Friction of Human Skin against Different Fabrics for Medical Use
Abstract
:1. Introduction
2. Experimental Section
Material and Methods
3. Results and Discussion
4. Conclusions
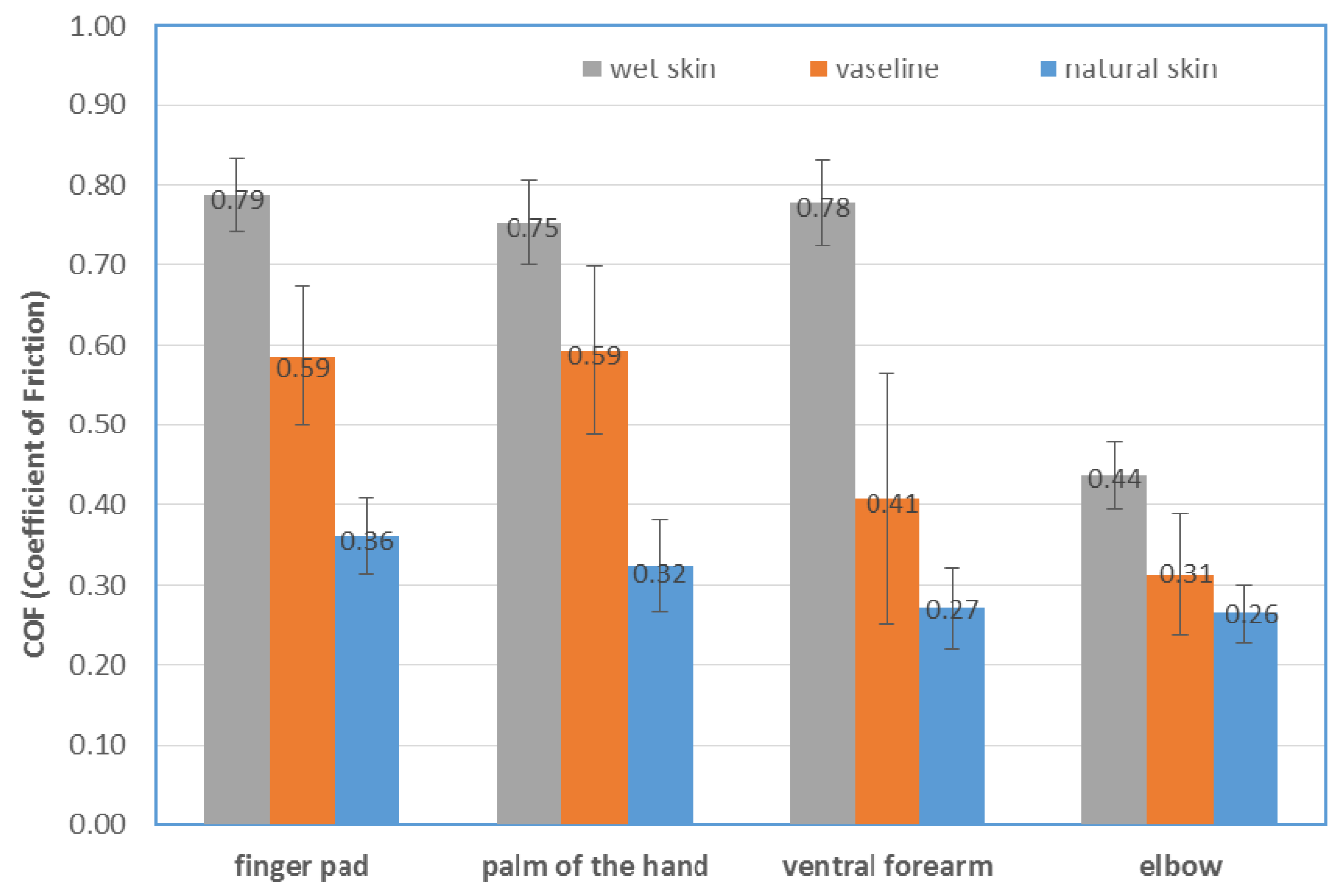
- Results demonstrated that the coefficient of friction (COF) of a reference hospital fabric against skin is influenced by the human body region and lubricating/physiological skin conditions (skin moisture content).
- For the different body regions, the average COF of wet skin exceeded those in the natural skin condition by a factor of more than two, with the friction increasing with the moisture content. In this way, moisture (e.g., due to incontinence) can accelerate/promote skin decubitus formation.
- For the different body regions, the coefficient of friction always increases with the addition of Vaseline if compared to the natural skin conditions. The spreading of Vaseline on the skin can act as a barrier to lock moisture in the skin.
- Natural skin conditions (dry skin) produce the lowest COF for the different body regions.
- Concerning the effect of different body regions, the coefficient of friction varies significantly along the human body. The observed variations were mainly attributed to differences in skin hydration, with a tendency to greater friction at regions such as the finger pad and the palm of the hand, due to higher skin hydration.
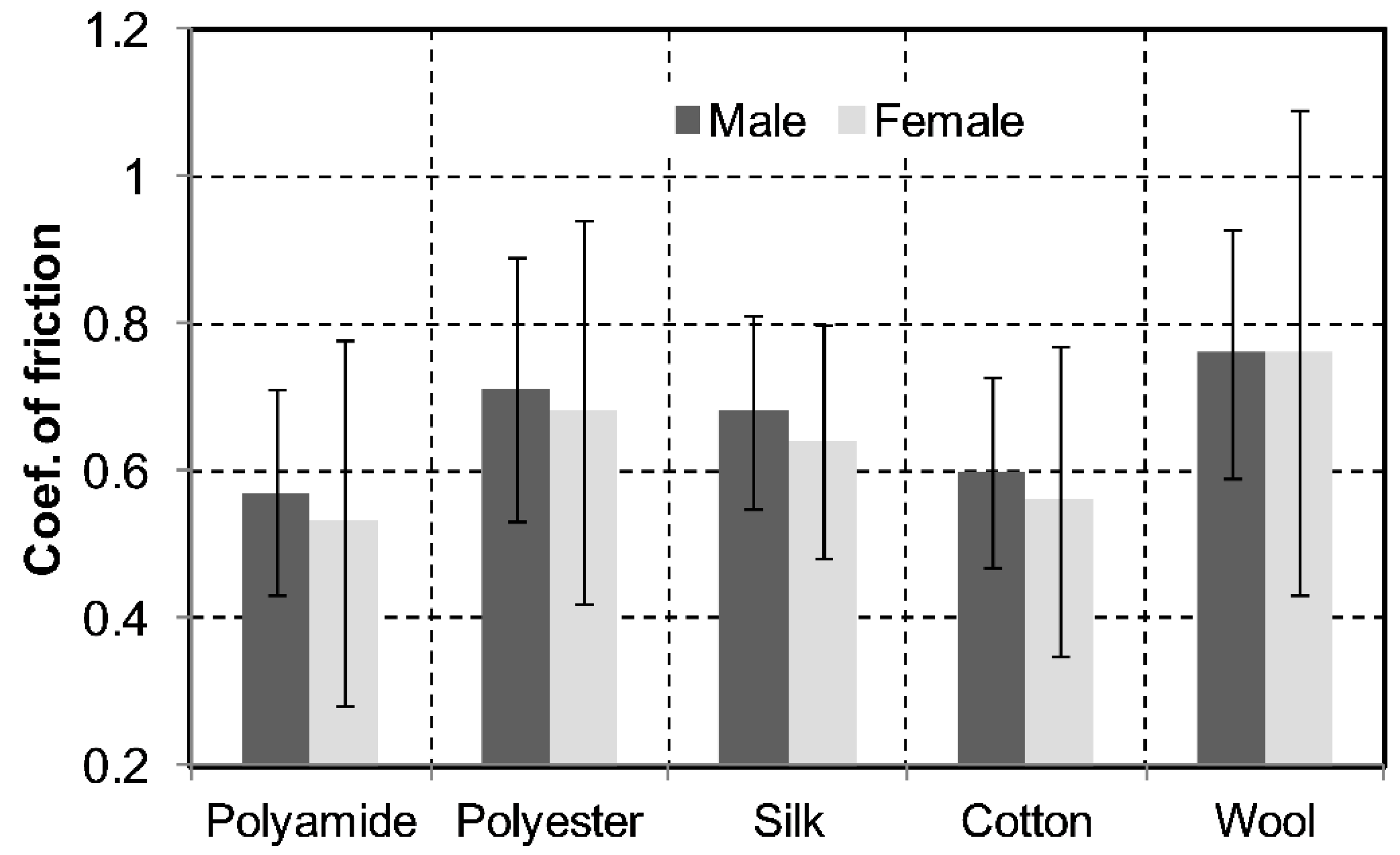
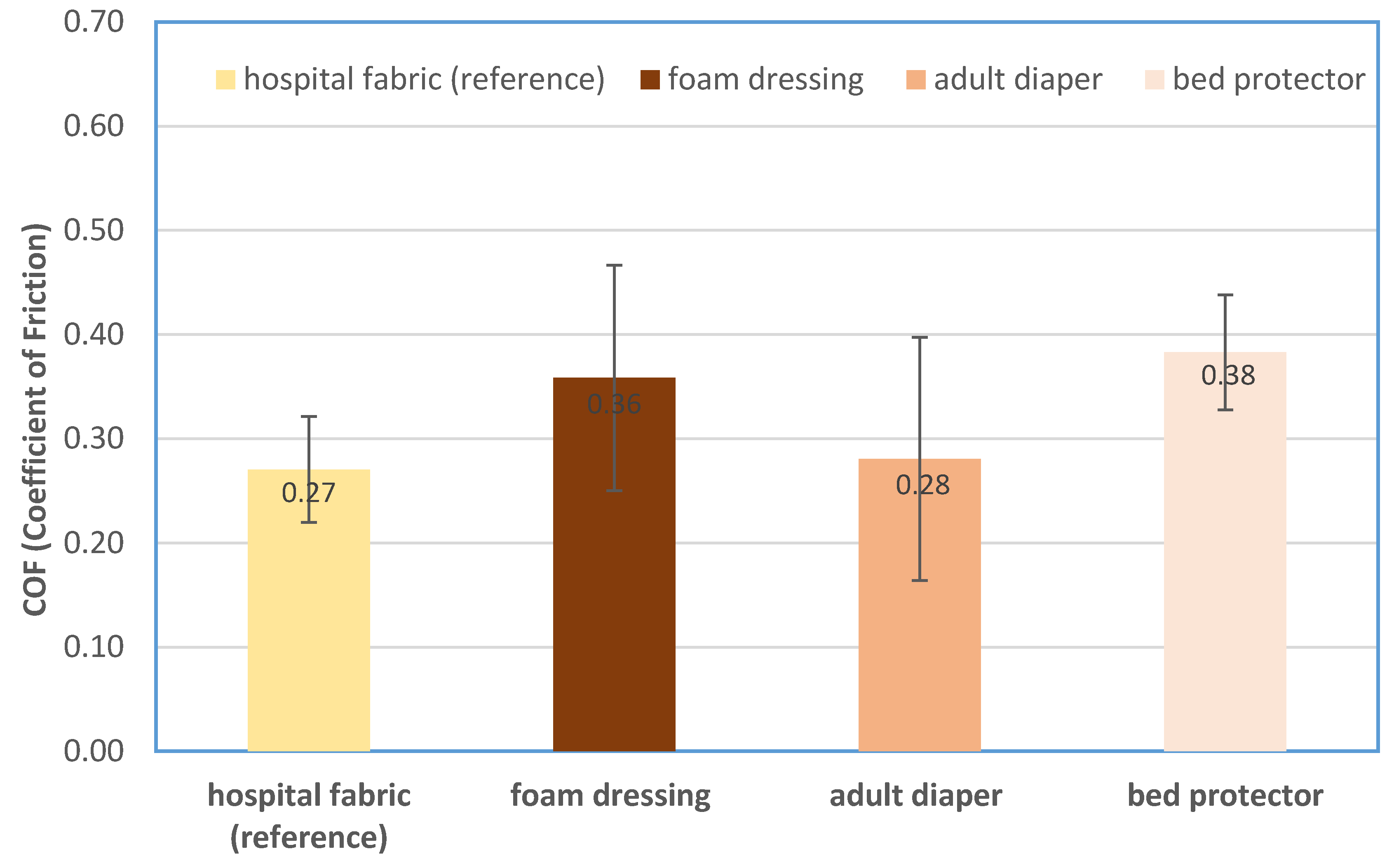
- In this investigation, no significant correlation was found for the COF of the four different hospital fabrics.
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Jost, H.P. Lubrication (Tribology) Education and Research. In A Report on the Present Position and the Industry’s Needs; Department of Education and Science, Her Majesty’s Stationery Office (HMSO): London, UK, 1966. [Google Scholar]
- Johnson, S.A.; Gorman, D.M.; Adams, M.J.; Briscoe, B.J. The friction and lubrication of human stratum corneum. In Tribology Series—Thin Films in Tribology. In Proceedings of the 19th Leeds-Lyon Symposium on Tribology held at the Institute of Tribology, University of Leeds, Amsterdam, The Netherlands, 8–11 September 1993; Dowson, D., et al., Eds.; Volume 25, pp. 663–672.
- Dowson, D. Tribology and the skin surface. In Bioengineering of the skin: Skin surface imaging and analysis; Wilhelm, K.-P., Elsner, P., Berardesca, E., Maibach, H.I., Eds.; CRC Press: Boca Raton, FL, USA, 1997; pp. 159–180. [Google Scholar]
- Adams, M.; Briscoe, B.; Johnson, S. Friction and lubrication of human skin. Tribol. Lett. 2007, 26, 239–253. [Google Scholar] [CrossRef]
- Koudine, A.A.; Barquins, M.; Anthoine, P.H.; Aubert, L.; Leveque, J.L. Frictional properties of skin: proposal of a new approach. Int. J. Cosmet. Sci. 2000, 22, 11–20. [Google Scholar] [CrossRef] [PubMed]
- Pailler-Mattei, C.; Zahouani, H. Study of adhesion forces and mechanical properties of human skin in vivo. J. Adhes. Sci. Technol. 2004, 18, 1739–1758. [Google Scholar] [CrossRef]
- Gerhardt, L.-C.; Strassle, V.; Lenz, A.; Spencer, N.D.; Derler, S. Influence of epidermal hydration on the friction of human skin against textiles. J. R. Soc. Interface 2008, 5, 1317–1328. [Google Scholar] [CrossRef] [PubMed]
- Hendriks, C.; Franklin, S. Influence of surface roughness, material and climate conditions on the friction of human skin. Tribol. Lett. 2010, 37, 361–373. [Google Scholar] [CrossRef]
- Nacht, S.; Close, J.-A.; Yeung, D.; Gans, E.H. Skin friction coefficient: Changes induced by skin hydration and emollient application and correlation with perceived skin feel. J. Soc. Cosmet. Chem. 1981, 32, 55–65. [Google Scholar]
- Adams, M.; Briscoe, B.; Johnson, S. Friction and lubrication of human skin. Tribol. Lett. 2007, 26, 239–253. [Google Scholar] [CrossRef]
- Johnson, S.A.; Gorman, D.M.; Adams, M.J.; Briscoe, B.J. The friction and lubrication of human stratum corneum. In Tribology Series Thin Films in Tribology, Proceedings of the 19th Leeds-Lyon Symposium on Tribology held at the Institute of Tribology, University of Leeds; Dowson, D., Ed.; Elsevier: Amsterdam, The Netherlands; Volume 25, pp. 663–672.
- Denda, M. Dry Skin and Moisturizers: Chemistry and Function; LodeA, M., Maibach, N.H., Eds.; CRC Press: Boca Raton, FL, USA, 2000; pp. 147–153. [Google Scholar]
- Wolfram, L.J. Friction of skin. J. Soc. Cosmet. Chem. 1983, 34, 465–476. [Google Scholar]
- Hills, R.J.; Unsworth, A.; Ive, F.A. A comparative study of the frictional properties of emollient bath additives using porcine skin. Br. J. Dermatol. 1994, 130, 37–41. [Google Scholar] [CrossRef] [PubMed]
- Johnson, S.A.; Gorman, D.M.; Adams, M.J.; Briscoe, B.J. The Friction and Lubrication of Human Stratum Corneum. In Proceedings of the 19th Leeds-Lyon Symposium on Tribology, Thin Films in Tribology, Leeds, UK, 8–11 September 1992; Elsevier Science Publishers: Amsterdam, The Netherlands, 1993; pp. 663–672. [Google Scholar]
- Derler, S.; Gerhardt, L.-C. Tribology of Skin: Review and Analysis of Experimental Results for the Friction Coefficient of Human Skin. Tribol. Lett. 2012, 45, 1–27. [Google Scholar] [CrossRef]
- Van Der Heide, E.; Zeng, X.; Masen, M.A. Skin tribology: Science friction? 2013, 1, 130–142. [Google Scholar] [CrossRef]
- Xu, F.; Li, T.J.; Seffen, K.A. Skin thermal pain modeling—A holistic method. J. Therm. Biol. 2008, 33, 223–237. [Google Scholar] [CrossRef]
- Essick, G.K.; McGlone, F.; Dancer, C.; Fabricant, D.; Ragin, Y.; Phillips, N. Therese Jones, Steve Guest, Quantitative assessment of pleasant touch. Neurosci. Biobehav. Rev. 2010, 34, 192–203. [Google Scholar] [CrossRef] [PubMed]
- Barnes, C.J.; Childs, T.H.C.; Henson, B.; Southee, C.H. Surface finish and touch—a case study in a new human factors tribology. Wear 2004, 257, 740–750. [Google Scholar] [CrossRef]
- Ramalho, A.; Silva, C.L.; Pais, A.A.C.C.; Sousa, J.J.S. In vivo friction study of human palmoplantar skin against glass. Tribol. Fin. J. Tribol. 2006, 25, 14–23. [Google Scholar]
- Ramalho, A.; Szekeres, N.P.; Fernandes, E. Friction and tactile perception of textile fabrics. Tribol. Int. 2013, 63, 29–33. [Google Scholar] [CrossRef]
- Ramalho, A.; Silva, C.L.; Pais, A.A.C.C.; Sousa, J.J.S. In vivo friction study of human skin: Influence of moisturizers on different anatomical sites. Wear 2007, 263, 1044–1049. [Google Scholar] [CrossRef]
- Nacht, S.; Close, J.-A.; Yeung, D.; Gans, E.H. Skin friction coefficient: changes induced by skin hydration and emollient application and correlation with perceived skin feel. J. Soc. Cosmet. Chem. 1981, 32, 55–65. [Google Scholar]
- Kenins, P. Influence of fiberb type and moisture on measured fabric-to-skin friction. Text. Res. J. 1994, 64, 722–728. [Google Scholar] [CrossRef]
- Derler, S.; Schrade, U.; Gerhardt, L.-C. Tribology of human skin and mechanical skin equivalents in contact with textiles. Wear 2007, 263, 1112–1116. [Google Scholar] [CrossRef]
- Johnson, S.A.; Gorman, D.M.; Adams, M.J.; Briscoe, B.J. The friction and lubrication of human stratum corneum. In Thin Films in Tribology; Dowson, D., Ed.; Elsevier Science Publishers: Amsterdam, The Netherlands, 1993; pp. 663–672. [Google Scholar]
- Cua, A.B.; Wilhelm, K.P.; Maibach, H.I. Frictional properties of human skin: Relation to age, sex and anatomical region, stratum corneum hydration and transepidermal water loss. Br. J. Dermatol. 1990, 123, 473–479. [Google Scholar] [CrossRef] [PubMed]
- Zhu, Y.H.; Song, S.P.; Luo, W.; Elias, P.M.; Man, M.Q. Characterization of skin friction coefficient, and relationship to stratum corneum hydration in a normal Chinese population. Skin Pharmacol. Physiol. 2011, 24, 81–86. [Google Scholar] [CrossRef] [PubMed]

© 2016 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons by Attribution (CC-BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Vilhena, L.; Ramalho, A. Friction of Human Skin against Different Fabrics for Medical Use. Lubricants 2016, 4, 6. https://doi.org/10.3390/lubricants4010006
Vilhena L, Ramalho A. Friction of Human Skin against Different Fabrics for Medical Use. Lubricants. 2016; 4(1):6. https://doi.org/10.3390/lubricants4010006
Chicago/Turabian StyleVilhena, Luís, and Amílcar Ramalho. 2016. "Friction of Human Skin against Different Fabrics for Medical Use" Lubricants 4, no. 1: 6. https://doi.org/10.3390/lubricants4010006
APA StyleVilhena, L., & Ramalho, A. (2016). Friction of Human Skin against Different Fabrics for Medical Use. Lubricants, 4(1), 6. https://doi.org/10.3390/lubricants4010006





