The Influence of Maternal BMI on Adverse Pregnancy Outcomes in Older Women
Abstract
1. Introduction
2. Materials and Methods
2.1. Participants and Methods
2.2. Studied Variables
2.3. Statistical Analyses
3. Results
3.1. General Characteristics of Older Women
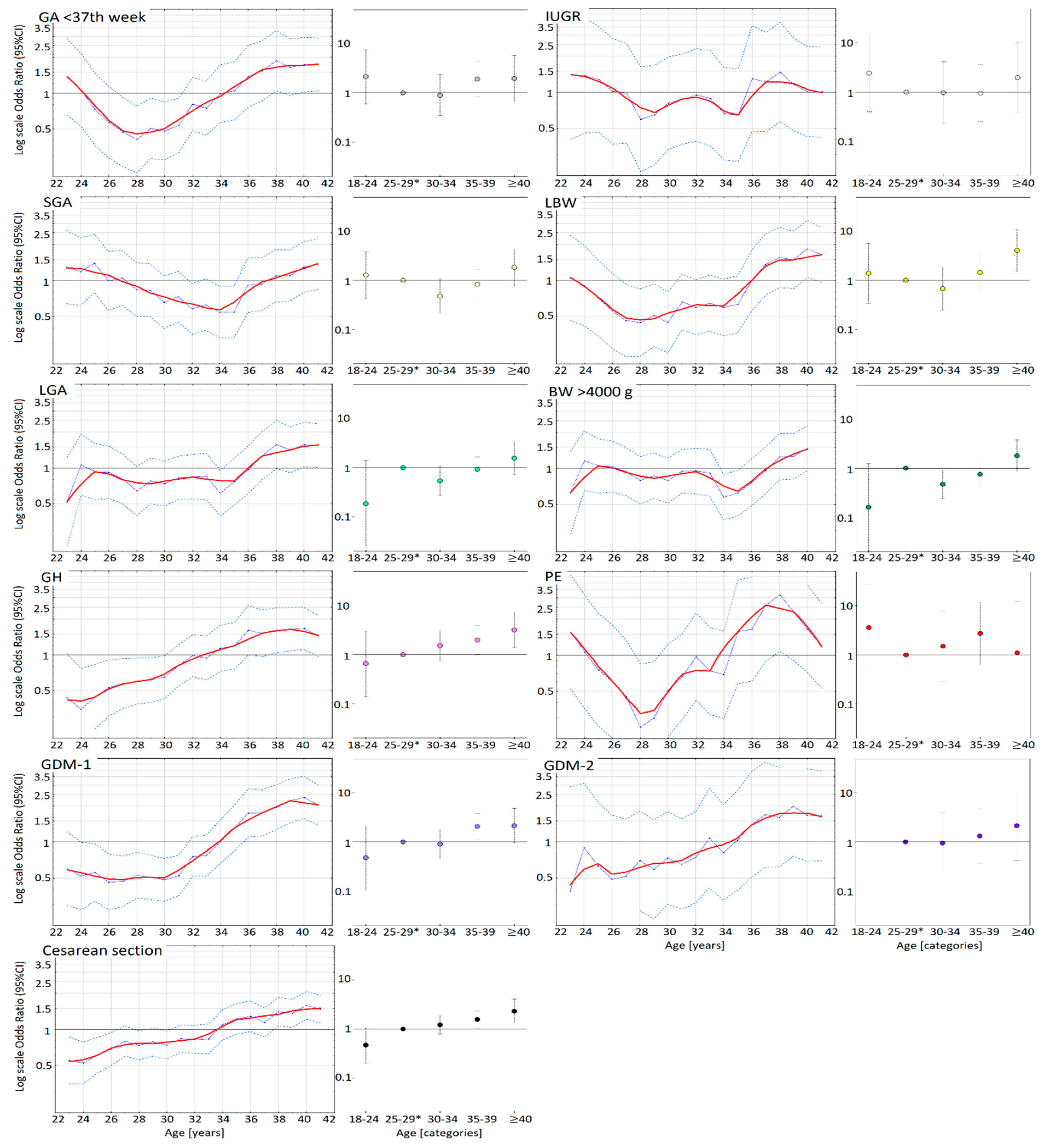
3.2. Effects of Maternal Age on the Adverse Pregnancy Results
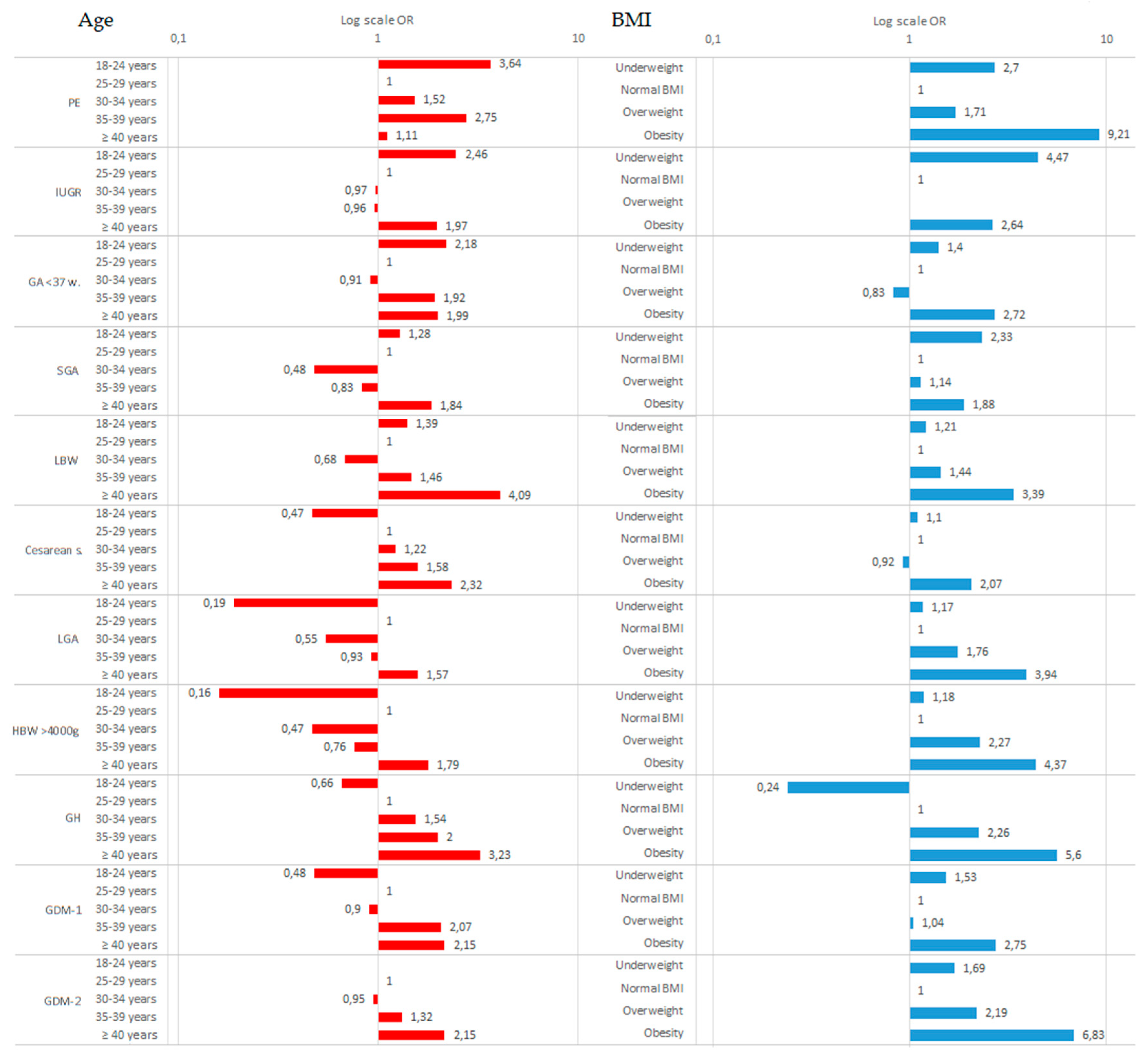
3.3. The Impact of Maternal BMI on the Effects Associated with Maternal Age
4. Discussion
Limitations and Advantages
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- He, P.; Chen, G.; Wang, Z.; Guo, C.; Zheng, X. The Role of Parental Education in Child Disability in China from 1987 to 2006. PLoS ONE 2017, 12, e0186623. [Google Scholar] [CrossRef]
- Fuchs, F.; Monet, B.; Ducruet, T.; Chaillet, N.; Audibert, F. Effect of Maternal Age on the Risk of Preterm Birth: A Large Cohort Study. PLoS ONE 2018, 13, e0191002. [Google Scholar] [CrossRef]
- Lean, S.C.; Derricott, H.; Jones, R.L.; Heazell, A.E.P. Advanced Maternal Age and Adverse Pregnancy Outcomes: A Systematic Review and Meta-Analysis. PLoS ONE 2017, 12, e0186287. [Google Scholar] [CrossRef]
- Marozio, L.; Picardo, E.; Filippini, C.; Mainolfi, E.; Berchialla, P.; Cavallo, F.; Tancredi, A.; Benedetto, C. Maternal Age over 40 Years and Pregnancy Outcome: A Hospital-Based Survey. J. Matern. Neonatal Med. 2017, 32, 1602–1608. [Google Scholar] [CrossRef]
- Grotegut, C.; Chisholm, C.A.; Johnson, L.N.C.; Brown, H.L.; Heine, R.P.; James, A.H. Medical and Obstetric Complications Among Pregnant Women Aged 45 and Older. PLoS ONE 2014, 9, e96237. [Google Scholar] [CrossRef]
- Kort, D.; Gosselin, J.; Choi, J.; Thornton, M.; Cleary-Goldman, J.; Sauer, M. Pregnancy After Age 50: Defining Risks for Mother and Child. Am. J. Perinatol. 2011, 29, 245–250. [Google Scholar] [CrossRef]
- Warraich, U.-E.-A.; Hussain, F.; Kayani, H.U.R. Aging-Oxidative Stress, Antioxidants and Computational Modeling. Heliyon 2020, 6, e04107. [Google Scholar] [CrossRef]
- Zhang, H.; Davies, K.P.; Forman, H.J. Oxidative Stress Response and Nrf2 Signaling in Aging. Free. Radic. Boil. Med. 2015, 88, 314–336. [Google Scholar] [CrossRef] [PubMed]
- Zuo, L.; Prather, E.R.; Stetskiv, M.; Garrison, D.E.; Meade, J.R.; Peace, T.I.; Zhou, T.; Zuo, L.; Zhou, T. Inflammaging and Oxidative Stress in Human Diseases: From Molecular Mechanisms to Novel Treatments. Int. J. Mol. Sci. 2019, 20, 4472. [Google Scholar] [CrossRef]
- Rayman, M.P.; Bath, S.C.; Westaway, J.; Williams, P.; Mao, J.; Vanderlelie, J.J.; Perkins, A.V.; Redman, C.W.G. Selenium Status in UK Pregnant Women and Its Relationship with Hypertensive Conditions of Pregnancy. Br. J. Nutr. 2015, 113, 249–258. [Google Scholar] [CrossRef]
- Lewandowska, M.; Więckowska, B.; Sajdak, S.; Lubiński, J. First Trimester Microelements and Their Relationships with Pregnancy Outcomes and Complications. Nutrients 2020, 12, 1108. [Google Scholar] [CrossRef] [PubMed]
- Lewandowska, M.; Sajdak, S.; Lubiński, J. Serum Selenium Level in Early Healthy Pregnancy as a Risk Marker of Pregnancy Induced Hypertension. Nutrients 2019, 11, 1028. [Google Scholar] [CrossRef]
- Lewandowska, M.; Sajdak, S.; Lubiński, J. The Role of Early Pregnancy Maternal Selenium Levels on the Risk for Small-for-Gestational Age Newborns. Nutrients 2019, 11, 2298. [Google Scholar] [CrossRef] [PubMed]
- Feng, H.; Wang, L.; Zhang, G.; Zhang, Z.; Guo, W. Oxidative Stress Activated by Keap-1/Nrf2 Signaling Pathway in Pathogenesis of Preeclampsia. Int. J. Clin. Exp. Pathol. 2020, 13, 382–392. [Google Scholar] [PubMed]
- Lewandowska, M.; Lubiński, J. Serum Microelements in Early Pregnancy and Their Risk of Large-for-Gestational Age Birth Weight. Nutrients 2020, 12, 866. [Google Scholar] [CrossRef]
- Lewandowska, M.; Więckowska, B.; Sajdak, S. Pre-Pregnancy Obesity, Excessive Gestational Weight Gain, and the Risk of Pregnancy-Induced Hypertension and Gestational Diabetes Mellitus. J. Clin. Med. 2020, 9, 1980. [Google Scholar] [CrossRef]
- Li, X.; Zhang, W.; Lin, J.; Liu, H.; Yang, Z.; Teng, Y.; Duan, S.; Li, Y.; Xie, Y.; Lin, X.; et al. Preterm Birth, Low Birthweight, and Small for Gestational Age Among Women With Preeclampsia: Does Maternal Age Matter? Pregnancy Hypertens. 2018, 13, 260–266. [Google Scholar] [CrossRef]
- Zhang, X.; Xu, H.; Hu, R.; Xiong, Y.; Gu, W.; Zhou, Q.; Li, X. Changing Trends of Adverse Pregnancy Outcomes With Maternal Age in Primipara With Singleton Birth: A Join Point Analysis of a Multicenter Historical Cohort Study in China in 2011–2012. Acta Obstet. Gynecol. Scand. 2019, 98, 997–1003. [Google Scholar] [CrossRef]
- Di Gravio, C.; Lawande, A.; Potdar, R.D.; Sahariah, S.A.; Gandhi, M.; Brown, N.; Chopra, H.; Sane, H.; Kehoe, S.H.; Marley-Zagar, E.; et al. The Association of Maternal Age With Fetal Growth and Newborn Measures: The Mumbai Maternal Nutrition Project (MMNP). Reprod. Sci. 2018, 26, 918–927. [Google Scholar] [CrossRef]
- Pinheiro, R.L.; Areia, A.L.; Mota-Pinto, A.; Donato, H. Advanced Maternal Age: Adverse Outcomes of Pregnancy, A Meta-Analysis. Acta Médica Portuguesa. 2019, 32, 219–226. [Google Scholar] [CrossRef]
- Londero, A.P.; Rossetti, E.; Pittini, C.; Cagnacci, A.; Driul, L. Maternal Age and the Risk of Adverse Pregnancy Outcomes: A Retrospective Cohort Study. BMC Pregnancy Childbirth 2019, 19. [Google Scholar] [CrossRef] [PubMed]
- Goisis, A.; Remes, H.; Barclay, K.J.; Martikainen, P.; Myrskylä, M. Advanced Maternal Age and the Risk of Low Birth Weight and Preterm Delivery: A Within-Family Analysis Using Finnish Population Registers. Am. J. Epidemiol. 2017, 186, 1219–1226. [Google Scholar] [CrossRef] [PubMed]
- McLennan, A.S.; Gyamfi-Bannerman, C.; Ananth, C.V.; Wright, J.D.; Siddiq, Z.; D’Alton, M.E.; Friedman, A.M. The Role of Maternal Age in Twin Pregnancy Outcomes. Am. J. Obstet. Gynecol. 2017, 217, 80.e1–80.e8. [Google Scholar] [CrossRef] [PubMed]
- Catalano, P.M.; Shankar, K. Obesity and Pregnancy: Mechanisms of Short Term and Long-Term Adverse Consequences for Mother and Child. BMJ. 2017, 356, j1. [Google Scholar] [CrossRef] [PubMed]
- Marchi, J.; Berg, M.; Dencker, A.; Olander, E.; Begley, C. Risks Associated with Obesity in Pregnancy, for the Mother and Baby: A Systematic Review of Reviews. Obes. Rev. 2015, 16, 621–638. [Google Scholar] [CrossRef]
- Dolin, C.D.; Kominiarek, M.A. Pregnancy in Women with Obesity. Obstet. Gynecol. Clin. North Am. 2018, 45, 217–232. [Google Scholar] [CrossRef] [PubMed]
- Biobaku, F.; Ghanim, H.; Batra, M.; Dandona, P. Macronutrient-Mediated Inflammation and Oxidative Stress: Relevance to Insulin Resistance, Obesity, and Atherogenesis. J. Clin. Endocrinol. Metab. 2019, 104, 6118–6128. [Google Scholar] [CrossRef]
- Kahveci, B.; Melekoglu, R.; Evruke, I.C.; Cetin, C. The Effect of Advanced Maternal Age on Perinatal Outcomes in Nulliparous Singleton Pregnancies. BMC Pregnancy Childbirth 2018, 18, 343. [Google Scholar] [CrossRef]
- Schummers, L.; A Hutcheon, J.; Hacker, M.R.; VanderWeele, T.J.; Williams, P.L.; McElrath, T.F.; Hernández-Diaz, S. Absolute Risks of Obstetric Outcomes Risks by Maternal Age at First Birth. Epidemiology 2018, 29, 379–387. [Google Scholar] [CrossRef]
- Shan, D.; Qiu, P.-Y.; Wu, Y.-X.; Chen, Q.; Li, A.-L.; Ramadoss, S.; Wang, R.-R.; Hu, Y.-Y. Pregnancy Outcomes in Women of Advanced Maternal Age: A Retrospective Cohort Study from China. Sci. Rep. 2018, 8, 12239. [Google Scholar] [CrossRef]
- Masturzo, B.; Di Martino, D.; Prefumo, F.; Cavoretto, P.; Germano, C.; Gennarelli, G.; Roletti, E.; Bottazzoli, E.; Fusè, F.; Ferrazzi, E.; et al. Higher Rate of Early-Onset Preeclampsia in Pregnancies Following Oocyte Donation According to Increasing Maternal Age. Arch. Gynecol. Obstet. 2019, 300, 861–867. [Google Scholar] [CrossRef] [PubMed]
- Cavazos-Rehg, P.; Krauss, M.J.; Spitznagel, E.L.; Bommarito, K.; Madden, T.; Olsen, M.A.; Subramaniam, H.; Peipert, J.F.; Bierut, L.J. Maternal Age and Risk of Labor and Delivery Complications. Matern. Child Heal. J. 2015, 19, 1202–1211. [Google Scholar] [CrossRef] [PubMed]
- Lamminpää, R.; Vehviläinen-Julkunen, K.; Gissler, M.; Heinonen, S. Preeclampsia Complicated by Advanced Maternal Age: A Registry-Based Study on Primiparous Women in Finland 1997–2008. BMC Pregnancy Childbirth 2012, 12, 47. [Google Scholar] [CrossRef] [PubMed]
- Klar, M.; Farthmann, J. Gestational Hypertension and Advanced Maternal Age. Lancet 2015, 386, 1627–1628. [Google Scholar] [CrossRef]
- Kanmaz, A.G.; Inan, A.H.; Beyan, E.; Ögür, S.; Budak, A. Effect of Advanced Maternal Age on Pregnancy Outcomes: A Single-Centre Data from a Tertiary Healthcare Hospital. J. Obstet. Gynaecol. 2019, 39, 1104–1111. [Google Scholar] [CrossRef]
- Kelsey, M.M.; Zeitler, P. Insulin Resistance of Puberty. Curr. Diabetes Rep. 2016, 16, 64. [Google Scholar] [CrossRef]
- Ghosh, A.; Freestone, N.S.; Anim-Nyame, N.; Fabbri-Arrigoni, F.I. Microvascular Function in pre-eclampsia Is Influenced by Insulin Resistance and an Imbalance of Angiogenic Mediators. Physiol. Rep. 2017, 5, e13185. [Google Scholar] [CrossRef]
- Jung, C.-H.; Jung, S.H.; Lee, B.; Rosenberg, M.; Reaven, G.M.; Kim, S.H. Relationship Among Age, Insulin Resistance, and Blood Pressure. J. Am. Soc. Hypertens. 2017, 11, 359–365.e2. [Google Scholar] [CrossRef]
- Nogues, P.; Dos Santos, E.; Jammes, H.; Berveiller, P.; Arnould, L.; Vialard, F.; Dieudonné, M.-N. Maternal Obesity Influences Expression and DNA Methylation of the Adiponectin and Leptin Systems in Human Third-Trimester Placenta. Clin. Epigenetics 2019, 11, 1–18. [Google Scholar] [CrossRef]
- Liu, B.; Xu, G.; Sun, Y.; Du, Y.; Gao, R.; Snetselaar, L.G.; Santillan, M.K.; Bao, W. Association Between Maternal Pre-Pregnancy Obesity and Preterm Birth According to Maternal Age and Race or Ethnicity: A Population-Based Study. Lancet Diabetes Endocrinol. 2019, 7, 707–714. [Google Scholar] [CrossRef]
- Ferrazzi, E.; Brembilla, G.; Cipriani, S.; Livio, S.; Paganelli, A.; Parazzini, F. Maternal Age and Body Mass Index at Term: Risk Factors for Requiring an Induced Labour for a Late-Term Pregnancy. Eur. J. Obstet. Gynecol. Reprod. Boil. 2018, 233, 151–157. [Google Scholar] [CrossRef] [PubMed]
- Patel, A.; Prakash, A.A.; Das, P.K.; Gupta, S.; Pusdekar, Y.V.; Hibberd, P.L. Maternal Anemia and Underweight As Determinants of Pregnancy Outcomes: Cohort Study in Eastern Rural Maharashtra, India. BMJ Open 2018, 8, e021623. [Google Scholar] [CrossRef]
- Girsen, A.I.; A Mayo, J.; Carmichael, S.L.; Phibbs, C.S.; Shachar, B.Z.; Stevenson, D.K.; Lyell, D.J.; Shaw, G.M.; Gould, J.B.; March of Dimes Prematurity Research Center at Stanford University School of Medicine. Women’s Prepregnancy Underweight as a Risk Factor for Preterm Birth: A Retrospective Study. BJOG Int. J. Obstet. Gynaecol. 2016, 123, 2001–2007. [Google Scholar] [CrossRef] [PubMed]
- Desyibelew, H.D.; Dadi, A.F. Burden and Determinants of Malnutrition Among Pregnant Women in Africa: A Systematic Review and Meta-Analysis. PLoS ONE 2019, 14, e0221712. [Google Scholar] [CrossRef] [PubMed]
| Maternal Characteristics/Pregnancy Outcomes | Women <35 Years (n = 433) | Women ≥35 Years (n = 479) | |
|---|---|---|---|
| Median (IQ Range)/n(%) | Median (IQ Range)/n(%) | p * | |
| Maternal age (years) | 30 (28–32) | 37 (36–39) | <0.001 |
| Primiparity | 244 (56.4%) | 138 (28.8%) | <0.001 |
| Treatment of infertility | 14 (3.2%) | 26 (5.4%) | 0.106 |
| Pre-pregnancy BMI (kg/m2) | 22.1 (20.3–24.9) | 23.6 (21.1–27.2) | <0.001 |
| BMI categories | <0.001 | ||
| Obesity | 36 (8.3%) | 62 (12.9%) | |
| Overweight | 70 (16.2%) | 103 (21.5%) | |
| Normal BMI | 295 (68.1%) | 299 (62.4%) | |
| Underweight | 32 (7.4%) | 15 (3.1%) | |
| Gestational weight gain (kg) | 14 (10–17) | 13 (10–17) | 0.010 |
| Smoking before pregnancy | 84 (19.4%) | 84 (17.5%) | 0.469 |
| Smoking in I trimester | 29 (6.7%) | 28 (5.8%) | 0.596 |
| Multivitamins in pregnancy | 273 (63%) | 254 (53%) | 0.002 |
| Education <12 years # | 22 (5.7%) | 48 (11.7%) | 0.003 |
| Lower financial status # | 62 (23.8%) | 69 (30%) | 0.125 |
| Fetal sex, son | 220 (50.8%) | 253 (52.8%) | 0.544 |
| Gestational age | 39 (38–40) | 39 (38–40) | <0.001 |
| Birth <37th week | 22 (5.1%) | 43 (9.0%) | 0.022 |
| IUGR | 10 (2.3%) | 11 (2.3%) | 0.991 |
| Birth weight | 3410 (3090–3700) | 3400 (3065–3745) | 0.947 |
| Birth weight in percentiles | 0.460 | ||
| <10th percentile | 30 (6.9%) | 42 (8.8%) | |
| 10–90 percentile | 365 (84.3%) | 376 (78.5%) | |
| >90th percentile | 38 (8.8%) | 61 (12.7%) | |
| Birth weight in grams | 0.696 | ||
| <2500 g | 19 (4.4%) | 41 (8.6%) | |
| 2500–4000 g | 375 (86.6%) | 380 (79.3%) | |
| >4000 g | 39 (9.0%) | 58 (12.1%) | |
| APGAR in 5th minute <7 | 0 (0%) | 2 (0.4%) | - |
| Cesarean section | 156 (36.0%) | 226 (47.2%) | 0.001 |
| GH | 41 (9.5%) | 72 (15.0%) | 0.011 |
| PE | 9 (2.1%) | 15 (3.1%) | 0.321 |
| GDM-1 | 38 (8.8%) | 87 (18.2%) | <0.001 |
| GDM-2 | 8 (1.8%) | 13 (2.7%) | 0.384 |
| Odds Ratios of Pregnancy Results for Maternal Age with Regard to the Age Range of 25–29 Years | |||||
|---|---|---|---|---|---|
| Outcomes | 18–24 Years OR (95% CI); p AOR (95% CI); p | 25–29 Years OR (95% CI); p AOR (95% CI); p | 30–34 Years OR (95% CI); p AOR (95% CI); p | 35–39 Years OR (95% CI); p AOR (95% CI); p | ≥40 Years OR (95% CI); p AOR (95% CI); p |
| PE | 3.64 (0.5–26.74); 0.204 | 1 | 1.52 (0.29–7.93); 0.622 | 2.75 (0.60–12.3); 0.184 | 1.11 (0.1–12.49); 0.933 |
| 3.48 (0.5–27.14); 0.234 | 1 | 1.50 (0.27–8.51); 0.646 | 2.21 (0.45–10.9); 0.329 | 0.64 (0.05–8.79); 0.740 | |
| IUGR | 2.46 (0.4–15.23); 0.334 | 1 | 0.97 (0.23–4.13); 0.970 | 0.96 (0.25–3.65); 0.946 | 1.97 (0.39–10.0); 0.413 |
| 1.51 (0.2–10.25); 0.673 | 1 | 1.15 (0.27–4.99); 0.849 | 1.30 (0.33–5.23); 0.708 | 2.40 (0.43–13.43); 0.319 | |
| GA <37th w. | 2.18 (0.6–7.84); 0.235 | 1 | 0.91 (0.34–2.4); 0.839 | 1.92 (0.84–4.42); 0.125 | 1.99 (0.67–5.89); 0.216 |
| 1.67 (0.4–7.13); 0.491 | 1 | 0.76 (0.27–2.13); 0.606 | 1.39 (0.56–3.44); 0.479 | 1.45 (0.45–4.72); 0.539 | |
| SGA | 1.28 (0.43–3.84); 0.662 | 1 | 0.48 (0.21–1.08); 0.077 | 0.83 (0.42–1.65); 0.596 | 1.84 (0.77–4.38); 0.169 |
| 0.63 (0.19–2.14); 0.463 | 1 | 0.47 (0.20–1.11); 0.085 | 0.83 (0.39–1.75); 0.622 | 1.64 (0.62–4.32); 0.317 | |
| LBW | 1.39 (0.34–5.67); 0.643 | 1 | 0.68 (0.25–1.87); 0.451 | 1.46 (0.63–3.43); 0.38 | 4.09 (1.52–11.0); 0.005 |
| 0.22 (0.02–2.66); 0.232 | 1 | 0.52 (0.13–2.17); 0.371 | 0.84 (0.24–2.89); 0.783 | 3.40 (0.81–14.36); 0.096 | |
| Cesarean .s | 0.47 (0.20–1.1); 0.081 | 1 | 1.22 (0.8–1.87); 0.361 | 1.58 (1.06–2.40); 0.023 | 2.32 (1.32–4.10); 0.004 |
| 0.38 (0.15–0.93); 0.034 | 1 | 1.31 (0.85–2.04); 0.225 | 1.71 (1.12–2.61); 0.013 | 2.62 (1.44–4.76); 0.002 | |
| LGA | 0.19 (0.02–1.43); 0.106 | 1 | 0.55 (0.28–1.10); 0.084 | 0.93 (0.52–1.7); 0.807 | 1.57 (0.72–3.44); 0.261 |
| 0.21 (0.03–1.81); 0.157 | 1 | 0.51 (0.25–1.04); 0.065 | 0.66 (0.35–1.26); 0.209 | 0.97 (0.41–2.27); 0.935 | |
| HBW > 4000 g | 0.16 (0.02–1.25); 0.081 | 1 | 0.47 (0.24–0.90); 0.030 | 0.76 (0.43–1.4); 0.346 | 1.79 (0.85–3.78); 0.127 |
| 0.16 (0.02–1.36); 0.094 | 1 | 0.50 (0.24–1.04); 0.062 | 0.69 (0.36–1.32); 0.259 | 1.45 (0.62–3.41); 0.394 | |
| GH | 0.66 (0.14–3.12); 0.602 | 1 | 1.54 (0.74–3.21); 0.244 | 2.00 (1.0–3.94); 0.044 | 3.23 (1.41–7.38); 0.005 |
| 0.54 (0.11–2.69); 0.450 | 1 | 1.84 (0.82–4.11); 0.137 | 2.34 (1.10–5.01); 0.028 | 3.09 (1.21–7.91); 0.018 | |
| GDM-1 | 0.48 (0.10–2.20); 0.342 | 1 | 0.90 (0.44–1.82); 0.767 | 2.07 (1.10–3.80); 0.019 | 2.15 (0.97–4.80); 0.061 |
| 0.39 (0.08–1.82); 0.228 | 1 | 1.11 (0.53–2.29); 0.789 | 2.55 (1.33–4.9); 0.005 | 2.72 (1.15–6.42); 0.023 | |
| GDM-2 | NC | 1 | 0.95 (0.22–4.06); 0.949 | 1.32 (0.36–4.9); 0.675 | 2.15 (0.42–11.0); 0.357 |
| NC | 1 | 0.48 (0.09–2.55); 0.385 | 0.72 (0.16–3.19); 0.670 | 0.96 (0.14–6.57); 0.969 | |
| Odds Ratios of Pregnancy Results for Maternal Age with Regard to the Age Range of 18–24 Years | |||||
|---|---|---|---|---|---|
| Outcomes | 18–24 Years OR (95% CI); p AOR (95% CI); p | 25–29 Years OR (95% CI); p AOR (95% CI); p | 30–34 Years OR (95% CI); p AOR (95% CI); p | 35–39 Years OR (95% CI); p AOR (95% CI); p | ≥40 Years OR (95% CI); p AOR (95% CI); p |
| PE | 1 | 0.28 (0.04–2.02); 0.204 | 0.42 (0.08–2.23); 0.306 | 0.76 (0.17–3.46); 0.719 | 0.31 (0.03–3.49); 0.339 |
| 1 | 0.29 (0.04–2.24); 0.234 | 0.43 (0.07–2.58); 0.357 | 0.64 (0.12–3.38); 0.595 | 0.18 (0.01–2.51); 0.205 | |
| IUGR | 1 | 0.41 (0.07–2.53); 0.334 | 0.40 (0.07–2.11); 0.278 | 0.39 (0.08–1.9); 0.243 | 0.80 (0.13–5.02); 0.814 |
| 1 | 0.66 (0.10–4.50); 0.673 | 0.76 (0.13–4.64); 0.769 | 0.86 (0.15–5.07); 0.871 | 1.59 (0.21–11.86); 0.651 | |
| GA <37 w. | 1 | 0.46 (0.13–1.66); 0.235 | 0.42 (0.13–1.38); 0.151 | 0.88 (0.3–2.62); 0.822 | 0.91 (0.25–3.33); 0.890 |
| 1 | 0.60 (0.14–2.57); 0.491 | 0.46 (0.11–1.83); 0.270 | 0.83 (0.22–3.12); 0.786 | 0.87 (0.19–3.93); 0.855 | |
| SGA | 1 | 0.78 (0.26–2.35); 0.662 | 0.37 (0.12–1.13); 0.081 | 0.65 (0.24–1.78); 0.404 | 1.44 (0.46–4.51); 0.533 |
| 1 | 1.58 (0.47–5.33); 0.463 | 0.75 (0.22–2.56); 0.641 | 1.31 (0.4–4.25); 0.655 | 2.59 (0.69–9.77); 0.161 | |
| LBW | 1 | 0.72 (0.18–2.92); 0.643 | 0.49 (0.13–1.88); 0.297 | 1.05 (0.31–3.62); 0.937 | 2.94 (0.77–11.2); 0.114 |
| 1 | 4.63 (0.38–57.0); 0.232 | 2.41 (0.2–29.71); 0.492 | 3.89 (0.35–42.9); 0.268 | 15.73 (1.3–196.9); 0.033 | |
| Cesarean s. | 1 | 2.13 (0.91–4.97); 0.081 | 2.60 (1.15–5.87); 0.022 | 3.36 (1.51–7.47); 0.003 | 4.94 (2.02–12.1); <0.001 |
| 1 | 2.67 (1.08–6.61); 0.034 | 3.50 (1.44–8.5); 0.006 | 4.55 (1.89–11.0); 0.001 | 6.97 (2.63–18.5); <0.001 | |
| LGA | 1 | 5.42 (0.7–42.06); 0.106 | 2.96 (0.38–22.9); 0.297 | 5.04 (0.67–37.7); 0.115 | 8.50 (1.06–68.0); 0.044 |
| 1 | 4.69 (0.55–40.0); 0.157 | 2.39 (0.28–20.2); 0.424 | 3.12 (0.38–25.6); 0.290 | 4.53 (0.51–40.0); 0.174 | |
| HBW > 4000 g | 1 | 6.15 (0.8–47.46); 0.081 | 2.92 (0.38–22.5); 0.304 | 4.68 (0.63–35.0); 0.133 | 11.02 (1.39–87.3); 0.023 |
| 1 | 6.17 (0.73–52.0); 0.094 | 3.08 (0.37–25.9); 0.301 | 4.23 (0.52–34.6); 0.179 | 8.95 (1.02–78.4); 0.048 | |
| GH | 1 | 1.51 (0.32–7.13); 0.602 | 2.33 (0.53–10.2); 0.261 | 3.03 (0.71–12.9); 0.135 | 4.88 (1.06–22.5); 0.042 |
| 1 | 1.86 (0.37–9.33); 0.450 | 3.42 (0.73–16.1); 0.119 | 4.36 (0.94–20.1); 0.059 | 5.76 (1.14–29.0); 0.034 | |
| GDM-1 | 1 | 2.09 (0.46–9.63); 0.342 | 1.88 (0.43–8.34); 0.405 | 4.33 (1.02–18.4); 0.047 | 4.51 (0.97–21.0); 0.055 |
| 1 | 2.60 (0.55–12.3); 0.228 | 2.87 (0.62–13.2); 0.176 | 6.64 (1.49–29.6); 0.013 | 7.06 (1.43–34.7); 0.016 | |
| GDM-2 | NC | - | - | - | - |
| NC | - | - | - | - | |
| Age (Years) | 25–29 Years (n = 144) | 35–39 Years (n = 403) | 40–45 Years (n = 76) | ||
|---|---|---|---|---|---|
| Outcomes/ BMI categories | Cases/Controls | Cases/Controls | OR(95%CI); p * | Cases/Controls | OR (95%CI); p * |
| PE | |||||
| Whole cohort | 2/131 | 14/333 | 2.75 (0.60–12.3); 0.184 | 1/59 | 1.11 (0.1–12.49); 0.933 |
| Underweight | 0/10 | 0/14 | 0/1 | ||
| Normal BMI | 1/94 | 6/224 | 2.52 (0.3–21.2); 0.396 | 1/36 | 2.61 (0.16–42.87); 0.501 |
| Overweight | 0/19 | 2/67 | 0/16 | ||
| Obesity | 1/8 | 6/28 | 1.71 (0.18–16.4); 0.640 | 0/6 | |
| BMI ≥25 kg/m2 | 1/27 | 8/95 | 2.27 (0.27–18.99); 0,448 | 0/22 | |
| IUGR | |||||
| Whole cohort | 3/140 | 8/391 | 0.96 (0.25–3.65); 0.946 | 3/71 | 1.97 (0.39–10.0); 0.413 |
| Underweight | 1/9 | 0/14 | 0/1 | ||
| Normal BMI | 2/99 | 4/252 | 0.79 (0.14–4.36); 0.783 | 3/37 | 4.01 (0.65–24.99); 0.136 |
| Overweight | 0/22 | 0/81 | 0/20 | ||
| Obesity | 0/10 | 4/44 | 0/13 | ||
| BMI ≥25 kg/m2 | 0/32 | 4/125 | 0/33 | ||
| GA <37th w. | |||||
| Whole cohort | 7/137 | 36/367 | 1.92 (0.84–4.42); 0.125 | 7/69 | 1.99 (0.67–5.89); 0.216 |
| Underweight | 0/10 | 1/13 | 0/1 | ||
| Normal BMI | 6/96 | 19/238 | 1.28 (0.5–3.3); 0.613 | 4/38 | 1.68 (0.45–6.3); 0.439 |
| Overweight | 0/22 | 5/78 | 2/18 | ||
| Obesity | 1/9 | 11/38 | 2.61 (0.3–22.87); 0.388 | 1/12 | 0.75 (0.04–13.7); 0.846 |
| BMI ≥25 kg/m2 | 1/31 | 16/116 | 4.28 (0.55–33.51); 0.167 | 3/30 | 3.10 (0.31–31.5); 0.339 |
| SGA | |||||
| Whole cohort | 13/113 | 31/324 | 0.83 (0.42–1.65); 0.596 | 11/52 | 1.84 (0.77–4.38); 0.169 |
| Underweight | 3/6 | 0/13 | 0/1 | ||
| Normal BMI | 8/84 | 17/216 | 0.83 (0.34–1.99); 0.67 | 8/27 | 3.11 (1.07–9.09); 0.038 |
| Overweight | 1/16 | 9/66 | 2.18 (0.26–18.49); 0.474 | 2/15 | 2.13 (0.18–26.03); 0.553 |
| Obesity | 1/7 | 5/29 | 1.21 (0.12–12.04); 0.873 | 1/9 | 0.78 (0.04–14.75); 0.867 |
| BMI ≥25 kg/m2 | 2/23 | 14/95 | 1.70 (0.36–7.99); 0.505 | 3/24 | 1.44 (0.22–9.41); 0.705 |
| LBW | |||||
| Whole cohort | 7/117 | 29/331 | 1.46 (0.63–3.43); 0.38 | 12/49 | 4.09 (1.52–11.0); 0.005 |
| Underweight | 0/9 | 1/12 | 0/1 | ||
| Normal BMI | 5/86 | 12/228 | 0.91 (0.31–2.65); 0.856 | 8/26 | 5.29 (1.59–17.58); 0.007 |
| Overweight | 1/15 | 7/65 | 1.62 (0.19–14.14); 0.665 | 3/13 | 3.46 (0.32–37.47); 0.307 |
| Obesity | 1/7 | 9/26 | 2.42 (0.26–22.49); 0.436 | 1/9 | 0.78 (0.04–14.75); 0.867 |
| BMI ≥25 kg/m2 | 2/22 | 16/91 | 1.93 (0.41–9.04); 0.402 | 4/22 | 2.00 (0.33–12.07); 0.450 |
| Cesarean s. | |||||
| Whole cohort | 50/94 | 184/219 | 1.58 (1.06–2.40); 0.023 | 42/34 | 2.32 (1.32–4.10); 0.004 |
| Underweight | 2/8 | 9/5 | 7.20 (1.08–47.96); 0.041 | 0/1 | |
| Normal BMI | 33/69 | 116/141 | 1.72 (1.06–2.79); 0.027 | 24/18 | 2.79 (1.33–5.84); 0.007 |
| Overweight | 9/13 | 28/55 | 0.74 (0.28–1.93); 0.532 | 8/12 | 0.96 (0.28–3.31); 0.952 |
| Obesity | 6/4 | 31/18 | 1.15 (0.29–4.62); 0.846 | 10/3 | 2.22 (0.37–13.54); 0.386 |
| BMI ≥25 kg/m2 | 15/17 | 59/73 | 0.92 (0.42–1.99); 0.824 | 18/15 | 1.36 (0.51–3.61); 0.537 |
| LGA | |||||
| Whole cohort | 18/113 | 48/324 | 0.93 (0.52–1.7); 0.807 | 13/52 | 1.57 (0.72–3.44); 0.261 |
| Underweight | 1/6 | 1/13 | 0.46 (0.03–8.69); 0.606 | 0/1 | |
| Normal BMI | 10/84 | 24/216 | 0.93 (0.43–2.04); 0.862 | 7/27 | 2.18 (0.76–6.28); 0.15 |
| Overweight | 5/16 | 8/66 | 0.39 (0.11–1.35); 0.136 | 3/15 | 0.64 (0.13–3.16); 0.583 |
| Obesity | 2/7 | 15/29 | 1.81 (0.33–9.82); 0.491 | 3/9 | 1.17 (0.15–9.01); 0.882 |
| BMI ≥25 kg/m2 | 7/23 | 23/95 | 0.80 (0.3–2.08); 0.641 | 6/24 | 0.82 (0.24–2.81); 0.754 |
| HBW >4000 g | |||||
| Whole cohort | 20/117 | 43/331 | 0.76 (0.43–1.4); 0.346 | 15/49 | 1.79 (0.85–3.78); 0.127 |
| Underweight | 1/9 | 1/12 | 0.75 (0.04–13.68); 0.846 | 0/1 | |
| Normal BMI | 11/86 | 17/228 | 0.58 (0.26–1.3); 0.185 | 8/26 | 2.41 (0.88–6.61); 0.089 |
| Overweight | 6/15 | 11/65 | 0.42 (0.14–1.33); 0.14 | 4/13 | 0.77 (0.18–3.34); 0.726 |
| Obesity | 2/7 | 14/26 | 1.89 (0.34–10.32); 0.465 | 3/9 | 1.17 (0.15–9.01); 0.882 |
| BMI ≥25 kg/m2 | 8/22 | 25/91 | 0.76 (0.3–1.9); 0.551 | 7/22 | 0.88 (0.27–2.83); 0.824 |
| GH | |||||
| Whole cohort | 11/131 | 56/333 | 2.00 (1.0–3.94); 0.044 | 16/59 | 3.23 (1.41–7.38); 0.005 |
| Underweight | 0/10 | 0/14 | 0/1 | ||
| Normal BMI | 7/94 | 27/224 | 1.62 (0.68–3.85); 0.275 | 5/36 | 1.87 (0.56–6.26); 0.313 |
| Overweight | 3/19 | 14/67 | 1.32 (0.34–5.09); 0.683 | 4/16 | 1.58 (0.31–8.15); 0.582 |
| Obesity | 1/8 | 15/28 | 4.29 (0.49–37.59); 0.189 | 7/6 | 9.33 (0.89–97.62); 0.062 |
| BMI ≥25 kg/m2 | 4/27 | 29/95 | 2.06 (0.67–6.38); 0.21 | 11/22 | 3.38 (0.94–12.08); 0.062 |
| GDM-1 | |||||
| Whole cohort | 14/127 | 73/320 | 2.07 (1.10–3.80); 0.019 | 14/59 | 2.15 (0.97–4.80); 0.061 |
| Underweight | 3/7 | 2/11 | 0.42 (0.06–3.21); 0.407 | 0/1 | |
| Normal BMI | 7/93 | 43/211 | 2.71 (1.17–6.24); 0.019 | 7/34 | 2.74 (0.89–8.37); 0.078 |
| Overweight | 2/20 | 13/67 | 1.94 (0.4–9.33); 0.408 | 2/16 | 1.25 (0.16–9.88); 0.832 |
| Obesity | 2/7 | 15/31 | 1.69 (0.31–9.16); 0.541 | 5/8 | 2.19 (0.32–15.04); 0.426 |
| BMI ≥25 kg/m2 | 4/27 | 28/98 | 1.93 (0.62–5.98); 0.255 | 7/24 | 1.97 (0.51–7.56); 0.324 |
| GDM-2 | |||||
| Whole cohort | 3/127 | 10/320 | 1.32 (0.36–4.9); 0.675 | 3/59 | 2.15 (0.42–11.0); 0.357 |
| Underweight | 0/7 | 1/11 | 0/1 | ||
| Normal BMI | 2/93 | 3/211 | 0.66 (0.11–4.02); 0.653 | 1/34 | 1.37 (0.12–15.57); 0.801 |
| Overweight | 0/20 | 3/67 | 2/16 | ||
| Obesity | 1/7 | 3/31 | 0.68 (0.06–7.52); 0.751 | 0/8 | |
| BMI ≥25 kg/m2 | 1/27 | 6/98 | 1.65 (0.19–14.33); 0.648 | 2/24 | 2.25 (0.19–26.41); 0.519 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lewandowska, M.; Sajdak, S.; Więckowska, B.; Manevska, N.; Lubiński, J. The Influence of Maternal BMI on Adverse Pregnancy Outcomes in Older Women. Nutrients 2020, 12, 2838. https://doi.org/10.3390/nu12092838
Lewandowska M, Sajdak S, Więckowska B, Manevska N, Lubiński J. The Influence of Maternal BMI on Adverse Pregnancy Outcomes in Older Women. Nutrients. 2020; 12(9):2838. https://doi.org/10.3390/nu12092838
Chicago/Turabian StyleLewandowska, Małgorzata, Stefan Sajdak, Barbara Więckowska, Nevena Manevska, and Jan Lubiński. 2020. "The Influence of Maternal BMI on Adverse Pregnancy Outcomes in Older Women" Nutrients 12, no. 9: 2838. https://doi.org/10.3390/nu12092838
APA StyleLewandowska, M., Sajdak, S., Więckowska, B., Manevska, N., & Lubiński, J. (2020). The Influence of Maternal BMI on Adverse Pregnancy Outcomes in Older Women. Nutrients, 12(9), 2838. https://doi.org/10.3390/nu12092838





