A Digital Cancer Ecosystem to Deliver Health and Psychosocial Education as Preventive Intervention
Abstract
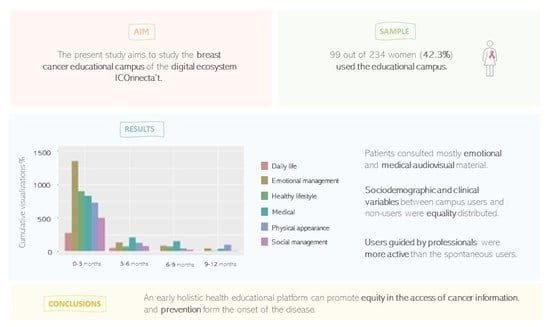
:Simple Summary
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Recruitment and Participants
2.3. ICOnnecta’t Intervention
2.4. Description of Level 2, the Virtual Campus
- The first thematic area is called “my emotions”. Here, patients can find videos, closed-questionnaires, experience-questions, and text information for the emotional impact of cancer, sadness, fear, and irritability.
- The second area is related to the disease and treatments. Resources in this area are videos, closed-questionnaires, and experience-questions about surgery, chemotherapy, radiotherapy, brachytherapy, breast reconstruction, and cancer-associated thrombosis.
- The third area is about “my personal relationships”, where information about children (both communication with them and their emotional experience), about the conspiracy of silence and on how to face the visits with the oncologist. Resources in this area are again videos, closed-questionnaires, experience-questions, and text information.
- The fourth area is related to the body, concretely about body image, hereditary cancer, and sexuality. Resources in this area are videos, closed-questionnaires, experience-questions, text information, and one infographic.
- The fifth area is about a healthy lifestyle, where information about nutrition and rest (sleep and recommendations for insomnia) is featured. In this area, all type of formats can be found.
- The sixth area is related to daily life and activities. This last section contains information about the taboo of cancer. Resources in this area are videos, closed-questionnaires, experience-questions, and text information.
2.5. Statistical Analyses
3. Results
3.1. Participant Characteristics
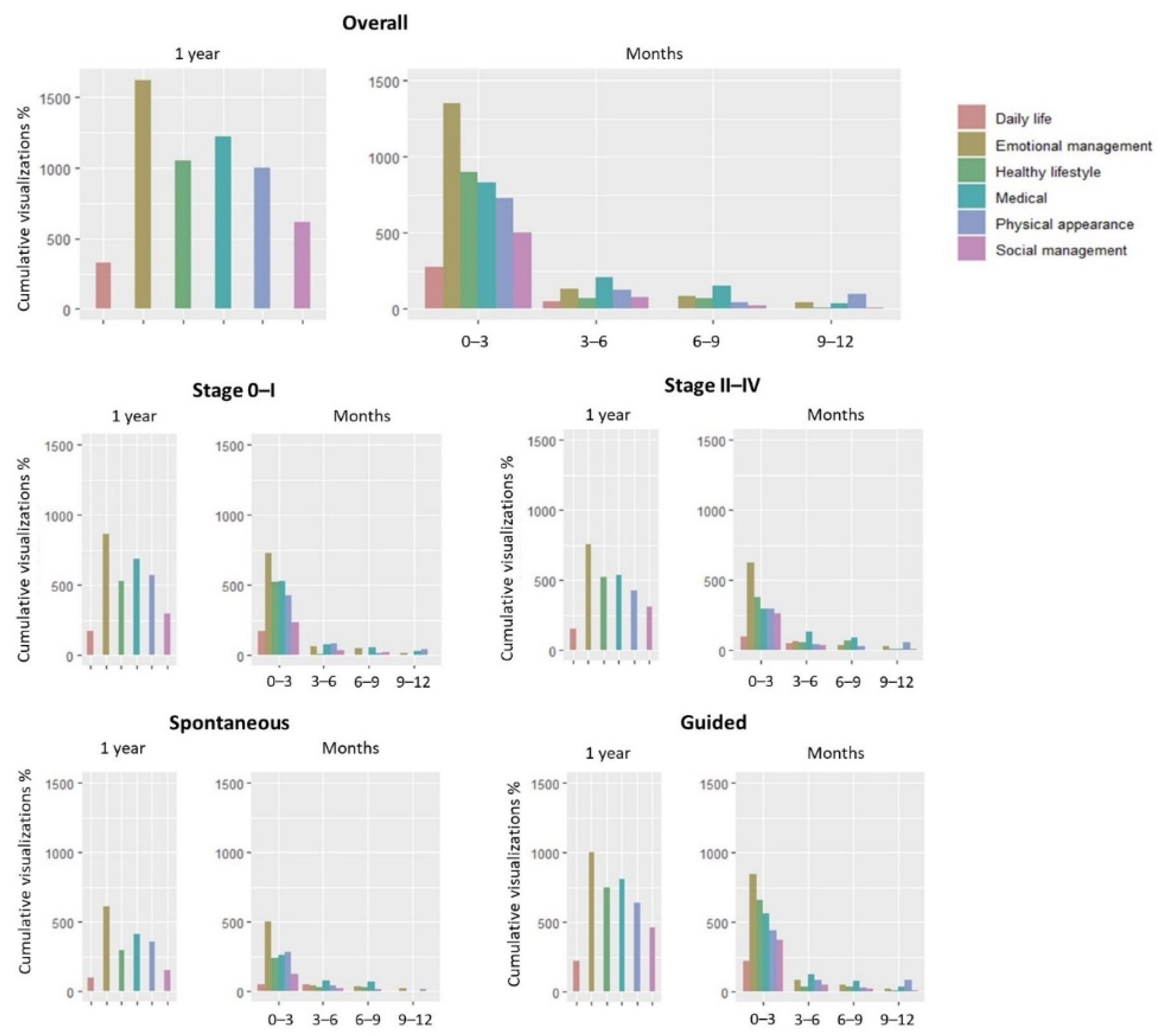
3.2. Resource Utilization
3.3. Patterns of Utilization: Guided vs. Spontaneous Use
3.4. Patterns of Utilization over Time
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- WHO. Breast Cancer Now Most Common Form of Cancer: WHO Taking Action. Available online: https://www.who.int/news/item/03-02-2021-breast-cancer-now-most-common-form-of-cancer-who-taking-action (accessed on 20 March 2021).
- Iacoviello, L.; Bonaccio, M.; de Gaetano, G.; Donati, M.B. Epidemiology of Breast Cancer, a Paradigm of the “Common Soil” Hypothesis. In Seminars in Cancer Biology; Academic Press: Cambridge, MA, USA, 2021; pp. 4–10. [Google Scholar]
- Sung, H.; Ferlay, J.; Siegel, R.L.; Laversanne, M.; Soerjomataram, I.; Jemal, A.; Bray, F. Global Cancer Statistics 2020: GLOBOCAN Estimates of Incidence and Mortality Worldwide for 36 Cancers in 185 Countries. CA Cancer J. Clin. 2021, 71, 209–249. [Google Scholar] [CrossRef]
- Clèries, R.; Rooney, R.M.; Vilardell, M.; Espinàs, J.A.; Dyba, T.; Borras, J.M. Assessing Predicted Age-Specific Breast Cancer Mortality Rates in 27 European Countries by 2020. Clin. Transl. Oncol. 2017, 20, 313–321. [Google Scholar] [CrossRef] [Green Version]
- Grassi, L. Psychiatric and Psychosocial Implications in Cancer Care: The Agenda of Psycho-Oncology. Epidemiol. Psychiatr. Sci. 2020, 29, e89. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ozkan, M. Psychosocial Adaptation during and after Breast Cancer. In Breast Disease: Management and Therapies; Springer: Berlin/Heidelberg, Germany, 2016; ISBN 9783319260129. [Google Scholar]
- Ciria-Suarez, L.; Jiménez-Fonseca, P.; Palacín-Lois, M.; Antoñanzas-Basa, M.; Fernández-Montes, A.; Manzano-Fernández, A.; Castelo, B.; Asensio-Martínez, E.; Hernando-Polo, S.; Calderon, C. Breast cancer patient experiences through a journey map: A qualitative study. PLoS ONE 2021, 16, e0257680. [Google Scholar] [CrossRef]
- Kim, S.C.; Hawkins, R.P.; Shah, D.V.; Gustafson, D.H.; Baker, T.B. Understanding how e-health interventions meet psychosocial needs of breast cancer patients: The pathways of influence on quality of life and cancer concerns. Psycho-Oncology 2020, 29, 1704–1712. [Google Scholar] [CrossRef]
- Yanez, B.R.; Buitrago, D.; Buscemi, J.; Iacobelli, F.; Adler, R.F.; Corden, M.E.; Perez-Tamayo, A.; Guitelman, J.; Penedo, F.J. Study design and protocol for My Guide: An e-health intervention to improve patient-centered outcomes among Hispanic breast cancer survivors. Contemp. Clin. Trials 2017, 65, 61–68. [Google Scholar] [CrossRef]
- Calderon, C.; Carmona-Bayonas, A.; Hernández, R.; Ghanem, I.; Castelo, B.; de Castro, E.M.; Ferreira, E.; Ciria, L.; Muñiz, M.; Jimenez-Fonseca, P. Effects of pessimism, depression, fatigue, and pain on functional health-related quality of life in patients with resected non-advanced breast cancer. Breast 2019, 44, 108–112. [Google Scholar] [CrossRef]
- Kumar, K.; Mattoo, S.K. Psychosocial Aspects of Breast Cancer. In Breast Cancer; Sharma, S.C., Mazumdar, A., Kaushik, R., Eds.; Springer: Singapore, 2022; pp. 567–571. [Google Scholar]
- Ochoa-Arnedo, C.; Prats, C.; Travier, N.; Marques-Feixa, L.; Flix-Valle, A.; de Frutos, M.L.; Domingo-Gil, E.; Medina, J.C.; Serra-Blasco, M. Stressful Life Events and Distress in Breast Cancer: A 5-Years Follow-Up. Int. J. Clin. Health Psychol. 2022, 22, 100303. [Google Scholar] [CrossRef] [PubMed]
- Chen, Y.; Ahmad, M. Effectiveness of adjunct psychotherapy for cancer treatment: A review. Futur. Oncol. 2018, 14, 1487–1496. [Google Scholar] [CrossRef]
- Oh, P.J.; Shin, S.R.; Ahn, H.S.; Kim, H.J. Meta-analysis of psychosocial interventions on survival time in patients with cancer. Psychol. Health 2015, 31, 396–419. [Google Scholar] [CrossRef]
- Samoil, D.; Kim, J.; Fox, C.; Papadakos, J.K. The importance of health literacy on clinical cancer outcomes: A scoping review. Ann. Cancer Epidemiol. 2021, 5, 30. [Google Scholar] [CrossRef]
- Baccolini, V.; Isonne, C.; Salerno, C.; Giffi, M.; Migliara, G.; Mazzalai, E.; Turatto, F.; Sinopoli, A.; Rosso, A.; De Vito, C.; et al. The association between adherence to cancer screening programs and health literacy: A systematic review and meta-analysis. Prev. Med. 2021, 155, 106927. [Google Scholar] [CrossRef]
- Plummer, L.C.; Chalmers, K.A. Health literacy and physical activity in women diagnosed with breast cancer. Psycho-Oncology 2016, 26, 1478–1483. [Google Scholar] [CrossRef]
- Hand, T.; Rosseau, N.A.; Stiles, C.E.; Sheih, T.; Ghandakly, E.; Oluwasanu, M.; Olopade, O.I. The global role, impact, and limitations of Community Health Workers (CHWs) in breast cancer screening: A scoping review and recommendations to promote health equity for all. Glob. Health Action 2021, 14, 1883336. [Google Scholar] [CrossRef]
- Brewer, L.C.; Fortuna, K.L.; Jones, C.; Walker, R.; Hayes, S.N.; Patten, C.A.; Cooper, L.A. Back to the Future: Achieving Health Equity Through Health Informatics and Digital Health. JMIR mHealth uHealth 2020, 8, e14512. [Google Scholar] [CrossRef]
- Kemp, E.; Trigg, J.; Beatty, L.; Christensen, C.; Dhillon, H.M.; Maeder, A.; Williams, P.A.H.; Koczwara, B. Health literacy, digital health literacy and the implementation of digital health technologies in cancer care: The need for a strategic approach. Health Promot. J. Aust. 2020, 32, 104–114. [Google Scholar] [CrossRef]
- Ochoa-Arnedo, C.; Flix-Valle, A.; Medina, J.C.; Escriche, E.; Rodríguez, A.; Villanueva, C.; Sumalla, E.C.; Alabèrnia-Segura, M.; Prats, C.; Corral, M.J.; et al. E-Health Iconnecta’t Program: An Ecosystem to Promote Wellbing in Cancer towards Oncommun European Proposal. Psicooncologia 2020, 17, 41–58. [Google Scholar] [CrossRef] [Green Version]
- Medina, J.C.; Flix-Valle, A.; Rodríguez-Ortega, A.; Hernández-Ribas, R.; de Frutos, M.L.; Ochoa-Arnedo, C. ICOnnecta’t: Development and Initial Results of a Stepped Psychosocial eHealth Ecosystem to Facilitate Risk Assessment and Prevention of Early Emotional Distress in Breast Cancer Survivors’ Journey. Cancers 2022, 14, 974. [Google Scholar] [CrossRef]
- Friedman, A.J.; Cosby, R.; Boyko, S.; Hatton-Bauer, J.; Turnbull, G. Effective Teaching Strategies and Methods of Delivery for Patient Education: A Systematic Review and Practice Guideline Recommendations. J. Cancer Educ. 2010, 26, 12–21. [Google Scholar] [CrossRef]
- Ochoa-Arnedo, C.; Medina, J.C.; Flix-Valle, A.; Anastasiadou, D. E-health ecosystem with integrated and stepped psychosocial services for breast cancer survivors: Study protocol of a multicentre randomised controlled trial. BMJ Open 2021, 11, e041548. [Google Scholar] [CrossRef]
- Arnedo, C.O.; Casellas-Grau, A. Positive Psychotherapy in Cancer: Facilitating Posttraumatic Growth in Assimilation and Accommodation of Traumatic Experience. In Comprehensive Guide to Post-Traumatic Stress Disorder; Springer: Cham, Switzerland, 2015; p. 114. [Google Scholar] [CrossRef]
- Ochoa-Arnedo, C.; Flix-Valle, A.; Casellas-Grau, A.; Casanovas-Aljaro, N.; Herrero, O.; Sumalla, E.C.; de Frutos, M.L.; Sirgo, A.; Rodríguez, A.; Campos, G.; et al. An exploratory study in breast cancer of factors involved in the use and communication with health professionals of Internet information. Support. Care Cancer 2020, 28, 4989–4996. [Google Scholar] [CrossRef]
- Mallmann, C.A.; Domröse, C.M.; Schröder, L.; Engelhardt, D.; Bach, F.; Rueckel, H.; Abramian, A.; Kaiser, C.; Mustea, A.; Faridi, A.; et al. Digital Technical and Informal Resources of Breast Cancer Patients From 2012 to 2020: Questionnaire-Based Longitudinal Trend Study. JMIR Cancer 2021, 7, e20964. [Google Scholar] [CrossRef]
- Crouch, E.; Gordon, N.P. Prevalence and Factors Influencing Use of Internet and Electronic Health Resources by Middle-Aged and Older Adults in a US Health Plan Population: Cross-Sectional Survey Study. JMIR Aging 2019, 2, e11451. [Google Scholar] [CrossRef]
- Faber, J.S.; Al-Dhahir, I.; Reijnders, T.; Chavannes, N.H.; Evers, A.W.M.; Kraal, J.J.; van den Berg-Emons, H.J.G.; Visch, V.T. Attitudes Toward Health, Healthcare, and eHealth of People With a Low Socioeconomic Status: A Community-Based Participatory Approach. Front Digit Health 2021, 3, 690182. [Google Scholar] [CrossRef]
- Silfee, V.J.; Lopez-Cepero, A.; Lemon, S.C.; Estabrook, B.; Nguyen, O.; Wang, M.L.; Rosal, M.C. Adapting a behavioral weight loss intervention for delivery via facebook: A pilot series among low-income postpartum women. JMIR Form Res. 2018, 2, 18. [Google Scholar] [CrossRef]
- Cavallo, D.N.; Martinez, R.; Webb Hooper, M.; Flocke, S. Feasibility of a social media-based weight loss intervention designed for low-SES adults. Transl. Behav. Med. 2021, 11, 981–992. [Google Scholar] [CrossRef]
- Greene, E.M.; O’Brien, E.C.; Kennelly, M.A.; O’Brien, O.A.; Lindsay, K.L.; McAuliffe, F.M. Acceptability of the pregnancy, exercise, and nutrition research study with smartphone app support (PEARS) and the use of mobile health in a mixed lifestyle intervention by pregnant obese and overweight women: Secondary analysis of a randomized controlled trial. JMIR mHealth uHealth. 2021, 9, 17189. [Google Scholar] [CrossRef]
- Mayberry, L.S.; Berg, C.A.; Harper, K.J.; Osborn, C.Y. The Design, Usability, and Feasibility of a Family-Focused Diabetes Self-Care Support mHealth Intervention for Diverse, Low-Income Adults with Type 2 Diabetes. J. Diabetes Res. 2016. [Google Scholar] [CrossRef] [Green Version]
- Patten, C.A.; Fu, S.; Vickerman, K.; Bock, M.J.; Nelson, D.; Zhu, S.H.; Balls-Berry, J.E.; Torres, A.J.; Brockman, T.A.; Hughes, C.A.; et al. Support person interventions to increase use of quitline services among racially diverse low-income smokers: A pilot study. Addict. Behav. Reports. 2019, 9, 100171. [Google Scholar] [CrossRef]
- Bae, S.S.; Baxter, S. YouTube videos in the English language as a patient education resource for cataract surgery. Int. Ophthalmol. 2017, 38, 1941–1945. [Google Scholar] [CrossRef]
- Sahin, A.N.; Sahin, A.S.; Schwenter, F.; Sebajang, H. YouTube Videos as a Source of Information on Colorectal Cancer: What Do Our Patients Learn? J. Cancer Educ. 2018, 34, 1160–1166. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Yurdaisik, I. Analysis of the Most Viewed First 50 Videos on YouTube about Breast Cancer. BioMed Res. Int. 2020, 2020, 2750148. [Google Scholar] [CrossRef] [PubMed]
- Lu, H.; Xie, J.; Gerido, L.H.; Cheng, Y.; Chen, Y.; Sun, L. Information Needs of Breast Cancer Patients: Theory-Generating Meta-Synthesis. J. Med. Internet Res. 2020, 22, e17907. [Google Scholar] [CrossRef] [PubMed]
- Singleton, A.C.; Raeside, R.; Hyun, K.K.; Partridge, S.R.; Di Tanna, G.L.; Hafiz, N.; Tu, Q.; Tat-Ko, J.; Sum, S.C.M.; Sherman, K.A.; et al. Electronic Health Interventions for Patients with Breast Cancer: Systematic Review and Meta-Analyses. J. Clin. Oncol. 2022, 40, 2257. [Google Scholar] [CrossRef]
- McRoy, S.; Rastegar-Mojarad, M.; Wang, Y.; Ruddy, K.J.; Haddad, T.C.; Liu, H. Assessing Unmet Information Needs of Breast Cancer Survivors: Exploratory Study of Online Health Forums Using Text Classification and Retrieval. JMIR Cancer 2018, 4, e9050. [Google Scholar] [CrossRef] [Green Version]
- Lally, R.M.; Kupzyk, K.A.; Bellavia, G.; Hydeman, J.; Gallo, S.; Helgeson, V.S.; Erwin, D.; Mills, A.C.; Brown, J.K. CaringGuidance™ after breast cancer diagnosis eHealth psychoeducational intervention to reduce early post-diagnosis distress. Support. Care Cancer 2019, 28, 2163–2174. [Google Scholar] [CrossRef] [Green Version]
- Ormel, I.; Magalhaes, M.; Josephson, D.; Tracey, L.; Law, S. How to know what to know: Information challenges for women in the diagnostic phase of breast cancer. Patient Educ. Couns. 2020, 104, 179–185. [Google Scholar] [CrossRef] [PubMed]
- Sheehy, E.M.; Lehane, E.; Quinn, E.; Livingstone, V.; Redmond, H.P.; Corrigan, M.A. Information Needs of Patients with Breast Cancer at Years One, Three, and Five After Diagnosis. Clin. Breast Cancer 2018, 18, e1269–e1275. [Google Scholar] [CrossRef]
- Drageset, S.; Lindstrøm, T.C.; Underlid, K. Coping with breast cancer: Between diagnosis and surgery. J. Adv. Nurs. 2009, 66, 149–158. [Google Scholar] [CrossRef]
- Tran, Y.; Lamprell, K.; Easpaig, B.N.G.; Arnolda, G.; Braithwaite, J. What information do patients want across their cancer journeys? A network analysis of cancer patients’ information needs. Cancer Med. 2018, 8, 155–164. [Google Scholar] [CrossRef]
- Jacobs, M.; Johnson, J. MyPath: Investigating Breast Cancer Patients’ Use of Personalized Health Information. Proc. ACM Hum.-Comput. Interact. 2018, 2, 1–21. [Google Scholar] [CrossRef]
- Houghton, L.C.; Howland, R.E.; McDonald, J.A. Mobilizing Breast Cancer Prevention Research Through Smartphone Apps: A Systematic Review of the Literature. Front. Public Health 2019, 7, 298. [Google Scholar] [CrossRef] [PubMed]
| Non-Users(n = 135) | Users(n = 99) | p-Value * | ||
|---|---|---|---|---|
| n(%) | n(%) | |||
| Age (terciles) | 0.116 | |||
| <47 | 38(28.1) | 34(34.3) | ||
| 47–55 | 44(32.6) | 39(39.4) | ||
| 56+ | 53(39.3) | 26(26.3) | ||
| Marital status | 0.107 | |||
| Married or common-law partner | 97(71.9) | 80(80.8) | ||
| Separated or divorced | 15(11.1) | 4(4.0) | ||
| Single | 8(5.9) | 8(8.1) | ||
| Widow | 5(3.7) | 1(1.0) | ||
| missing | 10(7.4) | 6(6.1) | ||
| Occupational status | 0.182 | |||
| Active | 37(27.4) | 33(33.3) | ||
| Work leave | 51(37.8) | 42(42.4) | ||
| Occupational disability | 3(2.2) | 0(0.0) | ||
| Retired | 13(9.6) | 4(4.0) | ||
| Passive | 20(14.8) | 11(11.1) | ||
| missing | 11(8.1) | 9(9.1) | ||
| Year of diagnosis | 0.573 | |||
| 2019 | 80(59.3) | 54(54.5) | ||
| 2020 | 54(40.0) | 43(43.4) | ||
| 2021 | 1(0.7) | 2(2.0) | ||
| Stage | 0.370 | |||
| 0-I | 68(50.4) | 44(44.4) | ||
| II-IV | 67(49.6) | 55(55.6) | ||
| Number of Resources | Total Number of Utilizations | Median Proportion of Utilized Resources, among Users (IQR) | Median Number of Resources Utilized per User, among Participants (IQR) | Women Who Have Utilized One Resource or More | |||||
|---|---|---|---|---|---|---|---|---|---|
| p-Value * | p-Value * | n | % (among Users) | % (Overall) | |||||
| Type of format | |||||||||
| Videos | 16 | 323 | 13% (6–31%) | <0.01 | 2 (1–5) | <0.01 | 85 | 85.9% | 36.3% |
| Closed questions | 16 | 144 | 0% (0–13%) | 0 (0–2) | 41 | 41.4% | 17.5% | ||
| Open questions | 15 | 50 | 0% (0–0%) | 0 (0–0) | 23 | 23.2% | 9.8% | ||
| Text | 15 | 195 | 7% (0–20%) | 1 (0–3) | 66 | 66.7% | 28.2% | ||
| Infographics | 4 | 45 | 0% (0–25%) | 0 (0–1) | 31 | 31.3% | 13.2% | ||
| Type of content | |||||||||
| Medical | 20 | 245 | 5% (0–15%) | <0.01 | 1 (0–3) | <0.01 | 67 | 67.7% | 28.6% |
| Emotional management | 17 | 275 | 6% (0–24%) | 1 (0–4) | 53 | 53.5% | 22.6% | ||
| Healthy lifestyle | 10 | 105 | 0% (0–10%) | 0 (0–1) | 41 | 41.4% | 17.5% | ||
| Social management | 8 | 49 | 0% (0–0%) | 0 (0–0) | 22 | 22.2% | 9.4% | ||
| Physical appearance | 7 | 70 | 0% (0–14%) | 0 (0–1) | 41 | 41.4% | 17.5% | ||
| Daily life | 4 | 13 | 0% (0–0%) | 0 (0–0) | 8 | 8.1% | 3.4% | ||
| Total | 66 | 757 | 6% (3–14%) | 4 (2–9) | 99 | 100.0% | 42.3% | ||
| Number of Available Resources | Median Proportion of Utilized Resources, among Users (IQR) | Median Number of Resources Utilized per User, among Users (IQR) | Women Who Utilized One Resource or More | |||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Total Number of Utilizations | p-Value * | n | % (among Subgroup -Spontaneous or Guided-) | % (among Users) | % (Overall) | |||||
| ESPONTANEOUS USE (n = 49) | ||||||||||
| Type of format | ||||||||||
| Videos | 16 | 125 | 13% (6–22%) | 0.053 | 2 (1–4) | 41 | 83.7% | 41.4% | 17.5% | |
| Closed questions | 16 | 40 | 0% (0–6%) | 0.256 | 0 (0–1) | 19 | 38.8% | 19.2% | 8.1% | |
| Open questions | 15 | 16 | 0% (0–0%) | 0.783 | 0 (0–0) | 11 | 22.4% | 11.1% | 4.7% | |
| Text | 15 | 68 | 7% (0–13%) | 0.035 | 1 (0–2) | 29 | 59.2% | 29.3% | 12.4% | |
| Infographics | 4 | 9 | 0% (0–0%) | 0.001 | 0 (0–0) | 8 | 16.3% | 8.1% | 3.4% | |
| Type of content | ||||||||||
| Medical | 20 | 83 | 5% (0–10%) | 0.033 | 1 (0–2) | 31 | 63.3% | 31.3% | 13.2% | |
| Emotional management | 17 | 104 | 0% (0–18%) | 0.096 | 0 (0–3) | 22 | 44.9% | 22.2% | 9.4% | |
| Healthy lifestyle | 10 | 30 | 0% (0–10%) | 0.076 | 0 (0–1) | 17 | 34.7% | 17.2% | 7.3% | |
| Social management | 8 | 12 | 0% (0–0%) | 0.048 | 0 (0–0) | 7 | 14.3% | 7.1% | 3.0% | |
| Physical appearance | 7 | 25 | 0% (0–14%) | 0.170 | 0 (0–1) | 18 | 36.7% | 18.2% | 7.7% | |
| Daily life | 4 | 4 | 0% (0–0%) | 0.450 | 0 (0–0) | 3 | 6.1% | 3.0% | 1.3% | |
| Total | 66 | 258 | 5% (3–11%) | 0.026 | 3 (2–8) | 49 | 100.0% | 49.5% | 20.9% | |
| GUIDED USE (n = 50) | ||||||||||
| Type of format | ||||||||||
| Videos | 16 | 198 | 19% (6–31%) | 3 (1–5) | 44 | 88.0% | 44.4% | 18.8% | ||
| Closed questions | 16 | 104 | 0% (0–13%) | 0 (0–2) | 22 | 44.0% | 22.2% | 9.4% | ||
| Open questions | 15 | 34 | 0% (0–2%) | 0 (0–0) | 12 | 24.0% | 12.1% | 5.1% | ||
| Text | 15 | 127 | 10% (0–20%) | 2 (0–3) | 37 | 74.0% | 37.4% | 15.8% | ||
| Infographics | 4 | 36 | 0% (0–25%) | 0 (0–1) | 23 | 46.0% | 23.2% | 9.8% | ||
| Type of content | ||||||||||
| Medical | 20 | 162 | 13% (0–20%) | 3 (0–4) | 36 | 72.0% | 36.4% | 15.4% | ||
| Emotional management | 17 | 171 | 9% (0–25%) | 2 (0–4) | 31 | 62.0% | 31.3% | 13.2% | ||
| Healthy lifestyle | 10 | 75 | 0% (0–20%) | 0 (0–2) | 24 | 48.0% | 24.2% | 10.3% | ||
| Social management | 8 | 37 | 0% (0–13%) | 0 (0–1) | 15 | 30.0% | 15.2% | 6.4% | ||
| Physical appearance | 7 | 45 | 0% (0–18%) | 0 (0–1) | 23 | 46.0% | 23.2% | 9.8% | ||
| Daily life | 4 | 9 | 0% (0–0%) | 0 (0–0) | 5 | 10.0% | 5.1% | 2.1% | ||
| Total | 66 | 499 | 10% (3–15%) | 7 (2–10) | 50 | 100.0% | 50.5% | 21.4% | ||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ciria-Suarez, L.; Costas, L.; Flix-Valle, A.; Serra-Blasco, M.; Medina, J.C.; Ochoa-Arnedo, C. A Digital Cancer Ecosystem to Deliver Health and Psychosocial Education as Preventive Intervention. Cancers 2022, 14, 3724. https://doi.org/10.3390/cancers14153724
Ciria-Suarez L, Costas L, Flix-Valle A, Serra-Blasco M, Medina JC, Ochoa-Arnedo C. A Digital Cancer Ecosystem to Deliver Health and Psychosocial Education as Preventive Intervention. Cancers. 2022; 14(15):3724. https://doi.org/10.3390/cancers14153724
Chicago/Turabian StyleCiria-Suarez, Laura, Laura Costas, Aida Flix-Valle, Maria Serra-Blasco, Joan C. Medina, and Cristian Ochoa-Arnedo. 2022. "A Digital Cancer Ecosystem to Deliver Health and Psychosocial Education as Preventive Intervention" Cancers 14, no. 15: 3724. https://doi.org/10.3390/cancers14153724
APA StyleCiria-Suarez, L., Costas, L., Flix-Valle, A., Serra-Blasco, M., Medina, J. C., & Ochoa-Arnedo, C. (2022). A Digital Cancer Ecosystem to Deliver Health and Psychosocial Education as Preventive Intervention. Cancers, 14(15), 3724. https://doi.org/10.3390/cancers14153724