Abstract
The growth of the elderly population is urging for more suitable biomaterials to allow the performance of better surgical and implant procedures and accelerate the patient’s healing because the elderly are more vulnerable to orthopedic and dental problems. β-phase Ti alloys can improve the mechanical properties of implants by reducing their elastic modulus and, consequently, the effects of stress shielding within bones. Therefore, the objective of this article is to study a novel ternary β-phase alloy of Ti10Mo8Nb produced by an electric arc furnace and rotary forge. The microstructure and mechanical properties of the Ti10Mo8Nb alloy were investigated in order to evaluate its suitability for biomedical applications and compare its characteristics with those present in Ti-alloys commerced or widely researched for prosthetic purposes. A tensile test, Vickers microhardness test, use of microstructure of optical microscopy for examination of microstructure, X-ray diffraction and hemolysis analysis were carried out. Thus, the Ti10Mo8Nb alloy showed suitable properties for biomedical applications, as well as having the potential to reduce the possibility to occur stress shielding after prosthetic implantations, especially for orthopedics and dentistry.
1. Introduction
The growth of the elderly population is a stimulating aspect for the advancement and diversity of novel biomaterials. A United Nations report indicates that the population over 60 years of age is expected to increase from 302 million in 2019 to 366 million in high-income countries in 2030 [1]. This information is consistent with the increase in this group even in countries whose socioeconomic structure is different. While in 2000 for 76.6% of the countries the elderly population did not represent 7% of their individuals, from 2050 onwards 57.5% of the countries will be considered aged societies (with an elderly population greater than 14%) [2,3,4]. It is therefore estimated that by 2050, approximately 1.5 billion people will be over 60 years of age. These numbers are supported, among other secondary elements, by the improvement in people’s health conditions [5].
Therefore, advances in tissue engineering and biomaterials have collaborated to assist in patient recovery. Among the areas benefiting from technological developments are orthopedics and dentistry, which have the elderly population as a vulnerable group due to the emergence of bone pathologies (e.g., osteoporosis that affects bones and teeth) [6]. Nevertheless, many materials used for bone grafting have significant restrictions that lead to new fractures within a period of up to 10 years for 60% of operated patients [7]. Such problems are potentiated once it is verified that at least 10% of patients have a slower recovery process due to factors related to age and diabetes [8]. Furthermore, for prosthetic dental implants, despite the high survival rates for fixed dental prostheses and implant-retained overdentures, common complications are observed during or after procedures, such as crown and ceramic fractures. These problems are correlated to materials properties that differ from the metallic and ceramic parts of implants, as well as to biological dental structure [9].
Thus, it is necessary to propose more suitable biomaterials to allow the performance of better surgical and implant procedures and accelerate the patient’s healing. Biomaterials span the groups of metallic, ceramic, polymeric and composite materials. Metals are highlighted in most orthopedics and dental applications because of their mechanical properties that allow restoring or stabilizing areas of the musculoskeletal system [10].
However, metallic devices might have a higher modulus of elasticity than bones, leading to the loss of bone tissue over time [10]. In this way, metals typically used in medicine such as titanium are reformulated by adding stabilizing β elements to their alloys [11]. Such elements allow a reduction in the elastic modulus, preventing bone resorption, while still ensuring considerable mechanical and chemical resistance characteristics of the alloy. Such alloys are formulated in a ternary way by combining titanium with Nb, Mo, V, Ta, Zr and Sn, for example [12,13].
On such elements, niobium was seen as interesting to replace, mainly, vanadium as an element of metal alloys (e.g., Ti6Al4V) used in the recent past for prosthetics. Vanadium in its elemental state is considered toxic and it is being correlated to cases of neurological disorders (e.g., Alzheimer’s) and organ inflammation [14,15]. Niobium, on the other hand, does not show this toxicity, although it maintains the same effect as a β stabilizing agent [16,17]. Moreover, the production of niobium has a strong relationship with Brazil, since the country has 16 million tons of that material, accounting for 91% of its production globally. It is also estimated that such reserves allow the supplementation of that material to the world for four centuries. Thus, studies related to the use of niobium favor both the development of more adequate biomedical devices and have a direct impact on the Brazilian production chain and global supplementation [18]. Another element that is used in biomedical applications is molybdenum. It was widely investigated for biomedical application because it has appropriate mechanical properties and biocompatibility, as well as being a strong stabilizer of β-phase for concentrations higher than 10% [19,20,21,22].
Although the use of niobium and molybdenum dates from the 1970s, studies of the microstructure of alloys with these elements are relatively recent [16]. Suresh S. et al. (2022) studied the effect of the concentration of niobium, molybdenum and chromium in titanium alloys, identifying that the porosity of the material is reduced and its mechanical properties improved with the addition of 8% Nb and 3% Mo–Cr to the alloy [23]. Suesawadwanid N. et al. (2022) investigated ways to improve the stress shielding effect on medical implants and observed that the ductility of the alloys was increased for high stabilizing β insertion, as in tests with Ti25Nb [24]. The results presented in the literature, however, are still limited to the correlation of the effects of different concentrations of stabilizing β elements on the material’s microstructure and, consequently, on its properties. These aspects are fundamental for proposing better solutions for biomaterials used as implants.
Thus, the objective of this article is to study a novel ternary β-phase alloy composed of titanium, molybdenum and niobium (Ti10Mo8Nb) produced by an electric arc furnace and rotary forge. The microstructure and mechanical properties of the Ti10Mo8Nb alloy were investigated and compared to the characteristics present in commercially prosthetic alloys used nowadays in order to propose a more suitable biomaterial for orthopedic and dental implants.
2. Materials and Methods
2.1. Alloy Processing of Ti10Mo8Nb
The samples of Ti10Mo8Nb alloy were obtained from the fusion of commercially pure (CP) titanium (Sandinox, Sorocaba, Brazil, 99.8% of purity), molybdenum (Sigma-Aldrich, Jurubatuba, Brazil, 99.9% of purity) and niobium (Sandinox, Sorocaba, Brazil, 99.9% of purity) in an electric arc furnace (LABMET, Campinas, Brazil) with inert atmosphere (argon gas) and crucible of water-cooled copper. Before melting, the metals were cleaned using chemical pickling in a solution formed by 50 mL of H2SO4 (98%) 20 mL of HF (48%), 20 mL of HNO3 (70%) and 10 mL of distilled water and weighed according to the composition studied. The ingot obtained with the melting was remelted 7 to 10 times in order to homogenize the alloy, turning it over before each time. The solubilization treatment was carried out in a tubular oven (LG&E, Louisville, KY, USA). The ingot was vacuum encapsulated in a quartz tube due to the reactivity of titanium with oxygen. The homogenization of the ingots was carried out at 1200 °C for a period of 24 h.
The ingots were cold-formed in such a way that there was a decrease in the diameter of the sample in the order of 20% in diameter. Rotary forging was carried out (equipment by FENN Torin, East Berlin, CT, USA) using models 6F (2² to 3/8²) and 3F (1/2² to 1/8²), with a speed of 1700 rotations per minute (rpm), 30 CV (HP). The ingots (in bar format after rotary swaging) were subjected to the solubilization heat treatment at 950 °C for 2 h, followed by rapid cooling in water. Thus, the ingots were sectioned into cylindric discs.
2.2. Tensile Test
Tensile test was managed in order to compare the mechanical properties of the Ti10Mo8Nb alloy with commercially pure (CP) Ti, Ti7.5Mo, Ti15Mo and Ti6Al4V. The test responses are critical for the development of biomedical implants due to the body load applied [24]. Five cylindrical tensile specimens were machined from Ti10Mo8Nb alloy in accordance with ASTM 638 EM. The uniaxial tensile tests were performed at room temperature on a servo-hydraulic testing machine (Instron, São José dos Pinhais, Brazil) and crosshead speed of 8.33 × 10−6 m/s−1 according to ASTM E 8M standard. The average values for ultimate tensile strength, yield strength at 0.2% offset, Young’s modulus and elongation were determined.
2.3. Microhardness Evaluation
Microhardness was evaluated in order to visualize material wear that has impact on prothetic development and aging of the material inside the body [25]. The Vickers microhardness test (HV) was carried out in accordance with ASTM E 384 using a microhardness tester (Shimadzu, Tamboré, Brazil). The microhardness tests were carried out on the 4 specimens. For each specimen, 9 measurements were made on HV and HB hardness scales, with a load equal to 200 g of force and lasting 10 s. The microstructure and the topography of the alloy after Vickers hardness test were investigated by optical microscope (Olympus, Tokyo, Japan).
2.4. Microstructural Characterization
The microstructure of the alloy after the tensile test was examined by optical microscopy (MO). Thus, the grain size and the physical characteristics of the Ti10Mo8Nb alloy were investigated. The samples for the microstructural characterization were ground, polished and etched with Kroll’s reagents (5 mL HF, 10 mL HNO3 and 85 mL H2O. Prolab, São Paulo, Brazil).
2.5. Fractography
For the study of fractography, scanning electron microscopy (SEM) was used to determine the cause of failure and the relationship between the failure mode and the microstructure of the material under analysis. The specimens submitted to traction were evaluated in order to analyze the fracture behavior. For the technique, SEM (Zeiss EVO LS-15, Jena, Germany) was used.
2.6. X-ray Diffraction Analysis
The phase identification was performed for identifying the presence of β-phase in the ternary alloy, using X-ray diffraction (XRD) equipment from Carls Zeiss model EVO MA (Jena, Germany) 15 at room temperature with Cu Kα radiation operated at 40 kV and 30 mA and 2θ in the range 10–90°.
2.7. Hemolysis
The hemolysis test was conducted in order to evaluate the in vitro cytotoxicity of the material and identify if it has compatibility to be placed invasively in the body without presenting a destructive response to blood cells. The test was performed following the ASTM F756-08 standard, with samples of Ti10Mo8Nb and CP Ti sterilized by UV for 30 min and subsequent application of 10 mL of 0.9% saline solution on the samples placed inside falcon tubes with anticoagulant of sodium citrate (3.2%). The positive control group was made with the addition of 0.2 mL of blood in 10 mL of distilled water and the negative control group was made with the addition of 0.2 mL of blood in 10 mL of 0.9% sodium chloride. A 0.2 mL solution made with 4 mL of blood with 5 mL of 0.9% saline solution was placed on the Ti10Mo8Nb and CP Ti samples, then stored in an oven at 37 °C for 1 h and then centrifuged for 5 min at 2500 rpm (model BE 4000 brushless). The absorbance reading was taken in a spectrometer using a wavelength of 540 nm.
3. Results and Discussion
In this study, the ingots of the β-phase ternary Ti10Mo8Nb were produced in disk format by arc furnace and rotary forge, as specified in the methodology. Thus the analysis of the microstructure and mechanical properties of the alloy could be carried out in order to assess its suitability for prosthetic purposes in orthopedic and dental areas. According to the standards ASTM E 8M and ASTM 638 EM, the specimens were machined and subjected to uniaxial tensile loading along their axes and registered in Table 1. The result showed that the Ti10Mo8Nb alloy exhibits higher tensile strength and yield strength values only than CP Ti. When compared to other titanium alloys currently studied for biomedical applications, the alloy showed lower tensile and yield strength. With a significantly higher plastic deformation than all others titanium alloys presented in Table 1, the Ti10Mo8Nb alloy reached 35%, which can be explained by the presence of Mo and Nb capable of improving the plasticity of the material [26,27].
The elastic modulus of the Ti10Mo8Nb alloy (91.0 + 1.0 GPa) was considered relatively high compared to other titanium alloys. However, it is lower than CP Ti and Ti6Al4V alloy, which was considered in the recent past an applicable alloy for biomedical applications. Mo and Nb alloying elements added to titanium are classified as β-phase stabilizers, which is identified as the phase with the lowest modulus of elasticity among the existing phases in titanium alloys [19,24,26,28]. From Table 1, it is also possible to observe that the Ti7.5Mo alloy (α-phase) exhibits the lowest elastic modulus value. This fact can be explained by the presence of the ω phase in the β-phase alloys, which occurs due to the fast cooling of the alloy and is facilitated by high concentrations of Mo, as with the Ti15Mo alloy. The ω phase can change the properties of the materials by improving the tensile strength and, on the other hand, reducing the plasticity and ductility of the materials (ω phase 1 and ω phase 2) [29,30].
The analysis of the modulus of elasticity possible from Table 1 is essential for reducing the effect of stress shielding in orthopedic and dental implants. Stress shielding occurs because bone, which supports the load by itself, now has the implant as a co-participant element in the load-carrying capacity. Therefore, as specified by Wolff’s law, the decrease in the stress over the bone causes a loss of mass and it becomes more fragile, thin and porous. Moreover, the occurrence of stress shielding occurs primarily due to differences in the modulus of elasticity of the implant and bone [31,32]. It is known that cortical bone, which is more compact and dense, has a typical modulus of elasticity between 2–30 GPa, as well as trabecular bone, which is more porous and spongy, and has a modulus of elasticity between 0.01–4.5 GPa. Thus, the production of implantable materials with a modulus of elasticity closer to that of bones favors the prevention of stress shielding and, consequently, bone tissue resorption [28,31,32,33,34].
Furthermore, the composition of binary, ternary or quaternary alloys with stabilizers α, α + β or β helps to reduce the elastic modulus. The β stabilizer is identified to ensure lower alloys’ elastic modulus. In the case of the proposed alloy, Mo is an isomorphic β element that can, above all, improve the mechanical strength of the alloy, as can be seen in the face of CP Ti characteristics in Table 1 [28].

Table 1.
Tensile test data of the Ti alloys for comparing their mechanical parameters [35,36,37,38,39].
Table 1.
Tensile test data of the Ti alloys for comparing their mechanical parameters [35,36,37,38,39].
| Alloys | Yield Strength (MPa) | Tensile Strength (MPa) | Elastic Modulus (GPa) | Elongation (%) | References |
|---|---|---|---|---|---|
| Ti10Mo8Nb | 691 ± 110 | 884 ± 75 | 91 ± 1 | 32 ± 8 | This study |
| CP Ti | 523 ± 11 | 673 ± 11 | 108 ± 4 | 24 ± 1 | Bocchetta P. et al. (2021), Sneddon S. et al. (2021), Weng W. et al. (2021), Souza B. L. et al. (2017), Ho W. et al. (2008) |
| Ti7.5Mo | 737 ± 18 | 1019 ± 15 | 70 ± 3 | 16 ± 1 | |
| Ti15Mo | 745 ± 13 | 921 ± 19 | 84 ± 1 | 25 ± 2 | |
| Ti6Al4V | 999 ± 13 | 1173 ± 17 | 113 ± 10 | 6 ± 1 |
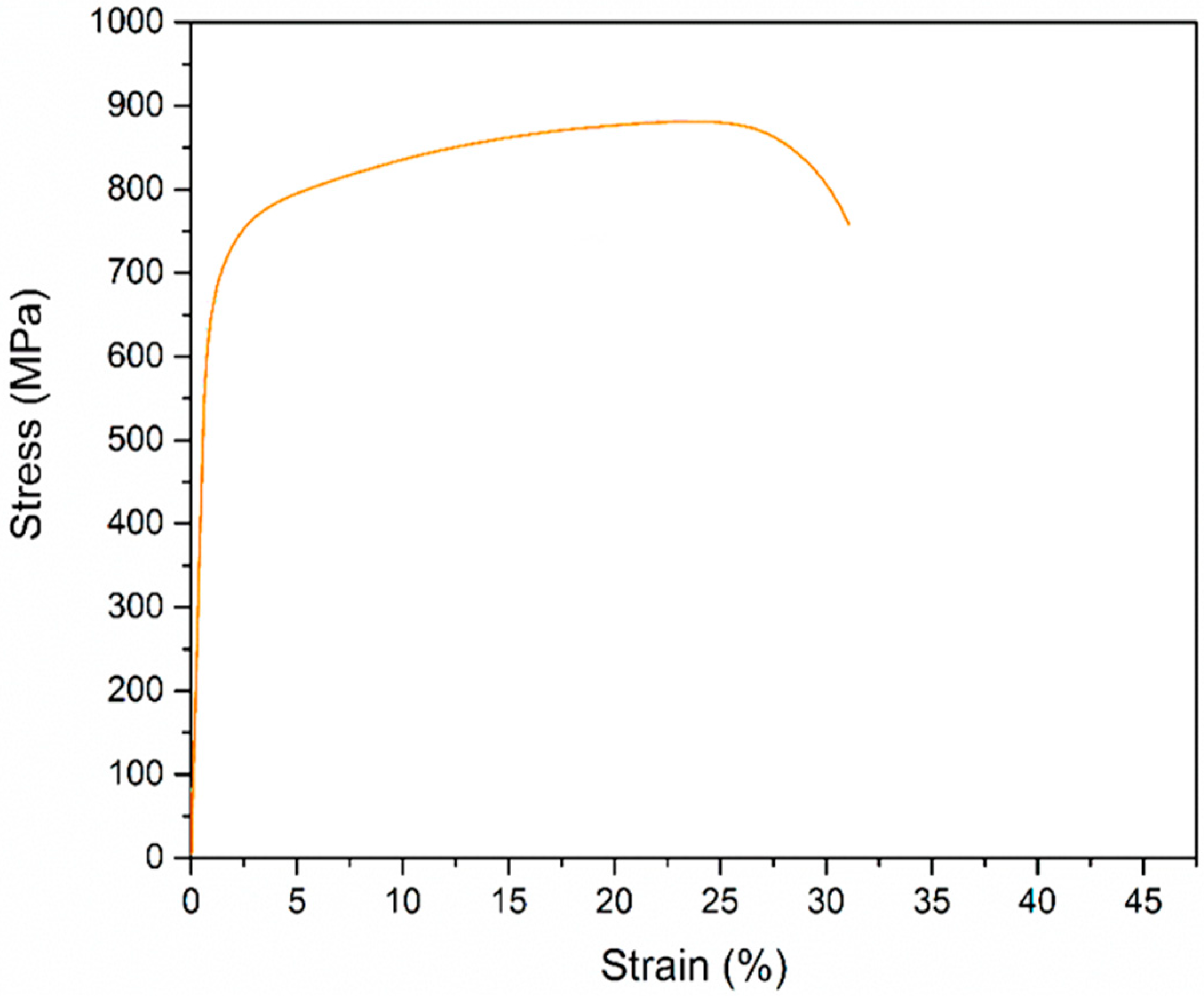
In view of the smallest cross-section of the sample, the applied force and the deformation suffered by the specimen, the result is the graph in Figure 1, which indicates the stress and deformation of the alloy. It presents an average strain of 32% until its rupture under a stress peak of 889 MPa. Sneddon S. et al. (2021) obtained the stress–strain relationship for Ti6Al4V alloy with 14.5% of strain under maximum stress of 1.02 GPa. Weng W. et al. (2021) evaluated that a CP Ti (grade 4) alloy presented an elongation to failure of 15% under a stress of 550 MPa. Their results are similar to those obtained by Ho W. et al. (2008). Therefore, comparing the stress–strain responses obtained by Ti10Mo8Nb alloy with the others alloys presented a better ductility behavior. According to Alabort E. et al. (2022), improvements in alloy ductility are valuable for microstructure engineering and it produces a consequent improvement in the implantable products that should carry out great loads in dentistry and orthopedics.
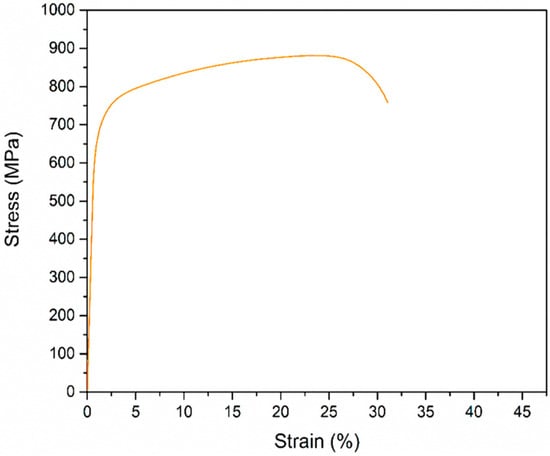
Figure 1.
Stress–strain average curve of the Ti10Mo8Nb alloy obtained from the tested samples.
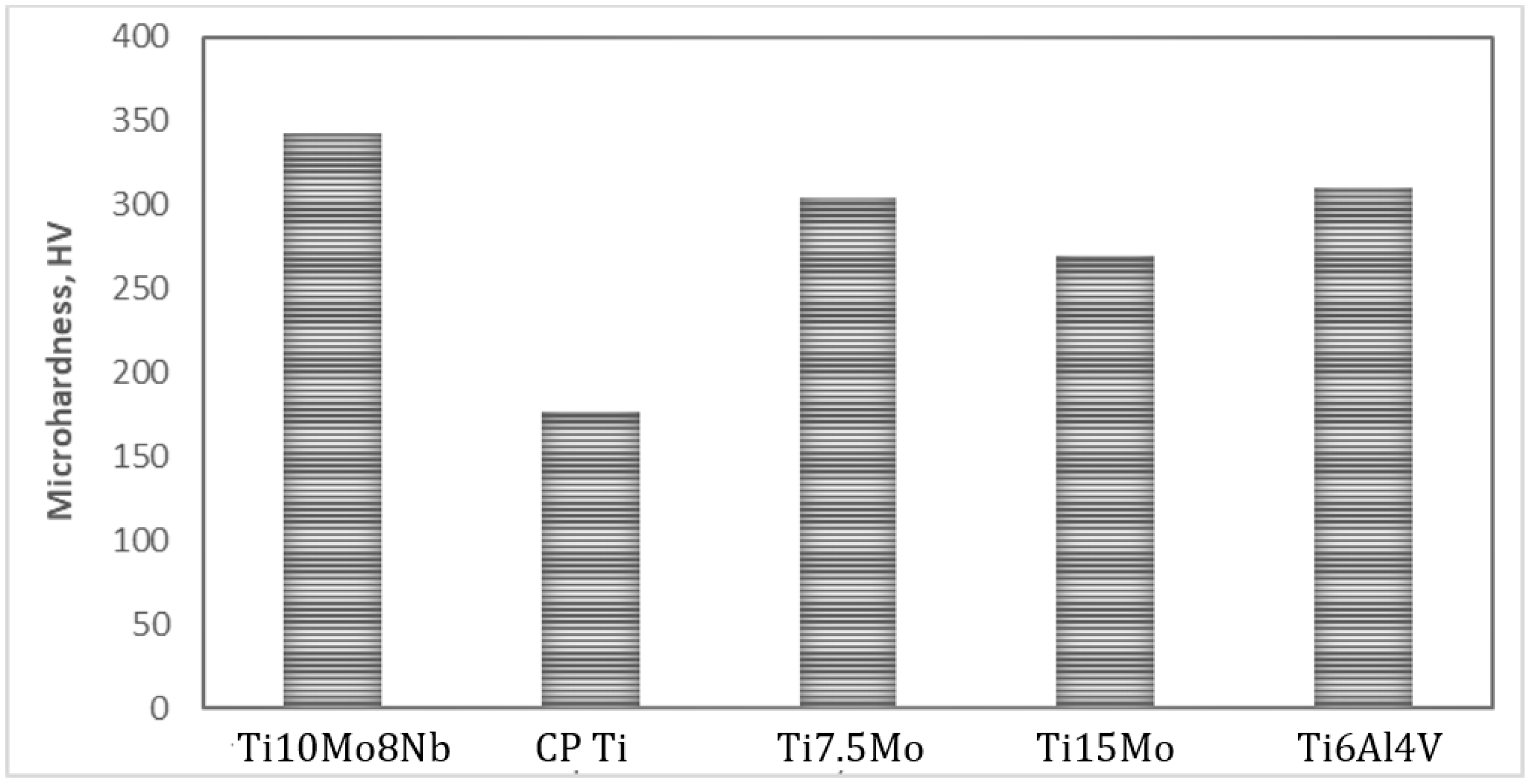
The measure of Vickers microhardness of the Ti10Mo8Nb alloy had an average HV of 342.4, as is shown in Figure 2. A literature review was carried out to compile other Vickers microhardness values of the Ti alloys.
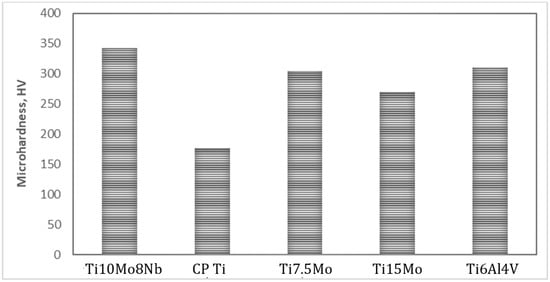
Figure 2.
Microhardness of the Ti10Mo8Nb alloy, CP Ti, Ti15Mo, Ti7.5 Mo and Ti6Al4V are shown for comparison based on Ho W. et al. (2008) results.
Based on studies performed by Weng W. et al. (2021), Rezende M. C. R. A. et al. (2017) and Xu et al. (2008), in alloys of the ternary TiMoNb system, the Vickers microhardness value tends to decrease as the niobium content increases. The experimental alloy Ti10Mo8Nb hardness of 342.4 HV is in agreement with the hardness values obtained by Xu et al. (2008), with an intermediate value for the hardness found for the Ti10Mo7Nb and Ti10Mo10Nb alloys. According to Wandra R. et al. (2022), β-phase Ti alloys with low surface hardness are problematic for orthopedic implants, because they might fail when a contact of metal-on-metal is established for an articulated prosthesis. Therefore, the result of 343.4 HV for Ti10Mo8Nb represents the highest one obtained for all alloys, demonstrating its advantages for biomedical applications.
As can be seen in Figure 2, the hardness of Ti10Mo8Nb alloy is higher than CP Ti, Ti7.5Mo, Ti15Mo and Ti6Al4V. Kaouka et al. (2017) report in their studies that researchers have admitted the association between wear resistance and hardness of materials, and that the greater the hardness, the greater the wear resistance of the biomaterial. Moreover, the optical micrographs (Figure 3) showed that the grain structure has an average width of 200 µm and its β grains have sub-grain boundaries, whose grain characteristic was also observed in the study led by Weng W. et al. (2021) and Rezende M.C.R.A. et al. (2017). The grain size has a direct influence on the material’s hardness and can be considered an element to justify the Ti10Mo8Nb hardness higher than for the other alloys.

Figure 3.
Optical micrographs of Ti10Mo8Nb show typical morphology of β-phase Ti alloys grains.
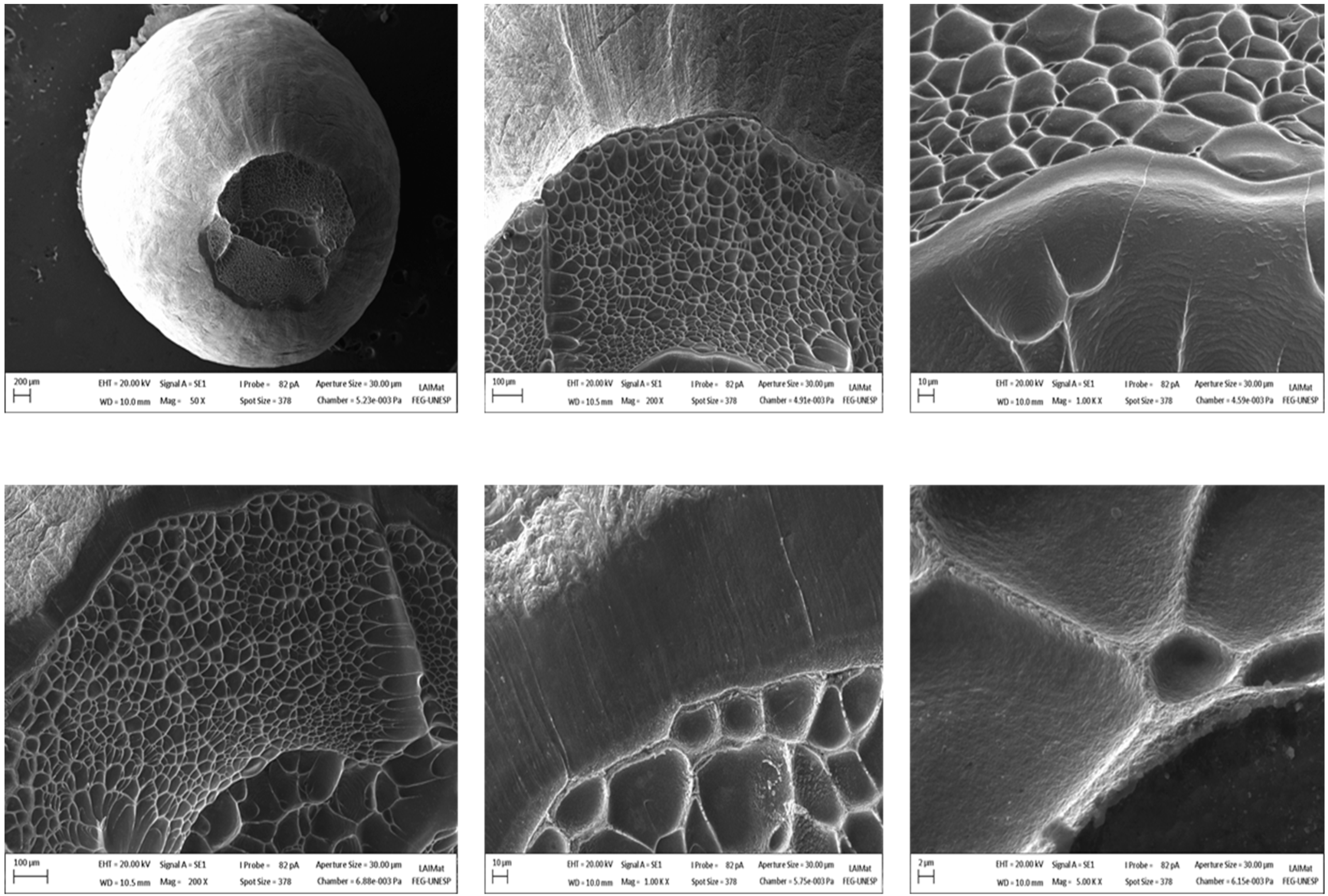
The typical fracture that occurred in specimens of Ti10Mo8Nb alloys was subjected to a uniaxial tensile load. The fracture occurred after necking the area in relation to the applied load. This fact is related to the critical shear stress that is reached under these loading conditions. The SEM fractographs of the heat-treated Ti10Mo8Nb alloys, after the tensile tests at room temperature, are shown in Figure 4. The results indicated the presence of spherical microcavities called dimples on the fracture surface of the specimen, which are related to regions that exhibited plastic deformation. It is important to note that the tensile stresses occur along the cross-section of the specimen, as the transverse expansion takes place and the dimples are then generated in that direction, characteristic of the behavior of ductile materials [40]. An irregular and fibrous appearance on the fracture surface of the Ti10Mo8Nb alloy was also observed, and the crack runs in the direction where the molybdenum-rich precipitates were found.
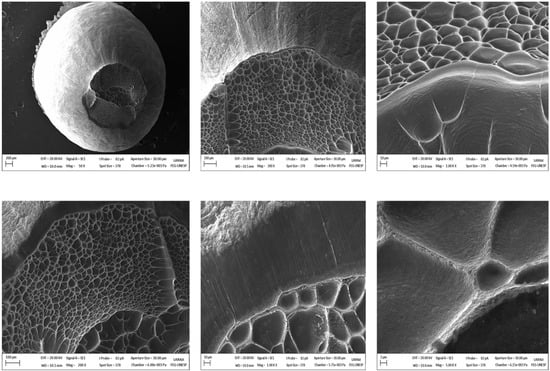
Figure 4.
Ti10Mo8Nb alloy fractography from different magnifications showing the microcavities (dimples) on its surface.
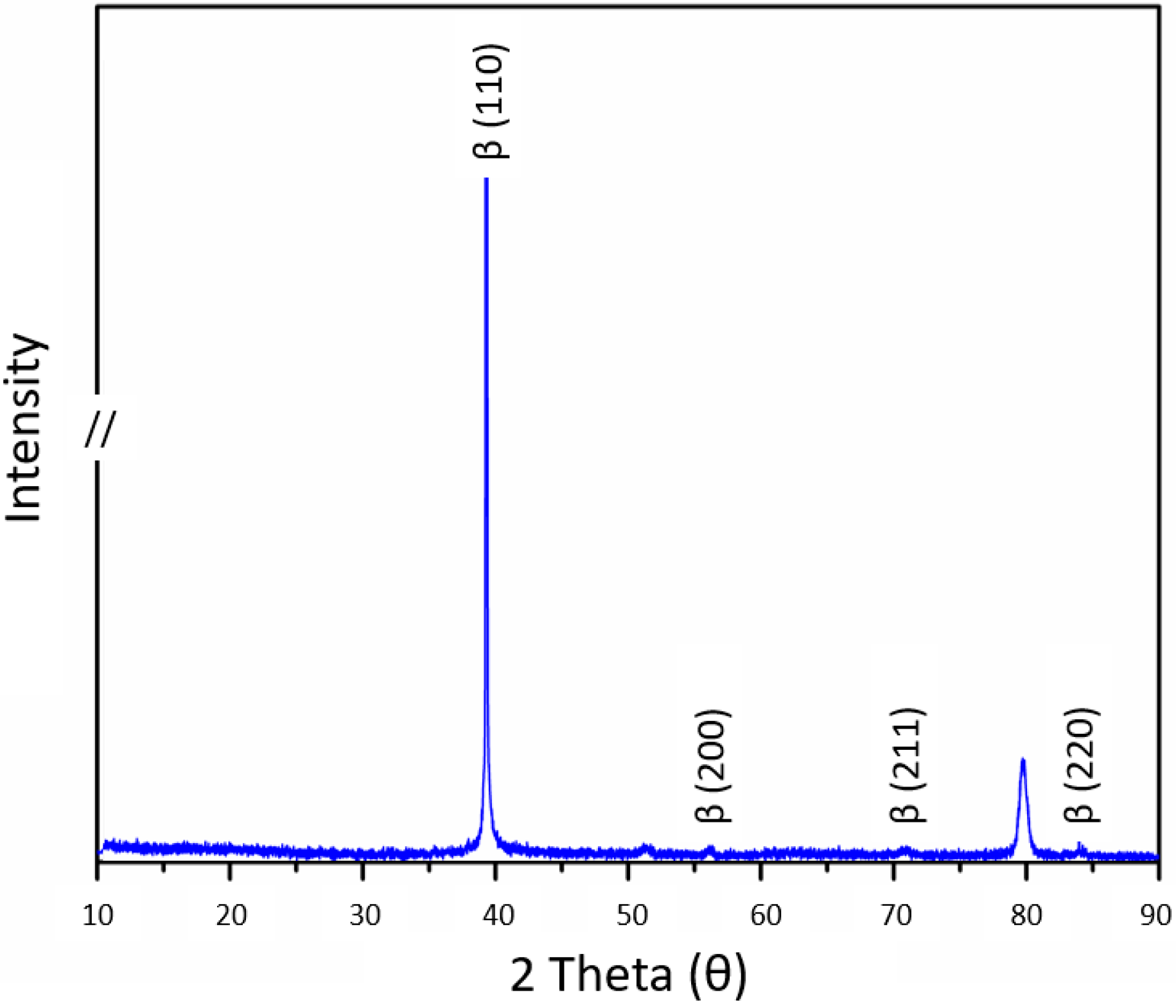
For the XRD obtained for the analyzed ternary alloy, intense and major Ti-β peaks were identified. In addition, the crystallographic plane of this Ti-β-phase was also indexed to these minority peaks, which were stabilized with the increase in the amount of Mo and Nb in the nominal composition of the alloys [25]. It was also observed that the Ti-β peaks were shifted towards lower diffraction angles, as illustrated in Figure 5, suggesting that Mo and Nb atoms may have been dissolved in these crystalline structures. The intensity of the peaks is consistent with findings available in the literature for the Ti-alloy composed of Mo and Nb with close concentrations [41,42]. According to its Mo-equivalence (% Moeq) of 12.24%, which is higher than 10.0%, it is classified as a β-metastable alloy [43,44]. Moreover, the peak marked at 51.5° and 79.5° can be related to the ω phase.
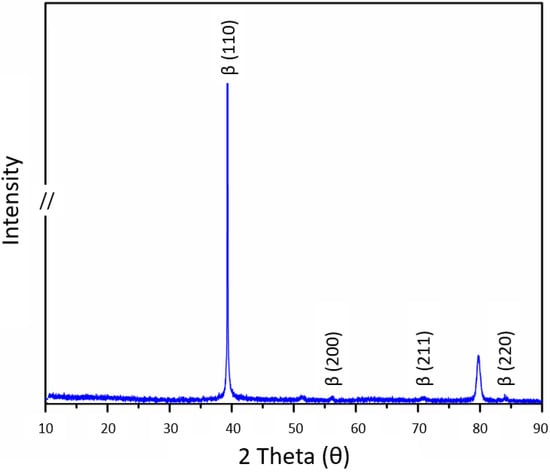
Figure 5.
XRD of the Ti10Mo8Nb alloy with Ti-β peaks highlighted.
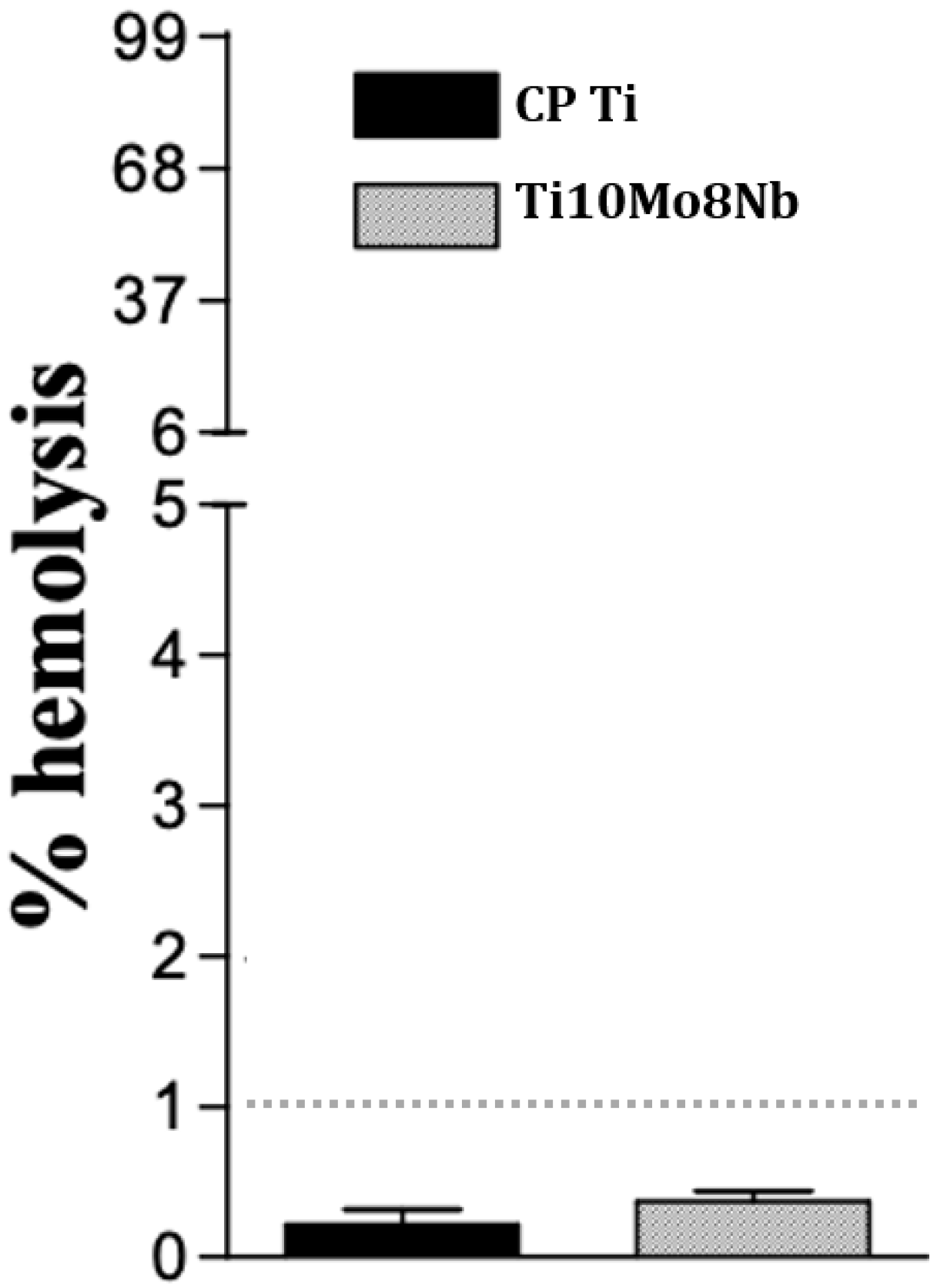
The hemolysis rate shown in Figure 6 represents the biocompatible response of the alloy, indicating an element of its suitability or not for biomedical implants. It is observed that there was no significant statistical variation between the alloys and both presented a hemolysis rate lower than 1%, considered an acceptable range for biomaterials [45]. Although other tests must be carried out to evaluate in greater detail the biocompatible behavior of the alloy, this result presented in hemolysis is relevant to indicate the suitability of the material regarding its inexpressive cytotoxicity and non-response to the destruction of blood cells.
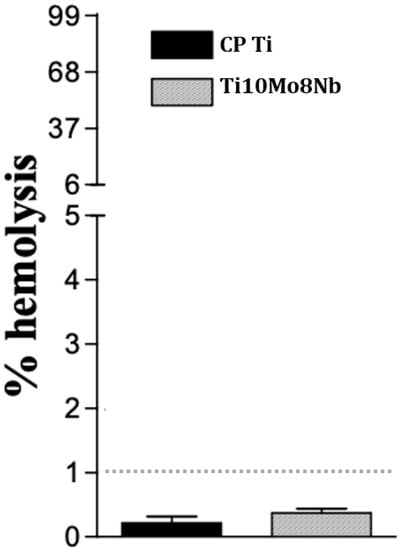
Figure 6.
Hemolysis test for Ti10Mo8Nb and CP Ti.
4. Conclusions
In this study, a ternary β-phase Ti10Mo8Nb alloy was created and its microstructure characteristic and mechanical properties were evaluated for the assessment of its suitability for biomedical applications through fractography, microhardness, XRD, SEM and tensile analyses.
The route and parameters used for the preparation of Ti10Mo8Nb alloys produced homogeneous materials. The β-phase was preferentially formed in the heat-treated Ti10Mo8Nb alloys. The increase in the amount of the β-phase in the nominal composition and in the microstructure of the alloy has contributed to improving the values of Vickers microhardness, yield strength, elastic modulus, compressive strength limit and rupture strength of these alloys, in relation to commercially produced Ti alloys. The fractographic analysis has indicated that the plastic deformation regions were reduced for the heat-treated Ti10Mo9Nb alloy, due to the greater amount of Mo precipitated regions. As a response to the mechanical tests, the alloy showed that its elastic modulus was higher than for other alloys such as Ti7.5Mo and Ti15Mo. This is related to the concentration of Nb and Mo stabilizing β elements. Finally, the hemolysis test indicates a low cytotoxicity response of the material and its appropriate biocompatible response.
Therefore, the Ti10Mo8Nb alloy showed suitable properties for biomedical applications, as well as having more advantageous characteristics than commercially produced Ti and other binary or ternary alloys, mainly reducing the possibility of occurring stress shielding after prosthetic implantations, especially for orthopedics and dentistry.
Author Contributions
Conceptualization, P.C., K.B.d.S. and J.P.A.C.; methodology, P.C. and F.B.V.; validation, P.C., G.S., E.G.M.B., M.d.L.N.M.M. and D.S.; formal analysis, P.C., K.B.d.S. and F.B.V.; investigation, P.C., K.B.d.S. and F.B.V.; resources, J.P.A.C., A.H.P.F. and A.P.R.A.C.; data curation, P.C., J.P.A.C., A.H.P.F. and A.P.R.A.C.; writing—original draft preparation, P.C., K.B.d.S. and F.B.V.; writing—review and editing, P.C. and F.B.V.; visualization, P.C., G.S., E.G.M.B., M.d.L.N.M.M. and D.S.; supervision, P.C., G.S., E.G.M.B., M.d.L.N.M.M., A.H.P.F., A.P.R.A.C. and D.S.; project administration, P.C.; funding acquisition, P.C. and A.P.R.A.C. All authors have read and agreed to the published version of the manuscript.
Funding
Partial funding support for this work was provided by the Brazilian federal government and the National Council for Scientific, Technological Development (CNPq) via Award Number 201271/2010-9 and Fapesp 2014/14533-3.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Dogra, S.; Dunstan, D.W.; Sugiyama, T.; Stathi, A.; Gardiner, P.A.; Owen, N. Active Aging and Public Health: Evidence, Implications, and Opportunities. Annu. Rev. Public Health 2022, 1, 439–459. [Google Scholar] [CrossRef] [PubMed]
- Gu, D.; Andreev, K.; Dupre, M.E. Major Trends in Population Growth Around the World. China CDC Wkly. 2021, 3, 604–613. [Google Scholar] [CrossRef] [PubMed]
- Guo, H.; Jiang, J.; Li, Y.; Liu, M.; Han, J. An Aging Giant at The Center of Global Warming: Population Dynamics and Its Effect on CO2 Emissions in China. Res. Sq. 2022, 1–26. [Google Scholar] [CrossRef]
- Dixon, A. The United Nations Decade of Healthy Ageing requires concerted global action. Nat. Aging 2021, 1, 2. [Google Scholar] [CrossRef]
- Massari, L.; Benazzo, F.; Falez, F.; Perugia, D.; Pietrogrande, L.; Setti, S.; Osti, R.; Vaienti, E.; Ruosi, C.; Cadossi, R. Biophysical stimulation of bone and cartilage: State of the art and future perspectives. Int. Orthop. 2019, 43, 539–551. [Google Scholar] [CrossRef] [Green Version]
- Herber, V.; Okutan, B.; Antonoglou, G.; Sommer, N.; Payer, M. Bioresorbable Magnesium-Based Alloys as Novel Biomaterials in Oral Bone Regeneration: General Review and Clinical Perspectives. J. Clin. Med. 2021, 10, 1842. [Google Scholar] [CrossRef] [PubMed]
- Marew, T.; Birhanu, G. Three dimensional printed nanostructure biomaterials for bone tissue engineering. Regen. Ther. 2021, 18, 102–111. [Google Scholar] [CrossRef]
- Zhou, J.; Zhang, Z.; Joseph, J.; Zhang, X.; Ferdows, B.E.; Patel, D.N.; Neal, D.; Chen, W.; Banfi, G.; Molinaro, R.; et al. Biomaterials and nanomedicine for bone regeneration: Progress and future prospects. Exploration 2021, 1, 20210011. [Google Scholar] [CrossRef]
- Sailer, I.; Karasan, D.; Todorovic, A.; Ligoutsikou, M.; Pjetursson, B.E. Prosthetic failures in dental implant therapy. Periodontology 2000 2022, 88, 130–144. [Google Scholar] [CrossRef]
- Lv, Y.; Wang, B.; Liu, G.; Tang, Y.; Lu, E.; Xie, K.; Lan, C.; Liu, J.; Qin, Z.; Wang, L. Metal Material, Properties and Design Methods of Porous Biomedical Scaffolds for Additive Manufacturing: A Review. Front. Bioeng. Biotechnol. 2021, 9, 641130. [Google Scholar] [CrossRef]
- Vahidshad, Y.; Khodabakhshi, A.H. Effect of Solution Treatment and Aging Temperature on α′ and Ti3Al(α2) Phase Formation and Mechanical Properties of Water-Quenched Ti–6Al–4V. Metallogr. Microstruct. Anal. 2022, 11, 59–71. [Google Scholar] [CrossRef]
- Rossi, M.; Amado, J.; Tobar, M.; Vicente, A.; Yañez, A.; Amigó, V. Effect of alloying elements on laser surface modification of powder metallurgy to improve surface mechanical properties of beta titanium alloys for biomedical application. J. Mater. Res. Technol. 2021, 14, 1222–1234. [Google Scholar] [CrossRef]
- Ali, T.; Wang, L.; Cheng, X.; Gu, D.; Zhou, Z.; Min, X. The effect of TiC on microstructure and mechanical properties of Ti-5553 beta phase titanium alloy. Mater. Des. 2022, 214, 110395. [Google Scholar] [CrossRef]
- Montiel-Flores, E.; Mejía-García, O.A.; Ordoñez-Librado, J.L.; Gutierrez-Valdez, A.L.; Espinosa-Villanueva, J.; Dorado-Martínez, C.; Reynoso-Erazo, L.; Tron-Alvarez, R.; Rodríguez-Lara, V.; Avila-Costa, M.R. Alzheimer-like cell death after vanadium pentoxide inhalation. Heliyon 2021, 7, e07856. [Google Scholar] [CrossRef]
- Feng, W.; Han, X.; Hu, H.; Chang, M.; Ding, L.; Xiang, H.; Chen, Y.; Li, Y. 2D vanadium carbide MXenzyme to alleviate ROS-mediated inflammatory and neurodegenerative diseases. Nat. Commun. 2021, 12, 2203. [Google Scholar] [CrossRef]
- Mohammad, N.; Ahmad, R.; Rosli, N.M.; Manan, M.A.; Marzuki, M.; Wahi, A. Sol gel deposited hydroxyapatite-based coating technique on porous titanium niobium for biomedical applications: A mini review. Mater. Today Proc. 2021, 41, 127–135. [Google Scholar] [CrossRef]
- Yolun, A.; Şimşek, M.; Kaya, M.; Annaç, E.E.; Köm, M.; Çakmak, Ö. Fabrication, characterization, and in vivo biocompatibility evaluation of titanium-niobium implants. Proc. Inst. Mech. Eng. Part H J. Eng. Med. 2020, 235, 99–108. [Google Scholar] [CrossRef]
- Omar, T.; Veiga, M.M. Is niobium critical for Canada? Extr. Ind. Soc. 2021, 8, 100898. [Google Scholar] [CrossRef]
- Li, H.-Y.; Zhao, R.-P.; Li, J.; Tamura, Y.; Spencer, C.; Stern, R.J.; Ryan, J.G.; Xu, Y.-G. Molybdenum isotopes unmask slab dehydration and melting beneath the Mariana arc. Nat. Commun. 2021, 12, 6015. [Google Scholar] [CrossRef]
- Zu, Y.; Yao, H.; Wang, Y.; Yan, L.; Gu, Z.; Chen, C.; Gao, L.; Yin, W. The age of bioinspired molybdenum-involved nanozymes: Synthesis, catalytic mechanisms, and biomedical applications. View 2021, 2, 20200188. [Google Scholar] [CrossRef]
- Glowka, K.; Zubko, M.; Świec, P.; Prusik, K.; Szklarska, M.; Chrobak, D.; Lábár, J.L.; Stróŝ, D. Influence of Molybdenum on the Microstructure, Mechanical Properties and Corrosion Resistance of Ti20Ta20Nb20(ZrHf)20−xMox (Where: X = 0, 5, 10, 15, 20) high entropy alloys. Materials 2022, 15, 393. [Google Scholar] [CrossRef] [PubMed]
- Redlich, C.; Schauer, A.; Scheibler, J.; Poehle, G.; Barthel, P.; Maennel, A.; Adams, V.; Weissgaerber, T.; Linke, A.; Quadbeck, P. In Vitro Degradation Behavior and Biocompatibility of Bioresorbable Molybdenum. Metals 2021, 11, 761. [Google Scholar] [CrossRef]
- Suresh, S.; Vinod, B.; Sujith, K.S.; Sudhakara, D. Investigation and performance of high niobium contain Ti-Al Alloys: Deformation behaviour and microstructural evolution. Mater. Today Proc. 2022. [Google Scholar] [CrossRef]
- Suesawadwanid, N.; Khantachawana, A.; Srirussamee, K.; Kondoh, K. Effect of Nb Content and water quenching on microstructure and mechanical properties of Ti-Nb alloys fabricated by spark plasma sintering. Powder Met. 2022, 1–13. [Google Scholar] [CrossRef]
- Rezende, M.C.R.A.; Felipe, J.C.; Nakazato, R.; Dutra, C.A.M.; Rangel, A.L.R.; Limírio, J.P.J.D.O.; Claro, A.P.R.A. Study of the Vickers hardness and corrosion behavior of experimental Ti-Mo alloy in dental office bleaching agents. Arch. Health Investig. 2017, 6. [Google Scholar] [CrossRef] [Green Version]
- Bocchetta, P.; Chen, L.-Y.; Tardelli, J.; Reis, A.; Almeraya-Calderón, F.; Leo, P. Passive Layers and Corrosion Resistance of Biomedical Ti-6Al-4V and β-Ti Alloys. Coatings 2021, 11, 487. [Google Scholar] [CrossRef]
- Xu, L.; Chen, Y.; Liu, Z.; Kong, F. The microstructure and properties of Ti–Mo–Nb alloys for biomedical application. J. Alloy. Compd. 2008, 453, 320–324. [Google Scholar] [CrossRef]
- Mohan, P.; Rajak, D.K.; Pruncu, C.I.; Behera, A.; Amigó-Borrás, V.; Elshalakany, A.B. Influence of β-phase stability in elemental blended Ti-Mo and Ti-Mo-Zr alloys. Micron 2020, 142, 102992. [Google Scholar] [CrossRef] [PubMed]
- Souza, B.L.M.d.; Nakazato, R.Z.; Claro, A.P.R.A.; Escada, A.L.d.A. Influência da agitação no crescimento de nanotubos de TiO2 na superfície de discos de titânio comercialmente puro. Matéria 2021, 26, 1–10. [Google Scholar] [CrossRef]
- Ho, W. Effect of omega phase on mechanical properties of Ti-Mo alloys for biomedical applications. J. Med. Biol. Eng. 2008, 28, 47–51. [Google Scholar]
- Yoon, S.; Schiffer, A.; Jang, I.G.; Lee, S.; Kim, T.-Y. Predictions of the elastic modulus of trabecular bone in the femoral head and the intertrochanter: A solitary wave-based approach. Biomech. Model. Mechanobiol. 2021, 20, 1733–1749. [Google Scholar] [CrossRef] [PubMed]
- Savio, D.; Bagno, A. When the Total Hip Replacement Fails: A Review on the Stress-Shielding Effect. Processes 2022, 10, 612. [Google Scholar] [CrossRef]
- Öhman-Mägi, C.; Holub, O.; Wu, D.; Hall, R.M.; Persson, C. Density and mechanical properties of vertebral trabecular bone—A review. JOR Spine 2021, 4, e1176. [Google Scholar] [CrossRef] [PubMed]
- Zhang, L.; Song, B.; Choi, S.-K.; Shi, Y. A topology strategy to reduce stress shielding of additively manufactured porous metallic biomaterials. Int. J. Mech. Sci. 2021, 197, 106331. [Google Scholar] [CrossRef]
- Sneddon, S.; Mulvihill, D.M.; Wielewski, E.; Dixon, M.; Rugg, D.; Li, P. Deformation and failure behaviour of a titanium alloy Ti-407 with reduced aluminium content: A comparison with Ti-6Al-4V in tension and compression. Mater. Charact. 2021, 172, 110901. [Google Scholar] [CrossRef]
- Weng, W.; Biesiekierski, A.; Lin, J.; Ozan, S.; Li, Y.; Wen, C. Development of beta-type Ti-Nb-Zr-Mo alloys for orthopedic applications. Appl. Mater. Today 2021, 22, 100968. [Google Scholar] [CrossRef]
- Alabort, E.; Tang, Y.; Barba, D.; Reed, R. Alloys-by-design: A low-modulus titanium alloy for additively manufactured biomedical implants. Acta Mater. 2022, 229, 117749. [Google Scholar] [CrossRef]
- Wandra, R.; Prakash, C.; Singh, S. Experimental investigation and optimization of surface roughness of β-Phase titanium alloy by ball burnishing assisted electrical discharge cladding for implant applications. Mater. Today Proc. 2021, 48, 975–980. [Google Scholar] [CrossRef]
- Kaouka, A.; Benarous, K.; Daas, A.; Tsipas, S.A. The Effects of Nb and Mo Addition on Microstructure and Mechanical Behaviour of Ti-6Al-4V Alloy. J. Surf. Sci. Technol. 2017, 33, 53–62. [Google Scholar] [CrossRef]
- Mandal, P.; Daniel, B.; Mathews, M.S.; Joseph, A.; Siby, C.; Devasia, J. Martensitic transformation in a α + β–Ti alloy after cryogenic treatment and its influencing to low elastic modulus biomaterials. Mater. Today Proc. 2021, 46, 2820–2826. [Google Scholar] [CrossRef]
- Hacisalihoglu, I.; Samancioglu, A.; Yildiz, F.; Purcek, G.; Alsaran, A. Tribocorrosion properties of different type titanium alloys in simulated body fluid. Wear 2015, 332–333, 679–686. [Google Scholar] [CrossRef]
- Raganya, M.L.; Moshokoa, N.M.; Obadele, B.; Olubambi, P.A.; Machaka, R. The microstructural and mechanical characterization of the β-type Ti-11.1Mo-10.8Nb alloy for biomedical applications. Iop Conf. Ser. Mater. Sci. Eng. 2019, 655, 012025. [Google Scholar] [CrossRef]
- Kolli, R.P.; Devaraj, A. A Review of Metastable Beta Titanium Alloys. Metals 2018, 8, 506. [Google Scholar] [CrossRef] [Green Version]
- Gabriel, S.; Panaino, J.; Santos, I.; Araujo, L.; Mei, P.; de Almeida, L.; Nunes, C. Characterization of a new beta titanium alloy, Ti–12Mo–3Nb, for biomedical applications. J. Alloy. Compd. 2012, 536, S208–S210. [Google Scholar] [CrossRef]
- Zamani, E.; Yahyaei, H.; Zamani, M. Evaluation of the mechanical properties and blood compatibility of Polycarbonate Urethane and fluorescent self-colored Polycarbonate Urethane as Polymeric Biomaterials. J. Polym. Res. 2021, 28, 112. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).