Potential Pitfalls on the 99mTc-Mebrofenin Hepatobiliary Scintigraphy in a Patient with Biliary Atresia Splenic Malformation Syndrome
Abstract
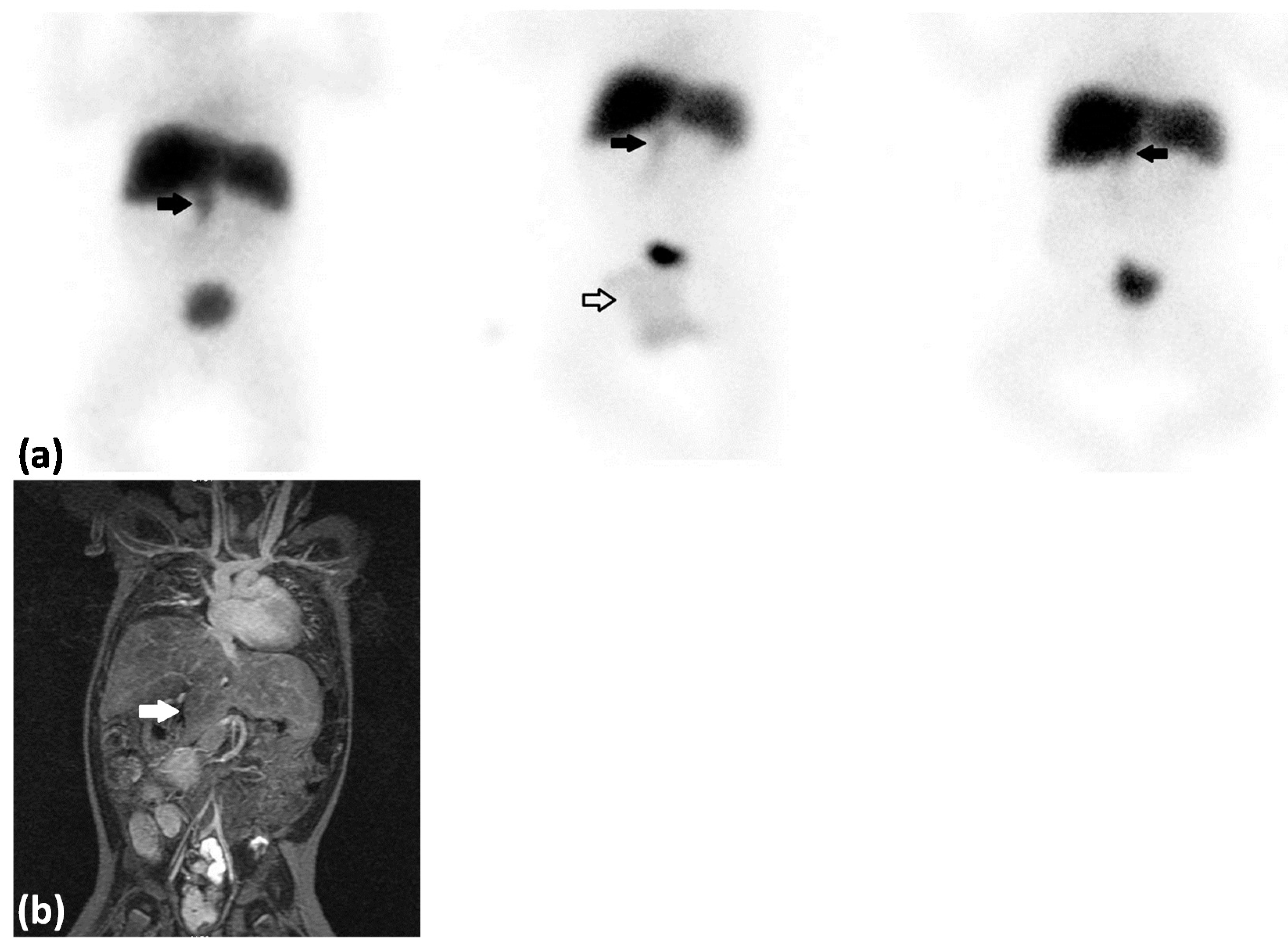
:
Conflicts of Interest
References
- Wildhaber, B.A. Biliary atresia: 50 years after the first Kasai. ISRN Surg. 2012, 2012, 1–15. [Google Scholar] [CrossRef] [PubMed]
- Petersen, C.; Davenport, M. Aetiology of biliary atresia: What is actually known? Orphanet J. Rare Dis. 2013, 8, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Schwarz, K.B.; Haber, B.H.; Rosenthal, P.; Mack, C.L.; Moore, J.; Bove, K.E.; Bezerra, J.A.; Kerkar, N.; Shneider, B.L.; Turmelle, Y.P.; et al. Extra-hepatic anomalies in infants with biliary atresia: Results of a large prospective North American multi-center study. Hepatology 2013, 58, 1724–1731. [Google Scholar] [CrossRef] [PubMed]
© 2016 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons by Attribution (CC-BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Maestri Brittain, J.; Borgwardt, L. Potential Pitfalls on the 99mTc-Mebrofenin Hepatobiliary Scintigraphy in a Patient with Biliary Atresia Splenic Malformation Syndrome. Diagnostics 2016, 6, 5. https://doi.org/10.3390/diagnostics6010005
Maestri Brittain J, Borgwardt L. Potential Pitfalls on the 99mTc-Mebrofenin Hepatobiliary Scintigraphy in a Patient with Biliary Atresia Splenic Malformation Syndrome. Diagnostics. 2016; 6(1):5. https://doi.org/10.3390/diagnostics6010005
Chicago/Turabian StyleMaestri Brittain, Jane, and Lise Borgwardt. 2016. "Potential Pitfalls on the 99mTc-Mebrofenin Hepatobiliary Scintigraphy in a Patient with Biliary Atresia Splenic Malformation Syndrome" Diagnostics 6, no. 1: 5. https://doi.org/10.3390/diagnostics6010005
APA StyleMaestri Brittain, J., & Borgwardt, L. (2016). Potential Pitfalls on the 99mTc-Mebrofenin Hepatobiliary Scintigraphy in a Patient with Biliary Atresia Splenic Malformation Syndrome. Diagnostics, 6(1), 5. https://doi.org/10.3390/diagnostics6010005





