The Effect of External Fixator Configurations on the Dynamic Compression Load: An Experimental and Numerical Study
Abstract
Featured Application
Abstract
1. Introduction
2. Materials and Methods
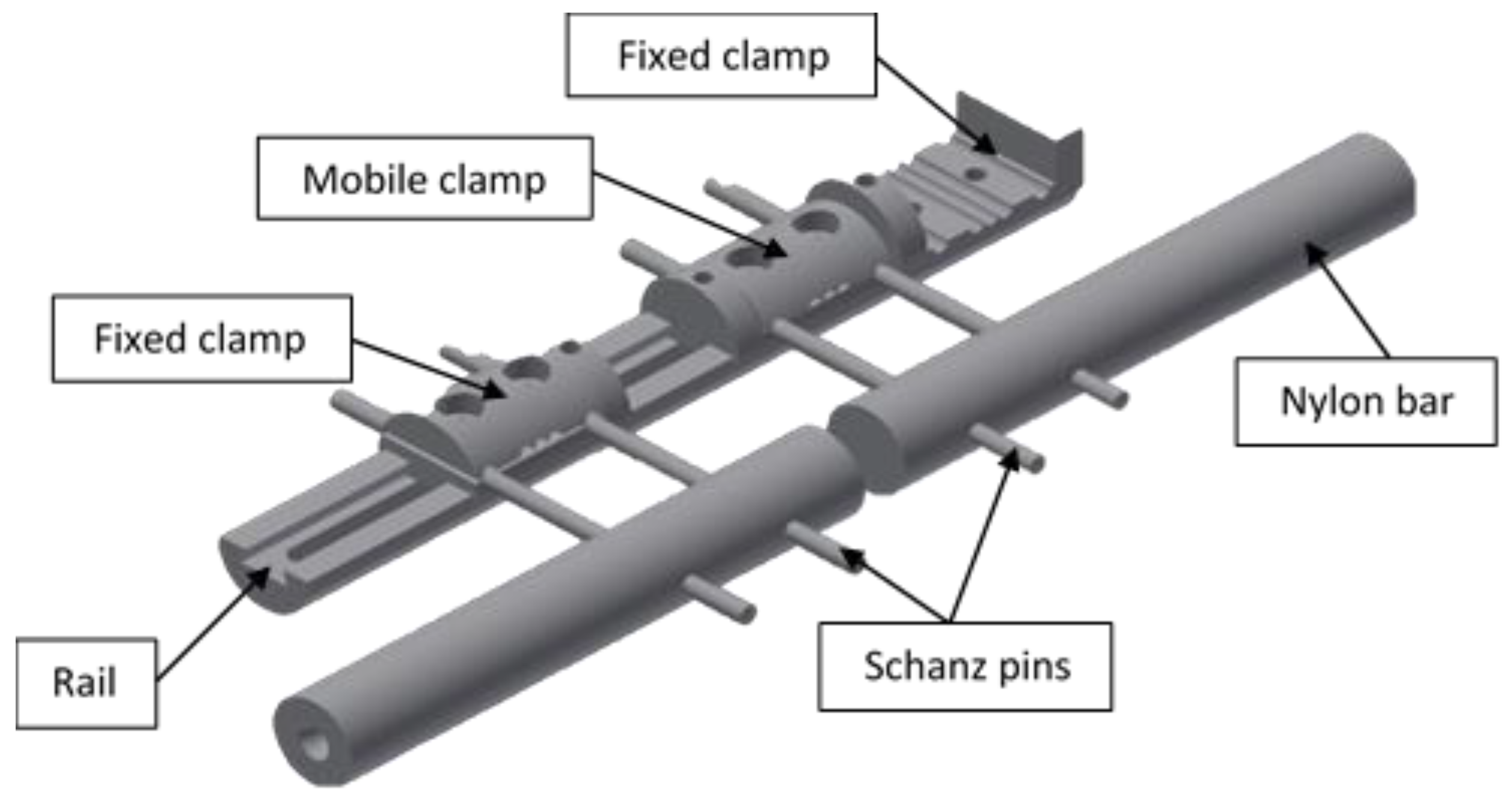
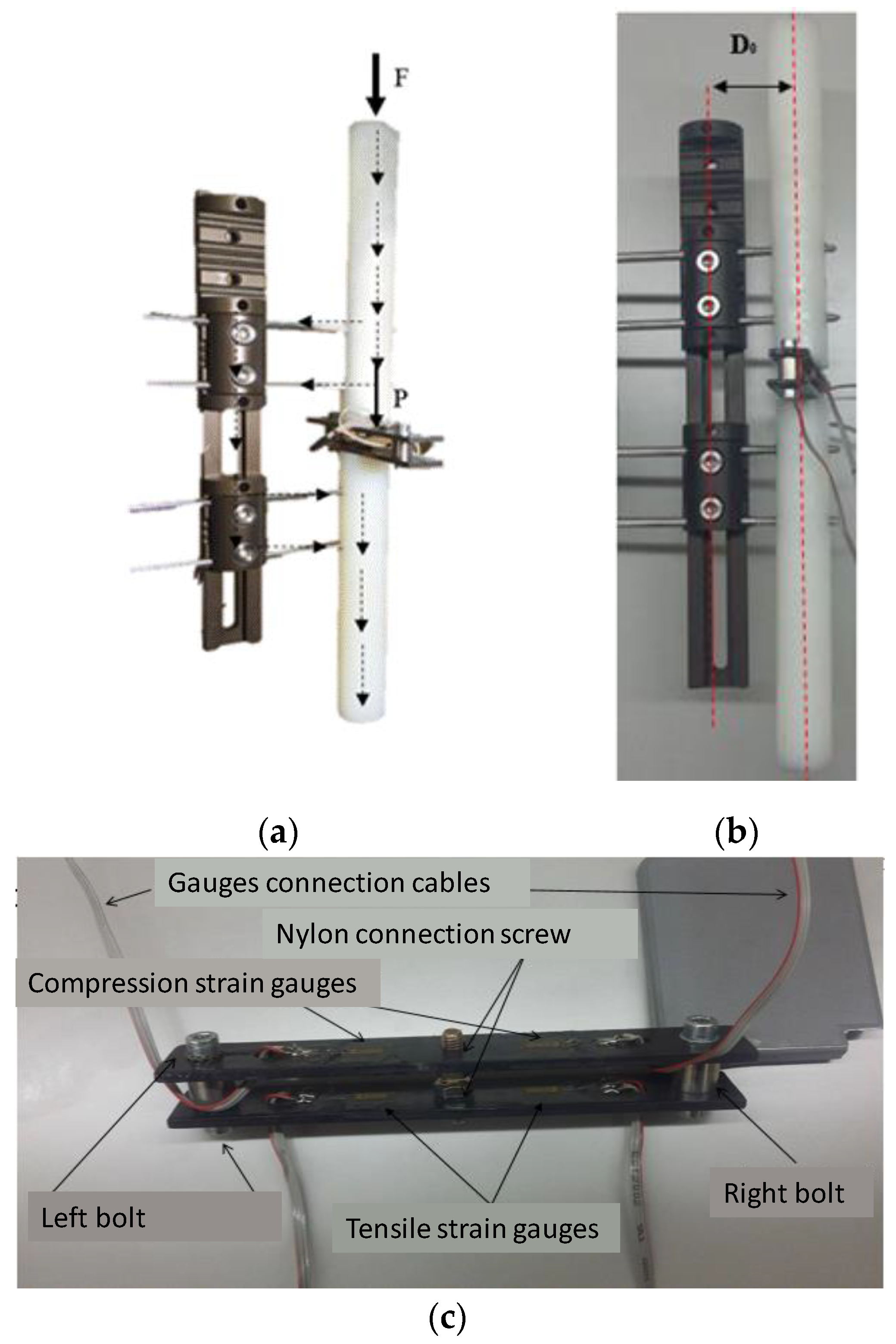
2.1. Experimental Measurements
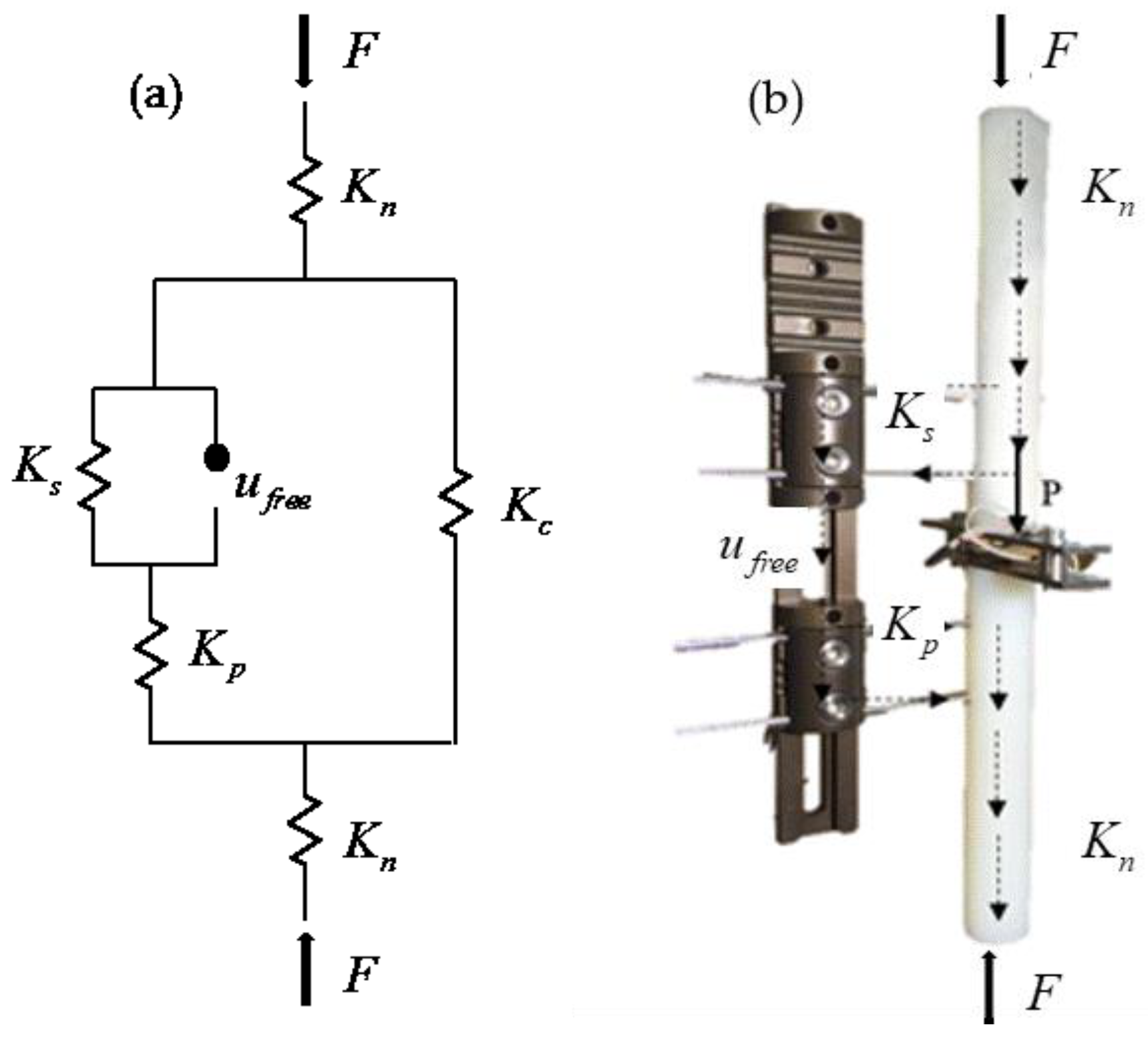
2.2. Finite Element Modeling
2.3. Validation Procedure
3. Results
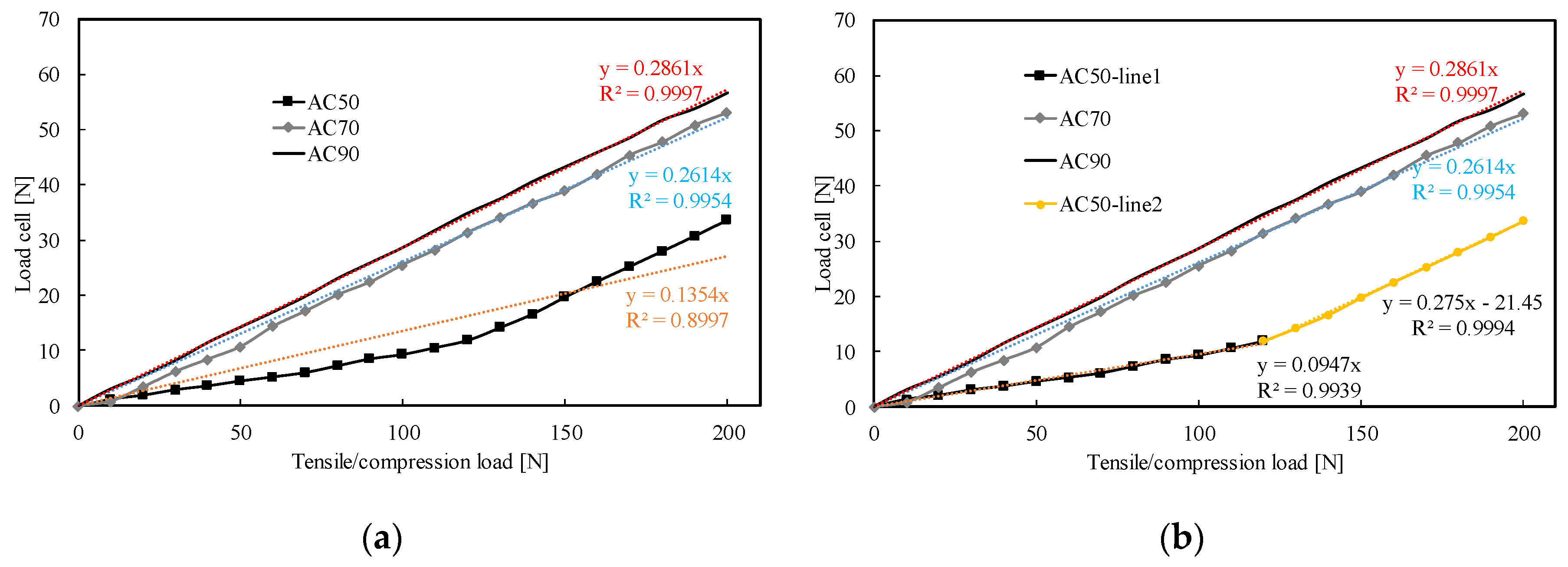
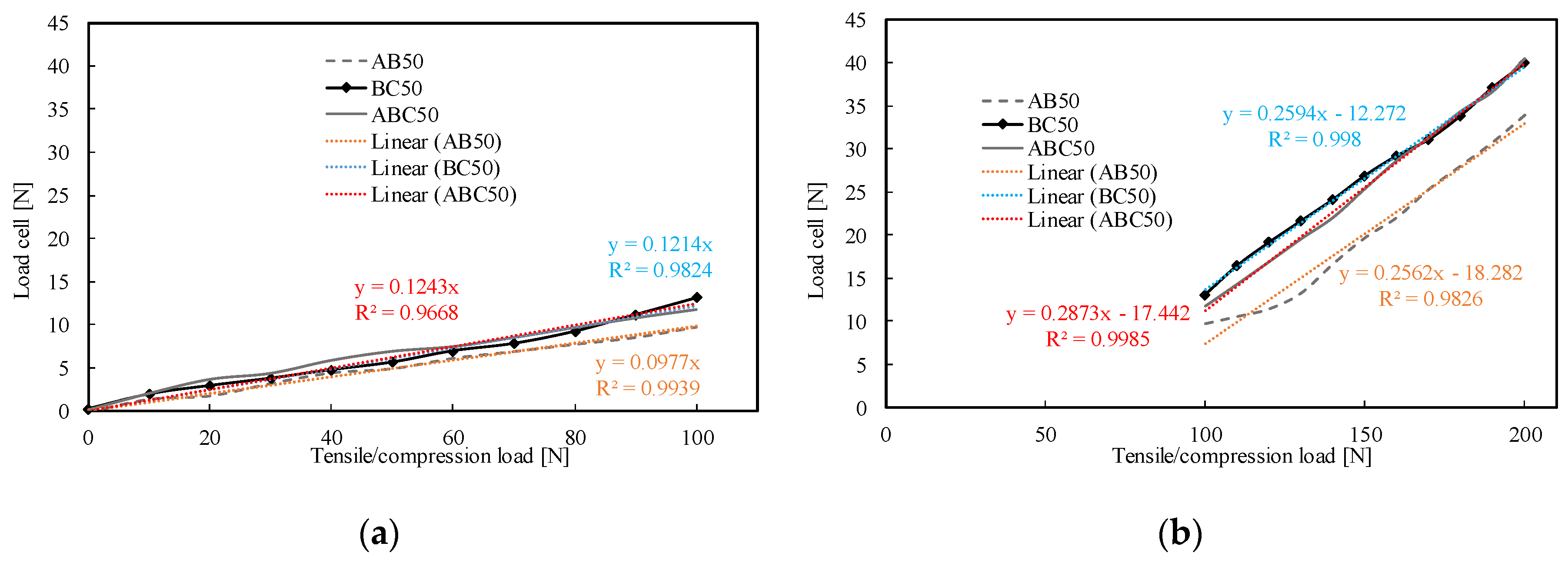
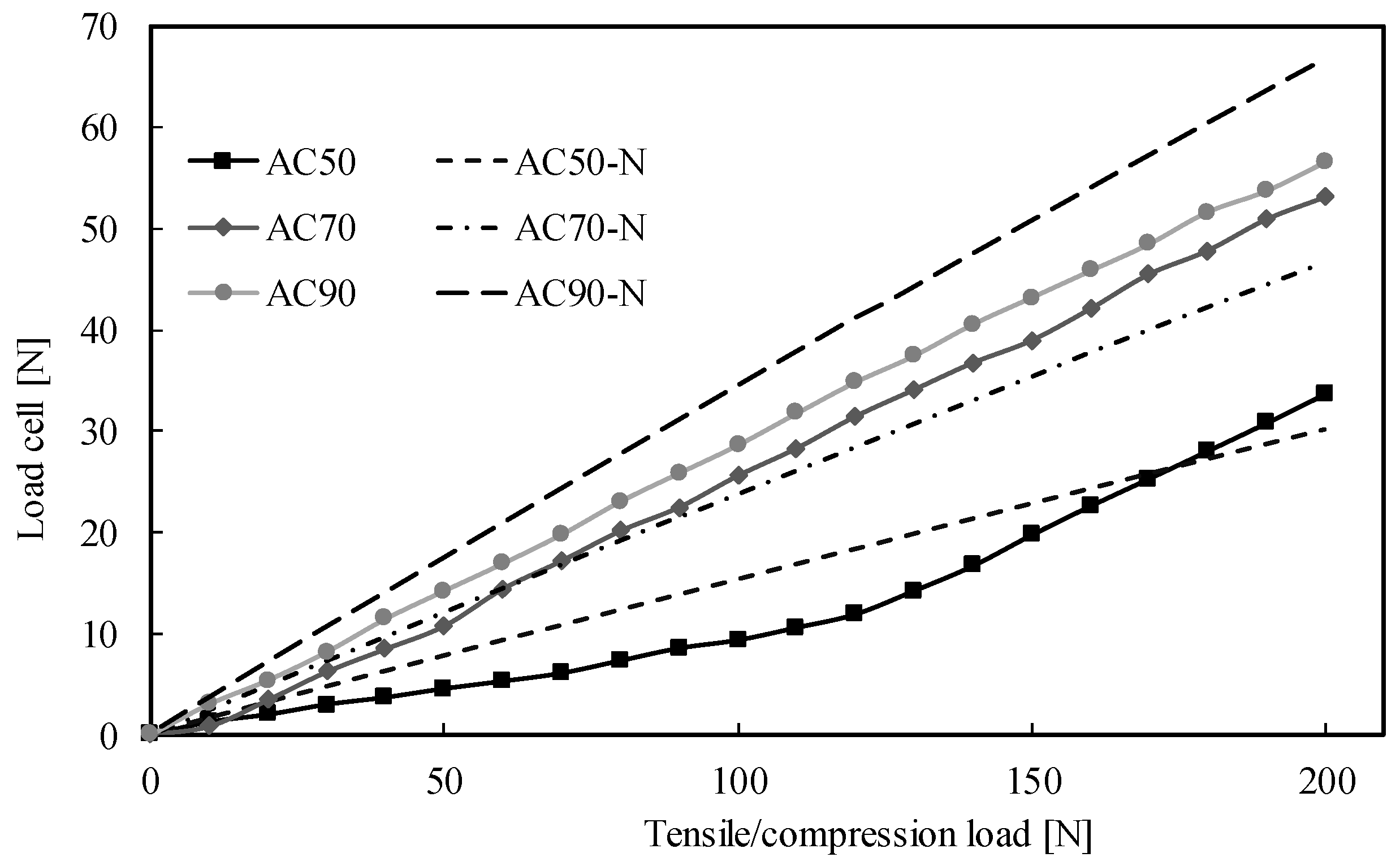
3.1. Experimental Results
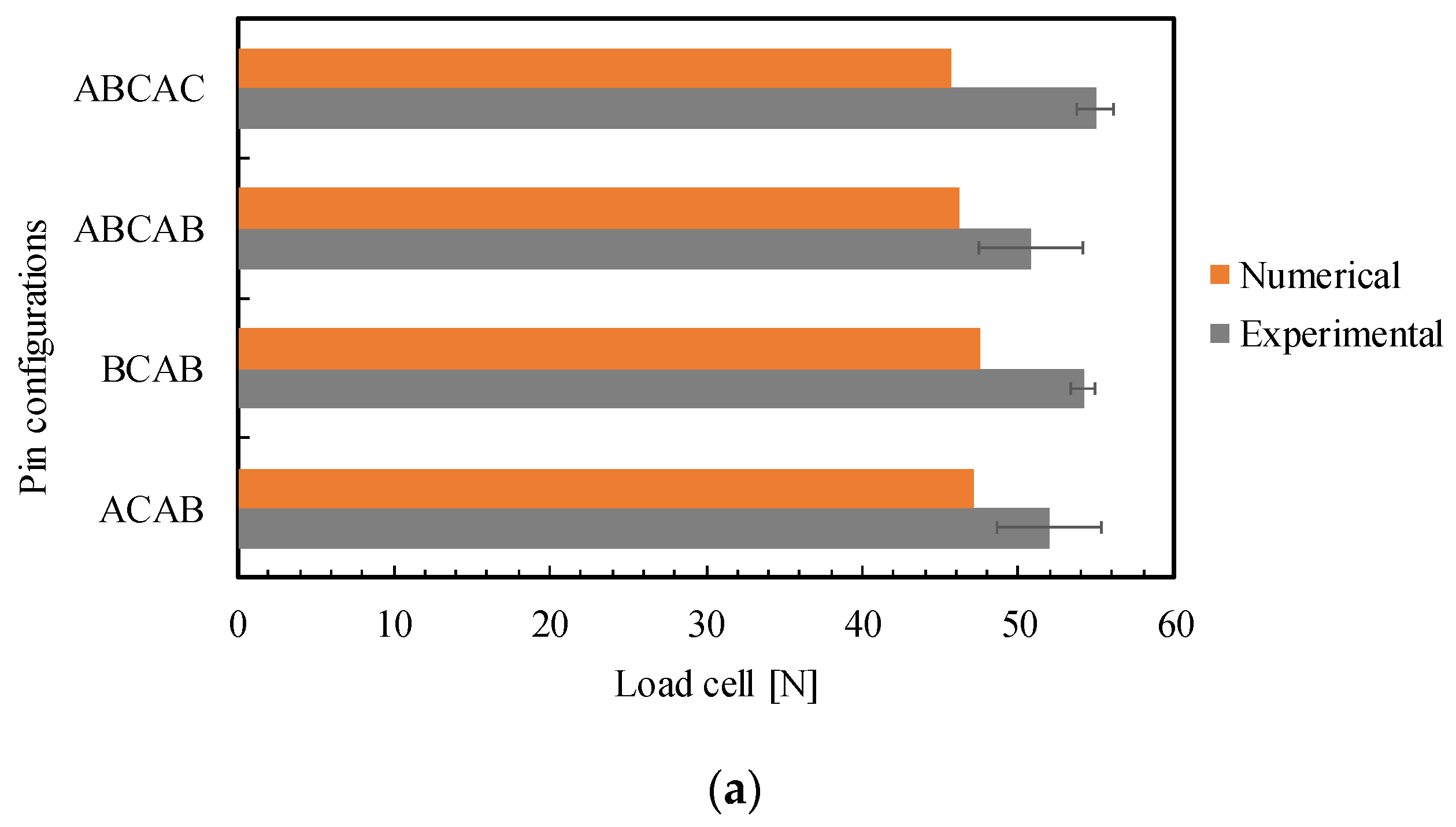
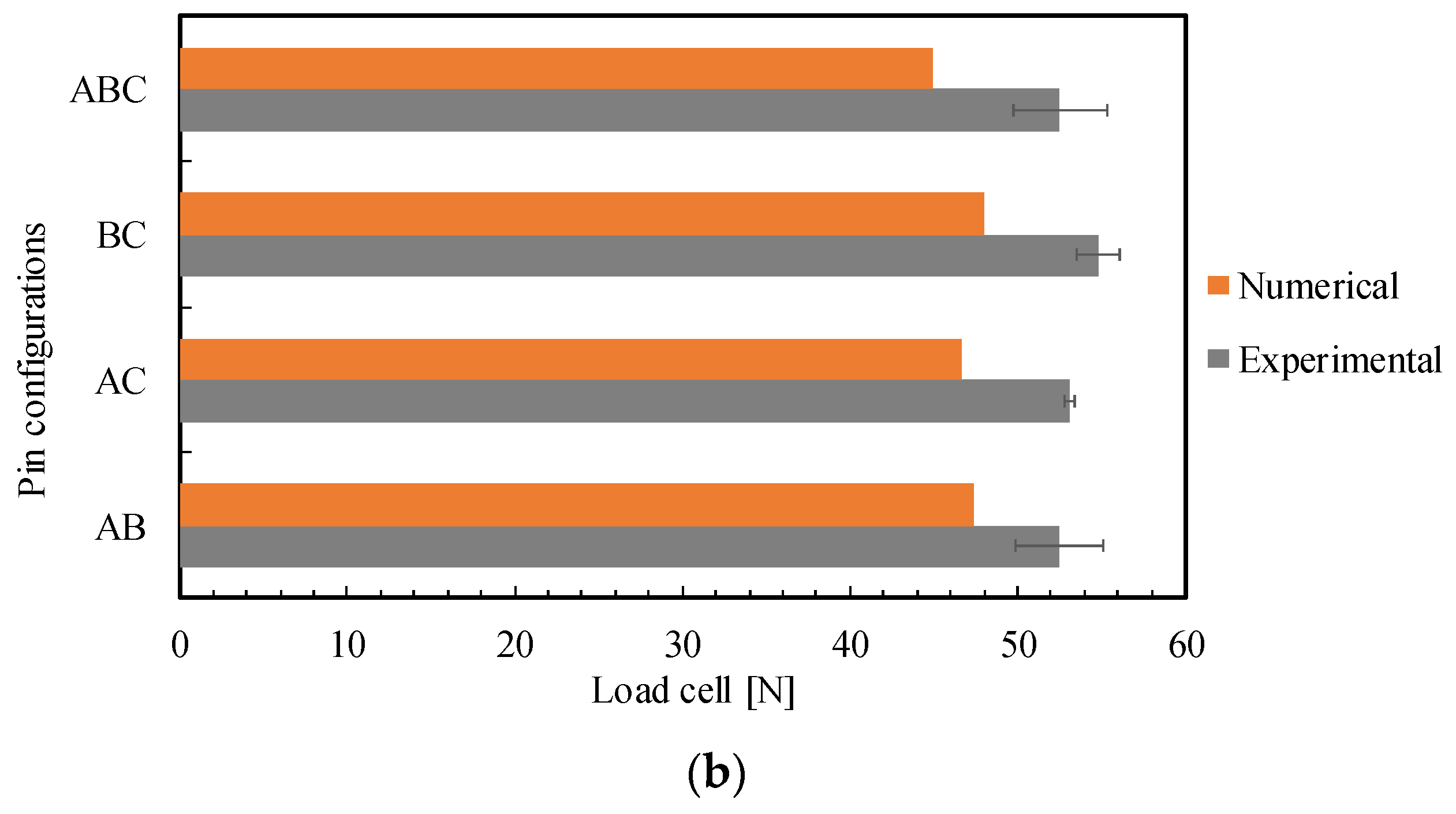
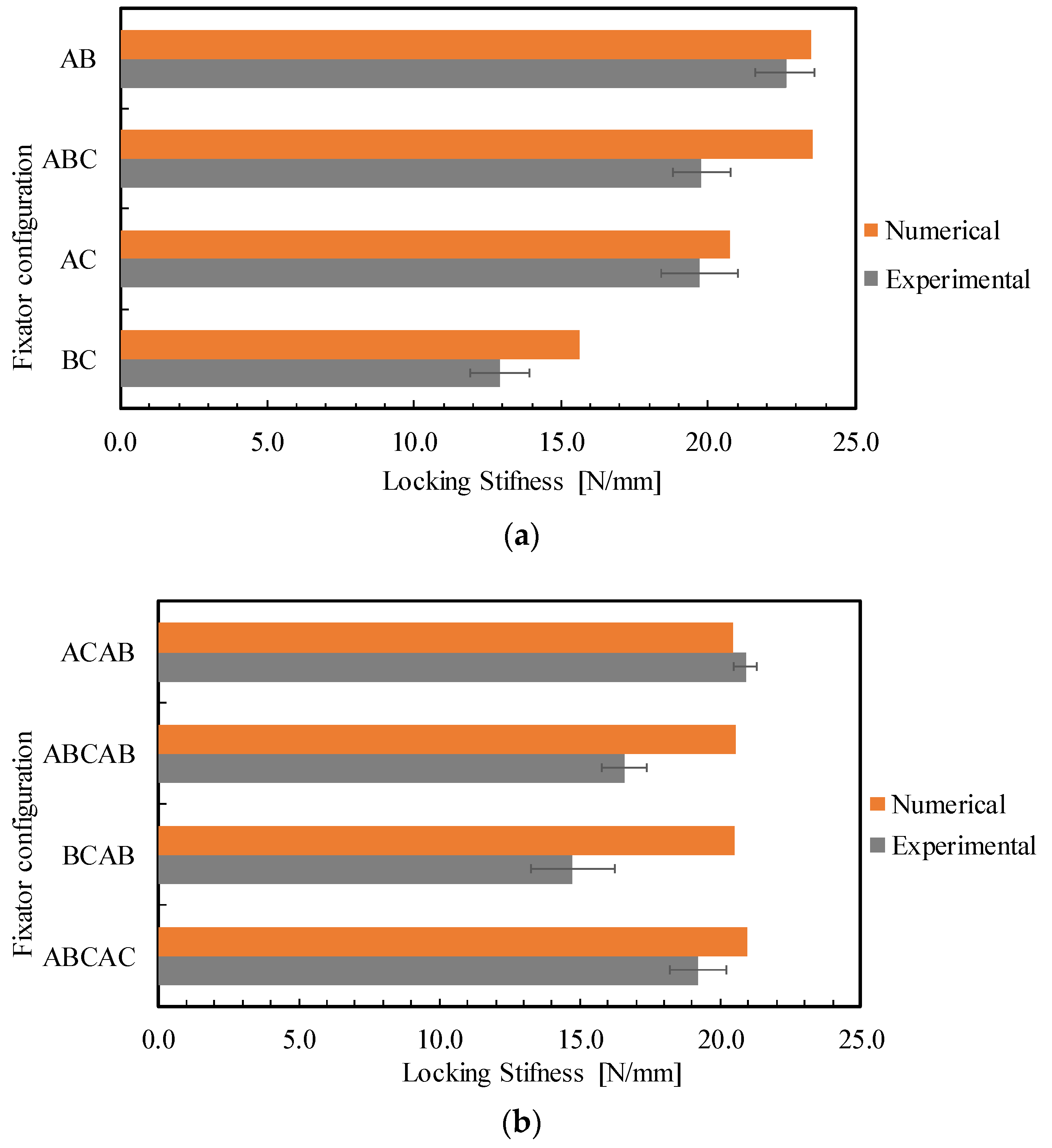
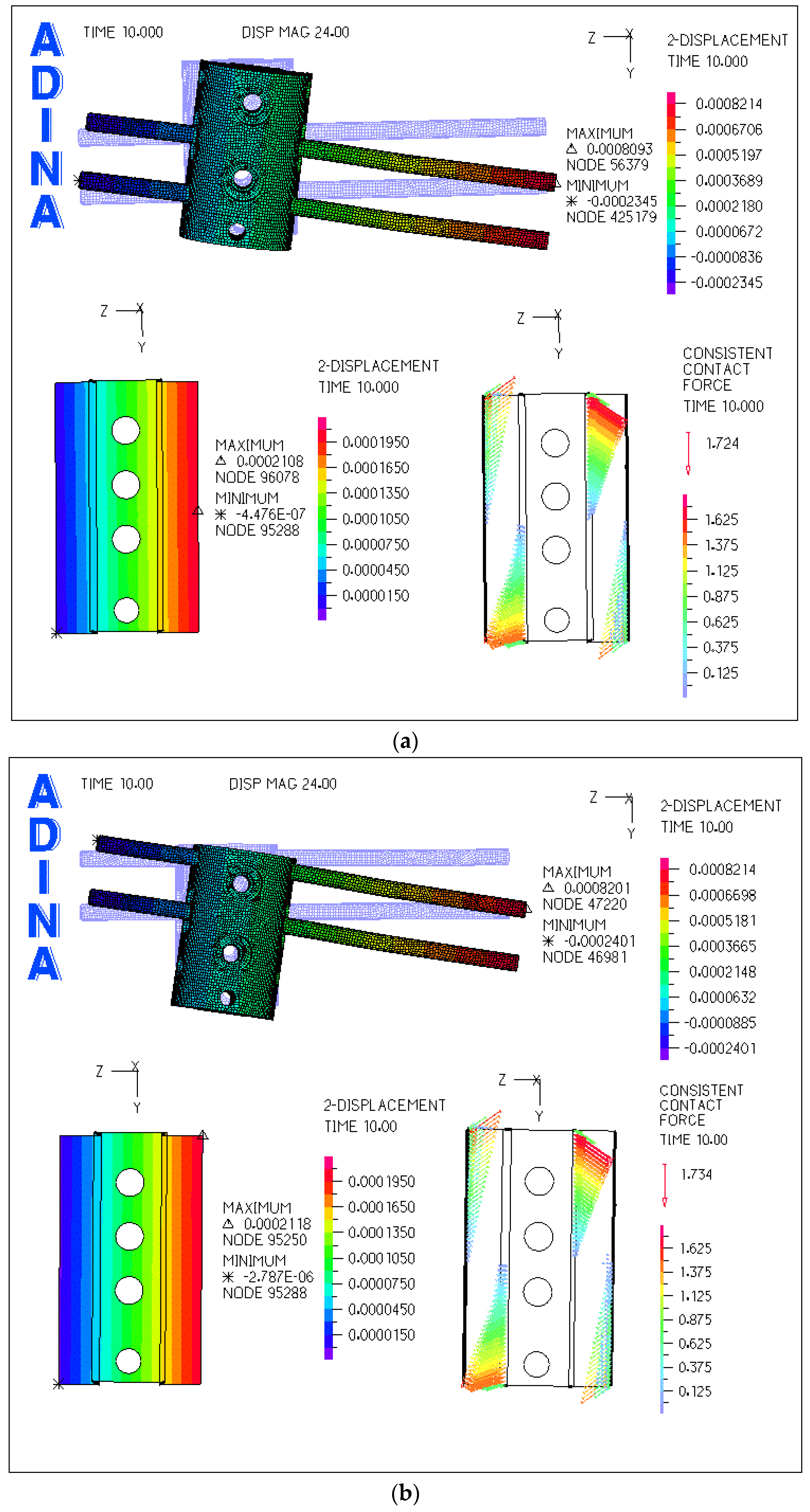
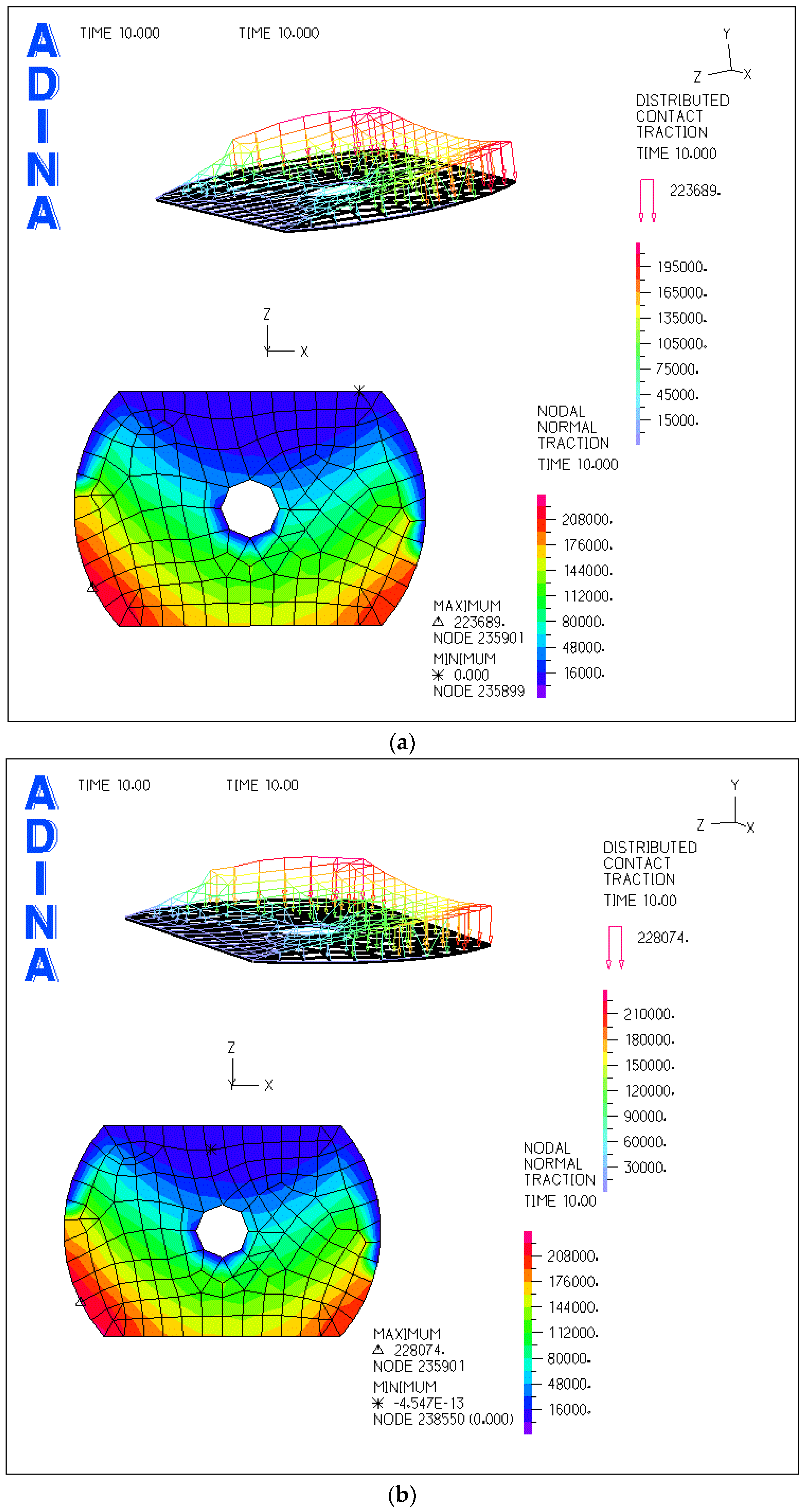
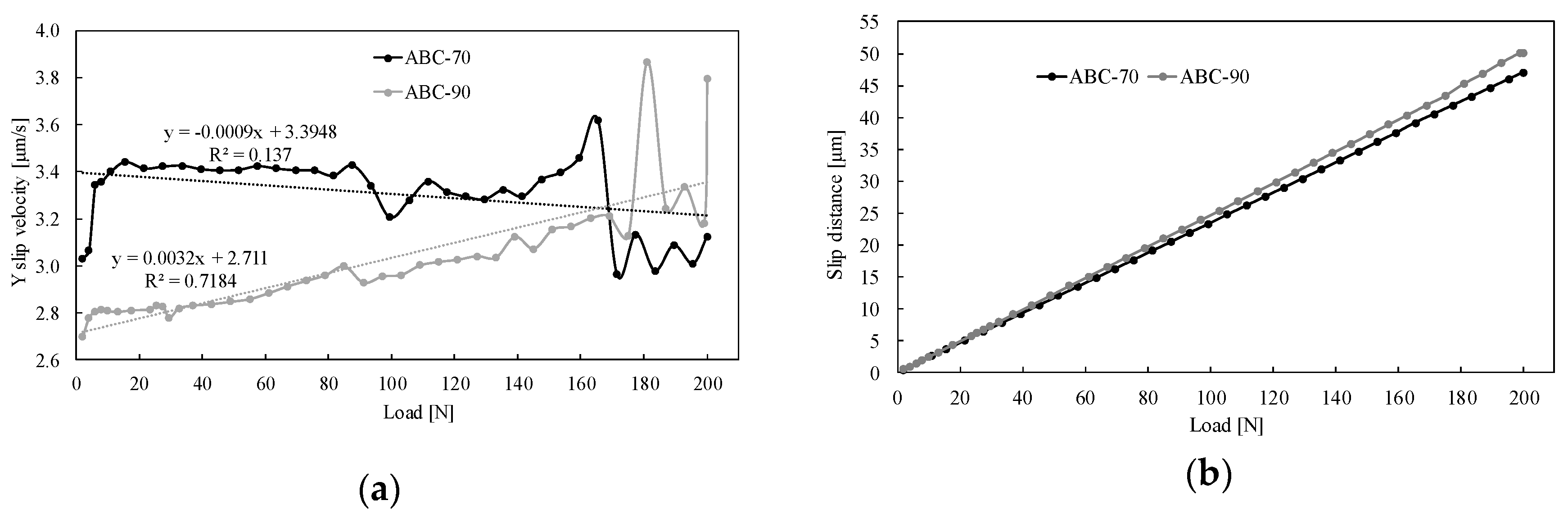
3.2. Comparison of FEM and Experimental Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Burgers, P.T.P.W.; Van Riel, M.P.J.M.; Vogels, L.M.M.; Stam, R.; Patka, P.; Van Lieshout, E.M.M. Rigidity of unilateral external fixators—A biomechanical study. Injury 2011, 42, 1449–1454. [Google Scholar] [CrossRef] [PubMed]
- Lin, D.L.; Kirk, K.L.; Murphy, K.P.; McHale, K.A.; Doukas, W.C. Evaluation of orthopaedic injuries in Operation Enduring Freedom. J. Orthop. Trauma 2004, 18, 300–305. [Google Scholar] [CrossRef] [PubMed]
- Johnson, E.N.; Burns, T.C.; Hayda, R.A.; Hospenthal, D.R.; Murray, C.K. Infectious Complications of Open Type III Tibial Fractures among Combat Casualties. Clin. Infect. Dis. 2007, 45, 409–415. [Google Scholar] [CrossRef] [PubMed]
- Tuttle, M.S.; Smith, W.R.; Williams, A.E.; Agudelo, J.F.; Hartshorn, C.J.; Moore, E.E.; Morgan, S.J. Safety and Efficacy of Damage Control External Fixation Versus Early Definitive Stabilization for Femoral Shaft Fractures in the Multiple-Injured Patient. J. Trauma Inj. Infect. Crit. Care 2009, 67, 602–605. [Google Scholar] [CrossRef] [PubMed]
- Yilihamu, Y.; Keremu, A.; Abulaiti, A.; Maimaiti, X.; Ren, P.; Yusufu, A. Outcomes of post-traumatic tibial osteomyelitis treated with an Orthofix LRS versus an Ilizarov external fixator. Injury 2017, 48, 1636–1643. [Google Scholar] [CrossRef]
- Court- Brown, C. Skeletal Trauma Basic Science, Management, and Reconstruction, British Editioral Society of Bone and Joint Surgery, 3rd ed.; Browner Bruce, D., Jupiter Jesse, B., Levine Alan, M., Trafton Peter, G., Eds.; Saunders: Philadelphia, PA, USA, 2003; ISBN 0-7216-9175-7. [Google Scholar]
- Sternick, M.B.; Dallacosta, D.; Bento, D.Á.; Do Reis, M.L. Relationship between rigidity of external fixator and number of pins: Computer analysis using finite elements. Rev. Bras. Ortop. 2012, 47, 646–650. [Google Scholar] [CrossRef]
- Shahid, M.K.; Malik, S. A Review of the Biomechanical Role of a Unilateral External Fixator in the Fracture Repair Process. EC Orthop. 3.1 2016, 3, 254–260. [Google Scholar]
- Ghiasi, M.S.; Chen, J.; Vaziri, A.; Rodriguez, E.K.; Nazarian, A. Bone fracture healing in mechanobiological modeling: A review of principles and methods. Bone Rep. 2017, 6, 87–100. [Google Scholar] [CrossRef]
- Loi, F.; Córdova, L.A.; Pajarinen, J.; Lin, T.; Yao, Z.; Goodman, S.B. Inflammation, fracture and bone repair. Bone 2016, 86, 119–130. [Google Scholar] [CrossRef]
- Claes, L.; Recknagel, S.; Ignatius, A. Fracture healing under healthy and inflammatory conditions. Nat. Rev. Rheumatol. 2012, 8, 133. [Google Scholar] [CrossRef]
- Willie, B.; Adkins, K.; Zheng, X.; Simon, U.; Claes, L. Mechanical characterization of external fixator stiffness for a rat femoral fracture model. J. Orthop. Res. 2008, 27, 687–693. [Google Scholar] [CrossRef] [PubMed]
- Hanume Gowda, S.N.; Archana, G. Treatment of infected non-union of long bones with monolateral external fixation (lrs). J. Evol. Med. Dent. Sci. 2014, 3, 14. [Google Scholar]
- Pal, C.P.; Kumar, H.; Kumar, D.; Dinkar, K.S.; Mittal, V.; Singh, N.K. Comparative study of the results of compound tibial shaft fractures treated by Ilizarov ring fixators and limb reconstruction system fixators. Chin. J. Traumatol. 2015, 18, 347–351. [Google Scholar] [CrossRef] [PubMed]
- Abulaiti, A.; Yilihamu, Y.; Yasheng, T.; Alike, Y.; Yusufu, A. The psychological impact of external fixation using the Ilizarov or Orthofix LRS method to treat tibial osteomyelitis with a bone defect. Injury 2017, 48, 2842–2846. [Google Scholar] [CrossRef] [PubMed]
- Laubscher, M.; Mitchell, C.; Timms, A.; Goodier, D.; Calder, P. Outcomes following femoral lengthening. Bone Jt. J. 2016, 98-B, 1382–1388. [Google Scholar] [CrossRef]
- Patra, S.R.; Kisan, D.; Madharia, D.; Panigrahi, N.K.; Samant, S.; Manoj, M.; Shiv, A.; Das, L.K. Management of infected non-unions of long bones using limb reconstruction system (LRS) fixator. Int. J. Res. Orthop. 2017, 3, 213. [Google Scholar] [CrossRef][Green Version]
- Gardner, T.N.; Evans, M.; Kenwright, J. The influence of external fixators on fracture motion during simulated walking. Med. Eng. Phys. 1996, 18, 305–313. [Google Scholar] [CrossRef]
- Strebe, S.; Kim, H.; Russell, J.P.; Hsieh, A.H.; Nascone, J.; O’Toole, R.V. Analysis of strategies to increase external fixator stiffness: Is double stacking worth the cost? Injury 2014, 45, 1049–1053. [Google Scholar] [CrossRef]
- ASTM. Standard Specification and Test Methods for External Skeletal Fixation Devices; ASTM F1541-01; ASTM: West Conshohocken, PA, USA, 2011. [Google Scholar]
- Messias, A.; Neto, M.A.; Amaro, A.M.; Nicolau, P.; Roseiro, L.M. Effect of round curvature of anterior implant-supported zirconia frameworks: Finite element analysis and in vitro study using digital image correlation. Comput. Methods Biomech. Biomed. Engin. 2017, 20, 1236–1248. [Google Scholar] [CrossRef]
- Lopes, V.M.M.; Neto, M.A.; Amaro, A.M.; Roseiro, L.M.; Paulino, M.F. FE and experimental study on how the cortex material properties of synthetic femurs affect strain levels. Med. Eng. Phys. 2017, 46, 96–109. [Google Scholar] [CrossRef]
- Ramos, A.; Simões, J.A. Tetrahedral versus hexahedral finite elements in numerical modelling of the proximal femur. Med. Eng. Phys. 2006, 28, 916–924. [Google Scholar] [CrossRef] [PubMed]
- Bathe, K. User’s Manual 2017; ADINA R&ID: Watertown, MA, USA, 2017. [Google Scholar]
- Chao, E.Y.; Aro, H.T.; Lewallen, D.G.; Kelly, P.J. The effect of rigidity on fracture healing in external fixation. Clin. Orthop. Relat. Res. 1989, 24–35. [Google Scholar]
- Mangukiya, H.J.; Mahajan, N.P.; Pawar, E.D.; Mane, A.; Manna, J. Functional and radiological outcome in management of compound tibia diaphyseal fracture with AO monolateral fixator versus Limb reconstruction system. J. Orthop. 2018, 15, 275–281. [Google Scholar] [CrossRef]
- Hente, R.; Füchtmeier, B.; Schlegel, U.; Ernstberger, A.; Perren, S.M. The influence of cyclic compression and distraction on the healing of experimental tibial fractures. J. Orthop. Res. 2004, 22, 709–715. [Google Scholar] [CrossRef] [PubMed]
- ARO, H.T.; Kelly, P.J.; Lewallen, D.G.; Chao, E.Y.S. The Effects of Physiologic Dynamic Compression on Bone Healing Under External Fixation. Clin. Orthop. Relat. Res. 1990, 256, 260–273. [Google Scholar] [CrossRef]
- Elmedin, M.; Vahid, A.; Nedim, P.; Nedžad, R. Finite element analysis and experimental testing of stiffness of the Sarafix external fixator. Procedia Eng. 2015, 100, 1598–1607. [Google Scholar] [CrossRef]
- Fragomen, A.T.; Rozbruch, S.R. The mechanics of external fixation. HSS J. 2007, 3, 13–29. [Google Scholar] [CrossRef]
- Burny, F.; Burny, W.; Donkerwolcke, M.; Behrens, M. Effect of callus development on the deformation of external fixation frames. Int. Orthop. 2012, 36, 2577–2580. [Google Scholar] [CrossRef][Green Version]
- Aarnes, G.T.; Steen, H.; Ludvigsen, P.; Waanders, N.A.; Huiskes, R.; Goldstein, S.A. In vivo assessment of regenerate axial stiffness in distraction osteogenesis. J. Orthop. Res. 2005, 23, 494–498. [Google Scholar] [CrossRef]
- Perren, S.M. Physical and biological aspects of fracture healing with special reference to internal fixation. Clin. Orthop. Relat. Res. 1979, 138, 175–196. [Google Scholar]
- Giotakis, N.; Narayan, B. Stability with unilateral external fixation in the tibia. Strateg. Trauma Limb Reconstr. 2007, 2, 13–20. [Google Scholar] [CrossRef] [PubMed]
- Wehner, T.; Claes, L.; Niemeyer, F.; Nolte, D.; Simon, U. Influence of the fixation stability on the healing time—A numerical study of a patient-specific fracture healing process. Clin. Biomech. 2010, 25, 606–612. [Google Scholar] [CrossRef] [PubMed]
- Kazmers, N.H.; Fragomen, A.T.; Rozbruch, S.R. Prevention of pin site infection in external fixation: A review of the literature. Strateg. Trauma Limb Reconstr. 2016, 11, 75–85. [Google Scholar] [CrossRef] [PubMed]
- Claes, L.; Blakytny, R.; Besse, J.; Bausewein, C.; Ignatius, A.; Willie, B. Late Dynamization by Reduced Fixation Stiffness Enhances Fracture Healing in a Rat Femoral Osteotomy Model. J. Orthop. Trauma 2011, 25, 169–174. [Google Scholar] [CrossRef] [PubMed]
- Tufekci, P.; Tavakoli, A.; Dlaska, C.; Neumann, M.; Shanker, M.; Saifzadeh, S.; Steck, R.; Schuetz, M.; Epari, D. Early mechanical stimulation only permits timely bone healing in sheep. J. Orthop. Res. 2018, 36, 1790–1796. [Google Scholar] [CrossRef] [PubMed]
- Marsell, R.; Einhorn, T.A. The biology of fracture healing. Injury 2011, 42, 551–555. [Google Scholar] [CrossRef]
- Tomlinson, R.E.; Silva, M.J. Skeletal Blood Flow in Bone Repair and Maintenance. Bone Res. 2013, 1, 311–322. [Google Scholar] [CrossRef]
- OReilly, A.; Hankenson, K.D.; Kelly, D.J. A computational model to explore the role of angiogenic impairment on endochondral ossification during fracture healing. Biomech. Model. Mechanobiol. 2016, 15, 1279–1294. [Google Scholar] [CrossRef]
- Pietsch, M.; Niemeyer, F.; Simon, U.; Ignatius, A.; Urban, K. Modelling the fracture-healing process as a moving-interface problem using an interface-capturing approach. Comput. Methods Biomech. Biomed. Eng. 2018, 21, 512–520. [Google Scholar] [CrossRef]
- Katz, Y.; Lubovsky, O.; Yosibash, Z. Patient-specific finite element analysis of femurs with cemented hip implants. Clin. Biomech. 2018, 58, 74–89. [Google Scholar] [CrossRef]
- Haider, I.T.; Goldak, J.; Frei, H. Femoral fracture load and fracture pattern is accurately predicted using a gradient-enhanced quasi-brittle finite element model. Med. Eng. Phys. 2018, 55, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Falcinelli, C.; Di Martino, A.; Gizzi, A.; Vairo, G.; Denaro, V. Mechanical behavior of metastatic femurs through patient-specific computational models accounting for bone-metastasis interaction. J. Mech. Behav. Biomed. Mater. 2019, 93, 9–22. [Google Scholar] [CrossRef] [PubMed]
- Haider, I.T.; Baggaley, M.; Brent Edwards, W. Subject-Specific Finite Element Models of the Tibia With Realistic Boundary Conditions Predict Bending Deformations Consistent With In Vivo Measurement. J. Biomech. Eng. 2020, 142, 021010. [Google Scholar] [CrossRef] [PubMed]
- Cristofolini, L.; Viceconti, M.; Cappello, A.; Toni, A. Mechanical validation of whole bone composite femur models. J. Biomech. 1996, 29, 525–535. [Google Scholar] [CrossRef]

| Configuration | Number of Pins in the Nylon Bars | Graphic Representation | |
|---|---|---|---|
| Upper | Bottom | ||
| AB | 2 | 2 |  |
| AC | 2 | 2 |  |
| BC | 2 | 2 |  |
| ABC | 3 | 3 |  |
| ACAB | 2 | 2 |  |
| BCAB | 2 | 2 |  |
| ABCAB | 3 | 2 |  |
| ABCAC | 3 | 2 |  |
| Material Property | Carbon Epoxy | Nylon | Anodized Aluminum 7076-T6 | AISI 316 L |
|---|---|---|---|---|
| E1 [GPA] | 101.40 | 8.30 | 71.70 | 200 |
| E2 [GPA] | 8.40 | 8.30 | 71.70 | 200 |
| E3 [GPA] | 8.40 | 8.30 | 71.70 | 200 |
| G12 [GPA] | 5.60 | 3.24 | 26.95 | 79.05 |
| G13 [GPA] | 5.60 | 3.24 | 26.95 | 79.05 |
| G23 [GPA] | 5.60 | 3.24 | 26.95 | 79.05 |
| v21 | 0.33 | 0.28 | 0.33 | 0.265 |
| v31 | 0.33 | 0.28 | 0.33 | 0.265 |
| v32 | 0.46 | 0.28 | 0.33 | 0.265 |
| TL [N] | CL [N] | Interfragmentary Deformation | ||||
|---|---|---|---|---|---|---|
| 50 [mm] | 70 [mm] | 90 [mm] | 50 [mm] | 70 [mm] | 90 [mm] | |
| 50 | 4.569 | 10.75 | 14.23 | 0.12% | 0.27% | 0.36% |
| 100 | 9.368 | 25.58 | 28.63 | 0.24% | 0.65% | 0.72% |
| 150 | 19.74 | 38.93 | 43.21 | 0.50% | 0.98% | 1.09% |
| 200 | 33.67 | 53.08 | 56.59 | 0.85% | 1.34% | 1.43% |
| Configuration | 50 [mm] | CL/TL | 70 [mm] | CL/TL | 90 [mm] | CL/TL |
|---|---|---|---|---|---|---|
| AB | 30.66 ± 4.97 | 15% | 52.44 ± 2.62 | 26% | 56.85 ± 1.20 | 28% |
| AC | 40.84 ± 5.69 | 20% | 53.14 ± 0.32 | 27% | 56.10 ± 0.66 | 28% |
| BC | 36.93 ± 5.65 | 18% | 54.79 ± 1.23 | 27% | 57.78 ± 0.90 | 29% |
| ABC | 39.24 ± 5.01 | 20% | 52.54 ± 2.75 | 26% | 57.39 ± 0.28 | 29% |
| ACAB | - | - | 51.96 ± 3.28 | 26% | - | - |
| BCAB | - | - | 54.14 ± 0.80 | 27% | - | - |
| ABCAB | - | - | 50.73 ± 3.33 | 25% | - | - |
| ABCAC | - | - | 54.93 ± 1.22 | 27% | - | - |
| Configuration | 70 [mm] | 90 [mm] | ||||
|---|---|---|---|---|---|---|
| Force [N] | Def. [%] | CL/TL | Force [N] | Def. [%] | CL/TL | |
| AB | 47.4 | 1.20 | 24% | 68.31 | 1.73 | 34% |
| AC | 46.61 | 1.18 | 23% | 66.77 | 1.69 | 33% |
| BC | 48.04 | 1.22 | 24% | 68.75 | 1.74 | 34% |
| ABC | 44.91 | 1.14 | 22% | 63.9 | 1.62 | 32% |
| ACAB | 47.12 | 1.20 | 24% | 65.75 | 1.67 | 33% |
| BCAB | 47.48 | 1.20 | 24% | 70.67 | 1.79 | 35% |
| ABCAB | 46.25 | 1.17 | 23% | 67.94 | 1.72 | 34% |
| ABCAC | 45.75 | 1.16 | 23% | 66.97 | 1.70 | 33% |
| Configuration | Upper Pins [MPa] | Upper-Nylon [MPa] | Bottom-Nylon [MPa] | ||||||
|---|---|---|---|---|---|---|---|---|---|
| A | B | C | A | B | C | A | B | C | |
| AB | 76.29 | 66.12 | - | 3.95 | 3.53 | - | 5.59 | 4.87 | - |
| AC | 66.68 | - | 70 | 3.75 | - | 3.47 | 5.28 | - | 4.92 |
| BC | - | 63.77 | 72.97 | - | 3.83 | 3.67 | - | 5.66 | 2.21 |
| ABC | 43.07 | 35.07 | 46.26 | 2.73 | 1.39 | 1.39 | 3.84 | 1.39 | 1.39 |
| ACAB | 69.82 | - | 66.48 | 3.74 | - | 3.46 | 5.60 | 4.88 | - |
| BCAB | - | 63.87 | 73.08 | - | 3.83 | 3.68 | 5.59 | 4.87 | - |
| ABCAB | 39.57 | 34.73 | 45.84 | 2.72 | 2.4 | 2.46 | 5.63 | 4.91 | - |
| ABCAC | 39.69 | 34.63 | 45.97 | 2.71 | 2.4 | 2.46 | 5.31 | - | 4.94 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Martins Amaro, A.; Fátima Paulino, M.; Manuel Roseiro, L.; Augusta Neto, M. The Effect of External Fixator Configurations on the Dynamic Compression Load: An Experimental and Numerical Study. Appl. Sci. 2020, 10, 3. https://doi.org/10.3390/app10010003
Martins Amaro A, Fátima Paulino M, Manuel Roseiro L, Augusta Neto M. The Effect of External Fixator Configurations on the Dynamic Compression Load: An Experimental and Numerical Study. Applied Sciences. 2020; 10(1):3. https://doi.org/10.3390/app10010003
Chicago/Turabian StyleMartins Amaro, Ana, Maria Fátima Paulino, Luis Manuel Roseiro, and Maria Augusta Neto. 2020. "The Effect of External Fixator Configurations on the Dynamic Compression Load: An Experimental and Numerical Study" Applied Sciences 10, no. 1: 3. https://doi.org/10.3390/app10010003
APA StyleMartins Amaro, A., Fátima Paulino, M., Manuel Roseiro, L., & Augusta Neto, M. (2020). The Effect of External Fixator Configurations on the Dynamic Compression Load: An Experimental and Numerical Study. Applied Sciences, 10(1), 3. https://doi.org/10.3390/app10010003








