Implications of Dietary Intake and Eating Behaviors for People with Serious Mental Illness: A Qualitative Study
Abstract
:1. Introduction
2. Materials and Methods
2.1. Design
2.2. Participants
2.3. Procedure
2.4. Thematic Analysis
3. Results
3.1. Study Population
3.2. Qualitative Findings
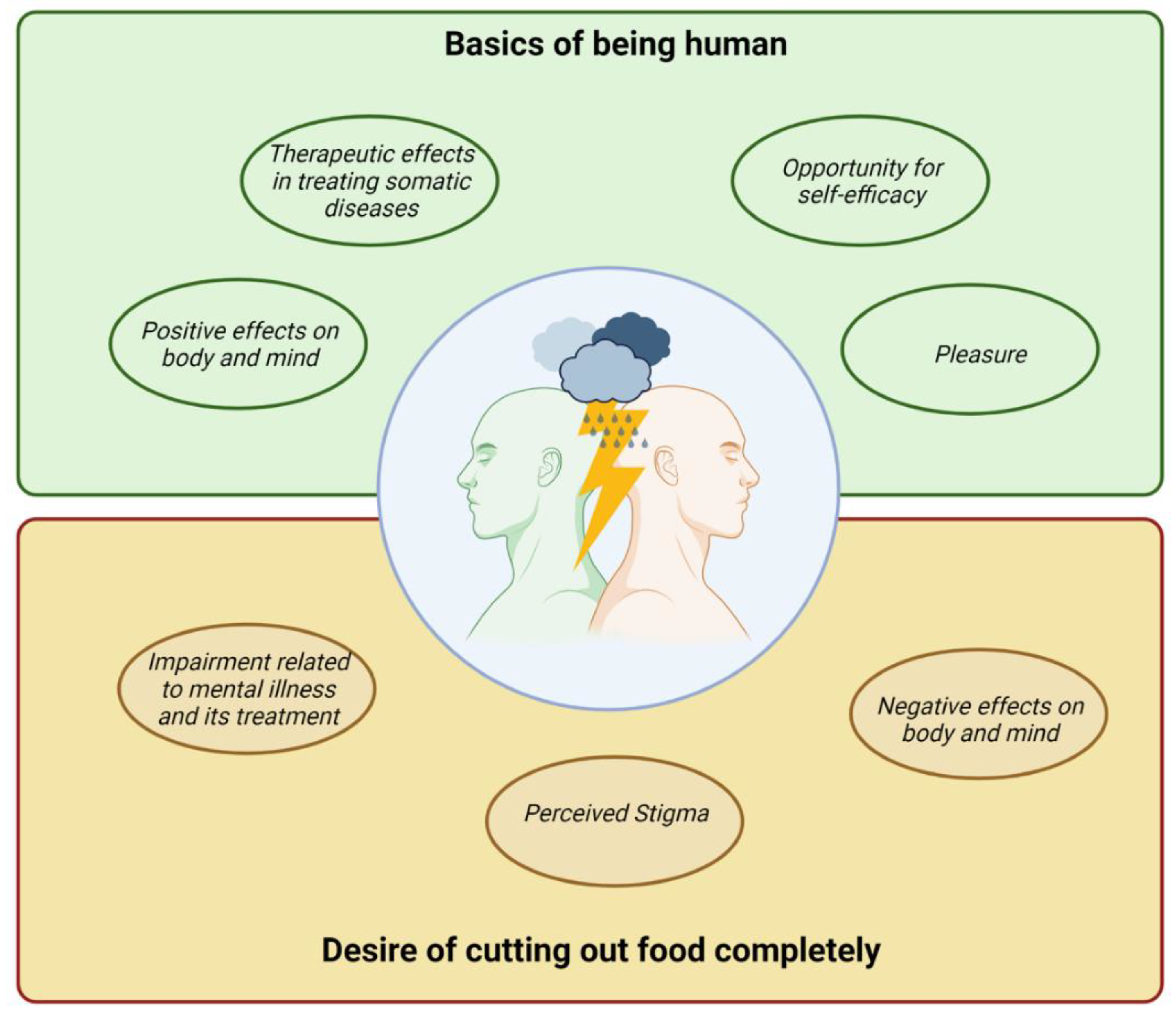
3.2.1. Positive Implications of Diet
Positive Effects on Body and Mind
“If I eat things that taste good to me, but are also generally considered healthy, then this has a positive effect for my mental well-being, I feel better, I have more energy and my digestion, for example, also gets better. So, it’s very important to me that my food tastes good and that it’s also good for my body. And [good] for the soul, yes” (Ulm04, female).
“Right when I eat healthy foods, which are healthy for my body, my mind just naturally benefits” (Syd05, female).
“Well, it’s already better, I now really eat a proper full meal with a salad and such and then I feel relatively long satiated and then that is just everything (…) Yes, one just feels better this way” (Ulm03, female).
“Fish in particular is a brain food, and I eat a lot of it. It helps me to focus on the issues, helps to concentrate. It’s also enjoyable, and healthy as well, good for your body” (Syd08, female).
Therapeutic Effects in Treating Somatic Illnesses
Pleasure
Opportunity for Self-Efficacy
3.2.2. Negative Implications of Diet
Negative Effects on Body and Mind
Impairment Related to Mental Illness and Its Treatment
“So, when I’m hungry and I don’t want the extra kilojoules, I just force down a cup of coffee and I manage to control my appetite. That’s how, I think how I’ve been maintaining my weight (…) We just want to eat all the time and it’s annoying me” (Syd12, male).
“Chocolate is not essential for life and that is now my first step, where I think to myself, alright, do not eat the first piece of chocolate to which I stick to very convulsively” (Ulm07, female).
Perceived Stigma
3.2.3. Inner Conflict Related to Diet
Inner Conflict
Missing Support
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Firth, J.; Siddiqi, N.; Koyanagi, A.; Siskind, D.; Rosenbaum, S.; Galletly, C.; Allan, S.; Caneo, C.; Carney, R.; Carvalho, A.F.; et al. The Lancet Psychiatry Commission: A blueprint for protecting physical health in people with mental illness. Lancet Psychiatry 2019, 6, 675–712. [Google Scholar] [CrossRef] [Green Version]
- Hjorthøj, C.; Stürup, A.E.; McGrath, J.; Nordentoft, M. Years of potential life lost and life expectancy in schizophrenia: A systematic review and meta-analysis. Lancet Psychiatry 2017, 4, 295–301. [Google Scholar] [CrossRef]
- Correll, C.U.; Solmi, M.; Veronese, N.; Bortolato, B.; Rosson, S.; Santonastaso, P.; Thapa-Chhetri, N.; Fornaro, M.; Gallicchio, D.; Collantoni, E.; et al. Prevalence, incidence and mortality from cardiovascular disease in patients with pooled and specific severe mental illness: A large-scale meta-analysis of 3,211,768 patients and 113,383,368 controls. World Psychiatry 2017, 16, 163–180. [Google Scholar] [CrossRef] [Green Version]
- Henderson, C.; Noblett, J.; Parke, H.; Clement, S.; Caffrey, A.; Gale-Grant, O.; Schulze, B.; Druss, B.; Thornicroft, G. Mental health-related stigma in health care and mental health-care settings. Lancet Psychiatry 2014, 1, 467–482. [Google Scholar] [CrossRef]
- Jones, S.; Howard, L.; Thornicroft, G. ‘Diagnostic overshadowing’: Worse physical health care for people with mental illness. Acta Psychiatr. Scand. 2008, 118, 169–171. [Google Scholar] [CrossRef]
- Dixon, L.B.; Holoshitz, Y.; Nossel, I. Treatment engagement of individuals experiencing mental illness: Review and update. World Psychiatry 2016, 15, 13–20. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Álvarez-Jiménez, M.; González-Blanch, C.; Crespo-Facorro, B.; Hetrick, S.; Rodríguez-Sánchez, J.M.; Pérez-Iglesias, R.; Vázquez-Barquero, J.L. Antipsychotic-Induced Weight Gain in Chronic and First-Episode Psychotic Disorders. CNS Drugs 2008, 22, 547–562. [Google Scholar] [CrossRef]
- Jackson, J.G.; Diaz, F.J.; Lopez, L.; de Leon, J. A combined analysis of worldwide studies demonstrates an association between bipolar disorder and tobacco smoking behaviors in adults. Bipolar Disord. 2015, 17, 575–597. [Google Scholar] [CrossRef]
- Myles, N.; Newall, H.D.; Curtis, J.; Nielssen, O.; Shiers, D.; Large, M. Tobacco use before, at, and after first-episode psychosis: A systematic meta-analysis. J. Clin. Psychiatry 2012, 73, 21015. [Google Scholar] [CrossRef]
- Wisdom, J.P.; Manuel, J.I. Prevalence of Substance Use in People With First-Episode Psychosis. J. Dual Diagn. 2011, 7, 39–49. [Google Scholar] [CrossRef]
- Vancampfort, D.; Firth, J.; Schuch, F.; Rosenbaum, S.; Mugisha, J.; Hallgren, M.; Probst, M.; Ward, P.; Gaughran, F.; De Hert, M.; et al. Sedentary behavior and physical activity levels in people with schizophrenia, bipolar disorder and major depressive disorder: A global systematic review and meta-analysis. World Psychiatry 2017, 16, 308–315. [Google Scholar] [CrossRef] [PubMed]
- Teasdale, S.B.; Ward, P.; Samaras, K.; Firth, J.; Stubbs, B.; Tripodi, E.; Burrows, T.L. Dietary intake of people with severe mental illness: Systematic review and meta-analysis. Br. J. Psychiatry 2019, 214, 251–259. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Cuerda, C.; Velasco, C.; Merchán-Naranjo, J.; García-Peris, P.; Arango, C. The effects of second-generation antipsychotics on food intake, resting energy expenditure and physical activity. Eur. J. Clin. Nutr. 2013, 68, 146–152. [Google Scholar] [CrossRef] [PubMed]
- Knolle-Veentjer, S.; Huth, V.; Ferstl, R.; Aldenhoff, J.B.; Hinze-Selch, D. Delay of gratification and executive performance in individuals with schizophrenia: Putative role for eating behavior and body weight regulation. J. Psychiatr. Res. 2008, 42, 98–105. [Google Scholar] [CrossRef]
- De Beaurepaire, R. Binge Eating Disorders in Antipsychotic-Treated Patients With Schizophrenia. J. Clin. Psychopharmacol. 2021, 41, 114–120. [Google Scholar] [CrossRef]
- Teasdale, S.B.; Müller-Stierlin, A.S.; Ruusunen, A.; Eaton, M.; Marx, W.; Firth, J. Prevalence of food insecurity in people with major depression, bipolar disorder, and schizophrenia and related psychoses: A systematic review and meta-analysis. Crit. Rev. Food Sci. Nutr. 2021, 1–18. [Google Scholar] [CrossRef]
- Teasdale, S.B.; Morell, R.; Lappin, J.M.; Curtis, J.; Watkins, A.; Ward, P.B. Prevalence and correlates of food insecurity in community-based individuals with severe mental illness receiving long-acting injectable antipsychotic treatment. Br. J. Nutr. 2020, 124, 470–477. [Google Scholar] [CrossRef] [Green Version]
- Marx, W.; Moseley, G.; Berk, M.; Jacka, F. Nutritional psychiatry: The present state of the evidence. Proc. Nutr. Soc. 2017, 76, 427–436. [Google Scholar] [CrossRef] [Green Version]
- Lassale, C.; Batty, G.D.; Baghdadli, A.; Jacka, F.; Sánchez-Villegas, A.; Kivimäki, M.; Akbaraly, T. Healthy dietary indices and risk of depressive outcomes: A systematic review and meta-analysis of observational studies. Mol. Psychiatry 2019, 24, 965–986. [Google Scholar] [CrossRef] [Green Version]
- Firth, J.; Marx, W.; Dash, S.; Carney, R.; Teasdale, S.; Solmi, M.; Stubbs, B.; Schuch, F.; Carvalho, A.F.; Jacka, F.; et al. The Effects of Dietary Improvement on Symptoms of Depression and Anxiety: A Meta-Analysis of Randomized Controlled Trials. Psychosom. Med. 2019, 81, 265–280. [Google Scholar] [CrossRef]
- O’Neill, S.; Minehan, M.; Knight-Agarwal, C.R.; Turner, M. Depression, Is It Treatable in Adults Utilising Dietary Interventions? A Systematic Review of Randomised Controlled Trials. Nutrients 2022, 14, 1398. [Google Scholar] [CrossRef] [PubMed]
- Chatterton, M.L.; Mihalopoulos, C.; O’Neil, A.; Itsiopoulos, C.; Opie, R.; Castle, D.; Dash, S.; Brazionis, L.; Berk, M.; Jacka, F. Economic evaluation of a dietary intervention for adults with major depression (the “SMILES” trial). BMC Public Health 2018, 18, 599. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Segal, L.; Twizeyemariya, A.; Zarnowiecki, D.; Niyonsenga, T.; Bogomolova, S.; Wilson, A.; O’Dea, K.; Parletta, N. Cost effectiveness and cost-utility analysis of a group-based diet intervention for treating major depression—The HELFIMED trial. Nutr. Neurosci. 2018, 23, 770–778. [Google Scholar] [CrossRef]
- Kreyenbuhl, J.; Lucksted, A.; Despeaux, K.; Sykes, V.M. Understanding women veterans’ experiences with and management of weight gain from medications for serious mental illness: A qualitative study. Psychiatr. Rehabil. J. 2019, 42, 238–245. [Google Scholar] [CrossRef]
- Haracz, K.; Hazelton, M.; James, C. The “Double Whammy”: Women’s Experiences of Weight Gain after Diagnosis and Treatment for Schizophrenia Spectrum Disorders. J. Nerv. Ment. Dis. 2018, 206, 303–309. [Google Scholar] [CrossRef] [PubMed]
- VanDyk, A.D.; Baker, C. Qualitative descriptive study exploring schizophrenia and the everyday effect of medication-induced weight gain. Int. J. Ment. Health Nurs. 2012, 21, 349–357. [Google Scholar] [CrossRef] [PubMed]
- Barre, L.K.; Ferron, J.C.; Davis, K.E.; Whitley, R. Healthy eating in persons with serious mental illnesses: Understanding and barriers. Psychiatr. Rehabil. J. 2011, 34, 304–310. [Google Scholar] [CrossRef]
- Ince, S.; Günüşen, N.P. The views and habits of the individuals with mental illness about physical activity and nutrition. Perspect. Psychiatr. Care 2018, 54, 586–595. [Google Scholar] [CrossRef]
- Every-Palmer, S.; Huthwaite, M.A.; Elmslie, J.L.; Grant, E.; Romans, S.E. Long-term psychiatric inpatients’ perspectives on weight gain, body satisfaction, diet and physical activity: A mixed methods study. BMC Psychiatry 2018, 18, 300. [Google Scholar] [CrossRef] [Green Version]
- Jimenez, D.E.; Aschbrenner, K.; Burrows, K.; Pratt, S.I.; Alegría, M.; Bartels, S.J. Perspectives of overweight Latinos with serious mental illness on barriers and facilitators to health behavior change. J. Lat. Psychol. 2015, 3, 11–22. [Google Scholar] [CrossRef] [Green Version]
- Jimenez, D.E.; Thomas, L.; Bartels, S.J. The role of serious mental illness in motivation, participation and adoption of health behavior change among obese/sedentary Latino adults. Ethn. Health 2017, 24, 889–896. [Google Scholar] [CrossRef] [PubMed]
- Lerbæk, B.; McCloughen, A.; Lauritsen, M.B.; Aagaard, J.; Nordgaard, J.; Jørgensen, R. Barriers and Possible Solutions to Providing Physical Health Care in Mental Health Care: A Qualitative Study of Danish Key Informants’ Perspectives. Issues Ment. Health Nurs. 2020, 42, 463–472. [Google Scholar] [CrossRef] [PubMed]
- Roberts, S.H.; Bailey, J.E. An ethnographic study of the incentives and barriers to lifestyle interventions for people with severe mental illness. J. Adv. Nurs. 2013, 69, 2514–2524. [Google Scholar] [CrossRef] [PubMed]
- Vazin, R.; McGinty, E.E.; Dickerson, F.; Dalcin, A.; Goldsholl, S.; Enriquez, M.O.; Jerome, G.J.; Gennusa, J.V.; Daumit, G.L. Perceptions of strategies for successful weight loss in persons with serious mental illness participating in a behavioral weight loss intervention: A qualitative study. Psychiatr. Rehabil. J. 2016, 39, 137–146. [Google Scholar] [CrossRef]
- Mn, A.W.; Denney-Wilson, E.; Curtis, J.; Teasdale, S.; Rosenbaum, S.; Ward, P.; Stein-Parbury, J. Keeping the body in mind: A qualitative analysis of the experiences of people experiencing first-episode psychosis participating in a lifestyle intervention programme. Int. J. Ment. Health Nurs. 2019, 29, 278–289. [Google Scholar] [CrossRef]
- Weinstein, L.C.; Chilton, M.; Turchi, R.; Klassen, A.C.; LaNoue, M.; Silvero, A.; Cabassa, L.J. ‘It’s common sense that an individual must eat’: Advocating for food justice with people with psychiatric disabilities through photovoice. Health Expect. 2020, 24, 161–173. [Google Scholar] [CrossRef]
- Teasdale, S.B.; Moerkl, S.; Moetteli, S.; Mueller-Stierlin, A. The Development of a Nutrition Screening Tool for Mental Health Settings Prone to Obesity and Cardiometabolic Complications: Study Protocol for the NutriMental Screener. Int. J. Environ. Res. Public Health 2021, 18, 11269. [Google Scholar] [CrossRef]
- Braun, V.; Clarke, V. Using thematic analysis in psychology. Qual. Res. Psychol. 2006, 3, 77–101. [Google Scholar] [CrossRef] [Green Version]
- Ceolin, G.; Breda, V.; Koning, E.; Meyyappan, A.C.; Gomes, F.A.; Moreira, J.D.; Gerchman, F.; Brietzke, E. A Possible Antidepressive Effect of Dietary Interventions: Emergent Findings and Research Challenges. Curr. Treat. Opt. Psychiatry 2022, 1–12. [Google Scholar] [CrossRef]
- Buyukkurt, A.; Bourguignon, C.; Antinora, C.; Farquhar, E.; Gao, X.; Passarella, E.; Sibthorpe, D.; Gou, K.; Saury, S.; Beaulieu, S.; et al. Irregular eating patterns associate with hypomanic symptoms in bipolar disorders. Nutr. Neurosci. 2019, 24, 23–34. [Google Scholar] [CrossRef]
- Sierra-Johnson, J.; Undén, A.-L.; Linestrand, M.; Rosell, M.; Sjogren, P.; Kolak, M.; De Faire, U.; Fisher, R.; Hellénius, M.-L. Eating Meals Irregularly: A Novel Environmental Risk Factor for the Metabolic Syndrome. Obesity 2008, 16, 1302–1307. [Google Scholar] [CrossRef] [PubMed]
- Pengpid, S.; Peltzer, K. Skipping Breakfast and Its Association with Health Risk Behaviour and Mental Health Among University Students in 28 Countries. Diabetes Metab. Syndr. Obes. Targets Ther. 2020, 13, 2889–2897. [Google Scholar] [CrossRef] [PubMed]
- Yi, Y.-H.; Kim, Y.-J.; Lee, S.-Y.; Lee, J.-G.; Jeong, D.-W.; Cho, Y.-H.; Tak, Y.-J.; Choi, E.-J.; Hwang, H.L.; Lee, S.-H. The Correlation of Meal Frequency and Nutrition with Mental Health Status in Women Aged 20–39 Years: The 5th Korea National Health and Nutrition Examination Survey. Korean J. Obes. 2015, 24, 101–107. [Google Scholar] [CrossRef]
- Christensen, L.; Pettijohn, L. Mood and carbohydrate cravings. Appetite 2001, 36, 137–145. [Google Scholar] [CrossRef]
- Macedo, I.C.; de Freitas, J.S.; Torres, I.L.D.S. The Influence of Palatable Diets in Reward System Activation: A Mini Review. Adv. Pharmacol. Sci. 2016, 2016, 7238679. [Google Scholar] [CrossRef] [Green Version]
- Shabbir, F.; Patel, A.; Mattison, C.; Bose, S.; Krishnamohan, R.; Sweeney, E.; Sandhu, S.; Nel, W.; Rais, A.; Sandhu, R.; et al. Effect of diet on serotonergic neurotransmission in depression. Neurochem. Int. 2013, 62, 324–329. [Google Scholar] [CrossRef]
- Dalkner, N.; Platzer, M.; Bengesser, S.; Birner, A.; Fellendorf, F.; Queissner, R.; Painold, A.; Mangge, H.; Fuchs, D.; Reininghaus, B.; et al. The role of tryptophan metabolism and food craving in the relationship between obesity and bipolar disorder. Clin. Nutr. 2017, 37, 1744–1751. [Google Scholar] [CrossRef]
- Knüppel, A.; Shipley, M.J.; Llewellyn, C.H.; Brunner, E. Sugar intake from sweet food and beverages, common mental disorder and depression: Prospective findings from the Whitehall II study. Sci. Rep. 2017, 7, 6287. [Google Scholar] [CrossRef] [Green Version]
- Warren, J.M.; Smith, N.; Ashwell, M. A structured literature review on the role of mindfulness, mindful eating and intuitive eating in changing eating behaviours: Effectiveness and associated potential mechanisms. Nutr. Res. Rev. 2017, 30, 272–283. [Google Scholar] [CrossRef]
- Emmer, C.; Bosnjak, M.; Mata, J. The association between weight stigma and mental health: A meta-analysis. Obes. Rev. 2019, 21, e12935. [Google Scholar] [CrossRef]
- Brownell, K.D.; Rodin, J. Medical, metabolic, and psychological effects of weight cycling. Arch. Intern. Med. 1994, 154, 1325–1330. [Google Scholar] [CrossRef] [PubMed]
- Quinn, D.M.; Puhl, R.M.; Reinka, M.A. Trying again (and again): Weight cycling and depressive symptoms in U.S. adults. PLoS ONE 2020, 15, e0239004. [Google Scholar] [CrossRef] [PubMed]
- Rhee, E.-J. Weight Cycling and Its Cardiometabolic Impact. J. Obes. Metab. Syndr. 2017, 26, 237–242. [Google Scholar] [CrossRef] [PubMed]
- Oh, T.J.; Moon, J.H.; Choi, S.H.; Lim, S.; Park, K.S.; Cho, N.H.; Jang, H.C. Body-Weight Fluctuation and Incident Diabetes Mellitus, Cardiovascular Disease, and Mortality: A 16-Year Prospective Cohort Study. J. Clin. Endocrinol. Metab. 2018, 104, 639–646. [Google Scholar] [CrossRef] [PubMed]
- Kanji, S.; Fonseka, T.M.; Marshe, V.S.; Sriretnakumar, V.; Hahn, M.K.; Müller, D.J. The microbiome-gut-brain axis: Implications for schizophrenia and antipsychotic induced weight gain. Eur. Arch. Psychiatry Clin. Neurosci. 2017, 268, 3–15. [Google Scholar] [CrossRef]
- Elman, I.; Borsook, D.; Lukas, S.E. Food Intake and Reward Mechanisms in Patients with Schizophrenia: Implications for Metabolic Disturbances and Treatment with Second-Generation Antipsychotic Agents. Neuropsychopharmacology 2006, 31, 2091–2120. [Google Scholar] [CrossRef]
- Mörkl, S.; Wagner-Skacel, J.; Lahousen, T.; Lackner, S.; Holasek, S.J.; Bengesser, S.A.; Painold, A.; Holl, A.K.; Reininghaus, E. The Role of Nutrition and the Gut-Brain Axis in Psychiatry: A Review of the Literature. Neuropsychobiology 2018, 79, 80–88. [Google Scholar] [CrossRef]
- Castellani, L.N.; Costa-Dookhan, K.A.; McIntyre, W.B.; Wright, D.C.; Flowers, S.A.; Hahn, M.; Ward, K.M. Preclinical and Clinical Sex Differences in Antipsychotic-Induced Metabolic Disturbances: A Narrative Review of Adiposity and Glucose Metabolism. J. Psychiatry Brain Sci. 2019, 4, e190013. [Google Scholar] [CrossRef] [Green Version]
- Tuncer, G.Z.; Duman, Z. An examination of emotional eating behavior in individuals with a severe mental disorder. Arch. Psychiatr. Nurs. 2020, 34, 531–536. [Google Scholar] [CrossRef]
- Opwis, M.; Schmidt, J.; Martin, A.; Salewski, C. Gender differences in eating behavior and eating pathology: The mediating role of rumination. Appetite 2017, 110, 103–107. [Google Scholar] [CrossRef]
- Romanos-Nanclares, A.; Zazpe, I.; Santiago, S.; Marín, L.; Rico-Campà, A.; Martín-Calvo, N. Influence of Parental Healthy-Eating Attitudes and Nutritional Knowledge on Nutritional Adequacy and Diet Quality among Preschoolers: The SENDO Project. Nutrients 2018, 10, 1875. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sankaranarayanan, A.; Johnson, K.; Mammen, S.J.; Wilding, H.E.; Vasani, D.; Murali, V.; Mitchison, D.; Castle, D.J.; Hay, P. Disordered Eating among People with Schizophrenia Spectrum Disorders: A Systematic Review. Nutrients 2021, 13, 3820. [Google Scholar] [CrossRef] [PubMed]
- Mörkl, S.; Stell, L.; Buhai, D.; Schweinzer, M.; Wagner-Skacel, J.; Vajda, C.; Lackner, S.; Bengesser, S.; Lahousen, T.; Painold, A.; et al. ‘An Apple a Day’? Psychiatrists, Psychologists and Psychotherapists Report Poor Literacy for Nutritional Medicine: International Survey Spanning 52 Countries. Nutrients 2021, 13, 822. [Google Scholar] [CrossRef] [PubMed]
| Total (n = 28) | Australia (n = 12) | Germany (n = 8) | Austria (n = 8) | |
|---|---|---|---|---|
| Sex, female; n (%) | 17 (61%) | 7 (58%) | 5 (63%) | 5 (63%) |
| Age, in years; m (sd) | 43.3 (13.5) | 40.0 (15.6) | 48.6 (10.7) | 43.1 (11.1) |
| Body mass index (BMI), in kg/m2; m (sd) | 31.3 (6.4) | 31.3 (5.0) | 35.6 (7.3) | 26.8 (3.7) |
| Obesity (BMI > 30 kg/m2); n (%) | 16 (57%) | 7 (58%) | 7 (88%) | 2 (25%) |
| Schizophrenia or related disorders (ICD-10 F2); n (%) | 16 (57%) | 11 (92%) | 3 (38%) | 2 (25%) |
| Affective disorders; n (%) | 18 (64%) | 5 (42%) | 5 (63%) | 6 (75%) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mueller-Stierlin, A.S.; Cornet, S.; Peisser, A.; Jaeckle, S.; Lehle, J.; Moerkl, S.; Teasdale, S.B. Implications of Dietary Intake and Eating Behaviors for People with Serious Mental Illness: A Qualitative Study. Nutrients 2022, 14, 2616. https://doi.org/10.3390/nu14132616
Mueller-Stierlin AS, Cornet S, Peisser A, Jaeckle S, Lehle J, Moerkl S, Teasdale SB. Implications of Dietary Intake and Eating Behaviors for People with Serious Mental Illness: A Qualitative Study. Nutrients. 2022; 14(13):2616. https://doi.org/10.3390/nu14132616
Chicago/Turabian StyleMueller-Stierlin, Annabel S., Sebastian Cornet, Anna Peisser, Selina Jaeckle, Jutta Lehle, Sabrina Moerkl, and Scott B. Teasdale. 2022. "Implications of Dietary Intake and Eating Behaviors for People with Serious Mental Illness: A Qualitative Study" Nutrients 14, no. 13: 2616. https://doi.org/10.3390/nu14132616
APA StyleMueller-Stierlin, A. S., Cornet, S., Peisser, A., Jaeckle, S., Lehle, J., Moerkl, S., & Teasdale, S. B. (2022). Implications of Dietary Intake and Eating Behaviors for People with Serious Mental Illness: A Qualitative Study. Nutrients, 14(13), 2616. https://doi.org/10.3390/nu14132616








