ADL-Focused Occupation-Based Neurobehavioral Evaluation Software: Addition of a Rasch-Based Stroke Subscale to Measure Outcomes
Abstract
1. Introduction
- Can an internally valid CVA scale be constructed and added to the A-ONE software?
- Does the newly developed A-ONE CVA software scale have external validity?
- Can the ADL and CVA scales of the A-ONE software be used to statistically significantly measure outcomes of an intervention program for stroke patients?
- Does the frequency of detecting statistically significant differences in the ADL and the CVA scales differ?
2. Materials and Methods
2.1. Participants
2.1.1. Internal Validation of a CVA Subscale
2.1.2. External Validation
2.1.3. Intervention Program
2.1.4. Outcomes Study
2.2. Instrument
2.3. Statistical Analyses
2.3.1. Construction of an NBI CVA Software Subscale and Internal Validation
2.3.2. A-ONE Software Construction
2.3.3. External Validity of the A-ONE CVA Software Subscale
2.3.4. Examination of the Intervention Program
2.3.5. Exploring the Significance of Outcome Measures Based on the A-ONE Software Scales
3. Results
3.1. Internal Validity
3.2. The A-ONE Software and External Validity of the CVA Subscale
3.3. Intervention Study
3.4. Outcome Study
4. Discussion
4.1. Construction of an Internally Valid Rasch-Based A-ONE NBI CVA Subscale
4.2. Incorporation of a Renewed CVA Scale into the A-ONE Software
4.3. Content of the Intervention Program
4.4. A-ONE Software Detection of Improved ADL Performance and Diminished Impact of Impairments on Performance
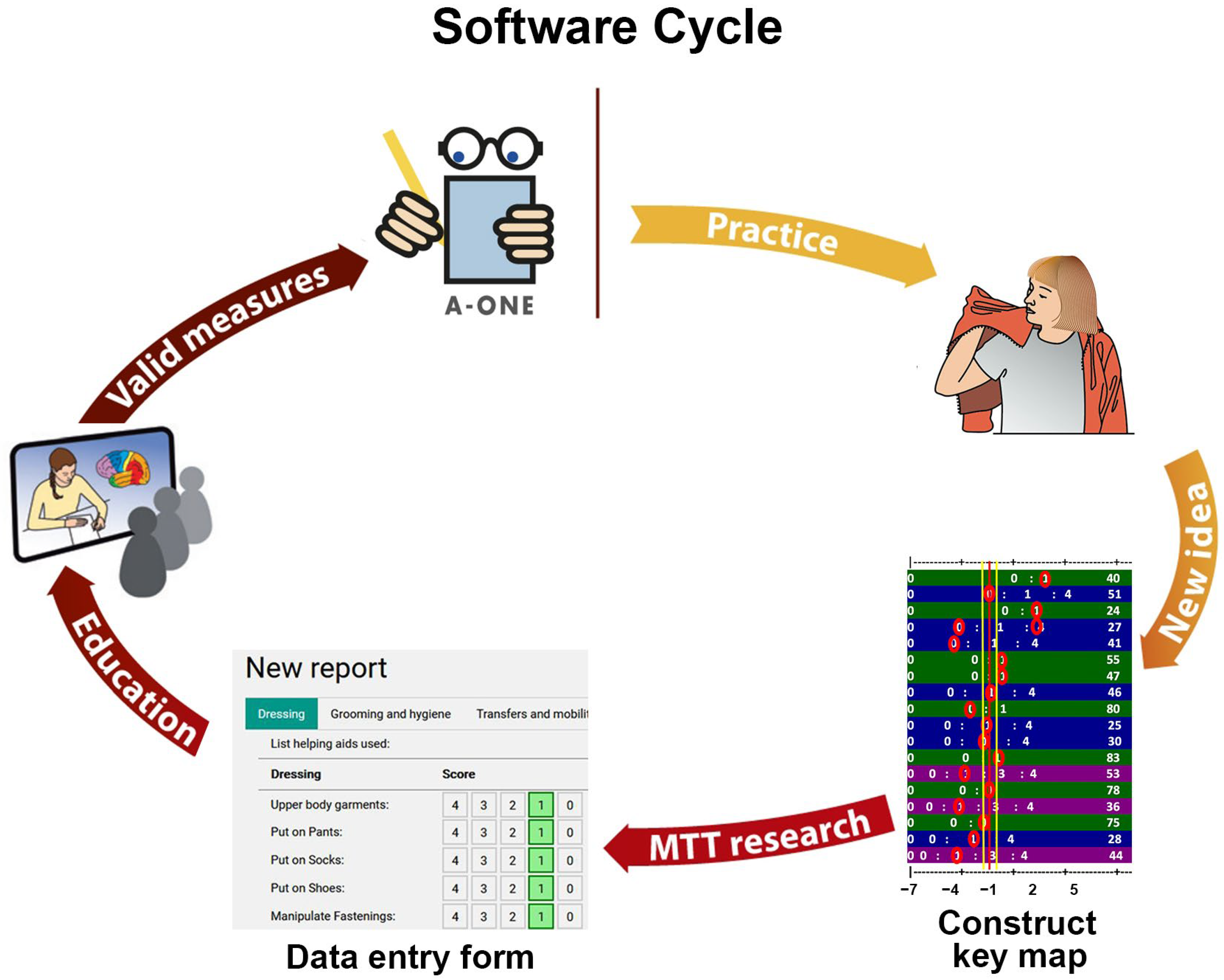
4.5. New Cycle of A-ONE Development
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| ADL | Activities of daily living |
| ALL-DIA | All Diagnoses subscale |
| A-ONE | ADL-focused Occupation-based Neurobehavioral Evaluation |
| CTT | Classical Test Theory |
| CVA | Cerebrovascular Accident |
| FI | Functional Independence |
| FIM | Functional Independence Measure |
| G | Separation Index |
| LCVA | Left Cerebrovascular Accident |
| MnSq | Mean Square |
| MSE | Mean Standard Error |
| MTT | Modern Test Theory |
| NB | Neurobehavior |
| NBI | Neurobehavioral impact |
| NBPIS | Neurobehavioral Pervasive Impairment Subscale |
| NBSIS | Neurobehavioral Specific Impairment Subscale |
| PCA | Principal Components Analysis |
| R | Reliability Coefficient |
| RCVA | Right Cerebrovascular Accident |
References
- National Institute of Neurological Disorders and Stroke (NINDS). Stroke Information Page. Available online: https://www.cdc.gov/stroke/data-research/facts-stats/ (accessed on 19 June 2025).
- Ghaziani, E.; Christensen, S.S.; Arens, C.H.; Wæhrens, E.E. Addressing ADL ability in people with poststroke cognitive impairments: A Danish survey of clinical practice. Scand. J. Occup. Ther. 2024, 31, 2318204. [Google Scholar] [CrossRef]
- Feigin, V.L.; Brainin, M.; Norrving, B.; Martins, S.O.; Pandian, J.; Lindsay, P.; Grupper, M.F.; Rautalin, I. World Stroke Organization: Global stroke fact sheet. Int. J. Stroke 2025, 20, 132–144. [Google Scholar] [CrossRef]
- Árnadóttir, G. Impact of neurobehavioral deficits on activities of daily living. In Stroke Rehabilitation: A Function-Based Approach, 5th ed.; Gillen, G., Nilsen, D.M., Eds.; Elsevier: Philadelphia, PA, USA, 2021; pp. 556–592. [Google Scholar]
- Árnadóttir, G. The Brain and Behavior: Assessing Cortical Dysfunction Through Activities of Daily Living; The C.V. Mosby: St. Louis, MO, USA, 1990. [Google Scholar]
- Árnadóttir, G. Measuring the Impact of Body Functions on Occupational Performance: Validation of the ADL-Focused Occupation-Based Neurobehavioral Evaluation (A-ONE). Ph.D. Thesis, Department of Community Medicine and Rehabilitation/Occupational Therapy, Umeå University, Umeå, Sweden, 2010. [Google Scholar]
- Llorens, L.A. Activity analysis: Agreement among factors in a sensory processing model. Am. J. Occup. Ther. 1986, 40, 103–110. [Google Scholar] [CrossRef]
- Árnadóttir, G. Contributing to an integrated profession: A model-based examination of the A-ONE. Scand. J. Occup. Ther. 2017, 24, 98–108. [Google Scholar] [CrossRef] [PubMed]
- Gillen, G. A fork in the road: An occupational hazard? (Eleanor Clarke Slagle Lecture). Am. J. Occup. Ther. 2013, 67, 641–652. [Google Scholar] [CrossRef] [PubMed]
- Gillen, G. ADL-focused Occupation-based Neurobehavioral Evaluation: The A-ONE. In Functional Cognition and Occupational Therapy: A Practical Approach to Treating Individuals with Cognitive Loss; Wolf, T.J., Edwards, D.F., Giles, G.M., Eds.; AOTA Press: Bethesda, MD, USA, 2019; pp. 131–139. [Google Scholar]
- Gillen, G. Cerebrovascular accident (stroke). In Pedretti‘s Occupational Therapy: Practice Skills for Physical Dysfunction, 8th ed.; McHugh Pendleton, H., Schultz-Krohn, W., Eds.; Elsevier: Philadelphia, PA, USA, 2018; pp. 1471–1525. [Google Scholar]
- Bond, T.G.; Yan, Z.; Heene, M. Applying the Rasch Model: Fundamental Measurement in the Human Sciences, 4th ed.; Routledge, Taylor and Francis Group: New York, NY, USA, 2021. [Google Scholar]
- Merbitz, C.; Morris, J.; Grip, J.C. Ordinal scales and foundations of misinference. Arch. Phys. Med. Rehabil. 1989, 70, 308–312. [Google Scholar] [PubMed]
- Árnadóttir, G.; Fisher, A.G. Rasch analysis of the ADL scale of the A-ONE. Am. J. Occup. Ther. 2008, 62, 51–60. [Google Scholar] [CrossRef]
- Árnadóttir, G.; Löfgren, B.; Fisher, A.G. Neurobehavioral functions evaluated in naturalistic contexts: Rasch analysis of the A-ONE Neurobehavioral Impact Scale. Scand. J. Occup. Ther. 2012, 19, 439–449. [Google Scholar] [CrossRef]
- Linacre, J.M. Instantaneous measurement and diagnosis. Phys. Med. Rehabil. 1997, 11, 315–324. [Google Scholar]
- Kielhofner, G.; Dobria, L.; Forsyth, K.; Basu, S. The construction of keyforms for obtaining instantaneous measures from the occupational performance history interview rating scales. OTJR Occup. Particip. Health 2005, 25, 23–32. [Google Scholar] [CrossRef]
- Bode, R.K.; Heinemann, A.W.; Kozlowski, A.J.; Pretz, C.R. Self-scoring templates for Motor and Cognitive subscales of the FIM instrument for persons with spinal cord injury. Arch. Phys. Med. Rehabil. 2014, 95, 676–679. [Google Scholar] [CrossRef]
- Grattan, E.S.; Velozo, C.A.; Skidmore, E.R.; Page, S.J.; Woodbury, M.L. Interpreting action research arm test assessment scores to plan treatment. OTJR Occup. Particip. Health 2019, 39, 64–73. [Google Scholar] [CrossRef]
- Jette, D.U.; Halbert, J.; Iverson, C.; Miceli, E.; Shah, P. Use of standardized outcome measures in physical therapist practice: Perceptions and applications. Phys. Ther. 2009, 89, 125–135. [Google Scholar] [CrossRef] [PubMed]
- Velozo, C.A.; Woodbury, M.L. Translating measurement findings into rehabilitation practice: An example using Fugl-Meyer Assessment-Upper Extremity with patients following stroke. J. Rehabil. Res. Dev. 2011, 48, 1211–1222. [Google Scholar] [CrossRef]
- Woodbury, M.L.; Anderson, K.; Finetto, C.; Fortune, A.; Dellenbach, B.; Grattan, E.; Hutchison, S. Matching task-difficulty to patient-ability during task practice improves upper extremity motor skill after stroke: A proof of concept study. Arch. Phys. Med. Rehabil. 2016, 97, 1863–1871. [Google Scholar] [CrossRef]
- Miyata, K.; Tamura, S.; Kobayashi, S.; Takeda, R.; Iwamoto, H. Berg balance scale is a valid measure for plan interventions and for assessing changes in postural balance in patients with stroke. J. Rehabil. Med. 2022, 54, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Árnadóttir, G.; Sigtryggsson, H.; Ingvarsson, G. Kynning á nýjum hugbúnaði fyrir iðjuþjálfa (Introduction to a new software for occupational therapists). Iðjuþjálfinn (Occup. Ther.) 2023, 44, 22–27. Available online: https://www.ii.is/media/idjuthjalfinn/Idjuthalfinn_2023.pdf (accessed on 14 December 2023).
- Yerxa, E.J. In search of good ideas for occupational therapy. Scand. J. Occup. Ther. 1994, 1, 7–15. [Google Scholar] [CrossRef]
- Fisher, A.G. Occupation-centred, occupation-based, occupation-focused: Same, same or different? Scand. J. Occup. Ther. 2013, 20, 162–173. [Google Scholar] [CrossRef]
- Fisher, A.G.; Marterella, A. Powerful Practice: A Model for Authentic Occupational Therapy; Center for Innovative OT Solutions: Fort Collins, CO, USA, 2019. [Google Scholar]
- Azouvi, P.; Olivier, S.; Montety, G.; Samuel, C.; Louis-Dreyfus, A.; Tesio, L. Behavioral assessment of unilateral neglect: Study of the psychometric properties of the Catherine Bergego Scale. Arch. Phys. Med. Rehabil. 2003, 84, 51–57. [Google Scholar] [CrossRef]
- Grattan, E.S.; Smith, B.H.; Mullen, K.; Woodbury, M.L. Unilateral spatial neglect may not be detected by performance-based functional neglect assessment. Am. J. Occup. Ther. 2024, 78, 7802180200. [Google Scholar] [CrossRef]
- Grattan, E.S.; Woodbury, M.L. Do neglect assessments detect neglect differently? Am. J. Occup. Ther. 2017, 71, 7103190050p1–7103190050p9. [Google Scholar] [CrossRef]
- Tham, K.; Bernspång, B.; Fisher, A.G. Development of Assessment of Awareness of Disability (AAD). Scand. J. Occup. Ther. 1999, 6, 184–190. [Google Scholar]
- Kottorp, A.; Petterson, I. Psychometric evaluation of an assessment of awareness using two different Rasch models. Scand. J. Occup. Ther. 2011, 18, 219–230. [Google Scholar] [CrossRef]
- Baum, C.M.; Edwards, D.F.; Boone, A.E.; Wolf, T.J. The Executive Function Performance Test. In Functional Cognition and Occupational Therapy: A Practical Approach to Treating Individuals with Cognitive Loss; Wolf, T.J., Edwards, D.F., Giles, G.M., Eds.; AOTA Press: Bethesda, MD, USA, 2019; pp. 67–73. [Google Scholar]
- Boone, A.E.; Wolf, T.J. Complex task performance assessment. In Functional Cognition and Occupational Therapy: A Practical Approach to Treating Individuals with Cognitive Loss; Wolf, T.J., Edwards, D.F., Giles, G.M., Eds.; AOTA Press: Bethesda, MD, USA, 2019; pp. 101–106. [Google Scholar]
- Higashi, Y.; Takabatake, S.; Matsubara, A.; Nishikawa, K.; Shigeta, H.; Árnadóttir, G. Reliability and validity of the Japanese version of the ADL-focused Occupation-based Neurobehavioural Evaluation (A-ONE J): Applying Rasch analysis methods. Hong Kong J. Occup. Ther. 2019, 32, 32–40. [Google Scholar] [CrossRef]
- Higashi, Y.; Matsubara, A.; Nishikawa, K.; Nishikawa, T.; Takabatake, S. A pilot study of reliability and validity of the ADL-focused Occupation-based Neurobehavioral Evaluation (A-ONE) in Japan. Jpn. J. Occup. Ther. 2017, 36, 194–203. [Google Scholar]
- Higashi, Y.; Takabatake, S.; Kaneda, T.; Nakaoka, K.; Ishihara, M. Reliability and validity of the Japanese version of the ADL-focused Occupation-based Neurobehavioral Evaluation (A-ONE) through classical test theory. Jpn. J. Occup. Ther. 2021, 40, 214–224. [Google Scholar]
- Kang, J.; Park, H.Y.; Kim, J.R.; Park, J.-H. Cross–cultural adaptation and psychometric evaluation of the Korean version of the A-ONE. Ther. Sci. Rehabil. 2021, 10, 29–128. [Google Scholar] [CrossRef]
- Steultjens, E.M.J. A-ONE; De Nederlandse versie (A-ONE; The Dutch version). Ned. Tidskr. Ergoter. (Dutch Occup. Ther. J.) 1998, 26, 100–104. [Google Scholar]
- Wright, B.D.; Linacre, J.M. Observations are always ordinal; measurements, however, must be interval. Arch. Phys. Med. Rehabil. 1989, 70, 857–860. [Google Scholar]
- Linacre, J.M.; Heinemann, A.W.; Wright, B.D.; Granger, C.V.; Hamilton, B.B. The structure and stability of the Functional Independence Measure. Arch. Phys. Med. Rehabil. 1994, 75, 127–132. [Google Scholar] [CrossRef]
- Lim, S.M.; Rodger, S.; Brown, T. Using Rasch analysis to establish the construct validity of rehabilitation assessment tools. IJTR 2009, 15, 251–260. [Google Scholar] [CrossRef]
- Tesio, L. Measuring behaviours and perceptions: Rasch analysis as a tool for rehabilitation research. J. Rehabil. Med. 2003, 35, 105–115. [Google Scholar] [CrossRef]
- Árnadóttir, G.; Löfgren, B.; Fisher, A. Difference in impact of neurobehavioural dysfunction on activities of daily living performance between right and left hemispheric stroke. J. Rehabil. Med. 2010, 42, 903–907. [Google Scholar] [CrossRef] [PubMed]
- Steultjens, E.M.J.; Dekker, J.; Bouter, L.M.; van de Nes, J.C.M.; Cup, E.H.C.; Van den Ende, C.H.M. Occupational therapy for stroke patients: A systematic review. Stroke 2003, 34, 676–687. [Google Scholar] [CrossRef] [PubMed]
- Wilkins, S.; Jung, B.; Wishart, L.; Edwards, M.; Norton, S.G. The effectiveness of community-based occupational therapy education and functional training programs for older adults: A critical literature review. Can. J. Occup. Ther. 2003, 70, 214–225. [Google Scholar] [CrossRef] [PubMed]
- Legg, L.; Drummond, A.; Leonardi-Bee, J.; Gladman, J.R.F.; Corr, S.; Donkervoort, M.; Edmans, J.; Gilbertson, L.; Jongbloed, L.; Logan, P.; et al. Occupational therapy for patients with problems in personal activities of daily living after stroke: Systematic review of randomised trials. BMJ 2007, 335, 922. [Google Scholar] [CrossRef] [PubMed]
- Wall, G.; Isbel, S.; Gustafsson, L.; Pearce, C. Occupation-based interventions to improve occupational performance and participation in the hospital setting: A systematic review. Disabil. Rehabil. 2023, 46, 2747–2768. [Google Scholar] [CrossRef]
- Linacre, M.J. Sample size and item calibration stability. Rasch Meas.Trans. 1994, 7, 328. [Google Scholar]
- Linacre, J.M. Optimizing rating scale category effectiveness. J. Appl. Meas. 2002, 3, 85–106. [Google Scholar]
- Linacre, J.M. WINSTEPS® Rasch Measurement Computer Software (Version 4.7.0). Available online: www.winsteps.com (accessed on 30 May 2021).
- Smith, R.M. Fit analysis in latent trait measurement models. J. Appl. Meas. 2000, 1, 199–218. [Google Scholar] [PubMed]
- Smith, R. The distributional properties of Rasch item fit statistics. Educ. Psychol. Meas. 1991, 51, 541–565. [Google Scholar] [CrossRef]
- Fisher, A.G. Occupational Therapy Intervention Process Model: A Model for Planning and Implementing Top-Down, Client-Centered, and Occupation-Based Interventions; Three Star Press, Inc.: Fort Collins, CO, USA, 2009. [Google Scholar]
- Árnadóttir, G.; Sverrisdóttir, L.H. Þjónustuyfirlit og klínísk vinna iðjuþjálfa (Service Model and Clinical Work in Occupational Therapy Practice). Iðjuþjálfinn (Occup. Ther.) 2016, 23–30. Available online: https://www.ii.is/media/idjuthjalfinn/idjuthjalfinn_OKT_2016_VEF.pdf (accessed on 14 December 2022).
- Wright, B.D.; Linacre, J.M. Reasonable mean-square fit values. Rasch Meas. Trans. 1994, 8, 370. Available online: www.rasch.org/rmt/rmt83b.htm (accessed on 19 June 2025).
- Fisher, W.P.J. Rating scale instrument quality criteria. Rasch Meas. Trans. 2007, 21, 1095. Available online: https://www.rasch.org/rmt/rmt211m.htm (accessed on 14 December 2022).
- Langhorne, P.; Bernhardt, J.; Kwakkel, G. Stroke rehabilitation. Lancet 2011, 377, 1693–1702. [Google Scholar] [CrossRef]
- Hildebrand, M.W.; Geller, D.; Proffitt, R. Practice guidelines–Occupational therapy practice guidelines for adults with stroke. Am. J. Occup Ther. 2023, 77, 7705397010. [Google Scholar] [CrossRef]
- Geller, D.; Winterbottom, L.; Goldberg, C.; Nilsen, D.M.; Mahoney, D.; Gillen, G. Systematic review briefs─Exercise for adults with stroke to improve ADL and/or functional mobility performance (2012–2019). Am. J. Occup. Ther. 2023, 77 (Suppl. S1), 7710393040. [Google Scholar] [CrossRef]
- Wolf, T.J.; Chuh, A.; Floyd, T.; McInnis, K.; Williams, E. Effectiveness of occupation-based interventions to improve areas of occupation and social participation after stroke: An evidence-based review. Am. J. Occup. Ther. 2015, 69, 6901180060p1–6901180060p11. [Google Scholar] [CrossRef]
- Nilsen, D.M.; Gillen, G.; Geller, D.; Hreha, K.; Osei, E.; Saleem, G.T. Effectiveness of interventions to improve occupational performance of people with motor impairments after stroke: An evidence-based review. Am. J. Occup. Ther. 2015, 69, 6901180030p1–6901180030p9. [Google Scholar] [CrossRef]
- Gibson, E.; Koh, C.; Eames, S.; Bennet, S.; Scott, A.M.; Hoffmann, T.C. Occupational therapy for cognitive impairment in stroke patients. Cochrane Database Syst. Rev. 2022, 3, CD006430. [Google Scholar] [CrossRef]
- Gillen, G.; Nilsen, D.M.; Attridge, J.; Banakos, E.; Morgan, M.; Winterbottom, L.; York, W. Effectiveness of interventions to improve occupational performance of people with cognitive impairments after stroke: An evidence-based review. Am. J. Occup. Ther. 2015, 69, 6901180040p1–6901180040p9. [Google Scholar] [CrossRef]
- Vásquez-Carrasko, E.; Jamett-Olivia, P.; Hernandez-Martinez, J.; Riquelme-Hernándes, C.; Villagrán-Silva, F.; Branco, B.H.M.; Sandoval, C.; Valdés-Badilla, P. Effectivenss of occupational therapy interventions on activities of daily living, cognitive function, and physical function in middle-aged and older people with chronic stroke: A systematic review with Meta analysis. J. Clin. Med. 2025, 14, 2197. [Google Scholar] [CrossRef]
- Wurzinger, H.E.; Abzhandadze, T.; Rafsten, L.; Sunnerhagen, K.S. Dependency in activites of daily living during the first year after stroke. Front. Neurol. 2021, 12, 736684. [Google Scholar] [CrossRef]
- Murdock, C.A. A critical evaluation of the Barthel Index, Part I. Br. J. Occup. Ther. 1992, 55, 109–111. [Google Scholar] [CrossRef]
- Tennant, A.; Geddes, J.M.L.; Chamberlain, M.A. The Barthel Index: An ordinal score or interval level measure? Clin. Rehabil. 1996, 10, 301–308. [Google Scholar] [CrossRef]
- Turunen, K.E.A.; Laari, S.P.K.; Kauranen, T.V.; Uimonen, J.; Mustanoja, S.; Tatlisumak, T.; Poutiainen, E. Domain-specific cognitive recovery after first-ever stroke: A 2-year follow-up. J. Int. Neuropsychol. Soc. 2018, 24, 117–127. [Google Scholar] [CrossRef] [PubMed]


| CVA | Total | ||
|---|---|---|---|
| Left | Right | ||
| Age | |||
| Mean | 67.7 | 65.3 | 66.6 |
| SD | 13.5 | 14.3 | 13.9 |
| Range | 22–89 | 22–91 | 22–91 |
| Gender n (%) | |||
| Male | 74 (55.6%) | 59 (44.4%) | 133 (59.9%) |
| Female | 40 (44.9%) | 49 (55.1%) | 89 (40.1%) |
| Total n (%) | 114 (51.4%) | 108 (48.6%) | 222 (100%) |
| Psychometric Test Person/Item Information | Rasch Model | Criteria | Criteria References | |
|---|---|---|---|---|
| Simple | Group | |||
| Number of persons | 222 | 222 | ≥150 | [12,49] |
| Item number | 53 | 49 | ≤53 | |
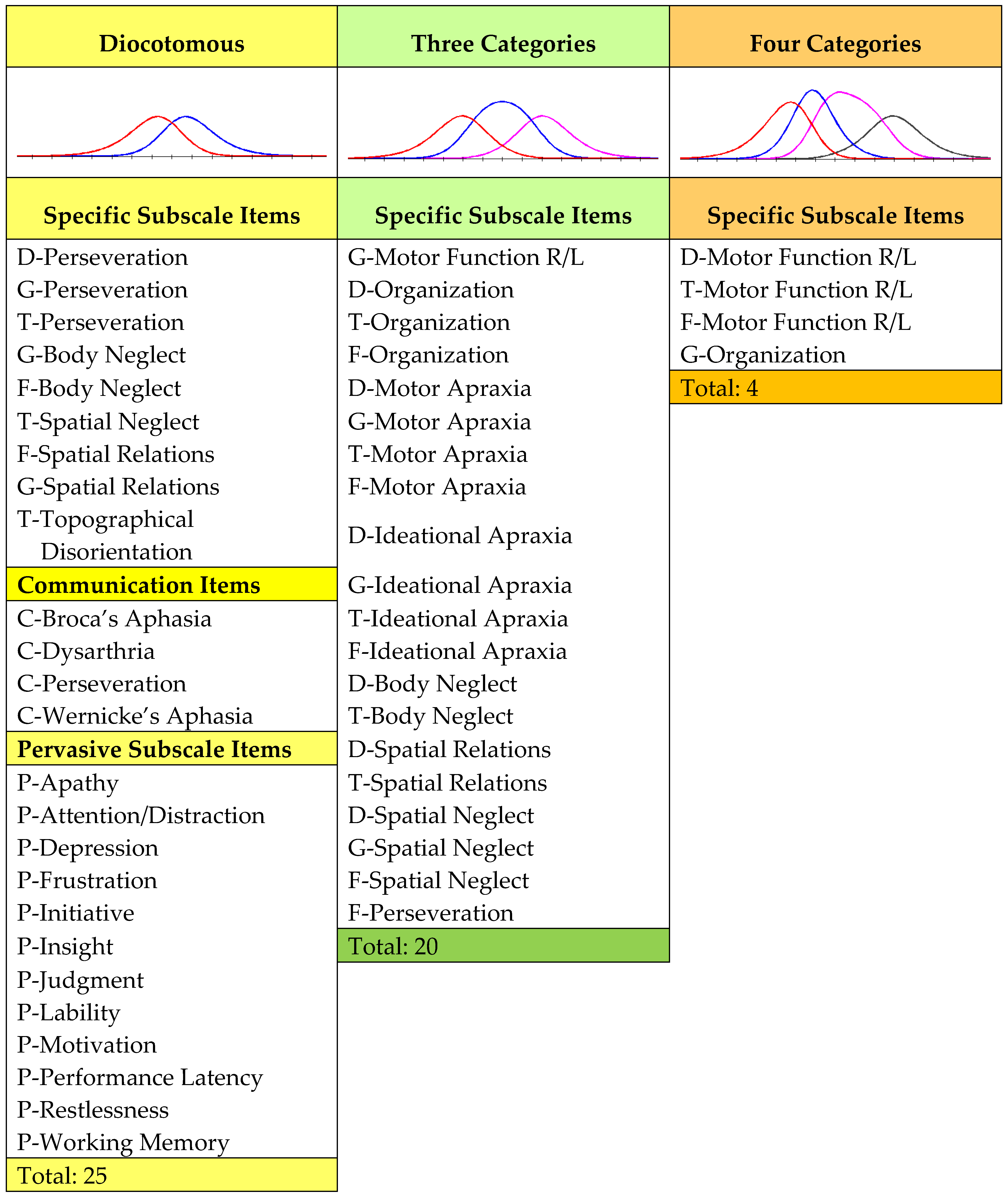
| Number of categories * | 2 | 2, 3, 4 = 9 | >2 | |
| Item Infit Misfit | 0 | 0 | MnSq ≥ 1.4; z > 2 | [12,14,56] |
| Item Outfit Misfit | 1 | 0 | MnSq ≥ 1.4; z > 2 | [12,14,56] |
| PCA: First contrast | 10% | 10% | ≤10% | [57] |
| Person separation | 2.24 | 2.26 | ≥2 | [12,14,56] |
| Person reliability coefficient | 0.83 | 0.84 | ≥0.8 | [57] |
| Item reliability coefficient | 0.98 | 0.97 | ≥0.8 | [57] |
| MSE persons * | 0.47 | 0.40 | ≤0.5 logit | [12] |
| MSE items | 0.24 | 0.20 | ≤0.5 logit | [12] |
| Score range * | 0–53 | 0–77 | >0–55 | |
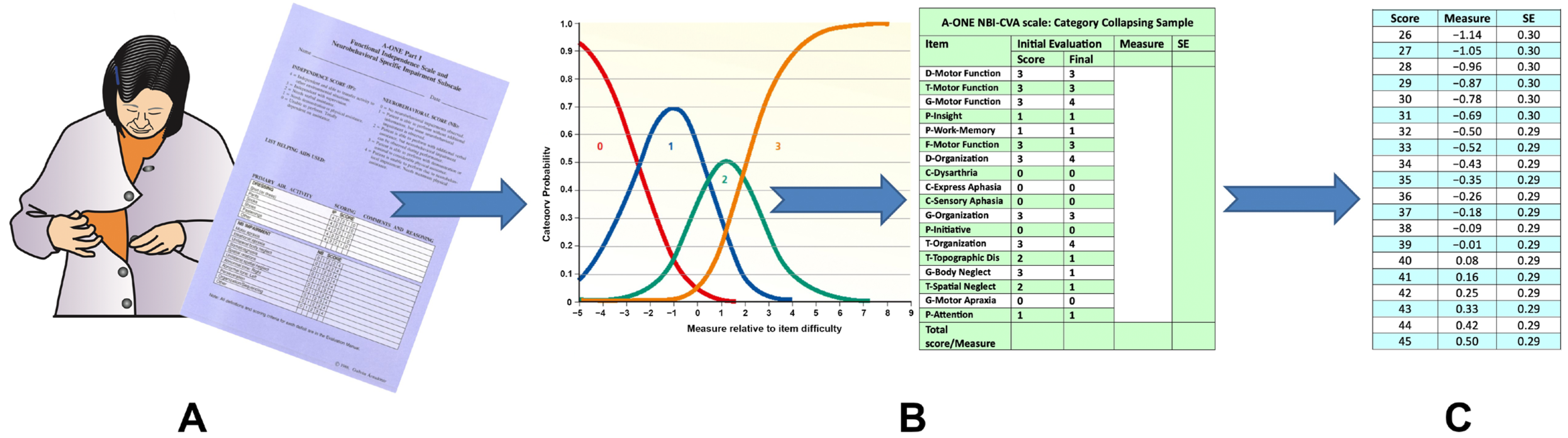
| Measurement Difference of Winsteps and A-ONE Software | ||||||||
|---|---|---|---|---|---|---|---|---|
| Persons | Age | Gender | A-ONE Measure * | A-ONE SE | Winsteps Measure | Winsteps SE | Measure Difference | SE Difference |
| 1-CVA-L | 82 | M | −0.79 | 0.29 | −0.69 | 0.29 | 0.10 | 0.00 |
| 2-CVA-L | 73 | F | −2.97 | 0.40 | −2.94 | 0.39 | 0.03 | 0.01 |
| 3-CVA-L | 72 | M | −2.27 | 0.35 | −2.29 | 0.34 | 0.02 | 0.01 |
| 4-CVA-L | 75 | M | −2.53 | 0.37 | −2.53 | 0.36 | 0.00 | 0.01 |
| 5-CVA-R | 22 | M | −3.50 | 0.45 | −3.45 | 0.44 | 0.05 | 0.01 |
| 6-CVA-R | 62 | M | −2.40 | 0.36 | −2.29 | 0.34 | 0.11 | 0.02 |
| 7-CVA-R | 84 | F | −3.31 | 0.43 | −3.26 | 0.42 | 0.05 | 0.01 |
| 8-CVA-L | 83 | M | −1.32 | 0.31 | −1.22 | 0.30 | 0.10 | 0.01 |
| 9-CVA-R | 73 | M | −1.51 | 0.31 | −1.56 | 0.31 | 0.05 | 0.00 |
| 10-CVA-L | 73 | F | −1.61 | 0.32 | −1.51 | 0.31 | 0.10 | 0.01 |
| 11-CVA-R | 70 | M | −3.72 | 0.48 | −3.66 | 0.47 | 0.06 | 0.01 |
| 12-CVA-R | 80 | F | −0.53 | 0.29 | −0.55 | 0.29 | 0.02 | 0.00 |
| 13-CVA-R | 71 | F | −3.96 | 0.51 | −3.89 | 0.50 | 0.07 | 0.01 |
| 14-CVA-R | 75 | M | −2.04 | 0.34 | −2.06 | 0.33 | 0.02 | 0.01 |
| 15-CVA-R | 72 | M | −2.15 | 0.34 | −2.06 | 0.33 | 0.09 | 0.01 |
| 16-CVA-R | 61 | M | −4.04 | 0.75 | −4.17 | 0.55 | 0.13 | 0.20 |
| 17-CVA-R | 70 | M | −3.13 | 0.41 | −3.10 | 0.40 | 0.03 | 0.01 |
| 18-CVA-R | 70 | M | −2.81 | 0.39 | −2.79 | 0.38 | 0.02 | 0.01 |
| 19-CVA-R | 54 | M | −1.82 | 0.33 | −1.57 | 0.32 | 0.25 | 0.01 |
| 20-CVA-L | 60 | F | −2.53 | 0.37 | −2.53 | 0.36 | 0.00 | 0.01 |
| 21-CVA-L | 78 | F | −1.51 | 0.31 | −1.56 | 0.31 | 0.05 | 0.00 |
| 22-CVA-L | 73 | M | −1.61 | 0.32 | −1.56 | 0.31 | 0.05 | 0.01 |
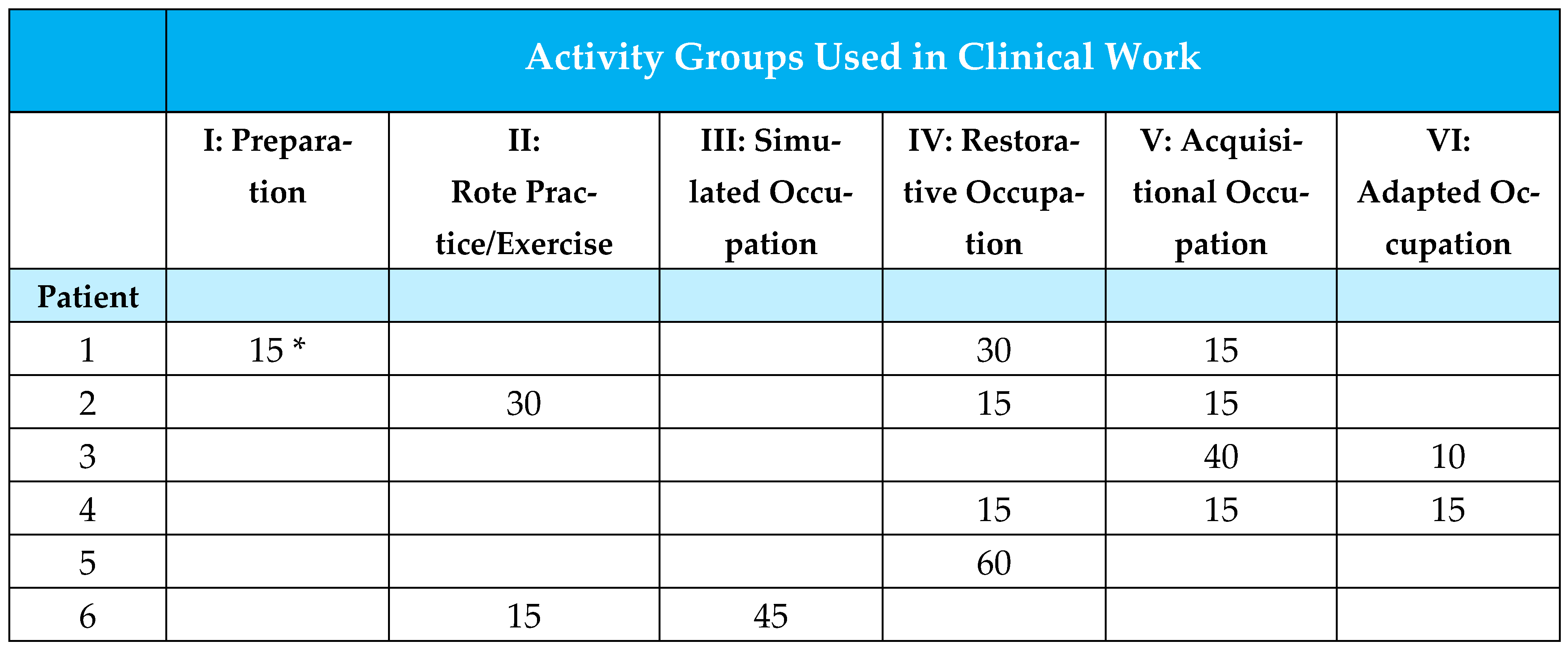
| Activity Groups Used for Intervention | |||||||
|---|---|---|---|---|---|---|---|
| Therapist | Sessions | I | II | III | IV | V | VI |
| 1 | 22 | 0 * | 225 | 470 | 445 | 0 | 30 |
| 2 | 23 | 10 | 35 | 0 | 380 | 295 | 45 |
| 3 | 11 | 0 | 0 | 60 | 140 | 80 | 0 |
| 4 | 9 | 0 | 0 | 235 | 235 | 60 | 0 |
| Total | 65 | 10 | 260 | 600 | 1.200 | 435 | 75 |
| (%) | 0.4% | 10.1% | 23.2% | 46.5% | 16.9% | 2.9% | |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Árnadóttir, G.; Atladóttir, L.H.; Ingvarsson, G.; Sigtryggsson, H.; Atlason, B.Á. ADL-Focused Occupation-Based Neurobehavioral Evaluation Software: Addition of a Rasch-Based Stroke Subscale to Measure Outcomes. Brain Sci. 2025, 15, 904. https://doi.org/10.3390/brainsci15090904
Árnadóttir G, Atladóttir LH, Ingvarsson G, Sigtryggsson H, Atlason BÁ. ADL-Focused Occupation-Based Neurobehavioral Evaluation Software: Addition of a Rasch-Based Stroke Subscale to Measure Outcomes. Brain Sciences. 2025; 15(9):904. https://doi.org/10.3390/brainsci15090904
Chicago/Turabian StyleÁrnadóttir, Guðrún, Laufey Halla Atladóttir, Garðar Ingvarsson, Helgi Sigtryggsson, and Bjarni Ármann Atlason. 2025. "ADL-Focused Occupation-Based Neurobehavioral Evaluation Software: Addition of a Rasch-Based Stroke Subscale to Measure Outcomes" Brain Sciences 15, no. 9: 904. https://doi.org/10.3390/brainsci15090904
APA StyleÁrnadóttir, G., Atladóttir, L. H., Ingvarsson, G., Sigtryggsson, H., & Atlason, B. Á. (2025). ADL-Focused Occupation-Based Neurobehavioral Evaluation Software: Addition of a Rasch-Based Stroke Subscale to Measure Outcomes. Brain Sciences, 15(9), 904. https://doi.org/10.3390/brainsci15090904




