Hybrid Lipid/Clay Carrier Systems Containing Annatto Oil for Topical Formulations
Abstract
:1. Introduction
2. Materials and Methods
2.1. Materials
2.2. Methods
2.2.1. Preparation of Nanoparticles
2.2.2. Particle Size, Polydispersity Index, and Zeta Potential
2.2.3. High-Resolution Transmission Electron Microscopy (HRTEM, FEI TITAN G2)
2.2.4. Thermal Analysis
2.2.5. X-ray Powder Diffraction (XRD)
2.2.6. Rheology
2.2.7. Cell Assays and Fluorescence Study
2.2.8. Statistical Analysis
3. Results
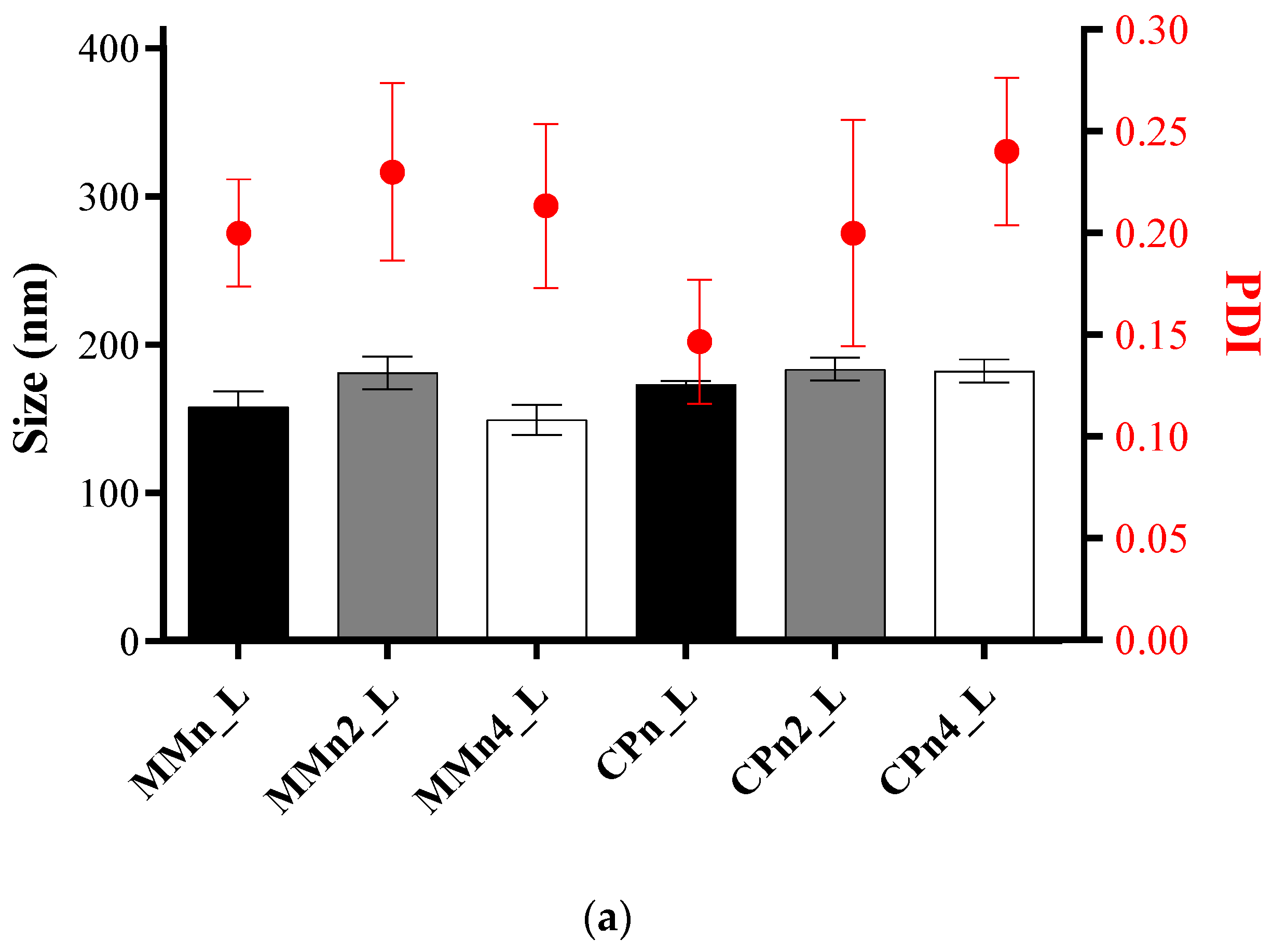
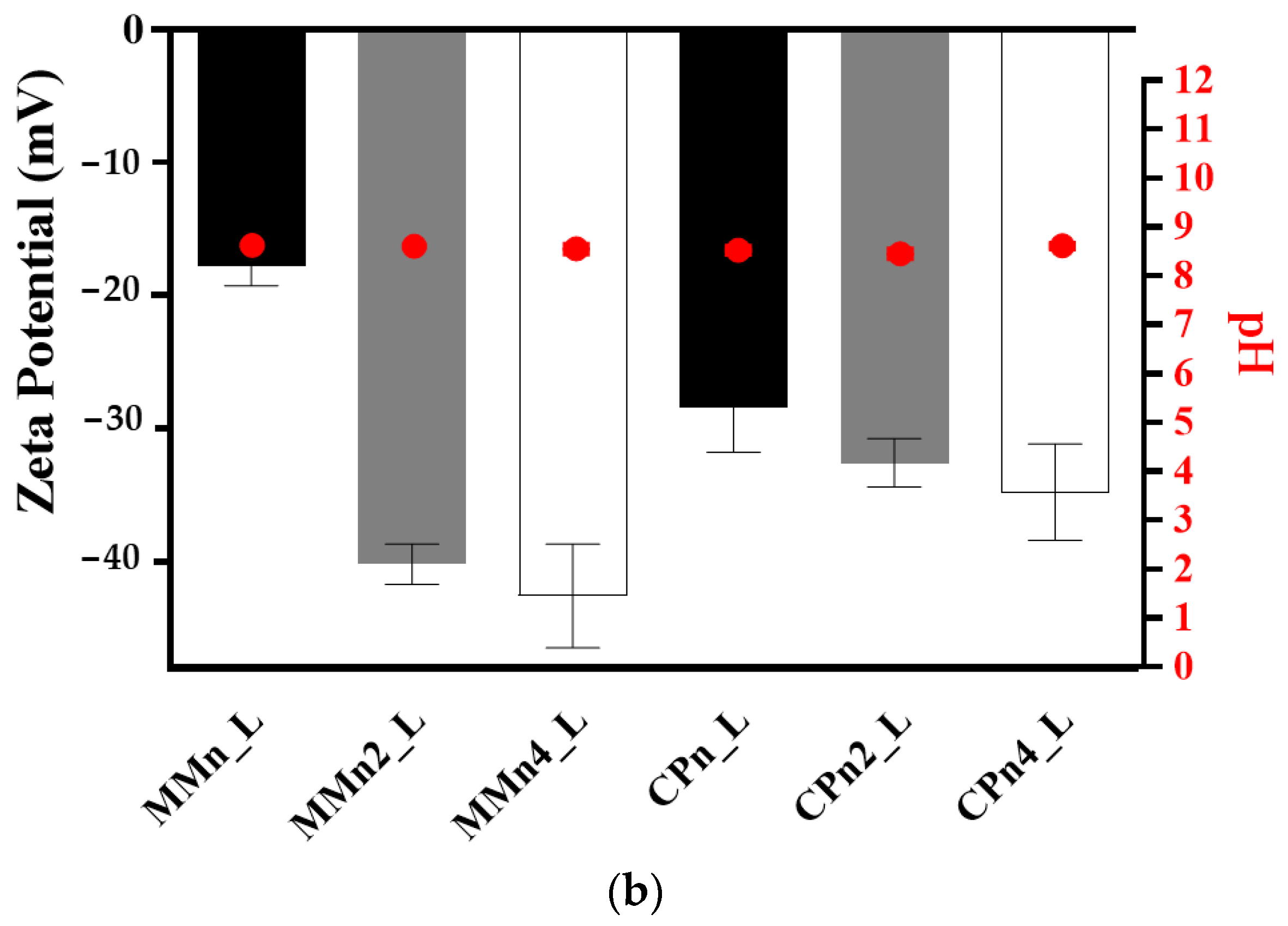
3.1. Particle Size, Polydispersity Index, and Zeta Potential
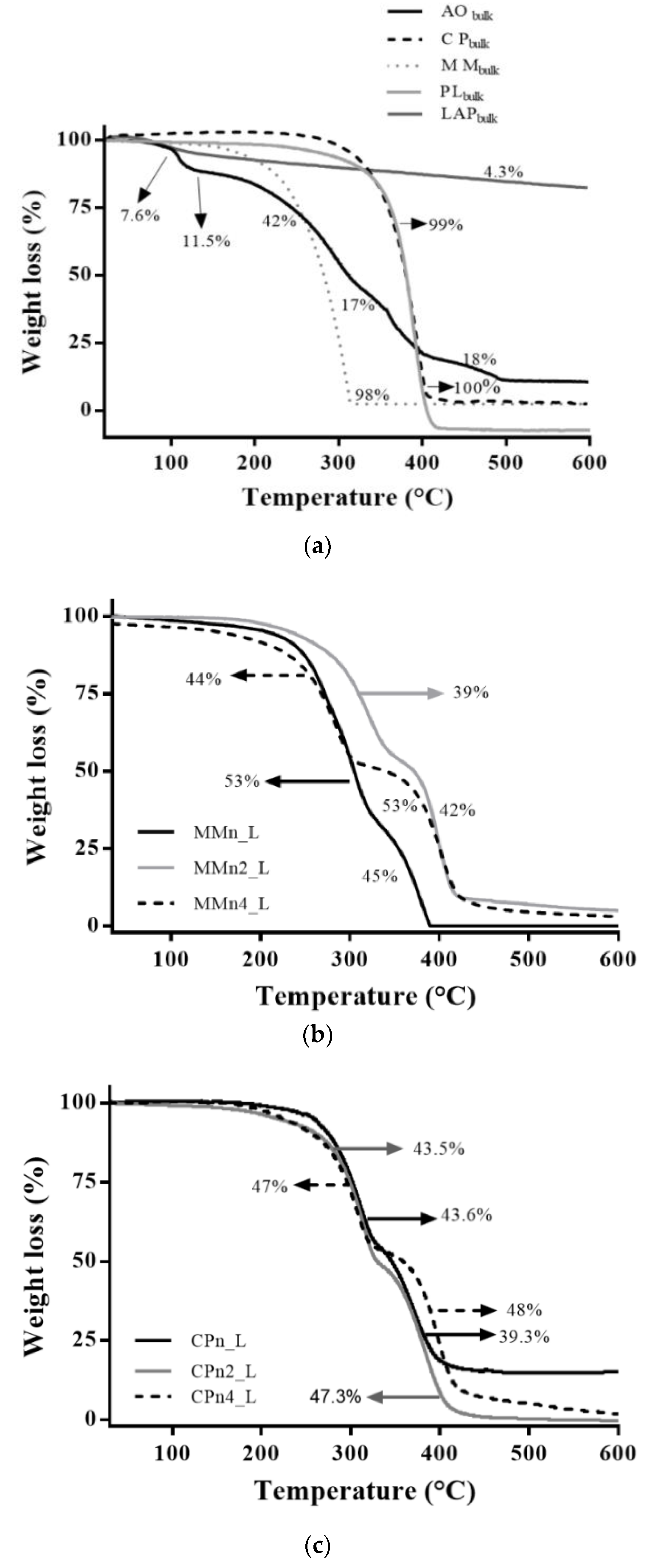
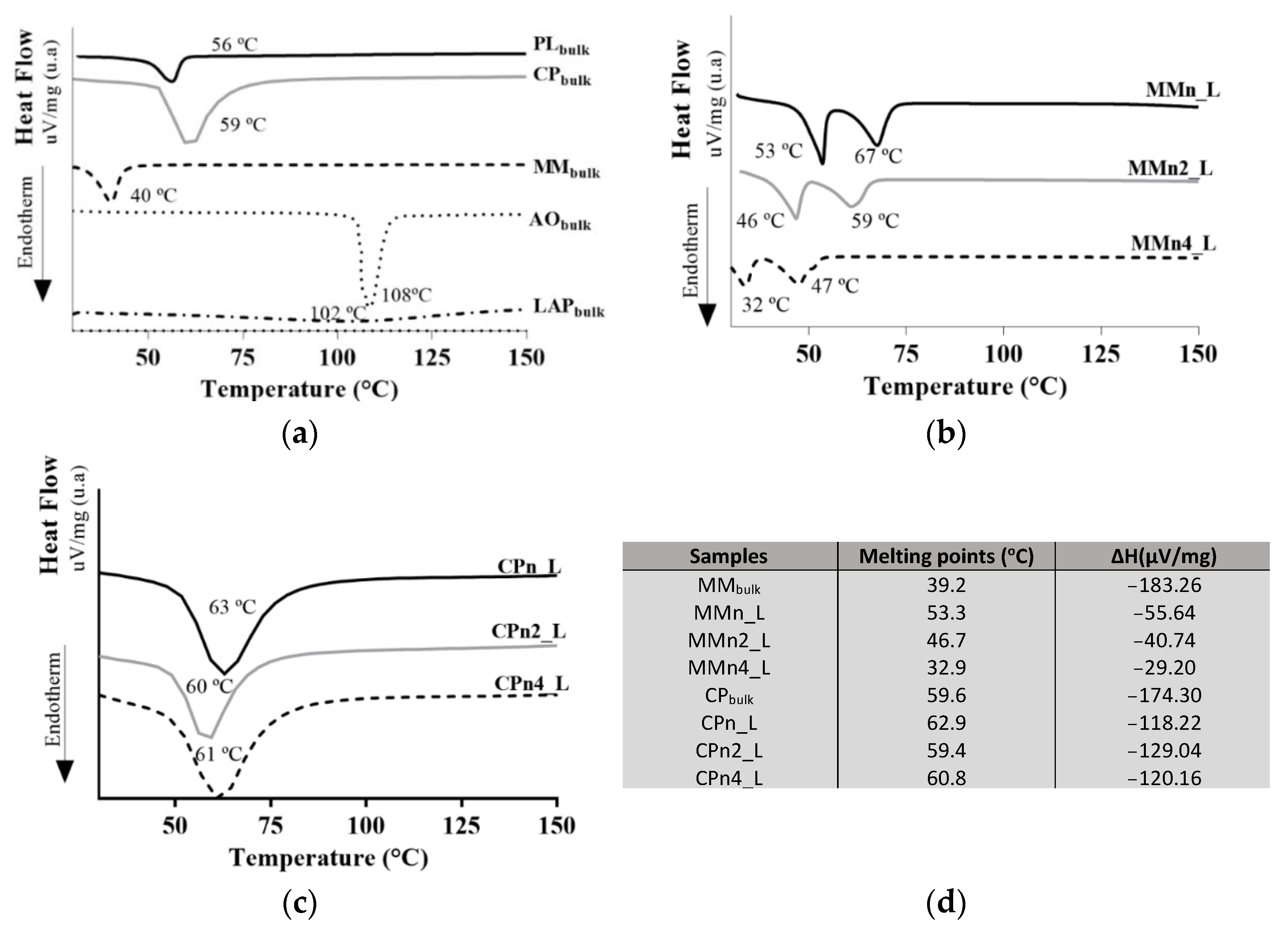
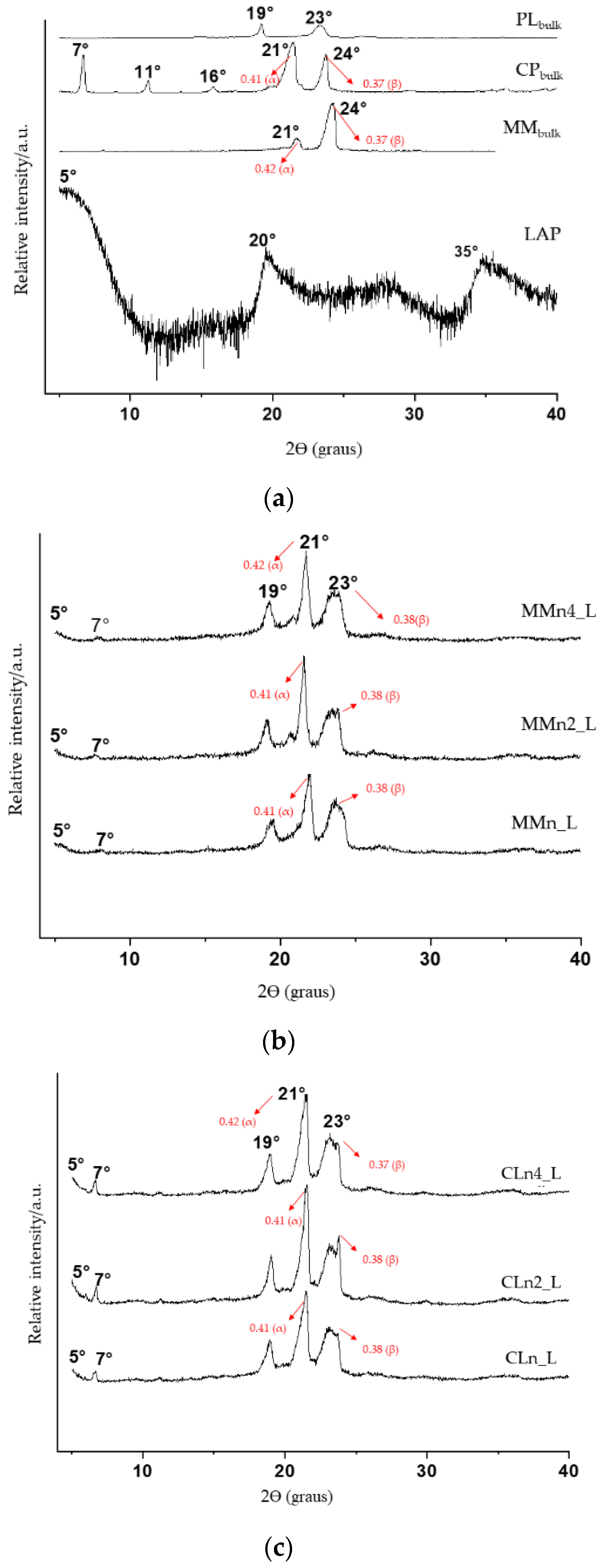
3.2. Thermal and X-ray Diffraction Analysis
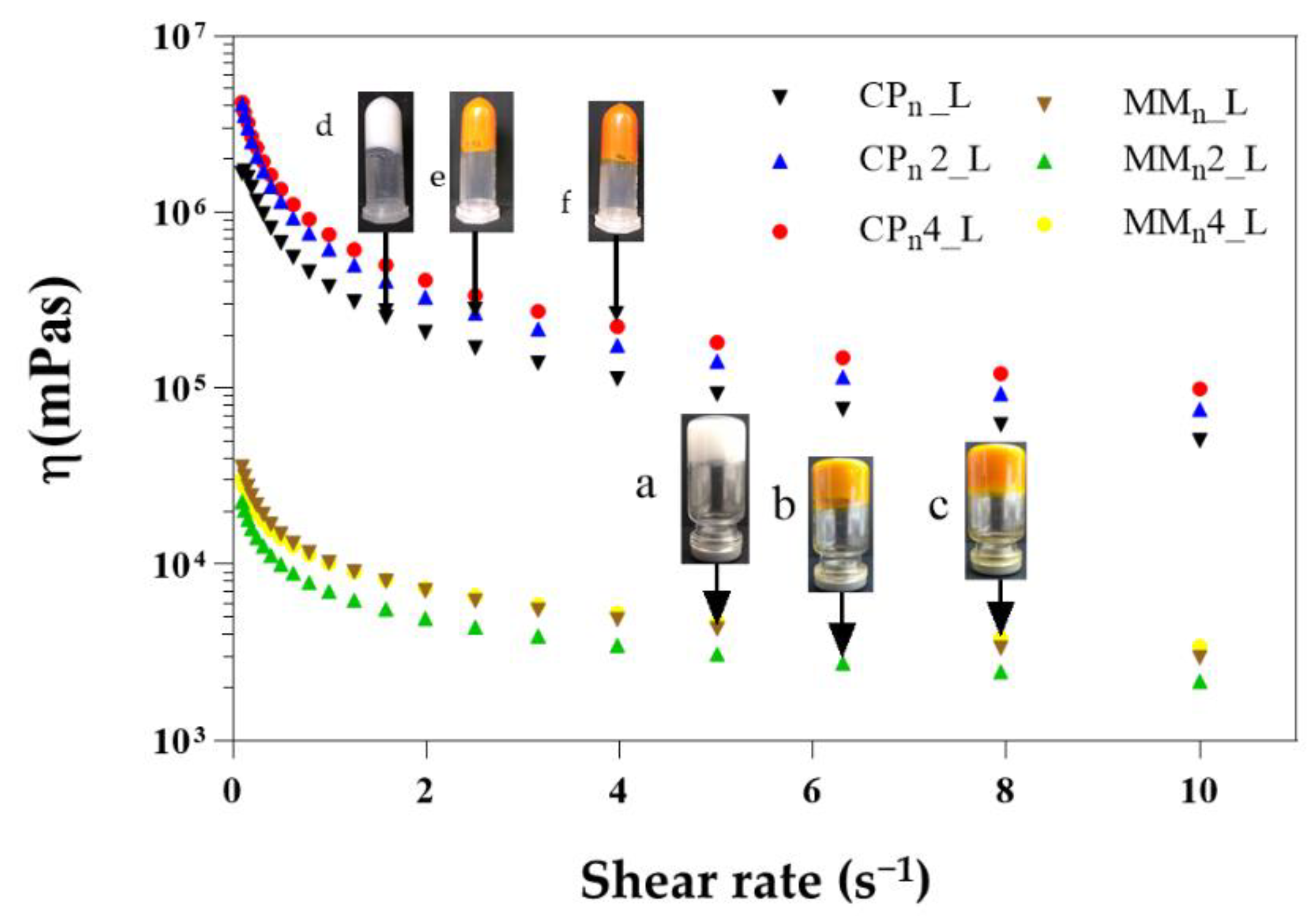
3.3. Rheology
3.4. Morphology Analysis
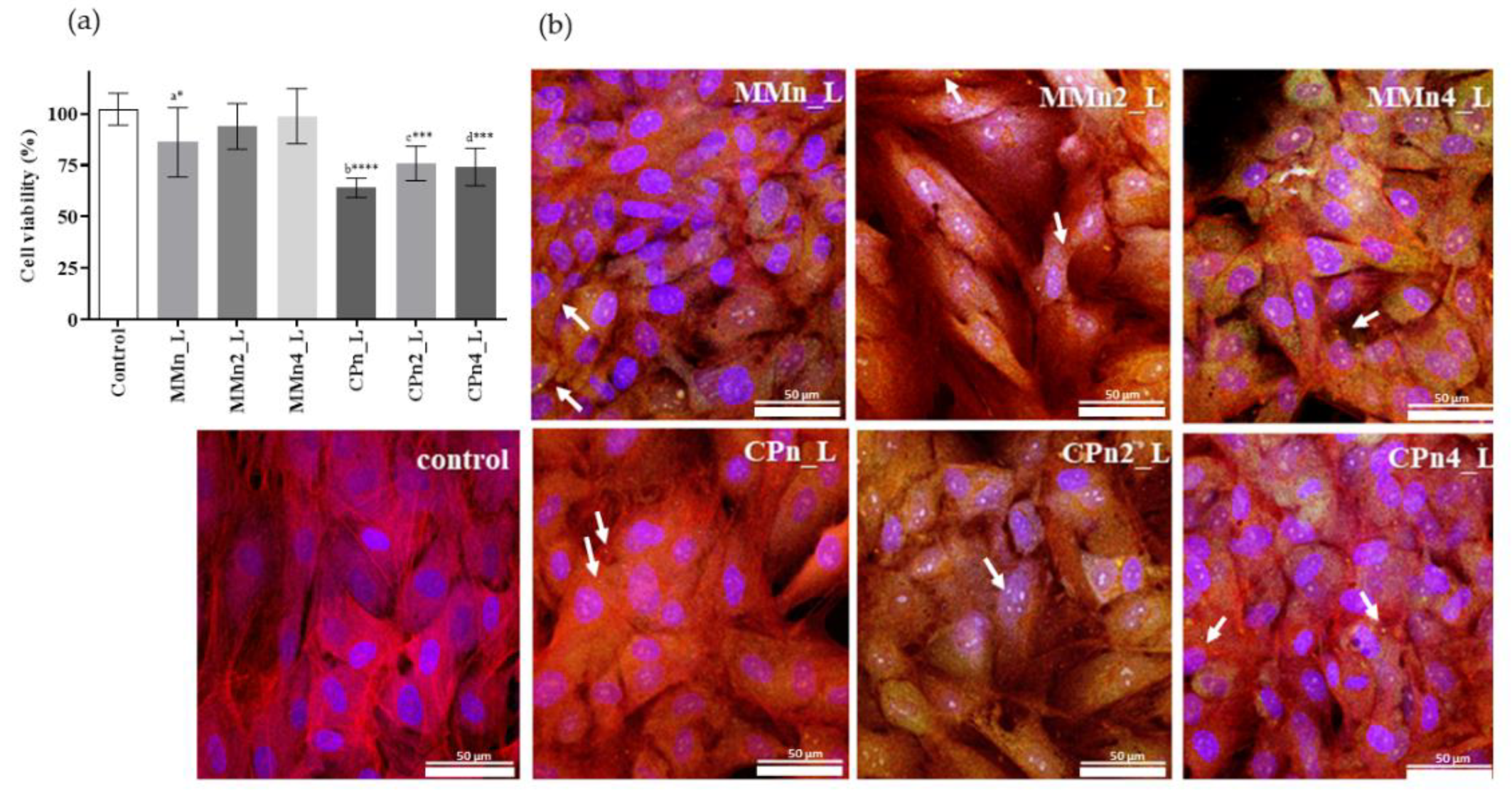
3.5. Cell Assays
4. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Paul, D.R.; Robeson, L.M. Polymer Nanotechnology: Nanocomposites. Polymer 2008, 49, 3187–3204. [Google Scholar] [CrossRef] [Green Version]
- Emmanuel, P. Giannelis. Polymer Layered Silicate Nanocomposites. Adv. Mater. 1996, 8, 29–35. [Google Scholar] [CrossRef]
- Nanobiotechnol, J.; Kim, H.Y.; Cheon, J.H.; Lee, S.H.; Min, J.Y.; Back, S.Y.; Song, J.G. Ternary Nanocomposite Carriers Based on Organic Clay-Lipid Vesicles as an Effective Colon-Targeted Drug Delivery System: Preparation and In Vitro/In Vivo Characterization. J. Nanobiotechnol. 2020, 18, 17. [Google Scholar] [CrossRef]
- Tenci, M.; Rossi, S.; Aguzzi, C.; Carazo, E.; Sandri, G.; Bonferoni, M.C.; Grisoli, P.; Viseras, C.; Caramella, C.M.; Ferrari, F. Carvacrol/Clay Hybrids Loaded into in Situ Gelling Films. Int. J. Pharm. 2017, 531, 676–688. [Google Scholar] [CrossRef] [PubMed]
- Aguzzi, C.; Cerezo, P.; Viseras, C.; Caramella, C. Use of Clays as Drug Delivery Systems: Possibilities and Limitations. Appl. Clay Sci. 2007, 36, 22–36. [Google Scholar] [CrossRef]
- Gaharwar, A.K.; Peppas, N.A.; Khademhosseini, A. Nanocomposite Hydrogels for Biomedical Applications. Biotechnol. Bioeng. 2014, 111, 441–453. [Google Scholar] [CrossRef] [Green Version]
- Nair, L.S.; Laurencin, C.T. Biodegradable Polymers as Biomaterials. Prog. Polym. Sci. 2007, 32, 762–798. [Google Scholar] [CrossRef]
- Moraes, J.D.D.; Bertolino, S.R.A.; Cuffini, S.L.; Ducart, D.F.; Bretzke, P.E.; Leonardi, G.R. Clay Minerals: Properties and Applications to Dermocosmetic Products and Perspectives of Natural Raw Materials for Therapeutic Purposes—A Review. Int. J. Pharm. 2017, 534, 213–219. [Google Scholar] [CrossRef]
- Viseras, C.; Carazo, E.; García-villén, F.; Sánchez-espejo, R.; Cerezo, P.; Aguzzi, C. Clay Minerals in Skin Drug Delivery. Clays Clay Miner. 2019, 58, 59–71. [Google Scholar] [CrossRef]
- Labanda, J.; Llorens, J. Effect of Aging Time on the Rheology of Laponite Dispersions. Colloids Surf. A Physicochem. Eng. Asp. 2008, 329, 1–6. [Google Scholar] [CrossRef]
- Da Silva, M.A.; Dreiss, C.A. Soft Nanocomposites: Nanoparticles to Tune Gel Properties. Polym. Int. 2016, 65, 268–279. [Google Scholar] [CrossRef] [Green Version]
- Tomás, H.; Alves, C.S.; Rodrigues, J. Laponite®: A Key Nanoplatform for Biomedical Applications? Nanomed. Nanotechnol. Biol. Med. 2018, 14, 2407–2420. [Google Scholar] [CrossRef] [PubMed]
- Gonçalves, M.; Figueira, P.; Maciel, D.; Rodrigues, J.; Qu, X.; Liu, C.; Tomás, H.; Li, Y. PH-Sensitive Laponite®/Doxorubicin/Alginate Nanohybrids with Improved Anticancer Efficacy. Acta Biomater. 2014, 10, 300–307. [Google Scholar] [CrossRef] [PubMed]
- Salcedo, I.; Aguzzi, C.; Sandri, G.; Bonferoni, M.C.; Mori, M.; Cerezo, P.; Sánchez, R.; Viseras, C.; Caramella, C. In Vitro Biocompatibility and Mucoadhesion of Montmorillonite Chitosan Nanocomposite: A New Drug Delivery. Appl. Clay Sci. 2012, 55, 131–137. [Google Scholar] [CrossRef]
- Gaharwar, A.K.; Schexnailder, P.J.; Kline, B.P.; Schmidt, G. Assessment of Using Laponite?? Cross-Linked Poly(Ethylene Oxide) for Controlled Cell Adhesion and Mineralization. Acta Biomater. 2011, 7, 568–577. [Google Scholar] [CrossRef]
- Dong, Y.; Feng, S.S. Poly(D,L-Lactide-Co-Glycolide)/Montmorillonite Nanoparticles for Oral Delivery of Anticancer Drugs. Biomaterials 2005, 26, 6068–6076. [Google Scholar] [CrossRef]
- Schäfer-Korting, M.; Mehnert, W.; Korting, H.C. Lipid Nanoparticles for Improved Topical Application of Drugs for Skin Diseases. Adv. Drug Deliv. Rev. 2007, 59, 427–443. [Google Scholar] [CrossRef]
- Doktorovova, S.; Souto, E.B. Nanostructured Lipid Carrier-Based Hydrogel Formulations for Drug Delivery: A Comprehensive Review. Expert Opnion Drug Deliv. 2009, 6, 165–176. [Google Scholar] [CrossRef]
- Müller, R.H.; Radtke, M.; Wissing, S.A. Solid Lipid Nanoparticles (SLN) and Nanostructured Lipid Carriers (NLC) in Cosmetic and Dermatological Preparations. Adv. Drug Deliv. Rev. 2002, 54, 131–155. [Google Scholar] [CrossRef]
- Souto, E.B.; Wissing, S.A.; Barbosa, C.M.; Müller, R.H. Development of a Controlled Release Formulation Based on SLN and NLC for Topical Clotrimazole Delivery. Int. J. Pharm. 2004, 278, 71–77. [Google Scholar] [CrossRef]
- Wissing, S.A.; Kayser, O.; Müller, R.H. Solid Lipid Nanoparticles for Parenteral Drug Delivery. Adv. Drug Deliv. Rev. 2004, 56, 1257–1272. [Google Scholar] [CrossRef] [PubMed]
- Attama, A.A. SLN, NLC, LDC: State of the Art in Drug and Active Delivery. Recent Pat. Drug Deliv. Formul. 2011, 5, 178–187. [Google Scholar] [CrossRef] [PubMed]
- Müller, R.H.; Shegokar, R.; Keck, C.M. 20 Years of Lipid Nanoparticles (SLN & NLC): Present State of Development & Industrial Applications. Curr. Drug Discov. Technol. 2011, 8, 207–227. [Google Scholar] [PubMed]
- de Melo Barbosa, R.; Severino, P.; Finkler, C.L.; de Paula, E. Lipid-Based Colloidal Carriers for Transdermal Administration of Bioactives. In Materials for Biomedical Engineering: Organic Micro and Nanostructures; Holban, A.-M., Grumezescu, A.M., Eds.; Elsevier Ltd.: Oxford, UK, 2019; pp. 369–397. [Google Scholar] [CrossRef]
- Souto, E.B.; Jäger, A.; Štěpánek, P.; Cano, A.; Viseras, C.; Barbosa, R.; Chorilli, M.; Zielinska, A.; Severino, P.; Naveros, B.C. Lipid Nanomaterials for Targeted Delivery of Dermocosmetic Ingredients: Advances in Photoprotection and Skin Anti-Aging. Pharmaceutics 2022, 12, 377. [Google Scholar] [CrossRef] [PubMed]
- Medina-flores, D.; Ulloa-urizar, G.; Camere-colarossi, R.; Caballero-garcía, S.; Mayta-Tovalino, F.; Valle-Mendoza, J. Antibacterial activity of Bixa orellana L. (achiote) against Streptococcus mutans and Streptococcus sanguinis. Asian Pac. J. Trop. Biomed. 2016, 6, 400–403. [Google Scholar] [CrossRef] [Green Version]
- Fleischer, T.C.; Ameade, E.P.K.; Mensah, M.L.K.; Sawer, I.K. Antimicrobial Activity of the Leaves and Seeds of Bixa Orellana. Fitoterapia 2003, 74, 136–138. [Google Scholar] [CrossRef]
- Monzote, L.; García, M.; Scull, R.; Cuellar, A.; Setzer, W.N. Antileishmanial Activity of the Essential Oil from Bixa Orellana. Phytother. Res. 2014, 28, 753–758. [Google Scholar] [CrossRef]
- Vilar, D.D.; Vilar, M.S.; Raffin, F.N.; Oliveira, M.R.; Franco, C.F.; de Athayde-Filho, P.F.; Diniz, M.D.; Barbosa-Filho, J.M. Traditional Uses, Chemical Constituents, and Biological Activities of Bixa orellana L.: A Review. Sci. World J. 2014, 2014, 857292. [Google Scholar] [CrossRef] [Green Version]
- Ibrahim, N.I.; Wong, S.K.; Mohamed, I.N.; Mohamed, N. Wound Healing Properties of Selected Natural Products. Int. J. Environ. Res. Public Health Rev. 2018, 15, 2360. [Google Scholar] [CrossRef] [Green Version]
- Aggarwal, B.B.; Sundaram, C.; Prasad, S.; Kannappan, R. Tocotrienols, the Vitamin E of the 21st Century: Its Potential against Cancer and Other Chronic Diseases. Biochem. Pharmacol. 2010, 80, 1613–1631. [Google Scholar] [CrossRef] [Green Version]
- Barrias, C.C.; Granja, P.L. Advanced Biofabrication Strategies for Skin Regeneration and Repair. Nanomedicine 2013, 8, 603–621. [Google Scholar] [CrossRef]
- Bueno, J.; Demirci, F.; Baser, K.H.C. Antimicrobial Strategies in Novel Drug Delivery Systems: Applications in the Treatment of Skin and Soft Tissue Infections. In The Microbiology of Skin, Soft Tissue, Bone and Joint Infections; Elsevier Inc.: London, UK, 2017; Volume 2, pp. 271–286. [Google Scholar] [CrossRef]
- Souto, E.B.; Yoshida, C.M.P.; Leonardi, G.R.; Cano, A. Lipid-Polymeric Films: Composition, Production and Applications in Wound Healing and Skin Repair. Pharm. Rev. 2021, 13, 1199. [Google Scholar] [CrossRef] [PubMed]
- Barbosa, D.M.; Ribeiro, L.N.; Casadei, B.R.; Da Silva, C.M.; Queiróz, V.A.; Duran, N.; De Araújo, D.R.; Severino, P.; De Paula, E. Solid Lipid Nanoparticles for Dibucaine Sustained Release. Pharmaceutics 2018, 10, 231. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Barbosa, R.M.; Casadei, B.R.; Duarte, E.L.; Severino, P.; Barbosa, L.R.S.; Duran, N.; De Paula, E. Electron Paramagnetic Resonance and Small-Angle X-ray Scattering Characterization of Solid Lipid Nanoparticles and Nanostructured Lipid Carriers for Dibucaine Encapsulation. Langmuir 2018, 34, 13296–13304. [Google Scholar] [CrossRef] [PubMed]
- Barbosa, R.M.; Da Silva, C.M.G.; Bella, T.S.; De Araújo, D.R.; Marcato, P.D.; Durán, N.; De Paula, E. Cytotoxicity of Solid Lipid Nanoparticles and Nanostructured Lipid Carriers Containing the Local Anesthetic Dibucaine Designed for Topical Application. J. Phys. Conf. Ser. 2013, 429, 012035. [Google Scholar] [CrossRef] [Green Version]
- Ribeiro, L.N.M.; Franz-Montan, M.; Breitkreitz, M.C.; Alcântara, A.C.S.; Castro, S.R.; Guilherme, V.A.; Barbosa, R.M.; de Paula, E. Nanostructured Lipid Carriers as Robust Systems for Topical Lidocaine-Prilocaine Release in Dentistry. Eur. J. Pharm. Sci. 2016, 93, 192–202. [Google Scholar] [CrossRef]
- Beloqui, A.; Solinis, M.A.; Rodriguez-Gascon, A.; Almeida, A.J.; Preat, V. Nanostructured Lipid Carriers: Promising Drug Delivery Systems for Future Clinics. Nanomedicine 2016, 12, 143–161. [Google Scholar] [CrossRef]
- Schubert, M.A.; Müller-Goymann, C.C. Characterisation of Surface-Modified Solid Lipid Nanoparticles (SLN): Influence of Lecithin and Nonionic Emulsifier. Eur. J. Pharm. Biopharm. 2005, 61, 77–86. [Google Scholar] [CrossRef]
- Müller, R.H.; Mäder, K.; Gohla, S. Solid lipid nanoparticles (SLN) for controlled drug delivery ± a review of the state of the art. Eur. J. Pharm. Biopharm. 2000, 50, 161–177. [Google Scholar] [CrossRef]
- Ferreira, M.A.; de Almeida Júnior, R.F.; Onofre, T.S.; Casadei, B.R.; Farias, K.J.; Severino, P.; de Oliveira Franco, C.F.; Raffin, F.N.; de Lima e Moura, T.F.; de Melo Barbosa, R. Annatto Oil Loaded Nanostructured Lipid Carriers: A Potential New Treatment for Cutaneous Leishmaniasis. Pharmaceutics 2021, 13, 1912. [Google Scholar] [CrossRef]
- Silva, G.F.; Gamarra, F.M.C.; Oliveira, A.L.; Cabral, F.A. Extraction of Bixin from Annatto Seeds Using Supercritical Carbon Dioxide. Braz. J. Chem. Eng. 2008, 25, 419–426. [Google Scholar] [CrossRef]
- Taham, T.; Cabral, F.A.; Barrozo, M.A.S. Extraction of Bixin from Annatto Seeds Using Combined Technologies. J. Supercrit. Fluids 2015, 100, 175–183. [Google Scholar] [CrossRef]
- Kanicky, J.R.; Shah, D.O. Effect of Degree, Type, and Position of Unsaturation on the PKa of Long-Chain Fatty Acids. J. Colloid Interface Sci. 2002, 256, 201–207. [Google Scholar] [CrossRef] [PubMed]
- Mitri, K.; Shegokar, R.; Gohla, S.; Anselmi, C.; Müller, R.H. Lipid Nanocarriers for Dermal Delivery of Lutein: Preparation, Characterization, Stability and Performance. Int. J. Pharm. 2011, 414, 267–275. [Google Scholar] [CrossRef]
- Bostan, L.E.; Clarkin, C.E.; Mousa, M.; Worsley, P.R.; Bader, D.L.; Dawson, J.I.; Evans, N.D. Synthetic Nanoclay Gels Do Not Cause Skin Irritation in Healthy Human Volunteers. ACS Biomater. Sci. Eng. Appl. 2021, 7, 2716–2722. [Google Scholar] [CrossRef] [PubMed]
- Battaglia, L.; Gallarate, M. Lipid Nanoparticles: State of the Art, New Preparation Methods and Challenges in Drug Delivery. Expert Opin. Drug Deliv. 2012, 9, 497–508. [Google Scholar] [CrossRef]
- Crowley, M. Remington: The Science and Practice of Pharmacy. In Remington: The Science And Practice Of Pharmacy; Trod, D.B., Ed.; Lippincott Williams & Wilkins: Philadelphia, PA, USA, 2006; pp. 745–775. [Google Scholar]
- Silva, M.C.D.; Botelho, J.R.; Conceição, M.M.; Lira, B.F.; Coutinho, M.A.; Dias, A.F.; Souza, A.G.; Filho, P.F.A. Thermogravimetric Investigations on the Thermal Degradation of Bixin, Derived from the Seeds of Annatto (Bixa orellana L.). J. Therm. Anal. Calorim. 2005, 79, 277–281. [Google Scholar] [CrossRef]
- Marcolino, V.A.; Zanin, G.M.; Durrant, L.R.; Benassi, M.D.T.; Matioli, G. Interaction of Curcumin and Bixin with β-Cyclodextrin: Complexation Methods, Stability, and Applications in Food. J. Agric. Food Chem. 2011, 59, 3348–3357. [Google Scholar] [CrossRef]
- Ramadhani, N.; Shabir, M.; McConville, C. Preparation and Characterisation of Kolliphor® P 188 and P 237 Solid Dispersion Oral Tablets Containing the Poorly Water Soluble Drug Disulfiram. Int. J. Pharm. 2014, 475, 514–522. [Google Scholar] [CrossRef]
- Aydın, A.A.; Okutan, H. High-Chain Fatty Acid Esters of Myristyl Alcohol with Even Carbon Number: Novel Organic Phase Change Materials for Thermal Energy Storage—1. Sol. Energy Mater. Sol. Cells 2011, 95, 2752–2762. [Google Scholar] [CrossRef]
- Teeranachaideekul, V.; Müller, R.H.; Junyaprasert, V.B. Encapsulation of Ascorbyl Palmitate in Nanostructured Lipid Carriers (NLC)—Effects of Formulation Parameters on Physicochemical Stability. Int. J. Pharm. 2007, 340, 198–206. [Google Scholar] [CrossRef] [PubMed]
- Kolenyak-Santos, F.; Garnero, C.; De Oliveira, R.N.; de Souza, A.L.R.; Chorilli, M.; Allegretti, S.M.; Longhi, M.R.; Chaud, M.V.; Gremião, M.P.D. Nanostructured Lipid Carriers as a Strategy to Improve the In Vitro Schistosomiasis Activity of Praziquantel. J. Nanosci. Nanotechnol. 2015, 15, 761–772. [Google Scholar] [CrossRef] [PubMed]
- de Souza, A.L.; Andreani, T.; Nunes, F.M.; Cassimiro, D.L.; de Almeida, A.E.; Ribeiro, C.A.; Sarmento, V.H.; Gremião, M.P.; Silva, A.M.; Souto, E.B. Loading of Praziquantel in the Crystal Lattice of Solid Lipid Nanoparticles. J. Therm. Anal. Calorim. 2012, 108, 353–360. [Google Scholar] [CrossRef]
- Bounabi, L.; Bouslah, N.; Haddadine, N.; Ouazib, F.; Barille, R. Development of Poly(2-Hydroxyethyl Methacrylate)/Clay Composites as Drug Delivery Systems of Paracetamol. J. Drug Deliv. Sci. Technol. 2016, 33, 58–65. [Google Scholar] [CrossRef] [Green Version]
- Scotter, M.J. Characterisation of the Coloured Thermal Degradation Products of Bixin from Annatto and a Revised Mechanism for Their Formation. Food Chem. 1995, 53, 177–185. [Google Scholar] [CrossRef]
- Ruktanonchai, U.; Limpakdee, S.; Meejoo, S.; Sakulkhu, U.; Bunyapraphatsara, N.; Junyaprasert, V.; Puttipipatkhachorn, S. The Effect of Cetyl Palmitate Crystallinity on Physical Properties of Gamma-Oryzanol Encapsulated in Solid Lipid Nanoparticles. Nanotechnology 2008, 19, 095701. [Google Scholar] [CrossRef]
- Pardeike, J.; Hommoss, A.; Müller, R.H. Lipid Nanoparticles (SLN, NLC) in Cosmetic and Pharmaceutical Dermal Products. Int. J. Pharm. 2009, 366, 170–184. [Google Scholar] [CrossRef]
- Rao, Y.Q. Gelatin-Clay Nanocomposites of Improved Properties. Polymer 2007, 48, 5369–5375. [Google Scholar] [CrossRef]
- Valencia, G.A.; Lourenco, R.V.; Bittante, A.M.; do Amaral Sobral, P.J. Physical and Morphological Properties of Nanocomposite Films Based on Gelatin and Laponite. Appl. Clay Sci. 2016, 124–125, 260–266. [Google Scholar] [CrossRef]
- Severino, P.; Pinho, S.C.; Souto, E.B.; Santana, M.H.A. Crystallinity of Dynasan® 114 and Dynasan® 118 Matrices for the Production of Stable Miglyol®—Loaded Nanoparticles. J. Therm. Anal. Calorim. 2012, 108, 101–108. [Google Scholar] [CrossRef]
- Souto, E.B.; Almeida, A.J.; Müller, R.H. Lipid Nanoparticles (SLN®, NLC®) for Cutaneous Drug Delivery: Structure, Protection and Skin Effects. J. Biomed. Nanotechnol. 2007, 3, 317–331. [Google Scholar] [CrossRef]
- Mehnert, W.; Mäder, K. Solid Lipid Nanoparticles: Production, Characterization and Applications. Adv. Drug Deliv. Rev. 2001, 47, 165–196. [Google Scholar] [CrossRef]
- Lutz, D.A.; Eddy, C.R.; Hunter, J.J. X-ray Diffraction Study of Some Normal Alkyl Esters of Long-Chain Acids. Lipids 1967, 2, 204–207. [Google Scholar] [CrossRef] [PubMed]
- Alexandre, M.; Dubois, P. Polymer-Layered Silicate Nanocomposites: Preparation, Properties and Uses of a New Class of Materials. Mater. Sci. Eng. R Rep. 2000, 28, 1–63. [Google Scholar] [CrossRef]
- Tawari, S.L.; Koch, D.L.; Cohen, C. Electrical Double-Layer Effects on the Brownian Diffusivity and Aggregation Rate of Laponite Clay Particles. J. Colloid Interface Sci. 2001, 240, 54–66. [Google Scholar] [CrossRef]
- Dávila, J.L.; d’Ávila, M.A. Laponite as a Rheology Modifier of Alginate Solutions: Physical Gelation and Aging Evolution. Carbohydr. Polym. 2017, 157, 1–8. [Google Scholar] [CrossRef]
- Garcês, A.; Amaral, M.H.; Sousa Lobo, J.M.; Silva, A.C. Formulations Based on Solid Lipid Nanoparticles (SLN) and Nanostructured Lipid Carriers (NLC) for Cutaneous Use: A Review. Eur. J. Pharm. Sci. 2017, 112, 159–167. [Google Scholar] [CrossRef]
- Benavides, T.; Mitjans, M.; Martinez, V.; Clapes, P.; Infante, M.R.; Clothier, R.H.; Vinardell, M.P. Assessment of Primary Eye and Skin Irritants by In Vitro Cytotoxicity and Phototoxicity Models: An In Vitro Approach of New Arginine-Based Surfactant-Induced Irritation. Toxicology 2004, 197, 229–237. [Google Scholar] [CrossRef]
- ISO 10993-5; Biological Evaluation of Medical Devices. Part 5: Tests for in Vitro Cytotoxicity. ISO: Geneva, Switzerland, 2009.
- Packer, L.; Weber, S.U.; Rimbach, G. Molecular Aspects of A-Tocotrienol Antioxidant Action and Cell Signalling. J. Nutr. 2001, 131, 369–373. [Google Scholar] [CrossRef] [Green Version]


| Samples | Lipid (%) | AObulk (%) | PLbulk (%) | H2O (%) | LAP (%) |
|---|---|---|---|---|---|
| MMn_L | 10 | - | 11.7 | 78.3 | 3 |
| MMn2_L | 10 | 2 | 11.7 | 76.6 | 3 |
| MMn4_L | 10 | 4 | 11.7 | 74.8 | 3 |
| CPn_L | 10 | - | 11.7 | 78.3 | 3 |
| CPn2_L | 10 | 2 | 11.7 | 76.6 | 3 |
| CPn4_L | 10 | 4 | 11.7 | 74.8 | 3 |
| Samples | Angle 2ϴ Experimental (°) | Lattice Spacings d (nm) |
|---|---|---|
| MM | 20.82 | 0.43-β’ |
| 24.26 | 0.37-β’ | |
| Mn_L | 21.61 | 0.41-α |
| 23.33 | 0.38-β’ | |
| Mn2_L | 21.50 | 0.41-α |
| 23.33 | 0.38-β’ | |
| Mn4_L | 21.33 | 0.42-α |
| 23,167 | 0.38-β’ | |
| CP | 21.49 | 0.41-α |
| 23.74 | 0.37-β’ | |
| CPn_L | 21.64 | 0.41-α |
| 23.42 | 0.38-β’ | |
| CPn2_L | 21.51 | 0.41-α |
| 23.51 | 0.38-β’ | |
| CPn4_L | 21.38 | 0.42-α |
| 23.83 | 0.37-β’ |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Barbosa, R.d.M.; Leite, A.M.; García-Villén, F.; Sánchez-Espejo, R.; Cerezo, P.; Viseras, C.; Faccendini, A.; Sandri, G.; Raffin, F.N.; Moura, T.F.A.d.L.e. Hybrid Lipid/Clay Carrier Systems Containing Annatto Oil for Topical Formulations. Pharmaceutics 2022, 14, 1067. https://doi.org/10.3390/pharmaceutics14051067
Barbosa RdM, Leite AM, García-Villén F, Sánchez-Espejo R, Cerezo P, Viseras C, Faccendini A, Sandri G, Raffin FN, Moura TFAdLe. Hybrid Lipid/Clay Carrier Systems Containing Annatto Oil for Topical Formulations. Pharmaceutics. 2022; 14(5):1067. https://doi.org/10.3390/pharmaceutics14051067
Chicago/Turabian StyleBarbosa, Raquel de Melo, Aliana Monteiro Leite, Fátima García-Villén, Rita Sánchez-Espejo, Pilar Cerezo, César Viseras, Angela Faccendini, Giuseppina Sandri, Fernanda Nervo Raffin, and Túlio Flávio Accioly de Lima e Moura. 2022. "Hybrid Lipid/Clay Carrier Systems Containing Annatto Oil for Topical Formulations" Pharmaceutics 14, no. 5: 1067. https://doi.org/10.3390/pharmaceutics14051067
APA StyleBarbosa, R. d. M., Leite, A. M., García-Villén, F., Sánchez-Espejo, R., Cerezo, P., Viseras, C., Faccendini, A., Sandri, G., Raffin, F. N., & Moura, T. F. A. d. L. e. (2022). Hybrid Lipid/Clay Carrier Systems Containing Annatto Oil for Topical Formulations. Pharmaceutics, 14(5), 1067. https://doi.org/10.3390/pharmaceutics14051067









