Ricinus communis Intoxications in Human and Veterinary Medicine—A Summary of Real Cases
Abstract
:1. Introduction

2. Ricin, a Toxic Lectin from Ricinus communis
3. Ricin, a Dual-Use Substance
4. Toxicity of Ricin and R. communis, Agglutinin
5. Ricinine
6. Ricin Intoxications in Humans
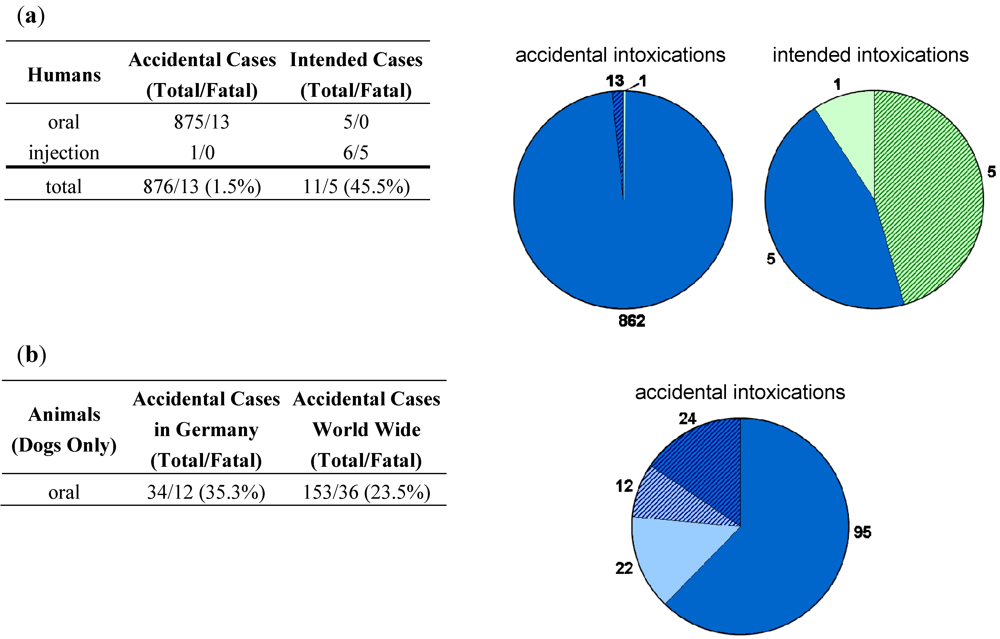
| Human Cases: Accidental | |||||
|---|---|---|---|---|---|
| Uptake/Ingestion | Outcome | Where | Detection and Diagnosis 1 | Ref. 2 | |
| 101 people (different age) | ingestion and injection of varying amounts of Ricinus communis derivates | 6 fatal | worldwide | circumstantial evidence | [33] |
| man (age 26) | in 1900 ingestion of unknown amount of castor seeds | recovered | UK | circumstantial evidence | [189] |
| juvenile (age 15) | in 1902 ingestion of 10 or 12 castor seeds | fatal | USA | circumstantial evidence | [190] |
| 4 adults (age unknown) | in 1903 ingestion of 1, 4, 6 and 14 castor seeds, respectively | recovered | Cuba | circumstantial evidence | [190] |
| man (age 50) | in 1903 ingestion of 2 castor seeds | recovered | UK | circumstantial evidence | [191] |
| man (age unknown) | in 1920 ingestion of 5 castor seeds | fatal | USA | circumstantial evidence | [192] |
| 2 women (age 22 and 41) | ingestion of 2.5-5 castor seeds for treatment of stomach convulsions | fatal | Hungary | circumstantial evidence | [193] |
| man (age unknown) | drinking of an extract made of a fistful castor seeds | fatal | Hungary | circumstantial evidence | [193] |
| man (age 24) | in 1934 ingestion of 15-20 castor seeds | fatal | Germany | circumstantial evidence | [194] |
| 4 adults (age unknown) | ingestion of 1-15 castor seeds | recovered | Austria | circumstantial evidence | [195] |
| child (age 7) | in 1941 ingestion of 4 castor seeds | recovered | Italy | circumstantial evidence | [196] |
| woman (age 60) | in 1948 ingestion of 10 castor seeds for relaxant | recovered | Brazil | circumstantial evidence | [178] |
| 2 people (age unknown) | in 1950-1952 ingestion of unknown amount of castor seeds | recovered | Italy | suspected | [197] |
| 10 children (age 11-13) | in 1958 ingestion of 0.5-6 castor seeds | recovered | Hungary | circumstantial evidence | [198] |
| man (age 42) | ingestion of 10 seeds | recovered | Poland | circumstantial evidence | [199] |
| 57 children (age 1-5, >5) | in 1962-1965 ingestion of unknown amount of castor seeds, on average 4-5 | recovered | India | circumstantial evidence | [170] |
| 443 children (age <19) | in 1964-1969 ingestion of unknown amount of castor seeds | recovered | USA | suspected | [200] |
| man (age 57) | in 1970 ingestion of unknown amount of castor seeds, which were thought to be scarlet runner beans | recovered | Netherlands | circumstantial evidence | [201] |
| 4 men (age 7-18) | ingestion of 1-2 castor seeds | recovered | India | circumstantial evidence | [202] |
| family of 4 people (age 8-44) | in 1974 ingestion of 2-10 castor seeds | recovered | Italy | circumstantial evidence | [203] |
| girl (age 17) | in 1965 ingestion of 1 castor seed | recovered | UK | circumstantial evidence | [204] |
| child (age unknown) | In the 1970s ingestion of unknown amount of castor seeds | recovered | India | circumstantial evidence | [205] |
| boy (age 4) | in 1979 ingestion of 4 castor seeds from an ornamental necklace | recovered | USA | circumstantial evidence | [171] |
| girl (age 2) | in 1979 ingestion of at least 1 castor seed | recovered | USA | circumstantial evidence | [171] |
| 7 children (age unknown) | in 1968-1970 ingestion of 1-10 castor seeds because of good taste | recovered | Croatia | circumstantial evidence | [179] |
| 7 adults (age unknown) | in 1968-1970 ingestion of 1-10 castor seeds as laxative | recovered | Croatia | circumstantial evidence | [179] |
| 2 children (ages 4 and 5) | in 1979 ingestion of unknown amount of castor seeds which were found in a canister together with walnuts | recovered | USA | circumstantial evidence | [206] |
| 4 adults (age 19-21) | ingestion of 0.5-1 castor seed | recovered | Denmark | circumstantial evidence | [207] |
| 10 children (age 6-8) | ingestion of 1-7 castor seeds and just contact, respectively | recovered | Spain | circumstantial evidence | [208] |
| 2 boys (age 17) | ingestion of 8 and 3 castor seeds | recovered | Israel | circumstantial evidence | [209] |
| 9 children (age 7 to 12) | in 1984 ingestion of 1-2 castor seeds which were taken to school | recovered | USA | circumstantial evidence | [165] |
| child (age 11) | ingestion of 1 castor seed during lesson in school | recovered | UK | circumstantial evidence | [210] |
| man (age 21) | ingestion of 12 castor seeds, which were thought to be hazelnuts | recovered | USA | circumstantial evidence | [211] |
| woman (age 80) | ingestion of unknown amount of shelled castor seeds out of ambiguous reasons | recovered | USA | circumstantial evidence | [211] |
| woman (age 52) | ingestion of 10-15 castor seeds without knowledge of its toxicity | recovered | Spain | circumstantial evidence | [212] |
| child (age 3) | ingestion of two or more castor seeds | recovered | USA | suspected | [166] |
| man (age 28) | ingestion of 4 castor seeds as treatment against constipation | recovered | USA | circumstantial evidence | [166] |
| man (age 39) | ingestion of 4 castor seeds, man declared, that he often eats roasted castor seeds | recovered | USA | circumstantial evidence | [166] |
| 28 children (age < 15) | in 1986 ingestion of unknown amount of castor seeds | recovered | Sri Lanka | suspected | [213] |
| man (age 36) | extract of 1 castor seed was injected, against migraine or out of curiosity | recovered | UK | circumstantial evidence | [174] |
| 3 patients (age unknown) | in 1966-1994 ingestion of unknown amount of castor seeds | recovered | Switzerland | circumstantial evidence | [176] |
| young adult (age unknown) | in 1995 ingestion of 10-15 castor seeds out of curiosity | recovered | Australia | circumstantial evidence | [173] |
| girl (age 20 months) | ingestion of 2 or more castor seeds | recovered | Canada | circumstantial evidence | [214] |
| 5 people (age unknown) | ingestion of unknown amount of castor seeds | recovered | Tunisia | not described | [215] |
| man (age 70) | ingestion of 10 castor seeds | recovered | Malta | circumstantial evidence | [172] |
| 120 people (different age) | in 1955 ingestion of varying amounts of castor seeds | 1 fatal | Europe | circumstantial evidence | [216] |
| child (age 3) | ingestion of 5-6 castor seeds | recovered | Germany | circumstantial evidence | [216] |
| man (age 69) | swallowing of 30 seeds without chewing; intended use: medical treatment of rheumatism, external application was recommended | recovered | Japan | circumstantial evidence | [180] |
| 46 children (age unknown) | in 1984-2001 ingestion of unknown amount of castor seeds | recovered | Sri Lanka | suspected | [169] |
| man (age 51) | ingestion of one green fruit of castor plant as treatment against cough | recovered | Oman | circumstantial evidence | [181] |
| woman (age unknown) | injection of 500 mL castor oil for hip augmentation by unlicensed practitioner | recovered | USA | detection of ricinine in urine | [182] |
| woman (age 56) | ingestion of 5 wild castor seeds as treatment against constipation | recovered | Korea | detection of ricin in urine | [177] |
| Georgi Markov (age 49) | in 1978 assassination of Markov: poking with an umbrella for injection of a pellet with channels probably containing ricin | fatal | UK | suspected | [117, 204, 206, 217, 218] |
| Vladimir Kostov | in 1978 attempted assassination of Kostov: shot in his back with an air pistol for injection of a pellet with channels probably containing ricin | recovered | France | suspected | [117] |
| man (age 21) | ingestion of 30 castor seeds in attempting suicide, only some were masticated | recovered | France | detection of ricin in plasma and urine | [219] |
| woman (age 38) | in 1985 ingestion of 24 chopped castor seeds in attempting suicide | recovered | USA | circumstantial evidence | [165] |
| woman (age 20) | ingestion of 12 castor seeds in attempting suicide | recovered | Spain | circumstantial evidence | [220] |
| adolescent (age 16) | ingestion of 2 castor seeds in attempting suicide | recovered | USA | circumstantial evidence | [221] |
| man (age 20) | subcutaneous suicidal injection of castor seed extract | fatal | Poland | suspected | [183] |
| man (age 53) | chewing of 13 castor seeds. The mastication product was injected in attempting suicide | recovered | France | circumstantial evidence | [187] |
| man (age 61) | intention: suicide, injection of a solution of crushed castor seeds | fatal | USA | detection of ricinine in urine | [184, 222] |
| man (age 56), woman (age 59) | injection of extracted ricin from castor seeds into his wife and himself | fatal | Belgium | detection of ricin in urine and syringe | [186] |
| man (age 49) | i.v. and s.c. injection of castor seed extract in attempting suicide | fatal | Belgium | detection of ricinine in blood, urine, and syringe | [185] |
| Animal cases: dogs | |||||
|---|---|---|---|---|---|
| Uptake/Ingestion | Outcome | Where | Detection and Diagnosis 1 | Ref. 2 | |
| 5 dogs | in 1977-1979 ingestion of organic fertilizer | 3 fatal | Germany | circumstantial evidence | [223] |
| 98 dogs | in 1989-2000 ingestion of unknown amount of castor seeds | 7 fatal | USA | suspected | [224] |
| 19 dogs | in 2001 ingestion of fertilizer containing castor seeds | 7 fatal | Germany | circumstantial evidence; detection of ricin in fertilizer | [225] |
| dog | in 2002 ingestion of castor seed cakes used as fertilizer | fatal | Brazil | circumstantial evidence | [226] |
| dog | in 1999 ingestion of fertilizer based on castor seeds | recovered | Brazil | circumstantial evidence | [227] |
| dog | in 1999 ingestion of motor oil based on castor oil | recovered | Brazil | circumstantial evidence | [227] |
| 35 dogs | in 2001-2003; details of intoxication not described | not described | USA | suspected | [188] |
| puppy | ingestion of unknown amount of castor beans | fatal | USA | detection of ricinine in stomach content | [228] |
| dog | ingestion of unknown amount of castor beans | recovered | Germany | circumstantial evidence | [229] |
| 2 dogs | ingestion of fertilizer composed of R. communis material | fatal | Belgium | detection of ricinine in gastric and intestinal content , liver and kidney | [230] |
| 15 dogs | in 2007 ingestion of soil conditioner with 10 % oil cake | 13 fatal | Korea | suspected | [231] |
| 9 dogs | in 2010, ingestion of fertilizer containing R. communis | 2 fatal | Germany | detection of ricinine in urine and ricin in fertilizer and soil | this paper |
| different farm animals, mostly cows | in 1873 ingestion of flaxseed flour contaminated with castor seeds | recovered | Germany | circumstantial evidence | [232] |
| 35 horses | in 1888 ingestion of flaxseed flour contaminated with castor seeds | 1 fatal | Germany | circumstantial evidence | [233] |
| 70 different animals | in 1950 ingestion of layers’ mash containing castor seed husks in meal | fatal 2 pigs, 1 heifer, 2 cattle | Ireland | circumstantial evidence | [234] |
| several 1000 ducks | in 1969-1971 ingestion of unknown amount of castor seeds | fatal for at least 10 ducks | USA | circumstantial evidence | [235] |
| 1 horse | in 1999 ingestion and aspiration of ~2 L filtrate made of crushed castor seeds mixed with water | fatal | Brazil | suspected | [236] |
| 45 sheep and goats | in 2005 ingestion of garden waste containing castor beans | fatal for 15 animals | Iran | circumstantial evidence | [237] |
7. Ricin Intoxications in Animals
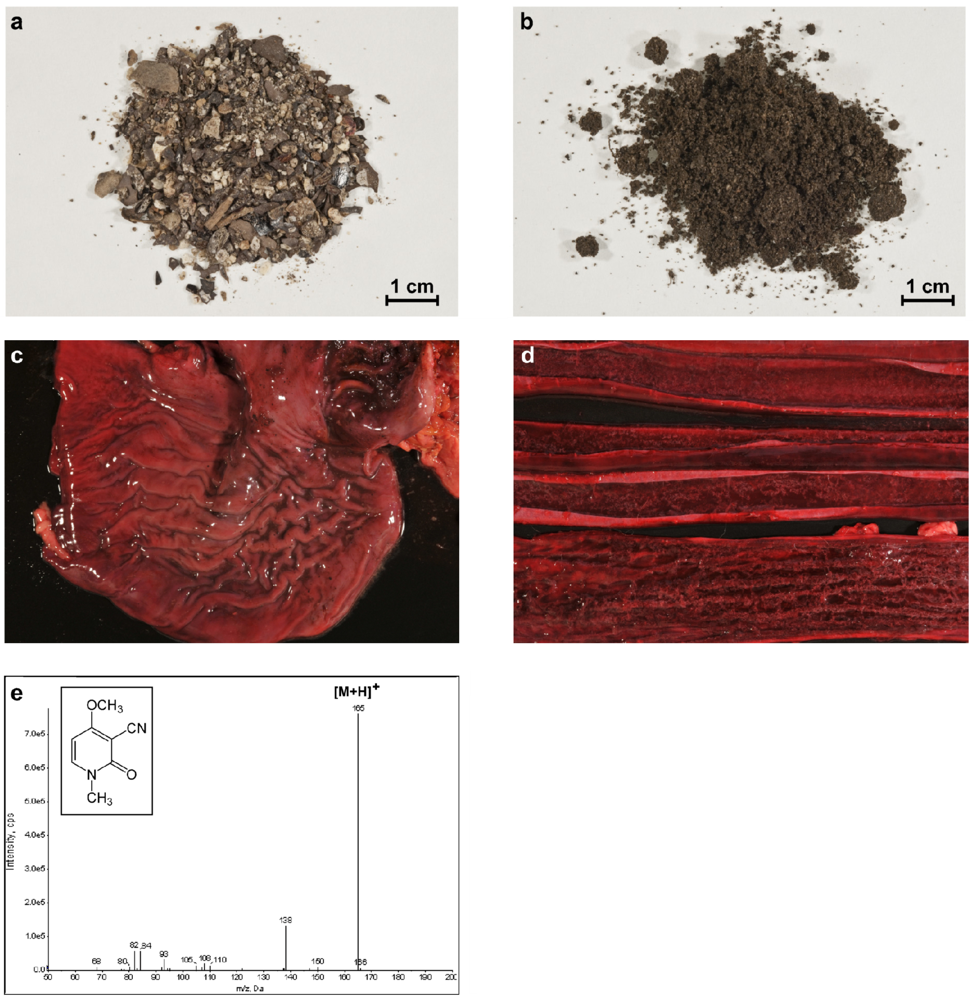
8. Detection of Ricin or Ricinus communis
9. Treatment and Vaccination
10. Conclusion
Acknowledgments
Conflict of Interest
References
- Scarpa, A.; Guerci, A. Various uses of the castor oil plant (Ricinus communis L.). A review. J. Ethnopharmacol. 1982, 5, 117–137. [Google Scholar] [CrossRef] [PubMed]
- Serpico, M.; White, R. Oil, Fat and Wax. In Ancient Egyptian Materials and Technology; Nicholson, P.T., Shaw, I., Eds.; Cambridge University Press: Cambridge, UK, 2000; pp. 390–428. [Google Scholar]
- Weiss, E.A. Oilseed Crops, 2nd ed; Blackwell Science Ltd.: Oxford, UK, 2000. [Google Scholar]
- Ogunniyi, D.S. Castor oil: A vital industrial raw material. Bioresour. Technol. 2006, 97, 1086–1091. [Google Scholar]
- Mutlu, H.; Meier, M.A.R. Castor oil as a renewable resource for the chemical industry. Eur. J. Lipid Sci. Technol. 2010, 112, 10–30. [Google Scholar]
- Parkouda, C.; Nielsen, D.S.; Azokpota, P.; Ouoba, L.I.I.; Amoa-Awua, W.K.; Thorsen, L.; Hounhouigan, J.D.; Jensen, J.S.; Tano-Debrah, K.; Diawara, B.; et al. The microbiology of alkaline-fermentation of indigenous seeds used as food condiments in Africa and Asia. Crit. Rev. Microbiol. 2009, 35, 139–156. [Google Scholar] [CrossRef] [PubMed]
- Odunfa, S.A. Microbiological and toxicological aspects of fermentation of castor oil seeds for ogiri production. J. Food Sci. 1985, 50, 1758–1759. [Google Scholar]
- De Lima da Silva, N.; Maciel, M.; Batistella, C.; Filho, R. Optimization of biodiesel production from castor oil. Appl. Biochem. Biotechnol. 2006, 130, 405–414. [Google Scholar]
- Berman, P.; Nizri, S.; Wiesman, Z. Castor oil biodiesel and its blends as alternative fuel. Biomass Bioenerg. 2011, 35, 2861–2866. [Google Scholar]
- Behl, C.R.; Pande, M.B.; Pande, D.P.; Radadia, M.S. Nutritive value of matured wilted castor (Ricinus communis Linn.) leaves for crossbred sheep. Indian J. Anim. Sci. 1986, 56, 473–474. [Google Scholar]
- Robb, J.G.; Laben, R.C.; Walker, H.G., Jr.; Herring, V. Castor meal in dairy rations. J. Dairy Sci. 1974, 57, 443–450. [Google Scholar]
- Gowda, N.K.S.; Pal, D.T.; Bellur, S.R.; Bharadwaj, U.; Sridhar, M.; Satyanarayana, M.L.; Prasad, C.S.; Ramachandra, K.S.; Sampath, K.T. Evaluation of castor (Ricinus communis) seed cake in the total mixed ration for sheep. J. Sci. Food Agric. 2009, 89, 216–220. [Google Scholar]
- Balogun, J.K.; Auta, J.; Abdullahi, S.A.; Agboola, O.E. Potentials of Castor Seed Meal (Ricinus communis L.) as Feed Ingredient for Oreochromis Niloticus. In Proceedings of the 19th Annual Conference Fisheries Society Nigeria, Ilorin, Nigeria, 29 November-3 December 2004; pp. 838–843.
- Diniz, L.L.; Valadares Filho, S.C.; de Oliveira, A.S.; Pina, D.S.; de Lima da Silva, N.; Benedeti, P.B.; Baião, G.F.; Campos, J.M.S.; Valadares, R.F.D. Castor bean meal for cattle finishing: 1-nutritional parameters. Livest. Sci. 2011, 135, 153–167. [Google Scholar]
- Vilhjalmsdottir, L.; Fisher, H. Castor bean meal as a protein source for chickens: Detoxification and determination of limiting amino acids. J. Nutr. 1971, 101, 1185–1192. [Google Scholar]
- Ani, A.O. Effects of graded levels of dehulled and cooked castor oil bean (Ricinus communis L.) meal and supplementary L-lysine on performance of broiler finishers. J. Trop. Agric. Food Environ. Ext. 2007, 6, 89–97. [Google Scholar]
- Tangl, H. On the feeding value of extracted castor-oil meal. Kiserletuegyi Koezlemenyek 1939, 41, 69–72. [Google Scholar]
- Alexander, J.; Benford, D.; Cockburn, A.; Cravedi, J.P.; Dogliotti, E.; di Domenico, A.; Férnandez-Cruz, M.L.; Fürst, P.; Fink-Gremmels, J.; Galli, C.L.; et al. Scientific opinion of the panel on contaminants in the food chain on a request from the European commision on ricin (from Ricinus communis) as undesirable substances in animal feed. EFSA J. 2008, 726, 1–38. [Google Scholar]
- Barnes, D.J.; Baldwin, B.S.; Braasch, D.A. Degradation of ricin in castor seed meal by temperature and chemical treatment. Ind. Crops Prod. 2009, 29, 509–515. [Google Scholar]
- Gupta, A.P.; Antil, R.S.; Narwal, R.P. Utilization of deoiled castor cake for crop production. Arch. Agron. Soil Sci. 2004, 50, 389–395. [Google Scholar]
- Lima, R.L.S.; Severino, L.S.; Sampaio, L.R.; Sofiatti, V.; Gomes, J.A.; Beltrão, N.E.M. Blends of castor meal and castor husks for optimized use as organic fertilizer. Ind. Crops Prod. 2011, 33, 364–368. [Google Scholar]
- Final report on the safety assessment of Ricinus communis (castor) seed oil, hydrogenated castor oil, glyceryl ricinoleate, glyceryl ricinoleate se, ricinoleic acid, potassium ricinoleate, sodium ricinoleate, zinc ricinoleate, cetyl ricinoleate, ethyl ricinoleate, glycol ricinoleate, isopropyl ricinoleate, methyl ricinoleate, and octyldodecyl ricinoleate. Int. J. Toxicol. 2007, 26, 31–77. [CrossRef]
- Anandan, S.; Kumar, G.K.A.; Ghosh, J.; Ramachandra, K.S. Effect of different physical and chemical treatments on detoxification of ricin in castor cake. Anim. Feed Sci. Technol. 2005, 120, 159–168. [Google Scholar]
- Gandhi, V.; Cherian, K.; Mulky, M. Detoxification of castor seed meal by interaction with sal seed meal. J. Am. Oil Chem. Soc. 1994, 71, 827–831. [Google Scholar]
- Puttaraj, S.; Bhagya, S.; Murthy, K.N.; Singh, N. Effect of detoxification of castor seed (Ricinus communis) protein isolate on its nutritional quality. Plant Food Hum. Nutr. 1994, 46, 63–70. [Google Scholar]
- Melo, W.C.; dos Santos, A.S.; Santa Anna, L.M.M.; Pereira, N., Jr. Acid and enzymatic hydrolysis of the residue from castor bean (Ricinus communis L.) oil extraction for ethanol production: Detoxification and biodiesel process integration. J. Braz. Chem. Soc. 2008, 19, 418–425. [Google Scholar] [CrossRef]
- De Oliveira, A.S.; Campos, J.M.S.; Oliveira, M.R.C.; Brito, A.F.; Filho, S.C.V.; Detmann, E.; Valadares, R.F.D.; de Souza, S.M.; Machado, O.L.T. Nutrient digestibility, nitrogen metabolism and hepatic function of sheep fed diets containing solvent or expeller castor seed meal treated with calcium hydroxide. Anim. Feed Sci. Technol. 2010, 158, 15–28. [Google Scholar]
- Auld, D.L.; Rolfe, R.D.; McKeon, T.A. Development of castor with reduced toxicity. J. New Seeds 2001, 3, 61–69. [Google Scholar]
- Knapp, O. Versuche zur Züchtung einer giftfreien Ricinussorte. Theor. Appl. Genet. 1943, 15, 97–100. [Google Scholar]
- Lowery, C.C.; Auld, D.L.; Rolfe, R.; McKeon, T.A.; Goodrum, J. Barriers to Commercialization of a Castor Cultivar with Reduced Concentration of Ricin. In Issues in New Crops and New Uses; Janick, J., Whipkey, A., Eds.; ASHS Press: Alexandria, VA, USA, 2002; pp. 97–100. [Google Scholar]
- Auld, D.L.; Pinkerton, S.D.; Boroda, E.; Lombard, K.A.; Murphy, C.K.; Kenworthy, K.E.; Becker, W.D.; Rolfe, R.D.; Ghetie, V. Registration of TTU-LRC castor germplasm with reduced levels of ricin and RCA120. Crop Sci. 2003, 43, 746–747. [Google Scholar]
- Kobert, R. Lehrbuch der Intoxikationen; Ferdinand Enke: Stuttgart, Germany, 1906. [Google Scholar]
- Stillmark, H. Ueber Ricin, ein giftiges Fragment aus den Samen von Ricinus comm. L und einigen anderen Euphorbiaceen; Kaiserliche Universität zu Dorpat: Tartu, Estonia, 1888. [Google Scholar]
- Bradberry, S.M.; Dickers, K.J.; Rice, P.; Griffiths, G.D.; Vale, J.A. Ricin poisoning. Toxicol. Rev. 2003, 22, 65–70. [Google Scholar]
- Endo, Y.; Mitsui, K.; Motizuki, M.; Tsurugi, K. The mechanism of action of ricin and related toxic lectins on eukaryotic ribosomes. The site and the characteristics of the modification in 28S ribosomal RNA caused by the toxins. J. Biol. Chem. 1987, 262, 5908–5912. [Google Scholar] [PubMed]
- Endo, Y.; Tsurugi, K. RNA N-glycosidase activity of ricin A-chain. Mechanism of action of the toxic lectin ricin on eukaryotic ribosomes. J. Biol. Chem. 1987, 262, 8128–8130. [Google Scholar] [PubMed]
- Lord, J.M.; Spooner, R.A. Ricin trafficking in plant and mammalian cells. Toxins 2011, 3, 787–801. [Google Scholar]
- Lappi, D.A.; Kapmeyer, W.; Beglau, J.M.; Kaplan, N.O. The disulfide bond connecting the chains of ricin. Proc. Natl. Acad. Sci. USA 1978, 75, 1096–1100. [Google Scholar]
- Baenziger, J.U.; Fiete, D. Structural determinants of Ricinus communis agglutinin and toxin specificity for oligosaccharides. J. Biol. Chem. 1979, 254, 9795–9799. [Google Scholar]
- Sandvig, K.; van Deurs, B. Endocytosis and intracellular transport of ricin: Recent discoveries. FEBS Lett. 1999, 452, 67–70. [Google Scholar]
- Olsnes, S.; Saltvedt, E.; Pihl, A. Isolation and comparison of galactose-binding lectins from Abrus precatorius and Ricinus communis. J. Biol. Chem. 1974, 249, 803–810. [Google Scholar]
- Olsnes, S.; Pihl, A. Different biological properties of the two constituent peptide chains of ricin, a toxic protein inhibiting protein synthesis. Biochemistry 1973, 12, 3121–3126. [Google Scholar]
- Lin, T.T.S.; Li, S.S.L. Purification and physicochemical properties of ricins and agglutinins from Ricinus communis. Eur. J. Biochem. 1980, 105, 453–459. [Google Scholar]
- Nicolson, G.L.; Blaustein, J. The interaction of Ricinus communis agglutinin with normal and tumor cell surfaces. Biochim. Biophys. Acta Biomembr. 1972, 266, 543–547. [Google Scholar]
- Tomita, M.; Kurokawa, T.; Onozaki, K.; Ichiki, N.; Osawa, T.; Ukita, T. Purification of galactose-binding phytoagglutinins and phytotoxin by affinity column chromatography using sepharose. Cell Mol. Life Sci. 1972, 28, 84–85. [Google Scholar]
- Roberts, L.M.; Lamb, F.I.; Pappin, D.J.; Lord, J.M. The primary sequence of Ricinus communis agglutinin. Comparison with ricin. J. Biol. Chem. 1985, 260, 15682–15686. [Google Scholar] [PubMed]
- Araki, T.; Funatsu, G. The complete amino acid sequence of the B-chain of ricin E isolated from small-grain castor bean seeds. Ricin E is a gene recombination product of ricin D and Ricinus communis agglutinin. Biochim. Biophys. Acta 1987, 911, 191–200. [Google Scholar] [CrossRef] [PubMed]
- Ladin, B.F.; Murray, E.E.; Halling, A.C.; Halling, K.C.; Tilakaratne, N.; Long, G.L.; Houston, L.L.; Weaver, R.F. Characterization of a cDNA encoding ricin E, a hybrid ricin-Ricinus communis agglutinin gene from the castor plant Ricinus communis. Plant Mol. Biol. 1987, 9, 287–295. [Google Scholar]
- Mise, T.; Funatsu, G.; Ishiguro, M.; Funatsu, M. Isolation and characterization of ricin E from castor beans. Agric. Biol. Chem. 1977, 41, 2041–2046. [Google Scholar]
- Lord, J.; Roberts, L.; Robertus, J. Ricin: Structure, mode of action, and some current application. FASEB J. 1994, 8, 201–208. [Google Scholar]
- Sweeney, E.C.; Tonevitsky, A.G.; Temiakov, D.E.; Agapov, I.I.; Saward, S.; Palmer, R.A. Preliminary crystallographic characterization of ricin agglutinin. Proteins Struct. Funct. Bioinf. 1997, 28, 586–589. [Google Scholar]
- Brandt, N.N.; Chikishev, A.Y.; Sotnikov, A.I.; Savochkina, Y.A.; Agapov, I.I.; Tonevitskii, A.G.; Kirpichnikov, M.P. Conformational difference between ricin and ricin agglutinin in solution and crystal. Dokl. Biochem. Biophys. 2001, 376, 26–28. [Google Scholar]
- Saltvedt, E. Structure and toxicity of pure ricinus agglutinin. Biochim. Biophys. Acta 1976, 451, 536–548. [Google Scholar]
- Cawley, D.B.; Hedblom, M.L.; Houston, L.L. Homology between ricin and Ricinus communis agglutinin: Amino terminal sequence analysis and protein synthesis inhibition studies. Arch. Biochem. Biophys. 1978, 190, 744–755. [Google Scholar]
- Olsnes, S.; Fernandez-Puentes, C.; Carrasco, L.; Vazquez, D. Ribosome inactivation by the toxic lectins abrin and ricin. Eur. J. Biochem. 1975, 60, 281–288. [Google Scholar]
- Zhan, J.; Zhou, P. A simplified method to evaluate the acute toxicity of ricin and ricinus agglutinin. Toxicology 2003, 186, 119–123. [Google Scholar]
- Lord, J.M.; Harley, S.M. Ricinus communis agglutinin B chain contains a fucosylated oligosaccharide side chain not present on ricin B chain. FEBS Lett. 1985, 189, 72–76. [Google Scholar]
- Sandvig, K.; Torgersen, M.L.; Engedal, N.; Skotland, T.; Iversen, T.-G. Protein toxins from plants and bacteria: Probes for intracellular transport and tools in medicine. FEBS Lett. 2010, 584, 2626–2634. [Google Scholar]
- Sandvig, K.; van Deurs, B. Membrane traffic exploited by protein toxins. Annu. Rev. Cell Dev. Biol. 2002, 18, 1–24. [Google Scholar]
- Lord, J.M.; Roberts, L.M.; Lencer, W.I. Entry of protein toxins into mammalian cells by crossing the endoplasmic reticulum membrane: Co-opting basic mechanisms of endoplasmic reticulum-associated degradation. Curr. Top. Microbiol. Immunol. 2006, 300, 149–168. [Google Scholar]
- Spooner, R.A.; Smith, D.C.; Easton, A.J.; Roberts, L.M.; Lord, J.M. Retrograde transport pathways utilised by viruses and protein toxins. Virol. J. 2006, 3, 26–35. [Google Scholar]
- Moya, M.; Dautry-Varsat, A.; Goud, B.; Louvard, D.; Boquet, P. Inhibition of coated pit formation in HEp2 cells blocks the cytotoxicity of diphtheria toxin but not that of ricin toxin. J. Cell Biol. 1985, 101, 548–559. [Google Scholar]
- Shurety, W.; Bright, N.A.; Luzio, J.P. The effects of cytochalasin D and phorbol myristate acetate on the apical endocytosis of ricin in polarised Caco-2 cells. J. Cell Sci. 1996, 109, 2927–2935. [Google Scholar]
- Iversen, T.-G.; Skretting, G.; Llorente, A.; Nicoziani, P.; van Deurs, B.; Sandvig, K. Endosome to Golgi transport of ricin is independent of clathrin and of the Rab9- and Rab11-GTPases. Mol. Biol. Cell 2001, 12, 2099–2107. [Google Scholar]
- Llorente, A.; Rapak, A.; Schmid, S.L.; van Deurs, B.; Sandvig, K. Expression of mutant dynamin inhibits toxicity and transport of endocytosed ricin to the Golgi apparatus. J. Cell Biol. 1998, 140, 553–563. [Google Scholar]
- Jackman, M.R.; Shurety, W.; Ellis, J.A.; Luzio, J.P. Inhibition of apical but not basolateral endocytosis of ricin and folate in Caco-2 cells by cytochalasin D. J. Cell Sci. 1994, 107, 2547–2556. [Google Scholar]
- Jackman, M.R.; Ellis, J.A.; Gray, S.R.; Shurety, W.; Luzio, J.P. Cell polarization is required for ricin sensitivity in a Caco-2 cell line selected for ricin resistance. Biochem. J. 1999, 341, 323–327. [Google Scholar]
- Van Deurs, B.; Sandvig, K.; Petersen, O.; Olsnes, S.; Simons, K.; Griffiths, G. Estimation of the amount of internalized ricin that reaches the trans-Golgi network. J. Cell Biol. 1988, 106, 253–267. [Google Scholar]
- van Deurs, B.; Tønnessen, T.I.; Petersen, O.W.; Sandvig, K.; Olsnes, S. Routing of internalized ricin and ricin conjugates to the Golgi complex. J. Cell Biol. 1986, 102, 37–47. [Google Scholar]
- Grimmer, S.; Iversen, T.-G.; van Deurs, B.; Sandvig, K. Endosome to Golgi transport of ricin is regulated by cholesterol. Mol. Biol. Cell 2000, 11, 4205–4216. [Google Scholar]
- Lauvrak, S.U.; Llorente, A.; Iversen, T.-G.; Sandvig, K. Selective regulation of the Rab9-independent transport of ricin to the Golgi apparatus by calcium. J. Cell Sci. 2002, 115, 3449–3456. [Google Scholar]
- Tjelle, T.E.; Brech, A.; Juvet, L.K.; Griffiths, G.; Berg, T. Isolation and characterization of early endosomes, late endosomes and terminal lysosomes: Their role in protein degradation. J. Cell Sci. 1996, 109, 2905–2914. [Google Scholar]
- Dang, H.; Klokk, T.I.; Schaheen, B.; McLaughlin, B.M.; Thomas, A.J.; Durns, T.A.; Bitler, B.G.; Sandvig, K.; Fares, H. Derlin-dependent retrograde transport from endosomes to the Golgi apparatus. Traffic 2011, 12, 1417–1431. [Google Scholar]
- Llorente, A.; Lauvrak, S.U.; van Deurs, B.; Sandvig, K. Induction of direct endosome to endoplasmic reticulum transport in chinese hamster ovary (CHO) cells (LDLF) with a temperature-sensitive defect in ε-coatomer protein (ε-Cop). J. Biol. Chem. 2003, 278, 35850–35855. [Google Scholar]
- Amessou, M.; Fradagrada, A.; Falguières, T.; Lord, J.M.; Smith, D.C.; Roberts, L.M.; Lamaze, C.; Johannes, L. Syntaxin 16 and syntaxin 5 are required for efficient retrograde transport of several exogenous and endogenous cargo proteins. J. Cell Sci. 2007, 120, 1457–1468. [Google Scholar]
- Rapak, A.; Falnes, P.O.; Olsnes, S. Retrograde transport of mutant ricin to the endoplasmic reticulum with subsequent translocation to cytosol. Proc. Natl. Acad. Sci. USA 1997, 94, 3783–3788. [Google Scholar]
- Majoul, I.; Sohn, K.; Wieland, F.T.; Pepperkok, R.; Pizza, M.; Hillemann, J.; Söling, H.-D. KDEL receptor (Erd2p)-mediated retrograde transport of the cholera toxin A subunit from the Golgi involves Copi, p23, and the COOH terminus of Erd2. J. Cell Biol. 1998, 143, 601–612. [Google Scholar]
- Lee, M.C.S.; Miller, E.A.; Goldberg, J.; Orci, L.; Schekman, R. Bi-directional protein transport between the ER and Golgi. Annu. Rev. Cell Dev. Biol. 2004, 20, 87–123. [Google Scholar]
- Spooner, R.A.; Watson, P.D.; Marsden, C.J.; Smith, D.C.; Moore, K.A.H.; Cook, J.P.; Lord, J.M.; Roberts, L.M. Protein disulphide-isomerase reduces ricin to its A and B chains in the endoplasmic reticulum. Biochem. J. 2004, 383, 285–293. [Google Scholar]
- Bellisola, G.; Fracasso, G.; Ippoliti, R.; Menestrina, G.; Rosén, A.; Soldà, S.; Udali, S.; Tomazzolli, R.; Tridente, G.; Colombatti, M. Reductive activation of ricin and ricin A-chain immunotoxins by protein disulfide isomerase and thioredoxin reductase. Biochem. Pharmacol. 2004, 67, 1721–1731. [Google Scholar]
- Deeks, E.D.; Cook, J.P.; Day, P.J.; Smith, D.C.; Roberts, L.M.; Lord, J.M. The low lysine content of ricin A chain reduces the risk of proteolytic degradation after translocation from the endoplasmic reticulum to the cytosol. Biochemistry 2002, 41, 3405–3413. [Google Scholar]
- Di Cola, A.; Frigerio, L.; Lord, J.M.; Ceriotti, A.; Roberts, L.M. Ricin A chain without its partner B chain is degraded after retrotranslocation from the endoplasmic reticulum to the cytosol in plant cells. Proc. Natl. Acad. Sci. USA 2001, 98, 14726–14731. [Google Scholar]
- Li, S.; Spooner, R.A.; Allen, S.C.H.; Guise, C.P.; Ladds, G.; Schnoder, T.; Schmitt, M.J.; Lord, J.M.; Roberts, L.M. Folding-competent and folding-defective forms of ricin A chain have different fates after retrotranslocation from the endoplasmic reticulum. Mol. Biol. Cell 2010, 21, 2543–2554. [Google Scholar]
- Meusser, B.; Hirsch, C.; Jarosch, E.; Sommer, T. ERAD: The long road to destruction. Nat. Cell Biol. 2005, 7, 766–772. [Google Scholar]
- Simpson, J.C.; Roberts, L.M.; Romisch, K.; Davey, J.; Wolf, D.H.; Lord, J.M. Ricin A chain utilises the endoplasmic reticulum-associated protein degradation pathway to enter the cytosol of yeast. FEBS Lett. 1999, 459, 80–84. [Google Scholar]
- Słomińska-Wojewódzka, M.; Gregers, T.F.; Wälchli, S.; Sandvig, K. EDEM is involved in retrotranslocation of ricin from the endoplasmic reticulum to the cytosol. Mol. Biol. Cell 2006, 17, 1664–1675. [Google Scholar]
- Sokołowska, I.; Wälchli, S.; Węgrzyn, G.; Sandvig, K.; Słomińska-Wojewódzka, M. A single point mutation in ricin A-chain increases toxin degradation and inhibits EDEM1-dependent ER retrotranslocation. Biochem. J. 2011, 436, 371–385. [Google Scholar]
- Spooner, R.A.; Hart, P.J.; Cook, J.P.; Pietroni, P.; Rogon, C.; Höhfeld, J.; Roberts, L.M.; Lord, J.M. Cytosolic chaperones influence the fate of a toxin dislocated from the endoplasmic reticulum. Proc. Natl. Acad. Sci. USA 2008, 105, 17408–17413. [Google Scholar]
- Chiou, J.-C.; Li, X.-P.; Remacha, M.; Ballesta, J.P.G.; Tumer, N.E. The ribosomal stalk is required for ribosome binding, depurination of the rRNA and cytotoxicity of ricin A chain in Saccharomyces cerevisiae. Mol. Microbiol. 2008, 70, 1441–1452. [Google Scholar]
- Lord, M.J.; Jolliffe, N.A.; Marsden, C.J.; Pateman, C.S.C.; Smith, D.C.; Spooner, R.A.; Watson, P.D.; Roberts, L.M. Ricin: Mechanisms of cytotoxicity. Toxicol. Rev. 2003, 22, 53–64. [Google Scholar]
- Dai, J.; Zhao, L.; Yang, H.; Guo, H.; Fan, K.; Wang, H.; Qian, W.; Zhang, D.; Li, B.; Wang, H.; et al. Identification of a novel functional domain of ricin responsible for its potent toxicity. J. Biol. Chem. 2011, 286, 12166–12171. [Google Scholar] [PubMed]
- Jetzt, A.E.; Cheng, J.-S.; Tumer, N.E.; Cohick, W.S. Ricin A-chain requires c-Jun N-terminal kinase to induce apoptosis in nontransformed epithelial cells. Int. J. Biochem. Cell Biol. 2009, 41, 2503–2510. [Google Scholar]
- Sestili, P.; Alfieri, R.; Carnicelli, D.; Martinelli, C.; Barbieri, L.; Stirpe, F.; Bonelli, M.; Petronini, P.G.; Brigotti, M. Shiga toxin 1 and ricin inhibit the repair of H2O2-induced DNA single strand breaks in cultured mammalian cells. DNA Repair 2005, 4, 271–277. [Google Scholar]
- Li, X.-P.; Baricevic, M.; Saidasan, H.; Tumer, N.E. Ribosome depurination is not sufficient for ricin-mediated cell death in Saccharomyces cerevisiae. Infect. Immun. 2007, 75, 417–428. [Google Scholar]
- Horrix, C.; Raviv, Z.; Flescher, E.; Voss, C.; Berger, M. Plant ribosome-inactivating proteins type II induce the unfolded protein response in human cancer cells. Cell Mol. Life Sci. 2011, 68, 1269–1281. [Google Scholar]
- Alford, S.C.; Pearson, J.; Carette, A.; Ingham, R.; Howard, P. Alpha-sarcin catalytic activity is not required for cytotoxicity. BMC Biochem. 2009, 10, 9–19. [Google Scholar]
- Morlon-Guyot, J.; Helmy, M.; Lombard-Frasca, S.; Pignol, D.; Pieroni, G.; Beaumelle, B. Identification of the ricin lipase site and implication in cytotoxicity. J. Biol. Chem. 2003, 278, 17006–17011. [Google Scholar]
- Nielsen, K.; Boston, R.S. Ribosome-inactiating proteins: A plant perspective. Annu. Rev. Plant Physiol. Plant Mol. Biol. 2001, 52, 785–816. [Google Scholar]
- Rüdiger, H.; Gabius, H.-J. Plant lectins: Occurrence, biochemistry, functions and application. Glycoconj. J. 2001, 18, 589–613. [Google Scholar]
- Van Dammes, E.J.M.; Hao, Q.; Chen, Y.; Barre, A.; Vandenbussche, F.; Desmyter, S.; Rougé, P.; Peumans, W.J. Ribosome-inactivating proteins: A family of plant proteins that do more than inactivate ribosomes. Crit. Rev. Plant Sci. 2001, 20, 395–465. [Google Scholar]
- Van Dammes, E.J.M.; Fouquaert, E.; Lannoo, N.; Vandenborre, G.; Schouppe, D.; Peumans, W.J. Novel concepts about the role of lectins in the plant cell. Adv. Exp. Med. Biol. 2011, 705, 271–294. [Google Scholar]
- Strebhardt, K.; Ullrich, A. Paul Ehrlich’s magic bullet concept: 100 years of progress. Nat. Rev. Cancer 2008, 8, 473–480. [Google Scholar]
- Zhou, X.-X.; Ji, F.; Zhao, J.-L.; Cheng, L.-F.; Xu, C.-F. Anti-cancer activity of anti-p185Her-2 ricin A chain immunotoxin on gastric cancer cells. J. Gastroenterol. Hepatol. 2010, 25, 1266–1275. [Google Scholar]
- Spitler, L.E.; del Rio, M.; Khentigan, A.; Wedel, N.I.; Brophy, N.A.; Miller, L.L.; Harkonen, W.S.; Rosendorf, L.L.; Lee, H.M.; Mischak, R.P.; et al. Therapy of patients with malignant melanoma using a monoclonal antimelanoma antibody-ricin A chain immunotoxin. Cancer Res. 1987, 47, 1717–1723. [Google Scholar] [PubMed]
- Frankel, A.E.; Woo, J.-H.; Neville, D.M. Principles of Cancer Biotherapy, 5th ed; Springer Netherlands: Dodrecht, the Netherlands, 2009. [Google Scholar]
- Schindler, J.; Gajavelli, S.; Ravandi, F.; Shen, Y.; Parekh, S.; Braunchweig, I.; Barta, S.; Ghetie, V.; Vitetta, E.; Verma, A. A phase I study of a combination of anti-CD19 and anti-CD22 immunotoxins (combotox) in adult patients with refractory B-lineage acute lymphoblastic leukaemia. Br. J. Haematol. 2011, 1–6. [Google Scholar]
- Wu, A.M.; Senter, P.D. Arming antibodies: Prospects and challenges for immunoconjugates. Nat. Biotechnol. 2005, 23, 1137–1146. [Google Scholar]
- Vitetta, E.S.; Thorpe, P.E.; Uhr, J.W. Immunotoxins: Magic bullets or misguided missiles? Trends Pharmacol. Sci. 1993, 14, 148–154. [Google Scholar]
- Baluna, R.; Vitetta, E.S. Vascular leak syndrome: A side effect of immunotherapy. Immunopharmacology 1997, 37, 117–132. [Google Scholar]
- Furman, R.R.; Grossbard, M.L.; Johnson, J.L.; Pecora, A.L.; Cassileth, P.A.; Jung, S.-H.; Peterson, B.A.; Nadler, L.M.; Freedman, A.; Bayer, R.-L.; et al. A phase III study of anti-B4-blocked ricin as adjuvant therapy post-autologous bone marrow transplant: CALGB 9254. Leuk. Lymphoma 2011, 52, 587–596. [Google Scholar]
- Audi, J.; Belson, M.; Patel, M.; Schier, J.; Osterloh, J. Ricin poisoning: A comprehensive review. J. Am. Med. Assoc. 2005, 294, 2342–2351. [Google Scholar]
- Franz, D.R.; Jaax, N.K. Ricin Toxin. In Medical Aspects of Chemical and Biological Warfare; Sidell, F.R., Takafuji, E.T., Franz, D.R., Eds.; TMM Publications: Washington, DC, USA, 1997; pp. 631–642. [Google Scholar]
- Zilinskas, R.A. Iraq’s biological weapons. J. Am. Med. Assoc. 1997, 278, 418–424. [Google Scholar]
- Kirby, R. Ricin toxin: A military history. CML Army Chem. Rev. 2004, PB 3-04, 38–40. [Google Scholar]
- Schieltz, D.M.; McGrath, S.C.; McWilliams, L.G.; Rees, J.; Bowen, M.D.; Kools, J.J.; Dauphin, L.A.; Gomez-Saladin, E.; Newton, B.N.; Stang, H.L.; et al. Analysis of active ricin and castor bean proteins in a ricin preparation, castor bean extract, and surface swabs from a public health investigation. Forensic. Sci. Int. 2011, 209, 70–79. [Google Scholar] [CrossRef] [PubMed]
- Moran, G.J. Threats in bioterrorism. II: CDC category B and C agents. Emerg. Med. Clin. North Am. 2002, 20, 311–330. [Google Scholar] [CrossRef] [PubMed]
- Crompton, R.; Gall, D. Georgi Markov-death in a pellet. Med. Leg. J. 1980, 48, 51–62. [Google Scholar]
- Despeyroux, D.; Walker, N.; Pearce, M.; Fisher, M.; McDonnell, M.; Bailey, S.C.; Griffiths, G.D.; Watts, P. Characterization of ricin heterogeneity by electrospray mass spectrometry, capillary electrophoresis, and resonant mirror. Anal. Biochem. 2000, 279, 23–36. [Google Scholar] [PubMed]
- Thullier, P.; Griffiths, G. Broad recognition of ricin toxins prepared from a range of Ricinus cultivars using immunochromatographic tests. Clin. Toxicol. (Phila.) 2009, 47, 643–650. [Google Scholar] [CrossRef] [PubMed]
- Ishiguro, M.; Tomi, M.; Funatsu, G.; Funatsu, M. Isolation and chemical properties of a ricin variant from castor bean. Toxicon 1976, 14, 157–164. [Google Scholar]
- Leshin, J.; Danielsen, M.; Credle, J.J.; Weeks, A.; O’Connell, K.P.; Dretchen, K. Characterization of ricin toxin family members from Ricinus communis. Toxicon 2010, 55, 658–661. [Google Scholar]
- Chan, A.P.; Crabtree, J.; Zhao, Q.; Lorenzi, H.; Orvis, J.; Puiu, D.; Melake-Berhan, A.; Jones, K.M.; Redman, J.; Chen, G.; et al. Draft genome sequence of the oilseed species Ricinus communis. Nat. Biotechnol. 2010, 28, 951–956. [Google Scholar]
- Sehgal, P.; Khan, M.; Kumar, O.; Vijayaraghavan, R. Purification, characterization and toxicity profile of ricin isoforms from castor beans. Food Chem. Toxicol. 2010, 48, 3171–3176. [Google Scholar]
- Sehgal, P.; Kumar, O.; Kameswararao, M.; Ravindran, J.; Khan, M.; Sharma, S.; Vijayaraghavan, R.; Prasad, G.B.K.S. Differential toxicity profile of ricin isoforms correlates with their glycosylation levels. Toxicology 2011, 282, 56–67. [Google Scholar]
- Fodstad, O.; Olsnes, S.; Pihl, A. Toxicity, distribution and elimination of the cancerostatic lectins abrin and ricin after parenteral injection into mice. Br. J. Cancer 1976, 34, 418–425. [Google Scholar]
- Poli, M.A.; Roy, C.; Huebner, K.D.; Franz, D.R.; Jaax, N.K. Ricin. In Medical Aspects of Biological Warfare, 2nd; Dembek, Z.F., Ed.; TMM Publications: Washington, DC, USA, 2007; pp. 323–335. [Google Scholar]
- Wannemacher, R.W.; Anderson, J.B. Inhalation Ricin: Aerosol Procedures, Animal Toxicology, and Therapy. In Inhalation Toxicology; Salem, H., Katz, S.A., Eds.; CRC Press Taylor & Francis Group: Boca Raton, FL, USA, 2006; pp. 973–982. [Google Scholar]
- Foxwell, B.M.; Detre, S.I.; Donovan, T.A.; Thorpe, P.E. The use of anti-ricin antibodies to protect mice intoxicated with ricin. Toxicology 1985, 34, 79–88. [Google Scholar]
- Olsnes, S.; Pappenheimer, A.M.; Meren, R. Lectins from Abrus precatorius and Ricinus communis: II. Hybrid toxins and their interaction with chain-specific antibodies. J. Immunol. 1974, 113, 842–847. [Google Scholar] [PubMed]
- Olsnes, S.; Refsnes, K.; Pihl, A. Mechanism of action of the toxic lectins abrin and ricin. Nature 1974, 249, 627–631. [Google Scholar]
- Fodstad, O.; Johannessen, J.V.; Schjerven, L.; Pihl, A. Toxicity of abrin and ricin in mice and dogs. J. Toxicol. Environ. Health 1979, 5, 1073–1084. [Google Scholar]
- He, X.; McMahon, S.; Henderson, T.D., II; Griffey, S.M.; Cheng, L.W. Ricin toxicokinetics and its sensitive detection in mouse sera or feces using immuno-PCR. PLoS One 2010, 5. [Google Scholar] [CrossRef]
- Jang, H.Y.; Kim, J.H. Isolation and biochemical properties of ricin from Ricinus communis. Korean Biochem. J. 1993, 26, 98–104. [Google Scholar]
- Lin, J.-Y.; Liu, S.-Y. Studies on the antitumor lectins isolated from the seeds of Ricinus communis (castor bean). Toxicon 1986, 24, 757–765. [Google Scholar]
- Roy, C.J.; Hale, M.; Hartings, J.M.; Pitt, L.; Duniho, S. Impact of inhalation exposure modality and particle size on the respiratory deposition of ricin in BALB/c mice. Inhal. Toxicol. 2003, 15, 619–638. [Google Scholar]
- Derenzini, M.; Bonetti, E.; Marionozzi, V.; Stirpe, F. Toxic effects of ricin: Studies on the pathogenesis of liver lesions. Virchows Arch. B 1976, 20, 15–28. [Google Scholar]
- Griffiths, G.D.; Phillips, G.J.; Holley, J. Inhalation toxicology of ricin preparations: Animal models, prophylactic and therapeutic approaches to protection. Inhal. Toxicol. 2007, 19, 873–887. [Google Scholar]
- Griffiths, G.D.; Rice, P.; Allenby, A.C.; Bailey, S.C.; Upshall, D.G. Inhalation toxicology and histopathology of ricin and abrin toxins. Inhal. Toxicol. 1995, 7, 269–288. [Google Scholar]
- Roy, C.J.; Reed, D.S.; Hutt, J.A. Aerobiology and inhalation exposure to biological select agents and toxins. Vet. Pathol. 2010, 47, 779–789. [Google Scholar]
- Ishiguro, M.; Mitarai, M.; Harada, H.; Sekine, I.; Nishimori, I.; Kikutani, M. Biochemical studies on oral toxicity of ricin. I. Ricin administered orally can impair sugar absorption by rat small intestine. Chem. Pharm. Bull. (Tokyo) 1983, 31, 3222–3227. [Google Scholar] [PubMed]
- Garber, E.A.E. Toxicity and detection of ricin and abrin in beverages. J. Food Prot. 2008, 71, 1875–1883. [Google Scholar]
- Cook, D.L.; David, J.; Griffiths, G.D. Retrospective identification of ricin in animal tissues following administration by pulmonary and oral routes. Toxicology 2006, 223, 61–70. [Google Scholar]
- Tuson, R.V. note on an alkaloid contained in the seeds of the Ricinus communis, or castor-oil plant. J. Chem. Soc. 1864, 17, 195–197. [Google Scholar]
- Böttcher, B. Zur Kenntnis des Ricinins. Ber. Dtsch. Chem. Ges. 1918, 51, 673–687. [Google Scholar]
- Späth, E.; Koller, G. Die Synthese des Ricinins. Ber. Dtsch. Chem. Ges. 1923, 56, 2454–2460. [Google Scholar]
- Späth, E.; Koller, G. Die Konstitution des Ricinins. Ber. Dtsch. Chem. Ges. 1923, 56, 880–887. [Google Scholar]
- Soriano-García, M.; Jiménez, M.E.; Reyes Vaca, R.; Toscano, R.A. Structure of ricinine. Acta Crystallogr. Sec. C 1989, 45, 957–959. [Google Scholar]
- Waller, G.R.; Skursky, L. Translocation and metabolism of ricinine in the castor bean plant, Ricinus communis L. Plant Physiol. 1972, 50, 622–626. [Google Scholar]
- Mann, D.F.; Byerrum, R.U. Activation of the de novo pathway for pyridine nucleotide biosynthesis prior to ricinine biosynthesis in castor beans. Plant Physiol. 1974, 53, 603–609. [Google Scholar]
- Ferraz, A.C.; Angelucci, M.E.M.; Da Costa, M.L.; Batista, I.R.; de Oliveira, B.H.; da Cunha, C. Pharmacological evaluation of ricinine, a central nervous system stimulant isolated from Ricinus communis. Pharmacol. Biochem. Behav. 1999, 63, 367–375. [Google Scholar]
- Ferraz, A.C.; Pereira, L.F.; Ribeiro, R.L.; Wolfman, C.; Medina, J.H.; Scorza, F.A.; Santos, N.F.; Cavalheiro, E.A.; da Cunha, C. Ricinine-elicited seizures: A novel chemical model of convulsive seizures. Pharmacol. Biochem. Behav. 2000, 65, 577–583. [Google Scholar]
- Ferraz, A.C.; Anselmo-Franci, J.A.; Perosa, S.R.; de Castro-Neto, E.F.; Bellissimo, M.I.; de Oliveira, B.H.; Cavalheiro, E.A.; Naffah-Mazzacoratti, M.D.G.; da Cunha, C. Amino acid and monoamine alterations in the cerebral cortex and hippocampus of mice submitted to ricinine-induced seizures. Pharmacol. Biochem. Behav. 2002, 72, 779–786. [Google Scholar]
- De Assis Junior, E.M.; Fernandes, I.M.d.S.; Santos, C.S.; de Mesquita, L.X.; Pereira, R.A.; Maracajá, P.B.; Soto-Blanco, B. Toxicity of castor bean (Ricinus communis) pollen to honeybees. Agric. Ecosyst. Environ. 2011, 141, 221–223. [Google Scholar]
- Upasani, S.M.; Kotkar, H.M.; Mendki, P.S.; Maheshwari, V.L. Partial characterization and insecticidal properties of Ricinus communis L. foliage flavonoids. Pest Manag. Sci. 2003, 59, 1349–1354. [Google Scholar] [CrossRef] [PubMed]
- Bigi, M.F.M.A.; Torkomian, V.L.V.; de Groote, S.T.C.S.; Hebling, M.J.A.; Bueno, O.C.; Pagnocca, F.C.; Fernandes, J.B.; Vieira, P.C.; da Silva, M.F.G.F. Activity of Ricinus communis (Euphorbiaceae) and ricinine against the leaf-cutting ant Atta sexdens rubropilosa (hymenoptera: Formicidae) and the symbiotic fungus Leucoagaricus gongylophorus. Pest Manag. Sci. 2004, 60, 933–938. [Google Scholar]
- Taylor, S.; Massiah, A.; Lomonossoff, G.; Roberts, L.M.; Lord, J.M.; Hartley, M. Correlation between the activities of five ribosome-inactivating proteins in depurination of tobacco ribosomes and inhibition of tobacco mosaic virus infection. Plant J. 1994, 5, 827–835. [Google Scholar]
- Sitton, D.; West, C.A. Casbene: An anti-fungal diterpene produced in cell-free extracts of Ricinus communis seedlings. Phytochemistry 1975, 14, 1921–1925. [Google Scholar]
- Figley, K.D.; Elrod, R.H. Endemic asthma due to castor bean dust. J. Am. Med. Assoc. 1928, 90, 79–82. [Google Scholar]
- Ratner, B.; Gruehl, H.L. Respiratory anaphylaxis (asthma) and ricin poisoning induced with castor bean dust. Am. J. Epidemiol. 1929, 10, 236–244. [Google Scholar]
- Alistair, E. Études de la ricine: III. Hypersensibilité a la ricine. Ann. Inst. Pasteur. 1914, 28, 605–607. [Google Scholar]
- Bashir, M.E.H.; Hubatsch, I.; Leinenbach, H.P.; Zeppezauer, M.; Panzani, R.C.; Hussein, I.H. Ric c 1 and Ric c 3, the allergenic 2S albumin storage proteins of Ricinus communis: Complete primary structures and phylogenetic relationships. Int. Arch. Allergy Immunol. 1998, 115, 73–82. [Google Scholar]
- Thorpe, S.C.; Kemeny, D.M.; Panzani, R.C.; McGurl, B.; Lord, M. Allergy to castor bean. II. Identification of the major allergens in castor bean seeds. J. Allergy Clin. Immunol. 1988, 82, 67–72. [Google Scholar] [CrossRef] [PubMed]
- Deus-de-Oliveira, N.; Felix, S.P.; Carrielo-Gama, C.; Fernandes, K.V.; Damatta, R.A.; Machado, O.L. Identification of critical amino acids in the IgE epitopes of Ric c 1 and Ric c 3 and the application of glutamic acid as an IgE blocker. PLoS One 2011, 6. [Google Scholar]
- Spies, J.R.; Coulson, E.J. Antigenic specificity relationships of castor bean meal, pollen, and allergenic fraction, cb-1a, of Ricinus commu. J. Allergy 1965, 36, 423–432. [Google Scholar]
- Rauber, A.; Heard, J. Castor bean toxicity re-examined: A new perspective. Vet. Hum. Toxicol. 1985, 27, 498–502. [Google Scholar]
- Challoner, K.R.; McCarron, M.M. Castor bean intoxication. Ann. Emerg. Med. 1990, 19, 1177–1183. [Google Scholar]
- Balint, G.A. Ricin: The toxic protein of castor oil seeds. Toxicology 1974, 2, 77–102. [Google Scholar]
- Reed, R.P. Castor oil seed poisoning: A concern for children. Med. J. Aust. 1998, 168, 423–424. [Google Scholar]
- Lucas, G.N. Plant poisoning in Sri Lankan children: A hospital based prospective study. Sri. Lanka. J. Child Health 2006, 35, 111–124. [Google Scholar]
- Ingle, V.; Kale, V.; Talwalkar, Y. Accidental poisoning in children with particular reference to castor beans. Indian J. Pediatr. 1966, 33, 237–240. [Google Scholar]
- Kinamore, P.A.; Jaeger, R.W.; de Castro, F.J. Abrus and ricinus ingestion: Management of three cases. Clin. Toxicol. 1980, 17, 401–405. [Google Scholar]
- Despott, E.; Cachia, M.J. A case of accidental ricin poisoning. Malta Med. J. 2004, 16, 39–41. [Google Scholar]
- Aplin, P.J.; Eliseo, T. Ingestion of castor oil plant seeds. Med. J. Aust. 1997, 167, 260–261. [Google Scholar]
- Fine, D.R.; Shepherd, H.A.; Griffiths, G.D.; Green, M. Sub-lethal poisoning by self-injection with ricin. Med. Sci. Law 1992, 32, 70–72. [Google Scholar]
- Krenzelok, E.P.; Mrvos, R. Friends and foes in the plant world: A profile of plant ingestions and fatalities. Clin. Toxicol. (Phila.) 2011, 49, 142–149. [Google Scholar] [CrossRef] [PubMed]
- Jaspersen-Schib, R.; Theus, L.; Guirguis-Oeschger, M.; Gossweiler, B.; Meier-Abt, P.J. Wichtige Pflanzenvergiftungen in der Schweiz 1966−1994: Eine Fallanalyse aus dem schweizerischen toxikologischen Informationszentrum (STIZ). Schweiz. Med. Wchnschr. 1996, 126, 1085–1098. [Google Scholar]
- Lim, H.; Kim, H.J.; Cho, Y.S. A case of ricin poisoning following ingestion of Korean castor bean. Emerg. Med. J. 2009, 26, 301–302. [Google Scholar]
- Castex, M.R. Intoxicacion y alergia por la ingestion de semillas de Ricinus communis. Prensa Méd. Argent 1949, 36, 345–349. [Google Scholar] [PubMed]
- Maretić, Z. Otrovanje sjemenkama ricinusa. Arh. Hig. Rada Toksikol. 1980, 31, 251–257. [Google Scholar]
- Nishiyama, T.; Oka, H.; Miyoshi, M.; Aibiki, M.; Maekawa, S.; Shirakawa, Y. Case of accidental ingestion of caster beans: Acute intoxication by ricin. Chudoku Kenkyu 2005, 18, 149–150. [Google Scholar]
- Al-Tamimi, F.A.; Hegazi, A.E. A case of castor bean poisoning. Sultan Qaboos Univ. Med. J. 2008, 8, 83–87. [Google Scholar]
- Smith, S.W.; Graber, N.M.; Johnson, R.C.; Barr, J.R.; Hoffman, R.S.; Nelson, L.S. Multisystem organ failure after large volume injection of castor oil. Ann. Plast. Surg. 2009, 62, 12–14. [Google Scholar]
- Targosz, D.; Winnik, L.; Szkolnicka, B. Suicidal poisoning with castor bean (Ricinus communis) extract injected subcutaneously-Case report. Clin. Toxicol. 2002, 40, 398–398. [Google Scholar]
- Watson, W.A.; Litovitz, T.L.; Klein-Schwartz, W.; Rodgers, G.C., Jr.; Youniss, J.; Reid, N.; Rouse, W.G.; Rembert, R.S.; Borys, D. 2003 annual report of the American Association of Poison Control Centers toxic exposure surveillance system. Am. J. Emerg. Med. 2004, 22, 335–404. [Google Scholar]
- Coopman, V.; De Leeuw, M.; Cordonnier, J.; Jacobs, W. Suicidal death after injection of a castor bean extract (Ricinus communis L.). Forensic. Sci. Int. 2009, 189, 13–20. [Google Scholar] [CrossRef]
- De Paepe, P.; Gijsenbergh, F.; Martens, F.; Piette, M.; Buylaert, W. Two fatal cases following ricin injection. Br. J. Clin. Pharmacol. 2005, 59, 125–126. [Google Scholar]
- Passeron, T.; Mantoux, F.; Lacour, J.P.; Roger, P.M.; Fosse, T.; Iannelli, A.; Ortonne, J.P. Infectious and toxic cellulitis due to suicide attempt by subcutaneous injection of ricin. Br. J. Dermatol. 2004, 150, 154–154. [Google Scholar]
- Milewski, L.M.; Khan, S.A. An overview of potentially life-threatening poisonous plants in dogs and cats. J. Vet. Emerg. Crit. Care 2006, 16, 25–33. [Google Scholar]
- Meldrum, W.P. Poisoning by castor oil seeds. Br. Med. J. 1900, Feb 10, 317–317. [Google Scholar]
- Bispham, W.N. Report of cases of poisoning by fruit of Ricinus communis. Am. J. Med. Sci. 1903, 126, 319–321. [Google Scholar]
- Burroughs, W.J. Poisonous effects of Ricinus communis. Br. Med. J. 1903, Oct 3, 836–836. [Google Scholar]
- Arnold, H.L. Poisoning from castor bean. Science 1924, 59, 577–577. [Google Scholar]
- Lipták, P. Rizinussamen-Vergiftungen. Arch. Toxicol. 1928, 1, A47–A48. [Google Scholar]
- Abdülkadir-Lütfi; Taeger, Tödliche Vergiftung durch Rizinussamen. Arch. Toxicol. 1935, 6, 97–98.
- Möschl, H. Zur Klinik und Pathogenese der Rizinvergiftung. Wien. Klin. Wchnschr. 1938, 51, 473–475. [Google Scholar]
- Koch, L.A.; Caplan, J. Castor bean poisoning. Am. J. Dis. Child 1942, 64, 485–486. [Google Scholar]
- Abbozzo, G. Klinisch-toxikologische Zusammenstellung der Vergiftungsfälle in Florenz im Triennium 1950-1952. Arch. Toxicol. 1953, 14, 435–444. [Google Scholar]
- Kaszás, T.; Papp, G. Ricinussamenvergiftung von Schulkindern. Arch. Toxikol. 1960, 18, 145–150. [Google Scholar]
- Karolini, T.; Zarnowska-Cwiertka, W. Case of poisoning with ricinus seeds. Przegl. Epidemiol. 1965, 19, 272–273. [Google Scholar]
- Krain, L.S.; Bucher, W.H.; Heidbreder, G.A. Trends in accidental poisoning in childhood. Los Angeles county experience. Clin. Pediatr. (Phila.) 1971, 10, 167–170. [Google Scholar] [CrossRef] [PubMed]
- Kingma, J. Ricin poisoning caused by chewing a castor bean. Ned Tijdschr Geneeskd 1971, 115, 1190–1191. [Google Scholar]
- Ramakrishnan, S.; Balasubramanian, K.; Madhavan, M. Biochemical and pathological studies on castor seed poisoning. J. Assoc. Physicians India 1972, 20, 781–784. [Google Scholar]
- Malizia, E.; Sarcinelli, L.; Andreucci, G. Ricinus poisoning: A familiar epidemy. Acta Pharmacol. Toxicol. (Copenh.) 1977, 41, 351–361. [Google Scholar]
- Knight, B. Ricin-a potent homicidal poison. Br. Med. J. 1979, 1, 350–351. [Google Scholar]
- Satpathy, R.; Das, B.B. Accidental poisoning in childhood. J. Indian Med. Assoc. 1979, 73, 190–192. [Google Scholar]
- Henry, G.W.; Schwenk, G.R., Jr.; Bohnert, P.A. Umbrellas and mole beans: A warning about acute ricin poisoning. J. Indiana State Med. Assoc. 1981, 74, 572–573. [Google Scholar]
- Vinther, S.; Matzen, P. Poisoning with the castor oil plant (Ricinus communis L.). Ugeskr. Laeger. 1983, 145, 1546–1547. [Google Scholar] [PubMed]
- Romanos, A.; Toledo, F.; Vazquez, G.; Guzman, J.; Serrano, M.L.; Velasco, Y.M.J. Intoxicacion por semillas de Ricinus communis. Nota clinica. Rev. Toxicol. (Elche Spain) 1983, 1, 30–32. [Google Scholar]
- Zifroni, A. Castor bean poisoning. Harefuah 1985, 108, 102–103. [Google Scholar]
- Painter, M.J.; Veitch, I.H.M.; Packer, J.M.V. A science lesson, a castor oil plant seed and a salford schoolboy. Commun. Med. 1985, 7, 208–210. [Google Scholar]
- Wedin, G.P.; Neal, J.S.; Everson, G.W.; Krenzelok, E.P. Castor bean poisoning. Am. J. Emerg. Med. 1986, 4, 259–261. [Google Scholar]
- Belzunegui, O.T.; Charles, A.B.; Hernandez, R.; Maravi Petri, E. Poisoning by ingestion of castor bean seeds. Apropos of a case. Med. Clin. (Barc.) 1988, 90, 716–717. [Google Scholar]
- Ravindra, F.R.; Dulitya, F.N. Poisoning with plants and mushrooms in Sri Lanka: A retrospective hospital based study. Vet. Hum. Toxicol. 1990, 32, 579–581. [Google Scholar]
- Palatnick, W.; Tenenbein, M. Hepatotoxicity from castor bean ingestion in a child. J. Toxicol. Clin. Toxicol. 2000, 38, 67–69. [Google Scholar]
- Hamouda, C.; Amamou, M.; Thabet, H.; Yacoub, M. Plant poisonings from herbal medication admitted to a tunisian toxicologic intensive care unit, 1983-1998. Vet. Hum. Toxicol. 2000, 42, 137–141. [Google Scholar]
- Frohne, D.; Pfänder, H.J. Ricinus communis. In Giftpflanzen-Ein Handbuch für Apotheker, Ärzte, Toxikologen und Biologen; Wissenschaftliche Verlagsgesellschaft mbH: Stuttgart, Germany, 2004. [Google Scholar]
- Klain, G.J.; Jaeger, J.J. Castor Seed Poisoning in Humans: A Review: Technical Report #453; Letterman Army Institute of Research: San Francisco, CA, USA, 1990; pp. 1–48. [Google Scholar]
- Papaloucas, M.; Papaloucas, C.; Stergioulas, A. Ricin and the assassination of Georgi Markov. Pak. J. Biol. Sci. 2008, 11, 2370–2371. [Google Scholar]
- Kopferschmitt, J.; Flesch, F.; Lugnier, A.; Sauder, P.; Jaeger, A.; Mantz, J.M. Acute voluntary intoxication by ricin. Hum. Toxicol. 1983, 2, 239–242. [Google Scholar]
- Garcia, F.M.; Alvarez, A.P.; Baneres, G.B.; Alegre, B.V. Poisoning caused by ricin seeds. Aten. Primaria 1996, 18, 203. [Google Scholar]
- Alao, A.O.; Yolles, J.C.; Armenta, W. Cybersuicide: The internet and suicide. Am. J. Psychiatry 1999, 156, 1836–1837. [Google Scholar]
- Johnson, R.C.; Lemire, S.W.; Woolfitt, A.R.; Ospina, M.; Preston, K.P.; Olson, C.T.; Barr, J.R. Quantification of ricinine in rat and human urine: A biomarker for ricin exposure. J. Anal. Toxicol. 2005, 29, 149–155. [Google Scholar]
- Krieger-Huber, S. Rizin-Vergiftungen mit tödlichem Ausgang bei Hunden nach Aufnahme des biologischen Naturdüngers “Oscorna Animalin”. Kleintier Praxis 1980, 25, 281–286. [Google Scholar]
- Albretsen, J.C.; Gwaltney-Brant, S.M.; Khan, S.A. Evaluation of castor bean toxicosis in dogs: 98 cases. J. Am. Anim. Hosp. Assoc. 2000, 36, 229–233. [Google Scholar]
- Ebbecke, M.; Hünefeld, D.; Schaper, A.; Desl, H. Increasing frequency of serious or fatal poisonings in dogs caused by organic fertilizers during the summer of 2001 in Germany. Clin. Toxicol. 2002, 40, 346–347. [Google Scholar]
- Soto-Blanco, B.; Sinhorini, I.L.; Gorniak, S.L.; Schumaher-Henrique, B. Ricinus communis cake poisoning in a dog. Vet. Hum. Toxicol. 2002, 44, 155–156. [Google Scholar]
- Cardoso, M.J.L.; Fernandes, H.S.; Lima, L.S.A.; Moutinho, F.Q.; Sakate, M. Accidental ingestion of Ricinus communis in dogs (Canis familiaris, L. 1758)-Case report. Vet. Notícias Uberlândia 2005, 11, 99–103. [Google Scholar]
- Mouser, P.; Filigenzi, M.S.; Puschner, B.; Johnson, V.; Miller, M.A.; Hooser, S.B. Fatal ricin toxicosis in a puppy confirmed by liquid chromatography/mass spectrometry when using ricinine as a marker. J. Vet. Diagn. Invest. 2007, 19, 216–220. [Google Scholar]
- Neika, D. Vergiftung mit Rizinussamen bei einem Hund - Fallbericht. Kleintiermedizin 2010, 11, 343–346. [Google Scholar]
- Roels, S.; Coopman, V.; Vanhaelen, P.; Cordonnier, J. Lethal ricin intoxication in two adult dogs: Toxicologic and histopathologic findings. J. Vet. Diagn. Invest. 2010, 22, 466–468. [Google Scholar]
- Hong, I.H.; Kwon, T.E.; Lee, S.K.; Park, J.K.; Ki, M.R.; Park, S.I.; Jeong, K.S. Fetal death of dogs after the ingestion of a soil conditioner. Exp. Toxicol. Pathol. 2011, 63, 113–117. [Google Scholar]
- Vigener, A. Untersuchung eines verfälschten Leinmehls. Arch. Pharm. 1874, 204, 495–506. [Google Scholar]
- Regensbogen, vergiftung durch Leinsamen bei Pferden. Berl. Tierarztl. Wchnschr. 1888, 46, 94–95.
- Geary, T. Castor bean poisoning. Vet. Rec. 1950, 62, 472–473. [Google Scholar]
- Jensen, W.I.; Allen, J.P. Naturally occurring and experimentally induced castor bean (Ricinus communis) poisoning in ducks. Avian Dis. 1981, 25, 184–194. [Google Scholar]
- Fernandes, W.R.; Baccarin, R.Y.A.; Michima, L.E.S. Equine poisoning by Ricinus communis: Case report. Rev. Bras. Saúde Prod. An. 2002, 3, 26–31. [Google Scholar]
- Aslani, M.R.; Maleki, M.; Mohri, M.; Sharifi, K.; Najjar-Nezhad, V.; Afshari, E. Castor bean (Ricinus communis) toxicosis in a sheep flock. Toxicon 2007, 49, 400–406. [Google Scholar]
- Miessner, H. Ueber die Giftigkeit der Rizinussamen. Mitt. des Kaiser Wilhelm-Instituts für Landwirtschaft in Bromberg 1909, 1, 15–265. [Google Scholar]
- Commission Directive 2009/141/EC of 23.11.2009. Off J Eur Union L 2009, 308, 20–23.
- Düngemittelverordnung -DüMv-, Attachment 2, Nr. 7.1.5. Available online: http://www.gesetze-im-internet.de/bundesrecht/d_mv_2008/gesamt.pdf (accessed on 04.08.2011).
- Koja, N.; Shibata, T.; Mochida, K. Enzyme-linked immunoassay of ricin. Toxicon 1980, 18, 611–618. [Google Scholar]
- Poli, M.A.; Rivera, V.R.; Hewetson, J.F.; Merrill, G.A. Detection of ricin by colorimetric and chemiluminescence ELISA. Toxicon 1994, 32, 1371–1377. [Google Scholar]
- Frankel, A.E.; Burbage, C.; Fu, T.; Tagge, E.; Chandler, J.; Willingham, M. Characterization of a ricin fusion toxin targeted to the interleukin-2 receptor. Protein Eng. 1996, 9, 913–919. [Google Scholar]
- Griffiths, G.D.; Newman, H.; Gee, D.J. Identification and quantification of ricin toxin in animal tissues using ELISA. J. Forensic. Sci. Soc. 1986, 26, 349–358. [Google Scholar]
- Leith, A.G.; Griffiths, G.D.; Green, M.A. Quantification of ricin toxin using a highly sensitive avidin/biotin enzyme-linked immunosorbent assay. J. Forensic. Sci. Soc. 1988, 28, 227–236. [Google Scholar]
- Pauly, D.; Kirchner, S.; Störmann, B.; Schreiber, T.; Kaulfuss, S.; Schade, R.; Zbinden, R.; Avondet, M.A.; Dorner, M.B.; Dorner, B.G. Simultaneous quantification of five bacterial and plant toxins from complex matrices using a multiplexed fluorescent magnetic suspension assay. Analyst 2009, 134, 2028–2039. [Google Scholar]
- Rubina, A.Y.; Dyukova, V.I.; Dementieva, E.I.; Stomakhin, A.A.; Nesmeyanov, V.A.; Grishin, E.V.; Zasedatelev, A.S. Quantitative immunoassay of biotoxins on hydrogel-based protein microchips. Anal. Biochem. 2005, 340, 317–329. [Google Scholar]
- Guglielmo-Viret, V.; Splettstoesser, W.; Thullier, P. An immunochromatographic test for the diagnosis of ricin inhalational poisoning. Clin. Toxicol. 2007, 45, 505–511. [Google Scholar]
- Zhuang, J.; Cheng, T.; Gao, L.; Luo, Y.; Ren, Q.; Lu, D.; Tang, F.; Ren, X.; Yang, D.; Feng, J.; et al. Silica coating magnetic nanoparticle-based silver enhancement immunoassay for rapid electrical detection of ricin toxin. Toxicon 2010, 55, 145–152. [Google Scholar]
- Lang, L.; Wang, Y.; Wang, C.; Zhao, Y.; Jia, P.; Fu, F. Determination of ricin by double antibody sandwich enzyme-linked immunosorbent assay in different samples. J. Int. Pharm. Res. 2009, 36, 12–16. [Google Scholar]
- Men, J.; Lang, L.; Wang, C.; Wu, J.; Zhao, Y.; Jia, P.Y.; Wei, W.; Wang, Y. Detection of residual toxin in tissues of ricin-poisoned mice by sandwich enzyme-linked immunosorbent assay and immunoprecipitation. Anal. Biochem. 2010, 401, 211–216. [Google Scholar]
- Shyu, H.F.; Chiao, D.J.; Liu, H.W.; Tang, S.S. Monoclonal antibody-based enzyme immunoassay for detection of ricin. Hybrid. Hybrid. 2002, 21, 69–73. [Google Scholar]
- Garber, E.A.; O’Brien, T.W. Detection of ricin in food using electrochemiluminescence-based technology. J. AOAC Int. 2008, 91, 376–382. [Google Scholar]
- He, X.; McMahon, S.; McKeon, T.A.; Brandon, D.L. Development of a novel immuno-PCR assay for detection of ricin in ground beef, liquid chicken egg, and mil. J. Food Prot. 2010, 73, 695–700. [Google Scholar]
- Zhang, H.; Zhao, Q.; Li, X.-F.; Le, X.C. Ultrasensitive assays for proteins. Analyst 2007, 132, 724–737. [Google Scholar]
- Lubelli, C.; Chatgilialoglu, A.; Bolognesi, A.; Strocchi, P.; Colombatti, M.; Stirpe, F. Detection of ricin and other ribosome-inactivating proteins by an immuno-polymerase chain reaction assay. Anal. Biochem. 2006, 355, 102–109. [Google Scholar]
- Narang, U.; Anderson, G.P.; Ligler, F.S.; Burans, J. Fiber optic-based biosensor for ricin. Biosens. Bioelectron. 1997, 12, 937–945. [Google Scholar]
- Shyu, R.-H.; Shyu, H.-F.; Liu, H.-W.; Tang, S.-S. Colloidal gold-based immunochromatographic assay for detection of ricin. Toxicon 2002, 40, 255–258. [Google Scholar]
- Weber, M.; Schulz, H. Immunological detection of ricin and castor seeds in beverages, food and consumer products. Toxichem. Krimtech. 2011, 78, 276–277. [Google Scholar]
- Dayan-Kenigsberg, J.; Bertocchi, A.; Garber, E.A. Rapid detection of ricin in cosmetics and elimination of artifacts associated with wheat lectin. J. Immunol. Methods 2008, 336, 251–254. [Google Scholar]
- Ding, S.; Gao, C.; Gu, L.-Q. Capturing single molecules of immunoglobulin and ricin with an aptamer-encoded glass nanopore. Anal. Chem. 2009, 81, 6649–6655. [Google Scholar]
- Kirby, R.; Cho, E.J.; Gehrke, B.; Bayer, T.; Park, Y.S.; Neikirk, D.P.; McDevitt, J.T.; Ellington, A.D. Aptamer-based sensor arrays for the detection and quantitation of proteins. Anal. Chem. 2004, 76, 4066–4075. [Google Scholar]
- Tang, J.; Xie, J.; Shao, N.; Yan, Y. The DNA aptamers that specifically recognize ricin toxin are selected by two in vitro selection methods. Electrophoresis 2006, 27, 1303–1311. [Google Scholar]
- Haes, A.J.; Giordano, B.C.; Collins, G.E. Aptamer-based detection and quantitative analysis of ricin using affinity probe capillary electrophoresis. Anal. Chem. 2006, 78, 3758–3764. [Google Scholar]
- Förster, C.; Oberthuer, D.; Gao, J.; Eichert, A.; Quast, F.G.; Betzel, C.; Nitsche, A.; Erdmann, V.A.; Furste, J.P. Crystallization and preliminary X-ray diffraction data of an LNA 7-mer duplex derived from a ricin aptamer. Acta Crystallogr. Sec. F 2009, 65, 881–885. [Google Scholar]
- Hesselberth, J.R.; Miller, D.; Robertus, J.; Ellington, A.D. In vitro selection of RNA molecules that inhibit the activity of ricin A-chain. J. Biol. Chem. 2000, 275, 4937–4942. [Google Scholar]
- Fan, S.; Wu, F.; Martiniuk, F.; Hale, M.L.; Ellington, A.D.; Tchou-Wong, K.M. Protective effects of anti-ricin A-chain RNA aptamer against ricin toxicity. World J. Gastroenterol. 2008, 14, 6360–6365. [Google Scholar]
- Lamont, E.A.; He, L.; Warriner, K.; Labuza, T.P.; Sreevatsan, S. A single DNA aptamer functions as a biosensor for ricin. Analyst 2011, 136, 3884–3895. [Google Scholar]
- Jayasena, S.D. Aptamers: An emerging class of molecules that rival antibodies in diagnostics. Clin. Chem. 1999, 45, 1628–1650. [Google Scholar]
- stin, A.; Bergström, T.; Fredriksson, S.A.; Nilsson, C. Solvent-assisted trypsin digestion of ricin for forensic identification by LC-ESI MS/MS. Anal. Chem. 2007, 79, 6271–6278. [Google Scholar]
- Fredriksson, S.A.; Hulst, A.G.; Artursson, E.; de Jong, A.L.; Nilsson, C.; van Baar, B.L. Forensic identification of neat ricin and of ricin from crude castor bean extracts by mass spectrometry. Anal. Chem. 2005, 77, 1545–1555. [Google Scholar]
- Brinkworth, C.S.; Pigott, E.J.; Bourne, D.J. Detection of intact ricin in crude and purified extracts from castor beans using matrix-assisted laser desorption ionization mass spectrometry. Anal. Chem. 2009, 81, 1529–1535. [Google Scholar]
- Brinkworth, C.S. Identification of ricin in crude and purified extracts from castor beans using on-target tryptic digestion and MALDI mass spectrometry. Anal. Chem. 2010, 82, 5246–5252. [Google Scholar]
- Norrgran, J.; Williams, T.L.; Woolfitt, A.R.; Solano, M.I.; Pirkle, J.L.; Barr, J.R. Optimization of digestion parameters for protein quantification. Anal. Biochem. 2009, 393, 48–55. [Google Scholar]
- Kull, S.; Pauly, D.; Störmann, B.; Kirchner, S.; Stämmler, M.; Dorner, M.B.; Lasch, P.; Naumann, D.; Dorner, B.G. Multiplex detection of microbial and plant toxins by immunoaffinity enrichment and matrix-assisted laser desorption/ionization mass spectrometry. Anal. Chem. 2010, 82, 2916–2924. [Google Scholar]
- Sehgal, P.; Rao, M.K.; Kumar, O.; Vijayaraghavan, R. Characterization of native and denatured ricin using MALDI-ToF/MS. Cell Mol. Biol. (Noisy-le-grand) 2010, 56, 1385–1399. [Google Scholar]
- Kalb, S.R.; Barr, J.R. Mass spectrometric detection of ricin and its activity in food and clinical samples. Anal. Chem. 2009, 81, 2037–2042. [Google Scholar]
- McGrath, S.C.; Schieltz, D.M.; McWilliams, L.G.; Pirkle, J.L.; Barr, J.R. Detection and quantification of ricin in beverages using isotope dilution tandem mass spectrometry. Anal. Chem. 2011, 83, 2897–2905. [Google Scholar]
- Duriez, E.; Fenaille, F.; Tabet, J.C.; Lamourette, P.; Hilaire, D.; Becher, F.; Ezan, E. Detection of ricin in complex samples by immunocapture and matrix-assisted laser desorption/ionization time-of-flight mass spectrometry. J. Proteome Res. 2008, 7, 4154–4163. [Google Scholar]
- Kumar, O.; Pradhan, S.; Sehgal, P.; Singh, Y.; Vijayaraghavan, R. Denatured ricin can be detected as native ricin by immunological methods, but nontoxic in vivo. J. Forensic. Sci. 2010, 55, 801–807. [Google Scholar]
- Lumor, S.E.; Hutt, A.; Ronningen, I.; Diez-Gonzalez, F.; Labuza, T.P. Validation of immunodetection (ELISA) of ricin using a biological activity assay. J. Food Sci. 2011, 76, 112–116. [Google Scholar]
- Jackson, L.S.; Zhang, Z.; Tolleson, W.H. Thermal stability of ricin in orange and apple juices. J. Food Sci. 2010, 75, T65–T71. [Google Scholar]
- Jackson, L.S.; Tolleson, W.H.; Chirtel, S.J. Thermal inactivation of ricin using infant formula as a food matrix. J. Agric. Food Chem. 2006, 54, 7300–7304. [Google Scholar]
- Ishiguro, M.; Takahashi, T.; Funatsu, G.; Hayashi, K.; Funatsu, M. Biochemical studies on ricin: I. Purification of ricin. J. Biochem. 1964, 55, 587–592. [Google Scholar]
- Brzezinski, J.L.; Craft, D.L. Evaluation of an in vitro bioassay for the detection of purified ricin and castor bean in beverages and liquid food matrices. J. Food Prot. 2007, 70, 2377–2382. [Google Scholar]
- Cole, K.D.; Gaigalas, A.; Almeida, J.L. Process monitoring the inactivation of ricin and model proteins by disinfectants using fluorescence and biological activity. Biotechnol. Prog. 2008, 24, 784–791. [Google Scholar]
- Lin, J.-Y.; Liu, K.; Chen, C.-C.; Tung, T.-C. Effect of crystalline ricin on the biosynthesis of protein, RNA, and DNA in experimental tumor cell. Cancer Res. 1971, 31, 921–924. [Google Scholar]
- Olsnes, S. Toxic proteins inhibiting protein synthesis. Naturwissenschaften 1972, 59, 497–502. [Google Scholar]
- Olsnes, S.; Pihl, A. Ricin-A potent inhibitor of protein synthesis. FEBS Lett. 1972, 20, 327–329. [Google Scholar]
- He, X.; Lu, S.; Cheng, L.W.; Rasooly, R.; Carter, J.M. Effect of food matrices on the biological activity of ricin. J. Food Prot. 2008, 71, 2053–2058. [Google Scholar]
- Hale, M.L. Microtiter-based assay for evaluating the biological activity of ribosome-inactivating proteins. Pharmacol. Toxicol. 2001, 88, 255–260. [Google Scholar]
- Heisler, I.; Keller, J.; Tauber, R.; Sutherland, M.; Fuchs, H. A colorimetric assay for the quantitation of free adenine applied to determine the enzymatic activity of ribosome-inactivating proteins. Anal. Biochem. 2002, 302, 114–122. [Google Scholar]
- Zamboni, M.; Brigotti, M.; Rambelli, F.; Montanaro, L.; Sperti, S. High-pressure-liquid-chromatographic and fluorimetric methods for the determination of adenine released from ribosomes by ricin and gelonin. Biochem. J. 1989, 259, 639–643. [Google Scholar]
- Roday, S.; Sturm, M.B.; Blakaj, D.; Schramm, V.L. Detection of an abasic site in RNA with stem-loop DNA beacons: Application to an activity assay for ricin toxin A-chain. J. Biochem. Biophys. Methods 2008, 70, 945–953. [Google Scholar]
- Hines, H.B.; Brueggemann, E.E.; Hale, M.L. High-performance liquid chromatography-mass selective detection assay for adenine released from a synthetic RNA substrate by ricin A chain. Anal. Biochem. 2004, 330, 119–122. [Google Scholar]
- Keener, W.K.; Rivera, V.R.; Young, C.C.; Poli, M.A. An activity-dependent assay for ricin and related RNA N-glycosidases based on electrochemiluminescence. Anal. Biochem. 2006, 357, 200–207. [Google Scholar]
- Pierce, M.; Kahn, J.N.; Chiou, J.; Tumer, N.E. Development of a quantitative RT-PCR assay to examine the kinetics of ribosome depurination by ribosome inactivating proteins using saccharomyces cerevisiae as a model. RNA 2011, 17, 201–210. [Google Scholar]
- Becher, F.; Duriez, E.; Volland, H.; Tabet, J.C.; Ezan, E. Detection of functional ricin by immunoaffinity and liquid chromatography-tandem mass spectrometry. Anal. Chem. 2007, 79, 659–665. [Google Scholar]
- Ishiguro, M.; Tanabe, S.; Matori, Y.; Sakakibara, R. Biochemical studies on oral toxicity of ricin. IV. A fate of orally administered ricin in rats. J. Pharmacobiodyn. 1992, 15, 147–156. [Google Scholar]
- Bingen, A.; Creppy, E.E.; Gut, J.P.; Dirheimer, G.; Kirn, A. The Kupffer cell is the first target in ricin-induced hepatitis. J. Submicrosc. Cytol. 1987, 19, 247–256. [Google Scholar]
- Zenilman, M.E.; Fiani, M.; Stahl, P.D.; Brunt, E.M.; Flye, M.W. Selective depletion of Kupffer cells in mice by intact ricin. Transplantation 1989, 47, 200–203. [Google Scholar]
- Zenilman, M.E.; Fiani, M.; Stahl, P.D.; Brunt, E.M.; Flye, M.W. Use of ricin A-chain to selectively deplete Kupffer cells. J. Surg. Res. 1988, 45, 82–89. [Google Scholar]
- Magnusson, S.; Berg, T. Endocytosis of ricin by rat liver cells in vivo and in vitro is mainly mediated by mannose receptors on sinusoidal endothelial cells. Biochem. J. 1993, 291, 749–755. [Google Scholar]
- Skilleter, D.N.; Paine, A.J.; Stirpe, F. A comparison of the accumulation of ricin by hepatic parenchymal and non-parenchymal cells and its inhibition of protein synthesis. Biochim. Biophys. Acta 1981, 677, 495–500. [Google Scholar]
- McGreal, E.P.; Miller, J.L.; Gordon, S. Ligand recognition by antigen-presenting cell C-type lectin receptors. Curr. Opin. Immunol. 2005, 17, 18–24. [Google Scholar]
- Bilzer, M.; Roggel, F.; Gerbes, A.L. Role of Kupffer cells in host defense and liver disease. Liver Int. 2006, 26, 1175–1186. [Google Scholar]
- Robinson, T.; Fowell, E. A chromatographic analysis for ricinine. Nature 1959, 183, 833–834. [Google Scholar]
- Hinkson, J.; Elliger, C.; Fuller, G. The effect of ammoniation upon ricinine in castor meal. J. Am. Oil Chem. Soc. 1972, 49, 196–199. [Google Scholar]
- Olaifa, J.I.; Matsumura, F.; Zeevaart, J.A.D.; Mullin, C.A.; Charalambous, P. Lethal amounts of ricinine in green peach aphids (Myzus persicae) (suzler) fed on castor bean plants. Plant Sci. 1991, 73, 253–256. [Google Scholar]
- Darby, S.M.; Miller, M.L.; Allen, R.O. Forensic determination of ricin and the alkaloid marker ricinine from castor bean extracts. J. Forensic. Sci. 2001, 46, 1033–1042. [Google Scholar]
- Melchert, H.U.; Pabel, E. Reliable identification and quantification of trichothecenes and other mycotoxins by electron impact and chemical ionization-gas chromatography-mass spectrometry, using an ion-trap system in the multiple mass spectrometry mode. Candidate reference method for complex matrices. J. Chromatogr. A 2004, 1056, 195–199. [Google Scholar]
- Wang, Z.; Li, D.; Zhou, Z.; Li, B.; Yang, W. A simple method for screening and quantification of ricinine in feed with HPLC and LC-MS. J. Chromatogr. Sci. 2009, 47, 585–588. [Google Scholar]
- Pruet, J.M.; Jasheway, K.R.; Manzano, L.A.; Bai, Y.; Anslyn, E.V.; Robertus, J.D. 7-substituted pterins provide a new direction for ricin A chain inhibitors. Eur. J. Med. Chem. 2011, 46, 3608–3615. [Google Scholar]
- Muldoon, D.F.; Stohs, S.J. Modulation of ricin toxicity in mice by biologically active substances. J. Appl. Toxicol. 1994, 14, 81–86. [Google Scholar]
- Poli, M.A.; Rivera, V.R.; Pitt, M.L.; Vogel, P. Aerosolized specific antibody protects mice from lung injury associated with aerosolized ricin exposure. Toxicon 1996, 34, 1037–1044. [Google Scholar]
- Pratt, T.S.; Pincus, S.H.; Hale, M.L.; Moreira, A.L.; Roy, C.J.; Tchou-Wong, K.-M. Oropharyngeal aspiration of ricin as a lung challenge model for evaluation of the therapeutic index of antibodies against ricin a-chain for post-exposure treatment. Exp. Lung Res. 2007, 33, 459–481. [Google Scholar]
- Ehrlich, P. Experimentelle Untersuchungen über Immunität. I. Ueber Ricin. Dtsch. Med. Wchnschr. 1891, 17, 976–979. [Google Scholar]
- Beyer, N.H.; Kogutowska, E.; Hansen, J.J.; Engelhart Illigen, K.E.; Heegaard, N.H. A mouse model for ricin poisoning and for evaluating protective effects of antiricin antibodies. Clin. Toxicol. (Phila.) 2009, 47, 219–225. [Google Scholar] [CrossRef] [PubMed]
- Pauly, D.; Dorner, M.; Zhang, X.; Hlinak, A.; Dorner, B.; Schade, R. Monitoring of laying capacity, immunoglobulin Y concentration, and antibody titer development in chickens immunized with ricin and botulinum toxins over a two-year perio. Poult. Sci. 2009, 88, 281–290. [Google Scholar]
- Hewetson, J.F.; Rivera, V.R.; Creasia, D.A.; Lemley, P.V.; Rippy, M.K.; Poli, M.A. Protection of mice from inhaled ricin by vaccination with ricin or by passive treatment with heterologous antibody. Vaccine 1993, 11, 743–746. [Google Scholar]
- Stéphanoff, M.A. tudes sur la ricine et l’antiricine. Ann. Inst. Pasteur. 1896, 10, 663–668. [Google Scholar]
- Houston, L.L. Protection of mice from ricin poisoning by treatment with antibodies directed against ricin. Clin. Toxicol. 1982, 19, 385–389. [Google Scholar]
- Lemley, P.V.; Thalley, B.S.; Stafford, D.C. Prophylactic and therapeutic efficacy of an avian antitoxin in ricin intoxication. Ther. Immunol. 1995, 2, 59–66. [Google Scholar]
- Godal, A.; Fodstad, Ø.; Pihl, A. Antibody formation against the cytotoxic proteins abrin and ricin in humans and mice. Int. J. Cancer 1983, 32, 515–521. [Google Scholar]
- Wang, Y.; Guo, L.; Zhao, K.; Chen, J.; Feng, J.; Sun, Y.; Li, Y.; Shen, B. Novel chimeric anti-ricin antibody C4C13 with neutralizing activity against ricin toxicity. Biotechnol. Lett. 2007, 29, 1811–1816. [Google Scholar]
- Pelat, T.; Hust, M.; Hale, M.; Lefranc, M.P.; Dubel, S.; Thullier, P. Isolation of a human-like antibody fragment (scFv) that neutralizes ricin biological activity. BMC Biotechnol. 2009, 9, 60–72. [Google Scholar]
- Pang, Y.P.; Park, J.G.; Wang, S.; Vummenthala, A.; Mishra, R.K.; McLaughlin, J.E.; Di, R.; Kahn, J.N.; Tumer, N.E.; Janosi, L.; et al. Small-molecule inhibitor leads of ribosome-inactivating proteins developed using the doorstop approach. PLoS One 2011, 6. [Google Scholar] [CrossRef]
- Bai, Y.; Monzingo, A.F.; Robertus, J.D. The X-ray structure of ricin A chain with a novel inhibitor. Arch. Biochem. Biophys. 2009, 483, 23–28. [Google Scholar]
- Hartley, P.G.; Alderton, M.R.; Dawson, R.M.; Wells, D. Ricin antitoxins based on lyotropic mesophases containing galactose amphiphiles. Bioconj. Chem. 2007, 18, 152–159. [Google Scholar]
- Dawson, R.M.; Alderton, M.R.; Wells, D.; Hartley, P.G. Monovalent and polyvalent carbohydrate inhibitors of ricin binding to a model of the cell-surface receptor. J. Appl. Toxicol. 2006, 26, 247–252. [Google Scholar]
- Stechmann, B.; Bai, S.K.; Gobbo, E.; Lopez, R.; Merer, G.; Pinchard, S.; Panigai, L.; Tenza, D.; Raposo, G.; Beaumelle, B.; et al. Inhibition of retrograde transport protects mice from lethal ricin challenge. Cell 2010, 141, 231–242. [Google Scholar]
- Smallshaw, J.E.; Richardson, J.A.; Pincus, S.; Schindler, J.; Vitetta, E.S. Preclinical toxicity and efficacy testing of RiVax, a recombinant protein vaccine against ricin. Vaccine 2005, 23, 4775–4784. [Google Scholar]
- Smallshaw, J.E.; Richardson, J.A.; Vitetta, E.S. RiVax, a recombinant ricin subunit vaccine, protects mice against ricin delivered by gavage or aeroso. Vaccine 2007, 25, 7459–7469. [Google Scholar]
- Smallshaw, J.E.; Vitetta, E.S. A lyophilized formulation of RiVax, a recombinant ricin subunit vaccine, retains immunogenicit. Vaccine 2010, 28, 2428–2435. [Google Scholar]
- Vitetta, E.S.; Smallshaw, J.E.; Coleman, E.; Jafri, H.; Foster, C.; Munford, R.; Schindler, J. A pilot clinical trial of a recombinant ricin vaccine in normal humans. Proc. Natl. Acad. Sci. USA 2006, 103, 2268–2273. [Google Scholar]
© 2011 by the authors; licensee MDPI, Basel, Switzerland This article is an open-access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Worbs, S.; Köhler, K.; Pauly, D.; Avondet, M.-A.; Schaer, M.; Dorner, M.B.; Dorner, B.G. Ricinus communis Intoxications in Human and Veterinary Medicine—A Summary of Real Cases. Toxins 2011, 3, 1332-1372. https://doi.org/10.3390/toxins3101332
Worbs S, Köhler K, Pauly D, Avondet M-A, Schaer M, Dorner MB, Dorner BG. Ricinus communis Intoxications in Human and Veterinary Medicine—A Summary of Real Cases. Toxins. 2011; 3(10):1332-1372. https://doi.org/10.3390/toxins3101332
Chicago/Turabian StyleWorbs, Sylvia, Kernt Köhler, Diana Pauly, Marc-André Avondet, Martin Schaer, Martin B. Dorner, and Brigitte G. Dorner. 2011. "Ricinus communis Intoxications in Human and Veterinary Medicine—A Summary of Real Cases" Toxins 3, no. 10: 1332-1372. https://doi.org/10.3390/toxins3101332
APA StyleWorbs, S., Köhler, K., Pauly, D., Avondet, M.-A., Schaer, M., Dorner, M. B., & Dorner, B. G. (2011). Ricinus communis Intoxications in Human and Veterinary Medicine—A Summary of Real Cases. Toxins, 3(10), 1332-1372. https://doi.org/10.3390/toxins3101332





