Abstract
Shigella spp. cause hundreds of millions of intestinal infections each year. They target the mucosa of the human colon and are an important model of intracellular bacterial pathogenesis. Shigella is a pathovar of Escherichia coli that is characterized by the presence of a large invasion plasmid, pINV, which encodes the characteristic type III secretion system and icsA used for cytosol invasion and cell-to-cell spread, respectively. First, we review recent advances in the genetic aspects of Shigella, shedding light on its evolutionary history within the E. coli lineage and its relationship to the acquisition of pINV. We then discuss recent insights into the processes that allow for the maintenance of pINV. Finally, we describe the role of the transcription activators VirF, VirB, and MxiE in the major virulence gene regulatory cascades that control the expression of the type III secretion system and icsA. This provides an opportunity to examine the interplay between these pINV-encoded transcriptional activators and numerous chromosome-encoded factors that modulate their activity. Finally, we discuss novel chromosomal genes icaR, icaT, and yccE that are regulated by MxiE. This review emphasizes the notion that Shigella and E. coli have walked the fine line between commensalism and pathogenesis for much of their history.
1. Introduction
Many gram-negative bacteria, such as Bordetella, Burkholderia, Citrobacter, Chlamydia, Escherichia, Pseudomonas, Rhizobium, Salmonella, Shigella, Xanthomonas, and Yersinia, interact with host cells using the syringe-shaped type III secretion system (T3SS) also known as the injectisome. This large proteinaceous complex injects substrate proteins into host cells to hijack them for the benefit of the bacteria that harbor it. Since 2015, spectacular progress has been made in describing its structure and function [1,2,3,4,5,6,7,8,9]. The T3SS is composed of the sorting platform that selects the protein substrates in the bacterial cytosol, the transmembrane needle complex that serves as a channel for the secretion of the substrates, the tip complex that triggers secretion upon sensing the physical contact with host cells, and the translocon that establishes the continuity between the needle complex and the host cytosol during the delivery of the substrates [7]. The Shigella flexneri T3SS has been one of the most extensively studied, providing us with an in-depth understanding of its role and function in pathogenesis (reviewed in [10,11,12]). In Shigella, the fate of the T3SS is tied to the large invasion plasmid that encodes it. Acquisition of this plasmid drove the evolution of Shigella spp. from Escherichia coli. This makes Shigella a powerful model to study the evolution of virulence and the interplay of the T3SS with its genome. Here, we focus on the emergence of the Shigella pathovar, the maintenance of the invasion plasmid, and the gene regulatory mechanisms that control the expression of the T3SS and of the cell-to-cell spread traits.
2. The Evolution of the Shigella Pathovar
Shigella spp. are gram-negative enterobacteria divided in four subgroups named S. boydii, S. dysenteriae, S. flexneri, and S. sonnei. Their unique pathogenesis, their lack of flagellar motility and inability to ferment lactose constitutes the hallmark of the Shigella genus established in the 1950s [13]. However, modern phylogeny approaches revealed that Shigella spp. are merely an Escherichia coli pathovar [14]. Shigella spp. infect the large intestine of humans and cause diarrheal symptoms ranging from watery to mucopurulent and bloody stools accompanied by inflammation (also known as dysentery). Shigella spp. cause 80–190 million infections [15,16], and approximately 200,000 deaths annually, with more than 50% of cases occurring in individuals younger than 5 years or older than 70 years [17]. S. flexneri is responsible for most cases and, similar to S. dysenteriae, is more common in low-income countries. By contrast, S. sonnei is responsible for most cases in high-income countries. [18]. Colony-forming units in the low hundreds can cause the disease in healthy humans [19], making Shigella more infectious than most other enterobacteria. Shigella has no known animal reservoirs and is therefore considered to be human specific. It is transmitted from person to person or by ingestion of contaminated water or food. As with other enterobacteria [20,21,22,23,24], increasing antibiotic resistance in Shigella spp. is a public health concern [20,25,26,27].
From an evolutionary perspective, Shigella emerged 35,000–270,000 years ago [28,29], contemporaneously with Homo sapiens. The evolutionary trajectories of S. dysenteriae, S. flexneri, and S. sonnei. are unique [30,31,32]. In the case of S. dysenteriae and S. sonnei, modern historical events and societal changes have greatly accelerated their expansion and spread. Shigella spp. have adapted to their human host by losing or inactivating chromosomal genes detrimental to pathogenesis [33,34]. Thus, the number of chromosomal genes in Shigella is reduced compared to their commensalistic E. coli counterparts, a phenomenon shared with several bacterial pathogens. In a remarkable example of convergent evolution, some Shigella strains lost the same chromosomal genes through disruption by discrete insertion sequences [28,35]. Thus, an intriguing question about Shigella is whether it emerged once [36], or on multiple occasions [28] within the E. coli lineage. Since these seminal studies, the number of sequenced E. coli genomes has increased dramatically, allowing further study of their phylogeny [37,38,39]. For example, analysis of 10,667 chromosome sequences, including 1283 from Shigella spp., using the fast distance estimation method MASH revealed 14 E. coli phylogroups [37]. Two of these, named Shig1 and Shig2, consisted exclusively of Shigella strains, with an overrepresentation of S. flexneri and S. sonnei, respectively, and contained most of the Shigella genomes in the dataset (Table 1). This analysis confirmed on an unprecedented scale that Shigella shared several of the hallmarks of bacterial pathogens. Indeed, Shig1 and Shig2 strains had a lower guanine-cytosine content, smaller genomes, and higher rates of gene loss and duplication on average than other E. coli phylogroups. The analyses also revealed that S. sonnei in Shig2 possesses a unique set of core genes that are not conserved in other phylogroups, highlighting its clonality and unique evolutionary origin. Nevertheless, Shigella strains were also found in seven other phylogroups (Table 1), with B1 being the most dominant. Interestingly, analyses measuring the conservation and loss of protein families confirmed the remarkable convergent evolution of Shig1 and Shigella from the B1 phylogroup. Taken together, this study provides a comprehensive overview of the diversity of Shigella, supporting the notion that it emerged multiple times.

Table 1.
Distribution of Shigella strains in E. coli phylogroups 1.
The evolution and pathogenesis of Shigella spp. and of the less virulent enteroinvasive E. coli (EIEC) is associated with the acquisition of a large invasion plasmid of 220 kbp, called pINV, which has a high degree of sequence conservation across strains [30,40,41,42,43]. The genome remodeling in EIECs is less pronounced than in Shigella. Therefore, EIECs can be described as an intermediate between commensal E. coli and Shigella, which may help us to understand the evolution of the Shigella-EIEC pathotype and the coevolution of the chromosome with pINV [42]. Since pINV played a key role in the emergence of Shigella and EIEC clades, each of them should have originated from an independent pINV acquisition event (Figure 1a). Although a consensus has emerged around this model [28,29,37,44], the fact that pINV is not conjugative, and therefore not susceptible to horizontal transfers, is a hurdle that, to our knowledge, has not yet been addressed. The alternative model proposes that pINV was acquired once by a common ancestor of all Shigella and a subset of E. coli [36] (Figure 1b). Shigella would have conserved pINV by adapting their genome to the pathogenic lifestyle, whereas non-EIEC E. coli would have lost it by failing to make these adaptations. This model accounts for the non-transmissibility of pINV, but it has its own set of challenges. Not least of these is that it requires the relatively unstable pINV to have been maintained over the evolutionary time required for the emergence of Shigella spp. Despite these limitations, we believe that the single acquisition model, or a hybrid model in which related Shigella clades may be the result of a single pINV acquisition event, should be considered in light of the large number of new sequences obtained since it was first described [36].
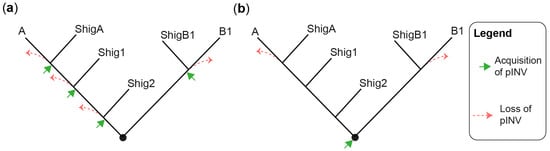
Figure 1.
Models for the emergence of Shigella from E. coli. (a) A tree illustrating the multiple pINV acquisition model. (b) A tree illustrating the single pINV acquisition model. These phylogenetic trees are qualitative and intended to be used for the sole purpose of illustrating the main difference between the two models in a straightforward manner. ShigA: Shigella from phylogroup A; ShigB1: Shigella from phylogroup B1; Shig1 and Shig2 as defined in the text and Table 1.
3. The Invasion Plasmid pINV
The discovery of pINV in the 1980s marked the beginning of the molecular era in the study of shigellosis [13]. The key feature of pINV is the pathogenicity island, called the entry region, which contains the mxi, spa, and ipa operons that encode the parts of the injectisome and the translocators needed for host cell invasion. Once Shigella reaches the host cytosol, the outer membrane protein IcsA, also encoded by pINV, propels Shigella through the formation of actin comets, which are critical for invading neighboring cells [45]. Other bacteria possessing a T3SS have operons similar to those of the entry region, although their genetic organization and names differ [7,46,47]. IcsA is unique to pINV, although unrelated proteins confer similar actin-mediated cell-to-cell spreading abilities to other bacteria [48]. Together, the entry region and icsA are required for the hallmark invasiveness of Shigella. In addition, several effector genes are distributed throughout the rest of the pINV, which abounds in insertion sequences that represent approximately 25% of the total sequence [40]. pINV also harbors genes unrelated to the T3SS that are transcribed in regular growth medium [41,49], but their contribution to pathogenesis is poorly characterized with few exceptions [50,51,52,53]. The pINV exists in two forms, designated A and B [54], and its phylogeny suggests that it was obtained through horizontal transfers. Since pINV is not conjugative, the mechanism of these transfers is unclear. However, one study reported that transfers of non-conjugative plasmids could occur at a low rate in E. coli biofilms [55]. To our knowledge, this phenomenon has not been implicated in the transfer of pINV.
The pINV is present in one to two copies per cell. Expression of T3SS-related genes renders the pINV unstable [56], resulting in a high rate of total or partial loss in the population. Nevertheless, S. flexneri uses five systems to maintain pINV. These include two partitioning systems parAB and stbAB, and three type II toxin–antitoxin (TA) systems vapBC (also known as mvpAT), ccdAB, and gmvAT [57]. By contrast, S. sonnei lacks ccdAB, gmvAT, and stbAB, and instead harbors the relBE partitioning system [58] (Figure 2). In S. flexneri, vapBC plays a dominant role in the stabilization of pINV at 37 °C, whereas gmvAT is the most important at 21 °C [59,60]. Although ccdAB is fully functional, its role can be masked by the presence of gmvAT and vapBC, suggesting that the latter two play a dominant role in the in vitro conditions tested. In the absence of the TA systems, ParAB stabilized the plasmid at 37 °C, whereas StbAB stabilized it at 21 °C in ΔparAB. These observations highlight the partial redundancy of these systems [60]. Both the ParAB and StbAB partitioning systems are functional, although their contribution to the stabilization of pINV in the presence of the TA systems is also undetectable [59]. The ability of type II TA systems to maintain a plasmid is based on the intrinsic toxicity of its toxin moiety and the shorter half-life of its antitoxin moiety [61,62]. When a daughter cell acquires a plasmid containing a type II TA system, the toxin is sequestered by the continued expression of the antitoxin. On the other hand, the loss of the plasmid reduces the amount of antitoxin, thereby killing the unfortunate daughter cell through the unchecked activity of the released toxin. This suggests that a protease must control the half-life of antitoxins. Genetic dissections suggested that both vapBC and gmvAT are regulated by lon [59]. Accordingly, a S. flexneri strain lacking the lon protease lost pINV 100 times more frequently.

Figure 2.
The invasion plasmid pINV. (a) pINV from S. flexneri strain M90T (accession number NC_024996.1). (b) pINV from S. sonnei strain 53 G (accession number NC_016833). The main features indicated in the outer rim are described in the legend. The open reading frames are represented by arrows and rectangles in the inner rims: the rims colored orange represent the top DNA strand, and the rims colored green represent the bottom DNA strand. The plasmid maps were created with Snapgene and Illustrator.
In addition, the position of the locus of the TA systems was found to influence the nature of pINV remodeling that leads to the loss of virulence [63]. In S. flexneri, the loss of virulence was mostly mediated by the deletion of the entry region through recombination events involving flanking insertion sequences. The displacement of vapBC near the entry region abolished most of these recombination events [63]. Thus, in addition to its global effect on the stability of pINV, vapBC can exert a local stabilizing effect on neighboring genes. This means that the variation in the position of the TA systems could have consequences, although its relevance in Shigella is unknown. Indeed, it is noteworthy that the position of vapBC is conserved in S. flexneri and S. sonnei (Figure 2). Finally, this study also characterized the reversible integration on pINV in the chromosome through the recombination of insertion sequences. This suggests a pathway for the transfer of pathogenicity islands from the plasmid to the chromosome.
The absence of gmvAT in S. sonnei destabilizes its pINV at room temperature [60]. Thus, the instability of pINV when S. sonnei is not in its host may explain why it is often transmitted from person to person [60]. It is arguable that the specific characteristics of S. sonnei’s pINV may allow further evolution of this lineage into an obligate pathogenic lifestyle. Interestingly, the reintroduction of the two missing TA systems ccdAB and gmvAT in S. sonnei stabilized its pINV, but not to the same extent as in S. flexneri [58]. A role for the relBE partitioning system unique to S. sonnei was rejected under the conditions tested. Instead, the data suggest that a K32R polymorphism in the toxin VapC toxin contributes to the instability of S. sonnei’s pINV. How this mutation affects the activity of VapBC is unknown, but a reduction in the endonuclease activity of the toxin was ruled out [58].
Taken together, the diverse combination of maintenance systems of the sonnei and the flexneri subgroups determines the stability of their respective versions of pINV, which affects their pathogenesis and epidemiology. Accordingly, these maintenance systems are practical for typing Shigella strains because they are better conserved than T3SS-related genes and reproduces the phylogeny obtained using chromosomal genes [64]. This supports the importance of these maintenance systems in the pathogenesis and the evolution of Shigella.
4. The Major Virulence Gene Regulatory Cascade in Shigella
The recent acquisition of pINV provides an opportunity to inspect its interaction with the chromosome at the gene expression level. In this section, we will focus on factors that directly control the expression of T3SS-related genes and icsA. Their expression is regulated by the temperature and the activation of the injectisomes. This occurs mainly at the transcriptional level through a virulence gene regulatory cascade consisting of the histone-like nucleoid structuring protein (H-NS) encoded in the chromosome, and the transcriptional activators VirF, VirB, and MxiE encoded in pINV (Figure 3a,b).
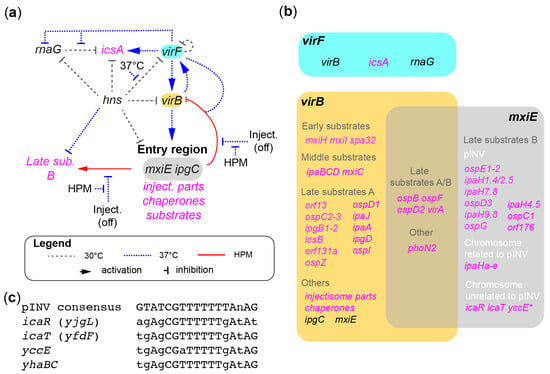
Figure 3.
The major gene regulatory cascade in Shigella. (a) The signaling network regulating the expression of the invasive (T3SS) and cell-to-cell spread (icsA) traits in Shigella. It is centered around a vertical axis composed of transcription activators virF, virB, and mxiE and negatively regulated by hns at 30 °C. Events dominating at 30 °C, 37 °C, and when the injectisomes (inject.) are activated by contact with the HPM are represented as indicated in the legend. The transcription regulators and their terminal targets are written in black and magenta, respectively. (b) The virF, virB, and mxiE regulon. (c) The MxiE boxes of novel chromosomal genes icaR, icaT, yccE, and yhaBC compared with the consensus MxiE box of pINV-related members of the MxiE regulon.
H-NS is the negative regulator of the cascade. It is a DNA-binding protein that silences the expression of horizontally transferred genes, which is also known as xenogeneic silencing [65]. For example, E. coli lacking H-NS increased expression of xenogenes with a high adenine-thymine content [66]. The structure of H-NS associated with DNA is unknown, but molecular dynamics predicted that H-NS uses a three-residue motif to bind the minor groove of DNA in adenine-thymine rich stretches separated by 8–17 base pairs in two possible binding modes [67,68]. Indeed, H-NS can bind a single stretch of DNA through a stiffening linear mode, which is dominant at physiological magnesium concentrations, or two stretches of DNA through a bridging mode, which is stabilized at supraphysiological magnesium concentrations [69]. H-NS can repress transcription initiation regardless of the binding mode used, while the bridging mode is hypothesized to also inhibit transcription elongation [68]. H-NS has multiple validated and potential binding sites in the entry region as well as in other regions of pINV and in T3SS-related chromosomal genes with a high adenine-thymine content (~65%). Indeed, H-NS silences the promoters of virF, virB, and most T3SS-related genes at room temperature (<32 °C) [65,70,71,72,73]. At temperatures similar to those of its host (37 °C), the binding of H-NS to the virF promoter is weakened, thereby allowing the production of the VirF protein [72,73]. A shorter version of VirF (VirF21; MW 21 kDa), generated from an alternative translation initiation codon also contributes to repressing the production of the full-length VirF protein at 30 °C [74,75]. This regulatory mechanism may contribute to maintaining tight control of virulence, but its role in pathogenesis is unknown.
The first step in the gene regulatory cascade is controlled by VirF. It is a transcriptional activator of the AraC family that stimulates the expression of virB and icsA at 37 °C [73] (Figure 3a,b). A minor role of VirF in the regulation of icsP, which encodes a post-translational regulator of icsA, has also been reported [76]. Thus, the regulation of these genes by VirF allows for the coordination of the expression of the invasion and cell-to-cell spreading traits, which, if you recall, are hallmarks of Shigella pathogenesis. VirF and H-NS have several partially overlapping binding sites around or downstream of the −10 box of icsA and its small RNA attenuator RnaG [77]. RnaG attenuates icsA expression at 30 °C and to some extent at 37 °C as well. In contrast, H-NS silences icsA at 30 °C, whereas at 37 °C VirF relieves H-NS-mediated silencing, thereby upregulating icsA transcription [77]. At 37 °C, VirF may also repress the expression of rnaG [77] and stabilize icsA mRNA by disrupting the transcription attenuation duplex the latter can form with RnaG [78]. Taken together, these studies suggest that VirF dual-activates icsA through the release of both H-NS transcriptional repression and RnaG attenuation of its mRNA. Similarly, virB is positively regulated by VirF and negatively regulated by H-NS [70]. However, the mechanism by which VirF activates virB has unique features. First, there is evidence that VirF must form a dimer to bind icsA, whereas this is not required for its binding to virB or rnaG [79,80]. Second, two DNA regions are required for the VirF-dependent expression of virB [81]. The first one is located in the virB promoter (−110 to −80), as expected. The second, however, is located in the coding sequence of the neighboring genes ipaA and acp (−976 to −402). Binding at both sites may be necessary to completely remove H-NS from the area. In brief, VirF is the master activator of the gene regulatory cascade and it acts primarily by inhibiting H-NS-mediated silencing. This allows VirF to directly control the expression of icsA required for cell-to-cell spread, and indirectly control the expression of the T3SS by regulating the expression of VirB.
The second step in the gene regulatory cascade is controlled by VirB. It is a transcriptional activator of the ParB family whose members are mostly DNA partition proteins. Nevertheless, VirB activates the transcription of T3SS-related genes in the entry region and elsewhere in pINV, hence playing the central role in the expression of the T3SS (Figure 3a,b). Its consensus binding sequence is known, although there are conflicting reports on its size [81,82,83,84]. The largest proposed binding site seems to be relevant because its occurrence is proportional to the number of genes regulated by VirB [81]. Furthermore, VirB is involved in two positive feedback loops that stimulate the transcription of its target genes as well as that of virF at 37 °C [83]. Interestingly, through interactions with its binding sites, VirB is recruited to distinct cellular foci in a manner similar to related proteins involved in plasmid partitioning [85]. Indeed, a single VirB DNA binding site of 25 base pairs installed on a small plasmid induced GFP-VirB objects visible by light microscopy, suggesting that VirB may form large oligomers on its target gene. Like VirF, VirB probably functions by displacing H-NS from its target genes. It does this likely by forming large oligomers that nucleate from binding sites that can be within a few hundred base pairs from the transcription start sites [71,76,84,86,87,88,89]. In the absence of H-NS, VirB was unable to stimulate transcription. This suggests that it acts as an antisilencing factor to derepress transcription [88]. It has been proposed that VirB relieves H-NS silencing by reducing negative supercoiling of the DNA in the vicinity of its binding sites [90]. In short, VirF together with VirB through the transcription of their target genes at 37 °C ensure that the T3SS is assembled and ready to function only when Shigella is in its host. VirB controls the expression of the invasive phenotype through the production of the injectisome parts, chaperones, and early, middle, and late substrates A. It also controls the expression of the third transcriptional activator MxiE [12].
The final step in the gene regulatory cascade is controlled by MxiE. It is a transcriptional activator of the AraC family that controls the expression of genes encoding a subset of the T3SS substrates called the late substrates B [12], also known as second wave effectors. The activity of MxiE is regulated at the post-translational level by the activity of the injectisome (Figure 3a). Prior to secretion, the formation of a 1:1 complex between IpgC and IpaB [91], or with IpaC, and between OspD1 and MxiE [92], prevents MxiE-IpgC-mediated transcriptional activation. By contrast, upon the T3SS-mediated secretion of the antiactivator OspD1 and the anticoactivators IpaB and IpaC, MxiE, in cooperation with its co-activator IpgC, activates the expression of genes encoding late substrates B [12,92,93,94], which are secreted last during host cell invasion. The genes regulated by MxiE and IpgC have a consensus MxiE box in their promoter [95,96]. The binding of a MxiE-IpgC complex to the MxiE box has been inferred from the comparable dampening of gene expression in ΔmxiE and ΔipgC strains [94], but has not been demonstrated. On the other hand, the existence of a MxiE-IpgC complex is supported by the co-elution of these proteins from an affinity column [97]. MxiE was thought to activate transcription by promoting the recruitment of the RNA polymerase, similar to known members of the AraC family [98]. However, in Shigella expressing a defective H-NS, MxiE is dispensable for the transcription of target genes [99]. This suggests that MxiE may activate transcription by inhibiting H-NS silencing similarly to VirF and VirB. Finally, MxiE and IpgC form a negative feedback loop that represses virB, but not icsA, in a VirF-dependent manner [81]. Whether, this requires the formation of a tripartite complex between these proteins is unknown. The genes activated by MxiE and IpgC were initially determined from a gene microarray focused on the virulence plasmid [100] (Figure 3b). Several of the genes regulated by MxiE have fascinating enzymatic activities that hijack the host cell immune response and programed cell death pathways [10,101,102,103,104,105,106,107]. Thus, the effectors encoded by MxiE-regulated genes are critical for post-invasion steps of pathogenesis, particularly for evading host defense. In brief, MxiE-mediated transcriptional regulation is critical for controlling the expression of the late substrate B, thereby contributing to the orderly secretion of substrates via the T3SS [12].
For years, the only MxiE-regulated chromosomal genes were ipaH genes, which have family members in pINV [96]. By contrast, a genome-wide transcriptome analysis of Shigella added two new genes to the MxiE regulon [49]. The proteins encoded by these genes are secreted by the T3SS as late substrates B [108]. We named them icaR (also known as gem3 or yjgL), and icaT (also known as gem1 or yfdF), which stand for invasion chromosome antigen with homology for a transcription regulator and a transposase, respectively. Interestingly, the appearance of icaR and icaT likely preceded the acquisition of pINV, as they are found in several E. coli phylogroups [108]. An independent genome-wide transcriptome analysis identified yccE as a third novel chromosomal gene regulated by MxiE and IpgC [99]. Indeed, yccE possessed a MxiE box and is regulated by the activity of the T3SS, similar to icaR and icaT. In addition, icaR (yjgL), icaT (yfdF), and yccE were previously reported to be upregulated in the absence of H-NS in E. coli [66], thereby supporting the notion that MxiE inhibits H-NS silencing to activate its target genes [99]. Upon re-examination of the raw data in [49], we found a short operon called yhaBC that harbors an unstudied MxiE-box that is remarkably similar to those of yccE, icaR, and icaT (Figure 3c). Furthermore, we confirmed that yccE and yhaBC are present in almost all E. coli strains harboring icaR and icaT [108] (Table A1). Based on this evidence, we speculate that, long before the acquisition of the modern pINV by Shigella, the E. coli lineage harbored one or more mobile genetic elements carrying these four ancient genes and their transcriptional regulators mxiE and ipgC or relatives. These four genes were independently transferred to the chromosome at about the same time, and silenced by the loss of their regulators until reactivated by the acquisition of pINV. Given their ancestral nature, these genes are unlikely to be critical for pathogenesis, although this has not been ruled out at the time of writing.
5. Chromosome Factors Modulating the Virulence Gene Regulatory Cascade
The activity of the virulence gene regulatory cascade is modulated by metabolic or environmental parameters that are sensed by several chromosome-encoded factors. In this section, the factors regulating virF and virB will be discussed in turn. For example, virF is the nexus of several signaling cross-talks involving proteins such as FIS, IHF, MiaA, and TGT, which have been reviewed elsewhere [73] (Figure 4a).
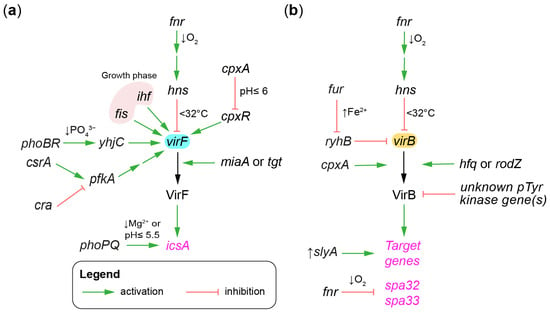
Figure 4.
Chromosome genes regulating the gene regulatory cascade. Chromosome genes and environmental cues modulating the expression of: (a) virF; (b) virB. The arrows toward virF and virB indicate transcriptional regulation. The arrows toward VirB indicate post-translational regulation. The arrows toward the black arrow joining virF-VirF or virB-VirB indicate post-transcriptional or translational regulation. Arrows toward VirB indicate post-translational regulation. The regulators and their terminal targets are written in black and magenta, respectively.
In addition, several two-component systems have been implicated in the adaptation of Shigella’s virulence to its environment [109]. For instance, during its journey through the gastrointestinal tract, Shigella switches from an acidic environment in the stomach to a near-neutral pH in the terminal ileum and in the descending colon [110]. The two-component system cpxAR, which is involved in the membrane stress response, regulates the expression of virF in a pH-dependent manner. At physiological pH (7.4), virF is well expressed, whereas at acidic pH (6.0), virF expression is reduced, resulting in a 10-fold reduction in S. sonnei invasiveness [111]. The response regulator CpxR directly binds to the virF promoter and is essential for its activity at both pHs [112], whereas the sensor kinase CpxA is only required for acidic pH repression [111]. These findings suggest that CpxR might be activated by another sensor kinase at physiological pH. The elongation factor P regulates this process by stimulating the translation of cpxA in S. flexneri [113]. Finally, CpxA promotes virB expression at the post-transcriptional level through an unknown mechanism [114] (Figure 4b).
PhoBR is a two-component system that is activated by phosphate starvation. PhoB moderately activated the expression of yhjC [115], which encodes a LysR transcriptional regulator that activates virF expression in Shigella. Indeed, YhjC binds directly to the virF promoter to activate its expression, and in ΔyhjC, the expression of virF and of its targets virB and icsA were downregulated, which dampened the invasiveness of this strain [116].
PhoPQ is a two-component system involved in the adaptation to low Mg2+ and the expression of acid resistance genes [117]. A ΔphoPQ strain was attenuated in cell invasion assays and in the Sereny test, and was more sensitive to the antimicrobial polymixin B. The expression of 11 genes, including icsA, was activated by PhoP, which directly bound their promoter. This two-component system is also involved in the regulation of pINV genes that are unrelated to the T3SS, but nonetheless involved in virulence [51,118].
The glycolysis pathway also modulates the expression of virF in S. flexneri. Indeed, a strain lacking pfkA, which encodes the major phoshphofructokinase, was attenuated due to reduced virF expression [119]. Two regulators of the glycolytic pathway, the mRNA binding protein csrA and the transcriptional regulator cra, also affected the virulence. This study suggested this was through their effect on pfkA. The mechanism by which pfkA regulates virF is currently unknown, but is likely indirect. Interestingly, csrA regulates the T3SS in other bacteria [120].
Iron levels in E. coli are sensed by the ferric uptake regulator protein (Fur). Iron (II)-bound Fur, also known as holo-Fur, represses most of its target genes [121,122,123], such as the small RNA RyhB. By contrast, when the cytosolic concentration of iron is low, the concentration of RyhB increases, which represses its own target genes [124,125]. In Shigella, RyhB binds to a complementary region in the coding sequence of VirB to repress its expression [126,127]. RyhB targets the template strand of VirB [127], suggesting a transcriptional interference mechanism. Therefore, a reduced amount of VirB through the action of RyhB would lead to a lower production of injectisome parts, and consequently to a reduction in the number of injectisomes on the bacterial surface. Indeed, overexpression of RyhB reduced plaque formation by 20-fold in a strain that contained an integral RyhB binding site in virB, whereas a strain with a disrupted binding site was unaffected [127]. The RyhB-mediated downregulation of VirB also decreased the expression of icsP [128], which is important for the proper function of IcsA in cell-to-cell spreading. Taken together, iron replete conditions enhanced the invasion phenotype by stimulating the T3SS and cell-to-cell spreading. By contrast, the stx gene, which encodes the Shiga toxin, is upregulated under iron-deficient conditions in E. coli and in S. dysenteriae [123,129,130]. This suggests that iron controls the balance between the invasion and Shiga toxin arms of S. dysenteriae pathogenesis.
T3SS expression is also repressed under anaerobic conditions via the activation of the fumarate and nitrate reduction regulatory protein (FNR). Two distinct mechanisms have been proposed. First, FNR represses the expression of genes encoding the switch regulator Spa32 and the injectisome part Spa33 by directly binding to their promoters [131]. Second, through an unknown mechanism FNR cascades to enhance the H-NS-mediated silencing of virF and virB, thereby inducing a broader downregulation of the T3SS than initially hypothesized [132]. The expression of several chromosome genes was also affected by oxygen deprivation in an FNR-dependent or -independent manner. This suggests an adaptation of Shigella to hypoxia that extends beyond the T3SS. Whether these adaptations are specific to Shigella or shared with E. coli has not been investigated to our knowledge.
VirB is also targeted at the post-transcriptional level. For example, the destabilization of the mRNA of virB by the RNA chaperone Hfq and the cytoskeletal protein RodZ could contribute to the repression of VirB production, particularly at 30 °C [133,134]. This process would potentially synergize with the H-NS silencing to restrict virulence at ambient temperatures. Several virulence-associated proteins have been identified in the Shigella phosphotyrosine proteome [135]. The phosphorylation of VirB on its Tyr100 could inhibit its function. Indeed, the introduction of a phosphomimetic mutation at this position prevented the expression of its target gene icsP. The abundance and significance of phospho-VirB and its cognate protein tyrosine kinase are unknown. The consensus sequence of the phosphosites is well conserved [135], suggesting that one or a small group of related kinases may be responsible for most of the phospotyrosines [136]. The significance of this mode of VirB regulation is unknown, but is probably minor compared to its transcriptional regulation.
SlyA is a transcriptional regulator of the MarR/SlyA family that activates the expression of chaperones and acid resistance genes, and represses genes in the histidine biosynthetic pathway. It is negatively autoregulated and positively regulated by PhoP [137]. It is also involved in the regulation of T3SS genes through an unknown mechanism. Indeed, in a ΔvirB strain, the production of SlyA at supraphysiological levels can rescue the expression of injectisome parts [137]. Notably, SlyA has been hypothesized to derepress H-NS-mediated silencing similarly to VirB [138], thus suggesting a general mechanism by which supraphysiological levels of SlyA could complement ΔvirB. The significance of SlyA as an alternative counter-silencing factor of the entry region in the context of infection is unknown.
To our knowledge, there are no chromosome-encoded factors, other than H-NS, that modulate the activity of mxiE or of its cognate protein. Since the function of MxiE normally occurs during the invasion of host cells, whose environmental conditions cannot be reproduced in vitro, the modulation of this transcriptional activator is difficult to study. It is therefore plausible that such modulatory processes are just waiting to be discovered.
6. Conclusions
The evolution of the different Shigella subgroups and of EIECs is linked to the acquisition of the invasion plasmid pINV. Although most strains converge towards similar genetic adaptation, such as shared gene attrition, it is reasonable to assume that they may not be at the same stage of coevolution of their chromosome with pINV. The comparative study of carefully selected Shigella and EIEC strains belonging to different phylogroups could be harnessed to reconstruct the evolutionary interactions between their genome and the pathogenic lifestyle conferred by pINV. A contrasting model of interest is Yersinia, which has its own T3SS-encoding plasmid and adopts an extracellular pathogenic lifestyle different from that of Shigella. Perhaps such approaches could be used to create predictive models of the future evolution of Shigella and Yersinia pathogenesis. Due to its recent emergence, Shigella pathogenesis can be described as an intermediate state between commensalism and obligate pathogenesis. Interestingly, the metastability of its virulence is mirrored by that of pINV, which is less stable in S. sonnei than in S. flexneri. The genetic interplay between the pINV and the chromosome extends to the expression of virulence traits. Indeed, the master silencer H-NS and a plethora of secondary regulators encoded in the chromosome modulate the virulence gene regulatory cascade centered around the pINV transcriptional activators VirF, VirB, and MxiE. This cross-talk is indeed surprisingly rich given the short evolutionary timeline of Shigella. Furthermore, the MxiE-regulated chromosomal genes icaR, icaT, yccE, and the poorly characterized yhaBC operon are conserved across E. coli phylogroups. Taken together, these observations support the idea that the last common ancestor of Shigella and several E. coli had a long association with pINV, its ancestors, or related plasmids. This provides further evidence that E. coli, including Shigella spp., have walked the fine line between commensalism and pathogenesis throughout much of their evolution. Future advances promise to deepen our understanding of the fluidity between commensalism and pathogenesis in E. coli and Shigella spp. Finally, the detailed understanding of the virulence gene regulatory cascade and its regulators provides opportunities to develop antivirulence therapeutic strategies. Indeed, small molecules that suppress the expression of the T3SS could be useful to contain Shigella outbreaks and to replace antibiotics.
Author Contributions
N.H.-A., F.O.M. and N.S. contributed to the literature searches, wrote the first draft of the subsections of the text, and edited the text; N.S. contributed Figure 2 and Table A1; S.M.P. edited the text and contributed to writing the final version; F.-X.C.-V. wrote the first draft, including the remaining figures and tables, edited the text, and wrote the final version. All authors have read and agreed to the published version of the manuscript.
Funding
This work was funded by the Faculty of Science of the University of Ottawa, the Discovery grant no. 05587 from the Natural Sciences and Engineering Research Council of Canada (NSERC) and the grant no. 159517 from the Canadian Institutes of Health Research (CIHR). N.H.-A. and N.S. previously held a scholarship from the NSERC CREATE program entitled Technologies for Microbiome Science and Engineering (TECHNOMISE), and F.O.M. is a PGSD NSERC Scholar.
Data Availability Statement
Not applicable.
Acknowledgments
The authors are grateful to the staff of the Faculty of Science and, more broadly, to the University of Ottawa for their support of our research activities. (in French) Les auteurs tiennent à remercier le personnel de la Faculté des sciences et plus largement de l’Université d’Ottawa pour leur soutien à nos activités de recherche.
Conflicts of Interest
The authors declare no conflict of interest. The funders had no role in the design of the study; in the collection, analyses, or interpretation of data; in the writing of the manuscript; or in the decision to publish the results.
Correction Statement
This article has been republished with a minor correction to resolve some typos and the readability of Table 1. This change does not affect the scientific content of the article.
Appendix A

Table A1.
Occurrence of yccE and yhaBC in strains in which icaR and icaT presence was previously investigated [109] 1.
Table A1.
Occurrence of yccE and yhaBC in strains in which icaR and icaT presence was previously investigated [109] 1.
| Phylogroups | Strains Name | Accession Number | yccE | yhaBC |
|---|---|---|---|---|
| Shigella | S. flexneri 5a str. M90T | NZ_CM001474.1 | Yes | Yes |
| S. flexneri 2a str. 301 | NC_00337.2 | Yes | Yes | |
| S. boydii Sb227 | NC_007613.1 | Yes | Yes | |
| S. sonnei strain SE6-1 | NZ_CP055292.1 | Yes | Yes | |
| S. sonnei Ss046 | CP000038.1 | Yes | No 2 | |
| S. dysenteriae Sd197 | NC_007606.1 | Yes | No 2 | |
| A | E. coli str. K-12 substr. MG1655 | U00096.3 | Yes | Yes |
| E. coli strain NCTC86 | NZ_CP019778.1 | Yes | Yes | |
| E. coli ETEC H10407 | NC_017633.1 | Yes | Yes | |
| E. coli HS | NC_009800.1 | Yes | Yes | |
| B1 | E. coli O103:H2 str. 12009 | NC_013353.1 | Yes | Yes |
| E. coli 55989 | NC_011748.1 | Yes | Yes | |
| E. coli W | NC_017635.1 | Yes | Yes | |
| E. coli O26: H11 str. 11368 | NC_013361.1 | Yes | Yes | |
| B2 | E. coli O127:H6 str. E2348/69 | NC_011601.1 | No | No |
| E. coli 536 | NC_008253.1 | No | No | |
| E. coli SE15 | NC_013654.1 | No | No | |
| E. coli ABU 83972 | NC_017631.1 | No | No | |
| E. coli CFT073 | NZ_CP051263.1 | No | No | |
| D | E. coli 042 | NC_017626.1 | Yes | Yes |
| E. coli UMN026 | NC_011751.1 | Yes | Yes | |
| E. coli SMS-3-5 | NC_010498.1 | Yes | Yes | |
| E. coli IAI39 | NC_011750.1 | Yes | Yes | |
| E | E. coli O157:H7 strain ATCC43888 | NZ_CP041623.1 | Yes | Yes |
| E. coli O157:H7 str. Sakai | NC_002695.1 | Yes | Yes | |
| E. coli O55:H7 str. CB9615 | NC_013941.1 | Yes | Yes | |
| E. coli O157:H7 str. EDL933 | NZ_CP008957.1 | Yes | Yes |
1 yccE and yhaBC are present in the same strains as icaR and icaT. One main exception: a partly disrupted icaR was observed in E. coli O127:H6 str. E2348/69, whereas icaT, yccE, and yhaBC were absent. icaR and icaT were also pseudogenes in S. sonnei Ss046 and S. dysenteriae Sd197 [109]. yhaC has a premature stop codon in S. flexneri 5a str. M90T. The BLAST reported in this table were performed with this truncated version; we have not investigated whether yhaC is integral in the other strains. 2 yhaBC is present as a pseudogene in these Shigella strains, similar to icaT [109].
References
- Hu, B.; Morado, D.R.; Margolin, W.; Rohde, J.R.; Arizmendi, O.; Picking, W.L.; Picking, W.D.; Liu, J. Visualization of the Type III Secretion Sorting Platform of Shigella flexneri. Proc. Natl. Acad. Sci. USA 2015, 112, 1047–1052. [Google Scholar] [CrossRef] [PubMed]
- Tachiyama, S.; Chang, Y.; Muthuramalingam, M.; Hu, B.; Barta, M.L.; Picking, W.L.; Liu, J.; Picking, W.D. The Cytoplasmic Domain of MxiG Interacts with MxiK and Directs Assembly of the Sorting Platform in the Shigella Type III Secretion System. J. Biol. Chem. 2019, 294, 19184–19196. [Google Scholar] [CrossRef] [PubMed]
- Hu, B.; Lara-Tejero, M.; Kong, Q.; Galán, J.E.; Liu, J. In Situ Molecular Architecture of the Salmonella Type III Secretion Machine. Cell 2017, 168, 1065–1074.e10. [Google Scholar] [CrossRef]
- Hu, J.; Worrall, L.J.; Vuckovic, M.; Hong, C.; Deng, W.; Atkinson, C.E.; Brett Finlay, B.; Yu, Z.; Strynadka, N.C.J. T3S Injectisome Needle Complex Structures in Four Distinct States Reveal the Basis of Membrane Coupling and Assembly. Nat. Microbiol. 2019, 4, 2010–2019. [Google Scholar] [CrossRef]
- Guo, E.Z.; Galán, J.E. Cryo-EM Structure of the Needle Filament Tip Complex of the Salmonella Type III Secretion Injectisome. Proc. Natl. Acad. Sci. USA 2021, 118, e2114552118. [Google Scholar] [CrossRef]
- Park, D.; Lara-Tejero, M.; Waxham, M.N.; Li, W.; Hu, B.; Galán, J.E.; Liu, J. Visualization of the Type III Secretion Mediated Salmonella-Host Cell Interface Using Cryo-Electron Tomography. eLife 2018, 7, e39514. [Google Scholar] [CrossRef]
- Deng, W.; Marshall, N.C.; Rowland, J.L.; McCoy, J.M.; Worrall, L.J.; Santos, A.S.; Strynadka, N.C.J.; Finlay, B.B. Assembly, Structure, Function and Regulation of Type III Secretion Systems. Nat. Rev. Microbiol. 2017, 15, 323–337. [Google Scholar] [CrossRef] [PubMed]
- Lara-Tejero, M.; Galán, J.E. The Injectisome, a Complex Nanomachine for Protein Injection into Mammalian Cells. EcoSal Plus 2019, 8, 245–259. [Google Scholar] [CrossRef] [PubMed]
- Hu, J.; Worrall, L.J.; Strynadka, N.C. Towards Capture of Dynamic Assembly and Action of the T3SS at near Atomic Resolution. Curr. Opin. Struct. Biol. 2020, 61, 71–78. [Google Scholar] [CrossRef] [PubMed]
- Schnupf, P.; Sansonetti, P.J. Shigella Pathogenesis: New Insights through Advanced Methodologies. Microbiol. Spectr. 2019, 7, 15–39. [Google Scholar] [CrossRef]
- Kang, E.; Crouse, A.; Chevallier, L.; Pontier, S.M.; Alzahrani, A.; Silué, N.; Campbell-Valois, F.-X.; Montagutelli, X.; Gruenheid, S.; Malo, D. Enterobacteria and Host Resistance to Infection. Mamm. Genome 2018, 29, 558–576. [Google Scholar] [CrossRef]
- Bajunaid, W.; Haidar-Ahmad, N.; Kottarampatel, A.H.; Manigat, F.O.; Silué, N.; Tchagang, C.F.; Tomaro, K.; Campbell-Valois, F.-X. The T3ss of Shigella: Expression, Structure, Function, and Role in Vacuole Escape. Microorganisms 2020, 8, 1933. [Google Scholar] [CrossRef]
- Lampel, K.A.; Formal, S.B.; Maurelli, A.T. A Brief History of Shigella. EcoSal Plus 2018, 8, 1–25. [Google Scholar] [CrossRef] [PubMed]
- Lan, R.; Reeves, P.R. Escherichia Coli in Disguise: Molecular Origins of Shigella. Microbes Infect. 2002, 4, 1125–1132. [Google Scholar] [CrossRef] [PubMed]
- Watkins, L.K.F.; Appiah, G.D. Shigellosis—Chapter 4—2020 Yellow Book|Travelers’ Health|CDC. Available online: https://wwwnc.cdc.gov/travel/yellowbook/2020/travel-related-infectious-diseases/shigellosis (accessed on 12 August 2022).
- Kotloff, K.L.; Riddle, M.S.; Platts-Mills, J.A.; Pavlinac, P.; Zaidi, A.K.M. Shigellosis. Lancet 2018, 391, 801–812. [Google Scholar] [CrossRef]
- GBD 2016 Diarrhoeal Disease Collaborators. Estimates of the Global, Regional, and National Morbidity, Mortality, and Aetiologies of Diarrhoea in 195 Countries: A Systematic Analysis for the Global Burden of Disease Study 2016. Lancet Infect. Dis. 2018, 18, 1211–1228. [Google Scholar] [CrossRef] [PubMed]
- Thompson, C.N.; Duy, P.T.; Baker, S. The Rising Dominance of Shigella sonnei: An Intercontinental Shift in the Etiology of Bacillary Dysentery. PLoS Negl. Trop. Dis. 2015, 9, e0003708. [Google Scholar] [CrossRef]
- Kothary, M.H.; Babu, U.S. Infective Dose of Foodborne Pathogens in Volunteers: A Review. J. Food Saf. 2001, 21, 49–73. [Google Scholar] [CrossRef]
- World Health Organization. List of Antibiotic Resistant Bacteria to Guide Research, Discovery and Development of New Antibiotics; World Health Organization: Geneva, Switzerland, 2017.
- Iredell, J.; Brown, J.; Tagg, K. Antibiotic Resistance in Enterobacteriaceae: Mechanisms and Clinical Implications. BMJ 2016, 352, h6420. [Google Scholar] [CrossRef]
- Lynch, J.P.; Clark, N.M.; Zhanel, G.G. Escalating Antimicrobial Resistance among Enterobacteriaceae: Focus on Carbapenemases. Expert Opin. Pharmacother. 2021, 22, 1455–1474. [Google Scholar] [CrossRef]
- Antimicrobial Resistance Collaborators. Global Burden of Bacterial Antimicrobial Resistance in 2019: A Systematic Analysis. Lancet 2022, 399, 629–655. [Google Scholar] [CrossRef]
- Center for Disease Control and Prevention (USA). Antibiotic Resistance Threats in the United States; Department of Health and Human Services: Washington, DC, USA, 2019. [CrossRef]
- Baker, S.; Scott, T.A. Antimicrobial-Resistant Shigella: Where Do We Go Next? Nat. Rev. Microbiol. 2023, 21, 409–410. [Google Scholar] [CrossRef]
- Lefèvre, S.; Njamkepo, E.; Feldman, S.; Ruckly, C.; Carle, I.; Lejay-Collin, M.; Fabre, L.; Yassine, I.; Frézal, L.; Pardos de la Gandara, M.; et al. Rapid Emergence of Extensively Drug-Resistant Shigella sonnei in France. Nat. Commun. 2023, 14, 462. [Google Scholar] [CrossRef]
- Mason, L.C.E.; Greig, D.R.; Cowley, L.A.; Partridge, S.R.; Martinez, E.; Blackwell, G.A.; Chong, C.E.; De Silva, P.M.; Bengtsson, R.J.; Draper, J.L.; et al. The Evolution and International Spread of Extensively Drug Resistant Shigella sonnei. Nat. Commun. 2023, 14, 1983. [Google Scholar] [CrossRef]
- Pupo, G.M.; Lan, R.; Reeves, P.R. Multiple Independent Origins of Shigella Clones of Escherichia coli and Convergent Evolution of Many of Their Characteristics. Proc. Natl. Acad. Sci. USA 2000, 97, 10567–10572. [Google Scholar] [CrossRef] [PubMed]
- The, H.C.; Thanh, D.P.; Holt, K.E.; Thomson, N.R.; Baker, S. The Genomic Signatures of Shigella Evolution, Adaptation and Geographical Spread. Nat. Rev. Microbiol. 2016, 14, 235–250. [Google Scholar] [CrossRef]
- Holt, K.E.; Baker, S.; Weill, F.-X.; Holmes, E.C.; Kitchen, A.; Yu, J.; Sangal, V.; Brown, D.J.; Coia, J.E.; Kim, D.W.; et al. Shigella sonnei Genome Sequencing and Phylogenetic Analysis Indicate Recent Global Dissemination from Europe. Nat. Genet. 2012, 44, 1056–1059. [Google Scholar] [CrossRef] [PubMed]
- Njamkepo, E.; Fawal, N.; Tran-Dien, A.; Hawkey, J.; Strockbine, N.; Jenkins, C.; Talukder, K.A.; Bercion, R.; Kuleshov, K.; Kolínská, R.; et al. Global Phylogeography and Evolutionary History of Shigella dysenteriae Type 1. Nat. Microbiol. 2016, 1, 16027. [Google Scholar] [CrossRef] [PubMed]
- Connor, T.R.; Barker, C.R.; Baker, K.S.; Weill, F.-X.; Talukder, K.A.; Smith, A.M.; Baker, S.; Gouali, M.; Pham Thanh, D.; Jahan Azmi, I.; et al. Species-Wide Whole Genome Sequencing Reveals Historical Global Spread and Recent Local Persistence in Shigella flexneri. eLife 2015, 4, e07335. [Google Scholar] [CrossRef]
- Maurelli, A.T.; Fernández, R.E.; Bloch, C.A.; Rode, C.K.; Fasano, A. “Black Holes” and Bacterial Pathogenicity: A Large Genomic Deletion That Enhances the Virulence of Shigella spp. and Enteroinvasive Escherichia coli. Proc. Natl. Acad. Sci. USA 1998, 95, 3943–3948. [Google Scholar] [CrossRef] [PubMed]
- Maurelli, A.T. Black holes, antivirulence genes, and gene inactivation in the evolution of bacterial pathogens. FEMS Microbiol. Lett. 2007, 267, 1–8. [Google Scholar] [CrossRef]
- Hawkey, J.; Monk, J.M.; Billman-Jacobe, H.; Palsson, B.; Holt, K.E. Impact of Insertion Sequences on Convergent Evolution of Shigella Species. PLoS Genet. 2020, 16, e1008931. [Google Scholar] [CrossRef]
- Escobar-Páramo, P.; Giudicelli, C.; Parsot, C.; Denamur, E. The Evolutionary History of Shigella and Enteroinvasive Escherichia coli Revised. J. Mol. Evol. 2003, 57, 140–148. [Google Scholar] [CrossRef] [PubMed]
- Abram, K.; Udaondo, Z.; Bleker, C.; Wanchai, V.; Wassenaar, T.M.; Robeson, M.S.; Ussery, D.W. Mash-Based Analyses of Escherichia Coli Genomes Reveal 14 Distinct Phylogroups. Commun. Biol. 2021, 4, 117. [Google Scholar] [CrossRef] [PubMed]
- Touchon, M.; Perrin, A.; de Sousa, J.A.M.; Vangchhia, B.; Burn, S.; O’Brien, C.L.; Denamur, E.; Gordon, D.; Rocha, E.P. Phylogenetic Background and Habitat Drive the Genetic Diversification of Escherichia coli. PLoS Genet. 2020, 16, e1008866. [Google Scholar] [CrossRef] [PubMed]
- Gonzalez-Alba, J.M.; Baquero, F.; Cantón, R.; Galán, J.C. Stratified Reconstruction of Ancestral Escherichia coli Diversification. BMC Genom. 2019, 20, 936. [Google Scholar] [CrossRef] [PubMed]
- Buchrieser, C.; Glaser, P.; Rusniok, C.; Nedjari, H.; D’Hauteville, H.; Kunst, F.; Sansonetti, P.; Parsot, C. The Virulence Plasmid PWR100 and the Repertoire of Proteins Secreted by the Type III Secretion Apparatus of Shigella flexneri. Mol. Microbiol. 2000, 38, 760–771. [Google Scholar] [CrossRef] [PubMed]
- Cervantes-Rivera, R.; Tronnet, S.; Puhar, A. Complete Genome Sequence and Annotation of the Laboratory Reference Strain Shigella flexneri Serotype 5a M90T and Genome-Wide Transcriptional Start Site Determination. BMC Genom. 2020, 21, 215–285. [Google Scholar] [CrossRef] [PubMed]
- Pasqua, M.; Michelacci, V.; Di Martino, M.L.; Tozzoli, R.; Grossi, M.; Colonna, B.; Morabito, S.; Prosseda, G. The Intriguing Evolutionary Journey of Enteroinvasive E. coli (EIEC) toward Pathogenicity. Front. Microbiol. 2017, 8, 2390. [Google Scholar] [CrossRef]
- Yang, F.; Yang, J.; Zhang, X.; Chen, L.; Jiang, Y.; Yan, Y.; Tang, X.; Wang, J.; Xiong, Z.; Dong, J.; et al. Genome Dynamics and Diversity of Shigella Species, the Etiologic Agents of Bacillary Dysentery. Nucleic Acids Res. 2005, 33, 6445–6458. [Google Scholar] [CrossRef] [PubMed]
- Sims, G.E.; Kim, S.-H. Whole-Genome Phylogeny of Escherichia coli/Shigella Group by Feature Frequency Profiles (FFPs). Proc. Natl. Acad. Sci. USA 2011, 108, 8329–8334. [Google Scholar] [CrossRef] [PubMed]
- Campbell-Valois, F.-X.; Pontier, S.M. Implications of Spatiotemporal Regulation of Shigella flexneri Type Three Secretion Activity on Effector Functions: Think Globally, Act Locally. Front. Cell. Infect. Microbiol. 2016, 6, 28. [Google Scholar] [CrossRef]
- Izoré, T.; Job, V.; Dessen, A. Biogenesis, Regulation, and Targeting of the Type III Secretion System. Structure 2011, 19, 603–612. [Google Scholar] [CrossRef] [PubMed]
- Abby, S.S.; Cury, J.; Guglielmini, J.; Néron, B.; Touchon, M.; Rocha, E.P.C. Identification of Protein Secretion Systems in Bacterial Genomes. Sci. Rep. 2016, 6, 23080. [Google Scholar] [CrossRef] [PubMed]
- Stevens, J.M.; Galyov, E.E.; Stevens, M.P. Actin-Dependent Movement of Bacterial Pathogens. Nat. Rev. Microbiol. 2006, 4, 91–101. [Google Scholar] [CrossRef]
- Silué, N.; Marcantonio, E.; Campbell-Valois, F.-X. RNA-Seq Analysis of the T3SA Regulon in Shigella flexneri Reveals Two New Chromosomal Genes Upregulated in the on-State. Methods 2020, 176, 71–81. [Google Scholar] [CrossRef]
- D’Hauteville, H.; Khan, S.; Maskell, D.J.; Kussak, A.; Weintraub, A.; Mathison, J.; Ulevitch, R.J.; Wuscher, N.; Parsot, C.; Sansonetti, P.J. Two MsbB Genes Encoding Maximal Acylation of Lipid A Are Required for Invasive Shigella flexneri to Mediate Inflammatory Rupture and Destruction of the Intestinal Epithelium. J. Immunol. 2002, 168, 5240–5251. [Google Scholar] [CrossRef]
- Goldman, S.R.; Tu, Y.; Goldberg, M.B. Differential Regulation by Magnesium of the Two MsbB Paralogs of Shigella flexneri. J. Bacteriol. 2008, 190, 3526–3537. [Google Scholar] [CrossRef]
- Sidik, S.; Kottwitz, H.; Benjamin, J.; Ryu, J.; Jarrar, A.; Garduno, R.; Rohde, J.R. A Shigella flexneri Virulence Plasmid Encoded Factor Controls Production of Outer Membrane Vesicles. G3 Genes Genomes Genet. 2014, 4, 2493–2503. [Google Scholar] [CrossRef] [PubMed]
- Meza-Segura, M.; Birtley, J.R.; Maldonado-Contreras, A.; Mueller, C.; Simin, K.J.; Stern, L.J.; McCormick, B.A. SepA Enhances Shigella Invasion of Epithelial Cells by Degrading Alpha-1 Antitrypsin and Producing a Neutrophil Chemoattractant. mBio 2021, 12, e0283321. [Google Scholar] [CrossRef]
- Lan, R.; Lumb, B.; Ryan, D.; Reeves, P.R. Molecular Evolution of Large Virulence Plasmid in Shigella Clones and Enteroinvasive Escherichia coli. Infect. Immun. 2001, 69, 6303–6309. [Google Scholar] [CrossRef] [PubMed]
- Maeda, S.; Ito, M.; Ando, T.; Ishimoto, Y.; Fujisawa, Y.; Takahashi, H.; Matsuda, A.; Sawamura, A.; Kato, S. Horizontal Transfer of Nonconjugative Plasmids in a Colony Biofilm of Escherichia coli. FEMS Microbiol. Lett. 2006, 255, 115–120. [Google Scholar] [CrossRef] [PubMed]
- Schuch, R.; Maurelli, A.T. Virulence Plasmid Instability in Shigella flexneri 2a Is Induced by Virulence Gene Expression. Infect. Immun. 1997, 65, 3686–3692. [Google Scholar] [CrossRef] [PubMed]
- Pilla, G.; Tang, C.M. Going around in Circles: Virulence Plasmids in Enteric Pathogens. Nat. Rev. Microbiol. 2018, 16, 484–495. [Google Scholar] [CrossRef] [PubMed]
- Martyn, J.E.; Pilla, G.; Hollingshead, S.; Winther, K.S.; Lea, S.; McVicker, G.; Tang, C.M. Maintenance of the Shigella sonnei Virulence Plasmid Is Dependent on Its Repertoire and Amino Acid Sequence of Toxin-Antitoxin Systems. J. Bacteriol. 2022, 204, e0051921. [Google Scholar] [CrossRef] [PubMed]
- McVicker, G.; Hollingshead, S.; Pilla, G.; Tang, C.M. Maintenance of the Virulence Plasmid in Shigella flexneri Is Influenced by Lon and Two Functional Partitioning Systems. Mol. Microbiol. 2019, 111, 1355–1366. [Google Scholar] [CrossRef] [PubMed]
- McVicker, G.; Tang, C.M. Deletion of Toxin-Antitoxin Systems in the Evolution of Shigella sonnei as a Host-Adapted Pathogen. Nat. Microbiol. 2016, 2, 16204–16211. [Google Scholar] [CrossRef]
- Fraikin, N.; Goormaghtigh, F.; Van Melderen, L. Type II Toxin-Antitoxin Systems: Evolution and Revolutions. J. Bacteriol. 2020, 202, e00763-19. [Google Scholar] [CrossRef] [PubMed]
- Kamruzzaman, M.; Wu, A.Y.; Iredell, J.R. Biological Functions of Type II Toxin-Antitoxin Systems in Bacteria. Microorganisms 2021, 9, 1276. [Google Scholar] [CrossRef]
- Pilla, G.; McVicker, G.; Tang, C.M. Genetic Plasticity of the Shigella Virulence Plasmid Is Mediated by Intra- and Inter-Molecular Events between Insertion Sequences. PLoS Genet. 2017, 13, e1007014-19. [Google Scholar] [CrossRef] [PubMed]
- Pilla, G.; Arcari, G.; Tang, C.M.; Carattoli, A. Virulence Plasmid PINV as a Genetic Signature for Shigella flexneri Phylogeny. Microb. Genom. 2022, 8, mgen000846. [Google Scholar] [CrossRef] [PubMed]
- Picker, M.A.; Wing, H.J. H-NS, Its Family Members and Their Regulation of Virulence Genes in Shigella Species. Genes 2016, 7, 112. [Google Scholar] [CrossRef] [PubMed]
- Lamberte, L.E.; Baniulyte, G.; Singh, S.S.; Stringer, A.M.; Bonocora, R.P.; Stracy, M.; Kapanidis, A.N.; Wade, J.T.; Grainger, D.C. Horizontally Acquired AT-Rich Genes in Escherichia Coli Cause Toxicity by Sequestering RNA Polymerase. Nat. Microbiol. 2017, 2, 16249. [Google Scholar] [CrossRef] [PubMed]
- Riccardi, E.; van Mastbergen, E.C.; Navarre, W.W.; Vreede, J. Predicting the Mechanism and Rate of H-NS Binding to AT-Rich DNA. PLoS Comput. Biol. 2019, 15, e1006845. [Google Scholar] [CrossRef] [PubMed]
- Shen, B.A.; Hustmyer, C.M.; Roston, D.; Wolfe, M.B.; Landick, R. Bacterial H-NS Contacts DNA at the Same Irregularly Spaced Sites in Both Bridged and Hemi-Sequestered Linear Filaments. iScience 2022, 25, 104429. [Google Scholar] [CrossRef]
- Liu, Y.; Chen, H.; Kenney, L.J.; Yan, J. A Divalent Switch Drives H-NS/DNA-Binding Conformations between Stiffening and Bridging Modes. Genes Dev. 2010, 24, 339–344. [Google Scholar] [CrossRef]
- Tobe, T.; Yoshikawa, M.; Mizuno, T.; Sasakawa, C. Transcriptional Control of the Invasion Regulatory Gene VirB of Shigella flexneri: Activation by VirF and Repression by H-NS. J. Bacteriol. 1993, 175, 6142–6149. [Google Scholar] [CrossRef]
- Beloin, C.; Dorman, C.J. An Extended Role for the Nucleoid Structuring Protein H-NS in the Virulence Gene Regulatory Cascade of Shigella flexneri. Mol. Microbiol. 2003, 47, 825–838. [Google Scholar] [CrossRef] [PubMed]
- Falconi, M.; Colonna, B.; Prosseda, G.; Micheli, G.; Gualerzi, C.O. Thermoregulation of Shigella and Escherichia coli EIEC Pathogenicity. A Temperature-Dependent Structural Transition of DNA Modulates Accessibility of VirF Promoter to Transcriptional Repressor H-NS. EMBO J. 1998, 17, 7033–7043. [Google Scholar] [CrossRef]
- Di Martino, M.L.; Falconi, M.; Micheli, G.; Colonna, B.; Prosseda, G. The Multifaceted Activity of the VirF Regulatory Protein in the Shigella Lifestyle. Front. Mol. Biosci. 2016, 3, 61. [Google Scholar] [CrossRef]
- Di Martino, M.L.; Romilly, C.; Wagner, E.G.H.; Colonna, B.; Prosseda, G. One Gene and Two Proteins: A Leaderless MRNA Supports the Translation of a Shorter Form of the Shigella VirF Regulator. mBio 2016, 7, e01860-16. [Google Scholar] [CrossRef] [PubMed]
- Skovajsová, E.; Colonna, B.; Prosseda, G.; Sellin, M.E.; Di Martino, M.L. The VirF21:VirF30 Protein Ratio Is Affected by Temperature and Impacts Shigella flexneri Host Cell Invasion. FEMS Microbiol. Lett. 2022, 369, fnac043. [Google Scholar] [CrossRef] [PubMed]
- Wing, H.J.; Yan, A.W.; Goldman, S.R.; Goldberg, M.B. Regulation of IcsP, the Outer Membrane Protease of the Shigella Actin Tail Assembly Protein IcsA, by Virulence Plasmid Regulators VirF and VirB. J. Bacteriol. 2004, 186, 699–705. [Google Scholar] [CrossRef] [PubMed]
- Tran, C.N.; Giangrossi, M.; Prosseda, G.; Brandi, A.; Di Martino, M.L.; Colonna, B.; Falconi, M. A Multifactor Regulatory Circuit Involving H-NS, VirF and an Antisense RNA Modulates Transcription of the Virulence Gene IcsA of Shigella flexneri. Nucleic Acids Res. 2011, 39, 8122–8134. [Google Scholar] [CrossRef] [PubMed]
- Giangrossi, M.; Giuliodori, A.M.; Tran, C.N.; Amici, A.; Marchini, C.; Falconi, M. VirF Relieves the Transcriptional Attenuation of the Virulence Gene IcsA of Shigella flexneri Affecting the IcsA mRNA-RnaG Complex Formation. Front. Microbiol. 2017, 8, 650. [Google Scholar] [CrossRef]
- Ragazzone, N.J.; Dow, G.T.; Garcia, G.A. Elucidation of Key Interactions between VirF and the VirB Promoter in Shigella flexneri Using E. coli MarA- and GadX-Based Homology Models and In Vitro Analysis of the DNA-Binding Domains of VirF and MarA. J. Bacteriol. 2022, 204, e0014322. [Google Scholar] [CrossRef]
- Dow, G.T.; Young, A.M.; Garcia, G.A. Elucidation of the DNA-Binding Activity of VirF from Shigella flexneri for the IcsA and RnaG Promoters and Characterization of the N-Terminal Domain To Identify Residues Crucial for Dimerization. J. Bacteriol. 2023, 205, e0001523. [Google Scholar] [CrossRef]
- McKenna, J.A.; Karney, M.M.A.; Chan, D.K.; Weatherspoon-Griffin, N.; Becerra Larios, B.; Pilonieta, M.C.; Munson, G.P.; Wing, H.J. The AraC/XylS Protein MxiE and Its Coregulator IpgC Control a Negative Feedback Loop in the Transcriptional Cascade That Regulates Type III Secretion in Shigella flexneri. J. Bacteriol. 2022, 204, e0013722. [Google Scholar] [CrossRef]
- Taniya, T.; Mitobe, J.; Nakayama, S.; Mingshan, Q.; Okuda, K.; Watanabe, H. Determination of the InvE Binding Site Required for Expression of IpaB of the Shigella sonnei Virulence Plasmid: Involvement of a ParB BoxA-like Sequence. J. Bacteriol. 2003, 185, 5158–5165. [Google Scholar] [CrossRef] [PubMed]
- Kane, K.A.; Dorman, C.J. VirB-Mediated Positive Feedback Control of the Virulence Gene Regulatory Cascade of Shigella flexneri. J. Bacteriol. 2012, 194, 5264–5273. [Google Scholar] [CrossRef]
- Weatherspoon-Griffin, N.; Picker, M.A.; Pew, K.L.; Park, H.S.; Ginete, D.R.; Karney, M.M.; Usufzy, P.; Castellanos, M.I.; Duhart, J.C.; Harrison, D.J.; et al. Insights into Transcriptional Silencing and Anti-Silencing in Shigella flexneri: A Detailed Molecular Analysis of the IcsP Virulence Locus. Mol. Microbiol. 2018, 108, 505–518. [Google Scholar] [CrossRef] [PubMed]
- Socea, J.N.; Bowman, G.R.; Wing, H.J. VirB, a Key Transcriptional Regulator of Virulence Plasmid Genes in Shigella flexneri, Forms DNA-Binding Site Dependent Foci in the Bacterial Cytoplasm. J. Bacteriol. 2021, 203, e00627-20. [Google Scholar] [CrossRef] [PubMed]
- Karney, M.M.; McKenna, J.A.; Weatherspoon-Griffin, N.; Karabachev, A.D.; Millar, M.E.; Potocek, E.A.; Wing, H.J. Investigating the DNA-Binding Site for VirB, a Key Transcriptional Regulator of Shigella Virulence Genes, Using an In Vivo Binding Tool. Genes 2019, 10, 149. [Google Scholar] [CrossRef] [PubMed]
- Basta, D.W.; Pew, K.L.; Immak, J.A.; Park, H.S.; Picker, M.A.; Wigley, A.F.; Hensley, C.T.; Pearson, J.S.; Hartland, E.L.; Wing, H.J. Characterization of the OspZ Promoter in Shigella flexneri and Its Regulation by VirB and H-NS. J. Bacteriol. 2013, 195, 2562–2572. [Google Scholar] [CrossRef] [PubMed]
- Turner, E.C.; Dorman, C.J. H-NS Antagonism in Shigella flexneri by VirB, a Virulence Gene Transcription Regulator That Is Closely Related to Plasmid Partition Factors. J. Bacteriol. 2007, 189, 3403–3413. [Google Scholar] [CrossRef] [PubMed]
- McKenna, J.A.; Wing, H.J. The Antiactivator of Type III Secretion, OspD1, Is Transcriptionally Regulated by VirB and H-NS from Remote Sequences in Shigella flexneri. J. Bacteriol. 2020, 202, e00072-20. [Google Scholar] [CrossRef] [PubMed]
- Picker, M.A.; Karney, M.M.A.; Gerson, T.M.; Karabachev, A.D.; Duhart, J.C.; McKenna, J.A.; Wing, H.J. Localized Modulation of DNA Supercoiling, Triggered by the Shigella Anti-Silencer VirB, Is Sufficient to Relieve H-NS-Mediated Silencing. Nucleic Acids Res. 2023, 51, 3679–3695. [Google Scholar] [CrossRef]
- Ferrari, M.L.; Charova, S.N.; Sansonetti, P.J.; Mylonas, E.; Gazi, A.D. Structural Insights of Shigella Translocator IpaB and Its Chaperone IpgC in Solution. Front. Cell. Infect. Microbiol. 2021, 11, 673122. [Google Scholar] [CrossRef]
- Parsot, C.; Ageron, E.; Penno, C.; Mavris, M.; Jamoussi, K.; d’Hauteville, H.; Sansonetti, P.; Demers, B. A Secreted Anti-Activator, OspD1, and Its Chaperone, Spa15, Are Involved in the Control of Transcription by the Type III Secretion Apparatus Activity in Shigella flexneri. Mol. Microbiol. 2005, 56, 1627–1635. [Google Scholar] [CrossRef]
- Kane, C.D.; Schuch, R.; Day, W.A.J.; Maurelli, A.T. MxiE Regulates Intracellular Expression of Factors Secreted by the Shigella flexneri 2a Type III Secretion System. J. Bacteriol. 2002, 184, 4409–4419. [Google Scholar] [CrossRef]
- Mavris, M.; Page, A.L.; Tournebize, R.; Demers, B.; Sansonetti, P.; Parsot, C. Regulation of Transcription by the Activity of the Shigella flexneri Type III Secretion Apparatus. Mol. Microbiol. 2002, 43, 1543–1553. [Google Scholar] [CrossRef]
- Mavris, M.; Sansonetti, P.J.; Parsot, C. Identification of the Cis-Acting Site Involved in Activation of Promoters Regulated by Activity of the Type III Secretion Apparatus in Shigella flexneri. J. Bacteriol. 2002, 184, 6751–6759. [Google Scholar] [CrossRef] [PubMed]
- Bongrand, C.; Sansonetti, P.J.; Parsot, C. Characterization of the Promoter, MxiE Box and 5′ UTR of Genes Controlled by the Activity of the Type III Secretion Apparatus in Shigella flexneri. PLoS ONE 2012, 7, e32862. [Google Scholar] [CrossRef] [PubMed]
- Pilonieta, M.C.; Munson, G.P. The Chaperone IpgC Copurifies with the Virulence Regulator MxiE. J. Bacteriol. 2008, 190, 2249–2251. [Google Scholar] [CrossRef] [PubMed]
- Martin, R.G.; Rosner, J.L. The AraC Transcriptional Activators. Curr. Opin. Microbiol. 2001, 4, 132–137. [Google Scholar] [CrossRef] [PubMed]
- Hall, C.P.; Jadeja, N.B.; Sebeck, N.; Agaisse, H. Characterization of MxiE- and H-NS-Dependent Expression of IpaH7.8, OspC1, YccE, and YfdF in Shigella flexneri. mSphere 2022, 7, e0048522. [Google Scholar] [CrossRef] [PubMed]
- Gall, T.L.; Mavris, M.; Martino, M.C.; Bernardini, M.L.; Denamur, E.; Parsot, C. Analysis of Virulence Plasmid Gene Expression Defines Three Classes of Effectors in the Type III Secretion System of Shigella flexneri. Microbiology 2005, 151, 951–962. [Google Scholar] [CrossRef]
- Wandel, M.P.; Pathe, C.; Werner, E.I.; Ellison, C.J.; Boyle, K.B.; von der Malsburg, A.; Rohde, J.; Randow, F. GBPs Inhibit Motility of Shigella flexneri but Are Targeted for Degradation by the Bacterial Ubiquitin Ligase IpaH9.8. Cell Host Microbe 2017, 22, 507–518.e5. [Google Scholar] [CrossRef]
- Li, P.; Jiang, W.; Yu, Q.; Liu, W.; Zhou, P.; Li, J.; Xu, J.; Xu, B.; Wang, F.; Shao, F. Ubiquitination and Degradation of GBPs by a Shigella Effector to Suppress Host Defence. Nature 2017, 551, 378–383. [Google Scholar] [CrossRef] [PubMed]
- Goers, L.; Kim, K.; Stedman, T.C.; Canning, P.J.; Mou, X.; Ernst, N.H.; Coers, J.; Lesser, C.F. Shigella IpaH9.8 Limits GBP1-Dependent LPS Release from Intracytosolic Bacteria to Suppress Caspase-4 Activation. Proc. Natl. Acad. Sci. USA 2023, 120, e2218469120. [Google Scholar] [CrossRef] [PubMed]
- Luchetti, G.; Roncaioli, J.L.; Chavez, R.A.; Schubert, A.F.; Kofoed, E.M.; Reja, R.; Cheung, T.K.; Liang, Y.; Webster, J.D.; Lehoux, I.; et al. Shigella Ubiquitin Ligase IpaH7.8 Targets Gasdermin D for Degradation to Prevent Pyroptosis and Enable Infection. Cell Host Microbe 2021, 29, 1521–1530.e10. [Google Scholar] [CrossRef] [PubMed]
- Hansen, J.M.; de Jong, M.F.; Wu, Q.; Zhang, L.-S.; Heisler, D.B.; Alto, L.T.; Alto, N.M. Pathogenic Ubiquitination of GSDMB Inhibits NK Cell Bactericidal Functions. Cell 2021, 184, 3178–3191.e18. [Google Scholar] [CrossRef] [PubMed]
- Li, Z.; Liu, W.; Fu, J.; Cheng, S.; Xu, Y.; Wang, Z.; Liu, X.; Shi, X.; Liu, Y.; Qi, X.; et al. Shigella Evades Pyroptosis by Arginine ADP-Riboxanation of Caspase-11. Nature 2021, 599, 290–295. [Google Scholar] [CrossRef] [PubMed]
- Alphonse, N.; Wanford, J.J.; Voak, A.A.; Gay, J.; Venkhaya, S.; Burroughs, O.; Mathew, S.; Lee, T.; Evans, S.L.; Zhao, W.; et al. A Family of Conserved Bacterial Virulence Factors Dampens Interferon Responses by Blocking Calcium Signaling. Cell 2022, 185, 2354–2369.e17. [Google Scholar] [CrossRef] [PubMed]
- Silué, N.; Campbell-Valois, F.-X. IcaR and IcaT Are Ancient Chromosome Genes Encoding Substrates of the Type III Secretion Apparatus in Shigella flexneri. mSphere 2022, 7, e00115-22. [Google Scholar] [CrossRef] [PubMed]
- Pasqua, M.; Coluccia, M.; Eguchi, Y.; Okajima, T.; Grossi, M.; Prosseda, G.; Utsumi, R.; Colonna, B. Roles of Two-Component Signal Transduction Systems in Shigella Virulence. Biomolecules 2022, 12, 1321. [Google Scholar] [CrossRef] [PubMed]
- Fallingborg, J. Intraluminal PH of the Human Gastrointestinal Tract. Dan. Med. Bull. 1999, 46, 183–196. [Google Scholar]
- Nakayama, S.; Watanabe, H. Involvement of CpxA, a Sensor of a Two-Component Regulatory System, in the PH-Dependent Regulation of Expression of Shigella sonnei VirF Gene. J. Bacteriol. 1995, 177, 5062–5069. [Google Scholar] [CrossRef]
- Nakayama, S.; Watanabe, H. Identification of CpxR as a Positive Regulator Essential for Expression of the Shigella sonnei VirF Gene. J. Bacteriol. 1998, 180, 3522–3528. [Google Scholar] [CrossRef]
- Marman, H.E.; Mey, A.R.; Payne, S.M. Elongation Factor P and Modifying Enzyme PoxA Are Necessary for Virulence of Shigella flexneri. Infect. Immun. 2014, 82, 3612–3621. [Google Scholar] [CrossRef]
- Mitobe, J.; Arakawa, E.; Watanabe, H. A Sensor of the Two-Component System CpxA Affects Expression of the Type III Secretion System through Posttranscriptional Processing of InvE. J. Bacteriol. 2005, 187, 107–113. [Google Scholar] [CrossRef]
- Yang, C.; Huang, T.-W.; Wen, S.-Y.; Chang, C.-Y.; Tsai, S.-F.; Wu, W.-F.; Chang, C.-H. Genome-Wide PhoB Binding and Gene Expression Profiles Reveal the Hierarchical Gene Regulatory Network of Phosphate Starvation in Escherichia coli. PLoS ONE 2012, 7, e47314. [Google Scholar] [CrossRef] [PubMed]
- Li, W.; Jiang, L.; Liu, X.; Guo, R.; Ma, S.; Wang, J.; Ma, S.; Li, S.; Li, H. YhjC Is a Novel Transcriptional Regulator Required for Shigella flexneri Virulence. Virulence 2021, 12, 1661–1671. [Google Scholar] [CrossRef] [PubMed]
- Lin, Z.; Cai, X.; Chen, M.; Ye, L.; Wu, Y.; Wang, X.; Lv, Z.; Shang, Y.; Qu, D. Virulence and Stress Responses of Shigella flexneri Regulated by PhoP/PhoQ. Front. Microbiol. 2017, 8, 2689. [Google Scholar] [CrossRef] [PubMed]
- Kaoukab-Raji, A.; Biskri, L.; Bernardini, M.-L.; Allaoui, A. Characterization of SfPgdA, a Shigella flexneri Peptidoglycan Deacetylase Required for Bacterial Persistence within Polymorphonuclear Neutrophils. Microbes Infect. 2012, 14, 619–627. [Google Scholar] [CrossRef] [PubMed]
- Gore, A.L.; Payne, S.M. CsrA and Cra Influence Shigella flexneri Pathogenesis. Infect. Immun. 2010, 78, 4674–4682. [Google Scholar] [CrossRef]
- Kusmierek, M.; Dersch, P. Regulation of Host–Pathogen Interactions via the Post-Transcriptional Csr/Rsm System. Curr. Opin. Microbiol. 2018, 41, 58–67. [Google Scholar] [CrossRef]
- Seo, S.W.; Kim, D.; Latif, H.; O’Brien, E.J.; Szubin, R.; Palsson, B.O. Deciphering Fur Transcriptional Regulatory Network Highlights Its Complex Role beyond Iron Metabolism in Escherichia coli. Nat. Commun. 2014, 5, 4910. [Google Scholar] [CrossRef]
- Troxell, B.; Hassan, H.M. Transcriptional Regulation by Ferric Uptake Regulator (Fur) in Pathogenic Bacteria. Front. Cell. Infect. Microbiol. 2013, 3, 59. [Google Scholar] [CrossRef] [PubMed]
- Mey, A.R.; Gómez-Garzón, C.; Payne, S.M. Iron Transport and Metabolism in Escherichia, Shigella, and Salmonella. EcoSal Plus 2021, 9, eESP00342020. [Google Scholar] [CrossRef]
- Massé, E.; Gottesman, S. A Small RNA Regulates the Expression of Genes Involved in Iron Metabolism in Escherichia coli. Proc. Natl. Acad. Sci. USA 2002, 99, 4620–4625. [Google Scholar] [CrossRef] [PubMed]
- Massé, E.; Vanderpool, C.K.; Gottesman, S. Effect of RyhB Small RNA on Global Iron Use in Escherichia coli. J. Bacteriol. 2005, 187, 6962–6971. [Google Scholar] [CrossRef] [PubMed]
- Murphy, E.R.; Payne, S.M. RyhB, an Iron-Responsive Small RNA Molecule, Regulates Shigella dysenteriae Virulence. Infect. Immun. 2007, 75, 3470–3477. [Google Scholar] [CrossRef] [PubMed]
- Broach, W.H.; Egan, N.; Wing, H.J.; Payne, S.M.; Murphy, E.R. VirF-Independent Regulation of Shigella VirB Transcription Is Mediated by the Small RNA RyhB. PLoS ONE 2012, 7, e38592. [Google Scholar] [CrossRef] [PubMed]
- Africa, L.A.A.; Murphy, E.R.; Egan, N.R.; Wigley, A.F.; Wing, H.J. The Iron-Responsive Fur/RyhB Regulatory Cascade Modulates the Shigella Outer Membrane Protease IcsP. Infect. Immun. 2011, 79, 4543–4549. [Google Scholar] [CrossRef] [PubMed]
- Calderwood, S.B.; Mekalanos, J.J. Iron Regulation of Shiga-like Toxin Expression in Escherichia coli Is Mediated by the Fur Locus. J. Bacteriol. 1987, 169, 4759–4764. [Google Scholar] [CrossRef] [PubMed]
- Svinarich, D.M.; Palchaudhuri, S. Regulation of the SLT-1A toxin operon by a ferric uptake regulatory protein in toxinogenic strains of Shigella dysenteria type 1. J. Diarrhoeal Dis. Res. 1992, 10, 139–145. [Google Scholar]
- Marteyn, B.; West, N.P.; Browning, D.F.; Cole, J.A.; Shaw, J.G.; Palm, F.; Mounier, J.; Prevost, M.-C.; Sansonetti, P.; Tang, C.M. Modulation of Shigella Virulence in Response to Available Oxygen In Vivo. Nature 2010, 465, 355–358. [Google Scholar] [CrossRef]
- Vergara-Irigaray, M.; Fookes, M.C.; Thomson, N.R.; Tang, C.M. RNA-Seq Analysis of the Influence of Anaerobiosis and FNR on Shigella flexneri. BMC Genom. 2014, 15, 438. [Google Scholar] [CrossRef]
- Mitobe, J.; Morita-Ishihara, T.; Ishihama, A.; Watanabe, H. Involvement of RNA-Binding Protein Hfq in the Post-Transcriptional Regulation of InvE Gene Expression in Shigella sonnei. J. Biol. Chem. 2008, 283, 5738–5747. [Google Scholar] [CrossRef] [PubMed]
- Mitobe, J.; Yanagihara, I.; Ohnishi, K.; Yamamoto, S.; Ohnishi, M.; Ishihama, A.; Watanabe, H. RodZ Regulates the Post-Transcriptional Processing of the Shigella sonnei Type III Secretion System. EMBO Rep. 2011, 12, 911–916. [Google Scholar] [CrossRef]
- Standish, A.J.; Teh, M.Y.; Tran, E.N.H.; Doyle, M.T.; Baker, P.J.; Morona, R. Unprecedented Abundance of Protein Tyrosine Phosphorylation Modulates Shigella flexneri Virulence. J. Mol. Biol. 2016, 428, 4197–4208. [Google Scholar] [CrossRef] [PubMed]
- Getz, L.J.; Runte, C.S.; Rainey, J.K.; Thomas, N.A. Tyrosine Phosphorylation as a Widespread Regulatory Mechanism in Prokaryotes. J. Bacteriol. 2019, 201, e00205-19. [Google Scholar] [CrossRef] [PubMed]
- Weatherspoon-Griffin, N.; Wing, H.J. Characterization of SlyA in Shigella flexneri Identifies a Novel Role in Virulence. Infect. Immun. 2016, 84, 1073–1082. [Google Scholar] [CrossRef] [PubMed]
- Lithgow, J.K.; Haider, F.; Roberts, I.S.; Green, J. Alternate SlyA and H-NS Nucleoprotein Complexes Control HlyE Expression in Escherichia coli K-12. Mol. Microbiol. 2007, 66, 685–698. [Google Scholar] [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).