Current Therapeutic Strategies and Novel Approaches in Osteosarcoma
Abstract
:1. Introduction
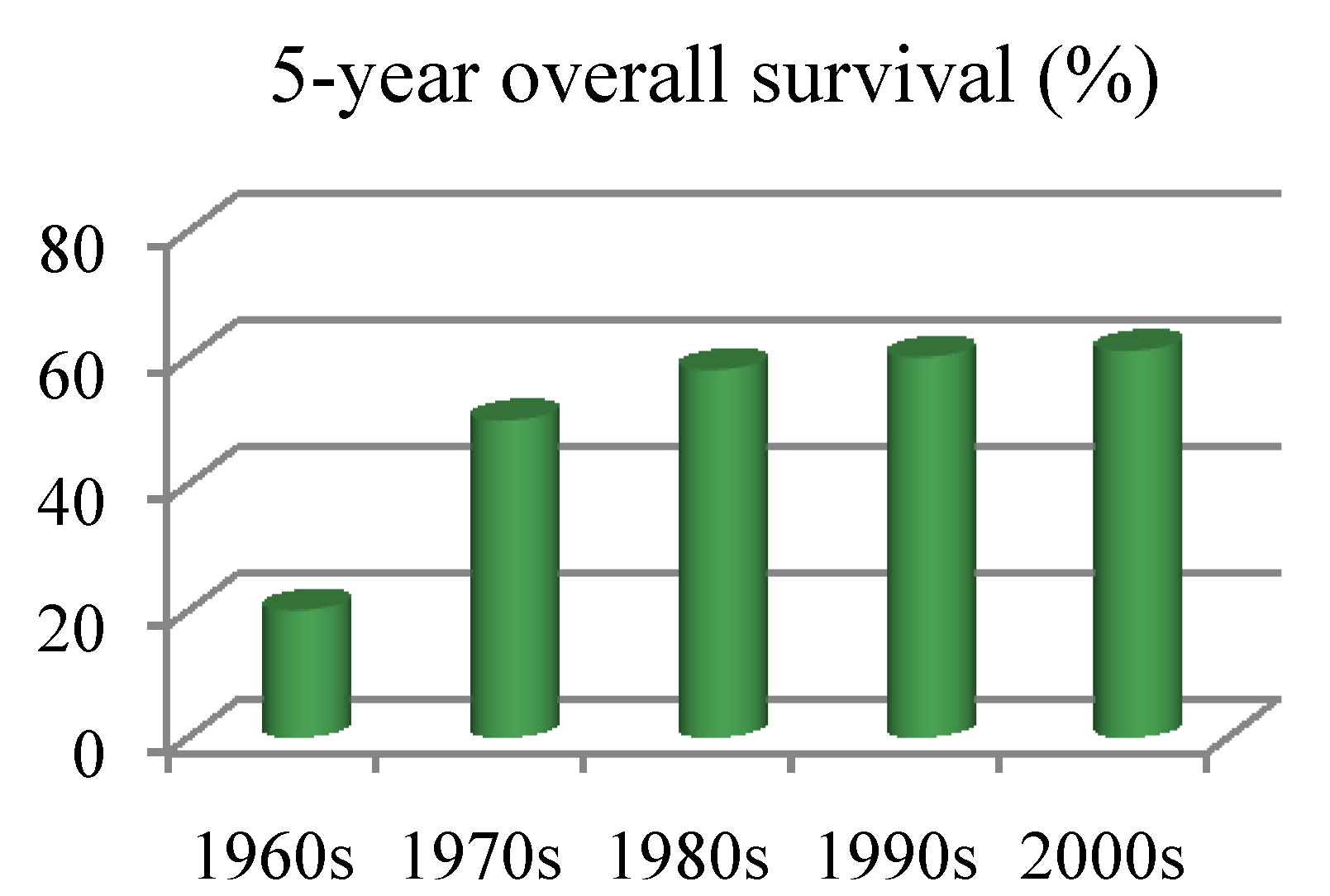
2. Current Therapies
2.1. Surgical Treatment
| Stage | Site | Grade | Metastasis |
|---|---|---|---|
| IA | Intracompartmental | Low | No |
| IB | Extracompartmental | Low | No |
| IIA | Intracompartmental | High | No |
| IIB | Extracompartmental | High | No |
| III | Any | Any | Regional or distant |
2.1.1. Amputation
| Margin | Dissection | Surgical option | |
|---|---|---|---|
| Limb-salvage | Amputation | ||
| Intralesional | Within tumor, intracapsular | Intracapsular, piece meal | Intracapsular |
| Marginal | Within reactive zone, extracapsular | Marginal en bloc | Marginal |
| Wide | Beyond reactive zone; Intracompartmental through normal tissue | Wide en bloc | Wide through-bone |
| Radical | Extracompartmental, normal tissue | Radical en bloc | Radical extra-articular |
2.1.2. Limb-Salvage Surgery
2.1.3. Limb Reconstruction
2.1.4. Local Recurrence after Surgery
2.1.5. Lung Metastasectomy
2.2. Chemotherapy
2.2.1. Standard Chemotherapy
| Agent | Mechanism of action |
|---|---|
| Doxorubicin | Doxorubicin intercalates at point of local uncoiling of the DNA double helix and inhibits the synthesis of DNA and RNA. |
| Cisplatin | Cisplatin, binding to tumor DNA, inhibits the DNA synthesis via the DNA crosslinks. |
| Methotrexate | Methotrexate is a folate antimetabolite and inhibits the synthesis of purine and thymidylic acid by binding dihydrofolate reductase. |
| Ifosfamide | Ifosfamide causes crosslinking of DNA strands, which inhibits the synthesis of DNA and protein. |
2.2.2. Novel Chemotherapies
2.2.3. Metastatic Osteosarcoma
2.3. Radiotherapy
2.3.1. Photon and Proton/Carbon Ion Radiotherapy
2.3.2. Prophylactic Irradiation for Lung Metastasis
2.3.3. Palliative Radiotherapy for Painful Bone Metastases
3. Emerging Therapies and New Therapeutic Targets
3.1. Immunomodulation
3.1.1. Interferons (IFNs)
3.1.2. Granulocyte-Macrophage Colony-Stimulating Factor (GM-CSF)
3.2. Intracellular Signal Pathway
3.2.1. Src
3.2.2. Mammalian Target of Rapamycin (mTOR)
3.2.3. Hedgehog (Hh)
3.3. Tyrosine Kinase Receptors
3.3.1. Insulin-like Growth Factor Receptor (IGF-R)
3.3.2. Human Epidermal Growth Factor Receptor 2 (HER-2)
3.3.3. Vascular Endothelial Growth Factor (VEGF)
3.3.4. Platelet-Derived Growth Factor (PDGF)
3.4. Drug Delivery System
3.5. Bone Metabolism
3.5.1. Bisphosphonates
3.5.2. RANK/RANKL/OPG Axis
4. Future Perspectives
Conflict of Interest
Acknowledgments
References
- Meyers, P.A.; Gorlick, R. Osteosarcoma. Pediatr. Clin. North Am. 1997, 44, 973–989. [Google Scholar] [CrossRef]
- Dorfman, H.D.; Czerniak, B. Bone cancers. Cancer 1995, 75, 203–210. [Google Scholar] [CrossRef]
- Stiller, C.A. International patterns of cancer incidence in adolescents. Cancer Treat. Rev. 2007, 33, 631–645. [Google Scholar] [CrossRef]
- Coventry, M.B.; Dahlin, D.C. Osteogenic sarcoma—A critical analysis of 430 cases. J. Bone Joint Surg. Am. 1957, 39, 741–757. [Google Scholar]
- Marcove, R.C.; Mike, V.; Hajek, J.V.; Levin, A.G.; Hutter, R.V. Osteogenic sarcoma under the age of twenty-one—A review of one hundred and forty-five operative cases. J. Bone Joint Surg. Am. 1970, 52, 411–423. [Google Scholar]
- Bacci, G.; Ferrari, S.; Bertoni, F.; Ruggieri, P.; Picci, P.; Longhi, A.; Casadei, R.; Fabbri, N.; Forni, C.; Versari, M.; et al. Long-term outcome for patients with nonmetastatic osteosarcoma of the extremity treated at the istituto ortopedico rizzoli according to the istituto ortopedico rizzoli/osteosarcoma-2 protocol: An updated report. J. Clin. Oncol. 2000, 18, 4016–4027. [Google Scholar]
- Kager, L.; Zoubek, A.; Potschger, U.; Kastner, U.; Flege, S.; Kempf-Bielack, B.; Branscheid, D.; Kotz, R.; Salzer-Kuntschik, M.; Winkelmann, W.; et al. Primary metastatic osteosarcoma: Presentation and outcome of patients treated on neoadjuvant cooperative osteosarcoma study group protocols. J. Clin. Oncol. 2003, 21, 2011–2018. [Google Scholar] [CrossRef]
- Bielack, S.; Kempf-Bielack, B.; Schwenzer, D.; Birkfellner, T.; Delling, G.; Ewerbeck, V.; Exner, G.U.; Fuchs, N.; Gobel, U.; Graf, N.; et al. Neoadjuvant therapy for localized osteosarcoma of extremities. Results from the cooperative osteosarcoma study group coss of 925 patients. Klin. Padiatr. 1999, 211, 260–270. [Google Scholar]
- Allison, D.C.; Carney, S.C.; Ahlmann, E.R.; Hendifar, A.; Chawla, S.; Fedenko, A.; Angeles, C.; Menendez, L.R. A meta-analysis of osteosarcoma outcomes in the modern medical era. Sarcoma 2012, 2012, 704872. [Google Scholar]
- Heymann, D.; Rédini, F. Bone sarcomas: Pathogenesis and new therapeutic approaches. IBMS BoneKEy 2011, 8, 402–414. [Google Scholar] [CrossRef]
- Jaffe, N.; Carrasco, H.; Raymond, K.; Ayala, A.; Eftekhari, F. Can cure in patients with osteosarcoma be achieved exclusively with chemotherapy and abrogation of surgery? Cancer 2002, 95, 2202–2210. [Google Scholar] [CrossRef]
- Marina, N.; Gebhardt, M.; Teot, L.; Gorlick, R. Biology and therapeutic advances for pediatric osteosarcoma. Oncologist 2004, 9, 422–441. [Google Scholar] [CrossRef]
- Bacci, G.; Ferrari, S.; Mercuri, M.; Longhi, A.; Fabbri, N.; Galletti, S.; Forni, C.; Balladelli, A.; Serra, M.; Picci, P. Neoadjuvant chemotherapy for osteosarcoma of the extremities in patients aged 41–60 years: Outcome in 34 cases treated with adriamycin, cisplatinum and ifosfamide between 1984 and 1999. Acta Orthop. 2007, 78, 377–384. [Google Scholar] [CrossRef]
- Rosen, G.; Caparros, B.; Huvos, A.G.; Kosloff, C.; Nirenberg, A.; Cacavio, A.; Marcove, R.C.; Lane, J.M.; Mehta, B.; Urban, C. Preoperative chemotherapy for osteogenic sarcoma: Selection of postoperative adjuvant chemotherapy based on the response of the primary tumor to preoperative chemotherapy. Cancer 1982, 49, 1221–1230. [Google Scholar]
- Bruland, O.S.; Hoifodt, H.; Saeter, G.; Smeland, S.; Fodstad, O. Hematogenous micrometastases in osteosarcoma patients. Clin. Cancer Res. 2005, 11, 4666–4673. [Google Scholar] [CrossRef]
- Marulanda, G.A.; Henderson, E.R.; Johnson, D.A.; Letson, G.D.; Cheong, D. Orthopedic surgery options for the treatment of primary osteosarcoma. Cancer Control 2008, 15, 13–20. [Google Scholar]
- Enneking, W.F.; Spanier, S.S.; Goodman, M.A. A system for the surgical staging of musculoskeletal sarcoma. Clin. Orthop. Relat. Res. 1980, 153, 106–120. [Google Scholar]
- Patel, S.J.; Lynch, J.W., Jr.; Johnson, T.; Carroll, R.R.; Schumacher, C.; Spanier, S.; Scarborough, M. Dose-intense ifosfamide/doxorubicin/cisplatin based chemotherapy for osteosarcoma in adults. Am. J. Clin. Oncol. 2002, 25, 489–495. [Google Scholar] [CrossRef]
- Friedman, M.A.; Carter, S.K. The therapy of osteogenic sarcoma: Current status and thoughts for the future. J. Surg. Oncol. 1972, 4, 482–510. [Google Scholar] [CrossRef]
- Grimer, R.J. Surgical options for children with osteosarcoma. Lancet Oncol. 2005, 6, 85–92. [Google Scholar] [CrossRef]
- Simon, M.A.; Aschliman, M.A.; Thomas, N.; Mankin, H.J. Limb-salvage treatment versus amputation for osteosarcoma of the distal end of the femur. J. Bone Joint Surg. Am. 1986, 68, 1331–1337. [Google Scholar]
- Rougraff, B.T.; Simon, M.A.; Kneisl, J.S.; Greenberg, D.B.; Mankin, H.J. Limb salvage compared with amputation for osteosarcoma of the distal end of the femur. A long-term oncological, functional, and quality-of-life study. J. Bone Joint Surg. Am. 1994, 76, 649–656. [Google Scholar]
- Grimer, R.J.; Taminiau, A.M.; Cannon, S.R. Surgical outcomes in osteosarcoma. J. Bone Joint Surg. Br. 2002, 84, 395–400. [Google Scholar] [CrossRef]
- Nagarajan, R.; Neglia, J.P.; Clohisy, D.R.; Robison, L.L. Limb salvage and amputation in survivors of pediatric lower-extremity bone tumors: What are the long-term implications? J. Clin. Oncol. 2002, 20, 4493–4501. [Google Scholar] [CrossRef]
- Smith, J.; Thompson, J.M. Phantom limb pain and chemotherapy in pediatric amputees. Mayo Clin. Proc. 1995, 70, 357–364. [Google Scholar] [CrossRef]
- Krane, E.J.; Heller, L.B. The prevalence of phantom sensation and pain in pediatric amputees. J. Pain Symptom Manage. 1995, 10, 21–29. [Google Scholar] [CrossRef]
- Bielack, S.S.; Kempf-Bielack, B.; Delling, G.; Exner, G.U.; Flege, S.; Helmke, K.; Kotz, R.; Salzer-Kuntschik, M.; Werner, M.; Winkelmann, W.; et al. Prognostic factors in high-grade osteosarcoma of the extremities or trunk: An analysis of 1,702 patients treated on neoadjuvant cooperative osteosarcoma study group protocols. J. Clin. Oncol. 2002, 20, 776–790. [Google Scholar] [CrossRef]
- Arndt, C.A.; Rose, P.S.; Folpe, A.L.; Laack, N.N. Common musculoskeletal tumors of childhood and adolescence. Mayo Clin. Proc. 2012, 87, 475–487. [Google Scholar] [CrossRef]
- Bielack, S.; Jurgens, H.; Jundt, G.; Kevric, M.; Kuhne, T.; Reichardt, P.; Zoubek, A.; Werner, M.; Winkelmann, W.; Kotz, R. Osteosarcoma: The coss experience. Cancer Treat. Res. 2009, 152, 289–308. [Google Scholar] [CrossRef]
- Gosheger, G.; Gebert, C.; Ahrens, H.; Streitbuerger, A.; Winkelmann, W.; Hardes, J. Endoprosthetic reconstruction in 250 patients with sarcoma. Clin. Orthop. Relat. Res. 2006, 450, 164–171. [Google Scholar] [CrossRef]
- Wittig, J.C.; Bickels, J.; Priebat, D.; Jelinek, J.; Kellar-Graney, K.; Shmookler, B.; Malawer, M.M. Osteosarcoma: A multidisciplinary approach to diagnosis and treatment. Am. Fam. Physician 2002, 65, 1123–1132. [Google Scholar]
- Ferrari, S.; Smeland, S.; Mercuri, M.; Bertoni, F.; Longhi, A.; Ruggieri, P.; Alvegard, T.A.; Picci, P.; Capanna, R.; Bernini, G.; et al. Neoadjuvant chemotherapy with high-dose ifosfamide, high-dose methotrexate, cisplatin, and doxorubicin for patients with localized osteosarcoma of the extremity: A joint study by the italian and scandinavian sarcoma groups. J. Clin. Oncol. 2005, 23, 8845–8852. [Google Scholar] [CrossRef]
- Gherlinzoni, F.; Picci, P.; Bacci, G.; Campanacci, D. Limb sparing versus amputation in osteosarcoma. Correlation between local control, surgical margins and tumor necrosis: Istituto rizzoli experience. Ann. Oncol. 1992, 3, S23–S27. [Google Scholar] [CrossRef]
- Ceelen, W.P.; Morris, S.; Paraskeva, P.; Pattyn, P. Surgical trauma, minimal residual disease and locoregional cancer recurrence. Cancer Treat. Res. 2007, 134, 51–69. [Google Scholar]
- Kotz, R.I.; Windhager, R.; Dominkus, M.; Robioneck, B.; Muller-Daniels, H. A self-extending paediatric leg implant. Nature 2000, 406, 143–144. [Google Scholar] [CrossRef]
- Maronna, U. The blauth total knee endoprosthesis. Eighteen years’ experience in practice. Int. Orthop. 1993, 17, 17–19. [Google Scholar]
- Wunder, J.S.; Leitch, K.; Griffin, A.M.; Davis, A.M.; Bell, R.S. Comparison of two methods of reconstruction for primary malignant tumors at the knee: A sequential cohort study. J. Surg. Oncol. 2001, 77, 89–99. [Google Scholar] [CrossRef]
- Jeys, L.M.; Grimer, R.J.; Carter, S.R.; Tillman, R.M. Periprosthetic infection in patients treated for an orthopaedic oncological condition. J. Bone Joint Surg. Am. 2005, 87, 842–849. [Google Scholar] [CrossRef]
- Gaur, A.H.; Liu, T.; Knapp, K.M.; Daw, N.C.; Rao, B.N.; Neel, M.D.; Rodriguez-Galindo, C.; Brand, D.; Adderson, E.E. Infections in children and young adults with bone malignancies undergoing limb-sparing surgery. Cancer 2005, 104, 602–610. [Google Scholar] [CrossRef]
- Grimer, R.J.; Belthur, M.; Chandrasekar, C.; Carter, S.R.; Tillman, R.M. Two-stage revision for infected endoprostheses used in tumor surgery. Clin. Orthop. Relat. Res. 2002, 395, 193–203. [Google Scholar] [CrossRef]
- Ceruso, M.; Falcone, C.; Innocenti, M.; Delcroix, L.; Capanna, R.; Manfrini, M. Skeletal reconstruction with a free vascularized fibula graft associated to bone allograft after resection of malignant bone tumor of limbs. Handchir. Mikrochir. Plast. Chir. 2001, 33, 277–282. [Google Scholar] [CrossRef]
- Manfrini, M. The role of vascularized fibula in skeletal reconstruction. Chir. Organi Mov. 2003, 88, 137–142. [Google Scholar]
- Uyttendaele, D.; de Schryver, A.; Claessens, H.; Roels, H.; Berkvens, P.; Mondelaers, W. Limb conservation in primary bone tumours by resection, extracorporeal irradiation and re-implantation. J. Bone Joint Surg. Br. 1988, 70, 348–353. [Google Scholar]
- Morello, E.; Vasconi, E.; Martano, M.; Peirone, B.; Buracco, P. Pasteurized tumoral autograft and adjuvant chemotherapy for the treatment of canine distal radial osteosarcoma: 13 cases. Vet. Surg. 2003, 32, 539–544. [Google Scholar] [CrossRef]
- Mankin, H.J.; Gebhardt, M.C.; Jennings, L.C.; Springfield, D.S.; Tomford, W.W. Long-term results of allograft replacement in the management of bone tumors. Clin. Orthop. Relat. Res. 1996, 324, 86–97. [Google Scholar] [CrossRef]
- Ortiz-Cruz, E.; Gebhardt, M.C.; Jennings, L.C.; Springfield, D.S.; Mankin, H.J. The results of transplantation of intercalary allografts after resection of tumors. A long-term follow-up study. J. Bone Joint Surg. Am. 1997, 79, 97–106. [Google Scholar]
- Berrey, B.H., Jr.; Lord, C.F.; Gebhardt, M.C.; Mankin, H.J. Fractures of allografts. Frequency, treatment, and end-results. J. Bone Joint Surg. Am. 1990, 72, 825–833. [Google Scholar]
- Hornicek, F.J.; Gebhardt, M.C.; Tomford, W.W.; Sorger, J.I.; Zavatta, M.; Menzner, J.P.; Mankin, H.J. Factors affecting nonunion of the allograft-host junction. Clin. Orthop. Relat. Res. 2001, 1, 87–98. [Google Scholar]
- Mankin, H.J.; Springfield, D.S.; Gebhardt, M.C.; Tomford, W.W. Current status of allografting for bone tumors. Orthopedics 1992, 15, 1147–1154. [Google Scholar]
- Kotz, R.; Salzer, M. Rotation-plasty for childhood osteosarcoma of the distal part of the femur. J. Bone Joint Surg. Am. 1982, 64, 959–969. [Google Scholar]
- Zeltzer, L.; Kellerman, J.; Ellenberg, L.; Dash, J.; Rigler, D. Psychologic effects of illness in adolescence. II. Impact of illness in adolescents—Crucial issues and coping styles. J. Pediatr. 1980, 97, 132–138. [Google Scholar] [CrossRef]
- Picci, P.; Sangiorgi, L.; Bahamonde, L.; Aluigi, P.; Bibiloni, J.; Zavatta, M.; Mercuri, M.; Briccoli, A.; Campanacci, M. Risk factors for local recurrences after limb-salvage surgery for high-grade osteosarcoma of the extremities. Ann. Oncol. 1997, 8, 899–903. [Google Scholar] [CrossRef]
- Bacci, G.; Longhi, A.; Fagioli, F.; Briccoli, A.; Versari, M.; Picci, P. Adjuvant and neoadjuvant chemotherapy for osteosarcoma of the extremities: 27 year experience at rizzoli institute, Italy. Eur. J. Cancer 2005, 41, 2836–2845. [Google Scholar] [CrossRef]
- Meyers, P.A.; Heller, G.; Healey, J.H.; Huvos, A.; Applewhite, A.; Sun, M.; LaQuaglia, M. Osteogenic sarcoma with clinically detectable metastasis at initial presentation. J. Clin. Oncol. 1993, 11, 449–453. [Google Scholar]
- Harris, M.B.; Gieser, P.; Goorin, A.M.; Ayala, A.; Shochat, S.J.; Ferguson, W.S.; Holbrook, T.; Link, M.P. Treatment of metastatic osteosarcoma at diagnosis: A pediatric oncology group study. J. Clin. Oncol. 1998, 16, 3641–3648. [Google Scholar]
- Goorin, A.M.; Harris, M.B.; Bernstein, M.; Ferguson, W.; Devidas, M.; Siegal, G.P.; Gebhardt, M.C.; Schwartz, C.L.; Link, M.; Grier, H.E. Phase II/III trial of etoposide and high-dose ifosfamide in newly diagnosed metastatic osteosarcoma: A pediatric oncology group trial. J. Clin. Oncol. 2002, 20, 426–433. [Google Scholar] [CrossRef]
- Ferguson, W.S.; Harris, M.B.; Goorin, A.M.; Gebhardt, M.C.; Link, M.P.; Shochat, S.J.; Siegal, G.P.; Devidas, M.; Grier, H.E. Presurgical window of carboplatin and surgery and multidrug chemotherapy for the treatment of newly diagnosed metastatic or unresectable osteosarcoma: Pediatric oncology group trial. J. Pediatr. Hematol. Oncol. 2001, 23, 340–348. [Google Scholar]
- Bacci, G.; Mercuri, M.; Briccoli, A.; Ferrari, S.; Bertoni, F.; Donati, D.; Monti, C.; Zanoni, A.; Forni, C.; Manfrini, M. Osteogenic sarcoma of the extremity with detectable lung metastases at presentation. Results of treatment of 23 patients with chemotherapy followed by simultaneous resection of primary and metastatic lesions. Cancer 1997, 79, 245–254. [Google Scholar] [CrossRef]
- Briccoli, A.; Rocca, M.; Salone, M.; Bacci, G.; Ferrari, S.; Balladelli, A.; Mercuri, M. Resection of recurrent pulmonary metastases in patients with osteosarcoma. Cancer 2005, 104, 1721–1725. [Google Scholar] [CrossRef]
- Marcove, R.C.; Lewis, M.M. Prolonged survival in osteogenic sarcoma with multiple pulmonary metastases. A case report and review of the literature. J. Bone Joint Surg. Am. 1973, 55, 1516–1520. [Google Scholar]
- Harting, M.T.; Blakely, M.L. Management of osteosarcoma pulmonary metastases. Semin. Pediatr. Surg. 2006, 15, 25–29. [Google Scholar] [CrossRef]
- Ward, W.G.; Mikaelian, K.; Dorey, F.; Mirra, J.M.; Sassoon, A.; Holmes, E.C.; Eilber, F.R.; Eckardt, J.J. Pulmonary metastases of stage iib extremity osteosarcoma and subsequent pulmonary metastases. J. Clin. Oncol. 1994, 12, 1849–1858. [Google Scholar]
- Glasser, D.B.; Lane, J.M.; Huvos, A.G.; Marcove, R.C.; Rosen, G. Survival, prognosis, and therapeutic response in osteogenic sarcoma. The memorial hospital experience. Cancer 1992, 69, 698–708. [Google Scholar] [CrossRef]
- Picci, P.; Bacci, G.; Campanacci, M.; Gasparini, M.; Pilotti, S.; Cerasoli, S.; Bertoni, F.; Guerra, A.; Capanna, R.; Albisinni, U.; et al. Histologic evaluation of necrosis in osteosarcoma induced by chemotherapy. Regional mapping of viable and nonviable tumor. Cancer 1985, 56, 1515–1521. [Google Scholar] [CrossRef]
- Bielack, S.; Carrle, D.; Casali, P. Osteosarcoma: Esmo clinical recommendations for diagnosis, treatment and follow-up. Ann. Oncol. 2009, 20, iv137–iv139. [Google Scholar] [CrossRef]
- Chou, A.J.; Gorlick, R. Chemotherapy resistance in osteosarcoma: Current challenges and future directions. Expert Rev. Anticancer Ther. 2006, 6, 1075–1085. [Google Scholar] [CrossRef]
- Campanacci, M.; Bacci, G.; Bertoni, F.; Picci, P.; Minutillo, A.; Franceschi, C. The treatment of osteosarcoma of the extremities: Twenty year’s experience at the istituto ortopedico rizzoli. Cancer 1981, 48, 1569–1581. [Google Scholar] [CrossRef]
- Enneking, W.F. Advances and treatment of primary bone tumors. J. Fla. Med. Assoc. 1979, 66, 28–30. [Google Scholar]
- Rosenburg, S.A.; Chabner, B.A.; Young, R.C.; Seipp, C.A.; Levine, A.S.; Costa, J.; Hanson, T.A.; Head, G.C.; Simon, R.M. Treatment of osteogenic sarcoma. I. Effect of adjuvant high-dose methotrexate after amputation. Cancer Treat. Rep. 1979, 63, 739–751. [Google Scholar]
- Rosen, G.; Murphy, M.L.; Huvos, A.G.; Gutierrez, M.; Marcove, R.C. Chemotherapy, en bloc resection, and prosthetic bone replacement in the treatment of osteogenic sarcoma. Cancer 1976, 37, 1–11. [Google Scholar] [CrossRef]
- De Kraker, J.; Voute, P.A. Experience with ifosfamide in paediatric tumours. Cancer Chemother. Pharmacol. 1989, 24, S28–S29. [Google Scholar]
- Bacci, G.; Ferrari, S.; Longhi, A.; Picci, P.; Mercuri, M.; Alvegard, T.A.; Saeter, G.; Donati, D.; Manfrini, M.; Lari, S.; et al. High dose ifosfamide in combination with high dose methotrexate, adriamycin and cisplatin in the neoadjuvant treatment of extremity osteosarcoma: Preliminary results of an italian sarcoma group/scandinavian sarcoma group pilot study. J. Chemother. 2002, 14, 198–206. [Google Scholar]
- Anninga, J.K.; Gelderblom, H.; Fiocco, M.; Kroep, J.R.; Taminiau, A.H.; Hogendoorn, P.C.; Egeler, R.M. Chemotherapeutic adjuvant treatment for osteosarcoma: Where do we stand? Eur. J. Cancer 2011, 47, 2431–2445. [Google Scholar] [CrossRef]
- Meyers, P.A.; Heller, G.; Healey, J.; Huvos, A.; Lane, J.; Marcove, R.; Applewhite, A.; Vlamis, V.; Rosen, G. Chemotherapy for nonmetastatic osteogenic sarcoma: The memorial sloan-kettering experience. J. Clin. Oncol. 1992, 10, 5–15. [Google Scholar]
- Avella, M.; Bacci, G.; McDonald, D.J.; di Scioscio, M.; Picci, P.; Campanacci, M. Adjuvant chemotherapy with six drugs (adriamycin, methotrexate, cisplatinum, bleomycin, cyclophosphamide and dactinomycin) for non-metastatic high grade osteosarcoma of the extremities. Results of 32 patients and comparison to 127 patients concomitantly treated with the same drugs in a neoadjuvant form. Chemioterapia 1988, 7, 133–137. [Google Scholar]
- Rollins, K.D.; Lindley, C. Pemetrexed: A multitargeted antifolate. Clin. Ther. 2005, 27, 1343–1382. [Google Scholar] [CrossRef]
- Vogelzang, N.J.; Rusthoven, J.J.; Symanowski, J.; Denham, C.; Kaukel, E.; Ruffie, P.; Gatzemeier, U.; Boyer, M.; Emri, S.; Manegold, C. Phase III study of pemetrexed in combination with cisplatin versus cisplatin alone in patients with malignant pleural mesothelioma. J. Clin. Oncol. 2003, 21, 2636–2644. [Google Scholar] [CrossRef]
- Scagliotti, G.V.; Parikh, P.; von Pawel, J.; Biesma, B.; Vansteenkiste, J.; Manegold, C.; Serwatowski, P.; Gatzemeier, U.; Digumarti, R.; Zukin, M. Phase III study comparing cisplatin plus gemcitabine with cisplatin plus pemetrexed in chemotherapy-naive patients with advanced-stage non-small-cell lung cancer. J. Clin. Oncol. 2008, 26, 3543–3551. [Google Scholar] [CrossRef]
- Ciuleanu, T.; Brodowicz, T.; Zielinski, C.; Kim, J.H.; Krzakowski, M.; Laack, E.; Wu, Y.-L.; Bover, I.; Begbie, S.; Tzekova, V. Maintenance pemetrexed plus best supportive care versus placebo plus best supportive care for non-small-cell lung cancer: A randomised, double-blind, phase 3 study. Lancet 2009, 374, 1432–1440. [Google Scholar] [CrossRef]
- Bodmer, N.; Walters, D.; Fuchs, B. Pemetrexed, a multitargeted antifolate drug, demonstrates lower efficacy in comparison to methotrexate against osteosarcoma cell lines. Pediatr. Blood Cancer 2008, 50, 905–908. [Google Scholar] [CrossRef]
- Duffaud, F.; Egerer, G.; Ferrari, S.; Rassam, H.; Boecker, U.; Bui-Nguyen, B. A phase II trial of second-line pemetrexed in adults with advanced/metastatic osteosarcoma. Eur. J. Cancer 2012, 48, 564–570. [Google Scholar]
- Warwick, A.B.; Malempati, S.; Krailo, M.; Melemed, A.; Gorlick, R.; Ames, M.M.; Safgren, S.L.; Adamson, P.C.; Blaney, S.M. Phase 2 trial of pemetrexed in children and adolescents with refractory solid tumors: A children's oncology group study. Pediatr. Blood Cancer 2012, 60, 237–241. [Google Scholar]
- Meyers, P.A.; Schwartz, C.L.; Krailo, M.D.; Healey, J.H.; Bernstein, M.L.; Betcher, D.; Ferguson, W.S.; Gebhardt, M.C.; Goorin, A.M.; Harris, M.; et al. Osteosarcoma: The addition of muramyl tripeptide to chemotherapy improves overall survival—A report from the children's oncology group. J. Clin. Oncol. 2008, 26, 633–638. [Google Scholar] [CrossRef]
- Ando, K.; Mori, K.; Corradini, N.; Redini, F.; Heymann, D. Mifamurtide for the treatment of nonmetastatic osteosarcoma. Expert Opin. Pharmacother. 2011, 12, 285–292. [Google Scholar] [CrossRef] [Green Version]
- Hudson, M.; Jaffe, M.R.; Jaffe, N.; Ayala, A.; Raymond, A.K.; Carrasco, H.; Wallace, S.; Murray, J.; Robertson, R. Pediatric osteosarcoma: Therapeutic strategies, results, and prognostic factors derived from a 10-year experience. J. Clin. Oncol. 1990, 8, 1988–1997. [Google Scholar]
- Rosen, G.; Holmes, E.C.; Forscher, C.A.; Lowenbraun, S.; Eckardt, J.J.; Eilber, F.R. The role of thoracic surgery in the management of metastatic osteogenic sarcoma. Chest Surg. Clin. N. Am. 1994, 4, 75–83. [Google Scholar]
- Mori, K.; Ando, K.; Heymann, D. Liposomal muramyl tripeptide phosphatidyl ethanolamine: A safe and effective agent against osteosarcoma pulmonary metastases. Expert Rev. Anticancer Ther. 2008, 8, 151–159. [Google Scholar] [CrossRef]
- Machak, G.N.; Tkachev, S.I.; Solovyev, Y.N.; Sinyukov, P.A.; Ivanov, S.M.; Kochergina, N.V.; Ryjkov, A.D.; Tepliakov, V.V.; Bokhian, B.Y.; Glebovskaya, V.V. Neoadjuvant chemotherapy and local radiotherapy for high-grade osteosarcoma of the extremities. Mayo Clin. Proc. 2003, 78, 147–155. [Google Scholar] [CrossRef]
- Delaney, G.; Jacob, S.; Featherstone, C.; Barton, M. The role of radiotherapy in cancer treatment: Estimating optimal utilization from a review of evidence-based clinical guidelines. Cancer 2005, 104, 1129–1137. [Google Scholar] [CrossRef]
- Schwarz, R.; Bruland, O.; Cassoni, A.; Schomberg, P.; Bielack, S. The role of radiotherapy in oseosarcoma. Cancer Treat. Res. 2009, 152, 147–164. [Google Scholar] [CrossRef]
- DeLaney, T.F.; Park, L.; Goldberg, S.I.; Hug, E.B.; Liebsch, N.J.; Munzenrider, J.E.; Suit, H.D. Radiotherapy for local control of osteosarcoma. Int. J. Radiat. Oncol. Biol. Phys. 2005, 61, 492–498. [Google Scholar] [CrossRef]
- Ozaki, T.; Flege, S.; Kevric, M.; Lindner, N.; Maas, R.; Delling, G.; Schwarz, R.; von Hochstetter, A.R.; Salzer-Kuntschik, M.; Berdel, W.E.; et al. Osteosarcoma of the pelvis: Experience of the cooperative osteosarcoma study group. J. Clin. Oncol. 2003, 21, 334–341. [Google Scholar] [CrossRef]
- Ozaki, T.; Flege, S.; Liljenqvist, U.; Hillmann, A.; Delling, G.; Salzer-Kuntschik, M.; Jurgens, H.; Kotz, R.; Winkelmann, W.; Bielack, S.S. Osteosarcoma of the spine: Experience of the cooperative osteosarcoma study group. Cancer 2002, 94, 1069–1077. [Google Scholar] [CrossRef]
- Lee, E.S. Treatment of bone sarcoma. Proc. R. Soc. Med. 1971, 64, 1179–1180. [Google Scholar]
- Phillips, T.L.; Sheline, G.E. Radiatio herapy of malignant bone tumors. Radiology 1969, 92, 1537–1545. [Google Scholar]
- Ciernik, I.F.; Niemierko, A.; Harmon, D.C.; Kobayashi, W.; Chen, Y.L.; Yock, T.I.; Ebb, D.H.; Choy, E.; Raskin, K.A.; Liebsch, N. Proton-based radiotherapy for unresectable or incompletely resected osteosarcoma. Cancer 2011, 117, 4522–4530. [Google Scholar] [CrossRef]
- Matsunobu, A.; Imai, R.; Kamada, T.; Imaizumi, T.; Tsuji, H.; Tsujii, H.; Shioyama, Y.; Honda, H.; Tatezaki, S.I. Impact of carbon ion radiotherapy for unresectable osteosarcoma of the trunk. Cancer 2012, 118, 4555–4563. [Google Scholar]
- Blakely, E.A.; Kronenberg, A. Heavy-ion radiobiology: New approaches to delineate mechanisms underlying enhanced biological effectiveness. Radiat. Res. 1998, 150, 126–145. [Google Scholar] [CrossRef]
- Kamada, T.; Tsujii, H.; Tsuji, H.; Yanagi, T.; Mizoe, J.-E.; Miyamoto, T.; Kato, H.; Yamada, S.; Morita, S.; Yoshikawa, K. Efficacy and safety of carbon ion radiotherapy in bone and soft tissue sarcomas. J. Clin. Oncol. 2002, 20, 4466–4471. [Google Scholar] [CrossRef]
- Spira, E.; Lubin, E. Extracorporeal irradiation of bone tumors. A preliminary report. Isr. J. Med. Sci. 1968, 4, 1015–1019. [Google Scholar]
- Araki, N.; Myoui, A.; Kuratsu, S.; Hashimoto, N.; Inoue, T.; Kudawara, I.; Ueda, T.; Yoshikawa, H.; Masaki, N.; Uchida, A. Intraoperative extracorporeal autogenous irradiated bone grafts in tumor surgery. Clin. Orthop. Relat. Res. 1999, 368, 196–206. [Google Scholar]
- Hong, A.; Stevens, G.; Stalley, P.; Pendlebury, S.; Ahern, V.; Ralston, A.; Estoesta, E.; Barrett, I. Extracorporeal irradiation for malignant bone tumors. Int. J. Radiat. Oncol. Biol. Phys. 2001, 50, 441–447. [Google Scholar] [CrossRef]
- Yamamoto, T.; Akisue, T.; Marui, T.; Nagira, K.; Kurosaka, M. Osteosarcoma of the distal radius treated by intraoperative extracorporeal irradiation. J. Hand Surg. Am. 2002, 27, 160–164. [Google Scholar] [CrossRef]
- Weichselbaum, R.R.; Cassady, J.R.; Jaffe, N.; Filler, R.M. Preliminary results of aggressive multimodality therapy for metastatic osteosarcoma. Cancer 1977, 40, 78–83. [Google Scholar] [CrossRef]
- Giritsky, A.S.; Etcubanas, E.; Mark, J.B. Pulmonary resection in children with metastatic osteogenic sarcoma: Improved survival with surgery, chemotherapy, and irradiation. J. Thorac. Cardiovasc. Surg. 1978, 75, 354–362. [Google Scholar]
- Rab, G.T.; Ivins, J.C.; Childs, D.S., Jr.; Cupps, R.E.; Pritchard, D.J. Elective whole lung irradiation in the treatment of osteogenic sarcoma. Cancer 1976, 38, 939–942. [Google Scholar] [CrossRef]
- Breur, K.; Cohen, P.; Schweisguth, O.; Hart, A.M. Irradiation of the lungs as an adjuvant therapy in the treatment of osteosarcoma of the limbs. An EORTC randomized study. Eur. J. Cancer 1978, 14, 461–471. [Google Scholar]
- Gilchrist, G.S.; Pritchard, D.J.; Dahlin, D.C.; Ivins, J.C.; Taylor, W.F.; Edmonson, J.H. Management of osteogenic sarcoma: A perspective based on the mayo clinic experience. Natl. Cancer Inst. Monogr. 1981, 56, 193–199. [Google Scholar]
- Whelan, J.S.; Burcombe, R.J.; Janinis, J.; Baldelli, A.M.; Cassoni, A.M. A systematic review of the role of pulmonary irradiation in the management of primary bone tumours. Ann. Oncol. 2002, 13, 23–30. [Google Scholar]
- French Bone Tumor Study Group. Age and dose of chemotherapy as major prognostic factors in a trial of adjuvant therapy of osteosarcoma combining two alternating drug combinations and early prophylactic lung irradiation. Cancer 1988, 61, 1304–1311. [CrossRef]
- Anderson, P.M.; Wiseman, G.A.; Dispenzieri, A.; Arndt, C.A.; Hartmann, L.C.; Smithson, W.A.; Mullan, B.P.; Bruland, O.S. High-dose samarium-153 ethylene diamine tetramethylene phosphonate: Low toxicity of skeletal irradiation in patients with osteosarcoma and bone metastases. J. Clin. Oncol. 2002, 20, 189–196. [Google Scholar] [CrossRef]
- Bruland, O.S.; Skretting, A.; Solheim, O.P.; Aas, M. Targeted radiotherapy of osteosarcoma using 153 sm-edtmp. A new promising approach. Acta Oncol. 1996, 35, 381–384. [Google Scholar] [CrossRef]
- Anderson, P.; Nunez, R. Samarium lexidronam (153sm-edtmp): Skeletal radiation for osteoblastic bone metastases and osteosarcoma. Expert Rev. Anticancer Ther. 2007, 7, 1517–1527. [Google Scholar] [CrossRef]
- Franzius, C.; Bielack, S.; Flege, S.; Eckardt, J.; Sciuk, J.; Jurgens, H.; Schober, O. High.-activity samarium-153-edtmp therapy followed by autologous peripheral blood stem cell support in unresectable osteosarcoma. Nuklearmedizin 2001, 40, 215–220. [Google Scholar]
- Whelan, J.; Patterson, D.; Perisoglou, M.; Bielack, S.; Marina, N.; Smeland, S.; Bernstein, M. The role of interferons in the treatment of osteosarcoma. Pediatr. Blood Cancer 2010, 54, 350–354. [Google Scholar]
- Einhorn, S.; Strander, H. Is interferon tissue specific?—Effect of human leukocyte and fibroblast interferons on the growth of lymphoblastoid and osteosarcoma cell lines. J. Gen. Virol. 1977, 35, 573–577. [Google Scholar] [CrossRef]
- Strander, H.; Einhorn, S. Effect of human leukocyte interferon on the growth of human osteosarcoma cells in tissue culture. Int. J. Cancer 1977, 19, 468–473. [Google Scholar] [CrossRef]
- Brosjo, O.; Bauer, H.C.; Brostrom, L.A.; Nilsson, O.S.; Reinholt, F.P.; Tribukait, B. Growth inhibition of human osteosarcomas in nude mice by human interferon-alpha: Significance of dose and tumor differentiation. Cancer Res. 1987, 47, 258–262. [Google Scholar]
- Mori, K.; Rédini, F.; Gouin, F.; Cherrier, B.; Heymann, D. Osteosarcoma: Current status of immunotherapy and future trends (review). Oncol. Rep. 2006, 15, 693–700. [Google Scholar]
- Muller, C.R.; Smeland, S.; Bauer, H.C.; Saeter, G.; Strander, H. Interferon-alpha as the only adjuvant treatment in high-grade osteosarcoma: Long term results of the karolinska hospital series. Acta Oncol. 2005, 44, 475–480. [Google Scholar] [CrossRef]
- Strander, H.; Bauer, H.C.; Brosjo, O.; Fernberg, J.O.; Kreicbergs, A.; Nilsonne, U.; Silfversward, C.; Signomklao, T.; Soderlund, V. Long-term adjuvant interferon treatment of human osteosarcoma. A pilot study. Acta Oncol. 1995, 34, 877–880. [Google Scholar] [CrossRef]
- Winkler, K.; Beron, G.; Kotz, R.; Salzer-Kuntschik, M.; Beck, J.; Beck, W.; Brandeis, W.; Ebell, W.; Erttmann, R.; Göbel, U. Neoadjuvant chemotherapy for osteogenic sarcoma: Results of a cooperative german/austrian study. J. Clin. Oncol. 1984, 2, 617–624. [Google Scholar]
- Anderson, P.M.; Markovic, S.N.; Sloan, J.A.; Clawson, M.L.; Wylam, M.; Arndt, C.A.; Smithson, W.A.; Burch, P.; Gornet, M.; Rahman, E. Aerosol granulocyte macrophage-colony stimulating factor: A low toxicity, lung-specific biological therapy in patients with lung metastases. Clin. Cancer Res. 1999, 5, 2316–2323. [Google Scholar]
- Arndt, C.A.; Koshkina, N.V.; Inwards, C.Y.; Hawkins, D.S.; Krailo, M.D.; Villaluna, D.; Anderson, P.M.; Goorin, A.M.; Blakely, M.L.; Bernstein, M.; et al. Inhaled granulocyte-macrophage colony stimulating factor for first pulmonary recurrence of osteosarcoma: Effects on disease-free survival and immunomodulation. A report from the children's oncology group. Clin. Cancer Res. 2010, 16, 4024–4030. [Google Scholar] [CrossRef]
- Yeatman, T.J. A renaissance for src. Nat. Rev. Cancer 2004, 4, 470–480. [Google Scholar] [CrossRef]
- Shor, A.C.; Keschman, E.A.; Lee, F.Y.; Muro-Cacho, C.; Letson, G.D.; Trent, J.C.; Pledger, W.J.; Jove, R. Dasatinib inhibits migration and invasion in diverse human sarcoma cell lines and induces apoptosis in bone sarcoma cells dependent on src kinase for survival. Cancer Res. 2007, 67, 2800–2808. [Google Scholar] [CrossRef]
- Manetti, F.; Santucci, A.; Locatelli, G.A.; Maga, G.; Spreafico, A.; Serchi, T.; Orlandini, M.; Bernardini, G.; Caradonna, N.P.; Spallarossa, A.; et al. Identification of a novel pyrazolo [3,4-d] pyrimidine able to inhibit cell proliferation of a human osteogenic sarcoma in vitro and in a xenograft model in mice. J. Med. Chem. 2007, 50, 5579–5588. [Google Scholar] [CrossRef]
- Hingorani, P.; Zhang, W.; Gorlick, R.; Kolb, E.A. Inhibition of src phosphorylation alters metastatic potential of osteosarcoma in vitro but not in vivo. Clin. Cancer Res. 2009, 15, 3416–3422. [Google Scholar] [CrossRef]
- Vilella-Bach, M.; Nuzzi, P.; Fang, Y.; Chen, J. The fkbp12-rapamycin-binding domain is required for fkbp12-rapamycin-associated protein kinase activity and g1 progression. J. Biol. Chem. 1999, 274, 4266–4272. [Google Scholar] [CrossRef]
- Ory, B.; Moriceau, G.; Redini, F.; Heymann, D. Mtor inhibitors (rapamycin and its derivatives) and nitrogen containing bisphosphonates: Bi-functional compounds for the treatment of bone tumours. Curr. Med. Chem. 2007, 14, 1381–1387. [Google Scholar] [CrossRef]
- Wan, X.; Mendoza, A.; Khanna, C.; Helman, L.J. Rapamycin inhibits ezrin-mediated metastatic behavior in a murine model of osteosarcoma. Cancer Res. 2005, 65, 2406–2411. [Google Scholar]
- Houghton, P.J.; Morton, C.L.; Kolb, E.A.; Gorlick, R.; Lock, R.; Carol, H.; Reynolds, C.P.; Maris, J.M.; Keir, S.T.; Billups, C.A.; et al. Initial testing (stage 1) of the mtor inhibitor rapamycin by the pediatric preclinical testing program. Pediatr. Blood Cancer 2008, 50, 799–805. [Google Scholar]
- Chawla, S.P.; Staddon, A.P.; Baker, L.H.; Schuetze, S.M.; Tolcher, A.W.; D'Amato, G.Z.; Blay, J.Y.; Mita, M.M.; Sankhala, K.K.; Berk, L.; et al. Phase II study of the mammalian target of rapamycin inhibitor ridaforolimus in patients with advanced bone and soft tissue sarcomas. J. Clin. Oncol. 2012, 30, 78–84. [Google Scholar]
- McMahon, A.P.; Ingham, P.W.; Tabin, C.J. 1 Developmental roles and clinical significance of hedgehog signaling. Curr. Top. Dev. Biol. 2003, 53, 1–114. [Google Scholar]
- Lum, L.; Beachy, P.A. The hedgehog response network: Sensors, switches, and routers. Science 2004, 304, 1755–1759. [Google Scholar] [CrossRef]
- Rubin, L.L.; de Sauvage, F.J. Targeting the hedgehog pathway in cancer. Nat. Rev. Drug Discov. 2006, 5, 1026–1033. [Google Scholar]
- Lin, T.L.; Matsui, W. Hedgehog pathway as a drug target: Smoothened inhibitors in development. Oncotargets Ther. 2012, 5, 47. [Google Scholar]
- Xu, F.-G.; Ma, Q.-Y.; Wang, Z. Blockade of hedgehog signaling pathway as a therapeutic strategy for pancreatic cancer. Cancer Lett. 2009, 283, 119–124. [Google Scholar]
- Rudin, C.M.; Hann, C.L.; Laterra, J.; Yauch, R.L.; Callahan, C.A.; Fu, L.; Holcomb, T.; Stinson, J.; Gould, S.E.; Coleman, B. Treatment of medulloblastoma with hedgehog pathway inhibitor gdc-0449. N. Engl. J. Med. 2009, 361, 1173–1178. [Google Scholar] [CrossRef]
- Von Hoff, D.D.; LoRusso, P.M.; Rudin, C.M.; Reddy, J.C.; Yauch, R.L.; Tibes, R.; Weiss, G.J.; Borad, M.J.; Hann, C.L.; Brahmer, J.R. Inhibition of the hedgehog pathway in advanced basal-cell carcinoma. N. Engl. J. Med. 2009, 361, 1164–1172. [Google Scholar] [CrossRef]
- Tang, J.Y.; Mackay-Wiggan, J.M.; Aszterbaum, M.; Yauch, R.L.; Lindgren, J.; Chang, K.; Coppola, C.; Chanana, A.M.; Marji, J.; Bickers, D.R. Inhibiting the hedgehog pathway in patients with the basal-cell nevus syndrome. N. Engl. J. Med. 2012, 366, 2180–2188. [Google Scholar] [CrossRef]
- Paget, C.; Duret, H.; Ngiow, S.F.; Kansara, M.; Thomas, D.M.; Smyth, M.J. Studying the role of the immune system on the antitumor activity of a hedgehog inhibitor against murine osteosarcoma. Oncoimmunology 2012, 1, 1313–1322. [Google Scholar]
- Hassan, S.E.; Bekarev, M.; Kim, M.Y.; Lin, J.; Piperdi, S.; Gorlick, R.; Geller, D.S. Cell surface receptor expression patterns in osteosarcoma. Cancer 2012, 118, 740–749. [Google Scholar] [CrossRef]
- Abdeen, A.; Chou, A.J.; Healey, J.H.; Khanna, C.; Osborne, T.S.; Hewitt, S.M.; Kim, M.; Wang, D.; Moody, K.; Gorlick, R. Correlation between clinical outcome and growth factor pathway expression in osteogenic sarcoma. Cancer 2009, 115, 5243–5250. [Google Scholar] [CrossRef]
- Wang, Y.H.; Han, X.D.; Qiu, Y.; Xiong, J.; Yu, Y.; Wang, B.; Zhu, Z.Z.; Qian, B.P.; Chen, Y.X.; Wang, S.F.; et al. Increased expression of insulin-like growth factor-1 receptor is correlated with tumor metastasis and prognosis in patients with osteosarcoma. J. Surg. Oncol. 2012, 105, 235–243. [Google Scholar] [CrossRef]
- Bagatell, R.; Herzog, C.E.; Trippett, T.M.; Grippo, J.F.; Cirrincione-Dall, G.; Fox, E.; Macy, M.; Bish, J.; Whitcomb, P.; Aikin, A.; et al. Pharmacokinetically guided phase 1 trial of the igf-1 receptor antagonist rg1507 in children with recurrent or refractory solid tumors. Clin. Cancer Res. 2011, 17, 611–619. [Google Scholar] [CrossRef]
- Kolb, E.A.; Kamara, D.; Zhang, W.; Lin, J.; Hingorani, P.; Baker, L.; Houghton, P.; Gorlick, R. R1507, a fully human monoclonal antibody targeting igf-1r, is effective alone and in combination with rapamycin in inhibiting growth of osteosarcoma xenografts. Pediatr. Blood Cancer 2010, 55, 67–75. [Google Scholar]
- Kolb, E.A.; Gorlick, R.; Houghton, P.J.; Morton, C.L.; Lock, R.B.; Tajbakhsh, M.; Reynolds, C.P.; Maris, J.M.; Keir, S.T.; Billups, C.A.; et al. Initial testing of dasatinib by the pediatric preclinical testing program. Pediatr. Blood Cancer 2008, 50, 1198–1206. [Google Scholar] [CrossRef]
- Gorlick, R.; Huvos, A.G.; Heller, G.; Aledo, A.; Beardsley, G.P.; Healey, J.H.; Meyers, P.A. Expression of her2/erbb-2 correlates with survival in osteosarcoma. J. Clin. Oncol. 1999, 17, 2781–2788. [Google Scholar]
- Kilpatrick, S.E.; Geisinger, K.R.; King, T.S.; Sciarrotta, J.; Ward, W.G.; Gold, S.H.; Bos, G.D. Clinicopathologic analysis of her-2/neu immunoexpression among various histologic subtypes and grades of osteosarcoma. Mod. Pathol. 2001, 14, 1277–1283. [Google Scholar]
- Ebb, D.; Meyers, P.; Grier, H.; Bernstein, M.; Gorlick, R.; Lipshultz, S.E.; Krailo, M.; Devidas, M.; Barkauskas, D.A.; Siegal, G.P.; et al. Phase II trial of trastuzumab in combination with cytotoxic chemotherapy for treatment of metastatic osteosarcoma with human epidermal growth factor receptor 2 overexpression: A report from the children’s oncology group. J. Clin. Oncol. 2012, 30, 2545–2551. [Google Scholar]
- Grignani, G.; Palmerini, E.; Dileo, P.; Asaftei, S.D.; D'Ambrosio, L.; Pignochino, Y.; Mercuri, M.; Picci, P.; Fagioli, F.; Casali, P.G.; et al. A phase ii trial of sorafenib in relapsed and unresectable high-grade osteosarcoma after failure of standard multimodal therapy: An. italian sarcoma group study. Ann. Oncol. 2012, 23, 508–516. [Google Scholar] [CrossRef]
- Zhang, L.; Leeman, E.; Carnes, D.C.; Graves, D.T. Human osteoblasts synthesize and respond to platelet-derived growth factor. Am. J. Physiol. 1991, 261, C348–C354. [Google Scholar]
- Sulzbacher, I.; Traxler, M.; Mosberger, I.; Lang, S.; Chott, A. Platelet-derived growth factor-aa and -alpha receptor expression suggests an autocrine and/or paracrine loop in osteosarcoma. Mod. Pathol. 2000, 13, 632–637. [Google Scholar]
- Kubo, T.; Piperdi, S.; Rosenblum, J.; Antonescu, C.R.; Chen, W.; Kim, H.S.; Huvos, A.G.; Sowers, R.; Meyers, P.A.; Healey, J.H.; et al. Platelet-derived growth factor receptor as a prognostic marker and a therapeutic target for imatinib mesylate therapy in osteosarcoma. Cancer 2008, 112, 2119–2129. [Google Scholar] [CrossRef]
- Sulzbacher, I.; Birner, P.; Dominkus, M.; Pichlhofer, B.; Mazal, P.R. Expression of platelet-derived growth factor-alpha receptor in human osteosarcoma is not a predictor of outcome. Pathology 2010, 42, 664–668. [Google Scholar]
- McGary, E.C.; Weber, K.; Mills, L.; Doucet, M.; Lewis, V.; Lev, D.C.; Fidler, I.J.; Bar-Eli, M. Inhibition of platelet-derived growth factor-mediated proliferation of osteosarcoma cells by the novel tyrosine kinase inhibitor sti571. Clin. Cancer Res. 2002, 8, 3584–3591. [Google Scholar]
- Bond, M.; Bernstein, M.L.; Pappo, A.; Schultz, K.R.; Krailo, M.; Blaney, S.M.; Adamson, P.C. A phase II study of imatinib mesylate in children with refractory or relapsed solid tumors: A children’s oncology group study. Pediatr. Blood Cancer 2008, 50, 254–258. [Google Scholar] [CrossRef]
- Wu, D.; Wan, M. Methylene diphosphonate-conjugated adriamycin liposomes: Preparation, characteristics, and targeted therapy for osteosarcomas in vitro and in vivo. Biomed. Microdevices 2012, 14, 497–510. [Google Scholar] [CrossRef]
- Alberts, D.S.; Muggia, F.M.; Carmichael, J.; Winer, E.P.; Jahanzeb, M.; Venook, A.P.; Skubitz, K.M.; Rivera, E.; Sparano, J.A.; DiBella, N.J.; et al. Efficacy and safety of liposomal anthracyclines in phase I/II clinical trials. Semin. Oncol. 2004, 31, 53–90. [Google Scholar] [CrossRef]
- O’Day, K.; Gorlick, R. Novel therapeutic agents for osteosarcoma. Expert Rev. Anticancer Ther. 2009, 9, 511–523. [Google Scholar] [CrossRef]
- Ory, B.; Heymann, M.F.; Kamijo, A.; Gouin, F.; Heymann, D.; Redini, F. Zoledronic acid suppresses lung metastases and prolongs overall survival of osteosarcoma-bearing mice. Cancer 2005, 104, 2522–2529. [Google Scholar] [CrossRef]
- Lamoureux, F.; Trichet, V.; Chipoy, C.; Blanchard, F.; Gouin, F.; Redini, F. Recent advances in the management of osteosarcoma and forthcoming therapeutic strategies. Expert Rev. Anticancer Ther. 2007, 7, 169–181. [Google Scholar] [CrossRef]
- Heymann, D.; Ory, B.; Gouin, F.; Green, J.R.; Rédini, F. Bisphosphonates: New therapeutic agents for the treatment of bone tumors. Trends Mol. Med. 2004, 10, 337–343. [Google Scholar] [CrossRef]
- Cheng, Y.Y.; Huang, L.; Lee, K.M.; Li, K.; Kumta, S.M. Alendronate regulates cell invasion and mmp-2 secretion in human osteosarcoma cell lines. Pediatr. Blood Cancer 2004, 42, 410–415. [Google Scholar] [CrossRef]
- Dass, C.R.; Choong, P.F. Zoledronic acid inhibits osteosarcoma growth in an orthotopic model. Mol. Cancer Ther. 2007, 6, 3263–3270. [Google Scholar] [CrossRef]
- Moriceau, G.; Ory, B.; Mitrofan, L.; Riganti, C.; Blanchard, F.; Brion, R.; Charrier, C.; Battaglia, S.; Pilet, P.; Denis, M.G. Zoledronic acid potentiates mtor inhibition and abolishes the resistance of osteosarcoma cells to rad001 (everolimus): Pivotal role of the prenylation process. Cancer Res. 2010, 70, 10329–10339. [Google Scholar] [CrossRef] [Green Version]
- Labrinidis, A.; Hay, S.; Liapis, V.; Ponomarev, V.; Findlay, D.M.; Evdokiou, A. Zoledronic acid inhibits both the osteolytic and osteoblastic components of osteosarcoma lesions in a mouse model. Clin. Cancer Res. 2009, 15, 3451–3461. [Google Scholar] [CrossRef]
- Labrinidis, A.; Hay, S.; Liapis, V.; Findlay, D.M.; Evdokiou, A. Zoledronic acid protects against osteosarcoma-induced bone destruction but lacks efficacy against pulmonary metastases in a syngeneic rat model. Int. J. Cancer 2010, 127, 345–354. [Google Scholar]
- Theoleyre, S.; Wittrant, Y.; Tat, S.K.; Fortun, Y.; Redini, F.; Heymann, D. The molecular triad opg/rank/rankl: Involvement in the orchestration of pathophysiological bone remodeling. Cytokine Growth Factor Rev. 2004, 15, 457–475. [Google Scholar] [CrossRef]
- Grimaud, E.; Soubigou, L.; Couillaud, S.; Coipeau, P.; Moreau, A.; Passuti, N.; Gouin, F.; Redini, F.; Heymann, D. Receptor activator of nuclear factor kappab ligand (rankl)/osteoprotegerin (opg) ratio is increased in severe osteolysis. Am. J. Pathol. 2003, 163, 2021–2031. [Google Scholar] [CrossRef]
- Mori, K.; Le Goff, B.; Berreur, M.; Riet, A.; Moreau, A.; Blanchard, F.; Chevalier, C.; Guisle-Marsollier, I.; Leger, J.; Guicheux, J.; et al. Human osteosarcoma cells express functional receptor activator of nuclear factor-kappa B. J. Pathol. 2007, 211, 555–562. [Google Scholar] [CrossRef]
- Lee, J.A.; Jung, J.S.; Kim, D.H.; Lim, J.S.; Kim, M.S.; Kong, C.B.; Song, W.S.; Cho, W.H.; Jeon, D.G.; Lee, S.Y.; et al. Rankl expression is related to treatment outcome of patients with localized, high-grade osteosarcoma. Pediatr. Blood Cancer 2011, 56, 738–743. [Google Scholar] [CrossRef]
- Lamoureux, F.; Richard, P.; Wittrant, Y.; Battaglia, S.; Pilet, P.; Trichet, V.; Blanchard, F.; Gouin, F.; Pitard, B.; Heymann, D.; et al. Therapeutic relevance of osteoprotegerin gene therapy in osteosarcoma: Blockade of the vicious cycle between tumor cell proliferation and bone resorption. Cancer Res. 2007, 67, 7308–7318. [Google Scholar] [CrossRef]
- Beristain, A.G.; Narala, S.R.; di Grappa, M.A.; Khokha, R. Homotypic rank signaling differentially regulates proliferation, motility and cell survival in osteosarcoma and mammary epithelial cells. J. Cell. Sci. 2012, 125, 943–955. [Google Scholar] [CrossRef]
- Anderson, P.; Kopp, L.; Anderson, N.; Cornelius, K.; Herzog, C.; Hughes, D.; Huh, W. Novel bone cancer drugs: Investigational agents and control paradigms for primary bone sarcomas (ewing’s sarcoma and osteosarcoma). Expert Opin. Investig. Drugs 2008, 17, 1703–1715. [Google Scholar] [CrossRef]
- Gobin, B.; Baud’huin, M.; Isidor, B.; Heymann, D.; Heymann, M.F. Monoclonal antibodies targeting rankl in bone metastasis treatment. In Monoclonal Antibodies in Oncology; Uckum, F.M., Ed.; eBook Future Medicine Ltd., 2013; Chapter 5; pp. 42–53. [Google Scholar]
- Heymann, D. Anti-rankl therapy for bone tumours: Basic, pre-clinical and clinical evidences. J. Bone Oncol. 2012, 1, 2–11. [Google Scholar] [CrossRef] [Green Version]
- Branstetter, D.G.; Nelson, S.D.; Manivel, J.C.; Blay, J.Y.; Chawla, S.; Thomas, D.M.; Jun, S.; Jacobs, I. Denosumab induces tumor reduction and bone formation in patients with giant-cell tumor of bone. Clin. Cancer Res. 2012, 18, 4415–4424. [Google Scholar] [CrossRef]
- Ando, K.; Mori, K.; Verrecchia, F.; Marc, B.; Rédini, F.; Heymann, D. Molecular alterations associated with osteosarcoma development. Sarcoma 2012, 2012, 523432. [Google Scholar]
© 2013 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Ando, K.; Heymann, M.-F.; Stresing, V.; Mori, K.; Rédini, F.; Heymann, D. Current Therapeutic Strategies and Novel Approaches in Osteosarcoma. Cancers 2013, 5, 591-616. https://doi.org/10.3390/cancers5020591
Ando K, Heymann M-F, Stresing V, Mori K, Rédini F, Heymann D. Current Therapeutic Strategies and Novel Approaches in Osteosarcoma. Cancers. 2013; 5(2):591-616. https://doi.org/10.3390/cancers5020591
Chicago/Turabian StyleAndo, Kosei, Marie-Françoise Heymann, Verena Stresing, Kanji Mori, Françoise Rédini, and Dominique Heymann. 2013. "Current Therapeutic Strategies and Novel Approaches in Osteosarcoma" Cancers 5, no. 2: 591-616. https://doi.org/10.3390/cancers5020591
APA StyleAndo, K., Heymann, M.-F., Stresing, V., Mori, K., Rédini, F., & Heymann, D. (2013). Current Therapeutic Strategies and Novel Approaches in Osteosarcoma. Cancers, 5(2), 591-616. https://doi.org/10.3390/cancers5020591







