Assessment of the Impact of Rapid Point-of-Care CD4 Testing in Primary Healthcare Clinic Settings: A Survey Study of Client and Provider Perspectives
Abstract
1. Introduction
- Risk of losing patients who may not return due to cost and distance; delays in diagnosis and treatment initiation;
- Patients who seek healthcare elsewhere become nontraceable, giving wrong addresses to clinics further away for eligibility resulting in unnecessary repeat testing and higher workloads in some PHC clinics [7];
- Incomplete or incorrect completion of request forms or labelling of test tubes;
- The rejection of sample quality (insufficient or clotted specimen);
- Specimen damage or loss through transport;
2. Materials and Methods
2.1. Study Design
2.2. Study Population
2.3. Study Setting
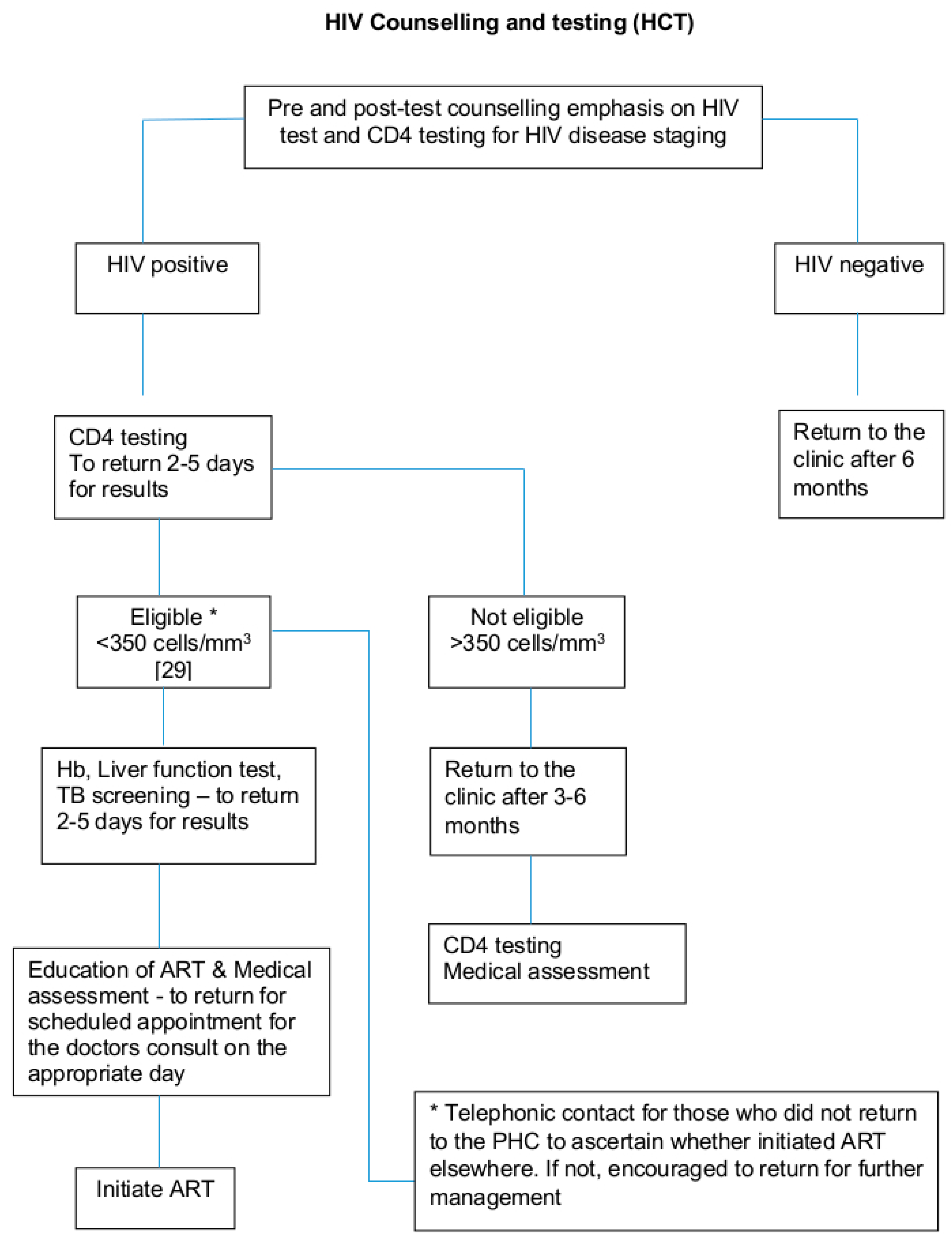
2.4. PHC Clinic Procedures
- Chronic care (diabetes; hypertension; cardiovascular diseases);
- Antenatal (breastfeeding; pregnancy; immunisations for children);
- Cancer (breast and ovarian);
- HIV education.
2.5. Study Procedures
- Are you happy to receive a CD4 test result on the same day? (n = 642)
- Would you rather wait for a CD4 test result or return to the clinic another day?
- How long did it take to get your CD4 test result?
- Do you know what a CD4 test result means?
- Are you ready to start ART if eligible?
- Do you think it is beneficial for the patient to get their CD4 result on the same day?
- What was the impact on your workload in giving CD4 results to the patient on the same day?
- Does having a CD4 result on the same day help you with patient management?
- Do you know what a CD4 test result means?
- Were you able to administer antiretrovirals (ARVs) to the patient on the same day you had the CD4 test result?
2.6. Data Handling and Recordkeeping
2.7. Ethics
2.8. Statistical Considerations
2.8.1. Sample Size
2.8.2. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Statistics South Africa (STATSA). Statistical Release P0302: Mid-Year Population Estimates. 2019. Available online: http://www.statssa.gov.za/?p=12362 (accessed on 31 August 2019).
- National Department of Health South Africa. Re: Implementation of the Universal Test and Treat Strategy for HIV Positive Patients and Differentiated Care for Stable Patients. 2016. Available online: https://sahivsoc.org/Files/22%208%2016%20Circular%20UTT%20%20%20Decongestion%20CCMT%20Directorate.pdf (accessed on 14 October 2019).
- World Health Organization. Guideline on When to Start Antiretroviral Therapy and on Pre-Exposure Prophylaxis for HIV; WHO: Geneva, Switzerland, 2015; Available online: https://apps.who.int/iris/bitstream/handle/10665/186275/9789241509565_eng.pdf (accessed on 30 September 2019).
- UNAIDS. South Africa UNAIDS 2017. Available online: https://www.unaids.org/en/regionscountries/countries/southafrica (accessed on 5 August 2018).
- Maillacheruvu, P.; McDuff, E. South Africa’s Return to Primary Care: The Struggles and Strides of the Primary Health Care System. J. Glob. Health 2014. Available online: https://www.ghjournal.org/south-africas-return-to-primary-care-the-struggles-and-strides-of-the-primary-health-care-system/ (accessed on 1 October 2019).
- Gous, N.M.; Berrie, L.; Dabula, P.; Stevens, W. South Africa’s experience with provision of quality HIV diagnostic services. Afr. J. Lab. Med. 2016, 5, 436. [Google Scholar] [CrossRef] [PubMed]
- Engel, N.; Davids, M.; Blankvoort, N.; Pai, N.P.; Dheda, K.; Pai, M. Compounding diagnostic delays: A qualitative study of point-of-care testing in South Africa. Trop. Med. Int. Health 2015, 20, 493–500. [Google Scholar] [CrossRef] [PubMed]
- Cloete, M.C.; Hampton, J.; Chetty, T.; Ngomane, T.; Spooner, E.; Zako, L.M.G.; Reddy, S.; Reddy, T.; Luthuli, N.; Ngobese, H.; et al. Evaluation of a health system intervention to improve virological management in an antiretroviral programme at a municipal clinic in central Durban. South. Afr. J. HIV Med. 2019, 20, 985. [Google Scholar] [CrossRef] [PubMed]
- Spooner, E.; Govender, K.; Reddy, T.; Ramjee, G.; Mbadi, N.; Singh, S.; Coutsoudis, A. Point-of-care HIV testing best practice for early infant diagnosis: An implementation study. BMC Public Health 2019, 19, 731. [Google Scholar] [CrossRef] [PubMed]
- Daneau, G.; Gous, N.; Scott, L.; Potgieter, J.; Kestens, L.; Stevens, W. Human Immunodeficiency Virus (HIV)-Infected Patients Accept Finger Stick Blood Collection for Point-Of-Care CD4 Testing. PLoS ONE 2016, 11, e0161891. [Google Scholar] [CrossRef] [PubMed]
- Govindasamy, D.; Ford, N.; Kranzer, K. Risk factors, barriers and facilitators for linkage to antiretroviral therapy care: A systematic review. AIDS 2012, 26, 2059–2067. [Google Scholar] [CrossRef]
- Jani, I.V.; Sitoe, N.E.; Alfai, E.R.; Chongo, P.L.; Quevedo, J.I.; Rocha, B.M.; Lehe, J.D.; Peter, T.F. Effect of point-of-care CD4 cell count tests on retention of patients and rates of antiretroviral therapy initiation in primary health clinics: An observational cohort study. Lancet 2011, 378, 1572–1579. [Google Scholar] [CrossRef]
- Vojnov, L.; Markby, J.; Boeke, C.; Harris, L.; Ford, N.; Peter, T. POC CD4 Testing Improves Linkage to HIV Care and Timeliness of ART Initiation in a Public Health Approach: A Systematic Review and Meta-Analysis. PLoS ONE 2016, 11, e0155256. [Google Scholar] [CrossRef]
- Stevens, W.S.; Gous, N.M.; MacLeod, W.B.; Long, L.C.; Variava, E.; Martinson, N.A.; Sanne, I.; Osih, R.; Scott, L.E. Multidisciplinary Point-of-Care Testing in South African Primary Health Care Clinics Accelerates HIV ART Initiation but Does Not Alter Retention in Care. J. Acquir. Immune Defic. Syndr. 2017, 76, 65–73. [Google Scholar] [CrossRef]
- Naidoo, P.; du Toit, E.; Dunbar, R.; Lombard, C.; Caldwell, J.; Detjen, A.; Squire, S.B.; Enarson, D.A.; Beyers, N. A comparison of multidrug-resistant tuberculosis treatment commencement times in MDRTBPlus line probe assay and Xpert(R) MTB/RIF-based algorithms in a routine operational setting in Cape Town. PLoS ONE 2014, 9, e103328. [Google Scholar] [CrossRef]
- Hyle, E.P.; Jani, I.V.; Lehe, J.; Su, A.E.; Wood, R.; Quevedo, J.; Losina, E.; Bassett, I.V.; Pei, P.P.; Paltiel, A.D.; et al. The clinical and economic impact of point-of-care CD4 testing in Mozambique and other resource-limited settings: A cost-effectiveness analysis. PLoS Med. 2014, 11, e1001725. [Google Scholar] [CrossRef] [PubMed]
- Ciaranello, A.L.; Myer, L.; Kelly, K.; Christensen, S.; Daskilewicz, K.; Doherty, K.; Bekker, L.G.; Hou, T.; Wood, R.; Francke, J.A.; et al. Point-of-care CD4 testing to inform selection of antiretroviral medications in South African antenatal clinics: A cost-effectiveness analysis. PLoS ONE 2015, 10, e0117751. [Google Scholar] [CrossRef] [PubMed]
- Pai, N.P.; Vadnais, C.; Denkinger, C.; Engel, N.; Pai, M. Point-of-care testing for infectious diseases: Diversity, complexity, and barriers in low- and middle-income countries. PLoS Med. 2012, 9, e1001306. [Google Scholar] [CrossRef] [PubMed]
- Jani, I.V.; Peter, T.F. How point-of-care testing could drive innovation in global health. N. Engl. J. Med. 2013, 368, 2319–2324. [Google Scholar] [CrossRef]
- Stime, K.J.; Garrett, N.; Sookrajh, Y.; Dorward, J.; Dlamini, N.; Olowolagba, A.; Sharma, M.; Barnabas, R.V.; Drain, P.K. Clinic flow for STI, HIV, and TB patients in an urban infectious disease clinic offering point-of-care testing services in Durban, South Africa. BMC Health Serv. Res. 2018, 18, 363. [Google Scholar] [CrossRef]
- Munkhuu, B.; Liabsuetrakul, T.; McNeil, E.; Janchiv, R. Feasibility of one-stop antenatal syphilis screening in Ulaanbaatar, Mongolia: Women and providers perspectives. Southeast Asian J. Trop. Med. Public Health 2009, 40, 861–870. [Google Scholar]
- Wynberg, E.; Cooke, G.; Shroufi, A.; Reid, S.D.; Ford, N. Impact of point-of-care CD4 testing on linkage to HIV care: A systematic review. J. Int. AIDS Soc. 2014, 17, 18809. [Google Scholar] [CrossRef]
- Jani, I.V.; Meggi, B.; Loquiha, O.; Tobaiwa, O.; Mudenyanga, C.; Zitha, A.; Mutsaka, D.; Mabunda, N.; Vubil, A.; Bollinger, T.; et al. Effect of point-of-care early infant diagnosis on antiretroviral therapy initiation and retention of patients. AIDS 2018, 32, 1453–1463. [Google Scholar] [CrossRef]
- Msimango, L.; Gibbs, A.; Shozi, H.; Ngobese, H.; Humphries, H.; Drain, P.K.; Garrett, N.; Dorward, J. Acceptability of Point-Of-Care Viral Load Testing to Facilitate Differentiated Care: A Qualitative Assessment of People Living with HIV and Healthcare Workers in South Africa; International AIDS Society: Mexico City, Mexico, 2019. [Google Scholar]
- Skhosana, M.; Reddy, S.; Reddy, T.; Ntoyanto, S.; Spooner, E.; Ramjee, G.; Ngomane, N.; Coutsoudis, A.; Kiepiela, P. PIMA point-of-care testing for CD4 counts in predicting antiretroviral initiation in HIV-infected individuals in KwaZulu-Natal, Durban, South Africa. South Afr. J. HIV Med. 2016, 17, 444. [Google Scholar]
- Reddy, S.; Ntoyanto, S.; Sakadavan, Y.; Reddy, T.; Mahomed, S.; Dlamini, M.; Spooner, B.; Ramjee, G.; Coutsoudis, A.; Ngomane, N.; et al. Detecting Mycobacterium tuberculosis using the loop-mediated isothermal amplification test in South Africa. Int. J. Tuberc. Lung Dis. 2017, 21, 1154–1160. [Google Scholar] [CrossRef] [PubMed]
- The Logic of Qualitative Survey Research and its Position in the Field of Social Research Methods. Available online: http://www.qualitative-research.net/index.php/fqs/article/view/1450/2946. (accessed on 1 November 2019).
- Sub Place Chesterville. Census. 2011. Available online: https://census2011.adrianfrith.com/place/599054041 (accessed on 30 September 2019).
- South African Department of Health. The South African Antiretroviral Treatment Guidelines. 2010. Available online: https://apps.who.int/medicinedocs/documents/s19153en/s19153en.pdf (accessed on 30 September 2019).
- Mtapuri-Zinyowera, S.; Chiyaka, E.T.; Mushayi, W.; Musuka, G.; Naluyinda-Kitabire, F.; Mushavi, A.; Chikwasha, V. PIMA Point of Care CD4+ Cell Count Machines in Remote MNCH Settings: Lessons Learned from Seven Districts in Zimbabwe. Infect. Dis. 2013, 6, 51–60. [Google Scholar] [CrossRef] [PubMed]
- Jain, K.; Mshweshwe-Pakela, N.T.; Charalambous, S.; Mabuto, T.; Hoffmann, C.J. Enhancing value and lowering costs of care: A qualitative exploration of a randomized linkage to care intervention in South Africa. AIDS Care 2019, 31, 481–488. [Google Scholar] [CrossRef]
- Fox, M.P.; Rosen, S. Patient retention in antiretroviral therapy programs up to three years on treatment in sub-Saharan Africa, 2007–2009: Systematic review. Trop. Med. Int. Health 2010, 15 (Suppl. 1), 1–15. [Google Scholar] [CrossRef] [PubMed]
- Larson, B.A.; Schnippel, K.; Ndibongo, B.; Xulu, T.; Brennan, A.T.; Long, L.C.; Fox, M.P.; Rosen, S. Rapid point-of-care CD4 testing at mobile HIV testing sites to increase linkage to care: An evaluation of a pilot program in South Africa. J. Acquir. Immune Defic. Syndr. 2012, 61, e13–e17. [Google Scholar] [CrossRef] [PubMed]
- Rosen, S.; Fox, M.P. Retention in HIV care between testing and treatment in sub-Saharan Africa: A systematic review. PLoS Med. 2011, 8, e1001056. [Google Scholar] [CrossRef] [PubMed]
- Mugglin, C.; Estill, J.; Wandeler, G.; Bender, N.; Egger, M.; Gsponer, T.; Keiser, O.; IeDEA Southern Africa. Loss to programme between HIV diagnosis and initiation of antiretroviral therapy in sub-Saharan Africa: Systematic review and meta-analysis. Trop. Med. Int. Health 2012, 17, 1509–1520. [Google Scholar] [CrossRef]
- Patten, G.E.; Wilkinson, L.; Conradie, K.; Isaakidis, P.; Harries, A.D.; Edginton, M.E.; De Azevedo, V.; van Cutsem, G. Impact on ART initiation of point-of-care CD4 testing at HIV diagnosis among HIV-positive youth in Khayelitsha, South Africa. J. Int. AIDS Soc. 2013, 16, 18518. [Google Scholar] [CrossRef]
- Losina, E.; Bassett, I.V.; Giddy, J.; Chetty, S.; Regan, S.; Walensky, R.P.; Ross, D.; Scott, C.A.; Uhler, L.M.; Katz, J.N.; et al. The “ART” of linkage: Pre-treatment loss to care after HIV diagnosis at two PEPFAR sites in Durban, South Africa. PLoS ONE 2010, 5, e9538. [Google Scholar] [CrossRef]
- Paparini, S.; Rhodes, T. The biopolitics of engagement and the HIV cascade of care: A synthesis of the literature on patient citizenship and antiretroviral therapy. Crit. Public Health 2016, 26, 501–517. [Google Scholar] [CrossRef]
- Mashamba-Thompson, T.P.; Jama, N.A.; Sartorius, B.; Drain, P.K.; Thompson, R.M. Implementation of Point-of-Care Diagnostics in Rural Primary Healthcare Clinics in South Africa: Perspectives of Key Stakeholders. Diagnostics 2017, 7, 3. [Google Scholar] [CrossRef] [PubMed]
- Rasti, R.; Nanjebe, D.; Karlstrom, J.; Muchunguzi, C.; Mwanga-Amumpaire, J.; Gantelius, J.; Mårtensson, A.; Rivas, L.; Galban, F.; Reuterswärd, P.; et al. Health care workers’ perceptions of point-of-care testing in a low-income country-A qualitative study in Southwestern Uganda. PLoS ONE 2017, 12, e0182005. [Google Scholar] [CrossRef]
- Mashamba-Thompson, T.P.; Sartorius, B.; Drain, P.K. Point-of-Care Diagnostics for Improving Maternal Health in South Africa. Diagnostics 2016, 6, 31. [Google Scholar] [CrossRef] [PubMed]
- Mashamba-Thompson, T.P.; Sartorius, B.; Drain, P.K. Operational assessment of point-of-care diagnostics in rural primary healthcare clinics of KwaZulu-Natal, South Africa: A cross-sectional survey. BMC Health Serv. Res. 2018, 18, 380. [Google Scholar] [CrossRef] [PubMed]
- Gous, N.; Takle, J.; Oppenheimer, A.; Schooley, A. Racing for results: Lessons learnt in improving the efficiency of HIV viral load and early infant diagnosis result delivery from laboratory to clinic. Expert Rev. Mol. Diagn. 2018, 18, 789–795. [Google Scholar] [CrossRef]
- Pai, N.P.; Wilkinson, S.; Deli-Houssein, R.; Vijh, R.; Vadnais, C.; Behlim, T.; Steben, M.; Engel, N.; Wong, T. Barriers to Implementation of Rapid and Point-of-Care Tests for Human Immunodeficiency Virus Infection: Findings from a Systematic Review (1996–2014). Point Care 2015, 14, 81–87. [Google Scholar] [CrossRef]
- Jones, C.H.; Howick, J.; Roberts, N.W.; Price, C.P.; Heneghan, C.; Plüddemann, A.; Thompson, M. Primary care clinicians’ attitudes towards point-of-care blood testing: A systematic review of qualitative studies. BMC Fam. Pract. 2013, 14, 117. [Google Scholar] [CrossRef]
- Engel, N.; Davids, M.; Blankvoort, N.; Dheda, K.; Pant, P.N.; Pai, M. Making HIV testing work at the point of care in South Africa: A qualitative study of diagnostic practices. BMC Health Serv. Res. 2017, 17, 408. [Google Scholar] [CrossRef]
- UNICEF: Key Considerations for Introducing New HIV Point-of-Care Diagnostic Technologies in National Health Systems. 2017. Available online: http://www.childrenandaidsorg/poc-toolkit-page. (accessed on 17 September 2019).
- Gupta, R.K.; Jordan, M.R.; Sultan, B.J.; Hill, A.; Davis, D.H.; Gregson, J.; Sawyer, A.W.; Hamers, R.L.; Ndembi, N.; Pillay, D.; et al. Global trends in antiretroviral resistance in treatment-naive individuals with HIV after rollout of antiretroviral treatment in resource-limited settings: A global collaborative study and meta-regression analysis. Lancet 2012, 380, 1250–1258. [Google Scholar] [CrossRef]
- Estill, J.; Aubrière, C.; Egger, M.; Johnson, L.; Wood, R.; Garone, D.; Gsponer, T.; Wandeler, G.; Boulle, A.; Davies, M.A.; et al. Viral load monitoring of antiretroviral therapy, cohort viral load and HIV transmission in Southern Africa: A mathematical modelling analysis. AIDS 2012, 26, 1403–1413. [Google Scholar] [CrossRef]
- UNAIDS. Fast-Track Ending the AIDS Epidemic by 2030. 2014. Available online: http://unaids.org/en/resources/documents/2014/JC2686 (accessed on 5 August 2019).
| (a) Are you happy to receive a CD4 test result on the same day? (n = 642) | Reasons | Illustrative Example | Overall n = 642 (%) | Lancers Road PHC n = 322 * (%) | Chesterville PHC n = 320 * (%) | p | Z | |
| Happy | Receive medical help | I like it because I will get assistance immediately if my results say so So that I know immediately if I’m supposed to start medication | 474 (73.8) | 237 (73.6) | 237 (74.1) | 0.9083 | −0.12 | |
| Saves time/money | I live far so it cost me a lot of money to come to the clinic So I won’t have to take time off work to come to the clinic | 125 (19.5) | 67 (20.8) | 58 (18.1) | 0.3875 | 0.86 | ||
| No delay or loss of test results | It will avoid the loss of results and being drawn the blood again due to loss of them. | 41 (6.4) | 18 (5.6) | 23 (7.2) | 0.4075 | −0.83 | ||
| Not Happy | Anxiety | I need time to get ready for the results | 2 (0.3) | 0 | 2 (0.6) | 0.1645 | −1.39 | |
| (b) Would you rather wait for a CD4 test result or return to clinic another day? * Not recorded for Lancers Road Clinic (n = 1) | Prefer to wait | Start Treatment | I would want to know if the treatment I am taking is working or not | 362 (56.4) | 155 (48.1) | 207 (64.7) | <0.0001 | −4.24 |
| Clinic inaccessibility | To save time and money for transport and I won’t have to come back again for results since I hate being in the clinic I will save time, money and won’t have to ask for leave at work for the second time | 209 (32.6) | 130 (40.4) | 79 (24.7) | <0.0001 | 4.24 | ||
| No anxiety | If I wait for my result, I can deal with the stress same time I won’t stress about the result if I get my result same day | 33 (5.1) | 19 (5.9) | 14 (4.4) | 0.3900 | 0.86 | ||
| No loss of samples | I like this because sometimes I come back for nothing, they tell me my blood was lost in the lab It can prevent loss of results | 15 (2.3) | 9 (2.8) | 6 (1.9) | 0.4518 | 0.75 | ||
| Not Wait | Not ready for results | It’s better if I come back another day because I’m always rushing back to work Because there would be a long queue | 22 (3.4) | 8 (2.5) | 14 (4.4) | 0.1870 | −1.32 | |
| (c) Do you know what a CD4 test result means? | Yes | CD4 cells/ Immune system | It tells how strong my CD4 cells I have Checking of soldier cells in the body It is your CD4 cell count. | 283 (44.1) | 153 (47.5) | 130 (40.6) | 0.0783 | 0.078 |
| Start treatment | It tells if you are ready to start treatment The results show the progress of the soldier cells in the body when taking medication. | 151 (23.5) | 69 (21.4) | 82 (25.6) | 0.2095 | −1.26 | ||
| Viral load | It tells how much the virus is decreasing in the body | 63 (9.8) | 30 (9.3) | 33 (10.3) | 0.6700 | −0.43 | ||
| HIV status | Tells me if I’m positive It tells me about HIV/AIDS | 16 (2.5) | 6 (1.9) | 10 (3.1) | 0.3300 | −0.97 | ||
| No | Don’t know | 129 (20.1) | 64 (19.9) | 65 (20.3) | 0.8994 | 0.899 | ||
| (d) Are you ready to start ART if eligible? *Not recorded (n = 3 from each PHC) | Yes | Will live/make me better | It will help me from getting other infections Because I want to be healthy and live longer So I can be able to live longer So that I can protect myself and cannot spread the virus | 286 (44.5) | 147 (45.7) | 139 (43.4) | 0.5577 | 0.59 |
| Make me better in order to look after my family | Because I want to live longer as I have a family I’m ready because I don’t want to die because I have children Because I have to, for the sake of my baby | 7 (1.1) | 6 (1.9) | 1 (0.3) | 0.0522 | 1.94 | ||
| Boost immune system/reduce viral load | I would start so that my CD4 levels stays high So it will increase my CD4 count | 47 (7.3) | 30 (9.3) | 17 (5.3) | 0.0515 | 1.95 | ||
| Ready | 34 (5.3) | 31 (9.6) | 3 (0.9) | <0.0001 | 4.94 | |||
| No choice | Because I have no choice It’s a must to start treatment whether I like it or not so that I can keep a healthy lifestyle | 15 (2.3) | 7 (2.2) | 8 (2.5) | 0.8019 | −0.25 | ||
| Don’t want to die | It’s my life so I have to be responsible as if I don’t take treatment, I will die I know if I don’t start treatment if my CD4 is low, I will get sick and die so I will take it | 17 (2.6) | 11 (3.4) | 6 (1.9) | 0.2370 | 1.18 | ||
| No | Not ready | It will be hard because I haven’t told anyone about my status because I know they won’t accept it | 23 (3.6) | 10 (3.1) | 13 (4.1) | 0.4964 | −0.68 | |
| On ARVs. already | 207 (32.2) | 77 (23.9) | 130 (40.6) | <0.0001 | −4.53 | |||
| (2a) Do you think it is beneficial for the patient to get their CD4 result on the same day? | Yes | Reasons | Illustrative Example | Overall n = 13 (%) | Lancers Road PHC n = 5 (%) | Chesterville PHC n = 8 (%) |
| Disease progression | They get to know how their immune system is doing Because they will be informed about the progression of the disease in the body | 6 (46.2) | 4 (80) | 2 (25) | ||
| Convenience | Some patients work cannot afford to come to the clinic every second week. Other patients come when the clinic is very busy while they also work | 2 (15.4) | 0 | 2 (25) | ||
| Start Treatment | Will speed up the process of initiating patients to ART and patients will get immediate care | 1 (7.7) | 0 | 1 (12.5) | ||
| No | Time off work | If they have asked for time off at work for that day of blood draw, they might not get a chance to come another day to collect results | 2 (15.4) | 0 | 2 (25) | |
| Not ready for results | It’s good and bad at the same time. It’s good for someone who’s been counselled well but others may not feel so good especially if they didn’t even think of results | 2 (15.4) | 1 (20%) | 1 (12.5) | ||
| (2b) What was the impact on your workload in giving CD4 results to the patient on the same day? | Beneficial | Reduce workload | It would make work easier and time saving because as a nurse, I won’t see the patient over and over again about something that could be done in a day. It will be easy as you know that you will be dealing with patients and finish all procedures at once rather than calling them back. | 4 (30.8) | 1 (20) | 3 (37.5) |
| Treat patients early | It gives clarity on their CD4 count on whether they are starting ARVs. or not | 2 (15.4) | 1 (20) | 1 (12.5) | ||
| Not beneficial | Increase workload | It will increase my work load because there’s too much administration when you initiate a person on treatment | 4 (30.8) | 3 (60) | 1 (12.5) | |
| Complete all other procedures | It will increase workload; more staff like phlebotomists to take bloods. Patients will need to be prepared for ARV therapy, assess readiness and acceptance. | 3 (23.0) | 0 | 3 (37.5) | ||
| (2c) Does having a CD4 result on the same day help you with patient clinical management? | Yes | Patient readiness | Because the patients gets all the information and help he/she needs on the same day | 6 (46.2) | 2 (40) | 4 (50) |
| Adherence | It helps a lot to manage the patients who has low CD4 count | 3 (23.0) | 2 (40) | 1 (12.5) | ||
| Follow up visits | The patient won’t have to come to the clinic for treatment so we won’t lose the patients | 1 (7.7) | 0 | 1 (12.5) | ||
| No | Assistance from other staff | It helps, but at the same time, it does not because there is a lot of tests that are done | 1 (7.7) | 0 | 1 (12.5) | |
| Training/Education | Yes, will definitely help, but on the other side, will be a disadvantage for patients who just tested positive; still a shock to them | 2 (15.4) | 1 (20) | 1 (12.5) | ||
| (2d) Do you know what a CD4 test result mean? | Yes | Start treatment | Yes if patients have CD4 of 500 or less they are started on ART. | 6 (46.2) | 0 | 6 (75.0) |
| Level of soldier cells | It tells me how high the level of soldier cells in the blood or how low the level of soldier cells in the blood | 5 (38.5) | 4 (80.0) | 1 (12.5) | ||
| Staging of HIV infection | It means patient is infected with the virus; gives me the picture of what stage the patient is in. | 1 (7.7) | 0 | 1 (12.5) | ||
| No | Don’t know | 1 (7.7) | 1 (20.0) | 0 | ||
| (2e) Were you able to administer ARVs. to the patient on the same day you had the CD4 test result? *Not recorded in Chesterville PHC for (e) (n = 1) | Yes | Pregnant women | I managed the initiation of pregnant women as they are started on ARVs. immediately, regardless of their CD4 count Because I was directed by CD4 results, but with pregnant women, you provide ARVs. at the same time, regardless of CD4 count | 4 (30.8) | 1 (20) | 3 (37.5) |
| Decrease Viral load | So it would help decrease the viral load | 1 (7.7) | 1 (20) | 0 | ||
| Treatment initiation | The CD4 count result guided me into initiating a patient | 1 (7.7) | 1 (20) | 0 | ||
| No | Require other blood tests | A patient is not initiated immediately; he/she needs to undergo some tests first We need to check other diseases like TB, tests for liver and kidneys before initiating ARVS | 4 (30.8) | 2 (40) | 2 (25) | |
| Patient education | That has not happened as yet in the clinic depending on the other things that need to be considered | 1 (7.7) | 0 | 1 (12.5) | ||
| Not job description | 1 (7.7) | 0 | 1 (12.5) |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Reddy, S.; Gibbs, A.; Spooner, E.; Ngomane, N.; Reddy, T.; |Luthuli, N.; Ramjee, G.; Coutsoudis, A.; Kiepiela, P. Assessment of the Impact of Rapid Point-of-Care CD4 Testing in Primary Healthcare Clinic Settings: A Survey Study of Client and Provider Perspectives. Diagnostics 2020, 10, 81. https://doi.org/10.3390/diagnostics10020081
Reddy S, Gibbs A, Spooner E, Ngomane N, Reddy T, |Luthuli N, Ramjee G, Coutsoudis A, Kiepiela P. Assessment of the Impact of Rapid Point-of-Care CD4 Testing in Primary Healthcare Clinic Settings: A Survey Study of Client and Provider Perspectives. Diagnostics. 2020; 10(2):81. https://doi.org/10.3390/diagnostics10020081
Chicago/Turabian StyleReddy, Shabashini, Andrew Gibbs, Elizabeth Spooner, Noluthando Ngomane, Tarylee Reddy, Nozipho |Luthuli, Gita Ramjee, Anna Coutsoudis, and Photini Kiepiela. 2020. "Assessment of the Impact of Rapid Point-of-Care CD4 Testing in Primary Healthcare Clinic Settings: A Survey Study of Client and Provider Perspectives" Diagnostics 10, no. 2: 81. https://doi.org/10.3390/diagnostics10020081
APA StyleReddy, S., Gibbs, A., Spooner, E., Ngomane, N., Reddy, T., |Luthuli, N., Ramjee, G., Coutsoudis, A., & Kiepiela, P. (2020). Assessment of the Impact of Rapid Point-of-Care CD4 Testing in Primary Healthcare Clinic Settings: A Survey Study of Client and Provider Perspectives. Diagnostics, 10(2), 81. https://doi.org/10.3390/diagnostics10020081




