Applications of Functionalized Carbon Nanotubes for the Therapy and Diagnosis of Cancer
Abstract
:1. Introduction
2. Carbon Nanotubes (CNTs) as Carriers of Molecules, Genes, and Proteins
2.1. CNTs as Carriers of Anticancer Molecules
2.2. CNTs as Carriers for Gene Therapy
2.3. CNTs as Carriers of Other Compounds
3. CNTs as Imaging Sources for Cancer Detection
3.1. CNTs for Fluorescence Imaging
3.2. CNTs for Raman Imaging
3.3. CNTs for Photoacoustic (PA) Imaging
3.4. CNTs for Magnetic Resonance Imaging (MRI)
4. Conclusions and Perspectives
Acknowledgments
Conflicts of Interest
References
- Ma, D.D.; Yang, W.X. Engineered nanoparticles induce cell apoptosis: Potential for cancer therapy. Oncotarget 2016, 7, 40882–40903. [Google Scholar] [CrossRef] [PubMed]
- Luo, J.; Solimini, N.L.; Elledge, S.J. Principles of cancer therapy: Oncogene and non-oncogene addiction. Cell 2009, 136, 823–837. [Google Scholar] [CrossRef] [PubMed]
- Hanahan, D.; Weinberg, R.A. The hallmarks of cancer. Cell 2000, 100, 57–70. [Google Scholar] [CrossRef]
- Ariga, K.; Minami, K.; Ebara, M.; Nakanishi, J. What are the emerging concepts and challenges in nano? Nanoarchitectonics, hand-operating nanotechnology and mechanobiology. Polym. J. 2016, 48, 371–389. [Google Scholar] [CrossRef]
- Aono, M.; Ariga, K. The way to nanoarchitectonics and the way of nanoarchitectonics. Adv. Mater. 2016, 28, 989–992. [Google Scholar] [CrossRef] [PubMed]
- Ariga, K.; Ji, Q.M.; Nakanishi, W.; Hill, J.P.; Aono, M. Nanoarchitectonics: A new materials horizon for nanotechnology. Mater. Horiz. 2015, 2, 406–413. [Google Scholar] [CrossRef]
- Nakanishi, W.; Minami, K.; Shrestha, L.K.; Ji, Q.M.; Hill, J.P.; Ariga, K. Bioactive nanocarbon assemblies: Nanoarchitectonics and applications. Nano Today 2014, 9, 378–394. [Google Scholar] [CrossRef]
- Ariga, K.; Kawakami, K.; Ebara, M.; Kotsuchibashi, Y.; Ji, Q.M.; Hill, J.P. Bioinspired nanoarchitectonics as emerging drug delivery systems. New J. Chem. 2014, 38, 5149–5163. [Google Scholar] [CrossRef]
- Moghimi, S.M.; Hunter, A.C.; Murray, J.C. Long-circulating and target-specific nanoparticles: Theory to practice. Pharmacol. Rev. 2001, 53, 283–318. [Google Scholar] [PubMed]
- Zhang, L.; Gu, F.X.; Chan, J.M.; Wang, A.Z.; Langer, R.S.; Farokhzad, O.C. Nanoparticles in medicine: Therapeutic applications and developments. Clin. Pharmacol. Ther. 2008, 83, 761–769. [Google Scholar] [CrossRef] [PubMed]
- Iijima, S. Helical microtubules of graphitic carbon. Nature 1991, 354, 56–58. [Google Scholar] [CrossRef]
- Lainioti, G.C.; Bounos, G.; Voyiatzis, G.A.; Kallitsis, J.K. Enhanced water vapor transmission through porous membranes based on melt blending of polystyrene sulfonate with polyethylene copolymers and their cnt nanocomposites. Polymers 2016, 8, 190. [Google Scholar] [CrossRef]
- Elhissi, A.; Ahmed, W.; Dhanak, V.R.; Subramani, K. Carbon nanotubes in cancer therapy and drug delivery. Micro Nano Technol. 2012, 2012, 347–363. [Google Scholar] [CrossRef] [PubMed]
- Wu, W.; Li, R.T.; Bian, X.C.; Zhu, Z.S.; Ding, D.; Li, X.L.; Jia, Z.J.; Jiang, X.Q.; Hu, Y.Q. Covalently combining carbon nanotubes with anticancer agent: Preparation and antitumor activity. ACS Nano 2009, 3, 2740–2750. [Google Scholar] [CrossRef] [PubMed]
- Sahoo, N.G.; Bao, H.; Pan, Y.; Pal, M.; Kakran, M.; Cheng, H.K.; Li, L.; Tan, L.P. Functionalized carbon nanomaterials as nanocarriers for loading and delivery of a poorly water-soluble anticancer drug: A comparative study. Chem. Commun. 2011, 47, 5235–5237. [Google Scholar] [CrossRef] [PubMed]
- Tian, Z.; Yin, M.; Ma, H.; Zhu, L.; Shen, H.; Jia, N. Supramolecular assembly and antitumor activity of multiwalled carbon nanotube-camptothecin complexes. J. Nanosci. Nanotechnol. 2011, 11, 953–958. [Google Scholar] [CrossRef] [PubMed]
- Tripisciano, C.; Rummeli, M.H.; Chen, X.C.; Borowiak-Palen, E. Multi-wall carbon nanotubes—A vehicle for targeted irinotecan drug delivery. Phys. Status Solidi B 2010, 247, 2673–2677. [Google Scholar] [CrossRef]
- Ali-Boucetta, H.; Al-Jamal, K.T.; McCarthy, D.; Prato, M.; Bianco, A.; Kostarelos, K. Multiwalled carbon nanotube-doxorubicin supramolecular complexes for cancer therapeutics. Chem. Commun. 2008, 4, 459–461. [Google Scholar] [CrossRef] [PubMed]
- Liu, Z.; Sun, X.M.; Nakayama-Ratchford, N.; Dai, H.J. Supramolecular chemistry on water-soluble carbon nanotubes for drug loading and delivery. ACS Nano 2007, 1, 50–56. [Google Scholar] [CrossRef] [PubMed]
- Dinan, N.M.; Atyabi, F.; Rouini, M.R.; Amini, M.; Golabchifar, A.A.; Dinarvand, R. Doxorubicin loaded folate-targeted carbon nanotubes: Preparation, cellular internalization, in vitro cytotoxicity and disposition kinetic study in the isolated perfused rat liver. Mater. Sci. Eng. C 2014, 39, 47–55. [Google Scholar] [CrossRef] [PubMed]
- Zhang, X.; Meng, L.; Lu, Q.; Fei, Z.; Dyson, P.J. Targeted delivery and controlled release of doxorubicin to cancer cells using modified single wall carbon nanotubes. Biomaterials 2009, 30, 6041–6047. [Google Scholar] [CrossRef] [PubMed]
- Li, R.B.; Wu, R.A.; Zhao, L.A.; Hu, Z.Y.; Guo, S.J.; Pan, X.L.; Zou, H.F. Folate and iron difunctionalized multiwall carbon nanotubes as dual-targeted drug nanocarrier to cancer cells. Carbon 2011, 49, 1797–1805. [Google Scholar] [CrossRef]
- Dhar, S.; Liu, Z.; Thomale, J.; Dai, H.J.; Lippard, S.J. Targeted single-wall carbon nanotube-mediated pt(iv) prodrug delivery using folate as a homing device. J. Am. Chem. Soc. 2008, 130, 11467–11476. [Google Scholar] [CrossRef] [PubMed]
- Hampel, S.; Kunze, D.; Haase, D.; Kramer, K.; Rauschenbach, M.; Ritschel, M.; Leonhardt, A.; Thomas, J.; Oswald, S.; Hoffmann, V.; et al. Carbon nanotubes filled with a chemotherapeutic agent: A nanocarrier mediates inhibition of tumor cell growth. Nanomedicine 2008, 3, 175–182. [Google Scholar] [CrossRef] [PubMed]
- Liu, Z.; Chen, K.; Davis, C.; Sherlock, S.; Cao, Q.Z.; Chen, X.Y.; Dai, H.J. Drug delivery with carbon nanotubes for in vivo cancer treatment. Cancer Res. 2008, 68, 6652–6660. [Google Scholar] [CrossRef] [PubMed]
- Lay, C.L.; Liu, H.Q.; Tan, H.R.; Liu, Y. Delivery of paclitaxel by physically loading onto poly(ethylene glycol) (peg)-graft-carbon nanotubes for potent cancer therapeutics. Nanotechnology 2010, 21, 065101. [Google Scholar] [CrossRef] [PubMed]
- Singh, R.; Pantarotto, D.; McCarthy, D.; Chaloin, O.; Hoebeke, J.; Partidos, C.D.; Briand, J.P.; Prato, M.; Bianco, A.; Kostarelos, K. Binding and condensation of plasmid DNA onto functionalized carbon nanotubes: Toward the construction of nanotube-based gene delivery vectors. J. Am. Chem. Soc. 2005, 127, 4388–4396. [Google Scholar] [CrossRef] [PubMed]
- Geyik, C.; Evran, S.; Timur, S.; Telefoncu, A. The covalent bioconjugate of multiwalled carbon nanotube and amino-modified linearized plasmid DNA for gene delivery. Biotechnol. Prog. 2014, 30, 224–232. [Google Scholar] [CrossRef] [PubMed]
- Liu, G.L.; Wang, Y.; Hu, Y.; Yu, X.B.; Zhu, B.; Wang, G.X. Functionalized multi-wall carbon nanotubes enhance transfection and expression efficiency of plasmid DNA in fish cells. Int. J. Mol. Sci. 2016, 17, 335. [Google Scholar] [CrossRef] [PubMed]
- Karmakar, A.; Bratton, S.M.; Dervishi, E.; Ghosh, A.; Mahmood, M.; Xu, Y.; Saeed, L.M.; Mustafa, T.; Casciano, D.; Radominska-Pandya, A.; et al. Ethylenediamine functionalized-single-walled nanotube (f-SWNT)-assisted in vitro delivery of the oncogene suppressor p53 gene to breast cancer MCF-7 cells. Int. J. Nanomed. 2011, 6, 1045–1055. [Google Scholar]
- Pantarotto, D.; Singh, R.; McCarthy, D.; Erhardt, M.; Briand, J.P.; Prato, M.; Kostarelos, K.; Bianco, A. Functionalized carbon nanotubes for plasmid DNA gene delivery. Angew. Chem. Int. Ed. 2004, 43, 5242–5246. [Google Scholar] [CrossRef] [PubMed]
- Gao, L.Z.; Nie, L.; Wang, T.H.; Qin, Y.J.; Guo, Z.X.; Yang, D.L.; Yan, X.Y. Carbon nanotube delivery of the GFP gene into mammalian cells. Chembiochem 2006, 7, 239–242. [Google Scholar] [CrossRef] [PubMed]
- Wang, X.; Ren, J.; Qu, X. Targeted rna interference of cyclin a2 mediated by functionalized single-walled carbon nanotubes induces proliferation arrest and apoptosis in chronic myelogenous leukemia k562 cells. ChemMedChem 2008, 3, 940–945. [Google Scholar] [CrossRef] [PubMed]
- Podesta, J.E.; Al-Jamal, K.T.; Herrero, M.A.; Tian, B.; Ali-Boucetta, H.; Hegde, V.; Bianco, A.; Prato, M.; Kostarelos, K. Antitumor activity and prolonged survival by carbon-nanotube-mediated therapeutic sirna silencing in a human lung xenograft model. Small 2009, 5, 1176–1185. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Z.H.; Yang, X.Y.; Zhang, Y.; Zeng, B.; Wang, Z.J.; Zhu, T.H.; Roden, R.B.S.; Chen, Y.S.; Yang, R.C. Delivery of telomerase reverse transcriptase small interfering RNA in complex with positively charged single-walled carbon nanotubes suppresses tumor growth. Clin. Cancer Res. 2006, 12, 4933–4939. [Google Scholar] [CrossRef] [PubMed]
- Varkouhi, A.K.; Foillard, S.; Lammers, T.; Schiffelers, R.M.; Doris, E.; Hennink, W.E.; Storm, G. SiRNA delivery with functionalized carbon nanotubes. Int. J. Pharm. 2011, 416, 419–425. [Google Scholar] [CrossRef] [PubMed]
- Bartholomeusz, G.; Cherukuri, P.; Kingston, J.; Cognet, L.; Lemos, R.; Leeuw, T.K.; Gumbiner-Russo, L.; Weisman, R.B.; Powis, G. In vivo therapeutic silencing of hypoxia-inducible factor 1 alpha (hif-1α) using single-walled carbon nanotubes noncovalently coated with siRNA. Nano Res. 2009, 2, 279–291. [Google Scholar] [CrossRef] [PubMed]
- Guo, C.; Al-Jamal, W.T.; Toma, F.M.; Bianco, A.; Prato, M.; Al-Jamal, K.T.; Kostarelos, K. Design of cationic multiwalled carbon nanotubes as efficient siRNA vectors for lung cancer xenograft eradication. Bioconjug. Chem. 2015, 26, 1370–1379. [Google Scholar] [CrossRef] [PubMed]
- Pan, B.F.; Cui, D.X.; Xu, P.; Ozkan, C.; Feng, G.; Ozkan, M.; Huang, T.; Chu, B.F.; Li, Q.; He, R.; et al. Synthesis and characterization of polyamidoamine dendrimer-coated multi-walled carbon nanotubes and their application in gene delivery systems. Nanotechnology 2009, 20, 183–187. [Google Scholar] [CrossRef] [PubMed]
- Van den Bossche, J.; Al-Jamal, W.T.; Tian, B.W.; Nunes, A.; Fabbro, C.; Bianco, A.; Prato, M.; Kostarelos, K. Efficient receptor-independent intracellular translocation of aptamers mediated by conjugation to carbon nanotubes. Chem. Commun. 2010, 46, 7379–7381. [Google Scholar] [CrossRef] [PubMed]
- Ruggiero, A.; Villa, C.H.; Holland, J.P.; Sprinkle, S.R.; May, C.; Lewis, J.S.; Scheinberg, D.A.; McDevitt, M.R. Imaging and treating tumor vasculature with targeted radiolabeled carbon nanotubes. Int. J. Nanomed. 2010, 5, 783–802. [Google Scholar]
- Meng, J.; Yang, M.; Jia, F.M.; Kong, H.; Zhang, W.Q.; Wang, C.Y.; Xing, J.M.; Xie, S.S.; Xu, H.Y. Subcutaneous injection of water-soluble multi-walled carbon nanotubes in tumor-bearing mice boosts the host immune activity. Nanotechnology 2010, 21, 145104–145112. [Google Scholar] [CrossRef] [PubMed]
- VanHandel, M.; Alizadeh, D.; Zhang, L.; Kateb, B.; Bronikowski, M.; Manohara, H.; Badie, B. Selective uptake of multi-walled carbon nanotubes by tumor macrophages in a murine glioma model. J. Neuroimmunol. 2009, 208, 3–9. [Google Scholar] [CrossRef] [PubMed]
- Ouyang, M.; White, E.E.; Ren, H.; Guo, Q.; Zhang, I.; Gao, H.; Yanyan, S.; Chen, X.; Weng, Y.; Da Fonseca, A.; et al. Metronomic doses of temozolomide enhance the efficacy of carbon nanotube CPG immunotherapy in an invasive glioma model. PLoS ONE 2016, 11, e0148139. [Google Scholar] [CrossRef] [PubMed]
- Fadel, T.R.; Sharp, F.A.; Vudattu, N.; Ragheb, R.; Garyu, J.; Kim, D.; Hong, E.; Li, N.; Haller, G.L.; Pfefferle, L.D.; et al. A carbon nanotube-polymer composite for T-cell therapy. Nat. Nanotechnol. 2014, 9, 639–647. [Google Scholar] [CrossRef] [PubMed]
- Shi Kam, N.W.; Jessop, T.C.; Wender, P.A.; Dai, H. Nanotube molecular transporters: Internalization of carbon nanotube-protein conjugates into mammalian cells. J. Am. Chem. Soc. 2004, 126, 6850–6851. [Google Scholar] [CrossRef] [PubMed]
- Weng, X.X.; Wang, M.Y.; Ge, J.; Yu, S.N.; Liu, B.H.; Zhong, J.; Kong, J.L. Carbon nanotubes as a protein toxin transporter for selective her2-positive breast cancer cell destruction. Mol. Biosyst. 2009, 5, 1224–1231. [Google Scholar] [CrossRef] [PubMed]
- Welsher, K.; Liu, Z.; Sherlock, S.P.; Robinson, J.T.; Chen, Z.; Daranciang, D.; Dai, H.J. A route to brightly fluorescent carbon nanotubes for near-infrared imaging in mice. Nat. Nanotechnol. 2009, 4, 773–780. [Google Scholar] [CrossRef] [PubMed]
- Robinson, J.T.; Hong, G.S.; Liang, Y.Y.; Zhang, B.; Yaghi, O.K.; Dai, H.J. In vivo fluorescence imaging in the second near-infrared window with long circulating carbon nanotubes capable of ultrahigh tumor uptake. J. Am. Chem. Soc. 2012, 134, 10664–10669. [Google Scholar] [CrossRef] [PubMed]
- Ghosh, D.; Bagley, A.F.; Na, Y.J.; Birrer, M.J.; Bhatia, S.N.; Belcher, A.M. Deep, noninvasive imaging and surgical guidance of submillimeter tumors using targeted m13-stabilized single-walled carbon nanotubes. Proc. Natl. Acad. Sci. USA 2014, 111, 13948–13953. [Google Scholar] [CrossRef] [PubMed]
- Antaris, A.L.; Robinson, J.T.; Yaghi, O.K.; Hong, G.S.; Diao, S.; Luong, R.; Dai, H.J. Ultra-low doses of chirality sorted (6,5) carbon nanotubes for simultaneous tumor imaging and photothermal therapy. ACS Nano 2013, 7, 3644–3652. [Google Scholar] [CrossRef] [PubMed]
- Lamprecht, C.; Gierlinger, N.; Heister, E.; Unterauer, B.; Plochberger, B.; Brameshuber, M.; Hinterdorfer, P.; Hild, S.; Ebner, A. Mapping the intracellular distribution of carbon nanotubes after targeted delivery to carcinoma cells using confocal Raman imaging as a label-free technique. J. Phys. Condens. Matter 2012, 24, 164206. [Google Scholar] [CrossRef] [PubMed]
- Zavaleta, C.; de la Zerda, A.; Liu, Z.; Keren, S.; Cheng, Z.; Schipper, M.; Chen, X.; Dai, H.; Gambhir, S.S. Noninvasive Raman spectroscopy in living mice for evaluation of tumor targeting with carbon nanotubes. Nano Lett. 2008, 8, 2800–2805. [Google Scholar] [CrossRef] [PubMed]
- Smith, B.R.; Zavaleta, C.; Rosenberg, J.; Tong, R.; Ramunas, J.; Liu, Z.; Dai, H.J.; Gambhir, S.S. High-resolution, serial intravital microscopic imaging of nanoparticle delivery and targeting in a small animal tumor model. Nano Today 2013, 8, 126–137. [Google Scholar] [CrossRef] [PubMed]
- Liu, Z.; Tabakman, S.; Sherlock, S.; Li, X.L.; Chen, Z.; Jiang, K.L.; Fan, S.S.; Dai, H.J. Multiplexed five-color molecular imaging of cancer cells and tumor tissues with carbon nanotube raman tags in the near-infrared. Nano Res. 2010, 3, 222–233. [Google Scholar] [CrossRef] [PubMed]
- De la Zerda, A.; Bodapati, S.; Teed, R.; May, S.Y.; Tabakman, S.M.; Liu, Z.; Khuri-Yakub, B.T.; Chen, X.Y.; Dai, H.J.; Gambhir, S.S. Family of enhanced photoacoustic imaging agents for high-sensitivity and multiplexing studies in living mice. ACS Nano 2012, 6, 4694–4701. [Google Scholar] [CrossRef] [PubMed]
- Galanzha, E.I.; Shashkov, E.V.; Kelly, T.; Kim, J.W.; Yang, L.L.; Zharov, V.P. In vivo magnetic enrichment and multiplex photoacoustic detection of circulating tumour cells. Nat. Nanotechnol. 2009, 4, 855–860. [Google Scholar] [CrossRef] [PubMed]
- Nguyen, V.P.; Oh, Y.; Ha, K.; Oh, J.; Kang, H.W. Enhancement of high-resolution photoacoustic imaging with indocyanine green-conjugated carbon nanotubes. Jpn. J. Appl. Phys. 2015, 54, 07HF04. [Google Scholar] [CrossRef]
- Xie, L.S.; Wang, G.H.; Zhou, H.; Zhang, F.; Guo, Z.D.; Liu, C.; Zhang, X.Z.; Zhu, L. Functional long circulating single walled carbon nanotubes for fluorescent/photoacoustic imaging-guided enhanced phototherapy. Biomaterials 2016, 103, 219–228. [Google Scholar] [CrossRef] [PubMed]
- Richard, C.; Doan, B.T.; Beloeil, J.C.; Bessodes, M.; Toth, E.; Scherman, D. Noncovalent functionalization of carbon nanotubes with amphiphilic GD3+ chelates: Toward powerful T1 and T2 MRI contrast agents. Nano Lett. 2008, 8, 232–236. [Google Scholar] [CrossRef] [PubMed]
- Marangon, I.; Menard-Moyon, C.; Kolosnjaj-Tabi, J.; Beoutis, M.L.; Lartigue, L.; Alloyeau, D.; Pach, E.; Ballesteros, B.; Autret, G.; Ninjbadgar, T.; et al. Covalent functionalization of multi-walled carbon nanotubes with a gadolinium chelate for efficient T-1-weighted magnetic resonance imaging. Adv. Funct. Mater. 2014, 24, 7173–7186. [Google Scholar]
- Wu, H.X.; Liu, G.; Wang, X.; Zhang, J.M.; Chen, Y.; Shi, J.L.; Yang, H.; Hu, H.; Yang, S.P. Solvothermal synthesis of cobalt ferrite nanoparticles loaded on multiwalled carbon nanotubes for magnetic resonance imaging and drug delivery. Acta Biomater. 2011, 7, 3496–3504. [Google Scholar] [CrossRef] [PubMed]
- Peci, T.; Dennis, T.J.S.; Baxendale, M. Iron-filled multiwalled carbon nanotubes surface-functionalized with paramagnetic Gd (III): A candidate dual-functioning MRI contrast agent and magnetic hyperthermia structure. Carbon 2015, 87, 226–232. [Google Scholar] [CrossRef]
- Wong, B.S.; Yoong, S.L.; Jagusiak, A.; Panczyk, T.; Ho, H.K.; Ang, W.H.; Pastorin, G. Carbon nanotubes for delivery of small molecule drugs. Adv. Drug Deliv. Rev. 2013, 65, 1964–2015. [Google Scholar] [CrossRef] [PubMed]
- Yang, F.; Jin, C.; Yang, D.; Jiang, Y.J.; Li, J.; Di, Y.; Hu, J.H.; Wang, C.C.; Ni, Q.X.; Fu, D.L. Magnetic functionalised carbon nanotubes as drug vehicles for cancer lymph node metastasis treatment. Eur. J. Cancer 2011, 47, 1873–1882. [Google Scholar] [CrossRef] [PubMed]
- Datir, S.R.; Das, M.; Singh, R.P.; Jain, S. Hyaluronate tethered, “smart” multiwalled carbon nanotubes for tumor-targeted delivery of doxorubicin. Bioconjug. Chem. 2012, 23, 2201–2213. [Google Scholar] [CrossRef] [PubMed]
- Shi, X.Y.; Wang, S.H.; Shen, M.W.; Antwerp, M.E.; Chen, X.S.; Li, C.; Petersen, E.J.; Huang, Q.G.; Weber, W.J.; Baker, J.R. Multifunctional dendrimer-modified multiwalled carbon nanotubes: Synthesis, characterization, and in vitro cancer cell targeting and imaging. Biomacromolecules 2009, 10, 1744–1750. [Google Scholar] [CrossRef] [PubMed]
- Yu, Y.; Kong, L.J.; Li, L.; Li, N.E.; Yan, P. Antitumor activity of doxorubicin-loaded carbon nanotubes incorporated poly(lactic-co-glycolic acid) electrospun composite nanofibers. Nanoscale Res. Lett. 2015, 10, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Tripisciano, C.; Kraemer, K.; Taylor, A.; Borowiak-Palen, E. Single-wall carbon nanotubes based anticancer drug delivery system. Chem. Phys. Lett. 2009, 478, 200–205. [Google Scholar] [CrossRef]
- Fonseca, C.; Simoes, S.; Gaspar, R. Paclitaxel-loaded plga nanoparticles: Preparation, physicochemical characterization and in vitro anti-tumoral activity. J. Control. Release 2002, 83, 273–286. [Google Scholar] [CrossRef]
- Li, C.; Yu, D.F.; Inoue, T.; Yang, D.J.; Milas, L.; Hunter, N.R.; Kim, E.E.; Wallace, S. Synthesis and evaluation of water-soluble polyethylene glycol-paclitaxel conjugate as a paclitaxel prodrug. Anti-Cancer Drug 1996, 7, 642–648. [Google Scholar] [CrossRef]
- Chan, J.Y.W.; Chu, A.C.Y.; Fung, K.P. Inhibition of p-glycoprotein expression and reversal of drug resistance of human hepatoma HEPG2 cells by multidrug resistance gene (MDR1) antisense RNA. Life Sci. 2000, 67, 2117–2124. [Google Scholar] [CrossRef]
- Suri, S.S.; Fenniri, H.; Singh, B. Nanotechnology-based drug delivery systems. J. Occup. Med. Toxicol. 2007, 2, 16. [Google Scholar] [CrossRef] [PubMed]
- Cheng, J.P.; Meziani, M.J.; Sun, Y.P.; Cheng, S.H. Poly(ethylene glycol)-conjugated multi-walled carbon nanotubes as an efficient drug carrier for overcoming multidrug resistance. Toxicol. Appl. Pharm. 2011, 250, 184–193. [Google Scholar] [CrossRef] [PubMed]
- Bates, K.; Kostarelos, K. Carbon nanotubes as vectors for gene therapy: Past achievements, present challenges and future goals. Adv. Drug Deliv. Rev. 2013, 65, 2023–2033. [Google Scholar] [CrossRef] [PubMed]
- Fortunati, E.; Bout, A.; Zanta, M.A.; Valerio, D.; Scarpa, M. In vitro and in vivo gene transfer to pulmonary cells mediated by cationic liposomes. Biochim. Biophys. Acta 1996, 1306, 55–62. [Google Scholar] [CrossRef]
- Rochat, T.; Morris, M.A. Gene therapy for cystic fibrosis by means of aerosol. J. Aerosol. Med. 2002, 15, 229–235. [Google Scholar] [CrossRef] [PubMed]
- Fischer, D.; Bieber, T.; Li, Y.; Elsasser, H.P.; Kissel, T. A novel non-viral vector for DNA delivery based on low molecular weight, branched polyethylenimine: Effect of molecular weight on transfection efficiency and cytotoxicity. Pharm. Res. 1999, 16, 1273–1279. [Google Scholar] [CrossRef] [PubMed]
- Coutelle, C.; Williamson, R. Liposomes and viruses for gene therapy of cystic fibrosis. J. Aerosol. Med. 1996, 9, 79–88. [Google Scholar] [CrossRef] [PubMed]
- Kostarelos, K.; Lacerda, L.; Pastorin, G.; Wu, W.; Wieckowski, S.; Luangsivilay, J.; Godefroy, S.; Pantarotto, D.; Briand, J.P.; Muller, S.; et al. Cellular uptake of functionalized carbon nanotubes is independent of functional group and cell type. Nat. Nanotechnol. 2007, 2, 108–113. [Google Scholar] [CrossRef] [PubMed]
- Kam, N.W.S.; Liu, Z.; Dai, H.J. Functionalization of carbon nanotubes via cleavable disulfide bonds for efficient intracellular delivery of siRNA and potent gene silencing. J. Am. Chem. Soc. 2005, 127, 12492–12493. [Google Scholar] [CrossRef] [PubMed]
- Dong, H.; Ding, L.; Yan, F.; Ji, H.; Ju, H. The use of polyethylenimine-grafted graphene nanoribbon for cellular delivery of locked nucleic acid modified molecular beacon for recognition of microRNA. Biomaterials 2011, 32, 3875–3882. [Google Scholar] [CrossRef] [PubMed]
- Jia, N.Q.; Lian, Q.; Shen, H.B.; Wang, C.; Li, X.Y.; Yang, Z.N. Intracellular delivery of quantum dots tagged antisense oligodeoxynucleotides by functionalized multiwalled carbon nanotubes. Nano Lett. 2007, 7, 2976–2980. [Google Scholar] [CrossRef] [PubMed]
- Gooding, M.; Malhotra, M.; Evans, J.C.; Darcy, R.; O’Driscoll, C.M. Oligonucleotide conjugates—Candidates for gene silencing therapeutics. Eur. J. Pharm. Biopharm. 2016, 107, 321–340. [Google Scholar] [CrossRef] [PubMed]
- Gopinath, S.C.; Lakshmipriya, T.; Chen, Y.; Arshad, M.K.; Kerishnan, J.P.; Ruslinda, A.R.; Al-Douri, Y.; Voon, C.H.; Hashim, U. Cell-targeting aptamers act as intracellular delivery vehicles. Appl. Microbiol. Biotechnol. 2016, 100, 6955–6969. [Google Scholar] [CrossRef] [PubMed]
- McDevitt, M.R.; Chattopadhyay, D.; Kappel, B.J.; Jaggi, J.S.; Schiffman, S.R.; Antczak, C.; Njardarson, J.T.; Brentjens, R.; Scheinberg, D.A. Tumor targeting with antibody-functionalized, radiolabeled carbon nanotubes. J. Nucl. Med. 2007, 48, 1180–1189. [Google Scholar] [CrossRef] [PubMed]
- Yang, L.; Ng, K.Y.; Lillehei, K.O. Cell-mediated immunotherapy: A new approach to the treatment of malignant glioma. Cancer Control 2003, 10, 138–147. [Google Scholar] [PubMed]
- Parney, I.F.; Hao, C.; Petruk, K.C. Glioma immunology and immunotherapy. Neurosurgery 2000, 46, 778–791. [Google Scholar] [PubMed]
- Hussey, S.L.; Peterson, B.R. Efficient delivery of streptavidin to mammalian cells: Clathrin-mediated endocytosis regulated by a synthetic ligand. J. Am. Chem. Soc. 2002, 124, 6265–6273. [Google Scholar] [CrossRef] [PubMed]
- Welsher, K.; Sherlock, S.P.; Dai, H.J. Deep-tissue anatomical imaging of mice using carbon nanotube fluorophores in the second near-infrared window. Proc. Natl. Acad. Sci. USA 2011, 108, 8943–8948. [Google Scholar] [CrossRef] [PubMed]
- Barone, P.W.; Baik, S.; Heller, D.A.; Strano, M.S. Near-infrared optical sensors based on single-walled carbon nanotubes. Nat. Mater. 2005, 4, 86–92. [Google Scholar] [CrossRef] [PubMed]
- Hong, G.S.; Lee, J.C.; Robinson, J.T.; Raaz, U.; Xie, L.M.; Huang, N.F.; Cooke, J.P.; Dai, H.J. Multifunctional in vivo vascular imaging using near-infrared II fluorescence. Nat. Med. 2012, 18, 1841–1846. [Google Scholar] [CrossRef] [PubMed]
- Liu, Z.A.; Li, X.L.; Tabakman, S.M.; Jiang, K.L.; Fan, S.S.; Dai, H.J. Multiplexed multicolor Raman imaging of live cells with isotopically modified single walled carbon nanotubes. J. Am. Chem. Soc. 2008, 130, 13540–13541. [Google Scholar] [CrossRef] [PubMed]
- Zavaleta, C.L.; Smith, B.R.; Walton, I.; Doering, W.; Davis, G.; Shojaei, B.; Natan, M.J.; Gambhir, S.S. Multiplexed imaging of surface enhanced Raman scattering nanotags in living mice using noninvasive Raman spectroscopy. Proc. Natl. Acad. Sci. USA 2009, 106, 13511–13516. [Google Scholar] [CrossRef] [PubMed]
- Liu, Z.; Tabakman, S.; Welsher, K.; Dai, H.J. Carbon nanotubes in biology and medicine: In vitro and in vivo detection, imaging and drug delivery. Nano Res. 2009, 2, 85–120. [Google Scholar] [CrossRef] [PubMed]
- Hong, G.; Diao, S.; Antaris, A.L.; Dai, H. Carbon nanomaterials for biological imaging and nanomedicinal therapy. Chem. Rev. 2015, 115, 10816–10906. [Google Scholar] [CrossRef] [PubMed]
- Wang, C.; Ma, X.X.; Ye, S.Q.; Cheng, L.; Yang, K.; Guo, L.; Li, C.H.; Li, Y.G.; Liu, Z. Protamine functionalized single-walled carbon nanotubes for stem cell labeling and in vivo raman/magnetic resonance/photoacoustic triple-modal imaging. Adv. Funct. Mater. 2012, 22, 2363–2375. [Google Scholar] [CrossRef]
- He, X.X.; Gao, J.H.; Gambhir, S.S.; Cheng, Z. Near-infrared fluorescent nanoprobes for cancer molecular imaging: Status and challenges. Trends Mol. Med. 2010, 16, 574–583. [Google Scholar] [CrossRef] [PubMed]
- Chance, B. Near-infrared images using continuous, phase-modulated, and pulsed light with quantitation of blood and blood oxygenation. Ann. N. Y. Acad. Sci. 1998, 838, 29–45. [Google Scholar] [CrossRef] [PubMed]
- Ishizawa, T.; Fukushima, N.; Shibahara, J.; Masuda, K.; Tamura, S.; Aoki, T.; Hasegawa, K.; Beck, Y.; Fukayama, M.; Kokudo, N. Real-time identification of liver cancers by using indocyanine green fluorescent imaging. Cancer 2009, 115, 2491–2504. [Google Scholar] [CrossRef] [PubMed]
- Sekijima, M.; Tojimbara, T.; Sato, S.; Nakamura, M.; Kawase, T.; Kai, K.; Urashima, Y.; Nakajima, I.; Fuchinoue, S.; Teraoka, S. An intraoperative fluorescent imaging system in organ transplantation. Transp. Proc. 2004, 36, 2188–2190. [Google Scholar] [CrossRef] [PubMed]
- Weissleder, R.; Tung, C.H.; Mahmood, U.; Bogdanov, A. In vivo imaging of tumors with protease-activated near-infrared fluorescent probes. Nat. Biotechnol. 1999, 17, 375–378. [Google Scholar] [CrossRef] [PubMed]
- Kim, S.; Lim, Y.T.; Soltesz, E.G.; De Grand, A.M.; Lee, J.; Nakayama, A.; Parker, J.A.; Mihaljevic, T.; Laurence, R.G.; Dor, D.M.; et al. Near-infrared fluorescent type ii quantum dots for sentinel lymph node mapping. Nat. Biotechnol. 2004, 22, 93–97. [Google Scholar] [CrossRef] [PubMed]
- Iizumi, Y.; Okazaki, T.; Ikehara, Y.; Ogura, M.; Fukata, S.; Yudasaka, M. Immunoassay with single-walled carbon nanotubes as near-infrared fluorescent labels. ACS Appl. Mater. Interfaces 2013, 5, 7665–7670. [Google Scholar] [CrossRef] [PubMed]
- Lim, Y.T.; Kim, S.; Nakayama, A.; Stott, N.E.; Bawendi, M.G.; Frangioni, J.V. Selection of quantum dot wavelengths for biomedical assays and imaging. Mol. Imaging 2003, 2, 50–64. [Google Scholar] [CrossRef] [PubMed]
- Diao, S.; Hong, G.S.; Robinson, J.T.; Jiao, L.Y.; Antaris, A.L.; Wu, J.Z.; Choi, C.L.; Dai, H.J. Chirality enriched (12,1) and (11,3) single-walled carbon nanotubes for biological imaging. J. Am. Chem. Soc. 2012, 134, 16971–16974. [Google Scholar] [CrossRef] [PubMed]
- Yi, H.J.; Ghosh, D.; Ham, M.H.; Qi, J.F.; Barone, P.W.; Strano, M.S.; Belcher, A.M. M13 phage-functionalized single-walled carbon nanotubes as nanoprobes for second near-infrared window fluorescence imaging of targeted tumors. Nano Lett. 2012, 12, 1176–1183. [Google Scholar] [CrossRef] [PubMed]
- Serpell, C.J.; Kostarelos, K.; Davis, B.G. Can carbon nanotubes deliver on their promise in biology? Harnessing unique properties for unparalleled applications. ACS Cent. Sci. 2016, 2, 190–200. [Google Scholar] [CrossRef] [PubMed]
- Jorio, A.; Pimenta, M.A.; Souza, A.G.; Saito, R.; Dresselhaus, G.; Dresselhaus, M.S. Characterizing carbon nanotube samples with resonance raman scattering. New J. Phys. 2003, 5, 1765–1768. [Google Scholar] [CrossRef]
- Hong, G.S.; Lee, J.C.; Jha, A.; Diao, S.; Nakayama, K.H.; Hou, L.Q.; Doyle, T.C.; Robinson, J.T.; Antaris, A.L.; Dai, H.J.; et al. Near-infrared ii fluorescence for imaging hindlimb vessel regeneration with dynamic tissue perfusion measurement. Circ. Cardiovasc. Imaging 2014, 7, 517–525. [Google Scholar] [CrossRef] [PubMed]
- Hong, G.S.; Diao, S.; Chang, J.L.; Antaris, A.L.; Chen, C.X.; Zhang, B.; Zhao, S.; Atochin, D.N.; Huang, P.L.; Andreasson, K.I.; et al. Through-skull fluorescence imaging of the brain in a new near-infrared window. Nat. Photonics 2014, 8, 723–730. [Google Scholar] [CrossRef] [PubMed]
- Diao, S.; Blackburn, J.L.; Hong, G.; Antaris, A.L.; Chang, J.; Wu, J.Z.; Zhang, B.; Cheng, K.; Kuo, C.J.; Dai, H. Fluorescence imaging in vivo at wavelengths beyond 1500 nm. Angew. Chem. Int. Ed. Engl. 2015, 54, 14758–14762. [Google Scholar] [CrossRef] [PubMed]
- Jorio, A.; Saito, R.; Hafner, J.H.; Lieber, C.M.; Hunter, M.; McClure, T.; Dresselhaus, G.; Dresselhaus, M.S. Structural (n,m) determination of isolated single-wall carbon nanotubes by resonant Raman scattering. Phys. Rev. Lett. 2001, 86, 1118–1121. [Google Scholar] [CrossRef] [PubMed]
- Rao, A.M.; Richter, E.; Bandow, S.; Chase, B.; Eklund, P.C.; Williams, K.A.; Fang, S.; Subbaswamy, K.R.; Menon, M.; Thess, A.; et al. Diameter-selective raman scattering from vibrational modes in carbon nanotubes. Science 1997, 275, 187–191. [Google Scholar] [CrossRef] [PubMed]
- Heller, D.A.; Baik, S.; Eurell, T.E.; Strano, M.S. Single-walled carbon nanotube spectroscopy in live cells: Towards long-term labels and optical sensors. Adv. Mater. 2005, 17, 2793–2799. [Google Scholar] [CrossRef]
- Heller, D.A.; Jin, H.; Martinez, B.M.; Patel, D.; Miller, B.M.; Yeung, T.K.; Jena, P.V.; Hobartner, C.; Ha, T.; Silverman, S.K.; et al. Multimodal optical sensing and analyte specificity using single-walled carbon nanotubes. Nat. Nanotechnol. 2009, 4, 114–120. [Google Scholar] [CrossRef] [PubMed]
- Wang, X.D.; Pang, Y.J.; Ku, G.; Xie, X.Y.; Stoica, G.; Wang, L.H.V. Noninvasive laser-induced photoacoustic tomography for structural and functional in vivo imaging of the brain. Nat. Biotechnol. 2003, 21, 803–806. [Google Scholar] [CrossRef] [PubMed]
- Ku, G.; Wang, L.H.V. Deeply penetrating photoacoustic tomography in biological tissues enhanced with an optical contrast agent. Opt. Lett. 2005, 30, 507–509. [Google Scholar] [CrossRef] [PubMed]
- Hoelen, C.G.; de Mul, F.F.; Pongers, R.; Dekker, A. Three-dimensional photoacoustic imaging of blood vessels in tissue. Opt. Lett. 1998, 23, 648–650. [Google Scholar] [CrossRef] [PubMed]
- Yang, K.; Hu, L.L.; Ma, X.X.; Ye, S.Q.; Cheng, L.; Shi, X.Z.; Li, C.H.; Li, Y.G.; Liu, Z. Multimodal imaging guided photothermal therapy using functionalized graphene nanosheets anchored with magnetic nanoparticles. Adv. Mater. 2012, 24, 1868–1872. [Google Scholar] [CrossRef] [PubMed]
- Ku, G.; Zhou, M.; Song, S.L.; Huang, Q.; Hazle, J.; Li, C. Copper sulfide nanoparticles as a new class of photoacoustic contrast agent for deep tissue imaging at 1064 nm. ACS Nano 2012, 6, 7489–7496. [Google Scholar] [CrossRef] [PubMed]
- Agarwal, A.; Huang, S.W.; O’Donnell, M.; Day, K.C.; Day, M.; Kotov, N.; Ashkenazi, S. Targeted gold nanorod contrast agent for prostate cancer detection by photoacoustic imaging. J. Appl. Phys. 2007, 102, 064701. [Google Scholar] [CrossRef]
- De la Zerda, A.; Liu, Z.A.; Bodapati, S.; Teed, R.; Vaithilingam, S.; Khuri-Yakub, B.T.; Chen, X.Y.; Dai, H.J.; Gambhir, S.S. Ultrahigh sensitivity carbon nanotube agents for photoacoustic molecular imaging in living mice. Nano Lett. 2010, 10, 2168–2172. [Google Scholar] [CrossRef] [PubMed]
- De la Zerda, A.; Zavaleta, C.; Keren, S.; Vaithilingam, S.; Bodapati, S.; Liu, Z.; Levi, J.; Smith, B.R.; Ma, T.J.; Oralkan, O.; et al. Carbon nanotubes as photoacoustic molecular imaging agents in living mice. Nat. Nanotechnol. 2008, 3, 557–562. [Google Scholar] [CrossRef] [PubMed]
- Doan, B.; Meme, S.; Beloeil, J. General principles of MRI. In The Chemistry of Contrast Agents in Medical Magnetic Resonance Imaging; Merbach, A., Helm, L., Tóth, É., Eds.; John Wiley and Sons, Ltd.: Chichester, UK, 2013. [Google Scholar]
- Sitharaman, B.; Kissell, K.R.; Hartman, K.B.; Tran, L.A.; Baikalov, A.; Rusakova, I.; Sun, Y.; Khant, H.A.; Ludtke, S.J.; Chiu, W.; et al. Superparamagnetic gadonanotubes are high-performance MRI contrast agents. Chem. Commun. 2005, 3915–3917. [Google Scholar] [CrossRef] [PubMed]
- Al Faraj, A.; Cieslar, K.; Lacroix, G.; Gaillard, S.; Canot-Soulas, E.; Cremillieux, Y. In vivo imaging of carbon nanotube biodistribution using magnetic resonance imaging. Nano Lett. 2009, 9, 1023–1027. [Google Scholar] [CrossRef] [PubMed]
- Al Faraj, A.; Fauvelle, F.; Luciani, N.; Lacroix, G.; Levy, M.; Cremillieux, Y.; Canet-Soulas, E. In vivo biodistribution and biological impact of injected carbon nanotubes using magnetic resonance techniques. Int. J. Nanomed. 2011, 6, 351–361. [Google Scholar] [CrossRef] [PubMed]
- Cerpa, A.; Kober, M.; Calle, D.; Negri, V.; Gavira, J.M.; Hernanz, A.; Briones, F.; Cerdan, S.; Ballesteros, P. Single-walled carbon nanotubes as anisotropic relaxation probes for magnetic resonance imaging. Medchemcomm 2013, 4, 669–672. [Google Scholar] [CrossRef]
- Doan, B.T.; Seguin, J.; Breton, M.; Le Beherec, R.; Bessodes, M.; Rodriguez-Manzo, J.A.; Banhart, F.; Beloeil, J.C.; Scherman, D.; Richard, C. Functionalized single-walled carbon nanotubes containing traces of iron as new negative MRI contrast agents for in vivo imaging. Contrast Media Mol. Imaging 2012, 7, 153–159. [Google Scholar] [CrossRef] [PubMed]
- Rivera, E.J.; Sethi, R.; Qu, F.F.; Krishnamurthy, R.; Muthupillai, R.; Alford, M.; Swanson, M.A.; Eaton, S.S.; Eaton, G.R.; Wilson, L.J. Nitroxide radicals@us-tubes: New spin labels for biomedical applications. Adv. Funct. Mater. 2012, 22, 3691–3698. [Google Scholar] [CrossRef]
- Sitharaman, B.; Jacobson, B.D.; Wadghiri, Y.Z.; Bryant, H.; Frank, J. The magnetic, relaxometric, and optical properties of gadolinium-catalyzed single walled carbon nanotubes. J. Appl. Phys. 2013, 113, 1106–1115. [Google Scholar] [CrossRef] [PubMed]
- Choi, J.H.; Nguyen, F.T.; Barone, P.W.; Heller, D.A.; Moll, A.E.; Patel, D.; Boppart, S.A.; Strano, M.S. Multimodal biomedical imaging with asymmetric single-walled carbon nanotube/iron oxide nanoparticle complexes. Nano Lett. 2007, 7, 861–867. [Google Scholar] [CrossRef] [PubMed]
- Dinesh, B.; Bianco, A.; Menard-Moyon, C. Designing multimodal carbon nanotubes by covalent multi-functionalization. Nanoscale 2016, 8, 18596–18611. [Google Scholar] [CrossRef] [PubMed]
- Firme, C.P., 3rd; Bandaru, P.R. Toxicity issues in the application of carbon nanotubes to biological systems. Nanomedicine 2010, 6, 245–256. [Google Scholar] [CrossRef] [PubMed]
- Bianco, A.; Kostarelos, K.; Prato, M. Making carbon nanotubes biocompatible and biodegradable. Chem. Commun. 2011, 47, 10182–10188. [Google Scholar] [CrossRef] [PubMed]


| Application | Chemical Structure of Carbon Nanotubes (CNTs) (Functional Group) | Study Design (in vitro/in vivo) | Results | Reference |
|---|---|---|---|---|
| HCPT | f-MWCNTs (diaminotriethylene glycol spacers) | MKN-28 (in vitro) | Superior antitumor activity | [14] |
| Hepatic H22 tumor bearing ICR mice (in vivo) | ||||
| CPT | f-MWCNTs (PVA) | MDA-MB23, A-5RT3 (in vitro) | 15-fold higher mortality than free CPT | [15] |
| CPT | f-MWCNTs (Pluronic P123) | HeLa (in vitro) | Enhanced antitumor activity over free CPT | [16] |
| Irinotecan | MWCNTs (open tips) | - | Higher filling amount of Irinotecan at a larger inner diameter tube | [17] |
| DOX | f-MWCNTs (dispersed Pluronic F127) | MCF-7 (in vitro) | Enhanced cytotoxicity on human breast cancer cells | [18] |
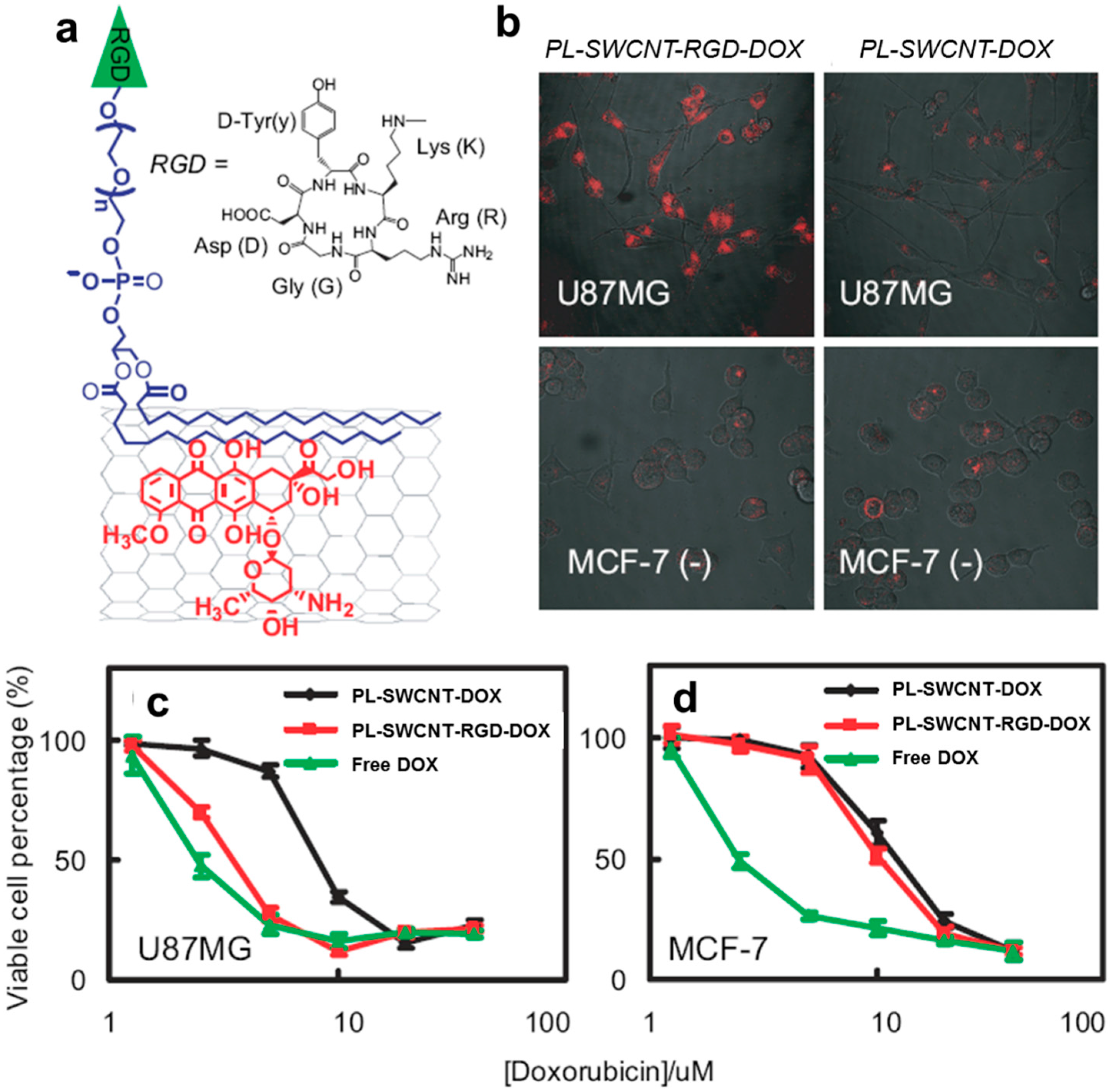
| DOX | f-SWCNTs (PEG and cyclic RGD) | U87MG, MCF-7 (in vitro) | Extremely high loading efficiency of ~400% | [19] |
| DOX | f-MWCNTs (PEG) | HeLa (in vitro) | Higher cell killing effect | [20] |
| DOX | f-SWCNTs ((CHI and/or ALG) and FA) | HeLa (in vitro) | Release of DOX at low pH. | [21] |
| DOX | f-MWCNTs (FA and iron NP) | HeLa (in vitro) | 6-fold higher delivering ability than free DOX | [22] |
| CDDP | SWCNTs | PC-3, DU145 (in vitro) | Smooth release profile until 72 h | [23] |
| CP | Oxidized MWCNTs (open tips) | EJ28 (in vitro) | Growth inhibition of bladder cancer cells | [24] |
| PTX | f-SWCNTs (PEG phospholipids) | 4T1 (in vitro) | 10-fold higher uptake than clinical Taxol® | [25] |
| Mice baring 4T1 tumors (in vivo) | ||||
| PTX | f-SWCNTs and f-MWCNTs (PEG) | MCF-7, HeLa (in vitro) | Growth suppression of cancer cells | [26] |
| Plasmid DNA | f-SWCNT (–NH3+, Lys-NH3+) | A549 (in vitro) | Up-regulation of marker gene expression over naked DNA | [27] |
| f-MWCNTs (-NH3+) | ||||
| Plasmid DNA | f-MWCNTs (–COOH) | Escherichia coli (in vitro) | Improvement for delivery of linear DNA fragments | [28] |
| Plasmid DNA | f-MWCNTs (–NH3+) | CIK (in vitro) | effective transfection in CIK cells than naked DNA | [29] |
| Plasmid DNA | f-SWCNTs (ethylenediamine) | MCF-7 (in vitro) | 40% apoptosis after 72 h exposure | [30] |
| Plasmid DNA | f-SWCNTs and f-MWCNTs (NH2) | HeLa (in vitro) | Higher pDNA uptake and gene expression than pDNA alone | [31] |
| Plasmid DNA | f-MWCNTs (NH2) | A375 (in vitro) | Successful delivery of the GFP gene in cultured cells | [32] |
| siRNA | f-SWCNTs (NH2) | K562 (in vitro) | Inhibition of cell proliferation and promotion of cancer apoptosis | [33] |
| siRNA | f-MWCNTs (NH3+) | Calu6, SVEC 4–10 and 2F2B, DU145 and C-33A, A549, MCF7, HeLa, HEK293, B16F10, NIH 3T3 (in vitro) | Delay of the tumor growth (in vitro) Increased survival of xenograft-bearing animals (in vivo) | [34] |
| Mice bearing Calu6 xenograft tumors (in vivo) | ||||
| siRNA | f-SWCNTs (–CONH-(CH2)6-NH3+Cl−) | TC-1 cells, 1H8 cells, LLC cells (in vitro) | Reduced tumor growth (in vivo) | [35] |
| Mice bearing Lewis lung carcinoma or HeLa cell xenografts (in vivo) | ||||
| siRNA | f-MWCNTs (-PEI and -pyridinium) | H1299 (in vitro) | 10%–30% silencing activity and a cytotoxicity of 10%–60% | [36] |
| siRNA | Pristine SWCNTs | MiaPaCa-2/HRE, MCF-7, MDA-MB-231, RGM1 (in vitro) | Significantly inhibition of Hif-1α expression (in vitro) | [37] |
| Mice bearing MiaPaCa-2/HRE tumors (in vivo) | ||||
| siRNA | f-MWCNTs ((NH3+) | Calu6 (in vitro) | Reduced tumor growth (in vivo) | [38] |
| Mice bearing Calu6 lung carcinoma (in vivo) | ||||
| ODNs | f-MWCNTs (polyamidoamine dendrimer modified) | MCF-7, MDA-MB-435, HepG2 (in vitro) | Inhibition of the cell growth (time- and dose-dependent)/Down-regulation of the expression of the cmyc gene and C-Myc protein | [39] |
| Aptamer | f-MWCNTs (–COOH) | MCF-7 (in vitro) | Internalization without affecting cell viability | [40] |
| Immunotherapy | f-SWCNTs (radiometal-ion chelates, E4G10) | Mice bearing LS174T (in vivo) | Reduction of tumor volume and improvement of median survival relative to controls | [41] |
| Immunotherapy | MWCNTs | Mice bearing H22 liver cancer (in vivo) | Promotion of inflammatory cytokine production and stimulation of macrophage phagocytosis | [42] |
| Immunotherapy | MWCNTs | Mice bearing GL261 (in vivo) | Increase of the macrophage influx into the glioma cells | [43] |
| Immunotherapy | f-SWCNTs (CpG) | Mice bearing glioma (in vivo) | Improvement of the survival of glioma bearing mice | [44] |
| Immunotherapy | f-bundled CNTs (MHC-1, αCD28, PLGA) | Mice bearing B16 melanoma (in vivo) | Action as an artificial antigen-presenting cell to expand T cells efficiently. | [45] |
| Protein | SWCNTs-biotin (Streptavidin) | HL60, human T cells (in vitro) | Consistent uptake pathway with endocytosis | [46] |
| Protein | f-MWCNTs (toxin protein RTA) | L-929, HeLa, HL7702, MCF-7, COS-7 (in vitro) | 3-fold higher cell death rate than RTA alone | [47] |
| Fluorescence imaging | f-SWCNTs (sodium cholate and PEG) | Mouse (in vivo) | High-resolution microscopy imaging of tumor vessels below thick skin | [48] |
| Fluorescence imaging | f-SWCNTs (poly(maleic anhydride-alt-1-octadecene)-PEG) | Mice bearing 4T1 breast cancer (in vivo) | in vivo real-time fluorescence video imaging of mouse hind limb vasculatures | [49] |
| Fluorescence imaging | f-SWCNTs (M13 virus) | Mice bearing ovarian cancer (in vivo) | Identification of sub-millimeter tumors | [50] |
| Fluorescence imaging | f-SWCNTs (C18-PMH-mPEG) | Mice bearing 4T1 breast cancer (in vivo) | Imaging of tumors at an intravenous injection of ∼4 μg SWCNT material | [51] |
| Raman imaging | f-DWCNTs (folic acid) | T24 (in vitro) | Application of the location mapping of carcinoma cells and tracking of their movements | [52] |
| Raman imaging | f-SWCNTs (RGD) | Mice bearing U87MG tumor (in vivo) | Accumulation for >72 h in tumor area | [53] |
| Raman imaging | f-SWCNTs (RGD) | Mice bearing U87MG tumor (in vivo) | 4-fold higher tumor binding than cyclo-(Arg-Ala-Asp-d-Phe-Lys)(RAD)-SWCNTs | [54] |
| Raman imaging | f-SWCNTs (Erbitux, RGD, anti-CEA, Rituxan, Herceptin) | MDA-MB-468, U87MG, LS174T, Raji, and BT474 (in vitro) | Feasibility of SWCNTs as NIR Raman tags for multi-color optical imaging and detection | [55] |
| Photoacoustic imaging | f-SWCNTs (Indocyanine Green dye-RGD) | Mice bearing U87MG tumor (in vivo) | sub-nanomolar sensitivities in living tissues and 20-fold higher cancer cell detection than previously-reported SWCNTs | [56] |
| Photoacoustic imaging | f-SWCNTs (gold-folic acid) | Mice bearing tumor (in vivo) | Improvement of detection sensitivity and specificity | [57] |
| Photoacoustic imaging | f-SWCNTs (Indocyanine Green dye) | - | 2-fold higher signal amplitudes than SWCNTs | [58] |
| Photoacoustic imaging | f-SWCNTs (Albumin/Ce6-EB) | Mice bearing SCC-7 tumor (in vivo) | long blood circulating behavior (48 h) | [59] |
| Magnetic resonance imaging | f-MWCNTs (Gd chelate) | Mice (in vivo) | in vivo feasibility studies using MRI (300 MHz) | [60] |
| Magnetic resonance imaging | f-SWCNTs (Gd ion) | Mice (in vivo) | Successful imaging of the uptake of Gd-CNTs in the liver and spleen | [61] |
| Magnetic resonance imaging | f-MWCNTs (CoFe2O4) | HeLa (in vitro) | Favor as T2 contrast agent | [62] |
| Magnetic resonance imaging | f-MWCNTs (iron NP and Gd ion) | - | Dual function of MRI and magnetic hyperthermia cancer therapy | [63] |
| Control of size | Cellular uptake | Drug loading | Functional surface | Water dispersibility | Toxicity | |
|---|---|---|---|---|---|---|
| Carbon nanotubes | Moderate | Fast (needle-like shape) | High (high aspect ratio) | High (high aspect ratio and inner/outer surface) | Low (hydrophilic polymer coating or conjugation) | Moderate |
| Polymer-based NPs | Easy | Moderate | Low (encapsulation) | Moderate | Moderate (hydrophilic polymer) | Low |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC-BY) license ( http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hwang, Y.; Park, S.-H.; Lee, J.W. Applications of Functionalized Carbon Nanotubes for the Therapy and Diagnosis of Cancer. Polymers 2017, 9, 13. https://doi.org/10.3390/polym9010013
Hwang Y, Park S-H, Lee JW. Applications of Functionalized Carbon Nanotubes for the Therapy and Diagnosis of Cancer. Polymers. 2017; 9(1):13. https://doi.org/10.3390/polym9010013
Chicago/Turabian StyleHwang, Yongsung, Sung-Hoon Park, and Jin Woo Lee. 2017. "Applications of Functionalized Carbon Nanotubes for the Therapy and Diagnosis of Cancer" Polymers 9, no. 1: 13. https://doi.org/10.3390/polym9010013
APA StyleHwang, Y., Park, S.-H., & Lee, J. W. (2017). Applications of Functionalized Carbon Nanotubes for the Therapy and Diagnosis of Cancer. Polymers, 9(1), 13. https://doi.org/10.3390/polym9010013







