Modulating Neural Circuits of Pain in Preclinical Models: Recent Insights for Future Therapeutics
Abstract
1. Introduction
2. Pain Imaging in Humans
3. Contributions of Optogenetics and Chemogenetics
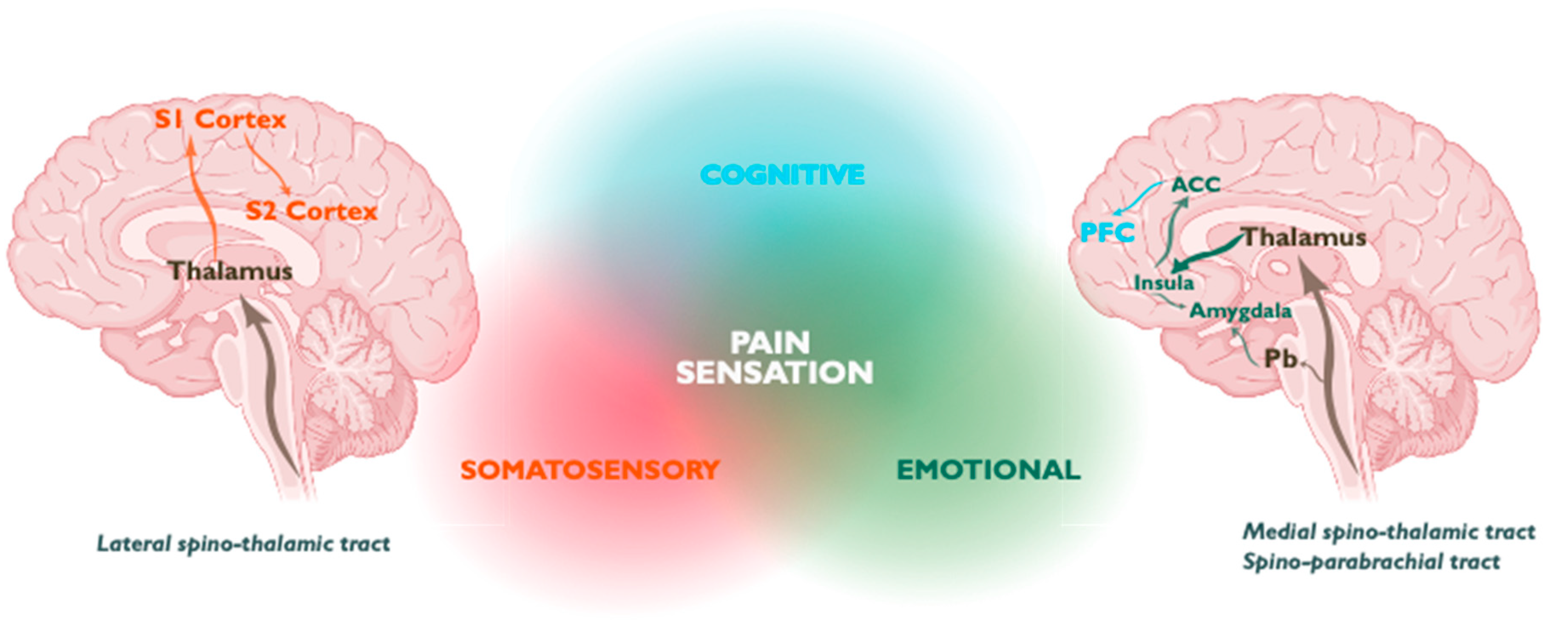
4. Manipulating the Brain “Pain Matrix”
4.1. Sensory-Discriminative Component
4.1.1. Somatosensory Cortex
4.1.2. Mid-Cingulate Cortex
4.2. Cognitive and Emotional Components of Pain
4.2.1. Anterior Cingulate Cortex (ACC)
4.2.2. Prefrontal Cortex (PFC)
4.2.3. Amygdala
4.2.4. Insular Cortex
4.3. Subcortical Areas Pathways
4.3.1. Thalamus
4.3.2. Descending Pain Pathways
5. New Pain Behaviour Assessments
6. Conclusions
Funding
Conflicts of Interest
References
- Baron, R. Neuropathic Pain: A Clinical Perspective. In Sensory Nerves; Canning, B.J., Spina, D., Eds.; Handbook of Experimental Pharmacology; Springer: Berlin/Heidelberg, Germany, 2009; Volume 194, pp. 3–30. ISBN 978-3-540-79089-1. [Google Scholar]
- Jensen, T.S. Anticonvulsants in Neuropathic Pain: Rationale and Clinical Evidence. Eur. J. Pain 2002, 6, 61–68. [Google Scholar] [CrossRef] [PubMed]
- Nalamachu, S. An Overview of Pain Management: The Clinical Efficacy and Value of Treatment. Am. J. Manag. Care 2013, 19, s261–s266. [Google Scholar] [PubMed]
- Alorfi, N.M. Pharmacological Methods of Pain Management: Narrative Review of Medication Used. Int. J. Gen. Med. 2023, 16, 3247–3256. [Google Scholar] [CrossRef] [PubMed]
- Krashin, D.; Murinova, N.; Sullivan, M. Challenges to Treatment of Chronic Pain and Addiction during the “Opioid Crisis”. Curr. Pain Headache Rep. 2016, 20, 65. [Google Scholar] [CrossRef] [PubMed]
- Skolnick, P. The Opioid Epidemic: Crisis and Solutions. Annu. Rev. Pharmacol. Toxicol. 2018, 58, 143–159. [Google Scholar] [CrossRef] [PubMed]
- Nguyen, J.-P.; Nizard, J.; Keravel, Y.; Lefaucheur, J.-P. Invasive Brain Stimulation for the Treatment of Neuropathic Pain. Nat. Rev. Neurol. 2011, 7, 699–709. [Google Scholar] [CrossRef] [PubMed]
- Ingvar, M. Pain and Functional Imaging. Phil. Trans. R. Soc. Lond. B 1999, 354, 1347–1358. [Google Scholar] [CrossRef] [PubMed]
- Melzack, R. Pain and the Neuromatrix in the Brain. J. Dent. Educ. 2001, 65, 1378–1382. [Google Scholar] [CrossRef] [PubMed]
- Garcia-Larrea, L.; Bastuji, H. Pain and Consciousness. Prog. Neuro-Psychopharmacol. Biol. Psychiatry 2018, 87, 193–199. [Google Scholar] [CrossRef]
- Legrain, V.; Iannetti, G.D.; Plaghki, L.; Mouraux, A. The Pain Matrix Reloaded: A Salience Detection System for the Body. Prog. Neurobiol. 2011, 93, 111–124. [Google Scholar] [CrossRef]
- Morton, D.; Jones, A.; Sandhu, J. Brain Imaging of Pain: State of the Art. J. Pain Res. 2016, 9, 613–624. [Google Scholar] [CrossRef]
- Merskey, H.; Bogduk, N.; International Association for the Study of Pain. Task Force on Taxonomy. In Classification of Chronic Pain: Descriptions of Chronic Pain Syndromes and Definitions of Pain Terms; IASP Press: Washington, DC, USA, 1994. [Google Scholar]
- Bushnell, M.C.; Čeko, M.; Low, L.A. Cognitive and Emotional Control of Pain and Its Disruption in Chronic Pain. Nat. Rev. Neurosci. 2013, 14, 502–511. [Google Scholar] [CrossRef]
- Davis, K.D.; Flor, H.; Greely, H.T.; Iannetti, G.D.; Mackey, S.; Ploner, M.; Pustilnik, A.; Tracey, I.; Treede, R.-D.; Wager, T.D. Brain Imaging Tests for Chronic Pain: Medical, Legal and Ethical Issues and Recommendations. Nat. Rev. Neurol. 2017, 13, 624–638. [Google Scholar] [CrossRef]
- Bastuji, H.; Frot, M.; Perchet, C.; Magnin, M.; Garcia-Larrea, L. Pain Networks from the inside: Spatiotemporal Analysis of Brain Responses Leading from Nociception to Conscious Perception. Hum. Brain Mapp. 2016, 37, 4301–4315. [Google Scholar] [CrossRef]
- Wager, T.D.; Atlas, L.Y.; Lindquist, M.A.; Roy, M.; Woo, C.-W.; Kross, E. An fMRI-Based Neurologic Signature of Physical Pain. N. Engl. J. Med. 2013, 368, 1388–1397. [Google Scholar] [CrossRef] [PubMed]
- Bornhövd, K.; Quante, M.; Glauche, V.; Bromm, B.; Weiller, C.; Büchel, C. Painful Stimuli Evoke Different Stimulus–Response Functions in the Amygdala, Prefrontal, Insula and Somatosensory Cortex: A Single-trial fMRI Study. Brain 2002, 125, 1326–1336. [Google Scholar] [CrossRef] [PubMed]
- Peyron, R.; Garcia-Larrea, L.; Deiber, M.P.; Cinotti, L.; Convers, P.; Sindou, M.; Mauguière, F.; Laurent, B. Electrical Stimulation of Precentral Cortical Area in the Treatment of Central Pain: Electrophysiological and PET Study. Pain 1995, 62, 275–286. [Google Scholar] [CrossRef] [PubMed]
- Petrovic, P.; Ingvar, M.; Stone-Elander, S.; Petersson, M.K.; Hansson, P. A PET Activation Study of Dynamic Mechanical Allodynia in Patients with Mononeuropathy. Pain 1999, 83, 459–470. [Google Scholar] [CrossRef] [PubMed]
- Witting, N.; Kupers, R.C.; Svensson, P.; Arendt–Nielsen, L.; Gjedde, A.; Jensen, T.S. Experimental Brush-Evoked Allodynia Activates Posterior Parietal Cortex. Neurology 2001, 57, 1817–1824. [Google Scholar] [CrossRef]
- Ducreux, D.; Attal, N.; Parker, F.; Bouhassira, D. Mechanisms of Central Neuropathic Pain: A Combined Psychophysical and fMRI Study in Syringomyelia. Brain 2006, 129, 963–976. [Google Scholar] [CrossRef]
- Hashmi, J.A.; Baliki, M.N.; Huang, L.; Baria, A.T.; Torbey, S.; Hermann, K.M.; Schnitzer, T.J.; Apkarian, A.V. Shape Shifting Pain: Chronification of Back Pain Shifts Brain Representation from Nociceptive to Emotional Circuits. Brain 2013, 136, 2751–2768. [Google Scholar] [CrossRef]
- Schweinhardt, P.; Lee, M.; Tracey, I. Imaging Pain in Patients: Is It Meaningful? Curr. Opin. Neurol. 2006, 19, 392–400. [Google Scholar] [CrossRef]
- Schweinhardt, P.; Glynn, C.; Brooks, J.; McQuay, H.; Jack, T.; Chessell, I.; Bountra, C.; Tracey, I. An fMRI Study of Cerebral Processing of Brush-Evoked Allodynia in Neuropathic Pain Patients. NeuroImage 2006, 32, 256–265. [Google Scholar] [CrossRef] [PubMed]
- Roza, C.; Martinez-Padilla, A. Asymmetric Lateralization during Pain Processing. Symmetry 2021, 13, 2416. [Google Scholar] [CrossRef]
- Garcia-Larrea, L.; Peyron, R. Pain Matrices and Neuropathic Pain Matrices: A Review. Pain 2013, 154 (Suppl. S1), S29–S43. [Google Scholar] [CrossRef] [PubMed]
- Saksham, S.; Sanjana, P.S.; Shefali, M.; Soham, N.; Sujith, K. Developments in Application of Optogenetics in Pain and Anxiety: A Literature Review. Sci. Collect. InterConf+ 2023, 31, 209–225. [Google Scholar] [CrossRef]
- Deisseroth, K. Optogenetics. Nat. Methods 2011, 8, 26–29. [Google Scholar] [CrossRef] [PubMed]
- Huidobro, N.; De la Torre-Valdovinos, B.; Mendez, A.; Treviño, M.; Arias-Carrion, O.; Chavez, F.; Gutierrez, R.; Manjarrez, E. Optogenetic Noise-Photostimulation on the Brain Increases Somatosensory Spike Firing Responses. Neurosci. Lett. 2018, 664, 51–57. [Google Scholar] [CrossRef]
- Armbruster, B.N.; Li, X.; Pausch, M.H.; Herlitze, S.; Roth, B.L. Evolving the Lock to Fit the Key to Create a Family of G Protein-Coupled Receptors Potently Activated by an Inert Ligand. Proc. Natl. Acad. Sci. USA 2007, 104, 5163–5168. [Google Scholar] [CrossRef]
- Smith, K.S.; Bucci, D.J.; Luikart, B.W.; Mahler, S.V. DREADDS: Use and Application in Behavioral Neuroscience. Behav. Neurosci. 2016, 130, 137–155. [Google Scholar] [CrossRef]
- Nagai, Y.; Miyakawa, N.; Takuwa, H.; Hori, Y.; Oyama, K.; Ji, B.; Takahashi, M.; Huang, X.-P.; Slocum, S.T.; DiBerto, J.F.; et al. Deschloroclozapine, a Potent and Selective Chemogenetic Actuator Enables Rapid Neuronal and Behavioral Modulations in Mice and Monkeys. Nat. Neurosci. 2020, 23, 1157–1167. [Google Scholar] [CrossRef] [PubMed]
- Gross, J.; Schnitzler, A.; Timmermann, L.; Ploner, M. Gamma Oscillations in Human Primary Somatosensory Cortex Reflect Pain Perception. PLoS Biol. 2007, 5, e133. [Google Scholar] [CrossRef] [PubMed]
- Cardin, J.A.; Carlén, M.; Meletis, K.; Knoblich, U.; Zhang, F.; Deisseroth, K.; Tsai, L.-H.; Moore, C.I. Driving Fast-Spiking Cells Induces Gamma Rhythm and Controls Sensory Responses. Nature 2009, 459, 663–667. [Google Scholar] [CrossRef] [PubMed]
- Tan, L.L.; Oswald, M.J.; Heinl, C.; Retana Romero, O.A.; Kaushalya, S.K.; Monyer, H.; Kuner, R. Gamma Oscillations in Somatosensory Cortex Recruit Prefrontal and Descending Serotonergic Pathways in Aversion and Nociception. Nat. Commun. 2019, 10, 983. [Google Scholar] [CrossRef] [PubMed]
- Ziegler, K.; Folkard, R.; Gonzalez, A.J.; Burghardt, J.; Antharvedi-Goda, S.; Martin-Cortecero, J.; Isaías-Camacho, E.; Kaushalya, S.; Tan, L.L.; Kuner, T.; et al. Primary Somatosensory Cortex Bidirectionally Modulates Sensory Gain and Nociceptive Behavior in a Layer-Specific Manner. Nat. Commun. 2023, 14, 2999. [Google Scholar] [CrossRef] [PubMed]
- Tan, L.L.; Pelzer, P.; Heinl, C.; Tang, W.; Gangadharan, V.; Flor, H.; Sprengel, R.; Kuner, T.; Kuner, R. A Pathway from Midcingulate Cortex to Posterior Insula Gates Nociceptive Hypersensitivity. Nat. Neurosci. 2017, 20, 1591–1601. [Google Scholar] [CrossRef] [PubMed]
- Barthas, F.; Sellmeijer, J.; Hugel, S.; Waltisperger, E.; Barrot, M.; Yalcin, I. The Anterior Cingulate Cortex Is a Critical Hub for Pain-Induced Depression. Biol. Psychiatry 2015, 77, 236–245. [Google Scholar] [CrossRef] [PubMed]
- Chen, T.; Taniguchi, W.; Chen, Q.-Y.; Tozaki-Saitoh, H.; Song, Q.; Liu, R.-H.; Koga, K.; Matsuda, T.; Kaito-Sugimura, Y.; Wang, J.; et al. Top-down Descending Facilitation of Spinal Sensory Excitatory Transmission from the Anterior Cingulate Cortex. Nat. Commun. 2018, 9, 1886. [Google Scholar] [CrossRef] [PubMed]
- Bouchatta, O.; Aby, F.; Sifeddine, W.; Bouali-Benazzouz, R.; Brochoire, L.; Manouze, H.; Fossat, P.; Ba M’Hamed, S.; Bennis, M.; Landry, M. Pain Hypersensitivity in a Pharmacological Mouse Model of Attention-Deficit/Hyperactivity Disorder. Proc. Natl. Acad. Sci. USA 2022, 119, e2114094119. [Google Scholar] [CrossRef]
- Huang, J.; Gadotti, V.M.; Chen, L.; Souza, I.A.; Huang, S.; Wang, D.; Ramakrishnan, C.; Deisseroth, K.; Zhang, Z.; Zamponi, G.W. A Neuronal Circuit for Activating Descending Modulation of Neuropathic Pain. Nat. Neurosci. 2019, 22, 1659–1668. [Google Scholar] [CrossRef]
- Zhang, Z.; Gadotti, V.M.; Chen, L.; Souza, I.A.; Stemkowski, P.L.; Zamponi, G.W. Role of Prelimbic GABAergic Circuits in Sensory and Emotional Aspects of Neuropathic Pain. Cell Rep. 2015, 12, 752–759. [Google Scholar] [CrossRef]
- Qi, X.; Cui, K.; Zhang, Y.; Wang, L.; Tong, J.; Sun, W.; Shao, S.; Wang, J.; Wang, C.; Sun, X.; et al. A Nociceptive Neuronal Ensemble in the Dorsomedial Prefrontal Cortex Underlies Pain Chronicity. Cell Rep. 2022, 41, 111833. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Q.; Hu, S.; Talay, R.; Xiao, Z.; Rosenberg, D.; Liu, Y.; Sun, G.; Li, A.; Caravan, B.; Singh, A.; et al. A Prototype Closed-Loop Brain–Machine Interface for the Study and Treatment of Pain. Nat. Biomed. Eng. 2021, 7, 533–545. [Google Scholar] [CrossRef] [PubMed]
- Sun, G.; Zeng, F.; McCartin, M.; Zhang, Q.; Xu, H.; Liu, Y.; Chen, Z.S.; Wang, J. Closed-Loop Stimulation Using a Multiregion Brain-Machine Interface Has Analgesic Effects in Rodents. Sci. Transl. Med. 2022, 14, eabm5868. [Google Scholar] [CrossRef] [PubMed]
- Meda, K.S.; Patel, T.; Braz, J.M.; Malik, R.; Turner, M.L.; Seifikar, H.; Basbaum, A.I.; Sohal, V.S. Microcircuit Mechanisms through Which Mediodorsal Thalamic Input to Anterior Cingulate Cortex Exacerbates Pain-Related Aversion. Neuron 2019, 102, 944–959.e3. [Google Scholar] [CrossRef] [PubMed]
- Huang, J.; Zhang, Z.; Gambeta, E.; Chen, L.; Zamponi, G.W. An Orbitofrontal Cortex to Midbrain Projection Modulates Hypersensitivity after Peripheral Nerve Injury. Cell Rep. 2021, 35, 109033. [Google Scholar] [CrossRef] [PubMed]
- Gu, L.; Uhelski, M.L.; Anand, S.; Romero-Ortega, M.; Kim, Y.; Fuchs, P.N.; Mohanty, S.K. Pain Inhibition by Optogenetic Activation of Specific Anterior Cingulate Cortical Neurons. PLoS ONE 2015, 10, e0117746. [Google Scholar] [CrossRef] [PubMed]
- Tovote, P.; Esposito, M.S.; Botta, P.; Chaudun, F.; Fadok, J.P.; Markovic, M.; Wolff, S.B.E.; Ramakrishnan, C.; Fenno, L.; Deisseroth, K.; et al. Midbrain Circuits for Defensive Behaviour. Nature 2016, 534, 206–212. [Google Scholar] [CrossRef] [PubMed]
- Mazzitelli, M.; Marshall, K.; Pham, A.; Ji, G.; Neugebauer, V. Optogenetic Manipulations of Amygdala Neurons Modulate Spinal Nociceptive Processing and Behavior Under Normal Conditions and in an Arthritis Pain Model. Front. Pharmacol. 2021, 12, 668337. [Google Scholar] [CrossRef]
- Corder, G.; Ahanonu, B.; Grewe, B.F.; Wang, D.; Schnitzer, M.J.; Scherrer, G. An Amygdalar Neural Ensemble That Encodes the Unpleasantness of Pain. Science 2019, 363, 276–281. [Google Scholar] [CrossRef]
- Samineni, V.K.; Grajales-Reyes, J.G.; Copits, B.A.; O’Brien, D.E.; Trigg, S.L.; Gomez, A.M.; Bruchas, M.R.; Gereau, R.W. Divergent Modulation of Nociception by Glutamatergic and GABAergic Neuronal Subpopulations in the Periaqueductal Gray. eNeuro 2017, 4, ENEURO.0129-16.2017. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Y.; Huang, X.; Xin, W.-J.; He, S.; Deng, J.; Ruan, X. Somatostatin Neurons from Periaqueductal Gray to Medulla Facilitate Neuropathic Pain in Male Mice. J. Pain 2023, 24, 1020–1029. [Google Scholar] [CrossRef] [PubMed]
- Winke, N.; Aby, F.; Jercog, D.; Girard, D.; Grivet, Z.; Landry, M.; Castell, L.; Valjent, E.; Valerio, S.; Fossat, P.; et al. Brainstem Somatostatin-Expressing Cells Promote Analgesia during Negative Emotional States. Res. Sq. 2022. [Google Scholar] [CrossRef]
- Taylor, N.E.; Pei, J.; Zhang, J.; Vlasov, K.Y.; Davis, T.; Taylor, E.; Weng, F.-J.; Van Dort, C.J.; Solt, K.; Brown, E.N. The Role of Glutamatergic and Dopaminergic Neurons in the Periaqueductal Gray/Dorsal Raphe: Separating Analgesia and Anxiety. eNeuro 2019, 6, ENEURO.0018-18.2019. [Google Scholar] [CrossRef] [PubMed]
- François, A.; Low, S.A.; Sypek, E.I.; Christensen, A.J.; Sotoudeh, C.; Beier, K.T.; Ramakrishnan, C.; Ritola, K.D.; Sharif-Naeini, R.; Deisseroth, K.; et al. A Brainstem-Spinal Cord Inhibitory Circuit for Mechanical Pain Modulation by GABA and Enkephalins. Neuron 2017, 93, 822–839.e6. [Google Scholar] [CrossRef] [PubMed]
- Aby, F.; Lorenzo, L.-E.; Grivet, Z.; Bouali-Benazzouz, R.; Martin, H.; Valerio, S.; Whitestone, S.; Isabel, D.; Idi, W.; Bouchatta, O.; et al. Switch of Serotonergic Descending Inhibition into Facilitation by a Spinal Chloride Imbalance in Neuropathic Pain. Sci. Adv. 2022, 8, eabo0689. [Google Scholar] [CrossRef] [PubMed]
- Ganley, R.P.; De Sousa, M.M.; Werder, K.; Öztürk, T.; Mendes, R.; Ranucci, M.; Wildner, H.; Zeilhofer, H.U. Targeted Anatomical and Functional Identification of Antinociceptive and Pronociceptive Serotonergic Neurons That Project to the Spinal Dorsal Horn. eLife 2023, 12, e78689. [Google Scholar] [CrossRef]
- Cai, Y.-Q.; Wang, W.; Hou, Y.-Y.; Pan, Z.Z. Optogenetic Activation of Brainstem Serotonergic Neurons Induces Persistent Pain Sensitization. Mol. Pain 2014, 10, 70. [Google Scholar] [CrossRef] [PubMed]
- Kucharczyk, M.W.; Di Domenico, F.; Bannister, K. Distinct Brainstem to Spinal Cord Noradrenergic Pathways Inversely Regulate Spinal Neuronal Activity. Brain 2022, 145, 2293–2300. [Google Scholar] [CrossRef]
- Hickey, L.; Li, Y.; Fyson, S.J.; Watson, T.C.; Perrins, R.; Hewinson, J.; Teschemacher, A.G.; Furue, H.; Lumb, B.M.; Pickering, A.E. Optoactivation of Locus Ceruleus Neurons Evokes Bidirectional Changes in Thermal Nociception in Rats. J. Neurosci. 2014, 34, 4148–4160. [Google Scholar] [CrossRef]
- Kohro, Y.; Matsuda, T.; Yoshihara, K.; Kohno, K.; Koga, K.; Katsuragi, R.; Oka, T.; Tashima, R.; Muneta, S.; Yamane, T.; et al. Spinal Astrocytes in Superficial Laminae Gate Brainstem Descending Control of Mechanosensory Hypersensitivity. Nat. Neurosci. 2020, 23, 1376–1387. [Google Scholar] [CrossRef] [PubMed]
- Neugebauer, V. Amygdala Pain Mechanisms. In Pain Control; Schaible, H.-G., Ed.; Springer: Berlin/Heidelberg, Germany, 2015; pp. 261–284. ISBN 978-3-662-46450-2. [Google Scholar]
- Neugebauer, V.; Galhardo, V.; Maione, S.; Mackey, S.C. Forebrain Pain Mechanisms. Brain Res. Rev. 2009, 60, 226–242. [Google Scholar] [CrossRef] [PubMed]
- Neugebauer, V.; Li, W.; Bird, G.C.; Han, J.S. The Amygdala and Persistent Pain. Neuroscientist 2004, 10, 221–234. [Google Scholar] [CrossRef] [PubMed]
- Kuner, R.; Kuner, T. Cellular Circuits in the Brain and Their Modulation in Acute and Chronic Pain. Physiol. Rev. 2021, 101, 213–258. [Google Scholar] [CrossRef] [PubMed]
- Vartiainen, N.; Perchet, C.; Magnin, M.; Creac’h, C.; Convers, P.; Nighoghossian, N.; Mauguière, F.; Peyron, R.; Garcia-Larrea, L. Thalamic Pain: Anatomical and Physiological Indices of Prediction. Brain 2016, 139, 708–722. [Google Scholar] [CrossRef] [PubMed]
- Baron, R.; May, A. Headache and Pain; IASP: Washington, DC, USA, 2015; ISBN 978-1-4963-3205-9. [Google Scholar]
- Liebeskind, J.C.; Guilbaud, G.; Besson, J.-M.; Oliveras, J.-L. Analgesia from Electrical Stimulation of the Periaqueductal Gray Matter in the Cat: Behavioral Observations and Inhibitory Effects on Spinal Cord Interneurons. Brain Res. 1973, 50, 441–446. [Google Scholar] [CrossRef] [PubMed]
- Basbaum, A.I.; Fields, H.L. Endogenous Pain Control Mechanisms: Review and Hypothesis. Ann. Neurol. 1978, 4, 451–462. [Google Scholar] [CrossRef] [PubMed]
- Forni, M.; Thorbergsson, P.T.; Thelin, J.; Schouenborg, J. 3D Microelectrode Cluster and Stimulation Paradigm Yield Powerful Analgesia without Noticeable Adverse Effects. Sci. Adv. 2021, 7, eabj2847. [Google Scholar] [CrossRef] [PubMed]
- Millan, M.J. Descending Control of Pain. Prog. Neurobiol. 2002, 66, 355–474. [Google Scholar] [CrossRef]
- Bouali-Benazzouz, R.; Benazzouz, A. COVID-19 Infection and Parkinsonism: Is There a Link? Mov. Disord. 2021, 36, 1737–1743. [Google Scholar] [CrossRef]
- Zhang, H.; Lecker, I.; Collymore, C.; Dokova, A.; Pham, M.C.; Rosen, S.F.; Crawhall-Duk, H.; Zain, M.; Valencia, M.; Filippini, H.F.; et al. Cage-Lid Hanging Behavior as a Translationally Relevant Measure of Pain in Mice. Pain 2021, 162, 1416–1425. [Google Scholar] [CrossRef] [PubMed]
- Ferland, S.; Wang, F.; De Koninck, Y.; Ferrini, F. An Improved Conflict Avoidance Assay Reveals Modality-Specific Differences in Pain Hypersensitivity across Sexes. Pain 2024, 165, 1304–1316. [Google Scholar] [CrossRef] [PubMed]
- Dolensek, N.; Gehrlach, D.A.; Klein, A.S.; Gogolla, N. Facial Expressions of Emotion States and Their Neuronal Correlates in Mice. Science 2020, 368, 89–94. [Google Scholar] [CrossRef] [PubMed]
| Pain Component | Brain Area | Type of Stimulation | Method | Protocol | Pain Outcome | References |
|---|---|---|---|---|---|---|
| Sensory | S1 | Inhibition of excitatory neurons | Optogenetic ArchT | Continuous light | Mechanical hypersensitivity only with MCC stimulation | [38] |
| Inhibition of excitatory neurons | Optogenetic ArchT | Continuous (minutes) or intermittent light | Prevent Capsaicin hypersensitivity | [38] | ||
| Activation of L6 | Optogenetic ChR2 | Continuous 5 or 20 Hz | Mechanical hypersensitivity Aversive response | [37] | ||
| Activation of L5 | Optogenetic ChR2 | Continuous 5 s or 20 Hz | Reduce Mechanical sensitivity No Aversive response | [37] | ||
| Inhibition of L5 | Optogenetic stGtACR2 | Continuous 5 s or 20 Hz | Mechanical hypersensitivity | [37] | ||
| activation of PV neurons | Optogenetic ChR2 | 40 or 80 Hz | Mechanical hypersensitivity Aversive response | [36] | ||
| Thalamus | Activation MD-ACC | Optogenetic ChR2 | 20 Hz/5 ms | Light Aversion | [47] | |
| Inhibition MD-ACC | Optogenetic Arch | Continuous | Light Preference | [47] | ||
| Cognitive | Posterior Insula | Lesion of PI | Cell death | NA | Mechanical hypersensitivity | [39] |
| Activation of MCC-PI | Optogenetic ChR2 | 30 Hz | Mechanical hypersensitivity | [38] | ||
| Activation ACC-PI | Optogenetic ChR2 | 2 Hz/5 ms | Mechanical hypersensitivity | [41] | ||
| PFC | Activation of PFC-vlPAG | Optogenetic ChR2 | Continuous (minutes) | Mechanical and thermal analgesia in neuropathic pain model | [42] | |
| Inhibition of PFC-vlPAG | Optogenetic NpHR | Continuous (minutes) | Mechanical hypersensitivity in neuropathic pain | [42] | ||
| Activation of PFC PV Inhibition of PFC PV | Optogenetic ChR2 Optogenetic Arch3.0 | 40 Hz/10 ms Continuous | Hyperalgesia in neuropathic animals Analgesia in neuropathic animals | [43] | ||
| Activation of excitatory ensembles of PFC | Chemogenetic, HDM3q | CNO | Mechanical hypersensitivity | [44] | ||
| Orbitofrontal Cortex | Activation of glutamate neurons | Chemogenetic HDM3q | CNO | Mechanical analgesia in neuropathic pain | [48] | |
| Activation of excitatory neurons | Optogenetic ChR2 | 10 Hz | Mechanical analgesia in neuropathic pain | [48] | ||
| Emotional | ACC | Activation | Electrical stimulation | Mechanical hypersensitivity | [40] | |
| Activation of inhibitory neurons of ACC | Optogenetic ChR2 | 10 Hz/20 ms | Decrease spontaneous pain behaviour | [49] | ||
| Activation of ACC-SC | Optogenetic ChR2 | 20 Hz/40 ms | Mechanical hypersensitivity | [40] | ||
| Inhibition of ACC-SC | Optogenetic Arch | Continuous | Mechanical analgesia in neuropathic pain | [40] | ||
| Activation of ACC-PI | Optogenetic ChR2 | 2 Hz/5 ms | Mechanical and thermal hypersensitivity | [41] | ||
| Inhibition of ACC-PI | Optogenetic ArchT | Continuous | Mechanical and thermal analgesia | [41] | ||
| CeA | Activation of CeA-PAG | Not tested | Not tested | Thermal analgesia | [50] | |
| Activation of BLA to CeA | Optogenetic ChR2 | 20 Hz | Increase activity of spinal neuron | [51] | ||
| Inhibition of CeA output neurons | Optogenetic NpHR3.0 | Continuous | Decrease activity of spinal neurons | [51] | ||
| BLA | Inhibition of BLA | Chemogenetic | CNO | Place preference | [52] | |
| Activation of BLA to PFC | Optogenetic ChR2 | 10 Hz | Mechanical and thermal hyperalgesia in neuropathic pain | [42] | ||
| Inhibition of BLA to PFC | Optogenetic NpHR3.0 | Continuous | Mechanical and thermal analgesia | [42] | ||
| Activation of BLA to ACC | Optogenetic ChR2 | 20 Hz/5 ms | Place preference in neuropathic pain | [47] | ||
| Descending Pathways | PAG | vlPAG activation | Chemogenetic | CNO | Thermal analgesia | [53] |
| vlPAG inhibition | Chemogenetic | CNO | Mechanical and thermal hyperalgesia | [50] | ||
| vlPAG Glutamate neurons activation | Optogenetic ChR2 Chemogenetic | NA CNO | Mechanical and thermal analgesia | [50,53] | ||
| vlPAG GABA neurons activation | Chemogenetic | CNO | Mechanical and thermal hyperalgesia | [53] | ||
| vlPAG SST neurons | Chemogenetic | CNO | Mechanical and thermal hyperalgesia | [54] | ||
| vlPAG SST neurons activation | Optogenetic ChR2 | 2 Hz/5 ms | Increased activity of spinal neurons | [55] | ||
| vlPAG dopamine neurons activation | Chemogenetic | CNO | Mechanical and thermal analgesia | [56] | ||
| RVM | Activation of GABA neurons | Optogenetic ChR2 | 15 Hz | Mechanical hypersensitivity | [57] | |
| Activation of 5HT neurons | Optogenetic ChR2 chemogenetic | 5 Hz/5 ms CNO | Mechanical and thermal analgesia | [58,59] | ||
| Activation of 5HT neurons | Optogenetic ChR2 | 20 Hz/15 ms 5 Hz/5 ms | Mechanical and thermal hyperalgesia in neuropathic pain | [58,60] | ||
| LC | Activation of LC and LC to SC | Optogenetic ChR2 | 5 Hz/20 ms | Decreased spinal neuro response | [61] | |
| Dorsal LC | Optogenetic ChR2 | Continuous | Thermal analgesia/hyperalgesia | [62] | ||
| LC-SC | NA | NA | Hyperalgesia | [63] |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Viellard, J.; Bouali-Benazzouz, R.; Benazzouz, A.; Fossat, P. Modulating Neural Circuits of Pain in Preclinical Models: Recent Insights for Future Therapeutics. Cells 2024, 13, 997. https://doi.org/10.3390/cells13120997
Viellard J, Bouali-Benazzouz R, Benazzouz A, Fossat P. Modulating Neural Circuits of Pain in Preclinical Models: Recent Insights for Future Therapeutics. Cells. 2024; 13(12):997. https://doi.org/10.3390/cells13120997
Chicago/Turabian StyleViellard, Juliette, Rabia Bouali-Benazzouz, Abdelhamid Benazzouz, and Pascal Fossat. 2024. "Modulating Neural Circuits of Pain in Preclinical Models: Recent Insights for Future Therapeutics" Cells 13, no. 12: 997. https://doi.org/10.3390/cells13120997
APA StyleViellard, J., Bouali-Benazzouz, R., Benazzouz, A., & Fossat, P. (2024). Modulating Neural Circuits of Pain in Preclinical Models: Recent Insights for Future Therapeutics. Cells, 13(12), 997. https://doi.org/10.3390/cells13120997







