Basic Quality Controls Used in Skin Tissue Engineering
Abstract
1. Introduction
2. Biology of the Skin
3. Regeneration of the Skin
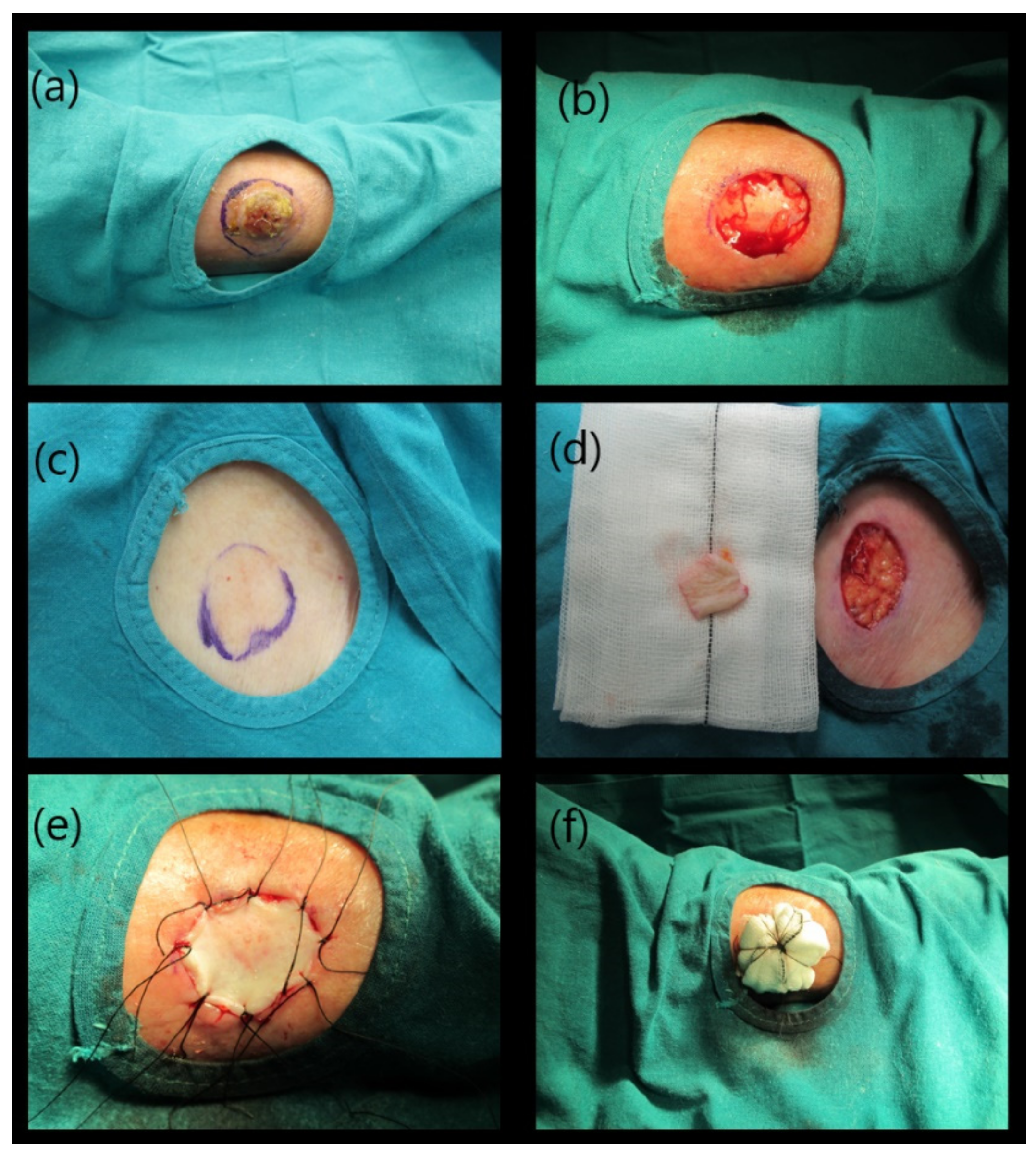
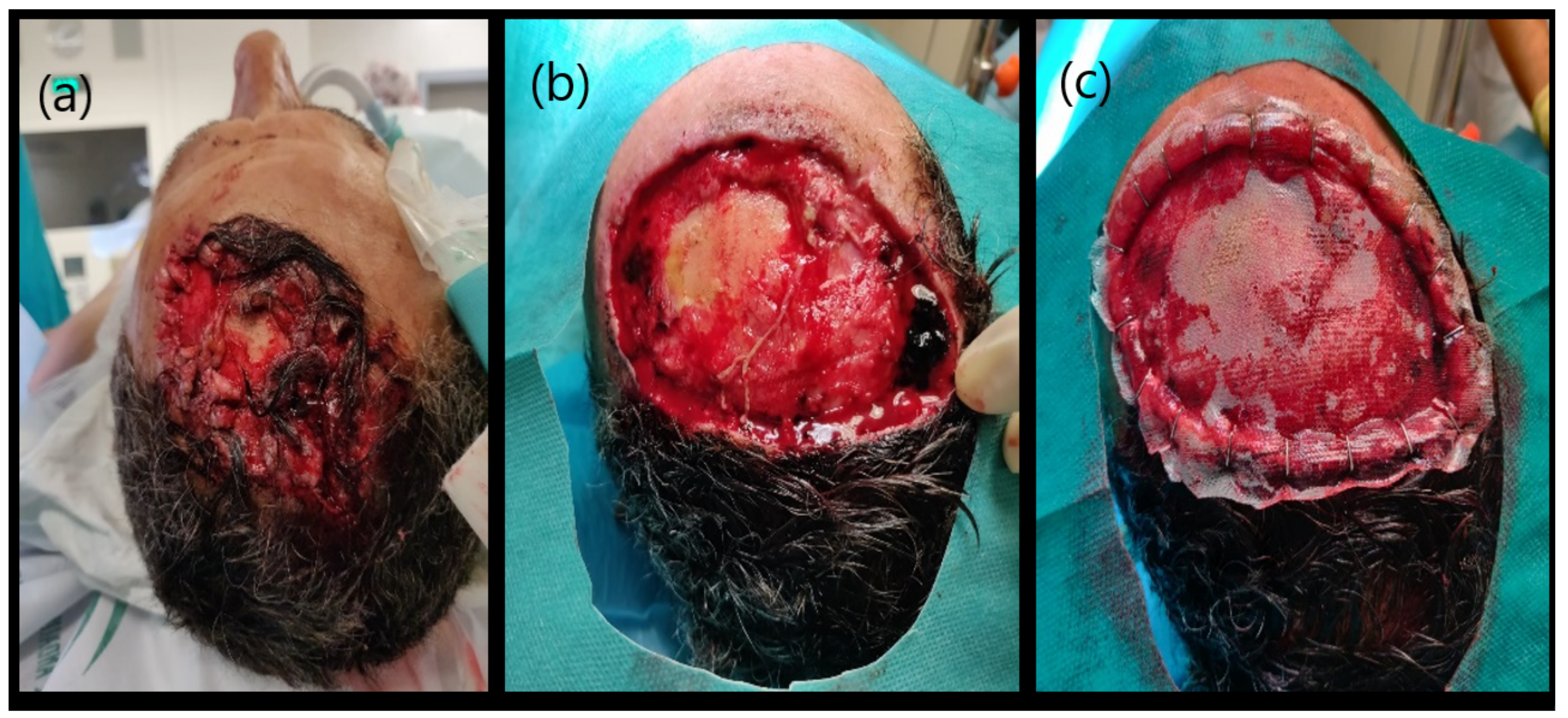
4. Current Surgical Strategies for Skin Repair
5. Skin Tissue Engineering
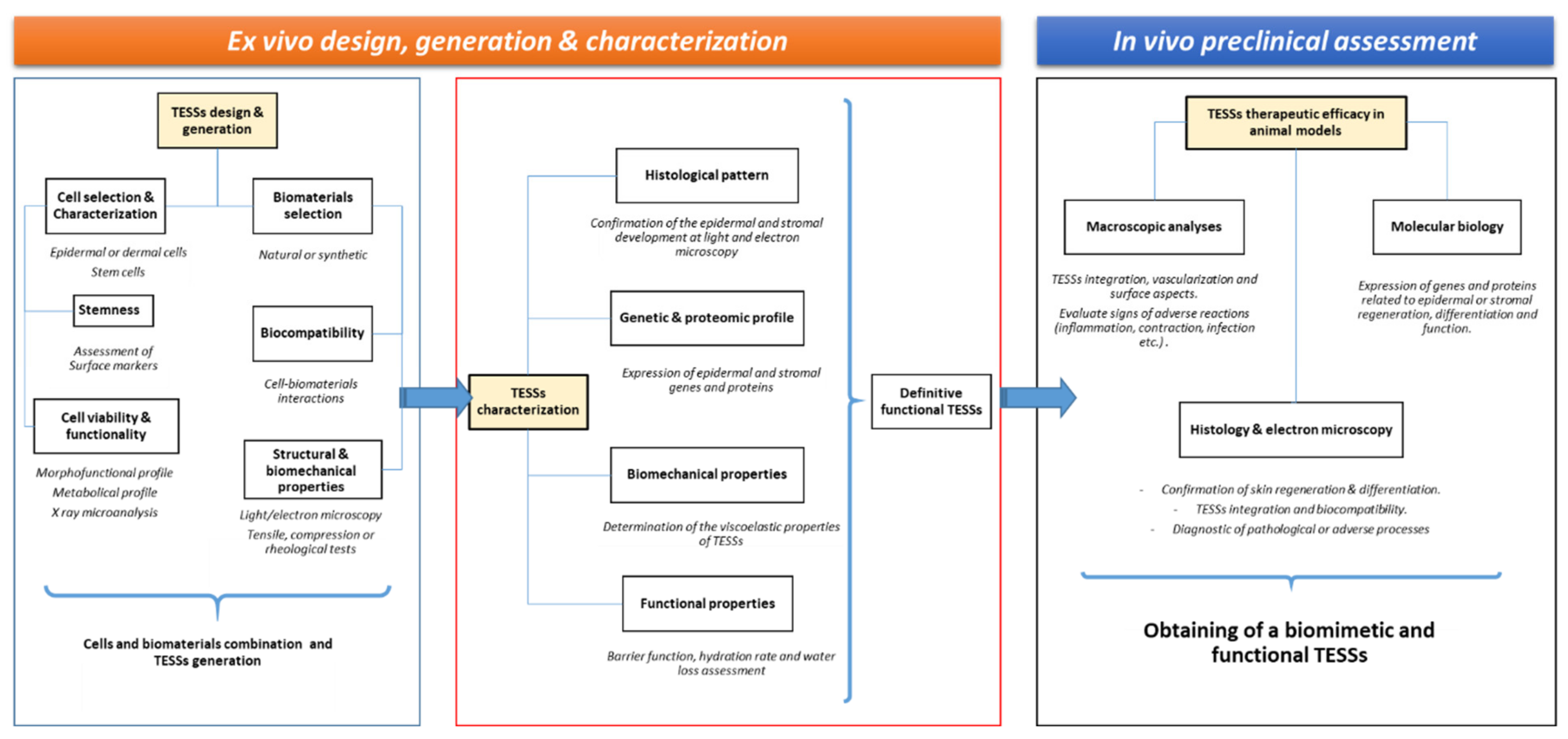
6. Quality Controls in Skin Tissue Engineering
7. Ex Vivo Quality Controls
7.1. Assessment of the Cell Viability and Functionality
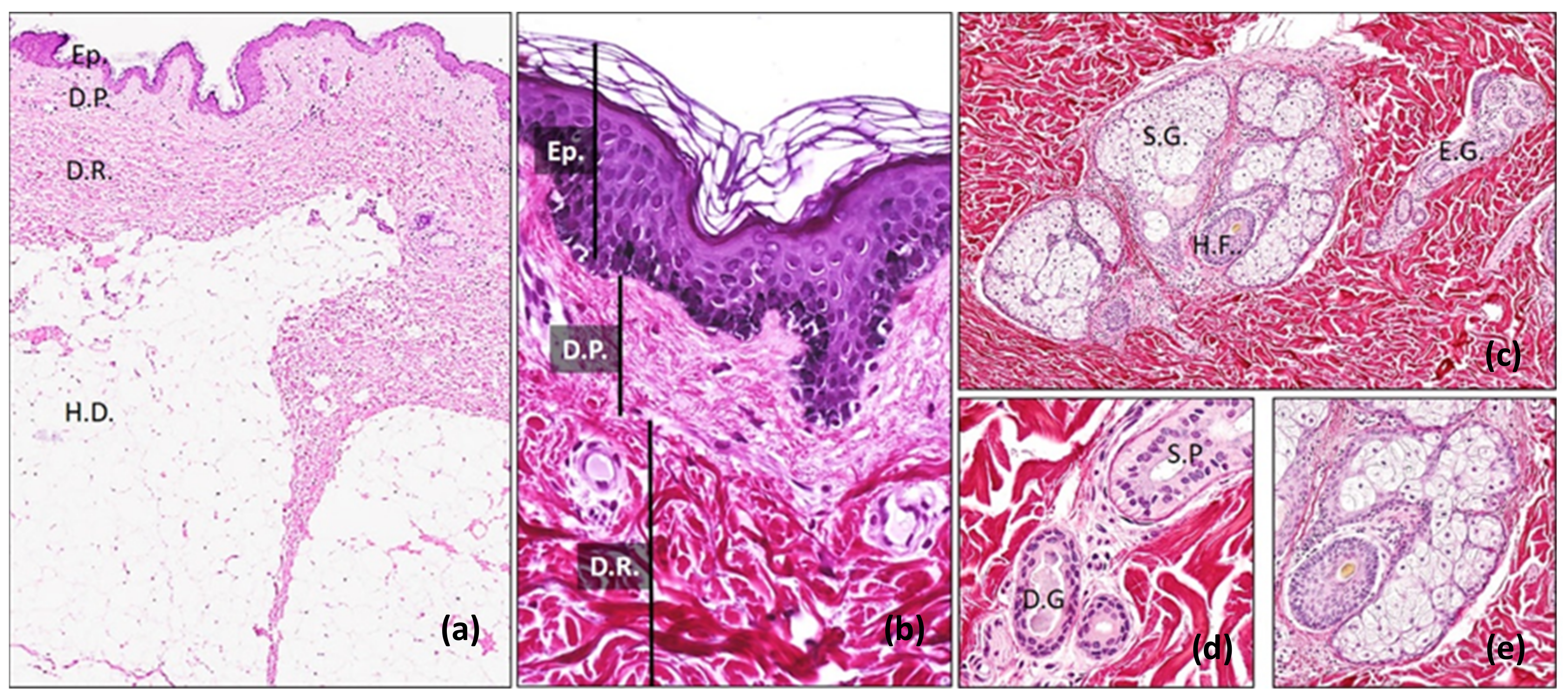
7.2. Histological Assessment
7.3. Transmission Electron Microscopy
7.4. Molecular Biology
7.5. Biomechanical Characterization
7.6. Functional Evaluation
- Surface hydration: human stratum corneum electrical conductance depend on their water content. This is the reason why capacitance and/or conductance methods are commonly used to measure water content of TESSs and development of barrier function in vivo.
- Transepidermal water loss (TEWL). TEWL is the amount of water vapor evaporating from a fixed surface of the skin per unit time. It is measured using sensors that detect changes in water vapor density. Niacinamide flux: Permeability of niacinamide has been revealed as a sensitive invasive method to measure the barrier function in cultured skin substitutes.
8. In Vivo Quality Controls
8.1. Macroscopic Evaluation
8.2. Histological and Ultrastructural Analyses
8.3. Molecular Biology
8.4. Biomechanical Characterization
9. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Li, M.; Urmacher, C.D. Histology for Pathologists, 3rd ed.; Lippincott Williams & Wilkins: Philadelphia, PA, USA, 2007. [Google Scholar]
- Sheridan, R. Closure of the excised burn wound: Autografts, semipermanent skin substitutes, and permanent skin substitutes. Clin. Plast. Surg. 2009, 36, 643–651. [Google Scholar] [CrossRef]
- Mills, S. Histology for Pathologists; Lippincott Williams & Wilkins: Philadelphia, PA, USA, 2019. [Google Scholar]
- Bragulla, H.H.; Homberger, D.G. Structure and functions of keratin proteins in simple, stratified, keratinized and cornified epithelia. J. Anat. 2009, 214, 516–559. [Google Scholar] [CrossRef] [PubMed]
- Vela-Romera, A.; Carriel, V.; Martín-Piedra, M.A.; Aneiros-Fernández, J.; Campos, F.; Chato-Astrain, J.; Prados-Olleta, N.; Campos, A.; Alaminos, M.; Garzón, I. Characterization of the human ridged and non-ridged skin: A comprehensive histological, histochemical and immunohistochemical analysis. Histochem. Cell Biol. 2019, 151, 57–73. [Google Scholar] [CrossRef] [PubMed]
- Murphy, G. Histology of the Skin. Lever’s Histopathology of the Skin, 9th ed.; Lippincott Williams & Wilkins: Philadelphia, PA, USA, 2005. [Google Scholar]
- Morrison, K.M.; Miesegaes, G.R.; Lumpkin, E.A.; Maricich, S.M. Mammalian Merkel cells are descended from the epidermal lineage. Dev. Biol. 2009, 336, 76–83. [Google Scholar] [CrossRef]
- Carriel, V.S.; Aneiros-Fernandez, J.; Arias-Santiago, S.; Garzón, I.J.; Alaminos, M.; Campos, A. A novel histochemical method for a simultaneous staining of melanin and collagen fibers. J. Histochem. Cytochem. 2011, 59, 270–277. [Google Scholar] [CrossRef]
- John, D.B.; Marilyn Gamble, M. (Eds.) Theory and Practice of Histological Techniques; Elsevier Health Sciences: Amsterdam, The Netherlands, 2008. [Google Scholar]
- Jiang, L.W.; Chen, H.; Lu, H. Using human epithelial amnion cells in human de-epidermized dermis for skin regeneration. J. Dermatol. Sci. 2016, 81, 26–34. [Google Scholar] [CrossRef]
- Halfter, W.; Oertle, P.; Monnier, C.A.; Camenzind, L.; Reyes-Lua, M.; Hu, H.; Candiello, J.; Labilloy, A.; Balasubramani, M.; Henrich, P.B.; et al. New concepts in basement membrane biology. FEBS J. 2015, 282, 4466–4479. [Google Scholar] [CrossRef]
- Philips, C.; Cornelissen, M.; Carriel, V. Evaluation methods as quality control in the generation of decellularized peripheral nerve allografts. J. Neural. Eng. 2018, 15, 021003. [Google Scholar] [CrossRef] [PubMed]
- Wick, M.R. (Ed.) Diagnostic Histochemistry; Cambridge University Press: New York, NY, USA, 2008. [Google Scholar]
- Aneiros-Fernández, J.; Husein-ElAhmed, H.; Arias-Santiago, S.; Campos, A.; Carriel, V.; Sánchez-Montesinos, I.; Garcia del Moral, R.; Sánchez, G.; O’Valle, F.; Aneiros, J. Expression of smoothelin and smooth muscle actin in the skin. Histol. Histopathol. 2011, 26, 673–678. [Google Scholar]
- Godoy-Guzmán, C.; Nuñez, C.; Orihuela, P.; Campos, A.; Carriel, V. Distribution of extracellular matrix molecules in human uterine tubes during the menstrual cycle: A histological and immunohistochemical analysis. J. Anat. 2018, 233, 73–85. [Google Scholar] [CrossRef]
- Fernández Morales, E.; Gálvez Alcaraz, L.; Fernández-Crehuet Navajas, J.; Gómez Gracia, E.; Salinas Martínez, J. Epidemiology of Burns in Malaga, Spain. Burns 1997, 23, 323–332. [Google Scholar] [CrossRef]
- Ruiz-Villaverde, R.; Aneiros-Fernández, J. Primary Cutaneous Carcinosarcoma: A cutaneous neoplasm with an exceptional presentation. Sultan Qaboos Univ. Med. J. 2018, 18, e114–e115. [Google Scholar] [CrossRef]
- Aguayo-Carreras, P.; Ruiz-Villaverde, R.; Aneiros-Fernandez, J.; Almodovar Real, A.; Ruiz-Carrascosa, J.C.; Naranjo-Sintes, R. Excrescent tumor on the left sole in a middle-aged man. J. Dtsch. Dermatol. Ges. 2018, 16, 226–229. [Google Scholar] [CrossRef]
- Wells, A.; Nuschke, A.; Yates, C.C. Skin tissue repair: Matrix microenvironmental influences. Matrix Biol. 2016, 49, 25–36. [Google Scholar] [CrossRef]
- Clark, R.A.; Ghosh, K.; Tonnesen, M.G. Tissue engineering for cutaneous wounds. J. Investig. Dermatol. 2007, 127, 1018–1029. [Google Scholar] [CrossRef] [PubMed]
- Klicksa, J.; Von Molitora, E.; Ertongur-Fauthb, T.; Rudolfa, R.; Hafnera, M. In vitro skin three-dimensional models and their applications. J. Cell. Biotechnol. 2017, 3, 21–39. [Google Scholar] [CrossRef]
- Singer, A.J.; Clark, R.A. Cutaneous wound healing. N. Engl. J. Med. 1999, 341, 738–746. [Google Scholar] [CrossRef]
- Ghosh, K.; Clark, R. Wound repair: Basic biology to tissue engineering. In Principles of Tissue Engineering; Elsevier: Amsterdam, The Netherlands, 2007. [Google Scholar]
- Leong, A.S.; Gilham, P. A new, rapid, microwave-stimulated method of staining melanocytic lesions. Stain Technol. 1989, 64, 81–85. [Google Scholar] [CrossRef]
- Shevchenko, R.V.; James, S.L.; James, S.E. A review of tissue-engineered skin bioconstructs available for skin reconstruction. J. R. Soc. Interface 2010, 7, 229–258. [Google Scholar] [CrossRef] [PubMed]
- Carriel, V.; Alaminos, M.; Garzon, I.; Campos, A.; Cornelissen, M. Tissue engineering of the peripheral nervous system. Expert Rev. Neurother. 2014, 14, 301–318. [Google Scholar] [CrossRef]
- González-Quevedo, D.; Díaz-Ramos, M.; Chato-Astrain, J.; Sánchez-Porras, D.; Tamimi, I.; Campos, A.; Campos, F.; Carriel, V. Improving the regenerative microenvironment during tendon healing by using nanostructured fibrin/agarose-based hydrogels in a rat Achilles tendon injury model. Bone Joint J. 2020, 102-B, 1095–1106. [Google Scholar] [CrossRef] [PubMed]
- Naves, L.B.; Dhand, C.; Almeida, L.; Rajamani, L.; Ramakrishna, S. In vitro skin models and tissue engineering protocols for skin graft applications. Essays Biochem. 2016, 60, 357–369. [Google Scholar] [PubMed]
- Boyce, S.T.; Lalley, A.L. Tissue engineering of skin and regenerative medicine for wound care. Burns Trauma 2018, 6, 4. [Google Scholar] [CrossRef] [PubMed]
- Yu, J.R.; Navarro, J.; Coburn, J.C.; Mahadik, B.; Molnar, J.; Holmes, J.H., IV; Nam, A.J.; Fisher, J.P. Current and Future Perspectives on Skin Tissue Engineering: Key Features of Biomedical Research, Translational Assessment, and Clinical Application. Adv. Healthc. Mater. 2019, 8, e1801471. [Google Scholar] [CrossRef] [PubMed]
- Pereira, R.F.; Barrias, C.C.; Granja, P.L.; Bartolo, P.J. Advanced biofabrication strategies for skin regeneration and repair. Nanomedicine 2013, 8, 603–621. [Google Scholar] [CrossRef]
- Vig, K.; Chaudhari, A.; Tripathi, S.; Dixit, S.; Sahu, R.; Pillai, S.; Dennis, V.A.; Singh, S.R. Advances in Skin Regeneration Using Tissue Engineering. Int. J. Mol. Sci. 2017, 18, 789. [Google Scholar] [CrossRef]
- Goodarzi, P.; Falahzadeh, K.; Nematizadeh, M.; Farazandeh, P.; Payab, M.; Larijani, B. Tissue Engineered Skin Substitutes. Adv. Exp. Med. Biol. 2018, 1107, 143–188. [Google Scholar]
- Vacanti, C.A. The history of tissue engineering. J. Cell. Mol. Med. 2006, 10, 569–576. [Google Scholar] [CrossRef]
- Cunha, C.; Panseri, S.; Antonini, S. Emerging nanotechnology approaches in tissue engineering for peripheral nerve regeneration. Nanomedicine 2011, 7, 50–59. [Google Scholar] [CrossRef]
- Gonzalez-Quevedo, D.; Martinez-Medina, I.; Campos, A.; Campos, F.; Carriel, V. Tissue engineering strategies for the treatment of tendon injuries: A systematic review and meta-analysis of animal models. Bone Jt. Res. 2018, 7, 318–324. [Google Scholar] [CrossRef]
- Curtis, R.M.; Brewer, J.H.; Rose, I.W., Jr. New techniques for local treatment of burns. JAMA 1951, 147, 741–743. [Google Scholar] [CrossRef]
- Rheinwald, J.G.; Green, H. Serial cultivation of strains of human epidermal keratinocytes: The formation of keratinizing colonies from single cells. Cell 1975, 6, 331–343. [Google Scholar] [CrossRef]
- Gallico, G.G.; O’Connor, N.E.; Compton, C.C.; Kehinde, O.; Green, H. Permanent coverage of large burn wounds with autologous cultured human epithelium. N. Engl. J. Med. 1984, 311, 448–451. [Google Scholar] [CrossRef] [PubMed]
- Odessey, R. Addendum: Multicenter experience with cultured epidermal autograft for treatment of burns. J. Burn. Care Rehabil. 1992, 13, 174–180. [Google Scholar] [CrossRef]
- Hafemann, B.; Hettich, R.; Ensslen, S.; Kowol, B.; Zühlke, A.; Ebert, R.; Königs, M.; Kirkpatrick, C.J. Treatment of skin defects using suspensions of in vitro cultured keratinocytes. Burns 1994, 20, 168–172. [Google Scholar] [CrossRef]
- Williamson, J.S.; Snelling, C.F.; Clugston, P.; Macdonald, I.B.; Germann, E. Cultured epithelial autograft: Five years of clinical experience with twenty-eight patients. J. Trauma 1995, 39, 309–319. [Google Scholar] [CrossRef]
- Larouche, D.; Paquet, C.; Fradette, J.; Carrier, P.; Auger, F.A.; Germain, L. Regeneration of Skin and Cornea by Tissue Engineering. In Stem Cells in Regenerative Medicine: Methods and Protocols; Audet, W.L.S.J., Ed.; Humana Press: Totowa, NJ, USA, 2009; p. 482. [Google Scholar]
- Lazic, T.; Falanga, V. Bioengineered skin constructs and their use in wound healing. Plast. Reconstr. Surg. 2011, 127 (Suppl. S1), 75S–90S. [Google Scholar] [CrossRef] [PubMed]
- Harrison, C.A.; Gossiel, F.; Layton, C.M.; Bullock, A.J.; Johnson, T.; Blumsohn, A.; MacNeil, S. Use of an in vitro model of tissue-engineered skin to investigate the mechanism of skin graft contraction. Tissue Eng. 2006, 12, 3119–3133. [Google Scholar] [CrossRef]
- Medalie, D.A.; Eming, S.A.; Tompkins, R.G.; Yarmush, M.L.; Krueger, G.G.; Morgan, J.R. Evaluation of human skin reconstituted from composite grafts of cultured keratinocytes and human acellular dermis transplanted to athymic mice. J. Investig. Dermatol. 1996, 107, 121–127. [Google Scholar] [CrossRef]
- Burke, J.F.; Yannas, I.V.; Quinby, W.C.; Bondoc, C.C.; Jung, W.K. Successful use of a physiologically acceptable artificial skin in the treatment of extensive burn injury. Ann. Surg. 1981, 194, 413–428. [Google Scholar] [CrossRef]
- Chato-Astrain, J.; Philips, C.; Campos, F.; Durand-Herrera, D.; García-García, O.D.; Roosens, A.; Alaminos, M.; Campos, A.; Carriel, V. Detergent-based decellularized peripheral nerve allografts: An in vivo preclinical study in the rat sciatic nerve injury model. J. Tissue Eng. Regen. Med. 2020, 14, 789–806. [Google Scholar] [CrossRef]
- Dixit, S.; Baganizi, D.R.; Sahu, R.; Dosunmu, E.; Chaudhari, A.; Vig, K.; Pillai, S.R.; Singh, S.R.; Dennis, V.A. Immunological challenges associated with artificial skin grafts: Available solutions and stem cells in future design of synthetic skin. J. Biol. Eng. 2017, 11, 49. [Google Scholar] [CrossRef]
- Cuono, C.; Langdon, R.; McGuire, J. Use of cultured epidermal autografts and dermal allografts as skin replacement after burn injury. Lancet 1986, 1, 1123–1124. [Google Scholar] [CrossRef]
- Chakraborty, J.; Roy, S.; Ghosh, S. Regulation of decellularized matrix mediated immune response. Biomater. Sci. 2020, 8, 1194–1215. [Google Scholar] [CrossRef] [PubMed]
- Bell, E.; Ehrlich, H.P.; Buttle, D.J.; Nakatsuji, T. Living tissue formed in vitro and accepted as skin-equivalent tissue of full thickness. Science 1981, 211, 1052–1054. [Google Scholar] [CrossRef] [PubMed]
- Black, A.F.; Bouez, C.; Perrier, E.; Schlotmann, K.; Chapuis, F.; Damour, O. Optimization and characterization of an engineered human skin equivalent. Tissue Eng. 2005, 11, 723–733. [Google Scholar] [CrossRef]
- Turnbull, G.; Clarke, J.; Picard, F.; Zhang, W.; Riches, P.; Li, B.; Shu, W. 3D biofabrication for soft tissue and cartilage engineering. Med. Eng. Phys. 2020, 82, 13–39. [Google Scholar] [CrossRef]
- Horch, R.E.; Kopp, J.; Kneser, U.; Beier, J.; Bach, A.D. Tissue engineering of cultured skin substitutes. J. Cell. Mol. Med. 2005, 9, 592–608. [Google Scholar] [CrossRef]
- Balasubramani, M.; Kumar, T.R.; Babu, M. Skin substitutes: A review. Burns 2001, 27, 534–544. [Google Scholar] [CrossRef]
- Priya, S.G.; Jungvid, H.; Kumar, A. Skin tissue engineering for tissue repair and regeneration. Tissue Eng. Part B Rev. 2008, 14, 105–118. [Google Scholar] [CrossRef]
- Han, C.M.; Zhang, L.P.; Sun, J.Z.; Shi, H.F.; Zhou, J.; Gao, C.Y. Application of collagen-chitosan/fibrin glue asymmetric scaffolds in skin tissue engineering. J. Zhejiang Univ. Sci. B 2010, 11, 524–530. [Google Scholar] [CrossRef] [PubMed]
- Damour, O.; Gueugniaud, P.Y.; Berthin-Maghit, M.; Rousselle, P.; Berthod, F.; Sahuc, F.; Collombel, C. A dermal substrate made of collagen--GAG--chitosan for deep burn coverage: First clinical uses. A dermal substrate made of collagen-GAG-chitosan for deep burn coverage: First clinical uses. Clin. Mater. 1994, 15, 273–276. [Google Scholar] [CrossRef]
- Lee, S.B.; Jeon, H.W.; Lee, Y.W.; Lee, Y.M.; Song, K.W.; Park, M.H.; Nam, Y.S.; Ahn, H.C. Bio-artificial skin composed of gelatin and (1→3), (1→6)-beta-glucan. Biomaterials 2003, 24, 2503–2511. [Google Scholar] [CrossRef]
- Gibbs, S.; van den Hoogenband, H.M.; Kirtschig, G.; Richters, C.D.; Spiekstra, S.W.; Breetveld, M.; Scheper, R.J.; de Boer, E.M. Autologous full-thickness skin substitute for healing chronic wounds. Br. J. Dermatol. 2006, 155, 267–274. [Google Scholar] [CrossRef] [PubMed]
- Meana, A.; Iglesias, J.; Del Rio, M.; Larcher, F.; Madrigal, B.; Fresno, M.F.; Martin, C.; San Roman, F.; Tevar, F. Large surface of cultured human epithelium obtained on a dermal matrix based on live fibroblast-containing fibrin gels. Burns 1998, 24, 621–630. [Google Scholar] [CrossRef]
- Blackwood, K.A.; McKean, R.; Canton, I.; Freeman, C.O.; Franklin, K.L.; Cole, D.; Brook, I.; Farthing, P.; Rimmer, S.; Haycock, J.W.; et al. Development of biodegradable electrospun scaffolds for dermal replacement. Biomaterials 2008, 29, 3091–3104. [Google Scholar] [CrossRef]
- Auger, F.A.; Berthod, F.; Moulin, V.; Pouliot, R.; Germain, L. Tissue-engineered skin substitutes: From in vitro constructs to in vivo applications. Biotechnol. Appl. Biochem. 2004, 39 Pt 3, 263–275. [Google Scholar]
- Egea-Guerrero, J.J.; Carmona, G.; Correa, E.; Mata, R.; Arias-Santiago, S.; Alaminos, M.; Gacto, P.; Cuende, N. Transplant of tissue-engineered artificial autologous human skin in Andalusia: An example of coordination and institutional collaboration. In Transplantation Proceedings; Elsevier: Amsterdam, The Netherlands, 2019; Volume 51, pp. 3047–3050. [Google Scholar]
- Prodinger, C.M.; Reichelt, J.; Bauer, J.W.; Laimer, M. Current and Future Perspectives of Stem Cell Therapy in Dermatology. Ann. Dermatol. 2017, 29, 667–687. [Google Scholar] [CrossRef] [PubMed]
- Martin-Piedra, M.A.; Alfonso-Rodriguez, C.A.; Zapater, A.; Durand-Herrera, D.; Chato-Astrain, J.; Campos, F. Effective use of mesenchymal stem cells in human skin substitutes generated by tissue engineering. Eur. Cell. Mater. 2019, 37, 233–249. [Google Scholar] [CrossRef]
- Altman, A.M.; Yan, Y.; Matthias, N.; Bai, X.; Rios, C.; Mathur, A.B.; Song, Y.H.; Alt, E.U. IFATS collection: Human adipose-derived stem cells seeded on a silk fibroin-chitosan scaffold enhance wound repair in a murine soft tissue injury model. Stem. Cells 2009, 27, 250–258. [Google Scholar] [CrossRef] [PubMed]
- Huang, S.; Lu, G.; Wu, Y.; Jirigala, E.; Xu, Y.; Ma, K.; Fu, X. Mesenchymal stem cells delivered in a microsphere-based engineered skin contribute to cutaneous wound healing and sweat gland repair. J. Dermatol. Sci. 2012, 66, 29–36. [Google Scholar] [CrossRef]
- Klingenberg, J.M.; McFarland, K.L.; Friedman, A.J.; Boyce, S.T.; Aronow, B.J.; Supp, D.M. Engineered human skin substitutes undergo large-scale genomic reprogramming and normal skin-like maturation after transplantation to athymic mice. The influence of pancreas-derived stem cells on scaffold based skin regeneration. Biomaterials 2009, 30, 789–796. [Google Scholar]
- Ojeh, N.; Pastar, I.; Tomic-Canic, M.; Stojadinovic, O. Stem Cells in Skin Regeneration, Wound Healing, and Their Clinical Applications. Int. J. Mol. Sci. 2015, 16, 25476–25501. [Google Scholar] [CrossRef] [PubMed]
- Golchin, A.; Farahany, T.Z.; Khojasteh, A.; Soleimanifar, F.; Ardeshirylajimi, A. The Clinical Trials of Mesenchymal Stem Cell Therapy in Skin Diseases: An Update and Concise Review. Curr. Stem Cell Res. Ther. 2019, 14, 22–33. [Google Scholar] [CrossRef] [PubMed]
- Nourian Dehkordi, A.; Mirahmadi Babaheydari, F.; Chehelgerdi, M.; Raeisi Dehkordi, S. Skin tissue engineering: Wound healing based on stem-cell-based therapeutic strategies. Stem Cell Res. Ther. 2019, 10, 111. [Google Scholar] [CrossRef]
- Vermette, M.; Trottier, V.; Ménard, V.; Saint-Pierre, L.; Roy, A.; Fradette, J. Production of a new tissue-engineered adipose substitute from human adipose-derived stromal cells. Biomaterials 2007, 28, 2850–2860. [Google Scholar] [CrossRef]
- Frueh, F.S.; Später, T.; Körbel, C.; Scheuer, C.; Simson, A.C.; Lindenblatt, N.; Giovanoli, P.; Menger, M.D.; Laschke, M.W. Prevascularization of dermal substitutes with adipose tissue-derived microvascular fragments enhances early skin grafting. Sci. Rep. 2018, 8, 10977. [Google Scholar] [CrossRef]
- Abaci, H.E.; Guo, Z.; Coffman, A.; Gillette, B.; Lee, W.H.; Sia, S.K.; Christiano, A.M. Human Skin Constructs with Spatially Controlled Vasculature Using Primary and iPSC-Derived Endothelial Cells. Adv. Healthc. Mater. 2016, 5, 1800–1807. [Google Scholar] [CrossRef] [PubMed]
- Yan, W.C.; Davoodi, P.; Vijayavenkataraman, S.; Tian, Y.; Ng, W.C.; Fuh, J.Y.H.; Robinson, K.S.; Wang, C.H. 3D bioprinting of skin tissue: From pre-processing to final product evaluation. Adv. Drug Deliv. Rev. 2018, 132, 270–295. [Google Scholar] [CrossRef] [PubMed]
- Kim, B.S.; Kwon, Y.W.; Kong, J.S.; Park, G.T.; Gao, G.; Han, W.; Kim, M.B.; Lee, H.; Kim, J.H.; Cho, D.W. 3D cell printing of in vitro stabilized skin model and in vivo pre-vascularized skin patch using tissue-specific extracellular matrix bioink: A step towards advanced skin tissue engineering. Biomaterials 2018, 168, 38–53. [Google Scholar] [CrossRef]
- Jorgensen, A.M.; Varkey, M.; Gorkun, A.; Clouse, C.; Xu, L.; Chou, Z.; Murphy, S.V.; Molnar, J.; Lee, S.J.; Yoo, J.J.; et al. Bioprinted Skin Recapitulates Normal Collagen Remodeling in Full-Thickness Wounds. Tissue Eng. Part A 2020, 26, 512–526. [Google Scholar] [CrossRef]
- Barros, N.; Kim, H.; Goudie, M.J.; Lee, K.; Bandaru, P.; Banton, E.A.; Sarikhani, E.; Sun, W.; Zhang, S.; Cho, H.J.; et al. Biofabrication of endothelial cell, dermal fibroblast, and multilayered keratinocyte layers for skin tissue engineering. Biofabrication 2021, 13, 035030. [Google Scholar] [CrossRef]
- Zhou, F.; Hong, Y.; Liang, R.; Zhang, X.; Liao, Y.; Jiang, D.; Zhang, J.; Sheng, Z.; Xie, C.; Peng, Z.; et al. Rapid printing of bio-inspired 3D tissue constructs for skin regeneration. Biomaterials 2020, 258, 120287. [Google Scholar] [CrossRef] [PubMed]
- Waldeck, H.; Chung, A.S.; Kao, W.J. Interpenetrating polymer networks containing gelatin modified with PEGylated RGD and soluble KGF: Synthesis, characterization, and application in in vivo critical dermal wound. J. Biomed. Mater. Res. Part A Off. J. Soc. Biomater. Jpn. Soc. Biomater. Aust. Soc. Biomater. Korean Soc. Biomater. 2007, 82, 861–871. [Google Scholar] [CrossRef]
- Kim, B.S.; Lee, J.S.; Gao, G.; Cho, D.W. Direct 3D cell-printing of human skin with functional transwell system. Biofabrication 2017, 9, 025034. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Q.; Wen, J.; Liu, C.; Ma, C.; Bai, F.; Leng, X.; Chen, Z.; Xie, Z.; Mi, J.; Wu, X. Early-stage bilayer tissue-engineered skin substitute formed by adult skin progenitor cells produces an improved skin structure in vivo. Stem Cell Res. Ther. 2020, 11, 407. [Google Scholar] [CrossRef]
- Sierra-Sánchez, Á.; Fernández-González, A.; Lizana-Moreno, A.; Espinosa-Ibáñez, O.; Martinez-Lopez, A.; Guerrero-Calvo, J.; Fernández-Porcel, N.; Ruiz-García, A.; Ordóñez-Luque, A.; Carriel, V.; et al. Hyaluronic acid biomaterial for human tissue-engineered skin substitutes: Preclinical comparative in vivo study of wound healing. J. Eur. Acad. Dermatol. Venereol. 2020, 34, 2414–2427. [Google Scholar] [CrossRef]
- Lammers, G.; Verhaegen, P.D.; Ulrich, M.M.; Schalkwijk, J.; Middelkoop, E.; Weiland, D.; Nillesen, S.T.; Van Kuppevelt, T.H.; Daamen, W.F. An overview of methods for the in vivo evaluation of tissue-engineered skin constructs. Tissue Eng. Part B Rev. 2011, 17, 33–55. [Google Scholar] [CrossRef]
- Sun, M.; Wang, X.; Zhao, B. Quality estimation and influence factors of the larger chemically acellular nerve allografts in vitro. Chin. J. Reparative Reconstr. Surg. 2006, 20, 779–782. [Google Scholar]
- Boyce, S.T.; Simpson, P.S.; Rieman, M.T.; Warner, P.M.; Yakuboff, K.P.; Bailey, J.K.; Nelson, J.K.; Fowler, L.A.; Kagan, R.J. Randomized, Paired-Site Comparison of Autologous Engineered Skin Substitutes and Split-Thickness Skin Graft for Closure of Extensive, Full-Thickness Burns. J. Burn Care Res. 2017, 38, 61–70. [Google Scholar] [CrossRef] [PubMed]
- Bhardwaj, N.; Chouhan, D.; Mandal, B.B. Tissue Engineered Skin and Wound Healing: Current Strategies and Future Directions. Curr. Pharm. Des. 2017, 23, 3455–3482. [Google Scholar] [CrossRef] [PubMed]
- Durand-Herrera, D.; Campos, F.; Jaimes-Parra, B.D.; Sánchez-López, J.D.; Fernández-Valadés, R.; Alaminos, M.; Campos, A.; Carriel, V. Wharton’s jelly-derived mesenchymal cells as a new source for the generation of microtissues for tissue engineering applications. Histochem. Cell. Biol. 2018, 150, 379–393. [Google Scholar] [CrossRef]
- Shahabeddin, L.; Berthod, F.; Damour, O.; Collombel, C. Characterization of skin reconstructed on a chitosan-cross-linked collagen-glycosaminoglycan matrix. Skin Pharmacol. 1990, 3, 107–114. [Google Scholar] [CrossRef]
- Boyce, S.T. Skin substitutes from cultured cells and collagen-GAG polymers. Med. Biol. Eng. Comput. 1998, 36, 791–800. [Google Scholar] [CrossRef] [PubMed]
- Supp, A.P.; Wickett, R.R.; Swope, V.B.; Harriger, M.D.; Hoath, S.B.; Boyce, S.T. Incubation of cultured skin substitutes in reduced humidity promotes cornification in vitro and stable engraftment in athymic mice. Wound Repair Regen. 1999, 7, 226–237. [Google Scholar] [CrossRef]
- Boelsma, E.; Gibbs, S.; Faller, C.; Ponec, M. Characterization and comparison of reconstructed skin models: Morphological and immunohistochemical evaluation. Acta Derm. Venereol. 2000, 80, 82–88. [Google Scholar] [PubMed]
- Lee, D.Y.; Ahn, H.T.; Cho, K.H. A new skin equivalent model: Dermal substrate that combines de-epidermized dermis with fibroblast-populated collagen matrix. J. Dermatol. Sci. 2000, 23, 132–137. [Google Scholar] [CrossRef]
- Boyce, S.T.; Supp, A.P.; Swope, V.B.; Warden, G.D. Vitamin C regulates keratinocyte viability, epidermal barrier, and basement membrane in vitro, and reduces wound contraction after grafting of cultured skin substitutes. J. Investig. Dermatol. 2002, 118, 565–572. [Google Scholar] [CrossRef]
- Boyce, S.T.; Kagan, R.J.; Yakuboff, K.P.; Meyer, N.A.; Rieman, M.T.; Greenhalgh, D.G.; Warden, G.D. Cultured skin substitutes reduce donor skin harvesting for closure of excised, full-thickness burns. Ann. Surg. 2002, 235, 269–279. [Google Scholar] [CrossRef]
- Swope, V.B.; Supp, A.P.; Schwemberger, S.; Babcock, G.; Boyce, S. Increased expression of integrins and decreased apoptosis correlate with increased melanocyte retention in cultured skin substitutes. Pigment. Cell. Res. 2006, 19, 424–433. [Google Scholar] [CrossRef]
- Ng, K.W.; Hutmacher, D.W. Reduced contraction of skin equivalent engineered using cell sheets cultured in 3D matrices. Biomaterials 2006, 27, 4591–4598. [Google Scholar] [CrossRef]
- Armour, A.D.; Powell, H.M.; Boyce, S.T. Fluorescein diacetate for determination of cell viability in tissue-engineered skin. Tissue Eng. Part C Methods 2008, 14, 89–96. [Google Scholar] [CrossRef]
- Perng, C.K.; Kao, C.L.; Yang, Y.P.; Lin, H.T.; Lin, W.B.; Chu, Y.R.; Wang, H.J.; Ma, H.; Ku, H.H.; Chiou, S.H. Culturing adult human bone marrow stem cells on gelatin scaffold with pNIPAAm as transplanted grafts for skin regeneration. J. Biomed. Mater. Res. Part A Off. J. Soc. Biomater. Jpn. Soc. Biomater. Aust. Soc. Biomater. Korean Soc. Biomater. 2008, 84, 622–630. [Google Scholar] [CrossRef]
- Barai, N.D.; Boyce, S.T.; Hoath, S.B.; Visscher, M.O.; Kasting, G.B. Improved barrier function observed in cultured skin substitutes developed under anchored conditions. Skin Res. Technol. 2008, 14, 418–424. [Google Scholar] [CrossRef]
- Jean, J.; Lapointe, M.; Soucy, J.; Pouliot, R. Development of an in vitro psoriatic skin model by tissue engineering. J. Dermatol. Sci. 2009, 53, 19–25. [Google Scholar] [CrossRef]
- Kleiser, S.; Nyström, A. Interplay between Cell-Surface Receptors and Extracellular Matrix in Skin. Biomolecules 2020, 10, 1170. [Google Scholar] [CrossRef]
- Wang, X.; Liu, Y.; Deng, Z.; Dong, R.; Liu, Y.; Hu, S.; Li, Y.; Jin, Y. Inhibition of dermal fibrosis in self-assembled skin equivalents by undifferentiated keratinocytes. J. Dermatol. Sci. 2009, 53, 103–111. [Google Scholar] [CrossRef] [PubMed]
- Cho, D.I.; Kim, M.R.; Jeong, H.Y.; Jeong, H.C.; Jeong, M.H.; Yoon, S.H.; Kim, Y.S.; Ahn, Y. Mesenchymal stem cells reciprocally regulate the M1/M2 balance in mouse bone marrow-derived macrophages. Exp. Mol. Med. 2014, 46, e70. [Google Scholar] [CrossRef] [PubMed]
- Klingenberg, J.M.; McFarland, K.L.; Friedman, A.J.; Boyce, S.T.; Aronow, B.J.; Supp, D.M. Engineered human skin substitutes undergo large-scale genomic reprogramming and normal skin-like maturation after transplantation to athymic mice. J. Investig. Dermatol. 2010, 130, 587–601. [Google Scholar] [CrossRef] [PubMed]
- Smith, L.E.; Bonesi, M.; Smallwood, R.; Matcher, S.J.; MacNeil, S. Using swept-source optical coherence tomography to monitor the formation of neo-epidermis in tissue-engineered skin. J. Tissue Eng. Regen. Med. 2010, 4, 652–658. [Google Scholar] [CrossRef]
- Thakoersing, V.S.; Gooris, G.S.; Mulder, A.; Rietveld, M.; El Ghalbzouri, A.; Bouwstra, J.A. Unraveling barrier properties of three different in-house human skin equivalents. Tissue Eng. Part C Methods 2012, 18, 1–11. [Google Scholar] [CrossRef]
- Marxa, U.; Pickerta, D.; Heymerb, A.; Schmitt, R. Non-invasive quality control for production processes of artificial s kin equivalents by optical coherence tomography. Procedia CIRP 2013, 5, 128–132. [Google Scholar] [CrossRef]
- Klar, A.S.; Güven, S.; Biedermann, T.; Luginbühl, J.; Böttcher-Haberzeth, S.; Meuli-Simmen, C.; Meuli, M.; Martin, I.; Scherberich, A.; Reichmann, E. Tissue-engineered dermo-epidermal skin grafts prevascularized with adipose-derived cells. Biomaterials 2014, 35, 5065–5078. [Google Scholar] [CrossRef] [PubMed]
- Foubert, P.; Barillas, S.; Gonzalez, A.D.; Alfonso, Z.; Zhao, S.; Hakim, I.; Meschter, C.; Tenenhaus, M.; Fraser, J.K. Uncultured adipose-derived regenerative cells (ADRCs) seeded in collagen scaffold improves dermal regeneration, enhancing early vascularization and structural organization following thermal burns. Burns 2015, 41, 1504–1516. [Google Scholar] [CrossRef] [PubMed]
- Chung, E.; Rybalko, V.Y.; Hsieh, P.L.; Leal, S.L.; Samano, M.A.; Willauer, A.N.; Stowers, R.S.; Natesan, S.; Zamora, D.O.; Christy, R.J.; et al. Fibrin-based stem cell containing scaffold improves the dynamics of burn wound healing. Wound Repair Regen. 2016, 24, 810–819. [Google Scholar] [CrossRef]
- Ng, W.L.; Qi, J.T.Z.; Yeong, W.Y.; Naing, M.W. Proof-of-concept: 3D bioprinting of pigmented human skin constructs. Biofabrication 2018, 10, 025005. [Google Scholar] [CrossRef]
- Gil-Cifuentes, L.; Jiménez, R.A.; Fontanilla, M.R. Evaluation of collagen type I scaffolds including gelatin-collagen microparticles and Aloe vera in a model of full-thickness skin wound. Drug Deliv. Transl. Res. 2019, 9, 25–36. [Google Scholar] [CrossRef]
- Zahiri, M.; Khanmohammadi, M.; Goodarzi, A.; Ababzadeh, S.; Sagharjoghi Farahani, M.; Mohandesnezhad, S.; Bahrami, N.; Nabipour, I.; Ai, J. Encapsulation of curcumin loaded chitosan nanoparticle within poly (ε-caprolactone) and gelatin fiber mat for wound healing and layered dermal reconstitution. Int. J. Biol. Macromol. 2020, 153, 1241–1250. [Google Scholar] [CrossRef]
- Tiirikainen, M.L.; Woetmann, A.; Norsgaard, H.; Santamaria-Babí, L.F.; Lovato, P. Ex vivo culture of lesional psoriasis skin for pharmacological testing. J. Dermatol. Sci. 2020, 97, 109–116. [Google Scholar] [CrossRef]
- Breuls, R.G.; Mol, A.; Petterson, R.; Oomens, C.W.; Baaijens, F.P.; Bouten, C.V. Monitoring local cell viability in engineered tissues: A fast, quantitative, and nondestructive approach. Tissue Eng. 2003, 9, 269–281. [Google Scholar] [CrossRef] [PubMed]
- Marquardt, L.M.; Sakiyama-Elbert, S.E. Engineering peripheral nerve repair. Curr. Opin. Biotechnol. 2013, 24, 887–892. [Google Scholar] [CrossRef]
- Freshney, R.; Stacey, G.; Auerbach, J. Culture of Human Stem Cells, 1st ed.; Wiley-Liss: New York, NY, USA, 2007. [Google Scholar]
- Armeni, T.; Damiani, E.; Battino, M.; Greci, L.; Principato, G. Lack of in vitro protection by a common sunscreen ingredient on UVA-induced cytotoxicity in keratinocytes. Toxicology 2004, 203, 165–178. [Google Scholar] [CrossRef] [PubMed]
- Garzón, I.; Carriel, V.; Marín-Fernández, A.B.; Oliveira, A.C.; Garrido-Gómez, J.; Campos, A.; Sánchez-Quevedo Mdel, C.; Alaminos, M. A combined approach for the assessment of cell viability and cell functionality of human fibrochondrocytes for use in tissue engineering. PLoS ONE 2012, 7, e51961. [Google Scholar] [CrossRef] [PubMed]
- Dai, N.T.; Yeh, M.K.; Liu, D.D.; Adams, E.F.; Chiang, C.H.; Yen, C.Y.; Shih, C.M.; Sytwu, H.K.; Chen, T.M.; Wang, H.J.; et al. A co-cultured skin model based on cell support membranes. Biochem. Biophys. Res. Commun. 2005, 329, 905–908. [Google Scholar] [CrossRef] [PubMed]
- Vicanová, J.; Boelsma, E.; Mommaas, A.M.; Kempenaar, J.A.; Forslind, B.; Pallon, J.; Egelrud, T.; Koerten, H.K.; Ponec, M. Normalization of epidermal calcium distribution profile in reconstructed human epidermis is related to improvement of terminal differentiation and stratum corneum barrier formation. J. Investig. Dermatol. 1998, 111, 97–106. [Google Scholar] [CrossRef]
- Martin-Piedra, M.A.; Garzon, I.; Oliveira, A.C.; Alfonso-Rodriguez, C.A.; Carriel, V.; Scionti, G.; Alaminos, M. Cell viability and proliferation capability of long-term human dental pulp stem cell cultures. Cytotherapy 2014, 16, 266–277. [Google Scholar] [CrossRef] [PubMed]
- Campos, F.; Bonhome-Espinosa, A.B.; Vizcaino, G.; Rodriguez, I.A.; Duran-Herrera, D.; López-López, M.T.; Sánchez-Montesinos, I.; Alaminos, M.; Sánchez-Quevedo, M.C.; Carriel, V. Generation of genipin cross-linked fibrin-agarose hydrogel tissue-like models for tissue engineering applications. Biomed. Mater. 2018, 13, 025021. [Google Scholar] [CrossRef] [PubMed]
- Dvali, L.T.; Dagum, A.B.; Pang, C.Y.; Kerluke, L.D.; Catton, P.; Pennock, P.; Mahoney, J.L. Effect of radiation on skin expansion and skin flap viability in pigs. Plast. Reconstr. Surg. 2000, 106, 624–629. [Google Scholar] [CrossRef]
- Miyazaki, H.; Tsunoi, Y.A.; Takami Sato, S.; Akashi, M.; Saitoh, D. A novel strategy to engineer pre-vascularized 3-dimensional skin substitutes to achieve efficient, functional engraftment. Sci. Rep. 2019, 9, 7797. [Google Scholar] [CrossRef] [PubMed]
- Mazzini, G.; Danova, M. Fluorochromes for DNA Staining and Quantitation. Methods Mol. Biol. 2017, 1560, 239–259. [Google Scholar]
- Mazzini, G.; Ferrari, C.; Erba, E. Dual excitation multi- fluorescence flow cytometry for detailed analyses of viability and apoptotic cell transition. Eur. J. Histochem. 2003, 47, 289–298. [Google Scholar] [CrossRef][Green Version]
- Alaminos, M.; Sanchez-Quevedo, M.C.; Muñoz-Avila, J.I.; García, J.M.; Crespo, P.V.; González-Andrades, M.; Campos, A. Evaluation of the viability of cultured corneal endothelial cells by quantitative electron probe X-ray microanalysis. J. Cell. Physiol. 2007, 211, 692–698. [Google Scholar] [CrossRef]
- Vico, M.; Rodríguez-Morata, A.; Garzón, I.; Campos, F.; Jaimes-Parra, B.; Pérez-Köhler, B.; Buján, J.; Alaminos, M.; Sánchez-Quevedo, M.C. Cell viability evaluation of transdifferentiated endothelial-like cells by quantitative electron-probe X-ray microanalysis for tissue engineering. Histol. Histopathol. 2015, 30, 1333–1340. [Google Scholar]
- Tylko, G. Cells on biomaterials--some aspects of elemental analysis by means of electron probes. J. Microsc. 2016, 261, 185–195. [Google Scholar] [CrossRef]
- Carriel, V.; Campos, F.; Aneiros-Fernández, J.; Kiernan, J.A. Tissue Fixation and Processing for the Histological Identification of Lipids. Methods Mol. Biol. 2017, 1560, 197–206. [Google Scholar]
- Carriel, V.; Garzón, I.; Alaminos, M.; Cornelissen, M. Histological assessment in peripheral nerve tissue engineering. Neural Regen. Res. 2014, 9, 1657–1660. [Google Scholar] [CrossRef] [PubMed]
- Muhart, M.; McFalls, S.; Kirsner, R.S.; Elgart, G.W.; Kerdel, F.; Sabolinski, M.L.; Hardin-Young, J.; Eaglstein, W.H. Behavior of tissue-engineered skin: A comparison of a living skin equivalent, autograft, and occlusive dressing in human donor sites. Arch. Dermatol. 1999, 135, 913–918. [Google Scholar] [CrossRef]
- Carriel, V.; Garzón, I.; Jiménez, J.M.; Oliveira, A.C.; Arias-Santiago, S.; Campos, A.; Sánchez-Quevedo, M.C.; Alaminos, M. Epithelial and stromal developmental patterns in a novel substitute of the human skin generated with fibrin-agarose biomaterials. Cells Tissues Organs. 2012, 196, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Chardack, W.M. The use of synthetic substitutes for skin in the treatment of burns. Mil. Med. 1962, 127, 335–344. [Google Scholar] [CrossRef] [PubMed]
- Chato-Astrain, J.; Campos, F.; Roda, O.; Miralles, E.; Durand-Herrera, D.; Sáez-Moreno, J.A.; García-García, S.; Alaminos, M.; Campos, A.; Carriel, V. In vivo Evaluation of Nanostructured Fibrin-Agarose Hydrogels With Mesenchymal Stem Cells for Peripheral Nerve Repair. Front. Cell. Neurosci. 2018, 12, 501. [Google Scholar] [CrossRef]
- Lamme, E.N.; de Vries, H.J.; van Veen, H.; Gabbiani, G.; Westerhof, W.; Middelkoop, E. Extracellular matrix characterization during healing of full-thickness wounds treated with a collagen/elastin dermal substitute shows improved skin regeneration in pigs. J. Histochem. Cytochem. 1996, 44, 1311–1322. [Google Scholar] [CrossRef] [PubMed]
- Butler, C.E.; Orgill, D.P.; Yannas, I.V.; Compton, C.C. Effect of keratinocyte seeding of collagen-glycosaminoglycan membranes on the regeneration of skin in a porcine model. Plast. Reconstr. Surg. 1998, 101, 1572–1579. [Google Scholar] [CrossRef] [PubMed]
- Compton, C.C.; Butler, C.E.; Yannas, I.V.; Warland, G.; Orgill, D.P. Organized skin structure is regenerated in vivo from collagen-GAG matrices seeded with autologous keratinocytes. J. Investig. Dermatol. 1998, 110, 908–916. [Google Scholar] [CrossRef]
- Lamme, E.N.; van Leeuwen, R.T.; Jonker, A.; van Marle, J.; Middelkoop, E. Living skin substitutes: Survival and function of fibroblasts seeded in a dermal substitute in experimental wounds. J. Investig. Dermatol. 1998, 111, 989–995. [Google Scholar] [CrossRef]
- Pandit, A.; Ashar, R.; Feldman, D. The effect of TGF-beta delivered through a collagen scaffold on wound healing. J. Investig. Surg. 1999, 12, 89–100. [Google Scholar]
- Lamme, E.N.; Van Leeuwen, R.T.; Brandsma, K.; Van Marle, J.; Middelkoop, E. Higher numbers of autologous fibroblasts in an artificial dermal substitute improve tissue regeneration and modulate scar tissue formation. J. Pathol. 2000, 190, 595–603. [Google Scholar] [CrossRef]
- Grant, I.; Warwick, K.; Marshall, J.; Green, C.; Martin, R. The co-application of sprayed cultured autologous keratinocytes and autologous fibrin sealant in a porcine wound model. Br. J. Plast. Surg. 2002, 55, 219–227. [Google Scholar] [CrossRef] [PubMed]
- Breitbart, A.S.; Laser, J.; Parrett, B.; Porti, D.; Grant, R.T.; Grande, D.A.; Mason, J.M. Accelerated diabetic wound healing using cultured dermal fibroblasts retrovirally transduced with the platelet-derived growth factor B gene. Accelerated diabetic wound healing using cultured dermal fibroblasts retrovirally transduced with the platelet-derived growth factor B gene. Ann. Plast. Surg. 2003, 51, 409–414. [Google Scholar]
- Middelkoop, E.; van den Bogaerdt, A.J.; Lamme, E.N.; Hoekstra, M.J.; Brandsma, K.; Ulrich, M.M. Porcine wound models for skin substitution and burn treatment. Biomaterials 2004, 25, 1559–1567. [Google Scholar] [CrossRef]
- Llames, S.G.; Del Rio, M.; Larcher, F.; García, E.; García, M.; Escamez, M.J.; Jorcano, J.L.; Holguín, P.; Meana, A. Human plasma as a dermal scaffold for the generation of a completely autologous bioengineered skin. Transplantation 2004, 77, 350–355. [Google Scholar] [CrossRef]
- Price, R.D.; Das-Gupta, V.; Harris, P.A.; Leigh, I.M.; Navsaria, H.A. The role of allogenic fibroblasts in an acute wound healing model. Plast. Reconstr. Surg. 2004, 113, 1719–1729. [Google Scholar] [CrossRef]
- Druecke, D.; Lamme, E.N.; Hermann, S.; Pieper, J.; May, P.S.; Steinau, H.U.; Steinstraesser, L. Modulation of scar tissue formation using different dermal regeneration templates in the treatment of experimental full-thickness wounds. Wound Repair Regen. 2004, 12, 518–527. [Google Scholar] [CrossRef]
- Myers, S.R.; Partha, V.N.; Soranzo, C.; Price, R.D.; Navsaria, H.A. Hyalomatrix: A temporary epidermal barrier, hyaluronan delivery, and neodermis induction system for keratinocyte stem cell therapy. Tissue Eng. 2007, 13, 2733–2741. [Google Scholar] [CrossRef]
- Richters, C.D.; Pirayesh, A.; Hoeksema, H.; Kamperdijk, E.W.; Kreis, R.W.; Dutrieux, R.P.; Monstrey, S.; Hoekstra, M.J. Development of a dermal matrix from glycerol preserved allogeneic skin. Cell. Tissue. Bank. 2008, 9, 309–315. [Google Scholar] [CrossRef][Green Version]
- Breen, A.M.; Dockery, P.; O’Brien, T.; Pandit, A.S. The use of therapeutic gene eNOS delivered via a fibrin scaffold enhances wound healing in a compromised wound model. Biomaterials 2008, 29, 3143–3151. [Google Scholar] [CrossRef] [PubMed]
- Bao, L.; Yang, W.; Mao, X.; Mou, S.; Tang, S. Agar/collagen membrane as skin dressing for wounds. Biomed. Mater. 2008, 3, 044108. [Google Scholar] [CrossRef] [PubMed]
- Windsor, M.L.; Eisenberg, M.; Gordon-Thomson, C.; Moore, G.P. A novel model of wound healing in the SCID mouse using a cultured human skin substitute. Australas. J. Dermatol. 2009, 50, 29–35. [Google Scholar] [CrossRef] [PubMed]
- Scherer, S.S.; Pietramaggiori, G.; Matthews, J.; Perry, S.; Assmann, A.; Carothers, A.; Demcheva, M.; Muise-Helmericks, R.C.; Seth, A.; Vournakis, J.N.; et al. Poly-N-acetyl glucosamine nanofibers: A new bioactive material to enhance diabetic wound healing by cell migration and angiogenesis. Ann. Surg. 2009, 250, 322–330. [Google Scholar] [CrossRef] [PubMed]
- Matsumoto, Y.; Kuroyanagi, Y. Design of a matrix for cultured dermal substitute suitable for simultaneous transplantation with auto-skin graft: Evaluation in animal test. J. Biomater. Sci. Polym. Ed. 2010, 21, 83–94. [Google Scholar] [CrossRef]
- Lammers, G.; Gilissen, C.; Nillesen, S.T.; Uijtdewilligen, P.J.; Wismans, R.G.; Veltman, J.A.; Daamen, W.F.; van Kuppevelt, T.H. High density gene expression microarrays and gene ontology analysis for identifying processes in implanted tissue engineering constructs. Biomaterials 2010, 31, 8299–8312. [Google Scholar] [CrossRef]
- Huang, S.; Xu, Y.; Wu, C.; Sha, D.; Fu, X. In vitro constitution and in vivo implantation of engineered skin constructs with sweat glands. Biomaterials 2010, 31, 5520–5525. [Google Scholar] [CrossRef]
- Nillesen, S.T.; Lammers, G.; Wismans, R.G.; Ulrich, M.M.; Middelkoop, E.; Spauwen, P.H.; Faraj, K.A.; Schalkwijk, J.; Daamen, W.F.; van Kuppevelt, T.H. Design and in vivo evaluation of a molecularly defined acellular skin construct: Reduction of early contraction and increase in early blood vessel formation. Acta Biomater. 2011, 7, 1063–1071. [Google Scholar] [CrossRef]
- Michael, S.; Sorg, H.; Peck, C.T.; Reimers, K.; Vogt, P.M. The mouse dorsal skin fold chamber as a means for the analysis of tissue engineered skin. Burns 2013, 39, 82–88. [Google Scholar] [CrossRef] [PubMed]
- Van Kilsdonk, J.W.; van den Bogaard, E.H.; Jansen, P.A.; Bos, C.; Bergers, M.; Schalkwijk, J. An in vitro wound healing model for evaluation of dermal substitutes. Wound Repair Regen. 2013, 21, 890–896. [Google Scholar] [CrossRef] [PubMed]
- Udeabor, S.E.; Herrera-Vizcaíno, C.; Sader, R.; Kirkpatrick, C.J.; Al-Maawi, S.; Ghanaati, S. Characterization of the Cellular Reaction to a Collagen-Based Matrix: An In Vivo Histological and Histomorphometrical Analysis. Materials 2020, 13, 2730. [Google Scholar] [CrossRef]
- Breitbart, A.S.; Mason, J.M.; Urmacher, C.; Barcia, M.; Grant, R.T.; Pergolizzi, R.G.; Grande, D.A. Gene-enhanced tissue engineering: Applications for wound healing using cultured dermal fibroblasts transduced retrovirally with the PDGF-B gene. Ann. Plast. Surg. 1999, 43, 632–639. [Google Scholar] [CrossRef] [PubMed]
- Breitbart, A.S.; Grande, D.A.; Laser, J.; Barcia, M.; Porti, D.; Malhotra, S.; Kogon, A.; Grant, R.T.; Mason, J.M. Treatment of ischemic wounds using cultured dermal fibroblasts transduced retrovirally with PDGF-B and VEGF121 genes. Ann. Plast. Surg. 2001, 46, 555–561. [Google Scholar] [CrossRef] [PubMed]
- Lamme, E.N.; van Leeuwen, R.T.; Mekkes, J.R.; Middelkoop, E. Allogeneic fibroblasts in dermal substitutes induce inflammation and scar formation. Wound Repair Regen. 2002, 10, 152–160. [Google Scholar] [CrossRef]
- Marghoob, A.A.; Swindle, L.D.; Moricz, C.Z.; Sanchez Negron, F.A.; Slue, B.; Halpern, A.C.; Kopf, A.W. Instruments and new technologies for the in vivo diagnosis of melanoma. J. Am. Acad. Dermatol. 2003, 49, 777–797. [Google Scholar] [CrossRef]
- De Vries, H.J.; Middelkoop, E.; van Heemstra-Hoen, M.; Wildevuur, C.H.; Westerhof, W. Stromal cells from subcutaneous adipose tissue seeded in a native collagen/elastin dermal substitute reduce wound contraction in full thickness skin defects. Lab. Investig. J. Tech. Methods Pathol. 1995, 73, 532–540. [Google Scholar]
- Hansbrough, J.F.; Morgan, J.L.; Greenleaf, G.E.; Bartel, R. Composite grafts of human keratinocytes grown on a polyglactin mesh-cultured fibroblast dermal substitute function as a bilayer skin replacement in full-thickness wounds on athymic mice. J Burn. Care Rehabil. 1993, 14, 485–494. [Google Scholar] [CrossRef]
- Doillon, C.J.; Whyne, C.F.; Berg, R.A.; Olson, R.M.; Silver, F.H. Fibroblast-collagen sponge interactions and the spatial deposition of newly synthesized collagen fibers in vitro and in vivo. Scan. Electron Microsc. 1984, Pt 3, 1313–1320. [Google Scholar]
- De Vries, H.J.; Mekkes, J.R.; Middelkoop, E.; Hinrichs, W.L.; Wildevuur, C.R.; Westerhof, W. Dermal substitutes for full-thickness wounds in a one-stage grafting model. Wound Repair Regen. 1993, 1, 244–252. [Google Scholar] [CrossRef] [PubMed]
- Wang, H.J.; Pieper, J.; Schotel, R.; van Blitterswijk, C.A.; Lamme, E.N. Stimulation of skin repair is dependent on fibroblast source and presence of extracellular matrix. Tissue Eng. 2004, 10, 1054–1064. [Google Scholar] [CrossRef] [PubMed]
- Godwin, A.R.F.; Singh, M.; Lockhart-Cairns, M.P.; Alanazi, Y.F.; Cain, S.A.; Baldock, C. The role of fibrillin and microfibril binding proteins in elastin and elastic fibre assembly. Matrix Biol. 2019, 84, 17–30. [Google Scholar] [CrossRef]
- Pontiggia, L.; Biedermann, T.; Meuli, M.; Widmer, D.; Böttcher-Haberzeth, S.; Schiestl, C.; Schneider, J.; Braziulis, E.; Montaño, I.; Meuli-Simmen, C.; et al. Markers to evaluate the quality and self-renewing potential of engineered human skin substitutes in vitro and after transplantation. J. Investig. Dermatol. 2009, 129, 480–490. [Google Scholar] [CrossRef] [PubMed]
- Pereira, R.F.; Barrias, C.C.; Bártolo, P.J.; Granja, P.L. Cell-instructive pectin hydrogels crosslinked via thiol-norbornene photo-click chemistry for skin tissue engineering. Acta Biomater. 2018, 66, 282–293. [Google Scholar] [CrossRef]
- Zajac, E.; Schweighofer, B.; Kupriyanova, T.A.; Juncker-Jensen, A.; Minder, P.; Quigley, J.P.; Deryugina, E.I. Angiogenic capacity of M1- and M2-polarized macrophages is determined by the levels of TIMP-1 complexed with their secreted proMMP-9. Exp. Mol. Med. 2014, 46, e70. [Google Scholar] [CrossRef]
- Pavelka, M.; Jürgen, R. Functional Ultrastructure: Atlas of Tissue Biology and Pathology; Springer: Berlin/Heidelberg, Germany, 2015. [Google Scholar]
- Auxenfans, C.; Fradette, J.; Lequeux, C.; Germain, L.; Kinikoglu, B.; Bechetoille, N.; Braye, F.; Auger, F.A.; Damour, O. Evolution of three dimensional skin equivalent models reconstructed in vitro by tissue engineering. Eur. J. Dermatol. 2009, 19, 107–113. [Google Scholar] [CrossRef]
- Carriel, V.; Scionti, G.; Campos, F.; Roda, O.; Castro, B.; Cornelissen, M.; Garzón, I.; Alaminos, M. In vitro characterization of a nanostructured fibrin agarose bio-artificial nerve substitute. J. Tissue Eng. Regen. Med. 2017, 11, 1412–1426. [Google Scholar] [CrossRef]
- Tearney, G.J.; Brezinski, M.E.; Bouma, B.E.; Boppart, S.A.; Pitris, C.; Southern, J.F.; Fujimoto, J.G. In vivo endoscopic optical biopsy with optical coherence tomography. Science 1997, 276, 2037–2039. [Google Scholar] [CrossRef]
- Welzel, J.; Lankenau, E.; Birngruber, R.; Engelhardt, R. Optical coherence tomography of the human skin. J. Am. Acad. Dermatol. 1997, 37, 958–963. [Google Scholar] [CrossRef]
- Gambichler, T.; Moussa, G.; Sand, M.; Sand, D.; Altmeyer, P.; Hoffmann, K. Applications of optical coherence tomography in dermatology. J. Dermatol. Sci. 2005, 40, 85–94. [Google Scholar] [CrossRef] [PubMed]
- Deegan, A.J.; Wang, W.; Men, S.; Li, Y.; Song, S.; Xu, J.; Wang, R.K. Optical coherence tomography angiography monitors human cutaneous wound healing over time. Quant. Imaging Med. Surg. 2018, 8, 135–150. [Google Scholar] [CrossRef]
- Ulrich, M.; Stockfleth, E.; Roewert-Huber, J.; Astner, S. Noninvasive diagnostic tools for nonmelanoma skin cancer. Br. J. Dermatol. 2007, 157 (Suppl. S2), 56–58. [Google Scholar] [CrossRef]
- Moulisová, V.; Jiřík, M.; Schindler, C.; Červenková, L.; Pálek, R.; Rosendorf, J.; Arlt, J.; Bolek, L.; Šůsová, S.; Nietzsche, S.; et al. Novel morphological multi-scale evaluation system for quality assessment of decellularized liver scaffolds. J. Tissue Eng. 2020, 11, 2041731420921121. [Google Scholar] [CrossRef] [PubMed]
- Freytes, D.O.; Rundell, A.E.; Vande Geest, J.; Vorp, D.A.; Webster, T.J.; Badylak, S.F. Analytically derived material properties of multilaminated extracellular matrix devices using the ball-burst test. Biomaterials 2005, 26, 5518–5531. [Google Scholar] [CrossRef]
- Badylak, S.; Kokini, K.; Tullius, B.; Whitson, B. Strength over time of a resorbable bioscaffold for body wall repair in a dog model. J. Surg. Res. 2001, 99, 282–287. [Google Scholar] [CrossRef] [PubMed]
- Ko, R.; Kazacos, E.A.; Snyder, S.; Ernst, D.M.; Lantz, G.C. Tensile strength comparison of small intestinal submucosa body wall repair. J. Surg. Res. 2006, 135, 9–17. [Google Scholar] [CrossRef] [PubMed]
- Gloeckner, D.C.; Sacks, M.S.; Billiar, K.L.; Bachrach, N. Mechanical evaluation and design of a multilayered collagenous repair biomaterial. J. Biomed. Mater. Res. 2000, 52, 365–373. [Google Scholar] [CrossRef]
- Shah, R.G.; De Vore, D.; Silver, F.H. Biomechanical analysis of decellularized dermis and skin: Initial in vivo observations using optical cohesion tomography and vibrational analysis. J. Biomed. Mater. Res. Part A Off. J. Soc. Biomater. Jpn. Soc. Biomater. Aust. Soc. Biomater. Korean Soc. Biomater. 2018, 106, 1421–1427. [Google Scholar] [CrossRef] [PubMed]
- Heraud, S.; Delalleau, A.; Houcine, A.; Guiraud, B.; Bacqueville, D.; Payre, B.; Delisle, M.B.; Bessou-Touya, S.; Damour, O. Structural and Biomechanical Characterization of a Scaffold-Free Skin Equivalent Model via Biophysical Methods. Skin Pharmacol. Physiol. 2020, 33, 17–29. [Google Scholar] [CrossRef]
- Lafrance, H.; Yahia, L.; Germain, L.; Auger, F.A. Mechanical properties of human skin equivalents submitted to cyclic tensile forces. Skin Res. Technol. 1998, 4, 228–236. [Google Scholar] [CrossRef] [PubMed]
- Lafrance, H.; Guillot, M.; Germain, L.; Auger, F.A. A method for the evaluation of tensile properties of skin equivalents. Med. Eng. Phys. 1995, 17, 537–543. [Google Scholar] [CrossRef]
- Zahouani, H.; Pailler-Mattei, C.; Sohm, B.; Vargiolu, R.; Cenizo, V.; Debret, R. Characterization of the mechanical properties of a dermal equivalent compared with human skin in vivo by indentation and static friction tests. Skin Res. Technol. 2009, 15, 68–76. [Google Scholar] [CrossRef] [PubMed]
- Ahlfors, J.E.; Billiar, K.L. Biomechanical and biochemical characteristics of a human fibroblast-produced and remodeled matrix. Biomaterials 2007, 28, 2183–2191. [Google Scholar] [CrossRef]
- Berthod, F.; Saintigny, G.; Chretien, F.; Hayek, D.; Collombel, C.; Damour, O. Optimization of thickness, pore size and mechanical properties of a biomaterial designed for deep burn coverage. Clin. Mater. 1994, 15, 259–265. [Google Scholar] [CrossRef]
- Sasso, M.; Palmieri, G.; Chiappini, G.; Amodio, D. Characterization of hyperelastic rubber-like materials by biaxial and uniaxial stretching tests based on optical methods. Polym. Test. 2008, 27, 995–1004. [Google Scholar] [CrossRef]
- Boyce, S.T.; Supp, A.P.; Harriger, M.D.; Pickens, W.L.; Wickett, R.R.; Hoath, S.B. Surface electrical capacitance as a noninvasive index of epidermal barrier in cultured skin substitutes in athymic mice. J. Investig. Dermatol. 1996, 107, 82–87. [Google Scholar] [CrossRef]
- Higounenc, I.; Démarchez, M.; Régnier, M.; Schmidt, R.; Ponec, M.; Shroot, B. Improvement of epidermal differentiation and barrier function in reconstructed human skin after grafting onto athymic nude mice. Arch. Dermatol. Res. 1994, 286, 107–114. [Google Scholar] [CrossRef]
- Kasting, G.B.; Filloon, T.G.; Francis, W.R.; Meredith, M.P. Improving the sensitivity of in vitro skin penetration experiments. Pharm. Res. 1994, 11, 1747–1754. [Google Scholar] [CrossRef]
- Barai, N.D.; Supp, A.P.; Kasting, G.B.; Visscher, M.O.; Boyce, S.T. Improvement of epidermal barrier properties in cultured skin substitutes after grafting onto athymic mice. Skin Pharmacol. Physiol. 2007, 20, 21–28. [Google Scholar] [CrossRef]
- Zor, F.; Selek, F.N.; Orlando, G.; Williams, D.F. Biocompatibility in regenerative nanomedicine. Nanomedicine 2019, 14, 2763–2775. [Google Scholar] [CrossRef] [PubMed]
- Al-Maawi, S.; Mota, C.; Kubesch, A.; James Kirkpatrick, C.; Moroni, L.; Ghanaati, S. Multiwell three-dimensional systems enable in vivo screening of immune reactions to biomaterials: A new strategy toward translational biomaterial research. J. Mater. Sci. Mater. Med. 2019, 30, 61. [Google Scholar] [CrossRef]
- Campos, F.; Bonhome-Espinosa, A.B.; Carmona, R.; Durán, J.D.G.; Kuzhir, P.; Alaminos, M.; López-López, M.T.; Rodriguez, I.A.; Carriel, V. In vivo time-course biocompatibility assessment of biomagnetic nanoparticles-based biomaterials for tissue engineering applications. Mater. Sci. Eng. C Mater. Biol. Appl. 2021, 118, 111476. [Google Scholar] [CrossRef] [PubMed]
- Carriel, V.; Vizcaíno-López, G.; Chato-Astrain, J.; Durand-Herrera, D.; Alaminos, M.; Campos, A.; Sánchez-Montesinos, I.; Campos, F. Scleral surgical repair through the use of nanostructured fibrin/agarose-based films in rabbits. Exp. Eye Res. 2019, 186, 107717. [Google Scholar] [CrossRef]
- Mikos, A.G.; McIntire, L.V.; Anderson, J.M.; Babensee, J.E. Host response to tissue engineered devices. Adv. Drug Deliv. Rev. 1998, 33, 111–139. [Google Scholar] [PubMed]
- Southern, E.M. Detection of specific sequences among DNA fragments separated by gel electrophoresis. J. Mol. Biol. 1975, 98, 503–517. [Google Scholar] [CrossRef]
- Badylak, S.F. The extracellular matrix as a biologic scaffold material. Biomaterials 2007, 28, 3587–3593. [Google Scholar] [CrossRef]
- Yannas, I.V.; Burke, J.F.; Warpehoski, M.; Stasikelis, P.; Skrabut, E.M.; Orgill, D.; Giard, D.J. Prompt, long-term functional replacement of skin. Trans. Am. Soc. Artif. Intern. Organs. 1981, 27, 19–23. [Google Scholar]


| Advantages | Limitations | |
|---|---|---|
| Autografts |
|
|
| Allografts/Xenografts |
|
|
| Dressings |
|
|
| Tissue-engineered skin substitutes |
|
|
| Construct | Macroscopic Evaluation | Cell Viability | Histology | Immunohisto-Chemistry | Gene Expression | Electron Microscopy | Epidermal Barrier |
|---|---|---|---|---|---|---|---|
| Collagen-GAG-chitosan + FBs & KCs [91] | HE | X | |||||
| Collagen-GAG + human FBs & KCs [92] | HE | SEC | |||||
| Fibrin + human FBs & KCs [62] | HE | Keratin 10, (pan)cytokeratin, laminin, type IV collagen | |||||
| Collagen-GAG + human FBs & KCs [93] | Toluidine blue | ||||||
| Human DED + KCs vs RHE [94] | MTT | HE | Keratin 1, keratin 6, keratin 10, SKALP, transglutaminase I, involucrin, loricrin, SPRRs | ||||
| DED + collagen + human FBs & KCs [95] | HE | Keratin 1, involucrin, loricrin, filaggrin | |||||
| Collagen-GAG + human FBs & KCs +/− Vit C [96] | BrdU, MTT | HE | Collagen IV, collagen VII, laminin 5 | X | SEC | ||
| Collagen-GAG + human FBs & KCs [97] | X | HE | |||||
| Collagen-GAG-chitosan + serum + human FBs & KCs [53] | Hematoxylin-phloxine-saffron | Keratin 10, keratin 14, transglutaminase, fibronectin, elastin, fibrillin 1, filaggrin, laminin, involucrin, integrin, collagen I, III, IV, V, Ki67 | X | ||||
| Collagen + human FBs & KCs & melanocytes [98] | HE | Integrin, fibronectin, laminin, collagen IV, HLA-ABC | SEC | ||||
| Collagen-GAG or PLGA +/− human FBs & KCs [99] | X | Live/dead | HE | (Pan)cytokeratin, laminin, collagen I, HLA-ABC | X | ||
| Acellular human dermis + human FBs & KCs [61] | HE | a-SMA, collagen IV, VII, BP180 antigen (collagen XVII), Ki67 | |||||
| Collagen-GAG + human KCs & FBs [100] | FdA, MTT | HE | |||||
| Gelatin-acrylamide + human BMSCs [101] | MTT | (Pan)cytokeratin, e-cadherin anti-CD13, CD34, CD44, CD45, CD49b, CD81, AC133, SH2, SH3 | X | ||||
| PLLA vs PLGA + human KCs & FBs [63] | MTT | HE, Picrosirius red staining | Anti CD31, CD68, CD45RC | X | |||
| Collagen-GAG + human FBs & KCs [102] | MTT | Toluidine Blue | Transepidermal water loss, H2O penetration, 14C-niacinamide permeability | ||||
| Dermal component + human healthy vs psoriatic FBs & KCs [103] | X | Masson’s trichrome | Keratin 10, involucrin, loricrin, filaggrin, laminin V, Ki67 | ||||
| Collagen-elastin + pancreatic SCs [70] | MTT, DAPI | HE | Keratin 10, keratin 14, fillagrin | PDX-1, GATA-1 genes | |||
| Poly-N-acetyl-glucosamine vs cellulose [104] | Trypan blue, MTT | X | |||||
| DED + KCs & FBs [105] | HE | Keratin 5, keratin 10, integrin | Collagen, bFGF, TGFb1 mRNA | X | |||
| Collagen + SGC + EGF + human FBs & KCs [106] | MTT | HE | Keratin 7, keratin 14, keratin 19, CEA | ||||
| Collagen-GAG + human FBs & KCs [107] | HE | KRT2, KRT15, loricrin, CILP, POSTN, OGN | DEFB4, KRT2, S100A7A, S100A12, SPRR2C, LOR, CD36, TCNI, GDA | ||||
| DED + collagen + human FBs & KCs [108] | HE | ||||||
| FDM vs LEM vs FTM [109] | HE | Keratin 10, keratin 16, filaggrin, loricrin, involucrin, aquoporin 3 | X | Benzocaine diffusion | |||
| Fibrin-agarose + human FBs & KCs [65] | HE, Picrosirius red staining, Alcian blue, Gomori, Orcein | Keratin 1, keratin 5, keratin 10, filaggrin, involucrin | X | ||||
| Human KCs [110] | MTT | HE | OCT | ||||
| Fibrin/collagen + KCs +/− FBs, SVF, ASCs [111] | HE | Keratin 16, keratin 17, a-SMA, laminin 5, collagen I, anti CD31, CD34, CD73, CD90, aSMA, DAPI, vWF, Ki67 | X | ||||
| Collagen + ADRCs [112] | HE | Anti CD31, CD45, CD90, CD34 | |||||
| DED + hAECs + human FBs | HE, Periodic acid-Schiff | Keratin 10, keratin 14, keratin 18, keratin 19, filaggrin, laminin, desmoglein, collagen IV, Ki67 | X | ||||
| Pegylated fibrin + ASCs [113] | HE, Alizarin Red S, Oil Red O, Sirius red/Fast green | a-SMA, anti CD68, CD206 | |||||
| Collagen-GAG +/− ad-MVF [75] | HE, Sirius red | (Pan)cytokeratin, anti CD31, GFP/CD31 | |||||
| S-dECM vs Collagen type I-HSE bioink [78] | Live/dead | HE, Masson’s trichrome, Alcian blue, laminin, DAPI | Anti CD31, CD34, CD133, CD45 | Wettability, permeability, SEC | |||
| 3D pigmented human skin construct [114] | X | HE, Fontana Masson | Keratin 1, keratin 6, collagen IV, VII, anti HMB45 | X | |||
| Type I collagen + gelatin-collagen microparticles and Aloe vera [115] | MTT | HE | |||||
| FN-G + HUVEC + FBs + KCs (87) | X | Live/dead | HE, Masson’s trichrome | Laminin 5, anti CD31 | |||
| Fibrin-agarose + MSCs [67] | HE, Picrosirius red, Periodic acid-Schiff, Alcian blue | Keratin 5, keratin 10, filaggrin, HLA I-II | X | X | |||
| PCL-NCs/Cur + EnSCs [116] | MTT | Wettability | |||||
| Lesional psoriatic skin [117] | HE | Keratin 16, anti CD3, CD23, CD28 | IL17, IL8 |
| Construct | Macroscopic Evaluation | Cell Viability | Histology | Immunohisto Chemistry | Gene Expression | Electron Microscopy | Epidermal Barrier |
|---|---|---|---|---|---|---|---|
| Polivinyl alcohol [138] | X | HE | |||||
| Collagen-GAG +/− KCs [139] | X | HE | |||||
| Collagen + rat FBs [52] | X | HE | |||||
| Collagen, polyglactin or PEU [78] | X | HE | Laminin | ||||
| Polyglactin + human FBs & KCs [116] | X | HE | Involucrin, laminin | ||||
| Collagen + rat KCs +/− fibrin [41] | X | Collagen IV | X | ||||
| Collagen-GAG-chitosan [59] | X | HE | |||||
| Acellular human DED + human KCs [31] | X | HE, Masson’s trichrome | Keratin 10, keratin 16, involucrin, laminin, collagen IV | ||||
| Collagen-GAG + human FBs & KCs [110] | X | HE | SEC | ||||
| Collagen-elastin hydrosylate [140] | HE | Fibronectin, laminin, chondroitin sulfate, elastin, vWF | X | ||||
| Collagen -GAG + porcine KCs [141] | X | HE | |||||
| Fibrin + human FBs & KCs [44] | HE | Laminin, type IV collagen, (pan)cytokeratin, keratin 10 | |||||
| Collagen-GAG + porcine KCs [142] | X | HE | (Pan)cytokeratin, integrin, involucrin, laminin, collagen VII, factor VIII, Ki67 | ||||
| Collagen-elastin hydrosylate + porcine FBs [143] | HE, Herovici stain | Vimentin, vWF | |||||
| Collagen-GAG + human FBs & KCs [93] | X | HLA-ABC | SEC | ||||
| Collagen +/− TGFB [144] | HE, Modified Masson’s trichrome | ||||||
| Collagen-elastin hidrosylate +/− porcine FBs [145] | X | HE | Elastin, a-SMA | ||||
| Collagen-GAG + human FBs & KCs [97] | X | HE | |||||
| Collagen-GAG + human FBs & KCs +/− Vit C [96] | X | BrdU, MTT | HE | Collagen IV, collagen VII, laminin 5 | X | SEC | |
| Collagen-GAG + fibrin & porcine KCs [146] | X | Keratin 6, keratin 14 | |||||
| Gelatin-B-glucan +/− human FBs & KCs [60] | HE | ||||||
| PGA +/− murine FBs +/− transfected PDGF [147] | HE | Anti-PDGF | PDGF-B | ||||
| Biological and synthetic scaffolds +/− porcine FBs [148] | X | HE, Masson’s trichrome | |||||
| Plasma + human FBs & KCs [149] | X | HE, Masson’s trichrome | (Pan)cytokeratin, keratin 5, keratin 10, involucrin, laminin, loricrin, vimentin | ||||
| GAG −/− porcine FBs +/− porcine KCs [150] | X | HE | Keratin 6, collagen VII | Autosomal DNA, male DNA | |||
| Collagen +/− GAG or PEGT/PBT [151] | X | HE, Sirius red | vWF, vimentin, Ki67 | ||||
| Collagen-GAG or PLGA +/− human FBs & KCs [99] | X | HE | (Pan)cytokeratin, laminin, collagen I, HLA-ABC | X | |||
| Acellular human dermis + human FBs & KCs [61] | X | ||||||
| Collagen + human FBs & KCs & melanocytes [98] | X | HE | HLA-ABC | ||||
| PEGylated-RGD gelatin & KGF-1 [82] | X | HE | |||||
| GAG + porcine KCs [152] | X | HE, Mallory’s trichromate | |||||
| Human DED [153] | X | HE, elastica von Giesson | a-SMA | ||||
| Fibrin +/− eNOS expressing vector [154] | X | HE, Masson’s trichrome, Picrosirius red | Anti CD31, e-NOS | ||||
| Gelatin-acrylamide + human BMSCs [101] | X | HE | (Pan)cytokeratin, e-cadherin anti-CD13, CD105 | ||||
| Agar-collagen [155] | X | HE | |||||
| Collagen-GAG + human KCs & FBs [100] | FdA, MTT | HE | |||||
| PLLA vs PLGA + human KCs & FBs [63] | X | HE | Anti CD31, CD68, CD45 | X | |||
| Collagen + human FBs & KCs [156] | X | HE, orcein, periodic acid-Schiff | (Pan)cytokeratin, vimentin, HLA-DR, HBG | ||||
| Silk fibroin-chitosan + ASCs [68] | X | HE | Keratin 19, a-SMA, vWF, Ki67 | ||||
| Collagen-elastin + pancreatic SCs [70] | X | MTT, DAPI | HE | Keratin 10, keratin 14, fillagrin | PDX-1, GATA-1 genes | ||
| Poly-N-acetyl-glucosamine vs cellulose [157] | X | HE | PECAM-1, anti CD45, CD31, Ki67, p63 | MMP3, uPAR, VEGF | |||
| Collagen-GAG + human FBs & KCs [107] | X | HE | KRT2, KRT15, loricrin, CILP, POSTN, OGN | DEFB4, KRT2, S100A7A, S100A12, SPRR2C, LOR, CD36, TCNI, GDA | |||
| Hyalluronic acid-collagen +/− human FBs [158] | X | MTT | HE | Vimentin | |||
| Collagen-GAG + GFs [159] | HE | Muscle-specific desmin, anti-CD8 alpha, collagen IV | X | ||||
| Collagen + SGC + EGF + human FBs & KCs [160] | X | HE | |||||
| Collagen-GAG + GFs [161] | X | HE, Elastin von Gieson, Verhoeff’s elastic tissue, Masson’s trichrome | a-SMA, elastin, collagen I, III, IV, dermatan sulfate | X | |||
| Fibrin-agarose + human FBs & KCs [65] | HE, Picrosirius red staining, Alcian blue, Gomori, Orcein | Keratin 1, keratin 5, keratin 10, filaggrin, involucrin | X | ||||
| Collagen + BM-MSC +/− EGF [69] | X | HE | Keratin 5, CEA | ||||
| Type I collagen gel + collagen-elastin [162] | X | HE, Masson’s trichrome | a-SMA | ||||
| DED + Collagen-GAG vs Collagen-elastin + KCs [163] | X | HE, elastica van Gieson | Keratin 10, filaggrin, cathepsin V, loricrin | ||||
| Fibrin/collagen + KCs +/− FBs, SVF, ASCs [111] | X | HE | Keratin 16, keratin 17, a-SMA, laminin 5, collagen I, anti CD31, CD34, CD73, CD90, aSMA, DAPI, vWF, Ki67 | X | |||
| Collagen + ADRCs [112] | X | HE, Masson Trichrome | a-SMA, anti CD31, CD45, CD90, CD146 | ||||
| Pegylated fibrin + ASCs [113] | X | HE, DAPI, Alizarin Red S, Oil Red O | a-SMA, lectin, anti CD68, CD206 | ||||
| 3D printing vHSEs [76] | X | HE | Keratin 10, keratin 14, loricrin, anti CD31, Ki67 | ||||
| Collagn-GAG +/− ad-MVF [75] | HE | (Pan)cytokeratin, anti CD31, GFP/CD31 | |||||
| S-dECM bioink +/− EPCs + ASCs [78] | HE | Keratin 10, anti CD31 | |||||
| FN-G + HVEC + FBs + KCs [128] | X | HE, Masson’s trichrome | Anti CD31, HLA-ABC | ||||
| Type I collagen + gelatin-collagen microparticles and Aloe vera [115] | X | MTT | HE | ||||
| Fibrin-agarose + MSCs [67] | HE, Picrosirius red, Periodic acid-Schiff, Alcian blue | Keratin 5, keratin 10, filaggrin, HLA I-II | X | X | |||
| PCL-NCs/Cur + EnSCs [116] | X | HE, Masson’s trichrome | Wettability |
| Technique | Tissue/Cells | Reference | |
|---|---|---|---|
| Epidermal | P63 | Migrating keratinocytes | [162] |
| (Pan)cytokeratin | Keratinocytes | [68,75,77,92,101,107,117,165,166,167] | |
| Keratin 6 | Hyperproliferative keratinocytes | [94,107,146,168] | |
| Keratin 5 | Basal keratinocytes | [112,128,149,169] | |
| Keratin 14 | Basal keratinocytes | [76,89,90,115,117,146,160] | |
| Keratin 15 | Basal keratinocytes | [107] | |
| Keratin 16 | Basal keratinocytes | [111,128,168] | |
| Keratin 19 | Basal keratinocytes | [68,89,90,138,160] | |
| Keratin 1 | Suprabasal keratinocytes | [53,94,95,117,128] | |
| Keratin 10 | Suprabasal keratinocytes | [16,76,78,90,94,107,115,128,149,168,169] | |
| CD185 | Keratinocyte stem cell markers | [94] | |
| Involucrin | Cornified envelope keratinocytes | [36,46,67,78,95,103,117,128,149,168,170] | |
| Loricrin | Cornified envelope keratinocytes | [76,94,95,103,107,114,149,168] | |
| Fillaggrin | Granular keratinocytes | [53,67,90,95,103,114,115,128,168,169] | |
| Transglutaminase | Granular keratinocytes | [53,89] | |
| Integrin | Attaching keratinocytes | [98,105,117,147,171,172] | |
| 6-Integrin | Keratinocyte stem cell markers | [53,94] | |
| Dermal | A-smooth muscle actin | Myofibroblasts & mature blood vessels | [61,68,82,107,111,112,117,147,161,173] |
| Type I collagen | (Newly formed) dermis | [53,89,92,111,161,173,174] | |
| Type III collagen | (Newly formed) dermis | [53,89,161,174] | |
| Type V collagen | (Newly formed) dermis | [53,98,169,174] | |
| Elastin | Elastic fibers | [36,46,107,161] | |
| Fibrillin-1 | Microfibrils (elastic fiber formation) | [53,174] | |
| Fibronectin | Wounded dermis | [53,89,98,107,174] | |
| Vimentin | Fibroblasts | [68,117,143,149,151,173,175,176] | |
| CD68 | Monocytes/macrophagues | [63,107] | |
| CD45RC | Lymphocytes | [63,162] | |
| BM | Type VII collagen | Basement membrane | [53,89,107,117,143] |
| Desmoglein | Basement membrane | [90] | |
| BM and BV | Type IV collagen | Blood vessels & basement membrane | [10,46,89,96,107,161] |
| Laminin | Blood vessels & basement membrane | [10,53,78,89,92,96,98,107,114,128,149,162,170] | |
| BV | CD31 | Blood vessels | [63,75,78,112,114,128,154] |
| Factor VIII | Blood vessels/endothelial cells | [117] | |
| PECAM-1 | Blood vessels | [162] | |
| Von Willebrand factor | Blood vessels | [68,107,143,151,173] | |
| D2-40 protein | Lymphatic vessels | [5] | |
| Other | Desmin | Muscle cells | [76] |
| Ki67 | Proliferating cells | [10,61,68,103,114,117,151,162] | |
| HMB-45 | Anti-melanoma antibody | [107] | |
| S-100 protein | Schwann cells | [135] | |
| Labels | Endothelial nitric oxide synthase | In situ transfected cells | [154] |
| Vascular endothelial growth factor | In situ transfected cells | [76,177] | |
| Human leukocyte antigen (HLA) | Transplanted cell “label” | [92,117,143,169,173] | |
| Immune Response | CD68 | Macrophages | [63,106] |
| CD45 | Lymphocytes | [63] |
| Reference | TESSs | Biomechanical Evaluation In Vitro | Biomechanical Evaluation In Vivo | Parameters |
|---|---|---|---|---|
| Kim et al. [78] | S-dECM bioink | Rheological properties | ||
| Zahiri et al. [116] | PCL vs PCL/Gela vs PCL/Gela/NCs/Cur (+EnSCs) | Uniaxial loaded by tensile test | Tensile strength (MPa) | |
| Freytes et al. [187] | Five different ECM scaffolds before and after treatment with peracetic acid (PAA): SS, SIS, UBS, UBM, UBS + UBM. This study also compared the mechanical properties of two- and four-layer ECM scaffolds | Tensile test Ball-burst test | Ball-burst strength (N) | |
| Badylak et al. [188] | SISHRD | Ball-burst test | Ball-burst test | Survival time/Ball burst load (pounds) |
| Ko et al. [189] | SIS | Tensile strength test | Tensile strength test | Mean Tensile Strength (N/cm) |
| Gloeckner et al. [190] | Graftpatch® (Clarivate, London, UK) vs SIS vs GLBP | Stress-based biaxial test | ||
| Pandit et al. [144] | Collagen va collagen + TGF-B | Instron tester in uniaxial tension | Ultimate tensile strength, Stiffness, Failure strain | |
| Shah et al. [191] | Decellularized human dermis | OCT and vibrational analysis | OCT and vibrational analysis | Resonant Frequency |
| Heraud et al. [192] | SFSE | Suction experimental device Cutometer 580® (Microcaya, Bilbao, Spain) | Ue, the immediate elastic elongation; Uf, the total elongation; Uv, the viscous (creep) elongation; Ur, the immediate recovery; Ur/Ue, the elastic ratio; Ur/Uf, the relative elastic recovery; and Uv/Ue, the viscous ratio | |
| Lafrance et al. [193] | hKCs seeded on our anchorage based a human type supplemented with elastin DE, I+III CG + GAGS | Indentation method | Deflection (A in mm) | |
| Lafrance et al. [194] | FBs + type I bovine collagen | Tensile tests: indentation test | Tensile Strength | |
| Zahouani et al. [195] | FBs + Human skin vs Dermal substitute (bovine collagens 95% type I, 5% type III + chitosan + chrondroitin-4, sulfate | New bio-tribometer working at a low contact pressure | Young modulus | |
| Ahlfors et al. [196] | Collagen gel vs Fibrin gel vs CDM + vs native skin | Custom tissue inflation device | Failure tension, failure strain, and ultimate tensile strength (kPa) | |
| Berthod et al. [197] | Collagen + chondroitins 4-, 6-sulphate + chitosan | Tensile strength test | Tensile Strength, ultimate elongation and Young’s modulus |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Linares-Gonzalez, L.; Rodenas-Herranz, T.; Campos, F.; Ruiz-Villaverde, R.; Carriel, V. Basic Quality Controls Used in Skin Tissue Engineering. Life 2021, 11, 1033. https://doi.org/10.3390/life11101033
Linares-Gonzalez L, Rodenas-Herranz T, Campos F, Ruiz-Villaverde R, Carriel V. Basic Quality Controls Used in Skin Tissue Engineering. Life. 2021; 11(10):1033. https://doi.org/10.3390/life11101033
Chicago/Turabian StyleLinares-Gonzalez, Laura, Teresa Rodenas-Herranz, Fernando Campos, Ricardo Ruiz-Villaverde, and Víctor Carriel. 2021. "Basic Quality Controls Used in Skin Tissue Engineering" Life 11, no. 10: 1033. https://doi.org/10.3390/life11101033
APA StyleLinares-Gonzalez, L., Rodenas-Herranz, T., Campos, F., Ruiz-Villaverde, R., & Carriel, V. (2021). Basic Quality Controls Used in Skin Tissue Engineering. Life, 11(10), 1033. https://doi.org/10.3390/life11101033








