Development and Application of MAGIC-f Gel in Cancer Research and Medical Imaging
Abstract
:1. Introduction
2. Development of MAGIC-f Gel
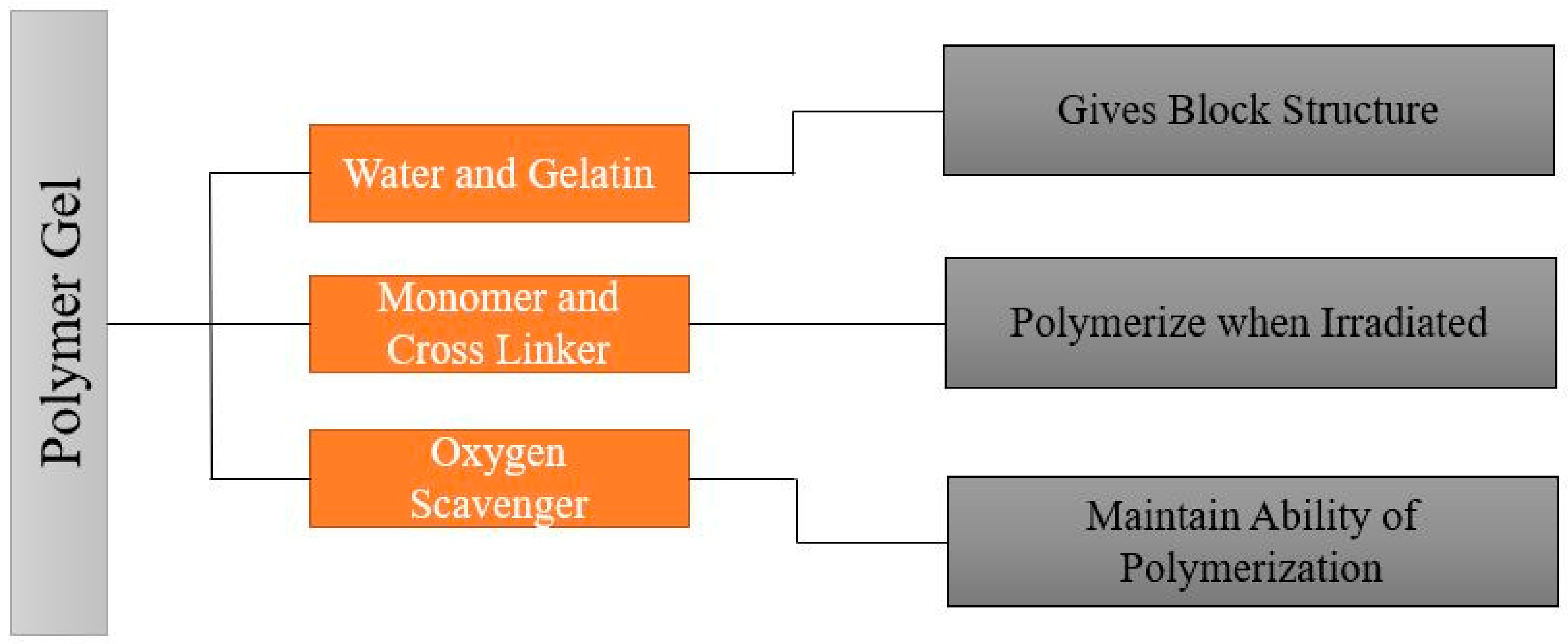
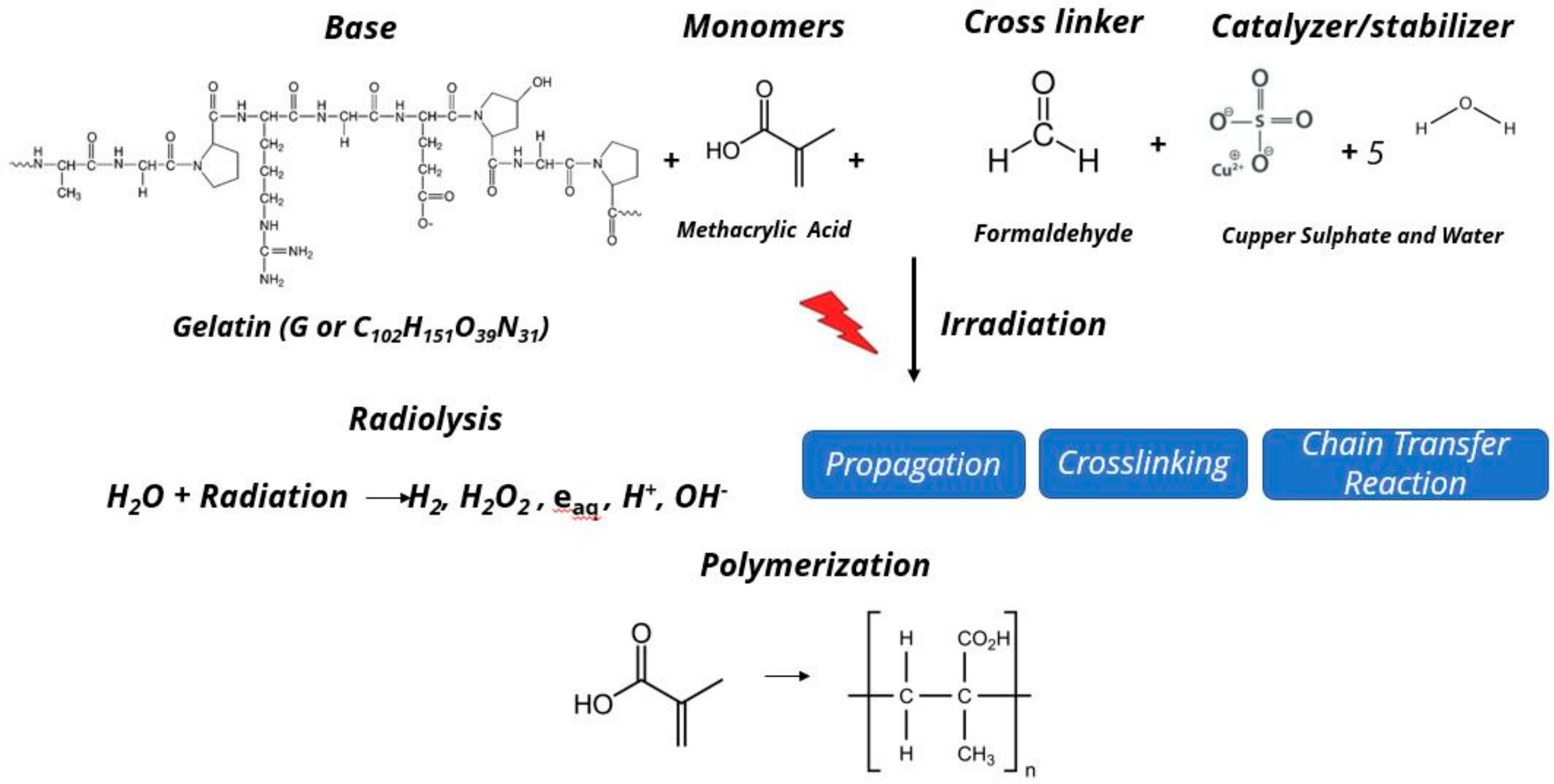
3. MAGIC-Gel Composition and Fabrication
4. Irradiation of MAGIC-f Gel
5. Evaluation of MAGIC-f Gel Dosimeter
6. Application of MAGIC-f Gel
7. Discussion and Future Works
8. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Acknowledgments
Conflicts of Interest
References
- Baldock, C. (Ed.) Historical Overview of the Development of Gel Dosimetry: A Personal Perspective; IOP Publishing: Bristol, UK, 2006; Volume 56, p. 002. [Google Scholar]
- Watanabe, Y.; Warmington, L.; Gopishankar, N. Three-dimensional radiation dosimetry using polymer gel and solid radiochromic polymer: From basics to clinical applications. World J. Radiol. 2017, 9, 112. [Google Scholar] [CrossRef]
- Baldock, C.; De Deene, Y.; Doran, S.; Ibbott, G.; Jirasek, A.; Lepage, M.; McAuley, K.; Oldham, M.; Schreiner, L.J. Polymer gel dosimetry. Phys. Med. Biol. 2010, 55, R1. [Google Scholar] [CrossRef] [PubMed]
- Quevedo, A.L.; Nicolucci, P.; Borges, L.F. Evaluation of the response of modified MAGIC-f polymeric gel using a clinical brachytherapy source and Monte Carlo simulation with package PENELOPE. Rev. Bras. de Fis. Med. (Online) 2016, 10, 2–6. [Google Scholar] [CrossRef]
- Lepage, M.; Jayasakera, P.; Bäck, S.Å.J.; Baldock, C. Dose resolution optimization of polymer gel dosimeters using different monomers. Phys. Med. Biol. 2001, 46, 2665. [Google Scholar] [CrossRef]
- Shevtsov, M.A.; Nikolaev, B.P.; Yakovleva, L.Y.; Marchenko, Y.Y.; Dobrodumov, A.V.; Mikhrina, A.L.; Martynova, M.G.; Bystrova, O.A.; Yakovenko, I.V.; Ischenko, A.M. Superparamagnetic iron oxide nanoparticles conjugated with epidermal growth factor (SPION–EGF) for targeting brain tumors. Int. J. Nanomed. 2014, 9, 273. [Google Scholar] [CrossRef] [Green Version]
- Ab Razak, N.N.A.N.; Abd Rahman, A.; Kandaiya, S.; Shahrim, I.; Zakiah, N.; Yahaya, N.F.Z.; Yann, E.K. Role of anti-oxidants on normoxic methacrylic acid gelatin (MAG) polymer gel dosimeter at 6-MV photon beam using single spin echo MRI. Malays. J. Anal. Sci. 2014, 18, 423–433. [Google Scholar]
- Day, M.; Stein, G. Chemical effects of ionizing radiation in some gels. Nature 1950, 166, 146–147. [Google Scholar] [CrossRef]
- Alexander, P.; Charlesby, A.; Ross, M. The degradation of solid polymethylmethacrylate by ionizing radiation. Proc. R. Soc. Lond. Ser. A Math. Phys. Sci. 1954, 223, 392–404. [Google Scholar]
- Hoecker, F.E.; Watkins, I. Radiation polymerization dosimetry. Int. J. Appl. Radiat. Isotopes. 1958, 3, 31–35. [Google Scholar] [CrossRef]
- Boni, A. A polyacrylamide gamma dosimeter. Radiat. Res. 1961, 14, 374–380. [Google Scholar] [CrossRef]
- Audet, C.; Schreiner, L. (Eds.) Radiation dosimetry by NMR relaxation time measurements of irradiated polymer solutions. In Proceedings of the International Society for Magnetic Resonance in Medicine, San Francisco, CA, USA, 10–16 August 1991. [Google Scholar]
- Gore, J.; Kang, Y. Measurement of radiation dose distributions by nuclear magnetic resonance (NMR) imaging. Phys. Med. Biol. 1984, 29, 1189. [Google Scholar] [CrossRef] [PubMed]
- Fricke, H.; Morse, S. The chemical action of roentgen rays on dilute ferrosulphate solutions as a measure of dose. Am. J. Roentgenol. Radium Ther. Nucl. Med. 1927, 18, 430–432. [Google Scholar]
- Schreiner, L. (Ed.) Review of Fricke gel Dosimeters; IOP Publishing: Bristol, UK, 2004; Volume 3, p. 003. [Google Scholar]
- Kennan, R.; Maryanski, M.; Zhong, J.; Gore, J. Hydrodynamic effects and cross relaxation in cross linked polymer gels. Proc. Int. Soc. Magn. Reson. Med. (New York) 1992, 1, 11. [Google Scholar]
- Spevacek, J.; Dvorak, P.; Cechak, T.; Novotny, J., Jr.; Marek, M. The use of gel dosimetry of Fricke type in three-dimensional dosimetry; DRO: Demanovska Dolina, Slovak Republic, 2001; Volume 1, pp. 129–132. [Google Scholar]
- Appleby, A.; Christman, E.; Leghrouz, A. Imaging of spatial radiation dose distribution in agarose gels using magnetic resonance. Med. Phys. 1987, 14, 382–384. [Google Scholar] [CrossRef] [PubMed]
- Schulz, R.; DeGuzman, A.; Nguyen, D.; Gore, J. Dose-response curves for Fricke-infused agarose gels as obtained by nuclear magnetic resonance. Phys. Med. Biol. 1990, 35, 1611. [Google Scholar] [CrossRef]
- Olsson, L.E.; Westrin, B.A.; Fransson, A.; Nordell, B. Diffusion of ferric ions in agarose dosimeter gels. Phys. Med. Biol. 1992, 37, 2243. [Google Scholar] [CrossRef]
- Baldock, C.; Harris, P.; Piercy, A.; Healy, B. Experimental determination of the diffusion coefficient in two-dimensions in ferrous sulphate gels using the finite element method. Australas. Phys. Eng. Sci. Med. 2001, 24, 19. [Google Scholar] [CrossRef]
- Kron, T.; Jonas, D.; Pope, J.M. Fast T1 imaging of dual gel samples for diffusion measurements in NMR dosimetry gels. Magn. Reson. Imaging 1997, 15, 211–221. [Google Scholar] [CrossRef]
- Maryanski, M.; Gore, J.; Schulz, R. 3-D radiation dosimetry by MRI: Solvent proton relaxation enhancement by radiation-controlled polymerisation and cross-linking in gels. Proc. Int. Soc. Magn. Reson. Med. (New York) 1992. [Google Scholar]
- Maryanski, M.; Schulz, R.; Ibbott, G.; Gatenby, J.; Xie, J.; Horton, D.; Gore, J.C. Magnetic resonance imaging of radiation dose distributions using a polymer-gel dosimeter. Phys. Med. Biol. 1994, 39, 1437. [Google Scholar] [CrossRef]
- Maryanski, M.; Gore, J.; Schulz, R. Three-Dimensional Detection, Dosimetry and Imaging of an Energy Field by Formation of a Polymer in a Gel. U.S. Patent 5,321,357, 14 June 1994. [Google Scholar]
- Baldock, C.; Burford, R.; Billingham, N.; Wagner, G.; Patval, S.; Badawi, R.D.; Keevil, S.F. Experimental procedure for the manufacture and calibration of polyacrylamide gel (PAG) for magnetic resonance imaging (MRI) radiation dosimetry. Phys. Med. Biol. 1998, 43, 695. [Google Scholar] [CrossRef]
- Pappas, E.; Maris, T.; Angelopoulos, A.; Paparigopoulou, M.; Sakelliou, L.; Sandilos, P.; Voyiatzi, S.; Vlachos, L. A new polymer gel for magnetic resonance imaging (MRI) radiation dosimetry. Phys. Med. Biol. 1999, 44, 2677. [Google Scholar] [CrossRef] [PubMed]
- Fong, P.M.; Keil, D.C.; Does, M.D.; Gore, J.C. Polymer gels for magnetic resonance imaging of radiation dose distributions at normal room atmosphere. Phys. Med. Biol. 2001, 46, 3105. [Google Scholar] [CrossRef]
- De Deene, Y.; Venning, A.; Hurley, C.; Healy, B.; Baldock, C. Dose–response stability and integrity of the dose distribution of various polymer gel dosimeters. Phys. Med. Biol. 2002, 47, 2459. [Google Scholar] [CrossRef]
- Senden, R.; De Jean, P.; McAuley, K.; Schreiner, L. Polymer gel dosimeters with reduced toxicity: A preliminary investigation of the NMR and optical dose–response using different monomers. Phys. Med. Biol. 2006, 51, 3301. [Google Scholar] [CrossRef]
- De Deene, Y.; Hurley, C.; Venning, A.; Vergote, K.; Mather, M.; Healy, B.J.; Baldock, C. A basic study of some normoxic polymer gel dosimeters. Phys. Med. Biol. 2002, 47, 3441. [Google Scholar] [CrossRef]
- Fernandes, J.P.; Pastorello, B.F.; de Araújo, D.B.; Baffa, O. (Eds.) Formaldehyde Increases MAGIC Gel Dosimeter Melting Point and Sensitivity; IOP Publishing: Bristol, UK, 2009; Volume 53, p. N53. [Google Scholar]
- Gustavsson, H.; Karlsson, A.; Bäck, S.A.J.; Olsson, L.E.; Haraldsson, P.; Engström, P.; Nyström, H. MAGIC-type polymer gel for three-dimensional dosimetry: Intensity-modulated radiation therapy verification. Med. Phys. 2003, 30, 1264–1271. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Marques, T.; Schwarcke, M.; Garrido, C.; Baffa, O.; Nicolucci, P. (Eds.) Dosimetric Properties of MAGIC-f Polymer Gel Assessed to Radiotherapy Clinical Beams; IOP Publishing: Bristol, UK, 2010; Volume 250, p. 012012. [Google Scholar]
- Pavoni, J.; Baffa, O. An evaluation of dosimetric characteristics of MAGIC gel modified by adding formaldehyde (MAGIC-f). Radiat. Meas. 2012, 47, 1074–1082. [Google Scholar] [CrossRef]
- Pavoni, J.; Pike, T.; Snow, J.; DeWerd, L.; Baffa, O. Tomotherapy dose distribution verification using MAGIC-f polymer gel dosimetry. Med. Phys. 2012, 39, 2877–2884. [Google Scholar] [CrossRef] [PubMed]
- Heufelder, J.; Stiefel, S.; Pfaender, M.; Lüdemann, L.; Grebe, G.; Heese, J. Use of BANG® polymer gel for dose measurements in a 68 MeV proton beam. Med. Phys. 2003, 30, 1235–1240. [Google Scholar] [CrossRef]
- Gustavsson, H.; Bäck, S.Å.J.; Medin, J.; Grusell, E.; Olsson, L.E. Linear energy transfer dependence of a normoxic polymer gel dosimeter investigated using proton beam absorbed dose measurements. Phys. Med. Biol. 2004, 49, 3847. [Google Scholar] [CrossRef]
- Zeidan, O.; Sriprisan, S.; Lopatiuk-Tirpak, O.; Kupelian, P.; Meeks, S.; Hsi, W.; Li, Z.; Palta, J.R.; Maryanski, M.J. Dosimetric evaluation of a novel polymer gel dosimeter for proton therapy. Med. Phys. 2010, 37, 2145–2152. [Google Scholar] [CrossRef]
- Jirasek, A.; Duzenli, C. Relative effectiveness of polyacrylamide gel dosimeters applied to proton beams: Fourier transform Raman observations and track structure calculations. Med. Phys. 2002, 29, 569–577. [Google Scholar] [CrossRef]
- Lopatiuk-Tirpak, O.; Su, Z.; Li, Z.; Zeidan, O.; Meeks, S.; Maryanski, M. Direct response to proton beam linear energy transfer (LET) in a novel polymer gel dosimeter formulation. Technol. Cancer Res. Treat. 2012, 11, 441–445. [Google Scholar] [CrossRef]
- Gustavsson, H.; Bäck, S.Å.J.; Lepage, M.; Rintoul, L.; Baldock, C. Development and optimization of a 2-hydroxyethylacrylate MRI polymer gel dosimeter. Phys. Med. Biol. 2004, 49, 227. [Google Scholar] [CrossRef]
- Bäck, S.Å.J.; Medin, J.; Magnusson, P.; Olsson, P.; Grusell, E.; Olsson, L.E. Ferrous sulphate gel dosimetry and MRI for proton beam dose measurements. Phys. Med. Biol. 1999, 44, 1983. [Google Scholar] [CrossRef] [PubMed]
- Pianoschi, T.; Alva, M.; Santanna, M.; Baffa, O.; Nicolucci, P. MAGIC-f Gel Dosimetry for Clinical Electron Beam; IOP Publishing: Bristol, UK, 2010; Volume 250, p. 012037. [Google Scholar]
- Oldham, M.; Siewerdsen, J.H.; Shetty, A.; Jaffray, D.A. High resolution gel-dosimetry by optical-CT and MR scanning. Med. Phys. 2001, 28, 1436–1445. [Google Scholar] [CrossRef] [Green Version]
- Hilts, M.; Audet, C.; Duzenli, C.; Jirasek, A. Polymer gel dosimetry using x-ray computed tomography: A feasibility study4. Phys. Med. Biol. 2000, 45, 2559. [Google Scholar] [CrossRef] [PubMed]
- De Deene, Y.; De Wagter, C.; Van Duyse, B.; Derycke, S.; De Neve, W.; Achten, E. Three-dimensional dosimetry using polymer gel and magnetic resonance imaging applied to the verification of conformal radiation therapy in head-and-neck cancer. Radiother. Oncol. 1998, 48, 283–291. [Google Scholar] [CrossRef]
- Maryanski, M.J.; Gore, J.C.; Kennan, R.P.; Schulz, R.J. NMR relaxation enhancement in gels polymerized and cross-linked by ionizing radiation: A new approach to 3D dosimetry by MRI. Magn. Reson. Imaging 1993, 11, 253–258. [Google Scholar] [CrossRef]
- Mather, M.L.; De Deene, Y.; Whittaker, A.K.; Simon, G.P.; Rutgers, R.; Baldock, C. Investigation of ultrasonic properties of PAG and MAGIC polymer gel dosimeters. Phys. Med. Biol. 2002, 47, 4397. [Google Scholar] [CrossRef]
- Mather, M.L.; Whittaker, A.K.; Baldock, C. Ultrasound evaluation of polymer gel dosimeters. Phys. Med. Biol. 2002, 47, 1449. [Google Scholar] [CrossRef]
- Baldock, C.; Rintoul, L.; Keevil, S.; Pope, J.; George, G. Fourier transform Raman spectroscopy of polyacrylamide gels (PAGs) for radiation dosimetry. Phys. Med. Biol. 1998, 43, 3617. [Google Scholar] [CrossRef]
- Trapp, J.; Bäck, S.Å.J.; Lepage, M.; Michael, G.; Baldock, C. An experimental study of the dose response of polymer gel dosimeters imaged with x-ray computed tomography. Phys. Med. Biol. 2001, 46, 2939. [Google Scholar] [CrossRef] [PubMed]
- Masoumi, H.; Mokhtari-Dizaji, M.; Arbabi, A.; Bakhshandeh, M. Determine the dose distribution using ultrasound parameters in MAGIC-f polymer gels. Dose-Response 2016, 14, 1559325815625647. [Google Scholar] [CrossRef] [Green Version]
- Watanabe, Y.; Kubo, H. A variable echo-number method for estimating in MRI-based polymer gel dosimetry. Med. Phys. 2011, 38, 975–982. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ibbott, G.S. (Ed.) Applications of Gel Dosimetry; IOP Publishing: Bristol, UK, 2004; Volume 3, p. 007. [Google Scholar]
- McJury, M.; Oldham, M.; Cosgrove, V.P.; Murphy, P.S.; Doran, S.; O Leach, M.; Webb, S. Radiation dosimetry using polymer gels: Methods and applications. Br. J. Radiol. 2000, 73, 919–929. [Google Scholar] [CrossRef]
- MacDougall, N.; Pitchford, W.; Smith, M. A systematic review of the precision and accuracy of dose measurements in photon radiotherapy using polymer and Fricke MRI gel dosimetry. Phys. Med. Biol. 2002, 47, R107. [Google Scholar] [CrossRef]
- Andrews, H.L.; Murphy, R.E.; LeBrun, E.J. Gel dosimeter for depth-dose measurements. Rev. Sci. Instrum. 1957, 28, 329–332. [Google Scholar] [CrossRef]
- Haraldsson, P.; Bäck, S.; Magnusson, P.; Olsson, L. Dose response characteristics and basic dose distribution data for a polymerization-based dosemeter gel evaluated using MR. Br. J. Radiol. 2000, 73, 58–65. [Google Scholar] [CrossRef]
- Oldham, M.; Baustert, I.; Lord, C.; Smith, T.A.D.; McJury, M.; Warrington, A.P.; O Leach, M.; Webb, S. An investigation into the dosimetry of a nine-field tomotherapy irradiation using BANG-gel dosimetry. Phys. Med. Biol. 1998, 43, 1113. [Google Scholar] [CrossRef] [PubMed]
- Baldock, C.; Hasler, C.; Keevil, S.; Greener, A.; Billingham, N.; Burford, R. A dosimetry phantom for external beam radiation therapy of the breast using radiation-sensitive polymer gels and MRI. Med. Phys. 1996, 23, 1490. [Google Scholar]
- Love, P.; Evans, P.; Leach, M.; Webb, S. Polymer gel measurement of dose homogeneity in the breast: Comparing MLC intensity modulation with standard wedged delivery. Phys. Med. Biol. 2003, 48, 1065. [Google Scholar] [CrossRef]
- Trapp, J.; Partridge, M.; Hansen, V.N.; Childs, P.; Bedford, J.; Warrington, A.P.; O Leach, M.; Webb, S. The use of gel dosimetry for verification of electron and photon treatment plans in carcinoma of the scalp. Phys. Med. Biol. 2004, 49, 1625. [Google Scholar] [CrossRef] [PubMed]
- Hill, B.; Venning, A.; Baldock, C. The dose response of normoxic polymer gel dosimeters measured using X-ray CT. Br. J. Radiol. 2005, 78, 623–630. [Google Scholar] [CrossRef]
- Webb, S. The Physics of Conformal Radiotherapy: Advances in Technology (PBK); CRC Press: Boca Raton, FL, USA, 1997. [Google Scholar]
- Schreiner, L.; Crooks, I.; Evans, M.; Keller, B.; Parker, W. Imaging of HDR brachytherapy dose distributions using NMR Fricke-gelatin dosimetry. Magn. Reson. Imaging 1994, 12, 901–907. [Google Scholar] [CrossRef]
- Olsen, D.; Hellesnes, J. Absorbed dose distribution measurements in brachytherapy using ferrous sulphate gel and magnetic resonance imaging. Br. J. Radiol. 1994, 67, 1121–1126. [Google Scholar] [CrossRef]
- Gelfi, C.; Righetti, P.G. Polymerization kinetics of polyacrylamide gels II. Effect of temperature. Electrophoresis 1981, 2, 220–228. [Google Scholar] [CrossRef]
- Maryanski, M.; Audet, C.; Gore, J. Effects of crosslinking and temperature on the dose response of a BANG polymer gel dosimeter. Phys. Med. Biol. 1997, 42, 303. [Google Scholar] [CrossRef]
- Omidian, H.; Hashemi, S.; Sammes, P.; Meldrum, I. Modified acrylic-based superabsorbent polymers. Effect of temperature and initiator concentration. Polymer 1998, 39, 3459–3466. [Google Scholar] [CrossRef]
- Gambarini, G.; Gomarasca, G.; Marchesini, R.; Pecci, A.; Pirola, L.; Tomatis, S. Three-dimensional determination of absorbed dose by spectrophotometric analysis of ferrous-sulphate agarose gel. Nucl. Instrum. Methods Phys. Res. Sect. A: Accel. Spectrometers Detect. Assoc. Equip. 1999, 422, 643–648. [Google Scholar] [CrossRef]
- Gambarini, G. Gel Dosimetry in Neutron Capture Therapy. In Proceedings of the DOSGEL 2001, 2nd International Conference on Radiotherapy Gel Dosimetry, Brisbane, Australia, 18–21 November 2001; p. 92. [Google Scholar]
- Gambarini, G.; Birattari, C.; Colombi, C.; Pirola, L.; Rosi, G. Fricke gel dosimetry in boron neutron capture therapy. Radiat. Prot. Dosim. 2002, 101, 419–422. [Google Scholar] [CrossRef] [PubMed]
- Antoniou, P.; Bousbouras, P.; Sandaltzopoulos, R.; Kaldoudi, E. Investigating the potential of polymer gel dosimetry for interventional radiology: First results. Phys. Med. Biol. 2008, 53, N127. [Google Scholar] [CrossRef] [PubMed]
- Maryanski, M.; Schulz, R.; Gore, G. Three dimensional dose distributions for 160 MeV protons using MRI of the tissue-equivalent BANG polymer-gel dosimeter. In Proceedings of the PTCOG Newsletter, MA, USA, 1994; Volume 14, pp. 10–11. [Google Scholar]
- Schubert, J. Radiation Chemistry—An Introduction: AJ Swallow; Longman Group, Ltd.: Pergamon, Turkey; London, UK, 1973; p. 275. [Google Scholar]
- Ramm, U.W.U.; Bocks, M.; Kraemer, M.; Bankamp, A.; Damrau, M.; Thilman, C.; Bottcher, H.D.; LaK, G.S. Three-dimensional BANG™gel dosimetry in conformal carbon. Phys. Med. Biol. 2000, 45, N95. [Google Scholar] [CrossRef] [PubMed]
- Pantelis, E.; Karlis, A.; Kozicki, M.; Papagiannis, P.; Sakelliou, L.; Rosiak, J. Polymer gel water equivalence and relative energy response with emphasis on low photon energy dosimetry in brachytherapy. Phys. Med. Biol. 2004, 49, 3495. [Google Scholar] [CrossRef]
- Vergote, K.; De Deene, Y.; Claus, F.; De Gersem, W.; Van Duyse, B.; Paelinck, L.; Achten, E.; De Neve, W.; De Wagter, C. Application of monomer/polymer gel dosimetry to study the effects of tissue inhomogeneities on intensity-modulated radiation therapy (IMRT) dose distributions. Radiother. Oncol. 2003, 67, 119–128. [Google Scholar] [CrossRef]
- Gum, F.; Scherer, J.; Bogner, L.; Solleder, M.; Rhein, B.; Bock, M. Preliminary study on the use of an inhomogeneous anthropomorphic Fricke gel phantom and 3D magnetic resonance dosimetry for verification of IMRT treatment plans. Phys. Med. Biol. 2002, 47, N67. [Google Scholar] [CrossRef]
- Ølberg, S.; Skretting, A.; Bruland, Ø.; Olsen, D.R. Dose distribution measurements by MRI of a phantom containing lung tissue equivalent compartments made of ferrous sulphate gel. Phys. Med. Biol. 2000, 45, 2761. [Google Scholar] [CrossRef] [PubMed]
- Borges, J.; BenComo, J.; Ibbott, G. A 3 Dimensional Gel Dosimetry Lung Equivalent (WIP). In Proceedings of the AAPM Annual Meeting, San Diego, CA, USA, 10–14 August 2003. [Google Scholar]
- Schwarcke, M.; Marques, T.; Garrido, C.; Nicolucci, P.; Baffa, O. (Eds.) MAGIC-f Gel in Nuclear Medicine Dosimetry: Study in an External Beam of Iodine-131; IOP Publishing: Bristol, UK, 2010; Volume 250, p. 012082. [Google Scholar]
- da Silveira, M.A.; Pavoni, J.F.; Salmon, C.E.G.; Baffa, O. Tridimensional dosimetry for prostate IMRT treatments using MAGIC-f gel by MRI. Radiat. Meas. 2014, 71, 369–373. [Google Scholar] [CrossRef]
- Quevedo, A.; Luo, G.; Galhardo, E.; Price, M.; Nicolucci, P.; Gore, J.C.; Zu, Z. Polymer gel dosimetry by nuclear Overhauser enhancement (NOE) magnetic resonance imaging. Phys. Med. Biol. 2018, 63, 15NT03. [Google Scholar] [CrossRef]
- Alva, M.; Pianoschi, T.; Takeda, F.; Alves, T.; Haddad, C.; Nicolucci, P. SU-GG-I-90: Dose Distribution of Small Fields through MAGIC-F Gel Dosimetry and PENELOPE-Monte Carlo Simulation. Med. Phys. 2010, 37, 3122. [Google Scholar] [CrossRef]
- Alva, M.; Pianoschi, T.; Marques, T.; Santanna, M.M.; Baffa, O.; Nicolucci, P. Monte Carlo Simulation of MAGIC-f gel for Radiotherapy using PENELOPE. JPhCS 2010, 250, 012067. [Google Scholar]
- Khosravi, H.; Ghazikhanlousani, K.; Rahimi, A. Use of gold nanoparticles in MAGIC-f gels to 18 MeV photon enhancement. Nanomed. J. 2019, 6, 67–73. [Google Scholar]
- Watanabe, Y.; Perera, G.M.; Mooij, R.B. Image distortion in MRI-based polymer gel dosimetry of gamma knife stereotactic radiosurgery systems. Med. Phys. 2002, 29, 797–802. [Google Scholar] [CrossRef] [PubMed]
- Hilts, M.; Jirasek, A.; Duzenli, C. Technical considerations for implementation of x-ray CT polymer gel dosimetry. Phys. Med. Biol. 2005, 50, 1727. [Google Scholar] [CrossRef] [PubMed]
- Brown, S.; Venning, A.; De Deene, Y.; Vial, P.; Oliver, L.; Adamovics, J.; Baldock, C. Radiological properties of the PRESAGE and PAGAT polymer dosimeters. Appl. Radiat. Isot. 2008, 66, 1970–1974. [Google Scholar] [CrossRef] [PubMed]
- Haraldsson, P.; Karlsson, A.; Wieslander, E.; Gustavsson, H.; Bäck, S.Å.J. Dose response evaluation of a low-density normoxic polymer gel dosimeter using MRI. Phys. Med. Biol. 2006, 51, 919. [Google Scholar] [CrossRef] [PubMed]


| Studies | Environment/Conditions | Evaluation and Comparison Method | Result |
|---|---|---|---|
| Pavoni et al., 2012 [35] | MAGIC-f gel with 3% formaldehyde | MRI | High thermal stability. Dependence on varying among of dose, dose rate and fractionation is very less. |
| Pavoni et al., 2012 [36] | Tomotherapy device | MRI | A high similarity was found in the comparison of dose distribution measured from the gel and calculated from the treatment planning system (TPS). |
| Khosravi et al., 2019 [87] | Gold nano particles (GNP) are embedded in MAGIC-f gel | MRI and Geant4 | Percentage depth dose (PDD) of GNP embedded MAGIC-f gel is enhanced when exposed to 18 MeV photons. |
| Schwarcke et al., 2010 [83] | MAGIC-f gel is exposed to 131I source. | MRI and PENELOPE | Monte Carlo simulation is more accurate for MAGIC-f gel dosimetry than dosimetry of thermo luminescent (TLD), thus showing its potential in application in nuclear medicine. |
| Silveira et al., 2014 [84] | Intensity-modulated radiation therapy (IMRT) treatments | MRI | Qualifies the quality assurance standard of the IMRT treatment system. |
| Pianoschi et al., 2010 [43] | MAGIC-f gel is exposed to 6 MeV electron beam | MRI | Feasible to calculate PDDs and beam profile in electron beam therapy. |
| Quevedo et al., 2016 [4] | Clinical brachytherapy. | MRI and PENELOPE | Effective in dosimetry of the high gradient source used in clinical brachytherapy. |
| Marques et al., 2012 [34] | Various Beams used in Radiotherapy | MRI and PENELOPE | Shows linear relationship to all energies produced by different beams used in radiotherapy. |
| Alva et al., 2010 [87]. | Conformal radiation therapy | PENELOPE and MRI | Effective in using small fields, especially in radiosurgery and in dosimetric calculation in conformal radiation therapy. |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Dhakal, R.; Yosofvand, M.; Moussa, H. Development and Application of MAGIC-f Gel in Cancer Research and Medical Imaging. Appl. Sci. 2021, 11, 7783. https://doi.org/10.3390/app11177783
Dhakal R, Yosofvand M, Moussa H. Development and Application of MAGIC-f Gel in Cancer Research and Medical Imaging. Applied Sciences. 2021; 11(17):7783. https://doi.org/10.3390/app11177783
Chicago/Turabian StyleDhakal, Rabin, Mohammad Yosofvand, and Hanna Moussa. 2021. "Development and Application of MAGIC-f Gel in Cancer Research and Medical Imaging" Applied Sciences 11, no. 17: 7783. https://doi.org/10.3390/app11177783
APA StyleDhakal, R., Yosofvand, M., & Moussa, H. (2021). Development and Application of MAGIC-f Gel in Cancer Research and Medical Imaging. Applied Sciences, 11(17), 7783. https://doi.org/10.3390/app11177783








