Risk and Mitigation of African Swine Fever Virus in Feed
Abstract
Simple Summary
Abstract
1. Risk of ASFV to the Swine Industry
2. Introduction of Feed Risk
3. Certain Ingredients Support ASFV Stability
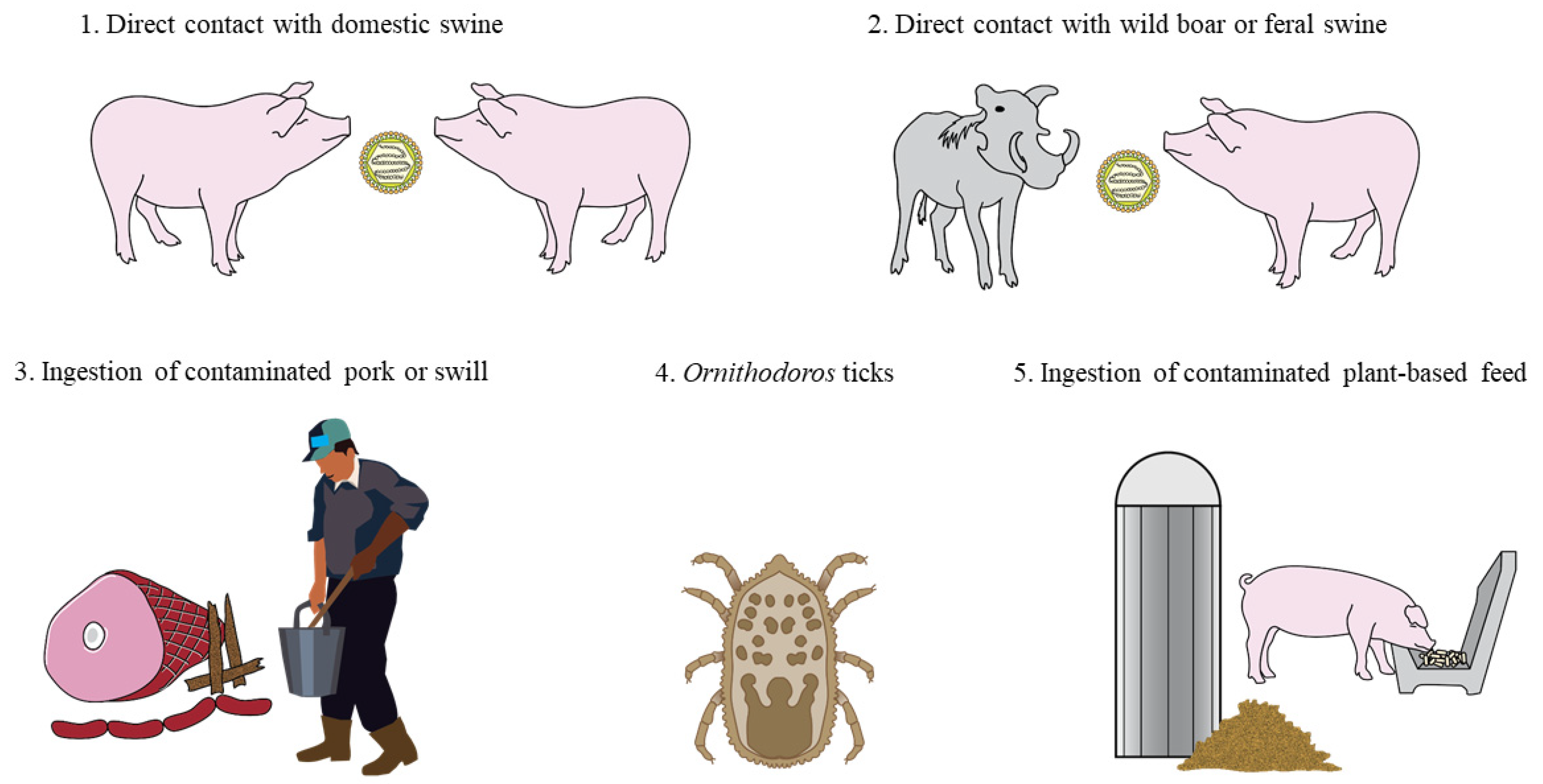
4. ASFV Transmission through Plant-Based Feed
5. Reducing ASFV Risk through Feed Biosecurity
6. Physical Mitigation Methods for ASFV in Feed
7. Chemical Mitigation Methods for ASFV in Feed
8. Conclusions
Funding
Acknowledgments
Conflicts of Interest
References
- Woonwong, Y.; Do Tien, D.; Thanawongnuwech, R. The Future of the Pig Industry After the Introduction of African Swine Fever into Asia. Anim. Front. 2020, 10, 30–37. [Google Scholar] [CrossRef]
- Sang, H.; Miller, G.; Lokhandwala, S.; Sangewar, N.; Waghela, S.D.; Bishop, R.P.; Mwangi, W. Progress toward Development of Effective and Safe African Swine Fever Virus Vaccines. Front. Vet. Sci. 2020, 7, 84. [Google Scholar] [CrossRef]
- Carriquiry, M.; Elobeid, A.; Swenson, D.; Hayes, D. Impacts of African Swine Fever in Iowa and the United States; Iowa State University Digital Repository: Ames, IA, USA, 2020. [Google Scholar]
- Alonso, C.; Borca, M.; Dixon, L.; Revilla, Y.; Rodriguez, F.; Escribano, J.M.; Ictv Report, C. ICTV Virus Taxonomy Profile: Asfarviridae. J. Gen. Virol. 2018, 99, 613–614. [Google Scholar] [CrossRef]
- Ghedin, E.; Sengamalay, N.A.; Shumway, M.; Zaborsky, J.; Feldblyum, T.; Subbu, V.; Spiro, D.J.; Sitz, J.; Koo, H.; Bolotov, P.; et al. Large-scale sequencing of human influenza reveals the dynamic nature of viral genome evolution. Nature 2005, 437, 1162–1166. [Google Scholar] [CrossRef]
- Galindo, I.; Alonso, C. African Swine Fever Virus: A Review. Viruses 2017, 9, 103. [Google Scholar] [CrossRef]
- Blome, S.; Gabriel, C.; Beer, M. Pathogenesis of African swine fever in domestic pigs and European wild boar. Virus Res. 2013, 173, 122–130. [Google Scholar] [CrossRef]
- Olesen, A.S.; Lohse, L.; Boklund, A.; Halasa, T.; Gallardo, C.; Pejsak, Z.; Belsham, G.J.; Rasmussen, T.B.; Bøtner, A. Transmission of African swine fever virus from infected pigs by direct contact and aerosol routes. Vet. Microbiol. 2017, 211, 92–102. [Google Scholar] [CrossRef]
- Olesen, A.S.; Belsham, G.J.; Bruun Rasmussen, T.; Lohse, L.; Bødker, R.; Halasa, T.; Boklund, A.; Bøtner, A. Potential routes for indirect transmission of African swine fever virus into domestic pig herds. Transbound. Emerg. Dis. 2020, 67, 1472–1484. [Google Scholar] [CrossRef]
- Burrage, T.G. African swine fever virus infection in Ornithodoros ticks. Virus Res. 2013, 173, 131–139. [Google Scholar] [CrossRef] [PubMed]
- Niederwerder, M.C.; Rowland, R.R. Is There a Risk for Introducing Porcine Reproductive and Respiratory Syndrome Virus (PRRSV) through the Legal Importation of Pork? Food Environ. Virol. 2017, 9, 1–13. [Google Scholar] [CrossRef]
- McVicar, J.W.; Mebus, C.A.; Becker, H.N.; Belden, R.C.; Gibbs, E.P.J. Induced African swine fever in feral pigs. J. Am. Vet. Med. Assoc. 1981, 179, 441–446. [Google Scholar]
- Rock, D.L. Challenges for African swine fever vaccine development-“… perhaps the end of the beginning”. Vet. Microbiol. 2017, 206, 52–58. [Google Scholar] [CrossRef]
- Eustace Montgomery, R. On a Form of Swine Fever Occurring in British East Africa (Kenya Colony). J. Comp. Pathol. Ther. 1921, 34, 159–191. [Google Scholar] [CrossRef]
- Rowlands, R.J.; Michaud, V.; Heath, L.; Hutchings, G.; Oura, C.; Vosloo, W.; Dwarka, R.; Onashvili, T.; Albina, E.; Dixon, L.K. African swine fever virus isolate, Georgia, 2007. Emerg. Infect. Dis. 2008, 14, 1870–1874. [Google Scholar] [CrossRef]
- Malogolovkin, A.; Yelsukova, A.; Gallardo, C.; Tsybanov, S.; Kolbasov, D. Molecular characterization of African swine fever virus isolates originating from outbreaks in the Russian Federation between 2007 and 2011. Vet. Microbiol. 2012, 158, 415–419. [Google Scholar] [CrossRef] [PubMed]
- Pejsak, Z.; Truszczyński, M.; Niemczuk, K.; Kozak, E.; Markowska-Daniel, I. Epidemiology of African Swine Fever in Poland since the detection of the first case. Pol. J. Vet. Sci. 2014, 17, 665–672. [Google Scholar] [CrossRef]
- Olsevskis, E.; Guberti, V.; Serzants, M.; Westergaard, J.; Gallardo, C.; Rodze, I.; Depner, K. African swine fever virus introduction into the EU in 2014: Experience of Latvia. Res. Vet. Sci. 2016, 105, 28–30. [Google Scholar] [CrossRef] [PubMed]
- Forth, J.H.; Forth, L.F.; Václavek, P.; Barták, P.; Höper, D.; Beer, M.; Blome, S. Whole-Genome Sequence of an African Swine Fever Virus Isolate from the Czech Republic. Microbiol. Resour. Announc. 2020, 9. [Google Scholar] [CrossRef]
- Zhou, X.; Li, N.; Luo, Y.; Liu, Y.; Miao, F.; Chen, T.; Zhang, S.; Cao, P.; Li, X.; Tian, K.; et al. Emergence of African Swine Fever in China, 2018. Transbound. Emerg. Dis. 2018. [Google Scholar] [CrossRef] [PubMed]
- Wang, T.; Sun, Y.; Qiu, H.J. African swine fever: An unprecedented disaster and challenge to China. Infect. Dis. Poverty 2018, 7, 111. [Google Scholar] [CrossRef]
- Heilmann, M.; Lkhagvasuren, A.; Adyasuren, T.; Khishgee, B.; Bold, B.; Ankhanbaatar, U.; Fusheng, G.; Raizman, E.; Dietze, K. African Swine Fever in Mongolia: Course of the Epidemic and Applied Control Measures. Vet. Sci. 2020, 7, 24. [Google Scholar] [CrossRef]
- Le, V.P.; Jeong, D.G.; Yoon, S.W.; Kwon, H.M.; Trinh, T.B.N.; Nguyen, T.L.; Bui, T.T.N.; Oh, J.; Kim, J.B.; Cheong, K.M.; et al. Outbreak of African Swine Fever, Vietnam, 2019. Emerg. Infect. Dis. 2019, 25. [Google Scholar] [CrossRef]
- Kim, H.J.; Cho, K.H.; Lee, S.K.; Kim, D.Y.; Nah, J.J.; Kim, H.J.; Kim, H.J.; Hwang, J.Y.; Sohn, H.J.; Choi, J.G.; et al. Outbreak of African swine fever in South Korea, 2019. Transbound. Emerg. Dis. 2020, 67, 473–475. [Google Scholar] [CrossRef]
- Smith, D.; Cooper, T.; Pereira, A.; Jong, J. Counting the cost: The potential impact of African Swine Fever on smallholders in Timor-Leste. One Health (Amst. Neth.) 2019, 8, 100109. [Google Scholar] [CrossRef] [PubMed]
- Boklund, A.; Dhollander, S.; Chesnoiu Vasile, T.; Abrahantes, J.C.; Bøtner, A.; Gogin, A.; Gonzalez Villeta, L.C.; Gortázar, C.; More, S.J.; Papanikolaou, A.; et al. Risk factors for African swine fever incursion in Romanian domestic farms during 2019. Sci. Rep. 2020, 10, 10215. [Google Scholar] [CrossRef]
- Zani, L.; Dietze, K.; Dimova, Z.; Forth, J.H.; Denev, D.; Depner, K.; Alexandrov, T. African Swine Fever in a Bulgarian Backyard Farm-A Case Report. Vet. Sci. 2019, 6, 94. [Google Scholar] [CrossRef]
- Forth, J.H.; Tignon, M.; Cay, A.B.; Forth, L.F.; Hoper, D.; Blome, S.; Beer, M. Comparative Analysis of Whole-Genome Sequence of African Swine Fever Virus Belgium 2018/1. Emerg. Infect. Dis. 2019, 25, 1249–1252. [Google Scholar] [CrossRef]
- Milićević, V.; Kureljušić, B.; Maksimović Zorić, J.; Savić, B.; Stanojević, S.; Milakara, E. First Occurence of African Swine Fever in Serbia. Acta Vet. (Beogr.) 2019, 69, 443–449. [Google Scholar] [CrossRef]
- Sauter-Louis, C.; Forth, J.H.; Probst, C.; Staubach, C.; Hlinak, A.; Rudovsky, A.; Holland, D.; Schlieben, P.; Göldner, M.; Schatz, J.; et al. Joining the club: First detection of African swine fever in wild boar in Germany. Transbound. Emerg. Dis. 2020. [Google Scholar] [CrossRef] [PubMed]
- Stevenson, G.W.; Hoang, H.; Schwartz, K.J.; Burrough, E.R.; Sun, D.; Madson, D.; Cooper, V.L.; Pillatzki, A.; Gauger, P.; Schmitt, B.J.; et al. Emergence of Porcine epidemic diarrhea virus in the United States: Clinical signs, lesions, and viral genomic sequences. J. Vet. Diagn. Investig. Off. Publ. Am. Assoc. Vet. Lab. Diagn. Inc. 2013, 25, 649–654. [Google Scholar] [CrossRef]
- Wang, L.; Byrum, B.; Zhang, Y. Detection and genetic characterization of deltacoronavirus in pigs, Ohio, USA, 2014. Emerg. Infect. Dis. 2014, 20, 1227–1230. [Google Scholar] [CrossRef]
- Wang, Y.; Grunewald, M.; Perlman, S. Coronaviruses: An Updated Overview of Their Replication and Pathogenesis. Methods Mol. Biol. (Cliftonn. J.) 2020, 2203, 1–29. [Google Scholar] [CrossRef]
- Niederwerder, M.C.; Hesse, R.A. Swine enteric coronavirus disease: A review of 4 years with porcine epidemic diarrhoea virus and porcine deltacoronavirus in the United States and Canada. Transbound. Emerg. Dis. 2018, 65, 660–675. [Google Scholar] [CrossRef] [PubMed]
- Jung, K.; Saif, L.J. Porcine epidemic diarrhea virus infection: Etiology, epidemiology, pathogenesis and immunoprophylaxis. Vet. J. (Lond. Engl. 1997) 2015, 204, 134–143. [Google Scholar] [CrossRef] [PubMed]
- Bevins, S.N.; Lutman, M.; Pedersen, K.; Barrett, N.; Gidlewski, T.; Deliberto, T.J.; Franklin, A.B. Spillover of Swine Coronaviruses, United States. Emerg. Infect. Dis. 2018, 24, 1390–1392. [Google Scholar] [CrossRef]
- SDRS. October Domestic Disease Monitoring Report; Swine Disease Reporting System: Ames, IA, USA, 2020; Available online: https://www.swinehealth.org/wp-content/uploads/2020/10/SDRS_report-_32.pdf (accessed on 6 October 2020).
- Su, Y.; Hou, Y.; Prarat, M.; Zhang, Y.; Wang, Q. New variants of porcine epidemic diarrhea virus with large deletions in the spike protein, identified in the United States, 2016–2017. Arch. Virol. 2018, 163, 2485–2489. [Google Scholar] [CrossRef] [PubMed]
- Huang, Y.W.; Dickerman, A.W.; Pineyro, P.; Li, L.; Fang, L.; Kiehne, R.; Opriessnig, T.; Meng, X.J. Origin, evolution, and genotyping of emergent porcine epidemic diarrhea virus strains in the United States. mBio 2013, 4, e00737-13. [Google Scholar] [CrossRef]
- Stoian, A.M.M.; Petrovan, V.; Constance, L.A.; Olcha, M.; Dee, S.; Diel, D.G.; Sheahan, M.A.; Rowland, R.R.R.; Patterson, G.; Niederwerder, M.C. Stability of classical swine fever virus and pseudorabies virus in animal feed ingredients exposed to transpacific shipping conditions. Transbound. Emerg. Dis. 2020, 67, 1623–1632. [Google Scholar] [CrossRef]
- Dee, S.; Neill, C.; Singrey, A.; Clement, T.; Cochrane, R.; Jones, C.; Patterson, G.; Spronk, G.; Christopher-Hennings, J.; Nelson, E. Modeling the transboundary risk of feed ingredients contaminated with porcine epidemic diarrhea virus. BMC Vet. Res. 2016, 12, 51. [Google Scholar] [CrossRef] [PubMed]
- Dee, S.; Clement, T.; Schelkopf, A.; Nerem, J.; Knudsen, D.; Christopher-Hennings, J.; Nelson, E. An evaluation of contaminated complete feed as a vehicle for porcine epidemic diarrhea virus infection of naive pigs following consumption via natural feeding behavior: Proof of concept. BMC Vet. Res. 2014, 10, 176. [Google Scholar] [CrossRef]
- Schumacher, L.L.; Woodworth, J.C.; Jones, C.K.; Chen, Q.; Zhang, J.; Gauger, P.C.; Stark, C.R.; Main, R.G.; Hesse, R.A.; Tokach, M.D.; et al. Evaluation of the minimum infectious dose of porcine epidemic diarrhea virus in virus-inoculated feed. Am. J. Vet. Res. 2016, 77, 1108–1113. [Google Scholar] [CrossRef] [PubMed]
- Pasick, J.; Berhane, Y.; Ojkic, D.; Maxie, G.; Embury-Hyatt, C.; Swekla, K.; Handel, K.; Fairles, J.; Alexandersen, S. Investigation into the role of potentially contaminated feed as a source of the first-detected outbreaks of porcine epidemic diarrhea in Canada. Transbound. Emerg. Dis. 2014, 61, 397–410. [Google Scholar] [CrossRef]
- Bowman, A.S.; Krogwold, R.A.; Price, T.; Davis, M.; Moeller, S.J. Investigating the introduction of porcine epidemic diarrhea virus into an Ohio swine operation. BMC Vet. Res. 2015, 11, 38. [Google Scholar] [CrossRef] [PubMed]
- Perri, A.M.; Poljak, Z.; Dewey, C.; Harding, J.C.S.; O’Sullivan, T.L. An epidemiological investigation of the early phase of the porcine epidemic diarrhea (PED) outbreak in Canadian swine herds in 2014: A case-control study. Prev. Vet. Med. 2018, 150, 101–109. [Google Scholar] [CrossRef]
- Perri, A.M.; Poljak, Z.; Dewey, C.; Harding, J.C.S.; O’Sullivan, T.L. Network analyses using case-control data to describe and characterize the initial 2014 incursion of porcine epidemic diarrhea (PED) in Canadian swine herds. Prev. Vet. Med. 2019, 162, 18–28. [Google Scholar] [CrossRef]
- Sasaki, Y.; Alvarez, J.; Sekiguchi, S.; Sueyoshi, M.; Otake, S.; Perez, A. Epidemiological factors associated to spread of porcine epidemic diarrhea in Japan. Prev. Vet. Med. 2016, 123, 161–167. [Google Scholar] [CrossRef]
- Sung, M.H.; Lin, C.N.; Chiou, M.T.; Cheng, I.J.; Thanh, Q.H.; Chao, D.Y.; Lan, Y.C. Phylogeographic investigation of 2014 porcine epidemic diarrhea virus (PEDV) transmission in Taiwan. PLoS ONE 2019, 14, e0213153. [Google Scholar] [CrossRef]
- Jurado, C.; Mur, L.; Pérez Aguirreburualde, M.S.; Cadenas-Fernández, E.; Martínez-López, B.; Sánchez-Vizcaíno, J.M.; Perez, A. Risk of African swine fever virus introduction into the United States through smuggling of pork in air passenger luggage. Sci. Rep. 2019, 9, 14423. [Google Scholar] [CrossRef]
- Niederwerder, M.C.; Stoian, A.M.M.; Rowland, R.R.R.; Dritz, S.S.; Petrovan, V.; Constance, L.A.; Gebhardt, J.T.; Olcha, M.; Jones, C.K.; Woodworth, J.C.; et al. Infectious Dose of African Swine Fever Virus When Consumed Naturally in Liquid or Feed. Emerg. Infect. Dis. 2019, 25, 891–897. [Google Scholar] [CrossRef]
- VanderWaal, K.; Perez, A.; Torremorrell, M.; Morrison, R.M.; Craft, M. Role of animal movement and indirect contact among farms in transmission of porcine epidemic diarrhea virus. Epidemics 2018, 24, 67–75. [Google Scholar] [CrossRef]
- Dee, S.; Shah, A.; Cochrane, R.; Clement, T.; Singrey, A.; Edler, R.; Spronk, G.; Niederwerder, M.; Nelson, E. Use of a demonstration project to evaluate viral survival in feed: Proof of concept. Transbound. Emerg. Dis. 2020. [Google Scholar] [CrossRef] [PubMed]
- Dee, S.A.; Niederwerder, M.C.; Patterson, G.; Cochrane, R.; Jones, C.; Diel, D.; Brockhoff, E.; Nelson, E.; Spronk, G.; Sundberg, P. The risk of viral transmission in feed: What do we know, what do we do? Transbound. Emerg. Dis. 2020, 67, 2365–2371. [Google Scholar] [CrossRef] [PubMed]
- Nurmoja, I.; Mõtus, K.; Kristian, M.; Niine, T.; Schulz, K.; Depner, K.; Viltrop, A. Epidemiological analysis of the 2015–2017 African swine fever outbreaks in Estonia. Prev. Vet. Med. 2020, 181, 104556. [Google Scholar] [CrossRef] [PubMed]
- Wen, X.; He, X.; Zhang, X.; Zhang, X.; Liu, L.; Guan, Y.; Zhang, Y.; Bu, Z. Genome sequences derived from pig and dried blood pig feed samples provide important insights into the transmission of African swine fever virus in China in 2018. Emerg. Microbes Infect. 2019, 8, 303–306. [Google Scholar] [CrossRef] [PubMed]
- Zhai, S.L.; Wei, W.K.; Sun, M.F.; Lv, D.H.; Xu, Z.H. African swine fever spread in China. Vet. Rec. 2019, 184, 559. [Google Scholar] [CrossRef] [PubMed]
- Dee, S.A.; Bauermann, F.V.; Niederwerder, M.C.; Singrey, A.; Clement, T.; de Lima, M.; Long, C.; Patterson, G.; Sheahan, M.A.; Stoian, A.M.M.; et al. Survival of viral pathogens in animal feed ingredients under transboundary shipping models. PLoS ONE 2018, 13, e0194509. [Google Scholar] [CrossRef] [PubMed]
- SHIC. Swine Disease Matrix. 2018. Available online: https://www.swinehealth.org/swine-disease-matrix/ (accessed on 18 September 2018).
- Bryan, M.; Zimmerman, J.J.; Berry, W.J. The use of half-lives and associated confidence intervals in biological research. Vet. Res. Commun. 1990, 14, 235–240. [Google Scholar] [CrossRef]
- Stoian, A.M.M.; Zimmerman, J.; Ji, J.; Hefley, T.J.; Dee, S.; Diel, D.G.; Rowland, R.R.R.; Niederwerder, M.C. Half-Life of African Swine Fever Virus in Shipped Feed. Emerg. Infect. Dis. 2019, 25, 2261–2263. [Google Scholar] [CrossRef]
- Pietschmann, J.; Guinat, C.; Beer, M.; Pronin, V.; Tauscher, K.; Petrov, A.; Keil, G.; Blome, S. Course and transmission characteristics of oral low-dose infection of domestic pigs and European wild boar with a Caucasian African swine fever virus isolate. Arch. Virol. 2015, 160, 1657–1667. [Google Scholar] [CrossRef] [PubMed]
- Howey, E.B.; O’Donnell, V.; de Carvalho Ferreira, H.C.; Borca, M.V.; Arzt, J. Pathogenesis of highly virulent African swine fever virus in domestic pigs exposed via intraoropharyngeal, intranasopharyngeal, and intramuscular inoculation, and by direct contact with infected pigs. Virus Res. 2013, 178, 328–339. [Google Scholar] [CrossRef]
- McVicar, J.W. Quantitative aspects of the transmission of African swine fever. Am. J. Vet. Res. 1984, 45, 1535–1541. [Google Scholar] [PubMed]
- de Carvalho Ferreira, H.C.; Weesendorp, E.; Elbers, A.R.; Bouma, A.; Quak, S.; Stegeman, J.A.; Loeffen, W.L. African swine fever virus excretion patterns in persistently infected animals: A quantitative approach. Vet. Microbiol. 2012, 160, 327–340. [Google Scholar] [CrossRef] [PubMed]
- Plowright, W.; Parker, J.; Pierce, M.A. The epizootiology of African swine fever in Africa. Vet. Rec. 1969, 85, 668–674. [Google Scholar]
- Greig, A. Pathogenesis of African swine fever in pigs naturally exposed to the disease. J. Comp. Pathol. 1972, 82, 73–79. [Google Scholar] [CrossRef]
- Blázquez, E.; Pujols, J.; Segalés, J.; Rodríguez, F.; Crenshaw, J.; Rodríguez, C.; Ródenas, J.; Polo, J. Commercial feed containing porcine plasma spiked with African swine fever virus is not infective in pigs when administered for 14 consecutive days. PLoS ONE 2020, 15, e0235895. [Google Scholar] [CrossRef] [PubMed]
- Pereira De Oliveira, R.; Hutet, E.; Duhayon, M.; Guionnet, J.M.; Paboeuf, F.; Vial, L.; Le Potier, M.F. Successful Infection of Domestic Pigs by Ingestion of the European Soft Tick O. Erraticus That Fed on African Swine Fever Virus Infected Pig. Viruses 2020, 12, 300. [Google Scholar] [CrossRef] [PubMed]
- Heuschele, W.P. Studies on the pathogenesis of African swine fever. I. Quantitative studies on the sequential development of virus in pig tissues. Arch. Fur Die Gesamte Virusforsch. 1967, 21, 349–356. [Google Scholar] [CrossRef]
- Colgrove, G.S.; Haelterman, E.O.; Coggins, L. Pathogenesis of African swine fever in young pigs. Am. J. Vet. Res. 1969, 30, 1343–1359. [Google Scholar] [PubMed]
- Plowright, W.; Parker, J.; Staple, R.F. The growth of a virulent strain of African swine fever virus in domestic pigs. J. Hyg. 1968, 66, 117–134. [Google Scholar] [CrossRef]
- Patterson, G.; Niederwerder, M.C.; Dee, S.A. Risks to animal health associated with imported feed ingredients. J. Am. Vet. Med. Assoc. 2019, 254, 790–791. [Google Scholar] [CrossRef]
- Patterson, G.; Niederwerder, M.C.; Spronk, G.; Dee, S.A. Quantification of soya-based feed ingredient entry from ASFV-positive countries to the United States by ocean freight shipping and associated seaports. Transbound. Emerg. Dis. 2020. [Google Scholar] [CrossRef] [PubMed]
- SHIC. Feed Ingredient Safety Decision Tree Matrix; Swine Health Information Center: Ames, IA, USA, 2018; Available online: https://www.swinehealth.org/wp-content/uploads/2018/09/Feed-Ingredient-Safety.pdf (accessed on 9 December 2020).
- Reicks, D.L. Effective biosecurity to protect North American studs and clients from emerging infectious disease. Theriogenology 2019, 137, 82–87. [Google Scholar] [CrossRef]
- Stewart, S.C.; Dritz, S.S.; Woodworth, J.C.; Paulk, C.; Jones, C.K. A review of strategies to impact swine feed biosecurity. Anim. Health Res. Rev. 2020, 21, 61–68. [Google Scholar] [CrossRef]
- Bellini, S.; Rutili, D.; Guberti, V. Preventive measures aimed at minimizing the risk of African swine fever virus spread in pig farming systems. Acta Vet. Scand. 2016, 58, 82. [Google Scholar] [CrossRef]
- Guinat, C.; Gogin, A.; Blome, S.; Keil, G.; Pollin, R.; Pfeiffer, D.U.; Dixon, L. Transmission routes of African swine fever virus to domestic pigs: Current knowledge and future research directions. Vet. Rec. 2016, 178, 262–267. [Google Scholar] [CrossRef] [PubMed]
- Scott, A.; McCluskey, B.; Brown-Reid, M.; Grear, D.; Pitcher, P.; Ramos, G.; Spencer, D.; Singrey, A. Porcine epidemic diarrhea virus introduction into the United States: Root cause investigation. Prev. Vet. Med. 2016, 123, 192–201. [Google Scholar] [CrossRef]
- Rhouma, M.; Lachapelle, V.; Comeau, G.; Quessy, S.; Zanabria, R.; Provost, F.; Italiano, C.; Holley, R.; Smillie, J.; Brockhoff, E.; et al. Identification and selection of animal health and food safety-related risk factors to be included in the Canadian Food Inspection Agency’s risk assessment model for livestock feed mills. Food Control 2021, 121. [Google Scholar] [CrossRef]
- Pudenz, C.C.; Schulz, L.L.; Tonsor, G.T. Adoption of Secure Pork Supply Plan Biosecurity by U.S. Swine Producers. Front. Vet. Sci. 2019, 6, 146. [Google Scholar] [CrossRef]
- Swine Health Information Center (SHIC). Holding Time Calculations for Feed Ingredients to Mitigate Virus Transmission; SHIC: Ames, IA, USA, 2020; Available online: https://www.swinehealth.org/wp-content/uploads/2020/02/Holding-Time-Calculations-for-Feed-Ingredients-to-Mitigate-Virus-Transmission-Print-02.04.20.pdf (accessed on 4 February 2020).
- CFIA. Import Requirements for Plant-Based Feed Ingredients Imported for Use in Livestock Feed. Canadian Food Inspection Agency Health of Animals Act and Health of Animals Regulations. 2019. Available online: https://www.inspection.gc.ca/animal-health/terrestrial-animals/diseases/reportable/african-swine-fever/plant-based-feed-ingredients/eng/1553706365334/1553706365585#a51 (accessed on 7 January 2021).
- Anonymous. Strategic Approach to the Management of African Swine Fever for the EU Working Document. European Commission Directorate-General for Health and Food Safety, Directorate G—Crisis management in food, animals and plants, SANTE/7113/2015—Rev 12. 2015. Available online: https://ec.europa.eu/food/sites/food/files/animals/docs/ad_control-measures_asf_wrk-doc-sante-2015-7113.pdf (accessed on 7 January 2021).
- Fischer, M.; Mohnke, M.; Probst, C.; Pikalo, J.; Conraths, F.J.; Beer, M.; Blome, S. Stability of African swine fever virus on heat-treated field crops. Transbound. Emerg. Dis. 2020, 67, 2318–2323. [Google Scholar] [CrossRef]
- Sindryakova, I.P.; Morgunov, Y.P.; Chichikin, A.Y.; Gazaev, I.K.; Kudryashov, D.A.; Tsybanov, S.Z. The Influence of Temperature on the Russian Isolate of African Swine Fever Virus in Pork Products and Feed with Extrapolation to Natural Conditions. Sel’skokhozyaistvennaya Biol. 2016, 51, 467–474. [Google Scholar] [CrossRef]
- Trudeau, M.P.; Verma, H.; Sampedro, F.; Urriola, P.E.; Shurson, G.C.; Goyal, S.M. Environmental persistence of porcine coronaviruses in feed and feed ingredients. PLoS ONE 2017, 12, e0178094. [Google Scholar] [CrossRef]
- Trudeau, M.P.; Verma, H.; Sampedro, F.; Urriola, P.E.; Shurson, G.C.; McKelvey, J.; Pillai, S.D.; Goyal, S.M. Comparison of Thermal and Non-Thermal Processing of Swine Feed and the Use of Selected Feed Additives on Inactivation of Porcine Epidemic Diarrhea Virus (PEDV). PLoS ONE 2016, 11, e0158128. [Google Scholar] [CrossRef]
- Trudeau, M.P.; Verma, H.; Urriola, P.E.; Sampedro, F.; Shurson, G.C.; Goyal, S.M. Survival of porcine epidemic diarrhea virus (PEDV) in thermally treated feed ingredients and on surfaces. Porc. Health Manag. 2017, 3, 17. [Google Scholar] [CrossRef]
- Jackman, J.A.; Boyd, R.D.; Elrod, C.C. Medium-chain fatty acids and monoglycerides as feed additives for pig production: Towards gut health improvement and feed pathogen mitigation. J. Anim. Sci. Biotechnol. 2020, 11, 44. [Google Scholar] [CrossRef] [PubMed]
- Thormar, H.; Isaacs, C.E.; Brown, H.R.; Barshatzky, M.R.; Pessolano, T. Inactivation of enveloped viruses and killing of cells by fatty acids and monoglycerides. Antimicrob. Agents Chemother. 1987, 31, 27. [Google Scholar] [CrossRef]
- Sabbaghi, A.; Miri, S.M.; Keshavarz, M.; Zargar, M.; Ghaemi, A. Inactivation methods for whole influenza vaccine production. Rev. Med. Virol. 2019, 29, e2074. [Google Scholar] [CrossRef]
- Niederwerder, M.C.; Dee, S.; Diel, D.G.; Stoian, A.M.M.; Constance, L.A.; Olcha, M.; Petrovan, V.; Patterson, G.; Cino-Ozuna, A.G.; Rowland, R.R.R. Mitigating the risk of African swine fever virus in feed with anti-viral chemical additives. Transbound. Emerg. Dis. 2020. [Google Scholar] [CrossRef]
- Jackman, J.A.; Hakobyan, A.; Zakaryan, H.; Elrod, C.C. Inhibition of African swine fever virus in liquid and feed by medium-chain fatty acids and glycerol monolaurate. J. Anim. Sci. Biotechnol. 2020, 11, 114. [Google Scholar] [CrossRef]
- Dee, S.A.; Niederwerder, M.C.; Edler, R.; Hanson, D.; Singrey, A.; Cochrane, R.; Spronk, G.; Nelson, E. An evaluation of additives for mitigating the risk of virus-contaminated feed using an ice-block challenge model. Transbound. Emerg. Dis. 2020. [Google Scholar] [CrossRef]
- Dee, S.; DeJong, J.; Neill, C.; Ratliff, B.; Singrey, A.; Hansen, E.; Nelson, E.; Keegan, J.; Gaines, A. Inactivation of porcine epidemic diarrhea virus in contaminated swine feed through inclusion of a dry lactic acid-based product. J. Swine Health Prod. 2020, 28, 213–216. [Google Scholar]
- Dee, S.; Neill, C.; Clement, T.; Singrey, A.; Christopher-Hennings, J.; Nelson, E. An evaluation of porcine epidemic diarrhea virus survival in individual feed ingredients in the presence or absence of a liquid antimicrobial. Porc. Health Manag. 2015, 1, 9. [Google Scholar] [CrossRef] [PubMed]
- Gebhardt, J.T.; Cochrane, R.A.; Woodworth, J.C.; Jones, C.K.; Niederwerder, M.C.; Muckey, M.B.; Stark, C.R.; Tokach, M.D.; DeRouchey, J.M.; Goodband, R.D.; et al. Evaluation of the effects of flushing feed manufacturing equipment with chemically treated rice hulls on porcine epidemic diarrhea virus cross-contamination during feed manufacturing. J. Anim. Sci. 2018, 96, 4149–4158. [Google Scholar] [CrossRef] [PubMed]
- Gebhardt, J.T.; Woodworth, J.C.; Jones, C.K.; Tokach, M.D.; Gauger, P.C.; Main, R.G.; Zhang, J.; Chen, Q.; DeRouchey, J.M.; Goodband, R.D.; et al. Determining the impact of commercial feed additives as potential porcine epidemic diarrhea virus mitigation strategies as determined by polymerase chain reaction analysis and bioassay. Transl. Anim. Sci. 2019, 3, 93–102. [Google Scholar] [CrossRef] [PubMed]
- Dee, S.; Neill, C.; Clement, T.; Christopher-Hennings, J.; Nelson, E. An evaluation of a liquid antimicrobial (Sal CURB®) for reducing the risk of porcine epidemic diarrhea virus infection of naïve pigs during consumption of contaminated feed. BMC Vet. Res. 2014, 10, 220. [Google Scholar] [CrossRef] [PubMed]
- Lerner, A.B.; Cochrane, R.A.; Gebhardt, J.T.; Dritz, S.S.; Jones, C.K.; DeRouchey, J.M.; Tokach, M.D.; Goodband, R.D.; Bai, J.; Porter, E.; et al. Effects of medium chain fatty acids as a mitigation or prevention strategy against porcine epidemic diarrhea virus in swine feed. J. Anim. Sci. 2020, 98. [Google Scholar] [CrossRef]
- Gebhardt, J.T.; Thomson, K.A.; Woodworth, J.C.; Dritz, S.S.; Tokach, M.D.; DeRouchey, J.M.; Goodband, R.D.; Jones, C.K.; Cochrane, R.A.; Niederwerder, M.C.; et al. Effect of dietary medium-chain fatty acids on nursery pig growth performance, fecal microbial composition, and mitigation properties against porcine epidemic diarrhea virus following storage. J. Anim. Sci. 2020, 98. [Google Scholar] [CrossRef]
- Cottingim, K.M.; Verma, H.; Urriola, P.E.; Sampedro, F.; Shurson, G.C.; Goyal, S.M. Feed additives decrease survival of delta coronavirus in nursery pig diets. Porc. Health Manag. 2017, 3, 5. [Google Scholar] [CrossRef] [PubMed]

| ASFV Strain | Route | Dose | Infection | Reference |
|---|---|---|---|---|
| Georgia 2007 | Drinking in media † | 100 | 37.5% | [51] |
| Georgia 2007 | Drinking in media † | 101 | 44.4% | [51] |
| Armenia 2008 | Oronasal | 100.5–101.4 ‡ | 12.5% | [62] |
| Malawi 1983 | Intraoropharyngeal | 102 | 0% | [63] |
| Malawi 1983 | Intranasopharyngeal | 102 | 50% | [63] |
| Georgia 2007 | Drinking in media † | 102 | 75% | [51] |
| Dominican Republic 1979 | Intranasal/oral | 102.7 | 0% | [64] |
| Georgia 2007 | Eating in complete feed † | 103 | 0% | [51] |
| Malta 1978 | Intranasal | 103 | 60% | [65] |
| Georgia 2007 | Drinking in media † | 103 | 83.3% | [51] |
| Netherlands 1986 | Intranasal | 103.5 | 60% | [65] |
| Dominican Republic 1979 | Intranasal/oral | 103.7 | 12.5% | [64] |
| East African | Eating in liquid or moistened solid feed † | 103.7–106.1 | 0% | [66] |
| East African | Intranasal | 103.7–103.9 | 100% | [66] |
| Tanzania KWH/12 | Drinking in cow milk † | 104 | 0% | [67] |
| Georgia 2007 | Eating in complete feed † | 104 | 40% | [51] |
| Malta 1978 | Intranasal | 104 | 100% | [65] |
| Georgia 2007 | Drinking in media † | 104 | 100% | [51] |
| Malawi 1983 | Intranasopharyngeal | 104 | 100% | [63] |
| Malawi 1983 | Intraoropharyngeal | 104 | 100% | [63] |
| Georgia 2007 | Eating porcine plasma in complete feed † | 104.3 | 0% | [68] |
| Brazil 1978 | Intranasal | 104.5 | 100% | [65] |
| Dominican Republic 1979 | Intranasal/oral | 104.7 | 87.5% | [64] |
| Georgia 2007 | Eating soft ticks in brioche † | 104–105 | 33% | [69] |
| Georgia 2007 | Eating porcine plasma in complete feed † | 105 | 0% | [68] |
| Unknown | Eating infectious material † | 105 ¶ | MID | [70] |
| Tanzania KWH/12 | Drinking in cow milk † | 105 | 37.5% | [67] |
| Georgia 2007 | Eating in complete feed † | 105 | 44.4% | [51] |
| Tengani | Intranasal | 105 | 100% | [70] |
| Georgia 2007 | Eating in brioche † | 105.5 | 0% | [69] |
| Dominican Republic 1979 | Intranasal/oral | 105.7 | 90% | [64] |
| Georgia 2007 | Eating in complete feed † | 106 | 25% | [51] |
| Tanzania KWH/12 | Drinking in cow milk † | 106 | 75% | [67] |
| Malawi 1983 | Intranasopharyngeal | 106 | 100% | [63] |
| Malawi 1983 | Intraoropharyngeal | 106 | 100% | [63] |
| Georgia 2007 | Eating soft ticks in brioche † | 106–107 | 100% | [69] |
| Georgia 2007 | Eating in complete feed † | 107 | 40% | [51] |
| Tanzania KWH/12 | Drinking in cow milk † | 107 | 100% | [67] |
| Hinde WH II | Oral | 107–107.5 | 100% | [71] |
| Hinde WH II | Eating in dry feed † | 107–107.5 | 100% | [71] |
| Tengani | Intranasal | 107.2 | 100% | [72] |
| Georgia 2007 | Eating in complete feed † | 108 | 50% | [51] |
| Tanzania KWH/12 | Drinking in cow milk † | 108 | 100% | [67] |
| Kenya | Eating feces or urine contaminated feed † | ND | 100% | [14] |
| Kenya | Eating in sweet potatoes or bananas † | ND | 0% | [14] |
| Pathogen | Mitigant Composition | Inclusion Rate | Testing Method | Outcome or Effects | Reference |
|---|---|---|---|---|---|
| ASFV | Aqueous formaldehyde and propionic acid, MCFA (C6:C8:C10) | 0.03–1.0% | Cell culture; tested in complete feed and ingredients at mean 12.3 °C temperature in a 30-day transoceanic shipment model | Dose-dependent inactivation; reduced infectivity in feed ingredients; decreased viral DNA quantity in feed a | [94] |
| ASFV | MCFA (C8:C10:C12); GML | 0.25–2.0% | Cell culture; complete feed stored for 30 min or 1 day at room temperature | Decreased virus titers in cell culture by MCFA and GML; dose-dependent antiviral activity by GML; reduced infectivity in complete feed by GML at ≥1.0%; no effect on viral DNA | [95] |
| PRRSV, SVA, PEDV | Aqueous formaldehyde, organic acids, acidifiers, HMTBa, SCFA, MCFA, LCFA, GML, and essential oils | 0.1–3.0% | Ingestion of complete feed via natural consumption for 15 days | Decreased clinical signs and virus detection in biological samples; increased weight gain b | [96] |
| PEDV | Lactic acid | 0.75–1.5% | Stored in complete feed at 20 °C for 1 day | Reduced infectivity in feed | [97] |
| PEDV | Aqueous formaldehyde and propionic acid | 0.33% | Stored in complete feed and ingredients under winter conditions (mean temperature between −9 °C and −18 °C) for 30 days | Reduced infectivity in feed and ingredients; decreased viral RNA quantity in feed | [98] |
| PEDV | Aqueous formaldehyde and propionic acid; MCFA (C6:C8:C10) | 0.36–11.1% | Tested in rice hulls flushed through feed manufacturing equipment after complete feed | Decreased viral RNA quantity in rice hull flush a | [99] |
| PEDV | Benzoic acid and essential oils | 0.02–0.5% | Stored in complete feed for 42 days | Decreased viral RNA quantity in feed on combination treatment with both additives; no effect on virus infectivity in feed | [100] |
| PEDV | Aqueous formaldehyde and propionic acid; MCFA (C6:C8:C10) | 0.33–2.0% | Tested in complete feed and ingredients at a mean 6.1 °C temperature in a 37-day transoceanic shipment model | Reduced infectivity in feed ingredients; decreased viral RNA quantity in feed a | [41] |
| PEDV | Aqueous formaldehyde and propionic acid | 0.32% | Ingestion of complete feed via natural consumption for 14 days | Prevented transmission to pigs through contaminated feed; decreased viral RNA quantity in feed | [101] |
| PEDV | Organic acids, acidifiers, sucrose, and sodium chloride | 0.2–0.4% | Stored in complete feed at 25 °C for 21 days | Increased rate of virus decay in complete feed c | [89] |
| PEDV | Aqueous formaldehyde and propionic acid; MCFA (C6:C8:C10) | 0.125–1.0% | Stored in complete feed at room temperature for 1 day | Reduced infectivity in feed; dose-dependent decreased viral RNA quantity in feed | [102] |
| PEDV | MCFA (C6:C8:C10) | 0.25–1.5% | Stored in complete feed at a mean 25.8 °C temperature for 40 days pre-inoculation; stored at room temperature for 3 days post-inoculation | Dose-dependent decreased viral RNA quantity in feed | [103] |
| PDCoV | Organic acids, acidifiers, sucrose, and sodium chloride | Low: 0.2–3.0% High: 0.4–6.0% | Stored in complete feed at 25 °C for 35 days | No effect at lower concentrations; increased rate of virus decay in complete feed at higher concentrations d | [104] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the author. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Niederwerder, M.C. Risk and Mitigation of African Swine Fever Virus in Feed. Animals 2021, 11, 792. https://doi.org/10.3390/ani11030792
Niederwerder MC. Risk and Mitigation of African Swine Fever Virus in Feed. Animals. 2021; 11(3):792. https://doi.org/10.3390/ani11030792
Chicago/Turabian StyleNiederwerder, Megan C. 2021. "Risk and Mitigation of African Swine Fever Virus in Feed" Animals 11, no. 3: 792. https://doi.org/10.3390/ani11030792
APA StyleNiederwerder, M. C. (2021). Risk and Mitigation of African Swine Fever Virus in Feed. Animals, 11(3), 792. https://doi.org/10.3390/ani11030792






