1. Introduction
Education, behavioral interventions, condom usage, abstinence, testing, and knowing one’s serostatus have been the primary means of preventing and controlling the spread of the human immunodeficiency virus (HIV) [
1,
2]. In this work, we develop a model to estimate the effect of a newer method, pre-exposure prophylaxis (PrEP), for reducing the prevalence of HIV. There are two types of HIV infection, type-1 and type-2. We focus on type-1 HIV for this investigation as PrEP has not been shown to be effective against type-2 HIV [
3].
PrEP was approved in 2012 by the Food and Drug Administration and is the prescribed use of antiretroviral medications (tenofovir and emtricitabine) [
4]. When PrEP is taken properly, it is proven to prevent exposed uninfected individuals from acquiring HIV by creating a barrier between the pathogen and CD4 cells (the cells HIV replicates through), thereby severing the chain of infection [
5]. The PrEP protocol requires all participants to regularly undergo testing for HIV and other sexually transmitted infections/diseases (STIs/STDs) to provide early detection of HIV, decrease risk from STIs, and to establish early serostatus monitoring. The PrEP protocol provides the opportunity to start antiretroviral treatment (ART) early in the HIV life cycle, controlling the viral load and helping reduce the spread of HIV while offering optimistic patient treatment [
6,
7].
Mathematical epidemiological models incorporating PrEP are extremely sparse [
8,
9,
10]. The limited availability of studies and explorations of the impact of PrEP use for those at high risk of developing HIV is the motivation for this paper. We focus on the U.S. population and, after reviewing the CDC Atlas and HIV Case Surveillance reports, we determined the highest risk subgroup of interest was the combination of male-to-male sexual contact (MSM), injection drug users, and the combination of MSM using injection drugs [
11,
12]. We developed a compartmental model to explore the long-term effectiveness of PrEP usage.
2. Methods
We initially develop a simple Susceptible (S), Infected (I), stage 3 HIV/AIDS (A), or SIA, model. Parameter information and values vary greatly across the different models previously explored by others, with some having significant uncertainty [
13,
14,
15]. We use the SIA model primarily to obtain parameters from the available CDC data by matching our results to the recorded data before PrEP usage was available. We determined our HIV and AIDS-related death rates along with the progression rate from HIV to AIDS directly from the anonymous and publicly accessible 2008 to 2018 CDC case surveillance data, which includes all 50 states, the District of Columbia, American Samoa, Guam, the Northern Mariana Islands, Puerto Rico, and the U.S. Virgin Islands [
11].
After determining the appropriate parameters, we extend our simple model into a more complex model that includes the use of PrEP and condoms. The new model divides the total Susceptibles into four subgroups: those using no protection , those using PrEP , those using condoms , and those using both PrEP and condoms . The total infected compartment is subdivided into 4 subgroups , one for each corresponding susceptible group, while the AIDS compartment remains unchanged. We call this model the SPCBIA model.
The limiting assumptions we make are:
The death rates associated with HIV and AIDS have become steady and stable.
The rate of disease progression from HIV to AIDS is held constant with the acknowledgement that it is likely to decrease over time considering current data trends.
We specifically looked at scenarios where the percentage of the high-risk population using various prophylaxis options is held constant. We do include the possibility that there may be medically required PrEP medication discontinuation.
Some of those within the AIDS compartment receive ART and may still transmit HIV.
We exclude the cost of PrEP and the associated ancillary support services from the model since we are accessing data exclusive to the United States. As of July 2021, the Affordable Care Act requires all non-grandfathered in private health plans to cover the associated costs without cost sharing [
16]. We acknowledge that other countries do not have this requirement and that this may thus affect PrEP access.
2.1. The SIA Model
As mentioned above, we use an SIA model to help define some parameters. In the simple SIA model, the susceptible population may die of natural causes, move to the infected compartment, or remain susceptible. The infected individuals may die from natural causes or infection-related causes, or they may progress to the stage 3 HIV/AIDS compartment. Once an infected individual has progressed to AIDS, they may die from natural causes or from disease-related causes. They may also continue to infect. There is a parameter to adjust the transmission probability per partner for the greater infectiousness of AIDS over HIV.
Our non-normalized equations for the SIA model are:
We begin our numerical simulations using total numbers in each compartment followed by normalization. Here, is the total population, is the rate at which people enter the susceptible population, is the average number of sexual partners an individual has per year, is the transmission probability per partner, and is a modification parameter for those with AIDS and actively infecting susceptible individuals. is larger than 1, as AIDS is more virulent than HIV. The average death rate by natural causes is given by , is the progression rate from HIV into AIDS, is the HIV-related death rate, is the AIDS-related death rate, and is the infection rate of AIDS individuals still able to transmit HIV.
2.2. The SPCBIA Model
In the SPCBIA model we now include PrEP and condom usage and explore the resulting infection projections. As before, each susceptible compartment allows for natural death or infection. There is an allowance for those using PrEP who discontinue usage and return to the general susceptible compartment for various medical reasons or life decisions. The condom usage compartment also allows for the discontinued usage of condoms, as this is the current trend in our high-risk group [
17]. In the case that someone in the
compartment should cease using PrEP, it is assumed they will continue using condoms and return to that compartment. All four infected subgroups, similarly to the SIA model, allow for natural death, infection-related death, and progression to the AIDS state. Likewise, the AIDS compartment still allows for continued infection.
Our non-normalized equations for the SPCBIA model are:
The new parameters are defined as follows: is the sum of the individual infected subgroups, is the proportion of starting PrEP, is the proportion of starting to use condoms, is the proportion of using both PrEP and condoms, is the portion of who stop using PrEP and move back to , is the proportion of stopping condoms use and returning to , is a modification parameter to account for PrEP effectiveness, is a modification parameter to account for condom effectiveness, and is a modification parameter to account for the compounded effectiveness of using both.
Equations (4) and (5) simply represent how to calculate the total susceptible population and the total infected population, respectively. The remaining equations calculate the time evolution of the individual categories within each larger population. As an example, we discuss Equation (11) which calculates how the number of infected PrEP users changes with time. The number of Ip cases can decrease through natural death (, death through HIV , or can be transferred to another category , i.e., the development of AIDS. Similarly, an increase in the number of Ip cases is proportional to the susceptible population using PrEP, (P), with the proportionality constant including terms involving the number of partners per year (r), the probability of transmission , the probability of meeting an infected partner , and an estimation of PrEP effectiveness (1 − k).
Numerically, the solution for the coupled set of equations is carried out using Runge–Kutta integration methods with a time step of 0.001 years. For the SIA model we checked that our results were consistent with analytic equilibrium calculations.
3. Results
3.1. Determination of Parameters
As noted earlier, there are multiple parameters that are not well established for the epidemiological models. We have tried to reduce this problem by comparing the results of a simple model with the CDC data, initially without PrEP.
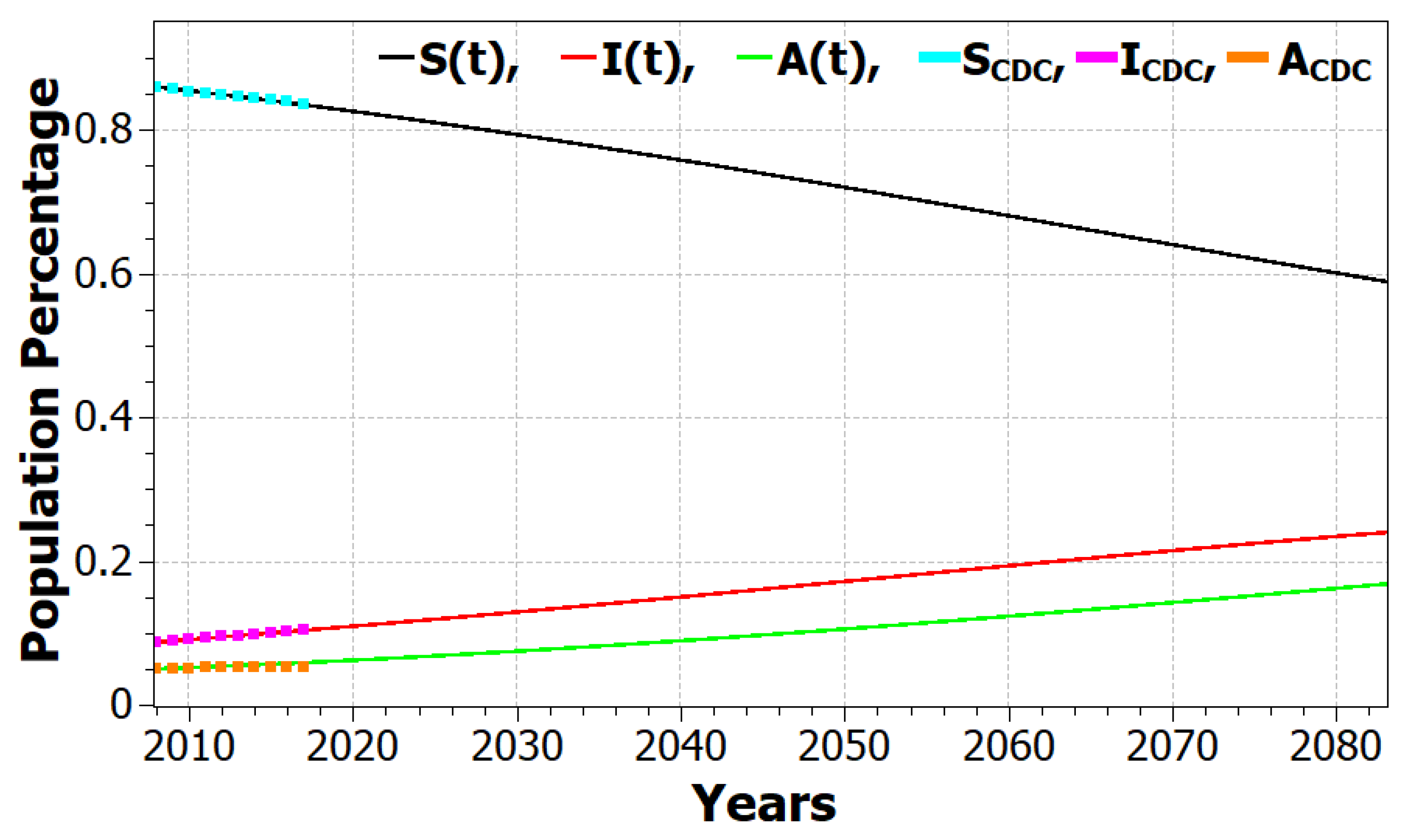
Table 1 presents yearly data containing information from CDC case surveillance data related to the estimated high-risk population and infections. These data are used to calculate
Figure 1, which plots the normalized percentages for the different categories with projections from our SIA model.
We note that
Table 1 contains estimated values for N, the total high-risk population. No value for this is given in the CDC data. To make this estimate, we took 3.9% of the U.S. population for each year minus the reported HIV and AIDS-related deaths [
18].
As mentioned earlier, we use the data in
Figure 1 along with our SIA model results to help determine some of the unknown (or disputed) parameters in the SIA model. We found good agreement, as shown in
Figure 1, with the parameters listed in
Table 2. We chose to use two average sexual partners per year and adjusted the remaining parameters to best match the CDC surveillance data. The key parameters that were determined in this way were
and
.
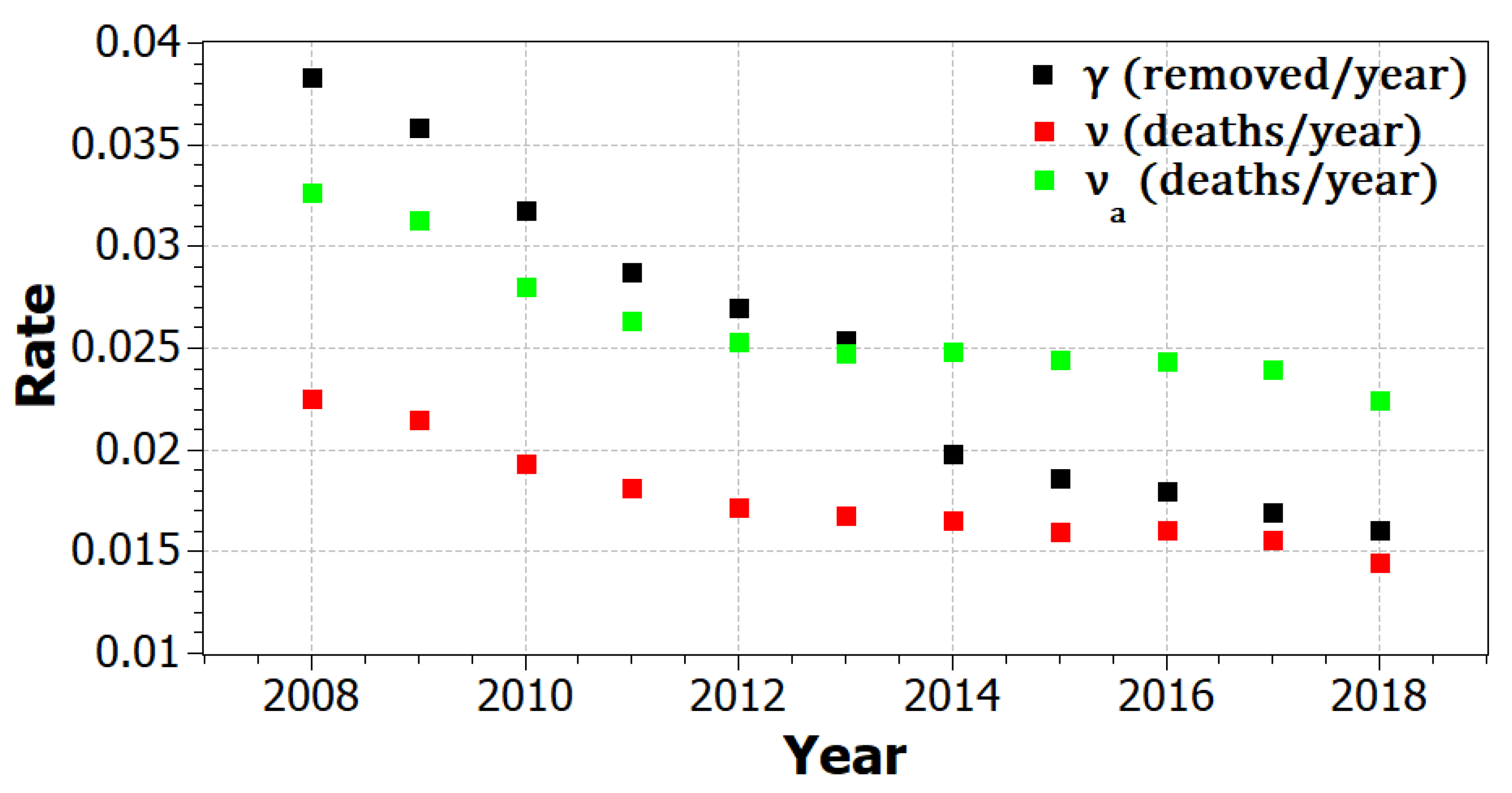
We note that PrEP was introduced in 2012. This information helped determine various rates in our model involving PrEP.
Figure 2 shows how several death rates and development of AIDS rate evolved during this period. It is easily seen that the rates in
Figure 2 are nearly constant after 2012. Because of this, we simply used the values from 2017 for our parameters in
Table 2.
Having used the data from 2008 to 2018 to determine some parameters, as discussed above, we now use the full SPCBIA model, starting at the year 2017, to make our detailed calculations for how the use of PrEP impacts the number of infected people. Because our starting year is different, compared to the earlier set of parameters, many parameters are different from those in
Table 2. The new parameters are listed in
Table 3; any that do not appear are the same as those in
Table 2.
We now explore several aspects of HIV propagation in the SPCBIA model. Specifically, we examine the following issues:
- (1)
We calculate long-term populations and outcomes under an optimistic scenario defined as the complete proper usage of PrEP. This scenario utilizes different values of initial PrEP usage and identifies what values of PrEP usage may provide substantial improvements. Our optimistic values are 90% PrEP effectiveness, 91% condom effectiveness, and 99% effectiveness for those using both PrEP and condoms.
- (2)
We examine the outcomes of a pessimistic scenario utilizing a low level of PrEP effectiveness by assuming that PrEP protocol adherence is wholly inconsistent and that there is a possibility of intravenous drug use. The pessimistic model uses 50% PrEP effectiveness, 64% condom effectiveness, and 82% effectiveness for those using both PrEP and condoms.
- (3)
We explore the impact of how the average number of sexual partners per year affects the projection outcomes by comparing the results for two and four average sexual partners per year.
- (4)
We look at a 50-year benchmark for various starting percentages of those using PrEP to explore outcomes as a function of PrEP usage.
3.2. Optimistic Scenario Results
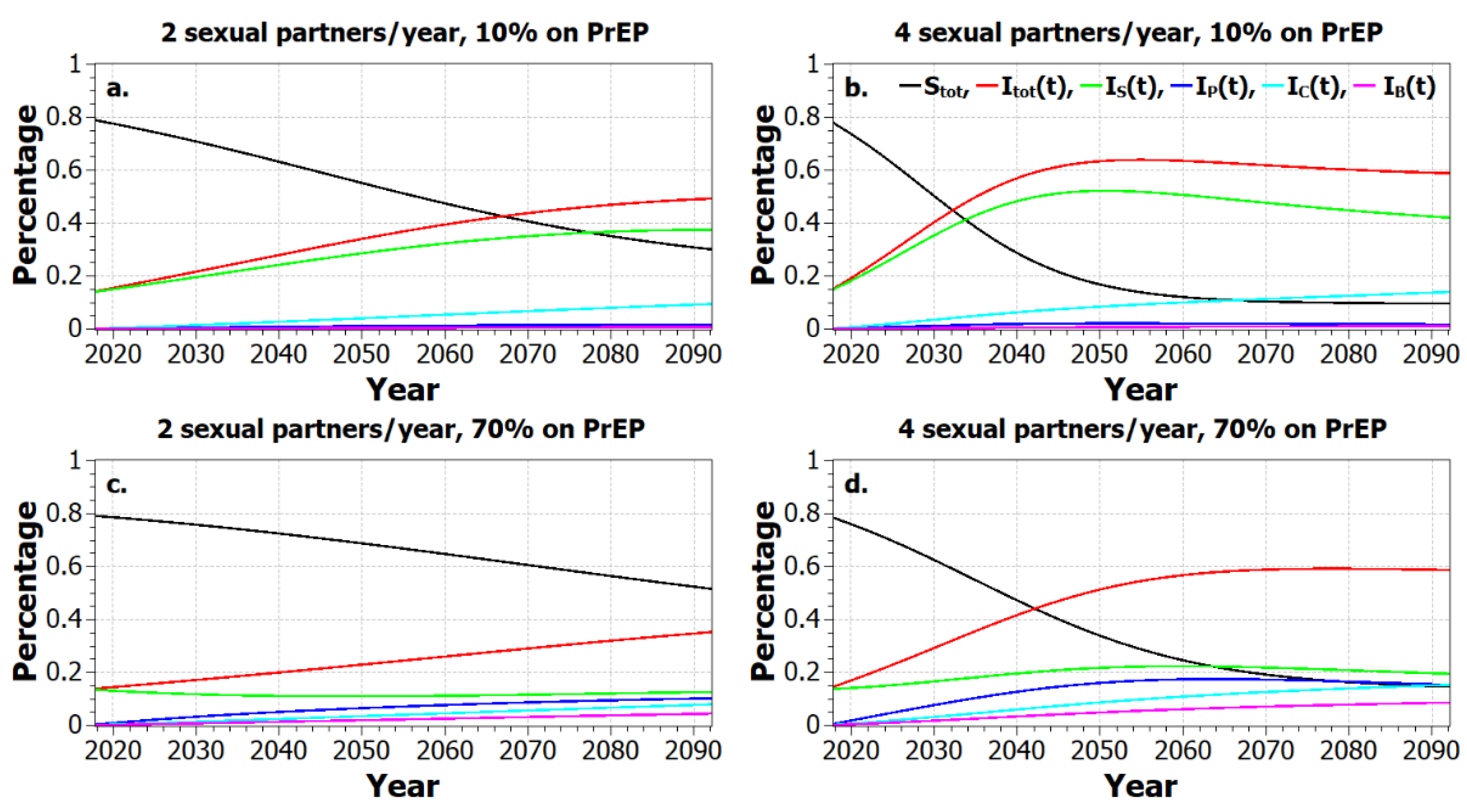
Figure 3 presents the results for the time-dependent populations using the optimistic case parameters. The plots in (a) and (b) show projections for the case when we hold PrEP usage at the lower value of 10% but change the average sexual partners per year from two to four. The results are dramatic. In both cases, the number of infections increases as time increases. After 75 years, the percentage of the population who are infected is 40% for two partners per year and rises to 60% for four partners per year. The plots in (c) and (d) show similar projection data except that PrEP use is held at 70%. The situation is significantly improved when a larger fraction of the population is using PrEP. In (c), 15% of the population is infected after 75 years with sexual partners per year at two. This produces a stable population over time. Even with four partners per year, higher PrEP usage can make a significant difference in outcomes; the long-term infected percentage is 33% lower in this case when PrEP use is increased from 10% to 70%. This can be seen by comparing
Figure 3b with
Figure 3d.
3.3. Pessimistic Scenario Results
Figure 4 presents the results for the time-dependent populations using the pessimistic case parameters. The plots in (a) and (b) show projections for holding PrEP usage at 10% and changing the average sexual partners per year from two to four. Long-term total infections are 50% for two sexual partners per year and 60% for four sexual partners per year. We do not see a stable set of populations develop as they did before. Again, PrEP usage was set at 70% for (c) and (d). We see in (c) that the increase to 70% PrEP usage for two sexual partners per year leads to the infected compartment decreasing to 38%, still a significant improvement over 10% PrEP usage from (a). However, there is not a significant improvement in infections in (d) for four sexual partners per year over the 10% PrEP usage in (b). There is a redistribution between the subcategories for infected, but the total infected is 59% in both cases.
3.4. 50-Year Benchmark
We can examine the long-term effectiveness of different scenarios by holding the sexual partners per year steady at two and watching the 50-year benchmark for different PrEP usage percentages.
Figure 5 displays this information for the optimistic and pessimistic cases. When 50% of the high-risk population is on PrEP, compared to no use of PrEP, there is a reduction in the infected percentage by half for the optimistic case and by 27% for the pessimistic case.
3.5. Condom versus PrEP Usage
We comment on the use of condoms versus the use of PrEP in our results. First, we note that our models already assume that 35% of the high-risk population are using condoms, which is consistent with recent data in the U.S. When used properly, condoms and PrEP are close to being equally effective. Thus, in this case, an increase in condom use numerically is nearly equivalent to an increase in PrEP usage. If used inconsistently, exclusive use of condoms is slightly better than exclusive use of PrEP (at the 25-year mark, condoms-only gives an infection percentage of 19.5% while PrEP-only gives 26.3%). However, as considered in the Discussion section below, different subgroups may have reasons to prefer one method over the other. Simultaneous use of both condoms and PrEP would not make a substantial difference in the results for the optimistic scenario; however, it would substantially improve the pessimistic scenario results.
4. Discussion
It is clear from these results that PrEP can be a highly effective tool in mitigating and controlling the spread of HIV infections. Proper PrEP usage is ideal but even under the pessimistic scenario, the projections for HIV infections are still significantly reduced when the average number of sexual partners is two. The importance of the number of average sexual partners per year is more prominent in the pessimistic case and suggests that improper PrEP usage and an increased number of partners minimize the long-term effectiveness of PrEP for mitigating HIV management.
We emphasize that our model and its results are based on U.S. data as a whole. Policy decisions, both in the U.S. and other countries, should include the consideration of subgroups involving educational level, race, ethnicity, and economic status. In addition, because PrEP usage does involve minimal monitoring, ease of access is also important.
Our model does not currently discriminate between the various subgroups that are included in the high-risk population. However, the model may be modified to selectively analyze a chosen age range, ethnicity, or a specified income range, for example. This would require appropriate parameters for each subgroup. The model is only limited by the availability of data. We note that the CDC case surveillance data will allow for breakdowns by age, race/ethnicity, gender, and transmission categories with the caveat that some data can be suppressed due to agreements between the CDC and state level HIV surveillance initiatives [
11].
Clearly, policy decisions need to be based on the cost and effectiveness of different methods of preventing HIV infections. When used properly, condoms and PrEP are close to being equally effective. Condom usage is inexpensive and does not require monitoring. In addition, condoms may be cost-effective in less well-developed countries or among lower income groups. PrEP also requires access to care which could be an issue in some African countries, for instance. However, there is widespread reluctance to use condoms. To illustrate, in the U.S. only about 35% of the high-risk population uses condoms consistently, and this number has been dropping in recent years. The percentage of men in the 18–24 age range using condoms is even lower, suggesting that they might particularly benefit from a push to use PrEP [
17,
19]. This is particularly important for young black men who have a 25% chance of being infected with HIV by age 25 [
20]. There are many other countries where consistent condom use is near or below 50%. This includes, for example, Namibia at 46% [
21], Bangladesh at 34–50% [
22], and Thailand at 55% [
23].
We note that, in the U.S. after the Affordable Care Act, the use of PrEP and its associated costs are mandated to be free under most insurance plans, including Medicare and Medicaid. This suggests that it is reasonable to encourage PrEP use within the U.S. as economic considerations have been removed.
This exploration utilizes the most recent data available from the CDC case surveillance data and projections can be improved upon as more salient data are collected, allowing for a better evaluation of some of the key parameters. Future work should include allowances for growth in the percentage of PrEP usage over time as more physicians and clinicians become more knowledgeable about PrEP and raise awareness with patients that are at risk of HIV infection.
5. Conclusions and Policy Implications
These results support current PrEP policy in the United States. The results offer insights into additional assessment of how aggressively PrEP usage should be encouraged compared to the current prescribing trend. This study emphasizes the importance of information about PrEP protocol adherence and analysis of HIV infections that occur while using PrEP. As these data are currently not part of the CDC Atlas case surveillance database, we suggest their future inclusion. Additionally, these models can be applied at a state or local level, instead of nationally, with proper modifications allowing for a comparison at all levels for HIV mitigation and adherence to the current DHAP strategic plan. If modified and applied to smaller groups, these models may be utilized in social sciences to detect disparities between such smaller groups in order to better inform policy.
As discussed above, the average number of sexual partners per year for the target population may have great importance. These data are not currently provided by the CDC and perhaps are not collected. As our calculations indicate that both proper PrEP usage and reducing the number of partners are important, this could be an important policy thrust. Some subgroups have a disproportionately high risk of becoming infected with HIV and may benefit greatly from PrEP. One such group is the young black MSM group mentioned earlier. The higher HIV rates associated with this group suggest an emphasis should be placed on bridging this disparity by insuring an increase in PrEP awareness and access [
19,
24].
One possible means to address the importance regarding the average number of sexual partners per year while on PrEP but not using condoms would be qualitative studies. These studies could probe PrEP participant understanding, attitudes, and knowledge about medication effectiveness with populations with a larger number of sexual partners, repeated exposures, opportunistic infections, or coinfections (e.g., do patients taking PrEP understand that other STIs may enhance their susceptibility to HIV?) [
25,
26,
27]. Another suggestion might be a possible protocol adjustment which includes a questionnaire at follow-up patient visits and interviews to emphasize patient understanding of medication effectiveness when individuals have a larger number of sexual partners.
Author Contributions
Conceptualization, J.L. and R.E.C.; Methodology, J.L. and R.E.C.; Programming, J.L.; Validation, J.L. and R.E.C.; Formal analysis, J.L. and R.E.C.; Investigation, J.L. and R.E.C.; Data curation, J.L.; Writing—original draft preparation, J.L.; Writing—review and editing, J.L. and R.E.C.; Supervision, R.E.C. All authors have read and agreed to the published version of the manuscript.
Funding
This research received no external funding.
Institutional Review Board Statement
Ethics approval was not applicable as the study is computational/mathematical and utilizes anonymous publicly available data with no human or animal subjects.
Informed Consent Statement
Not applicable.
Data Availability Statement
The data produced and used are provided and code will be made available by request.
Conflicts of Interest
The authors declare no conflict of interest.
References
- CDC. Division of HIV/AIDS Prevention Strategic Plan 2017–2020. 2017; pp. 1–25. Available online: https://www.cdc.gov/hiv/pdf/dhap/cdc-hiv-dhap-external-strategic-plan.pdf (accessed on 11 November 2019).
- United Nations Joint Programme on HIV/AIDS (UNAIDS). 90-90-90 an Ambitious Treatment Target to Help End the AIDS Epidemic; United Nations: New York, NY, USA, 2014; 40p, Available online: http://www.unaids.org/sites/default/files/media_asset/90-90-90_en.pdf (accessed on 11 November 2019).
- Campbell-Yesufu, O.T.; Gandhi, R.T. Update on human immunodeficiency virus (HIV)-2 infection. Clin. Infect. Dis. 2011, 52, 780–787. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- FDA. FDA In Brief: FDA Continues to Encourage Ongoing Education about the Benefits and Risks Associated with PrEP, Including Additional Steps to Help Reduce the Risk of Getting HIV; U.S. Food and Drug Administration: Silver Spring, MD, USA, 2019. Available online: https://www.fda.gov/news-events/fda-brief/fda-brief-fda-continues-encourage-ongoing-education-about-benefits-and-risks-associated-prep (accessed on 17 November 2019).
- Kearney, B.P.; Flaherty, J.F.; Shah, J. Tenofovir disoproxil fumarate: Clinical pharmacology and pharmacokinetics. Clin. Pharmacokinet. 2004, 43, 595–612. [Google Scholar] [CrossRef] [PubMed]
- Falkenhagen, A.; Joshi, S. Genetic Strategies for HIV Treatment and Prevention. Mol. Ther. Nucleic Acids. 2018, 13, 514–533. [Google Scholar] [CrossRef] [Green Version]
- Hill, A.L. Mathematical models of HIV latency. Curr. Top. Microbiol. Immunol. 2018, 417, 131–156. [Google Scholar] [CrossRef]
- Silva, C.J.; Torres, D.F.M. Modeling and optimal control of HIV/AIDS prevention through PrEP. Discrete Contin. Dyn. Syst. Ser. S. 2018, 11, 2. [Google Scholar] [CrossRef]
- Kim, S.B.; Yoon, M.; Ku, N.S.; Kim, M.H.; Song, J.E.; Ahn, J.Y.; Jeong, S.J.; Kim, C.; Kwon, H.D.; Lee, J.; et al. Mathematical modeling of HIV prevention measures including pre-exposure prophylaxis on HIV incidence in South Korea. PLoS ONE 2014, 9, e90080. [Google Scholar] [CrossRef] [Green Version]
- Hammack, P.L.; Meyer, I.H.; Krueger, E.A.; Lightfoot, M.; Frost, D.M. HIV testing and pre-exposure prophylaxis (PrEP) use, familiarity, and attitudes among gay and bisexual men in the United States: A national probability sample of three birth cohorts. PLoS ONE 2018, 13, e0202806. [Google Scholar] [CrossRef]
- CDC. Atlas Plus HIV, Hepatitits, STD, TB, Social Determinates of Health Data; Centers for Disease Control and Prevention: Atlanta, GA, USA, 2021. Available online: https://gis.cdc.gov/grasp/nchhstpatlas/tables.html (accessed on 27 April 2021).
- Prejean, J.; Song, R.; Hernandez, A.; Ziebell, R.; Green, T.; Walker, F.; Lin, L.S.; An, Q.; Mermin, J.; Lansky, A.; et al. Estimated HIV incidence in the United States, 2006–2009. PLoS ONE 2011, 6, e17502. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Jacquez, J.A.; Simon, C.P.; Koopman, J.; Sattenspiel, L.; Perry, T. Modeling and analyzing HIV transmission: The effect of contact patterns. Math. Biosci. 1988, 92, 119–199. [Google Scholar] [CrossRef] [Green Version]
- Naresh, R.; Tripathi, A.; Sharma, D. Modelling and analysis of the spread of AIDS epidemic with immigration of HIV infectives. Math. Comput. Model. 2009, 49, 880–892. [Google Scholar] [CrossRef]
- Hyman, J.M.; Li, J.; Ann Stanley, E. The differential infectivity and staged progression models for the transmission of HIV. Math. Biosci. 1999, 155, 77–109. [Google Scholar] [CrossRef]
- CMS.gov. FAQS About Affordable Care Act Implementation Part 47. CCIIO OG MWRD 671 2021. Available online: https://www.cms.gov/CCIIO/Resources/Fact-Sheets-and-FAQs/Downloads/FAQs-Part-47.pdf (accessed on 5 August 2022).
- Paz-bailey, G.; Mendoza, M.C.B.; Finlayson, T.; Wejnert, C.; Le, B.; Rose, C.; Raymond, H.F.; Prejean, J.; NHBS Study Group. Trends in condom use among MSM in the United States: The role of antiretroviral therapy and seroadaptive strategies. AIDS 2016, 30, 1985. [Google Scholar] [CrossRef] [PubMed]
- LGBT Demographic Data Interactive. The Williams Institute, UCLA School of Law. 2019. Available online: https://williamsinstitute.law.ucla.edu/visualization/lgbt-stats/?topic=LGBT#density (accessed on 5 January 2020).
- Zhang Kudon, H.; Mulatu, M.S.; Song, W.; Heitgerd, J.; Rao, S. Trends in Condomless Sex Among MSM Who Participated in CDC-Funded HIV Risk-Reduction Interventions in the United States, 2012–2017. JPHMP 2022, 28, 170–173. [Google Scholar] [CrossRef] [PubMed]
- Crosby, R.A.; Mena, L.; Vickers Smith, R. Promoting positive condom use experiences among young black MSM: A randomized controlled trial of a brief, clinic-based intervention. Health Educ. Res. 2018, 33, 197–204. [Google Scholar] [CrossRef] [PubMed]
- Russell, C.; Tahlil, K.; Davis, M.; Winston, A.; Amaambo, T.; Hamunime, N.; Pietersen, I.; Jordan, M.R.; Tang, A.M.; Hong, S.Y. Barriers to condom use among key populations in Namibia. Int. J. STD AIDS 2019, 30, 1417–1424. [Google Scholar] [CrossRef] [PubMed]
- International Centre for Diarrhoeal Disease Research, Bangladesh. Behavioural and Serological Surveillance on Males Having Sex with Males, Male Sex Workers and Hijra, 2015. AIDS/STD Programme (ASP) Technical Report. 2017. Available online: https://asp.portal.gov.bd/sites/default/files/files/asp.portal.gov.bd/page/4129b6d9_3565_48d5_8f89_ef37abb51732/2020-08-10-21-45-ac75def954198f99d473dde36882dbcd.pdf (accessed on 7 August 2022).
- Prakot, S.; Kiertiburanakul, S.; Janepanish Visudtibhan, J. Prevalence of Condom Use and Its Related Factors Among Men Who Have Sex with Men in Thailand. Rama Med. J. 2019, 42, 49–59. [Google Scholar] [CrossRef]
- Kanny, D.; Jeffries, I.V.W.L.; Chapin-Bardales, J.; Denning, P.; Cha, S.; Finlayson, T.; Wejnert, C.; Abrego, M.; Al-Tayyib, A.; Anderson, B.; et al. Racial/Ethnic Disparities in HIV Preexposure Prophylaxis among Men Who Have Sex with Men—23 Urban Areas, 2017. MMWR Morb. Mortal. Wkly. Rep. 2019, 68, 801–806. [Google Scholar] [CrossRef] [PubMed]
- Hayes, R.; Watson-Jones, D.; Celum, C.; van de Wijgert, J.; Wasserheit, J. Treatment of sexually transmitted infections for HIVprevention: End of the road or new beginning? AIDS 2010, 24, S15–S26. [Google Scholar] [CrossRef] [PubMed]
- Peterman, T.A.; Newman, D.R.; Maddox, L.; Schmitt, K.; Shiver, S. High Risk for HIV following Syphilis Diagnosis among Men in Florida, 2000–2011. Public Health Rep. 2014, 129, 164–169. [Google Scholar] [CrossRef] [PubMed]
- Pathela, P.; Braunstein, S.L.; Blank, S.; Schillinger, J.A. HIV Incidence Among Men with and Those Without Sexually Transmitted Rectal Infections: Estimates from Matching Against an HIV Case Registry. Clin. Infect. Dis. 2013, 57, 1203–1209. [Google Scholar] [CrossRef] [PubMed] [Green Version]
| Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).