Effects of Temperature and Water Types on the Decay of Coronavirus: A Review
Abstract
:1. Introduction
2. Methods
2.1. Literature Search and Data Selection
2.2. Data Analysis
3. Results and Discussion
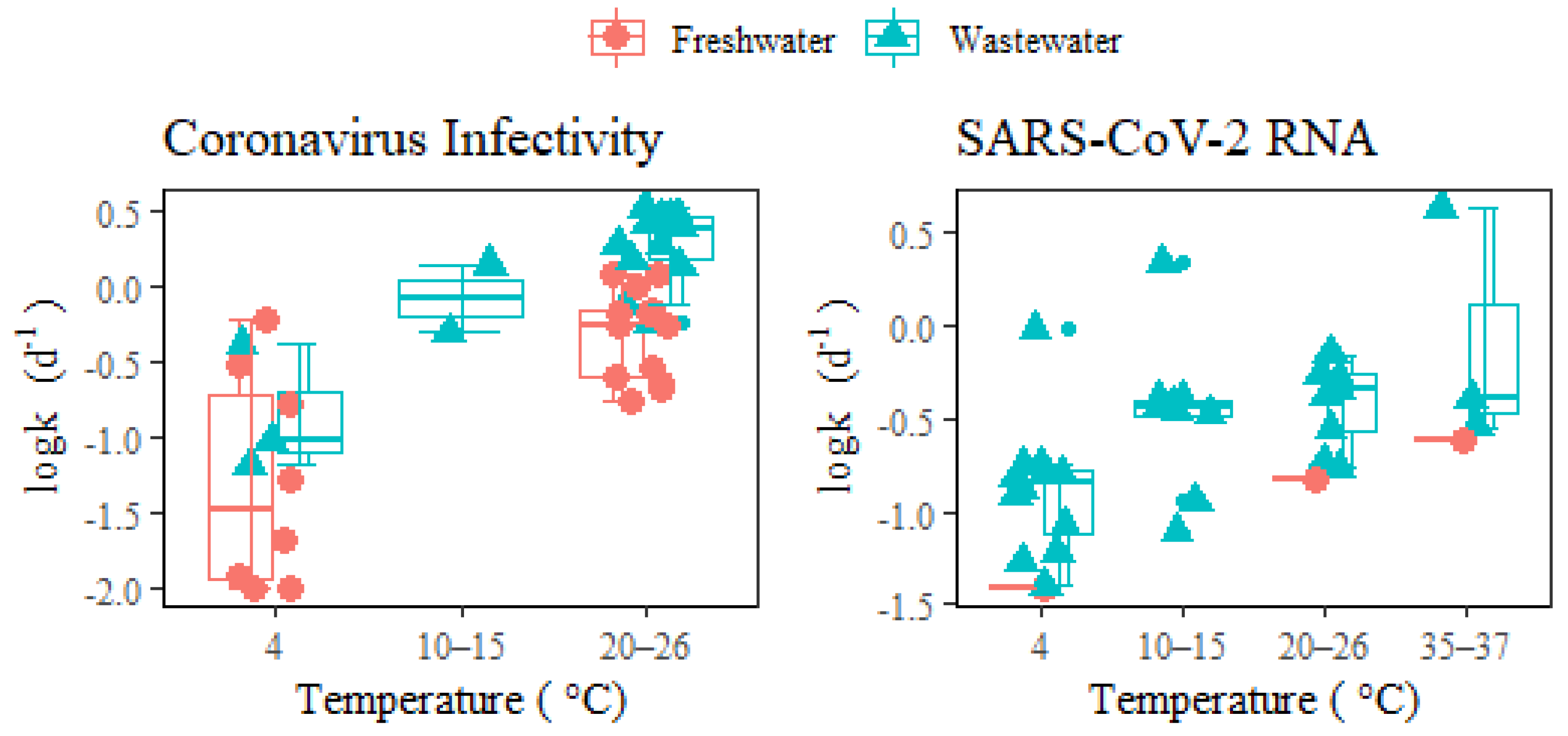
3.1. Overview of Coronavirus Decay Rates in Waters
3.2. Effect of Wastewater Dilution on Coronavirus Decay
3.3. Effect of Temperature on Coronavirus Decay
3.4. Sensitivity of WBE Back-Calculation to the Decay of SARS-CoV-2
3.5. Comparison of Coronavirus Decay Rates in Wastewater to Norovirus and Other Viruses
3.6. Implications, Limitations, and Future Perspectives
4. Conclusions
- SARS-CoV-2 RNA, as the biomarker for WBE investigations, has much lower decay rates and was less influenced by wastewater temperature variations than viable coronaviruses. However, higher wastewater temperature in summer or tropical regions could still increase the sensitivity of WBE back-calculations considerably from 0.06 to 0.18, resulting in a two-times higher relative variance in back-estimation of COVID-19 cases;
- Wastewater dilution by stormwater inflow might alleviate the decay of coronavirus infectivity. Cold weather along with heavy rainfall events and urban floods could further increase the risk of environmental transmission by improving virus survivability in wastewater;
- As an enveloped RNA virus, coronavirus experienced more rapid decay in wastewater than nonenveloped viruses such as norovirus, which led to the increased sensitivity of WBE back-estimation to in-sewer decay and, consequently, to a greater need to incorporate the decay rate as a correction factor;
- There is a lack of studies on coronavirus decay in saltwater, unlike some other, more extensively studied, waterborne enteric pathogens. Salt groundwater intrusion or the municipal usage of seawater (i.e., toilet flushing) in sewers might enhance the decay of coronavirus infectivity during wastewater transportation to wastewater treatment plants (WWTPs). However, this hypothesis needs further supporting experimental data.
Supplementary Materials
Author Contributions
Funding
Data Availability Statement
Conflicts of Interest
References
- Paital, B.; Das, K.; Malekdar, F.; Sandoval, M.A.; Niaragh, E.K.; Frontistis, Z.; Behera, T.R.; Balacco, G.; Sangkham, S.; Hati, A.K.; et al. A State-of-the-Art Review on SARS-CoV-2 Virus Removal Using Different Wastewater Treatment Strategies. Environments 2022, 9, 110. [Google Scholar] [CrossRef]
- Li, X.; Zhang, S.; Shi, J.; Luby, S.P.; Jiang, G. Uncertainties in estimating SARS-CoV-2 prevalence by wastewater-based epidemiology. Chem. Eng. J. 2021, 415, 129039. [Google Scholar] [CrossRef]
- Li, X.; Kulandaivelu, J.; Zhang, S.; Shi, J.; Sivakumar, M.; Mueller, J.; Luby, S.; Ahmed, W.; Coin, L.; Jiang, G. Data-driven estimation of COVID-19 community prevalence through wastewater-based epidemiology. Sci. Total Environ. 2021, 789, 147947. [Google Scholar] [CrossRef]
- Mousazadeh, M.; Ashoori, R.; Paital, B.; Kabdaşlı, I.; Frontistis, Z.; Hashemi, M.; Sandoval, M.A.; Sherchan, S.; Das, K.; Emamjomeh, M.M. Wastewater Based Epidemiology Perspective as a Faster Protocol for Detecting Coronavirus RNA in Human Populations: A Review with Specific Reference to SARS-CoV-2 Virus. Pathogens 2021, 10, 1008. [Google Scholar] [CrossRef]
- Ahmed, W.; Angel, N.; Edson, J.; Bibby, K.; Bivins, A.; O’Brien, J.W.; Choi, P.M.; Kitajima, M.; Simpson, S.L.; Li, J.; et al. First confirmed detection of SARS-CoV-2 in untreated wastewater in Australia: A proof of concept for the wastewater surveillance of COVID-19 in the community. Sci. Total Environ. 2020, 728, 138764. [Google Scholar] [CrossRef]
- Li, X.; Zhang, S.; Sherchan, S.; Orive, G.; Lertxundi, U.; Haramoto, E.; Honda, R.; Kumar, M.; Arora, S.; Kitajima, M.; et al. Correlation between SARS-CoV-2 RNA concentration in wastewater and COVID-19 cases in community: A systematic review and meta-analysis. J. Hazard. Mater. 2023, 441, 129848. [Google Scholar] [CrossRef]
- Pinon, A.; Vialette, M. Survival of viruses in water. Intervirology 2018, 61, 214–222. [Google Scholar] [CrossRef]
- Boehm, A.B.; Silverman, A.I.; Schriewer, A.; Goodwin, K. Systematic review and meta-analysis of decay rates of waterborne mammalian viruses and coliphages in surface waters. Water Res. 2019, 164, 114898. [Google Scholar] [CrossRef]
- Silverman, A.I.; Boehm, A.B. Systematic review and meta-analysis of the persistence and disinfection of human coronaviruses and their viral surrogates in water and wastewater. Environ. Sci. Technol. Lett. 2020, 7, 544–553. [Google Scholar] [CrossRef]
- Guo, Y.; Sivakumar, M.; Jiang, G. Decay of four enteric pathogens and implications to wastewater-based epidemiology: Effects of temperature and wastewater dilutions. Sci. Total Environ. 2022, 819, 152000. [Google Scholar] [CrossRef]
- Chick, H. An investigation of the laws of disinfection. J. Hyg. 1908, 8, 92–158. [Google Scholar] [CrossRef] [Green Version]
- Sala-Comorera, L.; Reynolds, L.J.; Martin, N.A.; O’Sullivan, J.J.; Meijer, W.G.; Fletcher, N.F. Decay of infectious SARS-CoV-2 and surrogates in aquatic environments. Water Res. 2021, 201, 117090. [Google Scholar] [CrossRef]
- De Rijcke, M.; Shaikh, H.M.; Mees, J.; Nauwynck, H.; Vandegehuchte, M.B. Environmental stability of porcine respiratory coronavirus in aquatic environments. PLoS ONE 2021, 16, e0254540. [Google Scholar] [CrossRef]
- Bivins, A.; Greaves, J.; Fischer, R.; Yinda, K.C.; Ahmed, W.; Kitajima, M.; Munster, V.J.; Bibby, K. Persistence of SARS-CoV-2 in water and wastewater. Environ. Sci. Technol. Lett. 2020, 7, 937–942. [Google Scholar] [CrossRef]
- Gundy, P.M.; Gerba, C.P.; Pepper, I.L. Survival of coronaviruses in water and wastewater. Food Environ. Virol. 2008, 1, 10–14. [Google Scholar] [CrossRef] [Green Version]
- Casanova, L.; Rutala, W.A.; Weber, D.J.; Sobsey, M.D. Survival of surrogate coronaviruses in water. Water Res. 2009, 43, 1893–1898. [Google Scholar] [CrossRef]
- de Oliveira, L.C.; Torres-Franco, A.F.; Lopes, B.C.; Santos, B.; Costa, E.A.; Costa, M.S.; Reis, M.T.P.; Melo, M.C.; Polizzi, R.B.; Teixeira, M.M.; et al. Viability of SARS-CoV-2 in river water and wastewater at different temperatures and solids content. Water Res. 2021, 195, 117002. [Google Scholar] [CrossRef]
- Ye, Y.; Ellenberg, R.M.; Graham, K.E.; Wigginton, K.R. Survivability, partitioning, and recovery of enveloped viruses in untreated municipal wastewater. Environ. Sci. Technol. 2016, 50, 5077–5085. [Google Scholar] [CrossRef]
- Weidhaas, J.; Aanderud, Z.T.; Roper, D.K.; VanDerslice, J.; Gaddis, E.B.; Ostermiller, J.; Hoffman, K.; Jamal, R.; Heck, P.; Zhang, Y.; et al. Correlation of SARS-CoV-2 RNA in wastewater with COVID-19 disease burden in sewersheds. Sci. Total Environ. 2021, 775, 145790. [Google Scholar] [CrossRef]
- Ahmed, W.; Bertsch, P.M.; Bibby, K.; Haramoto, E.; Hewitt, J.; Huygens, F.; Gyawali, P.; Korajkic, A.; Riddell, S.; Sherchan, S.P.; et al. Decay of SARS-CoV-2 and surrogate murine hepatitis virus RNA in untreated wastewater to inform application in wastewater-based epidemiology. Environ. Res. 2020, 191, 110092. [Google Scholar] [CrossRef]
- Hokajärvi, A.-M.; Rytkönen, A.; Tiwari, A.; Kauppinen, A.; Oikarinen, S.; Lehto, K.-M.; Kankaanpää, A.; Gunnar, T.; Al-Hello, H.; Blomqvist, S.; et al. The detection and stability of the SARS-CoV-2 RNA biomarkers in wastewater influent in Helsinki, Finland. Sci. Total Environ. 2021, 770, 145274. [Google Scholar] [CrossRef]
- Burnet, J.B.; Cauchie, H.M.; Walczak, C.; Goeders, N.; Ogorzaly, L. Persistence of endogenous RNA biomarkers of SARS-CoV-2 and PMMoV in raw wastewater: Impact of temperature and implications for wastewater-based epidemiology. Sci. Total Environ. 2023, 857, 159401. [Google Scholar] [CrossRef]
- Yang, S.; Dong, Q.; Li, S.; Cheng, Z.; Kang, X.; Ren, D.; Xu, C.; Zhou, X.; Liang, P.; Sun, L.; et al. Persistence of SARS-CoV-2 RNA in wastewater after the end of the COVID-19 epidemics. J. Hazard. Mater. 2022, 429, 128358. [Google Scholar] [CrossRef]
- Sun, Z.P.; Yang, S.Y.; Cai, X.; Han, W.D.; Hu, G.W.; Qian, Y.; Wang, Y.Y.; Zhang, R.; Xie, Y.H.; Qu, D. Survival of SARS-CoV-2 in artificial seawater and on the surface of inanimate materials. J. Med. Virol. 2022, 94, 3982–3987. [Google Scholar] [CrossRef]
- Lee, Y.J.; Kim, J.H.; Choi, B.-S.; Choi, J.-H.; Jeong, Y.-I. Characterization of Severe Acute Respiratory Syndrome Coronavirus 2 stability in multiple water matrices. J. Korean Med. Sci. 2020, 35, e330. [Google Scholar] [CrossRef]
- Mahlknecht, J. Presence and persistence of SARS-CoV-2 in aquatic environments: A mini-review. Curr. Opin. Environ. Sci. Health 2022, 29, 100385. [Google Scholar] [CrossRef]
- Mordecai, G.J.; Hewson, I. Coronaviruses in the sea. Front. Microbiol. 2020, 11, 1795. [Google Scholar] [CrossRef]
- Seyer, A.; Şanlıdağ, T. The fate of SARS-CoV-2 in the marine environments: Are marine environments safe from COVID-19? Erciyes Med. J. 2021, 43, 606–607. [Google Scholar] [CrossRef]
- Farkas, K.; Cooper, D.M.; McDonald, J.E.; Malham, S.K.; de Rougemont, A.; Jones, D.L. Seasonal and spatial dynamics of enteric viruses in wastewater and in riverine and estuarine receiving waters. Sci. Total Environ. 2018, 634, 1174–1183. [Google Scholar] [CrossRef]
- Wang, J.; Li, F.; Liu, Z.; Li, N. COVID-19 outbreaks linked to imported frozen food in China: Status and challege. China CDC Wkly. 2022, 4, 483–487. [Google Scholar] [CrossRef]
- Qian, J.; Yu, Q.; Jiang, L.; Yang, H.; Wu, W. Food cold chain management improvement: A conjoint analysis on COVID-19 and food cold chain systems. Food Control 2022, 137, 108940. [Google Scholar] [CrossRef]
- Liang, L.; Goh, S.G.; Gin, K.Y.H. Decay kinetics of microbial source tracking (MST) markers and human adenovirus under the effects of sunlight and salinity. Sci. Total Environ. 2017, 574, 165–175. [Google Scholar] [CrossRef]
- Huang, C.; Hu, Y.; Wang, L.; Wang, Y.; Li, N.; Guo, Y.; Feng, Y.; Xiao, L.; Stams, A.J.M. Environmental transport of emerging human-pathogenic Cryptosporidium species and subtypes through combined sewer overflow and wastewater. Appl. Environ. Microbiol. 2017, 83, e00682-17. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Steele, J.A.; Blackwood, A.D.; Griffith, J.F.; Noble, R.T.; Schiff, K.C. Quantification of pathogens and markers of fecal contamination during storm events along popular surfing beaches in San Diego, California. Water Res. 2018, 136, 137–149. [Google Scholar] [CrossRef]
- Astrom, J.; Pettersson, T.J.; Reischer, G.H.; Hermansson, M. Short-term microbial release during rain events from on-site sewers and cattle in a surface water source. J. Water Health 2013, 11, 430–442. [Google Scholar] [CrossRef]
- Carratala, A.; Rusinol, M.; Rodriguez-Manzano, J.; Guerrero-Latorre, L.; Sommer, R.; Girones, R. Environmental effectors on the inactivation of human adenoviruses in water. Food. Environ. Virol. 2013, 5, 203–214. [Google Scholar] [CrossRef]
- Aquino de Carvalho, N.; Stachler, E.N.; Cimabue, N.; Bibby, K. Evaluation of phi6 persistence and suitability as an enveloped virus surrogate. Environ. Sci. Technol. 2017, 51, 8692–8700. [Google Scholar] [CrossRef]
- Ye, Y.; Chang, P.H.; Hartert, J.; Wigginton, K.R. Reactivity of enveloped virus genome, proteins, and lipids with free chlorine and UV254. Environ. Sci. Technol. 2018, 52, 7698–7708. [Google Scholar] [CrossRef]
- Guo, Y.; Li, J.; O’Brien, J.; Sivakumar, M.; Jiang, G. Back-estimation of norovirus infections through wastewater-based epidemiology: A systematic review and parameter sensitivity. Water Res. 2022, 219, 118610. [Google Scholar] [CrossRef]
- Kauppinen, A.; Miettinen, I.T. Persistence of Norovirus GII genome in drinking water and wastewater at different temperatures. Pathogens 2017, 6, 48. [Google Scholar] [CrossRef]
- Skraber, S.; Ogorzaly, L.; Helmi, K.; Maul, A.; Hoffmann, L.; Cauchie, H.M.; Gantzer, C. Occurrence and persistence of enteroviruses, noroviruses and F-specific RNA phages in natural wastewater biofilms. Water Res. 2009, 43, 4780–4789. [Google Scholar] [CrossRef]
- Muirhead, A.; Zhu, K.; Brown, J.; Basu, M.; Brinton, M.A.; Costa, F.; Hayat, M.J.; Stauber, C.E. Zika virus RNA persistence in sewage. Environ. Sci. Technol. Lett. 2020, 7, 659–664. [Google Scholar] [CrossRef]
- Chandra, F.; Lee, W.L.; Armas, F.; Leifels, M.; Gu, X.; Chen, H.; Wuertz, S.; Alm, E.J.; Thompson, J. Persistence of Dengue (Serotypes 2 and 3), Zika, yellow fever, and murine hepatitis virus RNA in untreated wastewater. Environ. Sci. Technol. Lett. 2021, 8, 785–791. [Google Scholar] [CrossRef]
- Bibby, K.; Fischer, R.J.; Casson, L.W.; Stachler, E.; Haas, C.N.; Munster, V.J. Persistence of Ebola virus in sterilized wastewater. Environ. Sci. Technol. Lett. 2015, 2, 245–249. [Google Scholar] [CrossRef]
- Slade, J.S.; Pike, E.B.; Eglin, R.P.; Colbourne, J.S.; Kurtz, J.B. The survival of human immunodeficiency virus in water, sewage and sea-water. Water Sci. Technol. 1989, 21, 55–59. [Google Scholar] [CrossRef]
- Deng, M.Y.; Cliver, D.O. Persistence of inoculated hepatitis-a virus in mixed human and animal wastes. Appl. Environ. Microbiol. 1995, 61, 87–91. [Google Scholar] [CrossRef] [Green Version]
- Enriquez, C.E.; Gerba, C.P.; Hurst, C.J. Survival of the enteric adenoviruses 40 and 41 in tap, sea, and wastewater. Water Res. 1995, 29, 2548–2553. [Google Scholar] [CrossRef]
- Farkas, K.; Walker, D.I.; Adriaenssens, E.M.; McDonald, J.E.; Hillary, L.S.; Malham, S.K.; Jones, D.L. Viral indicators for tracking domestic wastewater contamination in the aquatic environment. Water Res. 2020, 181, 115926. [Google Scholar] [CrossRef]
- Shi, J.; Li, X.; Zhang, S.; Sharma, E.; Sivakumar, M.; Sherchan, S.P.; Jiang, G. Enhanced decay of coronaviruses in sewers with domestic wastewater. Sci. Total Environ. 2021, 813, 151919. [Google Scholar] [CrossRef]
- Zhang, S.; Sharma, E.; Tiwaric, A.; Sherchand, S.; Gao, S.; Zhou, X.; Shi, J.; Jiang, G. The Reduction of SARS-CoV-2 RNA concentration in the presence of sewer biofilms. Int. J. Hyg. Environ. Health, 2023; submitted. [Google Scholar]
- Morales Medina, W.R.; D’Elia, S.; Fahrenfeld, N.L. Accumulation of SARS-CoV-2 RNA in sewer biofilms. ACS EST Water 2022, 2, 1844–1851. [Google Scholar] [CrossRef]
- Skraber, S.; Helmi, K.; Willame, R.; Ferreol, M.; Gantzer, C.; Hoffmann, L.; Cauchie, H.M. Occurrence and persistence of bacterial and viral faecal indicators in wastewater biofilms. Water Sci. Technol. 2007, 55, 377–385. [Google Scholar] [CrossRef]
- Brooks, Y.; Aslan, A.; Tamrakar, S.; Murali, B.; Mitchell, J.; Rose, J.B. Analysis of the persistence of enteric markers in sewage polluted water on a solid matrix and in liquid suspension. Water Res. 2015, 76, 201–212. [Google Scholar] [CrossRef]
- Ho, J.; Stange, C.; Suhrborg, R.; Wurzbacher, C.; Drewes, J.E.; Tiehm, A. SARS-CoV-2 wastewater surveillance in Germany: Long-term RT-digital droplet PCR monitoring, suitability of primer/probe combinations and biomarker stability. Water Res. 2022, 210, 117977. [Google Scholar] [CrossRef] [PubMed]
- Amoah, I.D.; Kumari, S.; Bux, F. Coronaviruses in wastewater processes: Source, fate and potential risks. Environ. Int. 2020, 143, 105962. [Google Scholar] [CrossRef] [PubMed]
- Gholipour, S.; Mohammadi, F.; Nikaeen, M.; Shamsizadeh, Z.; Khazeni, A.; Sahbaei, Z.; Mousavi, S.M.; Ghobadian, M.; Mirhendi, H. COVID-19 infection risk from exposure to aerosols of wastewater treatment plants. Chemosphere 2021, 273, 129701. [Google Scholar] [CrossRef]


| Methods | Culture | RT-qPCR | Total |
|---|---|---|---|
| Number of decay tests in wastewater | 18 | 33 | 51 |
| Number of decay tests in freshwater | 21 | 3 | 24 |
| Number of decay tests in saline water | 3 | 1 | 4 |
| Total | 42 | 37 | 79 |
| References | [12,13,14,15,16,17,18] | [14,19,20,21,22,23] |
| Target | Water Types | 4 °C | 10–15 °C | 20–26 °C | 37 °C |
|---|---|---|---|---|---|
| Coronavirus Infectivity | Wastewater | 0.066–0.42 | 0.5–1.4 | 0.6–3.4 | NA |
| Freshwater | 0.01–0.61 | NA | 0.2–1.2 | NA | |
| Seawater | 1.1 | NA | 2.0–2.1 | NA | |
| SARS-CoV-2 RNA | Wastewater | 0.04–0.18 | 0.08–0.4 | 0.17–0.70 | 0.29–0.41 |
| Freshwater | 0.039 | NA | 0.15 | 0.25 | |
| Seawater | NA | NA | 0.14 | NA |
| Df | Sum Sq | Mean Sq | F Value | p (>F) | ||
|---|---|---|---|---|---|---|
| Water type | 2 | 7.248 | 3.624 | 9.332 | 0.000262 | *** |
| Method | 1 | 15.904 | 15.904 | 40.954 | 1.68 × 10−8 | *** |
| Temperature | 1 | 12.485 | 12.485 | 32.151 | 3.17 × 10−7 | *** |
| Water type: method | 1 | 0.495 | 0.495 | 1.275 | 0.262756 | |
| Water type: temperature | 2 | 1.162 | 0.581 | 1.496 | 0.231343 | |
| Method: temperature | 1 | 4.781 | 4.781 | 12.311 | 0.000804 | *** |
| Water type: method: temperature | 1 | 1.098 | 1.098 | 2.826 | 0.097312 | |
| Residuals | 68 | 26.407 | 0.388 |
| Parameters | Water Type | Coronavirus Infectivity | SARS-CoV-2 RNA |
|---|---|---|---|
| k20 | Wastewater | 1.37 ± 0.10 | 0.30 ± 0.04 |
| Freshwater | 0.47 ± 0.07 | 0.11 ± 0.01 | |
| λ | Wastewater | 1.14 ± 0.05 | 1.02 ± 0.01 |
| R2 | Freshwater | 1.10 ± 0.05 | 1.05 ± 0.01 |
| Wastewater | 0.72 | 0.20 | |
| Freshwater | 0.42 | 0.99 |
| Temperature | Wastewater | Freshwater | Sea Water | Average |
|---|---|---|---|---|
| 4 °C | 0.06 | 0.02 | NA | 0.06 |
| 12–15 °C | 0.15 | NA | NA | 0.15 |
| 20–26 °C | 0.23 | 0.08 | 0.07 | 0.21 |
| 37 °C | 0.18 | 0.12 | NA | 0.16 |
| Average | 0.14 | 0.07 | 0.07 | 0.13 |
| Virus | Method | 4–6 °C | 10–25 °C | 30–37 °C | References |
|---|---|---|---|---|---|
| Norovirus | RT-qPCR | 0.02–0.06 | 0.02–0.10 | 0.05–0.21 | [40,41] |
| Zika | RT-qPCR | 0.025–0.046 | 0.11–0.58 | 0.27–0.89 | [42] |
| Dengue | RT-qPCR | 0.008–0.052 | 0.50–0.55 | 0.55–0.61 | [43] |
| Yellow fever | RT-qPCR | 0.032–0.047 | 0.52 | 0.88 | |
| Murine hepatitis virus | RT-qPCR | 0–0.003 | 0.37 | 0.45 | |
| Coronavirus | RT-qPCR | 0.04–0.18 | 0.08–0.70 | 0.29–0.41 | [12,13,14,15,16,17,18,19,20,21,22,23] |
| culture | 0.066–0.42 | 0.5–3.4 | |||
| Ebolavirus | culture | 0.35–1.08 | [44] | ||
| Human Immunodeficiency Virus | culture | 0.80 | [45] | ||
| Hepatitis A | culture | 0.047–0.066 | 0.10–0.28 | 0.34 | [46] |
| Adenovirus | culture | 0.10 | 0.10 | [47] |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Guo, Y.; Liu, Y.; Gao, S.; Zhou, X.; Sivakumar, M.; Jiang, G. Effects of Temperature and Water Types on the Decay of Coronavirus: A Review. Water 2023, 15, 1051. https://doi.org/10.3390/w15061051
Guo Y, Liu Y, Gao S, Zhou X, Sivakumar M, Jiang G. Effects of Temperature and Water Types on the Decay of Coronavirus: A Review. Water. 2023; 15(6):1051. https://doi.org/10.3390/w15061051
Chicago/Turabian StyleGuo, Ying, Yanchen Liu, Shuhong Gao, Xu Zhou, Muttucumaru Sivakumar, and Guangming Jiang. 2023. "Effects of Temperature and Water Types on the Decay of Coronavirus: A Review" Water 15, no. 6: 1051. https://doi.org/10.3390/w15061051





