Hepatocellular Carcinoma, Fibrolamellar Variant: Diagnostic Pathologic Criteria and Molecular Pathology Update. A Primer
Abstract
:1. Introduction
2. Gross Anatomy and Microscopy
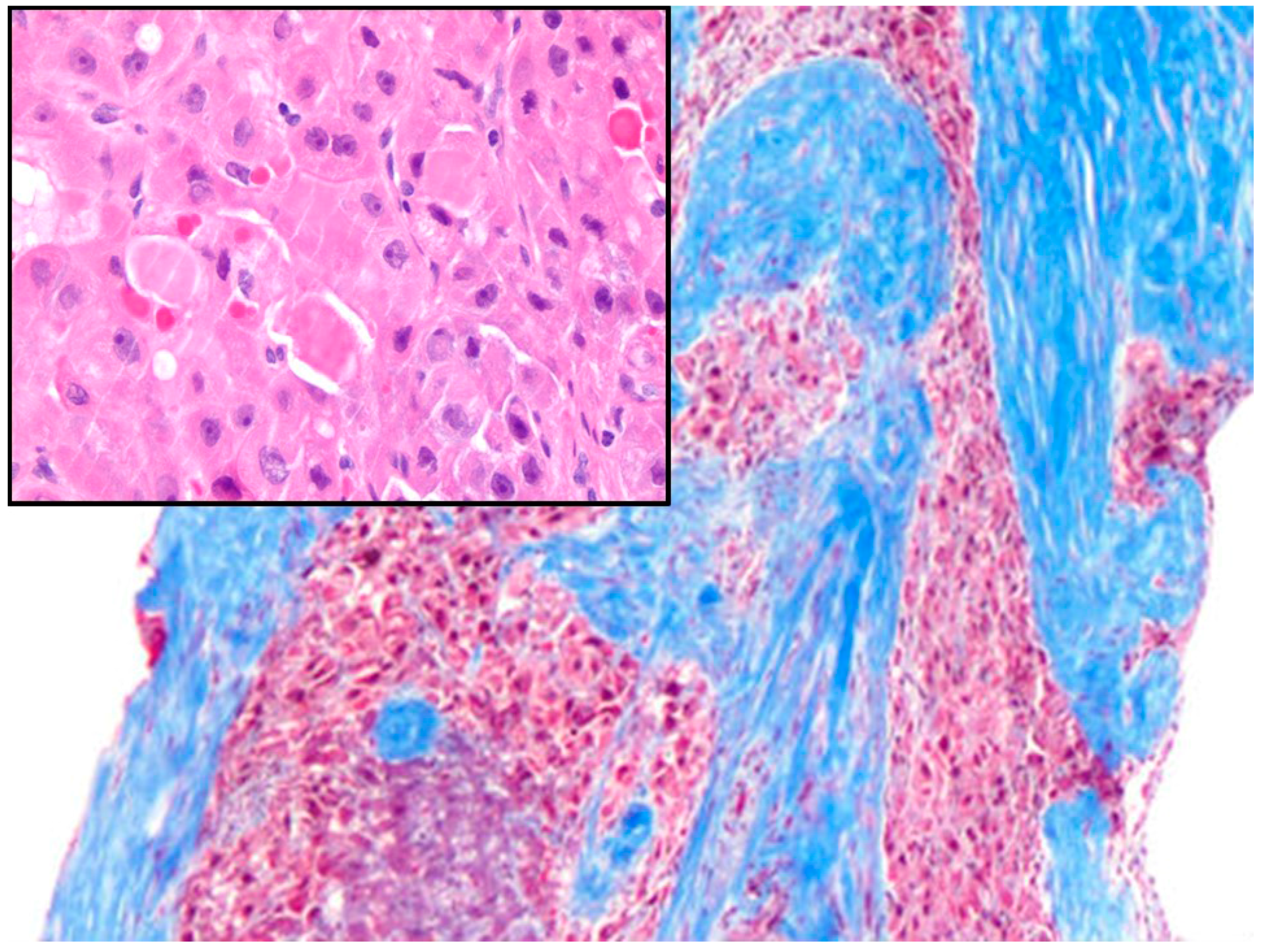
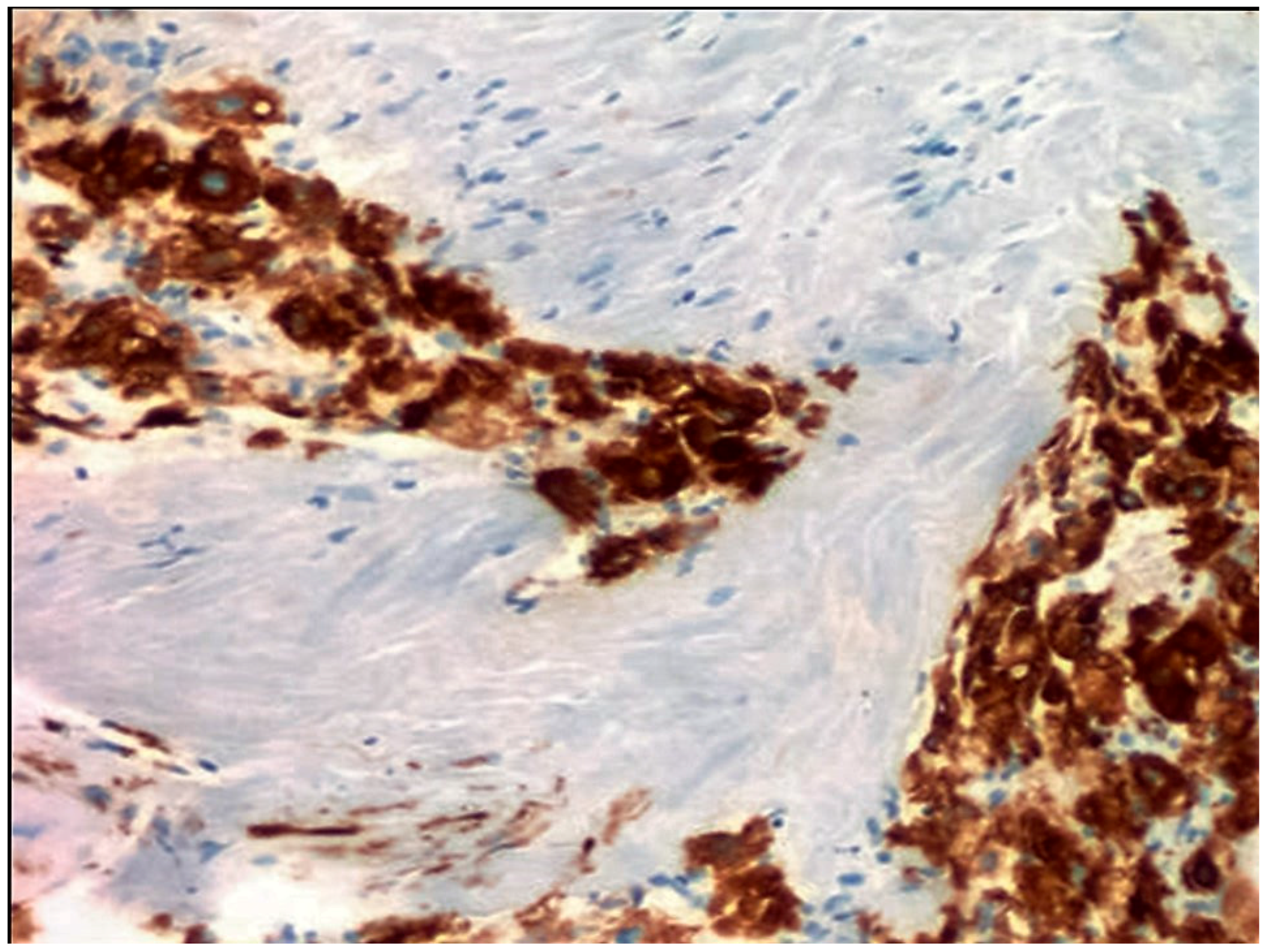
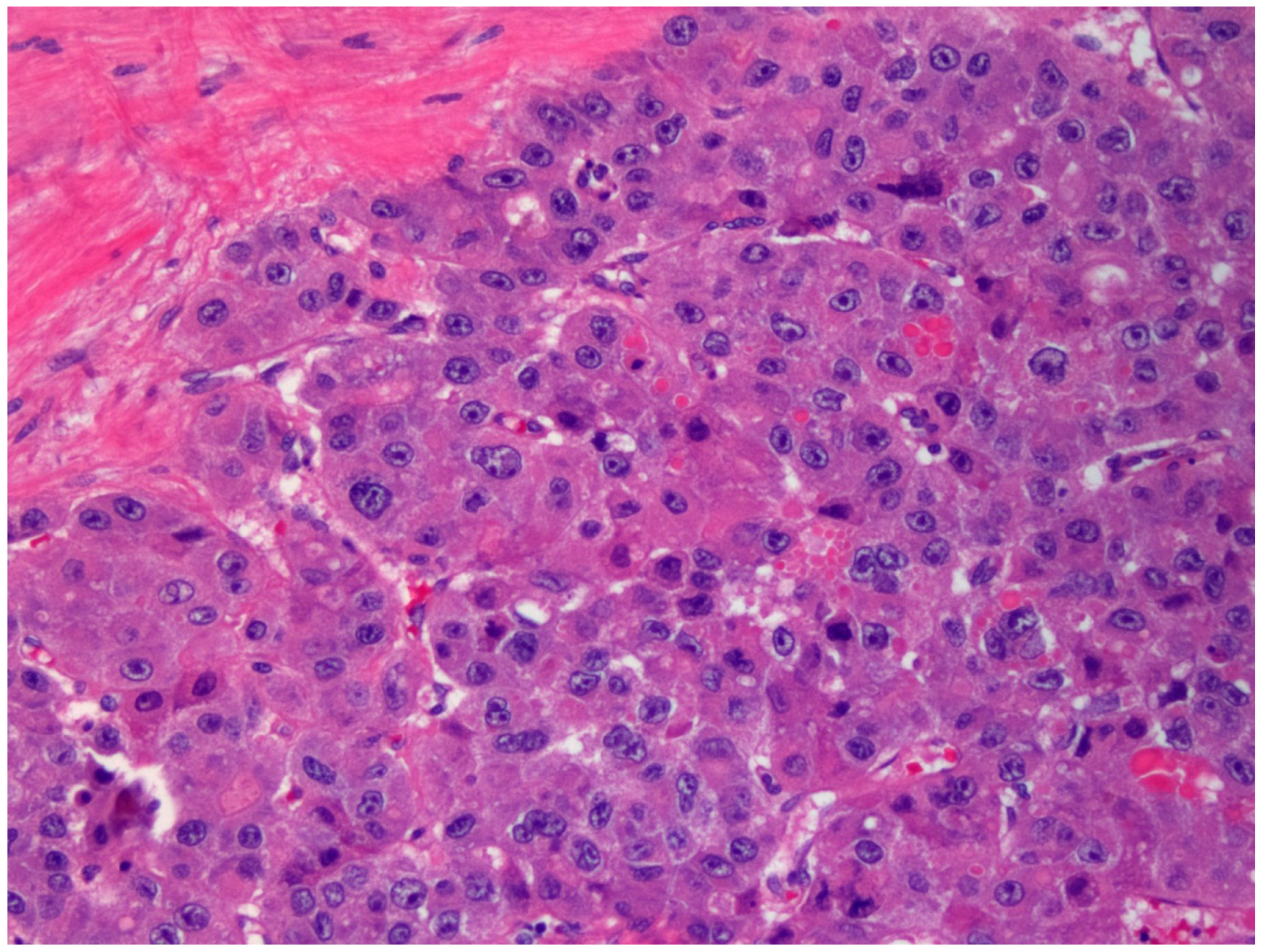
| Age | Tumors | |
|---|---|---|
| FL-HCC | SV-HCC | |
| Youth | Middle-Aged Adults | |
| Distinguishing Parameters | ||
| Hx. Chronic Liver Disease/Cirrhosis | (–) | (+) |
| LN involvement | (±) | (–) |
| Histologic triad (see notes below) | (+) | (–) |
| IHC: HepPar1, p-CEA, Arginase-1 | (+) | (+) |
| IHC: CK-7 (K-7) * | (+) | (–) |
| IHC: NE markers (e.g. NSE, CGA) | (±) | (–) |
| IHC: Glypican-3 | (±) | (+) |
3. Molecular Pathways
4. Conclusions
Acknowledgments
Conflicts of Interest
References
- Sergi, C. Fibrolamellar carcinoma: A distinct variant of hepatocellular carcinoma that is still surrounded by unveils mysteries. J. Cancer Ther. 2014, 5, 1325–1331. [Google Scholar] [CrossRef] [Green Version]
- Tanaka, Y.; Inoue, T.; Horie, H. International pediatric liver cancer pathological classification: Current trend. Int. J. Clin. Oncol. 2013, 18, 946–954. [Google Scholar] [CrossRef] [PubMed]
- Fabbretti, G.; Sergi, C.; Consalez, G.; Faa, G.; Brisigotti, M.; Romeo, G.; Callea, F. Genetic variants of α-1-antitrypsin (AAT). Liver 1992, 12, 296–301. [Google Scholar] [CrossRef] [PubMed]
- Allan, B.J.; Wang, B.; Davis, J.S.; Parikh, P.P.; Perez, E.A.; Neville, H.L.; Sola, J.E. A review of 218 pediatric cases of hepatocellular carcinoma. J. Pediatr. Surg. 2014, 49, 166–171. [Google Scholar] [CrossRef] [PubMed]
- Dominguez-Malagon, H.; Gaytan-Graham, S. Hepatocellular carcinoma: An update. Ultrastruct. Pathol. 2001, 25, 497–516. [Google Scholar] [PubMed]
- Eghtesad, B.; Aucejo, F. Liver transplantation for malignancies. J. Gastrointest. Cancer 2014, 45, 353–362. [Google Scholar] [CrossRef] [PubMed]
- Callea, F.; Sergi, C.; Fabbretti, G.; Brisigotti, M.; Cozzutto, C.; Medicina, D. Precancerous lesions of the biliary tree. J. Surg. Oncol. 1993, 3, 131–133. [Google Scholar] [CrossRef]
- Simonsen, K.; Rode, A.; Nicoll, A.; Villadsen, G.; Espelund, U.; Lim, L.; Angus, P.; Arachchi, N.; Vilstrup, H.; Nexo, E.; et al. Vitamin B12 and its binding proteins in hepatocellular carcinoma and chronic liver diseases. Scand. J. Gastroenterol. 2014, 49, 1096–1102. [Google Scholar] [CrossRef] [PubMed]
- Kanai, T.; Takabayashi, T.; Kawano, Y.; Kuramochi, S.; Miyazawa, N. A case of postoperative recurrence of fibrolamellar hepatocellular carcinoma with increased vitamin B12 binding capacity in a young Japanese female. Jpn. J. Clin. Oncol. 2004, 34, 346–351. [Google Scholar] [CrossRef] [PubMed]
- Kwee, H.G. Fibrolamellar hepatocellular carcinoma. Am. Fam. Phys. 1989, 40, 175–177. [Google Scholar]
- Warnes, T.W.; Smith, A. Tumour markers in diagnosis and management. Baillieres Clin. Gastroenterol. 1987, 1, 63–89. [Google Scholar] [CrossRef]
- Meriggi, F.; Forni, E. [Surgical therapy of hepatic fibrolamellar carcinoma]. Ann. Ital. Chir. 2007, 78, 53–58. [Google Scholar] [PubMed]
- Matsuda, M.; Amemiya, H.; Kawaida, H.; Okamoto, H.; Hosomura, N.; Asakawa, M.; Sano, K.; Motosugi, U.; Ichikawa, T.; Nakazawa, T.; et al. Typical fibrolamellar hepatocellular carcinoma in a Japanese boy: Report of a case. Surg. Today 2014, 44, 1359–1366. [Google Scholar] [CrossRef] [PubMed]
- Tanaka, K.; Honna, T.; Kitano, Y.; Kuroda, T.; Tanaka, K.; Morikawa, N.; Matsuda, H.; Kawashima, N.; Matsuoka, K.; Miyauchi, J. Combined fibrolamellar carcinoma and cholangiocarcinoma exhibiting biphenotypic antigen expression: A case report. J. Clin. Pathol. 2005, 58, 884–887. [Google Scholar] [CrossRef] [PubMed]
- McCloskey, J.J.; Germain-Lee, E.L.; Perman, J.A.; Plotnick, L.P.; Janoski, A.H. Gynecomastia as a presenting sign of fibrolamellar carcinoma of the liver. Pediatrics 1988, 82, 379–382. [Google Scholar] [PubMed]
- Muramori, K.; Taguchi, S.; Taguchi, T.; Kohashi, K.; Furuya, K.; Tokuda, K.; Ishii, E. High aromatase activity and overexpression of epidermal growth factor receptor in fibrolamellar hepatocellular carcinoma in a child. J. Pediatr. Hematol. Oncol. 2011, 33, e195–e197. [Google Scholar] [CrossRef] [PubMed]
- Agarwal, V.R.; Takayama, K.; van Wyk, J.J.; Sasano, H.; Simpson, E.R.; Bulun, S.E. Molecular basis of severe gynecomastia associated with aromatase expression in a fibrolamellar hepatocellular carcinoma. J. Clin. Endocrinol. Metab. 1998, 83, 1797–800. [Google Scholar] [CrossRef] [PubMed]
- Asrani, S.K.; LaRusso, N.F. Fibrolamellar hepatocellular carcinoma presenting with Budd-Chiari syndrome, right atrial thrombus, and pulmonary emboli. Hepatology 2012, 55, 977–978. [Google Scholar] [CrossRef] [PubMed]
- Lamberts, R.; Nitsche, R.; de Vivie, R.E.; Peitsch, W.; Schauer, A.; Schuster, R.; Tebbe, U.; Kreuzer, H.; Creutzfeldt, W. Budd-Chiari syndrome as the primary manifestation of a fibrolamellar hepatocellular carcinoma. Digestion 1992, 53, 200–209. [Google Scholar] [CrossRef] [PubMed]
- Herrmann, G. Immunohistochemical study of HBV antigens in 338 liver cell carcinomas. Z. Gastroenterol. 1999, 37, 329–342. [Google Scholar] [PubMed]
- Dadke, D.; Jaganath, P.; Krishnamurthy, S.; Chiplunkar, S. The detection of HBV antigens and HBx-transcripts in an Indian fibrolamellar carcinoma patient: A case study. Liver 2002, 22, 87–91. [Google Scholar] [CrossRef] [PubMed]
- Davison, F.D.; Fagan, E.A.; Portmann, B.; Williams, R. HBV-DNA sequences in tumor and nontumor tissue in a patient with the fibrolamellar variant of hepatocellular carcinoma. Hepatology 1990, 12, 676–679. [Google Scholar] [CrossRef] [PubMed]
- Sooklim, K.; Sriplung, H.; Piratvisuth, T. Histologic subtypes of hepatocellular carcinoma in the southern Thai population. Asian Pac. J. Cancer Prev. 2003, 4, 302–306. [Google Scholar] [PubMed]
- Arora, R. Fibrolamellar hepatocellular carcinoma presenting as obstructive jaundice: Uncommon presentation of a rare entity. Pol. J. Radiol. 2015, 80, 168–171. [Google Scholar] [CrossRef] [PubMed]
- Rousseau, C.; Ronot, M.; Sibileau, E.; Boulay-Coletta, I.; Lewin, M.; Duchatelle, V.; Vilgrain, V.; Zins, M. Central element in liver masses, helpful, or pitfall? Abdom. Imaging 2015, 40, 1904–1925. [Google Scholar] [CrossRef] [PubMed]
- Valentino, P.L.; Ling, S.C.; Ng, V.L.; John, P.; Bonasoni, P.; Castro, D.A.; Taylor, G.; Chavhan, G.B.; Kamath, B.M. The role of diagnostic imaging and liver biopsy in the diagnosis of focal nodular hyperplasia in children. Liver Int. 2014, 34, 227–234. [Google Scholar] [CrossRef] [PubMed]
- Liu, S.; Wah Chan, K.; Tong, J.; Wang, Y.; Wang, B.; Qiao, L. PET-CT scan is a valuable modality in the diagnosis of fibrolamellar hepatocellular carcinoma: A case report and a summary of recent literature. QJM 2011, 104, 477–483. [Google Scholar] [CrossRef] [PubMed]
- Liu, S.; Chan, K.W.; Wang, B.; Qiao, L. Fibrolamellar hepatocellular carcinoma. Am. J. Gastroenterol. 2009, 104, 2617–2624. [Google Scholar] [CrossRef] [PubMed]
- Kim, T.; Hori, M.; Onishi, H. Liver masses with central or eccentric scar. Semin. Ultrasound CT MRI 2009, 30, 418–425. [Google Scholar] [CrossRef]
- Kamaya, A.; Maturen, K.E.; Tye, G.A.; Liu, Y.I.; Parti, N.N.; Desser, T.S. Hypervascular liver lesions. Semin. Ultrasound CT MRI 2009, 30, 387–407. [Google Scholar] [CrossRef]
- McHugh, P.P.; Gilbert, J.; Vera, S.; Koch, A.; Ranjan, D.; Gedaly, R. α-Fetoprotein and tumour size are associated with microvascular invasion in explanted livers of patients undergoing transplantation with hepatocellular carcinoma. HPB 2010, 12, 56–61. [Google Scholar] [CrossRef] [PubMed]
- Stipa, F.; Yoon, S.S.; Liau, K.H.; Fong, Y.; Jarnagin, W.R.; D’Angelica, M.; Abou-Alfa, G.; Blumgart, L.H.; DeMatteo, R.P. Outcome of patients with fibrolamellar hepatocellular carcinoma. Cancer 2006, 106, 1331–1338. [Google Scholar] [CrossRef] [PubMed]
- Maniaci, V.; Davidson, B.R.; Rolles, K.; Dhillon, A.P.; Hackshaw, A.; Begent, R.H.; Meyer, T. Fibrolamellar hepatocellular carcinoma: Prolonged survival with multimodality therapy. Eur. J. Surg. Oncol. 2009, 35, 617–621. [Google Scholar] [CrossRef] [PubMed]
- Jaeck, D. The significance of hepatic pedicle lymph nodes metastases in surgical management of colorectal liver metastases and of other liver malignancies. Ann. Surg. Oncol. 2003, 10, 1007–1011. [Google Scholar] [CrossRef] [PubMed]
- Callea, F.; Sergi, C.; Medicina, D.; Pizzorni, S.; Brisigotti, M.; Fabbretti, G.; Bonino, F. From immunohistochemistry to in situ hybridization. Liver 1992, 12, 290–295. [Google Scholar] [CrossRef] [PubMed]
- Torbenson, M. Fibrolamellar carcinoma: 2012 update. Scientifica 2012, 2012, 743790. [Google Scholar] [CrossRef] [PubMed]
- Ross, H.M.; Daniel, H.D.; Vivekanandan, P.; Kannangai, R.; Yeh, M.M.; Wu, T.T.; Makhlouf, H.R.; Torbenson, M. Fibrolamellar carcinomas are positive for CD68. Mod. Pathol. 2011, 24, 390–395. [Google Scholar] [CrossRef] [PubMed]
- Darcy, D.G.; Malek, M.M.; Kobos, R.; Klimstra, D.S.; DeMatteo, R.; La Quaglia, M.P. Prognostic factors in fibrolamellar hepatocellular carcinoma in young people. J. Pediatr. Surg. 2015, 50, 153–156. [Google Scholar] [CrossRef] [PubMed]
- Patonai, A.; Erdelyi-Belle, B.; Korompay, A.; Somoracz, A.; Torzsok, P.; Kovalszky, I.; Barbai, T.; Raso, E.; Lotz, G.; Schaff, Z.; et al. Molecular characteristics of fibrolamellar hepatocellular carcinoma. Pathol. Oncol. Res. 2013, 19, 63–70. [Google Scholar] [CrossRef] [PubMed]
- Chagas, A.L.; Kikuchi, L.; Herman, P.; Alencar, R.S.; Tani, C.M.; Diniz, M.A.; Pugliese, V.; Rocha Mde, S.; D’Albuquerque, L.A.; Carrilho, F.J.; et al. Clinical and pathological evaluation of fibrolamellar hepatocellular carcinoma: A single center study of 21 cases. Clinics 2015, 70, 207–213. [Google Scholar] [CrossRef]
- Wolosz, D.; Walczak, A.; Wilczynski, G.M.; Szparecki, G.; Wilczek, E.; Gornicka, B. Deleted in liver cancer 1 expression and localization in hepatocellular carcinoma tissue sections. Oncol. Lett. 2014, 8, 785–788. [Google Scholar] [CrossRef] [PubMed]
- Ward, S.C.; Huang, J.; Tickoo, S.K.; Thung, S.N.; Ladanyi, M.; Klimstra, D.S. Fibrolamellar carcinoma of the liver exhibits immunohistochemical evidence of both hepatocyte and bile duct differentiation. Mod. Pathol. 2010, 23, 1180–1190. [Google Scholar] [CrossRef] [PubMed]
- Brumm, C.; Schulze, C.; Charels, K.; Morohoshi, T.; Kloppel, G. The significance of α-fetoprotein and other tumour markers in differential immunocytochemistry of primary liver tumours. Histopathology 1989, 14, 503–513. [Google Scholar] [CrossRef] [PubMed]
- Shafizadeh, N.; Ferrell, L.D.; Kakar, S. Utility and limitations of glypican-3 expression for the diagnosis of hepatocellular carcinoma at both ends of the differentiation spectrum. Mod. Pathol. 2008, 21, 1011–1018. [Google Scholar] [CrossRef] [PubMed]
- Zhou, S.; Parham, D.M.; Yung, E.; Pattengale, P.; Wang, L. Quantification of glypican 3, β-catenin and claudin-1 protein expression in hepatoblastoma and paediatric hepatocellular carcinoma by colour deconvolution. Histopathology 2015. [Google Scholar] [CrossRef] [PubMed]
- Klein, W.M.; Molmenti, E.P.; Colombani, P.M.; Grover, D.S.; Schwarz, K.B.; Boitnott, J.; Torbenson, M.S. Primary liver carcinoma arising in people younger than 30 years. Am. J. Clin. Pathol. 2005, 124, 512–518. [Google Scholar] [CrossRef] [PubMed]
- Ang, C.S.; Kelley, R.K.; Choti, M.A.; Cosgrove, D.P.; Chou, J.F.; Klimstra, D.; Torbenson, M.S.; Ferrell, L.; Pawlik, T.M.; Fong, Y.; et al. Clinicopathologic characteristics and survival outcomes of patients with fibrolamellar carcinoma: Data from the fibrolamellar carcinoma consortium. Gastrointest. Cancer Res. 2013, 6, 3–9. [Google Scholar] [PubMed]
- Lildballe, D.L.; Nguyen, K.Q.; Poulsen, S.S.; Nielsen, H.O.; Nexo, E. Haptocorrin as marker of disease progression in fibrolamellar hepatocellular carcinoma. Eur. J. Surg. Oncol. 2011, 37, 72–79. [Google Scholar] [CrossRef] [PubMed]
- Patonai, A.; Erdelyi-Belle, B.; Korompay, A.; Somoracz, A.; Straub, B.K.; Schirmacher, P.; Kovalszky, I.; Lotz, G.; Kiss, A.; Schaff, Z. Claudins and tricellulin in fibrolamellar hepatocellular carcinoma. Virchows Arch. 2011, 458, 679–688. [Google Scholar] [CrossRef] [PubMed]
- Rosa, M.; Mohammadi, A. Cytologic features of fibrolamellar carcinoma with mucin production: A rare variant of combined hepatocellular-cholangiocarcinoma. Diagn. Cytopathol. 2014, 42, 431–435. [Google Scholar] [CrossRef] [PubMed]
- Gulati, G.; Saran, R.K. Fine needle aspiration cytology of fibrolamellar hepatocellular carcinoma: Recognizing the oncocytic hepatocyte. Indian J. Pathol. Microbiol. 2009, 52, 288–289. [Google Scholar] [CrossRef] [PubMed]
- Montero, A.; Allende, H.; Tallada, N.; Ramon y Cajal, S.; Margarit, C.; Viladomiu, L. Fine needle aspiration cytology of massive bilateral ovarian metastasis of fibrolamellar hepatocellular carcinoma. Acta Cytol. 2007, 51, 682–683. [Google Scholar] [PubMed]
- Renshaw, A.A.; Haja, J.; Wilbur, D.C.; Miller, T.R.; Cytology Committee College of American Pathologists. Fine-needle aspirates of hepatocellular carcinoma that are misclassified as adenocarcinoma: Correlating cytologic features and performance in the College of American Pathologists Nongynecologic Cytology Program. Arch. Pathol. Lab. Med. 2006, 130, 19–22. [Google Scholar] [PubMed]
- Sarode, V.R.; Castellani, R.; Post, A. Fine-needle aspiration cytology and differential diagnoses of fibrolamellar hepatocellular carcinoma metastatic to the mediastinum: Case report. Diagn. Cytopathol. 2002, 26, 95–98. [Google Scholar] [CrossRef] [PubMed]
- Al-Bahrani, R.; Abuetabh, Y.; Zeitouni, N.; Sergi, C. Cholangiocarcinoma: Risk factors, environmental influences and oncogenesis. Ann. Clin. Lab. Sci. 2013, 43, 195–210. [Google Scholar] [PubMed]
- Sergi, C.; Adam, S.; Kahl, P.; Otto, H.F. The remodeling of the primitive human biliary system. Early Hum. Dev. 2000, 58, 167–178. [Google Scholar] [CrossRef]
- Sergi, C.; Adam, S.; Kahl, P.; Otto, H.F. Study of the malformation of ductal plate of the liver in Meckel syndrome and review of other syndromes presenting with this anomaly. Pediatr. Dev. Pathol. 2000, 3, 568–583. [Google Scholar] [CrossRef] [PubMed]
- Sergi, C.; Kahl, P.; Otto, H.F. Contribution of apoptosis and apoptosis-related proteins to the malformation of the primitive intrahepatic biliary system in Meckel syndrome. Am. J. Pathol. 2000, 156, 1589–1598. [Google Scholar] [CrossRef]
- Sergi, C.; Benstz, J.; Feist, D.; Nutzenadel, W.; Otto, H.F.; Hofmann, W.J. Bile duct to portal space ratio and ductal plate remnants in liver disease of infants aged less than 1 year. Pathology 2008, 40, 260–277. [Google Scholar] [CrossRef] [PubMed]
- Corti, B.; D’Errico, A.; Pierangeli, F.; Fiorentino, M.; Altimari, A.; Grigioni, W.F. Primary paraganglioma strictly confined to the liver and mimicking hepatocellular carcinoma: An immunohistochemical and in situ hybridization study. Am. J. Surg. Pathol. 2002, 26, 945–949. [Google Scholar] [CrossRef] [PubMed]
- Cheuk, W.; Chan, J.K. Clear cell variant of fibrolamellar carcinoma of the liver. Arch. Pathol. Lab. Med. 2001, 125, 1235–1238. [Google Scholar] [PubMed]
- Kannangai, R.; Vivekanandan, P.; Martinez-Murillo, F.; Choti, M.; Torbenson, M. Fibrolamellar carcinomas show overexpression of genes in the RAS, MAPK, PIK3, and xenobiotic degradation pathways. Hum. Pathol. 2007, 38, 639–644. [Google Scholar] [CrossRef] [PubMed]
- Allegra, C.J.; Rumble, R.B.; Hamilton, S.R.; Mangu, P.B.; Roach, N.; Hantel, A.; Schilsky, R.L. Extended RAS gene mutation testing in metastatic colorectal carcinoma to predict response to anti-epidermal growth factor receptor monoclonal antibody therapy: American Society of Clinical Oncology Provisional Clinical Opinion update 2015. J. Clin. Oncol. 2015. [Google Scholar] [CrossRef] [PubMed]
- Dietel, M.; Johrens, K.; Laffert, M.V.; Hummel, M.; Blaker, H.; Pfitzner, B.M.; Lehmann, A.; Denkert, C.; Darb-Esfahani, S.; Lenze, D.; et al. A 2015 update on predictive molecular pathology and its role in targeted cancer therapy: A review focussing on clinical relevance. Cancer Gene Ther. 2015, 22, 417–430. [Google Scholar] [CrossRef] [PubMed]
- Shanbhogue, A.K.; Prasad, S.R.; Takahashi, N.; Vikram, R.; Sahani, D.V. Recent advances in cytogenetics and molecular biology of adult hepatocellular tumors: Implications for imaging and management. Radiology 2011, 258, 673–693. [Google Scholar] [CrossRef] [PubMed]
- Shimokawa, H.; Satoh, K. 2015 ATVB Plenary Lecture: Translational research on rho-kinase in cardiovascular medicine. Arterioscler. Thromb. Vasc. Biol. 2015, 35, 1756–1769. [Google Scholar] [CrossRef] [PubMed]
- Buhler, S.; Laufer, S.A. p38 MAPK inhibitors: A patent review (2012–2013). Expert Opin. Ther. Pat. 2014, 24, 535–554. [Google Scholar] [CrossRef] [PubMed]
- Carbajo-Pescador, S.; Mauriz, J.L.; Garcia-Palomo, A.; Gonzalez-Gallego, J. FoxO proteins: Regulation and molecular targets in liver cancer. Curr. Med. Chem. 2014, 21, 1231–1246. [Google Scholar] [CrossRef] [PubMed]
- Zeng, L.; Tang, W.J.; Yin, J.J.; Zhou, B.J. Signal transductions and nonalcoholic fatty liver: A mini-review. Int. J. Clin. Exp. Med. 2014, 7, 1624–1631. [Google Scholar] [PubMed]
- Matsuda, S.; Kobayashi, M.; Kitagishi, Y. Roles for PI3K/AKT/PTEN Pathway in Cell Signaling of Nonalcoholic Fatty Liver Disease. ISRN Endocrinol. 2013, 2013, 472432. [Google Scholar] [CrossRef] [PubMed]
- Tsukamoto, H. Metabolic reprogramming and cell fate regulation in alcoholic liver disease. Pancreatology 2015, 15, S61–S65. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Riehle, K.J.; Yeh, M.M.; Yu, J.J.; Kenerson, H.L.; Harris, W.P.; Park, J.O.; Yeung, R.S. mTORC1 and FGFR1 signaling in fibrolamellar hepatocellular carcinoma. Mod. Pathol. 2015, 28, 103–110. [Google Scholar] [CrossRef] [PubMed]
- Cornella, H.; Alsinet, C.; Sayols, S.; Zhang, Z.; Hao, K.; Cabellos, L.; Hoshida, Y.; Villanueva, A.; Thung, S.; Ward, S.C.; et al. Unique genomic profile of fibrolamellar hepatocellular carcinoma. Gastroenterology 2015, 148, 806–818. [Google Scholar] [CrossRef] [PubMed]
- Graham, R.P.; Jin, L.; Knutson, D.L.; Kloft-Nelson, S.M.; Greipp, P.T.; Waldburger, N.; Roessler, S.; Longerich, T.; Roberts, L.R.; Oliveira, A.M.; et al. DNAJB1-PRKACA is specific for fibrolamellar carcinoma. Mod. Pathol. 2015, 28, 822–829. [Google Scholar] [CrossRef] [PubMed]
- Honeyman, J.N.; Simon, E.P.; Robine, N.; Chiaroni-Clarke, R.; Darcy, D.G.; Lim, I.I.; Gleason, C.E.; Murphy, J.M.; Rosenberg, B.R.; Teegan, L.; et al. Detection of a recurrent DNAJB1-PRKACA chimeric transcript in fibrolamellar hepatocellular carcinoma. Science 2014, 343, 1010–1014. [Google Scholar] [CrossRef] [PubMed]
- Darcy, D.G.; Chiaroni-Clarke, R.; Murphy, J.M.; Honeyman, J.N.; Bhanot, U.; LaQuaglia, M.P.; Simon, S.M. The genomic landscape of fibrolamellar hepatocellular carcinoma: Whole genome sequencing of ten patients. Oncotarget 2015, 6, 755–770. [Google Scholar] [CrossRef] [PubMed]
- Lim, I.I.; Farber, B.A.; LaQuaglia, M.P. Advances in fibrolamellar hepatocellular carcinoma: A review. Eur. J. Pediatr. Surg. 2014, 24, 461–466. [Google Scholar] [CrossRef] [PubMed]
- Edmondson, H.A. Differential diagnosis of tumors and tumor-like lesions of liver in infancy and childhood. AMA J. Dis. Child 1956, 91, 168–186. [Google Scholar] [CrossRef] [PubMed]
- Arslan, I.; Oner, K.; Kilicturgay, S.; Agar, N.; Alpaslan, F. Fibrolamellar hepatocellular carcinoma ”It is not a ordinary case for Mediterranean countries”. HPB Surg. 1995, 9, 51–53. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Craig, J.R.; Peters, R.L.; Edmondson, H.A.; Omata, M. Fibrolamellar carcinoma of the liver: A tumor of adolescents and young adults with distinctive clinico-pathologic features. Cancer 1980, 46, 372–379. [Google Scholar] [CrossRef]
- Bahitham, W.; Liao, X.; Peng, F.; Bamforth, F.; Chan, A.; Mason, A.; Stone, B.; Stothard, P.; Sergi, C. Mitochondriome and cholangiocellular carcinoma. PLoS ONE 2014, 9, e104694. [Google Scholar] [CrossRef] [PubMed]
© 2015 by the author; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons by Attribution (CC-BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sergi, C.M. Hepatocellular Carcinoma, Fibrolamellar Variant: Diagnostic Pathologic Criteria and Molecular Pathology Update. A Primer. Diagnostics 2016, 6, 3. https://doi.org/10.3390/diagnostics6010003
Sergi CM. Hepatocellular Carcinoma, Fibrolamellar Variant: Diagnostic Pathologic Criteria and Molecular Pathology Update. A Primer. Diagnostics. 2016; 6(1):3. https://doi.org/10.3390/diagnostics6010003
Chicago/Turabian StyleSergi, Consolato M. 2016. "Hepatocellular Carcinoma, Fibrolamellar Variant: Diagnostic Pathologic Criteria and Molecular Pathology Update. A Primer" Diagnostics 6, no. 1: 3. https://doi.org/10.3390/diagnostics6010003
APA StyleSergi, C. M. (2016). Hepatocellular Carcinoma, Fibrolamellar Variant: Diagnostic Pathologic Criteria and Molecular Pathology Update. A Primer. Diagnostics, 6(1), 3. https://doi.org/10.3390/diagnostics6010003






