Recent Advances in Molecular and Genetic Research on Uveal Melanoma
Abstract
1. Introduction
2. Genetic Landscape of UM: Latest Findings
2.1. GNAQ/11 Mutations
2.2. CYSLTR2 Mutation
2.3. PLCβ4 Mutation
2.4. SF3B1 Mutations
2.5. SRSF2 Mutations
2.6. EIF1AX Mutations
2.7. BAP1 Mutations
2.8. MAPKAPK5 Mutations
2.9. Chromosomal Alterations
2.10. Latest Findings

3. Novel Biomarkers
3.1. Novel Biomarkers for Diagnosis
3.1.1. Circulating Tumor Cells (CTCs)
3.1.2. Circulating Tumor DNA (ctDNA)
3.1.3. Extracellular Vesicles (EVs)
3.1.4. Aqueous and Vitreous Humor Markers
3.1.5. miRNA Biomarkers
3.2. Novel Biomarkers for Prognosis and Personalized Therapies
4. Altered Molecular Mechanisms in UM
4.1. Metabolic Pathways
4.2. Autophagy and Mitophagy
4.3. mTOR and β-Catenin Signaling Pathways
4.4. Inflammatory Signaling Pathways
4.5. Gene Expression Pathways
4.6. Hypoxia
4.7. MAPK Pathway
4.8. JAK/STAT Pathway
4.9. Other Molecular Mechanisms
| Pathways/Mechanisms | Key Findings/Genes | Impact in UM | Risk Categories | References |
|---|---|---|---|---|
| Metabolic pathways | BAP1 mutations leading to OXPHOS gene set expression variations (GLUT3, HK1, CPT1A) | Alteration of cancer cell metabolism, contributing to therapeutic resistance | High-risk: OXPHOShigh Low-risk: OXPHOSlow | [152,156,157,158,159,160,161,162,163] |
| mTOR and β-catenin signaling pathways | CircRNA circ_0119872, FASN, ZNF704, SORBS3, LKB1 regulated by HGF | Regulation of cell growth, survival and differentiation | High-risk: associated with low survival | [177,178,179,180,181,182,183,184] |
| Inflammatory signaling pathways | IL6-JAK-STAT3, NF-κB (NFKB1), COX-2 (PTGS2), CXCL10, nine-gene inflammatory signature including ITGA5 and P2RX4 | Influence on immune microenvironment and tumor progression | High-risk: associated with poor prognosis Low-risk: ITGA5 and P2RX4 | [185,186,187,188,216] |
| Autophagy and mitophagy | Gene signatures related to autophagy and mitophagy; Autophagy-linked lncRNAs | Correlation with UM survival rates and molecular characteristics | High-risk: dysregulated autophagy genes | [168,169,170,171,172,191] |
| Gene expression pathways | BAP1, m6A RNA methylation, DNA methylation, EGFR resistance, histone PTMs | Effects on chromatin compaction, gene expression and resistance pathways | High-risk: abnormal DNA methylation and histone PTMs | [192,194,195,196] |
| Hypoxia | Hypoxia-regulated genes: P4HA1, P4HA2 | Association with metastasis, aggressive phenotypes, and poor outcomes | High-risk: hypoxic tumors | [197,199,200,201] |
| MAPK pathway | Activating mutations in GNAQ/11 STING high expression | Activation of MAPK pathway, driving UM progression Enhancement of UM cell invasion and migration; increase of the activity of p38-MAPK signaling | High-risk: activated MAPK pathway | [42,204] |
| JAK/STAT pathway | HTR2B, IL6/JAK/STAT3 and related pathways | Aberrant activation linked to increased tumor growth and malignancy | High-risk: dysregulated JAK/STAT pathway | [206,207] |
| Other molecular mechanisms | HDAC7, KIT, PDCD2L, HES6, NRP1, EMT factors | Various roles in proliferation, metastasis, and survival | High-risk: overexpression of HDAC7, KIT, PDCD2L, NRP1 | [208,209,210,211] |
5. Immune Microenvironment
5.1. Gene Expression and Immune Responses
5.2. TILs in High-Risk UMs
5.3. Immune Subtypes (IS) and Their Prognostic Significance
6. Current and Emerging Therapeutics
6.1. Histone Deacetylase Inhibitors (HDACi)
6.2. MAPK Signaling Pathway Inhibitors
6.3. Hippo/YAP Pathway Inhibitors
6.4. Advanced Drug Delivery Systems
6.5. Emerging Approaches
6.5.1. BAP1-defective Cancers
6.5.2. CAR T-Cell Therapy (Reviewed in [283])
6.5.3. Human Endogenous Retroviruses (HERVs)
| Therapeutic Strategies | Advantages | Disadvantages | References |
|---|---|---|---|
| Histone deacetylase inhibitors | Target epigenetic regulation Enhance immune response Synergistic potential with other treatments Specific HDAC targeting | Variable efficacy Side effects and toxicity Potential for resistance development Limited long-term data Cost and accessibility | [251,253,254,255,257] |
| MAPK signaling pathway inhibitors | Targeted action against a crucial signaling pathway Clinical trials ongoing Tested in combination therapies | Limited efficacy shown so far Potential adverse effects Ongoing research needed for conclusive results | [259,260,261] |
| Hippo/YAP pathway inhibitors | Novel target for treatment Demonstrates synergistic effects with other therapies Promising preclinical results | Early-stage research Complex pathway interactions may complicate treatment Specificity and toxicity concerns | [270,271] |
| Advanced drug delivery systems | Enhanced targeting of tumor cells Innovative delivery techniques like nanoparticles and radioembolization Potential combination with immunotherapy | High complexity and cost Significant regulatory hurdles Limited data on long-term efficacy and safety | [274,277] |
| Emerging approaches | BAP1-defective cancers: Targeting with BET inhibitors shows high specificity CAR T-cell therapy: Effective in preclinical models, promising for checkpoint-resistant melanomas Human endogenous retroviruses (HERVs): Potential new targets for low-mutational cancers | BAP1-defective cancers: High metastatic risk and lower survival rates CAR T-cell therapy: Early-stage clinical trials, results pending; HLA downregulation or loss on cancer cells can limit the therapy effectiveness Human endogenous retroviruses (HERVs): Need more research to confirm clinical relevance | [282,283,284,285,286,287,288] |
7. Challenges and Future Directions
7.1. Development of Models for Preclinical Studies and Personalized Therapies
7.2. Limited Treatment Options for MUM
7.3. Identification of Novel Therapeutic Targets
7.4. Improved Diagnostic and Prognostic Tools
7.5. Exploration of Immunotherapeutic Approaches
7.6. Identification of Prognostic Biomarkers and Therapy Responses
7.7. Intraoperative Imaging and Surgical Techniques
7.8. Evaluating the Relationship between the Microbiome and the Immunotherapy Response
7.9. Advancing the Development of Oncolytic Viruses
7.10. Employing Artificial Intelligence (AI) in the Prognostic Analysis
8. Conclusions
Author Contributions
Funding
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Singh, S.R.K.; Malapati, S.J.; Kumar, R.; Willner, C.; Wang, D. NCDB Analysis of Melanoma 2004–2015: Epidemiology and Outcomes by Subtype, Sociodemographic Factors Impacting Clinical Presentation, and Real-World Survival Benefit of Immunotherapy Approval. Cancers 2021, 13, 1455. [Google Scholar] [CrossRef]
- Rodriguez, D.A.; Sanchez, M.I.; Decatur, C.L.; Correa, Z.M.; Martin, E.R.; Harbour, J.W. Impact of Genetic Ancestry on Prognostic Biomarkers in Uveal Melanoma. Cancers 2020, 12, 3208. [Google Scholar] [CrossRef] [PubMed]
- Jager, M.J.; Shields, C.L.; Cebulla, C.M.; Abdel-Rahman, M.H.; Grossniklaus, H.E.; Stern, M.-H.; Carvajal, R.D.; Belfort, R.N.; Jia, R.; Shields, J.A.; et al. Uveal Melanoma. Nat. Rev. Dis. Primers 2020, 6, 24. [Google Scholar] [CrossRef]
- Carvajal, R.D.; Sacco, J.J.; Jager, M.J.; Eschelman, D.J.; Olofsson Bagge, R.; Harbour, J.W.; Chieng, N.D.; Patel, S.P.; Joshua, A.M.; Piperno-Neumann, S. Advances in the Clinical Management of Uveal Melanoma. Nat. Rev. Clin. Oncol. 2023, 20, 99–115. [Google Scholar] [CrossRef]
- Bustamante, P.; Piquet, L.; Landreville, S.; Burnier, J.V. Uveal Melanoma Pathobiology: Metastasis to the Liver. Semin. Cancer Biol. 2021, 71, 65–85. [Google Scholar] [CrossRef] [PubMed]
- Harbour, J.W. The Genetics of Uveal Melanoma: An Emerging Framework for Targeted Therapy. Pigment. Cell Melanoma Res. 2012, 25, 171–181. [Google Scholar] [CrossRef]
- Kaliki, S.; Shields, C.L. Uveal Melanoma: Relatively Rare but Deadly Cancer. Eye 2017, 31, 241–257. [Google Scholar] [CrossRef]
- Rantala, E.S.; Hernberg, M.M.; Piperno-Neumann, S.; Grossniklaus, H.E.; Kivelä, T.T. Metastatic Uveal Melanoma: The Final Frontier. Prog. Retin. Eye Res. 2022, 90, 101041. [Google Scholar] [CrossRef] [PubMed]
- Shao, F.; Pang, X.; Baeg, G.H. Targeting the JAK/STAT Signaling Pathway for Breast Cancer. Curr. Med. Chem. 2021, 28, 5137–5151. [Google Scholar] [CrossRef]
- Zhang, S.; Yang, G. IL22RA1/JAK/STAT Signaling Acts as a Cancer Target Through Pan-Cancer Analysis. Front. Immunol. 2022, 13, 915246. [Google Scholar] [CrossRef]
- Popova, N.V.; Jücker, M. The Role of mTOR Signaling as a Therapeutic Target in Cancer. Int. J. Mol. Sci. 2021, 22, 1743. [Google Scholar] [CrossRef] [PubMed]
- Parsons, M.J.; Tammela, T.; Dow, L.E. WNT as a Driver and Dependency in Cancer. Cancer Discov. 2021, 11, 2413–2429. [Google Scholar] [CrossRef] [PubMed]
- Yu, L.; Wei, J.; Liu, P. Attacking the PI3K/Akt/mTOR Signaling Pathway for Targeted Therapeutic Treatment in Human Cancer. Semin. Cancer Biol. 2022, 85, 69–94. [Google Scholar] [CrossRef] [PubMed]
- Robertson, A.G.; Shih, J.; Yau, C.; Gibb, E.A.; Oba, J.; Mungall, K.L.; Hess, J.M.; Uzunangelov, V.; Walter, V.; Danilova, L.; et al. Integrative Analysis Identifies Four Molecular and Clinical Subsets in Uveal Melanoma. Cancer Cell 2017, 32, 204–220.e15. [Google Scholar] [CrossRef] [PubMed]
- Algazi, A.P.; Tsai, K.K.; Shoushtari, A.N.; Munhoz, R.R.; Eroglu, Z.; Piulats, J.M.; Ott, P.A.; Johnson, D.B.; Hwang, J.; Daud, A.I.; et al. Clinical Outcomes in Metastatic Uveal Melanoma Treated with PD-1 and PD-L1 Antibodies. Cancer 2016, 122, 3344–3353. [Google Scholar] [CrossRef] [PubMed]
- Rossi, E.; Pagliara, M.M.; Orteschi, D.; Dosa, T.; Sammarco, M.G.; Caputo, C.G.; Petrone, G.; Rindi, G.; Zollino, M.; Blasi, M.A.; et al. Pembrolizumab as First-Line Treatment for Metastatic Uveal Melanoma. Cancer Immunol. Immunother. 2019, 68, 1179–1185. [Google Scholar] [CrossRef] [PubMed]
- Klemen, N.D.; Wang, M.; Rubinstein, J.C.; Olino, K.; Clune, J.; Ariyan, S.; Cha, C.; Weiss, S.A.; Kluger, H.M.; Sznol, M. Survival after Checkpoint Inhibitors for Metastatic Acral, Mucosal and Uveal Melanoma. J. Immunother. Cancer 2020, 8, e000341. [Google Scholar] [CrossRef] [PubMed]
- Hu, D.-N.; Yu, G.-P.; McCormick, S.A.; Schneider, S.; Finger, P.T. Population-Based Incidence of Uveal Melanoma in Various Races and Ethnic Groups. Am. J. Ophthalmol. 2005, 140, 612–617. [Google Scholar] [CrossRef] [PubMed]
- Weis, E.; Shah, C.P.; Lajous, M.; Shields, J.A.; Shields, C.L. The Association between Host Susceptibility Factors and Uveal Melanoma: A Meta-Analysis. Arch. Ophthalmol. 2006, 124, 54–60. [Google Scholar] [CrossRef]
- Murali, R.; Wiesner, T.; Scolyer, R.A. Tumours Associated with BAP1 Mutations. Pathology 2013, 45, 116–126. [Google Scholar] [CrossRef]
- Shields, C.L.; Kaliki, S.; Cohen, M.N.; Shields, P.W.; Furuta, M.; Shields, J.A. Prognosis of Uveal Melanoma Based on Race in 8100 Patients: The 2015 Doyne Lecture. Eye 2015, 29, 1027–1035. [Google Scholar] [CrossRef] [PubMed]
- Walpole, S.; Pritchard, A.L.; Cebulla, C.M.; Pilarski, R.; Stautberg, M.; Davidorf, F.H.; de la Fouchardière, A.; Cabaret, O.; Golmard, L.; Stoppa-Lyonnet, D.; et al. Comprehensive Study of the Clinical Phenotype of Germline BAP1 Variant-Carrying Families Worldwide. J. Natl. Cancer Inst. 2018, 110, 1328–1341. [Google Scholar] [CrossRef] [PubMed]
- Lawrence, M.S.; Stojanov, P.; Polak, P.; Kryukov, G.V.; Cibulskis, K.; Sivachenko, A.; Carter, S.L.; Stewart, C.; Mermel, C.H.; Roberts, S.A.; et al. Mutational Heterogeneity in Cancer and the Search for New Cancer-Associated Genes. Nature 2013, 499, 214–218. [Google Scholar] [CrossRef] [PubMed]
- Royer-Bertrand, B.; Torsello, M.; Rimoldi, D.; El Zaoui, I.; Cisarova, K.; Pescini-Gobert, R.; Raynaud, F.; Zografos, L.; Schalenbourg, A.; Speiser, D.; et al. Comprehensive Genetic Landscape of Uveal Melanoma by Whole-Genome Sequencing. Am. J. Hum. Genet. 2016, 99, 1190–1198. [Google Scholar] [CrossRef] [PubMed]
- Chalmers, Z.R.; Connelly, C.F.; Fabrizio, D.; Gay, L.; Ali, S.M.; Ennis, R.; Schrock, A.; Campbell, B.; Shlien, A.; Chmielecki, J.; et al. Analysis of 100,000 Human Cancer Genomes Reveals the Landscape of Tumor Mutational Burden. Genome Med. 2017, 9, 34. [Google Scholar] [CrossRef] [PubMed]
- Kwon, J.; Lee, D.; Lee, S.-A. BAP1 as a Guardian of Genome Stability: Implications in Human Cancer. Exp. Mol. Med. 2023, 55, 745–754. [Google Scholar] [CrossRef] [PubMed]
- Cohen, Y.; Goldenberg-Cohen, N.; Parrella, P.; Chowers, I.; Merbs, S.L.; Pe’er, J.; Sidransky, D. Lack of BRAF Mutation in Primary Uveal Melanoma. Investig. Ophthalmol. Vis. Sci. 2003, 44, 2876–2878. [Google Scholar] [CrossRef]
- Cruz, F.; Rubin, B.P.; Wilson, D.; Town, A.; Schroeder, A.; Haley, A.; Bainbridge, T.; Heinrich, M.C.; Corless, C.L. Absence of BRAF and NRAS Mutations in Uveal Melanoma. Cancer Res. 2003, 63, 5761–5766. [Google Scholar]
- Janssen, C.S.; Sibbett, R.; Henriquez, F.L.; McKay, I.C.; Kemp, E.G.; Roberts, F. The T1799A Point Mutation Is Present in Posterior Uveal Melanoma. Br. J. Cancer 2008, 99, 1673–1677. [Google Scholar] [CrossRef]
- Midena, E.; Bonaldi, L.; Parrozzani, R.; Tebaldi, E.; Boccassini, B.; Vujosevic, S. In Vivo Detection of Monosomy 3 in Eyes with Medium-Sized Uveal Melanoma Using Transscleral Fine Needle Aspiration Biopsy. Eur. J. Ophthalmol. 2006, 16, 422–425. [Google Scholar] [CrossRef]
- Bonaldi, L.; Midena, E.; Filippi, B.; Tebaldi, E.; Marcato, R.; Parrozzani, R.; Amadori, A. FISH Analysis of Chromosomes 3 and 6 on Fine Needle Aspiration Biopsy Samples Identifies Distinct Subgroups of Uveal Melanomas. J. Cancer Res. Clin. Oncol. 2008, 134, 1123–1127. [Google Scholar] [CrossRef] [PubMed]
- Shields, C.L.; Say, E.A.T.; Hasanreisoglu, M.; Saktanasate, J.; Lawson, B.M.; Landy, J.E.; Badami, A.U.; Sivalingam, M.D.; Hauschild, A.J.; House, R.J.; et al. Personalized Prognosis of Uveal Melanoma Based on Cytogenetic Profile in 1059 Patients over an 8-Year Period: The 2017 Harry S. Gradle Lecture. Ophthalmology 2017, 124, 1523–1531. [Google Scholar] [CrossRef] [PubMed]
- Demirci, H.; Niziol, L.M.; Ozkurt, Z.; Slimani, N.; Ozgonul, C.; Liu, T.; Musch, D.C.; Materin, M. Do Largest Basal Tumor Diameter and the American Joint Committee on Cancer’s Cancer Staging Influence Prognostication by Gene Expression Profiling in Choroidal Melanoma. Am. J. Ophthalmol. 2018, 195, 83–92. [Google Scholar] [CrossRef] [PubMed]
- Harbour, J.W.; Chao, D.L. A Molecular Revolution in Uveal Melanoma: Implications for Patient Care and Targeted Therapy. Ophthalmology 2014, 121, 1281–1288. [Google Scholar] [CrossRef] [PubMed]
- Jager, M.J.; Brouwer, N.J.; Esmaeli, B. The Cancer Genome Atlas Project: An Integrated Molecular View of Uveal Melanoma. Ophthalmology 2018, 125, 1139–1142. [Google Scholar] [CrossRef] [PubMed]
- Bakhoum, M.F.; Esmaeli, B. Molecular Characteristics of Uveal Melanoma: Insights from the Cancer Genome Atlas (TCGA) Project. Cancers 2019, 11, 1061. [Google Scholar] [CrossRef] [PubMed]
- Van Raamsdonk, C.D.; Bezrookove, V.; Green, G.; Bauer, J.; Gaugler, L.; O’Brien, J.M.; Simpson, E.M.; Barsh, G.S.; Bastian, B.C. Frequent Somatic Mutations of GNAQ in Uveal Melanoma and Blue Naevi. Nature 2009, 457, 599–602. [Google Scholar] [CrossRef] [PubMed]
- Van Raamsdonk, C.D.; Griewank, K.G.; Crosby, M.B.; Garrido, M.C.; Vemula, S.; Wiesner, T.; Obenauf, A.C.; Wackernagel, W.; Green, G.; Bouvier, N.; et al. Mutations in GNA11 in Uveal Melanoma. N. Engl. J. Med. 2010, 363, 2191–2199. [Google Scholar] [CrossRef]
- Goldsmith, Z.G.; Dhanasekaran, D.N. G Protein Regulation of MAPK Networks. Oncogene 2007, 26, 3122–3142. [Google Scholar] [CrossRef]
- Field, M.G.; Harbour, J.W. Recent Developments in Prognostic and Predictive Testing in Uveal Melanoma. Curr. Opin. Ophthalmol. 2014, 25, 234–239. [Google Scholar] [CrossRef]
- Chen, X.; Wu, Q.; Tan, L.; Porter, D.; Jager, M.J.; Emery, C.; Bastian, B.C. Combined PKC and MEK Inhibition in Uveal Melanoma with GNAQ and GNA11 Mutations. Oncogene 2014, 33, 4724–4734. [Google Scholar] [CrossRef] [PubMed]
- Ma, J.; Weng, L.; Bastian, B.C.; Chen, X. Functional Characterization of Uveal Melanoma Oncogenes. Oncogene 2021, 40, 806–820. [Google Scholar] [CrossRef] [PubMed]
- Hitchman, T.D.; Bayshtok, G.; Ceraudo, E.; Moore, A.R.; Lee, C.; Jia, R.; Wang, N.; Pachai, M.R.; Shoushtari, A.N.; Francis, J.H.; et al. Combined Inhibition of Gαq and MEK Enhances Therapeutic Efficacy in Uveal Melanoma. Clin. Cancer Res. 2021, 27, 1476–1490. [Google Scholar] [CrossRef] [PubMed]
- Taylor, V.G.; Bommarito, P.A.; Tesmer, J.J.G. Structure of the Regulator of G Protein Signaling 8 (RGS8)-Gαq Complex: Molecular Basis for Gα Selectivity. J. Biol. Chem. 2016, 291, 5138–5145. [Google Scholar] [CrossRef] [PubMed]
- Hewitt, N.; Ma, N.; Arang, N.; Martin, S.A.; Prakash, A.; DiBerto, J.F.; Knight, K.M.; Ghosh, S.; Olsen, R.H.J.; Roth, B.L.; et al. Catalytic Site Mutations Confer Multiple States of G Protein Activation. Sci. Signal. 2023, 16, eabq7842. [Google Scholar] [CrossRef] [PubMed]
- Liang, C.; Peng, L.Y.; Zou, M.; Chen, X.; Chen, Y.; Chen, H.; Xiao, L.; Yan, N.; Zhang, J.; Zhao, Q.; et al. Heterogeneity of GNAQ/11 Mutation Inversely Correlates with the Metastatic Rate in Uveal Melanoma. Br. J. Ophthalmol. 2021, 105, 587–592. [Google Scholar] [CrossRef] [PubMed]
- Moore, A.R.; Ceraudo, E.; Sher, J.J.; Guan, Y.; Shoushtari, A.N.; Chang, M.T.; Zhang, J.Q.; Walczak, E.G.; Kazmi, M.A.; Taylor, B.S.; et al. Recurrent Activating Mutations of G-Protein-Coupled Receptor CYSLTR2 in Uveal Melanoma. Nat. Genet. 2016, 48, 675–680. [Google Scholar] [CrossRef] [PubMed]
- Nell, R.J.; Menger, N.V.; Versluis, M.; Luyten, G.P.M.; Verdijk, R.M.; Madigan, M.C.; Jager, M.J.; van der Velden, P.A. Involvement of Mutant and Wild-Type CYSLTR2 in the Development and Progression of Uveal Nevi and Melanoma. BMC Cancer 2021, 21, 164. [Google Scholar] [CrossRef] [PubMed]
- Johansson, P.; Aoude, L.G.; Wadt, K.; Glasson, W.J.; Warrier, S.K.; Hewitt, A.W.; Kiilgaard, J.F.; Heegaard, S.; Isaacs, T.; Franchina, M.; et al. Deep Sequencing of Uveal Melanoma Identifies a Recurrent Mutation in PLCB4. Oncotarget 2016, 7, 4624–4631. [Google Scholar] [CrossRef]
- Phan, H.T.N.; Kim, N.H.; Wei, W.; Tall, G.G.; Smrcka, A.V. Uveal Melanoma-Associated Mutations in PLCβ4 Are Constitutively Activating and Promote Melanocyte Proliferation and Tumorigenesis. Sci. Signal. 2021, 14, eabj4243. [Google Scholar] [CrossRef]
- Moore, A.R.; Ran, L.; Guan, Y.; Sher, J.J.; Hitchman, T.D.; Zhang, J.Q.; Hwang, C.; Walzak, E.G.; Shoushtari, A.N.; Monette, S.; et al. GNA11 Q209L Mouse Model Reveals RasGRP3 as an Essential Signaling Node in Uveal Melanoma. Cell Rep. 2018, 22, 2455–2468. [Google Scholar] [CrossRef] [PubMed]
- Chen, X.; Wu, Q.; Depeille, P.; Chen, P.; Thornton, S.; Kalirai, H.; Coupland, S.E.; Roose, J.P.; Bastian, B.C. RasGRP3 Mediates MAPK Pathway Activation in GNAQ Mutant Uveal Melanoma. Cancer Cell 2017, 31, 685–696.e6. [Google Scholar] [CrossRef] [PubMed]
- Phelps, G.B.; Hagen, H.R.; Amsterdam, A.; Lees, J.A. MITF Deficiency Accelerates GNAQ-Driven Uveal Melanoma. Proc. Natl. Acad. Sci. USA 2022, 119, e2107006119. [Google Scholar] [CrossRef] [PubMed]
- Martin, M.; Maßhöfer, L.; Temming, P.; Rahmann, S.; Metz, C.; Bornfeld, N.; van de Nes, J.; Klein-Hitpass, L.; Hinnebusch, A.G.; Horsthemke, B.; et al. Exome Sequencing Identifies Recurrent Somatic Mutations in EIF1AX and SF3B1 in Uveal Melanoma with Disomy 3. Nat. Genet. 2013, 45, 933–936. [Google Scholar] [CrossRef] [PubMed]
- Harbour, J.W.; Roberson, E.D.O.; Anbunathan, H.; Onken, M.D.; Worley, L.A.; Bowcock, A.M. Recurrent Mutations at Codon 625 of the Splicing Factor SF3B1 in Uveal Melanoma. Nat. Genet. 2013, 45, 133–135. [Google Scholar] [CrossRef] [PubMed]
- Tate, J.G.; Bamford, S.; Jubb, H.C.; Sondka, Z.; Beare, D.M.; Bindal, N.; Boutselakis, H.; Cole, C.G.; Creatore, C.; Dawson, E.; et al. COSMIC: The Catalogue of Somatic Mutations in Cancer. Nucleic Acids Res. 2019, 47, D941–D947. [Google Scholar] [CrossRef] [PubMed]
- Darman, R.B.; Seiler, M.; Agrawal, A.A.; Lim, K.H.; Peng, S.; Aird, D.; Bailey, S.L.; Bhavsar, E.B.; Chan, B.; Colla, S.; et al. Cancer-Associated SF3B1 Hotspot Mutations Induce Cryptic 3′ Splice Site Selection through Use of a Different Branch Point. Cell Rep. 2015, 13, 1033–1045. [Google Scholar] [CrossRef] [PubMed]
- Drabarek, W.; van Riet, J.; Nguyen, J.Q.N.; Smit, K.N.; van Poppelen, N.M.; Jansen, R.; Medico-Salsench, E.; Vaarwater, J.; Magielsen, F.J.; Brands, T.; et al. Identification of Early-Onset Metastasis in SF3B1 Mutated Uveal Melanoma. Cancers 2022, 14, 846. [Google Scholar] [CrossRef] [PubMed]
- Yu, L.; Zhou, D.; Zhang, G.; Ren, Z.; Luo, X.; Liu, P.; Plouffe, S.W.; Meng, Z.; Moroishi, T.; Li, Y.; et al. Co-Occurrence of BAP1 and SF3B1 Mutations in Uveal Melanoma Induces Cellular Senescence. Mol. Oncol. 2022, 16, 607–629. [Google Scholar] [CrossRef]
- Bigot, J.; Lalanne, A.I.; Lucibello, F.; Gueguen, P.; Houy, A.; Dayot, S.; Ganier, O.; Gilet, J.; Tosello, J.; Nemati, F.; et al. Splicing Patterns in SF3B1-Mutated Uveal Melanoma Generate Shared Immunogenic Tumor-Specific Neoepitopes. Cancer Discov. 2021, 11, 1938–1951. [Google Scholar] [CrossRef]
- Yao, T.; Zhang, Z.; Li, Q.; Huang, R.; Hong, Y.; Li, C.; Zhang, F.; Huang, Y.; Fang, Y.; Cao, Q.; et al. Long-Read Sequencing Reveals Alternative Splicing-Driven, Shared Immunogenic Neoepitopes Regardless SF3B1 Status in Uveal Melanoma. Cancer Immunol. Res. 2023, 11, 1671–1687. [Google Scholar] [CrossRef] [PubMed]
- Zhang, S.; Mao, M.; Lv, Y.; Yang, Y.; He, W.; Song, Y.; Wang, Y.; Yang, Y.; Al Abo, M.; Freedman, J.A.; et al. A Widespread Length-Dependent Splicing Dysregulation in Cancer. Sci. Adv. 2022, 8, eabn9232. [Google Scholar] [CrossRef] [PubMed]
- Field, M.G.; Durante, M.A.; Anbunathan, H.; Cai, L.Z.; Decatur, C.L.; Bowcock, A.M.; Kurtenbach, S.; Harbour, J.W. Punctuated Evolution of Canonical Genomic Aberrations in Uveal Melanoma. Nat. Commun. 2018, 9, 116. [Google Scholar] [CrossRef] [PubMed]
- van Poppelen, N.M.; Drabarek, W.; Smit, K.N.; Vaarwater, J.; Brands, T.; Paridaens, D.; Kiliç, E.; de Klein, A. SRSF2 Mutations in Uveal Melanoma: A Preference for In-Frame Deletions? Cancers 2019, 11, 1200. [Google Scholar] [CrossRef]
- Seiler, M.; Peng, S.; Agrawal, A.A.; Palacino, J.; Teng, T.; Zhu, P.; Smith, P.G.; Cancer Genome Atlas Research Network; Buonamici, S.; Yu, L. Somatic Mutational Landscape of Splicing Factor Genes and Their Functional Consequences across 33 Cancer Types. Cell Rep. 2018, 23, 282–296.e4. [Google Scholar] [CrossRef] [PubMed]
- Akin-Bali, D.F. Bioinformatics Analysis of GNAQ, GNA11, BAP1, SF3B1, SRSF2, EIF1AX, PLCB4, and CYSLTR2 Genes and Their Role in the Pathogenesis of Uveal Melanoma. Ophthalmic Genet. 2021, 42, 732–743. [Google Scholar] [CrossRef] [PubMed]
- Öther-Gee Pohl, S.; Myant, K.B. Alternative RNA Splicing in Tumour Heterogeneity, Plasticity and Therapy. Dis. Model. Mech. 2022, 15, dmm049233. [Google Scholar] [CrossRef] [PubMed]
- Chaudhuri, J.; Si, K.; Maitra, U. Function of Eukaryotic Translation Initiation Factor 1A (eIF1A) (Formerly Called eIF-4C) in Initiation of Protein Synthesis. J. Biol. Chem. 1997, 272, 7883–7891. [Google Scholar] [CrossRef] [PubMed]
- Krishnamoorthy, G.P.; Davidson, N.R.; Leach, S.D.; Zhao, Z.; Lowe, S.W.; Lee, G.; Landa, I.; Nagarajah, J.; Saqcena, M.; Singh, K.; et al. EIF1AX and RAS Mutations Cooperate to Drive Thyroid Tumorigenesis through ATF4 and C-MYC. Cancer Discov. 2019, 9, 264–281. [Google Scholar] [CrossRef] [PubMed]
- Barbagallo, C.; Stella, M.; Broggi, G.; Russo, A.; Caltabiano, R.; Ragusa, M. Genetics and RNA Regulation of Uveal Melanoma. Cancers 2023, 15, 775. [Google Scholar] [CrossRef]
- Masoomian, B.; Shields, J.A.; Shields, C.L. Overview of BAP1 Cancer Predisposition Syndrome and the Relationship to Uveal Melanoma. J. Curr. Ophthalmol. 2018, 30, 102–109. [Google Scholar] [CrossRef] [PubMed]
- Campagne, A.; Lee, M.-K.; Zielinski, D.; Michaud, A.; Le Corre, S.; Dingli, F.; Chen, H.; Shahidian, L.Z.; Vassilev, I.; Servant, N.; et al. BAP1 Complex Promotes Transcription by Opposing PRC1-Mediated H2A Ubiquitylation. Nat. Commun. 2019, 10, 348. [Google Scholar] [CrossRef] [PubMed]
- Harbour, J.W.; Onken, M.D.; Roberson, E.D.O.; Duan, S.; Cao, L.; Worley, L.A.; Council, M.L.; Matatall, K.A.; Helms, C.; Bowcock, A.M. Frequent Mutation of BAP1 in Metastasizing Uveal Melanomas. Science 2010, 330, 1410–1413. [Google Scholar] [CrossRef] [PubMed]
- Matatall, K.A.; Agapova, O.A.; Onken, M.D.; Worley, L.A.; Bowcock, A.M.; Harbour, J.W. BAP1 Deficiency Causes Loss of Melanocytic Cell Identity in Uveal Melanoma. BMC Cancer 2013, 13, 371. [Google Scholar] [CrossRef] [PubMed]
- Rambow, F.; Rogiers, A.; Marin-Bejar, O.; Aibar, S.; Femel, J.; Dewaele, M.; Karras, P.; Brown, D.; Chang, Y.H.; Debiec-Rychter, M.; et al. Toward Minimal Residual Disease-Directed Therapy in Melanoma. Cell 2018, 174, 843–855.e19. [Google Scholar] [CrossRef] [PubMed]
- Djulbegovic, M.B.; Taylor, D.J.; Uversky, V.N.; Galor, A.; Shields, C.L.; Karp, C.L. Intrinsic Disorder in BAP1 and Its Association with Uveal Melanoma. Genes. 2022, 13, 1703. [Google Scholar] [CrossRef]
- Soltysova, A.; Dvorska, D.; Kajabova, V.H.; Pecimonova, M.; Cepcekova, K.; Ficek, A.; Demkova, L.; Buocikova, V.; Babal, P.; Juras, I.; et al. Uncovering Accurate Prognostic Markers for High-Risk Uveal Melanoma through DNA Methylation Profiling. Clin. Transl. Med. 2023, 13, e1317. [Google Scholar] [CrossRef] [PubMed]
- Cargnello, M.; Roux, P.P. Activation and Function of the MAPKs and Their Substrates, the MAPK-Activated Protein Kinases. Microbiol. Mol. Biol. Rev. 2011, 75, 50–83. [Google Scholar] [CrossRef]
- Lalonde, E.; Ewens, K.; Richards-Yutz, J.; Ebrahimzedeh, J.; Terai, M.; Gonsalves, C.F.; Sato, T.; Shields, C.L.; Ganguly, A. Improved Uveal Melanoma Copy Number Subtypes Including an Ultra-High-Risk Group. Ophthalmol. Sci. 2022, 2, 100121. [Google Scholar] [CrossRef]
- Ewens, K.G.; Kanetsky, P.A.; Richards-Yutz, J.; Al-Dahmash, S.; De Luca, M.C.; Bianciotto, C.G.; Shields, C.L.; Ganguly, A. Genomic Profile of 320 Uveal Melanoma Cases: Chromosome 8p-Loss and Metastatic Outcome. Investig. Ophthalmol. Vis. Sci. 2013, 54, 5721–5729. [Google Scholar] [CrossRef]
- Chao, A.-N.; Rose, K.; Racher, H.; Altomare, F.; Krema, H. Cytogenetic Abnormalities for Predicting the Risk of Metastases in Choroidal and Ciliary Body Melanoma. Investig. Ophthalmol. Vis. Sci. 2023, 64, 15. [Google Scholar] [CrossRef] [PubMed]
- Solomon, D.A.; Ramani, B.; Eiger-Moscovich, M.; Milman, T.; Uludag, G.; Crawford, J.B.; Phan, I.; Char, D.H.; Shields, C.L.; Eagle, R.C.; et al. Iris and Ciliary Body Melanocytomas Are Defined by Solitary GNAQ Mutation Without Additional Oncogenic Alterations. Ophthalmology 2022, 129, 1429–1439. [Google Scholar] [CrossRef] [PubMed]
- Mukhana, L.; Aissa, A.A.; Ahmed, A.a.M.; Saakyan, S.V.; Tsygankov, A.Y.; Blagonravov, M.L.; Azova, M.M. Association of BARD1 and BRIP1 Gene Polymorphisms with the Risk of Uveal Melanoma. Bull. Exp. Biol. Med. 2023, 175, 399–403. [Google Scholar] [CrossRef] [PubMed]
- Ahmad, T.R.; Pekmezci, M.; Bloomer, M.M.; Grenert, J.P.; Afshar, A.R. Next-Generation Sequencing of a Large Uveal Melanoma with Whole Genome Doubling and a PBRM1 Mutation. Am. J. Ophthalmol. Case Rep. 2023, 31, 101861. [Google Scholar] [CrossRef] [PubMed]
- Lee, W.S.; Lee, J.; Choi, J.J.; Kang, H.G.; Lee, S.C.; Kim, J.H. Paired Comparisons of Mutational Profiles before and after Brachytherapy in Asian Uveal Melanoma Patients. Sci. Rep. 2021, 11, 18594. [Google Scholar] [CrossRef]
- Abdel-Rahman, M.H.; Sample, K.M.; Pilarski, R.; Walsh, T.; Grosel, T.; Kinnamon, D.; Boru, G.; Massengill, J.B.; Schoenfield, L.; Kelly, B.; et al. Whole Exome Sequencing Identifies Candidate Genes Associated with Hereditary Predisposition to Uveal Melanoma. Ophthalmology 2020, 127, 668–678. [Google Scholar] [CrossRef]
- Pérez-Pérez, M.; Agostino, A.; De Sola-Llamas, C.G.; Ruvolo, M.; Vilches-Arenas, A.; Relimpio-López, M.I.; Espejo-Arjona, F.; Macías-García, L.; De Miguel-Rodríguez, M.; García-Escudero, A.; et al. Next-generation Sequencing of Uveal Melanoma with Clinical and Histological Correlations: Prognostic Value of New Mutations in the PI3K/AKT/mTOR Pathway. Clin. Exper Ophthalmol. 2023, 51, 822–834. [Google Scholar] [CrossRef] [PubMed]
- American Joint Committee on Cancer. AJCC Cancer Staging Manual, 8th ed.; Amin, M.B., Greene, F.L., Edge, S.B., Eds.; corrected at 3rd printing; AJCC, American Joint Committee on Cancer: Chicago, IL, USA, 2017; ISBN 978-3-319-40617-6. [Google Scholar]
- Chen, M.; Zhao, H. Next-Generation Sequencing in Liquid Biopsy: Cancer Screening and Early Detection. Hum. Genom. 2019, 13, 34. [Google Scholar] [CrossRef] [PubMed]
- Lone, S.N.; Nisar, S.; Masoodi, T.; Singh, M.; Rizwan, A.; Hashem, S.; El-Rifai, W.; Bedognetti, D.; Batra, S.K.; Haris, M.; et al. Liquid Biopsy: A Step Closer to Transform Diagnosis, Prognosis and Future of Cancer Treatments. Mol. Cancer 2022, 21, 79. [Google Scholar] [CrossRef]
- Nikanjam, M.; Kato, S.; Kurzrock, R. Liquid Biopsy: Current Technology and Clinical Applications. J. Hematol. Oncol. 2022, 15, 131. [Google Scholar] [CrossRef]
- Yu, D.; Li, Y.; Wang, M.; Gu, J.; Xu, W.; Cai, H.; Fang, X.; Zhang, X. Exosomes as a New Frontier of Cancer Liquid Biopsy. Mol. Cancer 2022, 21, 56. [Google Scholar] [CrossRef]
- de Bruyn, D.P.; Beasley, A.B.; Verdijk, R.M.; van Poppelen, N.M.; Paridaens, D.; de Keizer, R.O.B.; Naus, N.C.; Gray, E.S.; de Klein, A.; Brosens, E.; et al. Is Tissue Still the Issue? The Promise of Liquid Biopsy in Uveal Melanoma. Biomedicines 2022, 10, 506. [Google Scholar] [CrossRef] [PubMed]
- Beasley, A.B.; Chen, F.K.; Isaacs, T.W.; Gray, E.S. Future Perspectives of Uveal Melanoma Blood Based Biomarkers. Br. J. Cancer 2022, 126, 1511–1528. [Google Scholar] [CrossRef]
- Martel, A.; Mograbi, B.; Romeo, B.; Gastaud, L.; Lalvee, S.; Zahaf, K.; Fayada, J.; Nahon-Esteve, S.; Bonnetaud, C.; Salah, M.; et al. Assessment of Different Circulating Tumor Cell Platforms for Uveal Melanoma: Potential Impact for Future Routine Clinical Practice. Int. J. Mol. Sci. 2023, 24, 11075. [Google Scholar] [CrossRef]
- Beasley, A.B.; Isaacs, T.W.; Vermeulen, T.; Freeman, J.; DeSousa, J.-L.; Bhikoo, R.; Hennessy, D.; Reid, A.; Chen, F.K.; Bentel, J.; et al. Analysis of Circulating Tumour Cells in Early-Stage Uveal Melanoma: Evaluation of Tumour Marker Expression to Increase Capture. Cancers 2021, 13, 5990. [Google Scholar] [CrossRef] [PubMed]
- Gast, C.E.; Silk, A.D.; Zarour, L.; Riegler, L.; Burkhart, J.G.; Gustafson, K.T.; Parappilly, M.S.; Roh-Johnson, M.; Goodman, J.R.; Olson, B.; et al. Cell Fusion Potentiates Tumor Heterogeneity and Reveals Circulating Hybrid Cells That Correlate with Stage and Survival. Sci. Adv. 2018, 4, eaat7828. [Google Scholar] [CrossRef] [PubMed]
- Dietz, M.S.; Sutton, T.L.; Walker, B.S.; Gast, C.E.; Zarour, L.; Sengupta, S.K.; Swain, J.R.; Eng, J.; Parappilly, M.; Limbach, K.; et al. Relevance of Circulating Hybrid Cells as a Non-Invasive Biomarker for Myriad Solid Tumors. Sci. Rep. 2021, 11, 13630. [Google Scholar] [CrossRef]
- Parappilly, M.S.; Chin, Y.; Whalen, R.M.; Anderson, A.N.; Robinson, T.S.; Strgar, L.; Sutton, T.L.; Conley, P.; Klocke, C.; Gibbs, S.L.; et al. Circulating Neoplastic-Immune Hybrid Cells Predict Metastatic Progression in Uveal Melanoma. Cancers 2022, 14, 4617. [Google Scholar] [CrossRef]
- Schwarzenbach, H.; Hoon, D.S.B.; Pantel, K. Cell-Free Nucleic Acids as Biomarkers in Cancer Patients. Nat. Rev. Cancer 2011, 11, 426–437. [Google Scholar] [CrossRef]
- Valle-Inclan, J.E.; Stangl, C.; de Jong, A.C.; van Dessel, L.F.; van Roosmalen, M.J.; Helmijr, J.C.A.; Renkens, I.; Janssen, R.; de Blank, S.; de Witte, C.J.; et al. Optimizing Nanopore Sequencing-Based Detection of Structural Variants Enables Individualized Circulating Tumor DNA-Based Disease Monitoring in Cancer Patients. Genome Med. 2021, 13, 86. [Google Scholar] [CrossRef]
- Escalona-Noguero, C.; Alarcón-Iniesta, H.; López-Valls, M.; Del Carpio, L.P.; Piulats, J.M.; Somoza, Á.; Sot, B. Detection of the Uveal Melanoma-Associated Mutation GNAQ Q209P from Liquid Biopsy Using CRISPR/Cas12a Technology. Anal. Chem. 2023, 95, 16692–16700. [Google Scholar] [CrossRef] [PubMed]
- Welsh, J.A.; Goberdhan, D.C.I.; O’Driscoll, L.; Buzas, E.I.; Blenkiron, C.; Bussolati, B.; Cai, H.; Di Vizio, D.; Driedonks, T.A.P.; Erdbrügger, U.; et al. Minimal Information for Studies of Extracellular Vesicles (MISEV2023): From Basic to Advanced Approaches. J. Extracell. Vesicles 2024, 13, e12404. [Google Scholar] [CrossRef] [PubMed]
- Möller, A.; Lobb, R.J. The Evolving Translational Potential of Small Extracellular Vesicles in Cancer. Nat. Rev. Cancer 2020, 20, 697–709. [Google Scholar] [CrossRef] [PubMed]
- Eldh, M.; Olofsson Bagge, R.; Lässer, C.; Svanvik, J.; Sjöstrand, M.; Mattsson, J.; Lindnér, P.; Choi, D.-S.; Gho, Y.S.; Lötvall, J. MicroRNA in Exosomes Isolated Directly from the Liver Circulation in Patients with Metastatic Uveal Melanoma. BMC Cancer 2014, 14, 962. [Google Scholar] [CrossRef] [PubMed]
- Piquet, L.; Coutant, K.; Mitchell, A.; Ben Anes, A.; Bollmann, E.; Schoonjans, N.; Bérubé, J.; Bordeleau, F.; Brisson, A.; Landreville, S. Extracellular Vesicles from Ocular Melanoma Have Pro-Fibrotic and Pro-Angiogenic Properties on the Tumor Microenvironment. Cells 2022, 11, 3828. [Google Scholar] [CrossRef] [PubMed]
- Tsering, T.; Laskaris, A.; Abdouh, M.; Bustamante, P.; Parent, S.; Jin, E.; Ferrier, S.T.; Arena, G.; Burnier, J.V. Uveal Melanoma-Derived Extracellular Vesicles Display Transforming Potential and Carry Protein Cargo Involved in Metastatic Niche Preparation. Cancers 2020, 12, 2923. [Google Scholar] [CrossRef] [PubMed]
- Surman, M.; Hoja-Łukowicz, D.; Szwed, S.; Kędracka-Krok, S.; Jankowska, U.; Kurtyka, M.; Drożdż, A.; Lityńska, A.; Stępień, E.; Przybyło, M. An Insight into the Proteome of Uveal Melanoma-Derived Ectosomes Reveals the Presence of Potentially Useful Biomarkers. Int. J. Mol. Sci. 2019, 20, 3789. [Google Scholar] [CrossRef] [PubMed]
- Pessuti, C.L.; Costa, D.F.; Ribeiro, K.S.; Abdouh, M.; Tsering, T.; Nascimento, H.; Commodaro, A.G.; Marcos, A.A.A.; Torrecilhas, A.C.; Belfort, R.N.; et al. Characterization of Extracellular Vesicles Isolated from Different Liquid Biopsies of Uveal Melanoma Patients. J. Circ. Biomark. 2022, 11, 36–47. [Google Scholar] [CrossRef] [PubMed]
- Wróblewska, J.P.; Lach, M.S.; Kulcenty, K.; Galus, Ł.; Suchorska, W.M.; Rösel, D.; Brábek, J.; Marszałek, A. The Analysis of Inflammation-Related Proteins in a Cargo of Exosomes Derived from the Serum of Uveal Melanoma Patients Reveals Potential Biomarkers of Disease Progression. Cancers 2021, 13, 3334. [Google Scholar] [CrossRef]
- Velez, G.; Nguyen, H.V.; Chemudupati, T.; Ludwig, C.A.; Toral, M.; Reddy, S.; Mruthyunjaya, P.; Mahajan, V.B. Liquid Biopsy Proteomics of Uveal Melanoma Reveals Biomarkers Associated with Metastatic Risk. Mol. Cancer 2021, 20, 39. [Google Scholar] [CrossRef]
- Im, D.H.; Peng, C.-C.; Xu, L.; Kim, M.E.; Ostrow, D.; Yellapantula, V.; Bootwalla, M.; Biegel, J.A.; Gai, X.; Prabakar, R.K.; et al. Potential of Aqueous Humor as a Liquid Biopsy for Uveal Melanoma. Int. J. Mol. Sci. 2022, 23, 6226. [Google Scholar] [CrossRef] [PubMed]
- Peng, C.-C.; Sirivolu, S.; Pike, S.; Kim, M.E.; Reiser, B.; Li, H.-T.; Liang, G.; Xu, L.; Berry, J.L. Diagnostic Aqueous Humor Proteome Predicts Metastatic Potential in Uveal Melanoma. Int. J. Mol. Sci. 2023, 24, 6825. [Google Scholar] [CrossRef] [PubMed]
- Midena, G.; Parrozzani, R.; Frizziero, L.; Esposito, G.; Micera, A.; Midena, E. Expression of GNAQ, BAP1, SF3B1, and EIF1AX Proteins in the Aqueous Humor of Eyes Affected by Uveal Melanoma. Investig. Ophthalmol. Vis. Sci. 2024, 65, 15. [Google Scholar] [CrossRef] [PubMed]
- Velez, G.; Wolf, J.; Dufour, A.; Mruthyunjaya, P.; Mahajan, V.B. Cross-Platform Identification and Validation of Uveal Melanoma Vitreous Protein Biomarkers. Investig. Ophthalmol. Vis. Sci. 2023, 64, 14. [Google Scholar] [CrossRef] [PubMed]
- Demirci, H.; Tang, L.; Demirci, F.Y.; Ozgonul, C.; Weber, S.; Sundstrom, J. Investigating Vitreous Cytokines in Choroidal Melanoma. Cancers 2023, 15, 3701. [Google Scholar] [CrossRef] [PubMed]
- Yang, C.; Wei, W. The miRNA Expression Profile of the Uveal Melanoma. Sci. China Life Sci. 2011, 54, 351–358. [Google Scholar] [CrossRef] [PubMed]
- Falzone, L.; Romano, G.L.; Salemi, R.; Bucolo, C.; Tomasello, B.; Lupo, G.; Anfuso, C.D.; Spandidos, D.A.; Libra, M.; Candido, S. Prognostic Significance of Deregulated microRNAs in Uveal Melanomas. Mol. Med. Rep. 2019, 19, 2599–2610. [Google Scholar] [CrossRef]
- Mitchell, P.S.; Parkin, R.K.; Kroh, E.M.; Fritz, B.R.; Wyman, S.K.; Pogosova-Agadjanyan, E.L.; Peterson, A.; Noteboom, J.; O’Briant, K.C.; Allen, A.; et al. Circulating microRNAs as Stable Blood-Based Markers for Cancer Detection. Proc. Natl. Acad. Sci. USA 2008, 105, 10513–10518. [Google Scholar] [CrossRef] [PubMed]
- Zhou, W.-D.; Shao, L.; Dong, L.; Zhang, R.-H.; Li, Y.-F.; Li, H.-Y.; Wu, H.-T.; Shi, X.-H.; Wei, W.-B. Circulating MicroRNAs as Quantitative Biomarkers for Diagnosis and Prognosis of Uveal Melanoma. Front. Oncol. 2022, 12, 854253. [Google Scholar] [CrossRef]
- Wróblewska, J.P.; Lach, M.S.; Rucinski, M.; Piotrowski, I.; Galus, L.; Suchorska, W.M.; Kreis, S.; Marszałek, A. MiRNAs from Serum-Derived Extracellular Vesicles as Biomarkers for Uveal Melanoma Progression. Front. Cell Dev. Biol. 2022, 10, 1008901. [Google Scholar] [CrossRef]
- Field, M.G.; Durante, M.A.; Decatur, C.L.; Tarlan, B.; Oelschlager, K.M.; Stone, J.F.; Kuznetsov, J.; Bowcock, A.M.; Kurtenbach, S.; Harbour, J.W. Epigenetic Reprogramming and Aberrant Expression of PRAME Are Associated with Increased Metastatic Risk in Class 1 and Class 2 Uveal Melanomas. Oncotarget 2016, 7, 59209–59219. [Google Scholar] [CrossRef] [PubMed]
- Schefler, A.C.; Koca, E.; Bernicker, E.H.; Correa, Z.M. Relationship between Clinical Features, GEP Class, and PRAME Expression in Uveal Melanoma. Graefes Arch. Clin. Exp. Ophthalmol. 2019, 257, 1541–1545. [Google Scholar] [CrossRef] [PubMed]
- Field, M.G.; Decatur, C.L.; Kurtenbach, S.; Gezgin, G.; van der Velden, P.A.; Jager, M.J.; Kozak, K.N.; Harbour, J.W. PRAME as an Independent Biomarker for Metastasis in Uveal Melanoma. Clin. Cancer Res. 2016, 22, 1234–1242. [Google Scholar] [CrossRef] [PubMed]
- Gelmi, M.C.; Gezgin, G.; van der Velden, P.A.; Luyten, G.P.M.; Luk, S.J.; Heemskerk, M.H.M.; Jager, M.J. PRAME Expression: A Target for Cancer Immunotherapy and a Prognostic Factor in Uveal Melanoma. Investig. Ophthalmol. Vis. Sci. 2023, 64, 36. [Google Scholar] [CrossRef]
- Kurtenbach, S.; Sanchez, M.I.; Kuznetsoff, J.; Rodriguez, D.A.; Weich, N.; Dollar, J.J.; Cruz, A.; Kurtenbach, S.; Field, M.G.; Durante, M.A.; et al. PRAME Induces Genomic Instability in Uveal Melanoma. Oncogene 2023, 43, 555–565. [Google Scholar] [CrossRef] [PubMed]
- Dorsett, D.; Ström, L. The Ancient and Evolving Roles of Cohesin in Gene Expression and DNA Repair. Curr. Biol. 2012, 22, R240–R250. [Google Scholar] [CrossRef] [PubMed]
- Daniloski, Z.; Smith, S. Loss of Tumor Suppressor STAG2 Promotes Telomere Recombination and Extends the Replicative Lifespan of Normal Human Cells. Cancer Res. 2017, 77, 5530–5542. [Google Scholar] [CrossRef] [PubMed]
- Van Den Eynden, G.G.; Majeed, A.W.; Illemann, M.; Vermeulen, P.B.; Bird, N.C.; Høyer-Hansen, G.; Eefsen, R.L.; Reynolds, A.R.; Brodt, P. The Multifaceted Role of the Microenvironment in Liver Metastasis: Biology and Clinical Implications. Cancer Res. 2013, 73, 2031–2043. [Google Scholar] [CrossRef]
- Herwig, M.C.; Bergstrom, C.; Wells, J.R.; Höller, T.; Grossniklaus, H.E. M2/M1 Ratio of Tumor Associated Macrophages and PPAR-Gamma Expression in Uveal Melanomas with Class 1 and Class 2 Molecular Profiles. Exp. Eye Res. 2013, 107, 52–58. [Google Scholar] [CrossRef]
- Tan, Y.; Pan, J.; Deng, Z.; Chen, T.; Xia, J.; Liu, Z.; Zou, C.; Qin, B. Monoacylglycerol Lipase Regulates Macrophage Polarization and Cancer Progression in Uveal Melanoma and Pan-Cancer. Front. Immunol. 2023, 14, 1161960. [Google Scholar] [CrossRef]
- Fu, L.; Huang, Q.; Wu, Y.; Chen, D. Prognostic Analysis of Uveal Melanoma Based on the Characteristic Genes of M2-Type Macrophages in the Tumor Microenvironment. BMC Bioinform. 2023, 24, 280. [Google Scholar] [CrossRef] [PubMed]
- Pan, L.-S.; Ackbarkha, Z.; Zeng, J.; Huang, M.-L.; Yang, Z.; Liang, H. Immune Marker Signature Helps to Predict Survival in Uveal Melanoma. Math. Biosci. Eng. 2021, 18, 4055–4070. [Google Scholar] [CrossRef] [PubMed]
- Bande, M.; Fernandez-Diaz, D.; Fernandez-Marta, B.; Rodriguez-Vidal, C.; Lago-Baameiro, N.; Silva-Rodríguez, P.; Paniagua, L.; Blanco-Teijeiro, M.J.; Pardo, M.; Piñeiro, A. The Role of Non-Coding RNAs in Uveal Melanoma. Cancers 2020, 12, 2944. [Google Scholar] [CrossRef] [PubMed]
- Aughton, K.; Kalirai, H.; Coupland, S.E. MicroRNAs and Uveal Melanoma: Understanding the Diverse Role of These Small Molecular Regulators. Int. J. Mol. Sci. 2020, 21, 5648. [Google Scholar] [CrossRef] [PubMed]
- Zuo, J.; Ye, H.; Tang, J.; Lu, J.; Wan, Q. Development of a 3-MicroRNA Signature and Nomogram for Predicting the Survival of Patients with Uveal Melanoma Based on TCGA and GEO Databases. J. Ophthalmol. 2022, 2022, 9724160. [Google Scholar] [CrossRef] [PubMed]
- Xia, F.; Yu, Z.; Deng, A.; Gao, G. Identification of Molecular Subtyping System and Four-Gene Prognostic Signature with Immune-Related Genes for Uveal Melanoma. Exp. Biol. Med. 2022, 247, 246–262. [Google Scholar] [CrossRef] [PubMed]
- van Essen, T.H.; van Pelt, S.I.; Bronkhorst, I.H.G.; Versluis, M.; Némati, F.; Laurent, C.; Luyten, G.P.M.; van Hall, T.; van den Elsen, P.J.; van der Velden, P.A.; et al. Upregulation of HLA Expression in Primary Uveal Melanoma by Infiltrating Leukocytes. PLoS ONE 2016, 11, e0164292. [Google Scholar] [CrossRef] [PubMed]
- Ren, Y.; Yan, C.; Wu, L.; Zhao, J.; Chen, M.; Zhou, M.; Wang, X.; Liu, T.; Yi, Q.; Sun, J. iUMRG: Multi-Layered Network-Guided Propagation Modeling for the Inference of Susceptibility Genes and Potential Drugs against Uveal Melanoma. NPJ Syst. Biol. Appl. 2022, 8, 18. [Google Scholar] [CrossRef]
- Chatterjee, S.; Behnam Azad, B.; Nimmagadda, S. The Intricate Role of CXCR4 in Cancer. Adv. Cancer Res. 2014, 124, 31–82. [Google Scholar] [CrossRef]
- Bakalian, S.; Marshall, J.-C.; Logan, P.; Faingold, D.; Maloney, S.; Di Cesare, S.; Martins, C.; Fernandes, B.F.; Burnier, M.N. Molecular Pathways Mediating Liver Metastasis in Patients with Uveal Melanoma. Clin. Cancer Res. 2008, 14, 951–956. [Google Scholar] [CrossRef]
- Yang, H.; Tan, S.; Qiao, J.; Xu, Y.; Gui, Z.; Meng, Y.; Dong, B.; Peng, G.; Ibhagui, O.Y.; Qian, W.; et al. Non-Invasive Detection and Complementary Diagnosis of Liver Metastases via Chemokine Receptor 4 Imaging. Cancer Gene Ther. 2022, 29, 1827–1839. [Google Scholar] [CrossRef] [PubMed]
- Wang, M.M.; Chen, C.; Lynn, M.N.; Figueiredo, C.R.; Tan, W.J.; Lim, T.S.; Coupland, S.E.; Chan, A.S.Y. Applying Single-Cell Technology in Uveal Melanomas: Current Trends and Perspectives for Improving Uveal Melanoma Metastasis Surveillance and Tumor Profiling. Front. Mol. Biosci. 2020, 7, 611584. [Google Scholar] [CrossRef] [PubMed]
- Durante, M.A.; Rodriguez, D.A.; Kurtenbach, S.; Kuznetsov, J.N.; Sanchez, M.I.; Decatur, C.L.; Snyder, H.; Feun, L.G.; Livingstone, A.S.; Harbour, J.W. Single-Cell Analysis Reveals New Evolutionary Complexity in Uveal Melanoma. Nat. Commun. 2020, 11, 496. [Google Scholar] [CrossRef] [PubMed]
- Duchartre, Y.; Kim, Y.-M.; Kahn, M. The Wnt Signaling Pathway in Cancer. Crit. Rev. Oncol. Hematol. 2016, 99, 141–149. [Google Scholar] [CrossRef] [PubMed]
- Dey, A.; Varelas, X.; Guan, K.-L. Targeting the Hippo Pathway in Cancer, Fibrosis, Wound Healing and Regenerative Medicine. Nat. Rev. Drug Discov. 2020, 19, 480–494. [Google Scholar] [CrossRef] [PubMed]
- Hu, X.; Li, J.; Fu, M.; Zhao, X.; Wang, W. The JAK/STAT Signaling Pathway: From Bench to Clinic. Signal Transduct. Target. Ther. 2021, 6, 402. [Google Scholar] [CrossRef] [PubMed]
- Tanaka, M.; Siemann, D.W. Therapeutic Targeting of the Gas6/Axl Signaling Pathway in Cancer. Int. J. Mol. Sci. 2021, 22, 9953. [Google Scholar] [CrossRef]
- Dey, P.; Kimmelman, A.C.; DePinho, R.A. Metabolic Codependencies in the Tumor Microenvironment. Cancer Discov. 2021, 11, 1067–1081. [Google Scholar] [CrossRef]
- Goodwin, J.; Neugent, M.L.; Lee, S.Y.; Choe, J.H.; Choi, H.; Jenkins, D.M.R.; Ruthenborg, R.J.; Robinson, M.W.; Jeong, J.Y.; Wake, M.; et al. The Distinct Metabolic Phenotype of Lung Squamous Cell Carcinoma Defines Selective Vulnerability to Glycolytic Inhibition. Nat. Commun. 2017, 8, 15503. [Google Scholar] [CrossRef]
- Daemen, A.; Peterson, D.; Sahu, N.; McCord, R.; Du, X.; Liu, B.; Kowanetz, K.; Hong, R.; Moffat, J.; Gao, M.; et al. Metabolite Profiling Stratifies Pancreatic Ductal Adenocarcinomas into Subtypes with Distinct Sensitivities to Metabolic Inhibitors. Proc. Natl. Acad. Sci. USA 2015, 112, E4410–E4417. [Google Scholar] [CrossRef]
- Han, A.; Purwin, T.J.; Bechtel, N.; Liao, C.; Chua, V.; Seifert, E.; Sato, T.; Schug, Z.T.; Speicher, D.W.; Harbour, J.W.; et al. BAP1 Mutant Uveal Melanoma Is Stratified by Metabolic Phenotypes with Distinct Vulnerability to Metabolic Inhibitors. Oncogene 2021, 40, 618–632. [Google Scholar] [CrossRef] [PubMed]
- Moorman, H.R.; Poschel, D.; Klement, J.D.; Lu, C.; Redd, P.S.; Liu, K. Osteopontin: A Key Regulator of Tumor Progression and Immunomodulation. Cancers 2020, 12, 3379. [Google Scholar] [CrossRef] [PubMed]
- Chen, C.; Zhao, S.; Karnad, A.; Freeman, J.W. The Biology and Role of CD44 in Cancer Progression: Therapeutic Implications. J. Hematol. Oncol. 2018, 11, 64. [Google Scholar] [CrossRef] [PubMed]
- Sun, S.; Guo, B.; Xu, L.; Shi, R. Integrated Analysis Reveals the Dysfunction of Signaling Pathways in Uveal Melanoma. BMC Cancer 2022, 22, 734. [Google Scholar] [CrossRef]
- Zhao, H.; Chen, Y.; Shen, P.; Gong, L. Construction and Validation of a Novel Prognostic Signature for Uveal Melanoma Based on Five Metabolism-Related Genes. Math. Biosci. Eng. 2021, 18, 8045–8063. [Google Scholar] [CrossRef] [PubMed]
- Wang, W.; Zhao, H.; Wang, S. Identification of a Novel Immune-Related Gene Signature for Prognosis and the Tumor Microenvironment in Patients with Uveal Melanoma Combining Single-Cell and Bulk Sequencing Data. Front. Immunol. 2023, 14, 1099071. [Google Scholar] [CrossRef]
- Longhitano, L.; Broggi, G.; Giallongo, S.; Failla, M.; Puzzo, L.; Avitabile, T.; Tibullo, D.; Distefano, A.; Pittalà, V.; Reibaldi, M.; et al. Heme Oxygenase-1 Overexpression Promotes Uveal Melanoma Progression and Is Associated with Poor Clinical Outcomes. Antioxidants 2022, 11, 1997. [Google Scholar] [CrossRef]
- Zhang, L.; Li, X.; Zhang, J.; Xu, G. Prognostic Implication and Oncogenic Role of PNPO in Pan-Cancer. Front. Cell Dev. Biol. 2021, 9, 763674. [Google Scholar] [CrossRef] [PubMed]
- Deliktas, O.; Gedik, M.E.; Koc, I.; Gunaydin, G.; Kiratli, H. Modulation of AMPK Significantly Alters Uveal Melanoma Tumor Cell Viability. Ophthalmic Res. 2023, 66, 1230–1244. [Google Scholar] [CrossRef]
- Chua, V.; Han, A.; Bechtel, N.; Purwin, T.J.; Hunter, E.; Liao, C.; Harbour, J.W.; Aplin, A.E. The AMP-Dependent Kinase Pathway Is Upregulated in BAP1 Mutant Uveal Melanoma. Pigment. Cell Melanoma Res. 2022, 35, 78–87. [Google Scholar] [CrossRef]
- Giblin, W.; Bringman-Rodenbarger, L.; Guo, A.H.; Kumar, S.; Monovich, A.C.; Mostafa, A.M.; Skinner, M.E.; Azar, M.; Mady, A.S.; Chung, C.H.; et al. The Deacylase SIRT5 Supports Melanoma Viability by Influencing Chromatin Dynamics. J. Clin. Investig. 2021, 131, e138926. [Google Scholar] [CrossRef]
- Guo, X.; Yu, X.; Li, F.; Xia, Q.; Ren, H.; Chen, Z.; Xing, Y. Identification of Survival-Related Metabolic Genes and a Novel Gene Signature Predicting the Overall Survival for Patients with Uveal Melanoma. Ophthalmic Res. 2022, 65, 516–528. [Google Scholar] [CrossRef] [PubMed]
- Onorati, A.V.; Dyczynski, M.; Ojha, R.; Amaravadi, R.K. Targeting Autophagy in Cancer. Cancer 2018, 124, 3307–3318. [Google Scholar] [CrossRef]
- Miller, D.R.; Thorburn, A. Autophagy and Organelle Homeostasis in Cancer. Dev. Cell 2021, 56, 906–918. [Google Scholar] [CrossRef] [PubMed]
- Rademaker, G.; Boumahd, Y.; Peiffer, R.; Anania, S.; Wissocq, T.; Liégeois, M.; Luis, G.; Sounni, N.E.; Agirman, F.; Maloujahmoum, N.; et al. Myoferlin Targeting Triggers Mitophagy and Primes Ferroptosis in Pancreatic Cancer Cells. Redox Biol. 2022, 53, 102324. [Google Scholar] [CrossRef]
- Debnath, J.; Gammoh, N.; Ryan, K.M. Autophagy and Autophagy-Related Pathways in Cancer. Nat. Rev. Mol. Cell Biol. 2023, 24, 560–575. [Google Scholar] [CrossRef] [PubMed]
- Giatromanolaki, A.N.; Charitoudis, G.S.; Bechrakis, N.E.; Kozobolis, V.P.; Koukourakis, M.I.; Foerster, M.H.; Sivridis, E.L. Autophagy Patterns and Prognosis in Uveal Melanomas. Mod. Pathol. 2011, 24, 1036–1045. [Google Scholar] [CrossRef]
- Zhao, Y.; Wang, W.; Min, I.; Wyrwas, B.; Moore, M.; Zarnegar, R.; Fahey, T.J. BRAF V600E-Dependent Role of Autophagy in Uveal Melanoma. J. Cancer Res. Clin. Oncol. 2017, 143, 447–455. [Google Scholar] [CrossRef]
- Zheng, Z.; Zhang, L.; Tu, Z.; Deng, Y.; Yin, X. An Autophagy-Related Prognostic Signature Associated with Immune Microenvironment Features of Uveal Melanoma. Biosci. Rep. 2021, 41, BSR20203812. [Google Scholar] [CrossRef]
- Cui, Y.; Zheng, M.; Chen, J.; Xu, N. Autophagy-Related Long Non-Coding RNA Signature as Indicators for the Prognosis of Uveal Melanoma. Front. Genet. 2021, 12, 625583. [Google Scholar] [CrossRef]
- Chen, Y.; Chen, L.; Wang, J.; Tan, J.; Wang, S. Identification of Six Autophagy-Related-lncRNA Prognostic Biomarkers in Uveal Melanoma. Dis. Markers 2021, 2021, 2401617. [Google Scholar] [CrossRef]
- Liu, B.; Yao, X.; Zhang, C.; Li, W.; Wang, Y.; Liao, Q.; Li, Z.; Huang, Q.; Zhang, Y.; Wu, W. LINC01278 Induces Autophagy to Inhibit Tumour Progression by Suppressing the mTOR Signalling Pathway. Oxid. Med. Cell Longev. 2023, 2023, 8994901. [Google Scholar] [CrossRef]
- Onishi, M.; Yamano, K.; Sato, M.; Matsuda, N.; Okamoto, K. Molecular Mechanisms and Physiological Functions of Mitophagy. EMBO J. 2021, 40, e104705. [Google Scholar] [CrossRef] [PubMed]
- Poole, L.P.; Macleod, K.F. Mitophagy in Tumorigenesis and Metastasis. Cell Mol. Life Sci. 2021, 78, 3817–3851. [Google Scholar] [CrossRef]
- Liu, C.; Wu, Z.; Wang, L.; Yang, Q.; Huang, J.; Huang, J. A Mitophagy-Related Gene Signature for Subtype Identification and Prognosis Prediction of Hepatocellular Carcinoma. Int. J. Mol. Sci. 2022, 23, 12123. [Google Scholar] [CrossRef] [PubMed]
- Amirouchene-Angelozzi, N.; Nemati, F.; Gentien, D.; Nicolas, A.; Dumont, A.; Carita, G.; Camonis, J.; Desjardins, L.; Cassoux, N.; Piperno-Neumann, S.; et al. Establishment of Novel Cell Lines Recapitulating the Genetic Landscape of Uveal Melanoma and Preclinical Validation of mTOR as a Therapeutic Target. Mol. Oncol. 2014, 8, 1508–1520. [Google Scholar] [CrossRef] [PubMed]
- Yoo, J.H.; Shi, D.S.; Grossmann, A.H.; Sorensen, L.K.; Tong, Z.; Mleynek, T.M.; Rogers, A.; Zhu, W.; Richards, J.R.; Winter, J.M.; et al. ARF6 Is an Actionable Node That Orchestrates Oncogenic GNAQ Signaling in Uveal Melanoma. Cancer Cell 2016, 29, 889–904. [Google Scholar] [CrossRef]
- Yang, X.; Li, Y.; Liu, Y.; Xu, X.; Wang, Y.; Yan, Y.; Zhou, W.; Yang, J.; Wei, W. Novel Circular RNA Expression Profile of Uveal Melanoma Revealed by Microarray. Chin. J. Cancer Res. 2018, 30, 656–668. [Google Scholar] [CrossRef]
- Liu, S.; Chen, L.; Chen, H.; Xu, K.; Peng, X.; Zhang, M. Circ_0119872 Promotes Uveal Melanoma Development by Regulating the miR-622/G3BP1 Axis and Downstream Signalling Pathways. J. Exp. Clin. Cancer Res. 2021, 40, 66. [Google Scholar] [CrossRef]
- Luo, J.; Li, H.; Xiu, J.; Zeng, J.; Feng, Z.; Zhao, H.; Li, Y.; Wei, W. Elevated ZNF704 Expression Is Associated with Poor Prognosis of Uveal Melanoma and Promotes Cancer Cell Growth by Regulating AKT/mTOR Signaling. Biomark. Res. 2023, 11, 38. [Google Scholar] [CrossRef]
- Han, A.; Mukha, D.; Chua, V.; Purwin, T.J.; Tiago, M.; Modasia, B.; Baqai, U.; Aumiller, J.L.; Bechtel, N.; Hunter, E.; et al. Co-Targeting FASN and mTOR Suppresses Uveal Melanoma Growth. Cancers 2023, 15, 3451. [Google Scholar] [CrossRef] [PubMed]
- Bao, R.; Surriga, O.; Olson, D.J.; Allred, J.B.; Strand, C.A.; Zha, Y.; Carll, T.; Labadie, B.W.; Bastos, B.R.; Butler, M.; et al. Transcriptional Analysis of Metastatic Uveal Melanoma Survival Nominates NRP1 as a Therapeutic Target. Melanoma Res. 2021, 31, 27–37. [Google Scholar] [CrossRef] [PubMed]
- Proteau, S.; Krossa, I.; Husser, C.; Guéguinou, M.; Sella, F.; Bille, K.; Irondelle, M.; Dalmasso, M.; Barouillet, T.; Cheli, Y.; et al. LKB1-SIK2 Loss Drives Uveal Melanoma Proliferation and Hypersensitivity to SLC8A1 and ROS Inhibition. EMBO Mol. Med. 2023, 15, e17719. [Google Scholar] [CrossRef] [PubMed]
- Matsuo, H.; Kamatani, T.; Hamba, Y.; Boroevich, K.A.; Tsunoda, T. Association between High Immune Activity and Worse Prognosis in Uveal Melanoma and Low-Grade Glioma in TCGA Transcriptomic Data. BMC Genom. 2022, 23, 351. [Google Scholar] [CrossRef] [PubMed]
- Jager, M.J.; Ly, L.V.; El Filali, M.; Madigan, M.C. Macrophages in Uveal Melanoma and in Experimental Ocular Tumor Models: Friends or Foes? Prog. Retin. Eye Res. 2011, 30, 129–146. [Google Scholar] [CrossRef] [PubMed]
- Zhang, C.; Wu, S. BAP1 Mutations Inhibit the NF-κB Signaling Pathway to Induce an Immunosuppressive Microenvironment in Uveal Melanoma. Mol. Med. 2023, 29, 126. [Google Scholar] [CrossRef] [PubMed]
- Zhang, F.; Deng, Y.; Wang, D.; Wang, S. Construction and Verification of the Molecular Subtype and a Novel Prognostic Signature Based on Inflammatory Response-Related Genes in Uveal Melanoma. J. Clin. Med. 2023, 12, 861. [Google Scholar] [CrossRef] [PubMed]
- Meng, S.; Zhu, T.; Fan, Z.; Cheng, Y.; Dong, Y.; Wang, F.; Wang, X.; Dong, D.; Yuan, S.; Zhao, X. Integrated Single-Cell and Transcriptome Sequencing Analyses Develops a Metastasis-Based Risk Score System for Prognosis and Immunotherapy Response in Uveal Melanoma. Front. Pharmacol. 2023, 14, 1138452. [Google Scholar] [CrossRef] [PubMed]
- Luo, H.; Ma, C. Identification of Prognostic Genes in Uveal Melanoma Microenvironment. PLoS ONE 2020, 15, e0242263. [Google Scholar] [CrossRef]
- Khan, M.; Ai, M.; Du, K.; Song, J.; Wang, B.; Lin, J.; Ren, A.; Chen, C.; Huang, Z.; Qiu, W.; et al. Pyroptosis Relates to Tumor Microenvironment Remodeling and Prognosis: A Pan-Cancer Perspective. Front. Immunol. 2022, 13, 1062225. [Google Scholar] [CrossRef]
- Conway, E.; Rossi, F.; Fernandez-Perez, D.; Ponzo, E.; Ferrari, K.J.; Zanotti, M.; Manganaro, D.; Rodighiero, S.; Tamburri, S.; Pasini, D. BAP1 Enhances Polycomb Repression by Counteracting Widespread H2AK119ub1 Deposition and Chromatin Condensation. Mol. Cell 2021, 81, 3526–3541.e8. [Google Scholar] [CrossRef] [PubMed]
- Linder, B.; Grozhik, A.V.; Olarerin-George, A.O.; Meydan, C.; Mason, C.E.; Jaffrey, S.R. Single-Nucleotide-Resolution Mapping of m6A and m6Am throughout the Transcriptome. Nat. Methods 2015, 12, 767–772. [Google Scholar] [CrossRef] [PubMed]
- Li, X.; Ma, B.; Zhang, W.; Song, Z.; Zhang, X.; Liao, M.; Li, X.; Zhao, X.; Du, M.; Yu, J.; et al. The Essential Role of N6-Methyladenosine RNA Methylation in Complex Eye Diseases. Genes. Dis. 2023, 10, 505–520. [Google Scholar] [CrossRef] [PubMed]
- Zhang, C.; Wu, S. Hypomethylation of CD3D Promoter Induces Immune Cell Infiltration and Supports Malignant Phenotypes in Uveal Melanoma. FASEB J. 2023, 37, e23128. [Google Scholar] [CrossRef] [PubMed]
- Herwig-Carl, M.C.; Sharma, A.; Tischler, V.; Pelusi, N.; Loeffler, K.U.; Holz, F.G.; Zeschnigk, M.; Landreville, S.; Auw-Haedrich, C.; Noberini, R.; et al. Mass Spectrometry-Based Profiling of Histone Post-Translational Modifications in Uveal Melanoma Tissues, Human Melanocytes, and Uveal Melanoma Cell Lines—A Pilot Study. Investig. Ophthalmol. Vis. Sci. 2024, 65, 27. [Google Scholar] [CrossRef] [PubMed]
- D’Aguanno, S.; Mallone, F.; Marenco, M.; Del Bufalo, D.; Moramarco, A. Hypoxia-Dependent Drivers of Melanoma Progression. J. Exp. Clin. Cancer Res. 2021, 40, 159. [Google Scholar] [CrossRef] [PubMed]
- Majmundar, A.J.; Wong, W.J.; Simon, M.C. Hypoxia-Inducible Factors and the Response to Hypoxic Stress. Mol. Cell 2010, 40, 294–309. [Google Scholar] [CrossRef] [PubMed]
- Chang, S.-H.; Worley, L.A.; Onken, M.D.; Harbour, J.W. Prognostic Biomarkers in Uveal Melanoma: Evidence for a Stem Cell-like Phenotype Associated with Metastasis. Melanoma Res. 2008, 18, 191–200. [Google Scholar] [CrossRef]
- Zhao, J.; Yi, Q.; Li, K.; Chen, L.; Dai, L.; Feng, J.; Li, Y.; Zhou, M.; Sun, J. A Multi-Omics Deep Learning Model for Hypoxia Phenotype to Predict Tumor Aggressiveness and Prognosis in Uveal Melanoma for Rationalized Hypoxia-Targeted Therapy. Comput. Struct. Biotechnol. J. 2022, 20, 3182–3194. [Google Scholar] [CrossRef]
- Kaluz, S.; Zhang, Q.; Kuranaga, Y.; Yang, H.; Osuka, S.; Bhattacharya, D.; Devi, N.S.; Mun, J.; Wang, W.; Zhang, R.; et al. Targeting HIF-Activated Collagen Prolyl 4-Hydroxylase Expression Disrupts Collagen Deposition and Blocks Primary and Metastatic Uveal Melanoma Growth. Oncogene 2021, 40, 5182–5191. [Google Scholar] [CrossRef]
- Liang, D.; Xiao-Feng, H.; Guan-Jun, D.; Er-Ling, H.; Sheng, C.; Ting-Ting, W.; Qin-Gang, H.; Yan-Hong, N.; Ya-Yi, H. Activated STING Enhances Tregs Infiltration in the HPV-Related Carcinogenesis of Tongue Squamous Cells via the c-Jun/CCL22 Signal. Biochim. Biophys. Acta 2015, 1852, 2494–2503. [Google Scholar] [CrossRef] [PubMed]
- Dai, E.; Han, L.; Liu, J.; Xie, Y.; Zeh, H.J.; Kang, R.; Bai, L.; Tang, D. Ferroptotic Damage Promotes Pancreatic Tumorigenesis through a TMEM173/STING-Dependent DNA Sensor Pathway. Nat. Commun. 2020, 11, 6339. [Google Scholar] [CrossRef] [PubMed]
- Zhou, X.; Meng, F.; Xu, B.; Ma, R.; Cheng, Y.; Wu, J.; Qian, J. STING Promotes Invasion and Migration of Uveal Melanoma through p38-MAPK Signaling. Oncol. Rep. 2024, 51, 23. [Google Scholar] [CrossRef] [PubMed]
- Zhang, X.; Bai, X.-C.; Chen, Z.J. Structures and Mechanisms in the cGAS-STING Innate Immunity Pathway. Immunity 2020, 53, 43–53. [Google Scholar] [CrossRef] [PubMed]
- Benhassine, M.; Le-Bel, G.; Guérin, S.L. Contribution of the STAT Family of Transcription Factors to the Expression of the Serotonin 2B (HTR2B) Receptor in Human Uveal Melanoma. Int. J. Mol. Sci. 2022, 23, 1564. [Google Scholar] [CrossRef] [PubMed]
- Mo, Q.; Wan, L.; Schell, M.J.; Jim, H.; Tworoger, S.S.; Peng, G. Integrative Analysis Identifies Multi-Omics Signatures That Drive Molecular Classification of Uveal Melanoma. Cancers 2021, 13, 6168. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Y.; Ding, P.; Wang, Y.; Shao, C.; Guo, K.; Yang, H.; Feng, Y.; Ning, J.; Pan, M.; Wang, P.; et al. HDAC7/c-Myc Signaling Pathway Promotes the Proliferation and Metastasis of Choroidal Melanoma Cells. Cell Death Dis. 2023, 14, 38. [Google Scholar] [CrossRef] [PubMed]
- Horvathova Kajabova, V.; Soltysova, A.; Demkova, L.; Plesnikova, P.; Lyskova, D.; Furdova, A.; Babal, P.; Smolkova, B. KIT Expression Is Regulated by DNA Methylation in Uveal Melanoma Tumors. Int. J. Mol. Sci. 2021, 22, 10748. [Google Scholar] [CrossRef] [PubMed]
- Gao, H.; Xu, C.; Liang, J.; Ge, S.; Zhang, F.; Tuo, Y.; Shi, H.; Han, A. Pan-Cancer Analysis of Oncogenic Role of Programmed Cell Death 2 Like (PDCD2L) and Validation in Colorectal Cancer. Cancer Cell Int. 2022, 22, 100. [Google Scholar] [CrossRef] [PubMed]
- Pandiani, C.; Strub, T.; Nottet, N.; Cheli, Y.; Gambi, G.; Bille, K.; Husser, C.; Dalmasso, M.; Béranger, G.; Lassalle, S.; et al. Single-Cell RNA Sequencing Reveals Intratumoral Heterogeneity in Primary Uveal Melanomas and Identifies HES6 as a Driver of the Metastatic Disease. Cell Death Differ. 2021, 28, 1990–2000. [Google Scholar] [CrossRef] [PubMed]
- Chu, W.; Song, X.; Yang, X.; Ma, L.; Zhu, J.; He, M.; Wang, Z.; Wu, Y. Neuropilin-1 Promotes Epithelial-to-Mesenchymal Transition by Stimulating Nuclear Factor-Kappa B and Is Associated with Poor Prognosis in Human Oral Squamous Cell Carcinoma. PLoS ONE 2014, 9, e101931. [Google Scholar] [CrossRef] [PubMed]
- Luo, M.; Hou, L.; Li, J.; Shao, S.; Huang, S.; Meng, D.; Liu, L.; Feng, L.; Xia, P.; Qin, T.; et al. VEGF/NRP-1axis Promotes Progression of Breast Cancer via Enhancement of Epithelial-Mesenchymal Transition and Activation of NF-κB and β-Catenin. Cancer Lett. 2016, 373, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Matkar, P.N.; Singh, K.K.; Rudenko, D.; Kim, Y.J.; Kuliszewski, M.A.; Prud’homme, G.J.; Hedley, D.W.; Leong-Poi, H. Novel Regulatory Role of Neuropilin-1 in Endothelial-to-Mesenchymal Transition and Fibrosis in Pancreatic Ductal Adenocarcinoma. Oncotarget 2016, 7, 69489–69506. [Google Scholar] [CrossRef] [PubMed]
- Ma, L.; Zhai, B.; Zhu, H.; Li, W.; Jiang, W.; Lei, L.; Zhang, S.; Qiao, H.; Jiang, X.; Sun, X. The miR-141/Neuropilin-1 Axis Is Associated with the Clinicopathology and Contributes to the Growth and Metastasis of Pancreatic Cancer. Cancer Cell Int. 2019, 19, 248. [Google Scholar] [CrossRef] [PubMed]
- Lei, S.; Zhang, Y. Identification of Survival-Related Genes and a Novel Gene-Based Prognostic Signature Involving the Tumor Microenvironment of Uveal Melanoma. Int. Immunopharmacol. 2021, 96, 107816. [Google Scholar] [CrossRef]
- Chen, P.W.; Mellon, J.K.; Mayhew, E.; Wang, S.; He, Y.G.; Hogan, N.; Niederkorn, J.Y. Uveal Melanoma Expression of Indoleamine 2,3-Deoxygenase: Establishment of an Immune Privileged Environment by Tryptophan Depletion. Exp. Eye Res. 2007, 85, 617–625. [Google Scholar] [CrossRef] [PubMed]
- Lachota, M.; Lennikov, A.; Malmberg, K.-J.; Zagozdzon, R. Bioinformatic Analysis Reveals Central Role for Tumor-Infiltrating Immune Cells in Uveal Melanoma Progression. J. Immunol. Res. 2021, 2021, 9920234. [Google Scholar] [CrossRef]
- Biswas, P.; Dai, Y.; Stuehr, D.J. Indoleamine Dioxygenase and Tryptophan Dioxygenase Activities Are Regulated through GAPDH- and Hsp90-Dependent Control of Their Heme Levels. Free Radic. Biol. Med. 2022, 180, 179–190. [Google Scholar] [CrossRef]
- Terai, M.; Londin, E.; Rochani, A.; Link, E.; Lam, B.; Kaushal, G.; Bhushan, A.; Orloff, M.; Sato, T. Expression of Tryptophan 2,3-Dioxygenase in Metastatic Uveal Melanoma. Cancers 2020, 12, 405. [Google Scholar] [CrossRef]
- Liu, J.; Lu, J.; Li, W. A Comprehensive Prognostic and Immunological Analysis of a Six-Gene Signature Associated With Glycolysis and Immune Response in Uveal Melanoma. Front. Immunol. 2021, 12, 738068. [Google Scholar] [CrossRef]
- Figueiredo, C.R.; Kalirai, H.; Sacco, J.J.; Azevedo, R.A.; Duckworth, A.; Slupsky, J.R.; Coulson, J.M.; Coupland, S.E. Loss of BAP1 Expression Is Associated with an Immunosuppressive Microenvironment in Uveal Melanoma, with Implications for Immunotherapy Development. J. Pathol. 2020, 250, 420–439. [Google Scholar] [CrossRef] [PubMed]
- Kaler, C.J.; Dollar, J.J.; Cruz, A.M.; Kuznetsoff, J.N.; Sanchez, M.I.; Decatur, C.L.; Licht, J.D.; Smalley, K.S.M.; Correa, Z.M.; Kurtenbach, S.; et al. BAP1 Loss Promotes Suppressive Tumor Immune Microenvironment via Upregulation of PROS1 in Class 2 Uveal Melanomas. Cancers 2022, 14, 3678. [Google Scholar] [CrossRef] [PubMed]
- Li, J.; Cao, D.; Jiang, L.; Zheng, Y.; Shao, S.; Zhuang, A.; Xiang, D. ITGB2-ICAM1 Axis Promotes Liver Metastasis in BAP1-Mutated Uveal Melanoma with Retained Hypoxia and ECM Signatures. Cell Oncol. 2023, 1–15. [Google Scholar] [CrossRef] [PubMed]
- Chen, Y.; Zheng, A.; Zhang, Y.; Xiao, M.; Zhao, Y.; Wu, X.; Li, M.; Du, F.; Chen, Y.; Chen, M.; et al. Dysregulation of B7 Family and Its Association with Tumor Microenvironment in Uveal Melanoma. Front. Immunol. 2022, 13, 1026076. [Google Scholar] [CrossRef] [PubMed]
- Moreaux, J.; Kassambara, A.; Hose, D.; Klein, B. STEAP1 Is Overexpressed in Cancers: A Promising Therapeutic Target. Biochem. Biophys. Res. Commun. 2012, 429, 148–155. [Google Scholar] [CrossRef] [PubMed]
- Zhao, C.; Xiong, K.; Ji, Z.; Liu, F.; Li, X. The Prognostic Value and Immunological Role of STEAP1 in Pan-Cancer: A Result of Data-Based Analysis. Oxid. Med. Cell Longev. 2022, 2022, 8297011. [Google Scholar] [CrossRef] [PubMed]
- Sun, X.; Li, Q.; Xu, G. Identification and Validation of an Immune-Relevant Risk Signature Predicting Survival Outcome and Immune Infiltration in Uveal Melanoma. Int. Ophthalmol. 2023, 43, 4689–4700. [Google Scholar] [CrossRef] [PubMed]
- Li, P.; Lu, M.; Shi, J.; Hua, L.; Gong, Z.; Li, Q.; Shultz, L.D.; Ren, G. Dual Roles of Neutrophils in Metastatic Colonization Are Governed by the Host NK Cell Status. Nat. Commun. 2020, 11, 4387. [Google Scholar] [CrossRef]
- Chan, I.S.; Knútsdóttir, H.; Ramakrishnan, G.; Padmanaban, V.; Warrier, M.; Ramirez, J.C.; Dunworth, M.; Zhang, H.; Jaffee, E.M.; Bader, J.S.; et al. Cancer Cells Educate Natural Killer Cells to a Metastasis-Promoting Cell State. J. Cell Biol. 2020, 219, e202001134. [Google Scholar] [CrossRef]
- Neo, S.Y.; Oliveira, M.M.S.; Tong, L.; Chen, Y.; Chen, Z.; Cismas, S.; Burduli, N.; Malmerfelt, A.; Teo, J.K.H.; Lam, K.-P.; et al. Natural Killer Cells Drive 4-1BBL Positive Uveal Melanoma towards EMT and Metastatic Disease. J. Exp. Clin. Cancer Res. 2024, 43, 13. [Google Scholar] [CrossRef]
- Zhang, Y.; Zhang, Z. The History and Advances in Cancer Immunotherapy: Understanding the Characteristics of Tumor-Infiltrating Immune Cells and Their Therapeutic Implications. Cell Mol. Immunol. 2020, 17, 807–821. [Google Scholar] [CrossRef] [PubMed]
- Andrieu, C.; McNamee, N.; Larkin, A.-M.; Maguire, A.; Menon, R.; Mueller-Eisert, J.; Horgan, N.; Kennedy, S.; Gullo, G.; Crown, J.; et al. Clinical Impact of Immune Checkpoint Inhibitor (ICI) Response, DNA Damage Repair (DDR) Gene Mutations and Immune-Cell Infiltration in Metastatic Melanoma Subtypes. Med. Sci. 2022, 10, 26. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Xu, Y.; Dai, X.; Lin, X.; Shan, Y.; Ye, J. The Prognostic Landscape of Adaptive Immune Resistance Signatures and Infiltrating Immune Cells in the Tumor Microenvironment of Uveal Melanoma. Exp. Eye Res. 2020, 196, 108069. [Google Scholar] [CrossRef] [PubMed]
- Zoroquiain, P.; Esposito, E.; Logan, P.; Aldrees, S.; Dias, A.B.; Mansure, J.J.; Santapau, D.; Garcia, C.; Saornil, M.A.; Belfort Neto, R.; et al. Programmed Cell Death Ligand-1 Expression in Tumor and Immune Cells Is Associated with Better Patient Outcome and Decreased Tumor-Infiltrating Lymphocytes in Uveal Melanoma. Mod. Pathol. 2018, 31, 1201–1210. [Google Scholar] [CrossRef]
- Singh, L.; Singh, M.K.; Kenney, M.C.; Jager, M.J.; Rizvi, M.A.; Meel, R.; Lomi, N.; Bakhshi, S.; Sen, S.; Kashyap, S. Prognostic Significance of PD-1/PD-L1 Expression in Uveal Melanoma: Correlation with Tumor-Infiltrating Lymphocytes and Clinicopathological Parameters. Cancer Immunol. Immunother. 2021, 70, 1291–1303. [Google Scholar] [CrossRef] [PubMed]
- Zhang, C.; Xiao, J.; Fa, L.; Jiang, F.; Jiang, H.; Zhou, L.; Xu, Z. Identification of Co-Expressed Gene Networks Promoting CD8+ T Cell Infiltration and Having Prognostic Value in Uveal Melanoma. BMC Ophthalmol. 2023, 23, 354. [Google Scholar] [CrossRef] [PubMed]
- Pan, C.; Wu, Q.; Feng, N. A Systematic Pan-Cancer Study Demonstrates the Oncogenic Function of Heterogeneous Nuclear Ribonucleoprotein C. Aging 2022, 14, 2880–2901. [Google Scholar] [CrossRef] [PubMed]
- Gao, G.; Yu, Z.; Zhao, X.; Fu, X.; Liu, S.; Liang, S.; Deng, A. Immune Classification and Identification of Prognostic Genes for Uveal Melanoma Based on Six Immune Cell Signatures. Sci. Rep. 2021, 11, 22244. [Google Scholar] [CrossRef] [PubMed]
- Wan, Q.; Ren, X.; Tang, J.; Ma, K.; Deng, Y. Cross Talk between Tumor Stemness and Microenvironment for Prognosis and Immunotherapy of Uveal Melanoma. J. Cancer Res. Clin. Oncol. 2023, 149, 11951–11968. [Google Scholar] [CrossRef]
- Reichstein, D.A.; Brock, A.L. Radiation Therapy for Uveal Melanoma: A Review of Treatment Methods Available in 2021. Curr Opin Ophthalmol 2021, 32, 183–190. [Google Scholar] [CrossRef]
- Rodriguez-Vidal, C.; Fernandez-Diaz, D.; Fernandez-Marta, B.; Lago-Baameiro, N.; Pardo, M.; Silva, P.; Paniagua, L.; Blanco-Teijeiro, M.J.; Piñeiro, A.; Bande, M. Treatment of Metastatic Uveal Melanoma: Systematic Review. Cancers 2020, 12, 2557. [Google Scholar] [CrossRef] [PubMed]
- Mallone, F.; Sacchetti, M.; Lambiase, A.; Moramarco, A. Molecular Insights and Emerging Strategies for Treatment of Metastatic Uveal Melanoma. Cancers 2020, 12, 2761. [Google Scholar] [CrossRef] [PubMed]
- de Miguel, M.; Calvo, E. T Cell Engagers in Solid Tumors Kick the Door Down. Cancer Cell 2021, 39, 1461–1463. [Google Scholar] [CrossRef] [PubMed]
- Dolgin, E. TCR Bispecific Boosts Survival in Uveal Melanoma. Cancer Discov. 2021, 11, 1312. [Google Scholar] [CrossRef] [PubMed]
- Chen, L.N.; Carvajal, R.D. Tebentafusp for the Treatment of HLA-A*02:01-Positive Adult Patients with Unresectable or Metastatic Uveal Melanoma. Expert. Rev. Anticancer Ther. 2022, 22, 1017–1027. [Google Scholar] [CrossRef]
- Nathan, P.; Hassel, J.C.; Rutkowski, P.; Baurain, J.-F.; Butler, M.O.; Schlaak, M.; Sullivan, R.J.; Ochsenreither, S.; Dummer, R.; Kirkwood, J.M.; et al. Overall Survival Benefit with Tebentafusp in Metastatic Uveal Melanoma. N. Engl. J. Med. 2021, 385, 1196–1206. [Google Scholar] [CrossRef]
- Carvajal, R.D.; Butler, M.O.; Shoushtari, A.N.; Hassel, J.C.; Ikeguchi, A.; Hernandez-Aya, L.; Nathan, P.; Hamid, O.; Piulats, J.M.; Rioth, M.; et al. Clinical and Molecular Response to Tebentafusp in Previously Treated Patients with Metastatic Uveal Melanoma: A Phase 2 Trial. Nat. Med. 2022, 28, 2364–2373. [Google Scholar] [CrossRef] [PubMed]
- Bi, G.; Jiang, G. The Molecular Mechanism of HDAC Inhibitors in Anticancer Effects. Cell Mol. Immunol. 2006, 3, 285–290. [Google Scholar] [PubMed]
- Souri, Z.; Jochemsen, A.G.; Wierenga, A.P.A.; Kroes, W.G.M.; Verdijk, R.M.; van der Velden, P.A.; Luyten, G.P.M.; Jager, M.J. Expression of HDACs 1, 3 and 8 Is Upregulated in the Presence of Infiltrating Lymphocytes in Uveal Melanoma. Cancers 2021, 13, 4146. [Google Scholar] [CrossRef]
- Levidou, G.; Gajdzis, P.; Cassoux, N.; Donizy, P.; Masaoutis, C.; Gajdzis, M.; Gardrat, S.; Pergaris, A.; Danas, E.; Klijanienko, J.; et al. Histone Deacetylase (HDAC)-1, -2, -4, and -6 in Uveal Melanomas: Associations with Clinicopathological Parameters and Patients’ Survival. Cancers 2021, 13, 4763. [Google Scholar] [CrossRef]
- Landreville, S.; Agapova, O.A.; Matatall, K.A.; Kneass, Z.T.; Onken, M.D.; Lee, R.S.; Bowcock, A.M.; Harbour, J.W. Histone Deacetylase Inhibitors Induce Growth Arrest and Differentiation in Uveal Melanoma. Clin. Cancer Res. 2012, 18, 408–416. [Google Scholar] [CrossRef] [PubMed]
- Palamaris, K.; Moutafi, M.; Gakiopoulou, H.; Theocharis, S. Histone Deacetylase (HDAC) Inhibitors: A Promising Weapon to Tackle Therapy Resistance in Melanoma. Int. J. Mol. Sci. 2022, 23, 3660. [Google Scholar] [CrossRef] [PubMed]
- Ny, L.; Jespersen, H.; Karlsson, J.; Alsén, S.; Filges, S.; All-Eriksson, C.; Andersson, B.; Carneiro, A.; Helgadottir, H.; Levin, M.; et al. The PEMDAC Phase 2 Study of Pembrolizumab and Entinostat in Patients with Metastatic Uveal Melanoma. Nat. Commun. 2021, 12, 5155. [Google Scholar] [CrossRef] [PubMed]
- Jespersen, H.; Olofsson Bagge, R.; Ullenhag, G.; Carneiro, A.; Helgadottir, H.; Ljuslinder, I.; Levin, M.; All-Eriksson, C.; Andersson, B.; Stierner, U.; et al. Concomitant Use of Pembrolizumab and Entinostat in Adult Patients with Metastatic Uveal Melanoma (PEMDAC Study): Protocol for a Multicenter Phase II Open Label Study. BMC Cancer 2019, 19, 415. [Google Scholar] [CrossRef] [PubMed]
- Souri, Z.; Jochemsen, A.G.; Versluis, M.; Wierenga, A.P.A.; Nemati, F.; van der Velden, P.A.; Kroes, W.G.M.; Verdijk, R.M.; Luyten, G.P.M.; Jager, M.J. HDAC Inhibition Increases HLA Class I Expression in Uveal Melanoma. Cancers 2020, 12, 3690. [Google Scholar] [CrossRef] [PubMed]
- Sundaramurthi, H.; García-Mulero, S.; Tonelotto, V.; Slater, K.; Marcone, S.; Piulats, J.M.; Watson, R.W.; Tobin, D.J.; Jensen, L.D.; Kennedy, B.N. Uveal Melanoma Cell Line Proliferation Is Inhibited by Ricolinostat, a Histone Deacetylase Inhibitor. Cancers 2022, 14, 782. [Google Scholar] [CrossRef] [PubMed]
- Nencetti, S.; Cuffaro, D.; Nuti, E.; Ciccone, L.; Rossello, A.; Fabbi, M.; Ballante, F.; Ortore, G.; Carbotti, G.; Campelli, F.; et al. Identification of Histone Deacetylase Inhibitors with (Arylidene)Aminoxy Scaffold Active in Uveal Melanoma Cell Lines. J. Enzym. Inhib. Med. Chem. 2021, 36, 34–47. [Google Scholar] [CrossRef] [PubMed]
- Carvajal, R.D.; Piperno-Neumann, S.; Kapiteijn, E.; Chapman, P.B.; Frank, S.; Joshua, A.M.; Piulats, J.M.; Wolter, P.; Cocquyt, V.; Chmielowski, B.; et al. Selumetinib in Combination with Dacarbazine in Patients with Metastatic Uveal Melanoma: A Phase III, Multicenter, Randomized Trial (SUMIT). J. Clin. Oncol. 2018, 36, 1232–1239. [Google Scholar] [CrossRef]
- Piperno-Neumann, S.; Larkin, J.; Carvajal, R.D.; Luke, J.J.; Schwartz, G.K.; Hodi, F.S.; Sablin, M.-P.; Shoushtari, A.N.; Szpakowski, S.; Chowdhury, N.R.; et al. Genomic Profiling of Metastatic Uveal Melanoma and Clinical Results of a Phase I Study of the Protein Kinase C Inhibitor AEB071. Mol. Cancer Ther. 2020, 19, 1031–1039. [Google Scholar] [CrossRef]
- Piperno-Neumann, S.; Carlino, M.S.; Boni, V.; Loirat, D.; Speetjens, F.M.; Park, J.J.; Calvo, E.; Carvajal, R.D.; Nyakas, M.; Gonzalez-Maffe, J.; et al. A Phase I Trial of LXS196, a Protein Kinase C (PKC) Inhibitor, for Metastatic Uveal Melanoma. Br. J. Cancer 2023, 128, 1040–1051. [Google Scholar] [CrossRef]
- Bauer, S.; Larkin, J.; Hodi, F.S.; Stephen, F.; Kapiteijn, E.H.W.; Schwartz, G.K.; Calvo, E.; Yerramilli-Rao, P.; Piperno-Neumann, S.; Carvajal, R.D. A Phase Ib Trial of Combined PKC and MEK Inhibition with Sotrastaurin and Binimetinib in Patients with Metastatic Uveal Melanoma. Front. Oncol. 2023, 12, 975642. [Google Scholar] [CrossRef] [PubMed]
- Visser, M.; Papillon, J.P.N.; Luzzio, M.; LaMarche, M.J.; Fan, J.; Michael, W.; Wang, D.; Zhang, A.; Straub, C.; Mathieu, S.; et al. Discovery of Darovasertib (NVP-LXS196), a Pan-PKC Inhibitor for the Treatment of Metastatic Uveal Melanoma. J. Med. Chem. 2024, 67, 1447–1459. [Google Scholar] [CrossRef] [PubMed]
- Fan, G.; Liu, L.; Ye, J.; Xiao, W.; Xiong, X.-F. Design, Synthesis and Evaluation of Quinazoline Derivatives as Gαq/11 Proteins Inhibitors against Uveal Melanoma. Bioorg Chem. 2023, 143, 107005. [Google Scholar] [CrossRef] [PubMed]
- Hussain, M.; Cummins, M.C.; Endo-Streeter, S.; Sondek, J.; Kuhlman, B. Designer Proteins That Competitively Inhibit Gαq by Targeting Its Effector Site. J. Biol. Chem. 2021, 297, 101348. [Google Scholar] [CrossRef] [PubMed]
- Wang, R.; Tahiri, H.; Yang, C.; Landreville, S.; Callejo, S.; Hardy, P. MiR-181a-5p Inhibits Uveal Melanoma Development by Targeting GNAQ and AKT3. Am. J. Cancer Res. 2023, 13, 293–306. [Google Scholar]
- Yu, F.-X.; Luo, J.; Mo, J.-S.; Liu, G.; Kim, Y.C.; Meng, Z.; Zhao, L.; Peyman, G.; Ouyang, H.; Jiang, W.; et al. Mutant Gq/11 Promote Uveal Melanoma Tumorigenesis by Activating YAP. Cancer Cell 2014, 25, 822–830. [Google Scholar] [CrossRef] [PubMed]
- Feng, X.; Degese, M.S.; Iglesias-Bartolome, R.; Vaque, J.P.; Molinolo, A.A.; Rodrigues, M.; Zaidi, M.R.; Ksander, B.R.; Merlino, G.; Sodhi, A.; et al. Hippo-Independent Activation of YAP by the GNAQ Uveal Melanoma Oncogene through a Trio-Regulated Rho GTPase Signaling Circuitry. Cancer Cell 2014, 25, 831–845. [Google Scholar] [CrossRef]
- Kim, Y.J.; Lee, S.C.; Kim, S.E.; Kim, S.H.; Kim, S.K.; Lee, C.S. YAP Activity Is Not Associated with Survival of Uveal Melanoma Patients and Cell Lines. Sci. Rep. 2020, 10, 6209. [Google Scholar] [CrossRef]
- Feng, X.; Arang, N.; Rigiracciolo, D.C.; Lee, J.S.; Yeerna, H.; Wang, Z.; Lubrano, S.; Kishore, A.; Pachter, J.A.; König, G.M.; et al. A Platform of Synthetic Lethal Gene Interaction Networks Reveals That the GNAQ Uveal Melanoma Oncogene Controls the Hippo Pathway through FAK. Cancer Cell 2019, 35, 457–472.e5. [Google Scholar] [CrossRef]
- Paradis, J.S.; Acosta, M.; Saddawi-Konefka, R.; Kishore, A.; Gomes, F.; Arang, N.; Tiago, M.; Coma, S.; Lubrano, S.; Wu, X.; et al. Synthetic Lethal Screens Reveal Cotargeting FAK and MEK as a Multimodal Precision Therapy for GNAQ-Driven Uveal Melanoma. Clin. Cancer Res. 2021, 27, 3190–3200. [Google Scholar] [CrossRef]
- Tarin, M.; Némati, F.; Decaudin, D.; Canbezdi, C.; Marande, B.; Silva, L.; Derrien, H.; Jochemsen, A.G.; Gardrat, S.; Piperno-Neumann, S.; et al. FAK Inhibitor-Based Combinations with MEK or PKC Inhibitors Trigger Synergistic Antitumor Effects in Uveal Melanoma. Cancers 2023, 15, 2280. [Google Scholar] [CrossRef] [PubMed]
- Arang, N.; Lubrano, S.; Ceribelli, M.; Rigiracciolo, D.C.; Saddawi-Konefka, R.; Faraji, F.; Ramirez, S.I.; Kim, D.; Tosto, F.A.; Stevenson, E.; et al. High-Throughput Chemogenetic Drug Screening Reveals PKC-RhoA/PKN as a Targetable Signaling Vulnerability in GNAQ-Driven Uveal Melanoma. Cell Rep. Med. 2023, 4, 101244. [Google Scholar] [CrossRef] [PubMed]
- Tao, H.; Tan, J.; Zhang, H.; Ren, H.; Cai, Z.; Liu, H.; Wen, B.; Du, J.; Li, G.; Chen, S.; et al. cGAS-STING Pathway Activation and Systemic Anti-Tumor Immunity Induction via Photodynamic Nanoparticles with Potent Toxic Platinum DNA Intercalator Against Uveal Melanoma. Adv Sci 2023, 10, e2302895. [Google Scholar] [CrossRef] [PubMed]
- Huis In ’t Veld, R.V.; Ma, S.; Kines, R.C.; Savinainen, A.; Rich, C.; Ossendorp, F.; Jager, M.J. Immune Checkpoint Inhibition Combined with Targeted Therapy Using a Novel Virus-like Drug Conjugate Induces Complete Responses in a Murine Model of Local and Distant Tumors. Cancer Immunol. Immunother. 2023, 72, 2405–2422. [Google Scholar] [CrossRef] [PubMed]
- Ma, S.; Huis In’t Veld, R.V.; Houy, A.; Stern, M.-H.; Rich, C.; Ossendorp, F.A.; Jager, M.J. In Vitro Testing of the Virus-Like Drug Conjugate Belzupacap Sarotalocan (AU-011) on Uveal Melanoma Suggests BAP1-Related Immunostimulatory Capacity. Investig. Ophthalmol. Vis. Sci. 2023, 64, 10. [Google Scholar] [CrossRef] [PubMed]
- Ponti, A.; Denys, A.; Digklia, A.; Schaefer, N.; Hocquelet, A.; Knebel, J.-F.; Michielin, O.; Dromain, C.; Duran, R. First-Line Selective Internal Radiation Therapy in Patients with Uveal Melanoma Metastatic to the Liver. J. Nucl. Med. 2020, 61, 350–356. [Google Scholar] [CrossRef] [PubMed]
- Kennedy, A.S.; Nutting, C.; Jakobs, T.; Cianni, R.; Notarianni, E.; Ofer, A.; Beny, A.; Dezarn, W.A. A First Report of Radioembolization for Hepatic Metastases from Ocular Melanoma. Cancer Investig. 2009, 27, 682–690. [Google Scholar] [CrossRef] [PubMed]
- Xing, M.; Prajapati, H.J.; Dhanasekaran, R.; Lawson, D.H.; Kokabi, N.; Eaton, B.R.; Kim, H.S. Selective Internal Yttrium-90 Radioembolization Therapy (90Y-SIRT) Versus Best Supportive Care in Patients with Unresectable Metastatic Melanoma to the Liver Refractory to Systemic Therapy: Safety and Efficacy Cohort Study. Am. J. Clin. Oncol. 2017, 40, 27–34. [Google Scholar] [CrossRef]
- Tabotta, F.; Gnesin, S.; Dunet, V.; Ponti, A.; Digklia, A.; Boughdad, S.; Schaefer, N.; Prior, J.O.; Villard, N.; Tsoumakidou, G.; et al. 99mTc-Macroaggregated Albumin SPECT/CT Predictive Dosimetry and Dose-Response Relationship in Uveal Melanoma Liver Metastases Treated with First-Line Selective Internal Radiation Therapy. Sci. Rep. 2023, 13, 13118. [Google Scholar] [CrossRef]
- Fiorentzis, M.; Sokolenko, E.A.; Bechrakis, N.E.; Ting, S.; Schmid, K.W.; Sak, A.; Stuschke, M.; Seitz, B.; Berchner-Pfannschmidt, U. Electrochemotherapy with Bleomycin Enhances Radiosensitivity of Uveal Melanomas: First In Vitro Results in 3D Cultures of Primary Uveal Melanoma Cell Lines. Cancers 2021, 13, 3086. [Google Scholar] [CrossRef]
- Xu, Y.-Y.; Ren, Z.-L.; Liu, X.-L.; Zhang, G.-M.; Huang, S.-S.; Shi, W.-H.; Ye, L.-X.; Luo, X.; Liu, S.-W.; Li, Y.-L.; et al. BAP1 Loss Augments Sensitivity to BET Inhibitors in Cancer Cells. Acta Pharmacol. Sin. 2022, 43, 1803–1815. [Google Scholar] [CrossRef] [PubMed]
- Arman, I.; Haus-Cohen, M.; Reiter, Y. The Intracellular Proteome as a Source for Novel Targets in CAR-T and T-Cell Engagers-Based Immunotherapy. Cells 2022, 12, 27. [Google Scholar] [CrossRef] [PubMed]
- Forsberg, E.M.V.; Lindberg, M.F.; Jespersen, H.; Alsén, S.; Bagge, R.O.; Donia, M.; Svane, I.M.; Nilsson, O.; Ny, L.; Nilsson, L.M.; et al. HER2 CAR-T Cells Eradicate Uveal Melanoma and T-Cell Therapy-Resistant Human Melanoma in IL2 Transgenic NOD/SCID IL2 Receptor Knockout Mice. Cancer Res. 2019, 79, 899–904. [Google Scholar] [CrossRef] [PubMed]
- Forsberg, E.M.V.; Riise, R.; Saellström, S.; Karlsson, J.; Alsén, S.; Bucher, V.; Hemminki, A.E.; Olofsson Bagge, R.; Ny, L.; Nilsson, L.M.; et al. Treatment with Anti-HER2 Chimeric Antigen Receptor Tumor-Infiltrating Lymphocytes (CAR-TILs) Is Safe and Associated with Antitumor Efficacy in Mice and Companion Dogs. Cancers 2023, 15, 648. [Google Scholar] [CrossRef] [PubMed]
- Jilani, S.; Saco, J.D.; Mugarza, E.; Pujol-Morcillo, A.; Chokry, J.; Ng, C.; Abril-Rodriguez, G.; Berger-Manerio, D.; Pant, A.; Hu, J.; et al. CAR-T Cell Therapy Targeting Surface Expression of TYRP1 to Treat Cutaneous and Rare Melanoma Subtypes. Nat. Commun. 2024, 15, 1244. [Google Scholar] [CrossRef] [PubMed]
- Saini, S.K.; Ørskov, A.D.; Bjerregaard, A.-M.; Unnikrishnan, A.; Holmberg-Thydén, S.; Borch, A.; Jensen, K.V.; Anande, G.; Bentzen, A.K.; Marquard, A.M.; et al. Human Endogenous Retroviruses Form a Reservoir of T Cell Targets in Hematological Cancers. Nat. Commun. 2020, 11, 5660. [Google Scholar] [CrossRef] [PubMed]
- Bendall, M.L.; Francis, J.H.; Shoushtari, A.N.; Nixon, D.F. Specific Human Endogenous Retroviruses Predict Metastatic Potential in Uveal Melanoma. JCI Insight 2022, 7, e147172. [Google Scholar] [CrossRef] [PubMed]
- Aughton, K.; Shahidipour, H.; Djirackor, L.; Coupland, S.E.; Kalirai, H. Characterization of Uveal Melanoma Cell Lines and Primary Tumor Samples in 3D Culture. Transl. Vis. Sci. Technol. 2020, 9, 39. [Google Scholar] [CrossRef] [PubMed]
- Farhoumand, L.S.; Fiorentzis, M.; Kraemer, M.M.; Sak, A.; Stuschke, M.; Rassaf, T.; Hendgen-Cotta, U.; Bechrakis, N.E.; Berchner-Pfannschmidt, U. The Adrenergic Receptor Antagonist Carvedilol Elicits Anti-Tumor Responses in Uveal Melanoma 3D Tumor Spheroids and May Serve as Co-Adjuvant Therapy with Radiation. Cancers 2022, 14, 3097. [Google Scholar] [CrossRef]
- Baqai, U.; Purwin, T.J.; Bechtel, N.; Chua, V.; Han, A.; Hartsough, E.J.; Kuznetsoff, J.N.; Harbour, J.W.; Aplin, A.E. Multi-Omics Profiling Shows BAP1 Loss Is Associated with Upregulated Cell Adhesion Molecules in Uveal Melanoma. Mol. Cancer Res. 2022, 20, 1260–1271. [Google Scholar] [CrossRef]
- Farhoumand, L.S.; Liu, H.; Tsimpaki, T.; Hendgen-Cotta, U.B.; Rassaf, T.; Bechrakis, N.E.; Fiorentzis, M.; Berchner-Pfannschmidt, U. Blockade of SS-Adrenergic Receptors by Nebivolol Enables Tumor Control Potential for Uveal Melanoma in 3D Tumor Spheroids and 2D Cultures. Int. J. Mol. Sci. 2023, 24, 5894. [Google Scholar] [CrossRef] [PubMed]
- Gonçalves, J.; Emmons, M.F.; Faião-Flores, F.; Aplin, A.E.; Harbour, J.W.; Licht, J.D.; Wink, M.R.; Smalley, K.S.M. Decitabine Limits Escape from MEK Inhibition in Uveal Melanoma. Pigment. Cell Melanoma Res. 2020, 33, 507–514. [Google Scholar] [CrossRef] [PubMed]
- Kraemer, M.M.; Tsimpaki, T.; Berchner-Pfannschmidt, U.; Bechrakis, N.E.; Seitz, B.; Fiorentzis, M. Calcium Electroporation Reduces Viability and Proliferation Capacity of Four Uveal Melanoma Cell Lines in 2D and 3D Cultures. Cancers 2022, 14, 2889. [Google Scholar] [CrossRef] [PubMed]
- Sokolenko, E.A.; Berchner-Pfannschmidt, U.; Ting, S.C.; Schmid, K.W.; Bechrakis, N.E.; Seitz, B.; Tsimpaki, T.; Kraemer, M.M.; Fiorentzis, M. Optimisation of the Chicken Chorioallantoic Membrane Assay in Uveal Melanoma Research. Pharmaceutics 2021, 14, 13. [Google Scholar] [CrossRef] [PubMed]
- Weidmann, C.; Bérubé, J.; Piquet, L.; de la Fouchardière, A.; Landreville, S. Expression of the Serotonin Receptor 2B in Uveal Melanoma and Effects of an Antagonist on Cell Lines. Clin. Exp. Metastasis 2018, 35, 123–134. [Google Scholar] [CrossRef] [PubMed]
- Richards, J.R.; Yoo, J.H.; Shin, D.; Odelberg, S.J. Mouse Models of Uveal Melanoma: Strengths, Weaknesses, and Future Directions. Pigment. Cell Melanoma Res. 2020, 33, 264–278. [Google Scholar] [CrossRef] [PubMed]
- Stei, M.M.; Loeffler, K.U.; Holz, F.G.; Herwig, M.C. Animal Models of Uveal Melanoma: Methods, Applicability, and Limitations. Biomed. Res. Int. 2016, 2016, 4521807. [Google Scholar] [CrossRef] [PubMed]
- Yin, J.; Zhao, G.; Kalirai, H.; Coupland, S.E.; Jochemsen, A.G.; Forn-Cuní, G.; Wierenga, A.P.A.; Jager, M.J.; Snaar-Jagalska, B.E.; Groenewoud, A. Zebrafish Patient-Derived Xenograft Model as a Preclinical Platform for Uveal Melanoma Drug Discovery. Pharmaceuticals 2023, 16, 598. [Google Scholar] [CrossRef] [PubMed]
- Bérubé, M.; Deschambeault, A.; Boucher, M.; Germain, L.; Petitclerc, E.; Guérin, S.L. MMP-2 Expression in Uveal Melanoma: Differential Activation Status Dictated by the Cellular Environment. Mol. Vis. 2005, 11, 1101–1111. [Google Scholar]
- Tsimpaki, T.; Anastasova, R.; Liu, H.; Seitz, B.; Bechrakis, N.E.; Berchner-Pfannschmidt, U.; Kraemer, M.M.; Fiorentzis, M. Calcium Electroporation versus Electrochemotherapy with Bleomycin in an In Vivo CAM-Based Uveal Melanoma Xenograft Model. Int. J. Mol. Sci. 2024, 25, 938. [Google Scholar] [CrossRef]
- Kuznetsoff, J.N.; Owens, D.A.; Lopez, A.; Rodriguez, D.A.; Chee, N.T.; Kurtenbach, S.; Bilbao, D.; Roberts, E.R.; Volmar, C.-H.; Wahlestedt, C.; et al. Dual Screen for Efficacy and Toxicity Identifies HDAC Inhibitor with Distinctive Activity Spectrum for BAP1-Mutant Uveal Melanoma. Mol. Cancer Res. 2021, 19, 215–222. [Google Scholar] [CrossRef]
- Nemati, F.; De Koning, L.; Gentien, D.; Assayag, F.; Henry, E.; Ait Rais, K.; Pierron, G.; Mariani, O.; Nijnikoff, M.; Champenois, G.; et al. Patient Derived Xenografts (PDX) Models as an Avatar to Assess Personalized Therapy Options in Uveal Melanoma: A Feasibility Study. Curr. Oncol. 2023, 30, 9090–9103. [Google Scholar] [CrossRef] [PubMed]
- Lescot, T.; Lebel-Cormier, M.-A.; Seniwal, B.; Gros-Louis, P.; Bellerive, C.; Landreville, S.; Beaulieu, L.; Fortin, M.-A. Tumor Shape-Specific Brachytherapy Implants by 3D-Printing, Precision Radioactivity Painting, and Biomedical Imaging. Adv. Health Mater. 2023, 12, e2300528. [Google Scholar] [CrossRef] [PubMed]
- Roy, V.; Magne, B.; Vaillancourt-Audet, M.; Blais, M.; Chabaud, S.; Grammond, E.; Piquet, L.; Fradette, J.; Laverdière, I.; Moulin, V.J.; et al. Human Organ-Specific 3D Cancer Models Produced by the Stromal Self-Assembly Method of Tissue Engineering for the Study of Solid Tumors. Biomed. Res. Int. 2020, 2020, 6051210. [Google Scholar] [CrossRef] [PubMed]
- Ventin, M.; Cattaneo, G.; Arya, S.; Jia, J.; Gelmi, M.C.; Sun, Y.; Maggs, L.; Ksander, B.R.; Verdijk, R.M.; Boland, G.M.; et al. Chimeric Antigen Receptor T Cell with an Inducible Caspase 9 Suicide Gene Eradicates Uveal Melanoma Liver Metastases via B7-H3 Targeting. Clin. Cancer Res. 2024. [Google Scholar] [CrossRef] [PubMed]
- Chattopadhyay, C.; Kim, D.W.; Gombos, D.S.; Oba, J.; Qin, Y.; Williams, M.D.; Esmaeli, B.; Grimm, E.A.; Wargo, J.A.; Woodman, S.E.; et al. Uveal Melanoma: From Diagnosis to Treatment and the Science in Between. Cancer 2016, 122, 2299–2312. [Google Scholar] [CrossRef] [PubMed]
- Piulats, J.M.; Watkins, C.; Costa-García, M.; Del Carpio, L.; Piperno-Neumann, S.; Rutkowski, P.; Hassel, J.C.; Espinosa, E.; De La Cruz-Merino, L.; Ochsenreither, S.; et al. Overall Survival from Tebentafusp versus Nivolumab plus Ipilimumab in First-Line Metastatic Uveal Melanoma: A Propensity Score-Weighted Analysis. Ann. Oncol. 2023, 35, 317–326. [Google Scholar] [CrossRef] [PubMed]
- Lapadula, D.; Farias, E.; Randolph, C.E.; Purwin, T.J.; McGrath, D.; Charpentier, T.H.; Zhang, L.; Wu, S.; Terai, M.; Sato, T.; et al. Effects of Oncogenic Gαq and Gα11 Inhibition by FR900359 in Uveal Melanoma. Mol. Cancer Res. 2019, 17, 963–973. [Google Scholar] [CrossRef] [PubMed]
- Roelofs, K.A.; Grewal, P.; Lapere, S.; Larocque, M.; Murtha, A.; Weis, E. Optimising Prediction of Early Metastasis-Free Survival in Uveal Melanoma Using a Four-Category Model Incorporating Gene Expression Profile and Tumour Size. Br. J. Ophthalmol. 2022, 106, 724–730. [Google Scholar] [CrossRef]
- Hussain, R.N.; Coupland, S.E.; Kalirai, H.; Taktak, A.F.G.; Eleuteri, A.; Damato, B.E.; Groenewald, C.; Heimann, H. Small High-Risk Uveal Melanomas Have a Lower Mortality Rate. Cancers 2021, 13, 2267. [Google Scholar] [CrossRef]
- Schank, T.E.; Hassel, J.C. Immunotherapies for the Treatment of Uveal Melanoma-History and Future. Cancers 2019, 11, 1048. [Google Scholar] [CrossRef] [PubMed]
- Chen, Y.; Chen, X.; Wang, X. Identification of a Prognostic Model Using Cuproptosis-Related Genes in Uveal Melanoma. Front. Cell Dev. Biol. 2022, 10, 973073. [Google Scholar] [CrossRef] [PubMed]
- Lamas, N.J.; Martel, A.; Nahon-Estève, S.; Goffinet, S.; Macocco, A.; Bertolotto, C.; Lassalle, S.; Hofman, P. Prognostic Biomarkers in Uveal Melanoma: The Status Quo, Recent Advances and Future Directions. Cancers 2021, 14, 96. [Google Scholar] [CrossRef] [PubMed]
- Grewal, D.S.; Cummings, T.J.; Mruthyunjaya, P. Outcomes of 27-Gauge Vitrectomy-Assisted Choroidal and Subretinal Biopsy. Ophthalmic Surg. Lasers Imaging Retin. 2017, 48, 406–415. [Google Scholar] [CrossRef]
- Salarian, M.; Yang, H.; Turaga, R.C.; Tan, S.; Qiao, J.; Xue, S.; Gui, Z.; Peng, G.; Han, H.; Mittal, P.; et al. Precision Detection of Liver Metastasis by Collagen-Targeted Protein MRI Contrast Agent. Biomaterials 2019, 224, 119478. [Google Scholar] [CrossRef]
- Zhou, Z.; Qutaish, M.; Han, Z.; Schur, R.M.; Liu, Y.; Wilson, D.L.; Lu, Z.-R. MRI Detection of Breast Cancer Micrometastases with a Fibronectin-Targeting Contrast Agent. Nat. Commun. 2015, 6, 7984. [Google Scholar] [CrossRef] [PubMed]
- Li, J.; Yang, S.; Liu, Z.; Wang, G.; He, P.; Wei, W.; Yang, M.; Deng, Y.; Gu, P.; Xie, X.; et al. Imaging Cellular Aerobic Glycolysis Using Carbon Dots for Early Warning of Tumorigenesis. Adv. Mater. 2021, 33, e2005096. [Google Scholar] [CrossRef]
- Ophir, J.; Céspedes, I.; Ponnekanti, H.; Yazdi, Y.; Li, X. Elastography: A Quantitative Method for Imaging the Elasticity of Biological Tissues. Ultrason. Imaging 1991, 13, 111–134. [Google Scholar] [CrossRef]
- Chen, W.; Yang, W.; Li, D.; Wang, Z.; Zhao, Q.; Li, Y.; Cui, R.; Shen, L. Value of the Strain Ratio in the Differential Diagnosis of Intraocular Tumors by Elastosonography: A Retrospective Case-Control Study. Indian. J. Ophthalmol. 2023, 71, 983–988. [Google Scholar] [CrossRef] [PubMed]
- Spencer, C.N.; McQuade, J.L.; Gopalakrishnan, V.; McCulloch, J.A.; Vetizou, M.; Cogdill, A.P.; Khan, M.A.W.; Zhang, X.; White, M.G.; Peterson, C.B.; et al. Dietary Fiber and Probiotics Influence the Gut Microbiome and Melanoma Immunotherapy Response. Science 2021, 374, 1632–1640. [Google Scholar] [CrossRef]
- Routy, B.; Lenehan, J.G.; Miller, W.H.; Jamal, R.; Messaoudene, M.; Daisley, B.A.; Hes, C.; Al, K.F.; Martinez-Gili, L.; Punčochář, M.; et al. Fecal Microbiota Transplantation plus Anti-PD-1 Immunotherapy in Advanced Melanoma: A Phase I Trial. Nat. Med. 2023, 29, 2121–2132. [Google Scholar] [CrossRef] [PubMed]
- Brănişteanu, D.E.; Porumb-Andrese, E.; Porumb, V.; Stărică, A.; Moraru, A.D.; Nicolescu, A.C.; Zemba, M.; Brănişteanu, C.I.; Brănişteanu, G.; Brănişteanu, D.C. New Treatment Horizons in Uveal and Cutaneous Melanoma. Life 2023, 13, 1666. [Google Scholar] [CrossRef] [PubMed]
- Chandrabhatla, A.S.; Horgan, T.M.; Cotton, C.C.; Ambati, N.K.; Shildkrot, Y.E. Clinical Applications of Machine Learning in the Management of Intraocular Cancers: A Narrative Review. Investig. Ophthalmol. Vis. Sci. 2023, 64, 29. [Google Scholar] [CrossRef] [PubMed]
- Koseoglu, N.D.; Corrêa, Z.M.; Liu, T.Y.A. Artificial Intelligence for Ocular Oncology. Curr. Opin. Ophthalmol. 2023, 34, 437–440. [Google Scholar] [CrossRef]
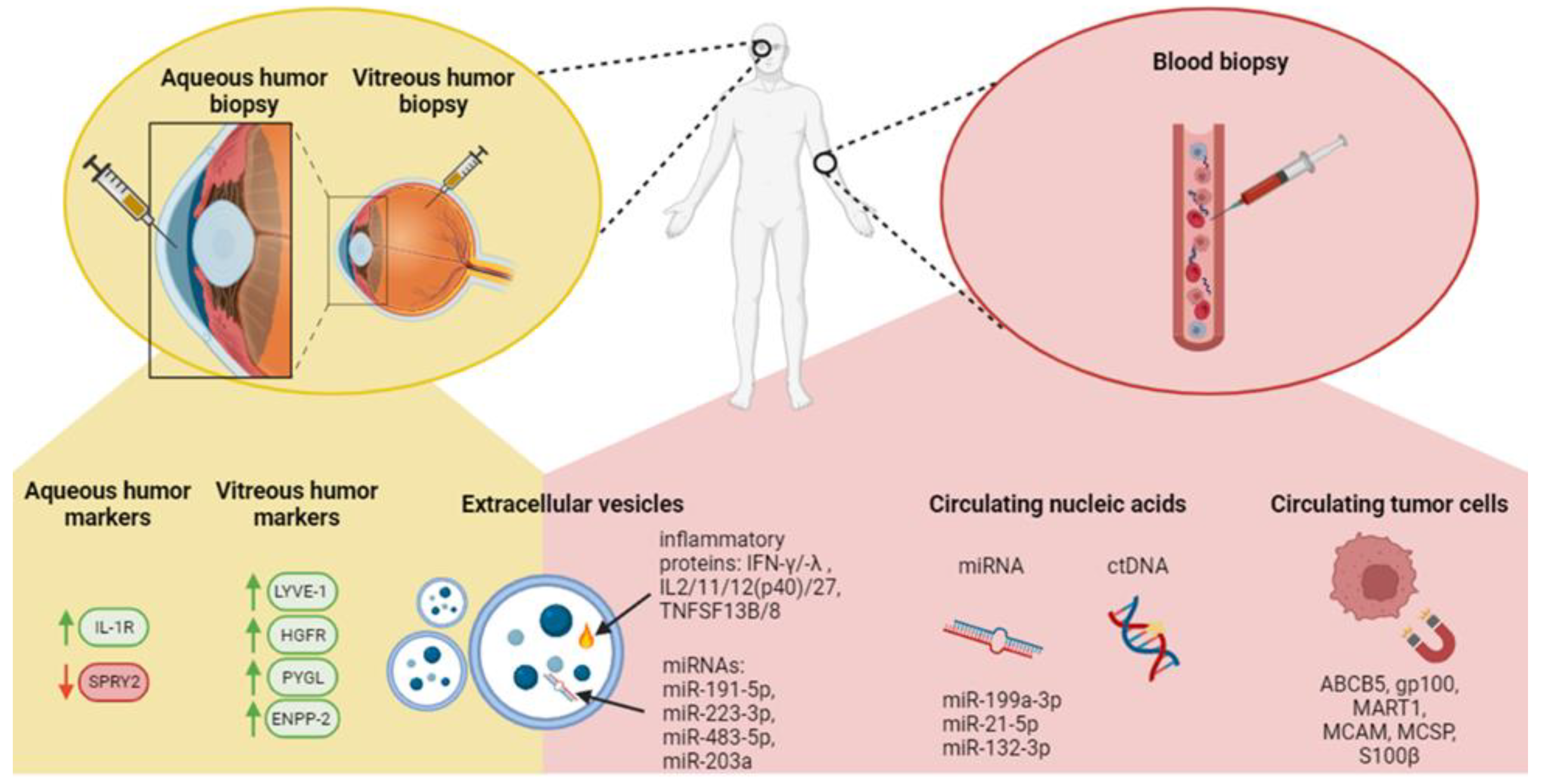
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Fuentes-Rodriguez, A.; Mitchell, A.; Guérin, S.L.; Landreville, S. Recent Advances in Molecular and Genetic Research on Uveal Melanoma. Cells 2024, 13, 1023. https://doi.org/10.3390/cells13121023
Fuentes-Rodriguez A, Mitchell A, Guérin SL, Landreville S. Recent Advances in Molecular and Genetic Research on Uveal Melanoma. Cells. 2024; 13(12):1023. https://doi.org/10.3390/cells13121023
Chicago/Turabian StyleFuentes-Rodriguez, Aurélie, Andrew Mitchell, Sylvain L. Guérin, and Solange Landreville. 2024. "Recent Advances in Molecular and Genetic Research on Uveal Melanoma" Cells 13, no. 12: 1023. https://doi.org/10.3390/cells13121023
APA StyleFuentes-Rodriguez, A., Mitchell, A., Guérin, S. L., & Landreville, S. (2024). Recent Advances in Molecular and Genetic Research on Uveal Melanoma. Cells, 13(12), 1023. https://doi.org/10.3390/cells13121023







