Artificial Intelligence in Pharmaceutical Technology and Drug Delivery Design
Abstract
1. Introduction
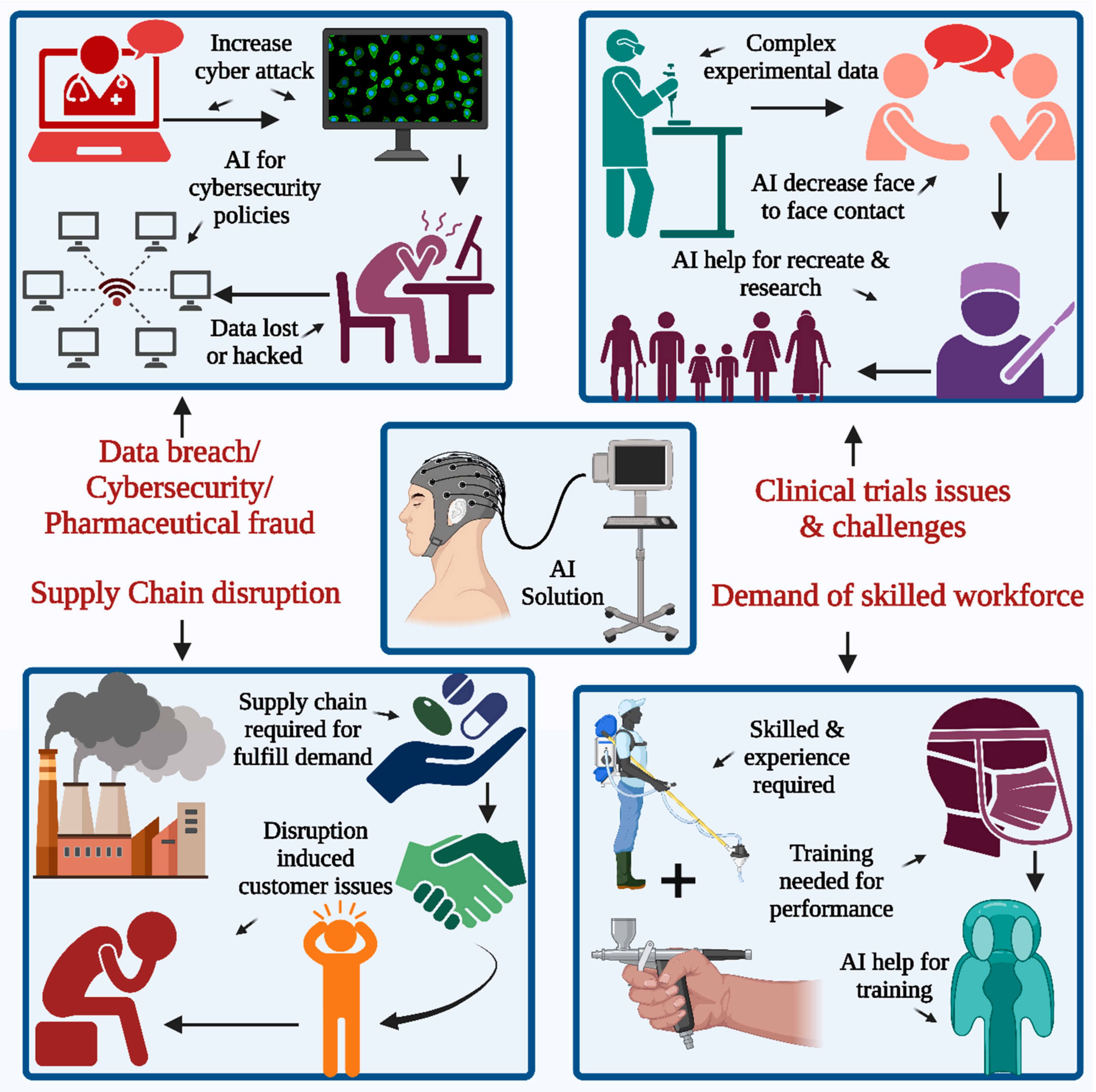
2. Current Pharmaceutical Challenges and the Role of AI
2.1. Supervised AI Learning
- Drug Discovery and Design: Supervised learning algorithms can be used to predict the activity or properties of new drug candidates. By training on a dataset of known compounds and their associated activities, the model can learn patterns and relationships between molecular features and desired outcomes. This enables the prediction of the activity, potency, or toxicity of novel compounds, aiding in drug discovery and design [38].
- Predictive Maintenance and Quality Control: In pharmaceutical manufacturing, supervised learning can be utilized for predictive maintenance and quality control. By training on data from manufacturing processes, equipment sensor data, or quality testing results, the model can learn to predict equipment failure, product quality deviations, or process abnormalities, allowing for proactive maintenance and quality assurance [39].
- Drug Target Identification: Supervised learning techniques can help identify potential drug targets by analyzing biological data. By training on data that include information about genetic, proteomic, or transcriptomic features and their relationship to drug response or disease progression, the model can learn patterns and identify potential targets for further investigation [40].
- Disease Diagnosis and Prognosis: Supervised learning models can be used to diagnose diseases or predict patient outcomes based on medical data. By training on labeled datasets containing patient characteristics, clinical data, and disease outcomes, the model can learn to classify patients into different disease categories or predict disease progression or treatment response [41].
- Adverse Event Detection: Supervised learning algorithms can be applied to pharmacovigilance data to identify and classify adverse events associated with drugs. By training on labeled adverse event reports, the model can learn to recognize patterns and identify potential safety signals, helping in the detection and characterization of adverse events [42].
- Predictive Modeling for Clinical Trials: Supervised learning can be used to predict outcomes in clinical trials. By training on historical clinical trial data, including patient characteristics, treatment interventions, and trial outcomes, the model can learn to predict patient response, treatment efficacy, or safety outcomes. This information can guide trial design and optimize patient selection [43].
2.2. Unsupervised AI Learning
- Clustering: Clustering algorithms group data points based on their similarities, allowing the identification of natural groupings or clusters within the data. In pharmaceutical applications, clustering can be applied to various datasets, such as gene expression profiles, chemical structures, or patient data, to uncover subgroups with similar characteristics. This can aid in target identification, patient stratification, and identifying distinct classes of compounds or diseases [46].
- Dimensionality Reduction: Dimensionality reduction techniques, such as principal component analysis (PCA) and t-distributed stochastic neighbor embedding (t-SNE), are used to reduce the complexity of high-dimensional datasets while preserving meaningful information. These methods can help visualize and explore complex datasets, identify key variables or features, and support decision-making processes. Dimensionality reduction can be applied to various types of pharmaceutical data, including gene expression data, drug activity profiles, or imaging data [47].
- Anomaly Detection: Anomaly detection algorithms identify rare or unusual data points that deviate significantly from the expected patterns. In the pharmaceutical industry, anomaly detection can be useful for detecting adverse events, identifying potential safety concerns, and uncovering data quality issues. Unsupervised anomaly detection techniques, such as the local outlier factor (LOF) or isolation forest, can help highlight abnormal patterns or data points that warrant further investigation [48].
- Association Rule Mining: Association rule mining techniques, such as the Apriori algorithm, aim to discover interesting relationships or associations between items in a dataset. In the pharmaceutical context, association rule mining can be applied to drug–drug interactions, adverse event data, or co-occurrence patterns between medical conditions and medications. These techniques can provide insights into potential drug interactions, identify medication patterns, or support pharmacovigilance activities [49].
- Topic Modeling: Topic modeling algorithms, such as latent Dirichlet allocation (LDA), extract latent topics or themes from large text datasets. In the pharmaceutical industry, topic modeling can be used to analyze the scientific literature, clinical trial reports, or social media data to identify key research themes, emerging trends, or patient sentiments. This can aid in literature mining, competitive intelligence, or understanding patient perspectives [50,51].
| AI/Machine Learning Models | Description/Usage | References |
|---|---|---|
| Generative Adversarial Networks (GANs) | GANs are widely used in drug product development to generate novel chemical structures and optimize their properties. GANs consist of a generator network that creates new molecules and a discriminator network that evaluates their quality, leading to the generation of structurally diverse and functionally optimized drug candidates. | [52] |
| Recurrent Neural Networks (RNNs) | RNNs are commonly employed for sequence-based tasks in drug development, such as predicting protein structures, analyzing genomic data, and designing peptide sequences. They capture sequential dependencies and can generate new sequences based on learned patterns. | [53] |
| Convolutional Neural Networks (CNNs) | CNNs are effective in image-based tasks, including analyzing molecular structures and identifying potential drug targets. They can extract relevant features from molecular images and aid in drug design and target identification | [54] |
| Long Short-Term Memory Networks (LSTMs) | LSTMs are a type of RNN that excel in modeling and predicting temporal dependencies. They have been used in pharmacokinetics and pharmacodynamics studies to predict drug concentration-time profiles and evaluate drug efficacy. | [55] |
| Transformer Models | Transformer models, such as the popular BERT (Bidirectional Encoder Representations from Transformers), have been employed in natural language processing tasks in the pharmaceutical domain. They can extract useful information from the scientific literature, patent databases, and clinical trial data, enabling researchers to make informed decisions in drug development. | [56] |
| Reinforcement Learning (RL) | RL techniques have been applied to optimize drug dosing strategies and develop personalized treatment plans. RL algorithms learn from interactions with the environment to make sequential decisions, aiding in dose optimization, and improving patient outcomes. | [57] |
| Bayesian Models | Bayesian models, such as Bayesian networks and Gaussian processes, are employed for uncertainty quantification and decision-making in drug development. They enable researchers to make probabilistic predictions, assess risks, and optimize experimental designs. | [58,59] |
| Deep Q-Networks (DQNs) | DQNs, a combination of deep learning and reinforcement learning, have been used to optimize drug discovery processes by predicting the activity of compounds and suggesting high-potential candidates for further experimentation. | [60,61] |
| Autoencoders | Autoencoders are unsupervised learning models used for dimensionality reduction and feature extraction in drug development. They can capture essential characteristics of molecules and assist in compound screening and virtual screening. | [62,63] |
| Graph Neural Networks (GNNs) | GNNs are designed to process graph-structured data, making them suitable for drug discovery tasks that involve molecular structures. They can model molecular graphs, predict properties, and aid in virtual screening and de novo drug design. | [64,65] |
3. AI for Drug Discovery
3.1. Target Identification
3.2. Virtual Screening
3.3. Structure-Activity Relationship (SAR) Modeling
3.4. De Novo Drug Design
3.5. Optimization of Drug Candidates
3.6. Drug Repurposing
3.7. Toxicity Prediction
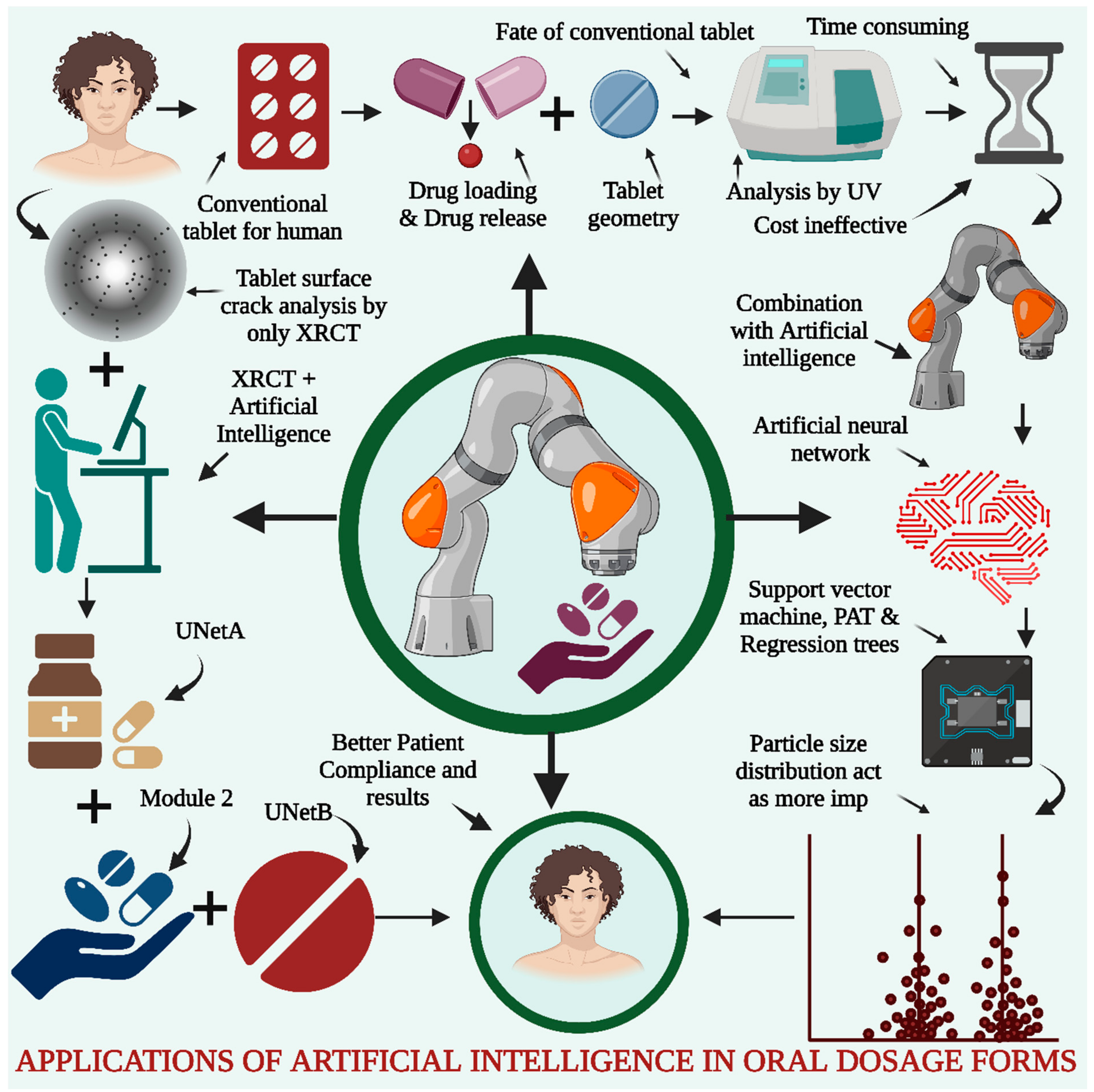
4. AI Tool Application in Dosage Form Designs
5. AI for Drug Delivery
5.1. AI for Oral Solid Dosage Form Development
| AI/Machine Learning Models | Description/Usage | References |
|---|---|---|
| Genetic Algorithms | Genetic algorithms are optimization techniques inspired by the principles of natural selection and genetics. They can be applied to optimize formulation compositions, drug release profiles, and process parameters to achieve desired dosage form characteristics. | [95] |
| Artificial Neural Networks (ANNs) | ANNs have been employed to model and optimize drug release kinetics from different dosage forms. They can assist in determining optimal formulations and predict the release behavior of active pharmaceutical ingredients (APIs) under various conditions. | [96] |
| Support Vector Machines (SVMs) | SVMs have been used in dosage form optimization to predict and model relationships between formulation variables, such as excipient composition, processing parameters, and drug release profiles. They aid in optimizing formulation design space. | [97] |
| Particle Swarm Optimization (PSO) | PSO is a population-based optimization algorithm that can be used for dosage form optimization. It has been applied to optimize particle size distribution, dissolution profiles, and other formulation parameters. | [98] |
| Artificial Intelligence-based Expert Systems | Expert systems utilize AI techniques, including rule-based systems and fuzzy logic, to simulate the decision-making process of human experts. They can be applied to dosage form optimization by considering multiple formulation and process variables. | [99] |
| Monte Carlo Simulation | Monte Carlo simulation methods have been used to optimize drug product performance by considering uncertainties and variability in formulation and process parameters. They aid in robust formulation and process design. | [100] |
| Computational Fluid Dynamics (CFD) | CFD simulations enable the optimization of fluid flow and mixing within dosage form manufacturing processes, such as granulation, coating, and drying. They help in designing efficient and uniform processes. | [101,102] |
| Response Surface Methodology (RSM) | RSM is a statistical technique that helps optimize dosage form formulations by modeling and analyzing the relationship between multiple variables and their effect on formulation responses. It aids in understanding and optimizing formulation parameters. | [103,104,105] |
| Artificial Neural Network–Genetic Algorithm (ANN-GA) Hybrid Models | Hybrid models combining ANN and GA techniques have been used for dosage form optimization. They can efficiently search the formulation space to identify optimal solutions and predict formulation characteristics. | |
| Multivariate Analysis Techniques | Multivariate analysis methods, such as principal component analysis (PCA) and partial least squares (PLS), have been employed in dosage form optimization. They aid in identifying critical formulation variables, reducing dimensionality, and optimizing formulation performance. | [106,107,108] |
5.1.1. Prediction of Dug Release through Formulations
5.1.2. Application of AI for 3D-Printed Dosage Forms
5.1.3. Application of AI for the Detection of Tablet Defects
5.1.4. AI for the Prediction of Physicochemical Stability
5.1.5. Contribution of AI to Dissolution Rate Predictions
5.2. AI for Nanomedicine
5.3. AI Application for Parenteral, Transdermal and Mucosal Route Products
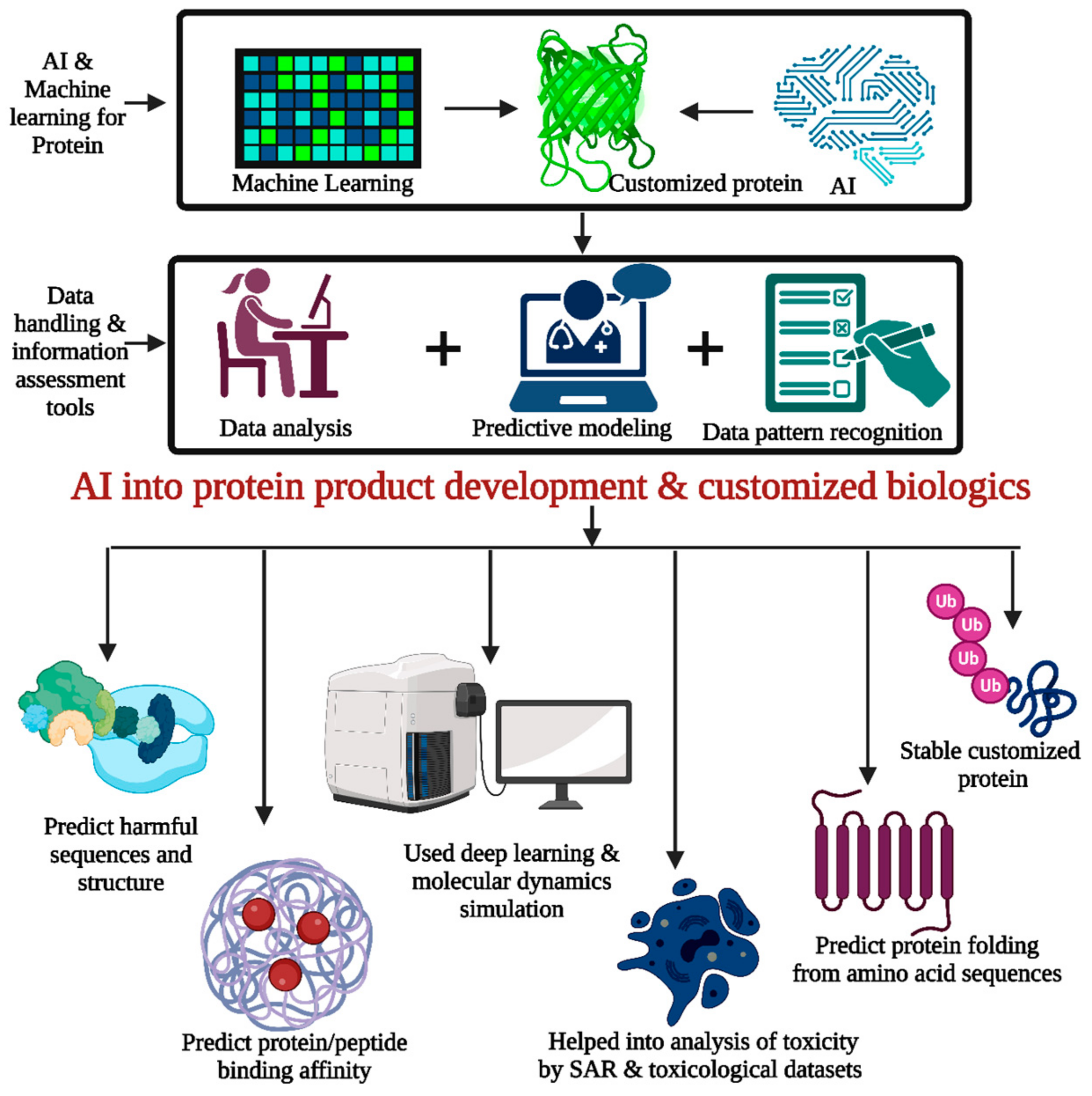
5.4. AI Tools for Biologics Product Development
5.5. AI in Medical Devices
- Diagnostic Assistance: AI algorithms can analyze medical imaging data such as X-rays, CT scans, and MRIs to assist healthcare professionals in detecting and diagnosing diseases. For example, AI-powered algorithms can help identify cancerous lesions in medical images or detect abnormalities in electrocardiograms (ECGs) [168].
- Remote Monitoring: AI-enabled medical devices can remotely monitor patients’ health conditions, allowing for the continuous tracking of vital signs and other relevant parameters. This is particularly useful for patients with chronic conditions who can receive personalized care from the comfort of their homes. AI algorithms can analyze the collected data and provide alerts or insights to healthcare providers [169].
- Wearable Devices: AI is integrated into wearable devices such as smartwatches, fitness trackers, and biosensors. These devices can monitor various health parameters, such as heart rate, sleep patterns, physical activity, and even blood glucose levels. AI algorithms help interpret the data and provide users with actionable insights for improving their health and well-being [170].
- Prosthetics and Rehabilitation: AI is used in advanced prosthetic devices to provide more natural movement and functionality. Machine learning algorithms can learn from user movements and adapt the prosthetic to better match the user’s intentions. AI can also assist in rehabilitation by analyzing motion and providing feedback to patients to improve their movements and track progress [171].
- Surgical Assistance: AI has found applications in surgical devices, aiding surgeons during procedures. For instance, robotic surgical systems use AI algorithms to assist surgeons in performing precise and minimally invasive procedures. AI can also analyze preoperative and intraoperative data to provide real-time guidance and improve surgical outcomes [172].
- Medication Management: AI-powered devices can help patients manage their medications effectively. Smart pill dispensers can remind patients to take their medications on time, dispense the correct dosage, and track adherence. AI algorithms can also analyze patient data, such as medical history and medication usage, to provide personalized recommendations for medication management [173].
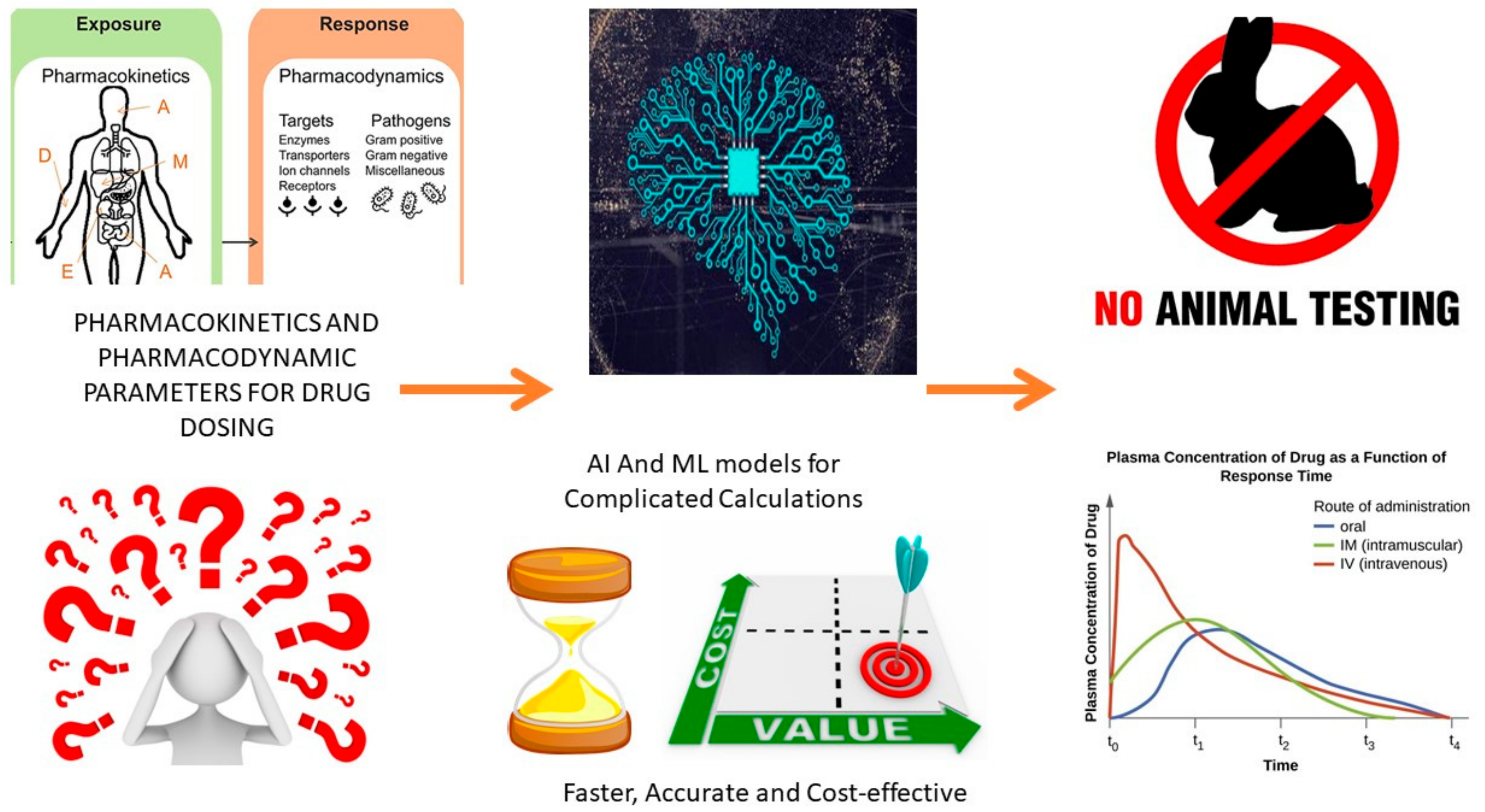
6. AI for Pharmacokinetics and Pharmacodynamics
6.1. AI-Based Methods to Predict Pharmacokinetic Parameters
6.2. AI-Based Computational Method for PBPK
6.3. Prediction of Drug Release and Absorption Parameters
6.4. Prediction of Metabolism and Excretion Parameters
| Algorithm/Software | Aim/Target | Advantage | Limitation | PK/PD/Both | Reference |
|---|---|---|---|---|---|
| Bayesian/WinBUGS | To handle data below the limit of quantification |
|
| Both | [205] |
| Bayesian/PKBUGS (v 1.1)/WinBUGS (v 1.3) | Pharmacokinetic analysis of sirolimus concentration data for therapeutic drug monitoring |
|
| PK | [206] |
| Support Vector Machine/Least Square-SVM | Drug concentration analysis of sample drug based on individual patient profile |
|
| PK | [207] |
| Support Vector Machine/Drug Administration Decision Support System (DADSS) and Random Sample Consensus RANSAC | Prediction of drug concentration, ideal dose, and dose intervals for a new patient |
|
| PK | [208] |
| Support Vector Machine/Profile Dependent SVM | Therapeutic drug monitoring of kidney transplant recipient |
|
| PK | [209] |
| Support Vector System + Random Forrest Model | Pharmacodynamic drug interaction based on Side-Effect Similarity (SES), Chemical Similarity (CS), and Target Protein Connectedness (TPC) |
|
| PD | [210] |
| Linear Regressions (LASSO)/Gradient Boosting Machines/XGBoost/Random Forest | Prediction of the plasma concentration–time series and area under the concentration-versus-time curve from 0 to 24 h after repeated dosing of Rifampicin |
|
| PK | [182] |
| XGBoost | Estimation of drug area under the curve (AUC) of tacrolimus or mycophenolate mofetil (MMF) |
|
| PK | [211,212] |
| Simulated Annealing k-Nearest-Neighbor (SA-kNN)/Partial Least-Square (PLS)/Multiple Linear Regression (MLR)/Sybyl version 6.7 | Prediction of pharmacokinetic parameters of antimicrobial agents in humans based on their molecular structure |
|
| Both | [213] |
| Drug Target Interaction Convolutional Neural Network (DTICNN) | Identification of the drug-target interactions and predict potential drug molecules |
|
| PD | [214] |
| Deep Long Short-Term Memory (DeepLSTM) | Computational methods to validate the interaction between drugs and target |
|
| PD | [215] |
7. Limitations of AI Tools
7.1. Lack of Transparency
7.2. Limited Availability of Data
7.3. Biases in Data
7.4. Inability to Incorporate New Data
7.5. Limited Ability to Account for Variability
7.6. Interpretation of Results
7.7. Ethical Considerations
7.8. Complex Biological Systems
7.9. Lack of Clinical Expertise
7.10. Inactive Molecules
8. Current Trend: Fairy Tale to the Holy Grail
- Drug Discovery and Development: AI is revolutionizing the drug discovery process by enabling virtual screening, molecular modeling, and predictive analytics. AI algorithms can analyze vast amounts of chemical and biological data to identify potential drug candidates, optimize lead compounds, and predict their properties. This expedites the identification and development of novel therapeutics.
- Precision Medicine: AI is being utilized to advance precision medicine approaches. By analyzing patient data, including genomics, proteomics, and clinical records, AI algorithms can identify patient subgroups, predict treatment responses, and assist in personalized treatment decision-making. AI also contributes to the development of biomarkers for disease diagnosis and prognosis.
- Drug Repurposing: AI is being applied to identify new uses for existing drugs, a process known as drug repurposing. By analyzing large datasets and biological knowledge, AI algorithms can identify potential drug–disease associations and repurpose approved drugs for new therapeutic indications. This approach offers a faster and more cost-effective route to drug development.
- Drug Formulation and Delivery: AI plays a role in optimizing drug formulations and delivery systems. AI models can predict drug release kinetics and absorption profiles and optimize formulations for enhanced efficacy and targeted delivery. AI is also used to design drug delivery devices and systems that improve patient adherence and convenience.
- Clinical Trial Optimization: AI is being leveraged to optimize clinical trials, improving efficiency and reducing costs. AI algorithms can aid in patient recruitment, identify suitable trial populations, and optimize trial protocols. AI also assists in the real-time monitoring and analysis of trial data, allowing for adaptive trial designs and faster decision-making.
- Regulatory Compliance and Safety: AI is increasingly used to support regulatory compliance and ensure drug safety. AI algorithms can analyze real-world data, adverse event reports, and the literature to identify potential safety issues and monitor post-marketing drug safety. AI also helps in pharmacovigilance, signal detection, and adverse event prediction.
- Supply Chain Optimization: AI is applied to optimize pharmaceutical supply chains, ensuring efficient manufacturing, inventory management, and distribution. AI algorithms can predict demand, optimize production schedules, and enhance quality control processes, contributing to more streamlined and cost-effective operations.
9. Futuristic Overview
10. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Krikorian, G.; Torreele, E. We Cannot Win the Access to Medicines Struggle Using the Same Thinking That Causes the Chronic Access Crisis. Health Hum. Rights 2021, 23, 119–127. [Google Scholar]
- Chavda, V.P.; Vihol, D.; Patel, A.; Redwan, E.M.; Uversky, V.N. Introduction to Bioinformatics, AI, and ML for Pharmaceuticals. In Bioinformatics Tools for Pharmaceutical Drug Product Development; John Wiley & Sons, Ltd.: Hoboken, NJ, USA, 2023; pp. 1–18. [Google Scholar]
- Scannell, J.W.; Blanckley, A.; Boldon, H.; Warrington, B. Diagnosing the Decline in Pharmaceutical R&D Efficiency. Nat. Rev. Drug Discov. 2012, 11, 191–200. [Google Scholar] [CrossRef] [PubMed]
- Munos, B. Lessons from 60 Years of Pharmaceutical Innovation. Nat. Rev. Drug Discov. 2009, 8, 959–968. [Google Scholar] [CrossRef]
- Mak, K.-K.; Pichika, M.R. Artificial Intelligence in Drug Development: Present Status and Future Prospects. Drug Discov. Today 2019, 24, 773–780. [Google Scholar] [CrossRef]
- Biggest Challenges Facing the Pharmaceutical Industry in 2023. Available online: https://www.pssindia.com/2023/01/23/biggest-challenges-facing-the-pharmaceutical-industry-in-2023/ (accessed on 5 May 2023).
- Chavda, V.; Valu, D.; Parikh, P.; Tiwari, N.; Chhipa, A.; Shukla, S.; Patel, S.; Balar, P.; Paiva-Santos, A.; Patravale, V. Conventional and Novel Diagnostic Tools for the Diagnosis of Emerging SARS-CoV-2 Variants. Vaccines 2023, 11, 374. [Google Scholar] [CrossRef]
- Zignify. Available online: https://zignify.net/what-is-supply-chain-disruption-and-what-are-its-causes/#:~:text=LogisticsDelaysandFailures,resultingincongestionanddelays (accessed on 2 May 2023).
- Kgmg. Available online: https://kpmg.com/xx/en/home/insights/2022/12/the-supply-chain-trends-shaking-up-2023.html (accessed on 2 May 2023).
- Times of India Pharmaceutical Supply Chain Management: Crises and Innovations. Available online: https://timesofindia.indiatimes.com/blogs/voices/pharmaceutical-supply-chain-management-crises-and-innovations/ (accessed on 15 May 2023).
- Sharma, R.; Shishodia, A.; Gunasekaran, A.; Min, H.; Munim, Z.H. The Role of Artificial Intelligence in Supply Chain Management: Mapping the Territory. Int. J. Prod. Res. 2022, 60, 7527–7550. [Google Scholar] [CrossRef]
- Grilo, A.L.; Mantalaris, A. The Increasingly Human and Profitable Monoclonal Antibody Market. Trends Biotechnol. 2019, 37, 9–16. [Google Scholar] [CrossRef] [PubMed]
- Sarpatwari, A.; Barenie, R.; Curfman, G.; Darrow, J.J.; Kesselheim, A.S. The US Biosimilar Market: Stunted Growth and Possible Reforms. Clin. Pharmacol. Ther. 2019, 105, 92–100. [Google Scholar] [CrossRef]
- Daka, A.; Peer, D. RNAi-Based Nanomedicines for Targeted Personalized Therapy. Adv. Drug Deliv. Rev. 2012, 64, 1508–1521. [Google Scholar] [CrossRef]
- Colombo, S.; Zeng, X.; Ragelle, H.; Foged, C. Complexity in the Therapeutic Delivery of RNAi Medicines: An Analytical Challenge. Expert Opin. Drug Deliv. 2014, 11, 1481–1495. [Google Scholar] [CrossRef]
- Müller, R. Junghanns Nanocrystal Technology, Drug Delivery and Clinical Applications. Int. J. Nanomed. 2008, 3, 295–310. [Google Scholar] [CrossRef] [PubMed]
- Jain, K.K.; Jain, K.K. Nanomolecular Diagnostics. In The Handbook of Nanomedicine; Springer: Berlin/Heidelberg, Germany, 2017; pp. 133–200. [Google Scholar] [CrossRef]
- Kalepu, S.; Nekkanti, V. Insoluble Drug Delivery Strategies: Review of Recent Advances and Business Prospects. Acta Pharm. Sin. B 2015, 5, 442–453. [Google Scholar] [CrossRef]
- Deloitte Using-Ai-to-Accelerate-Clinical-Trials. Available online: https://www2.deloitte.com/us/en/blog/health-care-blog/2022/using-ai-to-accelerate-clinical-trials.html (accessed on 1 May 2023).
- Dickherber, A.; Morris, S.A.; Grodzinski, P. NCI Investment in Nanotechnology: Achievements and Challenges for the Future. Wiley Interdiscip. Rev. Nanomed. Nanobio Technol. 2015, 7, 251–265. [Google Scholar] [CrossRef] [PubMed]
- National Nanotechnology Initiative. NNI Budget Supplements and Strategic Plans. Available online: https://www.nano.gov/NNIBudgetSupplementsandStrategicPlans (accessed on 1 May 2023).
- Colombo, S.; Beck-Broichsitter, M.; Bøtker, J.P.; Malmsten, M.; Rantanen, J.; Bohr, A. Transforming Nanomedicine Manufacturing toward Quality by Design and Microfluidics. Adv. Drug Deliv. Rev. 2018, 128, 115–131. [Google Scholar] [CrossRef]
- Troiano, G.; Nolan, J.; Parsons, D.; Van Geen Hoven, C.; Zale, S. A Quality by Design Approach to Developing and Manufacturing Polymeric Nanoparticle Drug Products. AAPS J. 2016, 18, 1354–1365. [Google Scholar] [CrossRef] [PubMed]
- Puri, M.; Pathak, Y.; Sutariya, V.K.; Tipparaju, S.; Moreno, W. Artificial Neural Network for Drug Design, Delivery and Disposition; Academic Press: Cambridge, MA, USA, 2015. [Google Scholar]
- Vyas, M.; Thakur, S.; Riyaz, B.; Bansal, K.; Tomar, B.; Mishra, V. Artificial Intelligence: The Beginning of a New Era in Pharmacy Profession. Asian J. Pharm. 2018, 12, 72–76. [Google Scholar]
- Hassanzadeh, P.; Atyabi, F.; Dinarvand, R. The Significance of Artificial Intelligence in Drug Delivery System Design. Adv. Drug Deliv. Rev. 2019, 151–152, 169–190. [Google Scholar] [CrossRef]
- Chavda, V.; Bezbaruah, R.; Valu, D.; Desai, S.; Chauhan, N.; Marwadi, S.; Deka, G.; Ding, Z. Clinical Applications of “Omics” Technology as a Bioinformatic Tool. In Bioinformatics Tools for Pharmaceutical Drug Product Development; John Wiley & Sons, Ltd.: Hoboken, NJ, USA, 2023; pp. 117–145. [Google Scholar]
- Sacha, G.M.; Varona, P. Artificial Intelligence in Nanotechnology. Nanotechnology 2013, 24, 452002. [Google Scholar] [CrossRef]
- Wong, W.; Chee, E.; Li, J.; Wang, X. Recurrent Neural Network-Based Model Predictive Control for Continuous Pharmaceutical Manufacturing. Mathematics 2018, 6, 242. [Google Scholar] [CrossRef]
- Wise, J.; Möller, A.; Christie, D.; Kalra, D.; Brodsky, E.; Georgieva, E.; Jones, G.; Smith, I.; Greiffenberg, L.; McCarthy, M.; et al. The Positive Impacts of Real-World Data on the Challenges Facing the Evolution of Biopharma. Drug Discov. Today 2018, 23, 788–801. [Google Scholar] [CrossRef]
- Taylor, D.; Bowden, S.G.; Knorr, R.; Wilson, D.R.; Proudfoot, J.; Dunlop, A.E. The Pistoia Alliance Controlled Substance Compliance Service Project: From Start to Finish. Drug Discov. Today 2015, 20, 175–180. [Google Scholar] [CrossRef] [PubMed]
- Lee, C.K.H.; Choy, K.L.; Chan, Y.N. A Knowledge-Based Ingredient Formulation System for Chemical Product Development in the Personal Care Industry. Comput. Chem. Eng. 2014, 65, 40–53. [Google Scholar] [CrossRef]
- Schmidhuber, J. Deep Learning in Neural Networks: An Overview. Neural Netw. 2015, 61, 85–117. [Google Scholar] [CrossRef] [PubMed]
- When Virtual Screening Yields Inactive Drugs: Dealing with False Theoretical Friends—Cerón-Carrasco—2022—ChemMedChem—Wiley Online Library. Available online: https://chemistry-europe.onlinelibrary.wiley.com/doi/full/10.1002/cmdc.202200278 (accessed on 27 June 2023).
- Roboticsbiz. Ai-in-Drug-Discovery-Benefits-Drawback-and-Challenges. Available online: https://roboticsbiz.com/ai-in-drug-discovery-benefits-drawback-and-challenges/ (accessed on 5 May 2023).
- Sarker, I.H. Machine Learning: Algorithms, Real-World Applications and Research Directions. SN Comput. Sci. 2021, 2, 160. [Google Scholar] [CrossRef]
- Sarker, I.H. AI-Based Modeling: Techniques, Applications and Research Issues Towards Automation, Intelligent and Smart Systems. SN Comput. Sci. 2022, 3, 158. [Google Scholar] [CrossRef]
- Dara, S.; Dhamercherla, S.; Jadav, S.S.; Babu, C.M.; Ahsan, M.J. Machine Learning in Drug Discovery: A Review. Artif. Intell. Rev. 2022, 55, 1947–1999. [Google Scholar] [CrossRef]
- Kavasidis, I.; Lallas, E.; Gerogiannis, V.C.; Charitou, T.; Karageorgos, A. Predictive Maintenance in Pharmaceutical Manufacturing Lines Using Deep Transformers. Procedia Comput. Sci. 2023, 220, 576–583. [Google Scholar] [CrossRef]
- Bagherian, M.; Sabeti, E.; Wang, K.; Sartor, M.A.; Nikolovska-Coleska, Z.; Najarian, K. Machine Learning Approaches and Databases for Prediction of Drug–Target Interaction: A Survey Paper. Brief. Bioinform. 2021, 22, 247–269. [Google Scholar] [CrossRef]
- Kumar, Y.; Koul, A.; Singla, R.; Ijaz, M.F. Artificial Intelligence in Disease Diagnosis: A Systematic Literature Review, Synthesizing Framework and Future Research Agenda. J. Ambient. Intell. Humaniz. Comput. 2023, 14, 8459–8486. [Google Scholar] [CrossRef]
- Chapman, A.B.; Peterson, K.S.; Alba, P.R.; DuVall, S.L.; Patterson, O.V. Detecting Adverse Drug Events with Rapidly Trained Classification Models. Drug Saf. 2019, 42, 147–156. [Google Scholar] [CrossRef]
- Elkin, M.E.; Zhu, X. Predictive Modeling of Clinical Trial Terminations Using Feature Engineering and Embedding Learning. Sci. Rep. 2021, 11, 3446. [Google Scholar] [CrossRef]
- Chavda, V.P.; Sorathiya, A.; Valu, D.; Marwadi, S. Role of Data Mining in Bioinformatics. In Computation in BioInformatics: Multidisciplinary Applications; John Wiley & Sons: Hoboken, NJ, USA, 2021; pp. 69–84. [Google Scholar] [CrossRef]
- Parikh, S.; Patel, R.; Khunt, D.; Chavda, V.P.; Vora, L. Data Analytics and Data Visualization for the Pharmaceutical Industry. In Bioinformatics Tools for Pharmaceutical Drug Product Development; John Wiley & Sons, Ltd.: Hoboken, NJ, USA, 2023; pp. 55–76. ISBN 978-1-119-86572-8. [Google Scholar]
- Karim, M.R.; Beyan, O.; Zappa, A.; Costa, I.G.; Rebholz-Schuhmann, D.; Cochez, M.; Decker, S. Deep Learning-Based Clustering Approaches for Bioinformatics. Brief. Bioinform. 2021, 22, 393–415. [Google Scholar] [CrossRef]
- Vamathevan, J.; Clark, D.; Czodrowski, P.; Dunham, I.; Ferran, E.; Lee, G.; Li, B.; Madabhushi, A.; Shah, P.; Spitzer, M.; et al. Applications of Machine Learning in Drug Discovery and Development. Nat. Rev. Drug Discov. 2019, 18, 463–477. [Google Scholar] [CrossRef] [PubMed]
- Goldstein, M.; Uchida, S. A Comparative Evaluation of Unsupervised Anomaly Detection Algorithms for Multivariate Data. PLoS ONE 2016, 11, e0152173. [Google Scholar] [CrossRef] [PubMed]
- Noguchi, Y.; Ueno, A.; Otsubo, M.; Katsuno, H.; Sugita, I.; Kanematsu, Y.; Yoshida, A.; Esaki, H.; Tachi, T.; Teramachi, H. A New Search Method Using Association Rule Mining for Drug-Drug Interaction Based on Spontaneous Report System. Front. Pharmacol. 2018, 9, 197. [Google Scholar] [CrossRef] [PubMed]
- Liu, L.; Tang, L.; Dong, W.; Yao, S.; Zhou, W. An Overview of Topic Modeling and Its Current Applications in Bioinformatics. SpringerPlus 2016, 5, 1608. [Google Scholar] [CrossRef]
- Zhao, W.; Chen, J.J.; Perkins, R.; Liu, Z.; Ge, W.; Ding, Y.; Zou, W. A Heuristic Approach to Determine an Appropriate Number of Topics in Topic Modeling. BMC Bioinform. 2015, 16, S8. [Google Scholar] [CrossRef] [PubMed]
- Sousa, T.; Correia, J.; Pereira, V.; Rocha, M. Generative Deep Learning for Targeted Compound Design. J. Chem. Inf. Model. 2021, 61, 5343–5361. [Google Scholar] [CrossRef] [PubMed]
- Rajalingham, R.; Piccato, A.; Jazayeri, M. Recurrent Neural Networks with Explicit Representation of Dynamic Latent Variables Can Mimic Behavioral Patterns in a Physical Inference Task. Nat. Commun. 2022, 13, 5865. [Google Scholar] [CrossRef]
- Nag, S.; Baidya, A.T.K.; Mandal, A.; Mathew, A.T.; Das, B.; Devi, B.; Kumar, R. Deep Learning Tools for Advancing Drug Discovery and Development. 3 Biotech 2022, 12, 110. [Google Scholar] [CrossRef]
- Liu, X.; Liu, C.; Huang, R.; Zhu, H.; Liu, Q.; Mitra, S.; Wang, Y. Long Short-Term Memory Recurrent Neural Network for Pharmacokinetic-Pharmacodynamic Modeling. Int. J. Clin. Pharmacol. Ther. 2021, 59, 138–146. [Google Scholar] [CrossRef]
- Turchin, A.; Masharsky, S.; Zitnik, M. Comparison of BERT Implementations for Natural Language Processing of Narrative Medical Documents. Inform. Med. Unlocked 2023, 36, 101139. [Google Scholar] [CrossRef]
- Huo, L.; Tang, Y. Multi-Objective Deep Reinforcement Learning for Personalized Dose Optimization Based on Multi-Indicator Experience Replay. Appl. Sci. 2022, 13, 325. [Google Scholar] [CrossRef]
- Olivier, A.; Shields, M.D.; Graham-Brady, L. Bayesian Neural Networks for Uncertainty Quantification in Data-Driven Materials Modeling. Comput. Methods Appl. Mech. Eng. 2021, 386, 114079. [Google Scholar] [CrossRef]
- Magris, M.; Iosifidis, A. Bayesian Learning for Neural Networks: An Algorithmic Survey. Artif. Intell. Rev. 2023. [Google Scholar] [CrossRef]
- Pham, T.-H.; Qiu, Y.; Zeng, J.; Xie, L.; Zhang, P. A Deep Learning Framework for High-Throughput Mechanism-Driven Phenotype Compound Screening and Its Application to COVID-19 Drug Repurposing. Nat. Mach. Intell. 2021, 3, 247–257. [Google Scholar] [CrossRef]
- Meyers, J.; Fabian, B.; Brown, N. De Novo Molecular Design and Generative Models. Drug Discov. Today 2021, 26, 2707–2715. [Google Scholar] [CrossRef] [PubMed]
- Khadela, A.; Popat, S.; Ajabiya, J.; Valu, D.; Savale, S.; Chavda, V.P. AI, ML and Other Bioinformatics Tools for Preclinical and Clinical Development of Drug Products. In Bioinformatics Tools for Pharmaceutical Drug Product Development; Wiley: Hoboken, NJ, USA, 2023; pp. 255–284. ISBN 978-1-119-86572-8. [Google Scholar]
- Koutroumpa, N.-M.; Papavasileiou, K.D.; Papadiamantis, A.G.; Melagraki, G.; Afantitis, A. A Systematic Review of Deep Learning Methodologies Used in the Drug Discovery Process with Emphasis on In Vivo Validation. Int. J. Mol. Sci. 2023, 24, 6573. [Google Scholar] [CrossRef]
- Tang, M.; Li, B.; Chen, H. Application of Message Passing Neural Networks for Molecular Property Prediction. Curr. Opin. Struct. Biol. 2023, 81, 102616. [Google Scholar] [CrossRef]
- Reiser, P.; Neubert, M.; Eberhard, A.; Torresi, L.; Zhou, C.; Shao, C.; Metni, H.; van Hoesel, C.; Schopmans, H.; Sommer, T.; et al. Graph Neural Networks for Materials Science and Chemistry. Commun. Mater. 2022, 3, 93. [Google Scholar] [CrossRef]
- Shah, H.; Chavda, V.; Soniwala, M.M. Applications of Bioinformatics Tools in Medicinal Biology and Biotechnology. In Bioinformatics Tools for Pharmaceutical Drug Product Development; Wiley: Hoboken, NJ, USA, 2023; pp. 95–116. ISBN 978-1-119-86572-8. [Google Scholar]
- Jenkins, J.L.; Bender, A.; Davies, J.W. In Silico Target Fishing: Predicting Biological Targets from Chemical Structure. Drug Discov. Today Technol. 2006, 3, 413–421. [Google Scholar] [CrossRef]
- Afzal, A.M.; Mussa, H.Y.; Turner, R.E.; Bender, A.; Glen, R.C. A Multi-Label Approach to Target Prediction Taking Ligand Promiscuity into Account. J. Cheminform. 2015, 7, 24. [Google Scholar] [CrossRef] [PubMed]
- Wang, L.; Xie, X.-Q. Computational Target Fishing: What Should Chemogenomics Researchers Expect for the Future of in Silico Drug Design and Discovery? Future Med. Chem. 2014, 6, 247–249. [Google Scholar] [CrossRef] [PubMed]
- Iorio, F.; Bosotti, R.; Scacheri, E.; Belcastro, V.; Mithbaokar, P.; Ferriero, R.; Murino, L.; Tagliaferri, R.; Brunetti-Pierri, N.; Isacchi, A.; et al. Discovery of Drug Mode of Action and Drug Repositioning from Transcriptional Responses. Proc. Natl. Acad. Sci. USA 2010, 107, 14621–14626. [Google Scholar] [CrossRef] [PubMed]
- Begam, B.F.; Kumar, J.S. A Study on Cheminformatics and Its Applications on Modern Drug Discovery. Procedia Eng. 2012, 38, 1264–1275. [Google Scholar] [CrossRef]
- Lomenick, B.; Olsen, R.W.; Huang, J. Identification of Direct Protein Targets of Small Molecules. ACS Chem. Biol. 2011, 6, 34–46. [Google Scholar] [CrossRef]
- Pushpakom, S.; Iorio, F.; Eyers, P.A.; Escott, K.J.; Hopper, S.; Wells, A.; Doig, A.; Guilliams, T.; Latimer, J.; McNamee, C.; et al. Drug Repurposing: Progress, Challenges and Recommendations. Nat. Rev. Drug Discov. 2019, 18, 41–58. [Google Scholar] [CrossRef]
- Nettles, J.H.; Jenkins, J.L.; Bender, A.; Deng, Z.; Davies, J.W.; Glick, M. Bridging Chemical and Biological Space: “Target Fishing” Using 2D and 3D Molecular Descriptors. J. Med. Chem. 2006, 49, 6802–6810. [Google Scholar] [CrossRef]
- Galati, S.; Di Stefano, M.; Martinelli, E.; Poli, G.; Tuccinardi, T. Recent Advances in In Silico Target Fishing. Molecules 2021, 26, 5124. [Google Scholar] [CrossRef]
- Chavda, V.P. Nanotherapeutics and Nanobiotechnology. In Applications of Targeted Nano Drugs and Delivery Systems; Elsevier: Amsterdam, The Netherlands, 2019; pp. 1–13. [Google Scholar]
- Colombo, S. Applications of Artificial Intelligence in Drug Delivery and Pharmaceutical Development. In Artificial Intelligence in Healthcare; Elsevier: Amsterdam, The Netherlands, 2020; pp. 85–116. [Google Scholar]
- Das, P.J.; Preuss, C.; Mazumder, B. Artificial Neural Network as Helping Tool for Drug Formulation and Drug Administration Strategies. In Artificial Neural Network for Drug Design, Delivery and Disposition; Elsevier: Amsterdam, The Netherlands, 2016; pp. 263–276. [Google Scholar]
- Bhhatarai, B.; Walters, W.P.; Hop, C.E.C.A.; Lanza, G.; Ekins, S. Opportunities and Challenges Using Artificial Intelligence in ADME/Tox. Nat. Mater. 2019, 18, 418–422. [Google Scholar] [CrossRef]
- Siepmann, J.; Siepmann, F. Modeling of Diffusion Controlled Drug Delivery. J. Control. Release 2012, 161, 351–362. [Google Scholar] [CrossRef]
- Yang, S.-Y.; Huang, Q.; Li, L.-L.; Ma, C.-Y.; Zhang, H.; Bai, R.; Teng, Q.-Z.; Xiang, M.-L.; Wei, Y.-Q. An Integrated Scheme for Feature Selection and Parameter Setting in the Support Vector Machine Modeling and Its Application to the Prediction of Pharmacokinetic Properties of Drugs. Artif. Intell. Med. 2009, 46, 155–163. [Google Scholar] [CrossRef]
- Yu, L.X.; Ellison, C.D.; Hussain, A.S. Predicting Human Oral Bioavailability Using in Silico Models. In Applications of Pharmacokinetic Principles in Drug Development; Springer: Boston, MA, USA, 2004; pp. 53–74. [Google Scholar]
- Menden, M.P.; Iorio, F.; Garnett, M.; McDermott, U.; Benes, C.H.; Ballester, P.J.; Saez-Rodriguez, J. Machine Learning Prediction of Cancer Cell Sensitivity to Drugs Based on Genomic and Chemical Properties. PLoS ONE 2013, 8, e61318. [Google Scholar] [CrossRef]
- Rafienia, M.; Amiri, M.; Janmaleki, M.; Sadeghian, A. Application of artificial neural networks in controlled drug delivery systems. Appl. Artif. Intell. 2010, 24, 807–820. [Google Scholar] [CrossRef]
- Cui, P.; Wang, S. Application of Microfluidic Chip Technology in Pharmaceutical Analysis: A Review. J. Pharm. Anal. 2019, 9, 238–247. [Google Scholar] [CrossRef] [PubMed]
- Esch, E.W.; Bahinski, A.; Huh, D. Organs-on-Chips at the Frontiers of Drug Discovery. Nat. Rev. Drug Discov. 2015, 14, 248–260. [Google Scholar] [CrossRef] [PubMed]
- Kim, S.M.; Yang, Y.; Oh, S.J.; Hong, Y.; Seo, M.; Jang, M. Cancer-Derived Exosomes as a Delivery Platform of CRISPR/Cas9 Confer Cancer Cell Tropism-Dependent Targeting. J. Control. Release 2017, 266, 8–16. [Google Scholar] [CrossRef]
- Shuler, M.L. Organ-, Body- and Disease-on-a-Chip Systems. Lab. Chip 2017, 17, 2345–2346. [Google Scholar] [CrossRef]
- Balogh, G.T.; Müller, J.; Könczöl, Á. PH-Gradient PAMPA-Based in Vitro Model Assay for Drug-Induced Phospholipidosis in Early Stage of Drug Discovery. Eur. J. Pharm. Sci. 2013, 49, 81–89. [Google Scholar] [CrossRef]
- Avdeef, A.; Artursson, P.; Neuhoff, S.; Lazorova, L.; Gråsjö, J.; Tavelin, S. Caco-2 Permeability of Weakly Basic Drugs Predicted with the Double-Sink PAMPA Method. Eur. J. Pharm. Sci. 2005, 24, 333–349. [Google Scholar] [CrossRef]
- Lou, H.; Lian, B.; Hageman, M.J. Applications of Machine Learning in Solid Oral Dosage Form Development. J. Pharm. Sci. 2021, 110, 3150–3165. [Google Scholar] [CrossRef] [PubMed]
- Jiang, J.; Ma, X.; Ouyang, D.; Williams, R.O. Emerging Artificial Intelligence (AI) Technologies Used in the Development of Solid Dosage Forms. Pharmaceutics 2022, 14, 2257. [Google Scholar] [CrossRef] [PubMed]
- Han, R.; Xiong, H.; Ye, Z.; Yang, Y.; Huang, T.; Jing, Q.; Lu, J.; Pan, H.; Ren, F.; Ouyang, D. Predicting Physical Stability of Solid Dispersions by Machine Learning Techniques. J. Control. Release 2019, 311, 16–25. [Google Scholar] [CrossRef] [PubMed]
- Navya, K.; Kamaraj, R.; Bharathi, M. The Trending Role of Artificial Intelligence and Its Applications in Formulation of Solid Dosage Forms: A Review. ECS Trans. 2022, 107, 20049–20055. [Google Scholar] [CrossRef]
- Bannigan, P.; Aldeghi, M.; Bao, Z.; Häse, F.; Aspuru-Guzik, A.; Allen, C. Machine Learning Directed Drug Formulation Development. Adv. Drug Deliv. Rev. 2021, 175, 113806. [Google Scholar] [CrossRef]
- Sun, Y.; Peng, Y.; Chen, Y.; Shukla, A.J. Application of Artificial Neural Networks in the Design of Controlled Release Drug Delivery Systems. Adv. Drug Deliv. Rev. 2003, 55, 1201–1215. [Google Scholar] [CrossRef]
- Mukhamediev, R.I.; Popova, Y.; Kuchin, Y.; Zaitseva, E.; Kalimoldayev, A.; Symagulov, A.; Levashenko, V.; Abdoldina, F.; Gopejenko, V.; Yakunin, K.; et al. Review of Artificial Intelligence and Machine Learning Technologies: Classification, Restrictions, Opportunities and Challenges. Mathematics 2022, 10, 2552. [Google Scholar] [CrossRef]
- Sengupta, S.; Basak, S.; Peters, R. Particle Swarm Optimization: A Survey of Historical and Recent Developments with Hybridization Perspectives. Mach. Learn. Knowl. Extr. 2018, 1, 157–191. [Google Scholar] [CrossRef]
- Paul, D.; Sanap, G.; Shenoy, S.; Kalyane, D.; Kalia, K.; Tekade, R.K. Artificial Intelligence in Drug Discovery and Development. Drug Discov. Today 2021, 26, 80–93. [Google Scholar] [CrossRef]
- Eberle, L.G.; Sugiyama, H.; Schmidt, R. Improving Lead Time of Pharmaceutical Production Processes Using Monte Carlo Simulation. Comput. Chem. Eng. 2014, 68, 255–263. [Google Scholar] [CrossRef]
- Böhling, P.; Khinast, J.G.; Jajcevic, D.; Davies, C.; Carmody, A.; Doshi, P.; Am Ende, M.T.; Sarkar, A. Computational Fluid Dynamics-Discrete Element Method Modeling of an Industrial-Scale Wurster Coater. J. Pharm. Sci. 2019, 108, 538–550. [Google Scholar] [CrossRef]
- Song, Y.; Zhou, T.; Bai, R.; Zhang, M.; Yang, H. Review of CFD-DEM Modeling of Wet Fluidized Bed Granulation and Coating Processes. Processes 2023, 11, 382. [Google Scholar] [CrossRef]
- Mahapatra, A.P.K.; Saraswat, R.; Botre, M.; Paul, B.; Prasad, N. Application of Response Surface Methodology (RSM) in Statistical Optimization and Pharmaceutical Characterization of a Patient Compliance Effervescent Tablet Formulation of an Antiepileptic Drug Levetiracetam. Future J. Pharm. Sci. 2020, 6, 82. [Google Scholar] [CrossRef]
- Malakar, J.; Nayak, A.K.; Goswami, S. Use of Response Surface Methodology in the Formulation and Optimization of Bisoprolol Fumarate Matrix Tablets for Sustained Drug Release. ISRN Pharm. 2012, 2012, 730624. [Google Scholar] [CrossRef] [PubMed]
- Madgulkar, A.; Bhalekar, M.; Kolhe, V.; Kenjale, Y. Formulation and Optimization of Sustained Release Tablets of Venlafaxine Resinates Using Response Surface Methodology. Indian J. Pharm. Sci. 2009, 71, 387. [Google Scholar] [CrossRef] [PubMed]
- Kundu, P.; Paul, V.; Kumar, V.; Mishra, I.M. Formulation Development, Modeling and Optimization of Emulsification Process Using Evolving RSM Coupled Hybrid ANN-GA Framework. Chem. Eng. Res. Des. 2015, 104, 773–790. [Google Scholar] [CrossRef]
- Shi, G.; Lin, L.; Liu, Y.; Chen, G.; Luo, Y.; Wu, Y.; Li, H. Pharmaceutical Application of Multivariate Modelling Techniques: A Review on the Manufacturing of Tablets. RSC Adv. 2021, 11, 8323–8345. [Google Scholar] [CrossRef] [PubMed]
- Ferreira, A.P.; Tobyn, M. Multivariate Analysis in the Pharmaceutical Industry: Enabling Process Understanding and Improvement in the PAT and QbD Era. Pharm. Dev. Technol. 2015, 20, 513–527. [Google Scholar] [CrossRef]
- Ghourichay, M.P.; Kiaie, S.H.; Nokhodchi, A.; Javadzadeh, Y. Formulation and Quality Control of Orally Disintegrating Tablets (ODTs): Recent Advances and Perspectives. BioMed Res. Int. 2021, 2021, 6618934. [Google Scholar] [CrossRef]
- Jivraj, M.; Martini, L.G.; Thomson, C.M. An Overview of the Different Excipients Useful for the Direct Compression of Tablets. Pharm. Sci. Technol. Today 2000, 3, 58–63. [Google Scholar] [CrossRef]
- Galata, D.L.; Könyves, Z.; Nagy, B.; Novák, M.; Mészáros, L.A.; Szabó, E.; Farkas, A.; Marosi, G.; Nagy, Z.K. Real-Time Release Testing of Dissolution Based on Surrogate Models Developed by Machine Learning Algorithms Using NIR Spectra, Compression Force and Particle Size Distribution as Input Data. Int. J. Pharm. 2021, 597, 120338. [Google Scholar] [CrossRef] [PubMed]
- Petrović, J.; Ibrić, S.; Betz, G.; Đurić, Z. Optimization of Matrix Tablets Controlled Drug Release Using Elman Dynamic Neural Networks and Decision Trees. Int. J. Pharm. 2012, 428, 57–67. [Google Scholar] [CrossRef]
- Han, R.; Yang, Y.; Li, X.; Ouyang, D. Predicting Oral Disintegrating Tablet Formulations by Neural Network Techniques. Asian J. Pharm. Sci. 2018, 13, 336–342. [Google Scholar] [CrossRef] [PubMed]
- Obeid, S.; Madžarević, M.; Krkobabić, M.; Ibrić, S. Predicting Drug Release from Diazepam FDM Printed Tablets Using Deep Learning Approach: Influence of Process Parameters and Tablet Surface/Volume Ratio. Int. J. Pharm. 2021, 601, 120507. [Google Scholar] [CrossRef] [PubMed]
- Alhijjaj, M.; Nasereddin, J.; Belton, P.; Qi, S. Impact of Processing Parameters on the Quality of Pharmaceutical Solid Dosage Forms Produced by Fused Deposition Modeling (FDM). Pharmaceutics 2019, 11, 633. [Google Scholar] [CrossRef]
- Muñiz Castro, B.; Elbadawi, M.; Ong, J.J.; Pollard, T.; Song, Z.; Gaisford, S.; Pérez, G.; Basit, A.W.; Cabalar, P.; Goyanes, A. Machine Learning Predicts 3D Printing Performance of over 900 Drug Delivery Systems. J. Control. Release 2021, 337, 530–545. [Google Scholar] [CrossRef]
- Vaz, V.M.; Kumar, L. 3D Printing as a Promising Tool in Personalized Medicine. AAPS PharmSciTech 2021, 22, 49. [Google Scholar] [CrossRef]
- Ma, X.; Kittikunakorn, N.; Sorman, B.; Xi, H.; Chen, A.; Marsh, M.; Mongeau, A.; Piché, N.; Williams, R.O.; Skomski, D. Application of Deep Learning Convolutional Neural Networks for Internal Tablet Defect Detection: High Accuracy, Throughput, and Adaptability. J. Pharm. Sci. 2020, 109, 1547–1557. [Google Scholar] [CrossRef]
- Yost, E.; Chalus, P.; Zhang, S.; Peter, S.; Narang, A.S. Quantitative X-Ray Microcomputed Tomography Assessment of Internal Tablet Defects. J. Pharm. Sci. 2019, 108, 1818–1830. [Google Scholar] [CrossRef]
- Khanam, J.J.; Foo, S.Y. A Comparison of Machine Learning Algorithms for Diabetes Prediction. ICT Express 2021, 7, 432–439. [Google Scholar] [CrossRef]
- Bhattamisra, S.K.; Banerjee, P.; Gupta, P.; Mayuren, J.; Patra, S.; Candasamy, M. Artificial Intelligence in Pharmaceutical and Healthcare Research. Big Data Cogn. Comput. 2023, 7, 10. [Google Scholar] [CrossRef]
- Wang, N.; Sun, H.; Dong, J.; Ouyang, D. PharmDE: A New Expert System for Drug-Excipient Compatibility Evaluation. Int. J. Pharm. 2021, 607, 120962. [Google Scholar] [CrossRef] [PubMed]
- Sun, D.D.; Lee, P.I. Evolution of Supersaturation of Amorphous Pharmaceuticals: The Effect of Rate of Supersaturation Generation. Mol. Pharm. 2013, 10, 4330–4346. [Google Scholar] [CrossRef]
- Gao, H.; Su, Y.; Wang, W.; Xiong, W.; Sun, X.; Ji, Y.; Yu, H.; Li, H.; Ouyang, D. Integrated Computer-Aided Formulation Design: A Case Study of Andrographolide/Cyclodextrin Ternary Formulation. Asian J. Pharm. Sci. 2021, 16, 494–507. [Google Scholar] [CrossRef] [PubMed]
- Dong, J.; Gao, H.; Ouyang, D. PharmSD: A Novel AI-Based Computational Platform for Solid Dispersion Formulation Design. Int. J. Pharm. 2021, 604, 120705. [Google Scholar] [CrossRef]
- Chavda, V.; Anand, K.; Apostolopoulos, V. Bioinformatics Tools for Pharmaceutical Drug Product Development; John Wiley & Sons: Hoboken, NJ, USA, 2023. [Google Scholar]
- Zarrinpar, A.; Lee, D.-K.; Silva, A.; Datta, N.; Kee, T.; Eriksen, C.; Weigle, K.; Agopian, V.; Kaldas, F.; Farmer, D.; et al. Individualizing Liver Transplant Immunosuppression Using a Phenotypic Personalized Medicine Platform. Sci. Transl. Med. 2016, 8, 333. [Google Scholar] [CrossRef]
- Ho, D.; Wang, P.; Kee, T. Artificial Intelligence in Nanomedicine. Nanoscale Horiz. 2019, 4, 365–377. [Google Scholar] [CrossRef]
- Das, K.P.; Chandra, J. Nanoparticles and Convergence of Artificial Intelligence for Targeted Drug Delivery for Cancer Therapy: Current Progress and Challenges. Front. Med. Technol. 2023, 4, 1067144. [Google Scholar] [CrossRef]
- Villa Nova, M.; Lin, T.P.; Shanehsazzadeh, S.; Jain, K.; Ng, S.C.Y.; Wacker, R.; Chichakly, K.; Wacker, M.G. Nanomedicine Ex Machina: Between Model-Informed Development and Artificial Intelligence. Front. Digit. Health 2022, 4, 799341. [Google Scholar] [CrossRef]
- Alshawwa, S.Z.; Kassem, A.A.; Farid, R.M.; Mostafa, S.K.; Labib, G.S. Nanocarrier Drug Delivery Systems: Characterization, Limitations, Future Perspectives and Implementation of Artificial Intelligence. Pharmaceutics 2022, 14, 883. [Google Scholar] [CrossRef]
- Thota, N.; Jiang, J. Computational Amphiphilic Materials for Drug Delivery. Front. Mater. 2015, 2, 64. [Google Scholar] [CrossRef]
- Huynh, L.; Neale, C.; Pomès, R.; Allen, C. Computational Approaches to the Rational Design of Nanoemulsions, Polymeric Micelles, and Dendrimers for Drug Delivery. Nanomed. Nanotechnol. Biol. Med. 2012, 8, 20–36. [Google Scholar] [CrossRef]
- He, Y.; Ye, Z.; Liu, X.; Wei, Z.; Qiu, F.; Li, H.-F.; Zheng, Y.; Ouyang, D. Can Machine Learning Predict Drug Nanocrystals? J. Control. Release 2020, 322, 274–285. [Google Scholar] [CrossRef] [PubMed]
- Egorov, E.; Pieters, C.; Korach-Rechtman, H.; Shklover, J.; Schroeder, A. Robotics, Microfluidics, Nanotechnology and AI in the Synthesis and Evaluation of Liposomes and Polymeric Drug Delivery Systems. Drug Deliv. Transl. Res. 2021, 11, 345–352. [Google Scholar] [CrossRef]
- Duarte, Y.; Márquez-Miranda, V.; Miossec, M.J.; González-Nilo, F. Integration of Target Discovery, Drug Discovery and Drug Delivery: A Review on Computational Strategies. WIREs Nanomed. Nanobiotechnol. 2019, 11, e1554. [Google Scholar] [CrossRef]
- Gonzalez-Ibanez, A.M.; Gonzalez-Nilo, F.; Cachau, R. The Collaboratory for Structural Nanobiology. Biophys. J. 2009, 96, 49a. [Google Scholar] [CrossRef]
- Nuhn, L. Artificial Intelligence Assists Nanoparticles to Enter Solid Tumours. Nat. Nanotechnol. 2023, 18, 550–551. [Google Scholar] [CrossRef]
- Lin, Z.; Chou, W.-C.; Cheng, Y.-H.; He, C.; Monteiro-Riviere, N.A.; Riviere, J.E. Predicting Nanoparticle Delivery to Tumors Using Machine Learning and Artificial Intelligence Approaches. Int. J. Nanomed. 2022, 17, 1365–1379. [Google Scholar] [CrossRef] [PubMed]
- Mohan, B.; Kamaraj, R.; Navyaja, K. Role of Artificial Intelligence in Parenteral Formulation: A Review. ECS Trans. 2022, 107, 20013–20020. [Google Scholar] [CrossRef]
- Pokhriyal, P.; Chavda, V.P.; Pathak, M. Future Prospects and Challenges in the Implementation of AI and ML in Pharma Sector. In Bioinformatics Tools for Pharmaceutical Drug Product Development; Wiley: Hoboken, NJ, USA, 2023; pp. 401–416. ISBN 978-1-119-86572-8. [Google Scholar]
- Wilco Image Processing Wilco Image Processing. Available online: https://www.wilco.com/technologies/image-processing/ (accessed on 5 May 2023).
- Bannigan, P.; Bao, Z.; Hickman, R.J.; Aldeghi, M.; Häse, F.; Aspuru-Guzik, A.; Allen, C. Machine Learning Models to Accelerate the Design of Polymeric Long-Acting Injectables. Nat. Commun. 2023, 14, 35. [Google Scholar] [CrossRef]
- Magill, E.; Demartis, S.; Gavini, E.; Dian Permana, A.; Raj Singh Thakur, R.; Faris Adrianto, M.; Waite, D.; Glover, K.; Picco, C.J.; Korelidou, A.; et al. Solid Implantable Devices for Sustained Drug Delivery. Adv. Drug Deliv. Rev. 2023, 199, 114950. [Google Scholar] [CrossRef] [PubMed]
- Wang, N.; Zhang, Y.; Wang, W.; Ye, Z.; Chen, H.; Hu, G.; Ouyang, D. How Can Machine Learning and Multiscale Modeling Benefit Ocular Drug Development? Adv. Drug Deliv. Rev. 2023, 196, 114772. [Google Scholar] [CrossRef] [PubMed]
- Vora, L.K.; Moffatt, K.; Tekko, I.A.; Paredes, A.J.; Volpe-Zanutto, F.; Mishra, D.; Peng, K.; Raj Singh Thakur, R.; Donnelly, R.F. Microneedle Array Systems for Long-Acting Drug Delivery. Eur. J. Pharm. Biopharm. 2021, 159, 44–76. [Google Scholar] [CrossRef]
- Wu, Y.; Vora, L.K.; Mishra, D.; Adrianto, M.F.; Gade, S.; Paredes, A.J.; Donnelly, R.F.; Singh, T.R.R. Nanosuspension-Loaded Dissolving Bilayer Microneedles for Hydrophobic Drug Delivery to the Posterior Segment of the Eye. Biomater. Adv. 2022, 137, 212767. [Google Scholar] [CrossRef] [PubMed]
- Bagde, A.; Dev, S.; Madhavi, K.; Sriram, L.; Spencer, S.D.; Kalvala, A.; Nathani, A.; Salau, O.; Mosley-Kellum, K.; Dalvaigari, H.; et al. Biphasic Burst and Sustained Transdermal Delivery in Vivo Using an AI-Optimized 3D-Printed MN Patch. Int. J. Pharm. 2023, 636, 122647. [Google Scholar] [CrossRef]
- Chavda, V.P.; Vora, L.K.; Pandya, A.K.; Patravale, V.B. Intranasal Vaccines for SARS-CoV-2: From Challenges to Potential in COVID-19 Management. Drug Discov. Today 2021, 26, 2619–2636. [Google Scholar] [CrossRef]
- Chavda, V.P.; Pandya, R.; Apostolopoulos, V. DNA Vaccines for SARS-CoV-2: Toward Third-Generation Vaccination Era. Expert Rev. Vaccines 2021, 20, 1549–1560. [Google Scholar] [CrossRef]
- Chavda, V.P.; Prajapati, R.; Lathigara, D.; Nagar, B.; Kukadiya, J.; Redwan, E.M.; Uversky, V.N.; Kher, M.N.; Patel, R. Therapeutic Monoclonal Antibodies for COVID-19 Management: An Update. Expert Opin. Biol. Ther. 2022, 22, 763–780. [Google Scholar] [CrossRef]
- Chavda, V.P.; Soni, S.; Vora, L.K.; Soni, S.; Khadela, A.; Ajabiya, J. MRNA-Based Vaccines and Therapeutics for COVID-19 and Future Pandemics. Vaccines 2022, 10, 2150. [Google Scholar] [CrossRef]
- Chavda, V.P.; Dawre, S.; Pandya, A.; Vora, L.K.; Modh, D.H.; Shah, V.; Dave, D.J.; Patravale, V. Lyotropic Liquid Crystals for Parenteral Drug Delivery. J. Control. Release 2022, 349, 533–549. [Google Scholar] [CrossRef]
- Chavda, V.P.; Pandya, A.; Kumar, L.; Raval, N.; Vora, L.K.; Pulakkat, S.; Patravale, V.; Salwa, D.Y.; Tang, B.Z. Exosome Nanovesicles: A Potential Carrier for Therapeutic Delivery. Nano Today 2023, 49, 101771. [Google Scholar] [CrossRef]
- Huang, Z.; Chavda, V.P.; Bezbaruah, R.; Uversky, V.N.; Palagati, S.; Patel, A.B.; Chen, Z.-S. An Ayurgenomics Approach: Prakriti-Based Drug Discovery and Development for Personalized Care. Front. Pharmacol. 2022, 13, 866827. [Google Scholar] [CrossRef] [PubMed]
- Chavda, V.P.; Balar, P.C.; Teli, D.; Davidson, M.; Bojarska, J.; Apostolopoulos, V. Antibody–Biopolymer Conjugates in Oncology: A Review. Molecules 2023, 28, 2605. [Google Scholar] [CrossRef] [PubMed]
- Chavda, V.P.; Bezbaruah, R.; Dolia, S.; Shah, N.; Verma, S.; Savale, S.; Ray, S. Convalescent Plasma (Hyperimmune Immunoglobulin) for COVID-19 Management: An Update. Process Biochem. 2023, 127, 66–81. [Google Scholar] [CrossRef] [PubMed]
- Kabra, R.; Singh, S. Evolutionary Artificial Intelligence Based Peptide Discoveries for Effective COVID-19 Therapeutics. Biochim. Biophys. Acta BBA Mol. Basis Dis. 2021, 1867, 165978. [Google Scholar] [CrossRef]
- Akbar, R.; Bashour, H.; Rawat, P.; Robert, P.A.; Smorodina, E.; Cotet, T.-S.; Flem-Karlsen, K.; Frank, R.; Mehta, B.B.; Vu, M.H.; et al. Progress and Challenges for the Machine Learning-Based Design of Fit-for-Purpose Monoclonal Antibodies. mAbs 2022, 14, 2008790. [Google Scholar] [CrossRef]
- Sharma, A.; Virmani, T.; Pathak, V.; Sharma, A.; Pathak, K.; Kumar, G.; Pathak, D. Artificial Intelligence-Based Data-Driven Strategy to Accelerate Research, Development, and Clinical Trials of COVID Vaccine. BioMed Res. Int. 2022, 2022, 7205241. [Google Scholar] [CrossRef]
- Dhakal, A.; McKay, C.; Tanner, J.J.; Cheng, J. Artificial Intelligence in the Prediction of Protein–Ligand Interactions: Recent Advances and Future Directions. Brief. Bioinform. 2022, 23, bbab476. [Google Scholar] [CrossRef]
- Vishnoi, S.; Matre, H.; Garg, P.; Pandey, S.K. Artificial Intelligence and Machine Learning for Protein Toxicity Prediction Using Proteomics Data. Chem. Biol. Drug Des. 2020, 96, 902–920. [Google Scholar] [CrossRef]
- Huang, Z.; Chavda, V.P.; Bezbaruah, R.; Dhamne, H.; Yang, D.-H.; Zhao, H.-B. CAR T-Cell Therapy for the Management of Mantle Cell Lymphoma. Mol. Cancer 2023, 22, 67. [Google Scholar] [CrossRef]
- Chavda, V.P.; Sugandhi, V.V.; Pardeshi, C.V.; Patil, R.J.; Joshi, M.; Patel, B.; Khadela, A.; Bezbaruah, R.; Bhattacharjee, B.; Balar, P.C.; et al. Engineered Exosomes for Cancer Theranostics: Next-Generation Tumor Targeting. J. Drug Deliv. Sci. Technol. 2023, 85, 104579. [Google Scholar] [CrossRef]
- Pinjala, P.; Tryphena, K.P.; Prasad, R.; Khatri, D.K.; Sun, W.; Singh, S.B.; Gugulothu, D.; Srivastava, S.; Vora, L. CRISPR/Cas9 Assisted Stem Cell Therapy in Parkinson’s Disease. Biomater. Res. 2023, 27, 46. [Google Scholar] [CrossRef] [PubMed]
- Sahel, D.K.; Vora, L.K.; Saraswat, A.; Sharma, S.; Monpara, J.; D’Souza, A.A.; Mishra, D.; Tryphena, K.P.; Kawakita, S.; Khan, S.; et al. CRISPR/Cas9 Genome Editing for Tissue-Specific In Vivo Targeting: Nanomaterials and Translational Perspective. Adv. Sci. 2023, 2207512. [Google Scholar] [CrossRef]
- Bezbaruah, R.; Ghosh, M.; Kumari, S.; Nongrang, L.; Ali, S.R.; Lahiri, M.; Waris, H.; Kakoti, B.B. Role of AI and ML in Epidemics and Pandemics. In Bioinformatics Tools for Pharmaceutical Drug Product Development; Wiley: Hoboken, NJ, USA, 2023; pp. 345–369. ISBN 978-1-119-86572-8. [Google Scholar]
- Koh, D.-M.; Papanikolaou, N.; Bick, U.; Illing, R.; Kahn, C.E.; Kalpathi-Cramer, J.; Matos, C.; Martí-Bonmatí, L.; Miles, A.; Mun, S.K.; et al. Artificial Intelligence and Machine Learning in Cancer Imaging. Commun. Med. 2022, 2, 133. [Google Scholar] [CrossRef]
- Malche, T.; Tharewal, S.; Tiwari, P.K.; Jabarulla, M.Y.; Alnuaim, A.A.; Hatamleh, W.A.; Ullah, M.A. Artificial Intelligence of Things- (AIoT-) Based Patient Activity Tracking System for Remote Patient Monitoring. J. Healthc. Eng. 2022, 2022, 8732213. [Google Scholar] [CrossRef] [PubMed]
- Verma, D.; Singh, K.R.; Yadav, A.K.; Nayak, V.; Singh, J.; Solanki, P.R.; Singh, R.P. Internet of Things (IoT) in Nano-Integrated Wearable Biosensor Devices for Healthcare Applications. Biosens. Bioelectron. X 2022, 11, 100153. [Google Scholar] [CrossRef]
- Nayak, S.; Kumar Das, R. Application of Artificial Intelligence (AI) in Prosthetic and Orthotic Rehabilitation. In Service Robotics; IntechOpen: London, UK, 2020. [Google Scholar]
- Bodenstedt, S.; Wagner, M.; Müller-Stich, B.P.; Weitz, J.; Speidel, S. Artificial Intelligence-Assisted Surgery: Potential and Challenges. Visc. Med. 2020, 36, 450–455. [Google Scholar] [CrossRef]
- Babel, A.; Taneja, R.; Mondello Malvestiti, F.; Monaco, A.; Donde, S. Artificial Intelligence Solutions to Increase Medication Adherence in Patients With Non-Communicable Diseases. Front. Digit. Health 2021, 3, 669869. [Google Scholar] [CrossRef]
- Insights/Artificial-Intelligence-in-Medical-Devices, K. Kantify Insights/Artificial-Intelligence-in-Medical-Devices. Available online: https://www.kantify.com/insights/artificial-intelligence-in-medical-devices (accessed on 5 May 2023).
- Devices, A.-I.-M. Artificial-Intelligence-Medical Devices. Available online: https://www.medicaldevice-network.com/comment/artificial-intelligence-medical/ (accessed on 5 May 2023).
- Ai-Medical-Devices-Three-Emerging-Industry-Applications, E. Emerj Ai-Medical-Devices-Three-Emerging-Industry-Applications. Available online: https://emerj.com/ai-sector-overviews/ai-medical-devices-three-emerging-industry-applications/ (accessed on 2 May 2023).
- FDA-AI-ML-Medical-Devices, M. Medtechdive FDA-AI-ML-Medical-Devices. Available online: https://www.medtechdive.com/news/FDA-AI-ML-medical-devices-5-takeaways/635908/ (accessed on 2 May 2023).
- Artificial Intelligence in Medicine. Available online: https://www.johner-institute.com/articles/software-iec-62304/and-more/artificial-intelligence/ (accessed on 2 May 2023).
- Tuntland, T.; Ethell, B.; Kosaka, T.; Blasco, F.; Zang, R.X.; Jain, M.; Gould, T.; Hoffmaster, K. Implementation of Pharmacokinetic and Pharmacodynamic Strategies in Early Research Phases of Drug Discovery and Development at Novartis Institute of Biomedical Research. Front. Pharmacol. 2014, 5, 174. [Google Scholar] [CrossRef]
- Mager, D.E.; Woo, S.; Jusko, W.J. Scaling Pharmacodynamics from In Vitro and Preclinical Animal Studies to Humans. Drug Metab. Pharmacokinet. 2009, 24, 16–24. [Google Scholar] [CrossRef]
- Alsultan, A.; Alghamdi, W.A.; Alghamdi, J.; Alharbi, A.F.; Aljutayli, A.; Albassam, A.; Almazroo, O.; Alqahtani, S. Clinical Pharmacology Applications in Clinical Drug Development and Clinical Care: A Focus on Saudi Arabia. Saudi Pharm. J. 2020, 28, 1217–1227. [Google Scholar] [CrossRef]
- Keutzer, L.; You, H.; Farnoud, A.; Nyberg, J.; Wicha, S.G.; Maher-Edwards, G.; Vlasakakis, G.; Moghaddam, G.K.; Svensson, E.M.; Menden, M.P.; et al. Machine Learning and Pharmacometrics for Prediction of Pharmacokinetic Data: Differences, Similarities and Challenges Illustrated with Rifampicin. Pharmaceutics 2022, 14, 1530. [Google Scholar] [CrossRef]
- Chavda, V.P.; Ertas, Y.N.; Walhekar, V.; Modh, D.; Doshi, A.; Shah, N.; Anand, K.; Chhabria, M. Advanced Computational Methodologies Used in the Discovery of New Natural Anticancer Compounds. Front. Pharmacol. 2021, 12, 702611. [Google Scholar] [CrossRef]
- Chaturvedula, A.; Calad-Thomson, S.; Liu, C.; Sale, M.; Gattu, N.; Goyal, N. Artificial Intelligence and Pharmacometrics: Time to Embrace, Capitalize, and Advance? CPT Pharmacomet. Syst. Pharmacol. 2019, 8, 440–443. [Google Scholar] [CrossRef] [PubMed]
- Patel, V.; Shah, M. Artificial Intelligence and Machine Learning in Drug Discovery and Development. Intell. Med. 2022, 2, 134–140. [Google Scholar] [CrossRef]
- Vatansever, S.; Schlessinger, A.; Wacker, D.; Kaniskan, H.Ü.; Jin, J.; Zhou, M.; Zhang, B. Artificial Intelligence and Machine Learning-aided Drug Discovery in Central Nervous System Diseases: State-of-the-arts and Future Directions. Med. Res. Rev. 2021, 41, 1427–1473. [Google Scholar] [CrossRef] [PubMed]
- Houy, N.; Le Grand, F. Optimal Dynamic Regimens with Artificial Intelligence: The Case of Temozolomide. PLoS ONE 2018, 13, e0199076. [Google Scholar] [CrossRef]
- Westreich, D.; Lessler, J.; Funk, M.J. Propensity Score Estimation: Neural Networks, Support Vector Machines, Decision Trees (CART), and Meta-Classifiers as Alternatives to Logistic Regression. J. Clin. Epidemiol. 2010, 63, 826–833. [Google Scholar] [CrossRef]
- Chintawar, S.; Gattani, V.; Vyas, S.; Dawre, S. Role of Artificial Intelligence in Machine Learning for Diagnosis and Radiotherapy. In Bioinformatics Tools for Pharmaceutical Drug Product Development; Wiley: Hoboken, NJ, USA, 2023; pp. 315–344. ISBN 978-1-119-86572-8. [Google Scholar]
- Suresh, A.; Udendhran, R.; Balamurgan, M. Hybridized Neural Network and Decision Tree Based Classifier for Prognostic Decision Making in Breast Cancers. Soft Comput. 2020, 24, 7947–7953. [Google Scholar] [CrossRef]
- Daoui, O.; Elkhattabi, S.; Chtita, S.; Elkhalabi, R.; Zgou, H.; Benjelloun, A.T. QSAR, Molecular Docking and ADMET Properties in Silico Studies of Novel 4,5,6,7-Tetrahydrobenzo[D]-Thiazol-2-Yl Derivatives Derived from Dimedone as Potent Anti-Tumor Agents through Inhibition of C-Met Receptor Tyrosine Kinase. Heliyon 2021, 7, e07463. [Google Scholar] [CrossRef]
- Zhuang, X.; Lu, C. PBPK Modeling and Simulation in Drug Research and Development. Acta Pharm. Sin. B 2016, 6, 430–440. [Google Scholar] [CrossRef] [PubMed]
- Healthcare Artificial Intelligence, Causal Machine Learning & Data Analytics—GNS Healthcare. Available online: https://www.aitiabio.com/new-technology/ (accessed on 5 May 2023).
- Jones, H.; Rowland-Yeo, K. Basic Concepts in Physiologically Based Pharmacokinetic Modeling in Drug Discovery and Development. CPT Pharmacomet. Syst. Pharmacol. 2013, 2, 63. [Google Scholar] [CrossRef] [PubMed]
- Obrezanova, O. Artificial Intelligence for Compound Pharmacokinetics Prediction. Curr. Opin. Struct. Biol. 2023, 79, 102546. [Google Scholar] [CrossRef] [PubMed]
- Mhatre, S.; Shukla, S.; Chavda, V.P.; Gandikota, L.; Patravale, V. AI and ML for Development of Cell and Gene Therapy for Personalized Treatment. In Bioinformatics Tools for Pharmaceutical Drug Product Development; Wiley: Hoboken, NJ, USA, 2023; pp. 371–400. ISBN 978-1-119-86572-8. [Google Scholar]
- Chou, W.-C.; Lin, Z. Machine Learning and Artificial Intelligence in Physiologically Based Pharmacokinetic Modeling. Toxicol. Sci. 2023, 191, 1–14. [Google Scholar] [CrossRef] [PubMed]
- Van Tran, T.T.; Tayara, H.; Chong, K.T. Artificial Intelligence in Drug Metabolism and Excretion Prediction: Recent Advances, Challenges, and Future Perspectives. Pharmaceutics 2023, 15, 1260. [Google Scholar] [CrossRef]
- Li, Y.; Meng, Q.; Yang, M.; Liu, D.; Hou, X.; Tang, L.; Wang, X.; Lyu, Y.; Chen, X.; Liu, K.; et al. Current Trends in Drug Metabolism and Pharmacokinetics. Acta Pharm. Sin. B 2019, 9, 1113–1144. [Google Scholar] [CrossRef]
- Parikh, P.K.; Savjani, J.K.; Gajjar, A.K.; Chhabria, M.T. Bioinformatics and Cheminformatics Tools in Early Drug Discovery. In Bioinformatics Tools for Pharmaceutical Drug Product Development; Wiley: Hoboken, NJ, USA, 2023; pp. 147–181. ISBN 978-1-119-86572-8. [Google Scholar]
- Alsmadi, M.M.; Idkaidek, N. The Analysis of Pethidine Pharmacokinetics in Newborn Saliva, Plasma, and Brain Extracellular Fluid After Prenatal Intrauterine Exposure from Pregnant Mothers Receiving Intramuscular Dose Using PBPK Modeling. Eur. J. Drug Metab. Pharmacokinet. 2023, 48, 281–300. [Google Scholar] [CrossRef]
- Zhang, Z.; Tang, W. Drug Metabolism in Drug Discovery and Development. Acta Pharm. Sin. B 2018, 8, 721–732. [Google Scholar] [CrossRef]
- Khan, S.R.; Al Rijjal, D.; Piro, A.; Wheeler, M.B. Integration of AI and Traditional Medicine in Drug Discovery. Drug Discov. Today 2021, 26, 982–992. [Google Scholar] [CrossRef]
- Selvaraj, C.; Chandra, I.; Singh, S.K. Artificial Intelligence and Machine Learning Approaches for Drug Design: Challenges and Opportunities for the Pharmaceutical Industries. Mol. Divers. 2022, 26, 1893–1913. [Google Scholar] [CrossRef]
- Zhou, H.; Hartford, A.; Tsai, K. A Bayesian Approach for PK/PD Modeling with PD Data Below Limit of Quantification. J. Biopharm. Stat. 2012, 22, 1220–1243. [Google Scholar] [CrossRef] [PubMed]
- Dansirikul, C.; Morris, R.G.; Tett, S.E.; Duffull, S.B. A Bayesian Approach for Population Pharmacokinetic Modelling of Sirolimus. Br. J. Clin. Pharmacol. 2006, 62, 420–434. [Google Scholar] [CrossRef] [PubMed]
- You, W.; Widmer, N.; De Micheli, G. Example-Based Support Vector Machine for Drug Concentration Analysis. In Proceedings of the 2011 Annual International Conference of the IEEE Engineering in Medicine and Biology Society, Boston, MA, USA, 30 August–3 September 2011; IEEE: New York, NY USA, 2011; pp. 153–157. [Google Scholar]
- You, W.; Simalatsar, A.; Widmer, N.; Micheli, G. De Personalized Drug Administrations Using Support Vector Machine. BioNanoScience 2013, 3, 378–393. [Google Scholar] [CrossRef]
- Camps-Valls, G.; Soria-Olivas, E.; Perez-Ruixo, J.J.; Artes-Rodriguez, A.; Jimenez-Torres, N.V. Therapeutic Drug Monitoring of Kidney Transplant Recipients Using Profiled Support Vector Machines. IEEE Trans. Syst. Man Cybern. Part C Appl. Rev. 2007, 37, 359–372. [Google Scholar] [CrossRef]
- Farhana, N.A.; Afendi, F.M.; Fitrianto, A.; Wijaya, S.H. Classification Modeling of Support Vector Machine (SVM) and Random Forest in Predicting Pharmacodynamics Interactions. J. Phys. Conf. Ser. 2021, 1863, 012067. [Google Scholar] [CrossRef]
- Woillard, J.-B.; Labriffe, M.; Prémaud, A.; Marquet, P. Estimation of Drug Exposure by Machine Learning Based on Simulations from Published Pharmacokinetic Models: The Example of Tacrolimus. Pharmacol. Res. 2021, 167, 105578. [Google Scholar] [CrossRef]
- Woillard, J.; Labriffe, M.; Debord, J.; Marquet, P. Tacrolimus Exposure Prediction Using Machine Learning. Clin. Pharmacol. Ther. 2021, 110, 361–369. [Google Scholar] [CrossRef]
- Ng, C.; Xiao, Y.; Putnam, W.; Lum, B.; Tropsha, A. Quantitative Structure–pharmacokinetic Parameters Relationships (QSPKR) Analysis of Antimicrobial Agents in Humans Using Simulated Annealing K-nearest-neighbor and Partial Least-square Analysis Methods**This Paper Was Presented in Part at the Annual Meeti. J. Pharm. Sci. 2004, 93, 2535–2544. [Google Scholar] [CrossRef]
- Peng, J.; Li, J.; Shang, X. A Learning-Based Method for Drug-Target Interaction Prediction Based on Feature Representation Learning and Deep Neural Network. BMC Bioinform. 2020, 21, 394. [Google Scholar] [CrossRef]
- Wang, Y.-B.; You, Z.-H.; Yang, S.; Yi, H.-C.; Chen, Z.-H.; Zheng, K. A Deep Learning-Based Method for Drug-Target Interaction Prediction Based on Long Short-Term Memory Neural Network. BMC Med. Inform. Decis. Mak. 2020, 20, 49. [Google Scholar] [CrossRef]
- Kiseleva, A.; Kotzinos, D.; De Hert, P. Transparency of AI in Healthcare as a Multilayered System of Accountabilities: Between Legal Requirements and Technical Limitations. Front. Artif. Intell. 2022, 5, 879603. [Google Scholar] [CrossRef] [PubMed]
- Kelly, C.J.; Karthikesalingam, A.; Suleyman, M.; Corrado, G.; King, D. Key Challenges for Delivering Clinical Impact with Artificial Intelligence. BMC Med. 2019, 17, 195. [Google Scholar] [CrossRef]
- Norori, N.; Hu, Q.; Aellen, F.M.; Faraci, F.D.; Tzovara, A. Addressing Bias in Big Data and AI for Health Care: A Call for Open Science. Patterns 2021, 2, 100347. [Google Scholar] [CrossRef]
- Manyika, J.; Silberg, J.; Presten, B. What Do We Do About the Biases in AI? Available online: https://hbr.org/2019/10/what-do-we-do-about-the-biases-in-ai (accessed on 5 May 2023).
- Sarmadi, A.; Hassanzadeganroudsari, M.; Soltani, M. Artificial Intelligence and Machine Learning Applications in Vaccine Development. In Bioinformatics Tools for Pharmaceutical Drug Product Development; Wiley: Hoboken, NJ, USA, 2023; pp. 233–253. ISBN 978-1-119-86572-8. [Google Scholar]
- Johnson, K.B.; Wei, W.; Weeraratne, D.; Frisse, M.E.; Misulis, K.; Rhee, K.; Zhao, J.; Snowdon, J.L. Precision Medicine, AI, and the Future of Personalized Health Care. Clin. Transl. Sci. 2021, 14, 86–93. [Google Scholar] [CrossRef] [PubMed]
- Ahmed, Z.; Mohamed, K.; Zeeshan, S.; Dong, X. Artificial Intelligence with Multi-Functional Machine Learning Platform Development for Better Healthcare and Precision Medicine. Database 2020, 2020, baaa010. [Google Scholar] [CrossRef]
- Gerke, S.; Minssen, T.; Cohen, G. Ethical and Legal Challenges of Artificial Intelligence-Driven Healthcare. In Artificial Intelligence in Healthcare; Elsevier: Amsterdam, The Netherlands, 2020; pp. 295–336. [Google Scholar]
- Naik, N.; Hameed, B.M.Z.; Shetty, D.K.; Swain, D.; Shah, M.; Paul, R.; Aggarwal, K.; Ibrahim, S.; Patil, V.; Smriti, K.; et al. Legal and Ethical Consideration in Artificial Intelligence in Healthcare: Who Takes Responsibility? Front. Surg. 2022, 9, 266. [Google Scholar] [CrossRef] [PubMed]
- FDA. Using Artificial Intelligence & Machine Learning in the Development of Drug and Biological Products; Food and Drug Administration: Silver Spring, MD, USA, 2023. [Google Scholar]
- Eslami, M.; Adler, A.; Caceres, R.S.; Dunn, J.G.; Kelley-Loughnane, N.; Varaljay, V.A.; Martin, H.G. Artificial Intelligence for Synthetic Biology. Available online: https://cacm.acm.org/magazines/2022/5/260341-artificial-intelligence-for-synthetic-biology/fulltext (accessed on 10 May 2023).
- Uddin, M.; Wang, Y.; Woodbury-Smith, M. Artificial Intelligence for Precision Medicine in Neurodevelopmental Disorders. NPJ Digit. Med. 2019, 2, 112. [Google Scholar] [CrossRef]
- Quazi, S. Artificial Intelligence and Machine Learning in Precision and Genomic Medicine. Med. Oncol. 2022, 39, 120. [Google Scholar] [CrossRef]
- Davenport, T.; Kalakota, R. The Potential for Artificial Intelligence in Healthcare. Future Healthc. J. 2019, 6, 94–98. [Google Scholar] [CrossRef]
- Lexa, K.W.; Carlson, H.A. Protein Flexibility in Docking and Surface Mapping. Q. Rev. Biophys. 2012, 45, 301–343. [Google Scholar] [CrossRef]
- Volkamer, A.; Riniker, S.; Nittinger, E.; Lanini, J.; Grisoni, F.; Evertsson, E.; Rodríguez-Pérez, R.; Schneider, N. Machine Learning for Small Molecule Drug Discovery in Academia and Industry. Artif. Intell. Life Sci. 2023, 3, 100056. [Google Scholar] [CrossRef]
- Schneider, P.; Walters, W.P.; Plowright, A.T.; Sieroka, N.; Listgarten, J.; Goodnow, R.A.; Fisher, J.; Jansen, J.M.; Duca, J.S.; Rush, T.S.; et al. Rethinking Drug Design in the Artificial Intelligence Era. Nat. Rev. Drug Discov. 2020, 19, 353–364. [Google Scholar] [CrossRef] [PubMed]
- Chavda, V.P.; Patel, K.; Patel, S.; Apostolopoulos, V. Artificial Intelligence and Machine Learning in Healthcare Sector. In Bioinformatics Tools for Pharmaceutical Drug Product Development; Wiley: Hoboken, NJ, USA, 2023; pp. 285–314. ISBN 978-1-119-86572-8. [Google Scholar]
- Astrazeneca Data Science & Artificial Intelligence: Unlocking New Science Insights. Available online: https://www.astrazeneca.com/r-d/data-science-and-ai.html (accessed on 5 May 2023).
- Stafford, K.A.; Anderson, B.M.; Sorenson, J.; van den Bedem, H. AtomNet PoseRanker: Enriching Ligand Pose Quality for Dynamic Proteins in Virtual High-Throughput Screens. J. Chem. Inf. Model. 2022, 62, 1178–1189. [Google Scholar] [CrossRef] [PubMed]
- Buntz, B. Prominent Firms Harnessing AI in Drug Discovery and Development. Drug Discov. Trends 2023, in press. [Google Scholar]
- Pfizer Artificial Intelligence: On a Mission to Make Clinical Drug Development Faster and Smarter. 2023; in press.
- Roche Personalised Healthcare. Available online: https://www.roche.com/about/strategy/personalised-healthcare (accessed on 5 May 2023).
- Chavda, V.P.; Patel, Z.; Parmar, Y.; Chavda, D. In Silico Protein Design and Virtual Screening. In Computation in BioInformatics: Multidisciplinary Applications; John Wiley & Sons: Hoboken, NJ, USA, 2021; pp. 85–99. [Google Scholar] [CrossRef]
- Levin, S.; Toerper, M.; Hamrock, E.; Hinson, J.S.; Barnes, S.; Gardner, H.; Dugas, A.; Linton, B.; Kirsch, T.; Kelen, G. Machine-Learning-Based Electronic Triage More Accurately Differentiates Patients With Respect to Clinical Outcomes Compared With the Emergency Severity Index. Ann. Emerg. Med. 2018, 71, 565–574.e2. [Google Scholar] [CrossRef] [PubMed]
- Chen, M.; Decary, M. Artificial Intelligence in Healthcare: An Essential Guide for Health Leaders. Healthc. Manag. Forum 2020, 33, 10–18. [Google Scholar] [CrossRef]
- Senior, A.W.; Evans, R.; Jumper, J.; Kirkpatrick, J.; Sifre, L.; Green, T.; Qin, C.; Žídek, A.; Nelson, A.W.R.; Bridgland, A.; et al. Improved Protein Structure Prediction Using Potentials from Deep Learning. Nature 2020, 577, 706–710. [Google Scholar] [CrossRef]



| AI Model Tools | Summary |
|---|---|
| DeepChem | An open-source library that provides a wide range of tools and models for drug discovery, including deep learning models for molecular property prediction, virtual screening, and generative chemistry. |
| RDKit | A widely used open-source cheminformatics library that offers various functionalities for molecule handling, substructure searching, and descriptor calculation. It can be integrated with machine learning frameworks for drug discovery applications. |
| ChemBERTa | A language model specifically designed for drug discovery tasks. It is based on the Transformer architecture and is pretrained on a large corpus of the chemical and biomedical literature, allowing it to generate molecular structures, predict properties, and assist in lead optimization. |
| GraphConv | A deep learning model architecture that operates on molecular graphs. It has been successful in predicting molecular properties, such as bioactivity and toxicity, by leveraging the structural information encoded in the graph representation of molecules. |
| AutoDock Vina | A popular docking software that uses machine learning techniques to predict the binding affinity between small molecules and protein targets. It can assist in virtual screening and lead optimization for drug discovery. |
| SMILES Transformer | A deep learning model that takes Simplified Molecular Input Line Entry System (SMILES) strings as input and generates molecular structures. It can be used for de novo drug design and lead optimization. |
| Schrödinger Suite | A comprehensive software package for drug discovery that incorporates various AI-driven tools. It includes modules for molecular modeling, virtual screening, ligand-based and structure-based drug design, and predictive modeling. |
| IBM RXN for Chemistry | An AI model designed to predict chemical reactions. It utilizes deep learning algorithms and large reaction datasets to generate potential reaction outcomes, aiding in the discovery of new synthetic routes and compound synthesis. |
| scape-DB | scape-DB (Extraction of Chemical and Physical Properties from the Literature-DrugBank) is a database that combines natural language processing and machine learning to extract chemical and biological data from the scientific literature. It provides valuable information for drug discovery research. |
| GENTRL (Generative Tensorial Reinforcement Learning) | A deep learning model that combines reinforcement learning with generative chemistry to design novel molecules with desired properties. It has been used for de novo drug design and optimization. |
| Sr. No. | Domain | Technology and Outcome | Industry and Collaborations |
|---|---|---|---|
| 1 | Drug design | Novel therapeutic antibodies | Exscientia |
| 2 | Molecular drug discovery | AtomNet–deep learning-driven computational platform for structure-based drug design | AtomWise |
| 3 | Gene mutation related disease | Machine learning based recursion operating system for biological and chemical datasets | Recursion |
| 4 | Drug design | Ligand- and structure-based de novo drug design, especially in multiparametric optimization | Iktos |
| 5 | Drug discovery | Generative modeling AI technology | Iktos and Galapagos |
| 6 | Drug development | Potential preclinical candidates | Iktos and Ono Pharma |
| 7 | Drug design | Rapid drug design by software “Makya” | Iktos and Sygnature Discovery |
| 8 | Drug discovery and Drug development | Pharma.AI, PandaMics, ALS.AI | Insilico Medicine |
| 9 | Drug target and Drug development | ChatPandaGPT | Insilico Medicine |
| 10 | Drug development | Protein motion in drug development lie RLY-4008 (Novel allosteric, pan mutant and isoform selective inhibitor of PI3Kα | Relay therapeutics |
| 11 | Drug discovery | AI and machine learning for selection of drug target | BenevolentAI |
| 12 | Drug target | Drug target selection for chronic kidney disease and idiopathic pulmonary fibrosis | BenevolentAI and AstraZeneca, GlaxoSmithKline, Pfizer |
| 13 | Clinical trials | AI in clinical trials | Pfizer and Vysioneer |
| 14 | Disease treatment | AI and supercomputing for oral COVID-19 treatment Paxloid | Pfizer |
| 15 | Drug discovery | NASH drugs and sequencing behemoth Illumina | AstraZeneca and Viking therapeutics |
| 16 | Drug development | Trials360.ai platform in clinical trials for site feasibility, site engagement and patient recruitment | Janssen |
| 17 | Drug research | Automate medical literature review by using natural language processing | Sanofi |
| 18 | Drug development | AI in drug development | BioMed X and Sanofi |
| 19 | Drug research and drug development | AI empowerment and AI exploration platforms | Novartis and Microsoft |
| 20 | Drug discovery | AI drug discovery platform | Bayer |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Vora, L.K.; Gholap, A.D.; Jetha, K.; Thakur, R.R.S.; Solanki, H.K.; Chavda, V.P. Artificial Intelligence in Pharmaceutical Technology and Drug Delivery Design. Pharmaceutics 2023, 15, 1916. https://doi.org/10.3390/pharmaceutics15071916
Vora LK, Gholap AD, Jetha K, Thakur RRS, Solanki HK, Chavda VP. Artificial Intelligence in Pharmaceutical Technology and Drug Delivery Design. Pharmaceutics. 2023; 15(7):1916. https://doi.org/10.3390/pharmaceutics15071916
Chicago/Turabian StyleVora, Lalitkumar K., Amol D. Gholap, Keshava Jetha, Raghu Raj Singh Thakur, Hetvi K. Solanki, and Vivek P. Chavda. 2023. "Artificial Intelligence in Pharmaceutical Technology and Drug Delivery Design" Pharmaceutics 15, no. 7: 1916. https://doi.org/10.3390/pharmaceutics15071916
APA StyleVora, L. K., Gholap, A. D., Jetha, K., Thakur, R. R. S., Solanki, H. K., & Chavda, V. P. (2023). Artificial Intelligence in Pharmaceutical Technology and Drug Delivery Design. Pharmaceutics, 15(7), 1916. https://doi.org/10.3390/pharmaceutics15071916









