Evaluation of Monolayer and Bilayer Buccal Films Containing Metoclopramide
Abstract
1. Introduction
2. Methods
2.1. Preparation of Films
2.1.1. Monolayer Formulations
2.1.2. Bilayer Formulations
2.2. Release Rate
2.2.1. USPI
2.2.2. Innovative Cell for Film Release
2.3. Raman Mapping of Film Surface
2.4. Image Analytics of Formulations
2.5. Preparation of Drug in Amorphous State
2.6. Film Thickness
2.7. Stability
2.8. Viscosity of Casting Solution
2.9. Metoclopramide Assay
2.9.1. HPLC
2.9.2. UV-VIS
3. Results and Discussion
3.1. Visual Observation of the Obtained Films
3.1.1. Monolayer Films
3.1.2. Bilayer Films
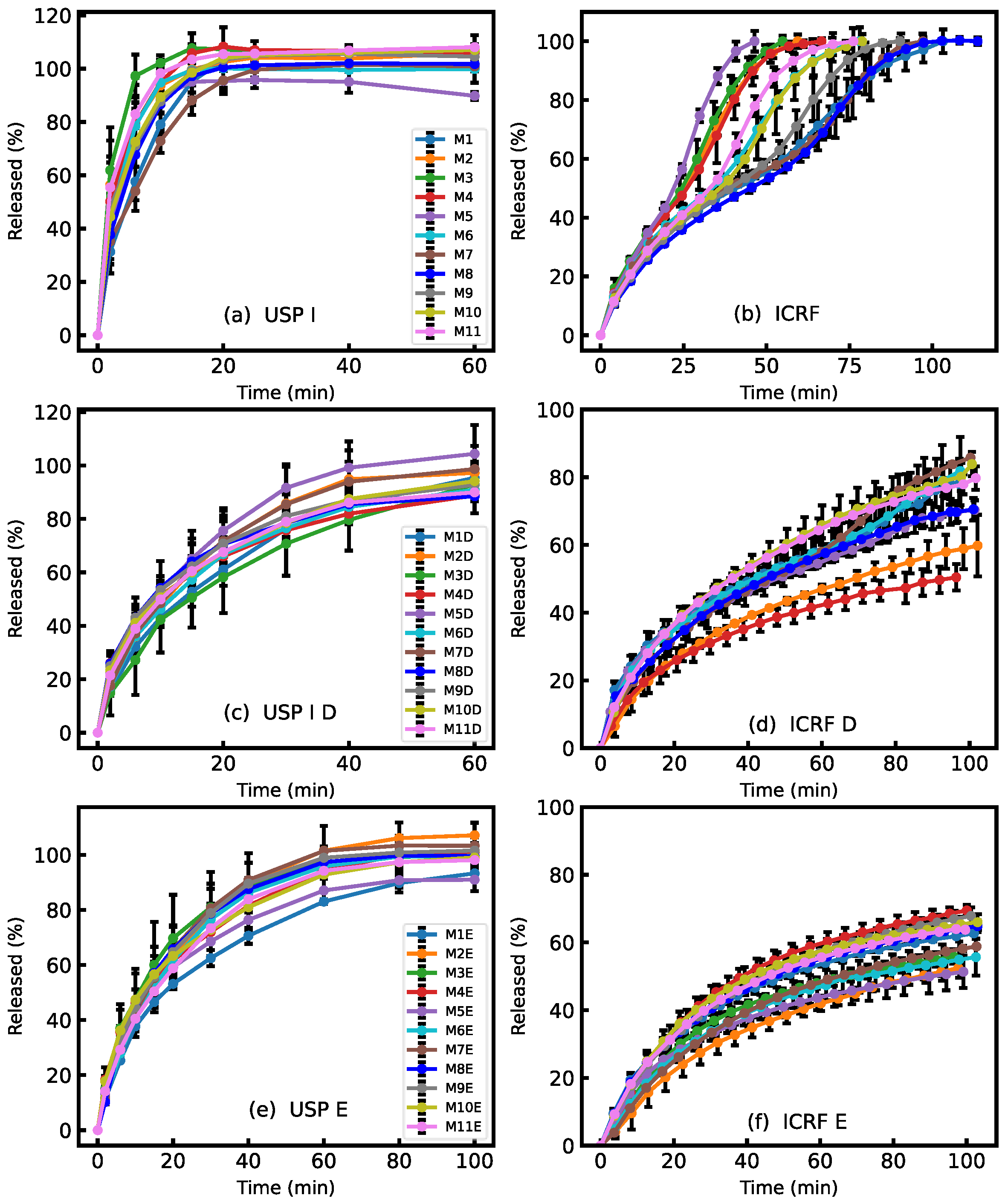
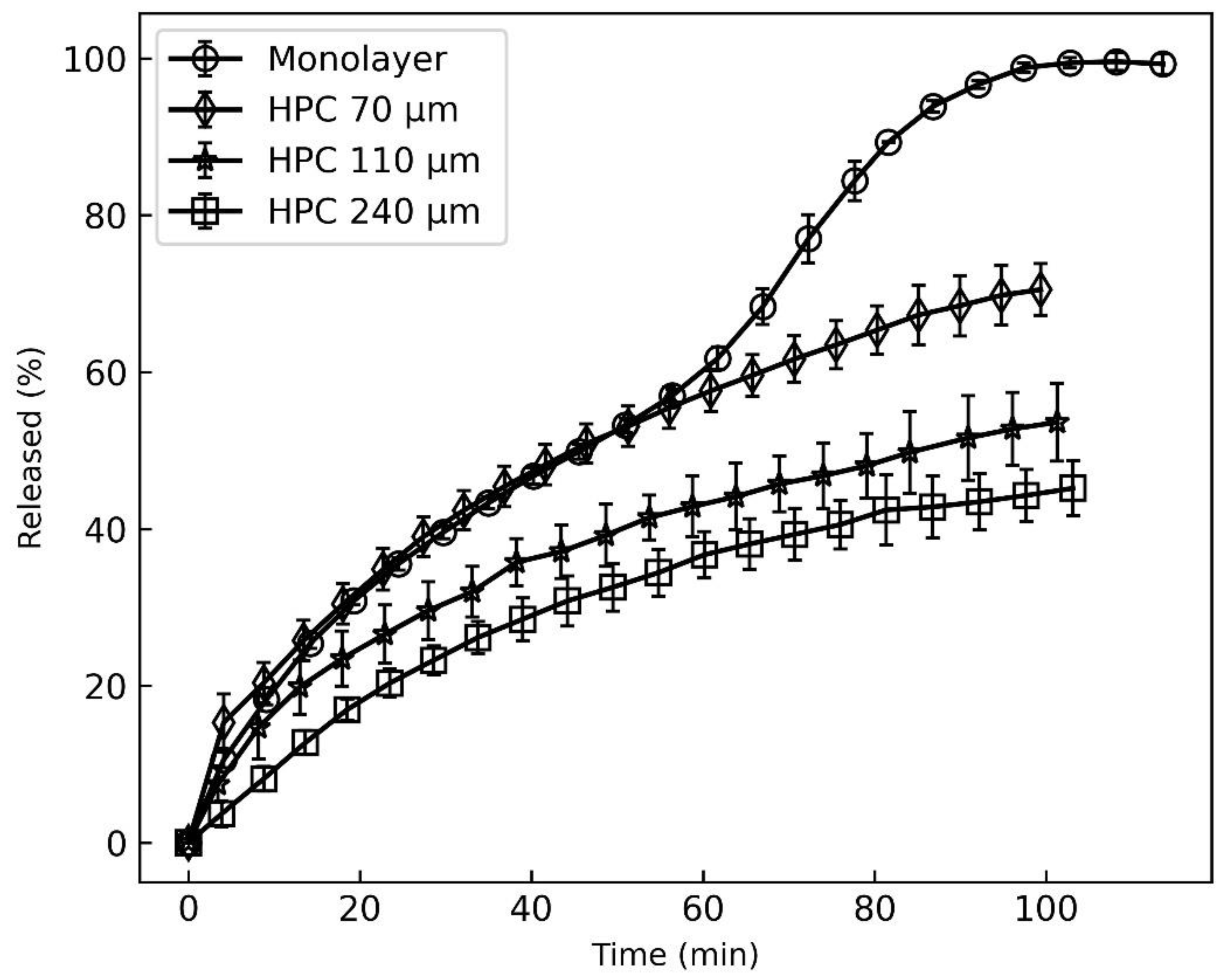
3.2. MCP Release Comparison of Mono- and Bilayer Films by Two Dissolution Methods
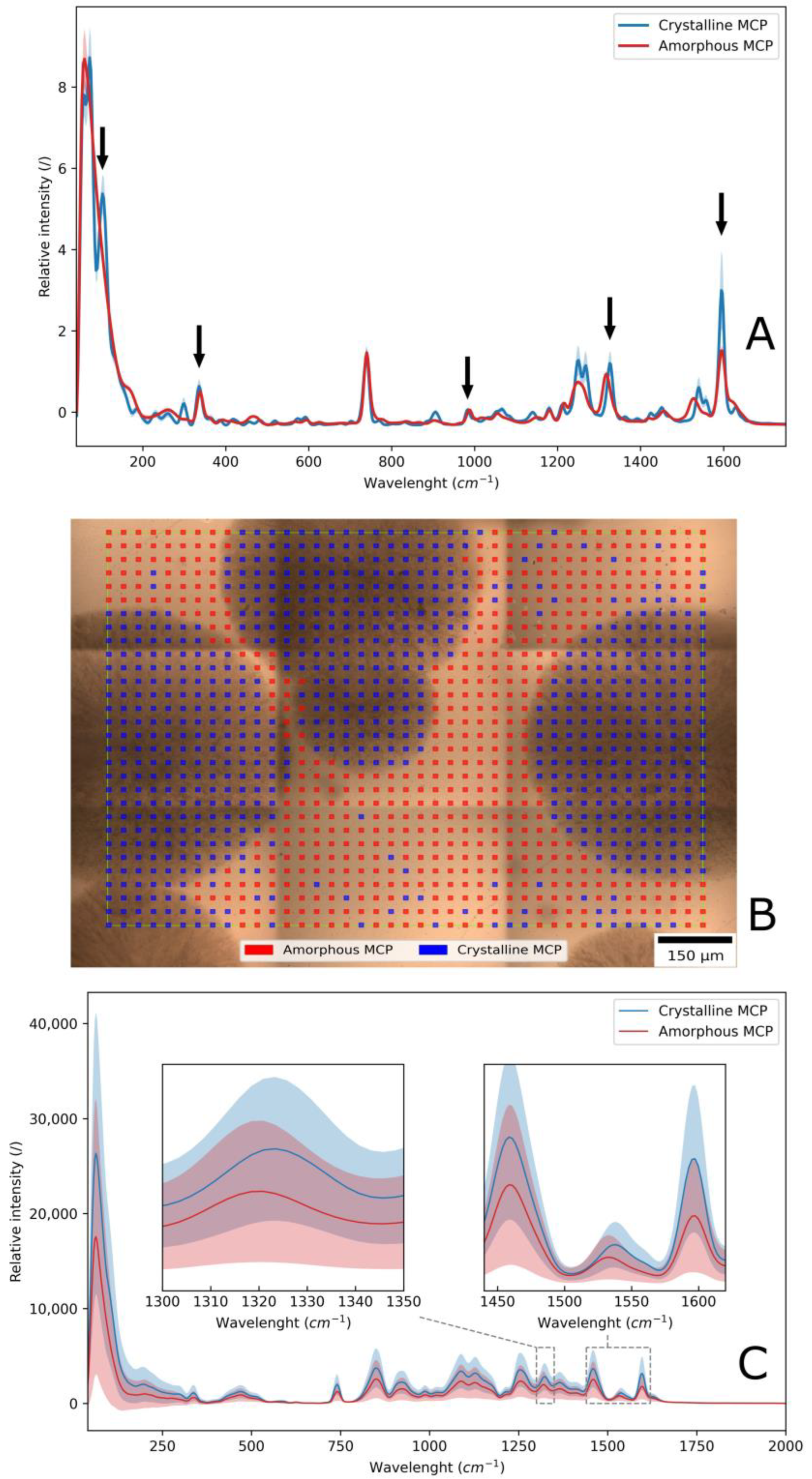
3.3. The Analysis of Drug Crystallization in the Film by Raman Microscopy
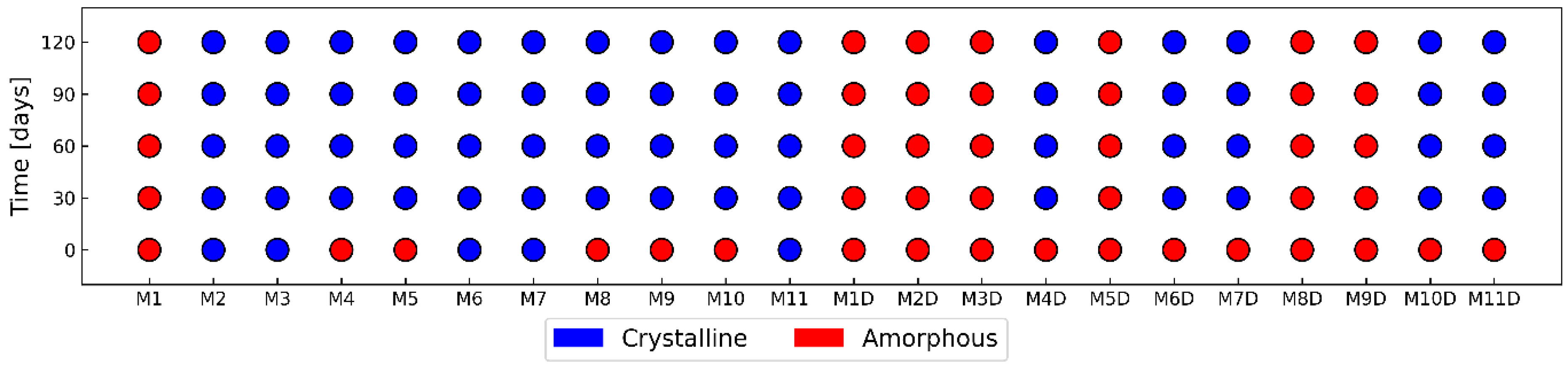
3.4. Analysis of MCP Physical Stability by Image Analytics
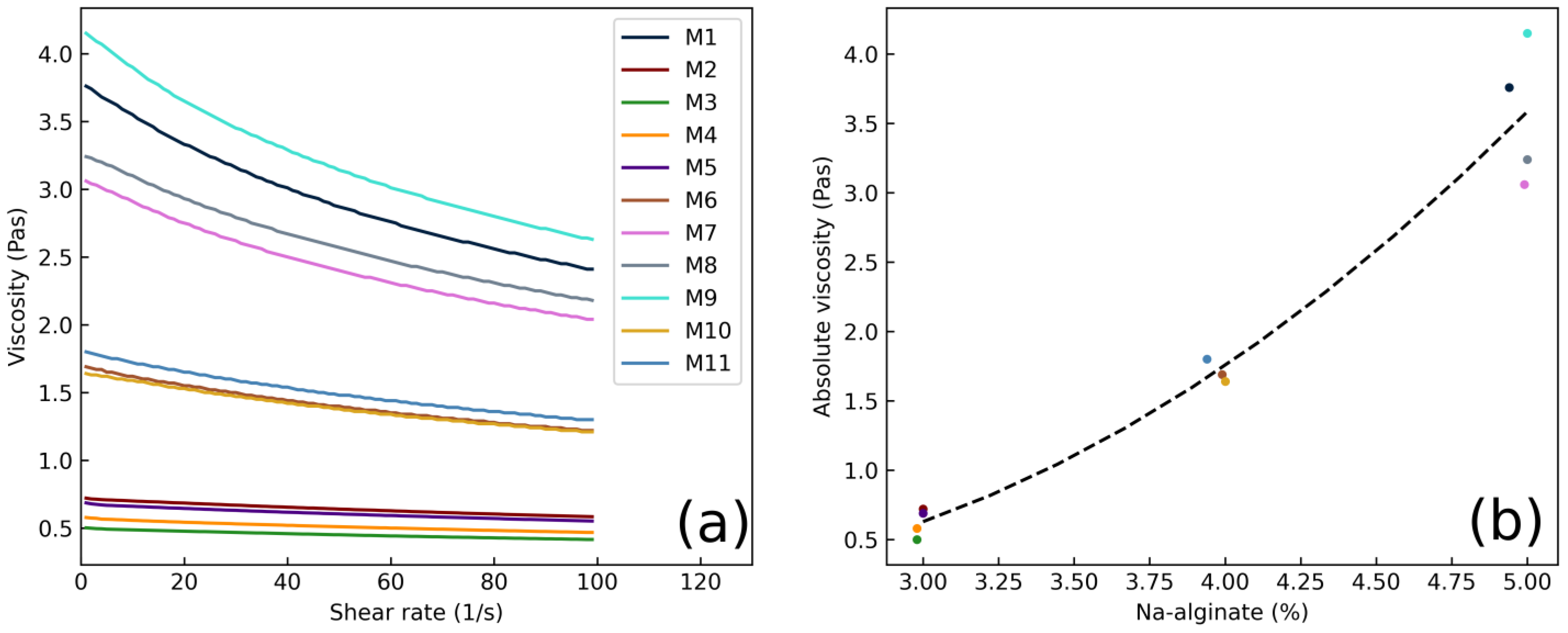
3.5. Viscosity of the Casting Solution
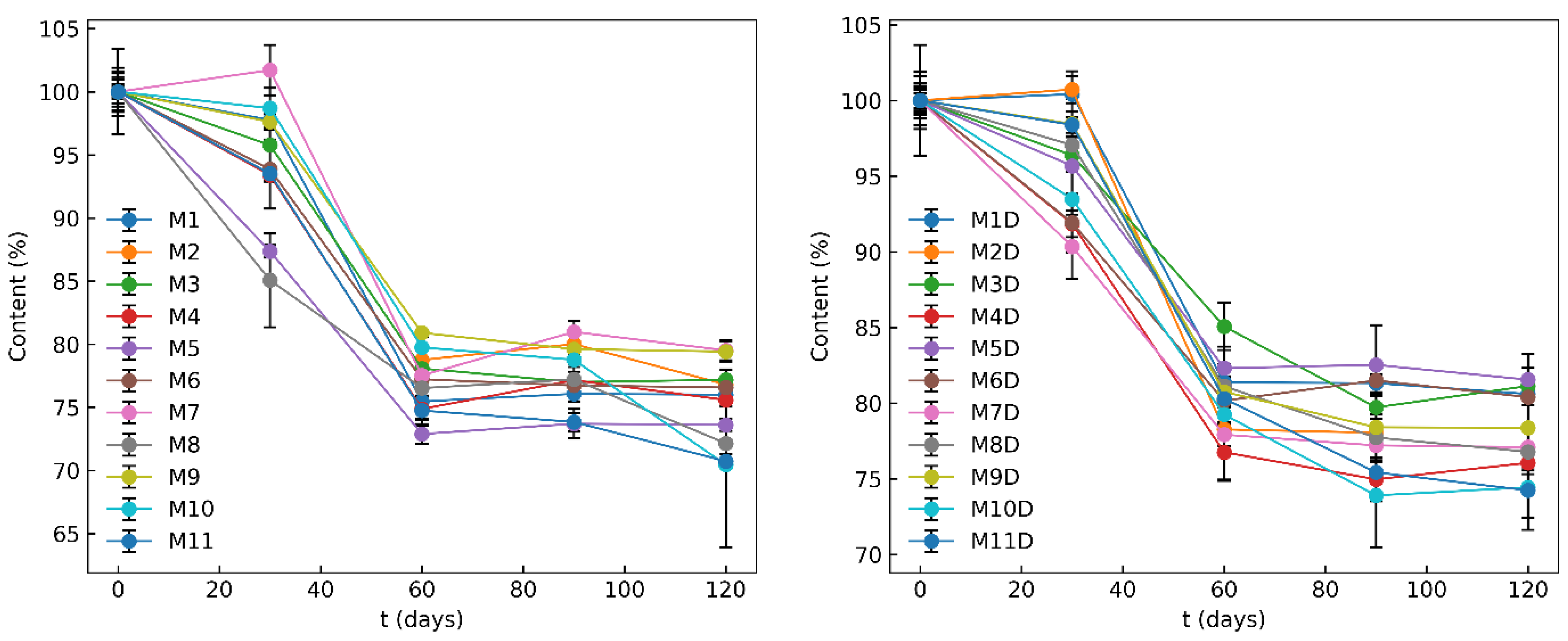
3.6. Chemical Stability of the MCP Film Formulations
4. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Morales, J.O.; McConville, J.T. Manufacture and Characterization of Mucoadhesive Buccal Films. Eur. J. Pharm. Biopharm. 2011, 77, 187–199. [Google Scholar] [CrossRef] [PubMed]
- Gilhotra, R.M.; Ikram, M.; Srivastava, S.; Gilhotra, N. A Clinical Perspective on Mucoadhesive Buccal Drug Delivery Systems. J. Biomed. Res. 2014, 28, 81–97. [Google Scholar] [CrossRef] [PubMed]
- Squier, C.A.; Nanny, D. Measurement of Blood Flow in the Oral Mucosa and Skin of the Rhesus Monkey Using Radiolabelled Microspheres. Arch. Oral Biol. 1985, 30, 313–318. [Google Scholar] [CrossRef] [PubMed]
- Sudhakar, Y.; Kuotsu, K.; Bandyopadhyay, A.K. Buccal Bioadhesive Drug Delivery--a Promising Option for Orally Less Efficient Drugs. J. Control. Release 2006, 114, 15–40. [Google Scholar] [CrossRef] [PubMed]
- Price, G.; Patel, D.A. Drug Bioavailability. In StatPearls; StatPearls Publishing: Treasure Island, FL, USA, 2023. [Google Scholar]
- Kleeberg, U.R.; Filbet, M.; Zeppetella, G. Fentanyl Buccal Tablet for Breakthrough Cancer Pain: Why Titrate? Pain Pract. 2011, 11, 185–190. [Google Scholar] [CrossRef]
- Hua, S. Advances in Nanoparticulate Drug Delivery Approaches for Sublingual and Buccal Administration. Front. Pharmacol. 2019, 10, 1328. [Google Scholar] [CrossRef] [PubMed]
- Ryan, J.L. Treatment of Chemotherapy-Induced Nausea in Cancer Patients. Eur. Oncol. 2010, 6, 14–16. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Bateman, D.N. Clinical Pharmacokinetics of Metoclopramide. Clin. Pharmacokinet. 1983, 8, 523–529. [Google Scholar] [CrossRef]
- Taylor, W.B.; Bateman, D.N. Oral Bioavailability of High-Dose Metoclopramide. Eur. J. Clin. Pharmacol. 1986, 31, 41–44. [Google Scholar] [CrossRef]
- Tizkam, H.; Fadhil, O.; Ghazy, E. Formulation and Evaluation of Metoclopramide Fast Dissolving Film (FDF). Syst. Rev. Pharm. 2020, 11, 1641–1646. [Google Scholar] [CrossRef]
- Auda, S.; Mahrous, G.; EL-Badry, M.; Fathalla, D. Development, Preparation and Evaluation of Oral Dissolving Films Containing Metoclopramide. Lat. Am. J. Pharm. 2014, 33, 1027–1033. [Google Scholar]
- Mady, O.; Hussien, S.; Abdelkader, D.H.; El-Dahaby, E. Metoclopramide Loaded Buccal Films for Potential Treatment of Migraine Symptoms: In Vitro and in Vivo Study. Pharm. Dev. Technol. 2023, 28, 650–659. [Google Scholar] [CrossRef] [PubMed]
- Sarwar, Z.; Farooq, M.; Adnan, S.; Saleem, M.U.; Masood, Z.; Mahmood, A. Development and Optimization of Metoclopramide Containing Polymeric Patches: Impact of Permeation Enhancers. Braz. J. Pharm. Sci. 2023, 58, e21131. [Google Scholar] [CrossRef]
- Zaman, M.; Hassan, R.; Razzaq, S.; Mahmood, A.; Amjad, M.W.; Raja, M.A.G.; Qaisar, A.A.; Majeed, A.; Hanif, M.; Tahir, R.A. Fabrication of Polyvinyl Alcohol Based Fast Dissolving Oral Strips of Sumatriptan Succinate and Metoclopramide HCL. Sci. Prog. 2020, 103, 0036850420964302. [Google Scholar] [CrossRef] [PubMed]
- Zaman, M.; Hassan, R.; Amjad, M.W.; Khan, S.M.; Gaffor Raja, M.A.; Shah, S.S.; Siddique, W.; Aman, W.; Abid, Z.; Butt, M.H. Formulation of Instant Disintegrating Buccal Films without Using Disintegrant: An in-Vitro Study. Pak. J. Pharm. Sci. 2021, 34, 2357–2364. [Google Scholar]
- Lao, L.L.; Venkatraman, S.S.; Peppas, N.A. A Novel Model and Experimental Analysis of Hydrophilic and Hydrophobic Agent Release from Biodegradable Polymers. J. Biomed. Mater. Res. Part A 2009, 90A, 1054–1065. [Google Scholar] [CrossRef] [PubMed]
- Al-Musa, S.; Abu Fara, D.; Badwan, A.A. Evaluation of Parameters Involved in Preparation and Release of Drug Loaded in Crosslinked Matrices of Alginate. J. Control. Release 1999, 57, 223–232. [Google Scholar] [CrossRef]
- Karaiskou, S.G.; Kouskoura, M.G.; Markopoulou, C.K. Modern Pediatric Formulations of the Soft Candies in the Form of a Jelly: Determination of Metoclopramide Content and Dissolution. Pharm. Dev. Technol. 2020, 25, 20–27. [Google Scholar] [CrossRef]
- Bartlett, J.A.; van der Voort Maarschalk, K. Understanding the Oral Mucosal Absorption and Resulting Clinical Pharmacokinetics of Asenapine. AAPS PharmSciTech 2012, 13, 1110–1115. [Google Scholar] [CrossRef]
- Remuñán-López, C.; Portero, A.; Vila-Jato, J.L.; Alonso, M.J. Design and Evaluation of Chitosan/Ethylcellulose Mucoadhesive Bilayered Devices for Buccal Drug Delivery. J. Control. Release 1998, 55, 143–152. [Google Scholar] [CrossRef]
- Kassem, A.A.; Issa, D.A.E.; Kotry, G.S.; Farid, R.M. Thiolated Alginate-Based Multiple Layer Mucoadhesive Films of Metformin Forintra-Pocket Local Delivery: In Vitro Characterization and Clinical Assessment. Drug Dev. Ind. Pharm. 2017, 43, 120–131. [Google Scholar] [CrossRef] [PubMed]
- Abruzzo, A.; Nicoletta, F.P.; Dalena, F.; Cerchiara, T.; Luppi, B.; Bigucci, F. Bilayered Buccal Films as Child-Appropriate Dosage Form for Systemic Administration of Propranolol. Int. J. Pharm. 2017, 531, 257–265. [Google Scholar] [CrossRef] [PubMed]
- Cui, Z.; Mumper, R.J. Bilayer Films for Mucosal (Genetic) Immunization via the Buccal Route in Rabbits. Pharm. Res. 2002, 19, 947–953. [Google Scholar] [CrossRef] [PubMed]
- Eleftheriadis, G.K.; Ritzoulis, C.; Bouropoulos, N.; Tzetzis, D.; Andreadis, D.A.; Boetker, J.; Rantanen, J.; Fatouros, D.G. Unidirectional Drug Release from 3D Printed Mucoadhesive Buccal Films Using FDM Technology: In Vitro and Ex Vivo Evaluation. Eur. J. Pharm. Biopharm. 2019, 144, 180–192. [Google Scholar] [CrossRef] [PubMed]
- Preis, M.; Woertz, C.; Schneider, K.; Kukawka, J.; Broscheit, J.; Roewer, N.; Breitkreutz, J. Design and Evaluation of Bilayered Buccal Film Preparations for Local Administration of Lidocaine Hydrochloride. Eur. J. Pharm. Biopharm. 2014, 86, 552–561. [Google Scholar] [CrossRef]
- Basahih, T.S.; Alamoudi, A.A.; El-Say, K.M.; Alhakamy, N.A.; Ahmed, O.A.A. Improved Transmucosal Delivery of Glimepiride via Unidirectional Release Buccal Film Loaded with Vitamin E TPGS-Based Nanocarrier. Dose-Response 2020, 18, 1559325820945164. [Google Scholar] [CrossRef]
- Vippagunta, S.R.; Brittain, H.G.; Grant, D.J.W. Crystalline Solids. Adv. Drug Deliv. Rev. 2001, 48, 3–26. [Google Scholar] [CrossRef]
- Senta-Loys, Z.; Bourgeois, S.; Pailler-Mattei, C.; Agusti, G.; Briançon, S.; Fessi, H. Formulation of Orodispersible Films for Paediatric Therapy: Investigation of Feasibility and Stability for Tetrabenazine as Drug Model. J. Pharm. Pharmacol. 2017, 69, 582–592. [Google Scholar] [CrossRef]
- Yang, F.; Su, Y.; Zhang, J.; DiNunzio, J.; Leone, A.; Huang, C.; Brown, C.D. Rheology Guided Rational Selection of Processing Temperature to Prepare Copovidone–Nifedipine Amorphous Solid Dispersions via Hot Melt Extrusion (HME). Mol. Pharm. 2016, 13, 3494–3505. [Google Scholar] [CrossRef]
- Verma, S.; Shlichta, P.J. Imaging Techniques for Mapping Solution Parameters, Growth Rate, and Surface Features during the Growth of Crystals from Solution. Prog. Cryst. Growth Charact. Mater. 2008, 54, 1–120. [Google Scholar] [CrossRef]
- Godec, P.; Pančur, M.; Ilenič, N.; Čopar, A.; Stražar, M.; Erjavec, A.; Pretnar, A.; Demšar, J.; Starič, A.; Toplak, M.; et al. Democratized Image Analytics by Visual Programming through Integration of Deep Models and Small-Scale Machine Learning. Nat. Commun. 2019, 10, 4551. [Google Scholar] [CrossRef]
- Grilc, B.; Zdovc, J.; Planinšek, O. Advanced Flow Cell Design for in Vitro Release Testing of Mucoadhesive Buccal Films. Acta Pharm. 2020, 70, 359–371. [Google Scholar] [CrossRef]
- Wang, S.-L.; Wong, Y.-C.; Cheng, W.-T.; Lin, S.-Y. A Continuous Process for Solid-State Dehydration, Amorphization and Recrystallization of Metoclopramide HCL Monohydrate Studied by Simultaneous DSC-FTIR Microspectroscopy. J. Therm. Anal. Calorim. 2011, 104, 261–264. [Google Scholar] [CrossRef]
- Metoclopramide Hydrochloride Monohydrate. Under Chapter: 04/2018:0674 in European Pharmacopoeia 11.2 Edition. Available online: https://pheur.edqm.eu/app/11-2/content/11-2/0674E.htm?highlight=on&terms=metoclopramide (accessed on 23 May 2023).
- Wong, T.W.; Ashikin, W.H.N.S.; Law, C.L. Evaporation and Diffusion Transport Properties and Mechanical Properties of Alginate Dried Film. Dry. Technol. 2014, 32, 117–125. [Google Scholar] [CrossRef]
- Grilc, B.; Felicijan, T.; Parfant, T.P.; Planinšek, O. Formulation and Characterization of Buccal Films Containing Valsartan with Additional Support from Image Analysis. AAPS PharmSciTech 2023, 24, 72. [Google Scholar] [CrossRef] [PubMed]
- Segale, L.; Mannina, P.; Giovannelli, L.; Muschert, S.; Pattarino, F. Formulation and Coating of Alginate and Alginate-Hydroxypropylcellulose Pellets Containing Ranolazine. J. Pharm. Sci. 2016, 105, 3351–3358. [Google Scholar] [CrossRef] [PubMed]
- Tang, L.; Hong, B.; Li, T.; Huang, B. Development of Bilayer Films Based on Shellac and Esterified Cellulose Nanocrystals for Buccal Drug Delivery. Cellulose 2019, 26, 1157–1167. [Google Scholar] [CrossRef]
- Gajdošová, M.; Vetchý, D.; Muselík, J.; Gajdziok, J.; Juřica, J.; Vetchá, M.; Hauptman, K.; Jekl, V. Bilayer Mucoadhesive Buccal Films with Prolonged Release of Ciclopirox Olamine for the Treatment of Oral Candidiasis: In Vitro Development, Ex Vivo Permeation Testing, Pharmacokinetic and Efficacy Study in Rabbits. Int. J. Pharm. 2021, 592, 120086. [Google Scholar] [CrossRef]
- Leopold, N.; Cîntǎ-Pînzaru, S.; Szabó, L.; Ileşan, D.; Chiş, V.; Cozar, O.; Kiefer, W. Raman and SERS Study of Metoclopramide at Different pH Values. J. Raman Spectrosc. 2010, 41, 248–255. [Google Scholar] [CrossRef]
- Wang, X.; Zhang, L.; Ma, D.; Tang, X.; Zhang, Y.; Yin, T.; Gou, J.; Wang, Y.; He, H. Characterizing and Exploring the Differences in Dissolution and Stability between Crystalline Solid Dispersion and Amorphous Solid Dispersion. AAPS PharmSciTech 2020, 21, 262. [Google Scholar] [CrossRef]
- Imtiaz, M.S.; Shoaib, M.H.; Yousuf, R.I.; Ali, F.R.; Saleem, M.T.; Khan, M.Z.; Sikandar, M. Formulation Development and Evaluation of Drug-in-Adhesive-Type Transdermal Patch of Metoclopramide HCl. Polym. Bull. 2022, 79, 1187–1200. [Google Scholar] [CrossRef]
- Lin, S.-Y. Molecular Perspectives on Solid-State Phase Transformation and Chemical Reactivity of Drugs: Metoclopramide as an Example. Drug Discov. Today 2015, 20, 209–222. [Google Scholar] [CrossRef] [PubMed]




| Formulation | Metoclopramide (%) | Na Alginate (%) | Xylitol (%) | pH | Water (%) |
|---|---|---|---|---|---|
| M1 | 0.8 | 5 | 3 | 4.5 | 91.2 |
| M2 | 1.4 | 3 | 1 | 6.0 | 94.6 |
| M3 | 0.8 | 3 | 1 | 4.5 | 95.2 |
| M4 | 1.4 | 3 | 3 | 4.5 | 92.6 |
| M5 | 0.8 | 3 | 3 | 6.0 | 93.2 |
| M6 | 1.1 | 4 | 2 | 5.5 | 92.9 |
| M7 | 1.4 | 5 | 1 | 4.5 | 92.6 |
| M8 | 0.8 | 5 | 1 | 6.0 | 93.2 |
| M9 | 1.4 | 5 | 3 | 6.0 | 90.6 |
| M10 | 1.1 | 4 | 2 | 5.5 | 92.9 |
| M11 | 1.1 | 4 | 2 | 5.5 | 92.9 |
| Time (min) | Mobile Phase A (Per Cent V/V) | Mobile Phase B (Per Cent V/V) |
|---|---|---|
| 0–1.5 | 95 | 5 |
| 1.5–16.5 | 95 → 42.5 | 5 → 57.5 |
| 16.5–17.5 | 95 | 5 |
| MCP | Na-Alginate | Xylitol | pH |
|---|---|---|---|
| 11.1 | −11.1 | −33.5 | −6.0 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Grilc, B.; Planinšek, O. Evaluation of Monolayer and Bilayer Buccal Films Containing Metoclopramide. Pharmaceutics 2024, 16, 354. https://doi.org/10.3390/pharmaceutics16030354
Grilc B, Planinšek O. Evaluation of Monolayer and Bilayer Buccal Films Containing Metoclopramide. Pharmaceutics. 2024; 16(3):354. https://doi.org/10.3390/pharmaceutics16030354
Chicago/Turabian StyleGrilc, Blaž, and Odon Planinšek. 2024. "Evaluation of Monolayer and Bilayer Buccal Films Containing Metoclopramide" Pharmaceutics 16, no. 3: 354. https://doi.org/10.3390/pharmaceutics16030354
APA StyleGrilc, B., & Planinšek, O. (2024). Evaluation of Monolayer and Bilayer Buccal Films Containing Metoclopramide. Pharmaceutics, 16(3), 354. https://doi.org/10.3390/pharmaceutics16030354






