A Narrative Review of the Classification and Use of Diagnostic Ultrasound for Conditions of the Achilles Tendon
Abstract
1. Introduction
2. Methods
3. A Word about Words
4. Imaging Modalities for the Hindfoot and Posterior Ankle
5. Enthesopathy
6. Achilles Tendonopathy
7. Calcific Tendonopathy
8. Retrocalcaneal and Superficial Calcaneal Bursitis
9. Paratenonopathy
10. Achilles Tendon Tears and Muscle Ruptures
11. Conclusions
Funding
Conflicts of Interest
References
- McGonagle, D.; Gibbon, W.; Emery, P. Classification of inflammatory arthritis by enthesitis. Lancet 1998, 352, 1137–1140. [Google Scholar] [CrossRef]
- D’Agostino, M.-A.; Olivieri, I. Enthesitis. Best Pract. Res. Clin. Rheumatol. 2006, 20, 473–486. [Google Scholar] [CrossRef] [PubMed]
- D’Agostino, M.-A.; Said-Nahal, R.; Brasseur, J.-L.; Dougados, M.; Breban, M. Assessment of peripheral enthesitis in the spondylarthropathies by ultrasonography combined with power Doppler: A cross-sectional study. Arthritis Rheum. 2003, 48, 523–533. [Google Scholar] [CrossRef] [PubMed]
- D’Agostino, M.A.; Aegerter, P.; Bechara, K.; Salliot, C.; Judet, O.; Chimenti, M.S.; Monnet, D.; Le Parc, J.-M.; Landais, P.; Breban, M. How to diagnose spondyloarthritis early? Accuracy of peripheral enthesitis detection by power Doppler ultrasonography. Ann. Rheum. Dis. 2011, 70, 1433–1440. [Google Scholar] [CrossRef] [PubMed]
- Mease, P.J. Measures of psoriatic arthritis: Tender and Swollen Joint Assessment, Psoriasis Area and Severity Index (PASI), Nail Psoriasis Severity Index (NAPSI), Modified Nail Psoriasis Severity Index (mNAPSI), Mander/Newcastle Enthesitis Index (MEI), Leeds Enthesit. Arthritis Rheum. 2011, 63, S64–S85. [Google Scholar] [CrossRef]
- McGonagle, D.; Stockwin, L.; Isaacs, J.; Emery, P. An enthesitis based model for the pathogenesis of spondyloarthropathy. Additive effects of microbial adjuvant and biomechanical factors at disease sites. J. Rheumatol. 2001, 28, 2155–2159. [Google Scholar]
- Mander, M.; Simpson, J.M.; McLellan, A.; Walker, D.A.; Goodacre, J.; Dick, W.C. Studies with an enthesis index as a method of clinical assessment in ankylosing spondylitis. Ann. Rheum. Dis. 1987, 46, 197–202. [Google Scholar] [CrossRef]
- Klauser, A.S.; Wipfler, E.; Dejaco, C.; Moriggl, B.; Duftner, C.; Schirmer, M. Diagnostic values of history and clinical examination to predict ultrasound signs of chronic and acute enthesitis. Clin. Exp. Rheumatol. 2008, 26, 548–553. [Google Scholar]
- Heuft-Dorenbosch, L.; Spoorenberg, A.; Van Tubergen, A.; Landewé, R.; Tempel, H.V.V.; Mielants, H.; Dougados, M.; Van Der Heijde, D. Assessment of enthesitis in ankylosing spondylitis. Ann. Rheum. Dis. 2003, 62, 127–132. [Google Scholar] [CrossRef]
- Maksymowych, W.P.; Mallon, C.; Morrow, S.; Shojania, K.; Olszynski, W.P.; Wong, R.L.; Sampalis, J.; Conner-Spady, B. Development and validation of the Spondyloarthritis Research Consortium of Canada (SPARCC) Enthesitis Index. Ann. Rheum. Dis. 2008, 68, 948–953. [Google Scholar] [CrossRef]
- Balint, P.V.; Kane, D.; Wilson, H.; McInnes, I.B.; Sturrock, R.D. Ultrasonography of entheseal insertions in the lower limb in spondyloarthropathy. Ann. Rheum. Dis. 2002, 61, 905–910. [Google Scholar] [CrossRef] [PubMed]
- Healy, P.J.; Helliwell, P.S. Measuring clinical enthesitis in psoriatic arthritis: Assessment of existing measures and development of an instrument specific to psoriatic arthritis. Arthritis Rheum. 2008, 59, 686–691. [Google Scholar] [CrossRef]
- Weinfeld, S.B. Achilles Tendon Disorders. Med. Clin. N. Am. 2014, 98, 331–338. [Google Scholar] [CrossRef] [PubMed]
- Puddu, G.; Ippolito, E.; Postacchini, F. A classification of achilles tendon disease. Am. J. Sports Med. 1976, 4, 145–150. [Google Scholar] [CrossRef] [PubMed]
- Kehl, A.S.; Corr, M.; Weisman, M.H. Review: Enthesitis: New Insights into Pathogenesis, Diagnostic Modalities, and Treatment. Arthritis Rheumatol. 2016, 68, 312–322. [Google Scholar] [CrossRef] [PubMed]
- McGonagle, D.; Marzo-Ortega, H.; O’Connor, P.; Gibbon, W.; Pease, C.; Reece, R.; Emery, P. The role of biomechanical factors and HLA-B27 in magnetic resonance imaging-determined bone changes in plantar fascia enthesopathy. Arthritis Rheum. 2002, 46, 489–493. [Google Scholar] [CrossRef]
- Erdem, C.; Sarikaya, S.; Erdem, L.; Özdolap, Ş.; Gündoğdu, S. MR imaging features of foot involvement in ankylosing spondylitis. Eur. J. Radiol. 2005, 53, 110–119. [Google Scholar] [CrossRef]
- Kamel, M.; Eid, H.; Mansour, R. Ultrasound detection of heel enthesitis: A comparison with magnetic resonance imaging. J. Rheumatol. 2003, 30, 774–778. [Google Scholar]
- Özdoğan, Ö.; Değirmenci, B.; Şenocak, Ö.; Gülbahar, S.; Arslan, G.; Taşçı, C.; Akalın, E.; Durak, H. Tc-99m HIG Scintigraphy in Detection of Active Inflammation in Ankylosing Spondylitis. Mol. Imaging Radionucl. Ther. 2011, 20, 52–58. [Google Scholar] [CrossRef]
- Østergaard, M.; Lambert, R.G. Imaging in ankylosing spondylitis. Ther. Adv. Musculoskelet. Dis. 2012, 4, 301–311. [Google Scholar] [CrossRef]
- Zellers, J.A.; Bley, B.C.; Pohlig, R.T.; Alghamdi, N.H.; Silbernagel, K.G. Frequency of Pathology on Diagnostic Ultrasound and Relationship to Patient Demographics in Individual with Insertional Achilles Tendonopathy. Int. J. Sports Phys. Ther. 2019, 14, 761–769. [Google Scholar] [CrossRef] [PubMed]
- Loiacono, C.; Palermi, S.; Massa, B.; Belviso, I.; Romano, V.; Di Gregorio, A.; Sirico, F.; Sacco, A.M. Tendonopathy: Pathophysiology, Therapeutic Options, and Role of Nutraceutics. A Narrative Literature Review. Medicina 2019, 55, 447. [Google Scholar] [CrossRef] [PubMed]
- Charnoff, J.; Naqvi, U. Tendinosis (Tendinitis) [Updated 28 April 2020]. In StatPearls [Internet]; StatPearls Publishing: Treasure Island, FL, USA, 2020. Available online: https://www.ncbi.nlm.nih.gov/books/NBK448174/ (accessed on 11 September 2020).
- Monestime, J.P.; Mayer, R.W.; Blackwood, A. Analyzing the ICD-10-CM Transition and Post-implementation Stages: A Public Health Institution Case Study. Perspect. Health Inf. Manag. 2019, 16, 1a. [Google Scholar] [PubMed]
- ICD-10-CM Code M67.879. ICD List. [Internet] 2020. Available online: https://icdlist.com/icd-10/M67.879 (accessed on 11 September 2020).
- ICD-10-CM Code M67.873. ICD List. [Internet] 2020. Available online: https://icdlist.com/icd-10/M67.873 (accessed on 11 September 2020).
- ICD-10-CM Code M67.874. ICD List. [Internet] 2020. Available online: https://icdlist.com/icd-10/M67.874 (accessed on 11 September 2020).
- ICD-10-CM Code M76.6. ICD.Codes. Available online: https://icd.codes/icd10cm/M766 (accessed on 11 September 2020).
- Almekinders, L.C.; Temple, J.D. Etiology, diagnosis, and treatment of tendonitis: An analysis of the literature. Med. Sci. Sports Exerc. 1998, 30, 1183–1190. [Google Scholar] [CrossRef]
- Khan, K.M.; Cook, J.L.; Kannus, P.; Maffulli, N.; Bonar, S.F. Time to abandon the “tendinitis” myth. BMJ 2002, 324, 626–627. [Google Scholar] [CrossRef]
- Alfredson, H.; Forsgren, S.; Thorsen, K.; Lorentzon, R. In vivo investigation of ECRB tendons with microdialysis technique—no signs of inflammation but high amounts of glutamate in tennis elbow. Acta Orthop. Scand. 2000, 71, 475–479. [Google Scholar] [CrossRef]
- Alfredson, H.; Forsgren, S.; Thorsen, K.; Lorentzon, R. In vivo microdialysis and immunohistochemical analyses of tendon tissue demonstrated high amounts of free glutamate and glutamate NMDAR1 receptors, but no signs of inflammation, in Jumper’s knee. J. Orthop. Res. 2001, 19, 881–886. [Google Scholar] [CrossRef]
- Zamora, A.J.; Marini, J.F. Tendon and myo-tendinous junction in an overloaded skeletal muscle of the rat. Brain Struct. Funct. 1988, 179, 89–96. [Google Scholar] [CrossRef]
- Andres, B.M.; Murrell, G.A. Treatment of tendonopathy: What works, what does not, and what is on the horizon. Clin. Orthop. Relat. Res. 2008, 466, 1539–1554. [Google Scholar] [CrossRef]
- Bass, L.E. Tendinopathy: Why the Difference Between Tendinitis and Tendinosis Matters. Int. J. Ther. Massage Bodyw. Res. Educ. Pr. 2012, 5, 14–17. [Google Scholar] [CrossRef]
- Kaeding, C.; Best, T.M. Tendinosis: Pathophysiology and nonoperative treatment. Sports Health 2009, 1, 284–292. [Google Scholar] [CrossRef] [PubMed]
- Khan, K.M.; Cook, J.L.; Bonar, F.; Astrom, M. Histopathology of common overuse tendon conditions: Update and implications for clinical management. Sports Med. 1999, 27, 393–408. [Google Scholar] [CrossRef] [PubMed]
- Sofka, C.M.; Adler, R.S.; Positano, R.; Pavlov, H.; Luchs, J.S. Haglund’s Syndrome: Diagnosis and Treatment Using Sonography. HSS J. 2006, 2, 27–29. [Google Scholar] [CrossRef] [PubMed]
- Haglund, P. Beitrag zur Klinik der Achillessehne. Z. Orthop 1927, 49, 49–58. [Google Scholar]
- Vaishya, R.; Agarwal, A.K.; Azizi, A.T.; Vijay, V. Haglund’s Syndrome: A Commonly Seen Mysterious Condition. Cureus 2016, 8, e820. [Google Scholar] [CrossRef]
- Van Dijk, C.N.; Van Sterkenburg, M.N.; Wiegerinck, J.I.; Karlsson, J.; Maffulli, N. Terminology for Achilles tendon related disorders. Knee Surg. Sports Traumatol. Arthrosc. 2011, 19, 835–841. [Google Scholar] [CrossRef]
- Sudoł-Szopińska, I.; Kwiatkowska, B.; Prochorec-Sobieszek, M.; Maśliński, W. Enthesopathies and enthesitis. Part 1. Etiopathogenesis. J. Ultrason. 2015, 15, 72–84. [Google Scholar] [CrossRef]
- Sudoł-Szopińska, I.; Kwiatkowska, B.; Prochorec-Sobieszek, M.; Pracoń, G.; Walentowska-Janowicz, M.; Maslinski, W. Enthesopathies and enthesitis. Part 2: Imaging studies. J. Ultrason. 2015, 15, 196–207. [Google Scholar] [CrossRef]
- Shaibani, A.; Workman, R.; Rothschild, B.M. The significance of enthesopathy as a skeletal phenomenon. Clin. Exp. Rheumatol. 1993, 11, 399–403. [Google Scholar]
- Gencc, H.; Cakit, B.D.; Tuncbilek, I.; Erdem, H.R.; Tuncbilek, I. Ultrasonographic evaluation of tendons and enthesal sites in rheumatoid arthritis: Comparison with ankylosing spondylitis and healthy subjects. Clin. Rheumatol. 2004, 24, 272–277. [Google Scholar] [CrossRef]
- Kaeley, G.S. Enthesitis in psoriatic arthritis (Part 2): Imaging. Rheumatology 2020, 59, i15–i20. [Google Scholar] [CrossRef] [PubMed]
- Maffulli, N.; Denaro, V.; Loppini, M. Letters to the Editor. Foot Ankle Int. 2012, 33, 807–808. [Google Scholar] [CrossRef] [PubMed]
- Bulstra, G.H.; Van Rheenen, T.A.; Scholtes, V.A. Can We Measure the Heel Bump? Radiographic Evaluation of Haglund’s Deformity. J. Foot Ankle Surg. 2015, 54, 338–340. [Google Scholar] [CrossRef] [PubMed]
- Eshed, I.; Bollow, M.; McGonagle, D.G.; Tan, A.L.; Althoff, C.E.; Asbach, P.; Hermann, K.G.A. MRI of enthesitis of the appendicular skeleton in spondyloarthritis. Ann. Rheum. Dis. 2007, 66, 1553–1559. [Google Scholar] [CrossRef] [PubMed]
- Barozzi, L.; Olivieri, I.; De Matteis, M.; Padula, A.; Pavlica, P. Seronegative spondylarthropathies: Imaging of spondylitis, enthesitis and dactylitis. Eur. J. Radiol. 1998, 27, S12–S17. [Google Scholar] [CrossRef]
- Haims, A.H.; Schweitzer, M.E.; Patel, R.S.; Hecht, P.; Wapner, K.L. MR imaging of the Achilles tendon: Overlap of findings in symptomatic and asymptomatic individuals. Skelet. Radiol. 2000, 29, 640–645. [Google Scholar] [CrossRef]
- Olivieri, I.; Gemignani, G.; Bini, C.; Grassi, L.; Pasero, G. Diffuse Achilles tendon thickening in juvenile onset seronegative HLA-B27 positive spondyloarthropathy. J. Rheumatol. 1988, 15, 381–382. [Google Scholar]
- Olivieri, I.; Barozzi, L.; Padula, A.; De Matteis, M.; Pierro, A.; Cantini, F.; Salvarani, C.; Pavlica, P. Retrocalcaneal bursitis in spondyloarthropathy: Assessment by ultrasonography and magnetic resonance imaging. J. Rheumatol. 1998, 25, 1352–1357. [Google Scholar]
- Weinreb, J.H.; Sheth, C.; Apostolakos, J.; McCarthy, M.-B.; Barden, B.; Cote, M.P.; Mazzocca, A.D. Tendon structure, disease, and imaging. Muscle Ligaments Tendons J. 2019, 4, 66–73. [Google Scholar] [CrossRef]
- Ring, E.F.J.; Ammer, K. Infrared thermal imaging in medicine. Physiol. Meas. 2012, 33, R33–R46. [Google Scholar] [CrossRef]
- Hildebrandt, C.; Raschner, C.; Ammer, K. An Overview of Recent Application of Medical Infrared Thermography in Sports Medicine in Austria. Sensors 2010, 10, 4700–4715. [Google Scholar] [CrossRef] [PubMed]
- Hoksrud, A.; Ohberg, L.; Alfredson, H.; Bahr, R. Color doppler ultrasound findings in patellar tendinopathy (jumper’s knee). Am. J. Sports Med. 2008, 36, 1813–1820. [Google Scholar] [CrossRef] [PubMed]
- Chaudhry, S.; Fernando, R.; Screen, H.; Waugh, C.; Tucker, A.; Morrissey, D. The use of medical infrared thermography in the detection of tendinopathy: A systematic review. Phys. Ther. Rev. 2016, 21, 75–82. [Google Scholar] [CrossRef]
- Sanz-López, F.; Martínez-Amat, A.; Hita-Contreras, F.; Valero-Campo, C.; Berzosa, C. Thermographic Assessment of Eccentric Overload Training Within Three Days of a Running Session. J. Strength Cond. Res. 2016, 30, 504–511. [Google Scholar] [CrossRef]
- Kannus, P. Etiology and pathophysiology of chronic tendon disorders in sports. Scand. J. Med. Sci. Sports 1997, 7, 78–85. [Google Scholar] [CrossRef]
- D’Agostino, M.-A.; Breban, M. Ultrasonography in inflammatory joint disease: Why should rheumatologists pay attention? Jt. Bone Spine 2002, 69, 252–255. [Google Scholar] [CrossRef]
- Grassi, W.; Salaffi, F.; Filippucci, E. Ultrasound in rheumatology. Best Pract. Res. Clin. Rheumatol. 2005, 19, 467–485. [Google Scholar] [CrossRef]
- D’Agostino, M.A. Ultrasound imaging in spondyloarthropathies. Best Pract. Res. Clin. Rheumatol. 2010, 24, 693–700. [Google Scholar] [CrossRef]
- Grassi, W.; Filippucci, E.; Farina, A.; Cervini, C. Sonographic imaging of tendons. Arthritis Rheum. 2000, 43, 969–976. [Google Scholar] [CrossRef]
- Grechenig, W.; Clement, H.; Bratschitsch, G.; Fankhauser, F.; Peicha, G. Sonographische Achillessehnendiagnostik [Ultrasound diagnosis of the Achilles tendon]. Orthopade 2002, 31, 319–325. [Google Scholar] [CrossRef]
- Carroll, M.; Dalbeth, N.; Boocock, M.; Rome, K. The assessment of lesions of the Achilles tendon by ultrasound imaging in inflammatory arthritis: A systematic review and meta-analysis. Semin. Arthritis Rheum. 2015, 45, 103–114. [Google Scholar] [CrossRef] [PubMed]
- Paavola, M.; Paakkala, T.; Kannus, P.; Järvinen, M. Ultrasonography in the differential diagnosis of Achilles tendon injuries and related disorders. A comparison between pre-operative ultrasonography and surgical findings. Acta Radiol. 1998, 39, 612–619. [Google Scholar] [CrossRef] [PubMed]
- Terslev, L.; Naredo, E.; Iagnocco, A.; Balint, P.V.; Wakefield, R.J.; Aegerter, P.; Aydin, S.Z.; Bachta, A.; Hammer, H.B.; Bruyn, G.A.W.; et al. Defining Enthesitis in Spondyloarthritis by Ultrasound: Results of a Delphi Process and of a Reliability Reading Exercise. Arthritis Rheum. 2014, 66, 741–748. [Google Scholar] [CrossRef] [PubMed]
- Gandjbakhch, F.; Terslev, L.; Joshua, F.; Wakefield, R.J.; Naredo, E.; D’Agostino, M.-A.; Force, O.U.T. Ultrasound in the evaluation of enthesitis: Status and perspectives. Arthritis Res. Ther. 2011, 13, R188. [Google Scholar] [CrossRef] [PubMed]
- Hodgson, R.J.; O’Connor, P.J.; Grainger, A.J. Tendon and ligament imaging. Br. J. Radiol. 2012, 85, 1157–1172. [Google Scholar] [CrossRef]
- Adler, R.; Sofka, C.M. Percutaneous Ultrasound-Guided Injections in the Musculoskeletal System. Ultrasound Q. 2003, 19, 3–12. [Google Scholar] [CrossRef]
- Kainberger, F.M.; Engel, A.; Barton, P.; Huebsch, P.; Neuhold, A.; Salomonowitz, E. Injury of the Achilles tendon: Diagnosis with sonography. Am. J. Roentgenol. 1990, 155, 1031–1036. [Google Scholar] [CrossRef]
- Bigeleisen, P.E. (Ed.) Ultrasound-Guided Regional Anesthesia and Pain Medicine; Lippincott Williams and Wilkins: London, UK, 2010. [Google Scholar]
- El-Khalek, A.M.A.; Borga, M.; El-Essawya, S.; El Sallab, R.M.; Ezzata, A. Role of ultrasonography in the evaluation of Achilles tendon disorders. Benha Med. J. 2016, 33, 54. [Google Scholar] [CrossRef]
- Robinson, P. Sonography of Common Tendon Injuries. Am. J. Roentgenol. 2009, 193, 607–618. [Google Scholar] [CrossRef]
- Paavola, M.; Kannus, P.; Järvinen, T. Achilles tendonopathy. J. Bone Jt. Surg. 2002, 84, 2062–2076. [Google Scholar] [CrossRef]
- Li, H.Y.; Hua, Y.H. Achilles Tendonopathy: Current Concepts about the Basic Science and Clinical Treatments. Biomed. Res. Int. 2016, 2016, 6492597. [Google Scholar] [CrossRef] [PubMed]
- Wiegerinck, J.I.; Kerkhoffs, G.M.; van Sterkenburg, M.N.; Sierevelt, I.N.; van Dijk, C.N. Treatment for insertional Achilles tendonopathy: A systematic review. Knee Surg. Sport Traumatol. Arthrosc. 2013, 21, 1345–1355. [Google Scholar] [CrossRef] [PubMed]
- Jonsson, P.; Lorentzon, R. Chronic Achilles tendon pain treated with eccentric calf-muscle training. Knee Surg. Sports Traumatol. Arthrosc. 2003, 11, 327–333. [Google Scholar] [CrossRef]
- Mafi, N.; Lorentzon, R.; Alfredson, H. Superior short-term results with eccentric calf muscle training compared to concentric training in a randomized prospective multicenter study on patients with chronic Achilles tendinosis. Knee Surg. Sports Traumatol. Arthrosc. 2000, 9, 42–47. [Google Scholar] [CrossRef]
- Nicholson, C.W.; Berlet, G.C.; Lee, T.H. Prediction of the Success of Nonoperative Treatment of Insertional Achilles Tendinosis Based on MRI. Foot Ankle Int. 2007, 28, 472–477. [Google Scholar] [CrossRef]
- Khan, K.M.; Forster, B.B.; Robinson, J.; Cheong, Y.; Louis, L.; MacLean, L.E.; Taunton, J. Are ultrasound and magnetic resonance imaging of value in assessment of Achilles tendon disorders? A two year prospective study. Br. J. Sports Med. 2003, 37, 149–153. [Google Scholar] [CrossRef]
- Hirji, Z.; Hunjun, J.S.; Choudur, H.N. Imaging of the Bursae. J. Clin. Imaging Sci. 2011, 1, 22. [Google Scholar] [CrossRef]
- McNally, E.G. Practical Musculoskeletal Ultrasound, 2nd ed.; Elsievier: Amsterdam, The Netherlands, 2014. [Google Scholar]
- Brinckmann, P.; Frobin, F.; Leivseth, G. Musculoskeletal Biomechanics; Thieme: New York, NY, USA, 2002. [Google Scholar]
- Berg, K.; Peck, J.; Boulger, C.; Bahner, D.P. Patellar tendon rupture: An ultrasound case report. BMJ Case Rep. 2013, 2013, bcr2012008189. [Google Scholar] [CrossRef]
- Aagesen, A.L.; Melek, M. Choosing the Right Diagnostic Imaging Modality in Musculoskeletal Diagnosis. Prim. Care Clin. Off. Pr. 2013, 40, 849–861. [Google Scholar] [CrossRef]
- O’Connor, P.J.; Grainger, A.J.; Morgan, S.R.; Smith, K.L.; Waterton, J.C.; Nash, A.F.P. Ultrasound assessment of tendons in asymptomatic volunteers: A study of reproducibility. Eur. Radiol. 2004, 14, 1968–1973. [Google Scholar] [CrossRef]
- Ricci, V.; Soylu, A.R.; Özçakar, L. Artifacts and Artistic Facts. Am. J. Phys. Med. Rehabil. 2019, 98, 521–525. [Google Scholar] [CrossRef] [PubMed]
- Baad, M.; Lu, Z.F.; Reiser, I.; Paushter, D. Clinical Significance of US Artifacts. Radiographics 2017, 37, 1408–1423. [Google Scholar] [CrossRef] [PubMed]
- Fornage, B.D. The hypoechoic normal tendon. A pitfall. J. Ultrasound Med. 1987, 6, 19–22. [Google Scholar] [CrossRef] [PubMed]
- Wu, W.-T.; Chang, K.-V.; Hsu, Y.-C.; Hsu, P.-C.; Ricci, V.; Özçakar, L. Artifacts in Musculoskeletal Ultrasonography: From Physics to Clinics. Diagnostics 2020, 10, 645. [Google Scholar] [CrossRef] [PubMed]
- De Miguel, E.; Muñoz-Fernández, S.; Castillo, C.; Cobo-Ibáñez, T.; Martín-Mola, E. Diagnostic accuracy of enthesis ultrasound in the diagnosis of early spondyloarthritis. Ann. Rheum. Dis. 2010, 70, 434–439. [Google Scholar] [CrossRef]
- Czyrny, Z. Diagnostic anatomy and diagnostics of enthesal pathologies of the rotator cuff. J. Ultrason. 2012, 12, 178–187. [Google Scholar] [CrossRef]
- Dębek, A.; Nowicki, P.; Czyrny, Z. Ultrasonographic diagnostics of pain in the lateral cubital compartment and proximal forearm. J. Ultrason. 2012, 12, 188–201. [Google Scholar] [CrossRef][Green Version]
- Feydy, A.; Lavie-Brion, M.-C.; Gossec, L.; Lavie, F.; Guerini, H.; Nguyen, C.; Rannou, F.; Drapé, J.-L.; Dougados, M. Comparative study of MRI and power Doppler ultrasonography of the heel in patients with spondyloarthritis with and without heel pain and in controls. Ann. Rheum. Dis. 2011, 71, 498–503. [Google Scholar] [CrossRef]
- Czyrny, Z. Sonographic and histological appearance of heel enthesopathy, what the “heel spurs” really are and what are their consequences. J. Ortop. Trauma Surg. Relat. Res. 2010, 2, 23–36. [Google Scholar]
- Maffulli, N.; Kader, D. Tendonopathy of tendo Achillis. J. Bone Jt. Surg. 2002, 84, 1–8. [Google Scholar] [CrossRef]
- D’Agostino, M.A.; Aegerter, P.; Jousse-Joulin, S.; Chary-Valckenaere, I.; Lecoq, B.; Gaudin, P.; Brault, I.; Schmitz, J.; Dehaut, F.-X.; Le Parc, J.-M.; et al. How to evaluate and improve the reliability of power Doppler ultrasonography for assessing enthesitis in spondyloarthritis. Arthritis Rheum. 2009, 61, 61–69. [Google Scholar] [CrossRef] [PubMed]
- Poulain, C.; D’Agostino, M.A.; Thibault, S.; Daures, J.P.; Ferkal, S.; Le Corvoisier, P.; Rahmouni, A.; Loeuille, D.; Dougados, M.; Claudepierre, P. Can power Doppler ultrasound of the entheses help in classifying recent axial spondyloarthritis? Data from the DESIR cohort. RMD Open 2018, 4, e000686. [Google Scholar] [CrossRef] [PubMed]
- Filippucci, E.; Aydin, S.Z.; Karadag, O.; Salaffi, F.; Gutierrez, M.; Direskeneli, H.; Grassi, W. Reliability of high-resolution ultrasonography in the assessment of Achilles tendon enthesopathy in seronegative spondyloarthropathies. Ann. Rheum. Dis. 2009, 68, 1850–1855. [Google Scholar] [CrossRef] [PubMed]
- De Miguel, E.; Cobo, T.; Rubio-Muñoz, P.; Naredo, E.; Usón, J.; Acebes, J.C.; Andréu, J.L.; Martín-Mola, E. Validity of enthesis ultrasound assessment in spondyloarthropathy. Ann. Rheum. Dis. 2008, 68, 169–174. [Google Scholar] [CrossRef] [PubMed]
- Kiris, A.; Kaya, A.; Ozgocmen, S.; Kocakoc, E. Assessment of enthesitis in ankylosing spondylitis by power Doppler ultrasonography. Skelet. Radiol. 2006, 35, 522–528. [Google Scholar] [CrossRef]
- Ahmed, M.M.; Elolemy, G.G.; Alfeeli, A.K.; Baqer, A.B.; Gad, A.M. Ultrasonographic Enthesopathy and Disease Activity in Psoriatic Arthritis. Open Access Maced. J. Med Sci. 2017, 5, 651–656. [Google Scholar] [CrossRef]
- Helliwell, P.S.; Fitzgerald, O.; Fransen, J.; Gladman, D.D.; Kreuger, G.G.; Duffin, K.C.; McHugh, N.; Mease, P.; Strand, V.; Waxman, R.; et al. The development of candidate composite disease activity and responder indices for psoriatic arthritis (GRACE project). Ann. Rheum. Dis. 2012, 72, 986–991. [Google Scholar] [CrossRef]
- Alcalde, M.; Acebes, J.C.; Cruz, M.; González-Hombrado, L.; Herrero-Beaumont, G.; Sánchez-Pernaute, O. A Sonographic Enthesitic Index of lower limbs is a valuable tool in the assessment of ankylosing spondylitis. Ann. Rheum. Dis. 2007, 66, 1015–1019. [Google Scholar] [CrossRef]
- Kaeley, G.S.; Eder, L.; Aydin, S.Z.; Gutierrez, M.; Bakewell, C. Enthesitis: A hallmark of psoriatic arthritis. Semin. Arthritis Rheum. 2018, 48, 35–43. [Google Scholar] [CrossRef]
- Gisondi, P.; Tinazzi, I.; El-Dalati, G.; Gallo, M.; Biasi, D.; Barbara, L.M.; Girolomoni, G. Lower limb enthesopathy in patients with psoriasis without clinical signs of arthropathy: A hospital-based case-control study. Ann. Rheum. Dis. 2008, 67, 26–30. [Google Scholar] [CrossRef]
- Eder, L.; Jayakar, J.; Thavaneswaran, A.; Haddad, A.; Chandran, V.; Salonen, D.; Rosen, C.F.; Gladman, D.D. Is the Madrid Sonographic Enthesitis Index Useful for Differentiating Psoriatic Arthritis from Psoriasis Alone and Healthy Controls? J. Rheumatol. 2014, 41, 466–472. [Google Scholar] [CrossRef]
- Aydin, S.Z.; Can, M.; Alibaz-Oner, F.; Keser, G.; Kurum, E.; Inal, V.; Yazisiz, V.; Birlik, M.; Emmungil, H.; Atagunduz, P.; et al. A relationship between spinal new bone formation in ankylosing spondylitis and the sonographically determined Achilles tendon enthesophytes. Rheumatol. Int. 2016, 36, 397–404. [Google Scholar] [CrossRef] [PubMed]
- Aydin, S.Z.; Filippucci, E.; Atagunduz, P.; Yavuz, S.; Grassi, W.; Direskeneli, H.; Aydin, S.Z. Sonographic measurement of Achilles tendon thickness in seronegative spondyloarthropathies. Eur. J. Rheumatol. 2014, 1, 7–10. [Google Scholar] [CrossRef] [PubMed]
- Boezaart, A.P.; Ihnatsenka, B. Ultrasound: Basic understanding and learning the language. Int. J. Shoulder Surg. 2010, 4, 55–62. [Google Scholar] [CrossRef] [PubMed]
- Thoirs, K.A.; Childs, J.T. Are Ultrasound Measurements of Achilles Tendon Size Reliable? A Systematic Review of Rater Reliability. Ultrasound Med. Biol. 2018, 44, 2476–2491. [Google Scholar] [CrossRef] [PubMed]
- Patel, N.N.; Labib, S.A. The Achilles Tendon in Healthy Subjects: An Anthropometric and Ultrasound Mapping Study. J. Foot Ankle Surg. 2018, 57, 285–288. [Google Scholar] [CrossRef] [PubMed]
- Holmes, G.B.; Lin, J. Etiologic factors associated with symptomatic Achilles tendonopathy. Foot Ankle Int. 2006, 27, 952–959. [Google Scholar] [CrossRef]
- Gaida, J.E.; Alfredson, L.; Kiss, Z.S.; Wilson, A.; Alfredson, H.; Cook, J. Dyslipidemia in Achilles tendonopathy is characteristic of insulin resistance. Med. Sci. Sports Exerc. 2009, 41, 1194–1197. [Google Scholar] [CrossRef]
- Franceschi, F.; Papalia, R.; Paciotti, M.; Franceschetti, E.; Di Martino, A.; Maffulli, N.; Denaro, V. Obesity as a risk factor for tendonopathy: A systematic review. Int. J. Endocrinol. 2014, 1, 10. [Google Scholar]
- Scott, R.T.; Hyer, C.F.; Granata, A. The correlation of Achilles tendonopathy and body mass index. Foot Ankle Spec. 2013, 6, 283–285. [Google Scholar] [CrossRef]
- Mokone, G.G.; Schwellnus, M.P.; Noakes, T.D.; Collins, M. The COL5A1 gene and Achilles tendon pathology. Scand. J. Med. Sci. Sports 2006, 16, 19–26. [Google Scholar] [CrossRef]
- Mokone, G.G.; Gajjar, M.; September, A.V.; Schwellnus, M.P.; Greenberg, J.; Noakes, T.D.; Collins, M. The Guanine-Thymine Dinucleotide Repeat Polymorphism within the Tenascin-C Gene is Associated with Achilles Tendon Injuries. Am. J. Sports Med. 2005, 33, 1016–1021. [Google Scholar] [CrossRef] [PubMed]
- Raleigh, S.M.; van der Merwe, L.; Ribbans, W.J.; Smith, R.K.; Schwellnus, M.P.; Collins, M. Variants within the MMP3 gene are associated with Achilles tendonopathy: Possible interaction with the COL5A1 gene. Br. J. Sports Med. 2009, 43, 514–520. [Google Scholar] [CrossRef] [PubMed]
- Cheng, Y.; Zhang, J.; Cai, Y. Utility of ultrasonography in assessing the effectiveness of extracorporeal shock wave therapy in insertional Achilles tendonopathy. BioMed Res. Int. 2016, 2016, 2580969. [Google Scholar] [CrossRef] [PubMed]
- Johansson, K.; Sarimo, J.J.; Lempainen, L.L.; Laitala-Leinonen, T.; Orava, S.Y. Calcific spurs at the insertion of the Achilles tendon: A clinical and histological study. Muscle Ligaments Tendons J. 2013, 2, 273–277. [Google Scholar]
- Buchanan, B.K.; DeLuca, J.P.; Lammlein, K.P. Technical Innovation Case Report: Ultrasound-Guided Prolotherapy Injection for Insertional Achilles Calcific Tendinosis. Case Reports Orthop. 2016, 2016, 1560161. [Google Scholar] [CrossRef]
- Lee, K.S.; Rosas, H.; Craig, J. Musculoskeletal Ultrasound: Elbow Imaging and Procedures. Semin. Musculoskelet. Radiol. 2010, 14, 449–460. [Google Scholar] [CrossRef]
- Martín-Hervás, C.; Romero, J.; Navas-Acién, A.; Reboiras, J.J.; Munuera, L. Ultrasonographic and magnetic resonance images of rotator cuff lesions compared with arthroscopy or open surgery findings. J. Shoulder Elb. Surg. 2001, 10, 410–415. [Google Scholar] [CrossRef]
- Williams, C.H.; Sternard, B.T. Bursitis. [Updated 2020 Aug 15]. In StatPearls [Internet]; StatPearls Publishing: Treasure Island, FL, USA, 2020. Available online: https://www.ncbi.nlm.nih.gov/books/NBK513340/ (accessed on 12 September 2020).
- InformedHealth.org [Internet]. Cologne, Germany: Institute for Quality and Efficiency in Health Care (IQWiG). 2006; Bursitis: Overview. 26 July 2018. Available online: https://www.ncbi.nlm.nih.gov/books/NBK525773/# (accessed on 12 September 2020).
- Schmidt, W.A.; Schmidt, H.; Schicke, B.; Gromnica-Ihle, E. Standard reference values for musculoskeletal ultrasonography. Ann. Rheum. Dis. 2004, 63, 988–994. [Google Scholar] [CrossRef]
- Hartgerink, P.; Fessell, D.P.; Jacobson, J.A.; Van Holsbeeck, M.T. Full-versus Partial-Thickness Achilles Tendon Tears: Sonographic Accuracy and Characterization in 26 Cases with Surgical Correlation. Radiology 2001, 220, 406–412. [Google Scholar] [CrossRef]
- Martinoli, C.E.; Derchi, L.; Pastorino, C.; Bertolotto, M.; Silvestri, E. Analysis of echotexture of tendons with US. Radiology 1993, 186, 839–843. [Google Scholar] [CrossRef] [PubMed]
- Asplund, C.A.; Best, T.M. Achilles tendon disorders. BMJ 2013, 346, f1262. [Google Scholar] [CrossRef] [PubMed]
- Agur, A. Grant’s Atlas of Anatomy, 9th ed.; Williams and Wilkins: Baltimore, MD, USA, 1991. [Google Scholar]
- Robinson, P.; White, L.M. The Biomechanics and Imaging of Soccer Injuries. Semin. Musculoskelet. Radiol. 2005, 9, 397–420. [Google Scholar] [CrossRef] [PubMed]
- Teitz, C.C.; Garrett, W.E.J.; Miniaci, A.; Lee, M.H.; Mann, R.A. Tendon Problems in Athletic Individuals. J. Bone Jt. Surg. Am. Vol. 1997, 79, 138–152. [Google Scholar] [CrossRef]
- Scheller, A.D.; Kasser, J.R.; Quigley, T.B. Tendon injuries about the ankle. Orthop. Clin. N. Am. 1980, 11, 801–811. [Google Scholar]
- Rees, J.; Maffulli, N.; Cook, J. Management of tendonopathy. Am. J. Sports Med. 2009, 37, 1855–1867. [Google Scholar] [CrossRef]
- Stecco, A.; Busoni, F.; Stecco, C.; Mattioli-Belmonte, M.; Soldani, P.; Condino, S.; Ermolao, A.; Zaccaria, M.; Gesi, M. Comparative ultrasonographic evaluation of the Achilles paratenon in symptomatic and asymptomatic subjects: An imaging study. Surg. Radiol. Anat. 2014, 37, 281–285. [Google Scholar] [CrossRef]
- Goodwin, D.W. Imaging of the Achilles’ tendon. Foot Ankle Clin. 2000, 5, 135–148. [Google Scholar]
- Waitches, G.M.; Rockett, M.; Brage, M.; Sudakoff, G. Ultrasonographic-surgical correlation of ankle tendon tears. J. Ultrasound Med. 1998, 17, 249–256. [Google Scholar] [CrossRef]
- Griffin, M.J.; Olson, K.; Heckmann, N.; Charlton, T.P. Realtime Achilles Ultrasound Thompson (RAUT) Test for the Evaluation and Diagnosis of Acute Achilles Tendon Ruptures. Foot Ankle Int. 2016, 38, 36–40. [Google Scholar] [CrossRef]
- Grechenig, W.; Clement, H.G.; Fellinger, M. Value of ultrasound imaging of the Achilles tendon in traumatology. Radiologe 1997, 37, 322–329. [Google Scholar] [CrossRef] [PubMed]
- Margetic, P.; Miklić, D.; Rakić-Ersek, V.; Doko, Z.; Lubina, Z.I.; Brkljacić, B. Comparison of ultrasonographic and intraoperative findings in Achilles tendon rupture. Coll. Antropol. 2007, 31, 279–284. [Google Scholar] [PubMed]
- Hess, G.W. Achilles tendon rupture: A review of etiology, population, anatomy, risk factors, and injury prevention. Foot Ankle Spec. 2010, 3, 29–32. [Google Scholar] [CrossRef] [PubMed]
- Zabraniecki, L.; Negrier, I.; Vergne, P.; Arnaud, M.; Bonnet, C.; Bertin, P.; Treves, R. Fluoroquinolone induced tendonopathy: Report of 6 cases. J. Rheumatol. 1996, 23, 516–520. [Google Scholar] [PubMed]
- Aström, M. Partial rupture in chronic Achilles tendonopathy. A retrospective analysis of 342 cases. Acta Orthop. Scand. 1998, 69, 404–407. [Google Scholar] [CrossRef] [PubMed]
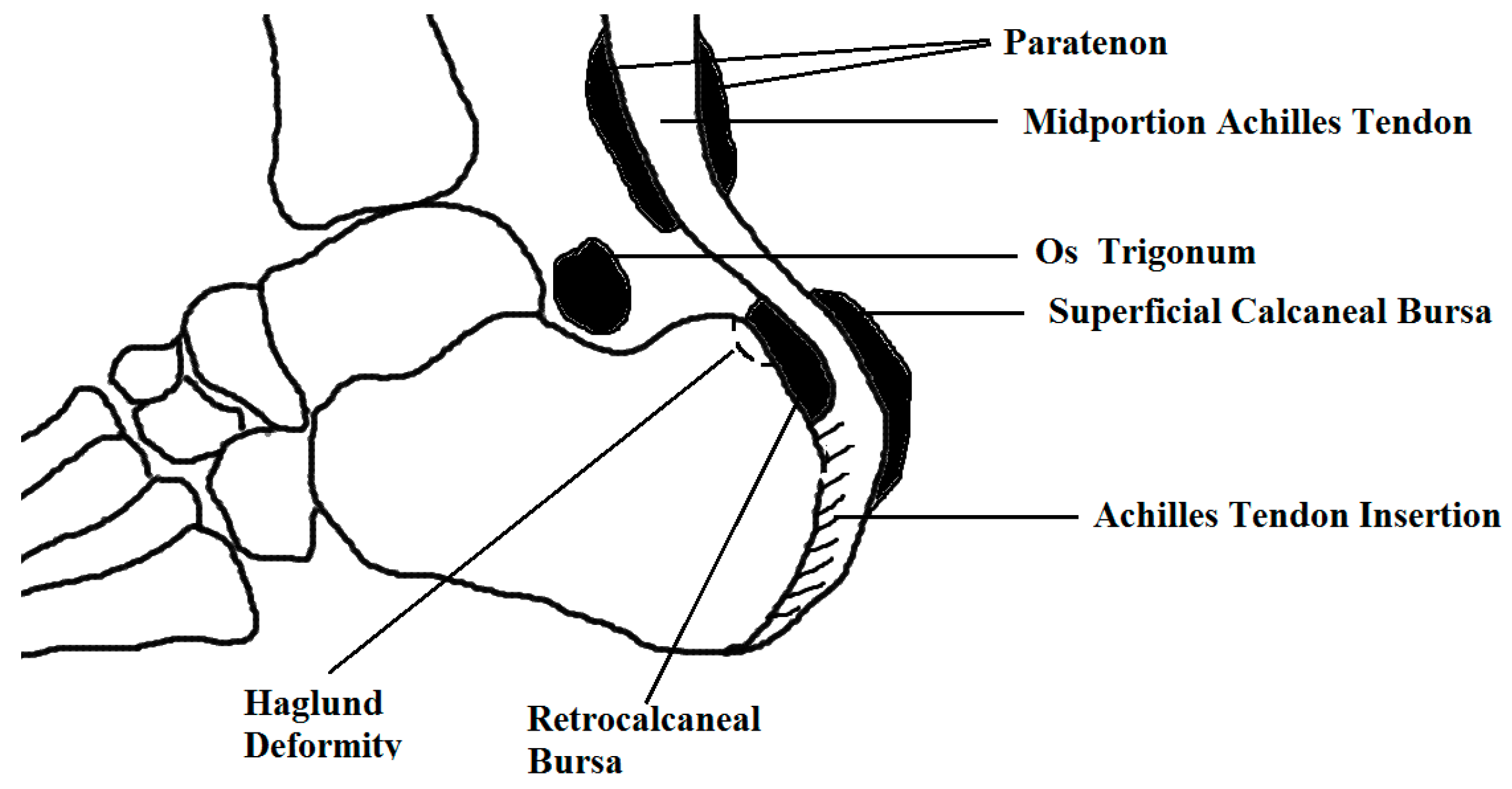
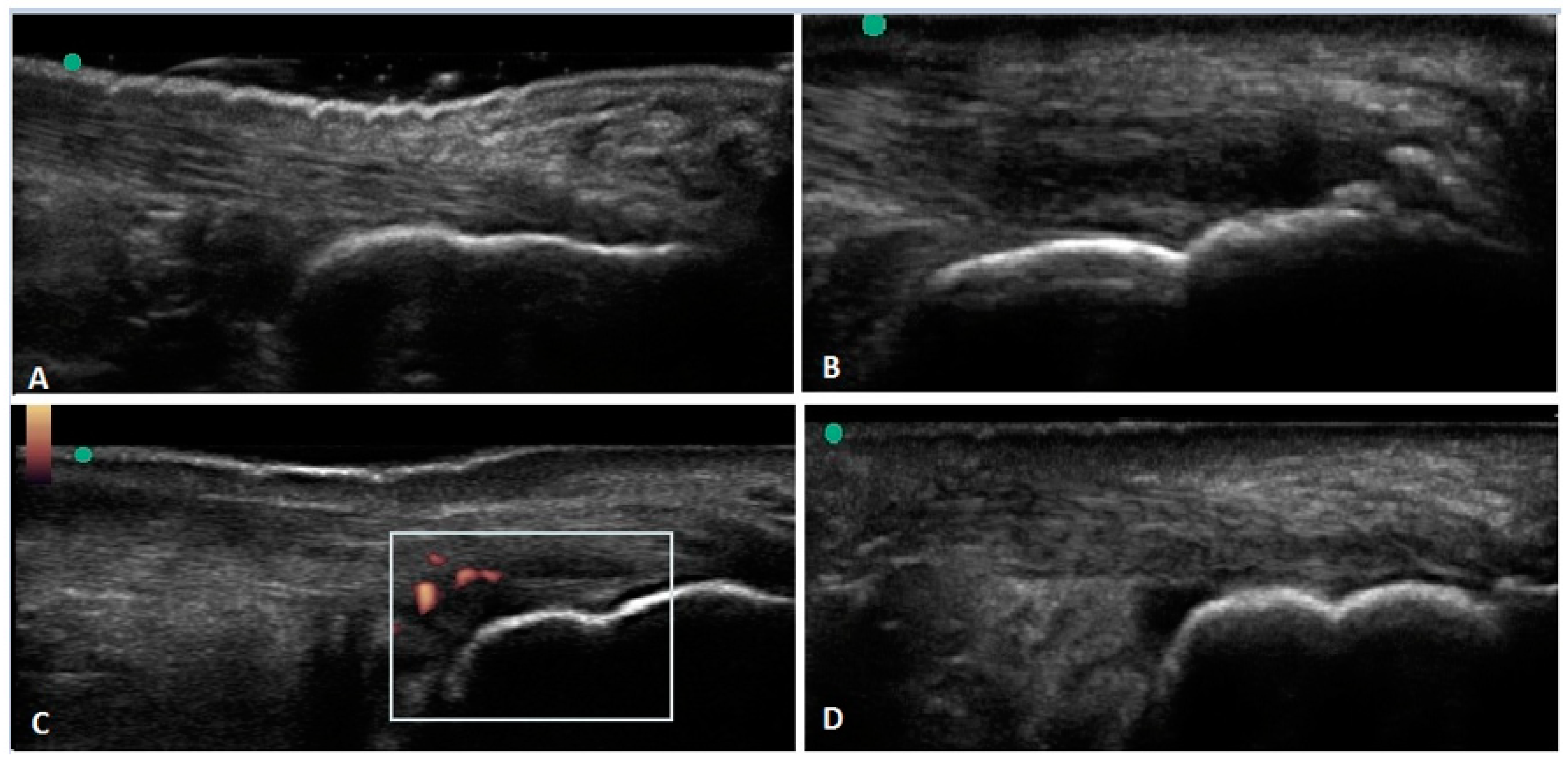
| Differential Diagnoses for Conditions of the Achilles Region |
|---|
| Midportion Achilles tendonopathy |
| Insertional Achilles tendonopathy * |
| Achilles paratenonopathy |
| Midportion Achilles calcific tendonopathy |
| Insertional Achilles calcific tendonopathy * |
| Enthesopathy |
| Retrocalcaneal bursitis *,¶ |
| Superficial calcaneal bursitis |
| Os trigonum syndrome |
| Tophaceous gout |
| Calcium pyrophosphate deposition disease |
| Achilles tendon xanthomata |
| Ruptured gastrocnemius |
| Ruptured plantaris |
| Ruptured popliteal cyst with extravasation down gastrocnemius |
| Calcaneal ossification (also known as Haglund deformity) ¶ |
| Condition | Ultrasound Findings | References |
|---|---|---|
| Enthesopathy |
| [9,10,11,12,66,69] |
| Tendonopathy |
| [70,71,72,73,74,75,76,77,78,79,80,81,82] |
| Bursitis |
| [83] |
| Paratenonopathy |
| [75,84] |
| Tendon tear |
| [75,85,86] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the author. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mascarenhas, S. A Narrative Review of the Classification and Use of Diagnostic Ultrasound for Conditions of the Achilles Tendon. Diagnostics 2020, 10, 944. https://doi.org/10.3390/diagnostics10110944
Mascarenhas S. A Narrative Review of the Classification and Use of Diagnostic Ultrasound for Conditions of the Achilles Tendon. Diagnostics. 2020; 10(11):944. https://doi.org/10.3390/diagnostics10110944
Chicago/Turabian StyleMascarenhas, Sheryl. 2020. "A Narrative Review of the Classification and Use of Diagnostic Ultrasound for Conditions of the Achilles Tendon" Diagnostics 10, no. 11: 944. https://doi.org/10.3390/diagnostics10110944
APA StyleMascarenhas, S. (2020). A Narrative Review of the Classification and Use of Diagnostic Ultrasound for Conditions of the Achilles Tendon. Diagnostics, 10(11), 944. https://doi.org/10.3390/diagnostics10110944




