Social Obstetrics as Niche-Development in Addressing Health Inequities
Abstract
1. Introduction
1.1. Health Inequities as a Persistent Problem
1.2. A Transitions Perspective on (Perinatal) Health Inequities
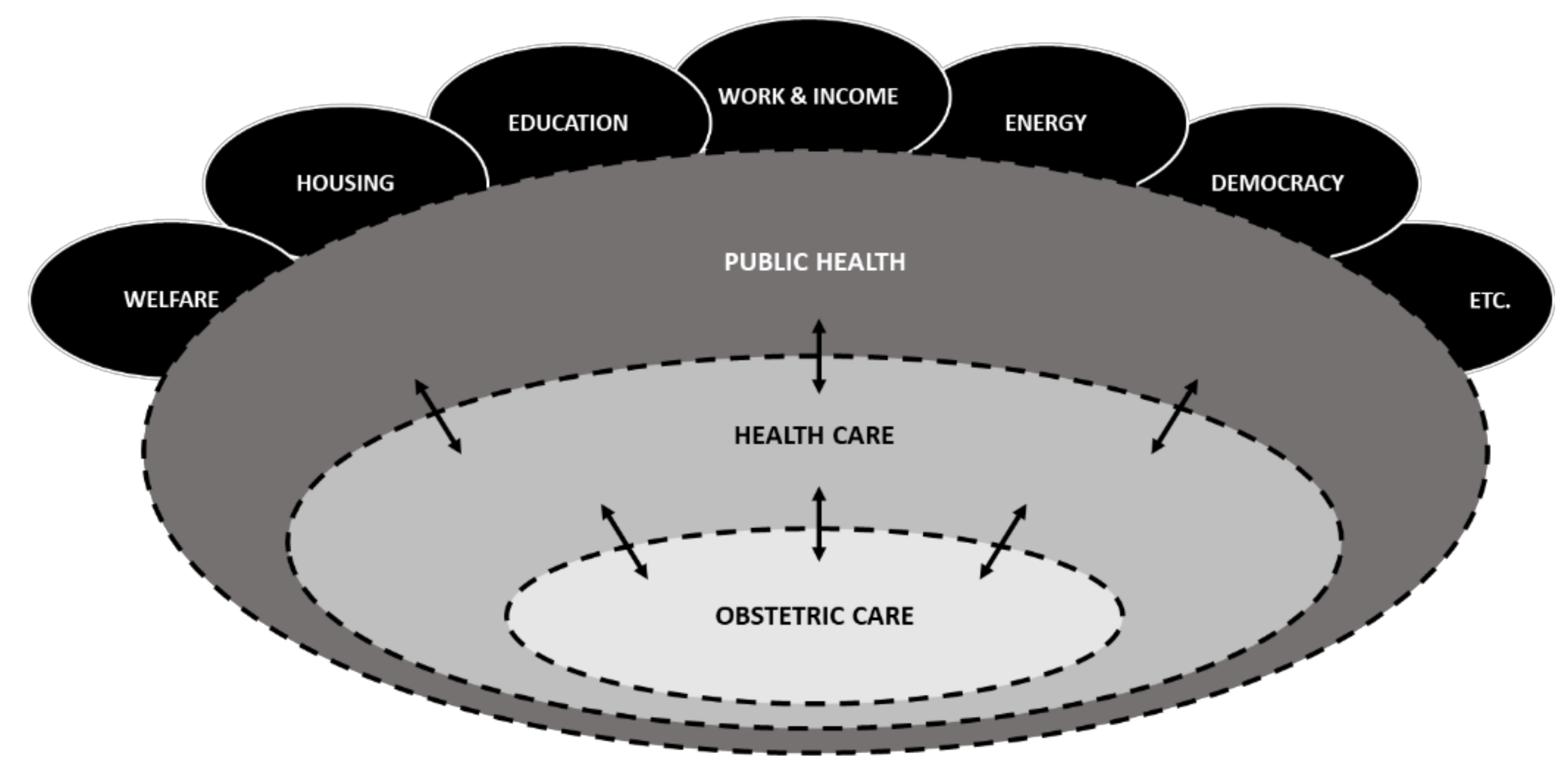
1.3. A Nested Systems Demarcation of Obstetric Care
2. Materials and Methods
3. Results
3.1. Historical Narrative of the Obstetric Care System
3.2. Current Obstacles and Future Shifts of the Obstetric Care System
- 1.
- Equal opportunities for all (newborn) children
“Previously, there was no attention for health inequities at birth. Therefore, we said that we need to look at socioeconomic patterns in perinatal health outcomes. And that we should call them like that: socioeconomic health inequities. And that perinatal mortality is caused by socioeconomic inequities in health”. Professional working at a municipal health service organization
- 2.
- Empowerment of (pregnant) women and (future) parents
“Parents always accept advice from grandparents, neighbors, best friends, uncles, aunts, etc. better than from professionals. I therefore want to strengthen their network and pick someone from it, who can guide the (future) mother. […] But often we do not even know their network.”
- 3.
- Open and easy access to obstetric care for all
“We have to enable future parents in finding financial support and requesting financial compensations. I think that this is quite a challenge [for them]. […] There should be a better overview.”
- 4.
- (Future) parents central in obstetric care
“I talk to them [future mothers] and ask them about their ideas concerning their pregnancy and whether they need anything. Often, they think that there is nothing they need. I ask them whether they were abused when they were young, for instance, and whether they ever received help for that. And whether they feel safe now.”
- 5.
- Cross-sectoral collaboration
“They [i.e., midwives] often do not know where to refer vulnerable pregnant women to. They know about multidisciplinary neighborhood teams, but do not know how to get in touch with us. […] That is why we thought we have to find a way to collaborate more.”
- 6.
- Structural policies aimed at prevention, impact, and continuity
“Previously we had a network which met every eight weeks. Everybody could talk about what they have been doing. But that network collapsed some years ago, as the municipality stopped financially supporting it. Something else was initiated. They keep initiating new stuff and then shut it down.”
4. Discussion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Mackenbach, J.P. The persistence of health inequalities in modern welfare states: The explanation of a paradox. Soc. Sci. Med. 2012, 75, 761–769. [Google Scholar] [CrossRef]
- Gezondheidsverschillen. Available online: https://www.vtv2018.nl/gezondheidsverschillen (accessed on 27 September 2021).
- Arcaya, M.C.; Arcaya, A.L.; Subramanian, S.V. Inequalities in health: Definitions, concepts, and theories. Glob. Health Action 2015, 8, 27106. [Google Scholar] [CrossRef] [PubMed]
- Baker, P.; Friel, S.; Kay, A.; Baum, F.; Strazdins, L.; MacKean, T. What Enables and Constrains the Inclusion of the Social Determinants of Health Inequities in Government Policy Agendas? A Narrative Review. Int. J. Health Policy Manag. 2017, 7, 101–111. [Google Scholar] [CrossRef] [PubMed]
- Beckfield, J.; Olafsdottir, S.; Bakhtiari, E. Health Inequalities in Global Context. Am. Behav. Sci. 2013, 57, 1014–1039. [Google Scholar] [CrossRef]
- Link, B.G.; Phelan, J. Social conditions as fundamental causes of disease. J. Health Soc. Behav. 1995, 80–94. [Google Scholar] [CrossRef]
- Woodward, A.; Kawachi, I. Why reduce health inequalities? J. Epidemiol. Community Health 2000, 54, 923–929. [Google Scholar] [CrossRef] [PubMed]
- Bambra, C.; Riordan, R.; Ford, J.; Matthews, F. The COVID-19 pandemic and health inequalities. J. Epidemiol. Community Health 2020, 74, 964–968. [Google Scholar] [CrossRef] [PubMed]
- Poeran, J.; Denktas, S.; Birnie, E.; Bonsel, G.J.; Steegers, E.A.P. Urban perinatal health inequalities. J. Matern. Fetal Neonatal Med. 2011, 24, 643–646. [Google Scholar] [CrossRef]
- Vos, A.A.; Denktaş, S.; Borsboom, G.J.J.M.; Bonsel, G.J.; Steegers, E.A.P. Differences in perinatal morbidity and mortality on the neighbourhood level in Dutch municipalities: A population based cohort study. BMC Pregnancy Childbirth 2015, 15, 201. [Google Scholar] [CrossRef]
- Euro-Peristat Project. European Perinatal Health Report. Core indicators of the health and care of pregnant women and babies in Europe in 2015. 2018. Available online: https://www.europeristat.com/images/EPHR2015_Euro-Peristat.pdf (accessed on 30 October 2021).
- Barker, D.J.P. The origins of the developmental origins theory. J. Intern. Med. 2007, 261, 412–417. [Google Scholar] [CrossRef]
- Barker, D.J.P. Adult Consequences of Fetal Growth Restriction. Clin. Obstet. Gynecol. 2006, 49, 270–283. [Google Scholar] [CrossRef]
- De Graaf, J.P.; Steegers, E.A.P.; Bonsel, G.J. Inequalities in perinatal and maternal health. Curr. Opin. Obstet. Gynecol. 2013, 25, 98–108. [Google Scholar] [CrossRef]
- Vos, A.A.; Posthumus, A.G.; Bonsel, G.J.; Steegers, E.A.; Denktaş, S. Deprived neighborhoods and adverse perinatal outcome: A systematic review and meta-analysis. Acta Obstet. Gynecol. Scand. 2014, 93, 727–740. [Google Scholar] [CrossRef]
- Flenady, V.; Koopmans, L.; Middleton, P.; Froen, J.F.F.; Smith, G.; Gibbons, K.; Coory, M.; Gordon, A.; Ellwood, D.; McIntyre, H.; et al. Major risk factors for stillbirth in high-income countries: A systematic review and meta-analysis. Lancet 2011, 377, 1331–1340. [Google Scholar] [CrossRef]
- Bertens, L.C.M.; Ochoa, L.B.; Van Ourti, T.; Steegers, E.A.P.; Been, J.V. Persisting inequalities in birth outcomes related to neighbourhood deprivation. J. Epidemiol. Community Health 2019, 74, 232–239. [Google Scholar] [CrossRef]
- Broerse, W.J.E.; Bunders-Aelen, J.G.F. Transitions in Health Systems: Dealing with Persistent Problems; VU University Press: Amsterdam, The Netherlands, 2010. [Google Scholar]
- Broerse, J.; Grin, J. Toward Sustainable Transitions in Healthcare Systems; Taylor & Francis: Oxfordshire, UK, 2017. [Google Scholar]
- Grin, J.; Rotmans, J.; Schot, J. Transitions to Sustainable Development: New Directions in the Study of Long Term Transformative Change; Routledge: New York, NY, USA, 2010. [Google Scholar]
- Loorbach, D.; Frantzeskaki, N.; Avelino, F. Sustainability Transitions Research: Transforming Science and Practice for Societal Change. Annu. Rev. Environ. Resour. 2017, 42, 599–626. [Google Scholar] [CrossRef]
- Lagendijk, J. Social Obstetrics: Addressing Inequalities in Perinatal Healthcare. 2020. Available online: https://repub.eur.nl/pub/130909/ (accessed on 30 October 2021).
- Marmot, M.; Allen, J.; Bell, R.; Bloomer, E.; Goldblatt, P. WHO European review of social determinants of health and the health divide. Lancet 2012, 380, 1011–1029. [Google Scholar] [CrossRef]
- Denktaş, S.; Bonsel, G.J.; Van Der Weg, E.J.; Voorham, A.J.J.; Torij, H.W.; De Graaf, J.P.; Wildschut, H.I.J.; Peters, I.; Birnie, E.; Steegers, E.A.P. An Urban Perinatal Health Programme of Strategies to Improve Perinatal Health. Matern. Child Health J. 2011, 16, 1553–1558. [Google Scholar] [CrossRef]
- de Jonge, H.C.C.; Lagendijk, J.; Saha, U.; Been, J.V.; Burdorf, A. Did an urban perinatal health programme in Rotterdam, The Netherlands, reduce adverse perinatal outcomes? Register-based retrospective cohort study. BMJ Open 2019, 9, e031357. [Google Scholar] [CrossRef]
- Denktaş, S.; Poeran, J.; Van Voorst, S.F.; A Vos, A.; De Jong-Potjer, L.C.; Waelput, A.J.M.; Birnie, E.; Bonsel, G.J.; Steegers, E.A.P. Design and outline of the Healthy Pregnancy 4 All study. BMC Pregnancy Childbirth 2014, 14, 253. [Google Scholar] [CrossRef]
- Waelput, A.J.M.; Sijpkens, M.K.; Lagendijk, J.; Van Minde, M.R.; Raat, H.; Ernst-Smelt, H.E.; De Kroon, M.L.A.; Rosman, A.N.; Been, J.V.; Bertens, L.C.M.; et al. Geographical differences in perinatal health and child welfare in the Netherlands: Rationale for the healthy pregnancy 4 all-2 program. BMC Pregnancy Childbirth 2017, 17, 254. [Google Scholar] [CrossRef] [PubMed]
- Brand, A.; Walker, D.K.; Hargreaves, M.; Rosenbach, M. Intermediate Outcomes, Strategies, and Challenges of Eight Healthy Start Projects. Matern. Child Health J. 2008, 14, 654–665. [Google Scholar] [CrossRef] [PubMed]
- NIRAS. Available online: https://www.sst.dk/-/media/Puljer/Midler-fra-sundhedspolitisk-udspil-til-s%C3%A5rbare-gravide/Tvaergaaende-evaluering.ashx?la=da&hash=BA12F099FFBD5CE4F5DC4DA28E6AD9D7E2CE436B (accessed on 14 October 2021).
- Renner, I.; Saint, V.; Neumann, A.; Ukhova, D.; Horstmann, S.; Boettinger, U.; Dreibus, M.; Kerl-Wienecke, A.; Wulff, P.; Mechthild, P.; et al. Improving psychosocial services for vulnerable families with young children: Strengthening links between health and social services in Germany. BMJ 2018, 363, k4786. [Google Scholar] [CrossRef] [PubMed]
- Super, S.; A Klerkx, L.W.; Hermens, N.; A Koelen, M. A multilevel transition perspective on embedding intersectoral action in local health policies. Health Promot. Int. 2020, 36, 1050–1061. [Google Scholar] [CrossRef]
- Hopwood, B.; Mellor, M.; O’Brien, G. Sustainable development: Mapping different approaches. Sustain. Dev. 2005, 13, 38–52. [Google Scholar] [CrossRef]
- Amelink-Verburg, P.M.; Buitendijk, S.E. Pregnancy and labour in the Dutch maternity care system: What is normal? The role division between midwives and obstetricians. J. Midwifery Women’s Health 2010, 55, 216–225. [Google Scholar] [CrossRef]
- Bais, J.J.M.; Pel, M. The basis of the Dutch obstetric system: Risk selection. Eur. Clin. Obstet. Gynaecol. 2006, 2, 209–212. [Google Scholar] [CrossRef]
- Acheson, D. Public health in England: The report of the Committee of Inquiry into the Future Development of the Public Health Function. Lond. Stn. Office 1998, 23–34. [Google Scholar]
- van Raak, R. Transition Policies; Connecting System Dynamics, Governance and Instruments in an Application to Dutch Healthcare; 2016. Available online: https://www.semanticscholar.org/paper/Transition-Policies%3B-connecting-system-dynamics%2C-in-Raak/7aa8b0c7a510df4849776d6ec8fa8898ad6b1aaa. (accessed on 10 October 2021).
- Hystad, P.; Davies, H.W.; Frank, L.; Van Loon, J.; Gehring, U.; Tamburic, L.; Brauer, M. Residential Greenness and Birth Outcomes: Evaluating the Influence of Spatially Correlated Built-Environment Factors. Environ. Health Perspect. 2014, 122, 1095–1102. [Google Scholar] [CrossRef]
- Nowak, L.A.; Giurgescu, C. The built environment and birth outcomes: A systematic review. MCN: Am. J. Matern. Child Nurs. 2017, 42, 14–20. [Google Scholar] [CrossRef]
- Miranda, L.M.; Messer, L.C.; Kroeger, G.L. Associations between the quality of the residential built environment and pregnancy outcomes among women in North Carolina. Environ. Health Perspect. 2012, 120, 471–477. [Google Scholar] [CrossRef]
- Barsties, L.S.; Daalderop, L.A.; Lagendijk, J.; van Steenbergen, F.; Been, J.V.; Bertens, L.C.; Waelput, A.J.; van Zoest, H.; Loorbach, D.; Steegers, E.A. Addressing perinatal health inequities in Dutch municipalities: Protocol for the Healthy Pregnancy 4 All-3 programme. Health Policy 2020, 125, 385–392. [Google Scholar] [CrossRef]
- Brown, R.R.; Rogers, B.C.; Werbeloff, L. Moving toward Water Sensitive Cities; Centre for Water Sensitive Cities: Melbourne, VIC, Australia, 2016; Available online: https://watersensitivecities.org.au/wp-content/uploads/2016/05/TMR_A4-1_MovingTowardWSC.pdf (accessed on 30 October 2021).
- Brown, R.R.; Rogers, B.C.; Werbeloff, L. A framework to guide transitions to water sensitive cities. In Urban Sustainability Transitions; Springer: Singapore, 2018; pp. 129–148. [Google Scholar]
- Avelino, F.; Grin, J.; Pel, B.; Jhagroe, S. The politics of sustainability transitions. J. Environ. Policy Plan. 2016, 18, 557–567. [Google Scholar] [CrossRef]
- Al-Gailani, S.; Davis, A. Introduction to “Transforming pregnancy since 1900”. Stud. Hist. Philos. Biol. Biomed. Sci. 2014, 47, 229. [Google Scholar] [CrossRef]
- Drife, J. The start of life: A history of obstetrics. Postgrad. Med. J. 2002, 78, 311–315. [Google Scholar] [CrossRef]
- Moore, T.G.; McDonald, M.; Carlon, L.; O’Rourke, K. Early childhood development and the social determinants of health inequities. Health Promot. Int. 2015, 30, ii102–ii115. [Google Scholar] [CrossRef]
- Hanson, C. A Cultural History of Pregnancy: Pregnancy, Medicine and Culture, 1750–2000; Palgrave Macmillan: London, UK, 2004. [Google Scholar]
- De Graaf, J.P.; Merkus, H.M.W.M.; Bonsel, G.J.; Steegers, E.A.P. Nederlandse Geboortezorg in Een Historisch Perspectief; Wonderbaby en Zorgenkind; Rotterdam Erasmus MC: Rotterdam, The Netherlands, 2017. [Google Scholar]
- Vos, A.A.; Leeman, A.; Waelput, A.J.; Bonsel, G.J.; Steegers, E.A.; Denktaş, S. Assessment and care for non-medical risk factors in current antenatal health care. Midwifery 2015, 31, 979–985. [Google Scholar] [CrossRef]
- Steegers, E. Embryonale gezondheid en preconceptiezorg. Ned. Tijdschr. Geneeskd. 2014, 158, A7373. [Google Scholar]
- Kuruvilla, S.; Sadana, R.; Montesinos, E.V.; Beard, J.; Vasdeki, J.F.; De Carvalho, I.A.; Thomas, R.B.; Drisse, M.-N.B.; Daelmans, B.; Goodman, T.; et al. A life-course approach to health: Synergy with sustainable development goals. Bull. World Health Organ. 2017, 96, 42–50. [Google Scholar] [CrossRef]
- van Lieburg, J.M.; Marland, H. Midwife regulation, education, and practice in the Netherlands during the nineteenth century. Med. Hist. 1989, 33, 296–317. [Google Scholar] [CrossRef][Green Version]
- van der Hoeve, J.; Gorter, E.; Benjamins, C.E.; van Loghem, J.J.; de Snoo, K.; Tuntler, J.H.; van den Berg, H.M.R. Nederlands Instituut voor Praeventieve Gezondheidszorg TNO. In Praeventieve Geneeskunde; TU Delft Library: Delft, The Netherlands, 1936. [Google Scholar]
- Wildman, K.; Blondel, B.; Nijhuis, J.; Defoort, P.; Bakoula, C. European indicators of health care during pregnancy, delivery and the postpartum period. Eur. J. Obstet. Gynecol. Reprod. Biol. 2003, 111, S53–S65. [Google Scholar] [CrossRef]
- Schuitmaker, T.J. Identifying and unravelling persistent problems. Technol. Forecast. Soc. Chang. 2012, 79, 1021–1031. [Google Scholar] [CrossRef]
- Johansen, F.; Bosch, S.V.D. The scaling-up of Neighbourhood Care: From experiment towards a transformative movement in healthcare. Futures 2017, 89, 60–73. [Google Scholar] [CrossRef]
- Swilling, M.; Annecke, E. Just Transitions: Explorations of Sustainability in an Unfair World; Juta and Company (Pty) Ltd.: Cape Town, South Africa, 2012. [Google Scholar]
- Williams, S.; Doyon, A. Justice in energy transitions. Environ. Innov. Soc. Trans. 2019, 31, 144–153. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Barsties, L.S.; Steenbergen, F.S.v.; Loorbach, D. Social Obstetrics as Niche-Development in Addressing Health Inequities. Sustainability 2021, 13, 12814. https://doi.org/10.3390/su132212814
Barsties LS, Steenbergen FSv, Loorbach D. Social Obstetrics as Niche-Development in Addressing Health Inequities. Sustainability. 2021; 13(22):12814. https://doi.org/10.3390/su132212814
Chicago/Turabian StyleBarsties, Lisa S., Frank S. van Steenbergen, and Derk Loorbach. 2021. "Social Obstetrics as Niche-Development in Addressing Health Inequities" Sustainability 13, no. 22: 12814. https://doi.org/10.3390/su132212814
APA StyleBarsties, L. S., Steenbergen, F. S. v., & Loorbach, D. (2021). Social Obstetrics as Niche-Development in Addressing Health Inequities. Sustainability, 13(22), 12814. https://doi.org/10.3390/su132212814