In Vitro and In Vivo Evaluation of a Folate-Targeted Copolymeric Submicrohydrogel Based on N-Isopropylacrylamide as 5-Fluorouracil Delivery System
Abstract
: Folate-targeted poly[(p-nitrophenyl acrylate)-co-(N-isopropylacrylamide)] nanohydrogel (F-SubMG) was loaded with 5-fluorouracil (5-FU) to obtain low (16.3 ± 1.9 μg 5-FU/mg F-SubMG) and high (46.8 ± 3.8 μg 5-FU/mg F-SubMG) load 5-FU-loaded F-SubMGs. The complete in vitro drug release took place in 8 h. The cytotoxicity of unloaded F-SubMGs in MCF7 and HeLa cells was low; although it increased for high F-SubMG concentration. The administration of 10 μM 5-FU by 5-FU-loaded F-SubMGs was effective on both cellular types. Cell uptake of F-SubMGs took place in both cell types, but it was higher in HeLa cells because they are folate receptor positive. After subcutaneous administration (28 mg 5-FU/kg b.w.) in Wistar rats, F-SubMGs were detected at the site of injection under the skin. Histological studies indicated that the F-SubMGs were surrounded by connective tissue, without any signs of rejections, even 60 days after injection. Pharmacokinetic study showed an increase in MRT (mean residence time) of 5-FU when the drug was administered by drug-loaded F-SubMGs.1. Introduction
5-Fluorouracil (5-FU) is one of the chemotherapeutic compounds most used for the treatment of a great variety of tumors [1], such as colorectal cancer [2-4], breast cancer [5], pancreatic cancer [6], or gastric cancer [7]. It is an antimetabolite of pyrimidine analogue type that acts mainly through the inhibition of synthesis of DNA and RNA during the S-phase of the cell cycle. It is metabolized rapidly in the body which may affect the therapeutic response of the drug [8-10]. Moreover, due to its short plasma half-life and poor oral absorption, 5-fluorouracil has been chosen to be included in different controlled release systems [8-13]. In this type of system, the drug is protected from degradation following administration, the delivery system can be administered close to the tumoral cells, the drug is released with a specific patron and the action of the drug on tumoral cells can be direct. Among them, many nano-size drug delivery systems (liposomes, liquid-core nanocapsules, dendrimers, polymer-drug conjugates, nanoparticles, polymeric micelles and polymeric nanogels) have been developed [14,15] for the treatment of pathologies as cancer [16,17]. Due to their size, nanocarries can penetrate within even small capillaries, and they can be taken up, in many cases, very efficiently by cells, internalized and stored into cytoplasm or different organelles [18]. Nanocarrier uptake into a cell depends on the cell-type, since some cells are more susceptible to include nonfuncionalized systems via their design. An active targeting strategy can improve the efficacy of the therapy and diminish side effects associated with drugs, since not all nanocarriers can overcome the cell membrane barrier without a targeting motif. To increase the delivery of a given drug to a specific target site, targeting ligands are conjugated to carriers [14]. Folate has been extensively investigated for targeting various tumor cells overexpressing folate receptors [14,19]. The folate in target drug delivery systems is primarily due to convenient and easy conjugation step and to the high affinity for the folate receptor after conjugation [20] which enables transportation of the conjugate via receptor mediated endocytosis.
Folate-targeted nanoparticles have shown to be effective in a number of tumors using folic acid-polymer conjugates [21] and liposomes [22]. Among nanocarriers, nanogels are promising vehicles for drug delivery. A hydrogel is a three-dimensional cross-linked network capable of swelling in biological fluids and retaining a large amount of fluids in the swollen state [23]. Nanogel particles are gels with dimensions in the colloidal range (10–1,000 nm). These nanosystems can be synthesized using very different monomers, which make them capable of responding to external stimuli such as pH or temperature [24,25]. Furthermore, the presence of reactive pendant groups in nanogels eases their vectorization forward specific cell motif by binding ligands as folate molecules.
In this work, folate-conjugate submicrogels (F-SubMGs), synthesized by Katime's research group [26], have been evaluated for antitumor therapy by loading them with 5-fluorouracil. Colloidal nanosize folate-conjugate hydrogels were prepared via a post-synthetic pathway starting with poly(p-nitrophenyl acrylate-co-N-isopropylacrylamide) [25,26]. A specific submicrogels composition with a folic acid concentration of 1.3 ± 0.8 mmol/g gel and an average size of 601 ± 28 nm was employed as a 5-fluorouracil delivery system in vitro, in the cellular lines MCF7 of breast cancer and HeLa of cervical cancer, and in vivo in female Wistar rats. Thus, administration of 5-FU by drug-loaded folate-conjugate submicrogels can be an approach to achieve high concentrations of the antineoplastic drug near to the target site for a given period of time, increasing its therapeutic effect.
2. Results and Discussion
2.1. In Vitro Studies
The size of F-SubMGs employed in this work was 601 ± 28 nm, which was determined in water by quasielastic light scattering [26]. 5-FU is not soluble in organic solvent, slightly soluble in metanol (5 mg/mL) [8], but its solubility increases to 13 mg/mL in aqueous medium [27]. Thus, load of F-SubMGs with the drug was carried out by swelling of nanocarriers in 5-FU solution in phosphate buffer (1 mM, pH 7.4) using two solutions of different concentrations, 0.4 mg 5-FU/mL and 7 mg 5-FU/mL. 5-FU loads were 16.3 ± 1.9 μg 5-FU/mg F-SubMG (named low load 5-FU-loaded F-SubMGs) and 46.8 ± 3.8 μg 5-FU/mg F-SubMG (named high load 5-FU-loaded F-SubMGs), respectively. SEM micrographs of 5-FU-loaded F-SubMGs showed a spherical morphology (Figure 1).
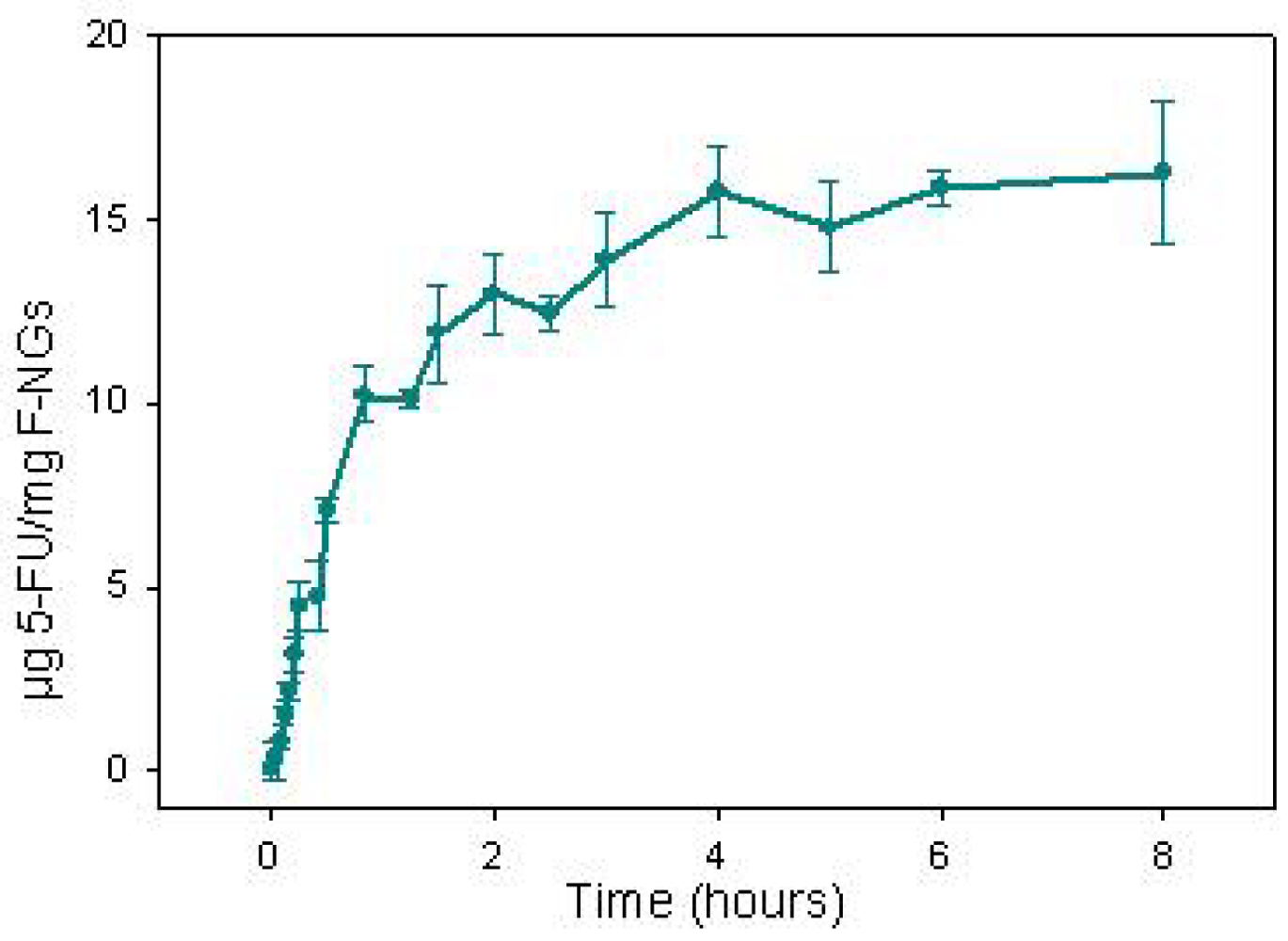
The in vitro release of drug from low load 5-FU-loaded F-SubMGs is shown in Figure 2. The release of the drug was complete in 8 h, and two 5-FU release stages with different rates were determined. A quick release of the most external 5-FU from F-SubMGs were observed during the first 50 min, which took place at a rate of 12.6 μg 5-FU/h per mg F-SubMGs (r2 = 0.97). Afterward, a slower rate of 0.85 μg 5-FU/h per mg F-SubMGs (r2 = 0.90) from 50 min to 8 h was determined.
In vitro experimental conditions employed in this work were based on previous studies, in which swelling of these submicrogels was determined to be pH-, ionic strength- and temperature-sensitive [25,26]. Taking into account that nanogel swelling increases with acid pH (pH 5.2), high ionic strength (more than 0.02 M) and temperature lower than 33 °C, 5-FU release from drug loaded F-SubMGs was carried out at 37 °C in phosphate buffer 1 mM and pH 7.4, similar to biological fluids conditions, in which drug solubility was favorable.
2.2. Cell Culture Studies
The over expression of folate receptors (FR) in many cancer cells [14,19] has been considered to target anticancer drug-loaded nanocarriers by binding folate molecules in the surface of such nanosystems, which can be transported via receptor mediated endocytosis. One of the main advantages of these controlled drug delivery systems is that the folate conjugate submicrogels could be included mainly in tumor cells, avoiding toxic effects in normal cells.
In this work, antitumoral efficiency of 5-fluorouracil loaded folate-conjugate submicrogels (5-FU-loaded F-SubMGs) has been evaluated in two cellular lines, MCF7 of breast cancer, and HeLa of cervical cancer, which are folate receptor negative (FR(−)) and folate receptor positive (FR(+)), respectively. Thus, on one hand, cellular uptake of folate conjugate submicrogels and submicrogels without folate were studied to evaluate the effect of folic acid on intracellular transport of nanocarriers. On the other hand, the viability of those cells lines was evaluated in the presence of unloaded, 5-FU-loaded F-SubMGs and 5-FU in solution.
Fluorescence markers are frequently used in cellular uptake studies [28,29]. In our case, in order to measure cell uptake, folate-conjugate submicrogels (F-SubMGs) as well as control submicrogels (SubMGs) were loaded with Alexa Fluor® 488.
The presence of submicrogels was confirmed in both cell types, which was easily observed by contrast microscopy and by fluorescence microscopy since Alexa Fluor® 488 has green fluorescence. Nevertheless, these methods do not show the amount of submicrogels inside the cell and to allow evaluation of the role of folic molecule in their vectorization. Therefore, studies with flow cytometry were carried out. Figure 3 shows plots of total nanogel-associated events as a function of incubation time, obtained from the corresponding histogram. The cells grown in the presence of Alexa Fluor® 488 were used as a control.
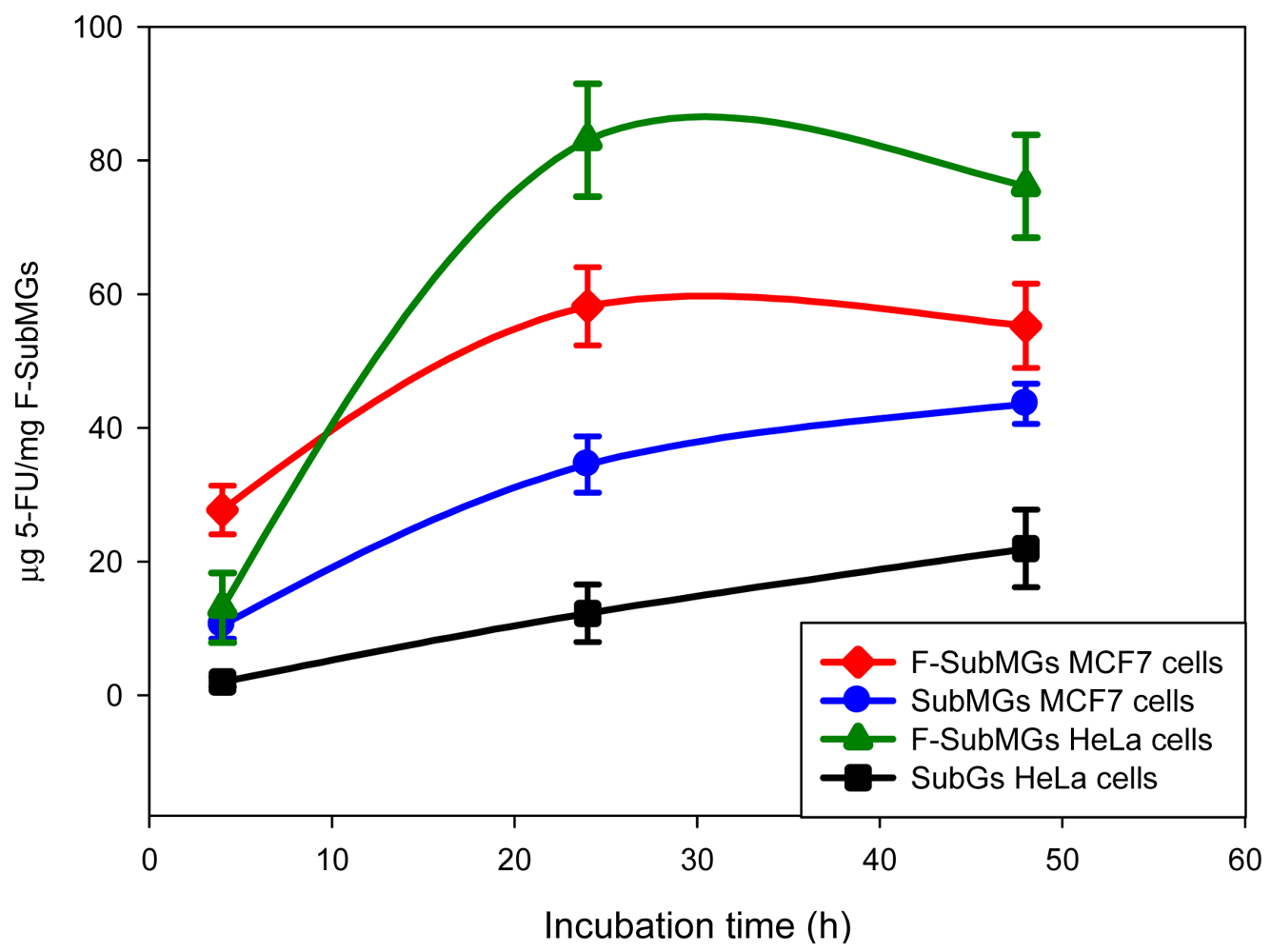
Cell uptake of control submicrogels (SubMGs) was observed in both cell types, and was larger for MCF7 cells at all incubation times (Figure 3). So that, after 4 h, 24 h and 48 h of incubation, penetration of SubMGs into cells was 10.51%, 34.52%, and 43.59%, respectively in MCF7 cells, and it was 2%, 12.26% and 21.94%, respectively in HeLa cells. Thus, the uptake of these SubMGs took place by unspecific mechanisms, and was more favorable in MCF7 cells.
Cell uptake of folate-submicrogels (F-SubMGs) was larger for MCF7 cells at 4 h of incubation (25%), than in HeLa cells (15%). However, the presence of folic acid on the nanogel surface caused a significant improvement of the submicrogels uptake in HeLa cells compared to MCF7 cells after 24 h of incubation (80.04% for HeLa; 58.18% for MCF7) whose level was maintained at 48 h (Figure 3).
These results can be related to the expression of folate receptor (FR) in one of two celullar lines studied. The carried out studies have shown that the FR type α levels in the tumors are variable and are generally relatively low in estrogen receptor positive (ER(+)) tumors [30]. It has been described that HeLa cells are FR(+), but MCF7 cells are FR(−) and ER(+) [31]. Therefore, the uptake of F-SubMGs in MCF7 is mainly by unspecific interactions, although the presence of folic acid seemed to improve the uptake when compared with that of control sample. In this way, Lee and co-workers [32] observed in MCF7 cells that the introduction of folate into adriamycin-loaded polyHis/PEG-folate micelles and PLLA/PEG-folate micelles enhanced the cell killing effect by active internalization with respect to the same micelles without folate.
Our studies on cell uptake of F-SubMGs showed that these submicrogels were internalized into both types of cells, independently of the presence of FR on their surface, although the percentage of HeLa cells that internalized the F-SubMGs was higher. In this way, studies carried out by Sonvico and co-workers [31] with folate-conjugated iron oxide nanoparticles showed that these nanoparticles were taken up by HeLa as well as MCF7 cells in a similar proportion after 30 min of incubation with the nanoparticles. Although in our studies, the percentage of cell uptake of folate conjugated submicrogels in HeLa cells was slightly larger than MCF7 cells. Therefore, the largest fluorescence signal in HeLa cells, which are FR(+), seemed to indicate that they are able to internalize more of this nanocarrier, thereby producing the entry of the functionalized submicrogels mainly by a receptor-mediated endocytosis.
Cell viability was evaluated by the methylthiazoletetrazolium (MTT) method to study the cytocompatibility of unloaded F-SubMGs and antitumoral availability of low load 5-FU-loaded F-SubMGs.
The range of cell survival, in the presence of low concentrations of unloaded F-SubMGs (80 μg/mL), was between 99 ± 8% and 96 ± 13% for MCF7 (Figure 4(A)), and between 94 ± 11% and 91 ± 12% for HeLa cells (Figure 4(B)) during 3 days of incubation. Thus, these F-SubMGs had good biocompatibility and produced minimal cytotoxicity. However, as the concentration of unloaded F-SubMGs increased up 400 μg/mL, a cytotoxicity effect was observed, specially in MCF7, whose range of cell survival was between 63 ± 3% and 80 ± 11%, whereas in HeLa cells was between 92 ± 4% and 87 ± 7%. Therefore, since MCF7 are FR(−), the greater sensitivity observed in these breast cancer cells may be related to nonspecific interactions, rather than a receptor-mediated endocytosis as was indicated above in studies of cellular uptake.
On the other hand, two concentrations of 5-FU (10 and 50 μM) were administered to MCF7 and HeLa cells by drug solution and by 5-FU-loaded F-SubMGs (Figure 5). The concentration range of free 5-FU was selected based on preliminary experiments, in which increasing concentrations of 5-drug from 0.01 μM to 1 mM were tested in culture. Those drug concentrations were in accordance with data reported in the literature [33-35]. The administration of 5-FU 10 μM in solution produced a decrease of the percentage of viability in MCF7 cells, which was between 91 ± 8% and 43 ± 3% after 3 days of incubation.
When the drug was administered by 5-FU-loaded F-SubMGs at the same drug concentration, the viability was lower (between 77 ± 12% and 32 ± 10%) (Figure 5(A)). Since this F-SubMGs concentration (80 μg/mL) did not cause cytotoxic effect on MCF7 cells (Figure 4(A)), the efficacy of 5-FU administered by 5-FU-loaded F-SubMGs was evident. When 5-FU concentration was larger (50 μM), a decrease in viability was also observed in the presence of the drug in solution (77 ± 10%–31 ± 4%) as well as 5-FU-loaded F-SubMGs (37 ± 2%–14 ± 2%). In this case, the decrease in cell viability is due to the drug administered by 5-FU-loaded F-SubMGs, but a percentage of the observed decrease must be attributed to the high F-SubMGs concentration (Figure 4(A)).
The survival of HeLa cells was not modified by increasing 5-FU concentration (Figure 5(C,D)), which indicated a lower sensitivity to this drug than MCF7 cells. The administration of 5-FU in solution at 10 and 50 μM caused a similar decrease in HeLa viability (87 ± 11%–40 ± 8% at 10 μM; 78 ± 4%–39 ± 2% at 50 μM). The administration of the drug by 5-FU-loaded F-NGs produced the same effect as the drug in solution at the beginning of the experiment, which was in accordance with the low percentage of F-NGs uptake at short time (Figure 4) and the kinetic release of the drug (Figure 2) from F-NGs.
2.3. In Vivo Studies: Biocompatibility and Pharmacokinetic
The in vitro 5-FU release, as well as the effect of 5-FU-loaded F-SubMGs on viability of MCF7 and HeLa cells, inform on the possible use of this system for targeted drug administration as potential antitumoral treatment. However, it is necessary to know the behavior of 5-FU-loaded F-SubMGs in vivo, because the presence of physiological substances, such as enzymes, ions, or cells, may influence the drug release. Moreover, the interaction between the 5-FU-loaded F-SubMGs and the living tissues can be harmless for the organism. So that, 5-FU-loaded F-SubMGs were subcutaneously administrated to rats in order to evaluate their biocompatibility and the plasma levels of the drug in blood stream. The small size of submicrogels allowed their subcutaneous implantation in the back of rats by injection using a conventional syringe. The amount of unloaded and drug-loaded F-SubMGs injected was 133 mg, which corresponds with the selected dose of 5-FU (28 mg 5-FU/kg b.w) taking into account the 5-FU load of the high load formulation (46.8 ± 3.8 μg 5-FU/mg F-SubMGs).
The maximum tolerated dose of 5-FU in rats is 100 mg/kg of body weight [36], and doses of 20 mg/kg of 5-FU has also been administered by intraperitoneal route in rats for seven days [37]. Furthermore, 35 and 50 mg/Kg b.w. have been subcutaneously administered in rats by polyester microspheres [38]. Hence, the dose utilized in our experiment was in accordance with above mentioned doses.
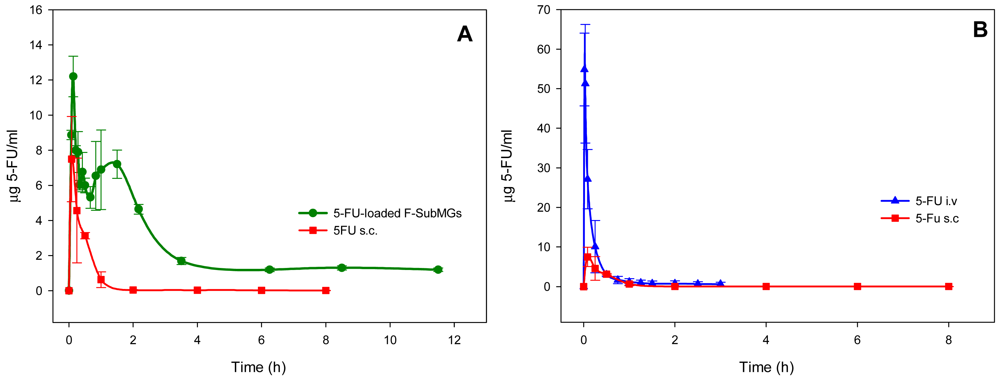
After administration of 5-FU loaded F-SubMGs (Figure 6(A)), the drug was detected in the blood stream at 5 min, and the maximum drug concentration (12.2 ± 1.1 μg/mL) was reached at 8 min. Then, the drug concentration in plasma decreased at 40 min, to increase again reaching a second maximum at 90 min (7.2 ± 0.8 μg/mL). From then, a decrease of 5-FU plasma concentration was observed up to 3.5 h, and 5-FU concentration was almost constant (≈1.2 μg/mL) up to 11.5 h. The plasma concentration of 5-FU obtained during the first stage of release from F-SubMGs can be considered the result of the quick release of the drug observed in vitro. Whereas, the following lower levels of the drug in vivo seemed to be caused by the slower second stage of in vitro 5-FU release from nanocarriers.
When 5-FU was intravenously administered at the same dose in solution, the maximum drug concentration was 55 ± 9 μg/mL and it was not detected starting at 3 h (Figure 6(B)). The subcutaneous injection of 5-FU in solution resulted in a maximum concentration of 7.2 ± 2 μg/mL, 5 min after administration, with the drug being detected in plasma for 8 h (Figure 6(B)).
Differences observed in residence time and in plasma concentration of 5-FU showed the effect of the administration route as well as the different formulation of the drug used. When a drug is given in different dosage forms or by different routes of administration, it will yield varying amounts of absorbed drug and, hence, differences in onset, intensity, and duration of the pharmacologic or clinical effect [39]. After its administration, the drug has to be released from the dosage form and then be absorbed into the systemic circulation by passing through various membranes, except when the drug is administered intravenously in the form of a solution [39]. A polymer drug delivery system exerts a protection on the loaded drug against its degradation or metabolism. In the case of 5-FU, its pharmacokinetic is characterized by a rapid distribution and elimination phases resulting in a short plasma half-life (10–20 min) [40].
After administration, 5-FU is metabolized by extracellular catabolic or intracellular anabolic pathways. More than 85% of an administered dose of this anticancer agent is degraded through the catabolic pathway in the liver by dihydropyrimidine dehydrogenase (DPD) [1,41], and only a reduced part of 5-FU is available for bioactivation. DPD is the rate-controlling enzyme of endogenous pyrimidine and fluoropyrimidine catabolism [1]. This enzyme is present in most of the tissues including liver and peripheral blood mononuclear cells, although the DPD activity is much greather in liver than in any other tissue as gastrointestinal tract, kidney and spleen [40]. DPD activity is highly variable in the population [1]. In this way, a considerable variability (interpatient and intrapatient) in pharmacokinetic studies of both bolus and continuous infusion therapy of 5-FU is thought to be due mainly to variability in DPD activity and consequent variability in the rate of catabolism. Moreover, DPD also displays a circadian variation [40].
Thus, the drug absorption from polymer drug delivery systems after administration depends on the release of the drug from the carrier, the permeability across the tissue barriers, the dissolution of the drug under physiological conditions, and finally, the drug metabolism.
As mentioned above, the administration route and the formulation of 5-FU determined pharmacokinetics and responses to the drug. The values of pharmacokinetic parameters of 5-FU are summarized in Table 1. MRT and AUC reflect the residence time and amount of free drug respectively, in systemic circulation. AUC values allow to calculate the absolute [AB (%) = (AUC0∞s.c./AUC0∞i.v.) × (i.v. dose/s.c. dose) × 100] and relative bioavailability [42] [RB (%) = (AUC0∞nanogel s.c./AUC0∞solution s.c.) × 100] of different formulations of 5-FU. The absolute bioavailability of 5-FU was 33% when the drug in solution was subcutaneously administrated, whereas the relative bioavailability of 5-FU was 983% when 5-FU-loaded F-SubMGs was subcutaneously administered. On the other hand, the mean residence time (MRT) showed a larger value (4.4 and 7.2 times larger) when 5-FU was subcutaneously administered by F-SubMGs, in comparison with the subcutaneous and intravenous administered of 5-FU in solution (Table 1). Therefore, the more prolonged presence of 5-FU in plasma after its administration by F-SubMGs, can be considered an advantage for drugs with short half-life, due to a protection on the drug loaded into polymeric systems against its degradation or metabolism. Moreover, side effects of 5-FU on whole body, could be minimized by maximizing the drug concentration in the target tissues due to a possible uptake into a cell via receptor mediated endocytosis as active targeting of 5-FU-loaded F-SubMGs.
To evaluate the biocompatibility of F-SubMGs and follow the morphological changes of subcutaneously administered submicrogels, animals were sacrificed 15, 30 and 60 days after injection, and the tissue of the injection site was removed. A fibrous capsule, around the injected nanocarriers under the skin, was observed in every moment of study. This fact can be considered in accordance with the normal body reaction to a biocompatible material, which consists in walling it off in an avascular, collagenous bag. This event was also observed after the injection of unloaded and 5-FU-loaded PLA and PLGA microspheres [38].
Fifteen days after the nanogel injection, histological studies showed groups of nanogel surrounded by connective tissue inside of the capsule (Figure 7(A)). Lymphocytes or mast cells were not observed in any case. After thirty days of submicrogels injection, the histological study did not show differences with regard to the studies carried out at earlier times. However, at day sixty, more disperse and smaller groups of submicrogels, as well as a significant amount of collagen fibers between them, were observed inside of the capsule and there were blood vessels close to submicrogels groups (Figure 7(B)), whose size was reduced. Differences between animals injected with 5-FU-loaded F-SubMGs and animals injected with unloaded F-SubMGs were not observed in any case or at any time.
The implantation of biocompatible material induces the activation of humoral and cellular mechanisms to produce inflammatory and healing responses of the material. Polymorphonuclear leukocytes, monocytes and lymphocytes are the cell types associated with this event [38]. Accumulation of extravessel liquids in the implant area was not detected, which was indicative that there was not an acute inflammatory response when the animals were sacrificed. Thus, unloaded and 5-FU-loaded F-SubMGs did not cause immunological processes when they were subcutaneously injected, since lymphocytes or mast cells were not observed in the implants, and signs of rejection of the implanted submicrogels did not exist in any case. Therefore, histological studies carried out indicate that folate conjugate submicrogels analyzed in this work present a high biocompatibility with tissue where they are placed.
3. Experimental Section
3.1. Materials
5-Fluorouracil (Sigma-Aldrich, Barcelona, Spain), NaOH, KCl, NaCl, Na2HPO4, KH2PO4, K2HPO4 (Panreac, Barcelona, Spain) and Isoflurane (Isoba® vet, Schering-Plough, S.A., Madrid, Spain) were used as received. All the chemicals used were of the highest commercially quality available. Milli-Q® water (Millipore, Madrid, Spain) was used.
3.2. Preparation of 5-Fluorouracil-Loaded Folate-Conjugate Submicrogels (F-SubMGs)
Sub-microgel sample NPA35EA4AMP0.5FOL [26], whose composition is 4-nitrophenyl acrylate (NPA) 30 mol%, 4-methylpyridine (4-MP) 14 mol%, ethylamine (EA) 16 mol%, N-isopropylacrylamide (NIPAM) 70 mol% and folic acid concentration 1.3 ± 0.8 mmol/g sub-microgel, was used to obtain 5-Fluorouracil-loaded sub-microgels. Briefly, poly[(p-nitrophenyl acrylate)-co-(N-isopropylacrylamide)] [p(NPA-co-NIPAM)] precursor microgels were synthesized and characterized [25]. The p-nitrophenyl carboxylate groups in the initial microgels ensured an easy chemical functionalization by the nucleophilic attack of free amines. Furthermore, these modification reactions can be monitored by UV spectroscopy because p-nitrophenol, the leaving group during nucleophilic substitution at the carboxylate group, shows a characteristic absorbance peak at 400 nm. These reactive sub-microgels were specifically and partially functionalized with 4-MP in a first functionalization sequence, by the reaction with 4-aminomethylpyridine. The second step of the synthesis strategy was the introduction of EA groups, which allows the subsequent coupling of folic acid with the primary amine group. The functionalization with EA was carried out by the nucleophilic attack with previously synthesized N-ter-butoxycarbonylethylenediamine.
Folate-conjugate submicrogels (F-SubMGs) were loaded with 5-FU by immersion in solutions of the drug with two solution with different concentration (0.4 mg/mL and 7 mg/mL) in phosphate buffer (1 mM, pH 7.4) at room temperature for 72 h. The suspension was centrifuged (41,000 rpm, 15 min, Beckman Oulter OptimaL-100XP Ultracentrifuge), and then, the pellet was freeze-dried (Heto PowerDry LL 1500 Freeze Dryer, Thermo Electron Corporation).
Morphology of 5-FU-loaded F-SubMGs was determined by SEM (Jeol JSM-6400 Electron Microscope, 150 s, 20 mA, 2 kV). The samples were fixed to an adhesive sheet on a rigid support and coated with gold for their later visualization.
3.3. Estimation of 5-Fluorouracil Content
To determine the amount of 5-FU included in the F-SubMGs, 10 mg of the drug-loaded submicrogels were swollen in 10 mL of phosphate buffer (1 mM, pH 7.4) at 25 °C (since LCST of PNIPA is 32 °C and NIPA gels are swollen at 25 °C) in orbital shaking (100 rpm) for 72 h. At intervals, the suspension was vigorously shaken in vortex and centrifuged (41,000 rpm, 15 min). Then, 100 μL of supernatant was collected, and used to determinate the amount of 5-FU by HPLC (Spectra-Physics SP8800 HPLC pump, SP 100 UV absorbance detector and SP 4400 computing integrator) [38]. The stationary phase was Spherisorb ODS2, C18, 5 μm (25 × 0.46 cm; Waters), and the mobile phase was KH2PO4 0.01 M, pH 4. The flow rate was set at 1 mL/min and the detector wavelength was 266 nm. For calibration curve, solutions of 5-FU in phosphate buffer (1 mM, pH 7.4) between 0.025–100 μg/mL were used, and a good linear correlation (r2 = 0.99) was obtained. The validity of the HPLC method was demonstrated from the precision of the assay calculating the coefficient of variation (CV) [43]. The CV for intra-run of 5-FU at 0.025, 0.1, 5 and 75 μg/mL were 4.1%, 3.1%, 2.1% and 1.4% respectively; and 7.7%, 6.5%, 3.7% and 2.4% for inter-run at the same concentrations. The 5-FU retention time was 6.81 ± 0.15 min. Stability of 5-FU was also studied by UV/Vis Spectra (188-600 nm) (UNICAM 8700 Spectrophotometer). The experiment was carried out in triplicate.
3.4. In Vitro Release of 5-Fluorouracil from Folate-Conjugate Submicrogels (F-SubMGs)
For drug release studies, 10 mg of 5-FU-loaded F-SubMGs were added to 2 mL phosphate buffer (1 mM, pH 7.4) contained in a dialysis bag (6–8000, Serva 20/32) which was placed in an erlenmeyer containing 10 mL of the same phosphate buffer at 37 °C and at constant shake (100 rpm) in an orbital incubator (Ecotron® Inforts AG CH-4103). At intervals, 100 μL of samples were withdrawn from the solution in order to follow the change in 5-FU concentration by HPLC method described above. The release medium removed from the vessel was replaced with the same volume of phosphate buffer. In drug release experiments, 5-FU concentrations was always very much lower than its solubility; thus, sink conditions were maintained. The experiments were carried out in triplicate. In order to determine the time for the drug to reach dialysis equilibrium, a solution of 5-FU (5 mL of 0.56 mg/mL) in phosphate buffer (1 mM, pH 7.4) were dialysed. The time at which the drug in solution needed to reach dialysis equilibrium was 1 h.
3.5. In Vitro Cell Culture Studies
3.5.1. Cell Culture Maintained
Human breast adenocarcinoma (MCF7) cells were obtained from von Kobbe and human cervical cancer (HeLa) cells were obtained from Dr. Tierrez. Cells were maintained in DMEM (Dulbecco's Modified Eagle Medium) + GlutaMax-I supplemented with 10% heat inactivated fetal bovine serum, penicillin (50 U/mL) (GIBCO®, Invitrogen Life Technologies, Grand Island, NY, USA), streptomycin (50 μg/mL) (Invitrogen Life Technologies) and gentamicin (50 μg/mL) (Sigma-Aldrich Company, UK) in a humidified incubator at 37 °C and 5% CO2 atmosphere (HERA cell, Sorvall Heraeus, Kendro Laboratory Products Gmbh, Hanau, Germany). Cells were plated in 75-cm2 flask (Sarstedt Ag and Co., Barcelona, Spain) and were passaged when reaching 95% confluence, by gentle trypsinization (0.05% trypsin/0.53 mM EDTA; Invitrogen Life Technologies).
3.5.2. Cellular Uptake of Submicrogels
Cellular uptake of submicrogels was investigated with a mono-culture of MCF7 and HeLa cells. Submicrogels (1 mg) were loaded with Alexa Fluor® 488 (A488; Molecular Probes, Eugene, OR) by immersion in a solution of A488 in DMSO (20 μg A488/100 μL DMSO) at 4 °C in dark for 48 h under orbital shaking (100 rpm). Then, submicrogels were freeze-drying at −110 °C. In order to establish a comparison between the cell uptake of folate-conjugate submicrogels (F-SubMGs) and submicrogels without folate, control submicrogels (SubMGs) of equivalent composition (sample R35EA4AMP0.5) [26] were used.
Cells were seeded in 24-well flat-bottom plates at 50,000 cells/well for MCF7 and 25,000 cells/well for HeLa. Twenty-four hours later, the medium was replaced with 1 mL medium with 1% FBS containing 377 μg of Alexa Fluor® 488-loaded submicrogels per mL of growth medium, which is very similar to the maximum concentration of submicrogels used in viability studies. As a control, cells were grown separately with 4 μL of Alexa Fluor® 488 per well in the absence of submicrogels. Cells were incubated during 24 h for microscopy studies and 4, 24 and 48 h for flow cytometry studies. Afterward, cells were washed three times with phosphate buffer saline (PBS) to remove submicrogels not internalized by the cells.
After final washing, PBS was replaced with 1 mL of growth medium in order to carry out microscopy studies. Localization of fluorescent dye was examined by light fluorescence microscopy (Leica DMIL microscope, Leica Microsystems, Switzerland). Cells cultures were photographed with a Leica DFC 300FX digital camera and used Leica Application Suite software for processing the pictures (Leica Microsystems, Switzerland).
Additionally, internalization of submicrogels into MCF7 and HeLa cells was evaluated using flow cytometry. Cells were harvested, washed with PBS, resuspended in PBS and analyzed in a FACScan flow cytometer using CellQuest software (BD Biosciences, Mountain View, CA, USA). Cells were analyzed by gating based on forward and side scatter. Results are expressed as percent positive cells for uptake of submicrogels referred to auto-fluorescence of cells.
3.5.3. Cytotoxicity Assay
Cell viability was evaluated by using the methylthiazoletetrazolium (MTT; Sigma-Aldrich) method. All experimental conditions were performed in quintuplicate. Each experiment was carried out in triplicate. In preliminary experiments, increasing concentrations of 5-FU from 0.01 μM to 1 mM were tested in culture. The selected drug concentrations were 10 and 50 μM. Cells were seeded in 96-well flat-bottom plates at 5,000 cells/well in the case of MCF7 and at 2500 cells/well in the case of HeLa. Twenty-four hours later, the medium was replaced with 100 μL medium with 1% fetal bovine serum (FBS; Invitrogen Life Technologies) containing F-SubMGs, 5-FU-loaded F-SubMGs or the drug in solution. The amount of F-SubMGs was between 80 μg/mL and 400 μg/mL (Table 2), which was in accordance with the concentration of 5-FU used in the experiment, considering the low load 5-FU-loaded F-SubMGs. After 1, 2 and 3 days, each well was added with 10 μL MTT solution (5 mg/mL). After 2 h incubation at 37 °C, 5% CO2, each well was replaced with 100 μL DMSO [44]. The cell viability was determined by measuring the absorbance at 570 nm using a spectrophotometer (Varioskan, Thermo Fisher Scientific, Barcelona, Spain). Results are presented as the percentage survival in relation to untreated control cells.
3.4. In Vivo 5-FU Administration
The study protocol was approved by the Animal Experimentation Ethics Committee of the Universidad Complutense de Madrid. Female Wistar rats, weighing 222 ± 4 g, were obtained from the Animalario of the Universidad Complutense de Madrid (Spain) which operates according to the requirements relating to animal experimentation regulations (DC 86/609/CEE; RD 223/1988; OM 13/X/1989, RD 1201/2005). Guidelines contained in NIH publication on the Principles of Laboratory Animal Care 85-23 revised in 1985 were followed throughout. The animals were housed in cages under environmentally controlled conditions of light (12:12 h light:dark cycle), temperature (22 ± 2 °C) and humidity (65–70%). They were fed standard rat food and water ad libitum. The surgical material used in the experiment was previously autoclaved. Just before injection, the dissolution solvent was put under ultraviolet light (Ecogen Lamp, Viber Lourmat, Intensity 7 mW/cm2) at 254 nm for 4 s because of the germicidal action of this wavelength.
Different groups of animals were established using six animals per group. Group 1: Animals injected with 133 mg of high load 5-FU-loaded F-SubMGs. Group 2: Animal injected with 133 mg of F-SubMGs without drug. Submicrogels were dispersed in 1 mL of saline solution (0.9% NaCl) and subcutaneously injected in the upper part of the back of the rat using a sterile syringe with a 1.2 × 40 mm nozzle (Microlance 3). Group 3: Animals subcutaneously injected with 1 mL of a saline solution of 5-FU. Group 4: Animals intravenously injected with 1 mL of a saline solution of 5-FU by femoral vein cannulation with polyethylene tubing. The dose of 5-FU used in those experiments was 28 mg/kg body weight (b.w.), and the amount of drug administered with submicrogels and in solution was 6.3 ± 0.1 mg/mL. The animals were anaesthetized with an equipment of isoflurane (Burtons, Series 5 T.C.V. Kent, UK).
3.5. Determination of 5-Fluorouracil in Plasma
At predetermined times after the injection of 5-FU-loaded F-SubMGs and the 5-FU solutions, animals were anaesthetized with isoflurane. Blood (0.3 mL) was collected by puncturing the jugular vein in heparinized (75 units = 15 μL) polypropylene tubes. Blood samples were taken from rats subcutaneously injected with 5-FU-loaded F-SubMGs at 1.5, 2, 3.5, 8.5, 11.5, 32, and 50 h after the injection and at 24 h intervals thereafter. Animals which were injected with 5-FU in solution, blood samples were taken 5, 15, 30 min, 1, 2, 4, 6, 8, 27, 48, 58, 72 h after subcutaneous administration; and 1, 2, 5, 15, 30, 45 min, 1, 1.25, 1.5, 2, 2.5, 3 and 4.5 h after intravenous administration. The heparinized blood was centrifuged at 10,000 rpm for 10 min in a Sigma 202 M centrifuge immediately after collection so as to obtain plasma. Plasma samples were then stored at −20 °C.
5-FU was extracted from plasma samples according to a modification of the method proposed by Buckpitt and Boyd [45]. 7.5 μL of trichloroacetic acid 2 M was added to 150 μL of plasma. After shaking and centrifugation (11,000 rpm, 10 min), supernatant was collected and placed into eppendorf tubes. 30 μL of phosphate buffer (0.5 M, pH 8) and 1.8 mL of ethyl acetate were added. After vigorous shaking for 10 min and centrifugation (11,000 rpm, 10 min), the organic phase was collected and evaporated at 55 °C. The samples were reconstituted with 50 μL of KH2PO4 0.01 M, pH 4, and 5-FU concentration was determined by the HPLC system [38]. For calibration, drug-free plasma pooled with known amounts of 5-FU, to obtain a 5-FU concentration between 0.01 μg/mL and 100 μg/mL, was used after undergoing the same extraction procedure. 5-FU standards were run for external standardization and a linear curve with a correlation coefficient of 0.99 was generated from the area under the peak measurements. The validity of the method was investigated by the determination of precision of the assay, which was demonstrated by the coefficients of variations (CV). For concentrations of 0.5, 10, 50 and 100 μg 5-FU/mL, CV for intra-run were 5.8, 5.5, 6.0 and 1.0%, respectively; and CV for inter-run were 4.6, 9.4, 6.3 and 3.2%, respectively. The 5-FU retention time was 6.3 ± 0.2 min.
3.6. Pharmacokinetic Parameters
Non-compartmental analysis was performed. The basic calculation are based on the area under the plasma concentration versus times curve (AUC) (zero moment) and the first moment curve (AUCM). The AUC can be calculated by the trapezoidal rule. The AUCM is the area under the concentration times time versus time curve, and it can be also calculated by the trapezoidal rule. From the AUC and AUCM values, the mean residence time (MRT) was calculated (MRT = AUMC/AUC) [46]. Data analysis of the pharmacokinetic parameters was performed by unpaired Student's t-test. A value of p < 0.05 was considered significant.
3.7. Biocompatibility Studies
Animals were sacrificed in CO2 atmosphere 15, 30 and 60 days after the subcutaneous injection of F-SubMGs. An incision was made on the rat back to remove the tissue around the place of the injection. A piece of the removed tissue, fixed with formol (10% v/v), was immersed in paraffin. Cuts (10 μm) were carried out with a paraffin microtome (Minot type). Samples were dyed using the alcian blue hemalum picro-indigo, the toluidine blue, and the hematoxilin-eosin methods [47] and histological studies were carried out.
4. Conclusions
We have evaluated folate-conjugate poly[(p-nitrophenyl acrylate)-co-(N-isopropylacrylamide)] submicrogels (F-SubMGs) as 5-Fluorouracil (5-FU) delivery systems. Submicrogels can be successfully loaded by swelling in 5-FU solutions in phosphate buffer. The complete in vitro drug release took place in 8 h with two stage drug release and different rates. Unloaded F-SubMGs are not toxic to MCF7 and HeLa cells in vitro up to high concentrations, and 5-FU-loaded F-SubMGs present effective elimination of carcinoma cells. The presence of folate in the submicrogels enhances their internalization in HeLa cells, which are receptor folate positive. In the case of MCF7 line, it is mainly produced by a nonspecific mechanism. Moreover, subcutaneous injection of F-SubMGs does not cause an acute inflammatory response or rejection signs. Subcutaneous drug administration by 5-FU-loaded F-SubMG increases the mean residence time of drug. Therefore, the developed non-toxic folate-conjugate submicrogels have high potential to control the release of 5-FU, which may lead to a new option for treating several cancer malignances.

 ); A488 SubMGs in MCF 7 cells (
); A488 SubMGs in MCF 7 cells (
 ); A488 F-SubMGs in HeLa cells (
); A488 F-SubMGs in HeLa cells (
 ); A488 SubMGs in HeLa cells (
); A488 SubMGs in HeLa cells (
 ).
).
 ); A488 SubMGs in MCF 7 cells (
); A488 SubMGs in MCF 7 cells (
 ); A488 F-SubMGs in HeLa cells (
); A488 F-SubMGs in HeLa cells (
 ); A488 SubMGs in HeLa cells (
); A488 SubMGs in HeLa cells (
 ).
).
 ) or with unloaded F-SubMGs at a concentration 80 μg/mL (
) or with unloaded F-SubMGs at a concentration 80 μg/mL (
 ); 400 μg/mL (
); 400 μg/mL (
 ); Concentration of F-SubMGs was in accordance with data of Table 2. Data were shown as mean ± SD (n = 15).
); Concentration of F-SubMGs was in accordance with data of Table 2. Data were shown as mean ± SD (n = 15).
 ) or with unloaded F-SubMGs at a concentration 80 μg/mL (
) or with unloaded F-SubMGs at a concentration 80 μg/mL (
 ); 400 μg/mL (
); 400 μg/mL (
 ); Concentration of F-SubMGs was in accordance with data of Table 2. Data were shown as mean ± SD (n = 15).
); Concentration of F-SubMGs was in accordance with data of Table 2. Data were shown as mean ± SD (n = 15).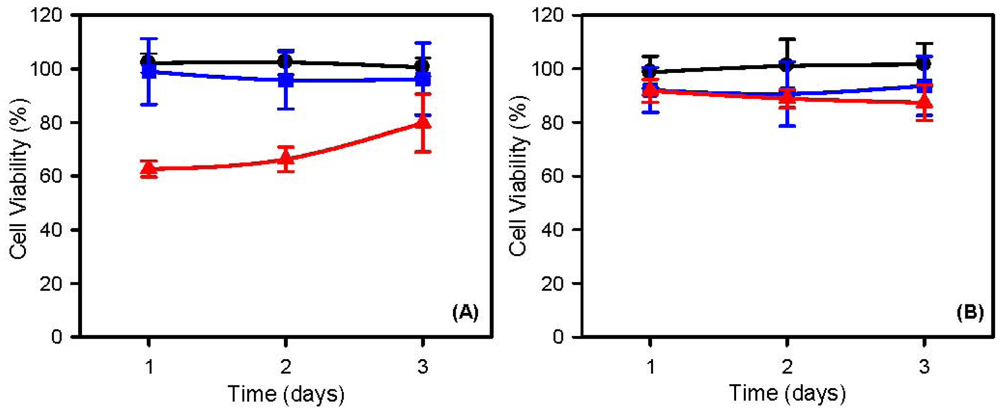
 ); 5-FU in solution (
); 5-FU in solution (
 ); 5-FU-loaded F-SubMGs (
); 5-FU-loaded F-SubMGs (
 ). Data were shown as mean±SD (n =15).
). Data were shown as mean±SD (n =15).
 ); 5-FU in solution (
); 5-FU in solution (
 ); 5-FU-loaded F-SubMGs (
); 5-FU-loaded F-SubMGs (
 ). Data were shown as mean±SD (n =15).
). Data were shown as mean±SD (n =15).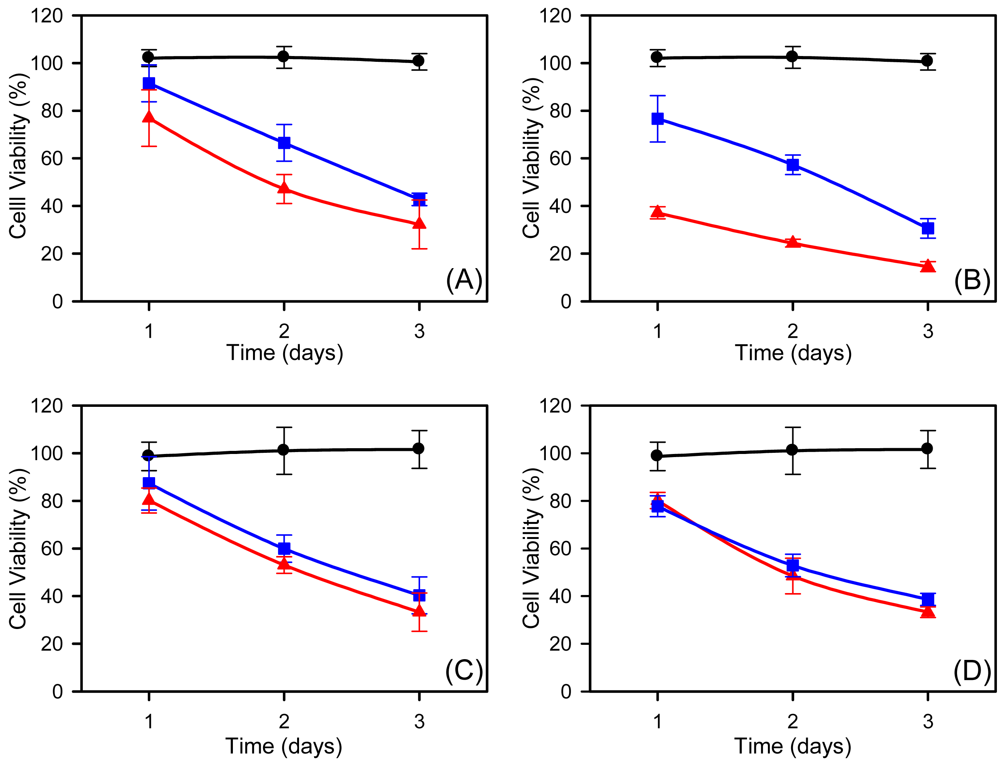

| 5-FU-loaded F-SubMGs | 5-FU s.c. | 5-FU i.v. | |
|---|---|---|---|
| AUC0∞(μg·h/mL) | 36.4 ± 2.3 a | 3.7 ± 1.1b | 11.2 ± 3.9 |
| AUMC0∞ (μg·h2/mL) | 233.4 ± 9.1a | 4.1 ± 0.7 | 10.4 ± 5.9 |
| MRT (h) | 6.5 ± 0.1a | 1.2 ± 0.4 | 0.9 ± 0.3 |
Data are presented as mean ± standard deviation (n = 6). Dose of 5-FU: 28 mg 5-FU/kg body weight; i.v.: intravenous administration; s.c.: subcutaneous administration. AUC: area under the plasma concentration versus times curve; AUMC: area under the concentration times time versus time curve; MRT: mean residence time;a: significant difference with regard to 5-FU s.c. y 5-FU i.v injection groups, p ≤ 0.05.b: significant difference with regard to 5-FU i.v injection group, p ≤ 0.05.
| Formulation | 5-FU load (μg 5-FU/mg F-SubMGs) | Concentration of F-SubMGs (μg/mL) to obtain | |
|---|---|---|---|
| 10 μM of 5-FU | 50 μM of 5-FU | ||
| Low load 5-FU-loaded F-SubMGs | 16.2 ± 1.9 | 80 | 400 |
Acknowledgments
The financial support from the Ministerio de Ciencia e Innovación of Spain (MAT 2010-21509-CO3-02) and the UCM-CAM for Consolidated Research Groups (Group 920613) is gratefully acknowledged. The authors are grateful to von Kobbe (Chimera Pharma of Bionostra Group) and Tierrez (Centro Nacional de Investigaciones Cardiovasculares, CNIC, Spain) for the gift of MCF7 and HeLa cell lines.
References
- Ofverholm, A.; Arkblad, E.; Skrtic, S.; Albertsson, P.; Shubbar, E.; Enerback, C. Two cases of 5-fluorouracil toxicity linked with gene variants in the DPYD gene. Clin. Biochem. 2010, 43, 331–334. [Google Scholar]
- Moehler, M.; Teufel, A.; Galle, P.R. New chemotherapeutic strategies in colorectal cancer. Recent Results Cancer Res. 2005, 165, 250–259. [Google Scholar]
- Goldberg, R.M.; Sargent, D.J.; Morton, R.F.; Fuchs, C.S.; Ramanathan, R.K.; Williamson, S.K.; Findlay, B.P.; Pitot, H.C.; Alberts, S. Randomized controlled trial of reduced-dose bolus fluorouracil plus leucovorin and irinotecan or infused fluorouracil plus leucovorin and oxaliplatin in patients with previously untreated metastatic colorectal cancer: A North American Intergroup Trial. J. Clin. Oncol. 2006, 24, 3347–3353. [Google Scholar]
- Pohl, A.; Lurje, G.; Manegold, P.C.; Lenz, H.J. Pharmacogenomics and -genetics in colorectal cancer. Adv. Drug Deliv. Rev. 2009, 61, 375–380. [Google Scholar]
- Yarden, Y.; Baselga, J.; Miles, D. Molecular approach to breast cancer treatment. Semin. Oncol. 2004, 31, 6–13. [Google Scholar]
- Gunzburg, W.H.; Lohr, M.; Salmons, B. Novel treatments and therapies in development for pancreatic cancer. Expert Opin. Investig. Drugs 2002, 11, 769–786. [Google Scholar]
- Nishiyama, M.; Eguchi, H. Pharmacokinetics and pharmacogenomics in gastric cancer chemotherapy. Adv. Drug Deliv. Rev. 2009, 61, 402–407. [Google Scholar]
- Zinutti, C.; Kedzierewicz, F.; Hoffman, M.; Benoit, J.P.; Maincent, P. Influence of the casting solvent on the physico-chemical properties of 5-fluorouracil loaded microspheres. Int. J. Pharm. 1996, 133, 97–105. [Google Scholar]
- Yuan, F.; Qin, X.; Zhou, D.; Xiang, Q.Y.; Wang, M.T.; Zhang, Z.R.; Huang, Y. In vitro cytotoxicity, in vivo biodistribution and antitumor activity of HPMA copolymer-5-fluorouracil conjugates. Eur. J. Pharm. Biopharm. 2008, 70, 770–776. [Google Scholar]
- Chung, T.W.; Lin, S.Y.; Liu, D.Z.; Tyan, Y.C.; Yang, J.S. Sustained release of 5-FU from poloxamer gels interpenetrated by crosslinking chitosan network. Int. J. Pharm. 2009, 382, 39–44. [Google Scholar]
- Blanco, M.D.; Sastre, R.L.; Teijon, C.; Olmo, R.; Teijon, J.M. 5-Fluorouracil-loaded microspheres prepared by spray-drying poly(D,L-lactide) and poly(lactide-co-glycolide) polymers: Characterization and drug release. J. Microencapsul. 2005, 22, 671–682. [Google Scholar]
- Blanco, M.D.; Guerrero, S.; Teijón, C.; Olmo, R.; Pastrana, L.; Katime, I.; Teijón, J.M. Preparation and characterization of nanoparticulate poly(N-isopropylacrylamide) hydrogel for the controlled release of anti-tumour drugs. Polym. Int. 2008, 57, 1215–1225. [Google Scholar]
- Sastre, R.L.; Blanco, M.D.; Teijón, C.; Olmo, R.; Teijón, J.M. Preparation and characterization of 5-Fluorouracil-loaded poly(ε-caprolactone) microspheres for drug administration. Drug Dev. Res. 2004, 63, 41–53. [Google Scholar]
- Kim, S.; Kim, J.H.; Jeon, O.; Kwon, I.C.; Park, K. Engineered polymers for advanced drug delivery. Eur. J. Pharm. Biopharm. 2009, 71, 420–430. [Google Scholar]
- Moghimi, S.M.; Hunter, A.C.; Murray, J.C. Nanomedicine: Current status and future prospects. FASEB J. 2005, 19, 311–330. [Google Scholar]
- Ferrari, M. Cancer nanotechnology: Opportunities and challenges. Nat. Rev. Cancer 2005, 5, 161–171. [Google Scholar]
- Jabr-Milane, L.S.; van Vlerken, L.E.; Yadav, S.; Amiji, M.M. Multi-functional nanocarriers to overcome tumor drug resistance. Cancer Treat. Rev. 2008, 34, 592–602. [Google Scholar]
- Vasir, J.K.; Labhasetwar, V. Biodegradable nanoparticles for cytosolic delivery of therapeutics. Adv. Drug Deliv. Rev. 2007, 59, 718–728. [Google Scholar]
- Ross, J.F.; Chaudhuri, P.K.; Ratnam, M. Differential regulation of folate receptor isoforms in normal and malignant tissues in vivo and in established cell lines. Physiologic and clinical implications. Cancer 1994, 73, 2432–2443. [Google Scholar]
- Park, E.K.; Lee, S.B.; Lee, Y.M. Preparation and characterization of methoxy poly(ethylene glycol)/poly(epsilon-caprolactone) amphiphilic block copolymeric nanospheres for tumor-specific folate-mediated targeting of anticancer drugs. Biomaterials 2005, 26, 1053–1061. [Google Scholar]
- Aronov, O.; Horowitz, A.T.; Gabizon, A.; Gibson, D. Folate-targeted PEG as a potential carrier for carboplatin analogs. Synthesis and in vitro studies. Bioconjug. Chem. 2003, 14, 563–574. [Google Scholar]
- Shmeeda, H.; Mak, L.; Tzemach, D.; Astrahan, P.; Tarshish, M.; Gabizon, A. Intracellular uptake and intracavitary targeting of folate-conjugated liposomes in a mouse lymphoma model with up-regulated folate receptors. Mol. Cancer Ther. 2006, 5, 818–824. [Google Scholar]
- Blanco, M.D.; Olmo, R.; Teijón, J.M. Hydrogels. In Encyclopedia of Pharmaceutical Technology; Swarbrick, J., Boylan, J.C., Eds.; Marcel Dekker: New York, NY, USA, 2002; pp. 1–25. [Google Scholar]
- Guerrero-Ramírez, L.G.; Nuño-Donlucas, S.M.; Cesteros, L.C.; Katime, I. Smart copolymeric nanohydrogels: Synthesis, characterization and properties. Mat. Chem. Phys. 2008, 112, 1088–1092. [Google Scholar]
- Pérez-Álvarez, L.; Sáez-Martínez, V.; Hernáez, E.; Katime, I. Synthesis and characterization of pH-sensitive microgels by derivatization of npa-based reactive copolymers. Mat. Chem. Phys. 2008, 112, 516–524. [Google Scholar]
- Pérez-Álvarez, L.; Sáez-Martínez, V.; Hernáez, E.; Katime, I. Specific pH-responsive folate-conjugate microgels designed for antitumor therapy. Macromol. Chem. Phys. 2009, 210, 467–477. [Google Scholar]
- Garcia, O.; Trigo, R.M.; Blanco, M.D.; Teijon, J.M. Influence of degree of crosslinking on 5-fluorouracil release from poly(2-hydroxyethyl methacrylate) hydrogels. Biomaterials 1994, 15, 689–694. [Google Scholar]
- Davda, J.; Labhasetwar, V. Characterization of nanoparticle uptake by endothelial cells. Int. J. Pharm. 2002, 233, 51–59. [Google Scholar]
- Panyam, J.; Sahoo, S.K.; Prabha, S.; Bargar, T.; Labhasetwar, V. Fluorescence and electron microscopy probes for cellular and tissue uptake of poly(D,L-lactide-co-glycolide) nanoparticles. Int. J. Pharm. 2003, 262, 1–11. [Google Scholar]
- Kelley, K.M.; Rowan, B.G.; Ratnam, M. Modulation of the folate receptor alpha gene by the estrogen receptor: Mechanism and implications in tumor targeting. Cancer Res. 2003, 63, 2820–2828. [Google Scholar]
- Sonvico, F.; Mornet, S.; Vasseur, S.; Dubernet, C.; Jaillard, D.; Degrouard, J.; Hoebeke, J.; Duguet, E.; Colombo, P.; Couvreur, P. Folate-conjugated iron oxide nanoparticles for solid tumor targeting as potential specific magnetic hyperthermia mediators: Synthesis, physicochemical characterization, and in vitro experiments. Bioconjug. Chem. 2005, 16, 1181–1188. [Google Scholar]
- Lee, E.S.; Na, K.; Bae, Y.H. Polymeric micelle for tumor pH and folate-mediated targeting. J. Control. Release 2003, 91, 103–113. [Google Scholar]
- MacCarron, P.A.; Woolfson, A.; McCafferty, D.F.; Price, J.H.; Sidhu, H.; Hickey, G.I. Cytotoxicity of 5-Fluorouracil released from a bioadhesive patch into uterine cervical tissue. Int. J. Pharm. 1997, 151, 69–74. [Google Scholar]
- Gupte, A.; Ciftci, K. Formulation and characterization of paclitaxel, 5-FU and paclitaxel +5-FU microspheres. Int. J. Pharm. 2004, 276, 93–106. [Google Scholar]
- Hernandez-Vargas, H.; Ballestar, E.; Carmona-Saez, P.; von Kobbe, C.; Banon-Rodriguez, I.; Esteller, M.; Moreno-Bueno, G.; Palacios, J. Transcriptional profiling of MCF7 breast cancer cells in response to 5-Fluorouracil: Relationship with cell cycle changes and apoptosis, and identification of novel targets of p53. Int. J. Cancer 2006, 119, 1164–1175. [Google Scholar]
- Spector, T.; Cao, S.; Rustum, Y.M.; Harrington, J.A.; Porter, D.J. Attenuation of the antitumor activity of 5-fluorouracil by (R)-5-fluoro-5,6-dihydrouracil. Cancer Res. 1995, 55, 1239–1241. [Google Scholar]
- Zacharakis, E.; Demetriades, H.; Pramateftakis, M.G.; Lambrou, I.; Zaraboukas, T.; Koliakos, G.; Kanellos, I.; Betsis, D. Effect of IGF-I on healing of colonic anastomoses in rats under 5-FU treatment. J. Surg. Res. 2008, 144, 138–144. [Google Scholar]
- Sastre, R.L.; Olmo, R.; Teijon, C.; Muniz, E.; Teijon, J.M.; Blanco, M.D. 5-Fluorouracil plasma levels and biodegradation of subcutaneously injected drug-loaded microspheres prepared by spray-drying poly(D,L-lactide) and poly(D,L-lactide-co-glycolide) polymers. Int. J. Pharm. 2007, 338, 180–190. [Google Scholar]
- Ritschel, W.A.; Kearns, G.L. Handbook of Basic Pharmacokinetics—Including Clinical Applications, 6th ed.; American Pharmacists Association (APhA): Washington, DC, USA, 2004. [Google Scholar]
- Ackland, S.P.; Garg, M.B.; Dunstan, R.H. Simultaneous determination of dihydrofluorouracil and 5-fluorouracil in plasma by high-performance liquid chromatography. Anal. Biochem. 1997, 246, 79–85. [Google Scholar]
- Diasio, R.B.; Harris, B.E. Clinical pharmacology of 5-fluorouracil. Clin. Pharmacokinet. 1989, 16, 215–237. [Google Scholar]
- Shin, S.C.; Choi, J.S.; Li, X. Enhanced bioavailability of tamoxifen after oral administration of tamoxifen with quercetin in rats. Int. J. Pharm. 2006, 313, 144–149. [Google Scholar]
- Shah, V.P.; Midha, K.K.; Dighe, S.; McGilveray, I.J.; Skelly, J.P.; Yacobi, A.; Layloff, T.; Viswanathan, C.T.; Cook, C.E.; McDowall, R.D.; et al. Analytical methods validation: Bioavailability, bioequivalence, and pharmacokinetic studies. J. Pharm. Sci. 1992, 81, 309–312. [Google Scholar]
- Han, X.; Liu, J.; Liu, M.; Xie, C.; Zhan, C.; Gu, B.; Liu, Y.; Feng, L.; Lu, W. 9-NC-loaded folate-conjugated polymer micelles as tumor targeted drug delivery system: Preparation and evaluation in vitro. Int. J. Pharm. 2009, 372, 125–131. [Google Scholar]
- Buckpitt, A.R.; Boyd, M.R. A sensitive method for determination of 5-fluorouracil and 5-fluoro-2′-deoxyuridine in human plasma by high-pressure liquid chromatography. Anal. Biochem. 1980, 106, 432–437. [Google Scholar]
- Berrozpe, J.D. Biofarmacia y Farmacocinética. In Farmacocinética; Berrozpe, J.D., Lanao, J.M., Delfina, J.M.P., Eds.; Síntesis: Madrid, Spain, 1997; Volume I. [Google Scholar]
- Humason, G.L. Animal Tissue Techniques, 4th ed.; Freeman W. H.: New York, NY, USA, 1979. [Google Scholar]
© 2011 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Blanco, M.D.; Guerrero, S.; Benito, M.; Fernández, A.; Teijón, C.; Olmo, R.; Katime, I.; Teijón, J.M. In Vitro and In Vivo Evaluation of a Folate-Targeted Copolymeric Submicrohydrogel Based on N-Isopropylacrylamide as 5-Fluorouracil Delivery System. Polymers 2011, 3, 1107-1125. https://doi.org/10.3390/polym3031107
Blanco MD, Guerrero S, Benito M, Fernández A, Teijón C, Olmo R, Katime I, Teijón JM. In Vitro and In Vivo Evaluation of a Folate-Targeted Copolymeric Submicrohydrogel Based on N-Isopropylacrylamide as 5-Fluorouracil Delivery System. Polymers. 2011; 3(3):1107-1125. https://doi.org/10.3390/polym3031107
Chicago/Turabian StyleBlanco, M. Dolores, Sandra Guerrero, Marta Benito, Ana Fernández, César Teijón, Rosa Olmo, Issa Katime, and José M. Teijón. 2011. "In Vitro and In Vivo Evaluation of a Folate-Targeted Copolymeric Submicrohydrogel Based on N-Isopropylacrylamide as 5-Fluorouracil Delivery System" Polymers 3, no. 3: 1107-1125. https://doi.org/10.3390/polym3031107
APA StyleBlanco, M. D., Guerrero, S., Benito, M., Fernández, A., Teijón, C., Olmo, R., Katime, I., & Teijón, J. M. (2011). In Vitro and In Vivo Evaluation of a Folate-Targeted Copolymeric Submicrohydrogel Based on N-Isopropylacrylamide as 5-Fluorouracil Delivery System. Polymers, 3(3), 1107-1125. https://doi.org/10.3390/polym3031107




