Household Food Insecurity Is Associated with Adverse Mental Health Indicators and Lower Quality of Life among Koreans: Results from the Korea National Health and Nutrition Examination Survey 2012–2013
Abstract
:1. Introduction
2. Methods and Materials
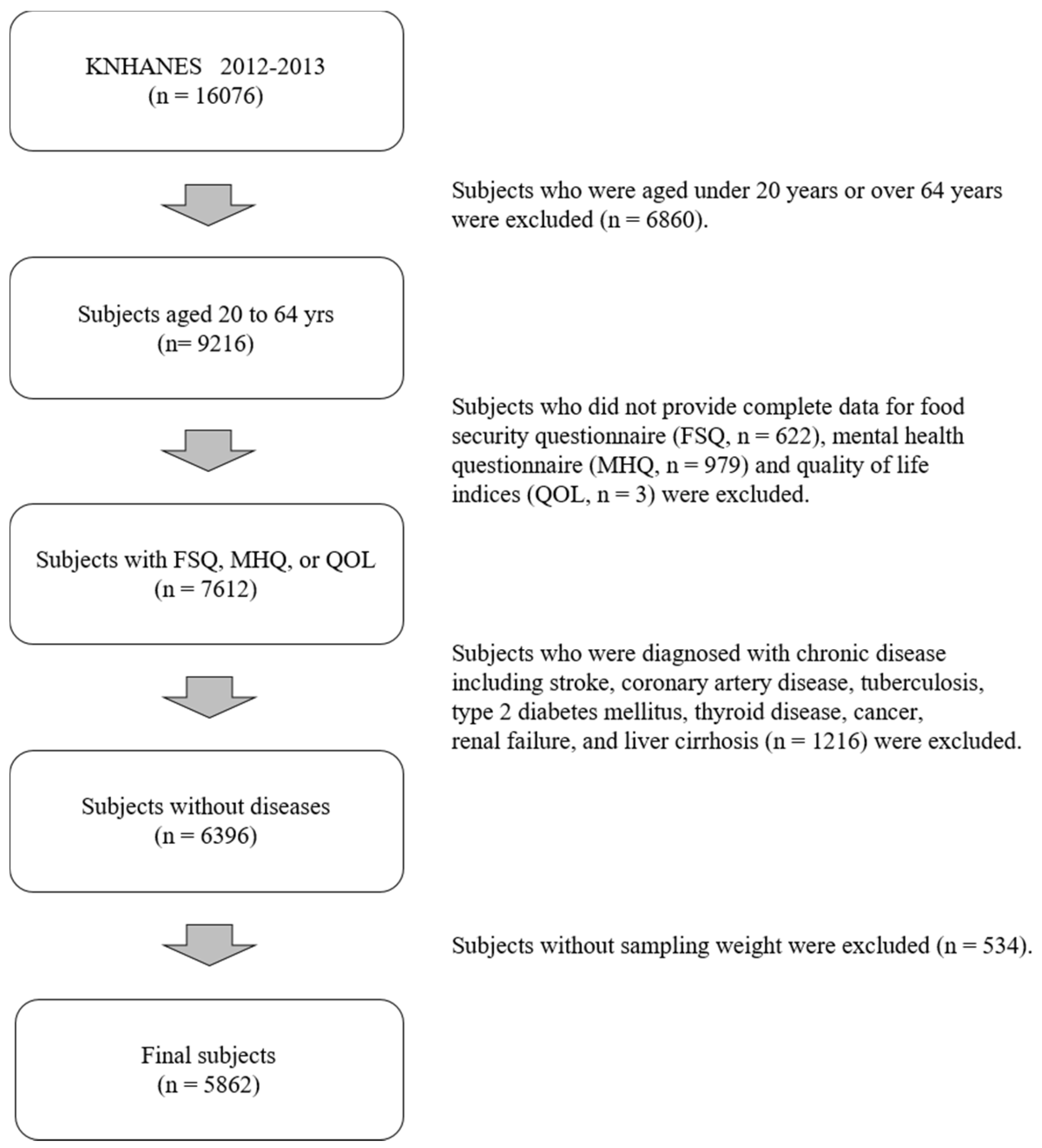
2.1. Study Population
2.2. Participants’ General Characteristics
2.3. Dietary Assessment
2.4. Household Food Security
2.5. Mental Health Indicators and Quality of Life
2.6. Statistical Analysis
3. Results
3.1. Participants’ Characteristics
3.2. Odds Ratios for Mental Health Indicators per Types of Household Food Insecurity
3.3. Odds Ratios for the Quality of Life per Types of Household Food Security
4. Discussion
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Food and Agriculture Organization of the United Nations; International Fund for Agricultural Development; World Food Programme. The State of Food Insecurity in the World 2015: Meeting the 2015 International Hunger Targets: Taking Stock of Uneven Progress. Available online: http://www.fao.org/3/a-i4646e.pdf (accessed on 5 May 2016).
- Gundersen, C. Food insecurity is an ongoing national concern. Adv. Nutr. 2013, 4, 36–41. [Google Scholar] [CrossRef] [PubMed]
- Food and Agriculture Organization of the United Nations. An Introduction to the Basic Concepts of Food Security. Available online: http://www.fao.org/docrep/013/al936e/al936e00.pdf (accessed on 7 May 2016).
- Coleman-Jensen, A.; Gregory, C.; Singh, A. Household food security in the United States in 2013. Available online: http://www.ers.usda.gov/publications/err-economic-research-report/err173.aspx (accessed on 15 June 2016).
- Kim, H.J.; Oh, K. Household food insecurity and dietary intake in Korea: Results from the 2012 Korea National Health and Nutrition Examination Survey. Public Health Nutr. 2015, 1, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Shen, X.; Gao, X.; Tang, W.; Mao, X.; Huang, J.; Cai, W. Food insecurity and malnutrition in Chinese elementary school students. Br. J. Nutr. 2015, 18, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Shariff, Z.M.; Khor, G.L. Obesity and household food insecurity: Evidence from a sample of rural households in Malaysia. Eur. J. Clin. Nutr. 2005, 59, 1049–1058. [Google Scholar] [CrossRef] [PubMed]
- Pérez-Escamilla, R.; Villalpando, S.; Shamah-Levy, T.; Méndez-Gómez Humarán, I. Household food insecurity, diabetes, and hypertension among Mexican adults: Results from Ensanut 2012. Salud Publica Mex 2014, 56 (Suppl. S1), s62–s70. [Google Scholar] [PubMed]
- Seligman, H.K.; Bindman, A.; Vittinghoff, E.; Kanaya, A.M.; Kushel, M.B. Food insecurity is associated with diabetes mellitus: Results from the National Health Examination and Nutritional Examination Survey 1999–2002. J. Gen. Intern. Med. 2007, 22, 1018–1023. [Google Scholar] [CrossRef] [PubMed]
- Kirkpatrick, S.S.; McIntyre, L.; Potestio, M. Child hunger and long-term adverse consequences for health. Arch. Pediatr. Adolesc. Med. 2010, 164, 754–762. [Google Scholar] [CrossRef] [PubMed]
- Gany, F.; Lee, T.; Ramirez, J.; Massie, D.; Moran, A.; Crist, M.; McNish, T.; Winkel, G.; Leng, J.C. Do our patients have enough to eat? Food insecurity among urban low-income cancer patients. J. Health Care Poor Underserved 2014, 25, 1153–1168. [Google Scholar] [CrossRef] [PubMed]
- Davison, K.M.; Kaplan, B.J. Food insecurity in adults with mood disorders: Prevalence estimates and associations with nutritional and psychological health. Ann. Gen. Psychiatry 2015, 14, 21. [Google Scholar] [CrossRef] [PubMed]
- Leung, C.W.; Epel, E.S.; Willett, W.C.; Rimm, E.B.; Laraia, B.A. Household food insecurity is positively associated with depression among low-income supplemental nutrition assistance program participants and income-eligible nonparticipants. J. Nutr. 2015, 145, 622–627. [Google Scholar] [CrossRef] [PubMed]
- Wang, E.A.; McGinnis, K.A.; Goulet, J.; Bryant, K.; Gibert, C.; Leaf, D.A.; Mattocks, K.; Fiellin, L.E.; Vogenthaler, N.; Justice, A.C.; et al. Food insecurity and health: Data from the Veterans Aging Cohort Study. Public Health Rep. 2015, 130, 261–268. [Google Scholar] [PubMed]
- Howard, L. Does food insecurity at home affect non-cognitive performance at school? A longitudinal analysis of elementary student classroom behavior. Econ. Educ. Rev. 2011, 30, 157–176. [Google Scholar] [CrossRef]
- Alaimo, K.; Olson, C.M.; Frongillo, E.A. Family food insufficiency, but not low family income, is positively associated with dysthymia and suicide symptoms in adolescents. J. Nutr. 2002, 132, 719–725. [Google Scholar] [PubMed]
- Vogenthaler, N.S.; Hadley, C.; Lewis, S.J.; Rodriguez, A.E.; Metsch, L.R.; del Rio, C. Food insufficiency among HIV-infected crack-cocaine users in Atlanta and Miami. Public Health Nutr. 2010, 13, 1478–1484. [Google Scholar] [CrossRef] [PubMed]
- Simmons, L.A.; Modesitt, S.C.; Brody, A.C.; Leggin, A.B. Food insecurity among cancer patients in Kentucky: A pilot study. J. Oncol. Pract. 2006, 2, 274–279. [Google Scholar] [CrossRef] [PubMed]
- Heflin, C.M.; Siesfert, K.; Willams, D.R. Food insufficiency and women’s mental health: Findings from a 3-year panel of welfare recipients. Soc. Sci. Med. 2005, 61, 1971–1982. [Google Scholar] [CrossRef] [PubMed]
- Korean Ministry of Health and Welfare. Korea Health Statistics 2013: Korea National Health and Nutrition Examination Survey (KNHANES). Available online: http://cdc.go.kr/CDC/cms/content/mobile/14/28314_view.html (accessed on 25 June 2016).
- Byeon, H.W. Comparative analysis of unweighted sample design and complex sample design related to the exploration of potential risk factors of dysphonia. J. Korea Acad. Ind. Cooperation Soc. 2012, 13, 2251–2258. [Google Scholar] [CrossRef]
- Craig, C.L.; Marshall, A.L.; Sjöström, M.; Bauman, A.E.; Booth, M.L.; Ainsworth, B.E.; Pratt, M.; Ekelund, U.; Yngve, A.; Sallis, J.F.; et al. International physical activity questionnaire: 12-country reliability and validity. Med. Sci. Sports Exerc. 2003, 35, 1381–1395. [Google Scholar] [CrossRef] [PubMed]
- Rural Resources Development Institute. Food Composition Table, 7th ed.; Rural Resources Development Institute: Suwon, Korea, 2006. [Google Scholar]
- Rural Resources Development Institute. Food Composition Table, 8th ed.; Rural Resources Development Institute: Suwon, Korea, 2011. [Google Scholar]
- Ministry of Health and Welfare. Dietary Reference Intakes for Koreans 2015; Ministry of Health and Welfare: Sejong, Korea, 2015.
- Kim, K.; Hong, S.A.; Kwon, S.O.; Choi, B.Y.; Kim, G.Y.; Oh, S.Y. Validation of food security measures for the Korean National Health and Nutrition Examination Survey. Korean J. Community Nutr. 2011, 16, 771–781. [Google Scholar] [CrossRef]
- Korean Centers for Disease Control and Prevention. Validation and Reliability Evaluation for EQ-5D in Korea. Available online: http://www.cdc.go.kr/CDC/info/CdcKrInfo0201.jsp?menuIds=HOME001-MNU1155-MNU1083-MNU1375-MNU0025%20&fid=28&q_valu=&cid=1742&pageNum=1 (accessed on 1 June 2016).
- Cho, G.E.; Lim, D.H.; Baek, M.; Lee, H.; Kim, S.J.; Kang, S.W. Epidemiologic survey committee of the Korean Ophthalmological Society. Visual impairment of Korean population: Prevalence and impact on mental health. Investig. Ophthalmol. Vis. Sci. 2015, 8, 4375–4381. [Google Scholar]
- Rim, T.H.; Lee, C.S.; Lee, S.C.; Chung, B.; Kim, S.S. Epidemiologic Survey Committee of the Korean Ophthalmological Society. Influence of visual acuity on suicidal ideation, suicide attempts, and depression in South Korea. Br. J. Ophthalmol. 2015, 99, 1112–1119. [Google Scholar] [CrossRef] [PubMed]
- Jeon, G.S.; Jang, S.N.; Rhee, S.J.; Kawachi, I.; Cho, S.I. Gender differences in correlates of mental health among elderly Koreans. J. Gerontol. B Psychol. Sci. Soc. Sci. 2007, 62, S323–S329. [Google Scholar] [CrossRef] [PubMed]
- Kaplan, R.M.; Anderson, J.P.; Wingard, D.L. Gender differences in health-related quality of life. Health Psychol. 1991, 10, 86–93. [Google Scholar] [CrossRef] [PubMed]
- Mercier, C.; Péladeau, N.; Tempier, R. Age, gender and quality of life. Community Ment. Health J. 1998, 34, 487–500. [Google Scholar] [CrossRef] [PubMed]
- Lasheras, C.; Patterson, A.M.; Casado, C. Effects of education on the quality of life, diet, and cardiovascular risk factors in an elderly Spanish community population. Exp. Aging Res. 2001, 27, 257–270. [Google Scholar] [CrossRef] [PubMed]
- Frischknecht, U.; Sabo, T.; Mann, K. Improved drinking behavior improves quality of life: A follow-up in alcohol-dependent subjects 7 years after treatment. Alcohol. Alcohol. 2013, 48, 579–584. [Google Scholar] [CrossRef] [PubMed]
- Teoman, N.; Ozcan, A.; Acar, B. The effect of exercise on physical fitness and quality of life in postmenopausal women. Maturitas 2004, 47, 71–77. [Google Scholar] [CrossRef]
- Mulder, I.; Tijhuis, M.; Smit, H.A.; Kromhout, D. Smoking cessation and quality of life: The effect of amount of smoking and time since quitting. Prev. Med. 2001, 33, 653–660. [Google Scholar] [CrossRef] [PubMed]
- Maluccio, J.A.; Palermo, T.; Kadiyala, S.; Rawar, R. Improving health-related quality of life among people living with HIV: Results from an impact evaluation of a food assistance program in Uganda. PLoS ONE 2015, 10, e0135879. [Google Scholar] [CrossRef] [PubMed]
- Lee, S. Marital status, gender, and subjective quality of life in Korea. Dev. Soc. 1998, 27, 35–49. [Google Scholar] [PubMed]
- Zhang, Y.; Ou, F.; Gao, S.; Gao, Q.; Hu, L.; Liu, Y. Effect of low income on health-related quality of life: A cross-sectional study in northeast China. Asia Pac. J. Public Health 2015, 27. [Google Scholar] [CrossRef] [PubMed]
- Melchior, M.; Caspi, A.; Howard, L.M.; Ambler, A.P.; Bolton, H.; Mountain, N.; Moffitt, T.E. Mental health context of food insecurity: A representative cohort of families with young children. Pediatrics 2009, 124, e564–e572. [Google Scholar] [CrossRef] [PubMed]
- Carter, K.N.; Kruse, K.; Blakely, T.; Collings, S. The association of food security with psychological distress in New Zealand and any gender differences. Soc. Sci. Med. 2011, 72, 1463–1471. [Google Scholar] [CrossRef] [PubMed]
- Grisaru, N.; Kaufman, R.; Mirsky, J.; Wirztum, E. Food insecurity and mental health: A pilot study of patients in a psychiatric emergency unit in Israel. Community Ment. Health J. 2011, 47, 513–519. [Google Scholar] [CrossRef] [PubMed]
- Kim, K.; Frongillo, E.A. Participation in food assistance programs modifies the relation of food insecurity with weight and depression in elders. J. Nutr. 2007, 137, 1005–1010. [Google Scholar] [PubMed]
- Gany, F.; Leng, J.; Ramirez, J.; Phillips, S.; Aragones, A.; Roberts, N.; Mujawar, M.I.; Costas-Muniz, R. Health-related quality of life of food-insecure ethnic minority patients with cancer. J. Oncol. Pract. 2015, 11, 396–402. [Google Scholar] [CrossRef] [PubMed]
- Kim, J.; Lee, Y. Frequency of dairy consumption and functional disability in older persons. J. Nutr. Health Aging 2011, 15, 795–800. [Google Scholar] [CrossRef] [PubMed]
- Kim, J.; Lee, Y.; Lee, S.Y. Legumes and soy products consumption and functional disability in older women. Maturita 2011, 69, 268–272. [Google Scholar] [CrossRef] [PubMed]
- Kim, J.; Lee, Y.; Lee, S.Y.; Kim, Y.O.; Chung, Y.S.; Park, S.B. Dietary patterns and functional disability in older Korean adults. Maturitas 2013, 76, 160–164. [Google Scholar] [CrossRef] [PubMed]
- Lopes, T.S.; Sichieri, R.; Salles-Costa, R.; Veiga, G.V.; Pereira, R.A. Family food insecurity and nutritional risk in adolescents from a low-income area of Rio de Janeiro, Brazil. J. Biosoc. Sci. 2013, 45, 661–674. [Google Scholar] [CrossRef] [PubMed]
- Organization for Economic Co-operation and Development. How’s Life? 2015, Measuring Well-Being. Available online: http://www.ifutureo.org/documentacion/hows%20life%202015.pdf (accessed on 20 June 2016).
- Organization for Economic Co-operation and Development. OECD Fact Book 2013: Economic, Environmental and Social Statistics. Available online: http://www.oecd-ilibrary.org/economics/oecd-factbook-2013_factbook-2013-en (accessed on 20 June 2016).
- Ministry of Health & Welfare. The 1st National Nutrition Care/Management in Korea. Available online: http://www.korea.kr/archive/expDocView.do?docId=32234 (accessed on 12 June 2016).
- Ministry of Health & Welfare. Elderly Care Service. Available online: http://www.129.go.kr/info/info04_view.jsp?n=51 (accessed on 14 June 2016).
- Park, S.A.; Yoon, E.Y. The effect of NutriPlus program among 1–5 years children in Daejeon Area-the improvement in nutritional status of children and nutrition knowledge and attitude of parents. Korean J. Community Nutr. 2013, 18, 1–10. [Google Scholar] [CrossRef]
| Food-Secure Household (n = 5413) | Food-Insecure Household without Hunger (n = 381) | Food-Insecure Household with Hunger (n = 68) | p ‡ | |
|---|---|---|---|---|
| Male %, (n) * | 39.2 (2120) | 34.4 (131) | 39.7 (27) | 0.146 |
| Age (year) † | 40.3 ± 0.2 | 40.1 ± 0.7 | 40.9 ± 1.8 | 0.842 |
| waist circumference (cm) | 79.9 ± 0.2 | 80.3 ± 0.7 | 80.6 ± 1.3 | 0.751 |
| Body mass index (kg/m2) | 23.7 ± 0.1 | 24.0 ± 0.3 | 23.6 ± 0.5 | 0.510 |
| Education %, (n) 1 | ||||
| ≤Elementary school | 7.4 (550) | 15.0 (57) | 32.4 (22) | <0.001 |
| ≤Middle school | 7.0 (435) | 10.8 (41) | 14.7 (10) | |
| ≤High school | 44.2 (2168) | 49.1 (187) | 30.9 (21) | |
| ≥University | 41.5 (2256) | 25.2 (96) | 22.1 (15) | |
| Income %, (n) 1 | ||||
| Lowest | 6.7 (362) | 19.8 (85) | 48.9 (33) | <0.001 |
| Lower middle | 24.6 (1295) | 44.8 (165) | 34.5 (21) | |
| Upper middle | 32.5 (1717) | 25.8 (98) | 13.3 (11) | |
| Highest | 36.3 (2004) | 9.7 (32) | 3.4 (3) | |
| Current smokers %, (n) | 25.4 (1375) | 30.4 (116) | 36.8 (25) | 0.035 |
| Current drinkers %, (n) | 62.3 (3372) | 53.3 (203) | 58.81 (40) | 0.010 |
| Physical activity %, (n) | 47.9 (2593) | 47.0 (179) | 44.1 (30) | 0.851 |
| Marital status %, (n) 1 | ||||
| Single | 27.5 (1020) | 27.7 (82) | 31.7 (16) | <0.001 |
| Married | 68.2 (4105) | 56.9 (234) | 38.6 (30) | |
| Married (alone) | 4.3 (278) | 15.4 (65) | 29.7 (22) | |
| Food assistance %, (n) | 1.0 (54) | 4.7 (18) | 8.8 (6) | <0.001 |
| Mental health | ||||
| Perceived stress %, (n) | 24.4 (1321) | 33.6 (128) | 41.2 (28) | <0.001 |
| Depressive symptom %, (n) | 9.4 (09) | 15.0 (57) | 38.2 (26) | <0.001 |
| Suicidal ideation %, (n) | 6.9 (373) | 11.5 (44) | 27.9 (19) | <0.001 |
| Quality of life | ||||
| Exercise ability %, (n) | 5.3 (287) | 13.4 (51) | 25.0 (17) | <0.001 |
| Self-management %, (n) | 1.1 (60) | 1.8 (7) | 8.8 (6) | <0.001 |
| Daily activity %, (n) | 3.1 (168) | 5.8 (22) | 22.1 (15) | <0.001 |
| Pain/discomfort %, (n) | 16.2 (877) | 22.8 (87) | 33.8 (23) | <0.001 |
| Anxiety/depression %, (n) | 8.3 (449) | 15.2 (58) | 30.9 (21) | <0.001 |
| Variables | Food-Secure Household (n = 5413) | Food-Insecure Household without Hunger (n = 381) | Food-Insecure Household with Hunger (n = 68) | p-Value |
|---|---|---|---|---|
| Energy 1 | 28.1 ± 0.8 | 31.7 ± 3.1 | 43.7 ± 6.1 | 0.029 |
| Protein 2 | 9.60 ± 0.5 | 8.70 ± 1.8 | 8.40 ± 4.5 | 0.868 |
| Protein 3 | 18.3 ± 0.7 | 23.1 ± 2.7 | 34.7 ± 6.6 | 0.003 |
| Fiber 3 | 97.6 ± 0.3 | 98.3 ± 0.7 | 98.9 ± 1.1 | 0.567 |
| Calcium 3 | 66.1 ± 0.8 | 70.7 ± 2.9 | 86.4 ± 3.4 | 0.002 |
| Phosphorous 3 | 7.80 ± 0.4 | 13.1 ± 2.1 | 24.5 ± 6.6 | <0.001 |
| Iron 3 | 19.6 ± 0.7 | 24.9 ± 2.7 | 29.9 ± 6.1 | 0.018 |
| Sodium 4 | 6.5 ± 0.4 | 8.60 ± 1.8 | 13.0 ± 4.2 | 0.072 |
| Potassium 4 | 66.0 ± 0.8 | 67.9 ± 2.9 | 84.7 ± 4.6 | 0.017 |
| Vitamin A 3 | 39.6 ± 0.8 | 46.7 ± 3.2 | 55.9 ± 7.1 | 0.006 |
| Vitamin B1 3 | 17.1 ± 0.7 | 25.4 ± 3.2 | 23.8 ± 5.5 | 0.003 |
| Vitamin B2 3 | 41.3 ± 0.8 | 45.7 ± 3.3 | 60.2 ± 7.3 | 0.023 |
| Niacin 3 | 24.5 ± 0.7 | 37.2 ± 3.4 | 46.1 ± 7.7 | <0.001 |
| Vitamin C 3 | 47.5 ± 1.0 | 59.8 ± 2.9 | 68.6 ± 6.4 | <0.001 |
| Food-Secure Household (n = 5413) | Food-Insecure Household without Hunger (n = 381) | p-Value | Food-Insecure Household with Hunger (n = 68) | p-Value | |
|---|---|---|---|---|---|
| Perceived stress * | |||||
| Unadjusted † | 1.00 (ref) | 1.56 (1.19–2.06) | 0.001 | 2.15 (1.26–3.68) | 0.005 |
| Multivariable adjusted 1 | 1.00 (ref) | 1.52 (1.15–2.01) | 0.003 | 1.96 (1.08–3.53) | 0.026 |
| Depressive symptom | |||||
| Unadjusted † | 1.00 (ref) | 1.68 (1.20–2.36) | 0.003 | 5.77 (3.29–10.1) | <0.001 |
| Multivariable adjusted 1 | 1.00 (ref) | 1.26 (0.89–1.78) | 0.185 | 3.64 (2.17–6.08) | <0.001 |
| Suicidal ideation | |||||
| Unadjusted † | 1.00 (ref) | 1.75 (1.13–2.72) | 0.013 | 5.24 (2.77–9.94) | <0.001 |
| Multivariable adjusted 1 | 1.00 (ref) | 1.33 (0.83–2.14) | 0.234 | 3.83 (2.02–7.23) | <0.001 |
| Food-Secure Household (n = 5413) | Food-Insecure Household without Hunger (n = 381) | p-Value | Food-Insecure Household with Hunger (n = 68) | p-Value | |
|---|---|---|---|---|---|
| Decreased Exercise ability * | |||||
| Unadjusted † | 1.00 (ref) | 2.78 (1.86–4.14) | <0.001 | 5.93 (3.15–11.2) | <0.001 |
| Multivariate adjusted 1 | 1.00 (ref) | 2.22 (1.45–3.40) | <0.001 | 3.22 (1.78–5.82) | <0.001 |
| Self-management | |||||
| Unadjusted † | 1.00 (ref) | 1.68 (0.77–3.66) | 0.191 | 8.23 (2.90–23.4) | <0.001 |
| Multivariate adjusted 1 | 1.00 (ref) | 1.15 (0.49–2.70) | 0.756 | 3.19 (0.94–10.8) | 0.062 |
| Decreased Daily activity | |||||
| Unadjusted † | 1.00 (ref) | 1.90 (1.10–3.28) | 0.021 | 9.05 (4.81–17.1) | <0.001 |
| Multivariate adjusted 2 | 1.00 (ref) | 1.21 (0.67–2.18) | 0.523 | 3.92 (1.87–8.20) | <0.001 |
| Pain/discomfort | |||||
| Unadjusted † | 1.00 (ref) | 1.54 (1.13–2.08) | 0.006 | 2.55 (1.40–4.65) | 0.002 |
| Multivariate adjusted 1 | 1.00 (ref) | 1.29 (0.95–1.76) | 0.108 | 1.69 (0.87–3.27) | 0.124 |
| Anxiety/depression | |||||
| Unadjusted † | 1.00 (ref) | 1.97 (1.36–2.87) | <0.001 | 4.84 (2.74–8.54) | <0.001 |
| Multivariate adjusted 1 | 1.00 (ref) | 1.49 (1.00–2.23) | 0.049 | 2.63 (1.52–4.55) | 0.001 |
© 2016 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC-BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Chung, H.-K.; Kim, O.Y.; Kwak, S.Y.; Cho, Y.; Lee, K.W.; Shin, M.-J. Household Food Insecurity Is Associated with Adverse Mental Health Indicators and Lower Quality of Life among Koreans: Results from the Korea National Health and Nutrition Examination Survey 2012–2013. Nutrients 2016, 8, 819. https://doi.org/10.3390/nu8120819
Chung H-K, Kim OY, Kwak SY, Cho Y, Lee KW, Shin M-J. Household Food Insecurity Is Associated with Adverse Mental Health Indicators and Lower Quality of Life among Koreans: Results from the Korea National Health and Nutrition Examination Survey 2012–2013. Nutrients. 2016; 8(12):819. https://doi.org/10.3390/nu8120819
Chicago/Turabian StyleChung, Hye-Kyung, Oh Yoen Kim, So Young Kwak, Yoonsu Cho, Kyong Won Lee, and Min-Jeong Shin. 2016. "Household Food Insecurity Is Associated with Adverse Mental Health Indicators and Lower Quality of Life among Koreans: Results from the Korea National Health and Nutrition Examination Survey 2012–2013" Nutrients 8, no. 12: 819. https://doi.org/10.3390/nu8120819
APA StyleChung, H.-K., Kim, O. Y., Kwak, S. Y., Cho, Y., Lee, K. W., & Shin, M.-J. (2016). Household Food Insecurity Is Associated with Adverse Mental Health Indicators and Lower Quality of Life among Koreans: Results from the Korea National Health and Nutrition Examination Survey 2012–2013. Nutrients, 8(12), 819. https://doi.org/10.3390/nu8120819





