Natural History and Prognostic Factors at First Relapse in Multiple Myeloma
Abstract
1. Introduction
2. Methods
2.1. Patients
2.2. Statistical Analyses
3. Results
3.1. Patients’ Characteristics
3.2. Treatment Sequences by Comparing Initial and Salvage Regimens
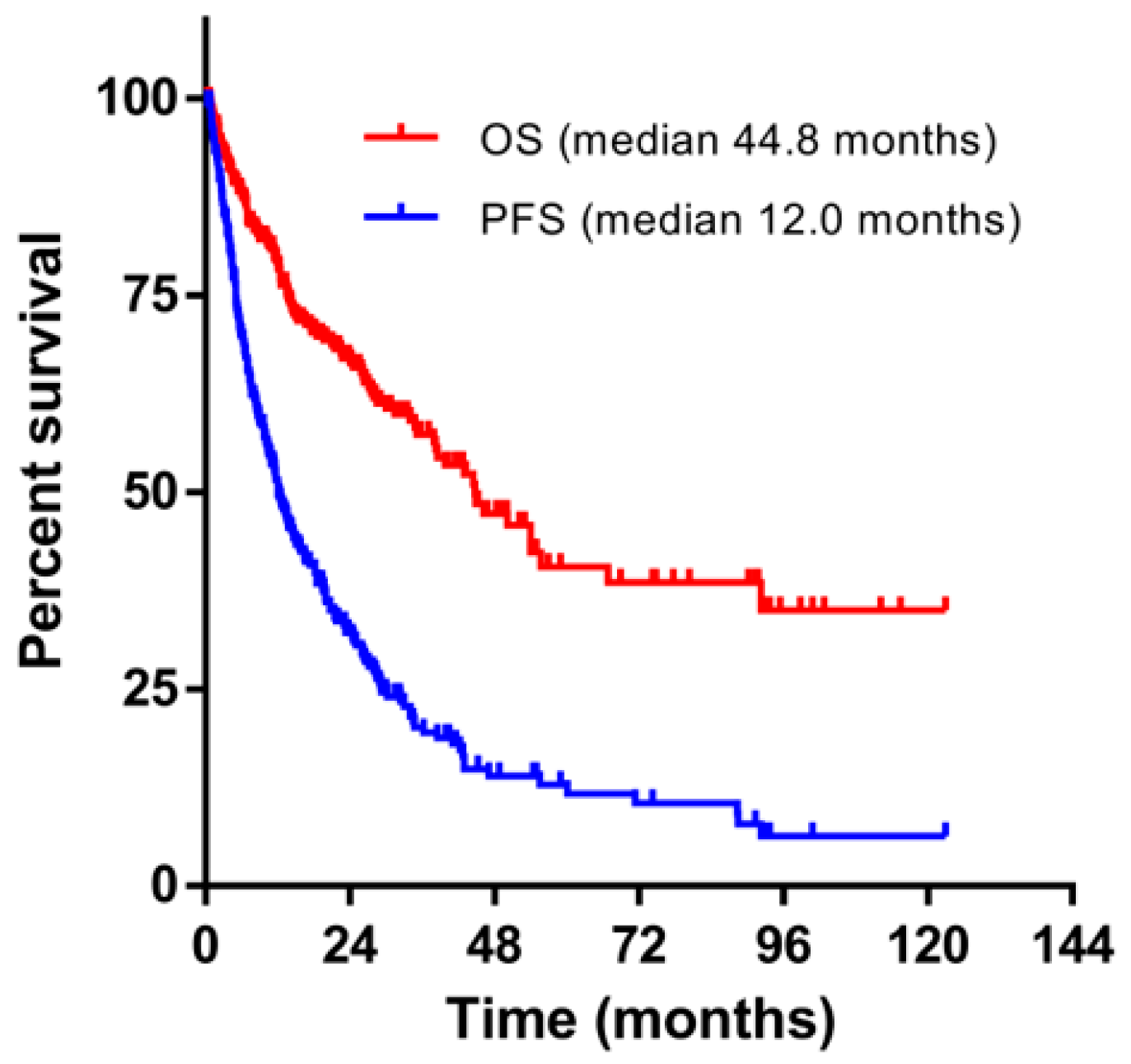
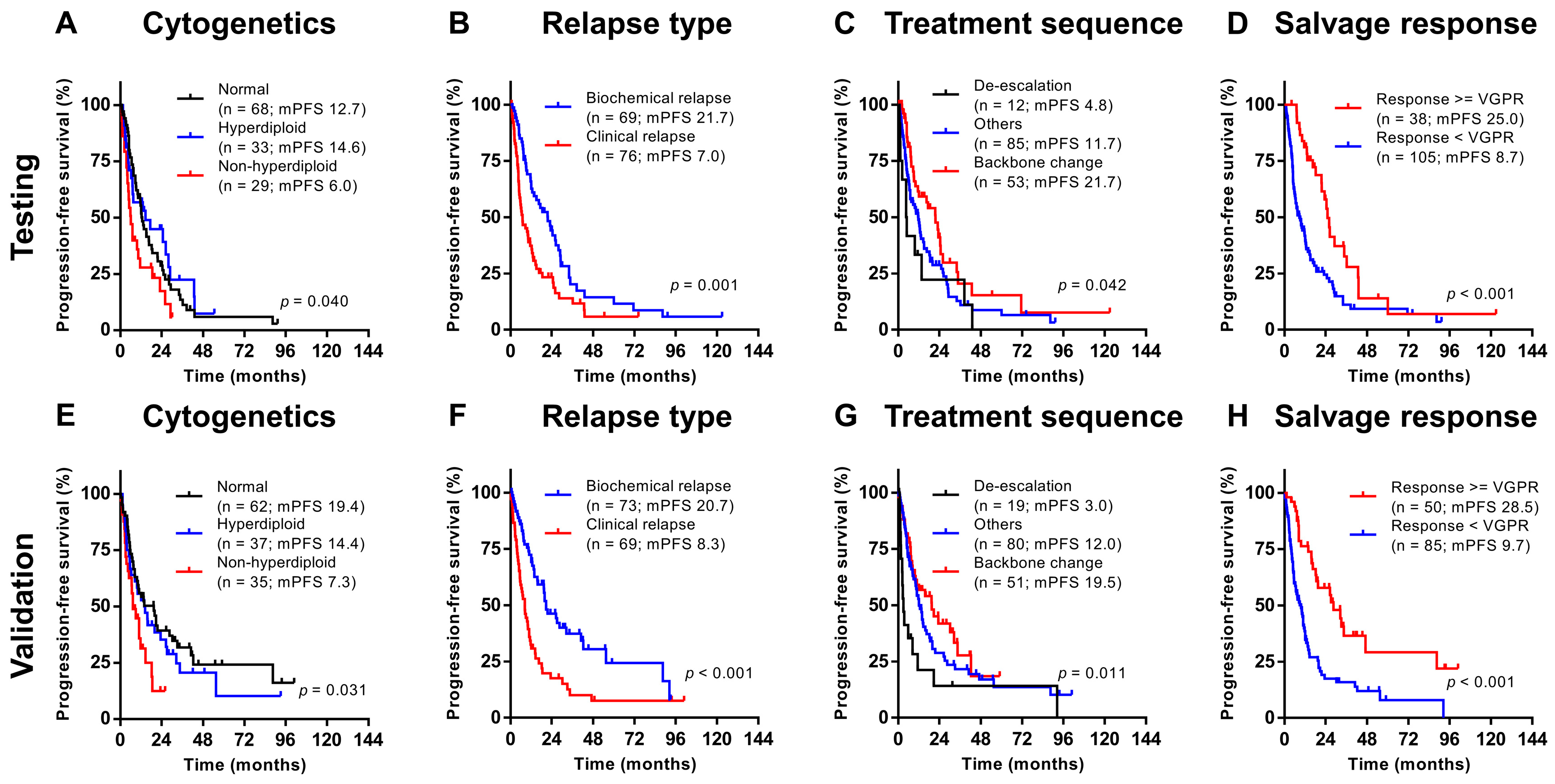
3.3. Survival Outcomes after First Relapse
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Rajkumar, S.V.; Dimopoulos, M.A.; Palumbo, A.; Blade, J.; Merlini, G.; Mateos, M.V.; Kumar, S.; Hillengass, J.; Kastritis, E.; Richardson, P.; et al. International Myeloma Working Group updated criteria for the diagnosis of multiple myeloma. Lancet Oncol. 2014, 15, e538–e548. [Google Scholar] [CrossRef]
- Ocio, E.M.; Richardson, P.G.; Rajkumar, S.V.; Palumbo, A.; Mateos, M.V.; Orlowski, R.; Kumar, S.; Usmani, S.; Roodman, D.; Niesvizky, R.; et al. New drugs and novel mechanisms of action in multiple myeloma in 2013: A report from the International Myeloma Working Group (IMWG). Leukemia 2014, 28, 525–542. [Google Scholar] [CrossRef]
- Sonneveld, P. Management of multiple myeloma in the relapsed/refractory patient. Hematol. Am. Soc. Hematol. Educ. Program. 2017, 2017, 508–517. [Google Scholar] [CrossRef] [PubMed]
- Harousseau, J.L.; Attal, M. How I treat first relapse of myeloma. Blood 2017, 130, 963–973. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Dingli, D.; Ailawadhi, S.; Bergsagel, P.L.; Buadi, F.K.; Dispenzieri, A.; Fonseca, R.; Gertz, M.A.; Gonsalves, W.I.; Hayman, S.R.; Kapoor, P.; et al. Therapy for Relapsed Multiple Myeloma: Guidelines From the Mayo Stratification for Myeloma and Risk-Adapted Therapy. Mayo. Clin. Proc. 2017, 92, 578–598. [Google Scholar] [CrossRef] [PubMed]
- Kumar, S.K.; Therneau, T.M.; Gertz, M.A.; Lacy, M.Q.; Dispenzieri, A.; Rajkumar, S.V.; Fonseca, R.; Witzig, T.E.; Lust, J.A.; Larson, D. Clinical course of patients with relapsed multiple myeloma. Mayo Clin. Proc. 2004, 79, 867–874. [Google Scholar] [CrossRef] [PubMed]
- Garderet, L.; Iacobelli, S.; Moreau, P.; Dib, M.; Lafon, I.; Niederwieser, D.; Masszi, T.; Fontan, J.; Michallet, M.; Gratwohl, A.; et al. Superiority of the triple combination of bortezomib-thalidomide-dexamethasone over the dual combination of thalidomide-dexamethasone in patients with multiple myeloma progressing or relapsing after autologous transplantation: The MMVAR/IFM 2005-04 Randomized Phase III Trial from the Chronic Leukemia Working Party of the European Group for Blood and Marrow Transplantation. J. Clin. Oncol. 2012, 30, 2475–2482. [Google Scholar]
- Stewart, A.K.; Rajkumar, S.V.; Dimopoulos, M.A.; Masszi, T.; Špička, I.; Oriol, A.; Hájek, R.; Rosiñol, L.; Siegel, D.S.; Mihaylov, G.G.; et al. Carfilzomib, lenalidomide, and dexamethasone for relapsed multiple myeloma. N. Engl. J. Med. 2015, 372, 142–152. [Google Scholar] [CrossRef]
- Lonial, S.; Dimopoulos, M.; Palumbo, A.; White, D.; Grosicki, S.; Spicka, I.; Walter-Croneck, A.; Moreau, P.; Mateos, M.V.; Magen, H.; et al. Elotuzumab Therapy for Relapsed or Refractory Multiple Myeloma. N. Engl. J. Med. 2015, 373, 621–631. [Google Scholar] [CrossRef]
- Moreau, P.; Masszi, T.; Grzasko, N.; Bahlis, N.J.; Hansson, M.; Pour, L.; Sandhu, I.; Ganly, P.; Baker, B.W.; Jackson, S.R.; et al. Oral Ixazomib, Lenalidomide, and Dexamethasone for Multiple Myeloma. N. Engl. J. Med. 2016, 374, 1621–1634. [Google Scholar] [CrossRef]
- Dimopoulos, M.A.; Oriol, A.; Nahi, H.; San-Miguel, J.; Bahlis, N.J.; Usmani, S.Z.; Rabin, N.; Orlowski, R.Z.; Komarnicki, M.; Suzuki, K.; et al. Daratumumab, Lenalidomide, and Dexamethasone for Multiple Myeloma. N. Engl. J. Med. 2016, 375, 1319–1331. [Google Scholar] [CrossRef] [PubMed]
- Palumbo, A.; Chanan-Khan, A.; Weisel, K.; Nooka, A.K.; Masszi, T.; Beksac, M.; Spicka, I.; Hungria, V.; Munder, M.; Mateos, M.V.; et al. Daratumumab, Bortezomib, and Dexamethasone for Multiple Myeloma. N. Engl. J. Med. 2016, 375, 754–766. [Google Scholar] [CrossRef]
- Rajkumar, S.V.; Harousseau, J.L. Next-generation multiple myeloma treatment: A pharmacoeconomic perspective. Blood 2016, 128, 2757–2764. [Google Scholar] [CrossRef]
- Tan, D.; Lee, J.H.; Chen, W.; Shimizu, K.; Hou, J.; Suzuki, K.; Nawarawong, W.; Huang, S.Y.; Sang Chim, C.; Kim, K.; et al. Recent advances in the management of multiple myeloma: Clinical impact based on resource-stratification. Consensus statement of the Asian Myeloma Network at the 16th international myeloma workshop. Leuk. Lymphoma. 2018, 29, 2305–2317. [Google Scholar] [CrossRef]
- Kim, K.; Lee, J.H.; Kim, J.S.; Min, C.K.; Yoon, S.S.; Shimizu, K.; Chou, T.; Kosugi, H.; Suzuki, K.; Chen, W.; et al. Clinical profiles of multiple myeloma in Asia-An Asian Myeloma Network study. Am. J. Hematol. 2014, 89, 751–756. [Google Scholar] [CrossRef]
- de Mel, S.; Chen, Y.; Gopalakrishnan, S.K.; Ooi, M.; Teo, C.; Tan, D.; Teo, M.L.; Tso, A.C.; Lee, L.K.; Nagarajan, C.; et al. The Singapore Myeloma Study Group Consensus Guidelines for the management of patients with multiple myeloma. Singapore Med. J. 2017, 58, 55–71. [Google Scholar] [CrossRef] [PubMed]
- Kumar, S.K.; LaPlant, B.; Chng, W.J.; Zonder, J.; Callander, N.; Fonseca, R.; Fruth, B.; Roy, V.; Erlichman, C.; Stewart, A.K.; et al. Dinaciclib, a novel CDK inhibitor, demonstrates encouraging single-agent activity in patients with relapsed multiple myeloma. Blood 2015, 125, 443–448. [Google Scholar] [CrossRef]
- Kumar, S.; Paiva, B.; Anderson, K.C.; Durie, B.; Landgren, O.; Moreau, P.; Munshi, N.; Lonial, S.; Bladé, J.; Mateos, M.V.; et al. International Myeloma Working Group consensus criteria for response and minimal residual disease assessment in multiple myeloma. Lancet Oncol. 2016, 17, e328–e346. [Google Scholar] [CrossRef]
- Wang, C.; Huang, X.F.; Cai, Q.Q.; Cao, X.X.; Duan, M.H.; Cai, H.; Zhou, D.B. Prognostic study for overall survival in patients with newly diagnosed POEMS syndrome. Leukemia 2017, 31, 100–106. [Google Scholar] [CrossRef] [PubMed]
- Chng, W.J.; Dispenzieri, A.; Chim, C.S.; Fonseca, R.; Goldschmidt, H.; Lentzsch, S.; Munshi, N.; Palumbo, A.; Miguel, J.S.; Sonneveld, P.; et al. IMWG consensus on risk stratification in multiple myeloma. Leukemia 2014, 28, 269–277. [Google Scholar] [CrossRef] [PubMed]
- Soekojo, C.Y.; Wang, G.M.; Chen, Y.; Casan, J.; Wolyncewicz, G.; Lin, A.; Poon, L.M.; de Mel, S.; Koh, L.P.; Tan, L.K.; et al. Role of Conventional Karyotyping in Multiple Myeloma in the Era of Modern Treatment and FISH Analysis. Clin. Lymphoma Myeloma Leuk. 2019, 19, e470–e477. [Google Scholar] [CrossRef] [PubMed]
- Tan, D.; Teoh, G.; Lau, L.C.; Lim, A.; Lim, T.H.; Yap, K.C.; Premalatha, P.; Lao, Z.T.; Wee, N.; Choo, C.; et al. An abnormal nonhyperdiploid karyotype is a significant adverse prognostic factor for multiple myeloma in the bortezomib era. Am. J. Hematol. 2010, 85, 752–756. [Google Scholar] [CrossRef] [PubMed]
- Jimenez-Zepeda, V.H.; Braggio, E. Dissecting Karyotypic Patterns in Non-Hyperdiploid Multiple Myeloma: An Overview on the Karyotypic Evolution. Clin. Lymphoma Myeloma Leuk. 2013, 13, 552–558. [Google Scholar] [CrossRef] [PubMed]
- Chakraborty, R.; Liu, H.D.; Rybicki, L.; Tomer, J.; Khouri, J.; Dean, R.M.; Faiman, B.M.; Kalaycio, M.; Samaras, C.J.; Majhail, N.S. Progression With Clinical Features Is Associated With Worse Subsequent Survival in Multiple Myeloma. Am. J. Hematol. 2019, 94, 439–445. [Google Scholar] [CrossRef]
- Brioli, A.; Melchor, L.; Cavo, M.; Morgan, G.J. The Impact of Intra-Clonal Heterogeneity on the Treatment of Multiple Myeloma. Br. J. Haematol. 2014, 165, 441–454. [Google Scholar] [CrossRef]
- Laubach, J.; Garderet, L.; Mahindra, A.; Gahrton, G.; Caers, J.; Sezer, O.; Voorhees, P.; Leleu, X.; Johnsen, H.E.; Streetly, M. Management of relapsed multiple myeloma: Recommendations of the International Myeloma Working Group. Leukemia 2016, 30, 1005–1017. [Google Scholar] [CrossRef]
- Corre, J.; Cleynen, A.; Robiou du Pont, S.; Buisson, L.; Bolli, N.; Attal, M.; Munshi, N.; Avet-Loiseau, H. Multiple myeloma clonal evolution in homogeneously treated patients. Leukemia 2018, 32, 2636–2647. [Google Scholar] [CrossRef]
- An, G.; Li, Z.; Tai, Y.T.; Acharya, C.; Li, Q.; Qin, X.; Yi, S.; Xu, Y.; Feng, X.; Li, C.; et al. The Impact of Clone Size on the Prognostic Value of Chromosome Aberrations by Fluorescence in Situ Hybridization in Multiple Myeloma. Clin. Cancer Res. 2015, 21, 2148–2156. [Google Scholar] [CrossRef]
- Niesvizky, R.; Richardson, P.G.; Rajkumar, S.V.; Coleman, M.; Rosiñol, L.; Sonneveld, P.; Schuster, M.W.; Irwin, D.; Stadtmauer, E.A.; Facon, T.; et al. The relationship between quality of response and clinical benefit for patients treated on the bortezomib arm of the international, randomized, phase 3 APEX trial in relapsed multiple myeloma. Br. J. Haematol. 2008, 143, 46–53. [Google Scholar] [CrossRef]
- Pineda-Roman, M.; Zangari, M.; van Rhee, F.; Anaissie, E.; Szymonifka, J.; Hoering, A.; Petty, N.; Crowley, J.; Shaughnessy, J.; Epstein, J.; et al. VTD Combination Therapy With Bortezomib-Thalidomide-Dexamethasone Is Highly Effective in Advanced and Refractory Multiple Myeloma. Leukemia 2008, 22, 1419–1427. [Google Scholar] [CrossRef]
- Harousseau, J.L.; Dimopoulos, M.A.; Wang, M.; Corso, A.; Chen, C.; Attal, M.; Spencer, A.; Yu, Z.; Olesnyckyj, M.; Zeldis, J.B.; et al. Better quality of response to lenalidomide plus dexamethasone is associated with improved clinical outcomes in patients with relapsed or refractory multiple myeloma. Haematologica 2010, 95, 1738–1744. [Google Scholar] [CrossRef] [PubMed][Green Version]

| Variables n (%) or Median (range) at Diagnosis | All Patients (n = 300) | Testing Cohort (n = 150) | Validation Cohort (n = 150) | p-Values |
|---|---|---|---|---|
| Male | 166 (55.3) | 79 (52.6) | 87 (58.0) | 0.353 |
| Heavy chain type IgG/IgA/others | 181/52/30 (n = 263) | 86/24/16 (n = 126) | 95/28/14 (n = 137) | 0.807 |
| Anemia * | 188 (63.9) (n = 294) | 93 (62.8) (n = 148) | 95 (65.1) (n = 146) | 0.690 |
| Hypercalcemia | 40 (14.4) (n = 277) | 20 (14.3) (n = 140) | 20 (14.6) (n = 137) | 0.941 |
| Renal insufficiency | 66 (22.7) (n = 291) | 36 (24.3) (n = 148) | 30 (21.0) (n = 143) | 0.496 |
| Bone lesions | 187 (66.5) (n = 281) | 102 (73.9) (n = 138) | 85 (59.4) (n = 143) | 0.010 |
| Extramedullary plasmacytoma | 54 (19.2) (n = 281) | 31 (22.5) (n = 138) | 23 (16.1) (n = 143) | 0.175 |
| Elevated LDH | 45 (19.6) (n = 230) | 19 (17.1) (n = 111) | 26 (21.8) (n = 119) | 0.366 |
| ISS I/II/III | 44/104/132 (n = 280) | 24/49/70 (n = 143) | 20/55/62 (n = 137) | 0.700 |
| Cytogenetics normal/hyperdiploid/non-hyperdiploid ** | 130/70/64 (n = 264) | 68/33/29 (n = 130) | 62/37/35 (n = 134) | 0.604 |
| High-risk FISH | 76 (31.8) (n = 239) | 37 (29.8) (n = 126) | 39 (34.5) (n = 113) | 0.394 |
| t(4;14)/t(14;16)/del(17p) *** | 43/2/42 | 20/1/19 | 23/1/23 | 0.986 |
| Upfront Treatment | ||||
| ASCT | 124 (41.3) | 58 (38.7) | 66 (44.0) | 0.348 |
| 1st line regimen: novel agents | 284 (94.7) | 141 (94.0) | 143 (95.3) | 0.607 |
| Best response ≥ VGPR | 141 (48.6) (n = 290) | 72 (49.3) (n = 146) | 69 (47.9) (n = 144) | 0.812 |
| At Relapse | ||||
| Age (years) | 66 (36–94) | 66.5 (42–91) | 65 (36–94) | 0.078 |
| Time from diagnosis to 1st relapse (months) | 22.7 (1.1–97.0) | 23.0 (2.6–76.4) | 21.5 (1.1–97.0) | 0.288 |
| Anemia | 85 (29.8) (n = 285) | 41 (28.4) (n = 144) | 44 (31.2) (n = 141) | 0.614 |
| Hypercalcemia | 13 (5.5) (n = 235) | 6 (5.0) (n = 121) | 7 (6.1) (n = 114) | 0.692 |
| Renal insufficiency | 40 (14.1) (n = 283) | 20 (14.0) (n = 143) | 20 (14.3) (n = 140) | 0.942 |
| Bone lesions | 102 (68.0) (n = 150) | 55 (71.4) (n = 77) | 47 (64.4) (n = 73) | 0.355 |
| Extramedullary plasmacytoma | 43 (21.3) (n = 202) | 24 (25.0) (n = 96) | 19 (17.9) (n = 106) | 0.220 |
| Clinical relapse | 145 (50.5) (n = 287) | 76 (52.4) (n = 145) | 69 (48.6) (n = 142) | 0.517 |
| Salvage treatment | ||||
| ASCT | 17 (5.7) | 5 (3.3) | 12 (8.0) | 0.080 |
| 2nd line regimen: newer agents | 57 (19.0) | 29 (19.3) | 28 (18.6) | 0.883 |
| Treatment sequence: backbone change | 104 (34.7) | 53 (35.3) | 51 (34.0) | 0.808 |
| Best response ≥ VGPR | 88 (31.7) (n = 278) | 38 (26.6) (n = 143) | 50 (37.0) (n = 135) | 0.061 |
| Variables at Diagnosis | OS HR (95% CI) | p-Values | PFS HR (95% CI) | p-Values |
|---|---|---|---|---|
| Male | 1.478 (0.889–2.457) | 0.132 | 0.951 (0.655–1.380) | 0.791 |
| Heavy chain type IgG | 1.000 | 1.000 | ||
| IgA | 0.803 (0.371–1.736) | 0.577 | 1.150 (0.696–1.900) | 0.587 |
| Others | 0.966 (0.342–2.728) | 0.948 | 1.161 (0.555–2.431) | 0.692 |
| Anemia | 1.348 (0.789–2.302) | 0.274 | 1.534 (1.020–2.307) | 0.040 |
| Hypercalcemia | 1.169 (0.574–2.380) | 0.667 | 1.281 (0.761–2.158) | 0.351 |
| Renal insufficiency | 1.123 (0.640–1.970) | 0.685 | 0.819 (0.532–1.262) | 0.365 |
| Bone lesions | 1.233 (0.676–2.250) | 0.494 | 1.401 (0.878–2.236) | 0.157 |
| Extramedullary plasmacytoma | 1.561 (0.920–2.649) | 0.099 | 1.161 (0.742–1.817) | 0.513 |
| Elevated LDH | 1.131 (0.500–2.558) | 0.767 | 1.165 (0.665–2.042) | 0.593 |
| ISS I | 1.000 | 1.000 | ||
| II | 2.147 (0.812–5.675) | 0.123 | 1.464 (0.784–2.733) | 0.232 |
| III | 2.612 (1.017–6.706) | 0.046 | 1.654 (0.908–3.012) | 0.100 |
| Cytogenetics normal | 1.000 | 1.000 | ||
| hyperdiploid | 1.137 (0.596–2.170) | 0.697 | 0.892 (0.542–1.468) | 0.653 |
| non-hyperdiploid | 1.945 (1.045–3.619) | 0.036 | 1.715 (1.053–2.794) | 0.030 |
| High-risk FISH | 1.588 (0.921–2.737) | 0.096 | 1.297 (0.835–2.015) | 0.247 |
| Upfront Treatment | ||||
| ASCT | 0.907 (0.534–1.541) | 0.718 | 0.938 (0.630–1.397) | 0.753 |
| 1st line regimen: novel agents | 1.165 (0.421–3.227) | 0.769 | 1.811 (0.788–4.162) | 0.162 |
| Best response ≥ VGPR | 1.340 (0.806–2.230) | 0.259 | 0.851 (0.582–1.245) | 0.406 |
| At Relapse | ||||
| Age > median | 1.307 (0.788–2.166) | 0.300 | 1.055 (0.724–1.536) | 0.781 |
| Time to relapse > median | 0.617 (0.373–1.020) | 0.060 | 0.465 (0.317–0.681) | <0.001 |
| Relapse after Jan 2016 * | 1.310 (0.741–2.317) | 0.353 | 1.064 (0.707–1.600) | 0.767 |
| Anemia ** | 2.842 (1.667–4.846) | <0.001 | 2.182 (1.440–3.307) | <0.001 |
| Hypercalcemia | 2.397 (0.734–7.829) | 0.148 | 2.307 (0.923–5.767) | 0.074 |
| Renal insufficiency | 1.193 (0.586–2.426) | 0.627 | 0.767 (0.437–1.347) | 0.356 |
| Bone lesions | 2.341 (1.066–5.145) | 0.034 | 1.675 (0.925–3.033) | 0.089 |
| Extramedullary plasmacytoma | 1.865 (0.910–3.821) | 0.089 | 2.179 (1.285–3.694) | 0.004 |
| Clinical relapse | 3.364 (1.931–5.862) | <0.001 | 1.896 (1.289–2.789) | 0.001 |
| Salvage treatment | ||||
| ASCT | 0.411 (0.057–2.975) | 0.379 | 0.337 (0.083–1.369) | 0.128 |
| 2nd line regimen: newer agents | 0.656 (0.323–1.334) | 0.244 | 0.686 (0.403–1.167) | 0.165 |
| Treatment sequence: de-escalation | 1.000 | 1.000 | ||
| others | 0.463 (0.213–1.005) | 0.051 | 0.722 (0.380–1.371) | 0.320 |
| backbone change | 0.321 (0.137–0.754) | 0.009 | 0.440 (0.220–0.880) | 0.020 |
| Best response ≥ VGPR | 0.460 (0.243–0.869) | 0.017 | 0.447 (0.284–0.703) | <0.001 |
| Variables at Diagnosis | OS HR (95% CI) | p-Values | PFS HR (95% CI) | p-Values |
|---|---|---|---|---|
| Cytogenetics: normal | 1.000 | 1.000 | ||
| hyperdiploid | 1.232 (0.630–2.408) | 0.543 | 1.670 (0.820–3.402) | 0.158 |
| non-hyperdiploid | 2.028 (1.026–4.008) | 0.042 | 2.386 (1.203–4.732) | 0.013 |
| At relapse | ||||
| Clinical relapse | 3.431 (1.929–6.103) | <0.001 | 5.351 (2.826–10.133) | <0.001 |
| Salvage treatment | ||||
| Treatment sequence: de-escalation | 1.000 | 1.000 | ||
| others | 0.393 (0.179–0.861) | 0.020 | 0.336 (0.151–0.748) | 0.008 |
| backbone change | 0.387 (0.160–0.939) | 0.036 | 0.319 (0.127–0.806) | 0.016 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Wang, C.; Soekojo, C.Y.; Mel, S.d.; Ooi, M.; Chen, Y.; Goh, A.Z.K.; Nagarajan, C.; Chng, W.J. Natural History and Prognostic Factors at First Relapse in Multiple Myeloma. Cancers 2020, 12, 1759. https://doi.org/10.3390/cancers12071759
Wang C, Soekojo CY, Mel Sd, Ooi M, Chen Y, Goh AZK, Nagarajan C, Chng WJ. Natural History and Prognostic Factors at First Relapse in Multiple Myeloma. Cancers. 2020; 12(7):1759. https://doi.org/10.3390/cancers12071759
Chicago/Turabian StyleWang, Chen, Cinnie Yentia Soekojo, Sanjay de Mel, Melissa Ooi, Yunxin Chen, Allan Zhi Kai Goh, Chandramouli Nagarajan, and Wee Joo Chng. 2020. "Natural History and Prognostic Factors at First Relapse in Multiple Myeloma" Cancers 12, no. 7: 1759. https://doi.org/10.3390/cancers12071759
APA StyleWang, C., Soekojo, C. Y., Mel, S. d., Ooi, M., Chen, Y., Goh, A. Z. K., Nagarajan, C., & Chng, W. J. (2020). Natural History and Prognostic Factors at First Relapse in Multiple Myeloma. Cancers, 12(7), 1759. https://doi.org/10.3390/cancers12071759





