Validation of the Measuring Protocol for the Infraspinatus Muscle with M-Mode Ultrasound in Asymptomatic Subjects. Intra- and Inter-examiner Reliability Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Ethical Considerations
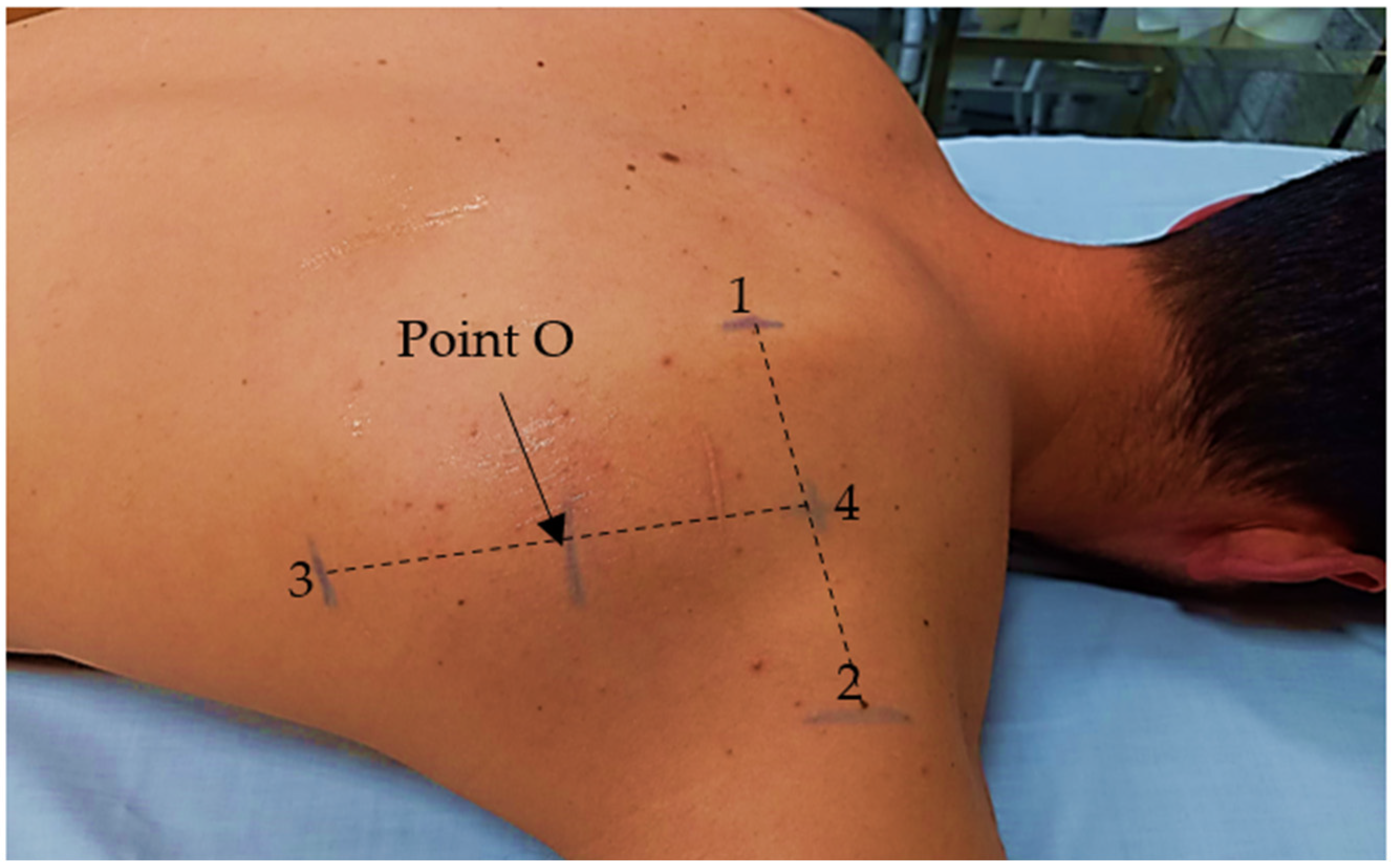
2.2. Data Collection and Analysis
2.3. Statistical Analysis
3. Results
- Negligible in MVIC vs. Gender, MVIC vs. Height, Relaxation velocity vs. BMI, Relaxation velocity vs. Weight, Thickness at rest vs. Age, Thickness at rest vs. Gender, Thickness in contraction vs. Gender and Thickness in contraction vs. Height comparisons.
- Low in Activation velocity vs. Age, Activation velocity vs. BMI, Activation velocity vs. Weight, Activation velocity vs. Work activity, MVIC vs. Age, MVIC vs. BMI, MVIC vs. Weight, Relaxation velocity vs. Age, Relaxation velocity vs. Work activity, Thickness at rest vs. BMI, Thickness at rest vs. Height, Thickness at rest vs. Weight, Thickness in contraction vs. Age, Thickness in contraction vs. BMI, Thickness in contraction vs. Dominant upper limb, Thickness in contraction vs. Weight and Thickness in contraction vs. Work activity.
- Moderate in the comparison of MVIC vs. Dominant upper limb.
- There is neither a high nor a very-high correlation (Table S1 (Supplementary Material)).
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Acknowledgments
Conflicts of Interest
References
- Fernández-Carnero, S.; Calvo-Lobo, C.; Garrido-Marin, A.; Arias-Buría, J.L. 2nd Rehabilitative Ultrasound Imaging Symposium in Physiotherapy—Madrid, Spain, 3–5 June 2016. Br. J. Sports Med. 2018, 52, A1–A6. [Google Scholar]
- Whittaker, J.L.; Ellis, R.; Hodges, P.W.; Osullivan, C.; Hides, J.; Carnero, S.F.; Arias-Buria, J.L.; Teyhen, D.S.; Stokes, M.J. Imaging with ultrasound in physical therapy: What is the PT’s scope of practice? A competency-based educational model and training recommendations. Br. J. Sports Med. 2019, 53, 1447–1453. [Google Scholar] [CrossRef]
- Vasseljen, O.; Fladmark, A.M.; Westad, C.; Torp, H.G. Onset in abdominal muscles recorded simultaneously by ultrasound imaging and intramuscular electromyography. J. Electromyogr. Kinesiol. 2009, 19, e23–e31. [Google Scholar] [CrossRef]
- Vasseljen, O.; Dahl, H.H.; Mork, P.J.; Torp, H.G. Muscle activity onset in the lumbar multifidus muscle recorded simultaneously by ultrasound imaging and intramuscular electromyography. Clin. Biomech. 2006, 21, 905–913. [Google Scholar] [CrossRef]
- Dieterich, A.; Petzke, F.; Pickard, C.; Davey, P.; Falla, D. Differentiation of gluteus medius and minimus activity in weight bearing and non-weight bearing exercises by M-mode ultrasound imaging. Man. Ther. 2015, 20, 715–722. [Google Scholar] [CrossRef]
- Romero-Morales, C.; Calvo-Lobo, C.; Navarro-Flores, E.; Mazoteras-Pardo, V.; García-Bermejo, P.; López-López, D.; Martínez-Jiménez, E.M.; De-la-Cruz-Torres, B. M-Mode Ultrasound Examination of Soleus Muscle in Healthy Subjects: Intra- and Inter-Rater Reliability Study. Healthcare 2020, 8, 555. [Google Scholar] [CrossRef]
- Dieterich, A.V.; Pickard, C.M.; Deshon, L.E.; Strauss, G.R.; Gibson, W.; Davey, P.; McKay, J. M-mode ultrasound used to detect the onset of deep muscle activity. J. Electromyogr. Kinesiol. 2015, 25, 224–231. [Google Scholar] [CrossRef]
- Scarlata, S.; Mancini, D.; Laudisio, A.; Raffaele, A.I. Reproducibility of diaphragmatic thickness measured by M-mode ultrasonography in healthy volunteers. Respir. Physiol. Neurobiol. 2018, 260, 58–62. [Google Scholar] [CrossRef] [PubMed]
- O’Sullivan, C.; Bentman, S.; Bennett, K.; Stokes, M. Rehabilitative Ultrasound Imaging of the Lower Trapezius Muscle: Technical Description and Reliability. J. Orthop. Sports Phys. Ther. 2007, 37, 620–626. [Google Scholar] [CrossRef]
- Koppenhaver, S.; Harris, D.; Harris, A.; O’Connor, E.; Dummar, M.; Croy, T.; Walker, M.; Flynn, T. The reliability of rehabilitative ultrasound imaging in the measurement of infraspinatus muscle function in the symptomatic and asymptomatic shoulders of patients with unilateral shoulder impingement syndrome. Int. J. Sports Phys. Ther. 2015, 10, 128–135. [Google Scholar]
- Deshon, L.; Strauss, G.R.; McKay, J.; Pickard, C.M. M-Mode Ultrasound Reveals Earlier Gluteus Minimus Activity in Individuals With Chronic Hip Pain During a Step-down Task. J. Orthop. Sports Phys. Ther. 2016, 46, 277–285. [Google Scholar] [CrossRef]
- Diaz Sánchez, S.; Conangla Ferrín, L.; Sánchez Barrancos, I.M.; Pujol Salud, J.; Tarrazo Suárez, J.A.; Morales Cano, J.M. Utilidad y fiabilidad de la ecografía clínica en Medicina Familiar: Ecocardioscopia y ecografía pulmonar. Aten. Primaria 2019, 51, 172–183. [Google Scholar] [CrossRef]
- Wilk, K.E.; Arrigo, C.A.; Andrews, J.R. Current Concepts: The Stabilizing Structures of the Glenohumeral Joint. J. Orthop. Sports Phys. Ther. 1997, 25, 364–379. [Google Scholar] [CrossRef]
- Bitter, N.L.; Clisby, E.F.; Jones, M.A.; Magarey, M.E.; Jaberzadeh, S.; Sandow, M.J. Relative contributions of infraspinatus and deltoid during external rotation in healthy shoulders. J. Shoulder Elb. Surg. 2007, 16, 563–568. [Google Scholar] [CrossRef]
- Yu, I.-Y.; Choo, Y.-K.; Kim, M.-H.; Oh, J.-S. The effects of pressure biofeedback training on infraspinatus muscle activity and muscle thickness. J. Electromyogr. Kinesiol. 2018, 39, 81–88. [Google Scholar] [CrossRef]
- Yu, I.-Y.; Lee, D.-K.; Kang, M.-J.; Oh, J.-S. Effects of 3 Infraspinatus Muscle Strengthening Exercises on Isokinetic Peak Torque and Muscle Activity. J. Sport Rehabilitation 2019, 28, 229–235. [Google Scholar] [CrossRef] [PubMed]
- Yu, I.-Y.; Kim, S.-Y.; Kang, M.-H. Strategies for controlling axial shoulder rotation change shoulder muscle activity during external rotation exercises. J. Shoulder Elb. Surg. 2020, 30, 1230–1237. [Google Scholar] [CrossRef] [PubMed]
- Delaney, S.; Worsley, P.; Warner, M.; Taylor, M.; Stokes, M. Assessing contractile ability of the quadriceps muscle using ultrasound imaging. Muscle Nerve 2010, 42, 530–538. [Google Scholar] [CrossRef] [PubMed]
- Henneman, E.; Somjen, G.; Carpenter, D.O. Functional significance of cell size in spinal motoneurons. J. Neurophysiol. 1965, 28, 560–580. [Google Scholar] [CrossRef] [PubMed]
- Hug, F.; Msc, L.L.; Nordez, A. Electromechanical delay measured during a voluntary contraction should be interpreted with caution. Muscle Nerve 2011, 44, 838. [Google Scholar] [CrossRef] [PubMed]
- Holtermann, A.; Roeleveld, K.; Karlsson, J.S. Inhomogeneities in muscle activation reveal motor unit recruitment. J. Electromyogr. Kinesiol. 2005, 15, 131–137. [Google Scholar] [CrossRef] [PubMed]
- Wakeling, J.M. The recruitment of different compartments within a muscle depends on the mechanics of the movement. Biol. Lett. 2008, 5, 30–34. [Google Scholar] [CrossRef] [PubMed]
- Kuwahara, Y.; Yuri, T.; Fujii, H.; Kiyoshige, Y. Functions of the subregions of the infraspinatus during lateral rotation. Surg. Radiol. Anat. 2017, 39, 1331–1336. [Google Scholar] [CrossRef]
- Hodson-Tole, E.F.; Loram, I.D.; Vieira, T.M. Myoelectric activity along human gastrocnemius medialis: Different spatial distributions of postural and electrically elicited surface potentials. J. Electromyogr. Kinesiol. 2013, 23, 43–50. [Google Scholar] [CrossRef]
- Vicente-Herrero, M.; García, L.C.; González, Á.L.; de la Torre, M.R.I. El hombro y sus patologías en medicina del trabajo. SEMERGEN-Med. Fam. 2009, 35, 197–202. [Google Scholar] [CrossRef]
- Bossuyt, P.M.; Reitsma, J.B.; Bruns, D.E.; Gatsonis, C.A.; Glasziou, P.P.; Irwig, L.; Lijmer, J.G.; Moher, D.; Rennie, D.; de Vet, H.C.W.; et al. STARD 2015: An Updated List of Essential Items for Reporting Diagnostic Accuracy Studies. Clin. Chem. 2015, 61, 1446–1452. [Google Scholar] [CrossRef]
- Broilo, C.; Schuster, R.C.; Dhein, W. Análise eletromiográfica de músculos do complexo do ombro durante exercícios de rotação externa com faixa elástica. Fisioter. Pesqui. 2019, 26, 329–336. [Google Scholar] [CrossRef]
- Kim, K.; Hwang, H.; Kim, S.; Lee, J.; Jeong, W.K. Can Shoulder Muscle Activity Be Evaluated With Ultrasound Shear Wave Elastography? Clin. Orthop. Relat. Res. 2018, 476, 1276–1283. [Google Scholar] [CrossRef]
- World Medical Association. World Medical Association Declaration of Helsinki: Ethical Principles for Medical Research Involving Human Subjects. JAMA J. Am. Med. Assoc. 2013, 310, 2191–2194. [Google Scholar] [CrossRef]
- Ehsani, F.; Salavati, M.; Arab, A.; Dolati, M. Ultrasound imaging transducer motion during standing postural tasks with and without using transducer fixator. Musculoskelet. Sci. Pract. 2017, 32, 57–63. [Google Scholar] [CrossRef]
- Park, J.-H.; Chung, S.W.; Lee, S.-J.; Lee, J.-W.; Oh, K.-S. Evaluation of the Electromyographic Amplitude-to-Work Ratio in the Infraspinatus Muscle During External Shoulder Rotation Exercises: A Comparison of Concentric Isotonic and Isokinetic Exercises. Orthop. J. Sports Med. 2020, 8, 2325967120932459. [Google Scholar] [CrossRef] [PubMed]
- Koo, T.K.; Li, M.Y. A Guideline of Selecting and Reporting Intraclass Correlation Coefficients for Reliability Research. J. Chiropr. Med. 2016, 15, 155–163. [Google Scholar] [CrossRef] [PubMed]
- Mukaka, M.M. Statistics corner: A guide to appropriate use of correlation coefficient in medical research. Malawi Med. J. 2012, 24, 69–71. [Google Scholar]
- Juul-Kristensen, B.; Bojsen-Møller, F.; Holst, E.; Ekdahl, C. Comparison of muscle sizes and moment arms of two rotator cuff muscles measured by Ultrasonography and Magnetic Resonance Imaging. Eur. J. Ultrasound 2000, 11, 161–173. [Google Scholar] [CrossRef]
- Wu, W.T.; Lin, J.A.; Chen, L.R.; Sun, W.Z.; Lin, C.P.; Özçakar, L.; Chang, K.V. Ultrasound Imaging, Guidance, and Treatment for Shoulder-related Pain Syndrome: A Bibliometric Analysis. Pain Physician 2022, 25, E1433–E1445. [Google Scholar]
- Özçakar, L.; Kara, M.; Chang, K.V.; Çarl, A.B.; Akkaya, N.; Tok, F.; Chen, W.-S.; Wang, T.-G.; Tekin, L.; Ulaşl, A.M.; et al. Nineteen reasons why physiatrists should do musculoskeletal ultrasound: EURO-MUSCULUS/USPRM recommendations. Am. J. Phys. Med. Rehabil. 2015, 94, 45. [Google Scholar] [CrossRef]
- Ma, A.J.T.; Tenan, M.S.; Haynes, C.A. Differences in muscle contraction onset as determined by ultrasound and electromyography. Muscle Nerve 2018, 59, 494–500. [Google Scholar] [CrossRef]


| n | 60 | |
| Gender, n (%) | Female | 29 (48.3) |
| Male | 31 (51.7) | |
| Age | 26.35 ± 11.60 | |
| Weight (kg) | 66.93 ± 11.15 | |
| Height (m) | 1.71 ± 0.09 | |
| BMI | 22.75 ± 2.84 | |
| Neck pain upper limb or shoulder, n (%) | No | 60 (100.0) |
| Work activity, n (%) | Student | 38 (63.3) |
| Worker | 22 (36.7) | |
| Sport activity, n (%) | No | 10 (16.7) |
| Yes | 50 (83.3) | |
| Dominant upper limb, n (%) | Left | 6 (10.0) |
| Right | 54 (90.0) | |
| Observed upper limb, n (%) | Left | 28 (46.7) |
| Right | 32 (53.3) |
| Observer 1 | Observer 2 | |||||||
|---|---|---|---|---|---|---|---|---|
| ICC (95%CI) | Average Measurement (95% CI) | SEM (95% CI) | MDC | ICC (95% CI) | Average Measurement (95% CI) | SEM (95% CI) | MDC | |
| Thickness at rest | 0.833 (0.728, 0.907) | 2.053 (1.87, 2.236) | 0.182 (0.138, 0.226) | 0.505 | 0.889 (0.847, 0.923) | 2.06 (1.932, 2.189) | 0.173 (0.149, 0.196) | 0.479 |
| Thickness in contraction | 0.861 (0.772, 0.923) | 2.399 (2.205, 2.593) | 0.176 (0.131, 0.221) | 0.488 | 0.933 (0.906, 0.954) | 2.421 (2.287, 2.556) | 0.137 (0.116, 0.158) | 0.380 |
| MVIC | 0.875 (0.794, 0.931) | 7.545 (6.103, 8.988) | 1.244 (0.883, 1.605) | 3.448 | 0.813 (0.745, 0.867) | 6.929 (6.039, 7.818) | 1.593 (1.321, 1.864) | 4.414 |
| Activation velocity | 0.547 (0.352, 0.72) | 0.382 (0.241, 0.523) | 0.273 (0.187, 0.359) | 0.758 | 0.499 (0.373, 0.619) | 0.51 (0.423, 0.597) | 0.292 (0.236, 0.348) | 0.809 |
| Relaxation velocity | 0.457 (0.252, 0.654) | 0.514 (0.278, 0.75) | 0.519 (0.331, 0.707) | 1.438 | 0.606 (0.494, 0.708) | 0.517 (0.442, 0.593) | 0.211 (0.182, 0.241) | 0.586 |
| ICC (95% CI) | Average Measurement (95% CI) | SEM (95% CI) | MDC | |
|---|---|---|---|---|
| Thickness at rest | 0.797 (0.633, 0.893) | 2.05 (1.873, 2.227) | 0.203 (0.139, 0.267) | 0.563 |
| Thickness in contraction | 0.89 (0.792, 0.943) | 2.399 (2.208, 2.59) | 0.158 (0.111, 0.204) | 0.437 |
| MVIC | 0.84 (0.705, 0.917) | 7.483 (6.042, 8.925) | 1.45 (1.013, 1.888) | 4.020 |
| Activation velocity | 0 (-0.322, 0.329) | 0.486 (0.331, 0.641) | 0.329 (0.213, 0.444) | 0.911 |
| Relaxation velocity | 0.474 (0.168, 0.698) | 0.513 (0.347, 0.678) | 0.338 (0.222, 0.455) | 0.938 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ortega-Santamaría, M.; Torralbo-Álvarez-Novoa, M.-E.; Cuenca-Zaldívar, J.-N.; Naranjo-Cinto, F.; Fernández-Carnero, S.; Pecos-Martín, D. Validation of the Measuring Protocol for the Infraspinatus Muscle with M-Mode Ultrasound in Asymptomatic Subjects. Intra- and Inter-examiner Reliability Study. Diagnostics 2023, 13, 582. https://doi.org/10.3390/diagnostics13040582
Ortega-Santamaría M, Torralbo-Álvarez-Novoa M-E, Cuenca-Zaldívar J-N, Naranjo-Cinto F, Fernández-Carnero S, Pecos-Martín D. Validation of the Measuring Protocol for the Infraspinatus Muscle with M-Mode Ultrasound in Asymptomatic Subjects. Intra- and Inter-examiner Reliability Study. Diagnostics. 2023; 13(4):582. https://doi.org/10.3390/diagnostics13040582
Chicago/Turabian StyleOrtega-Santamaría, Marina, María-Eugenia Torralbo-Álvarez-Novoa, Juan-Nicolás Cuenca-Zaldívar, Fermin Naranjo-Cinto, Samuel Fernández-Carnero, and Daniel Pecos-Martín. 2023. "Validation of the Measuring Protocol for the Infraspinatus Muscle with M-Mode Ultrasound in Asymptomatic Subjects. Intra- and Inter-examiner Reliability Study" Diagnostics 13, no. 4: 582. https://doi.org/10.3390/diagnostics13040582
APA StyleOrtega-Santamaría, M., Torralbo-Álvarez-Novoa, M.-E., Cuenca-Zaldívar, J.-N., Naranjo-Cinto, F., Fernández-Carnero, S., & Pecos-Martín, D. (2023). Validation of the Measuring Protocol for the Infraspinatus Muscle with M-Mode Ultrasound in Asymptomatic Subjects. Intra- and Inter-examiner Reliability Study. Diagnostics, 13(4), 582. https://doi.org/10.3390/diagnostics13040582








