Microaxial Left Ventricular Assist Device in Cardiogenic Shock: A Systematic Review and Meta-Analysis
Abstract
1. Introduction
2. Methodology
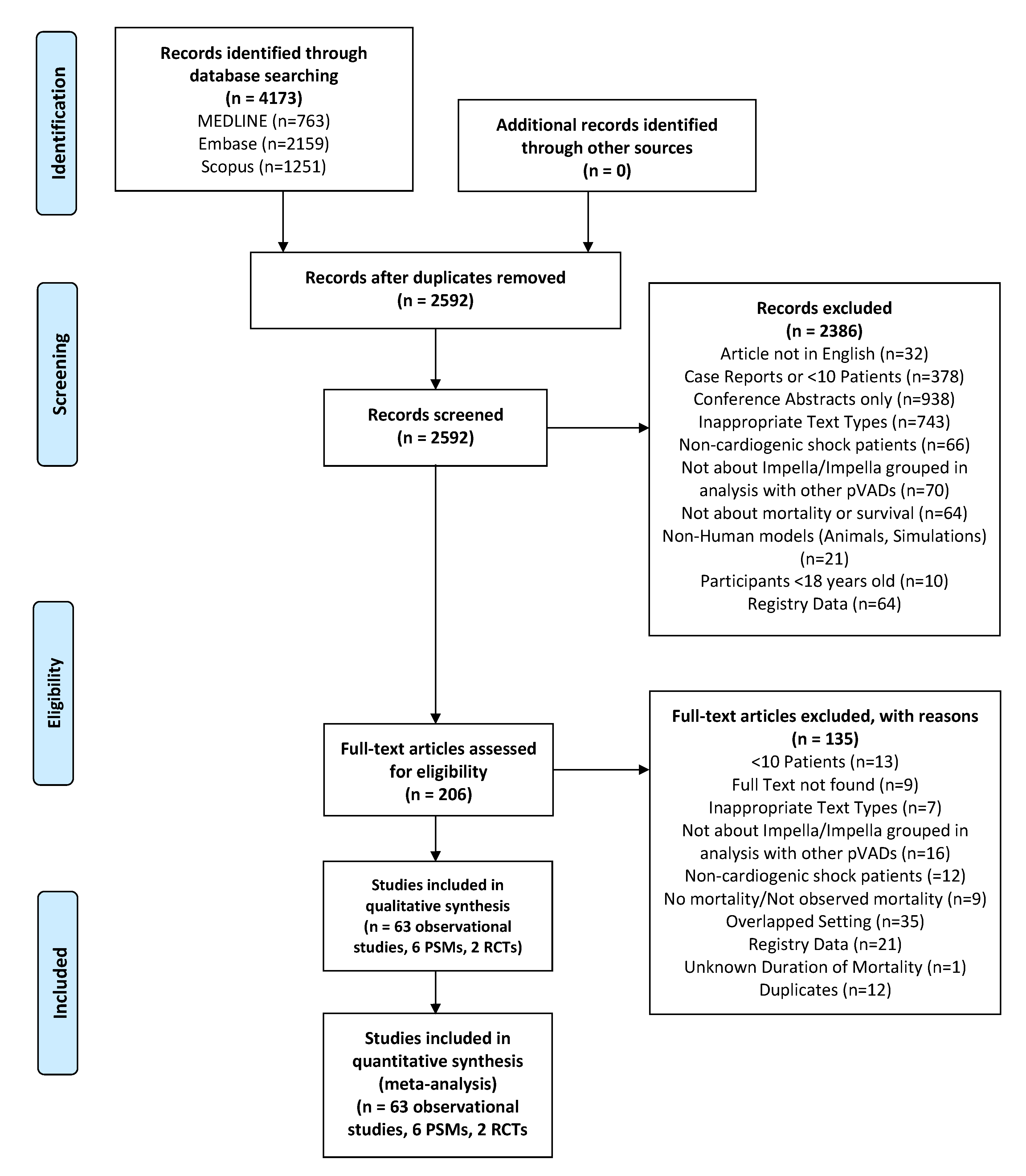
2.1. Search Strategy and Selection Criteria
2.2. Data Extraction
2.3. Risk of Bias and Certainty Assessment
2.4. Outcomes
2.5. Statistical Analysis
2.6. Role of the Funding Source
3. Results
3.1. Demographics of Included Studies
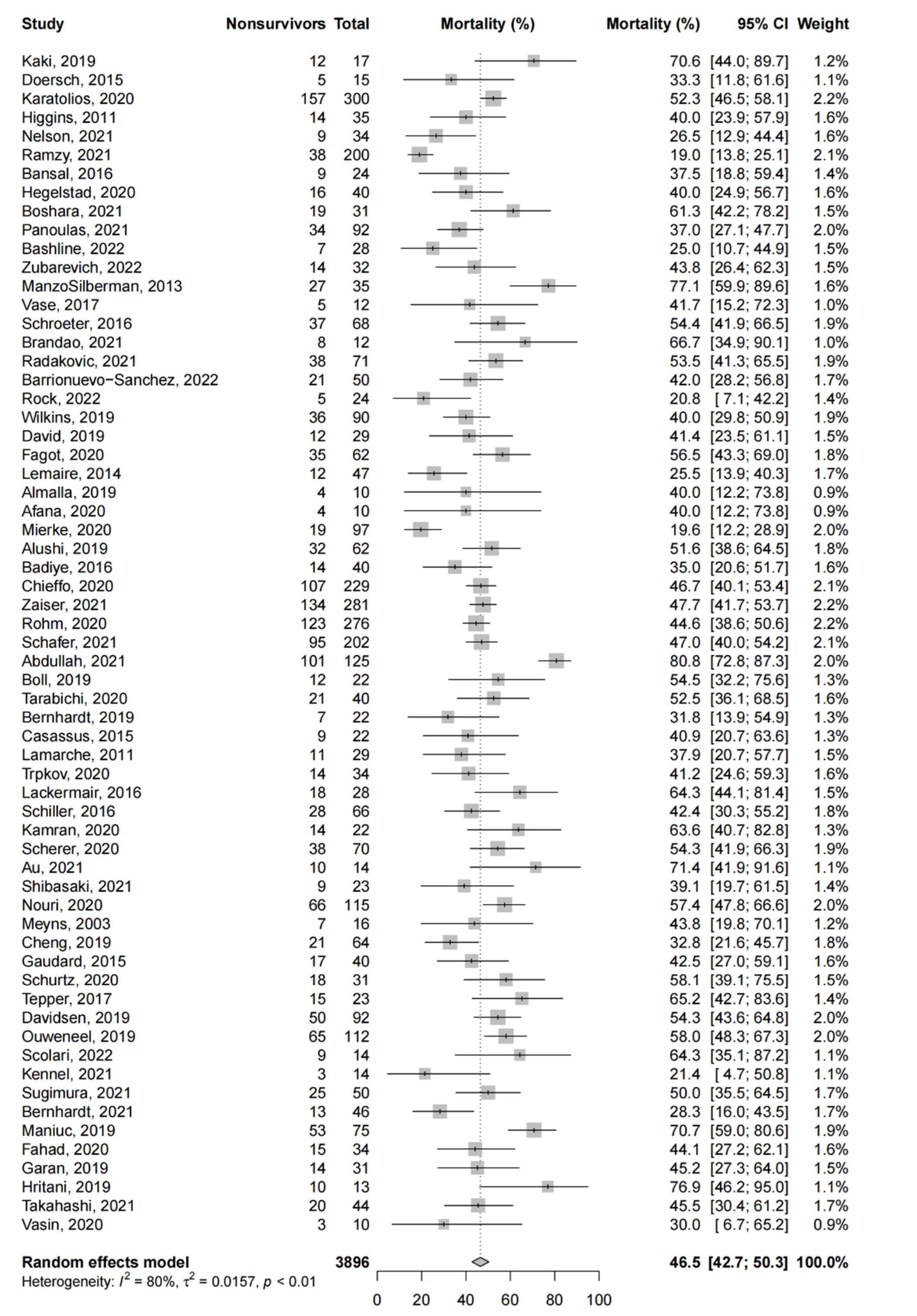
3.2. Primary Meta-Analysis
3.3. Secondary Outcomes
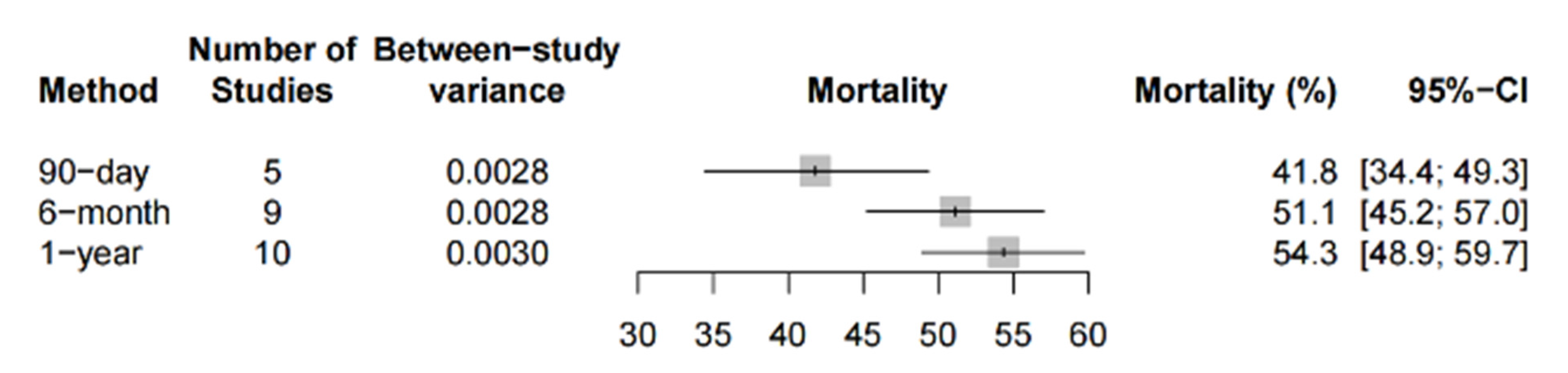
3.3.1. Long-Term Mortality
3.3.2. Complications
3.4. Risk of Bias and Certainty of Evidence Assessment
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Vahdatpour, C.; Collins, D.; Goldberg, S. Cardiogenic shock. J. Am. Heart. Assoc. 2019, 8, e011991. [Google Scholar] [CrossRef] [PubMed]
- Garcia-Garcia, C.; Rueda, F.; Oliveras, T.; Serra, J.; Labata, C.; Ferrer, M.; Bayes-Genis, A. P779 Cardiogenic shock in STEMI patients: Prevalence, management and acute phase mortality over the last three decades. Eur. Heart J. 2018, 39, ehy564.P779. [Google Scholar]
- Goldberg, R.J.; Spencer, F.A.; Gore, J.M.; Lessard, D.; Yarzebski, J. Thirty-year trends (1975 to 2005) in the magnitude of, management of, and hospital death rates associated with cardiogenic shock in patients with acute myocardial infarction: A population-based perspective. Circulation 2009, 119, 1211–1219. [Google Scholar] [CrossRef] [PubMed]
- De Chambrun, M.P.; Donker, D.W.; Combes, A. What’s new in cardiogenic shock? Intensive Care Med. 2020, 46, 1016–1019. [Google Scholar] [CrossRef]
- Baran, D.A.; Grines, C.L.; Bailey, S.; Burkhoff, D.; Hall, S.A.; Henry, T.D.; Hollenberg, S.M.; Kapur, N.K.; O’Neill, W.; Ornato, J.P.; et al. SCAI clinical expert consensus statement on the classification of cardiogenic shock. Catheter. Cardiovasc. Interv. 2019, 94, 29–37. [Google Scholar] [CrossRef]
- Fernando, S.M.; Price, S.; Mathew, R.; Slutsky, A.S.; Combes, A.; Brodie, D. Mechanical circulatory support in the treatment of cardiogenic shock. Curr. Opin. Crit. Care 2022, 28, 434–441. [Google Scholar] [CrossRef]
- Combes, A.; Price, S.; Slutsky, A.S.; Brodie, D. Temporary circulatory support for cardiogenic shock. Lancet 2020, 396, 199–212. [Google Scholar] [CrossRef]
- Shaefi, S.; O’Gara, B.; Kociol, R.; Joynt, K.; Mueller, A.; Nizamuddin, J.; Mahmood, E.; Talmor, D.; Shahul, S. Effect of Cardiogenic Shock Hospital Volume on Mortality in Patients With Cardiogenic Shock. J. Am. Heart Assoc. 2015, 4, e001462. [Google Scholar] [CrossRef]
- Iannaccone, M.; Albani, S.; Giannini, F.; Colangelo, S.; Boccuzzi, G.G.; Garbo, R.; Brilakis, E.S.; D’Ascenzo, F.; de Ferrari, G.M.; Colombo, A. Short term outcomes of Impella in cardiogenic shock: A review and meta-analysis of observational studies. Int. J. Cardiol. 2020, 324, 44–51. [Google Scholar] [CrossRef]
- Thiele, H.; Zeymer, U.; Neumann, F.-J.; Ferenc, M.; Olbrich, H.-G.; Hausleiter, J.; Richardt, G.; Hennersdorf, M.; Empen, K.; Fuernau, G.; et al. Intraaortic Balloon Support for Myocardial Infarction with Cardiogenic Shock. N. Engl. J. Med. 2012, 367, 1287–1296. [Google Scholar] [CrossRef]
- Kapur, N.K.; Jumean, M.F. Defining the Role for Percutaneous Mechanical Circulatory Support Devices for Medically Refractory Heart Failure. Curr. Heart Fail. Rep. 2013, 10, 177–184. [Google Scholar] [CrossRef]
- Smith, L.; Peters, A.; Mazimba, S.; Ragosta, M.; Taylor, A.M. Outcomes of patients with cardiogenic shock treated with TandemHeart® percutaneous ventricular assist device: Importance of support indication and definitive therapies as determinants of prognosis. Catheter. Cardiovasc. Interv. 2018, 92, 1173–1181. [Google Scholar] [CrossRef]
- Lemor, A.; Dehkordi, S.H.H.; Basir, M.B.; Villablanca, P.A.; Jain, T.; Koenig, G.C.; Alaswad, K.; Moses, J.W.; Kapur, N.K.; O’Neill, W. Impella Versus Extracorporeal Membrane Oxygenation for Acute Myocardial Infarction Cardiogenic Shock. Cardiovasc. Revascularization Med. 2020, 21, 1465–1471. [Google Scholar] [CrossRef]
- Cheung, A.W.; White, C.; Davis, M.K.; Freed, D.H. Short-term mechanical circulatory support for recovery from acute right ventricular failure: Clinical outcomes. J. Heart Lung Transplant. 2014, 33, 794–799. [Google Scholar] [CrossRef]
- Anderson, M.B.; Goldstein, J.; Milano, C.; Morris, L.D.; Kormos, R.L.; Bhama, J.; Kapur, N.K.; Bansal, A.; Garcia, J.; Baker, J.N.; et al. Benefits of a novel percutaneous ventricular assist device for right heart failure: The prospective RECOVER RIGHT study of the Impella RP device. J. Heart Lung Transplant. 2015, 34, 1549–1560. [Google Scholar] [CrossRef]
- Bansal, A.; Bhama, J.K.; Patel, R.; Desai, S.; Mandras, S.A.; Patel, H.; Collins, T.; Reilly, J.P.; Ventura, H.O.; Parrino, P.E. Using the Minimally Invasive Impella 5.0 via the Right Subclavian Artery Cutdown for Acute on Chronic Decompensated Heart Failure as a Bridge to Decision. Ochsner J. 2016, 16, 210–216. [Google Scholar]
- Griffith, B.P.; Anderson, M.B.; Samuels, L.E.; Pae Jr, W.E.; Naka, Y.; Frazier, O.H. The RECOVER I: A multicenter prospective study of Impella 5.0/LD for postcardiotomy circulatory support. J. Thorac. Cardiovasc. Surg. 2013, 145, 548–554. [Google Scholar] [CrossRef]
- O’Neill, W.W.; Grines, C.; Schreiber, T.; Moses, J.; Maini, B.; Dixon, S.R.; Ohman, E.M. Analysis of outcomes for 15,259 US patients with acute myocardial infarction cardiogenic shock (AMICS) supported with the Impella device. Am. Heart J. 2018, 202, 33–38. [Google Scholar] [CrossRef]
- Lima, B.; Kale, P.; Gonzalez-Stawinski, G.V.; Kuiper, J.J.; Carey, S.; Hall, S.A. Effectiveness and Safety of the Impella 5.0 as a Bridge to Cardiac Transplantation or Durable Left Ventricular Assist Device. Am. J. Cardiol. 2016, 117, 1622–1628. [Google Scholar] [CrossRef]
- Burkhoff, D.; Sayer, G.; Doshi, D.; Uriel, N. Hemodynamics of mechanical circulatory support. J. Am. Coll. Cardiol. 2015, 66, 2663–2674. [Google Scholar] [CrossRef]
- Burzotta, F.; Russo, G.; Previ, L.; Bruno, P.; Aurigemma, C.; Trani, C. Impella: Pumps overview and access site management. Minerva Cardioangiol. 2018, 66, 606–611. [Google Scholar] [CrossRef]
- Hill, J.; Banning, A.; Burzotta, F.; Chieffo, A.; Schieffer, B.; Schafer, A.; Mstelmaszuk-Zadykowicz, N.; Sun, S.; Spelman, T.; Doshi, S.; et al. A systematic literature review and meta-analysis of impella devices used in cardiogenic shock and high risk percutaneous coronary interventions. Interv. Cardiol. 2019, 11, 163. [Google Scholar] [CrossRef]
- Abiomed, I. Approves Impella 5.0 and Impella LD Extended Duration of Use to 14 Days for Cardiogenic Shock Derived from AMI or Cardiomyopathy; FDA: Silver Spring, MD, USA, 2019. [Google Scholar]
- Vargas, K.G.; Jäger, B.; Kaufmann, C.C.; Biagioli, A.; Watremez, S.; Gatto, F.; Özbek, C.; Razouk, A.; Geppert, A.; Huber, K. Impella in cardiogenic shock following acute myocardial infarction: A systematic review and meta-analysis. Wien. Klin. Wochenschr. 2020, 132, 716–725. [Google Scholar] [CrossRef]
- Page, M.J.; McKenzie, J.E.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetzlaff, J.M.; Akl, E.A.; Brennan, S.E.; et al. The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. Int. J. Surg. 2021, 88, 105906. [Google Scholar] [CrossRef]
- Iorio, A.; Spencer, F.A.; Falavigna, M.; Alba, A.; Lang, E.; Burnand, B.; McGinn, T.; Hayden, J.; Williams, K.; Shea, B.; et al. Use of GRADE for assessment of evidence about prognosis: Rating confidence in estimates of event rates in broad categories of patients. BMJ 2015, 350, h870. [Google Scholar] [CrossRef]
- Balshem, H.; Helfand, M.; Schünemann, H.J.; Oxman, A.D.; Kunz, R.; Brozek, J.; Vist, G.E.; Falck-Ytter, Y.; Meerpohl, J.; Norris, S.; et al. GRADE guidelines: 3. Rating the quality of evidence. J. Clin. Epidemiol. 2011, 64, 401–406. [Google Scholar] [CrossRef]
- Guyatt, G.H.; Oxman, A.D.; Kunz, R.; Woodcock, J.; Brozek, J.; Helfand, M.; GRADE Working Group. GRADE guidelines: 7. Rating the quality of evidence—Inconsistency. J. Clin. Epidemiol. 2011, 64, 1294–1302. [Google Scholar] [CrossRef]
- Lang, R.M.; Badano, L.P.; Mor-Avi, V.; Afilalo, J.; Armstrong, A.; Ernande, L.; Flachskampf, F.A.; Foster, E.; Goldstein, S.A.; Kuznetsova, T.; et al. Recommendations for cardiac chamber quantification by echocardiography in adults: An update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. J. Am. Soc. Echocardiogr. 2015, 28, 1–39.e14. [Google Scholar] [CrossRef]
- Wan, X.; Wang, W.; Liu, J.; Tong, T. Estimating the sample mean and standard deviation from the sample size, median, range and/or interquartile range. BMC Med. Res. Methodol. 2014, 14, 135. [Google Scholar] [CrossRef]
- DerSimonian, R.; Laird, N. Meta-analysis in clinical trials. Control. Clin. Trials 1986, 7, 177–188. [Google Scholar] [CrossRef]
- Clopper, C.J.; Pearson, E.S. The use of confidence or fiducial limits illustrated in the case of the binomial. Biometrika 1934, 26, 404–413. [Google Scholar] [CrossRef]
- Miller, J.J. The inverse of the Freeman–Tukey double arcsine transformation. Am. Stat. 1978, 32, 138. [Google Scholar]
- Austin, P.C. The use of propensity score methods with survival or time-to-event outcomes: Reporting measures of effect similar to those used in randomized experiments. Stat. Med. 2013, 33, 1242–1258. [Google Scholar] [CrossRef] [PubMed]
- Benson, K.; Hartz, A.J. A comparison of observational studies and randomized, controlled trials. N. Engl. J. Med. 2000, 342, 1878–1886. [Google Scholar] [CrossRef]
- Ioannidis, J.P.; Haidich, A.B.; Pappa, M.; Pantazis, N.; Kokori, S.I.; Tektonidou, M.G.; Lau, J. Comparison of evidence of treatment effects in randomized and nonrandomized studies. Jama 2001, 286, 821–830. [Google Scholar] [CrossRef]
- Jia, D.; Yang, I.X.; Ling, R.R.; Syn, N.; Poon, W.H.; Murughan, K.; Ramanathan, K. Vascular complications of extracorporeal membrane oxygenation: A systematic review and meta-regression analysis. Crit. Care Med. 2020, 48, e1269–e1277. [Google Scholar] [CrossRef]
- Afana, M.; Altawil, M.; Basir, M.; Alqarqaz, M.; Alaswad, K.; Eng, M.; O’Neill, W.W.; Lederman, R.J.; Greenbaum, A.B. Transcaval access for the emergency delivery of 5.0 liters per minute mechanical circulatory support in cardiogenic shock. Catheter. Cardiovasc. Interv. 2020, 97, 555–564. [Google Scholar] [CrossRef]
- Almalla, M.; Kersten, A.; Altiok, E.; Marx, N.; Schröder, J.W. Hemodynamic support with Impella ventricular assist device in patients undergoing TAVI: A single center experience. Catheter. Cardiovasc. Interv. 2019, 95, 357–362. [Google Scholar] [CrossRef]
- Alushi, B.; Douedari, A.; Froehlig, G.; Knie, W.; Wurster, T.H.; Leistner, D.M.; Staehli, B.-E.; Mochmann, H.-C.; Pieske, B.; Landmesser, U.; et al. Impella versus IABP in acute myocardial infarction complicated by cardiogenic shock. Open Heart 2019, 6, e000987. [Google Scholar] [CrossRef]
- Au, S.-Y.; Fong, K.-M.; Tsang, C.-F.S.; Chan, K.-C.A.; Wong, C.Y.; Ng, W.-Y.G.; Lee, K.Y.M. Veno-arterial extracorporeal membrane oxygenation with concomitant Impella versus concomitant intra-aortic-balloon-pump for cardiogenic shock. Perfusion 2021, 02676591211033947, online ahead of print. [Google Scholar] [CrossRef]
- Badiye, A.P.; Hernandez, G.A.; Novoa, I.; Chaparro, S.V. Incidence of Hemolysis in Patients with Cardiogenic Shock Treated with Impella Percutaneous Left Ventricular Assist Device. ASAIO J. 2016, 62, 11–14. [Google Scholar] [CrossRef]
- Bernhardt, A.M.; Potapov, E.; Schibilsky, D.; Ruhparwar, A.; Tschöpe, C.; Spillmann, F.; Benk, C.; Schmack, B.; Schmitto, J.D.; Napp, L.C.; et al. First in man evaluation of a novel circulatory support device: Early experience with the Impella 5.5 after CE mark approval in Germany. J. Heart Lung Transplant. 2021, 40, 850–855. [Google Scholar] [CrossRef]
- Bernhardt, A.M.; Zipfel, S.; Reiter, B.; Hakmi, S.; Castro, L.; Söffker, G.; Kluge, S.; Lubos, E.; Rybczinski, M.; Grahn, H.; et al. Impella 5.0 therapy as a bridge-to-decision option for patients on extracorporeal life support with unclear neurological outcomes. Eur. J. Cardio-Thorac. Surg. 2019, 56, 1031–1036. [Google Scholar] [CrossRef]
- Boll, G.; Fischer, A.; Kapur, N.K.; Salehi, P. Right Axillary Artery Conduit Is a Safe and Reliable Access for Implantation of Impella 5.0 Microaxial Pump. Ann. Vasc. Surg. 2018, 54, 54–59. [Google Scholar] [CrossRef]
- Boshara, A.; Patel, A.; Alasaad, M.; Dutcheshen, K.J.; LaLonde, T.A.; Schreiber, T.L.; Mehta, R.H.; Kaki, A.; Rosman, H.S. Cardiogenic Shock Complicating Acute Myocardial Infarction Treated With Percutaneous Coronary Intervention Supported by Impella: Implications of Advanced Age and Refractory Shock on Outcomes. Crit. Care Explor. 2021, 3, e0447. [Google Scholar] [CrossRef]
- Brandão, M.; Caeiro, D.; Pires-Morais, G.; Almeida, J.G.; Teixeira, P.G.; Silva, M.P.; Braga, P. Impella support for cardiogenic shock and high-risk percutaneous coronary intervention: A single-center experience. Rev. Port. Cardiol. 2021, 40, 853–861. [Google Scholar] [CrossRef]
- Casassus, F.; Corre, J.; Leroux, L.; Chevalereau, P.; Fresselinat, A.; Seguy, B.; Calderon, J.; Coste, P.; Ouattara, A.; Roques, X.; et al. The Use of Impella 2.5 in Severe Refractory Cardiogenic Shock Complicating an Acute Myocardial Infarction. J. Interv. Cardiol. 2015, 28, 41–50. [Google Scholar] [CrossRef]
- Cheng, R.; Tank, R.; Ramzy, D.; Azarbal, B.; Chung, J.; Esmailian, F.; Kobashigawa, J.A.; Moriguchi, J.D.; Arabia, F.A. Clinical Outcomes of Impella Microaxial Devices Used to Salvage Cardiogenic Shock as a Bridge to Durable Circulatory Support or Cardiac Transplantation. ASAIO J. 2019, 65, 642–648. [Google Scholar] [CrossRef]
- Chieffo, A.; Ancona, M.B.; Burzotta, F.; Pazzanese, V.; Briguori, C.; Trani, C.; Piva, T.; De Marco, F.; Di Biasi, M.; Pagnotta, P.; et al. Observational multicentre registry of patients treated with IMPella mechanical circulatory support device in ITaly: The IMP-IT registry. EuroIntervention 2020, 15, e1343–e1350. [Google Scholar] [CrossRef]
- David, C.H.; Quessard, A.; Mastroianni, C.; Hekimian, G.; Amour, J.; Leprince, P.; Lebreton, G. Mechanical circulatory support with the Impella 5.0 and the Impella Left Direct pumps for postcardiotomy cardiogenic shock at La Pitié-Salpêtrière Hospital. Eur. J. Cardio-Thorac. Surg. 2020, 57, 183–188. [Google Scholar] [CrossRef]
- Davidsen, C.; Packer, E.J.; Løland, K.H.; Rotevatn, S.; Nygreen, E.L.; Eriksen, E.; Øksnes, A.; Herstad, J.; Haaverstad, R.; Bleie, Ø.; et al. Impella use in acute myocardial infarction complicated by cardiogenic shock and cardiac arrest: Analysis of 10 years registry data. Resuscitation 2019, 140, 178–184. [Google Scholar] [CrossRef]
- Doersch, K.; Tong, C.W.; Gongora, E.; Konda, S.; Sareyyupoglu, B. Temporary Left Ventricular Assist Device Through an Axillary Access is a Promising Approach to Improve Outcomes in Refractory Cardiogenic Shock Patients. ASAIO J. 2015, 61, 253–258. [Google Scholar] [CrossRef]
- Fagot, J.; Bouisset, F.; Bonello, L.; Biendel, C.; Lhermusier, T.; Porterie, J.; Roncalli, J.; Galinier, M.; Elbaz, M.; Lairez, O.; et al. Early Evaluation of Patients on Axial Flow Pump Support for Refractory Cardiogenic Shock is Associated with Left Ventricular Recovery. J. Clin. Med. 2020, 9, 4130. [Google Scholar] [CrossRef]
- Fahad, F.; Shaukat, M.H.S.; Yager, N. Incidence and Outcomes of Acute Kidney Injury Requiring Renal Replacement Therapy in Patients on Percutaneous Mechanical Circulatory Support with Impella-CP for Cardiogenic Shock. Cureus 2020, 12, e6591. [Google Scholar] [CrossRef]
- Garan, A.R.; Takeda, K.; Salna, M.; Vandenberge, J.; Doshi, D.; Karmpaliotis, D.; Kirtane, A.J.; Takayama, H.; Kurlansky, P. Prospective Comparison of a Percutaneous Ventricular Assist Device and Venoarterial Extracorporeal Membrane Oxygenation for Patients With Cardiogenic Shock Following Acute Myocardial Infarction. J. Am. Heart Assoc. 2019, 8, e012171. [Google Scholar] [CrossRef]
- Gaudard, P.; Mourad, M.; Eliet, J.; Zeroual, N.; Culas, G.; Rouvière, P.; Albat, B.; Colson, P. Management and outcome of patients supported with Impella 5.0 for refractory cardiogenic shock. Crit. Care 2015, 19, 363. [Google Scholar] [CrossRef]
- Haurand, J.M.; Haberkorn, S.; Haschemi, J.; Oehler, D.; Aubin, H.; Akhyari, P.; Boeken, U.; Kelm, M.; Westenfeld, R.; Horn, P. Outcome of patients with non-ischaemic cardiogenic shock supported by percutaneous left ventricular assist device. ESC Heart Fail. 2021, 8, 3594–3602. [Google Scholar] [CrossRef]
- Helgestad, O.K.L.; Josiassen, J.; Hassager, C.; Jensen, L.O.; Holmvang, L.; Udesen, N.L.J.; Schmidt, H.; Ravn, H.B.; Moller, J.E. Contemporary trends in use of mechanical circulatory support in patients with acute MI and cardiogenic shock. Open Heart 2020, 7, e001214. [Google Scholar] [CrossRef]
- Higgins, J.; Lamarche, Y.; Kaan, A.; Stevens, L.-M.; Cheung, A. Microaxial Devices for Ventricular Failure: A Multicentre, Population-Based Experience. Can. J. Cardiol. 2011, 27, 725–730. [Google Scholar] [CrossRef]
- Hritani, A.W.; Wani, A.S.; Olet, S.; Lauterbach, C.J.; Allaqaband, S.Q.; Bajwa, T.; Jan, M.F. Secular Trend in the Use and Implementation of Impella in High-Risk Percutaneous Coronary Intervention and Cardiogenic Shock: A Real-World Experience. J. Invasive Cardiol. 2019, 31, E265–E270. [Google Scholar] [PubMed]
- Kaki, A.; Blank, N.; Alraies, M.C.; Jani, A.; Shemesh, A.; Kajy, M.; Laktineh, A.; Hasan, R.; Gade, C.L.; Mohamad, T.; et al. Axillary Artery Access for Mechanical Circulatory Support Devices in Patients With Prohibitive Peripheral Arterial Disease Presenting With Cardiogenic Shock. Am. J. Cardiol. 2019, 123, 1715–1721. [Google Scholar] [CrossRef] [PubMed]
- Kamran, H.; Batra, S.; Venesy, D.M.; Patten, R.D.; Waxman, S.; Pyne, C.; Shah, S.P. Outcomes of Impella CP insertion during cardiac arrest: A single center experience. Resuscitation 2019, 147, 53–56. [Google Scholar] [CrossRef] [PubMed]
- Karatolios, K.; Chatzis, G.; Markus, B.; Luesebrink, U.; Ahrens, H.; Divchev, D.; Syntila, S.; Jerrentrup, A.; Schieffer, B. Comparison of mechanical circulatory support with venoarterial extracorporeal membrane oxygenation or Impella for patients with cardiogenic shock: A propensity-matched analysis. Clin. Res. Cardiol. 2020, 110, 1404–1411. [Google Scholar] [CrossRef] [PubMed]
- Kennel, P.J.; Lumish, H.; Kaku, Y.; Fried, J.; Kirtane, A.J.; Karmpaliotis, D.; Takayama, H.; Naka, Y.; Sayer, G.; Uriel, N.; et al. A case series analysis on the clinical experience of Impella 5.5® at a large tertiary care centre. ESC Heart Fail. 2021, 8, 3720–3725. [Google Scholar] [CrossRef]
- Lackermair, K.; Sattler, S.; Huber, B.; Grabmaier, U.; Weckbach, L.; Bauer, A.; Theiss, H.; Hausleiter, J.; Mehilli, J.; Massberg, S.; et al. Retrospective analysis of circulatory support with the Impella CP® device in patients with therapy refractory cardiogenic shock. Int. J. Cardiol. 2016, 219, 200–203. [Google Scholar] [CrossRef]
- Lamarche, Y.; Cheung, A.; Ignaszewski, A.; Higgins, J.; Kaan, A.; Griesdale, D.; Moss, R. Comparative outcomes in cardiogenic shock patients managed with Impella microaxial pump or extracorporeal life support. J. Thorac. Cardiovasc. Surg. 2010, 142, 60–65. [Google Scholar] [CrossRef]
- Lemaire, A.; Anderson, M.B.; Lee, L.Y.; Scholz, P.; Prendergast, T.; Goodman, A.; Lozano, A.M.; Spotnitz, A.; Batsides, G. The Impella Device for Acute Mechanical Circulatory Support in Patients in Cardiogenic Shock. Ann. Thorac. Surg. 2014, 97, 133–138. [Google Scholar] [CrossRef]
- Maniuc, O.; Salinger, T.; Anders, F.; Müntze, J.; Liu, D.; Hu, K.; Ertl, G.; Frantz, S.; Nordbeck, P. Impella CP use in patients with non-ischaemic cardiogenic shock. ESC Heart Fail. 2019, 6, 863–866. [Google Scholar] [CrossRef]
- Manzo-Silberman, S.; Fichet, J.; Mathonnet, A.; Varenne, O.; Ricome, S.; Chaib, A.; Zuber, B.; Spaulding, C.; Cariou, A. Percutaneous left ventricular assistance in post cardiac arrest shock: Comparison of intra aortic blood pump and IMPELLA Recover LP2.5. Resuscitation 2013, 84, 609–615. [Google Scholar] [CrossRef]
- Meyns, B.; Dens, J.; Sergeant, P.; Herijgers, P.; Daenen, W.; Flameng, W. Initial experiences with the Impella device in patients with cardiogenic shock. Thorac. Cardiovasc. Surg. 2003, 51, 312–317. [Google Scholar]
- Mierke, J.; Loehn, T.; Ende, G.; Jahn, S.; Quick, S.; Speiser, U.; Jellinghaus, S.; Pfluecke, C.; Linke, A.; Ibrahim, K. Percutaneous Left Ventricular Assist Device Leads to Heart Rhythm Stabilisation in Cardiogenic Shock: Results from the Dresden Impella Registry. Heart Lung Circ. 2020, 30, 577–584. [Google Scholar] [CrossRef]
- Nelson, D.W.; Sundararajan, S.; Klein, E.; Joyce, L.D.; Durham, L.A.; Joyce, D.L.; Mohammed, A.A. Sustained Use of the Impella 5.0 Heart Pump Enables Bridge to Clinical Decisions in 34 Patients. Tex. Heart Inst. J. 2021, 48, e207260. [Google Scholar] [CrossRef]
- Nersesian, G.; Potapov, E.V.; Nelki, V.; Stein, J.; Starck, C.; Falk, V.; Schoenrath, F.; Krackhardt, F.; Tschöpe, C.; Spillmann, F. Propensity score-based analysis of 30-day survival in cardiogenic shock patients supported with different microaxial left ventricular assist devices. J. Card. Surg. 2021, 36, 4141–4152. [Google Scholar] [CrossRef]
- Nouri, S.N.; Malick, W.; Masoumi, A.; Fried, J.A.; Topkara, V.K.; Brener, M.I.; Ahmad, Y.; Prasad, M.; Rabbani, L.E.; Takeda, K.; et al. Impella percutaneous left ventricular assist device as mechanical circulatory support for cardiogenic shock: A retrospective analysis from a tertiary academic medical center. Catheter. Cardiovasc. Interv. 2020, 99, 37–47. [Google Scholar] [CrossRef]
- Ouweneel, D.M.; de Brabander, J.; Karami, M.; Sjauw, K.D.; Engström, A.E.; Vis, M.M.; Henriques, J.P. Real-life use of left ventricular circulatory support with Impella in cardiogenic shock after acute myocardial infarction: 12 years AMC experience. Eur. Heart J. Acute Cardiovasc. Care 2019, 8, 338–349. [Google Scholar] [CrossRef]
- Ouweneel, D.M.; Eriksen, E.; Sjauw, K.D.; van Dongen, I.M.; Hirsch, A.; Packer, E.J.; Vis, M.M.; Wykrzykowska, J.J.; Koch, K.T.; Baan, J.; et al. Percutaneous Mechanical Circulatory Support Versus Intra-Aortic Balloon Pump in Cardiogenic Shock After Acute Myocardial Infarction. J. Am. Coll. Cardiol. 2016, 69, 278–287. [Google Scholar] [CrossRef]
- Panoulas, V.; Monteagudo-Vela, M. Predictors of Short-term Survival in Cardiogenic Shock Patients Requiring Left Ventricular Support Using the Impella CP or 5.0. CJC Open 2021, 3, 1002–1009. [Google Scholar] [CrossRef]
- Pappalardo, F.; Schulte, C.; Pieri, M.; Schrage, B.; Contri, R.; Soeffker, G.; Greco, T.; Lembo, R.; Müllerleile, K.; Colombo, A.; et al. Concomitant implantation of Impella® on top of veno-arterial extracorporeal membrane oxygenation may improve survival of patients with cardiogenic shock. Eur. J. Heart Fail. 2016, 19, 404–412. [Google Scholar] [CrossRef]
- Radakovic, D.; Zittermann, A.; Knezevic, A.; Razumov, A.; Opacic, D.; Wienrautner, N.; Flottmann, C.; Rojas, S.V.; Fox, H.; Schramm, R.; et al. Left ventricular unloading during extracorporeal life support for myocardial infarction with cardiogenic shock: Surgical venting versus Impella device. Interact. Cardiovasc. Thorac. Surg. 2021, 34, 137–144. [Google Scholar] [CrossRef]
- Rohm, C.L.; Gadidov, B.; Ray, H.E.; Mannino, S.F.; Prasad, R. Vasopressors and Inotropes as Predictors of Mortality in Acute Severe Cardiogenic Shock Treated With the Impella Device. Cardiovasc. Revascularization Med. 2020, 31, 71–75. [Google Scholar] [CrossRef]
- Schäfer, A.; Westenfeld, R.; Sieweke, J.-T.; Zietzer, A.; Wiora, J.; Masiero, G.; Martinez, C.S.; Tarantini, G.; Werner, N. Complete Revascularisation in Impella-Supported Infarct-Related Cardiogenic Shock Patients Is Associated With Improved Mortality. Front. Cardiovasc. Med. 2021, 8, 678748. [Google Scholar] [CrossRef]
- Scherer, C.; Lüsebrink, E.; Kupka, D.; Stocker, T.J.; Stark, K.; Stremmel, C.; Orban, M.; Petzold, T.; Germayer, A.; Mauthe, K.; et al. Long-Term Clinical Outcome of Cardiogenic Shock Patients Undergoing Impella CP Treatment vs. Standard of Care. J. Clin. Med. 2020, 9, 3803. [Google Scholar] [CrossRef]
- Schiller, P.; Vikholm, P.; Hellgren, L. The Impella® Recover mechanical assist device in acute cardiogenic shock: A single-centre experience of 66 patients. Interact. Cardiovasc. Thorac. Surg. 2016, 22, 452–458. [Google Scholar] [CrossRef]
- Schroeter, M.R.; Herdis, K.; Wachter, A.; Annalen Bleckmann, M.D.; Hasenfu, G.; Wolfgang Schillinger, M.D. Use of the Impella device for acute coronary syndrome complicated by cardiogenic shock–experience from a single heart center with analysis of long-term mortality. J. Invasive Cardiol. 2016, 28, 467–472. [Google Scholar]
- Schurtz, G.; Rousse, N.; Saura, O.; Balmette, V.; Vincent, F.; Lamblin, N.; Porouchani, S.; Verdier, B.; Puymirat, E.; Robin, E.; et al. IMPELLA® or Extracorporeal Membrane Oxygenation for Left Ventricular Dominant Refractory Cardiogenic Shock. J. Clin. Med. 2021, 10, 759. [Google Scholar] [CrossRef]
- Seyfarth, M.; Sibbing, D.; Bauer, I.; Fröhlich, G.; Bott-Flügel, L.; Byrne, R.; Dirschinger, J.; Kastrati, A.; Schömig, A. A Randomized Clinical Trial to Evaluate the Safety and Efficacy of a Percutaneous Left Ventricular Assist Device Versus Intra-Aortic Balloon Pumping for Treatment of Cardiogenic Shock Caused by Myocardial Infarction. J. Am. Coll. Cardiol. 2008, 52, 1584–1588. [Google Scholar] [CrossRef]
- Sieweke, J.-T.; Akin, M.; Beheshty, J.-A.; Flierl, U.; Bauersachs, J.; Schäfer, A. Unloading in Refractory Cardiogenic Shock After Out-Of-Hospital Cardiac Arrest Due to Acute Myocardial Infarction—A Propensity Score-Matched Analysis. Front. Cardiovasc. Med. 2021, 8, 704312. [Google Scholar] [CrossRef]
- Sugimura, Y.; Katahira, S.; Immohr, M.B.; Sipahi, N.F.; Mehdiani, A.; Assmann, A.; Rellecke, P.; Tudorache, I.; Westenfeld, R.; Boeken, U.; et al. Initial experience covering 50 consecutive cases of large Impella implantation at a single heart centre. ESC Heart Fail. 2021, 8, 5168–5177. [Google Scholar] [CrossRef] [PubMed]
- Takahashi, K.; Kubo, S.; Ikuta, A.; Osakada, K.; Takamatsu, M.; Taguchi, Y.; Ohya, M.; Shimada, T.; Miura, K.; Tada, T.; et al. Incidence, predictors, and clinical outcomes of mechanical circulatory support-related complications in patients with cardiogenic shock. J. Cardiol. 2021, 79, 163–169. [Google Scholar] [CrossRef] [PubMed]
- Tarabichi, S.; Ikegami, H.; Russo, M.J.; Lee, L.Y.; Lemaire, A. The role of the axillary Impella 5.0 device on patients with acute cardiogenic shock. J. Cardiothorac. Surg. 2020, 15, 218. [Google Scholar] [CrossRef] [PubMed]
- Tepper, S.; Masood, M.F.; Garcia, M.B.; Pisani, M.; Ewald, G.A.; Lasala, J.M.; Bach, R.G.; Singh, J.; Balsara, K.R.; Itoh, A. Left Ventricular Unloading by Impella Device Versus Surgical Vent During Extracorporeal Life Support. Ann. Thorac. Surg. 2017, 104, 861–867. [Google Scholar] [CrossRef]
- Trpkov, C.; Gibson, J.D.; Miller, R.J.; Grant, A.D.; Schnell, G.; Har, B.J.; Clarke, B. Percutaneous Left Ventricular Assist Device in Cardiogenic Shock: A Five-Year Single Canadian Center Initial Experience. CJC Open 2020, 2, 370–378. [Google Scholar] [CrossRef]
- Vase, H.; Christensen, S.; Christiansen, A.; Therkelsen, C.J.; Christiansen, E.H.; Eiskjaer, H.; Poulsen, S.H. The Impella CP device for acute mechanical circulatory support in refractory cardiac arrest. Resuscitation 2017, 112, 70–74. [Google Scholar] [CrossRef]
- Vasin, S.; Philipp, A.; Floerchinger, B.; Rastogi, P.; Lunz, D.; Mueller, T.; Schmid, C.; Camboni, D. Increasing use of the Impella®-pump in severe cardiogenic shock: A word of caution. Interact. Cardiovasc. Thorac. Surg. 2020, 30, 711–714. [Google Scholar] [CrossRef]
- Wilkins, C.E.; Herrera, T.L.; Nagahiro, M.K.; Weathers, L.B.; Girotra, S.V.; Sandhu, F. Outcomes of Hemodynamic Support With Impella for Acute Myocardial Infarction Complicated by Cardiogenic Shock at a Rural Community Hospital Without On-Site Surgical Back-up. J. Invasive Cardiol. 2019, 31, E23–E29. [Google Scholar]
- Zaiser, A.S.; Fahrni, G.; Hollinger, A.; Knobel, D.T.; Bovey, Y.; Zellweger, N.M.; Siegemund, M. Adverse Events of Percutaneous Microaxial Left Ventricular Assist Devices—A Retrospective, Single-Centre Cohort Study. J. Clin. Med. 2021, 10, 3710. [Google Scholar] [CrossRef]
- Abdullah, K.Q.A.; Roedler, J.V.; Dahl, J.V.; Szendey, I.; Haake, H.; Eckardt, L.; Topf, A.; Ohnewein, B.; Jirak, P.; Motloch, L.J.; et al. Impella use in real-world cardiogenic shock patients: Sobering outcomes. PLoS ONE 2021, 16, e0247667. [Google Scholar] [CrossRef]
- Barrionuevo-Sánchez, M.I.; Ariza-Solé, A.; Ortiz-Berbel, D.; González-Costello, J.; Gómez-Hospital, J.A.; Lorente, V.; Comin-Colet, J. Usefulness of Impella support in different clinical settings in cardiogenic shock. J. Geriatr. Cardiol. JGC 2022, 19, 115. [Google Scholar]
- Bashline, M.J.; Rhinehart, Z.; Kola, O.; Fowler, J.; Kaczorowski, D.; Hickey, G. Impella 5.0 is associated with a reduction in vasoactive support and improves hemodynamics in cardiogenic shock: A single-center experience. Int. J. Artif. Organs 2022, 45, 462–469. [Google Scholar] [CrossRef]
- Ramzy, D.; Anderson, M.; Batsides, G.; Ono, M.; Silvestry, S.; D’Alessandro, D.A.; Funamoto, M.; Zias, E.A.; Lemaire, A.; Soltese, E. Early Outcomes of the First 200 US Patients Treated with Impella 5.5: A Novel Temporary Left Ventricular Assist Device. Innovations 2021, 16, 365–372. [Google Scholar] [CrossRef]
- Rock, J.R.; Kos, C.A.; Lemaire, A.; Ikegami, H.; Russo, M.J.; Moin, D.; Iyer, D. Single center first year experience and outcomes with Impella 5.5 left ventricular assist device. J. Cardiothorac. Surg. 2022, 17, 124. [Google Scholar] [CrossRef] [PubMed]
- Scolari, F.L.; Trott, G.; Schneider, D.; Goldraich, L.A.; Tonietto, T.F.; Moura, L.Z.; Bertoldi, E.G.; Rover, M.M.; Wolf, J.M.; de Souza, D.; et al. Cardiogenic shock treated with temporary mechanical circulatory support in Brazil: The effect of learning curve. Int. J. Artif. Organs 2022, 45, 292–300. [Google Scholar] [CrossRef] [PubMed]
- Shibasaki, I.; Masawa, T.; Abe, S.; Ogawa, H.; Takei, Y.; Tezuka, M.; Seki, M.; Kato, T.; Watanabe, R.; Koshiji, N.; et al. Benefit of veno-arterial extracorporeal membrane oxygenation combined with Impella (ECpella) therapy in acute coronary syndrome with cardiogenic shock. J. Cardiol. 2022, 80, 116–124. [Google Scholar] [CrossRef] [PubMed]
- Syntila, S.; Chatzis, G.; Markus, B.; Ahrens, H.; Waechter, C.; Luesebrink, U.; Divchev, D.; Schuett, H.; Tsalouchidou, P.-E.; Jerrentrup, A.; et al. Comparison of Mechanical Support with Impella or Extracorporeal Life Support in Post-Cardiac Arrest Cardiogenic Shock: A Propensity Scoring Matching Analysis. J. Clin. Med. 2021, 10, 3583. [Google Scholar] [CrossRef] [PubMed]
- Zubarevich, A.; Rad, A.A.; Szczechowicz, M.; Luedike, P.; Koch, A.; Pizanis, N.; Kamler, M.; Ruhparwar, A.; Weymann, A.; Schmack, B. Early Experience with the Impella Pump: Single Center Registry. Artif. Organs 2022, 46, 1689–1694. [Google Scholar] [CrossRef] [PubMed]
- Burzotta, F.; Trani, C.; Doshi, S.N.; Townend, J.; van Geuns, R.J.; Hunziker, P.; Schieffer, B.; Karatolios, K.; Møller, J.E.; Ribichini, F.L.; et al. Impella ventricular support in clinical practice: Collaborative viewpoint from a European expert user group. Int. J. Cardiol. 2015, 201, 684–691. [Google Scholar] [CrossRef]
- Ramzy, D.; Soltesz, E.; Anderson, M. New Surgical Circulatory Support System Outcomes. ASAIO J. 2020, 66, 746–752. [Google Scholar] [CrossRef]
- Rohm, C.L.; Gadidov, B.; Leitson, M.; Ray, H.E.; Prasad, R. Predictors of Mortality and Outcomes of Acute Severe Cardiogenic Shock Treated with the Impella Device. Am. J. Cardiol. 2019, 124, 499–504. [Google Scholar] [CrossRef]
- Shintani, A.K.; Girard, T.; Eden, S.K.; Arbogast, P.G.; Moons, K.G.M.; Ely, E.W. Immortal time bias in critical care research: Application of time-varying Cox regression for observational cohort studies*. Crit. Care Med. 2009, 37, 2939–2945. [Google Scholar] [CrossRef]
- Poon, W.H.; Ramanathan, K.; Ling, R.R.; Yang, I.X.; Tan, C.S.; Schmidt, M.; Shekar, K. Prone positioning during venovenous extracorporeal membrane oxygenation for acute respiratory distress syndrome: A systematic review and meta-analysis. Crit. Care 2021, 25, 292. [Google Scholar] [CrossRef]
- Ramanathan, K.; Shekar, K.; Ling, R.R.; Barbaro, R.P.; Wong, S.N.; Tan, C.S.; Brodie, D. Extracorporeal membrane oxygenation for COVID-19: A systematic review and meta-analysis. Crit. Care 2021, 25, 211. [Google Scholar] [CrossRef]
- Lévesque, L.E.; A Hanley, J.; Kezouh, A.; Suissa, S. Problem of immortal time bias in cohort studies: Example using statins for preventing progression of diabetes. BMJ 2010, 340, b5087. [Google Scholar] [CrossRef]
- Batsides, G.; Massaro, J.; Cheung, A.; Soltesz, E.; Ramzy, D.; Anderson, M.B. Outcomes of Impella 5.0 in cardiogenic shock: A systematic review and meta-analysis. Innovations 2018, 13, 254–260. [Google Scholar] [CrossRef]
- Glazier, J.J.; Kaki, A. Improving survival in cardiogenic shock: Is Impella the answer? Am. J. Med. 2018, 131, e403–e404. [Google Scholar] [CrossRef]
- Prondzinsky, R.; Lemm, H.; Swyter, M.; Wegener, N.; Unverzagt, S.; Carter, J.M.; Russ, M.; Schlitt, A.; Buerke, U.; Christoph, A.; et al. Intra-aortic balloon counterpulsation in patients with acute myocardial infarction complicated by cardiogenic shock: The prospective, randomized IABP SHOCK Trial for attenuation of multiorgan dysfunction syndrome*. Crit. Care Med. 2010, 38, 152–160. [Google Scholar] [CrossRef]
- Schmidt, M.; Burrell, A.; Roberts, L.; Bailey, M.; Sheldrake, J.; Rycus, P.T.; Hodgson, C.; Scheinkestel, C.; Cooper, D.J.; Thiagarajan, R.R.; et al. Predicting survival after ECMO for refractory cardiogenic shock: The survival after veno-arterial-ECMO (SAVE)-score. Eur. Heart J. 2015, 36, 2246–2256. [Google Scholar] [CrossRef]
- Basir, M.B.; Kapur, N.K.; Patel, K.; Salam, M.A.; Schreiber, T.; Kaki, A. National Cardiogenic Shock Initiative Investigators. Improved outcomes associated with the use of shock protocols: Updates from the National Cardiogenic Shock Initiative. Catheter. Cardiovasc. Interv. 2019, 93, 1173–1183. [Google Scholar]
- Basir, M.B.; Schreiber, T.; Dixon, S.; Alaswad, K.; Patel, K.; Almany, S.; Khandelwal, A.; Hanson, I.; George, A.; Ashbrook, M.; et al. Feasibility of early mechanical circulatory support in acute myocardial infarction complicated by cardiogenic shock: The Detroit cardiogenic shock initiative. Catheter. Cardiovasc. Interv. 2017, 91, 454–461. [Google Scholar] [CrossRef]
- Mourad, M.; Gaudard, P.; De La Arena, P.; Eliet, J.; Zeroual, N.; Rouvière, P.; Roubille, F.; Albat, B.; Colson, P.H. Circulatory Support with Extracorporeal Membrane Oxygenation and/or Impella for Cardiogenic Shock During Myocardial Infarction. ASAIO J. 2018, 64, 708–714. [Google Scholar] [CrossRef]
- O’Neill, W.W.; Kleiman, N.S.; Moses, J.; Henriques, J.P.S.; Dixon, S.; Massaro, J.; Palacios, I.; Maini, B.; Mulukutla, S.; Džavík, V.; et al. A Prospective, Randomized Clinical Trial of Hemodynamic Support With Impella 2.5 Versus Intra-Aortic Balloon Pump in Patients Undergoing High-Risk Percutaneous Coronary Intervention. Circulation 2012, 126, 1717–1727. [Google Scholar] [CrossRef]
- O’Neill, W.W.; Schreiber, T.; Wohns, D.H.W.; Rihal, C.; Naidu, S.S.; Civitello, A.; Dixon, S.R.; Massaro, J.M.; Maini, B.; Ohman, E.M. The Current Use of Impella 2.5 in Acute Myocardial Infarction Complicated by Cardiogenic Shock: Results from the USpella Registry. J. Interv. Cardiol. 2013, 27, 1–11. [Google Scholar] [CrossRef]
- Lauten, A.; Engström, A.E.; Jung, C.; Empen, K.; Erne, P.; Cook, S.; Windecker, S.; Bergmann, M.W.; Klingenberg, R.; Lüscher, T.F.; et al. Percutaneous left-ventricular support with the Impella-2.5-assist device in acute cardiogenic shock: Results of the Impella-EUROSHOCK-registry. Circ. Heart Fail. 2013, 6, 23–30. [Google Scholar] [CrossRef]
- Hirst, C.S.; Thayer, K.L.; Harwani, N.; Kapur, N.K. Post-Closure Technique to Reduce Vascular Complications Related to Impella CP. Cardiovasc. Revascularization Med. 2022, 39, 38–42. [Google Scholar] [CrossRef]
- Davidavicius, G.; Godino, C.; Shannon, J.; Takagi, K.; Bertoldi, L.; Mussardo, M.; Chieffo, A.; Arioli, F.; Ielasi, A.; Montorfano, M.; et al. Incidence of Overall Bleeding in Patients Treated With Intra-Aortic Balloon Pump During Percutaneous Coronary Intervention: 12-Year Milan Experience. JACC Cardiovasc. Interv. 2012, 5, 350–357. [Google Scholar] [CrossRef]
- De Jong, M.M.; Lorusso, R.; Al Awami, F.; Matteuci, F.; Parise, O.; Lozekoot, P.; Gelsomino, S. Vascular complications following intra-aortic balloon pump implantation: An updated review. Perfusion 2018, 33, 96–104. [Google Scholar] [CrossRef]

| Demographics | Study Type | Studies | Pooled Estimate | 95%CI |
|---|---|---|---|---|
| Patient Demographics | ||||
| Age (years) | Observational | 59 | 61.6 | 60.1–63.0 |
| RCT/PSM | 8 | 62.2 | 58.8–65.6 | |
| Male (%) | Observational | 59 | 75.0% | 70.9–78.8% |
| RCT/PSM | 8 | 82.2% | 70.5–90.0% | |
| Pre-Impella Characteristics | ||||
| Body Mass Index (kg/m2) | Observational | 18 | 27.4 | 26.8–28.0 |
| RCT/PSM | 2 | 25.7 | 23.1–28.2 | |
| LVEF (%) | Observational | 32 | 25.3 | 22.8–27.9 |
| RCT/PSM | 3 | 33.8 | 31.8–35.8 | |
| Hypertension (%) | Observational | 41 | 53.5% | 45.7–61.3% |
| RCT/PSM | 6 | 55.6% | 38.1–71.8% | |
| Hyperlipidemia (%) | Observational | 34 | 35.4% | 25.2–46.4% |
| RCT/PSM | 2 | 35.1% | 10.9–70.7% | |
| Diabetes Mellitus (%) | Observational | 48 | 30.6% | 27.2–34.1% |
| RCT/PSM | 7 | 28.8% | 20.1–39.4% | |
| Smoking (%) | Observational | 40 | 26.8% | 18.6–35.8% |
| RCT/PSM | 3 | 46.2% | 33.2–59.7% | |
| Heart Failure (%) | Observational | 24 | 20.3% | 10.0–32.7% |
| RCT/PSM | Was not reported in any of the studies | |||
| Previous AMI (%) | Observational | 26 | 20.7% | 14.3–27.9% |
| RCT/PSM | 5 | 32.5% | 15.6–55.5% | |
| Cerebrovascular Accident (%) | Observational | 29 | 7.5% | 5.0–10.2% |
| RCT/PSM | 3 | 1.3% | 0.4–4.0% | |
| Post-device Characteristics | ||||
| Duration of device support (days) | Observational | 38 | 6.2 | 4.7–7.7 |
| RCT/PSM | 7 | 2.9 | 1.5–4.3 | |
| Length of ICU stay (days) | Observational | 13 | 13.7 | 10.2–17.2 |
| RCT/PSM | 2 | 8.6 | 6.5–10.8 | |
| Length of hospital stay (days) | Observational | 6 | 20.6 | 13.0–28.2 |
| RCT/PSM | 3 | 15.3 | 12.0–18.7 | |
| Complication | Studies | Pooled Proportion (%) | 95% CI | I2 |
|---|---|---|---|---|
| Hemolysis | 32 | 24.9 | 14.9 to 36.4 | 94.8% |
| Access-site Bleeding | 23 | 25.8 | 14.7 to 38.5 | 94.9% |
| Device Malfunction | 17 | 5.9 | 3.1 to 9.3 | 58.8% |
| Limb Ischemia | 32 | 6.1 | 3.7 to 8.9 | 76.1% |
| Stroke | 32 | 5.5 | 2.9 to 8.5 | 77.6% |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Tan, S.R.; Low, C.J.W.; Ng, W.L.; Ling, R.R.; Tan, C.S.; Lim, S.L.; Cherian, R.; Lin, W.; Shekar, K.; Mitra, S.; et al. Microaxial Left Ventricular Assist Device in Cardiogenic Shock: A Systematic Review and Meta-Analysis. Life 2022, 12, 1629. https://doi.org/10.3390/life12101629
Tan SR, Low CJW, Ng WL, Ling RR, Tan CS, Lim SL, Cherian R, Lin W, Shekar K, Mitra S, et al. Microaxial Left Ventricular Assist Device in Cardiogenic Shock: A Systematic Review and Meta-Analysis. Life. 2022; 12(10):1629. https://doi.org/10.3390/life12101629
Chicago/Turabian StyleTan, Shien Ru, Christopher Jer Wei Low, Wei Lin Ng, Ryan Ruiyang Ling, Chuen Seng Tan, Shir Lynn Lim, Robin Cherian, Weiqin Lin, Kiran Shekar, Saikat Mitra, and et al. 2022. "Microaxial Left Ventricular Assist Device in Cardiogenic Shock: A Systematic Review and Meta-Analysis" Life 12, no. 10: 1629. https://doi.org/10.3390/life12101629
APA StyleTan, S. R., Low, C. J. W., Ng, W. L., Ling, R. R., Tan, C. S., Lim, S. L., Cherian, R., Lin, W., Shekar, K., Mitra, S., MacLaren, G., & Ramanathan, K. (2022). Microaxial Left Ventricular Assist Device in Cardiogenic Shock: A Systematic Review and Meta-Analysis. Life, 12(10), 1629. https://doi.org/10.3390/life12101629





