Update on Domestic Violence and Traumatic Brain Injury: A Narrative Review
Abstract
:1. Introduction
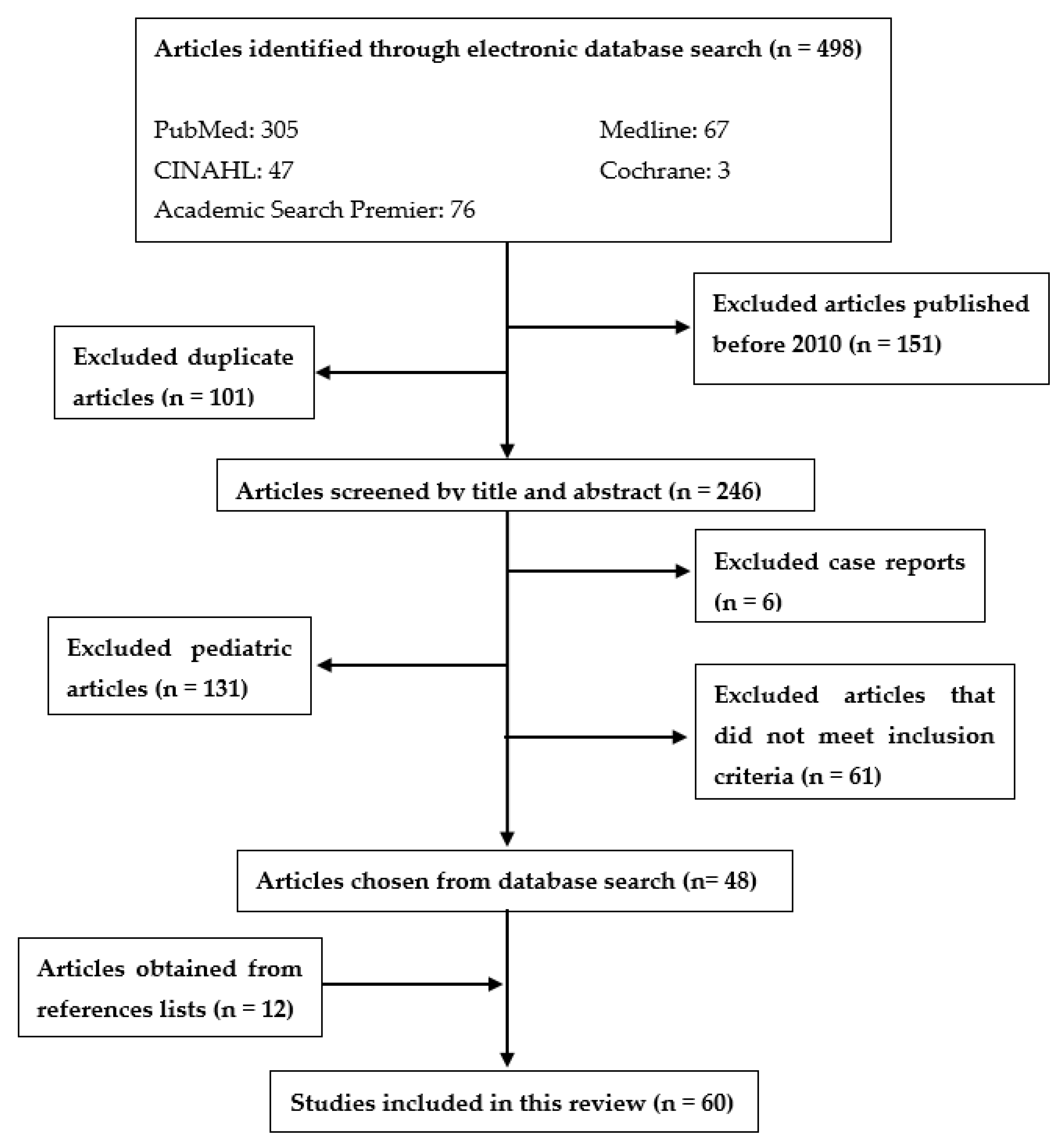
2. Materials and Methods
3. Prevalence and Demographics of TBI Related to Domestic Violence
3.1. Effects of Socioeconomic Status
3.2. Effect of Race
3.3. Veterans
3.4. Domestic Violence in the LGBTQIA+ Communities
3.5. Domestic Violence in the Elderly and Children
4. Diagnosis of TBI Secondary to Domestic Violence
4.1. Common Presenting Symptoms
4.2. Screening Tools
4.3. Neuroimaging Tools
5. Treatment Models
6. Outcomes of TBI Due to Domestic Violence
6.1. PTSD
6.2. Chronic Traumatic Encephalopathy
6.3. Risk to Future Generations
7. Effects of COVID-19 on Domestic Violence
8. Discussion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Trudel, T.M.; Scherer, M.J.; Elias, E. Understanding Traumatic Brain Injury: An Introduction. Except. Parent 2011, 41, 33–37. [Google Scholar]
- Campbell, J.C.; Anderson, J.C.; McFadgion, A.; Gill, J.; Zink, E.; Patch, M.; Callwood, G.; Campbell, D. The Effects of Intimate Partner Violence and Probable Traumatic Brain Injury on Central Nervous System Symptoms. J. Women’s Health 2018, 27, 761–767. [Google Scholar] [CrossRef]
- Murray, C.E.; Lundgren, K.; Olson, L.N.; Hunnicutt, G. Practice Update: What Professionals Who Are Not Brain Injury Specialists Need to Know About Intimate Partner Violence-Related Traumatic Brain Injury. Trauma Violence Abus. 2016, 17, 298–305. [Google Scholar] [CrossRef] [Green Version]
- Ivany, A.S.; Bullock, L.; Schminkey, D.; Wells, K.; Sharps, P.; Kools, S. Living in Fear and Prioritizing Safety: Exploring Women’s Lives After Traumatic Brain Injury from Intimate Partner Violence. Qual. Health Res. 2018, 28, 1708–1718, Article. [Google Scholar] [CrossRef] [PubMed]
- Brown, J.; Clark, D.; Pooley, A.E. Exploring the Use of Neurofeedback Therapy in Mitigating Symptoms of Traumatic Brain Injury in Survivors of Intimate Partner Violence. J. Aggress. Maltreatment Trauma 2019, 28, 764–783. [Google Scholar] [CrossRef]
- Patton Foushee, J. Domestic Violence, Concussion Injuries, and the Imaging Professional’s Role in Identifying Traumatic Brain Injury. Radiol. Technol. 2017, 89, 83–85. [Google Scholar]
- Price Snedaker, K. Women with Brain Injury: Past, Present and Future. Brain Inj. Prof. 2020, 17, 8–13, From EBSCOhost CINAHL with Full Text. [Google Scholar]
- Casper, S.T.; O’Donnell, K. The punch-drunk boxer and the battered wife: Gender and brain injury research. Soc. Sci. Med. 2020, 245, 112688. [Google Scholar] [CrossRef] [PubMed]
- Lifshitz, J.; Crabtree-Nelson, S.; Kozlowski, D.A. Traumatic Brain Injury in Victims of Domestic Violence. J. Aggress. Maltreatment Trauma 2019, 28, 655–659. [Google Scholar] [CrossRef]
- Ralston, B.; Rable, J.; Larson, T.; Handmaker, H.; Lifshitz, J. Forensic Nursing Examination to Screen for Traumatic Brain Injury following Intimate Partner Violence. J. Aggress. Maltreatment Trauma 2019, 28, 732–743. [Google Scholar] [CrossRef]
- Linton, K.F. Interpersonal violence and traumatic brain injuries among Native Americans and women. Brain Inj. 2015, 29, 639–643. [Google Scholar] [CrossRef] [PubMed]
- Furlow, B. Domestic Violence. Radiol. Technol. 2010, 82, 133–153. [Google Scholar]
- Rivara, F.; Adhia, A.; Lyons, V.; Massey, A.; Mills, B.; Morgan, E.; Simckes, M.; Rowhani-Rahbar, A. The Effects of Violence on Health. Health Aff. 2019, 38, 1622–1629. [Google Scholar] [CrossRef] [PubMed]
- Ballan, M.S.; Freyer, M.B.; Powledge, L. Intimate Partner Violence Among Men with Disabilities: The Role of Health Care Providers. Am. J. Men’s Health 2017, 11, 1536–1543. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Davis, A. Violence-related mild traumatic brain injury in women: Identifying a triad of postinjury disorders. J. Trauma Nurs. Off. J. Soc. Trauma Nurses 2014, 21, 300–308. [Google Scholar] [CrossRef]
- Zieman, G.; Bridwell, A.; Cárdenas, J.F. Traumatic Brain Injury in Domestic Violence Victims: A Retrospective Study at the Barrow Neurological Institute. J. Neurotrauma 2017, 34, 876–880. [Google Scholar] [CrossRef]
- Smirl, J.D.; Jones, K.E.; Copeland, P.; Khatra, O.; Taylor, E.H.; Van Donkelaar, P. Characterizing symptoms of traumatic brain injury in survivors of intimate partner violence. Brain Inj. 2019, 33, 1529–1538. [Google Scholar] [CrossRef] [PubMed]
- Valera, E.M.; Cao, A.; Pasternak, O.; Shenton, M.E.; Kubicki, M.; Makris, N.; Adra, N. White Matter Correlates of Mild Traumatic Brain Injuries in Women Subjected to Intimate-Partner Violence: A Preliminary Study. J. Neurotrauma 2019, 36, 661–668. [Google Scholar] [CrossRef]
- St Ivany, A.; Schminkey, D. Rethinking Traumatic Brain Injury from Intimate Partner Violence: A Theoretical Model of the Cycle of Transmission. J. Aggress. Maltreatment Trauma 2019, 28, 785–806. [Google Scholar] [CrossRef]
- Wong, J.; Mellor, D. Intimate partner violence and women’s health and wellbeing: Impacts, risk factors and responses. Contemp. Nurse 2014, 46, 170–179. [Google Scholar] [CrossRef]
- Iverson, K.M.; Dardis, C.M.; Pogoda, T.K. Traumatic brain injury and PTSD symptoms as a consequence of intimate partner violence. Compr. Psychiatry 2017, 74, 80–87. [Google Scholar] [CrossRef] [PubMed]
- Iverson, K.M.; Sayer, N.A.; Meterko, M.; Stolzmann, K.; Suri, P.; Gormley, K.; Nealon Seibert, M.; Yan, K.; Pogoda, T.K. Intimate Partner Violence Among Female OEF/OIF/OND Veterans Who Were Evaluated for Traumatic Brain Injury in the Veterans Health Administration: A Preliminary Investigation. J. Interpers. Violence 2020, 35, 2422–2445. [Google Scholar] [CrossRef]
- Ayton, D.; Pritchard, E.; Tsindos, T. Acquired Brain Injury in the Context of Family Violence: A Systematic Scoping Review of Incidence, Prevalence, and Contributing Factors. Trauma Violence Abus. 2021, 22, 3–17. [Google Scholar] [CrossRef]
- Bressler, A. Love and death. Sci. Am. Mind 2014, 25, 38–48. [Google Scholar] [CrossRef]
- Stockman, J.K.; Hayashi, H.; Campbell, J.C. Intimate Partner Violence and Its Health Impact on Ethnic Minority Women. J. Women’s Health 2015, 24, 62–79. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Banks, M.E.; Ackerman, R.J. Head and brain injuries experienced by African American women victims of intimate partner violence. Women Ther. 2002, 25, 133–143. [Google Scholar] [CrossRef]
- Bermea, A.M.; Slakoff, D.C.; Goldberg, A.E. Intimate Partner Violence in the LGBTQ+ Community: Experiences, Outcomes, and Implications for Primary Care. Prim. Care Clin. Off. Pract. 2021, 48, 329–337. [Google Scholar] [CrossRef] [PubMed]
- Dyar, C.; Messinger, A.M.; Newcomb, M.E.; Byck, G.R.; Dunlap, P.; Whitton, S.W. Development and Initial Validation of Three Culturally Sensitive Measures of Intimate Partner Violence for Sexual and Gender Minority Populations. J. Interpers. Violence 2021, 36, NP8824–NP8851. [Google Scholar] [CrossRef] [PubMed]
- Stephenson, R.; Finneran, C. The IPV-GBM Scale: A New Scale to Measure Intimate Partner Violence among Gay and Bisexual Men. PLoS ONE 2013, 8, e62592. [Google Scholar] [CrossRef] [Green Version]
- Peitzmeier, S.M.; Hughto, J.M.W.; Potter, J.; Deutsch, M.B.; Reisner, S.L. Development of a Novel Tool to Assess Intimate Partner Violence Against Transgender Individuals. J. Interpers. Violence 2019, 34, 2376–2397. [Google Scholar] [CrossRef]
- Higbee, M.; Eliason, J.; Weinberg, H.; Lifshitz, J.; Handmaker, H. Involving Police Departments in Early Awareness of Concussion Symptoms during Domestic Violence Calls. J. Aggress. Maltreatment Trauma 2019, 28, 826–837. [Google Scholar] [CrossRef]
- Richards, J.; Smithson, J.; Moberly, N.J.; Smith, A. “If It Goes Horribly Wrong the Whole World Descends on You”: The Influence of Fear, Vulnerability, and Powerlessness on Police Officers’ Response to Victims of Head Injury in Domestic Violence. Int. J. Environ. Res. Public Health 2021, 18, 7070. [Google Scholar] [CrossRef] [PubMed]
- Crowe, A.; Murray, C.E. Stigma from professional helpers toward survivors of intimate partner violence. Partn. Abus. 2015, 6, 157–179. [Google Scholar] [CrossRef]
- Relias Media—Continuing Medical Education Publishing. Available online: https://www.reliasmedia.com/articles/134507-use-screening-tools-partnerships-to-improve-identification-care-of-victims-of-ipv (accessed on 13 January 2022).
- Hunnicutt, G.; Lundgren, K.; Murray, C.; Olson, L. The Intersection of Intimate Partner Violence and Traumatic Brain Injury: A Call for Interdisciplinary Research. J. Fam. Violence 2017, 32, 471–480. [Google Scholar] [CrossRef] [Green Version]
- Haag, H.L.; Sokoloff, S.; MacGregor, N.; Broekstra, S.; Cullen, N.; Colantonio, A. Battered and Brain Injured: Assessing Knowledge of Traumatic Brain Injury Among Intimate Partner Violence Service Providers. J. Women’s Health 2019, 28, 990–996. [Google Scholar] [CrossRef] [Green Version]
- Liu, L.Y.; Bush, W.S.; Koyutürk, M.; Karakurt, G. Interplay between traumatic brain injury and intimate partner violence: Data driven analysis utilizing electronic health records. BMC Women’s Health 2020, 20, 269. [Google Scholar] [CrossRef] [PubMed]
- Campbell, J.; Jones, A.S.; Dienemann, J.; Kub, J.; Schollenberger, J.; O’Campo, P.; Gielen, A.C.; Wynne, C. Intimate Partner Violence and Physical Health Consequences. Arch. Intern. Med. 2002, 162, 1157. [Google Scholar] [CrossRef] [Green Version]
- Faugno, D.; Waszak, D.; Strack, G.B.; Brooks, M.A.; Gwinn, C.G. Strangulation Forensic Examination: Best Practice for Health Care Providers. Adv. Emerg. Nurs. J. 2013, 35, 314–327. [Google Scholar] [CrossRef]
- McClane, G.E.; Strack, G.B.; Hawley, D. A review of 300 attempted strangulation cases Part II: Clinical evaluation of the surviving victim. J. Emerg. Med. 2001, 21, 311–315. [Google Scholar] [CrossRef]
- Pritchard, E.; Tsindos, T.; Ayton, D. Practitioner perspectives on the nexus between acquired brain injury and family violence. Health Soc. Care Community 2019, 27, 1283–1294. [Google Scholar] [CrossRef] [PubMed]
- Goldin, Y.; Haag, H.L.; Trott, C.T. Screening for History of Traumatic Brain Injury Among Women Exposed to Intimate Partner Violence. PM&R 2016, 8, 1104–1110. [Google Scholar] [CrossRef] [PubMed]
- Nemeth, J.M.; Mengo, C.; Kulow, E.; Brown, A.; Ramirez, R. Provider Perceptions and Domestic Violence (DV) Survivor Experiences of Traumatic and Anoxic-Hypoxic Brain Injury: Implications for DV Advocacy Service Provision. J. Aggress. Maltreatment Trauma 2019, 28, 744–763. [Google Scholar] [CrossRef]
- Valera, E.M.; Campbell, J.; Gill, J.; Iverson, K.M. Correlates of Brain Injuries in Women Subjected to Intimate Partner Violence: Identifying the Dangers and Raising Awareness. J. Aggress. Maltreatment Trauma 2019, 28, 695–713. [Google Scholar] [CrossRef]
- Nelson, H.D.; Bougatsos, C.; Blazina, I. Screening Women for Intimate Partner Violence: A Systematic Review to Update the U.S. Preventive Services Task Force Recommendation. Ann. Intern. Med. 2012, 156, 796–808. [Google Scholar] [CrossRef] [Green Version]
- Hunnicutt, G.; Murray, C.; Lundgren, K.; Crowe, A.; Olson, L. Exploring Correlates of Probable Traumatic Brain Injury among Intimate Partner Violence Survivors. J. Aggress. Maltreatment Trauma 2019, 28, 677–694. [Google Scholar] [CrossRef]
- Baxter, K.; Hellewell, S.C. Traumatic Brain Injury within Domestic Relationships: Complications, Consequences and Contributing Factors. J. Aggress. Maltreatment Trauma 2019, 28, 660–676. [Google Scholar] [CrossRef]
- Valera, E.; Kucyi, A. Brain injury in women experiencing intimate partner-violence: Neural mechanistic evidence of an “invisible” trauma. Brain Imaging Behav. 2017, 11, 1664–1677. [Google Scholar] [CrossRef]
- Furlow, B. Computed tomography imaging of traumatic brain injury. Radiol. Technol. 2013, 84, 273CT–290CT. [Google Scholar]
- Kwako, L.E.; Glass, N.; Campbell, J.; Melvin, K.C.; Barr, T.; Gill, J.M. Traumatic brain injury in intimate partner violence: A critical review of outcomes and mechanisms. Trauma Violence Abus. 2011, 12, 115–126. [Google Scholar] [CrossRef]
- Sharp, D.J.; Scott, G.; Leech, R. Network dysfunction after traumatic brain injury. Nat. Rev. Neurol. 2014, 10, 156–166. [Google Scholar] [CrossRef]
- Valera, E.M.; Berenbaum, H. Brain injury in battered women. J. Consult. Clin. Psychol. 2003, 71, 797–804. [Google Scholar] [CrossRef]
- Birkley, E.L.; Eckhardt, C.I.; Dykstra, R.E. Posttraumatic Stress Disorder Symptoms, Intimate Partner Violence, and Relationship Functioning: A Meta-Analytic Review. J. Trauma. Stress 2016, 29, 397–405. [Google Scholar] [CrossRef] [PubMed]
- Cimino, A.N.; Yi, G.; Patch, M.; Alter, Y.; Campbell, J.C.; Gundersen, K.K.; Tang, J.T.; Tsuyuki, K.; Stockman, J.K. The Effect of Intimate Partner Violence and Probable Traumatic Brain Injury on Mental Health Outcomes for Black Women. J. Aggress. Maltreatment Trauma 2019, 28, 714–731. [Google Scholar] [CrossRef]
- Meyer, J.E.; Jammula, V.; Arnett, P.A. Head Trauma in a Community-Based Sample of Victims of Intimate Partner Violence: Prevalence, Mechanisms of Injury and Symptom Presentation. J. Interpers. Violence 2021, 8862605211016362. [Google Scholar] [CrossRef] [PubMed]
- Roberts, A.R.; Kim, J.H. Exploring the Effects of Head Injuries Among Battered Women. J. Soc. Serv. Res. 2005, 32, 33–47. [Google Scholar] [CrossRef]
- Schechter, D.S.; Moser, D.A.; Aue, T.; Gex-Fabry, M.; Pointet, V.C.; Cordero, M.I.; Suardi, F.; Manini, A.; Vital, M.; Sancho Rossignol, A.; et al. Maternal PTSD and corresponding neural activity mediate effects of child exposure to violence on child PTSD symptoms. PLoS ONE 2017, 12, e0181066. [Google Scholar] [CrossRef] [Green Version]
- Aupperle, R.L.; Allard, C.B.; Simmons, A.N.; Flagan, T.; Thorp, S.R.; Norman, S.B.; Paulus, M.P.; Stein, M.B. Neural responses during emotional processing before and after cognitive trauma therapy for battered women. Psychiatry Res. Neuroimaging 2013, 214, 48–55. [Google Scholar] [CrossRef]
- Mariani, M.; Alosco, M.L.; Mez, J.; Stern, R.A. Clinical Presentation of Chronic Traumatic Encephalopathy. Semin. Neurol. 2020, 40, 370–383. [Google Scholar] [CrossRef] [PubMed]
- Uretsky, M.; Nowinski, C.J. Chronic Traumatic Encephalopathy: Advocacy and Communicating with the Public. Semin. Neurol. 2020, 40, 461–468. [Google Scholar] [CrossRef] [PubMed]
- McKee, A.C. The Neuropathology of Chronic Traumatic Encephalopathy: The Status of the Literature. Semin. Neurol. 2020, 40, 359–369. [Google Scholar] [CrossRef]
- Valera, E.M. Increasing Our Understanding of an Overlooked Public Health Epidemic: Traumatic Brain Injuries in Women Subjected to Intimate Partner Violence. J. Women’s Health 2018, 27, 735–736. [Google Scholar] [CrossRef] [PubMed]
- Ellis, T.W.; Brownstein, S.; Beitchman, K.; Lifshitz, J. Restoring More than Smiles in Broken Homes: Dental and Oral Biomarkers of Brain Injury in Domestic Violence. J. Aggress. Maltreatment Trauma 2019, 28, 838–847. [Google Scholar] [CrossRef]
- Shifflett, C.M. Domestic Abuse and Brain Injury in Women. Women’s Health Act. 2017, 42, 6–7. [Google Scholar]
- Rowe, R.K.; Murphy, S.M.; Handmaker, H.; Lifshitz, J. Population-Level Epidemiology of Concussion Concurrent with Domestic Violence in Arizona, USA. J. Neurotrauma 2021, 38, 2301–2310. [Google Scholar] [CrossRef] [PubMed]
- Moreira, D.N.; Pinto da Costa, M. The impact of the Covid-19 pandemic in the precipitation of intimate partner violence. Int. J. Law Psychiatry 2020, 71, 101606. [Google Scholar] [CrossRef]
| Individuals at Increased Risk of TBI Secondary to Domestic Violence |
|---|
| Females of child-bearing age [12] |
| Individuals with disabilities [12] |
| Previous TBI (from domestic abuse or other cause) [2,3,15,16,17,18] |
| Low annual household income [11] |
| Minority races (Native American, Black, Asian) [2,11,19,20] |
| Female military veterans [21,22] |
| LGBTQIA+ communities [22] |
| Elderly (>60 years old) and children [13,23] |
| Author | Screening Tool | Population | Measuring Tool | Study Objective | Conclusions |
|---|---|---|---|---|---|
| Dyar et al., 2021 [28] | Sexual and gender minorities-specific IPV Conflict Tactics Scale | Sexual and gender minority populations who were assigned female at birth between ages 16 and 20 years old. | An assessment scale addressing SGM-specific IPV behaviors including perpetriation and victimization. | To create a comprehensive set of culturally appropriate measures captivating a broad range of types of IPV among sexual and gender minorities. | This tool demonstrated high reliability and validity. It improved upon previous scales by being cuturally sensitive and addressing unique forms of IPV experienced by this community. This tool can be further improved and evaluated by future research and use on SGMs who are assigned male at birth, as well as different age groups. |
| Stephenson and Finneran, 2013 [29] | IPV Gay and Bisexual Men (-GBM) scale | Gay and bisexual men in the USA with at least a 6th grade reading level. | Consist of 23 prompts in five domains: physical and sexual abuse, monitoring, controlling, HIV-related abuse, and emotional abuse, which takes about 15–20 min to complete. | Create a new scale to measure IPV among gay and bisexual men. | The IPV-GBM scale showed strong internal reliablity. Although there was minimal variations in content of the scale by race, the results showed that it seemed to be appropriate for use in white and black/African American populations. This scale showed a higher prevalence of IPV than other scales, indicating that it included more items that are experienced specifically by this population. Further testing is needed to create a scale that is applicable to larger samples of this population as well as other racial/ethinic groups. |
| Peitzmeier et al., 2019 [30] | Transgender-related IPV Tool | Transmasculine individuals: individuals assigned a female sex at birth who have a non-female gender identity. | Four questions assessing four domains: coercive control of gender transition or gender presentation, emphasizing undesirability of transgender individuals as intimate partners, blackmail via outing, and sabotaging transition. | Create a measurement tool to assess transgender-related IPV. | This study showed that the scale had adequate reliability and validity as compared with other measures. This tool was helpful for identifying dangers that transgender individuals may be facing, that would be otherwise missed by traditional meaurement tools. A revised 10-item scale is being developed, as these additional items may increase the tools sensitivity and validity. Using this tool will allow clinicians and researchers to better identify IPV experienced by transgender individuals. |
| Common Presenting Symptoms of TBI Secondary to Domestic Violence |
|---|
| Neurologic symptoms: headache, confusion, memory loss [38] |
| Gastrointestinal symptoms: malnutrition, alcoholic cirrhosis, loss of appetite, abdominal pain [37,38] |
| Genitourinary symptoms (may indicate sexual abuse): vaginal infections, STDs, vaginal bleeding, pelvic pain, UTI [38] |
| Symptoms that may indicate strangulation: hoarseness, petechiae in conjunctivae, scalp, and external ear [40] |
| Psychiatric symptoms: emotionally labile, restless, combative, catatonic [40] |
| Other common symptoms: bruises, back pain, acquired thrombocytopenia, post-traumatic wound infection [26,37] |
| Tool | Method of Administration | Primary Focus: TBI vs. IPV | Prompts Relating to TBI Secondary to IPV | Ways to Make the Tool Better at Screening for TBI Secondary to Domestic Violence |
|---|---|---|---|---|
| HELPS [2,42,46,47] | Professional interview | TBI | None, asks about injury to head, but not in relation to domestic violence. | When asking about injuries to the head, ask the cause. Specifically ask if the injury was inflicted by another individual and if so, who. |
| Brain Injury Screening Questionnaire (BISQ) [42] | Self-report | TBI | Asks about blows to the head. | Ask about the cause, i.e., have injuries ever been inflicted by their partner. Ask about other injuries to the face. |
| Ohio State University TBI Identification Method [42] | Interview | TBI | Addresses questions about TBI because of violent shaking. | Include prompts about blows to the face and head, ask if their partner has every physically abused them. |
| Traumatic Brain Injury Questionnaire [42] | Self-report | TBI | Asks about injury to face and injury secondary to cord around neck. | Further address injuries to the head and face, including blows to the head. Ask specifically if patient has ever acquired an injury from their partner. |
| Partner Violence Screen Questionnaire [12] | Interview | IPV | Have you been hit, kicked, punched, or otherwise hurt by somebody in the past year? | Follow up this prompt by asking about if there have been any injuries specifically to the head. |
| Hurt Insulted Threated or Screamed at Instrument [12] | Interview | IPV | How often does your partner physically hurt you? | Expand to ask about the type of physical abuse (blows, shaking, etc.) and if there has ever been an injury to the head. |
| Woman Abuse Screening Tool (WAST) [12] | Interview | IPV | Do arguments ever result in hitting, kicking, or pushing? Has your partner ever abused you physically? | Ask about body locations of physical abuse, including the head and face. Ask about timing of the most recent injury. |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Costello, K.; Greenwald, B.D. Update on Domestic Violence and Traumatic Brain Injury: A Narrative Review. Brain Sci. 2022, 12, 122. https://doi.org/10.3390/brainsci12010122
Costello K, Greenwald BD. Update on Domestic Violence and Traumatic Brain Injury: A Narrative Review. Brain Sciences. 2022; 12(1):122. https://doi.org/10.3390/brainsci12010122
Chicago/Turabian StyleCostello, Kellianne, and Brian D. Greenwald. 2022. "Update on Domestic Violence and Traumatic Brain Injury: A Narrative Review" Brain Sciences 12, no. 1: 122. https://doi.org/10.3390/brainsci12010122
APA StyleCostello, K., & Greenwald, B. D. (2022). Update on Domestic Violence and Traumatic Brain Injury: A Narrative Review. Brain Sciences, 12(1), 122. https://doi.org/10.3390/brainsci12010122






