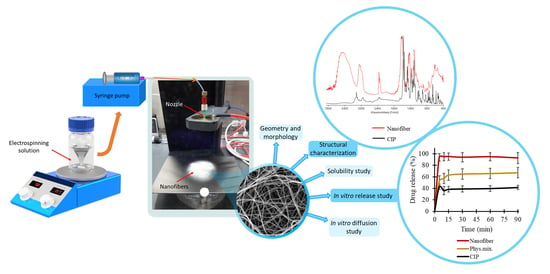
In Vitro Drug Release, Permeability, and Structural Test of Ciprofloxacin-Loaded Nanofibers
Abstract
1. Introduction
2. Materials and Methods
2.1. Materials
2.2. Methods
2.2.1. Preparation of the Solutions for Electrospinning
2.2.2. Electrospinning Procedure
2.2.3. Preparation of the Physical Mixture
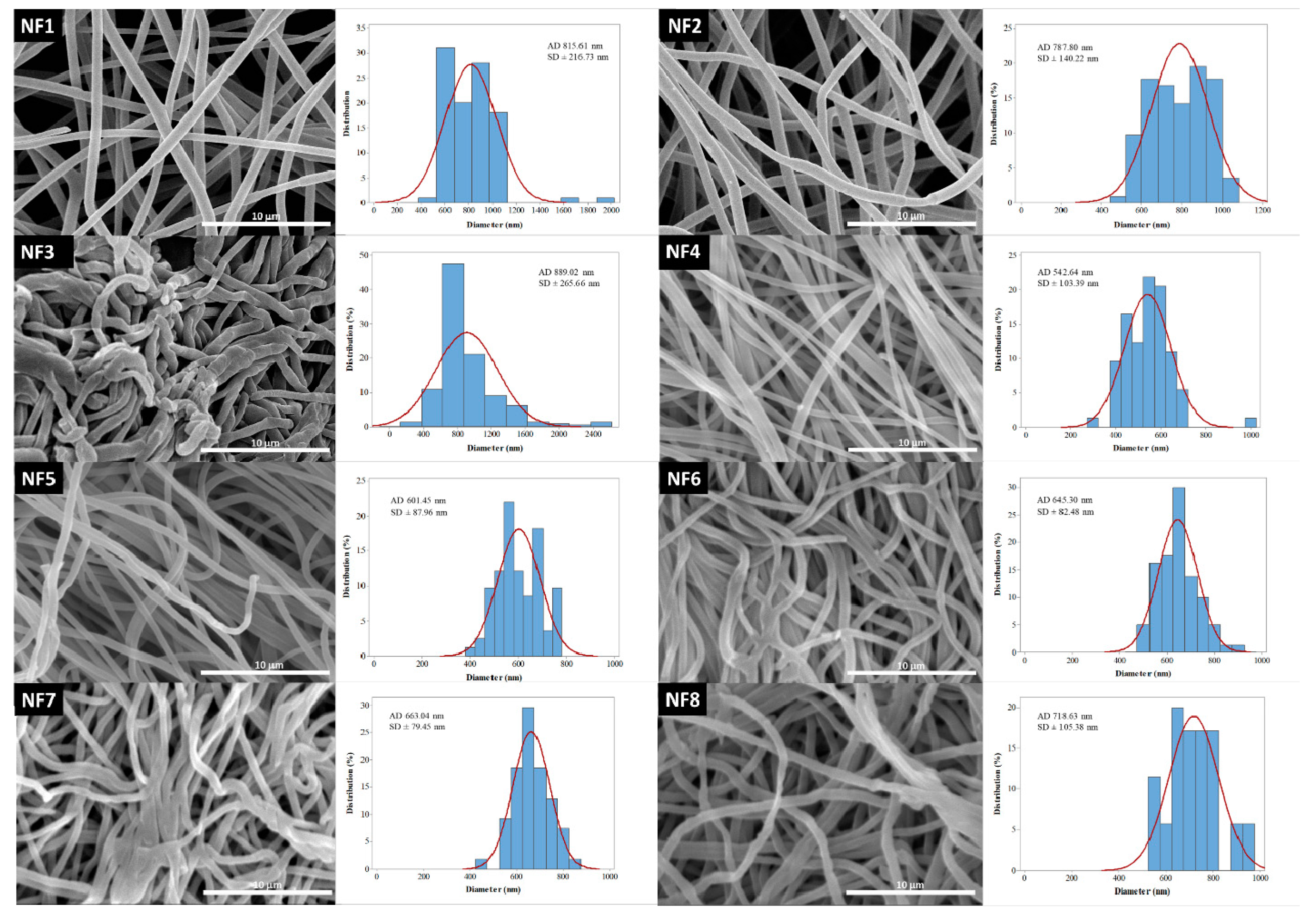
2.2.4. Size and Morphological Measurements
2.2.5. Structural Characterization
2.2.6. Drug Loading and Drug Entrapment Efficiency
2.2.7. Solubility Tests
2.2.8. In Vitro Drug Release Studies
2.2.9. Study of Drug-Release Kinetics and Mechanism
2.2.10. In Vitro Diffusion Study
2.2.11. Statistical Analysis
3. Results and Discussion
3.1. Optimization of the Electrospinning Parameters
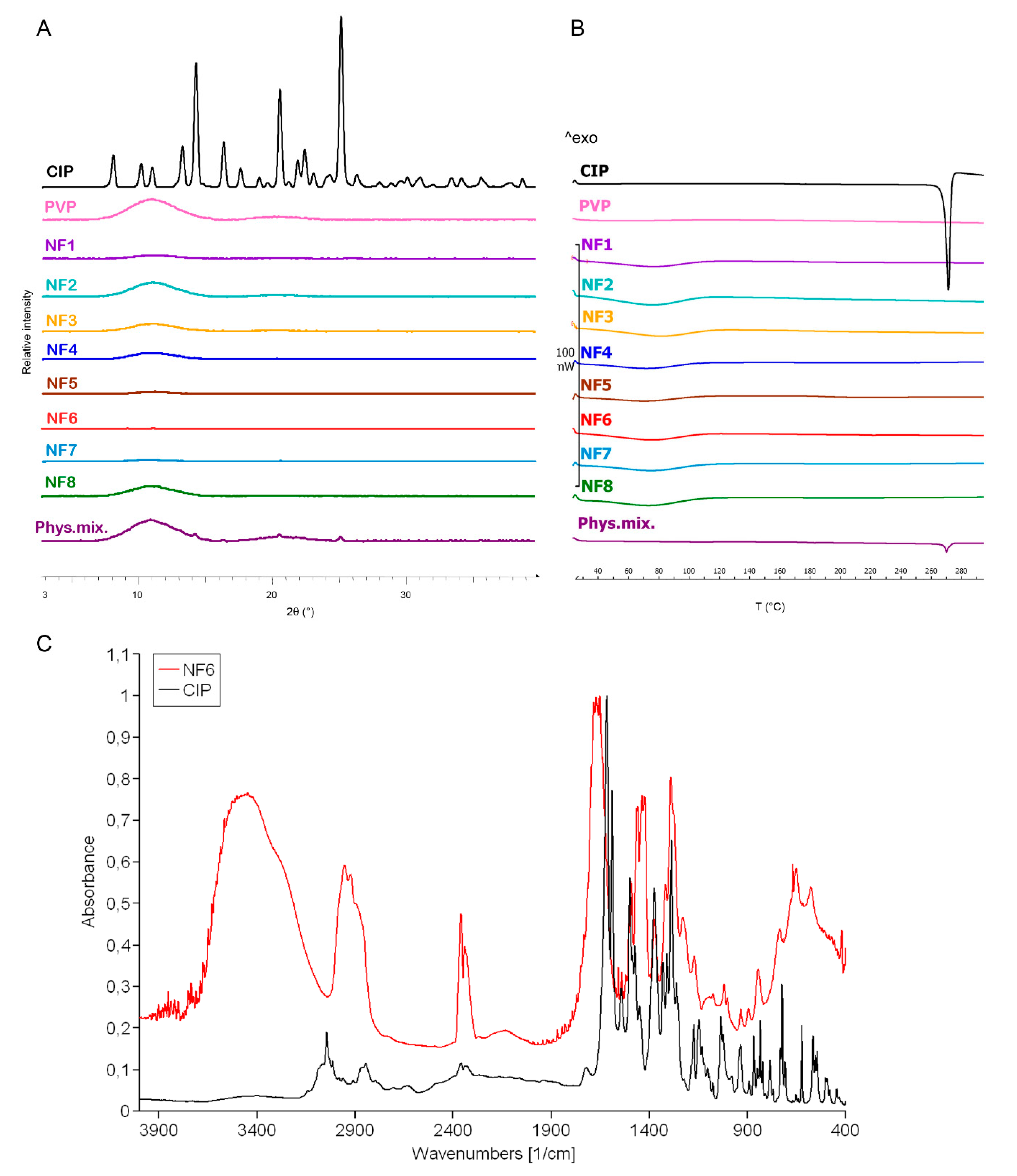
3.2. Structural Characterization
3.3. Drug Loading and Drug Entrapment Efficiency
3.4. Solubility Test
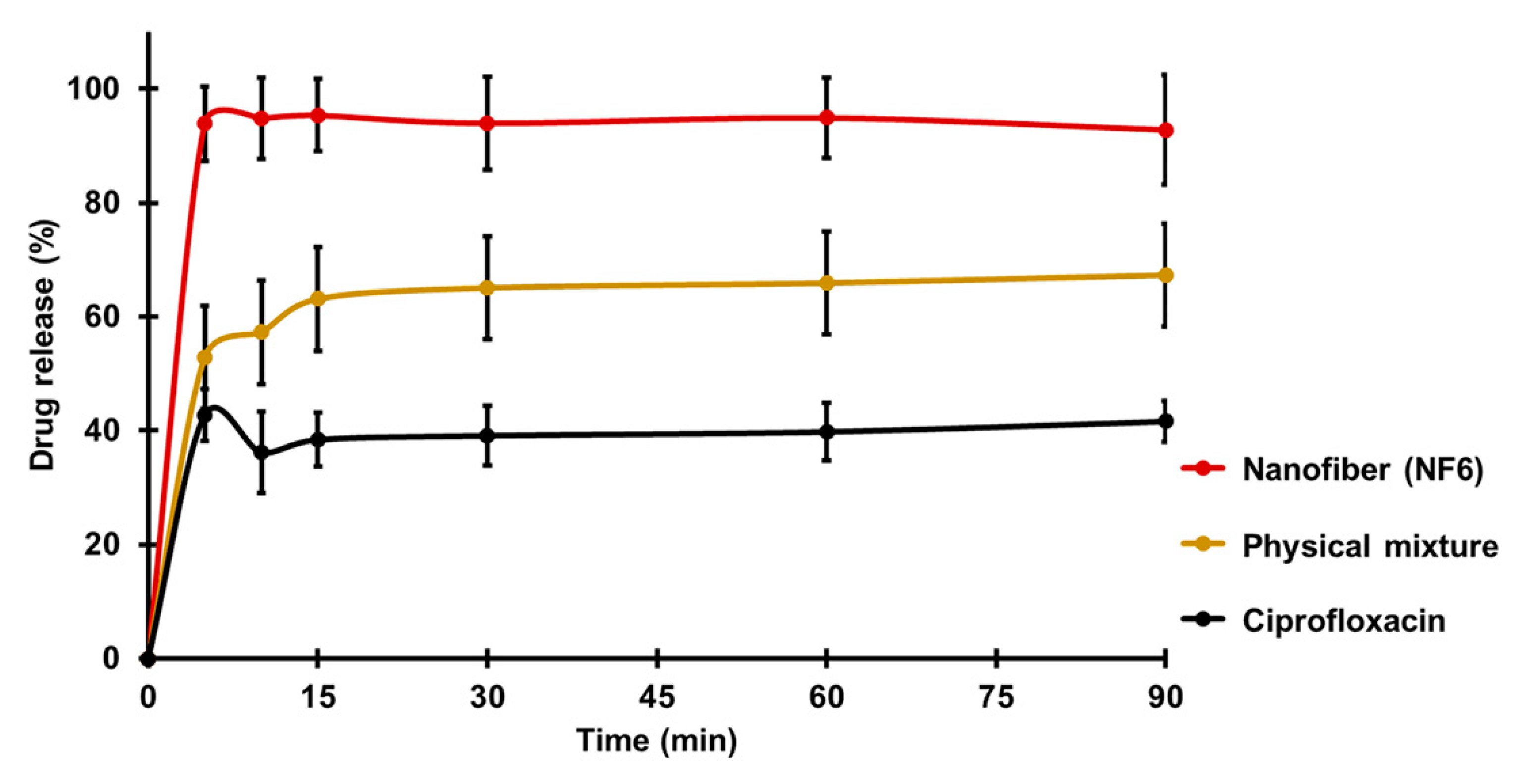
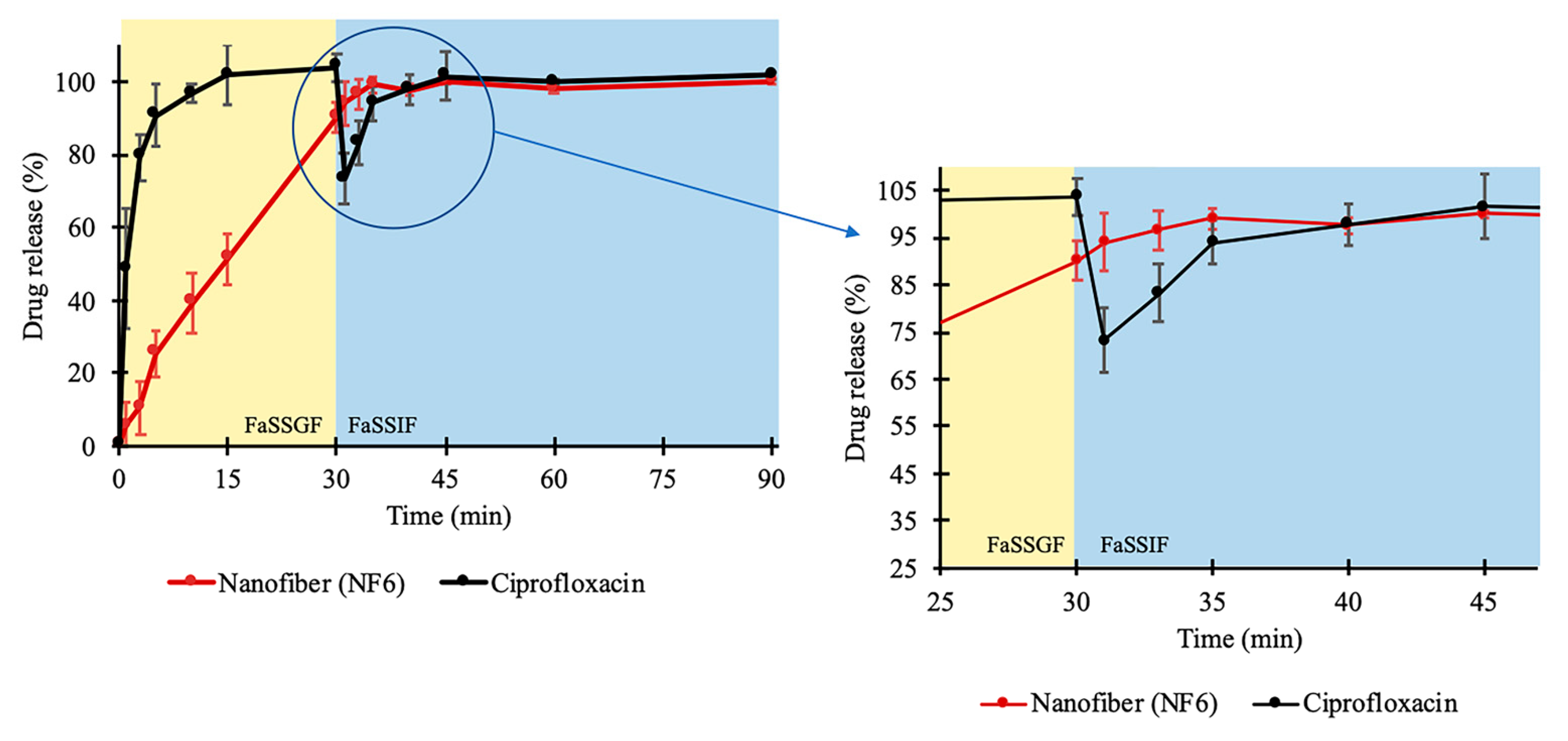
3.5. In Vitro Drug Release
3.6. Drug-Release Kinetics and Mechanism
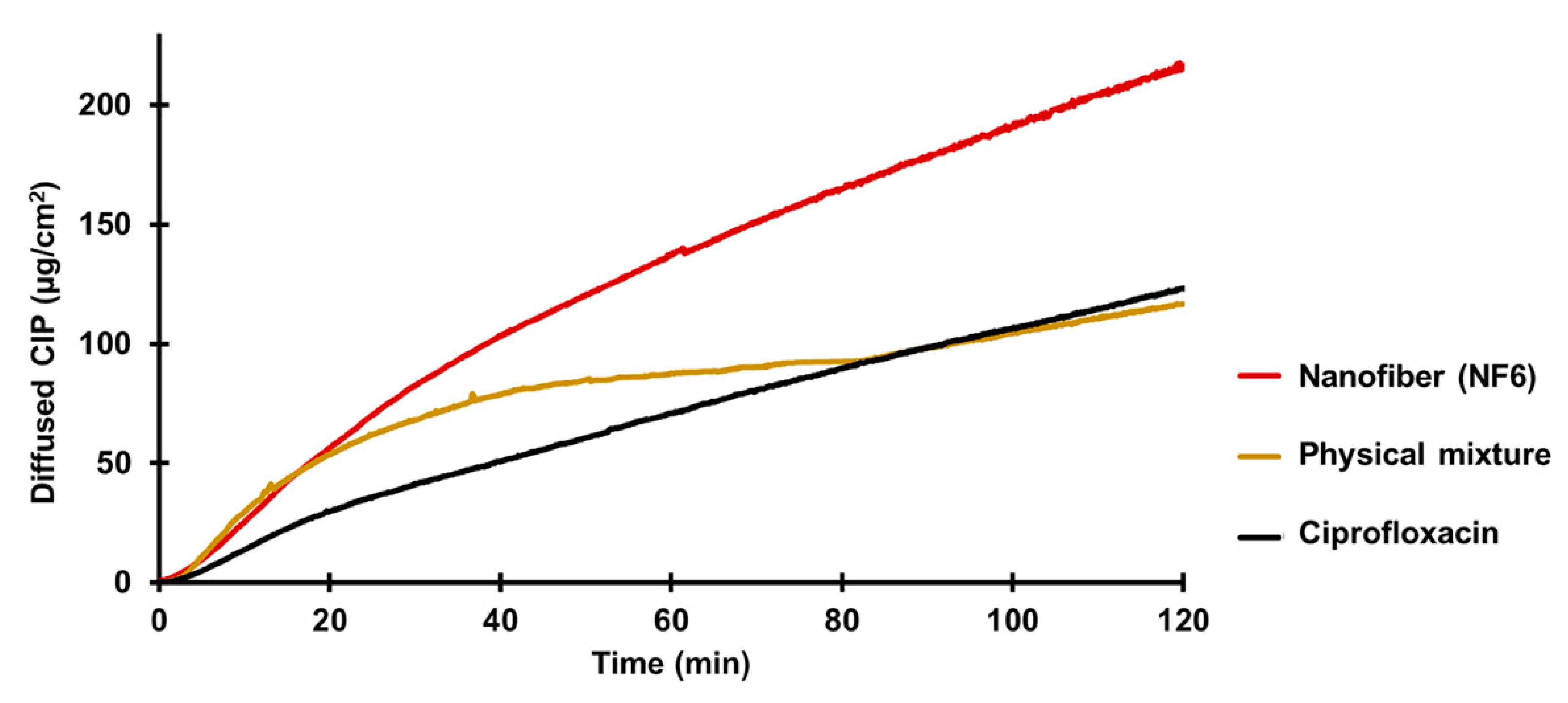
3.7. In Vitro Diffusion Study
4. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Di, L.; Kerns, E.; Carter, G. Drug-Like Property Concepts in Pharmaceutical Design. Curr. Pharm. Des. 2009, 15, 2184–2194. [Google Scholar] [CrossRef]
- Williams, H.D.; Trevaskis, N.L.; Charman, S.A.; Shanker, R.M.; Charman, W.N.; Pouton, C.W.; Porter, C.J.H. Strategies to Address Low Drug Solubility in Discovery and Development. Pharmacol. Rev. 2013, 65, 315–499. [Google Scholar] [CrossRef] [PubMed]
- Loftsson, T.; Brewster, M.E. Pharmaceutical Applications of Cyclodextrins: Basic Science and Product Development: Pharmaceutical Applications of Cyclodextrins. J. Pharm. Pharmacol. 2010, 62, 1607–1621. [Google Scholar] [CrossRef] [PubMed]
- Olivera, M.E.; Manzo, R.H.; Junginger, H.E.; Midha, K.K.; Shah, V.P.; Stavchansky, S.; Dressman, J.B.; Barends, D.M. Biowaiver Monographs for Immediate Release Solid Oral Dosage Forms: Ciprofloxacin Hydrochloride. J. Pharm. Sci. 2011, 100, 22–33. [Google Scholar] [CrossRef]
- Ross, D.; Riley, C. Aqueous Solubilities of Some Variously Substituted Quinolone Antimicrobials. Int. J. Pharm. 1990, 63, 237–250. [Google Scholar] [CrossRef]
- Caço, A.I.; Varanda, F.; Pratas de Melo, M.J.; Dias, A.M.A.; Dohrn, R.; Marrucho, I.M. Solubility of Antibiotics in Different Solvents. Part II. Non-Hydrochloride Forms of Tetracycline and Ciprofloxacin. Ind. Eng. Chem. Res. 2008, 47, 8083–8089. [Google Scholar] [CrossRef]
- Radacsi, N.; Ambrus, R.; Szabó-Révész, P.; van der Heijden, A.; ter Horst, J.H. Atmospheric Pressure Cold Plasma Synthesis of Submicrometer-Sized Pharmaceuticals with Improved Physicochemical Properties. Cryst. Growth Des. 2012, 12, 5090–5095. [Google Scholar] [CrossRef]
- Kariminia, S.; Shamsipur, A.; Shamsipur, M. Analytical Characteristics and Application of Novel Chitosan Coated Magnetic Nanoparticles as an Efficient Drug Delivery System for Ciprofloxacin. Enhanced Drug Release Kinetics by Low-Frequency Ultrasounds. J. Pharm. Biomed. Anal. 2016, 129, 450–457. [Google Scholar] [CrossRef]
- Zattoni, A. Flow Field-Flow Fractionation for the Analysis of Nanoparticles Used in Drug Delivery. J. Pharm. Biomed. Anal. 2014, 87, 53–61. [Google Scholar] [CrossRef] [PubMed]
- Jermain, S.V.; Brough, C.; Williams, R.O. Amorphous Solid Dispersions and Nanocrystal Technologies for Poorly Water-Soluble Drug Delivery—An Update. Int. J. Pharm. 2018, 535, 379–392. [Google Scholar] [CrossRef]
- Ogawa, N.; Hiramatsu, T.; Suzuki, R.; Okamoto, R.; Shibagaki, K.; Fujita, K.; Takahashi, C.; Kawashima, Y.; Yamamoto, H. Improvement in the Water Solubility of Drugs with a Solid Dispersion System by Spray Drying and Hot-Melt Extrusion with Using the Amphiphilic Polyvinyl Caprolactam-Polyvinyl Acetate-Polyethylene Glycol Graft Copolymer and d-Mannitol. Eur. J. Pharm. Sci. 2018, 111, 205–214. [Google Scholar] [CrossRef] [PubMed]
- Kumar, R. Nanotechnology Based Approaches to Enhance Aqueous Solubility and Bioavailability of Griseofulvin: A Literature Survey. J. Drug Deliv. Sci. Technol. 2019, 53, 101221. [Google Scholar] [CrossRef]
- Murdande, S.B.; Pikal, M.J.; Shanker, R.M.; Bogner, R.H. Solubility Advantage of Amorphous Pharmaceuticals: II. Application of Quantitative Thermodynamic Relationships for Prediction of Solubility Enhancement in Structurally Diverse Insoluble Pharmaceuticals. Pharm. Res. 2010, 27, 2704–2714. [Google Scholar] [CrossRef] [PubMed]
- Horter, D.; Dressman, J.B. Influence of Physicochemical Properties on Dissolution of Drugs in the Gastrointestinal Tractq. Adv. Drug Deliv. Rev. 2001, 46, 75–87. [Google Scholar] [PubMed]
- Günday, C.; Anand, S.; Gencer, H.B.; Munafò, S.; Moroni, L.; Fusco, A.; Donnarumma, G.; Ricci, C.; Hatir, P.C.; Türeli, N.G.; et al. Ciprofloxacin-Loaded Polymeric Nanoparticles Incorporated Electrospun Fibers for Drug Delivery in Tissue Engineering Applications. Drug Deliv. Transl. Res. 2020, 10, 706–720. [Google Scholar] [CrossRef] [PubMed]
- Arafa, M.G.; Mousa, H.A.; Afifi, N.N. Preparation of PLGA-Chitosan Based Nanocarriers for Enhancing Antibacterial Effect of Ciprofloxacin in Root Canal Infection. Drug Deliv. 2020, 27, 26–39. [Google Scholar] [CrossRef] [PubMed]
- Benedini, L.; Laiuppa, J.; Santillán, G.; Baldini, M.; Messina, P. Antibacterial Alginate/Nano-Hydroxyapatite Composites for Bone Tissue Engineering: Assessment of Their Bioactivity, Biocompatibility, and Antibacterial Activity. Mater. Sci. Eng. C 2020, 115, 111101. [Google Scholar] [CrossRef]
- Mocanu, A.-G.; Belu, I. Formulation and Characterization of Ciprofloxacin Loaded PLGA Microspheres for Applications in Orthopedic Infections. Curr. Health Sci. J. 2017, 43, 306–310. [Google Scholar] [CrossRef]
- Lamy, B.; Tewes, F.; Serrano, D.R.; Lamarche, I.; Gobin, P.; Couet, W.; Healy, A.M.; Marchand, S. New Aerosol Formulation to Control Ciprofloxacin Pulmonary Concentration. J. Control. Release 2018, 271, 118–126. [Google Scholar] [CrossRef]
- Khatib, I.; Tang, P.; Ruan, J.; Cipolla, D.; Dayton, F.; Blanchard, J.D.; Chan, H.-K. Formation of Ciprofloxacin Nanocrystals within Liposomes by Spray Drying for Controlled Release via Inhalation. Int. J. Pharm. 2020, 578, 119045. [Google Scholar] [CrossRef]
- Torge, A. Ciprofloxacin-Loaded Lipid-Core Nanocapsules as Mucus Penetrating Drug Delivery System Intended for the Treatment of Bacterial Infections in Cystic Fibrosis. Int. J. Pharm. 2017, 527, 92–102. [Google Scholar] [CrossRef]
- Tran, T.-T.; Vidaillac, C.; Yu, H.; Yong, V.F.L.; Roizman, D.; Chandrasekaran, R.; Lim, A.Y.H.; Low, T.B.; Tan, G.L.; Abisheganaden, J.A.; et al. A New Therapeutic Avenue for Bronchiectasis: Dry Powder Inhaler of Ciprofloxacin Nanoplex Exhibits Superior Ex Vivo Mucus Permeability and Antibacterial Efficacy to Its Native Ciprofloxacin Counterpart. Int. J. Pharm. 2018, 547, 368–376. [Google Scholar] [CrossRef]
- Rancan, F.; Contardi, M.; Jurisch, J.; Blume-Peytavi, U.; Vogt, A.; Bayer, I.S.; Schaudinn, C. Schaudinn Evaluation of Drug Delivery and Efficacy of Ciprofloxacin-Loaded Povidone Foils and Nanofiber Mats in a Wound-Infection Model Based on Ex Vivo Human Skin. Pharmaceutics 2019, 11, 527. [Google Scholar] [CrossRef]
- Yang, S.; Zhang, X.; Zhang, D. Electrospun Chitosan/Poly (Vinyl Alcohol)/Graphene Oxide Nanofibrous Membrane with Ciprofloxacin Antibiotic Drug for Potential Wound Dressing Application. Int. J. Mol. Sci. 2019, 20, 4395. [Google Scholar] [CrossRef] [PubMed]
- Paaver, U.; Heinämäki, J.; Laidmäe, I.; Lust, A.; Kozlova, J.; Sillaste, E.; Kirsimäe, K.; Veski, P.; Kogermann, K. Electrospun Nanofibers as a Potential Controlled-Release Solid Dispersion System for Poorly Water-Soluble Drugs. Int. J. Pharm. 2015, 479, 252–260. [Google Scholar] [CrossRef] [PubMed]
- Sipos, E.; Kósa, N.; Kazsoki, A.; Szabó, Z.-I.; Zelkó, R. Formulation and Characterization of Aceclofenac-Loaded Nanofiber Based Orally Dissolving Webs. Pharmaceutics 2019, 11, 417. [Google Scholar] [CrossRef] [PubMed]
- Villarreal-Gómez, L.J.; Cornejo-Bravo, J.M.; Vera-Graziano, R.; Grande, D. Electrospinning as a Powerful Technique for Biomedical Applications: A Critically Selected Survey. J. Biomater. Sci. Polym. Ed. 2016, 27, 157–176. [Google Scholar] [CrossRef] [PubMed]
- Ambekar, R.S.; Kandasubramanian, B. Advancements in Nanofibers for Wound Dressing: A Review. Eur. Polym. J. 2019, 117, 304–336. [Google Scholar] [CrossRef]
- Barhoum, A.; Pal, K.; Rahier, H.; Uludag, H.; Kim, I.S.; Bechelany, M. Nanofibers as New-Generation Materials: From Spinning and Nano-Spinning Fabrication Techniques to Emerging Applications. Appl. Mater. Today 2019, 17, 1–35. [Google Scholar] [CrossRef]
- Khodadadi, M.; Alijani, S.; Montazeri, M.; Esmaeilizadeh, N.; Sadeghi-Soureh, S.; Pilehvar-Soltanahmadi, Y. Recent Advances in Electrospun Nanofiber -mediated Drug Delivery Strategies for Localized Cancer Chemotherapy. J. Biomed. Mater. Res. A 2020, 108, 1444–1458. [Google Scholar] [CrossRef]
- Udomluck, N.; Koh, W.-G.; Lim, D.-J.; Park, H. Recent Developments in Nanofiber Fabrication and Modification for Bone Tissue Engineering. Int. J. Mol. Sci. 2019, 21, 99. [Google Scholar] [CrossRef]
- Park, S.; Park, K.; Yoon, H.; Son, J.; Min, T.; Kim, G. Apparatus for Preparing Electrospun Nanofibers: Designing an Electrospinning Process for Nanofiber Fabrication. Polym. Int. 2007, 56, 1361–1366. [Google Scholar] [CrossRef]
- Motamedi, A.S.; Mirzadeh, H.; Hajiesmaeilbaigi, F.; Bagheri-Khoulenjani, S.; Shokrgozar, M. Effect of Electrospinning Parameters on Morphological Properties of PVDF Nanofibrous Scaffolds. Prog. Biomater. 2017, 6, 113–123. [Google Scholar] [CrossRef]
- Pelipenko, J.; Kristl, J.; Janković, B.; Baumgartner, S.; Kocbek, P. The Impact of Relative Humidity during Electrospinning on the Morphology and Mechanical Properties of Nanofibers. Int. J. Pharm. 2013, 456, 125–134. [Google Scholar] [CrossRef] [PubMed]
- Sun, Y.; Zhu, L.; Wu, T.; Cai, T.; Gunn, E.M.; Yu, L. Stability of Amorphous Pharmaceutical Solids: Crystal Growth Mechanisms and Effect of Polymer Additives. AAPS J. 2012, 14, 380–388. [Google Scholar] [CrossRef]
- Yu, D.-G.; Zhang, X.-F.; Shen, X.-X.; Brandford-White, C.; Zhu, L.-M. Ultrafine Ibuprofen-Loaded Polyvinylpyrrolidone Fiber Mats Using Electrospinning: Ultrafine Ibuprofen-Loaded PVP Fibers. Polym. Int. 2009, 58, 1010–1013. [Google Scholar] [CrossRef]
- Suganya, S.; Senthil Ram, T.; Lakshmi, B.S.; Giridev, V.R. Herbal Drug Incorporated Antibacterial Nanofibrous Mat Fabricated by Electrospinning: An Excellent Matrix for Wound Dressings. J. Appl. Polym. Sci. 2011, 121, 2893–2899. [Google Scholar] [CrossRef]
- Quan, J.; Yu, Y.; Branford-White, C.; Williams, G.R.; Yu, D.-G.; Nie, W.; Zhu, L.-M. Preparation of Ultrafine Fast-Dissolving Feruloyl-Oleyl-Glycerol-Loaded Polyvinylpyrrolidone Fiber Mats via Electrospinning. Colloids Surf. B Biointerfaces 2011, 88, 304–309. [Google Scholar] [CrossRef] [PubMed]
- Dai, X.-Y.; Nie, W.; Wang, Y.-C.; Shen, Y.; Li, Y.; Gan, S.-J. Electrospun Emodin Polyvinylpyrrolidone Blended Nanofibrous Membrane: A Novel Medicated Biomaterial for Drug Delivery and Accelerated Wound Healing. J. Mater. Sci. Mater. Med. 2012, 23, 2709–2716. [Google Scholar] [CrossRef]
- Jiang, Y.-N.; Mo, H.-Y.; Yu, D.-G. Electrospun Drug-Loaded Core–Sheath PVP/Zein Nanofibers for Biphasic Drug Release. Int. J. Pharm. 2012, 438, 232–239. [Google Scholar] [CrossRef]
- Contardi, M.; Heredia-Guerrero, J.A.; Perotto, G.; Valentini, P.; Pompa, P.P.; Spanò, R.; Goldoni, L.; Bertorelli, R.; Athanassiou, A.; Bayer, I.S. Transparent Ciprofloxacin-Povidone Antibiotic Films and Nanofiber Mats as Potential Skin and Wound Care Dressings. Eur. J. Pharm. Sci. 2017, 104, 133–144. [Google Scholar] [CrossRef]
- Radacsi, N.; Campos, F.D.; Chisholm, C.R.I.; Giapis, K.P. Spontaneous Formation of Nanoparticles on Electrospun Nanofibres. Nat. Commun. 2018, 9, 4740. [Google Scholar] [CrossRef] [PubMed]
- He, P.; Zhong, Q.; Ge, Y.; Guo, Z.; Tian, J.; Zhou, Y.; Ding, S.; Li, H.; Zhou, C. Dual Drug Loaded Coaxial Electrospun PLGA/PVP Fiber for Guided Tissue Regeneration under Control of Infection. Mater. Sci. Eng. C 2018, 90, 549–556. [Google Scholar] [CrossRef] [PubMed]
- Li, H.; Zhang, Z.; Godakanda, V.U.; Chiu, Y.-J.; Angkawinitwong, U.; Patel, K.; Stapleton, P.G.; de Silva, R.M.; de Silva, K.M.N.; Zhu, L.-M.; et al. The Effect of Collection Substrate on Electrospun Ciprofloxacin-Loaded Poly(Vinylpyrrolidone) and Ethyl Cellulose Nanofibers as Potential Wound Dressing Materials. Mater. Sci. Eng. C 2019, 104, 109917. [Google Scholar] [CrossRef]
- Franco, P.; De Marco, I. The Use of Poly(N-Vinyl Pyrrolidone) in the Delivery of Drugs: A Review. Polymers 2020, 12, 1114. [Google Scholar] [CrossRef] [PubMed]
- Mann, J.; Dressman, J.; Rosenblatt, K.; Ashworth, L.; Muenster, U.; Frank, K.; Hutchins, P.; Williams, J.; Klumpp, L.; Wielockx, K.; et al. Validation of Dissolution Testing with Biorelevant Media: An OrBiTo Study. Mol. Pharm. 2017, 14, 4192–4201. [Google Scholar] [CrossRef]
- Sang, Q.; Williams, G.R.; Wu, H.; Liu, K.; Li, H.; Zhu, L.-M. Electrospun Gelatin/Sodium Bicarbonate and Poly(Lactide-Co-ε-Caprolactone)/Sodium Bicarbonate Nanofibers as Drug Delivery Systems. Mater. Sci. Eng. C 2017, 81, 359–365. [Google Scholar] [CrossRef]
- Yan, S.; Xiaoqiang, L.; Shuiping, L.; Xiumei, M.; Ramakrishna, S. Controlled Release of Dual Drugs from Emulsion Electrospun Nanofibrous Mats. Colloids Surf. B Biointerfaces 2009, 73, 376–381. [Google Scholar] [CrossRef]
- Cleeton, C.; Keirouz, A.; Chen, X.; Radacsi, N. Electrospun Nanofibers for Drug Delivery and Biosensing. ACS Biomater. Sci. Eng. 2019, 5, 4183–4205. [Google Scholar] [CrossRef]
- Radacsi, N.; Giapis, K.P.; Ovari, G.; Szabó-Révész, P.; Ambrus, R. Electrospun Nanofiber-Based Niflumic Acid Capsules with Superior Physicochemical Properties. J. Pharm. Biomed. Anal. 2019, 166, 371–378. [Google Scholar] [CrossRef]
- Karimi, K.; Pallagi, E.; Szabó-Révész, P.; Csóka, I.; Ambrus, R. Development of a Microparticle-Based Dry Powder Inhalation Formulation of Ciprofloxacin Hydrochloride Applying the Quality by Design Approach. Drug Des. Devel. Ther. 2016, 10, 3331–3343. [Google Scholar] [CrossRef] [PubMed]
- Kataria, K.; Gupta, A.; Rath, G.; Mathur, R.B.; Dhakate, S.R. In Vivo Wound Healing Performance of Drug Loaded Electrospun Composite Nanofibers Transdermal Patch. Int. J. Pharm. 2014, 469, 102–110. [Google Scholar] [CrossRef]
- Fallingborg, J. Intraluminal PH of the Human Gastrointestinal Tract. Dan. Med. Bull. 1999, 46, 183–196. [Google Scholar] [PubMed]
- Hansmann, S.; Miyaji, Y.; Dressman, J. An in Silico Approach to Determine Challenges in the Bioavailability of Ciprofloxacin, a Poorly Soluble Weak Base with Borderline Solubility and Permeability Characteristics. Eur. J. Pharm. Biopharm. 2018, 122, 186–196. [Google Scholar] [CrossRef] [PubMed]
- Permanadewi, I.; Kumoro, A.C.; Wardhani, D.H.; Aryanti, N. Modelling of Controlled Drug Release in Gastrointestinal Tract Simulation. J. Phys. Conf. Ser. 2019, 1295, 012063. [Google Scholar] [CrossRef]
- Supramaniam, J.; Adnan, R.; Mohd Kaus, N.H.; Bushra, R. Magnetic Nanocellulose Alginate Hydrogel Beads as Potential Drug Delivery System. Int. J. Biol. Macromol. 2018, 118, 640–648. [Google Scholar] [CrossRef] [PubMed]
- Harder, S.; Fuhr, U.; Beermann, D.; Staib, A. Ciprofloxacin Absorption in Different Regions of the Human Gastrointestinal Tract. Investigations with the Hf-Capsule. Br. J. Clin. Pharmacol. 1990, 30, 35–39. [Google Scholar] [CrossRef] [PubMed]
- Calonge, M.L.; Ilundáin, A. Na+-H+ Exchange Activity and Cellular PH Regulation in Enterocytes Isolated from Chick Small Intestine. Biochim. Biophys. Acta BBA Biomembr. 1990, 1029, 201–210. [Google Scholar] [CrossRef]

| Type of Nanocarrier | Excipients Applied in Nanocarrier | Aimed Indications | Targeted Organs | References |
|---|---|---|---|---|
| Polymeric nanoparticles (NP) in nanofibers (NF) | PLGA and PCL—NP PEOT/PBT—NF | tissue engineering | middle ear | [15] |
| Nanoparticles and coated nanoparticles | PLGA and chitosan (coat) | root canal infection | tooth | [16] |
| Composite nanoparticles | synthetic nano-HA and sodium alginate | tissue engineering | bone | [17] |
| Microspheres | PLGA | osteomyelitis, orthopedic infections | bone | [18] |
| Microparticles | calcium carbonate, sodium hyaluronate | lung infections | lungs | [19] |
| Nanocrystals inside liposomes | HSPC, cholesterol | lung infections | lungs | [20] |
| Amorphous nanoparticle complex | dextran sulfate | non-cystic fibrosis bronchiectasis | lungs | [21] |
| Lipid-core nanocapsules | PCL, sorbitan monostearate, oleic acid, polysorbate 80 | cystic fibrosis | lungs | [22] |
| Nanofibers | PVP | wound infections | skin | [23] |
| Nanofibers | PVA, chitosan, graphene oxide | wound infections | skin | [24] |
| Sample | PVP Solution (w/v %) | PVP:CIP (v/v) | Flow Rate (mL/h) |
|---|---|---|---|
| NF1 | 5 | 1:0 | 2 |
| NF2 | 20 | 1:3 | 2 |
| NF3 | 15 | 1:2 | 2 |
| NF4 | 10 | 1:1 | 0.5 |
| NF5 | 10 | 1:1 | 1 |
| NF6 | 10 | 1:1 | 2 |
| NF7 | 10 | 1:1 | 3 |
| NF8 | 10 | 1:1 | 4 |
| Sample | Fiber Morphology | Average Diameter (nm) | |
|---|---|---|---|
| NF1 | continuous | smooth | 815 ± 216 |
| NF2 | continuous | smooth | 787 ± 140 |
| NF3 | discontinuous | worm-like | 889 ± 265 |
| NF4 | continuous | smooth | 542 ± 103 |
| NF5 | continuous | smooth | 601 ± 87 |
| NF6 | continuous | smooth | 645 ± 82 |
| NF7 | continuous | smooth | 663 ± 79 |
| NF8 | continuous | rough | 718 ± 105 |
| Sample | NF1 | NF2 | NF3 | NF4 | NF5 | NF6 | NF7 | NF8 |
|---|---|---|---|---|---|---|---|---|
| NF1 | - | 1.77 | 4.54 * | 15.47 ** | 12.54 ** | 9.91 ** | 7.88 ** | 4.31 * |
| NF2 | 1.77 | - | 6.45 ** | 14.24 ** | 11.21 ** | 8.51 ** | 6.58 ** | 3.12 |
| NF3 | 4.54 * | 6.45 ** | - | 19.67 ** | 16.88 ** | 14.21 ** | 11.69 ** | 7.58 ** |
| NF4 | 15.47 ** | 14.24 ** | 19.67 ** | - | 3.19 | 5.53 ** | 5.85 ** | 7.46 ** |
| NF5 | 12.54 ** | 11.21 ** | 16.88 ** | 3.19 | - | 2.43 | 3.07 | 5.05 ** |
| NF6 | 9.91 ** | 8.51 ** | 14.21 ** | 5.53 ** | 2.43 | - | 0.88 | 3.15 |
| NF7 | 7.88 ** | 6.58 ** | 11.69 ** | 5.85 ** | 3.07 | 0.88 | - | 2.23 |
| NF8 | 4.31 * | 3.12 | 7.58 ** | 7.46 ** | 5.05 ** | 3.15 | 2.23 | - |

| Release Study | Single Medium (pH 7.4 PBS) | Two-Stage Biorelevant (FaSSGF) | Two-Stage Biorelevant (FaSSIF) | ||||
|---|---|---|---|---|---|---|---|
| Sample | CIP | Physical Mixture | Nanofiber (NF6) | CIP | Nanofiber (NF6) | CIP | Nanofiber (NF6) |
| Zero order | 0.3270 | 0.2955 | 0.6122 | 0.5820 | 0.9810 | 0.2687 | 0.2344 |
| Fist order | 0.8463 | 0.6565 | 0.9807 | 0.9085 | 0.9602 | 0.9276 | 0.9268 |
| Hixson–Crowell | 0.3449 | 0.3540 | 0.6431 | 0.9204 | 0.9873 | 0.6452 | 0.5282 |
| Higuchi | 0.8908 | 0.8632 | 0.9577 | 0.9502 | 0.9616 | 0.8273 | 0.8304 |
| Korsmeyer–Peppas | 0.8967 | 0.8684 | 0.9993 | 0.8895 | 0.9794 | 0.8717 | 0.9229 |
| Sample | J (µg/(cm2 h)) | Kp (cm/h) |
|---|---|---|
| CIP | 60.94 | 0.112 |
| Physical mixture | 58.80 | 0.105 |
| Nanofiber (NF6) | 107.71 | 0.217 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Uhljar, L.É.; Kan, S.Y.; Radacsi, N.; Koutsos, V.; Szabó-Révész, P.; Ambrus, R. In Vitro Drug Release, Permeability, and Structural Test of Ciprofloxacin-Loaded Nanofibers. Pharmaceutics 2021, 13, 556. https://doi.org/10.3390/pharmaceutics13040556
Uhljar LÉ, Kan SY, Radacsi N, Koutsos V, Szabó-Révész P, Ambrus R. In Vitro Drug Release, Permeability, and Structural Test of Ciprofloxacin-Loaded Nanofibers. Pharmaceutics. 2021; 13(4):556. https://doi.org/10.3390/pharmaceutics13040556
Chicago/Turabian StyleUhljar, Luca Éva, Sheng Yuan Kan, Norbert Radacsi, Vasileios Koutsos, Piroska Szabó-Révész, and Rita Ambrus. 2021. "In Vitro Drug Release, Permeability, and Structural Test of Ciprofloxacin-Loaded Nanofibers" Pharmaceutics 13, no. 4: 556. https://doi.org/10.3390/pharmaceutics13040556
APA StyleUhljar, L. É., Kan, S. Y., Radacsi, N., Koutsos, V., Szabó-Révész, P., & Ambrus, R. (2021). In Vitro Drug Release, Permeability, and Structural Test of Ciprofloxacin-Loaded Nanofibers. Pharmaceutics, 13(4), 556. https://doi.org/10.3390/pharmaceutics13040556