Wayfinding in People with Alzheimer’s Disease: Perspective Taking and Architectural Cognition—A Vision Paper on Future Dementia Care Research Opportunities
Abstract
1. Introduction
1.1. Dementia and Wayfinding
1.2. Aims and Scope
2. Wayfinding Challenges in the Context of Dementia of the Alzheimer’s Type
2.1. The Concepts of Wayfinding, Architectural Cognition, and Perspective Taking
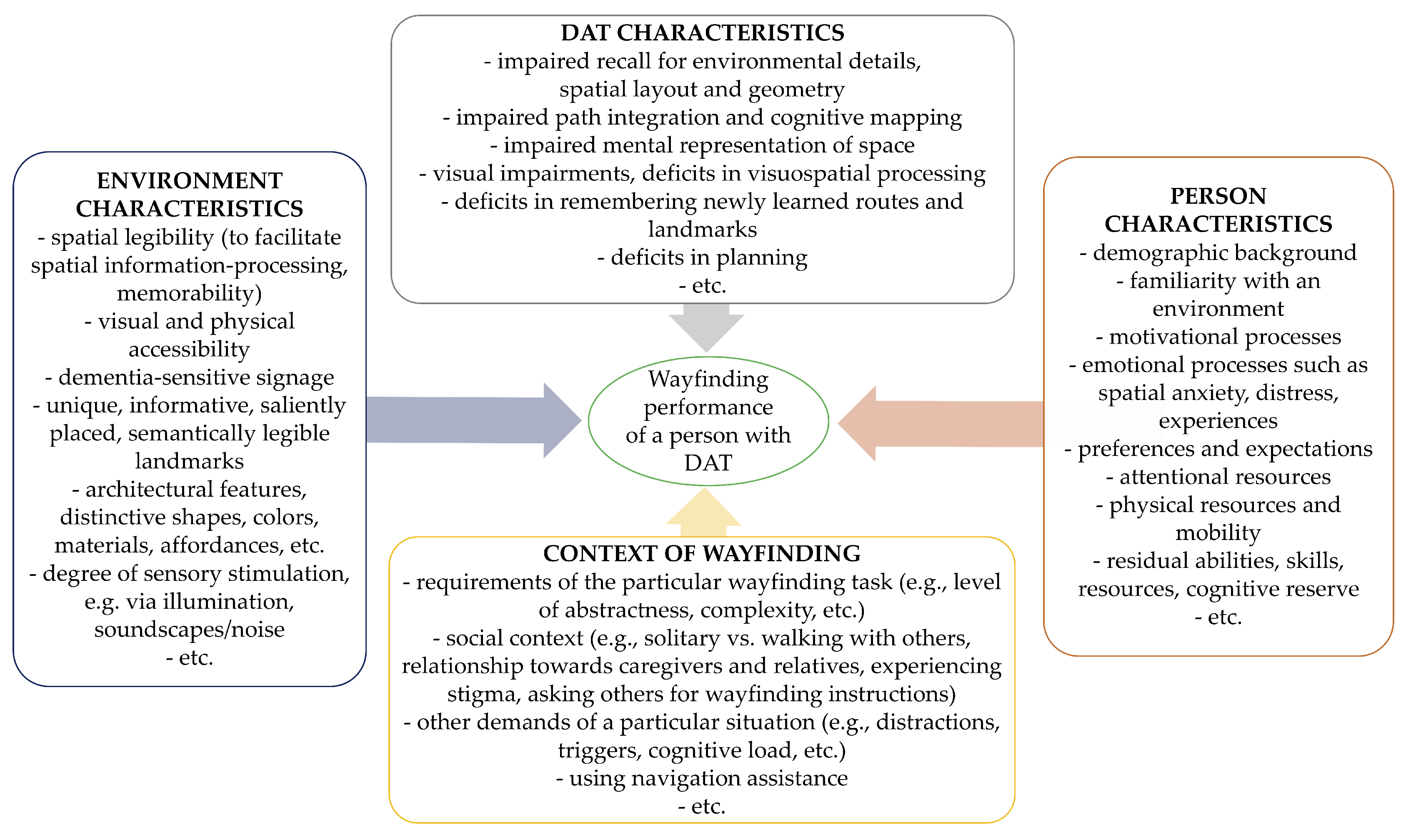
- In sum, successful wayfinding is linked a complex interplay of contributing factors, both spatial and non-spatial. Importantly, wayfinding is a highly complex cognitive problem-solving process, relying on several brain functions. Yet, in people living with DAT, neurodegeneration causes wayfinding processes to be disrupted, as the next section describes, and planning wayfinding support for this target group requires awareness and consideration of this complexity.
2.2. Wayfinding and Spatial Orientation in the Context of Dementia of the Alzheimer’s Type
- In sum, people with DAT can face challenges with all stages of wayfinding as defined in Section 2.1; and in both unfamiliar as well as familiar environments (depending on the stage of the disease): with spatial reasoning needed for planning routes, with monitoring whether one is on the chosen route towards the destination, with recognizing the destination, and with directing attention to information relevant for solving a particular wayfinding task.
2.3. Consequences of Wayfinding Challenges for People with Dementia
- In sum, for people with DAT, spatial orientation and wayfinding challenges can have strong behavioral, emotional, and social consequences. Hence, the next section develops a perspective, how wayfinding in people with dementia might be supported via the built environment.
3. Planning and Evaluating Dementia-Sensitive Built Space
3.1. The Concept of Dementia Sensitivity
- In sum, for dementia-sensitive environments, the impairments (e.g., processing environmental information; potentially being distracted by environmental cues that are irrelevant to solving a wayfinding task; or having a low threshold for sensory stimulation) in terms of the design of built space might be translated to simply relying on simplified geometries, landmarks, and spatial functions. However, in its full potential, built space would equally address a personal sense of coherence/meaningfulness, and an optimized ambience, while also offering dementia-sensitive engagement, and while supporting spatial orientation and wayfinding.
3.2. Environmental Design Principles
- In sum, the core component of dementia-sensitive indoor and outdoor environments is spatial legibility, the degree to which an environment facilitates spatial information-processing. In this context, simplicity and safety are key planning principles in current approaches. In the view of the authors, a dementia-sensitive built space must be tailored specifically to the needs and perspective of a person with dementia (e.g., via appropriate dementia-sensitive levels of stimulation and supportive orientation cues), whilst also offering factors that support positive, meaningful experiences (e.g., dementia-sensitive ambiences or sensory interaction that involves more than one sense). This requires evaluating planned and existing built environments from the perspective of people with dementia.
- A first challenge is acquiring informed consent, as the person may forget having agreed to participation, while already participating in the study. Researchers can use proxy consents by caregivers or relatives, or ongoing consent where the person is informed, and asked whether they like to continue, both at the beginning of the study, as well as continuously throughout the data collection [101].
- A second challenge is to refine participatory dementia-sensitive methods. To more closely integrate the perspective of people with dementia in research and planning processes, researchers may need to develop alternative measures [102] and creative analytic formats [103]. On a content level, this includes developing methods that do not overwhelm but support people with DAT to, from their perspective, identify useful wayfinding cues. For instance, they could identify wayfinding cues involving more than one sense, rather than landmarks/geometries that appeal mainly to the visual sense. In each case, we deem it important that the research revolves more closely around their perspective, even if it may be challenging to develop sensitive methods.
- A third challenge is that the plethora of studies about dementia-sensitive indoor (and to a lesser degree outdoor) environments makes it harder for non-researchers (i.e., planners of built space or dementia caregivers) to identify which studies are methodologically sound (e.g., simple geometries) and, hence, provide evidence for guidelines; and which ones show interesting directions, but contain study limitations and, hence, remain to be tested further (e.g., color recommendations). This also brings along the question how to translate research insights into practice (e.g., into an environmental design or intervention). Translation, in itself, is a complex endeavor [104,105] with many barriers (such as interpreting heterogeneous research outcomes) and practical issues (such as financial or organizational barriers).
- In addition, different research disciplines, e.g., psychological research and architectural planning, typically rely on different methods, paradigms, and expertise (e.g., [106]). Here, developing a shared terminology between disciplines may facilitate a more nuanced perspective taking [107]. In our view, structuring participatory research approaches, and reaching a common terminology of concepts might be valuable for fostering interdisciplinary collaborations. Also, researchers and planners, in a combined effort, could collaborate to reach their shared aim of supporting wayfinding via a dementia-sensitive built environment.
3.3. Environmental Interventions
- In sum, research about the perspective of people with dementia is beneficial to guide future environmental intervention approaches, e.g., by providing both the scientific knowledge as well as the evaluation methods for assessing dementia-sensitive environments.
- One challenge in the aforementioned context is that, based on the subjective individual perspective, needs, and abilities, researchers, planners, and caregivers often need to generalize insights to develop design principles or environmental interventions that accommodate the needs of a largest possible number of people. Yet, averaging individual backgrounds, e.g., cultural aspects, if applied without deeper reflection, may cause a design that is functional, but misses its full potential. In the view of the authors, this is where research could measure wayfinding challenges in field settings, and optimize spatial legibility and lived experience based on the perspective of people with DAT.
- Another challenge is that, while numerous discussions of how environmental factors can support people with dementia exist, few focus specifically on evaluating spatial orientation and wayfinding from the perspective of people with DAT. In our view, it is worthwhile to identify, in a more nuanced way, how to integrate the perspective of people with dementia in design and planning processes. For instance, from the perspective of a person with dementia, space is not only related to physical and social environments, but in itself may become an existential experience, where a sense of continuity, self-identity, sense of place-attachment, familiarity, and autonomy remain relevant existential concepts that need to be preserved [79].
3.4. Environmental Evaluation Tools and Strategies
- In sum, the key source for informing evaluation tools and strategies for dementia-sensitive environments is the perspective of people living with dementia. In particular, the use of contradicting information in dementia-sensitive strategies may indicate a need for identifying ways to continuously integrate research results into planning, and to translate research knowledge into support tools and interventions for planners. Such efforts could also distinguish results that are reliable, yet still falsifiable, from innovative pilot-studies that need follow-up studies. Thus, while, undoubtedly, such existing efforts are both timely and needed, they might benefit from further refinements based on research theory and experimental insights (also cf. [34,35,118]).
- A first challenge is that it currently remains unclear how the perspective of people with dementia could be further translated into early design and planning stages. We propose refining participatory methods and co-research, as Section 4 further describes.
- Additionally, it is unclear whether existing principles would work similarly both for indoor (care institutions) and outdoor environments (districts, public buildings). Broad design principles are useful as they raise awareness and sensitivity. Yet, if research results are applied without further reflection on the changing stages and needs in dementia and across generations, these principles might not reach their full potential.
- Additionally, in terms of advancing dementia-sensitive design and planning guidelines, one research avenue is to measure wayfinding challenges in a more nuanced way, and potentially over an extended period of time, to identify more responsive, dynamic solutions that respond to individual backgrounds and changing stages of the disease and aging.
3.5. Design and Planning Processes of Built Space
- In sum, the complexity of the design and planning process may be a reason why perspective taking of a person with limited resources is challenging. While the needs of people with vulnerabilities might be represented in specific guidelines/norms, various design requirements and stakeholder interactions can influence the final planning decisions and design outcomes.
- One challenge is that the design and planning process is highly complex, with multiple requirements and stakeholders influencing decision-making. These requirements can draw attention away from designing from the perspective of a person with dementia. We envision iterative interventions for planners that inform early stages of planning that emphasize the perspective of people with dementia. In addition, wayfinding processes in people with dementia rely on highly complex interactions between the person, context, and the environment. It is worthwhile to examine how these complexities can be generalized and translated into interventions for planners, without oversimplifying the perspective of people with dementia.
- A second challenge is that it can be hard for environmental planners to anticipate the perspective of a person with limited attentional, motivational, or physical resources. Additionally, research studies combining cognitive and behavioral measures in naturalistic tasks in the field are rare, and often contain low sample sizes. We envision that research using naturalistic tasks and in field settings can refine this perspective; while also translating this perspective into an appropriate format that can supplement existing design and planning processes. Furthermore, inclusive or participatory methods could be regarded as general requirement in future studies.
- A third challenge depends on whether all involved stakeholders in a planning and design process are equally interested in supporting people with dementia; specifically, if built space needs to serve diverse groups of users and various competing interests (such as in the retail context). Raising awareness on the importance of dementia-sensitive built space is one step. Yet, it may be needed to mandate principles for dementia sensitivity as a general requirement for urban planning, with the goal of establishing demographically sustainable future cities.
4. Opportunities for Future Dementia Care Research
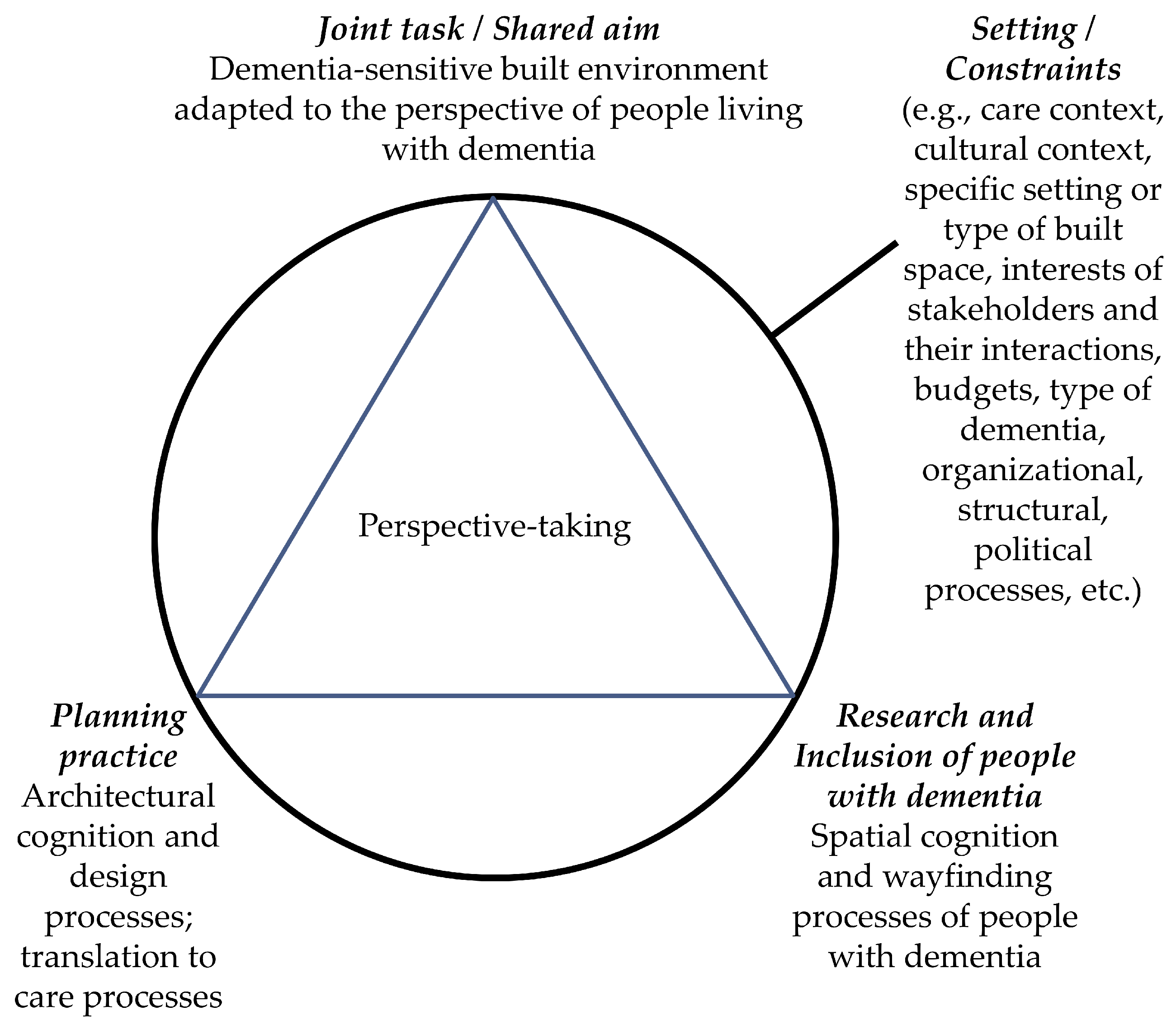
4.1. Interdisciplinary Research Vision
- Research: understanding the complexities and perspective of people with dementia during wayfinding, and advancing inclusive, interdisciplinary research methods, in order to indicate which residual abilities exist, and to identify how the person might be supported via the built environment (wayfinding processes and spatial cognition).
- Planning: integrating and translating research knowledge about the experiences and perspective of people with DAT into planning processes, to ultimately reach optimized dementia-sensitive outcomes that also impact care processes (planning processes and architectural/urban cognition).
4.2. Methods for Perspective Taking in Research
4.2.1. Inclusion of People with Dementia
4.2.2. Translating Laboratory Results back to Real-World Settings
4.2.3. Mixed Methods: Linking Spatial and Physiological Data
- In sum, future research could refine dementia-sensitive, inclusive research methods, so that affected people can voice their preferences for support structures in the built environment. Using mixed-method approaches, qualitative measures, such as photovoice, co-creation, or other participatory methods, can be combined with quantitative measures, such as systematic behavioral observations, and using naturalistic tasks in the field. Translating laboratory results back to real-world settings, but also identifying realistic paradigms and naturalistic tasks for laboratory research (e.g., using virtual reality), remain important avenues for future studies.
4.3. Methods for Perspective Taking in Design and Planning Practice
4.3.1. Analyzing Architectural Cognition and Design Processes
4.3.2. Supplementing the Perspective of People with Dementia into Planning and Design
4.3.3. Translating Research Insights back to Care Processes
- In sum, future research could more closely collaborate with planners, to understand architectural cognition, to identify opportunities for integrating the perspective of people with dementia into planning and design practice, as well as develop interventions that target raising awareness on the importance of wayfinding, to translate research evidence and knowledge to care processes.
4.4. Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- United Nations. 2019 Revision of World Population Prospects. United Nations (Ed.). 2019. Available online: https://population.un.org/wpp (accessed on 6. January 2021).
- World Health Organization. Decade of Healthy Ageing 2020–2030. 2015. Available online: https://www.who.int/ageing/decade-of-healthy-ageing (accessed on 7 August 2020).
- Alzheimer’s Disease International. World Alzheimer Report 2015: The Global Impact of Dementia: An Analysis of Prevalence, Incidence, Cost and Trends. 2015. Available online: https://www.alzint.org/resource/world-alzheimer-report-2015 (accessed on 5 January 2021).
- World Health Organization. Risk Factors for Dementia. 2016. Available online: https://www.alzheimers.org.uk/sites/default/files/pdf/factsheet_risk_factors_for_dementia.pdf (accessed on 7 August 2020).
- Prince, M.; Guerchet, M.; Prina, M. The Epidemiology and Impact of Dementia: Current State and Future Trends. First WHO Ministerial Conference on the Global Action Against Dementia (pp. 1–4). King’s College London: World Health Organization. 2015. Available online: https://www.who.int/mental_health/neurology/dementia/dementia_thematicbrief_epidemiology.pdf (accessed on 7 August 2020).
- World Health Organization. Global Action Plan on the Public Health Response to Dementia 2017–2025. Geneva. 2017. Available online: https://apps.who.int/iris/bitstream/handle/10665/259615/9789241513487-eng.pdf (accessed on 9 December 2020).
- Ritchie, H. Our World in Data: Urbanization. 2017. Available online: https://ourworldindata.org/urbanization (accessed on 20 August 2020).
- Cho, I.S.; Trivic, Z.; Nasution, I. Towards an Integrated Urban Space Framework for Emerging Urban Conditions in a High-Density Context. J. Urban Des. 2015, 20, 147–168. [Google Scholar] [CrossRef]
- Madanipour, A. Roles and Challenges of Urban Design. J. Urban Des. 2006, 11, 173–193. [Google Scholar] [CrossRef]
- Camarinha-Matos, L.M.; Afsarmanesh, H. Collaborative Networks in Active Ageing—A Roadmap Contribution to Demographic Sustainability. Prod. Plan. Control 2011, 23, 279–298. [Google Scholar] [CrossRef]
- Stern, E. Demographic Sustainability and Rural Development Policy. J. Maps 2013, 9, 154–160. [Google Scholar] [CrossRef]
- Marquardt, G. Mati: Mensch—Architektur—Technik—Interaktion Für Demografische Nachhaltigkeit; Fraunhofer IRB Verlag: Dresden/Stuttgart, Germany, 2015; ISBN 978-3816794721. [Google Scholar]
- Braak, H.; Braak, E. Neuropathological Stageing of Alzheimer-Related Changes. Acta Neuropathol. 1991, 82, 239–259. [Google Scholar] [CrossRef] [PubMed]
- Jolles, J. Cognitive, Emotional and Behavioral Dysfunctions in Aging and Dementia. In Aging of the Brain and Alzheimer’s Disease; Schwaab, D.F., Fliers, M., Mirmiram, M., VanGool, W.A., VanHaaren, F., Eds.; Elsevier: Amsterdam, The Netherlands, 1986; Volume 70, pp. 15–39. [Google Scholar]
- Whitwell, J.L. Progression of Atrophy in Alzheimer’s Disease and Related Disorders. Neurotox Res. 2010, 18, 339–346. [Google Scholar] [CrossRef]
- Maier, W.; Barnikol, U.B. Neurocognitive Disorders in DSM-5: Pervasive Changes in the Diagnostics of Dementia. Nervenarzt 2014, 85, 564–570. [Google Scholar] [CrossRef]
- Sachdev, P.S.; Blacker, D.; Blazer, D.G.; Ganguli, M.; Jeste, D.V.; Paulsen, J.S.; Petersen, R.C. Classifying Neurocognitive Disorders: The DSM-5 Approach. Nat. Rev. Neurol. 2014, 10, 634–642. [Google Scholar] [CrossRef]
- Willis, S.L.; Allen-Burge, R.; Dolan, M.M.; Bertrand, R.M.; Yesavage, J.; Taylor, J.L. Everyday Problem Solving among Individuals with Alzheimer’s Disease. Gerontologist 1998, 38, 569–577. [Google Scholar] [CrossRef]
- Lipowski, Z.J. Differentiating Delirium from Dementia in the Elderly. Clin. Gerontol. 2008, 1, 3–10. [Google Scholar] [CrossRef]
- Machleidt, W.; Bauer, M.; Lamprecht, F.; Rose, H.K.; Rohde-Dachser, C. Psychiatrie Psychosomatik Und Psychotherapie; Thieme: New York, NY, USA, 2004; Volume 7, ISBN 3134956071. [Google Scholar]
- World Health Organization. ICD-10-WHO-Version 2019. 2019. Available online: https://www.dimdi.de/static/de/klassifikationen/icd/icd-10-who/kode-suche/htmlamtl2019/block-f00-f09.htm (accessed on 8 December 2020).
- German Ministry of Health. Diagnose Demenz: Krankheitsbild Und Verlauf. 2020. Available online: https://www.bundesgesundheitsministerium.de/themen/pflege/online-ratgeber-demenz/krankheitsbild-und-verlauf.html (accessed on 7 August 2020).
- Grady, C.L.; Haxby, J.V.; Horwitz, B.; Sundaram, M.; Berg, G.; Schapiro, M.; Rapoport, S.I. Longitudinal Study of the Early Neuropsychological and Cerebral Metabolic Changes in Dementia of the Alzheimer Type. J. Clin. Exp. Neuropsychol. 1988, 10, 576–596. [Google Scholar] [CrossRef] [PubMed]
- Cherrier, M.M.; Mendez, M.; Perryman, K. Route Learning Performance in Alzheimer Disease Patients. Neuropsychiatry Neuropsychol. Behav. Neurol. 2001, 14, 159–168. Available online: https://www.ncbi.nlm.nih.gov/pubmed/11513099 (accessed on 25 August 2020).
- DeIpolyi, A.R.; Rankin, K.P.; Mucke, L.; Miller, B.L.; Gorno-Tempini, M.L. Spatial Cognition and the Human Navigation Network in AD and MCI. Neurology 2007, 69, 986–997. [Google Scholar] [CrossRef] [PubMed]
- Lithfous, S.; Dufour, A.; Despres, O. Spatial Navigation in Normal Aging and the Prodromal Stage of Alzheimer’s Disease: Insights from Imaging and Behavioral Studies. Age. Res Rev. 2013, 12, 201–213. [Google Scholar] [CrossRef] [PubMed]
- Golledge, R.G. Place Recognition and Wayfinding: Making Sense of Space. Geoforum 1992, 23, 199–214. [Google Scholar] [CrossRef]
- Mcshane, R.; Gedling, K.; Keene, J.; Fairburn, C.; Jacoby, R.; Hope, T. Getting Lost in Dementia: A Longitudinal Study of a Behavioral Symptom. Int. Psychogeriatr. 1998, 10, 253–260. [Google Scholar] [CrossRef]
- Bantry White, E.; Montgomery, P. Dementia, Walking Outdoors and Getting Lost: Incidence, Risk Factors and Consequences from Dementia-Related Police Missing-Person Reports. Aging Ment. Health 2015, 19, 224–230. [Google Scholar] [CrossRef]
- Mitchell, L.; Burton, E.; Raman, S. Dementia-Friendly Cities: Designing Intelligible Neighbourhoods for Life. J. Urban Des. 2004, 9, 89–101. [Google Scholar] [CrossRef]
- Mitchell, L.; Burton, E.; Raman, S.; Blackman, T.; Jenks, M.; Williams, K. Making the Outside World Dementia-Friendly: Design Issues and Considerations. Environ. Plan. B Plan. Des. 2016, 30, 605–632. [Google Scholar] [CrossRef]
- Passini, R.; Pigot, H.; Rainville, C.; Tétreault, M.-H. Wayfinding in a Nursing Home for Advanced Dementia of the Alzheimer’s Type. Environ. Behav. 2016, 32, 684–710. [Google Scholar] [CrossRef]
- Marquardt, G.; Schmieg, P. Dementia-Friendly Architecture: Environments That Facilitate Wayfinding in Nursing Homes. Am. J. Alzheimers Dis. Other Demen. 2009, 24, 333–340. [Google Scholar] [CrossRef]
- Fleming, R.Z.J.; Bennett, K. World Alzheimer Report—Design, Dignity, Dementia. In Dementia-Related Design and the Built Environment; Alzheimer’s Disease International: London, UK, 2020; Volume 1, Available online: https://www.alzint.org/resource/world-alzheimer-report-2020/ (accessed on 19 October 2020).
- Bundesministerium Für Familie, S.; Frauen Und Jugend (Bmfsfj) Und Bundesministerium Für Gesundheit (Bmg) Germany. Nationale Demenzstrategie (Translated: National Dementia Strategy); Publikationsversand der Bundesregierung: Berlin, Germany, 2020; Volume 3BR197, Available online: https://www.nationale-demenzstrategie.de/die-strategie (accessed on 8 August 2020).
- Ministry of Health Welfare and Sport. National Dementia Strategy 2021–2030; Ministry of Health Welfare and Sport: The Hague, The Netherlands, 2021. Available online: www.rijksoverheid.nl/VWS (accessed on 6 January 2021).
- O’Malley, M.; Innes, A.; Wiener, J.M. (Dis)Orientation and Design Preferences within an Unfamiliar Care Environment: A Content Analysis of Older Adults’ Qualitative Reports after Route Learning. Environ. Behav. 2020, 1–27. [Google Scholar] [CrossRef]
- Montello, D.R.; Sas, C. Human Factors of Wayfinding in Navigation. 2006. Available online: https://eprints.lancs.ac.uk/id/eprint/42335/1/MontelloSas.pdf (accessed on 1 July 2020).
- Montello, D.R.; Pick, H.L. Integrating Knowledge of Vertically Aligned Large-Scale Spaces. Environ. Behav. 2016, 25, 457–484. [Google Scholar] [CrossRef]
- Kitchin, R.M. Cognitive Maps: What Are They and Why Study Them? J. Environ. Psychol. 1994, 14, 1–19. [Google Scholar] [CrossRef]
- Carlson, L.A.; Hölscher, C.; Shipley, T.F.; Dalton, R.C. Getting Lost in Buildings. Curr. Dir. Psychol. Sci. 2010, 19, 284–289. [Google Scholar] [CrossRef]
- Kuliga, S.F.; Nelligan, B.; Dalton, R.C.; Marchette, S.; Shelton, A.L.; Carlson, L.; Hölscher, C. Exploring Individual Differences and Building Complexity in Wayfinding: The Case of the Seattle Central Library. Environ. Behav. 2019, 51, 622–665. [Google Scholar] [CrossRef]
- Wiener, J.M.; Büchner, S.J.; Hölscher, C. Taxonomy of Human Wayfinding Tasks: A Knowledge-Based Approach. Spatial Cogn. Comput. 2009, 9, 152–165. [Google Scholar] [CrossRef]
- Dalton, R.C.; Holscher, C.; Montello, D.R. Wayfinding as a Social Activity. Front Psychol. 2019, 10, 142. [Google Scholar] [CrossRef]
- Brorsson, A. Access to Everyday Activities in Public Space: Views of People with Dementia; Karolinska Institutet: Stockholm, Sweden, 2013; Available online: https://openarchive.ki.se/xmlui/handle/10616/41677 (accessed on 16 December 2020).
- Lee, S.Y.; Chaudhury, H.; Hung, L. Exploring Staff Perceptions on the Role of Physical Environment in Dementia Care Setting. Dementia 2016, 15, 743–755. [Google Scholar] [CrossRef]
- Hölscher, C.; Meilinger, T.; Vrachliotis, G.; Brösamle, M.; Knauff, M. Up the Down Staircase: Wayfinding Strategies in Multi-Level Buildings. J. Environ. Psychol. 2006, 26, 284–299. [Google Scholar] [CrossRef]
- Dalton, R.C.; Krukar, J.; Hölscher, C. Architectural Cognition and Behavior. In Handbook of Behavioral and Cognitive Geography; Montello, D.R., Ed.; Edward Elgar Publishing: Cheltenham, UK, 2018; pp. 337–356. [Google Scholar]
- Lynch, K. The Image of the City; MIT Press: Cambridge, MA, USA, 1960; Volume 11, ISBN 0262620014. [Google Scholar]
- Lynch, K. Reconsidering the Image of the City. In Cities of the Mind; Springer: Berlin, Germany, 1984; pp. 151–161. [Google Scholar]
- Montello, D.R. Spatial Cognition and Architectural Space: Research Perspectives. Archit. Des. 2014, 84, 74–79. [Google Scholar] [CrossRef]
- Nasar, J.L. Perception, Cognition, and Evaluation of Urban Places. In Public Places and Spaces; Altman, I., Zube, E.H., Eds.; Springer: Boston, MA, USA, 1989; pp. 31–56. [Google Scholar]
- Dalton, R.C.; Hölscher, C. Take One Building: Interdisciplinary Research Perspectives of the Seattle Central Library; Taylor & Francis/Routledge: Abingdon, UK, 2016; ISBN 1317114647. [Google Scholar]
- Brösamle, M.; Hölscher, C. Architects Seeing through the Eyes of Building Users. In Spatial Cognition in Architectural Design; Barkowsky, T., Bilda, Z., Hölscher, C., Vrachliotis, G., Eds.; Report No. 014-09/2007; Report Series of the Transregional Collaborative Research Center SFB/TR 8 Spatial Cognition; University of Bremen/Albert-Ludwigs University Freiburg: Melbourne, Australia, 2007; Volume SFB/TR 8, pp. 1–6. Available online: https://www.sfbtr8.spatial-cognition.de/papers/SFB_TR%208%20Rep%20014-09_2007.pdf (accessed on 8 August 2020).
- Brösamle, M.; Hölscher, C. The Architects’ Understanding of Human Navigation. In Movement and Orientation in Built Environments: Evaluating Design Rationale and User Cognition (within 2008 EDRAMOVE Intensive Session); Haq, S., Hölscher, C., Torgrude, S., Eds.; Report Series of the Transregional Collaborative Research Center SFB/TR 8 Spatial Cognition; Report No. 015-05/2008; University of Bremen/Albert-Ludwigs University Freiburg: Veracruz, Mexico, 2008; Volume SFB/TR 8, pp. 9–12. Available online: https://www.sfbtr8.spatial-cognition.de/papers/SFB_TR%208%20Rep%20015-05_2008.pdf#page=15 (accessed on 8 August 2020).
- Batson, C.D.; Early, S.; Salvarani, G. Perspective Taking: Imagining How Another Feels Versus Imaging How You Would Feel. Personal. Soc. Psychol. Bull. 2016, 23, 751–758. [Google Scholar] [CrossRef]
- Dalton, R.C.; Hölscher, C.; Spiers, H.J. Navigating Complex Buildings: Cognition, Neuroscience and Architectural Design. In Studying Visual and Spatial Reasoning for Design Creativity; Gero, J., Ed.; Springer: Dordrecht, The Netherlands, 2015; pp. 3–22. [Google Scholar]
- Davis, M.H. Measuring Individual Differences in Empathy: Evidence for a Multidimensional Approach. J. Personality Soc. Psychol. 1983, 44, 113–126. [Google Scholar] [CrossRef]
- Galinsky, A.D.; Maddux, W.W.; Gilin, D.; White, J.B. Why It Pays to Get inside the Head of Your Opponent: The Differential Effects of Perspective Taking and Empathy in Negotiations. Psychol. Sci. 2008, 19, 378–384. [Google Scholar] [CrossRef] [PubMed]
- Ruby, P.; Decety, J. What You Believe Versus What You Think They Believe: A Neuroimaging Study of Conceptual Perspective-Taking. Eur. J. Neurosci. 2003, 17, 2475–2480. [Google Scholar] [CrossRef] [PubMed]
- Monacelli, A.M.; Cushman, L.A.; Kavcic, V.; Duffy, C.J. Spatial Disorientation in Alzheimer’s Disease: The Remembrance of Things Passed. Neurology 2003, 61, 1491–1797. [Google Scholar] [CrossRef] [PubMed]
- Bierbrauer, A.; Kunz, L.; Gomes, C.A.; Luhmann, M.; Deuker, L.; Getzmann, S.; Axmacher, N. Unmasking Selective Path Integration Deficits in Alzheimer’s Disease Risk Carriers. Sci. Adv. 2020, 6, eaba1394. [Google Scholar] [CrossRef]
- Stangl, M.; Kanitscheider, I.; Riemer, M.; Fiete, I.; Wolbers, T. Sources of Path Integration Error in Young and Aging Humans. Nat. Commun. 2020, 11, 1–17. [Google Scholar] [CrossRef] [PubMed]
- Stangl, M.; Achtzehn, J.; Huber, K.; Dietrich, C.; Tempelmann, C.; Wolbers, T. Compromised Grid-Cell-Like Representations in Old Age as a Key Mechanism to Explain Age-Related Navigational Deficits. Curr. Biol. 2018, 28, 1108–1115 e6. [Google Scholar] [CrossRef]
- Wolbers, T.; Hegarty, M. What Determines Our Navigational Abilities? Trends Cogn. Sci. 2010, 14, 138–146. [Google Scholar] [CrossRef]
- Miniaci, M.C.; De Leonibus, E. Missing the Egocentric Spatial Reference: A Blank on the Map. F1000Res 2018, 7, 1–12. [Google Scholar] [CrossRef]
- Passini, R.; Rainville, C.; Marchand, N.; Joanette, Y. Wayfinding in Dementia of the Alzheimer Type: Planning Abilities. J. Clin. Exp. Neuropsychol. 1995, 17, 820–832. [Google Scholar] [CrossRef] [PubMed]
- Chiu, Y.C.; Algase, D.; Liang, J.; Liu, H.C.; Lin, K.N. Conceptualization and Measurement of Getting Lost Behavior in Persons with Early Dementia. Int. J. Geriatr Psychiatry 2005, 20, 760–768. [Google Scholar] [CrossRef] [PubMed]
- Caspi, E. Wayfinding Difficulties among Elders with Dementia in an Assisted Living Residence. Dementia 2014, 13, 429–450. [Google Scholar] [CrossRef] [PubMed]
- Foldi, N.S.; Schaefer, L.A.; White, R.E.; Johnson, R., Jr.; Berger, J.T.; Carney, M.T.; Macina, L.O. Effects of Graded Levels of Physical Similarity and Density on Visual Selective Attention in Patients with Alzheimer’s Disease. Neuropsychology 2005, 19, 5–17. [Google Scholar] [CrossRef]
- Davis, R.; Sikorskii, A. Eye Tracking Analysis of Visual Cues During Wayfinding in Early Stage Alzheimer’s Disease. Dement. Geriatr. Cogn. Disord. 2020, 49, 91–97. [Google Scholar] [CrossRef]
- Stern, Y. Cognitive Reserve and Alzheimer Disease. Alzheimer Dis. Assoc. Disord. 2006, 20, 69–74. Available online: https://journals.lww.com/alzheimerjournal/Abstract/2006/07001/Cognitive_Reserve_and_Alzheimer_Disease.10.aspx (accessed on 8 August 2020).
- Stern, Y. What Is Cognitive Reserve? Theory and Research Application of the Reserve Concept. J. Int. Neuropsychol. Soc. 2002, 8, 448–460. [Google Scholar] [CrossRef]
- Olsson, A.; Skovdahl, K.; Engstrom, M. Strategies Used by People with Alzheimer’s Disease for Outdoor Wayfinding: A Repeated Observational Study. Dementia 2019, 1–13. [Google Scholar] [CrossRef]
- Chiu, Y.C.; Algase, D.; Whall, A.; Liang, J.; Liu, H.C.; Lin, K.N.; Wang, P.N. Getting Lost: Directed Attention and Executive Functions in Early Alzheimer’s Disease Patients. Dement. Geriatr. Cogn. Disord. 2004, 17, 174–180. [Google Scholar] [CrossRef]
- Cummings, J.L. The Neuropsychiatric Inventory: Assessing Psychopathology in Dementia Patients. Neurology 1997, 48 (Suppl. 5–6), S10–S16. [Google Scholar] [CrossRef]
- Algase, D.L.; Son, G.R.; Beattie, E.; Song, J.A.; Leitsch, S.; Yao, L. The Interrelatedness of Wandering and Wayfinding in a Community Sample of Persons with Dementia. Dement. Geriatr. Cogn. Disord. 2004, 17, 231–239. [Google Scholar] [CrossRef]
- Cipriani, G.; Lucetti, C.; Nuti, A.; Danti, S. Wandering and Dementia. Psychogeriatrics 2014, 14, 135–142. [Google Scholar] [CrossRef] [PubMed]
- Forsund, L.H.; Grov, E.K.; Helvik, A.S.; Juvet, L.K.; Skovdahl, K.; Eriksen, S. The Experience of Lived Space in Persons with Dementia: A Systematic Meta-Synthesis. BMC Geriatr. 2018, 18, 1–27. [Google Scholar] [CrossRef] [PubMed]
- Marquardt, G. Kriterienkatalog Demenzfreundliche Architektur. Ph.D. Thesis, University of Dresden, Dresden, Germany, 19 December 2006. Available online: https://d-nb.info/985850043/34 (accessed on 8 August 2020).
- Dietz, B. Demenzsensible Architektur: Planen Und Gestalten Für Alle Sinne; Fraunhofer IRB Verlag: Stuttgart, Germany, 2018; ISBN 978-3738800326. [Google Scholar]
- Soilemezi, D.; Drahota, A.; Crossland, J.; Stores, R. The Role of the Home Environment in Dementia Care and Support: Systematic Review of Qualitative Research. Dementia 2019, 18, 1237–1272. [Google Scholar] [CrossRef] [PubMed]
- Twin Cities Habitat for Humanity. Age Well at Home—Transforming Homes into Safe, Smart Spaces for Aging Adults. 2020. Available online: https://www.tchabitat.org/blog/age-well-at-home-a-new-approach-to-home-modification-for-aging-adults (accessed on 16 November 2020).
- Smith, K.; Gee, S.; Sharrock, T.; Croucher, M. Developing a Dementia-Friendly Christchurch: Perspectives of People with Dementia. Australas J. Ageing 2016, 35, 188–192. [Google Scholar] [CrossRef]
- Imrie, R. Ableist Geographies, Disablist Spaces: Towards a Reconstruction of Golledge’s ’Geography and the Disabled’. Trans. Inst. Br. Geogr. 1996, 21, 397–403. [Google Scholar] [CrossRef]
- Oliver, M. The Social Model of Disability: Thirty Years On. Disabil. Soc. 2013, 28, 1024–1026. [Google Scholar] [CrossRef]
- United Nations. Convention on the Rights of Persons with Disabilities. 2008. Available online: https://www.un.org/development/desa/disabilities/convention-on-the-rights-of-persons-with-disabilities.html (accessed on 1 September 2020).
- Story, M.F. The Principles of Universal Design. In Universal Design Handbook; Preiser, W.F.E., Smith, K.H., Eds.; Mc Graw Hill: New York, NY, USA, 2001; ISBN 978-0-07-162922-5. [Google Scholar]
- Lawton, M.P.; Nahemow, L. Ecology and the Aging Process. In The Psychology of Adult Development and Aging; Eisdorfer, C., Lawton, M.P., Eds.; American Psychological Association: Washington, DC, USA, 1973; pp. 619–674. [Google Scholar]
- Lawton, M.P.; Simon, B. The Ecology of Social Relationships in Housing for the Elderly. Gerontologist 1968, 8, 108–115. [Google Scholar] [CrossRef] [PubMed]
- Kitwood, T. Dementia Reconsidered: The Person Comes First. Adult Lives: A Life Course Perspective; McGraw-Hill Education/Open University Press: Maidenhead, UK, 1997; Volume 89, ISBN 9780335198559. [Google Scholar]
- Antonovsky, A. The Salutogenic Model as a Theory to Guide Health Promotion. Health Promot. Int. 1996, 11, 11–18. [Google Scholar] [CrossRef]
- Golembiewski, J.A. Salutogenic Architecture in Healthcare Settings. In The Handbook of Salutogenesis; Mittelmark, M.B., Sagy, S., Eriksson, M., Bauer, G., Pelikan, J.M., Lindström, B., Espnes, G.A., Eds.; Springer: Berlin, Germany, 2017; pp. 267–276. [Google Scholar]
- Feddersen, E. 2.1 Orientierungslos? Architektur Und Raumgestaltung—Das Demenzsensible Krankenhaus: Grundlagen Und Praxis Einer Patientenorientierten Betreuung Und Versorgung; Horneber, M., Püllen, R., Hübner, J., Eds.; Kohlhammer: Stuttgart, Germany, 2019; pp. 41–58. [Google Scholar]
- Motzek, T.; Bueter, K.; Marquardt, G. Investigation of Eligible Picture Categories for Use as Environmental Cues in Dementia-Sensitive Environments. HERD 2017, 10, 64–73. [Google Scholar] [CrossRef]
- Day, K.; Carreon, D.; Stump, C. The Therapeutic Design of Environments for People with Dementia: A Review of the Empirical Research. Gerontologist 2000, 40, 397–416. [Google Scholar] [CrossRef]
- Howett, D.; Castegnaro, A.; Krzywicka, K.; Hagman, J.; Marchment, D.; Henson, R.; Chan, D. Differentiation of Mild Cognitive Impairment Using an Entorhinal Cortex-Based Test of Virtual Reality Navigation. Brain 2019, 142, 1751–1766. [Google Scholar] [CrossRef] [PubMed]
- Fleming, R.; Bennett, K.; Preece, T.; Phillipson, L. The Development and Testing of the Dementia Friendly Communities Environment Assessment Tool (DFC EAT). Int. Psychogeriatr. 2017, 29, 303–311. [Google Scholar] [CrossRef] [PubMed]
- Mitchell, L.; Burton, E. Neighbourhoods for Life: Designing Dementia-Friendly Outdoor Environments. Qual. Ageing Older Adults 2006, 7, 26–33. [Google Scholar] [CrossRef]
- Seetharaman, K.; Shepley, M.M.; Cheairs, C. The Saliency of Geographical Landmarks for Community Navigation: A Photovoice Study with Persons Living with Dementia. Dementia 2020, 1–22. [Google Scholar] [CrossRef]
- Alzheimer’s Society UK. Consent and Capacity of People with Dementia 2020. Available online: https://www.alzheimers.org.uk/dementia-professionals/dementia-experience-toolkit/how-recruit-people-dementia/consent-and-capacity (accessed on 16 November 2020).
- Wiersma, E.C. Using Photovoice with People with Early-Stage Alzheimer’s Disease: A Discussion of Methodology. Dementia 2011, 10, 203–216. [Google Scholar] [CrossRef]
- Parry, D.C.; Johnson, C.W. Contextualizing Leisure Research to Encompass Complexity in Lived Leisure Experience: The Need for Creative Analytic Practice. Leis. Sci. 2007, 29, 119–130. [Google Scholar] [CrossRef]
- Grimshaw, J.M.; Eccles, M.P.; Lavis, J.N.; Hill, S.J.; Squires, J.E. Knowledge Translation of Research Findings. Implement. Sci. 2012, 7, 1–17. [Google Scholar] [CrossRef]
- Philip, D. Essay: The Practical Failure of Architectural Psychology. J. Environ. Psychol. 1996, 16, 277–284. [Google Scholar] [CrossRef]
- Flade, A. Architektur: Psychologisch Betrachtet; Dieckmann, F., Röhrbein, R., Eds.; Huber Verlag: Mannheim, Germany, 2008; ISBN 3456846126. [Google Scholar]
- Dalton, R.C.; Mavros, P.; Kuliga, S.; Gath Morad, M.; Hölscher, C. Architectural Cognition Cards: A Card-Based Method for Introducing Spatial Cognition Research and User-Centred Thinking into the Design. Unpublished research article: In review in Architectural Science Review.
- Bundesministerium Für Gesundheit (Germany Ministry of Health). Rahmenempfehlungen Zum Umgang Mit Herausforderndem Verhalten Bei Menschen Mit Demenz in Der Stationären Altenhilfe. Forschungsbericht 007—Gesundheitsforschung; Bartholomeyczik, S., Halek, M., Riesner, C., Eds.; Germany Ministry of Health: Berlin, Germany, 2007. Available online: https://www.bundesgesundheitsministerium.de/fileadmin/Dateien/Publikationen/Pflege/Berichte/Bericht_Rahmenempfehlungen_zum_Umgang_mit_herausforderndem_Verhalten_bei_Menschen_mit_Demenz_in_der_stationaeren_Altenhilfe.pdf (accessed on 8 August 2020).
- Diegelmann, M.; Jansen, C.P.; Wahl, H.W.; Schilling, O.K.; Schnabel, E.L.; Hauer, K. Does a Physical Activity Program in the Nursing Home Impact on Depressive Symptoms? A Generalized Linear Mixed-Model Approach. Aging Ment. Health 2018, 22, 784–793. [Google Scholar] [CrossRef]
- Koscak Tivadar, B. Physical Activity Improves Cognition: Possible Explanations. Biogerontology 2017, 18, 477–483. [Google Scholar] [CrossRef]
- Van Hoof, J.; Kort, H.S.; Van Waarde, H.; Blom, M.M. Environmental Interventions and the Design of Homes for Older Adults with Dementia: An Overview. Am. J. Alzheimers Dis. Other Demen. 2010, 25, 202–232. [Google Scholar] [CrossRef]
- Nolan, B.A.; Mathews, R.M.; Harrison, M. Using External Memory Aids to Increase Room Finding by Older Adults with Dementia. Am. J. Alzheimers Dis Other Demen. 2001, 16, 251–254. [Google Scholar] [CrossRef] [PubMed]
- Nolan, B.A.D.; Mathews, R.M.; Truesdell-Todd, G.; Vandorp, A. Evaluation of the Effect of Orientation Cues on Wayfinding in Persons with Dementia. Alzheimer Care Today 2002, 3, 46–49. Available online: https://journals.lww.com/actjournalonline/Fulltext/2002/03010/Evaluation_of_the_Effect_of_Orientation_Cues_on.10.aspx (accessed on 16 November 2020).
- Wiener, J.M.; Pazzaglia, F. Ageing-and Dementia-Friendly Design: Theory and Evidence from Neuropsychology Can Contribute to Guidelines That Minimise Spatial Disorientation. Psarxiv 2020, 1–29. [Google Scholar] [CrossRef]
- Fleming, R.; Bennett, K. Assessing the Quality of Environmental Design of Nursing Homes for People with Dementia: Development of a New Tool. Australas J. Ageing 2015, 34, 191–194. [Google Scholar] [CrossRef] [PubMed]
- Gaber, S.N.; Nygard, L.; Brorsson, A.; Kottorp, A.; Malinowsky, C. Everyday Technologies and Public Space Participation among People with and without Dementia. Can. J. Occup. Ther. 2019, 86, 400–411. [Google Scholar] [CrossRef]
- Van Steenwinkel, I.; Van Audenhove, C.; Heylighen, A. Insights into Living with Dementia: Five Implications for Architectural Design. In Proceedings of the ARCH17: 3rd International Conference on Architecture, Research, Care and Health, Lyngby, Denmark, 26 April 2017; Available online: https://lirias.kuleuven.be/1951616?limo=0,https://www.researchgate.net/publication/314285517_Insights_into_living_with_dementia_Five_implications_for_architectural_design (accessed on 8 August 2020).
- O’Malley, M.; Innes, A.; Wiener, J.M. Decreasing Spatial Disorientation in Care-Home Settings: How Psychology Can Guide the Development of Dementia Friendly Design Guidelines. Dementia 2017, 16, 315–328. [Google Scholar] [CrossRef]
- Zeisel, J. Inquiry by Design: Environment/Behavior/Neuroscience in Architecture, Interiors, Landscape and Planning; WW Norton & Co., Wiley: New York, NY, USA, 2006. Available online: https://www.wiley.com/en-au/Inquiry+by+Design%3A+Environment+Behavior+Neuroscience+in+Architecture%2C+Interiors%2C+Landscape%2C+and+Planning-p-9780393731842 (accessed on 16 November 2020).
- Van Steenwinkel, I. Offering Architects Insights into Living with Dementia: Three Case Studies on Orientation in Space-Time-Identity. 2015. Available online: https://lirias.kuleuven.be/1900362?limo=0 (accessed on 1 November 2020).
- Brösamle, M. Sketches of Wayfinding Design: Empirical Studies of Architectural Design Processes. Ph.D. Thesis, Albert-Ludwigs-University Freiburg, Freiburg im Breisgau, Germany, 20 March 2014. Available online: https://freidok.uni-freiburg.de/data/9412 (accessed on 16 November 2020).
- Krukar, J.; Dalton, R.C.; Hölscher, C. Applying HCI Methods and Concepts to Architectural Design (or Why Architects Could Use HCI Even If They Don’t Know It). In Architecture and Interaction; Dalton, N.S., Schnädelbach, H., Wiberg, M., Varoudis, T., Eds.; Springer: Cham, Switzerland, 2016; pp. 17–35. [Google Scholar]
- Kuliga, S. Evaluating User Experience and Wayfinding Behaviour in Complex, Architectural Environments–Towards a User-Centred Approach of Building Usability. Ph.D. Thesis, Albert-Ludwigs University Freiburg, Freiburg im Breisgau, Germany, 7 November 2016. Available online: https://freidok.uni-freiburg.de/data/11386 (accessed on 16 November 2020).
- Bethell, J.; Commisso, E.; Rostad, H.M.; Puts, M.; Babineau, J.; Grinbergs-Saull, A.; Mcgilton, K.S. Patient Engagement in Research Related to Dementia: A Scoping Review. Dementia 2018, 17, 944–975. [Google Scholar] [CrossRef]
- De Boer, M.E.; Hertogh, C.M.; Droes, R.M.; Riphagen, I.; Jonker, C.; Eefsting, J.A. Suffering from Dementia—the Patient’s Perspective: A Review of the Literature. Int. Psychogeriatr. 2007, 19, 1021–1039. [Google Scholar] [CrossRef]
- Gorska, S.; Forsyth, K.; Maciver, D. Living with Dementia: A Meta-Synthesis of Qualitative Research on the Lived Experience. Gerontologist 2018, 58, e180–e196. [Google Scholar] [CrossRef]
- Kindell, J.; Keady, J.; Sage, K.; Wilkinson, R. Everyday Conversation in Dementia: A Review of the Literature to Inform Research and Practice. Int J. Lang. Commun. Disord. 2017, 52, 392–406. [Google Scholar] [CrossRef]
- Novek, S.; Wilkinson, H. Safe and Inclusive Research Practices for Qualitative Research Involving People with Dementia: A Review of Key Issues and Strategies. Dementia. 2019, 18, 1042–1059. [Google Scholar] [CrossRef] [PubMed]
- Prorok, J.C.; Horgan, S.; Seitz, D.P. Health Care Experiences of People with Dementia and Their Caregivers: A Meta-Ethnographic Analysis of Qualitative Studies. CMAJ 2013, 185, E669–E680. [Google Scholar] [CrossRef] [PubMed]
- Von Kutzleben, M.; Schmid, W.; Halek, M.; Holle, B.; Bartholomeyczik, S. Community-Dwelling Persons with Dementia: What Do They Need? What Do They Demand? What Do They Do? A Systematic Review on the Subjective Experiences of Persons with Dementia. Aging Ment. Health 2012, 16, 378–390. [Google Scholar] [CrossRef] [PubMed]
- Schneider-Landolf, M.; Spielmann, J.; Zitterbarth, W.; Smith, S.J.A. Handbook of Theme-Centered Interaction (Tci); Vandenhoeck et Ruprecht: Göttingen, Germany, 2017; ISBN 3525451903. [Google Scholar]
- De Boer, B.; Bozdemir, B.; Jansen, J.; Hermans, M.; Hamers, J.P.H.; Verbeek, H. The Homestead: Developing a Conceptual Framework through Co-Creation for Innovating Long-Term Dementia Care Environments. Int. J. Environ. Res. Public Health 2020, 18, 57. [Google Scholar] [CrossRef] [PubMed]
- Evans, D.; Robertson, J.; Candy, A. Use of Photovoice with People with Younger Onset Dementia. Dementia 2016, 15, 798–813. [Google Scholar] [CrossRef]
- Aflatoony, L.; Tonetto, L.M.; Campiglia, G.C.; Dubose, J.R. Photo Narrative: Co-Designing a Built Environment with Seniors with Mild Cognitive Impairments. In DRS2020: Synergy; Boess, S., Cheung, M., Cain, R., Eds.; Design Research Society: London, UK, Conference held online due to Covid19; 2020; pp. 1392–1407. [Google Scholar] [CrossRef]
- Diersch, N.; Wolbers, T. The Potential of Virtual Reality for Spatial Navigation Research across the Adult Lifespan. J. Exp. Biol. 2019, 222 (Suppl. 1), jeb187252. [Google Scholar] [CrossRef]
- Kuliga, S.; Charlton, J.; Rohaidi, H.F.; Isaac, L.Q.Q.; Hoelscher, C.; Joos, M. Developing a Replication of a Wayfinding Study. From a Large-Scale Real Building to a Virtual Reality Simulation. In Proceedings of the German Conference on Spatial Cognition; Šķilters, J., Newcombe, N.S., Uttal, D., Eds.; Online Proceedings: Conference postphoned to 2021 due to Covid19; Springer: Berlin, Germany, 2020; pp. 126–142. Available online: https://link.springer.com/chapter/10.1007/978-3-030-57983-8_11 (accessed on 8 August 2020).
- Kuliga, S.; Mavros, P.; Brösamle, M.; Hölscher, C. Comparing Human Wayfinding Behavior between a Real, Existing Building, a Virtual Replica, and Two Architectural Redesigns. In Proceedings of the German Conference on Spatial Cognition; Šķilters, J., Newcombe, N.S., Uttal, D., Eds.; Online Proceedings: Conference postphoned to 2021 due to Covid19; Springer: Berlin, Germany, 2020; pp. 160–179. Available online: https://www.springerprofessional.de/comparing-human-wayfinding-behavior-between-a-real-existing-buil/18310012 (accessed on 8 August 2020).
- Kuliga, S.F.; Thrash, T.; Dalton, R.C.; Hölscher, C. Virtual Reality as an Empirical Research Tool—Exploring User Experience in a Real Building and a Corresponding Virtual Model. Comput. Environ. Urban Syst. 2015, 54, 363–375. [Google Scholar] [CrossRef]
- Strong, J. Immersive Virtual Reality and Persons with Dementia: A Literature Review. J. Gerontol. Soc. Work 2020, 63, 209–226. [Google Scholar] [CrossRef]
- Taube, J.S.; Valerio, S.; Yoder, R.M. Is Navigation in Virtual Reality with Fmri Really Navigation? J. Cogn. Neurosci. 2013, 25, 1008–1019. [Google Scholar] [CrossRef]
- Wiener, J.M.; Carroll, D.; Moeller, S.; Bibi, I.; Ivanova, D.; Allen, P.; Wolbers, T. A Novel Virtual-Reality-Based Route-Learning Test Suite: Assessing the Effects of Cognitive Aging on Navigation. Behav Res. Methods 2020, 52, 630–640. [Google Scholar] [CrossRef]
- Schaat, S.; Koldrack, P.; Yordanova, K.; Kirste, T.; Teipel, S. Real-Time Detection of Spatial Disorientation in Persons with Mild Cognitive Impairment and Dementia. Gerontology 2020, 66, 85–94. [Google Scholar] [CrossRef] [PubMed]
- Teipel, S.; Konig, A.; Hoey, J.; Kaye, J.; Kruger, F.; Robillard, J.M.; Babiloni, C. Use of Nonintrusive Sensor-Based Information and Communication Technology for Real-World Evidence for Clinical Trials in Dementia. Alzheimers Dement. 2018, 14, 1216–1231. [Google Scholar] [CrossRef]
- Teipel, S.; Babiloni, C.; Hoey, J.; Kaye, J.; Kirste, T.; Burmeister, O.K. Information and Communication Technology Solutions for Outdoor Navigation in Dementia. Alzheimers Dement. 2016, 12, 695–707. [Google Scholar] [CrossRef]
- Schneider, S.; Kuliga, S.; Weiser, R.; Kammler, O.; Fuchkina, E. Vreval-a Bim-Based Framework for User-Centered Evaluation of Complex Buildings in Virtual Environments. In VR, AR & VISUALISATION|Explorations—Volume 2—eCAADe 36; Kępczyńska-Walczak, A., Białkowski, S., Eds.; Faculty of Civil Engineering, Architecture and Environmental Engineering, Lodz University of Technology: Lodz, Poland, 2018; pp. 833–842. Available online: http://ecaade.org/downloads/eCAADe-2018-Volume2.pdf (accessed on 8 August 2020).
- Wahl, H.W.; Iwarsson, S.; Oswald, F. Aging Well and the Environment: Toward an Integrative Model and Research Agenda for the Future. Gerontologist 2012, 52, 306–316. [Google Scholar] [CrossRef]
- Emiliani, P.L. Assistive Technology (at) Versus Mainstream Technology (Mst): The Research Perspective. Technol. Disabil. 2006, 18, 19–29. [Google Scholar] [CrossRef]
- Ludden, G.D.S.; Van Rompay, T.J.L.; Niedderer, K.; Tournier, I. Environmental Design for Dementia Care—Towards More Meaningful Experiences through Design. Maturitas 2019, 128, 10–16. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kuliga, S.; Berwig, M.; Roes, M. Wayfinding in People with Alzheimer’s Disease: Perspective Taking and Architectural Cognition—A Vision Paper on Future Dementia Care Research Opportunities. Sustainability 2021, 13, 1084. https://doi.org/10.3390/su13031084
Kuliga S, Berwig M, Roes M. Wayfinding in People with Alzheimer’s Disease: Perspective Taking and Architectural Cognition—A Vision Paper on Future Dementia Care Research Opportunities. Sustainability. 2021; 13(3):1084. https://doi.org/10.3390/su13031084
Chicago/Turabian StyleKuliga, Saskia, Martin Berwig, and Martina Roes. 2021. "Wayfinding in People with Alzheimer’s Disease: Perspective Taking and Architectural Cognition—A Vision Paper on Future Dementia Care Research Opportunities" Sustainability 13, no. 3: 1084. https://doi.org/10.3390/su13031084
APA StyleKuliga, S., Berwig, M., & Roes, M. (2021). Wayfinding in People with Alzheimer’s Disease: Perspective Taking and Architectural Cognition—A Vision Paper on Future Dementia Care Research Opportunities. Sustainability, 13(3), 1084. https://doi.org/10.3390/su13031084




