High-Throughput Incubation and Quantification of Agglutination Assays in a Microfluidic System
Abstract
1. Introduction
2. Materials and Methods
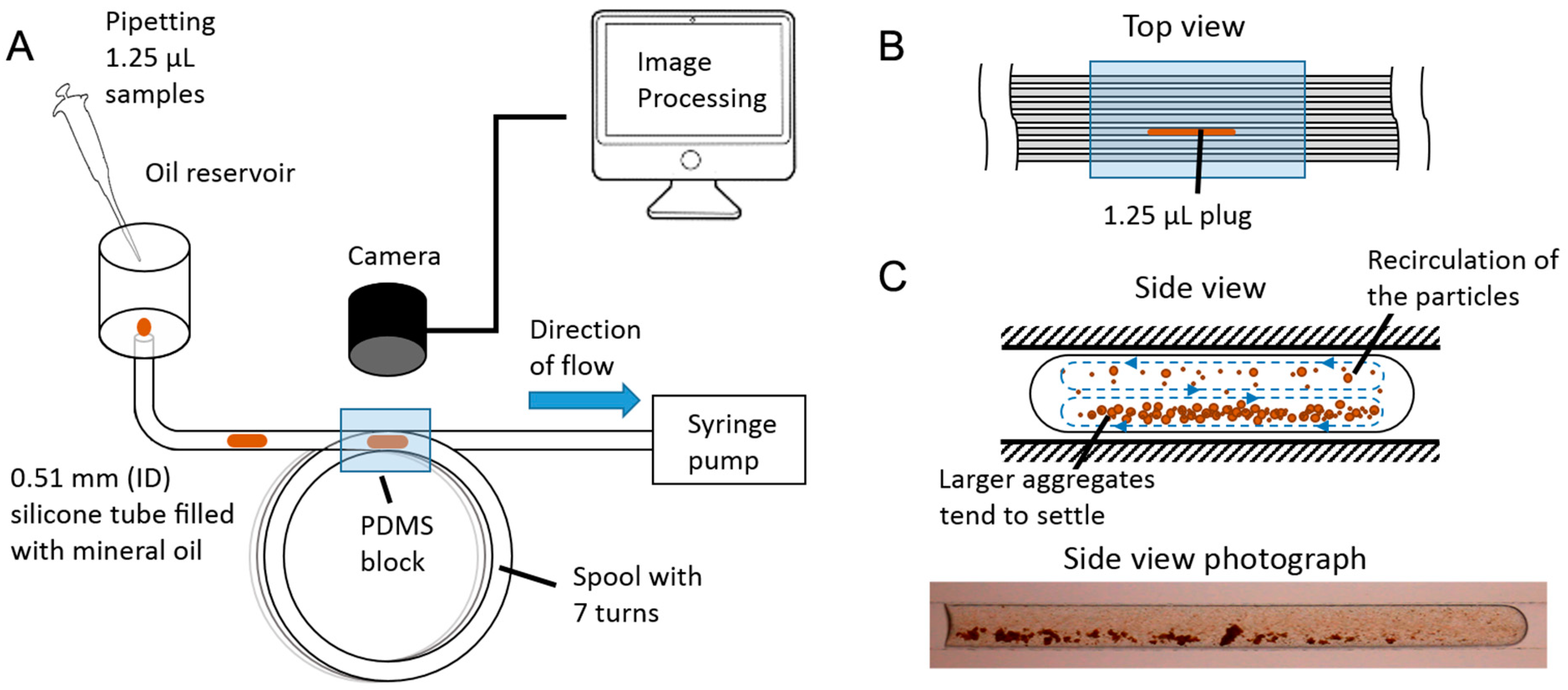
2.1. System Description
2.2 Assay Protocol
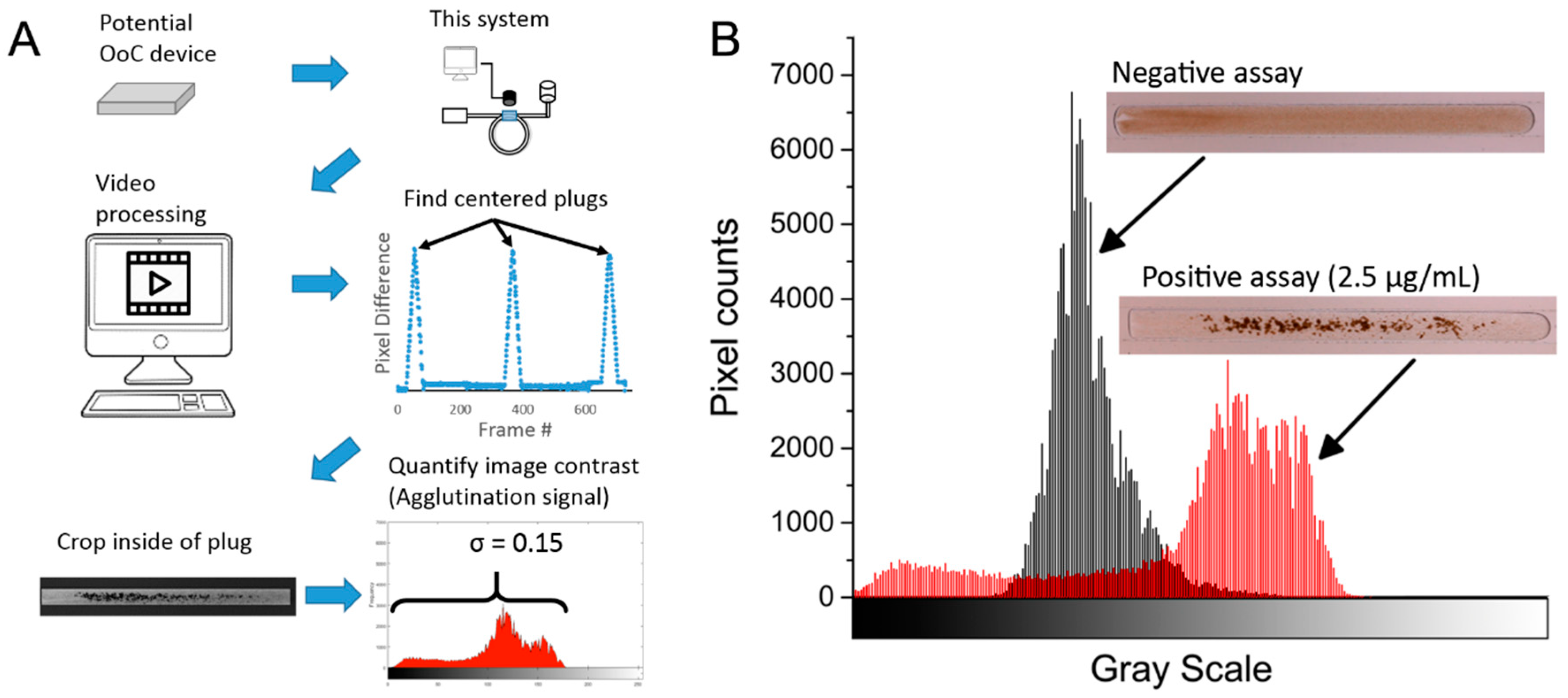
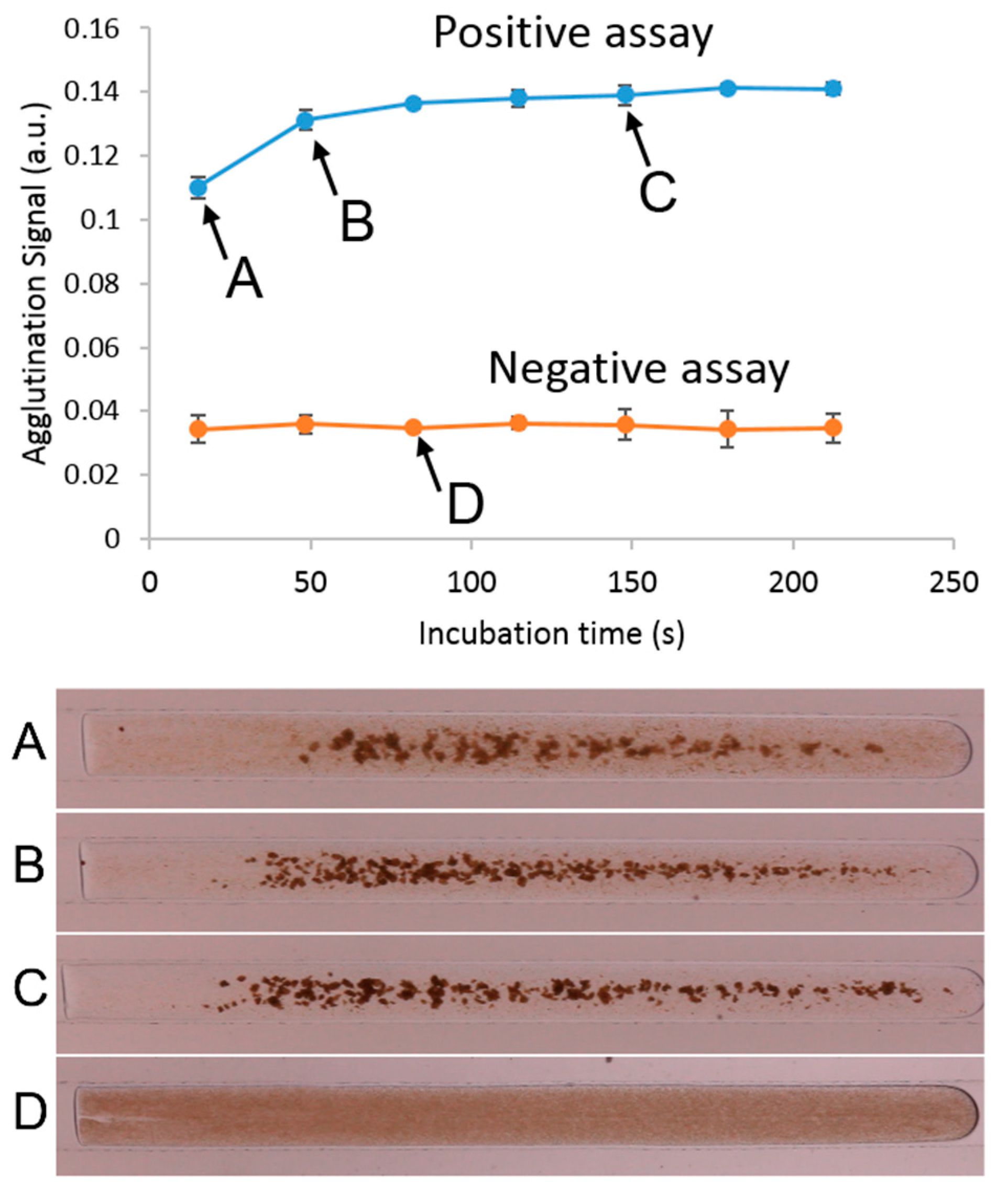
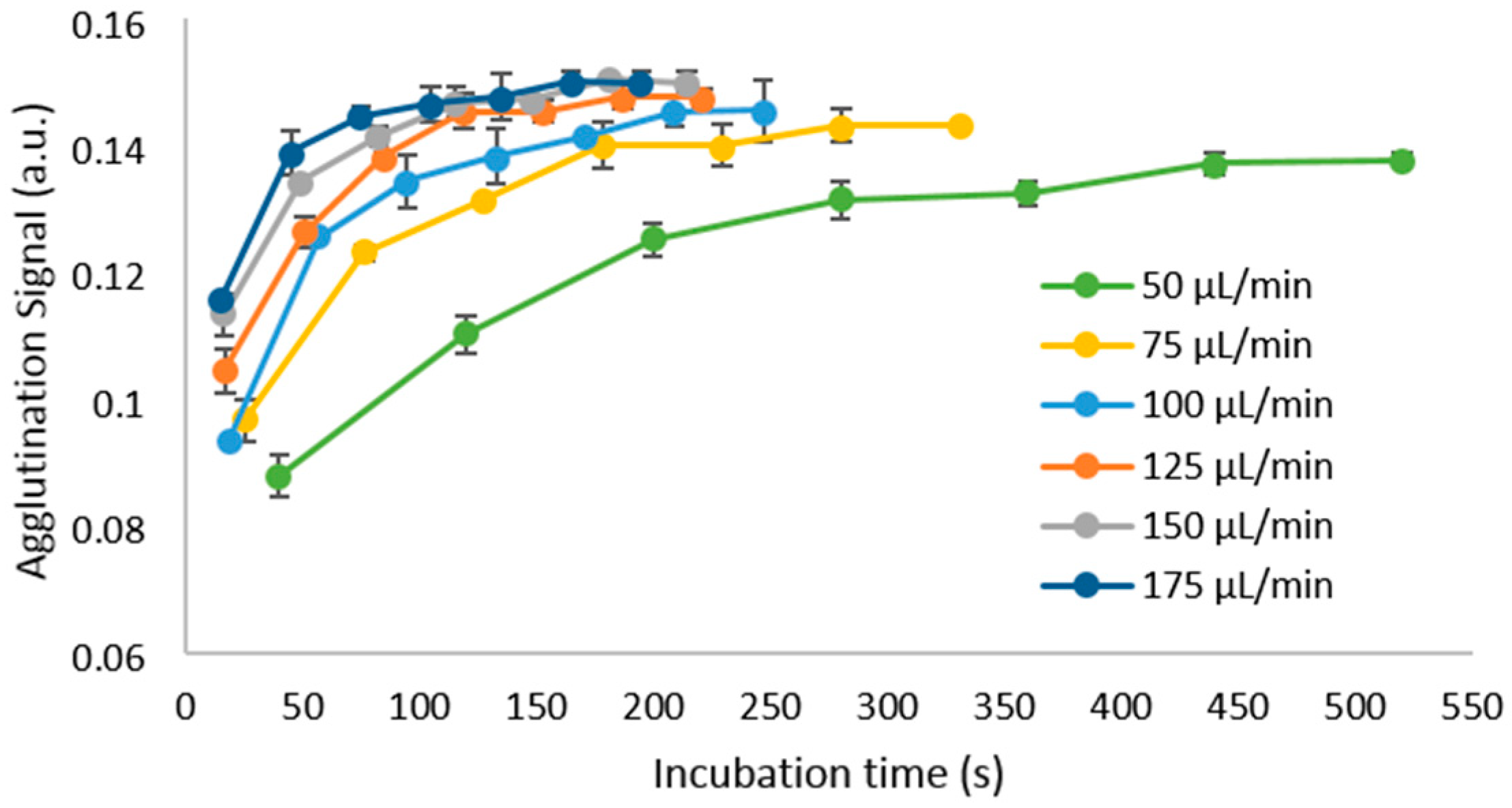
3. Results and Discussion
4. Conclusions
Author Contributions
Acknowledgments
Conflicts of Interest
References
- Sheldon, C.; Landry, M.L. Rapid antigen tests. In Advanced Techniques in Diagnostic Microbiology; Springer: New York, NY, USA, 2013; pp. 31–51. [Google Scholar]
- Jürgen, M.; Roppert, K.; Ertl, P. Microfluidic systems for pathogen sensing: A review. Sensors 2009, 9, 4804–4823. [Google Scholar]
- Andreotti, P.E.; Ludwig, G.V.; Peruski, A.H.; Tuite, J.J.; Morse, S.S.; Peruski, L.F. Immunoassay of infectious agents. BioTechniques 2003, 35, 850–861. [Google Scholar] [PubMed]
- Jongin, H.; Edel, J.B. Micro- and nanofluidic systems for high-throughput biological screening. Drug Discov. Today 2009, 14, 134–146. [Google Scholar]
- Guo, M.T.; Rotem, A.; Heyman, J.A.; Weitz, D.A. Droplet microfluidics for high-throughput biological assays. Lab Chip 2012, 12, 2146–2155. [Google Scholar] [CrossRef] [PubMed]
- Lim, C.T.; Zhang, Y. Bead-based microfluidic immunoassays: The next generation. Biosens. Bioelectron. 2007, 22, 1197–1204. [Google Scholar] [CrossRef] [PubMed]
- Molina-Bolivar, J.A.; Galisteo-Gonzalez, F. Latex immunoagglutination assays. J. Macromol. Sci. Part C Polym. Rev. 2005, 45, 59–98. [Google Scholar] [CrossRef]
- Bangs, L.B. Latex agglutination Tests. Am. Clin. Lab. News 1988, 7, 20–26. [Google Scholar]
- Singer, J.M.; Plotz, C.M. The Latex Fixation Test: I. Application to the serologic diagnosis of rheumatoid arthritis. Am. J. Med. 1956, 21, 888–892. [Google Scholar] [CrossRef]
- Igarashi, H.; Shingaki, M.; Fujikawa, H.; Ushioda, H.; Terayama, T. Detection of staphylococcal enterotoxins in food poisoning outbreaks by reversed passive latex agglutination. Zentralblatt Bakteriol. Mikrobiol. Hyg. I Abt. Suppl. 1985, 14, 255–257. [Google Scholar]
- Jurado, R.L.; Campbell, J.; Martin, P.D. Prozone phenomenon in secondary syphilis: Has its time arrived? Arch. Intern. Med. 1993, 153, 2496–2498. [Google Scholar] [CrossRef] [PubMed]
- Bhaskar, S.; Jain, N.K.; Mukherjee, R. Slide agglutination test for the diagnosis of pulmonary and extra-pulmonary tuberculosis. Tuber. Lung Dis. 1996, 77, 160–163. [Google Scholar] [CrossRef]
- Bhaskar, S.; Banavaliker, J.N.; Bhardwaj, K.; Upadhyay, P. A novel ultrasound-enhanced latex agglutination test for the detection of antibodies against Mycobacterium tuberculosis in serum. J. Immunol. Methods 2002, 262, 181–186. [Google Scholar] [CrossRef]
- Svahn, A.; Magnusson, M.; Jägdahl, L.E.N.A.; Schloss, L.; Kahlmeter, G.; Linde, A. Evaluation of three commercial enzyme-linked immunosorbent assays and two latex agglutination assays for diagnosis of primary Epstein-Barr Virus infection. J. Clin. Microbiol. 1997, 35, 2728–2732. [Google Scholar] [PubMed]
- Sanekata, T.; Yoshida, Y.; Okada, H. Detection of rotavirus in faeces by latex agglutination. J. Immunol. Methods 1981, 41, 377–385. [Google Scholar] [CrossRef]
- Quinn, T.C.; Riggin, C.H.; Kline, R.L.; Francis, H.; Mulanga, K.; Sension, M.G.; Fauci, A.S. Rapid latex agglutination assay using recombinant envelope polypeptide for the detection of antibody to the HIV. JAMA 1988, 260, 510–513. [Google Scholar] [CrossRef] [PubMed]
- Dusetty, P.; Velazquez, F.R.; Gutierrez-Escolano, A.L.; Ludert, J.E. Evaluation of the second generation of a commercial latex agglutination test for the detection of rotavirus antigens in fecal samples. J. Clin. Virol. 2013, 57, 88–90. [Google Scholar] [CrossRef] [PubMed]
- Sulahian, A.; Tabouret, M.; Ribaud, P.; Sarfati, J.; Gluckman, E.; Latge, J.P.; Derouin, F. Comparison of an enzyme immunoassay and latex agglutination test for detection of galactomannan in the diagnosis of invasive aspergillosis. Eur. J. Clin. Microbiol. Infect. Dis. 1996, 15, 139–145. [Google Scholar] [CrossRef] [PubMed]
- Maertens, J.; Theunissen, K.; Lagrou, K. Galactomannan testing. In Aspergillosis: From Diagnosis to Prevention; Springer: Haarlem, The Netherlands, 2009; pp. 105–124. [Google Scholar]
- Wadsworth, C.; Wadsworth, E. Efficacy of latex agglutination and quantification methods for determination of C-reactive protein (CRP) in pediatrie sera. Clin. Chim. Acta 1984, 138, 309–318. [Google Scholar] [CrossRef]
- Nakamura, N.; Hashimoto, K.; Matsunaga, T. Immunoassay method for the determination of immunoglobulin G using bacterial magnetic particles. Anal. Chem. 1991, 63, 268–272. [Google Scholar] [CrossRef] [PubMed]
- Lejon, V.; Legros, D.; Richer, M.; Ruiz, J.A.; Jamonneau, V.; Truc, P.; Doua, F.; Dje, N.; N’Siesi, F.X.; Bisser, S. IgM quantification in the cerebrospinal fluid of sleeping sickness patients by a latex card agglutination test. Trop. Med. Int. Health 2002, 7, 685–692. [Google Scholar] [CrossRef] [PubMed]
- Wang, J.; Kawde, A.; Erdem, A.; Salazar, M. Magnetic bead-based label-free electrochemical detection of DNA hybridization. Analyst 2001, 126, 2020–2024. [Google Scholar] [CrossRef] [PubMed]
- Kodzius, R.; Castro, D.; Chhina, S.; Parameswaran, A.M.; Foulds, I.G. DNA and protein detection based on microbead agglutination. In Proceedings of the Hilton Head Workshop on the Science and Technology of Solid-State Sensors, Actuators, and Microsystems, Hilton Head, SC, USA, 3–7 June 2012. [Google Scholar]
- Grundy, M.A.; Barnes, R.A.; Coakley, W.T. Highly sensitive detection of fungal antigens by ultrasound-enhanced latex agglutination. J. Med. Vet. Mycol. 1995, 33, 201–203. [Google Scholar] [CrossRef] [PubMed]
- Fujikawa, H.; Igarashi, H. Rapid latex agglutination test for detection of staphylococcal enterotoxins A to E that uses high-density latex particles. Appl. Environ. Microbiol. 1988, 54, 2345–2348. [Google Scholar] [PubMed]
- Ansorg, R.; Boom, R.; Rath, P.M. Detection of Aspergillus galactomannan antigen in foods and antibiotics. Mycoses 1997, 40, 353–357. [Google Scholar] [CrossRef] [PubMed]
- Verpoorte, E. Focusbeads and chips: New recipes for analysis. Lab Chip 2003, 3, 60N–68N. [Google Scholar] [PubMed]
- Degre, G.; Brunet, E.; Dodge, A.; Tabeling, P. Improving agglutination tests by working in microfluidic channels. Lab Chip 2005, 5, 691–694. [Google Scholar] [CrossRef] [PubMed]
- Choi, S.H.; Kim, D.S.; Kwon, T.H. Microinjection molded disposable microfluidic lab-on-a-chip for efficient detection of agglutination. Microsyst. Technol. 2009, 15, 309–316. [Google Scholar] [CrossRef]
- Chhina, S.K.; Perez, C.F.; Parameswaran, M. Microfluidic system to detect DNA amplicons using agglutination technique. J. Micromech. Microeng. 2012, 22, 115038. [Google Scholar] [CrossRef]
- Yu, X.; Hartmann, M.; Wang, Q.; Poetz, O.; Schneiderhan-Marra, N.; Stoll, D.; Kazmaier, C.; Joos, T.O. µFBI: a microfluidic bead-based immunoassay for multiplexed detection of proteins from a µL sample volume. PLoS ONE 2010, 5, e13125. [Google Scholar] [CrossRef] [PubMed]
- Ma, Z.; Zhang, P.; Cheng, Y.; Xie, S.; Zhang, S.; Ye, X. Homogeneous agglutination assay based on micro-chip sheathless flow cytometry. Biomicrofluidics 2015, 9, 066501. [Google Scholar] [CrossRef] [PubMed]
- Lucas, L.J.; Han, J.-H.; Chesler, J.; Yoon, J.-Y. Latex immunoagglutination assay for a vasculitis marker in a microfluidic device using static light scattering detection. Biosens. Bioelectron. 2007, 22, 2216–2222. [Google Scholar] [CrossRef] [PubMed]
- Han, Y.; Wu, H.; Liu, F.; Cheng, G.; Zhe, J. Label-free biomarker assay in a microresistive pulse sensor via immunoaggregation. Anal. Chem. 2014, 86, 9717–9722. [Google Scholar] [CrossRef] [PubMed]
- Afshar, R.; Moser, Y.; Lehnert, T.; Gijs, M.A.M. Three-dimensional magnetic focusing of superparamagnetic beads for on-chip agglutination assays. Anal. Chem. 2011, 83, 1022–1029. [Google Scholar] [CrossRef] [PubMed]
- Han, J.-H.; Kim, K.-S.; Yoon, J.-Y. The enhanced diffusional mixing for latex immunoagglutination assay in a microfluidic device. Anal. Chim. Acta 2007, 584, 252–259. [Google Scholar] [CrossRef] [PubMed]
- Kline, T.R.; Runyon, M.K.; Pothiawala, M.; Ismagilov, R.F. ABO, D blood typing and subtyping using plug-based microfluidics. Anal. Chem. 2008, 80, 6190–6197. [Google Scholar] [CrossRef] [PubMed]
- Teste, B.; Ali-Cherif, A.-A.; Viovy, J.L.; Malaquin, L. A low cost and high throughput magnetic bead-based immuno-agglutination assay in confined droplets. Lab Chip 2013, 10, 2344–2349. [Google Scholar] [CrossRef] [PubMed]
- Castro, D.; Kodzius, R.; Foulds, I.G. A simple system for in-droplet incubation and quantification of agglutination assays. MicroTAS Conf. Proc. 2013, 17, 1598–1600. [Google Scholar]
- Malmstadt, N.; Yager, P.; Hoffman, A.S.; Stayton, P.S. A smart microfluidic affinity chromatography matrix composed of poly (N-Isopropylacrylamide)-coated beads. Anal. Chem. 2003, 75, 2943–2949. [Google Scholar] [CrossRef] [PubMed]
- Malmstadt, N.; Hoffman, A.S.; Stayton, P.S. “Smart” mobile affinity matrix for microfluidic immunoassays. Lab Chip 2004, 4, 412–415. [Google Scholar] [CrossRef] [PubMed]
- Moser, Y.; Lehnert, T.; Gijs, M.A.M. On-chip immuno-agglutination assay with analyte capture by dynamic manipulation of superparamagnetic beads. Lab Chip 2009, 9, 3261–3267. [Google Scholar] [CrossRef] [PubMed]
- Huebner, A.; Sharma, S.; Srisa-Art, M.; Hollfelder, F.; Edel, J.B. Microdroplets: A sea of applications? Lab Chip 2008, 8, 1244–1254. [Google Scholar] [CrossRef] [PubMed]
- Phillips, T.W.; Lignos, I.G.; Maceiczyk, R.M. Nanocrystal synthesis in microfluidic reactors: Where next? Lab Chip 2014, 14, 3172–3180. [Google Scholar] [CrossRef] [PubMed]
- Dressler, O.; Solvas, X.; deMello, A. Chemical and biological dynamics using droplet-based microfluidics. Annu. Rev. Anal. Chem. 2017, 10, 1–24. [Google Scholar] [CrossRef] [PubMed]
- Beard, D.A. Taylor dispersion of a solute in a microfluidic channel. J. Appl. Phys. 2001, 89, 4667–4669. [Google Scholar] [CrossRef]
- Curcio, M.; Roeraade, J. Continuous segmented-flow polymerase chain reaction for high-throughput miniaturized DNA amplification. Anal. Chem. 2003, 75, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Song, H.; Tice, J.D.; Ismagilov, R.F. A microfluidic system for controlling reaction networks in time. Angew. Chem. 2003, 115, 792–796. [Google Scholar] [CrossRef]
- Kashid, M.N.; Gerlach, I.; Goetz, S.; Franzke, J.; Acker, J.F.; Platte, F.; Agar, D.W.; Turek, S. Internal circulation within the liquid slugs of a liquid- liquid slug-flow capillary microreactor. Ind. Eng. Chem. Res. 2005, 44, 5003–5010. [Google Scholar] [CrossRef]
- Handique, K.; Burns, M.A. Mathematical modeling of drop mixing in a slit-type microchannel. J. Micromech. Microeng. 2001, 11, 548. [Google Scholar] [CrossRef]
- Tice, J.D.; Song, H.; Lyon, A.D.; Ismagilov, R.F. Formation of droplets and mixing in multiphase microfluidics at low values of the reynolds and the capillary numbers. Langmuir 2003, 19, 9127–9133. [Google Scholar] [CrossRef]
- Kurup, G.K.; Basu, A.S. Hydrodynamic particle concentration inside a microfluidic plug. In Proceedings of the Micro Total Analysis Systems, Groningen, The Netherlands, 3–7 October 2010. [Google Scholar]
- Kurup, G.K.; Basu, A.S. Field-free particle focusing in microfluidic plugs. Biomicrofluidics 2012, 6, 22008–2200810. [Google Scholar] [CrossRef] [PubMed]
- Theberge, A.B.; Courtois, F.; Schaerli, Y.; Fischlechner, M.; Abell, C.; Hollfelder, F.; Huck, W.T.S. Microdroplets in microfluidics: An evolving platform for discoveries in chemistry and biology. Angew. Chem. Int. Ed. 2010, 49, 5846–5868. [Google Scholar] [CrossRef] [PubMed]
- Rastogi, V.; Velev, O.D. Development and evaluation of realistic microbioassays in freely suspended droplets on a chip. Biomicrofluidics 2007, 1, 014107. [Google Scholar] [CrossRef] [PubMed]
- Sivashankar, S.; Castro, D.; Buttner, U.; Foulds, I.G. Real-time agglutination within a microdroplet in a three phase fluidic well for detection of biomarkers. In Proceedings of the 18th International Conference on Miniaturized Systems for Chemistry and Life Sciences, San Antonio, TX, USA, 26–30 October 2014; pp. 2097–2100. [Google Scholar]
- Dombrowski, R.D.; Litster, J.D.; Wagner, N.J.; He, Y. Crystallization of α-lactose monohydrate in a drop-based microfluidic crystallizer. Chem. Eng. Sci. 2007, 62, 4802–4810. [Google Scholar] [CrossRef]
- Ildefonso, M.; Candoni, N.; Veesler, S. A cheap, easy microfluidic crystallization device ensuring universal solvent compatibility. Org. Process Res. Dev. 2012, 16, 556–560. [Google Scholar] [CrossRef]
- Zhang, S.; Ferté, N.; Candoni, N.; Veesler, S. Versatile microfluidic approach to crystallization. Org. Process Res. Dev. 2015, 19, 1837–1841. [Google Scholar] [CrossRef]
- Trivedi, V.; Doshi, A.; Kurup, G.K.; Ereifej, E.; Vandevord, P.J.; Basu, A.S. A modular approach for the generation, storage, mixing, and detection of droplet libraries for high throughput screening. Lab Chip 2010, 10, 2433–2442. [Google Scholar] [CrossRef] [PubMed]
- Van Steijn, V.; Korczyk, P.M.; Derzsi, L.; Abate, A.R.; Weitz, D.A.; Garstecki, P. Block-and-break generation of microdroplets with fixed volume. Biomicrofluidics 2013, 7, 24108. [Google Scholar] [CrossRef] [PubMed]
- Ali-Cherif, A.; Begolo, S.; Descroix, S.; Viovy, J.-L.; Malaquin, L. Programmable magnetic tweezers and droplet microfluidic device for high-throughput nanoliter multi-step assays. Angew. Chem. Int. Ed. 2012, 51, 10765–10769. [Google Scholar] [CrossRef] [PubMed]
- Zhu, Y.; Fang, Q. Analytical detection techniques for droplet microfluidics—A review. Anal. Chim. Acta 2013, 787, 24–35. [Google Scholar] [CrossRef] [PubMed]
- Henery, S.; George, T.; Hall, B.; Basiji, D.; Ortyn, W.; Morrissey, P. Quantitative image based apoptotic index measurement using multispectral imaging flow cytometry: A comparison with standard photometric methods. Apoptosis 2008, 13, 1054–1063. [Google Scholar] [CrossRef] [PubMed]
- Basiji, D.; O’Gorman, M.R. Imaging flow cytometry. J. Immunol. Methods 2015, 423, 1–2. [Google Scholar] [CrossRef] [PubMed]
- Basiji, D.A.; Ortyn, W.E.; Liang, L.; Venkatachalam, V.; Morrissey, P. Cellular image analysis and imaging by flow cytometry. Clin. Lab. Med. 2007, 27, 653–670. [Google Scholar] [CrossRef] [PubMed]
- Mohammed, M.I.; Haswell, S.; Gibson, I. Lab-on-a-chip or chip-in-a-lab: Challenges of commercialization lost in translation. Procedia Technol. 2015, 20, 54–59. [Google Scholar] [CrossRef]
- Haber, C. Microfluidics in commercial applications; an industry perspective. Lab Chip 2006, 6, 1118–1121. [Google Scholar] [PubMed]
- Mortensen, N.A.; Okkels, F.; Bruus, H. Reexamination of hagen-poiseuille flow: Shape dependence of the hydraulic resistance in microchannels. Phys. Rev. E 2005, 71, 057301. [Google Scholar] [CrossRef] [PubMed]
- De Ville, M.; Coquet, P.; Brunet, P.; Boukherroub, R. Simple and low-cost fabrication of PDMS microfluidic round channels by surface-wetting parameters optimization. Microfluid. Nanofluidics 2012, 12, 953–961. [Google Scholar] [CrossRef]
- Holmberg, A.; Blomstergren, A.; Nord, O.; Lukacs, M.; Lundeberg, J.; Uhlen, M. The biotin-streptavidin interaction can be reversibly broken using water at elevated temperatures. Electrophroesis 2005, 26, 501–510. [Google Scholar] [CrossRef] [PubMed]
- Bangs, L.B. New developments in particle-based immunoassays: Introduction. Pure Appl. Chem. 1996, 68, 1873–1879. [Google Scholar] [CrossRef]
- Castro, D.; Conchouso, D.; Arevalo, A.; Foulds, I.G. A study of the incubation of microbead agglutination assays in a microfluidic system. In Proceedings of the 2016 IEEE 11th Annual International Conference on Nano/Micro Engineered and Molecular Systems (NEMS), Sendai, Japan, 17–20 April 2016. [Google Scholar]
- Rattle, S.; Hofmann, O.; Price, C.; Kricka, L.J.; Wild, D. 2.10 Lab-on-a-chip, micro- and nanoscale immunoassay systems, and microarrays. In The Immunoassay Handbook; Elsevier: New York, NY, USA, 2013. [Google Scholar]
- Reverberi, R.; Reverberi, L. Factors affecting the antigen-antibody reaction. Blood Transfus. 2007, 5, 227–240. [Google Scholar] [PubMed]
- Teste, B.; Champ, J.; Londono, A.; Descroix, S.; Malaquin, L.; Viovy, J.; Draskovic, I.; Mottet, G. Chromatin immunoprecipitation in microfluidic droplets: Towards fast and cheap analyses. Lab Chip 2017, 17, 530–537. [Google Scholar] [CrossRef] [PubMed]
- Kundu, P.K.; Cohen, I.M.; Dowling, D.R. Fluid Mechanics, 5th ed.; Academic Press: Boston, MA, USA, 2012. [Google Scholar]
- Conchouso, D.; Castro, D.; Khan, S.A.; Foulds, I.G. Three-dimensional parallelization of microfluidic droplet generators for a litre per hour volume production of single emulsions. Lab Chip 2014, 14, 3011–3020. [Google Scholar] [CrossRef] [PubMed]
- Conchouso, D.; McKerricher, G.; Arevalo, A.; Castro, D.; Shamim, A.; Foulds, I.G. Comparison of capacitive and radio frequency resonator sensors for monitoring parallelized droplet microfluidic production. Lab Chip 2016, 16, 3210–3219. [Google Scholar] [CrossRef] [PubMed]
- Stamm, A.M.; Polt, S.S. False-negative cryptococcal antigen test. JAMA 1980, 244, 1359. [Google Scholar] [CrossRef] [PubMed]
- Louie, L.; Matsumura, S.O.; Choi, E.; Louie, M.; Simor, A.E. Evaluation of three rapid methods for detection of methicillin resistance in Staphylococcus aureus. J. Clin. Microbiol. 2000, 38, 2170–2173. [Google Scholar] [PubMed]
- Huh, D.; Hamilton, G.A.; Ingber, D.E. From 3D cell culture to organs-on-chips. Trends Cell Biol. 2011, 21, 745–754. [Google Scholar] [CrossRef] [PubMed]
- Zheng, F.; Fu, F.; Cheng, Y.; Wang, C.; Zhao, Y.; Gu, Z. Organ-on-a-chip systems: Microengineering to biomimic living systems. Small 2016, 12, 2253–2282. [Google Scholar] [CrossRef] [PubMed]
- Kodzius, R.; Schulze, F.; Gao, X.; Schneider, M.R. Organ-on-chip technology: Current state and future developments. Genes 2017, 8, 266. [Google Scholar] [CrossRef] [PubMed]
- Li, X.; Valadez, A.V.; Zuo, P.; Nie, Z. Microfluidic 3D cell culture: Potential application for tissue-based bioassays. Bioanalysis 2012, 4, 1509–1525. [Google Scholar] [CrossRef] [PubMed]
- Bhise, N.S.; Ribas, J.; Manoharan, V.; Zhang, Y.S.; Polini, A.; Massa, S.; Dokmeci, M.R.; Khademhosseini, A. Organ-on-a-chip platforms for studying drug delivery systems. J. Controll. Release 2014, 190, 82–93. [Google Scholar] [CrossRef] [PubMed]
- Damiati, S.; Kompella, U.; Damiati, S.; Kodzius, R. Microfluidic devices for drug delivery systems and drug screening. Genes 2018, 9, 103. [Google Scholar] [CrossRef] [PubMed]
- Wang, Z.; Samanipour, R.; Koo, K.; Kim, K. Organ-on-a-chip platforms for drug delivery and cell characterization: A review. Sens. Mater. 2015, 27, 487–506. [Google Scholar]
- Lee, P.J.; Hung, P.J.; Lee, L.P. An artificial liver sinusoid with a microfluidic endothelial-like barrier for primary hepatocyte culture. Biotechnol. Bioeng. 2007, 97, 1340–1346. [Google Scholar] [CrossRef] [PubMed]
- Goral, V.N.; Hsieh, Y.; Petzold, O.N.; Clark, J.S.; Yuen, P.K.; Faris, R.A. Perfusion-based microfluidic device for three-dimensional dynamic primary human hepatocyte cell culture in the absence of biological or synthetic matrices or coagulants. Lab Chip 2010, 10, 3380–3386. [Google Scholar] [CrossRef] [PubMed]
- Imura, Y.; Sato, K.; Yoshimura, E. Micro total bioassay system for ingested substances: Assessment of intestinal absorption, hepatic metabolism, and bioactivity. Anal. Chem. 2010, 82, 9983–9988. [Google Scholar] [CrossRef] [PubMed]
- Zhang, C.; Zhao, Z.; Rahim, N.A.A.; van Noort, D.; Yu, H. Towards a human-on-chip: Culturing multiple cell types on a chip with compartmentalized microenvironments. Lab Chip 2009, 9, 3185–3192. [Google Scholar] [CrossRef] [PubMed]
- Van Midwoud, P.M.; Groothuis, G.M.M.; Merema, M.T.; Verpoorte, E. Microfluidic biochip for the perifusion of precision-cut rat liver slices for metabolism and toxicology studies. Biotechnol. Bioeng. 2010, 105, 184–194. [Google Scholar] [CrossRef] [PubMed]
- Baudoin, R.; Griscom, L.; Prot, J.M.; Legallais, C.; Leclerc, E. Behavior of HepG2/C3A cell cultures in a microfluidic bioreactor. Biochem. Eng. J. 2011, 53, 172–181. [Google Scholar] [CrossRef]
- Capulli, A.K.; Tian, K.; Mehandru, N.; Bukhta, A.; Choudhury, S.F.; Suchyta, M.; Parker, K.K. Approaching the in vitro clinical trial: Engineering organs on chips. Lab Chip 2014, 14, 3181–3186. [Google Scholar] [CrossRef] [PubMed]
| Particle Diameter (µm) | Us (m/s) | Us (mm/day) |
|---|---|---|
| 1 | 3.26 × 10−7 | 28.2 |
| 2.8 | 2.56 × 10−6 | 221 |
| 5 | 8.6 × 10−6 | 705 |
| 10 | 3.26 × 10−5 | 2.82 × 103 |
| 50 | 8.16 × 10−4 | 7.05 × 104 |
| 100 | 3.26 × 10−3 | 2.82 × 105 |
| 500 | 8.16 × 10−2 | 7.05 × 106 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Castro, D.; Conchouso, D.; Kodzius, R.; Arevalo, A.; Foulds, I.G. High-Throughput Incubation and Quantification of Agglutination Assays in a Microfluidic System. Genes 2018, 9, 281. https://doi.org/10.3390/genes9060281
Castro D, Conchouso D, Kodzius R, Arevalo A, Foulds IG. High-Throughput Incubation and Quantification of Agglutination Assays in a Microfluidic System. Genes. 2018; 9(6):281. https://doi.org/10.3390/genes9060281
Chicago/Turabian StyleCastro, David, David Conchouso, Rimantas Kodzius, Arpys Arevalo, and Ian G. Foulds. 2018. "High-Throughput Incubation and Quantification of Agglutination Assays in a Microfluidic System" Genes 9, no. 6: 281. https://doi.org/10.3390/genes9060281
APA StyleCastro, D., Conchouso, D., Kodzius, R., Arevalo, A., & Foulds, I. G. (2018). High-Throughput Incubation and Quantification of Agglutination Assays in a Microfluidic System. Genes, 9(6), 281. https://doi.org/10.3390/genes9060281





