Vascular Abnormalities Detected with Chest CT in COVID-19: Spectrum, Association with Parenchymal Lesions, Cardiac Changes, and Correlation with Clinical Severity (COVID-CAVA Study)
Abstract
1. Introduction
2. Methods and Analysis
2.1. Study Design
2.1.1. Primary Objective
2.1.2. Secondary Objectives
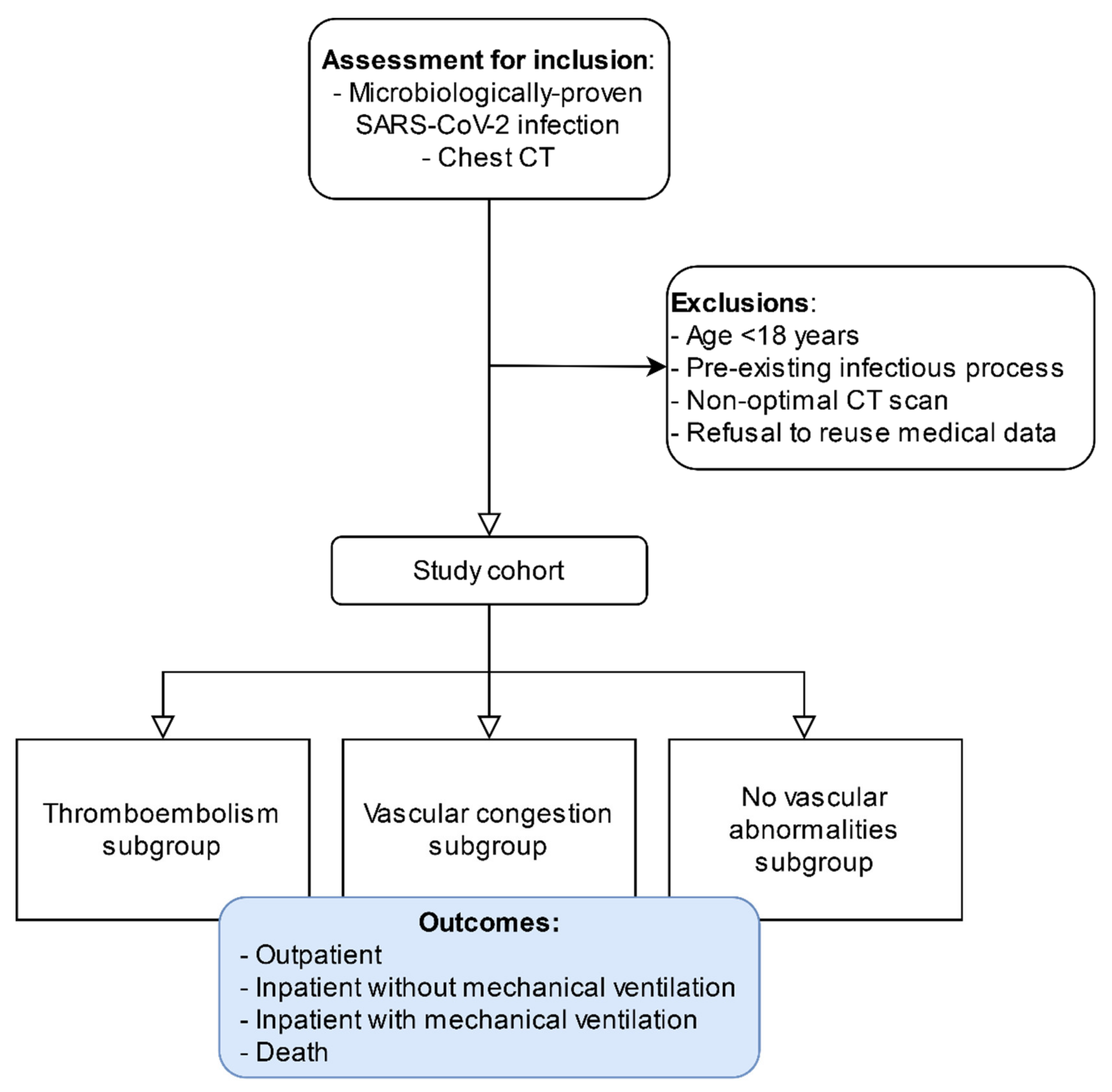
2.2. Patient Selection
2.2.1. Inclusion Criteria
2.2.2. Exclusion Criteria
2.2.3. Sample Size Calculation
3. Methodology and Data Analysis
3.1. CT Analysis
- -
- PE related abnormalities: the presence of embolic material, anatomic distribution based on segmental arteries, parenchymal changes and their distribution (PE present in the region of interest subject of parenchymal changes induced by the coronavirus), presence of perfusion defect–using iodine vs. water material decomposition if dual-energy CT was performed–assessment of right ventricle, left atrium, and pulmonary artery dimensions (diameters), and quantification of vascular obstruction using the Qanadli obstruction index (QOI) [28,29] and a modified Qanadli obstruction index (mQOI) based on the segmental analysis as follows:
- S: segmental QOI calculated for each segmental artery
- L: lobar QOI calculated for each lobar artery
- T: troncular QOI calculated for each pulmonary artery
- -
- Non-PE-related vascular abnormalities consist of visual assessment of VC (arterial and venous), manually drawn regions-of-interest in normal and abnormal parenchyma, quantification of vascular volumes and tissue volumes, quantification of venous dilatation, and arterial enlargement.
- -
- Non-vascular abnormalities include ground-glass opacities, consolidation, cysts, nodules, and pleural changes. Semi-quantitative assessment of SARS-CoV-2-related opacities is provided per segment: alveolar opacities (none, <50%, >50%) and per patient. A new relative volume-based index is calculated as follows:
- V: volume
- ROI: region of interest with parenchymal changes
- L: pulmonary lobe
3.2. Data Management
3.3. Statistical Analysis
4. Discussion and Clinical Relevance
5. Ethics and Dissemination
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Chen, N.; Zhou, M.; Dong, X.; Qu, J.; Gong, F.; Han, Y.; Qiu, Y.; Wang, J.; Liu, Y.; Wei, Y.; et al. Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: A descriptive study. Lancet 2020, 395, 507–513. [Google Scholar] [CrossRef]
- Grasselli, G.; Zangrillo, A.; Zanella, A.; Antonelli, M.; Cabrini, L.; Castelli, A.; Cereda, D.; Coluccello, A.; Foti, G.; Fumagalli, R.; et al. Baseline Characteristics and Outcomes of 1591 Patients Infected with SARS-CoV-2 Admitted to ICUs of the Lombardy Region, Italy. JAMA 2020, 323, 1574–1581. [Google Scholar] [CrossRef] [PubMed]
- Cui, S.; Chen, S.; Li, X.; Liu, S.; Wang, F. Prevalence of venous thromboembolism in patients with severe novel coronavirus pneumonia. J. Thromb. Haemost. 2020, 18, 1421–1424. [Google Scholar] [CrossRef] [PubMed]
- Escher, R.; Breakey, N.; Lämmle, B. Severe COVID-19 infection associated with endothelial activation. Thromb. Res. 2020, 190, 62. [Google Scholar] [CrossRef] [PubMed]
- Klok, F.A.; Kruip, M.; van der Meer, N.J.M.; Arbous, M.S.; Gommers, D.; Kant, K.M.; Kaptein, F.H.J.; van Paassen, J.; Stals, M.A.M.; Huisman, M.V.; et al. Incidence of thrombotic complications in critically ill ICU patients with COVID-19. Thromb. Res. 2020, 191, 145–147. [Google Scholar] [CrossRef] [PubMed]
- Poor, H.D.; Ventetuolo, C.E.; Tolbert, T.; Chun, G.; Serrao, G.; Zeidman, A.; Dangayach, N.S.; Olin, J.; Kohli-Seth, R.; Powell, C.A. COVID-19 critical illness pathophysiology driven by diffuse pulmonary thrombi and pulmonary endothelial dysfunction responsive to thrombolysis. Clin. Transl. Med. 2020, 10, e44. [Google Scholar] [CrossRef]
- Zhang, L.; Yan, X.; Fan, Q.; Liu, H.; Liu, X.; Liu, Z.; Zhang, Z. D-dimer levels on admission to predict in-hospital mortality in patients with Covid-19. J. Thromb. Haemost. 2020, 18, 1324–1329. [Google Scholar] [CrossRef]
- Cheng, Z.; Lu, Y.; Cao, Q.; Qin, L.; Pan, Z.; Yan, F.; Yang, W. Clinical Features and Chest CT Manifestations of Coronavirus Disease 2019 (COVID-19) in a Single-Center Study in Shanghai, China. AJR Am. J. Roentgenol. 2020, 215, 121–126. [Google Scholar] [CrossRef]
- Müller, N.L.; Ooi, G.C.; Khong, P.L.; Nicolaou, S. Severe acute respiratory syndrome: Radiographic and CT findings. AJR Am. J. Roentgenol. 2003, 181, 3–8. [Google Scholar] [CrossRef]
- Rubin, G.D.; Ryerson, C.J.; Haramati, L.B.; Sverzellati, N.; Kanne, J.P.; Raoof, S.; Schluger, N.W.; Volpi, A.; Yim, J.J.; Martin, I.B.K.; et al. The Role of Chest Imaging in Patient Management during the COVID-19 Pandemic: A Multinational Consensus Statement from the Fleischner Society. Chest 2020, 158, 106–116. [Google Scholar] [CrossRef]
- Wang, Y.; Dong, C.; Hu, Y.; Li, C.; Ren, Q.; Zhang, X.; Shi, H.; Zhou, M. Temporal Changes of CT Findings in 90 Patients with COVID-19 Pneumonia: A Longitudinal Study. Radiology 2020, 296, E55–E64. [Google Scholar] [CrossRef]
- Zhou, S.; Wang, Y.; Zhu, T.; Xia, L. CT Features of Coronavirus Disease 2019 (COVID-19) Pneumonia in 62 Patients in Wuhan, China. AJR Am. J. Roentgenol. 2020, 214, 1287–1294. [Google Scholar] [CrossRef]
- Zhu, Y.; Liu, Y.-L.; Li, Z.-P.; Kuang, J.-Y.; Li, X.-M.; Yang, Y.-Y.; Feng, S.-T. Clinical and CT imaging features of 2019 novel coronavirus disease (COVID-19). J. Infect. 2020. [Google Scholar] [CrossRef] [PubMed]
- Mergen, V.; Kobe, A.; Blüthgen, C.; Euler, A.; Flohr, T.; Frauenfelder, T.; Alkadhi, H.; Eberhard, M. Deep learning for automatic quantification of lung abnormalities in COVID-19 patients: First experience and correlation with clinical parameters. Eur. J. Radiol. Open 2020, 7, 100272. [Google Scholar] [CrossRef] [PubMed]
- ACoR. ACR Recommendations for the use of Chest Radiography and Computed Tomography (CT) for Suspected COVID-19 Infection. 2020. Available online: https://www.acr.org/Advocacy-and-Economics/ACR-Position-Statements/Recommendations-for-Chest-Radiography-and-CT-for-Suspected-COVID19-Infection (accessed on 29 April 2020).
- Grillet, F.; Behr, J.; Calame, P.; Aubry, S.; Delabrousse, E. Acute Pulmonary Embolism Associated with COVID-19 Pneumonia Detected with Pulmonary CT Angiography. Radiology 2020, 296, E186–E188. [Google Scholar] [CrossRef] [PubMed]
- Léonard-Lorant, I.; Delabranche, X.; Séverac, F.; Helms, J.; Pauzet, C.; Collange, O.; Schneider, F.; Labani, A.; Bilbault, P.; Molière, S.; et al. Acute Pulmonary Embolism in Patients with COVID-19 at CT Angiography and Relationship to d-Dimer Levels. Radiology 2020, 296, E189–E191. [Google Scholar] [CrossRef]
- Qanadli, S.D.; Beigelman-Aubry, C.; Rotzinger, D.C. Vascular Changes Detected with Thoracic CT in Coronavirus Disease (COVID-19) Might Be Significant Determinants for Accurate Diagnosis and Optimal Patient Management. AJR Am. J. Roentgenol. 2020, 215, W15. [Google Scholar] [CrossRef] [PubMed]
- Rotzinger, D.C.; Beigelman-Aubry, C.; von Garnier, C.; Qanadli, S.D. Pulmonary embolism in patients with COVID-19: Time to change the paradigm of computed tomography. Thromb. Res. 2020, 190, 58–59. [Google Scholar] [CrossRef] [PubMed]
- Marongiu, F.; Grandone, E.; Barcellona, D. Pulmonary thrombosis in 2019-nCoV pneumonia? J. Thromb. Haemost. 2020, 18, 1511–1513. [Google Scholar] [CrossRef]
- Tang, N.; Bai, H.; Chen, X.; Gong, J.; Li, D.; Sun, Z. Anticoagulant treatment is associated with decreased mortality in severe coronavirus disease 2019 patients with coagulopathy. J. Thromb. Haemost. 2020, 18, 1094–1099. [Google Scholar] [CrossRef]
- Gattinoni, L.; Coppola, S.; Cressoni, M.; Busana, M.; Rossi, S.; Chiumello, D. COVID-19 Does Not Lead to a “Typical” Acute Respiratory Distress Syndrome. Am. J. Respir. Crit. Care Med. 2020, 201, 1299–1300. [Google Scholar] [CrossRef]
- Henkel, M.; Weikert, T.; Marston, K.; Schwab, N.; Sommer, G.; Haslbauer, J.; Franzeck, F.; Anastasopoulos, C.; Stieltjes, B.; Michel, A.; et al. Lethal COVID-19: Radiologic-Pathologic Correlation of the Lungs. Radiol. Cardiothorac. Imaging 2020, 2, e200406. [Google Scholar] [CrossRef]
- Qanadli, S.D.; Rocha, A.C.; Rotzinger, D.C. Case Report: Intrapulmonary Arteriovenous Anastomoses in COVID-19-Related Pulmonary Vascular Changes: A New Player in the Arena? Front. Med. 2021, 8. [Google Scholar] [CrossRef]
- Deshpande, C. Thromboembolic Findings in COVID-19 Autopsies: Pulmonary Thrombosis or Embolism? Ann. Intern. Med. 2020, 173, 394–395. [Google Scholar] [CrossRef]
- Chow, S.C.; Shao, J.; Wang, H. Sample Size Calculations in Clinical Research, 2nd ed.; CRC Biostatistics Series; Chapman & Hall: London, UK, 2008; p. 89. [Google Scholar]
- Lodigiani, C.; Iapichino, G.; Carenzo, L.; Cecconi, M.; Ferrazzi, P.; Sebastian, T.; Kucher, N.; Studt, J.D.; Sacco, C.; Bertuzzi, A.; et al. Venous and arterial thromboembolic complications in COVID-19 patients admitted to an academic hospital in Milan, Italy. Thromb. Res. 2020, 191, 9–14. [Google Scholar] [CrossRef]
- Qanadli, S.D.; El Hajjam, M.; Vieillard-Baron, A.; Joseph, T.; Mesurolle, B.; Oliva, V.L.; Barré, O.; Bruckert, F.; Dubourg, O.; Lacombe, P. New CT index to quantify arterial obstruction in pulmonary embolism: Comparison with angiographic index and echocardiography. AJR Am. J. Roentgenol. 2001, 176, 1415–1420. [Google Scholar] [CrossRef]
- Rotzinger, D.C.; Knebel, J.-F.; Jouannic, A.-M.; Adler, G.; Qanadli, S.D. CT Pulmonary Angiography for Risk Stratification of Patients with Nonmassive Acute Pulmonary Embolism. Radiol. Cardiothorac. Imaging 2020, 2, e190188. [Google Scholar] [CrossRef]
- Harris, P.A.; Taylor, R.; Thielke, R.; Payne, J.; Gonzalez, N.; Conde, J.G. Research electronic data capture (REDCap)—A metadata-driven methodology and workflow process for providing translational research informatics support. J. Biomed. Inform. 2009, 42, 377–381. [Google Scholar] [CrossRef] [PubMed]
- Smetana, K., Jr.; Rosel, D.; BrÁbek, J. Raloxifene and Bazedoxifene Could Be Promising Candidates for Preventing the COVID-19 Related Cytokine Storm, ARDS and Mortality. In Vivo 2020, 34, 3027–3028. [Google Scholar] [CrossRef] [PubMed]
- Cavagna, E.; Muratore, F.; Ferrari, F. Pulmonary Thromboembolism in COVID-19: Venous Thromboembolism or Arterial Thrombosis? Radiol. Cardiothorac. Imaging 2020, 2, e200289. [Google Scholar] [CrossRef]
| Variable | Data | Variable Type |
|---|---|---|
| Disease severity | Outpatient, inpatient, death | Qualitative |
| Composite outcome | ICU admission or death | Dichotomic |
| Cardiovascular comorbidities | ||
| Hypertension | ||
| Atrial fibrillation | ||
| Coronary artery disease | ||
| Heart failure | ||
| Peripheral vascular disease | ||
| Stroke | ||
| Chronic kidney disease | ||
| Hemodialysis | ||
| Diabetes | ||
| COPD | ||
| Asthma | ||
| Cystic fibrosis | ||
| Onset to CT delay | Number of days | Ordinal |
| Onset to recovery delay | Number of days | Ordinal |
| Thromboprophylaxis or anticoagulants | Qualitative | Dichotomic |
| D-dimers | Plasma concentration | Continuous |
| PaO2 | Arterial blood partial pressure | Continuous |
| SaO2 | Venous blood O2 saturation | Continuous |
| C-reactive protein | Plasma concentration | Continuous |
| Thrombocytes | Count per microliter | Integer |
| Variable | Data | Variable Type | Segment | Lung | Patient |
|---|---|---|---|---|---|
| Left atrium size | 2 axes, continuous | Continuous | x | ||
| Right ventricle (RV) | Small axis | Continuous | x | ||
| Left ventricle (LV) | Small axis | Continuous | x | ||
| Pulmonary artery (PA) | Diameter | Continuous | x | ||
| Vascular congestion (VC) | Qualitative | Dichotomic | x | x | x |
| Vascular volume (VV) | Volumetric | Continuous | x | x | |
| Perfusion (PF) | Qualitative, iodine density map | Ordinal (decreased, normal, increased | x | x | |
| Venous-to-artery ratio (VRR) | Diameter ratio | Continuous | x | x | x |
| Pulmonary embolism (PE) | Qualitative | Dichotomic | x | x | x |
| Qanadli obstruction index (QOI) | Percentage | Ordinal (0–100% in 2.5% steps) | x | x | x |
| Modified QOI (mQOI) | Percentage | Ordinal (0–100% in 2.5% steps) | x | x | x |
| Ground glasses opacities (GGO) | Qualitative | Dichotomic | x | x | x |
| Alveolar consolidation | Qualitative | Dichotomic | x | x | x |
| Cyst | Qualitative | Dichotomic | x | x | x |
| Nodule | Qualitative | Dichotomic | x | x | x |
| Lung tissue volume (TV) | Volumetric | Continuous | x | x |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Qanadli, S.D.; Sauter, A.W.; Alkadhi, H.; Christe, A.; Poletti, P.-A.; Ebner, L.; Rotzinger, D.C. Vascular Abnormalities Detected with Chest CT in COVID-19: Spectrum, Association with Parenchymal Lesions, Cardiac Changes, and Correlation with Clinical Severity (COVID-CAVA Study). Diagnostics 2021, 11, 606. https://doi.org/10.3390/diagnostics11040606
Qanadli SD, Sauter AW, Alkadhi H, Christe A, Poletti P-A, Ebner L, Rotzinger DC. Vascular Abnormalities Detected with Chest CT in COVID-19: Spectrum, Association with Parenchymal Lesions, Cardiac Changes, and Correlation with Clinical Severity (COVID-CAVA Study). Diagnostics. 2021; 11(4):606. https://doi.org/10.3390/diagnostics11040606
Chicago/Turabian StyleQanadli, Salah D., Alexander W. Sauter, Hatem Alkadhi, Andreas Christe, Pierre-Alexandre Poletti, Lukas Ebner, and David C. Rotzinger. 2021. "Vascular Abnormalities Detected with Chest CT in COVID-19: Spectrum, Association with Parenchymal Lesions, Cardiac Changes, and Correlation with Clinical Severity (COVID-CAVA Study)" Diagnostics 11, no. 4: 606. https://doi.org/10.3390/diagnostics11040606
APA StyleQanadli, S. D., Sauter, A. W., Alkadhi, H., Christe, A., Poletti, P.-A., Ebner, L., & Rotzinger, D. C. (2021). Vascular Abnormalities Detected with Chest CT in COVID-19: Spectrum, Association with Parenchymal Lesions, Cardiac Changes, and Correlation with Clinical Severity (COVID-CAVA Study). Diagnostics, 11(4), 606. https://doi.org/10.3390/diagnostics11040606








