Scholar]
- Choksi, N.Y.; Kodavanti, P.R.; Tilson, H.A.; Booth, R.G. Effects of polychlorinated biphenyls (PCBs) on brain tyrosine hydroxylase activity and dopamine synthesis in rats. Fundam. Appl. Toxicol. 1997, 39, 76–80. [Google Scholar] [CrossRef]
- Dogan, H.O.; Alcigir, M.E. Assessment of epigenetic changes and oxidative DNA damage in rat pups exposed to polychlorinated biphenyls and the protective effect of curcumin in the prenatal period. J. Basic Clin. Physiol. Pharmacol. 2019, 30. [Google Scholar] [CrossRef]
- Fahr, M.; Laplaze, L.; Bendaou, N.; Hocher, V.; Mzibri, M.E.; Bogusz, D.; Smouni, A. Effect of lead on root growth. Front. Plant Sci. 2013, 4, 175. [Google Scholar] [CrossRef]
- Bellinger, D.C. Prenatal Exposures to Environmental Chemicals and Children’s Neurodevelopment: An Update. Saf. Health Work 2013, 4, 1–11. [Google Scholar] [CrossRef]
- Mameli, O.; Caria, M.A.; Melis, F.; Solinas, A.; Tavera, C.; Ibba, A.; Tocco, M.; Flore, C.; Sanna Randaccio, F. Neurotoxic effect of lead at low concentrations. Brain Res. Bull. 2001, 55, 269–275. [Google Scholar] [CrossRef]
- Bagchi, D.; Preuss, H.G. Effects of acute and chronic oval exposure of lead on blood pressure and bone mineral density in rats. J. Inorg. Biochem. 2005, 99, 1155–1164. [Google Scholar] [CrossRef] [PubMed]
- Benammi, H.; Erazi, H.; El Hiba, O.; Vinay, L.; Bras, H.; Viemari, J.C.; Gamrani, H. Disturbed sensorimotor and electrophysiological patterns in lead intoxicated rats during development are restored by curcumin I. PLoS ONE 2017, 12, e0172715. [Google Scholar] [CrossRef] [PubMed]
- Landgraf, M.N.; Nothacker, M.; Heinen, F. Diagnosis of fetal alcohol syndrome (FAS): German guideline version 2013. Eur. J. Paediatr. Neurol. 2013, 17, 437–446. [Google Scholar] [CrossRef] [PubMed]
- Zhang, W.; Peng, C.; Zheng, M.; Gao, W.; Zhu, J.; Lv, T.; Liu, L.; Liu, Z.; Li, H.; Xv, Y.; et al. Prenatal alcohol exposure causes the over-expression of DHAND and EHAND by increasing histone H3K14 acetylation in C57 BL/6 mice. Toxicol. Lett. 2014, 228, 140–146. [Google Scholar] [CrossRef] [PubMed]
- Yan, X.; Pan, B.; Lv, T.; Liu, L.; Zhu, J.; Shen, W.; Huang, X.; Tian, J. Inhibition of histone acetylation by curcumin reduces alcohol-induced fetal cardiac apoptosis. J. Biomed. Sci. 2017, 24, 1. [Google Scholar] [CrossRef]
- IARC Working Group on the Evaluation of Carcinogenic Risks to Humans. Some drinking-water disinfectants and contaminants, including arsenic. Monographs on chloramine, chloral and chloral hydrate, dichloroacetic acid, trichloroacetic acid and 3-chloro-4-(dichloromethyl)-5-hydroxy-2(5H)-furanone. IARC Monogr. Eval. Carcinog. Risks Hum. 2004, 84, 269–477. [Google Scholar]
- Milton, A.H.; Hussain, S.; Akter, S.; Rahman, M.; Mouly, T.A.; Mitchell, K. A Review of the Effects of Chronic Arsenic Exposure on Adverse Pregnancy Outcomes. Int. J. Environ. Res. Public Health 2017, 14, 556. [Google Scholar] [CrossRef]
- Poojan, S.; Kumar, S.; Verma, V.; Dhasmana, A.; Lohani, M.; Verma, M.K. Disruption of Skin Stem Cell Homeostasis following Transplacental Arsenicosis; Alleviation by Combined Intake of Selenium and Curcumin. PLoS ONE 2015, 10, e0142818. [Google Scholar]
- Ostensen, M.E.; Skomsvoll, J.F. Anti-inflammatory pharmacotherapy during pregnancy. Expert Opin. Pharmacother. 2004, 5, 571–580. [Google Scholar] [CrossRef]
- Kanakaris, N.K.; Roberts, C.S.; Giannoudis, P.V. Pregnancy-related pelvic girdle pain: An update. BMC Med. 2011, 9, 15. [Google Scholar] [CrossRef] [PubMed]
- Sareddy, G.R.; Kesanakurti, D.; Kirti, P.B.; Babu, P.P. Nonsteroidal anti-inflammatory drugs diclofenac and celecoxib attenuates Wnt/beta-catenin/Tcf signaling pathway in human glioblastoma cells. Neurochem. Res. 2013, 38, 2313–2322. [Google Scholar] [CrossRef] [PubMed]
- Nam, S.M.; Kim, J.W.; Yoo, D.Y.; Choi, J.H.; Kim, W.; Jung, H.Y.; Won, M.H.; Hwang, I.K.; Seong, J.K.; Yoon, Y.S. Comparison of pharmacological and genetic inhibition of cyclooxygenase-2: Effects on adult neurogenesis in the hippocampal dentate gyrus. J. Vet. Sci. 2015, 16, 245–251. [Google Scholar] [CrossRef] [PubMed]
- Wang, R.; Tian, S.; Yang, X.; Liu, J.; Wang, Y.; Sun, K. Celecoxib-induced inhibition of neurogenesis in fetal frontal cortex is attenuated by curcumin via Wnt/beta-catenin pathway. Life Sci. 2017, 185, 95–102. [Google Scholar] [CrossRef]
- Magos, L.; Clarkson, T.W. Overview of the clinical toxicity of mercury. Ann. Clin. Biochem. 2006, 43, 257–268. [Google Scholar] [CrossRef]
- Chehimi, L.; Roy, V.; Jeljeli, M.; Sakly, M. Chronic exposure to mercuric chloride during gestation affects sensorimotor development and later behaviour in rats. Behav. Brain Res. 2012, 234, 43–50. [Google Scholar] [CrossRef]
- Abu-Taweel, G.M. Neurobehavioral protective properties of curcumin against the mercury chloride treated mice offspring. Saudi J. Biol. Sci. 2019, 26, 736–743. [Google Scholar] [CrossRef]
- Mounce, B.C.; Cesaro, T.; Carrau, L.; Vallet, T.; Vignuzzi, M. Curcumin inhibits Zika and chikungunya virus infection by inhibiting cell binding. Antiviral Res. 2017, 142, 148–157. [Google Scholar] [CrossRef]
- Gao, Y.; Tai, W.; Wang, N.; Li, X.; Jiang, S.; Debnath, A.K.; Du, L.; Chen, S. Identification of Novel Natural Products as Effective and Broad-Spectrum Anti-Zika Virus Inhibitors. Viruses 2019, 11, 1019. [Google Scholar] [CrossRef]
- Lv, Y.; Gong, L.; Wang, Z.; Han, F.; Liu, H.; Lu, X.; Liu, L. Curcumin inhibits human cytomegalovirus by downregulating heat shock protein 90. Mol. Med. Rep. 2015, 12, 4789–4793. [Google Scholar] [CrossRef]
- Kutluay, S.B.; Doroghazi, J.; Roemer, M.E.; Triezenberg, S.J. Curcumin inhibits herpes simplex virus immediate-early gene expression by a mechanism independent of p300/CBP histone acetyltransferase activity. Virology 2008, 373, 239–247. [Google Scholar] [CrossRef] [PubMed]
- Ali, A.; Banerjea, A.C. Curcumin inhibits HIV-1 by promoting Tat protein degradation. Sci. Rep. 2016, 6, 27539. [Google Scholar] [CrossRef] [PubMed]
- Mazumder, A.; Raghavan, K.; Weinstein, J.; Kohn, K.W.; Pommier, Y. Inhibition of human immunodeficiency virus type-1 integrase by curcumin. Biochem. Pharmacol. 1995, 49, 1165–1170. [Google Scholar] [CrossRef]
- Zhou, X.; Zhang, B.; Cui, Y.; Chen, S.; Teng, Z.; Lu, G.; Wang, J.; Deng, X. Curcumin Promotes the Clearance of Listeria monocytogenes both In Vitro and In Vivo by Reducing Listeriolysin O Oligomers. Front. Immunol. 2017, 8, 574. [Google Scholar] [CrossRef] [PubMed]
- Baldissera, M.D.; Souza, C.F.; Zeppenfeld, C.C.; Descovi, S.; Machado, V.S.; Santos, R.C.V.; Baldisserotto, B. Efficacy of dietary curcumin supplementation as bactericidal for silver catfish against Streptococcus agalactiae. Microb. Pathog. 2018, 116, 237–240. [Google Scholar] [CrossRef] [PubMed]
- Wessler, S.; Muenzner, P.; Meyer, T.F.; Naumann, M. The anti-inflammatory compound curcumin inhibits Neisseria gonorrhoeae-induced NF-kappaB signaling, release of pro-inflammatory cytokines/chemokines and attenuates adhesion in late infection. Biol. Chem. 2005, 386, 481–490. [Google Scholar] [CrossRef] [PubMed]
- Chen, H.; Tang, Y.; Wang, H.; Chen, W.; Jiang, H. Curcumin alleviates lipopolysaccharide-induced neuroinflammation in fetal mouse brain. Restor. Neurol. Neurosci. 2018, 36, 583–592. [Google Scholar] [CrossRef]
- Ogurtsova, K.; da Rocha Fernandes, J.D.; Huang, Y.; Linnenkamp, U.; Guariguata, L.; Cho, N.H.; Cavan, D.; Shaw, J.E.; Makaroff, L.E. IDF Diabetes Atlas: Global estimates for the prevalence of diabetes for 2015 and 2040. Diabetes Res. Clin. Pract. 2017, 128, 40–50. [Google Scholar] [CrossRef]
- Coustan, D.R. Management of gestational diabetes mellitus: A self-fulfilling prophecy? JAMA 1996, 275, 1199–1200. [Google Scholar] [CrossRef]
- Ehrenberg, H.M.; Durnwald, C.P.; Catalano, P.; Mercer, B.M. The influence of obesity and diabetes on the risk of cesarean delivery. Am. J. Obstet. Gynecol. 2004, 191, 969–974. [Google Scholar] [CrossRef]
- Wang, F.; Xu, C.; Reece, E.A.; Li, X.; Wu, Y.; Harman, C.; Yu, J.; Dong, D.; Wang, C.; Yang, P.; et al. Protein kinase C-alpha suppresses autophagy and induces neural tube defects via miR-129-2 in diabetic pregnancy. Nat. Commun. 2017, 8, 15182. [Google Scholar] [CrossRef] [PubMed]
- Yang, X.; Borg, L.A.; Eriksson, U.J. Altered mitochondrial morphology of rat embryos in diabetic pregnancy. Anat. Rec. 1995, 241, 255–267. [Google Scholar] [CrossRef] [PubMed]
- Yang, X.; Borg, L.A.; Eriksson, U.J. Altered metabolism and superoxide generation in neural tissue of rat embryos exposed to high glucose. Am. J. Physil. 1997, 272, E173–E180. [Google Scholar] [CrossRef] [PubMed]
- Li, X.; Weng, H.; Xu, C.; Reece, E.A.; Yang, P. Oxidative stress-induced JNK1/2 activation triggers proapoptotic signaling and apoptosis that leads to diabetic embryopathy. Diabetes 2012, 61, 2084–2092. [Google Scholar] [CrossRef] [PubMed]
- Lu, X.; Wu, F.; Jiang, M.; Sun, X.; Tian, G. Curcumin ameliorates gestational diabetes in mice partly through activating AMPK. Pharm. Biol. 2019, 57, 250–254. [Google Scholar] [CrossRef]
- Wu, Y.; Wang, F.; Reece, E.A.; Yang, P. Curcumin ameliorates high glucose-induced neural tube defects by suppressing cellular stress and apoptosis. Am. J. Obstet. Gynecol. 2015, 212, 802.e1-8. [Google Scholar] [CrossRef]
- Abell, S.K.; De Courten, B.; Boyle, J.A.; Teede, H.J. Inflammatory and Other Biomarkers: Role in Pathophysiology and Prediction of Gestational Diabetes Mellitus. Int. J. Mol. Sci. 2015, 16, 13442–13473. [Google Scholar] [CrossRef]
- Kirwan, J.P.; Hauguel-De Mouzon, S.; Lepercq, J.; Challier, J.C.; Huston-Presley, L.; Friedman, J.E.; Kalhan, S.C.; Catalano, P.M. TNF-alpha is a predictor of insulin resistance in human pregnancy. Diabetes 2002, 51, 2207–2213. [Google Scholar] [CrossRef]
- Kautzky-Willer, A.; Fasching, P.; Jilma, B.; Waldhausl, W.; Wagner, O.F. Persistent elevation and metabolic dependence of circulating E-selectin after delivery in women with gestational diabetes mellitus. J. Clin. Endocrinol. Metab. 1997, 82, 4117–4121. [Google Scholar] [CrossRef]
- Krauss, T.; Emons, G.; Kuhn, W.; Augustin, H.G. Predictive value of routine circulating soluble endothelial cell adhesion molecule measurements during pregnancy. Clin. Chem. 2002, 48, 1418–1425. [Google Scholar] [CrossRef]
- Mrizak, I.; Arfa, A.; Fekih, M.; Debbabi, H.; Bouslema, A.; Boumaiza, I.; Zaouali, M.; Khan, N.A.; Tabka, Z. Inflammation and impaired endothelium-dependant vasodilatation in non obese women with gestational diabetes mellitus: Preliminary results. Lipids Health Dis. 2013, 12, 93. [Google Scholar] [CrossRef] [PubMed]
- Kadam, S.; Kanitkar, M.; Dixit, K.; Deshpande, R.; Seshadri, V.; Kale, V. Curcumin reverses diabetes-induced endothelial progenitor cell dysfunction by enhancing MnSOD expression and activity in vitro and in vivo. J. Tissue Eng. Regen. Med. 2018, 12, 1594–1607. [Google Scholar] [CrossRef] [PubMed]
- Almenara, C.C.P.; Oliveira, T.F.; Padilha, A.S. The Role of Antioxidants on the Prevention of Cadmium-Induced Endothelial Dysfunction. Curr. Pharm. Des. 2020. [Google Scholar] [CrossRef] [PubMed]
- Lan, C.; Chen, X.; Zhang, Y.; Wang, W.; Wang, W.E.; Liu, Y.; Cai, Y.; Ren, H.; Zheng, S.; Zhou, L.; et al. Curcumin prevents strokes in stroke-prone spontaneously hypertensive rats by improving vascular endothelial function. BMC Cardiovasc. Disord. 2018, 18, 43. [Google Scholar] [CrossRef]
- Karimian, M.S.; Pirro, M.; Johnston, T.P.; Majeed, M.; Sahebkar, A. Curcumin and Endothelial Function: Evidence and Mechanisms of Protective Effects. Curr. Pharm. Des. 2017, 23, 2462–2473. [Google Scholar] [CrossRef]
- Campbell, M.S.; Fleenor, B.S. The emerging role of curcumin for improving vascular dysfunction: A review. Crit. Rev. Food Sci. Nutr. 2018, 58, 2790–2799. [Google Scholar] [CrossRef]
- Koren, R.; Hochman, Y.; Koren, S.; Ziv-Baran, T.; Wiener, Y. Insulin treatment of patients with gestational diabetes: Does dosage play a role? J. Matern. Fetal Neonatal. Med. 2020, 1–7. [Google Scholar] [CrossRef]
- Burton, G.J.; Redman, C.W.; Roberts, J.M.; Moffett, A. Pre-eclampsia: Pathophysiology and clinical implications. BMJ 2019, 366, l2381. [Google Scholar] [CrossRef]
- Steegers, E.A.; von Dadelszen, P.; Duvekot, J.J.; Pijnenborg, R. Pre-eclampsia. Lancet 2010, 376, 631–644. [Google Scholar] [CrossRef]
- Mittal, M.; Siddiqui, M.R.; Tran, K.; Reddy, S.P.; Malik, A.B. Reactive oxygen species in inflammation and tissue injury. Antioxid. Redox Signal. 2014, 20, 1126–1167. [Google Scholar] [CrossRef]
- Torres-Cuevas, I.; Parra-Llorca, A.; Sanchez-Illana, A.; Nunez-Ramiro, A.; Kuligowski, J.; Chafer-Pericas, C.; Cernada, M.; Escobar, J.; Vento, M. Oxygen and oxidative stress in the perinatal period. Redox Biol. 2017, 12, 674–681. [Google Scholar] [CrossRef] [PubMed]
- Taysi, S.; Tascan, A.S.; Ugur, M.G.; Demir, M. Radicals, Oxidative/Nitrosative Stress and Preeclampsia. Mini Rev. Med. Chem. 2019, 19, 178–193. [Google Scholar] [CrossRef] [PubMed]
- Sies, H.; Berndt, C.; Jones, D.P. Oxidative Stress. Annu. Rev. Biochem. 2017, 86, 715–748. [Google Scholar] [CrossRef] [PubMed]
- Qi, L.; Jiang, J.; Zhang, J.; Zhang, L.; Wang, T. Curcumin Protects Human Trophoblast HTR8/SVneo Cells from H2O2-Induced Oxidative Stress by Activating Nrf2 Signaling Pathway. Antioxidants 2020, 9, 121. [Google Scholar] [CrossRef] [PubMed]
- Pratt, A.; Da Silva Costa, F.; Borg, A.J.; Kalionis, B.; Keogh, R.; Murthi, P. Placenta-derived angiogenic proteins and their contribution to the pathogenesis of preeclampsia. Angiogenesis 2015, 18, 115–123. [Google Scholar] [CrossRef]
- Szpera-Gozdziewicz, A.; Breborowicz, G.H. Endothelial dysfunction in the pathogenesis of pre-eclampsia. Front. Biosci. (Landmark Ed.) 2014, 19, 734–746. [Google Scholar] [CrossRef]
- Maynard, S.; Epstein, F.H.; Karumanchi, S.A. Preeclampsia and angiogenic imbalance. Annu. Rev. Med. 2008, 59, 61–78. [Google Scholar] [CrossRef]
- Carosella, E.D.; Gregori, S.; Rouas-Freiss, N.; LeMaoult, J.; Menier, C.; Favier, B. The role of HLA-G in immunity and hematopoiesis. Cell Mol. Life Sci. 2011, 68, 353–368. [Google Scholar] [CrossRef]
- Garcia, M.; Palma, M.B.; Verine, J.; Miriuka, S.; Inda, A.M.; Errecalde, A.L.; Desgrandchamps, F.; Carosella, E.D.; Tronik-Le Roux, D. The immune-checkpoint HLA-G/ILT4 is involved in the regulation of VEGF expression in clear cell renal cell carcinoma. BMC Cancer 2020, 20, 624. [Google Scholar] [CrossRef]
- Li, X.; Zhou, B.; Han, X.; Liu, H. Effect of nicotine on placental inflammation and apoptosis in preeclampsia-like model. Life Sci. 2020, 261, 118314. [Google Scholar] [CrossRef]
- Cotechini, T.; Komisarenko, M.; Sperou, A.; Macdonald-Goodfellow, S.; Adams, M.A.; Graham, C.H. Inflammation in rat pregnancy inhibits spiral artery remodeling leading to fetal growth restriction and features of preeclampsia. J. Exp. Med. 2014, 211, 165–179. [Google Scholar]
- Xue, P.; Zheng, M.; Gong, P.; Lin, C.; Zhou, J.; Li, Y.; Shen, L.; Diao, Z.; Yan, G.; Sun, H.; et al. Single administration of ultra-low-dose lipopolysaccharide in rat early pregnancy induces TLR4 activation in the placenta contributing to preeclampsia. PLoS ONE 2015, 10, e0124001. [Google Scholar]
- Shalini, V.; Pushpan, C.K.; Sindhu, G.; Jayalekshmy, A.; Helen, A. Tricin, flavonoid from Njavara reduces inflammatory responses in hPBMCs by modulating the p38MAPK and PI3K/Akt pathways and prevents inflammation associated endothelial dysfunction in HUVECs. Immunobiology 2016, 221, 137–144. [Google Scholar]
- Zhou, J.; Miao, H.; Li, X.; Hu, Y.; Sun, H.; Hou, Y. Curcumin inhibits placental inflammation to ameliorate LPS-induced adverse pregnancy outcomes in mice via upregulation of phosphorylated Akt. Inflamm. Res. 2017, 66, 177–185. [Google Scholar] [PubMed]
- Gong, P.; Liu, M.; Hong, G.; Li, Y.; Xue, P.; Zheng, M.; Wu, M.; Shen, L.; Yang, M.; Diao, Z.; et al. Curcumin improves LPS-induced preeclampsia-like phenotype in rat by inhibiting the TLR4 signaling pathway. Placenta 2016, 41, 45–52. [Google Scholar] [PubMed]
- Kim, Y.M.; Romero, R.; Oh, S.Y.; Kim, C.J.; Kilburn, B.A.; Armant, D.R.; Nien, J.K.; Gomez, R.; Mazor, M.; Saito, S.; et al. Toll-like receptor 4: A potential link between “danger signals” the innate immune system, and preeclampsia? Am. J. Obstet. Gynecol. 2005, 193, 921–927. [Google Scholar] [PubMed]
- Youn, H.S.; Saitoh, S.I.; Miyake, K.; Hwang, D.H. Inhibition of homodimerization of Toll-like receptor 4 by curcumin. Biochem. Pharmacol. 2006, 72, 62–69. [Google Scholar] [PubMed]
- Wang, B.; Xu, S.; Lu, X.; Ma, L.; Gao, L.; Zhang, S.Y.; Li, R.; Fu, L.; Wang, H.; Sun, G.P.; et al. Reactive oxygen species-mediated cellular genotoxic stress is involved in 1-nitropyrene-induced trophoblast cycle arrest and fetal growth restriction. Environ. Pollut. 2020, 260, 113984. [Google Scholar]
- Qi, L.; Jiang, J.; Zhang, J.; Zhang, L.; Wang, T. Maternal curcumin supplementation ameliorates placental function and fetal growth in mice with intrauterine growth retardationdagger. Biol. Reprod. 2020, 102, 1090–1101. [Google Scholar]
- Jaiswal, A.K. Nrf2 signaling in coordinated activation of antioxidant gene expression. Free Radic. Biol. Med. 2004, 36, 1199–1207. [Google Scholar]
- Yan, E.; Zhang, J.; Han, H.; Wu, J.; Gan, Z.; Wei, C.; Zhang, L.; Wang, C.; Wang, T. Curcumin Alleviates IUGR Jejunum Damage by Increasing Antioxidant Capacity through Nrf2/Keap1 Pathway in Growing Pigs. Animals 2019, 10, 41. [Google Scholar] [CrossRef]
- Niu, Y.; He, J.; Ahmad, H.; Shen, M.; Zhao, Y.; Gan, Z.; Zhang, L.; Zhong, X.; Wang, C.; Wang, T. Dietary Curcumin Supplementation Increases Antioxidant Capacity, Upregulates Nrf2 and Hmox1 Levels in the Liver of Piglet Model with Intrauterine Growth Retardation. Nutrients 2019, 11, 2978. [Google Scholar] [CrossRef]
- He, J.; Niu, Y.; Wang, F.; Wang, C.; Cui, T.; Bai, K.; Zhang, J.; Zhong, X.; Zhang, L.; Wang, T. Dietary curcumin supplementation attenuates inflammation, hepatic injury and oxidative damage in a rat model of intra-uterine growth retardation. Br. J. Nutr. 2018, 120, 537–548. [Google Scholar] [CrossRef]
- Niu, Y.; He, J.; Ahmad, H.; Wang, C.; Zhong, X.; Zhang, L.; Cui, T.; Zhang, J.; Wang, T. Curcumin attenuates insulin resistance and hepatic lipid accumulation in a rat model of intra-uterine growth restriction through insulin signalling pathway and sterol regulatory element binding proteins. Br. J. Nutr. 2019, 122, 616–624. [Google Scholar] [CrossRef]
- Da Fonseca, E.B.; Damiao, R.; Moreira, D.A. Preterm birth prevention. Best Pract. Res. Clin. Obstet. Gynaecol. 2020. [Google Scholar] [CrossRef]
- Challis, J.R.; Lye, S.J.; Gibb, W. Prostaglandins and parturition. Ann. N. Y. Acad. Sci. 1997, 828, 254–267. [Google Scholar] [CrossRef] [PubMed]
- Guo, Y.Z.; He, P.; Feng, A.M. Effect of curcumin on expressions of NF-kappaBp65, TNF-alpha and IL-8 in placental tissue of premature birth of infected mice. Asian Pac. J. Trop. Med. 2017, 10, 175–178. [Google Scholar] [CrossRef]
- Lim, R.; Barker, G.; Wall, C.A.; Lappas, M. Dietary phytophenols curcumin, naringenin and apigenin reduce infection-induced inflammatory and contractile pathways in human placenta, foetal membranes and myometrium. Mol. Hum. Reprod. 2013, 19, 451–462. [Google Scholar] [CrossRef]
- Prins, J.R.; Gomez-Lopez, N.; Robertson, S.A. Interleukin-6 in pregnancy and gestational disorders. J. Reprod. Immunol. 2012, 95, 1–14. [Google Scholar] [CrossRef]
- Devi, Y.S.; DeVine, M.; DeKuiper, J.; Ferguson, S.; Fazleabas, A.T. Inhibition of IL-6 signaling pathway by curcumin in uterine decidual cells. PLoS ONE 2015, 10, e0125627. [Google Scholar] [CrossRef]
- Cook, J.C.; Jacobson, C.F.; Gao, F.; Tassinari, M.S.; Hurtt, M.E.; DeSesso, J.M. Analysis of the nonsteroidal anti-inflammatory drug literature for potential developmental toxicity in rats and rabbits. Birth Defects Res. B Dev. Reprod. Toxicol. 2003, 68, 5–26. [Google Scholar] [CrossRef]
- Schoenfeld, A.; Bar, Y.; Merlob, P.; Ovadia, Y. NSAIDs: Maternal and fetal considerations. Am. J. Reprod. Immunol. 1992, 28, 141–147. [Google Scholar] [CrossRef]
- Park-Wyllie, L.; Mazzotta, P.; Pastuszak, A.; Moretti, M.E.; Beique, L.; Hunnisett, L.; Friesen, M.H.; Jacobson, S.; Kasapinovic, S.; Chang, D.; et al. Birth defects after maternal exposure to corticosteroids: Prospective cohort study and meta-analysis of epidemiological studies. Teratology 2000, 62, 385–392. [Google Scholar] [CrossRef]
- Dhillon, N.; Aggarwal, B.B.; Newman, R.A.; Wolff, R.A.; Kunnumakkara, A.B.; Abbruzzese, J.L.; Ng, C.S.; Badmaev, V.; Kurzrock, R. Phase II trial of curcumin in patients with advanced pancreatic cancer. Clin. Cancer Res. 2008, 14, 4491–4499. [Google Scholar] [CrossRef]
- Ruiz de Porras, V.; Layos, L.; Martinez-Balibrea, E. Curcumin: A therapeutic strategy for colorectal cancer? Semin. Cancer Biol. 2020. [Google Scholar] [CrossRef]
- Saghatelyan, T.; Tananyan, A.; Janoyan, N.; Tadevosyan, A.; Petrosyan, H.; Hovhannisyan, A.; Hayrapetyan, L.; Arustamyan, M.; Arnhold, J.; Rotmann, A.R.; et al. Efficacy and safety of curcumin in combination with paclitaxel in patients with advanced, metastatic breast cancer: A comparative, randomized, double-blind, placebo-controlled clinical trial. Phytomedicine 2020, 70, 153218. [Google Scholar] [CrossRef]
- Abd Wahab, N.A.; Lajis, N.H.; Abas, F.; Othman, I.; Naidu, R. Mechanism of Anti-Cancer Activity of Curcumin on Androgen-Dependent and Androgen-Independent Prostate Cancer. Nutrients 2020, 12, 679. [Google Scholar] [CrossRef]
- Heshmati, J.; Golab, F.; Morvaridzadeh, M.; Potter, E.; Akbari-Fakhrabadi, M.; Farsi, F.; Tanbakooei, S.; Shidfar, F. The effects of curcumin supplementation on oxidative stress, Sirtuin-1 and peroxisome proliferator activated receptor gamma coactivator 1alpha gene expression in polycystic ovarian syndrome (PCOS) patients: A randomized placebo-controlled clinical trial. Diabetes Metab. Syndr. 2020, 14, 77–82. [Google Scholar] [CrossRef]
- Hashemzadeh, K.; Davoudian, N.; Jaafari, M.R.; Mirfeizi, Z. The Effect of Nanocurcumin in Improvement of Knee Osteoarthritis: A Randomized Clinical Trial. Curr. Rheumatol. Rev. 2020, 16, 158–164. [Google Scholar] [CrossRef]
- Ganjali, S.; Sahebkar, A.; Mahdipour, E.; Jamialahmadi, K.; Torabi, S.; Akhlaghi, S.; Ferns, G.; Parizadeh, S.M.; Ghayour-Mobarhan, M. Investigation of the effects of curcumin on serum cytokines in obese individuals: A randomized controlled trial. Sci. World J. 2014, 2014, 898361. [Google Scholar] [CrossRef]
- Di Pierro, F.; Bressan, A.; Ranaldi, D.; Rapacioli, G.; Giacomelli, L.; Bertuccioli, A. Potential role of bioavailable curcumin in weight loss and omental adipose tissue decrease: Preliminary data of a randomized, controlled trial in overweight people with metabolic syndrome. Preliminary study. Eur. Rev. Med. Pharmacol. Sci. 2015, 19, 4195–4202. [Google Scholar] [PubMed]
- Neerati, P.; Devde, R.; Gangi, A.K. Evaluation of the effect of curcumin capsules on glyburide therapy in patients with type-2 diabetes mellitus. Phytother. Res. 2014, 28, 1796–1800. [Google Scholar] [CrossRef] [PubMed]
- Na, L.X.; Li, Y.; Pan, H.Z.; Zhou, X.L.; Sun, D.J.; Meng, M.; Li, X.X.; Sun, C.H. Curcuminoids exert glucose-lowering effect in type 2 diabetes by decreasing serum free fatty acids: A double-blind, placebo-controlled trial. Mol. Nutr. Food Res. 2013, 57, 1569–1577. [Google Scholar] [CrossRef] [PubMed]
| Curcumin Concentrations | Experimental Models | Outcomes | References |
|---|---|---|---|
| Fertilization and Fetal Development | |||
| 24 μM for 24 h | Mouse blastocyst | Increased ROS, apoptosis and embryo resorption; decreased fetal weight | [51] |
| 24 μM for 24 h | Mouse blastocyst | Increased apoptosis at blastocyst stage or early egg stage and trophoblastic giant cell | [52] |
| 20 μM for 24 h | Mouse blastocyst | Increased apoptosis, p21 and p53; decreased oocyte maturation and fertilization | [53] |
| 1500, 3000 and 10,000 ppm for 70 days | Rat | No gross or microscopic changes in organs: no reproductive parameters changes; small reduction in pre-weaning body weight gain of the F2 pups at 10.000 ppm dose level. | [54] |
| 0.015% of diet | Mouse and Rat | No effects on chromosomes, pregnancy rate, number of live and dead embryos | [55] |
| 31.25–500 µM | Human and mouse spermatozoa | Decreased sperm motility starting from 62.5 µM but decreased capacitation/acrosome reaction at all concentrations tested | [57] |
| 1 nM, 100 nM, 1 mM, 1 M | Human spermatozoa | Increased spermatozoa motility, reduced ROS formation and MDA production at 100 nM; decreased total and progressive motility at 1 mM and 1 M | [56] |
| Protection against Cytotoxic and Teratogenic Agents | |||
| 10 mg/Kg Curcumin ± 60 mg/Kg Retinoic Acid (RA) for 10 days | Mouse | Increased crown rump (CR) length and embryos weight; decreased cell number and sinusoid diameter in the embryonic liver tissue | [44] |
| 250 mg/kg Curcumin (for 1 h) ± 1 mg/kg Aroclor1254 for 28 days | Rat | Decreased 8-(OH)DG, 5-methycytosine and 5-hydroxymethycytosine levels; decreased karyopyknotic nuclei and shrunken or swollen cytoplasm in the migrating neurons | [68] |
| 16 g/Kg Curcumin ± 3 g/L Lead (Pb) for 82 days | Rat | Improved sensory and motor functions in neonatal rats | [73] |
| 75 mg/kg/d Curcumin ± 6 g/kg/d alcohol for 8 days | Mouse | Decreased HAT activity, DHAND; increased H3K14ac, EHAND; inhibited H3K14ac connection with DHAND and EHAND | [75] |
| 25 μM Curcumin ± 200 mM alcohol for 24 h | Cardiac progenitor cells | Decreased H3K9 acetylation and apoptosis reducing cleaved caspase-3 and cleaved caspase-8; increased bcl-2 | [76] |
| 100 mg/kg Curcumin ± 85 ppm Arsenic (As) for 10 days | Mouse | Increased number of EpASCs; decreased chromosomal aberrations; decreased AS accumulation in liver, skin, hair and kidney; decreased Nrf2, NFkB and IkB | [79] |
| 500 nmol/kg Curcumin ± 30 mg/kg Celecoxib for 4 days | Mouse | Increased neurogenesis upregulating GSK-3B and β−Catenin | [84] |
| 150 or 300 ppm Curcumin ± 10 ppm of HgCl2 for 35 days | Mouse | Increased body weight, anticipated hairgrowth and eye opening; increased memory, learning ability, and levels of dopamine, serotonin and acetylcholinesterase in forebrain of pups | [87] |
| 5, 10 and 20 μM (for 1 h) Curcumin ± 200 μM Methylglyoxal (MG) for 3 h | Mouse embryonic stem cells and blastocyst | Decreased DNA fragmentation, caspase-3 activation, cleavage of PARP, JNK activation and apoptosis; decreased ROS production | [46] |
| Viral and Bacterial Infections | |||
| 5 μM for 2 h | HeLa, BHK-21, Vero-E6 cells; CHIKV, VSV, ZIKV viruses | Reduced infectivity of ZIKV and CHIKV viruses by blocking the binding of viruses to cell surface | [88] |
| 0.2, 0.4 and 0.8 µg/mL for 2 days | HELF cells; HCMV virus | Reduced infectivity of HCML by decreasing Hsp90 protein expression | [90] |
| 20 μM for 2 h | HeLa and Vero cells; HSV-1 virus | Reduced HSV-1 infectivity and replication by decreasing ICP4 and ICP27 genes in a p300-independent way | [91] |
| 50 μM for 12 h | HEK-293T, J1.1, TZM-bl cells; HIV-1 virus | Inhibited HIV activity by degrading unfolded Tat protein in a proteasomal dependent way | [92] |
| 0.25 μM for 30 min | Recombinant HIV-1 integrase | Inhibited HIV-1 activity by blocking integrase function | [93] |
| 8 μg/mL for 30 min 200 mg/kg curcumin for 8 h | Mouse; J774 cells; L. Monocytogenes | Inhibited bacterial growth by interfering with the activity of listeriolysin O; protective effects against infection in mice | [94] |
| 150 mg/kg for 14 days | S. agalactiae; silver catfish | Bactericidal action against S. agalactiae; prevented occurrence of clinical signs | [95] |
| 100 μM for 1 h | HeLa cells; Neisseria gonorrhoeae | Interfered with bacterial binding to host cells in late infection; inhibited IkBa degradation and NF-kB activation; reduced TNFa, IL-8 and IL-6 secretion | [96] |
| 40 mg/kg for 2 h | Mouse; LPS | Restored neuronal cell morphology in fetal brain; reduced production of IL-6, Il-1B, COX-2, sICAM-1, sE-selectin, CCL-2, MCP-1 and CINC-1 | [97] |
| Gestational Diabetes | |||
| 100 mg/kg for 10 days | Mouse | Increased glucose tolerance by decreasing TBARS and increasing GSH, SOD and CAT; Enhanced AMPK activation and decreased HDAC4 and G6Pase expression | [105] |
| 20 μM for 24 h | Mouse embryos | Reduced neuronal tube defects and levels of 4-HNE and LPO; blocked ER stress by inhibiting pPERK, pIRE1α, peIF2α, CHOP, BiP and XBP1; reduced cleaved caspase3 and 8 | [106] |
| 10 μM for 1 h | RPEC cells | Reduced glucose‑induced toxicity and TNF‑α, IL‑6 and IL‑1β levels inhibiting AKT and mTOR activation | [45] |
| 7.5 mg/kg/day for 7 days | Endothelial progenitor cells (EPCs) from mouse | Restored tubule formation, and migration of EPCs; improved wound healing; reduced levels and activity of MnSOD. | [112] |
| Preeclampsia (PE) | |||
| 5 µM for 24 h | HTR8/SVneo cell line | Reduced apoptosis by increasing Bcl-2/Bax ratio and decreasing cleaved-caspase 3. Reduced oxidative stress by enhancing CAT and GSH-Px activity, and activating Nrf2. Increased HO-1, NQO1 expression. | [139] |
| 5 µM for 24 h | HTR8/SVneo, JEG3 and HMEC-1 cell lines | Increased cell growth, migration, proliferation and viability by activating AKT; increased tube formation, VEGFR2 HLA-G and FABP4 expression; increased DNMT3A and HSD11B2 expression | [47] |
| 100 µg/kg/d for 17 days | LPS-treated Mouse | Decreased systolic blood pressure, proteinuria, IL-6, IL-1B, TNFa, MCP-1 and MIP-1; increased live pups, fetal and placental weight; Decreased macrophages in placenta. | [134] |
| 360 µg/kg for 14 days | LPS-treated Rat | Decreased systolic blood pressure and proteinuria; improved trophoblast invasion and spiral artery remodeling; decreased TLR4, NF-κB, IL-6 and MCP-1 expressions | [135] |
| Fetal Growth Restriction (FGR) | |||
| 400 mg/kg/d for 18 days | Mouse | Decreased placental apoptosis; increased blood sinusoids area, CAT and GSH-Px in placenta; increased Nef2, HO-1, SOD2, CAT, NQO1 and GSH-Px in fetal liver | [139] |
| 400 mg/kg for 24 days | Pig | Decreased TNF-α, IL-1β and IL-6 serum levels; increased body weight; reduced insulin, glucose, and HOMA-IR levels by downregulating Irs1, Pik3c3, and Gsk3a | [30] |
| 200 mg/kg for 90 days | Pig | Increased Nrf2, SOD1, GCLC, GCLM, NQO1; decreased levels of TNFα, IL-6, IFNγ and caspase3, bax, bcl2, hsp70 mRNA expression. | [141] |
| 400 mg/kg for 24 days | Pig | Increased body-weight gain and Nrf2 and Hmox1 proteins in the liver of FGR piglets | [142] |
| 400 mg/kg for 6 weeks | Rat | Decreased TNF-α, IL-1β, IL-6, AST and ALT in the serum; decreased pNF-κB, pJAK2 and increased mRNA expression of genes of the Nfe2l2/ARE pathway in the liver. | [143] |
| 400 mg/kg for 6 weeks | Rat | Decreased insulin, glucose, HOMA-IR, pyruvate, TAG, total cholesterol and NEFA in the liver; decreased pIRS1, pAKT, pGSK-3, FASN and SREBP-1 in liver. | [144] |
| Preterm Birth | |||
| 100 mg/kg for 24 h | Mouse | Decreased NF-kBp65, TNFa and IL-8 in placental tissue; decreased serum levels of IL-8, SOD and MDA; increased live birth rate. | [147] |
| 30 and 60 µM for 24 h | Placental explants, Primary amnion cells and Myometrial cells | Decreased IL-6, IL-8, MMP-9, COX-2, PGE2 and PGF2a; decreased 8-Isoprostane and NF-kB/DNA binding. | [148] |
| 5, 10, 20, 30 and 40 µM for 1, 2 and 24 h | HuF and UIII cells | Decreased IL-6, gp130, pSTAT3, p50 and p65 expression | [150] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Tossetta, G.; Fantone, S.; Giannubilo, S.R.; Marzioni, D. The Multifaced Actions of Curcumin in Pregnancy Outcome. Antioxidants 2021, 10, 126. https://doi.org/10.3390/antiox10010126
Tossetta G, Fantone S, Giannubilo SR, Marzioni D. The Multifaced Actions of Curcumin in Pregnancy Outcome. Antioxidants. 2021; 10(1):126. https://doi.org/10.3390/antiox10010126
Chicago/Turabian StyleTossetta, Giovanni, Sonia Fantone, Stefano Raffaele Giannubilo, and Daniela Marzioni. 2021. "The Multifaced Actions of Curcumin in Pregnancy Outcome" Antioxidants 10, no. 1: 126. https://doi.org/10.3390/antiox10010126
APA StyleTossetta, G., Fantone, S., Giannubilo, S. R., & Marzioni, D. (2021). The Multifaced Actions of Curcumin in Pregnancy Outcome. Antioxidants, 10(1), 126. https://doi.org/10.3390/antiox10010126







