The Role of Early Revascularization and Biomarkers in the Management of Diabetic Foot Ulcers: A Single Center Experience
Abstract
1. Introduction
2. Materials and Methods
2.1. Laboratory Parameters and Biomarkers
2.2. Technique
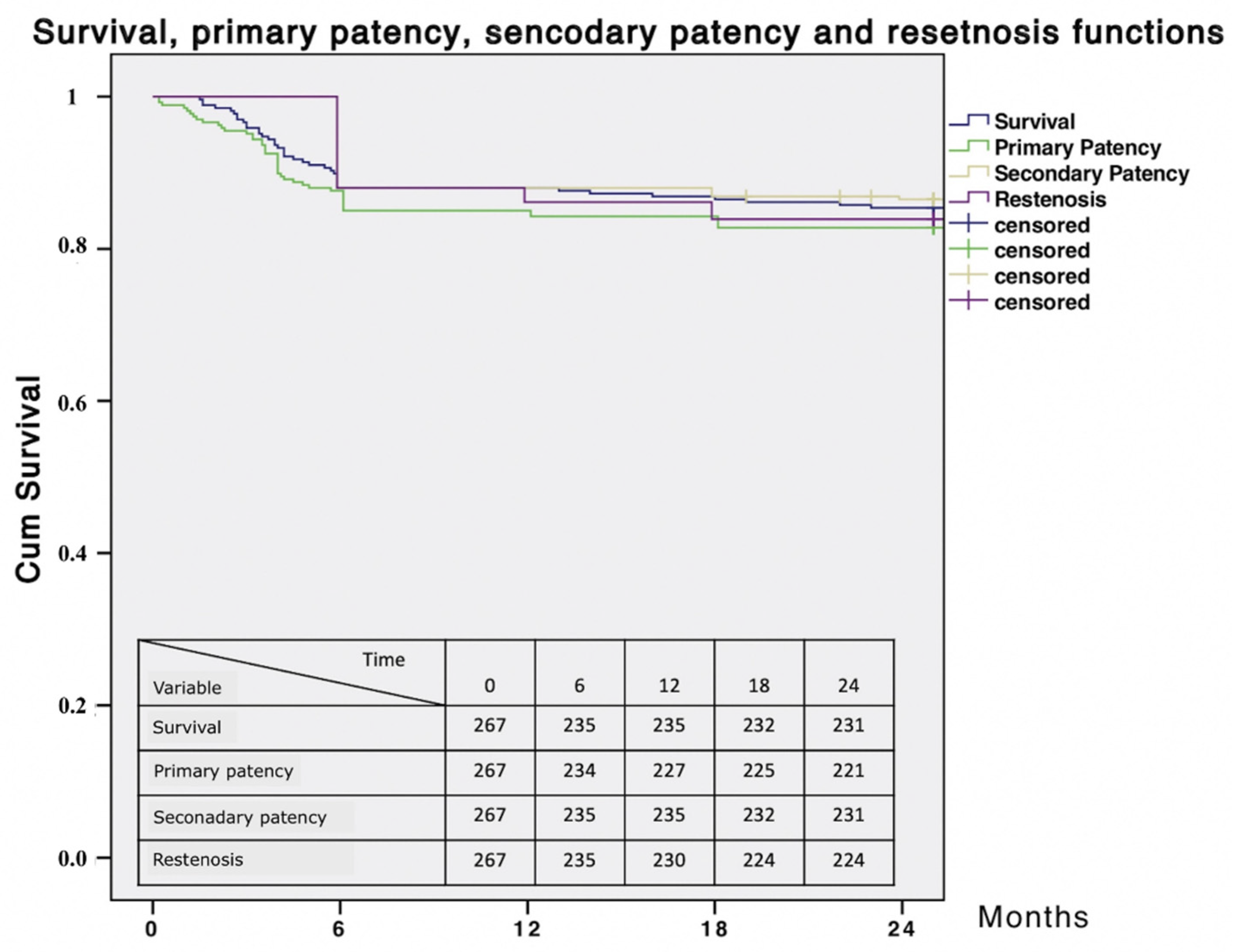
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Primadhi, R.A.; Herman, H. Diabetic foot: Which one comes first, the ulcer or the contracture? World J. Orthop. 2021, 12, 61–68. [Google Scholar] [CrossRef] [PubMed]
- Pérez-Panero, A.J.; Ruiz-Muñoz, M.; Cuesta-Vargas, A.I.; Gónzalez-Sánchez, M. Prevention, assessment, diagnosis and management of diabetic foot based on clinical practice guidelines: A systematic review. Medicine 2019, 98, e16877. [Google Scholar] [CrossRef] [PubMed]
- Dinoto, E.; Pecoraro, F.; Mirabella, D.; Ferlito, F.; Farina, A.; Lo Biundo, N.; Orlando-Conti, P.; Bajardi, G. A Single-Center Experience on Below-The-Knee Endovascular Treatment in Diabetic Patients. Transl. Med. UniSa 2020, 21, 21–23. [Google Scholar] [PubMed]
- Sinwar, P.D. The diabetic foot management—recent advance. Int. J. Surg. 2015, 15, 27–30. [Google Scholar] [CrossRef]
- Dinoto, E.; Pecoraro, F.; Cutrupi, A.; Bracale, U.M.; Panagrosso, M.; Bajardi, G. Single staged hybrid approach for multilevel aortic-iliac-femoral-popliteal disease. Int. J. Surg. Case Rep. 2020, 77S, S166–S169. [Google Scholar] [CrossRef] [PubMed]
- Chaudhary, N.; Huda, F.; Roshan, R.; Basu, S.; Rajput, D.; Singh, S.K. Lower Limb Amputation Rates in Patients With Diabetes and an Infected Foot Ulcer: A Prospective Observational Study. Wound Manag. Prev. 2021, 67, 22–30. [Google Scholar] [CrossRef]
- Johannesson, A.; Larsson, G.-U.; Ramstrand, N.; Turkiewicz, A.; Wiréhn, A.-B.; Atroshi, I. Incidence of lower-limb amputation in the diabetic and nondiabetic general population: A 10-year population-based cohort study of initial unilateral and contralateral amputations and reamputations. Diabetes Care 2009, 32, 275–280. [Google Scholar] [CrossRef] [PubMed]
- Khaleghi, M.; Singletary, L.A.; Kondragunta, V.; Bailey, K.R.; Turner, S.T.; Mosley, T.H., Jr.; Kullo, I.J. Haemostatic markers are associated with meas- ures of vascular disease in adults with hypertension. J. Hum. Hypertens. 2009, 23, 530–537. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Murabito, J.M.; Keyes, M.J.; Guo, C.Y.; Keaney, J.F., Jr.; Vasan, R.S.; D’Agostino, R.B., Sr.; Benjamin, E.J. Cross-sectional relations of multiple inflammatory biomarkers to peripheral arterial disease: The Framingham Offspring Study. Atherosclerosis 2009, 203, 509–514. [Google Scholar] [CrossRef] [PubMed]
- Cho, N.R.; Yu, Y.; Oh, C.K.; Ko, D.S.; Myung, K.; Lee, Y.; Na, H.S.; Kim, Y.H. Neuropeptide Y: A potential theranostic biomarker for diabetic peripheral neuropathy in patients with type-2 diabetes. Ther. Adv. Chronic Dis. 2021, 12, 20406223211041936. [Google Scholar] [CrossRef] [PubMed]
- von Elm, E.; Altman, D.G.; Egger, M.; Pocock, S.J.; Gøtzsche, P.C.; Vandenbroucke, J.P.; STROBE Initiative. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: Guidelines for reporting observational studies. Epidemiology 2007, 18, 800–804. [Google Scholar] [CrossRef] [PubMed]
- Levey, A.S.; Stevens, L.A.; Schmid, C.H.; Zhang, Y.; Castro, A.F., III; Feldman, H.I.; Kusek, J.W.; Eggers, P.; van Lente, F.; Greene, T.; et al. A new equation to estimate glomerular filtration rate. Ann. Intern. Med. 2009, 150, 604–612. [Google Scholar] [CrossRef] [PubMed]
- Norgren, L.; Hiatt, W.R.; Dormandy, J.A.; Nehler, M.R.; Harris, K.A.; Fowkes, F.G.; TASC II Working Group. Inter-Society Consensus for the Management of Peripheral Arterial Disease (TASC II). J. Vasc. Surg. 2007, 45, S5–S67. [Google Scholar] [CrossRef] [PubMed]
- Pecoraro, F.; Dinoto, E.; Pakeliani, D.; Mirabella, D.; Ferlito, F.; Bajardi, G. Efficacy and one-year outcomes of Luminor® paclitaxel-coated drug-eluting balloon in the treatment of popliteal artery atherosclerosis lesions. Ann. Vasc. Surg. 2021, 76, 370–377. [Google Scholar] [CrossRef]
- Pecoraro, F.; Pakeliani, D.; Bruno, S.; Dinoto, E.; Ferlito, F.; Mirabella, D.; Lachat, M.; Cudia, B.; Bajardi, G. Simultaneous Hybrid Treatment of Multilevel Peripheral Arterial Disease in Patients with Chronic Limb-Threatening Ischemia. J. Clin. Med. 2021, 10, 2865. [Google Scholar] [CrossRef] [PubMed]
- Balaz, P.; Rokosny, S.; Bafrnec, J.; Björck, M. The role of hybrid procedures in the management of peripheral vascular disease. Scand. J. Surg. 2012, 101, 232–237. [Google Scholar] [CrossRef] [PubMed]
- Dinoto, E.; Ferlito, F.; Urso, F.; Pakeliani, D.; Bajardi, G.; Pecoraro, F. Mechanical rotational thrombectomy in long femoropopliteal artery and stent occlusion in COVID-19 patient: Case report. Int. J. Surg. Case Rep. 2021, 84, 106133. [Google Scholar] [CrossRef] [PubMed]
- Taurino, M.; Persiani, F.; Ficarelli, R.; Filippi, F.; Dito, R.; Rizzo, L. The Role of the Profundoplasty in the Modern Management of Patient with Peripheral Vascular Disease. Ann. Vasc. Surg. 2017, 45, 16–21. [Google Scholar] [CrossRef] [PubMed]
- Khan, M.A.B.; Hashim, M.J.; King, J.K.; Govender, R.D.; Mustafa, H.; Al Kaabi, J. Epidemiology of Type 2 Diabetes—Global Burden of Disease and Forecasted Trends. J. Epidemiol. Glob. Health 2020, 10, 107–111. [Google Scholar] [CrossRef]
- Bracale, U.M.; Ammollo, R.P.; Hussein, E.A.; Hoballah, J.J.; Goeau-Brissonniere, O.; Taurino, M.; Setacci, C.; Pecoraro, F.; Bracale, G.; Collaborators. Managing Peripheral Artery Disease in Diabetic Patients: A Questionnaire Survey from Vascular Centers of the Mediterranean Federation for the Advancing of Vascular Surgery (MeFAVS). Ann. Vasc. Surg. 2020, 64, 239–245. [Google Scholar] [CrossRef] [PubMed]
- Zhang, P.; Lu, J.; Jing, Y.; Tang, S.; Zhu, D.; Bi, Y. Global epidemiology of diabetic foot ulceration: A systematic review and meta-analysis. Ann. Med. 2017, 49, 106. [Google Scholar] [CrossRef] [PubMed]
- Wojtasik-Bakalarz, J.; Ruzsa, Z.; Rakowski, T.; Nyerges, A.; Bartuś, K.; Stanek, A.; Dudek, D.; Surdacki, A.; Kleczyński, P.; Bartuś, S. Impact of Coronary Artery Disease and Diabetes Mellitus on the Long-Term Follow-Up in Patients after Retrograde Recanalization of the Femoropopliteal Arterial Region. J. Diabetes Res. 2019, 2019, 6036359. [Google Scholar] [CrossRef] [PubMed]
- Lepäntalo, M.; Apelqvist, J.; Setacci, C.; Ricco, J.B.; de Donato, G.; Becker, F.; Robert-Ebadi, H.; Cao, P.; Eckstein, H.H.; De Rango, P.; et al. Chapter V: Diabetic foot. Eur. J. Vasc. Endovasc. Surg. 2011, 42, S60–S74. [Google Scholar] [CrossRef]
- Olinic, D.M.; Spinu, M.; Olinic, M.; Homorodean, C.; Tataru, D.A.; Liew, A.; Schernthaner, G.H.; Stanek, A.; Fowkes, G.; Catalano, M. Epidemiology of peripheral artery disease in Europe: VAS Educational Paper. Int. Angiol. 2018, 37, 327–334. [Google Scholar] [CrossRef]
- Ye, Z.; Ali, Z.; Klee, G.G.; Mosley, T.H., Jr.; Kullo, I.J. Associations of candidate biomarkers of vascular disease with the ankle-brachial index and peripheral arterial disease. Am. J. Hypertens. 2013, 26, 495–502. [Google Scholar] [CrossRef] [PubMed]
- Jakubiak, G.K.; Pawlas, N.; Cieślar, G.; Stanek, A. Pathogenesis and Clinical Significance of In-Stent Restenosis in Patients with Diabetes. Int. J. Environ. Res. Public Health 2021, 18, 11970. [Google Scholar] [CrossRef] [PubMed]
- Zhu, X.; Chen, Y.; Xiang, L.; You, T.; Jiao, Y.; Xu, W.; Chen, J. The long-term prognostic significance of high-sensitive C-reactive protein to in-stent restenosis. Medicine 2018, 97, e10679. [Google Scholar] [CrossRef]
- Baktashian, M.; Saffar Soflaei, S.; Kosari, N.; Salehi, M.; Khosravi, A.; Ahmadinejad, M.; Moohebati, M.; Ebrahimi, M.; Rahmani, F.; Khameneh-Bagheri, R.; et al. Association of high level of hs-CRP with in-stent restenosis: A case-control study. Cardiovasc. Revasc. Med. 2019, 20, 583–587. [Google Scholar] [CrossRef] [PubMed]
- Ridker, P.M.; Stampfer, M.J.; Rifai, N. Novel risk factors for systemic atherosclerosis: A comparison of C-reactive protein, fibrinogen, homocysteine, lipoprotein(a), and standard cholesterol screening as predictors of peripheral arterial disease. JAMA 2001, 285, 2481–2485. [Google Scholar] [CrossRef] [PubMed]
- Takahara, M.; Iida, O.; Kohsaka, S.; Soga, Y.; Fujihara, M.; Shinke, T.; Amano, T.; Ikari, Y.; J-EVT and J-PCI Investigators. Diabetes mellitus and other cardiovascular risk factors in lower-extremity peripheral artery disease versus coronary artery disease: An analysis of 1,121,359 cases from the nationwide databases. Cardiovasc. Diabetol. 2019, 18, 155. [Google Scholar] [CrossRef] [PubMed]
- Kaplan, M.; Yavuz, F.; Kaplan, G.I.; Bursa, N.; Vuruşkan, E.; Sucu, M. Elabela as a novel marker: Well-correlated with WIfI amputation risk score in lower extremity arterial disease patients. Anatol. J. Cardiol. 2021, 25, 330–337. [Google Scholar] [CrossRef] [PubMed]
- Passaro, A.; Calzoni, F.; Volpato, S.; Nora, E.D.; Pareschi, P.L.; Zamboni, P.F.; Fellin, R.; Solini, A. Effect of metabolic control on homocysteine levels in type 2 diabetic patients: A 3-year follow-up. J. Intern. Med. 2003, 254, 264–271. [Google Scholar] [CrossRef]
- Flynn, E.R.; Lee, J.; Hutchens, Z.M., Jr.; Chade, A.R.; Maric-Bilkan, C. C-peptide preserves the renal microvascular architecture in the streptozotocin-induced diabetic rat. J. Diabetes Complicat. 2013, 27, 538–547. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Redlich, U.; Xiong, Y.Y.; Pech, M.; Tautenhahn, J.; Halloul, Z.; Lobmann, R.; Adolf, D.; Ricke, J.; Dudeck, O. Superiority of transcutaneous oxygen tension measurements in predicting limb salvage after below-the-knee angioplasty: A prospective trial in diabetic patients with critical limb ischemia. Cardiovasc. Intervent. Radiol. 2011, 34, 271–279. [Google Scholar] [CrossRef]
- Neufang, A.; Dorweiler, B.; Espinola-Klein, C.; Savvidis, S.; Doemland, M.; Schotten, S.; Vahl, C.F. Outcomes of complex femorodistal sequential autologous vein and biologic prosthesis composite bypass grafts. J. Vasc. Surg. 2014, 60, 1543–1553. [Google Scholar] [CrossRef][Green Version]
- Dinoto, E.; Pecoraro, F.; Ferlito, F.; Tortomasi, G.; Mirabella, D.; Bajardi, G. Multilevel diabetic foot revascularization in COVID 19 patient: Case report. Int. J. Surg. Case Rep. 2021, 84, 106132. [Google Scholar] [CrossRef] [PubMed]
- Ghoneim, B.; Elwan, H.; Eldaly, W.; Khairy, H.; Taha, A.; Gad, A. Management of critical lower limb ischemia in endovascular era: Experience from 511 patients. Int. J. Angiol. Off. Publ. Int. Coll. Angiol. Inc. 2014, 23, 197–206. [Google Scholar]
- Dinoto, E.; Ferlito, F.; Urso, F.; Mirabella, D.; Bajardi, G.; Pecoraro, F. Iliac-femoral stent-graft infection after hybrid procedure redo: Case report. Int. J. Surg. Case Rep. 2021, 84, 106096. [Google Scholar] [CrossRef] [PubMed]
- Conte, M.S.; Bradbury, A.W.; Kolh, P.; White, J.V.; Dick, F.; Fitridge, R.; Mills, J.L.; Ricco, J.B.; Suresh, K.R.; Murad, M.H.; et al. Global vascular guidelines on the management of chronic limb-threatening ischemia. J. Vasc. Surg. 2019, 69, 3S–125S.e40. [Google Scholar] [CrossRef] [PubMed]
- Pecoraro, F.; Bajardi, G.; Dinoto, E.; Vitale, G.; Bellisi, M.; Bracale, U.M. Endograft connector technique to treat popliteal artery aneurysm in a morbid obese patient. Vascular 2015, 23, 165–169. [Google Scholar] [CrossRef] [PubMed]
- Hardman, R.L.; Jazaeri, O.; Yi, J.; Smith, M.; Gupta, R. Overview of classification systems in peripheral artery disease. Semin. Intervent. Radiol. 2014, 31, 378–388. [Google Scholar] [CrossRef] [PubMed]
- Bracale, U.M.; Vitale, G.; Bajardi, G.; Narese, D.; Dinoto, E.; Giribono, A.M.; Ferrara, D.; Del Guercio, L.; Midiri, M.; Pecoraro, F. Use of the directional atherectomy for the treatment of femoro-popliteal lesions in patients with critical lower limb ischemia. Transl. Med. UniSa 2016, 15, 42–47. [Google Scholar] [PubMed]
- Aho, P.S.; Venermo, M. Hybrid procedures as a novel technique in the treatment of critical limb ischemia. Scand. J. Surg. 2012, 101, 107–113. [Google Scholar] [CrossRef] [PubMed]
- Stoner, M.C.; Calligaro, K.D.; Chaer, R.A.; Dietzek, A.M.; Farber, A.; Guzman, R.J.; Hamdan, A.D.; Landry, G.J.; Yamaguchi, D.J.; Society for Vascular Surgery. Reporting standards of the Society for Vascular Surgery for endovascular treatment of chronic lower extremity peripheral artery disease. J. Vasc. Surg. 2016, 64, e1–e21. [Google Scholar] [CrossRef]
- Dinoto, E.; Bajardi, G.; La Marca, M.A.; Ferlito, F.; Mirabella, D.; Pecoraro, F. Composite femoro-tibial bypass as alternative solution in complicated revascolarization: Case report. Int. J. Surg. Case Rep. 2021, 84, 106103. [Google Scholar] [CrossRef] [PubMed]
- Dosluoglu, H.H.; Lall, P.; Cherr, G.S.; Harris, L.M.; Dryjski, M.L. Role of simple and complex hybrid revascularization procedures for symptomatic lower extremity occlusive disease. J. Vasc. Surg. 2010, 51, 1425–1435.e1. [Google Scholar] [CrossRef] [PubMed]
- Forbes, T.L.; Harris, K.A. Current status of Canadian vascular surgery training: A survey of program directors. Can. J. Surg. 2005, 48, 311–318. [Google Scholar] [PubMed]
- Chang, R.W.; Goodney, P.P.; Baek, J.H.; Nolan, B.W.; Rzucidlo, E.M.; Powell, R.J. Long-term results of combined common femoral endarterectomy and iliac stenting/stent grafting for occlusive disease. J. Vasc. Surg. 2008, 48, 362–367. [Google Scholar] [CrossRef] [PubMed]
- Setacci, C.; Sirignano, P.; Mazzitelli, G.; Setacci, F.; Messina, G.; Galzerano, G.; de Donato, G. Diabetic foot: Surgical approach in emergency. Int. J. Vasc. Med. 2013, 2013, 296169. [Google Scholar] [CrossRef]


| Categories | Grade | N | % |
|---|---|---|---|
| Diabetes | None | 0 | 0 |
| Not rerquiring insulin | 40 | 15 | |
| Controlled by insulin | 199 | 75 | |
| Type 1 or uncontrolled | 28 | 10 | |
| Tobacco Use | None (>10 years ago) | 70 | 26 |
| Quit 1–10 bears ago | 45 | 17 | |
| Current within last year, <1 package per day | 113 | 42 | |
| Current within last year, >1 package per day | 39 | 15 | |
| Hypertension | None | 15 | 6 |
| Controlled with 1 drug | 66 | 25 | |
| Controlled with 2 drugs | 126 | 47 | |
| Requiring > 2 drugs or uncontrolled | 60 | 22 | |
| Renal Status | Normal | 86 | 32 |
| Evidence of renal disease, GFR > 90 mL/min/1.73 m2 | 77 | 29 | |
| GFR 60–89 mL/min/1.73 m2 | 41 | 15 | |
| GFR 30–59 mL/min/1.73 m2 | 43 | 16 | |
| GFR 15–29 mL/min/1.73 m2 | 5 | 2 | |
| GFR < 15 mL/min/1.73 m2 | 15 | 6 | |
| Cardiac status | Asymptomatic | 87 | 32 |
| Asymptomatic, but with remote myocardial infarction by history (6 months) | 72 | 27 | |
| Stable angina, ejection fraction 25% to 45%, controlled ectopy or asymptomatic arrhythmia, or history of congestive heart failure that is now well compensated | 76 | 28 | |
| Unstable angina, ejection fraction <25%, myocardial infarction ≤6 months | 32 | 12 | |
| Functional status | No impairment | 15 | 6 |
| Impaired, but able to carry out ADL without assistance | 49 | 18 | |
| Needs some assistance to carry out ADL or ambulatory assistance | 116 | 44 | |
| Requiring total assistance for ADL or nonambulatory | 87 | 32 | |
| ADL, Activities of daily living; FEV1, forced expiratory volume in 1 s; GFR, glomerular filtration rate | |||
| Categories | Grade | N | % |
|---|---|---|---|
| Antiplatelet Therpay | None | 64 | 24 |
| Single Agent | 155 | 58 | |
| Dual Therapy | 48 | 18 | |
| Lipid-lowering therapy | On statin and lipid testing within therapeutic range | 187 | 70 |
| On Statin but lipid levels not optimal | 48 | 18 | |
| On high-dose statin or requiring supplemental lipid medications | 15 | 6 | |
| Statin intolerant or patient with familial hypercholesterolemia | 17 | 6 | |
| Anticoagulation | No Hypercoagulable State | 242 | 91 |
| Unknow | 2 | 1 | |
| Low risk Hypercoagulable state | 0 | 0 | |
| High risk Hypercoagulable state | 23 | 8 |
| Categories | Grade | N | % |
|---|---|---|---|
| Rutherford Classification | 3 | 50 | 19 |
| 4 | 78 | 29 | |
| 5 | 110 | 41 | |
| 6 | 29 | 11 | |
| WIfi Classification | Clinical Stage 1 | 34 | 13 |
| Clinical Stage 2 | 29 | 11 | |
| Clinical Stage 3 | 50 | 22 | |
| Clinical Stage 4 | 145 | 54 | |
| TASC Classification | TASC B | 72 | 27 |
| TASC C | 131 | 49 | |
| TASC D | 64 | 24 |
| Variable | Time 0 | 12 Months |
|---|---|---|
| Serum Homocisteine (µmol/L) | 11.7 ± 2.1 | 11.5 ± 1.8 |
| Serum Folate (nmol/L) | 22 ± 6 | 28 ± 5 |
| Plasma Triglycerides (mg/dL) | 183 ± 21 | 151 ± 18 |
| Plasma Cholesterol (mg/dL) | 221 ± 6 | 190 ± 11 |
| LDL-Cholesterol (mg/dL) | 185 ± 6 | 90 ± 6 |
| HDL-Cholesterol (mg/dL) | 10 ± 7 | 23 ± 6 |
| Fasting plasma glucose (mg/dL) | 221 ± 53 | 153 ± 12 |
| HbA1c (%) | 8.4 ± 1.2 | 7.5 ± 1.8 |
| C-peptide (ng/mL) | 1.9 ± 1.2 | 0.9 ± 1.5 |
| Neuropeptide Y (pg/mL) | 2983 ± 88 | 2970 ± 95 |
| Elabela peptide(ng/mL) | 2.9 ± 2.1 | 1.8 ± 1.9 |
| Variable | Time 0 | 12 Months | |
|---|---|---|---|
| Rutherford Classification | |||
| Category 3 | Serum Homocisteine (µmol/L) | 10.7 ± 2.1 | 9.5 ± 0.4 |
| Fasting plasma glucose (mg/dL) | 150 ± 21 | 145 ± 1 | |
| C-peptide (ng/mL) | 1.9 ± 0.5 | 0.9 ± 0.2 | |
| Neuropeptide Y (pg/mL) | 2933 ± 38 | 2930 ± 20 | |
| Elabela peptide(ng/mL) | 2.8 ± 1 | 1.5 ± 1.4 | |
| Category 4 | Serum Homocisteine (µmol/L) | 11.8 ± 2.0 | 11.0 ± 1.2 |
| Fasting plasma glucose (mg/dL) | 185 ± 12 | 154 ± 7 | |
| C-peptide (ng/mL) | 11.8 ± 2.0 | 11.0 ± 1.2 | |
| Neuropeptide Y (pg/mL) | 2.0 ± 0.2 | 0.9 ± 0.5 | |
| Elabela peptide(ng/mL) | 2968 ± 23 | 2945 ± 22 | |
| Category 5 | Serum Homocisteine (µmol/L) | 11.8 ± 2.2 | 11.4 ± 1.7 |
| Fasting plasma glucose (mg/dL) | 191 ± 10 | 161 ± 3 | |
| C-peptide (ng/mL) | 2.3 ± 0.5 | 1.8 ± 0.5 | |
| Neuropeptide Y (pg/mL) | 3001 ± 12 | 2940 ± 44 | |
| Elabela peptide(ng/mL) | 3.3 ± 1.3 | 2.7 ± 0.5 | |
| Category 6 | Serum Homocisteine (µmol/L) | 12.3 ± 2.1 | 12.5 ± 1.7 |
| Fasting plasma glucose (mg/dL) | 205 ± 18 | 210 ± 3 | |
| C-peptide (ng/mL) | 2.4 ± 0.6 | 2.4 ± 0.7 | |
| Neuropeptide Y (pg/mL) | 3003 ± 15 | 3002 ± 41 | |
| Elabela peptide(ng/mL) | 3.5 ± 1.2 | 3.5 ± 0.2 | |
| WIfi Classification | |||
| Clinical Stage 1 | Serum Homocisteine (µmol/L) | 11.6 ± 2.2 | 11.4 ± 1.3 |
| Fasting plasma glucose (mg/dL) | 151 ± 23 | 147 ± 3 | |
| C-peptide (ng/mL) | 1.8 ± 0.5 | 0.8 ± 0.3 | |
| Neuropeptide Y (pg/mL) | 2943 ± 28 | 2935 ± 19 | |
| Elabela peptide (ng/mL) | 2.7 ± 0-9 | 1.6 ± 1.3 | |
| Clinical Stage 2 | Serum Homocisteine (µmol/L) | 11.9 ± 1.1 | 11.2 ± 1.1 |
| Fasting plasma glucose (mg/dL) | 187 ± 9 | 164 ± 3 | |
| C-peptide (ng/mL) | 1.9 ± 0.2 | 1.1 ± 0.4 | |
| Neuropeptide Y (pg/mL) | 2953 ± 32 | 2951 ± 12 | |
| Elabela peptide(ng/mL) | 2.8 ± 1.7 | 2.2 ± 0.2 | |
| Clinical Stage 3 | Serum Homocisteine (µmol/L) | 12.1 ± 1.4 | 11.5 ± 1.3 |
| Fasting plasma glucose (mg/dL) | 188 ± 13 | 169 ± 9 | |
| C-peptide (ng/mL) | 2.2 ± 0.7 | 1.9 ± 0.4 | |
| Neuropeptide Y (pg/mL) | 3014 ± 21 | 2990 ± 24 | |
| Elabela peptide(ng/mL) | 3.1 ± 0.3 | 2.55 ± 0.5 | |
| Clinical Stage 4 | Serum Homocisteine (µmol/L) | 12.7 ± 1.1 | 11.6 ± 2.1 |
| Fasting plasma glucose (mg/dL) | 210 ± 15 | 181 ± 30 | |
| C-peptide (ng/mL) | 2.4 ± 0.6 | 1.9 ± 0.7 | |
| Neuropeptide Y (pg/mL) | 3012 ± 12 | 2980 ± 63 | |
| Elabela peptide(ng/mL) | 3.3 ± 1.0 | 2.8 ± 0.2 |
| Categories | Grade | N | % |
|---|---|---|---|
| Diabetes | None | 0 | 0 |
| Not 12 equiring insulin | 0 | 0 | |
| Controlled by insulin | 16 | 100 | |
| Type 1 or uncontrolled | 0 | 0 | |
| Tobacco Use | None (>10 years ago) | 0 | 0 |
| Quit 1–10 bears ago | 2 | 12 | |
| Current within last year, <1 package per day | 8 | 50 | |
| Current within last year, > 1 package per day | 6 | 38 | |
| Hypertension | None | 0 | 0 |
| Controlled with 1 drug | 10 | 62 | |
| Controlled with 2 drugs | 5 | 32 | |
| Requiring > 2 drugs or uncontrolled | 1 | 6 | |
| Renal Status | Normal | 4 | 26 |
| Evidence of renal disease, GFR > 90 mL/min/1.73 m2 | 3 | 19 | |
| GFR 60–89 mL/min/1.73 m2 | 2 | 12 | |
| GFR 30–59 mL/min/1.73 m2 | 3 | 19 | |
| GFR 15–29 mL/min/1.73 m2 | 2 | 12 | |
| GFR < 15 mL/min/1.73 m2 | 2 | 12 | |
| Cardiac status | Asymptomatic | 2 | 12 |
| Asymptomatic, but with remote myocardial infarction by history (6 months) | 6 | 38 | |
| Stable angina, ejection fraction 25% to 45%, controlled ectopy or asymptomatic arrhythmia, or history of congestive heart failure that is now well compensated | 7 | 44 | |
| Unstable angina, ejection fraction <25%, myocardial infarction ≤6 months | 1 | 6 | |
| Patency BTK vessels before procedure | 3 | 0 | 0 |
| 2 | 2 | 12.5 | |
| 1 | 12 | 75 | |
| 0 | 2 | 12.5 |
| Variable | |
|---|---|
| Serum Homocisteine (µmol/L) | 13.7 ± 1.1 |
| Serum Folate (nmol/L) | 17 ± 5 |
| Plasma Triglycerides (mg/dL) | 223 ± 11 |
| Plasma Cholesterol (mg/dL) | 251 ± 7 |
| LDL-Cholesterol (mg/dL) | 195 ± 5 |
| HDL-Cholesterol (mg/dL) | 9 ± 4 |
| Fasting plasma glucose (mg/dL) | 271 ± 35 |
| HbA1c (%) | 9.4 ± 2.2 |
| C-peptide (ng/mL) | 1.7 ± 0.2 |
| Neuropeptide Y (pg/mL) | 3421 ± 75 |
| Elabela peptide(ng/mL) | 3.1 ± 1.2 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Dinoto, E.; Ferlito, F.; La Marca, M.A.; Tortomasi, G.; Urso, F.; Evola, S.; Guercio, G.; Marcianò, M.; Pakeliani, D.; Bajardi, G.; et al. The Role of Early Revascularization and Biomarkers in the Management of Diabetic Foot Ulcers: A Single Center Experience. Diagnostics 2022, 12, 538. https://doi.org/10.3390/diagnostics12020538
Dinoto E, Ferlito F, La Marca MA, Tortomasi G, Urso F, Evola S, Guercio G, Marcianò M, Pakeliani D, Bajardi G, et al. The Role of Early Revascularization and Biomarkers in the Management of Diabetic Foot Ulcers: A Single Center Experience. Diagnostics. 2022; 12(2):538. https://doi.org/10.3390/diagnostics12020538
Chicago/Turabian StyleDinoto, Ettore, Francesca Ferlito, Manfredi Agostino La Marca, Graziella Tortomasi, Francesca Urso, Salvatore Evola, Giovanni Guercio, Marco Marcianò, David Pakeliani, Guido Bajardi, and et al. 2022. "The Role of Early Revascularization and Biomarkers in the Management of Diabetic Foot Ulcers: A Single Center Experience" Diagnostics 12, no. 2: 538. https://doi.org/10.3390/diagnostics12020538
APA StyleDinoto, E., Ferlito, F., La Marca, M. A., Tortomasi, G., Urso, F., Evola, S., Guercio, G., Marcianò, M., Pakeliani, D., Bajardi, G., & Pecoraro, F. (2022). The Role of Early Revascularization and Biomarkers in the Management of Diabetic Foot Ulcers: A Single Center Experience. Diagnostics, 12(2), 538. https://doi.org/10.3390/diagnostics12020538






