Evidence Synthesis and Translation for Nutrition Interventions to Combat Micronutrient Deficiencies with Particular Focus on Food Fortification
Abstract
:1. Introduction
- (i)
- Nutrition-specific interventions (NSpI) “address the immediate causes of undernutrition, like inadequate dietary intake, and some of the underlying causes, like feeding practices and access to food” [8]. Food fortification and nutrient supplementation are prominent examples of these interventions that can rapidly increase an individual’s and targeted population’s exposure to a nutrient(s) [9].
- (ii)
- Nutrition-sensitive interventions (NSeI) “can address some of the underlying and basic causes of malnutrition by incorporating nutrition goals and actions from a wide range of sectors. They can also serve as delivery platforms for nutrition-specific interventions” [8]. Interventions may be located in sectors as diverse as agriculture [10], education [11], and social support [12]. In contrast to nutrient-oriented interventions, they generally focus on promoting food and diet quality and diversity to support consumption of a healthy, balanced diet.
2. Methods
2.1. Selection of Records
2.1.1. Systematic Reviews
2.1.2. Nutrition Guidelines and Policy Statements
“Category 1 interventions are interventions for which there are guidelines that have been recently approved by the WHO Guidelines Review Committee (GRC). Category 1 interventions also include those supported by recommendations and other forms of guidance that have been adopted or endorsed by the World Health Assembly”[21]
“Category 2 interventions are interventions for which systematic review(s) have been conducted but no recent guidelines are yet available that have been approved by the WHO Guidelines Review Committee”[21]
“Category 3 interventions are interventions for which available evidence is limited and systematic reviews have not yet been conducted”[21]
2.1.3. Implementation of Nutrition Actions
2.2. Data Extraction and Analysis
2.2.1. Systematic Reviews
2.2.2. Nutrition Guidelines and Policy Statements
2.2.3. Implementation of Nutrition Actions
3. Results
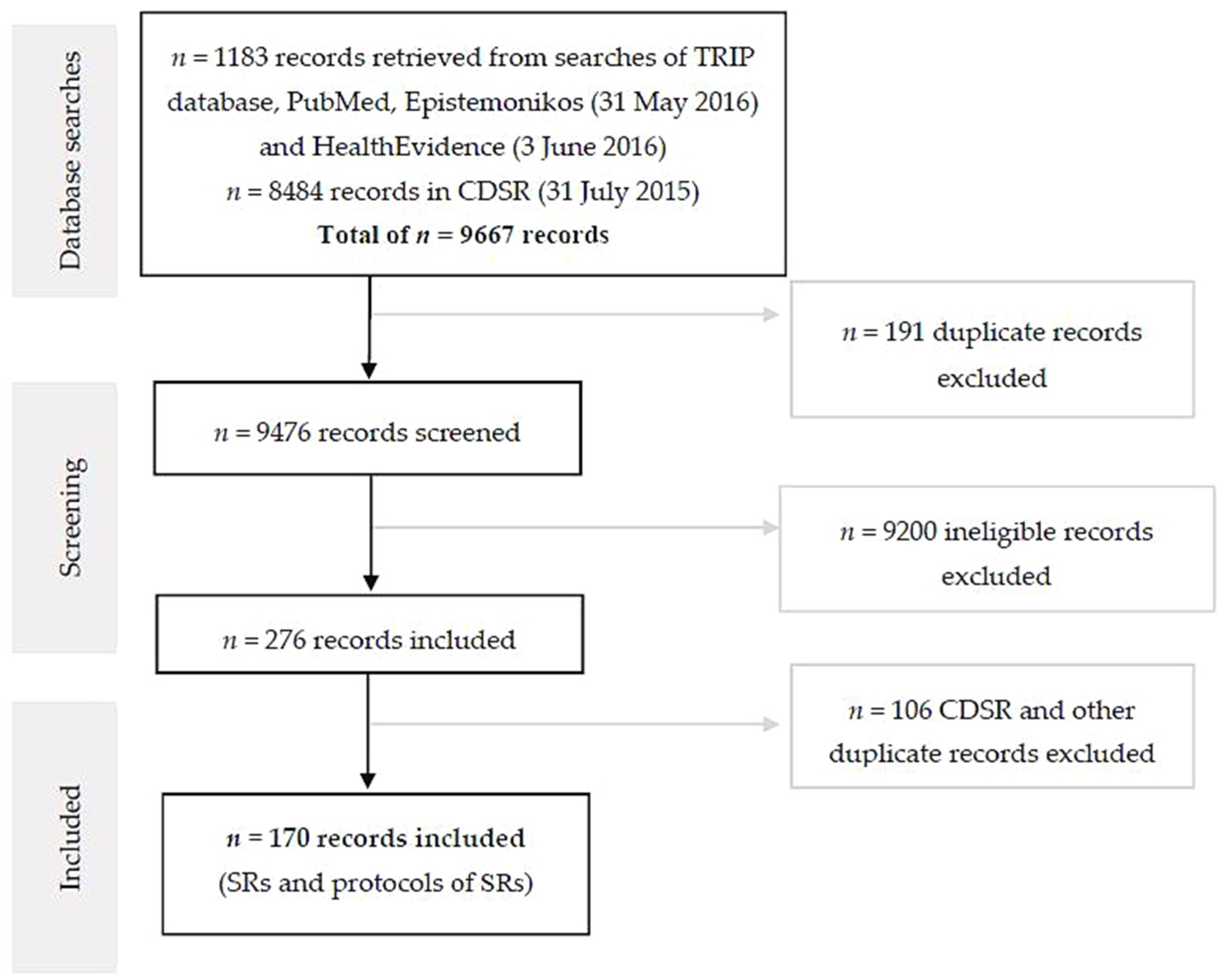
3.1. Systematic Reviews
3.2. Nutrition Guidelines and Policy Statements
3.3. Implementation of Nutrition Actions
4. Discussion
5. Conclusions
Author Contributions
Conflicts of Interest
Appendix A
| Database | Search Query | |
|---|---|---|
| PubMed | #1 | (Vitamin*[tiab] OR mineral*[tiab] OR nutrient*[tiab] OR micronutrient*[tiab]) AND (deficiency[tiab] OR deficiencies[tiab] OR malnutrition[tiab] OR undernutrition[tiab]) |
| #2 | “systematic review”[tiab] OR meta-analysis[pt] OR meta-analysis[tiab] | |
| #3 | #1 AND #2 | |
| Epistemonikos | ((title: ((Vitamin* OR mineral* OR nutrient* OR micronutrient*) AND (deficiency OR deficiencies OR malnutrition OR undernutrition)) OR abstract: ((Vitamin* OR mineral* OR nutrient* OR micronutrient*) AND (deficiency OR deficiencies OR malnutrition OR undernutrition))), by publication type: systematic reviews | |
| Health Evidence | ((Vitamin OR vitamins OR mineral OR minerals OR nutrient OR nutrients OR micronutrient OR micronutrients) AND (deficiency OR deficiencies OR malnutrition OR undernutrition)) | |
| TRIP | (Vitamin OR vitamins OR mineral OR minerals OR nutrient OR nutrients OR micronutrient OR micronutrients) AND (deficiency OR deficiencies OR malnutrition OR undernutrition) | |
| CDSR | Entire database screened previously for another study | |
| CDSR: Cochrane Database of Systematic Reviews | ||
References
- Food and Agriculture Organization of the United Nations (FAO); World Health Organization (WHO). Second International Conference on Nutrition: Conference Outcome Document: Rome Declaration on Nutrition; FAO: Rome, Italy; WHO: Geneva, Switzerland, 2014; Available online: http://www.fao.org/3/a-ml542e.pdf (accessed on 21 June 2016).
- Food and Agriculture Organization of the United Nations (FAO); World Health Organization (WHO). Second International Conference on Nutrition: Conference Outcome Document: Framework for Action; FAO: Rome, Italy; WHO: Geneva, Switzerland, 2014; Available online: http://www.fao.org/3/a-mm215e.pdf (accessed on 21 June 2016).
- General Assembly Proclaims the Decade of Action on Nutrition. Available online: http://www.who.int/nutrition/GA_decade_action/en/ (accessed on 20 June 2016).
- Codex Alimentarius Commission. General Principles for the Addition of Essential Nutrients to Foods. CAC/GL 9-1987; Codex Alimentarius Commission: Rome, Italy, 1987. [Google Scholar]
- Why Fortify? Available online: http://www.ffinetwork.org/why_fortify/index.html (accessed on 20 June 2016).
- Large Scale Food Fortification. Available online: http://www.gainhealth.org/programs/initiatives/ (accessed on 20 June 2016).
- Lawrence, M. Food Fortification: The Evidence, Ethics, and Politics of Adding Nutrients to Food; Oxford University Press: Oxford, UK, 2013. [Google Scholar]
- The United Nations Children’s Emergency Fund (UNICEF). Multi-Sectoral Approaches to Nutrition: Nutrition-Specific and Nutrition-Sensitive Interventions to Accelerate Progress; UNICEF: New York, NY, USA, 2014; Available online: http://www.unicef.org/eu/files/101322_000_Unicef_Brief_NutritionOverview_A4_v1r15.pdf (accessed on 5 June 2016).
- World Food Programme. Nutrition at the World Food Programme: Programming for Nutrition-Specific Interventions; World Food Programme: Rome, Italy, 2012; Available online: https://www.wfp.org/content/nutrition-world-food-programme-programming-nutrition-specific-interventions (accessed on 5 June 2016).
- Girard, A.W.; Self, J.L.; McAuliffe, C.; Olude, O. The effects of household food production strategies on the health and nutrition outcomes of women and young children: A systematic review. Paediatr. Perinat. Epidemiol. 2012, 26, 205–222. [Google Scholar] [CrossRef] [PubMed]
- Olney, D.K.; Pedehombga, A.; Ruel, M.T.; Dillon, A. A 2-year integrated agriculture and nutrition and health behavior change communication program targeted to women in burkina faso reduces anemia, wasting, and diarrhea in children 3–12.9 months of age at baseline: A Cluster-Randomized Controlled Trial. J. Nutr. 2015. [Google Scholar] [CrossRef] [PubMed]
- Ruel, M.T.; Alderman, H. Nutrition-sensitive interventions and programmes: How can they help to accelerate progress in improving maternal and child nutrition? Lancet 2013, 382, 536–551. [Google Scholar] [CrossRef]
- Nair, M.K.; Augustine, L.F.; Konapur, A. Food-Based Interventions to Modify Diet Quality and Diversity to Address Multiple Micronutrient Deficiency. Front. Public Health 2015, 3, 1–14. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization; Food and Agriculture Organization of the United Nations. Guidelines on food Fortification with Micronutrients. Available online: http://www.who.int/nutrition/publications/guide_food_fortification_micronutrients.pdf (access on 21 June 2016).
- Lefroy, J.; Ruel, M.; Verhofstadt, E.; Olney, D. The Micronutrient Impact of Multisectoral Programs Focusing on Nutrition: Examples from Conditional Cash Transfer, Microcredit with Education, and Agricultural Programs; International Food Policy Research Institute: Washington, DC, USA, 2008. [Google Scholar]
- International Food Policy Research Institute. Global Nutrition Report 2015: Actions and Accountability to Advance Nutrition and Sustainable Development; International Food Policy Research Institute: Washington, DC, USA, 2015; Available online: http://globalnutritionreport.org/the-report/the-report-2015/ (accessed on 3 December 2015).
- Uauy, R. Defining and addressing the nutritional needs of populations. Public Health Nutr. 2005, 8, 773–780. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization (WHO). WHO Handbook for Guideline Development, 2nd ed.; WHO: Geneva, Switzerland, 2014; Available online: http://www.who.int/kms/handbook_2nd_ed.pdf?ua=1 (accessed on 21 June 2016).
- Young, T.; Rohwer, A.; Volmink, J.; Clarke, M. What are the effects of teaching evidence-based health care (EBHC)? Overview of systematic reviews. PLoS ONE 2014, 9, 1–13. [Google Scholar] [CrossRef] [PubMed]
- E-Library of Evidence for Nutrition Actions (eLENA). Available online: http://www.who.int/elena/en/ (accessed on 6 June 2016).
- Interventions by Category Geneva. Available online: http://www.who.int/elena/categories/en/ (accessed on 6 June 2016).
- Global Database on the Implementation of Nutrition Actions (GINA). Available online: http://www.who.int/nutrition/gina/en/ (accessed on 6 June 2016).
- Lozoff, B.; Castillo, M.; Clark, K.M.; Smith, J.B. Iron-fortified vs. low-iron infant formula: Developmental outcome at 10 years. Arch. Pediatr. Adolesc. Med. 2012, 166, 208–215. [Google Scholar] [CrossRef] [PubMed]
- Datta, M.; Vitolins, M.Z. Food fortification and supplement use—Are there health implications? Crit. Rev. Food Sci. Nutr. 2016, 56, 2149–2159. [Google Scholar] [CrossRef] [PubMed]
- Nestle, M. Go forth and fortify. In Food Politics: How the Food Industry Influences Nutrition and Health; University of California Press: Berkley, CA, USA, 2013; pp. 285–298. [Google Scholar]
- Fardet, A.; Rock, E. Toward a new philosophy of preventive nutrition: From a reductionist to a holistic paradigm to improve nutritional recommendations. Adv. Nutr. 2014, 5, 430–446. [Google Scholar] [CrossRef] [PubMed]
- Pelletier, D.L.; Porter, C.M.; Aarons, G.A.; Wuehler, S.E.; Neufeld, L.M. Expanding the frontiers of population nutrition research: New questions, new methods, and new approaches. Adv. Nutr. 2013, 4, 92–114. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Addressing and Managing Conflicts of Interest: Report of a Technical Consultation Convened in Geneva, Switzerland, on 8–9 October 2015; WHO: Geneva, Switzerland, 2016; Available online: http://apps.who.int/iris/bitstream/10665/206554/1/9789241510530_eng.pdf (accessed on 15 June 2016).
| Type of Intervention | Number of Records |
|---|---|
| Fortification only | 29 (17.0%) |
| Supplementation only | 108 (63.5%) |
| Other interventions | 12 (7.0%) |
| Combined interventions | 21 (12.3%) |
| Total | 170 |
| Level of Supporting Evidence | Type of Intervention | |||
|---|---|---|---|---|
| Fortification | Supplementation | Other Interventions | Total | |
| Category 1 intervention | 3 | 21 | 13 | 37 |
| Category 2 intervention | 1 | 13 | 15 | 29 |
| Category 3 intervention | 3 | 0 | 0 | 3 |
| Total | 7 | 34 | 28 | 69 |
| Number of Actions | Nutrition Specific Actions | Nutrition Sensitive Actions | |
|---|---|---|---|
| Fortification | 293 | 292 | 1 |
| Supplementation | 438 | 438 | 0 |
| Other nutrition actions | 915 | 439 | 476 |
| Total | 1646 | 1169 | 477 |
© 2016 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC-BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lawrence, M.; Wingrove, K.; Naude, C.; Durao, S. Evidence Synthesis and Translation for Nutrition Interventions to Combat Micronutrient Deficiencies with Particular Focus on Food Fortification. Nutrients 2016, 8, 555. https://doi.org/10.3390/nu8090555
Lawrence M, Wingrove K, Naude C, Durao S. Evidence Synthesis and Translation for Nutrition Interventions to Combat Micronutrient Deficiencies with Particular Focus on Food Fortification. Nutrients. 2016; 8(9):555. https://doi.org/10.3390/nu8090555
Chicago/Turabian StyleLawrence, Mark, Kate Wingrove, Celeste Naude, and Solange Durao. 2016. "Evidence Synthesis and Translation for Nutrition Interventions to Combat Micronutrient Deficiencies with Particular Focus on Food Fortification" Nutrients 8, no. 9: 555. https://doi.org/10.3390/nu8090555
APA StyleLawrence, M., Wingrove, K., Naude, C., & Durao, S. (2016). Evidence Synthesis and Translation for Nutrition Interventions to Combat Micronutrient Deficiencies with Particular Focus on Food Fortification. Nutrients, 8(9), 555. https://doi.org/10.3390/nu8090555





