Ultrasonographic Assessment of the Diaphragm
Abstract
1. Introduction
2. Mechanisms of Diaphragm Muscle Injury Induced by Mechanical Ventilation
2.1. Disuse Atrophy
2.2. Concentric Load-Induced Injury
2.3. Eccentric Load-Induced Injury
2.4. Longitudinal Atrophy
3. Basics of Diaphragm Ultrasonography
3.1. Intercostal Approach
3.2. Subcostal Approach
4. Clinical Applications of Diaphragm Ultrasonography
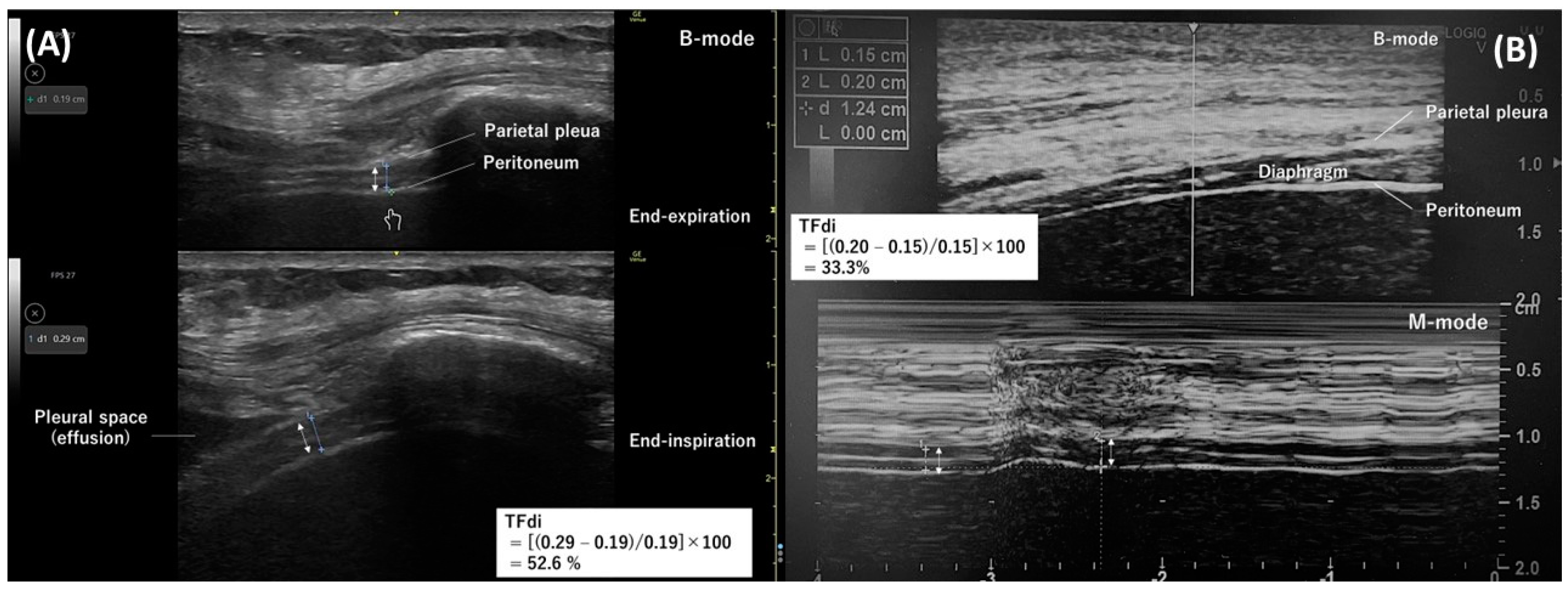
4.1. Evaluation of Diaphragm Thickness
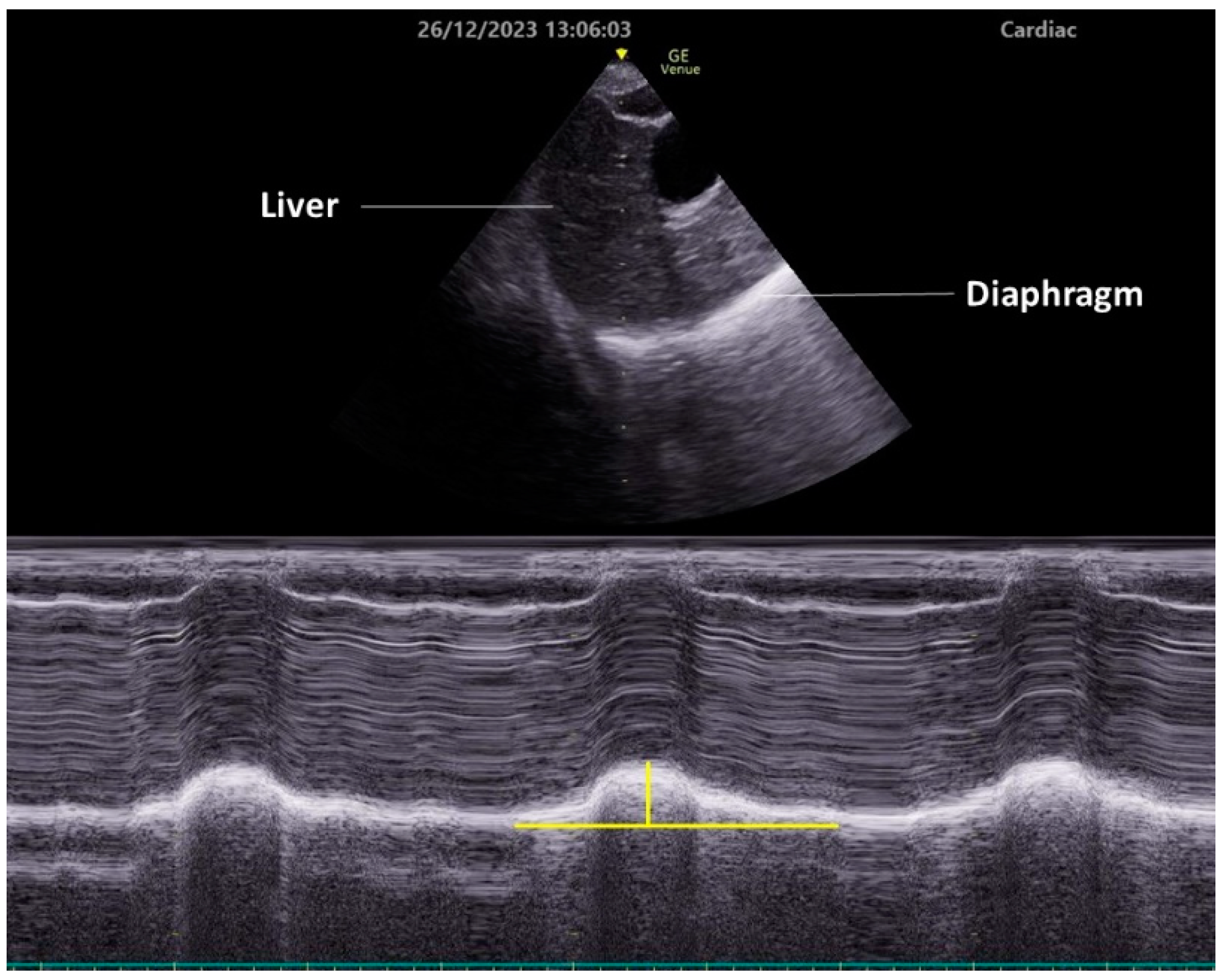
4.2. Evaluation of Diaphragm Function
4.3. Evaluation of Respiratory Effort
4.4. Prediction of Weaning Outcomes
5. Expert Consensus
6. Future Perspectives
7. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Tremblay, L.N.; Slutsky, A.S. Ventilator-induced lung injury: From the bench to the bedside. Intensive Care Med. 2006, 32, 24–33. [Google Scholar] [CrossRef]
- Goligher, E.C.; Brochard, L.J.; Reid, W.D.; Fan, E.; Saarela, O.; Slutsky, A.S.; Kavanagh, B.P.; Rubenfeld, G.D.; Ferguson, N.D. Diaphragmatic myotrauma: A mediator of prolonged ventilation and poor patient outcomes in acute respiratory failure. Lancet Respir. Med. 2019, 7, 90–98. [Google Scholar] [CrossRef]
- Kim, W.Y.; Suh, H.J.; Hong, S.B.; Koh, Y.; Lim, C.M. Diaphragm dysfunction assessed by ultrasonography: Influence on weaning from mechanical ventilation. Crit. Care Med. 2011, 39, 2627–2630. [Google Scholar] [CrossRef] [PubMed]
- Sassoon, C.S.H.H.; Caiozzo, V.J.; Manka, A.; Sieck, G.C. Altered diaphragm contractile properties with controlled mechanical ventilation. J. Appl. Physiol. 2002, 92, 2585–2595. [Google Scholar] [CrossRef]
- Shanely, R.A.; Zergeroglu, M.A.; Lennon, S.L.; Sugiura, T.; Yimlamai, T.; Enns, D.; Belcastro, A.; Powers, S.K. Mechanical ventilation-induced diaphragmatic atrophy is associated with oxidative injury and increased proteolytic activity. Am. J. Respir. Crit. Care Med. 2002, 166, 1369–1374. [Google Scholar] [CrossRef] [PubMed]
- Levine, S.; Nguyen, T.; Taylor, N.; Friscia, M.E.; Budak, M.T.; Rothenberg, P.; Zhu, J.; Sachdeva, R.; Sonnad, S.; Kaiser, L.R.; et al. Rapid disuse atrophy of diaphragm fibers in mechanically ventilated humans. N. Engl. J. Med. 2008, 358, 1327–1335. [Google Scholar] [CrossRef]
- Goligher, E.C.; Fan, E.; Herridge, M.S.; Murray, A.; Vorona, S.; Brace, D.; Rittayamai, N.; Lanys, A.; Tomlinson, G.; Singh, J.M.; et al. Evolution of diaphragm thickness during mechanical ventilation: Impact of inspiratory effort. Am. J. Respir. Crit. Care Med. 2015, 192, 1080–1088. [Google Scholar] [CrossRef]
- Dres, M.; Dube, B.P.; Mayaux, J.; Delemazure, J.; Reuter, D.; Brochard, L.; Similowski, T.; Demoule, A. Coexistence and impact of limb muscle and diaphragm weakness at time of liberation from mechanical ventilation in medical intensive care unit patients. Am. J. Respir. Crit. Care Med. 2017, 195, 57–66. [Google Scholar] [CrossRef]
- Goligher, E.C.; Dres, M.; Fan, E.; Rubenfeld, G.D.; Scales, D.C.; Herridge, M.S.; Vorona, S.; Sklar, M.C.; Rittayamai, N.; Lanys, A.; et al. Mechanical ventilation-induced diaphragm atrophy strongly impacts clinical outcomes. Am. J. Respir. Crit. Care Med. 2018, 197, 204–213. [Google Scholar] [CrossRef] [PubMed]
- Demoule, A.; Jung, B.; Prodanovic, H.; Molinari, N.; Chanques, G.; Coirault, C.; Matecki, S.; Duguet, A.; Similowski, T.; Jaber, S. Diaphragm dysfunction on admission to the intensive care unit: Prevalence, risk factors, and prognostic impact—A prospective study. Am. J. Respir. Crit. Care Med. 2013, 188, 213–219. [Google Scholar] [CrossRef]
- Heunks, L.M.A.; Doorduin, J.; van der Hoeven, J.G. Monitoring and preventing diaphragm injury. Curr. Opin. Crit. Care 2015, 21, 34–41. [Google Scholar] [CrossRef] [PubMed]
- Haaksma, M.E.; Smit, J.M.; Boussuges, A.; Demoule, A.; Dres, M.; Ferrari, G.; Formenti, P.; Goligher, E.C.; Heunks, L.; Lim, E.H.T.; et al. EXpert consensus On Diaphragm UltraSonography in the critically ill (EXODUS): A Delphi consensus statement on the measurement of diaphragm ultrasound-derived parameters in a critical care setting. Crit. Care 2022, 26, 99. [Google Scholar] [CrossRef] [PubMed]
- Petrof, B.J. Diaphragm Weakness in the Critically Ill: Basic Mechanisms Reveal Therapeutic Opportunities. Chest 2018, 154, 1395–1403. [Google Scholar] [CrossRef] [PubMed]
- Yang, L.; Luo, J.; Bourdon, J.; Lin, M.C.; Gottfried, S.B.; Petrof, B.J. Controlled mechanical ventilation leads to remodeling of the rat diaphragm. Am. J. Respir. Crit. Care Med. 2002, 166, 1135–1140. [Google Scholar] [CrossRef]
- Radell, P.J.; Remahl, S.; Nichols, D.G.; Eriksson, L.I. Effects of prolonged mechanical ventilation and inactivity on piglet diaphragm function. Intensive Care Med. 2002, 28, 358–364. [Google Scholar] [CrossRef] [PubMed]
- Levine, S.; Biswas, C.; Dierov, J.; Barsotti, R.; Shrager, J.B.; Nguyen, T.; Sonnad, S.; Kucharchzuk, J.C.; Kaiser, L.R.; Singhal, S.; et al. Increased proteolysis, myosin depletion, and atrophic AKT-FOXO signaling in human diaphragm disuse. Am. J. Respir. Crit. Care Med. 2011, 183, 483–490. [Google Scholar] [CrossRef] [PubMed]
- Jaber, S.; Petrof, B.J.; Jung, B.; Chanques, G.; Berthet, J.-P.; Rabuel, C.; Bouyabrine, H.; Courouble, P.; Koechlin-Ramonatxo, C.; Sebbane, M.; et al. Rapidly progressive diaphragmatic weakness and injury during mechanical ventilation in humans. Am. J. Respir. Crit. Care Med. 2011, 183, 364–371. [Google Scholar] [CrossRef]
- Orozco-levi, M.; Lloreta, J.; Minguella, J.; Serrano, S.; Broquetas, J.M.; Gea, J. Injury of the Human Diaphragm Associated with. Am. J. Respir. Crit. Care Med. 2001, 164, 1734–1739. [Google Scholar] [CrossRef]
- Jiang, T.X.; Reid, W.D.; Belcastro, A.; Road, J.D. Load dependence of secondary diaphragm inflammation and injury after acute inspiratory loading. Am. J. Respir. Crit. Care Med. 1998, 157, 230–236. [Google Scholar] [CrossRef]
- Lin, M.C.; Ebihara, S.; Dwairi, Q.E.L.; Hussain, S.N.A.; Yang, L.; Gottfried, S.B.; Comtois, A.; Petrof, B.J. Diaphragm sarcolemmal injury is induced by sepsis and alleviated by nitric oxide synthase inhibition. Am. J. Respir. Crit. Care Med. 1998, 158, 1656–1663. [Google Scholar] [CrossRef]
- Proske, U.; Morgan, D.L.; Proske, U.; Morgan, D.L. Muscle damage from eccentric exercise: Mechanism, mechanical signs, adaptation and clinical applications. J. Physiol. 2001, 537, 333–345. Available online: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2278966/pdf/tjp0537-0333.pdf (accessed on 1 June 2024). [CrossRef] [PubMed]
- García-Valdés, P.; Fernández, T.; Jalil, Y.; Peñailillo, L.; Damiani, L.F. Eccentric Contractions of the Diaphragm during Mechanical Ventilation. Respir. Care 2023, 68, 1757–1762. [Google Scholar] [CrossRef] [PubMed]
- Itagaki, T. Diaphragm-protective mechanical ventilation in acute respiratory failure. J. Med. Investig. 2022, 69, 165–172. [Google Scholar] [CrossRef] [PubMed]
- Pellegrini, M.; Hedenstierna, G.; Roneus, A.; Segelsjö, M.; Larsson, A.; Perchiazzi, G. The diaphragm acts as a brake during expiration to prevent lung collapse. Am. J. Respir. Crit. Care Med. 2017, 195, 1608–1616. [Google Scholar] [CrossRef]
- Goligher, E.C.; Dres, M.; Patel, B.K.; Sahetya, S.K.; Beitler, J.R.; Telias, I.; Yoshida, T.; Vaporidi, K.; Grieco, D.L.; Schepens, T.; et al. Lung- And diaphragm-protective ventilation. Am. J. Respir. Crit. Care Med. 2020, 202, 950–961. [Google Scholar] [CrossRef] [PubMed]
- Volta, C.A.; Dalla Corte, F.; Ragazzi, R.; Marangoni, E.; Fogagnolo, A.; Scaramuzzo, G.; Grieco, D.L.; Alvisi, V.; Rizzuto, C.; Spadaro, S. Expiratory flow limitation in intensive care: Prevalence and risk factors. Crit. Care 2019, 23, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Doorduin, J.; Roesthuis, L.H.; Jansen, D.; van der Hoeven, J.G.; van Hees, H.W.H.; Heunks, L.M.A. Respiratory Muscle Effort during Expiration in Successful and Failed Weaning from Mechanical Ventilation. Anesthesiology 2018, 129, 490–501. [Google Scholar] [CrossRef] [PubMed]
- Lindqvist, J.; Van Den Berg, M.; Van Der Pijl, R.; Hooijman, P.E.; Beishuizen, A.; Elshof, J.; de Waard, M.; Girbes, A.; Man, A.S.-D.; Shi, Z.-H.; et al. Positive end-expiratory pressure ventilation induces longitudinal atrophy in diaphragm fibers. Am. J. Respir. Crit. Care Med. 2018, 198, 472–485. [Google Scholar] [CrossRef]
- Dinino, E.; Gartman, E.J.; Sethi, J.M.; McCool, F.D. Diaphragm ultrasound as a predictor of successful extubation from mechanical ventilation. Thorax 2014, 69, 423–427. [Google Scholar] [CrossRef]
- Ferrari, G.; De Filippi, G.; Elia, F.; Panero, F.; Volpicelli, G.; Aprà, F. Diaphragm ultrasound as a new index of discontinuation from mechanical ventilation. Crit. Ultrasound J. 2014, 6, 8. [Google Scholar] [CrossRef]
- Farghaly, S.; Hasan, A.A. Diaphragm ultrasound as a new method to predict extubation outcome in mechanically ventilated patients. Aust. Crit. Care 2017, 30, 37–43. [Google Scholar] [CrossRef]
- Mariani, L.F.; Bedel, J.; Gros, A.; Lerolle, N.; Milojevic, K.; Laurent, V.; Hilly, J.; Troché, G.; Bedos, J.P.; Planquette, B. Ultrasonography for Screening and Follow-Up of Diaphragmatic Dysfunction in the ICU: A Pilot Study. J. Intensive Care Med. 2016, 31, 338–343. [Google Scholar] [CrossRef] [PubMed]
- Lerolle, N.; Guérot, E.; Dimassi, S.; Zegdi, R.; Faisy, C.; Fagon, J.-Y.; Diehl, J.-L. Ultrasonographic diagnostic criterion for severe diaphragmatic dysfunction after cardiac surgery. Chest 2009, 135, 401–407. [Google Scholar] [CrossRef] [PubMed]
- Carrillo-Esper, R.; Pérez-Calatayud, Á.A.; Arch-Tirado, E.; Díaz-Carrillo, M.A.; Garrido-Aguirre, E.; Tapia-Velazco, R.; Peña-Pérez, C.A.; Monteros, I.E.-D.L.; Meza-Márquez, J.M.; Flores-Rivera, O.I.; et al. Standardization of sonographic diaphragm thickness evaluations in healthy volunteers. Respir. Care 2016, 61, 920–924. [Google Scholar] [CrossRef] [PubMed]
- Boussuges, A.; Gole, Y.; Blanc, P. Diaphragmatic motion studied by M-mode ultrasonography. Chest 2009, 135, 391–400. [Google Scholar] [CrossRef] [PubMed]
- Gottesman, E.; McCool, F.D. Ultrasound evaluation of the paralyzed diaphragm. Am. J. Respir. Crit. Care Med. 1997, 155, 1570–1574. [Google Scholar] [CrossRef]
- Boon, A.J.; Harper, C.J.; Ghahfarokhi, L.S.; Strommen, J.A.; Watson, J.C.; Sorenson, E.J. Two-dimensional ultrasound imaging of the diaphragm: Quantitative values in normal subjects. Muscle Nerve 2013, 47, 884–889. [Google Scholar] [CrossRef]
- Matamis, D.; Soilemezi, E.; Tsagourias, M.; Akoumianaki, E.; Dimassi, S.; Boroli, F.; Richard, J.-C.M.; Brochard, L. Sonographic evaluation of the diaphragm in critically ill patients. Technique and clinical applications. Intensive Care Med. 2013, 39, 801–810. [Google Scholar] [CrossRef] [PubMed]
- Tuinman, P.R.; Jonkman, A.H.; Dres, M.; Shi, Z.-H.; Goligher, E.C.; Goffi, A.; de Korte, C.; Demoule, A.; Heunks, L. Respiratory muscle ultrasonography: Methodology, basic and advanced principles and clinical applications in ICU and ED patients—A narrative review. Intensive Care Med. 2020, 46, 594–605. [Google Scholar] [CrossRef]
- Goligher, E.C.; Laghi, F.; Detsky, M.E.; Farias, P.; Murray, A.; Brace, D.; Brochard, L.J.; Bolz, S.S.; Rubenfeld, G.D.; Kavanagh, B.P.; et al. Measuring diaphragm thickness with ultrasound in mechanically ventilated patients: Feasibility, reproducibility and validity. Intensive Care Med. 2015, 41, 642–649. [Google Scholar] [CrossRef]
- Cohn, D.; Benditt, J.O.; Eveloff, S.; McCool, F.D. Diaphragm thickening during inspiration. J. Appl. Physiol. 1997, 83, 291–296. [Google Scholar] [CrossRef] [PubMed]
- Da Conceicao, D.; Perlas, A.; Giron Arango, L.; Wild, K.; Li, Q.; Huszti, E.; Chowdhury, J.; Chan, V. Validation of a novel point-of-care ultrasound method to assess diaphragmatic excursion. Reg. Anesth. Pain Med. 2023. [Google Scholar] [CrossRef]
- Dubé, B.P.; Dres, M.; Mayaux, J.; Demiri, S.; Similowski, T.; Demoule, A. Ultrasound evaluation of diaphragm function in mechanically ventilated patients: Comparison to phrenic stimulation and prognostic implications. Thorax 2017, 72, 811–818. [Google Scholar] [CrossRef] [PubMed]
- Zambon, M.; Beccaria, P.; Matsuno, J.; Gemma, M.; Frati, E.; Colombo, S.; Cabrini, L.; Landoni, G.; Zangrillo, A. Mechanical Ventilation and Diaphragmatic Atrophy in Critically Ill Patients: An Ultrasound Study. Crit. Care Med. 2016, 44, 1347–1352. [Google Scholar] [CrossRef]
- Nakanishi, N.; Oto, J.; Ueno, Y.; Nakataki, E.; Itagaki, T.; Nishimura, M. Change in diaphragm and intercostal muscle thickness in mechanically ventilated patients: A prospective observational ultrasonography study. J. Intensive Care 2019, 7, 56. [Google Scholar] [CrossRef]
- Cammarota, G.; Sguazzotti, I.; Zanoni, M.; Messina, A.; Colombo, D.; Vignazia, G.L.; Vetrugno, L.; Garofalo, E.; Bruni, A.; Navalesi, P.; et al. Diaphragmatic Ultrasound Assessment in Subjects With Acute Hypercapnic Respiratory Failure Admitted to the Emergency Department. Respir. Care 2019, 64, 1469–1477. [Google Scholar] [CrossRef]
- Dos Santos Yamaguti, W.P.; Paulin, E.; Shibao, S.; Chammas, M.C.; Salge, J.M.; Ribeiro, M.; Cukier, A.; Carvalho, C.R.F. Air trapping: The major factor limiting diaphragm mobility in chronic obstructive pulmonary disease patients. Respirology 2008, 13, 138–144. [Google Scholar] [CrossRef] [PubMed]
- Schepens, T.; Dres, M.; Heunks, L.; Goligher, E.C. Diaphragm-protective mechanical ventilation. Curr Opin. Crit. Care 2019, 25, 77–85. [Google Scholar] [CrossRef]
- Vivier, E.; Dessap, A.M.; Dimassi, S.; Vargas, F.; Lyazidi, A.; Thille, A.W.; Brochard, L. Diaphragm ultrasonography to estimate the work of breathing during non-invasive ventilation. Intensive Care Med. 2012, 38, 796–803. [Google Scholar] [CrossRef]
- Umbrello, M.; Formenti, P.; Longhi, D.; Galimberti, A.; Piva, I.; Pezzi, A.; Mistraletti, G.; Marini, J.J.; Iapichino, G. Diaphragm ultrasound as indicator of respiratory effort in critically ill patients undergoing assisted mechanical ventilation: A pilot clinical study. Crit. Care 2015, 19, 161. [Google Scholar] [CrossRef]
- Oppersma, E.; Hatam, N.; Doorduin, J.; van der Hoeven, J.G.; Marx, G.; Goetzenich, A.; Fritsch, S.; Heunks, L.M.A.; Bruells, C.S. Functional assessment of the diaphragm by speckle tracking ultrasound during inspiratory loading. J. Appl. Physiol. 2017, 123, 1063–1070. [Google Scholar] [CrossRef]
- Poulard, T.; Bachasson, D.; Fossé, Q.; Niérat, M.-C.; Hogrel, J.-Y.; Demoule, A.; Gennisson, J.-L.; Dres, M. Poor Correlation between Diaphragm Thickening Fraction and Transdiaphragmatic Pressure in Mechanically Ventilated Patients and Healthy Subjects. Anesthesiology 2022, 136, 162–175. [Google Scholar] [CrossRef]
- De Troyer, A.; Boriek, A.M. Mechanics of the respiratory muscles. Compr. Physiol. 2011, 1, 1273–1300. [Google Scholar] [CrossRef]
- Spadaro, S.; Grasso, S.; Mauri, T.; Corte, F.D.; Alvisi, V.; Ragazzi, R.; Cricca, V.; Biondi, G.; Di Mussi, R.; Marangoni, E.; et al. Can diaphragmatic ultrasonography performed during the T-tube trial predict weaning failure? The role of diaphragmatic rapid shallow breathing index. Crit. Care 2016, 20, 305. [Google Scholar] [CrossRef] [PubMed]
- Palkar, A.; Narasimhan, M.; Greenberg, H.; Singh, K.; Koenig, S.; Mayo, P.; Gottesman, E. Diaphragm Excursion-Time Index: A New Parameter Using Ultrasonography to Predict Extubation Outcome. Chest 2018, 153, 1213–1220. [Google Scholar] [CrossRef]
- Vivier, E.; Muller, M.; Putegnat, J.B.; Steyer, J.; Barrau, S.; Boissier, F.; Bourdin, G.; Mekontso-Dessap, A.; Levrat, A.; Pommier, C.; et al. Inability of Diaphragm Ultrasound to Predict Extubation Failure: A Multicenter Study. Chest 2019, 155, 1131–1139. [Google Scholar] [CrossRef]
- Dres, M.; Goligher, E.C.; Heunks, L.M.A.; Brochard, L.J. Critical illness-associated diaphragm weakness. Intensive Care Med. 2017, 43, 1441–1452. [Google Scholar] [CrossRef] [PubMed]
- Jung, B.; Moury, P.H.; Mahul, M.; de Jong, A.; Galia, F.; Prades, A.; Albaladejo, P.; Chanques, G.; Molinari, N.; Jaber, S. Diaphragmatic dysfunction in patients with ICU-acquired weakness and its impact on extubation failure. Intensive Care Med. 2016, 42, 853–861. [Google Scholar] [CrossRef] [PubMed]
- Dres, M.; Demoule, A. Diaphragm dysfunction during weaning from mechanical ventilation: An underestimated phenomenon with clinical implications. Crit. Care 2018, 22, 73. [Google Scholar] [CrossRef]
- Mayo, P.; Volpicelli, G.; Lerolle, N.; Schreiber, A.; Doelken, P.; Vieillard-Baron, A. Ultrasonography evaluation during the weaning process: The heart, the diaphragm, the pleura and the lung. Intensive Care Med. 2016, 42, 1107–1117. [Google Scholar] [CrossRef]
- Coiffard, B.; Riegler, S.; Sklar, M.C.; Dres, M.; Vorona, S.; Reid, W.D.; Brochard, L.J.; Ferguson, N.D.; Goligher, E.C. Diaphragm echodensity in mechanically ventilated patients: A description of technique and outcomes. Crit. Care 2021, 25, 64. [Google Scholar] [CrossRef] [PubMed]
- Goutman, S.A.; Hamilton, J.D.; Swihart, B.; Foerster, B.; Feldman, E.L.; Rubin, J.M. Speckle tracking as a method to measure hemidiaphragm excursion. Muscle Nerve 2017, 55, 125–127. [Google Scholar] [CrossRef] [PubMed]
- Bachasson, D.; Dres, M.; Niérat, M.-C.; Gennisson, J.-L.; Hogrel, J.-Y.; Doorduin, J.; Similowski, T. Diaphragm shear modulus reflects transdiaphragmatic pressure during isovolumetric inspiratory efforts and ventilation against inspiratory loading. J. Appl. Physiol. 2019, 126, 699–707. [Google Scholar] [CrossRef] [PubMed]
| Parameter | Reference Value | Abnormal Values ※ | Cutoff Value Related to Outcome | References | |
|---|---|---|---|---|---|
| Healthy individual | End-expiratory thickness (mm) | male: 1.9 ± 0.4 | male: <1.7 | [34] | |
| female: 1.4 ± 0.3 | female: <1.3 | ||||
| TFdi | 37 ± 9% | <20% | [36] | ||
| 80 ± 50% | <20% | [37] | |||
| (maximal breathing) | |||||
| Excursion (mm) | male: 18 ± 3 | male: <10 | [35] | ||
| female: 16 ± 3 | female: <9 | ||||
| ICU patient | End-expiratory thickness (mm) | <1.7 | [29] | ||
| TFdi | <30~36% | [29,30,31] | |||
| Excursion (mm) | <10~14 <25 (maximal breathing) | [3,32,33] | |||
| Anatomy and physiology |
|
|
|
|
|
※ No consensus was achieved
|
| Ventilator impact |
|
|
|
| Transducer settings and technique |
Excursion
|
Thickness
|
Both
|
| Learning and expertise |
|
|
|
| Daily practice |
Skills necessary in daily practice
|
Useful indications
|
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Itagaki, T.; Akimoto, Y.; Takashima, T.; Oto, J. Ultrasonographic Assessment of the Diaphragm. Diagnostics 2024, 14, 1481. https://doi.org/10.3390/diagnostics14141481
Itagaki T, Akimoto Y, Takashima T, Oto J. Ultrasonographic Assessment of the Diaphragm. Diagnostics. 2024; 14(14):1481. https://doi.org/10.3390/diagnostics14141481
Chicago/Turabian StyleItagaki, Taiga, Yusuke Akimoto, Takuya Takashima, and Jun Oto. 2024. "Ultrasonographic Assessment of the Diaphragm" Diagnostics 14, no. 14: 1481. https://doi.org/10.3390/diagnostics14141481
APA StyleItagaki, T., Akimoto, Y., Takashima, T., & Oto, J. (2024). Ultrasonographic Assessment of the Diaphragm. Diagnostics, 14(14), 1481. https://doi.org/10.3390/diagnostics14141481






