Dietary Choline and Betaine and Risk of CVD: A Systematic Review and Meta-Analysis of Prospective Studies
Abstract
:1. Introduction
2. Materials and Methods
2.1. Data Sources
2.2. Study Selection
2.3. Data Abstraction
2.4. Quality Scoring
2.5. Statistical Analysis
3. Results
3.1. Study Characteristics
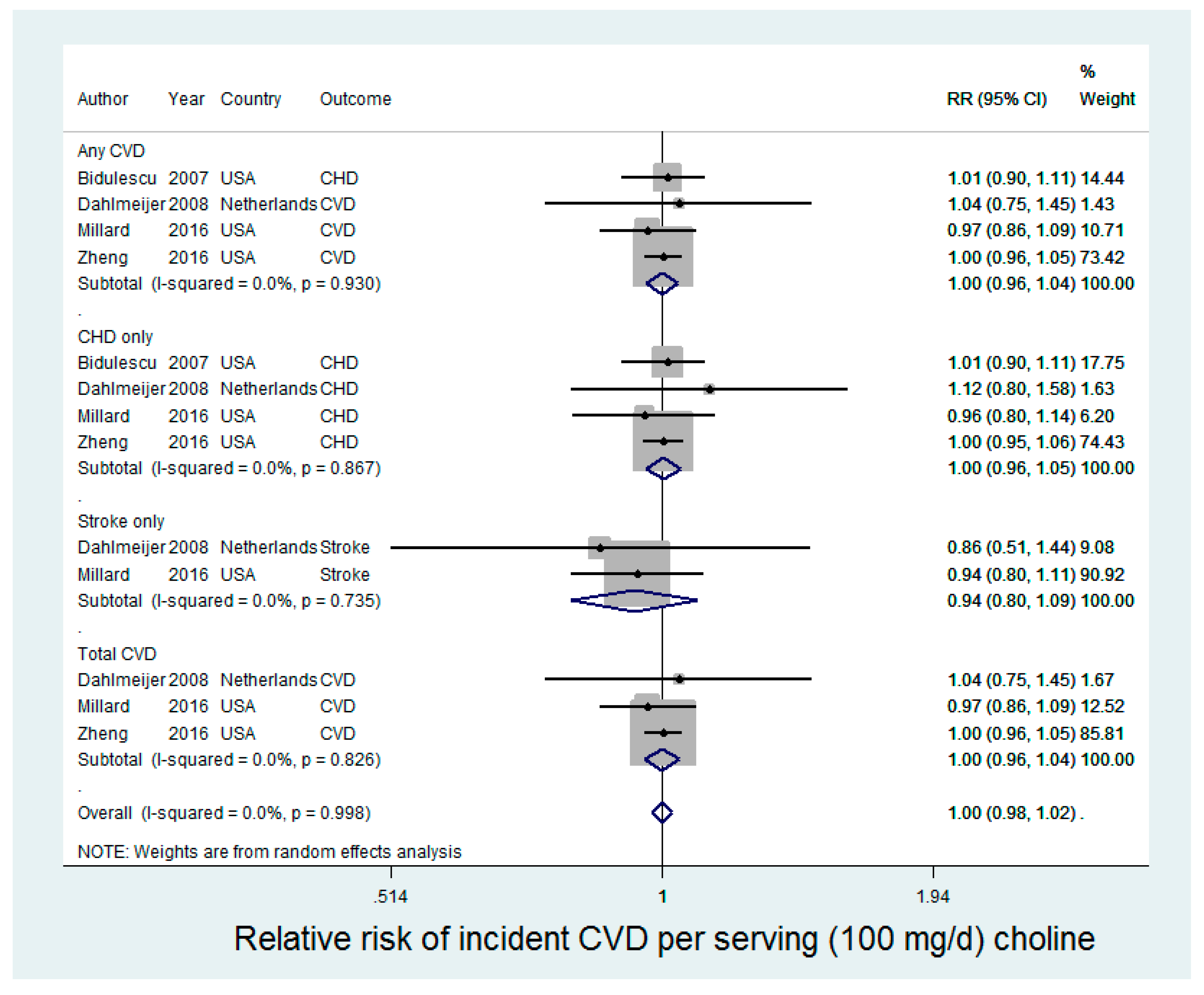
3.2. Choline and Incident CVD
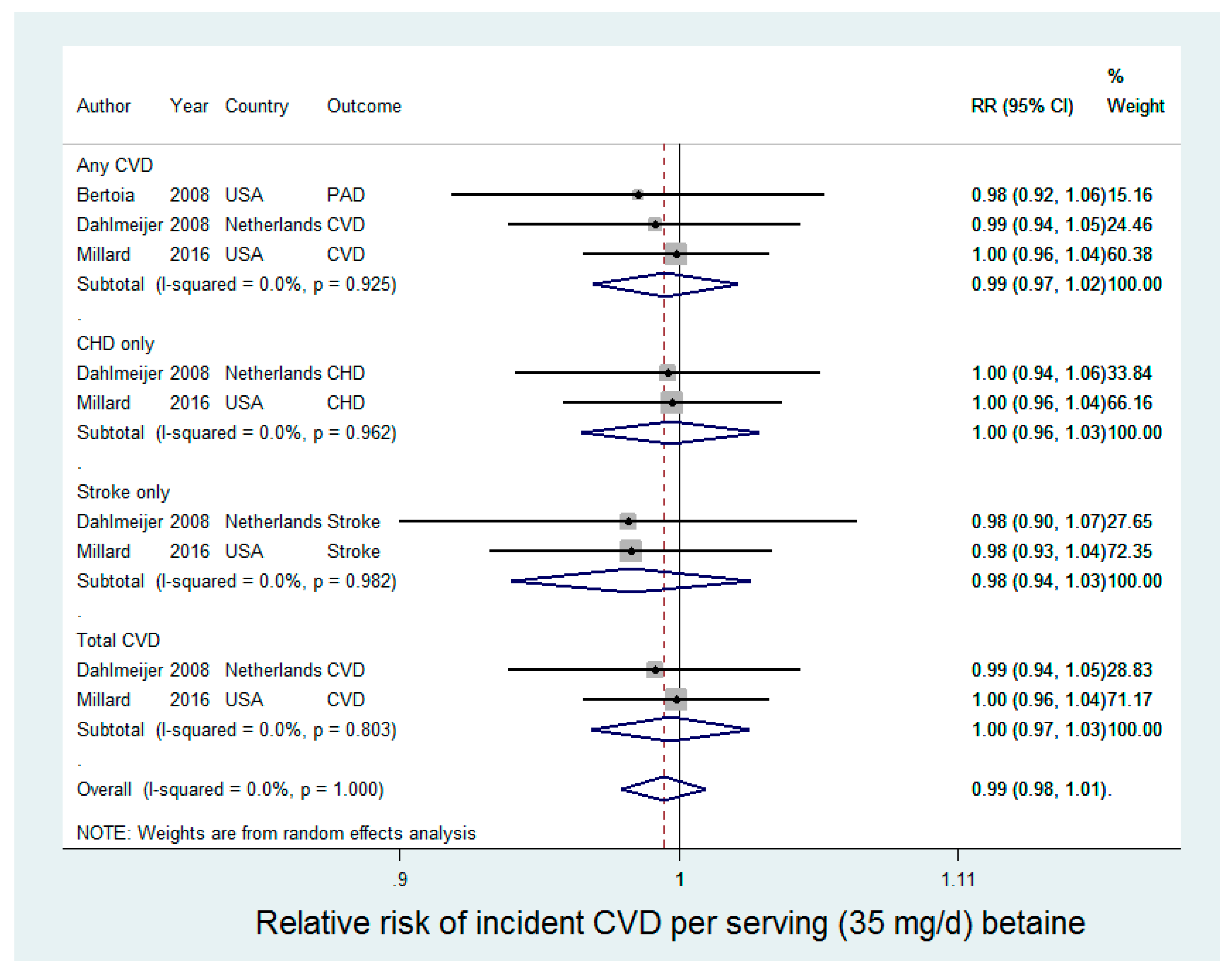
3.3. Betaine and Incident CVD
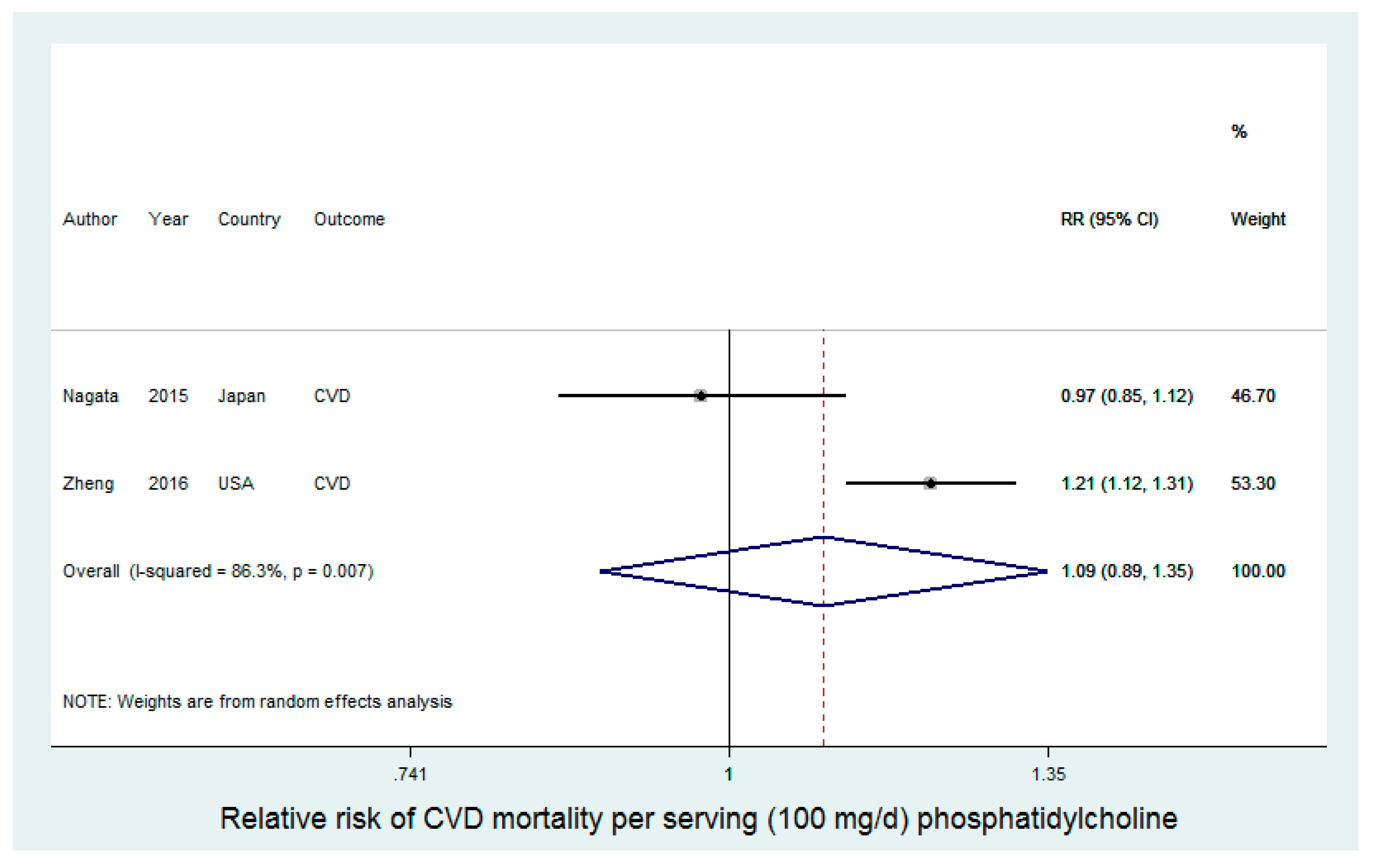
3.4. Choline and CVD Mortality
3.5. Betaine and CVD Mortality
3.6. Publication Bias
4. Discussion
Acknowledgments
Author Contributions
Conflicts of Interest
Appendix A. Database Search Strategy
References
- Tang, W.H.; Wang, Z.; Kennedy, D.J.; Wu, Y.; Buffa, J.A.; Agatisa-Boyle, B.; Li, X.S.; Levison, B.S.; Hazen, S.L. Gut microbiota-dependent trimethylamine n-oxide (TMAO) pathway contributes to both development of renal insufficiency and mortality risk in chronic kidney disease. Circ. Res. 2015, 116, 448–455. [Google Scholar] [CrossRef] [PubMed]
- Tang, W.H.; Wang, Z.; Levison, B.S.; Koeth, R.A.; Britt, E.B.; Fu, X.; Wu, Y.; Hazen, S.L. Intestinal microbial metabolism of phosphatidylcholine and cardiovascular risk. N. Engl. J. Med. 2013, 368, 1575–1584. [Google Scholar] [CrossRef] [PubMed]
- Tang, W.H.; Wang, Z.; Shrestha, K.; Borowski, A.G.; Wu, Y.; Troughton, R.W.; Klein, A.L.; Hazen, S.L. Intestinal microbiota-dependent phosphatidylcholine metabolites, diastolic dysfunction, and adverse clinical outcomes in chronic systolic heart failure. J. Card Fail. 2015, 21, 91–96. [Google Scholar] [CrossRef] [PubMed]
- Troseid, M.; Ueland, T.; Hov, J.R.; Svardal, A.; Gregersen, I.; Dahl, C.P.; Aakhus, S.; Gude, E.; Bjorndal, B.; Halvorsen, B.; et al. Microbiota-dependent metabolite trimethylamine-n-oxide is associated with disease severity and survival of patients with chronic heart failure. J. Intern. Med. 2015, 277, 717–726. [Google Scholar] [CrossRef] [PubMed]
- Koeth, R.A.; Wang, Z.; Levison, B.S.; Buffa, J.A.; Org, E.; Sheehy, B.T.; Britt, E.B.; Fu, X.; Wu, Y.; Li, L.; et al. Intestinal microbiota metabolism of l-carnitine, a nutrient in red meat, promotes atherosclerosis. Nat. Med. 2013, 19, 576–585. [Google Scholar] [CrossRef] [PubMed]
- Mente, A.; Chalcraft, K.; Ak, H.; Davis, A.D.; Lonn, E.; Miller, R.; Potter, M.A.; Yusuf, S.; Anand, S.S.; McQueen, M.J. The relationship between trimethylamine-n-oxide and prevalent cardiovascular disease in a multiethnic population living in canada. Can. J. Cardiol. 2015, 31, 1189–1194. [Google Scholar] [CrossRef] [PubMed]
- Senthong, V.; Li, X.S.; Hudec, T.; Coughlin, J.; Wu, Y.; Levison, B.; Wang, Z.; Hazen, S.L.; Tang, W.H. Plasma trimethylamine n-oxide, a gut microbe-generated phosphatidylcholine metabolite, is associated with atherosclerotic burden. J. Am. Coll. Cardiol. 2016, 67, 2620–2628. [Google Scholar] [CrossRef] [PubMed]
- Senthong, V.; Wang, Z.; Li, X.S.; Fan, Y.; Wu, Y.; Tang, W.H.; Hazen, S.L. Intestinal microbiota-generated metabolite trimethylamine-n-oxide and 5-year mortality risk in stable coronary artery disease: The contributory role of intestinal microbiota in a courage-like patient cohort. J. Am. Heart Assoc. 2016, 5. [Google Scholar] [CrossRef] [PubMed]
- Zeisel, S.H.; Mar, M.H.; Howe, J.C.; Holden, J.M. Concentrations of choline-containing compounds and betaine in common foods. J. Nutr. 2003, 133, 1302–1307. [Google Scholar] [PubMed]
- Hartiala, J.; Bennett, B.J.; Tang, W.H.; Wang, Z.; Stewart, A.F.; Roberts, R.; McPherson, R.; Lusis, A.J.; Hazen, S.L.; Allayee, H.; et al. Comparative genome-wide association studies in mice and humans for trimethylamine n-oxide, a proatherogenic metabolite of choline and l-carnitine. Arterioscler. Thromb. Vasc. Biol. 2014, 34, 1307–1313. [Google Scholar] [CrossRef] [PubMed]
- Bennett, B.J.; de Aguiar Vallim, T.Q.; Wang, Z.; Shih, D.M.; Meng, Y.; Gregory, J.; Allayee, H.; Lee, R.; Graham, M.; Crooke, R.; et al. Trimethylamine-n-oxide, a metabolite associated with atherosclerosis, exhibits complex genetic and dietary regulation. Cell. Metab. 2013, 17, 49–60. [Google Scholar] [CrossRef] [PubMed]
- Miller, C.A.; Corbin, K.D.; da Costa, K.A.; Zhang, S.; Zhao, X.; Galanko, J.A.; Blevins, T.; Bennett, B.J.; O’Connor, A.; Zeisel, S.H. Effect of egg ingestion on trimethylamine-n-oxide production in humans: A randomized, controlled, dose-response study. Am. J. Clin. Nutr. 2014, 100, 778–786. [Google Scholar] [CrossRef] [PubMed]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G.; Group, P. Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. PLoS Med. 2009, 6, e1000097. [Google Scholar] [CrossRef] [PubMed]
- Stroup, D.F.; Berlin, J.A.; Morton, S.C.; Olkin, I.; Williamson, G.D.; Rennie, D.; Moher, D.; Becker, B.J.; Sipe, T.A.; Thacker, S.B. Meta-analysis of observational studies in epidemiology: A proposal for reporting. Meta-analysis of observational studies in epidemiology (MOOSE) group. JAMA 2000, 283, 2008–2012. [Google Scholar] [CrossRef] [PubMed]
- Deeks, J.J.; Dinnes, J.; D’Amico, R.; Sowden, A.J.; Sakarovitch, C.; Song, F.; Petticrew, M.; Altman, D.G.; International Stroke Trial Collaborative Group; European Carotid Surgery Trial Collaborative Group. Evaluating non-randomised intervention studies. Health Technol. Assess. 2003, 7, 1–173. [Google Scholar] [CrossRef]
- Wells, G.A.; Shea, B.; O’Connell, D.; Peterson, J.; Welch, V.; Losos, M.; Tugwell, P. The Newcastle-Ottawa Scale (NOS) for Assessing the Quality of Nonrandomized Studies in Meta-analysis. Available online: http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp (accessed on 27 April 2017).
- Greenland, S.; Longnecker, M.P. Methods for trend estimation from summarized dose-response data, with applications to meta-analysis. Am. J. Epidemiol. 1992, 135, 1301–1309. [Google Scholar] [CrossRef] [PubMed]
- DerSimonian, R.; Laird, N. Meta-analysis in clinical trials. Control. Clin. Trials 1986, 7, 177–188. [Google Scholar] [CrossRef]
- Higgins, J.P.; Thompson, S.G. Quantifying heterogeneity in a meta-analysis. Stat. Med. 2002, 21, 1539–1558. [Google Scholar] [CrossRef] [PubMed]
- Egger, M.; Davey Smith, G.; Schneider, M.; Minder, C. Bias in meta-analysis detected by a simple, graphical test. BMJ 1997, 315, 629–634. [Google Scholar] [CrossRef] [PubMed]
- Cochrane Collaborative. Cochrane Handbook for Systematic Reviews of Interventions; Higgins, J.P.T., Green, S., Eds.; Cochrane Collaborative: London, UK, 2011. [Google Scholar]
- Bertoia, M.L.; Pai, J.K.; Cooke, J.P.; Joosten, M.M.; Mittleman, M.A.; Rimm, E.B.; Mukamal, K.J. Plasma homocysteine, dietary b vitamins, betaine, and choline and risk of peripheral artery disease. Atherosclerosis 2014, 235, 94–101. [Google Scholar] [CrossRef] [PubMed]
- Zheng, Y.; Li, Y.; Rimm, E.B.; Hu, F.B.; Albert, C.M.; Rexrode, K.M.; Manson, J.E.; Qi, L. Dietary phosphatidylcholine and risk of all-cause and cardiovascular-specific mortality among us women and men. Am. J. Clin. Nutr. 2016, 104, 173–180. [Google Scholar] [CrossRef] [PubMed]
- Millard, H.R.; Musani, S.K.; Dibaba, D.T.; Talegawkar, S.A.; Taylor, H.A.; Tucker, K.L.; Bidulescu, A. Dietary choline and betaine; associations with subclinical markers of cardiovascular disease risk and incidence of CVD, coronary heart disease and stroke: The Jackson Heart Study. Eur. J. Nutr. 2016. [Google Scholar] [CrossRef] [PubMed]
- Bidulescu, A.; Chambless, L.E.; Siega-Riz, A.M.; Zeisel, S.H.; Heiss, G. Usual choline and betaine dietary intake and incident coronary heart disease: The Atherosclerosis Risk in Communities (ARIC) study. BMC Cardiovasc. Disord. 2007, 7, 20. [Google Scholar] [CrossRef] [PubMed]
- Dalmeijer, G.W.; Olthof, M.R.; Verhoef, P.; Bots, M.L.; van der Schouw, Y.T. Prospective study on dietary intakes of folate, betaine, and choline and cardiovascular disease risk in women. Eur. J. Clin. Nutr. 2008, 62, 386–394. [Google Scholar] [CrossRef] [PubMed]
- Nagata, C.; Wada, K.; Tamura, T.; Konishi, K.; Kawachi, T.; Tsuji, M.; Nakamura, K. Choline and betaine intakes are not associated with cardiovascular disease mortality risk in Japanese men and women. J. Nutr. 2015, 145, 1787–1792. [Google Scholar] [CrossRef] [PubMed]
- Craciun, S.; Balskus, E.P. Microbial conversion of choline to trimethylamine requires a glycyl radical enzyme. Proc. Natl. Acad. Sci. USA 2012, 109, 21307–21312. [Google Scholar] [CrossRef] [PubMed]
- Zeisel, S.H.; da Costa, K.A. Choline: An essential nutrient for public health. Nutr. Rev. 2009, 67, 615–623. [Google Scholar] [CrossRef] [PubMed]
- Ueland, P.M. Choline and betaine in health and disease. J. Inherit. Metab. Dis. 2011, 34, 3–15. [Google Scholar] [CrossRef] [PubMed]
- Food and Nutrition Board; Institute of Medicine. Dietary Reference Intakes: Thiamin, Riboflavin, Niacin, Vitamin b-6, Vitamin b-12, Pantothenic Acid, Biotin, and Choline; National Academy Press: Washington, DC, USA, 1998; pp. 390–422. [Google Scholar]
- Patterson, K.Y.; Bhagwat, S.A.; Williams, J.R.; Howe, J.C.; Holden, J.M. USDA Database for the Choline Content of Common Foods; USDA: Beltsville, MD, USA, 2008.
- Cho, E.; Zeisel, S.H.; Jacques, P.; Selhub, J.; Dougherty, L.; Colditz, G.A.; Willett, W.C. Dietary choline and betaine assessed by food-frequency questionnaire in relation to plasma total homocysteine concentration in the Framingham Offspring Study. Am. J. Clin. Nutr. 2006, 83, 905–911. [Google Scholar] [PubMed]
- Meyer, K.A.; Benton, T.Z.; Bennett, B.J.; Jacobs, D.R., Jr.; Lloyd-Jones, D.M.; Gross, M.D.; Carr, J.J.; Gordon-Larsen, P.; Zeisel, S.H. Microbiota-dependent metabolite trimethylamine n-oxide and coronary artery calcium in the Coronary Artery Risk Development in Young Adults Study (CARDIA). J. Am. Heart Assoc. 2016, 5, e003970. [Google Scholar] [CrossRef] [PubMed]
- Bidulescu, A.; Chambless, L.E.; Siega-Riz, A.M.; Zeisel, S.H.; Heiss, G. Repeatability and measurement error in the assessment of choline and betaine dietary intake: The Atherosclerosis Risk in Ccommunities (ARIC) study. Nutr. J. 2009, 8, 14. [Google Scholar] [CrossRef] [PubMed]
- Willett, W.C.; Sampson, L.; Stampfer, M.J.; Rosner, B.; Bain, C.; Witschi, J.; Hennekens, C.H.; Speizer, F.E. Reproducibility and validity of a semiquantitative food frequency questionnaire. Am. J. Epidemiol. 1985, 122, 51–65. [Google Scholar] [CrossRef] [PubMed]
- Detopoulou, P.; Panagiotakos, D.B.; Antonopoulou, S.; Pitsavos, C.; Stefanadis, C. Dietary choline and betaine intakes in relation to concentrations of inflammatory markers in healthy adults: The ATTICA study. Am. J. Clin. Nutr. 2008, 87, 424–430. [Google Scholar] [PubMed]
| Author (Year) | Country | Study Sample | Study Period | Diet Assess-ment | Exposure Measure | Median Intake per Category (mg/Day) | Outcome Ascertain-ment | Outcome Measure | Sample Size | N Events | Total Person-Years | RR (95% CI) | Covariate Adjustment | Quality Score |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Bertoia (2014) [22] | United States | Women aged 44–69 at baseline (Nurses’ Health Study); men aged 40–75 at baseline (Health Professionals Follow-up Study) | 1990–2010 for women; 1986–2010 for men | FFQ | Total dietary choline (mg) and betaine (mg) | Women: (Choline: 246, 282, 307, 334, 377; Betaine: 67, 85, 101, 120, 159); Men: (Choline: 304, 348, 379, 415, 488; Betaine: 81, 102, 121, 144, 191) | Self-report with medical record adjudication | Peripheral artery disease | 116,852 (72,348 women, 44,504 men) | 790 (274 in women and 516 in men) | 1,302,032 (723,480 women, 578,552 men) | Q5 v Q1: Women: Choline: 1.07 (0.72–1.60); Betaine: 1.02 (0.69–1.52), Men: Choline: 1.24 (0.91–1.68); Betaine: 1.02 (0.77–1.35) | Age, total energy intake, race, smoking, hypertension, high cholesterol, diabetes, family history of MI, BMI, alcohol consumption, physical activity, aspirin use, postmenopausal hormone use (women only). | 6 |
| Bidulescu (2007) [25] | United States | Men and women in the biracial (European- and African-American) ARIC cohort, aged 45–64 at baseline | 1987–2002 | FFQ | Total dietary choline | Choline: 109, 250, 323, 403 | Self-report with medical record adjudication; community surveillance of hospital discharge and death certificate data | Coronary heart disease (CHD) | 14,430 | 1072 | 202,020 | Q4 v Q1: Choline: 1.09 (0.79–1.50) | Age, gender, education, total energy intake, dietary folate, methionine and vitamin B6, race, diabetes, field center, menopausal status (women only), dietary cholesterol, dietary intake of saturated fatty acids, animal fat, dietary fiber, and animal protein. | 8 |
| Dalmeijer (2008) [26] | Nether-lands | Female participants in a breast cancer screening sub-study of the Prospect-EPIC cohort | 1993–1997 (base-line) through 2004 | FFQ | Total dietary choline (mg) and betaine (mg) | Choline: 245, 282, 311, 356; Betaine: 162, 214, 257, 322 | Electronic hospital discharge database (Dutch Centre for Health Care Information) and death registries | CVD | 16,165 | 717 | 130,667 | Q4 v Q1: Choline: 1.04 (0.71–1.53); Betaine: 0.90 (0.69, 1.17) | Age; physical activity; smoking; diabetes; hypertension; BMI; hypercholesterolemia; systolic blood pressure; intake of total energy, protein, saturated fat, monounsaturated fat, polyunsaturated fat, alcohol, vitamin B2, vitamin B6, vitamin B12, folate, choline (betaine model), betaine (choline model). | 7 |
| CHD | 16,165 | 493 | 130,667 | Choline: 1.28 (0.86–1.91); Betaine: 0.95 (0.72, 1.25) | ||||||||||
| Stroke | 16,165 | 224 | 130,667 | Choline: 0.61 (0.33-1.13); Betaine: 0.83 (0.55, 1.25) | ||||||||||
| Millard (2016) [24] | United States | Men and women from the African-American Jackson Heart Study, aged 21–94 at baseline | 2000–2004 (base-line) through 2011 | FFQ | Total dietary choline (mg) and betaine (mg) | Choline: 125, 239, 332, 730; Betaine: 40.6, 87.4, 128, 478 | Self-report; hospital discharge; physician office visit records | CVD | 3924 | 153 | 35,316 | Q4 v Q1: Choline: 0.58 (0.28, 1.20); Betaine: 1.07 (0.66, 1.73) | Age, gender, smoking, systolic blood pressure, antihypertensive medication, fasting plasma glucose, total- to HDL-cholesterol ratio, dietary methionine, total energy intake. | 6 |
| CHD | 3924 | 124 | 35,316 | Choline: 0.66 (0.27, 1.60); Betaine: 1.20 (0.68, 2.11) | ||||||||||
| Stroke | 3924 | 75 | 35,316 | Choline: 0.41 (0.16, 1.09); Betaine: 0.56 (0.28, 1.14) | ||||||||||
| Nagata (2015) [27] | Japan | Men and women from the Takayama Study, aged 35+ at baseline | 1992–2008 | FFQ | Total dietary choline (mg) and betaine (mg) | Choline: Women: 307, 388, 442, 525, Men: 362, 445, 513, 614; Betaine: Women: 170, 239, 288, 377, Men: 208, 287, 350, 463 | Death certificates | CHD | 29,079 (15,724 women, 13,355 men) | 308 (154 women, 154 men) | Q4 v Q1: Women: Choline: 0.80 (0.40, 1.60); Betaine: 0.90 (0.53, 1.51), Men: Choline: 1.08 (0.57, 2.04); Betaine: 0.60 (0.37, 0.97) | Age; BMI; physical activity; smoking; education; marital status; menopausal status (women); vitamin supplement use; aspirin use; history of diabetes or hypertension; intakes of total energy, alcohol, saturated fat, polyunsaturated fat, folate, salt, and fruit. | 7 | |
| Stroke | 29,079 (15,724 women, 13,355 men) | 676 (349 women, 328 men) | 410,382 (227,083 women, 183,299 men) | Women: Choline: 1.02 (0.65, 1.60); Betaine: 1.04 (0.72, 1.49), Men: Choline: 0.98 (0.62, 1.55); Betaine: 0.84 (0.59, 1.20) | ||||||||||
| Zheng (2016) [23] | United States | 80,978 women (NHS), aged 34–59 at baseline; 39,434 men (HPFS), aged 40–75 at baseline | 1980–2012 women; 1986–2012 men | FFQ | Dietary phospha-tidyl-choline (mg) | Phosphatidyl-choline: Women: 130, 154,171, 191, 236; Men: 140, 166, 187, 212, 261 | Mortality: Death certificates and medical records; Morbidity: Self-report with confirmation by medical record review | CVD, mortality | 120,412 (80,978 women, 39,434 men) | 4357 (2297 women, 2060 men) | 2,828,658 (2,078,089 women, 748,911 men) | Pooled over gender: 1.26 (1.15, 1.39), Women: 1.19 (1.05, 1.35), Men: 1.39 (1.20, 1.61) | Age, BMI, race, marital status, menopausal status and HRT (women), family history of CVD, smoking, alcohol consumption, physical activity, presence of diabetes, hypertension, or hypercholesterolemia, regular aspirin use, dietary energy, trans fat, polyunsaturated-to-saturated fat ratio. | 7 |
| CVD, incidence | 120,412 | 15,344 | 3,199,530 | 1.00 (0.95, 1.06) | ||||||||||
| CHD, incidence | 120,412 | 11,305 | 3,201,620 | 1.01 (0.95, 1.07) |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Meyer, K.A.; Shea, J.W. Dietary Choline and Betaine and Risk of CVD: A Systematic Review and Meta-Analysis of Prospective Studies. Nutrients 2017, 9, 711. https://doi.org/10.3390/nu9070711
Meyer KA, Shea JW. Dietary Choline and Betaine and Risk of CVD: A Systematic Review and Meta-Analysis of Prospective Studies. Nutrients. 2017; 9(7):711. https://doi.org/10.3390/nu9070711
Chicago/Turabian StyleMeyer, Katie A., and Jonathan W. Shea. 2017. "Dietary Choline and Betaine and Risk of CVD: A Systematic Review and Meta-Analysis of Prospective Studies" Nutrients 9, no. 7: 711. https://doi.org/10.3390/nu9070711
APA StyleMeyer, K. A., & Shea, J. W. (2017). Dietary Choline and Betaine and Risk of CVD: A Systematic Review and Meta-Analysis of Prospective Studies. Nutrients, 9(7), 711. https://doi.org/10.3390/nu9070711




