Penetration Enhancers for Topical Drug Delivery to the Ocular Posterior Segment—A Systematic Review
Abstract
1. Introduction
2. Materials and Methods
2.1. Review Process
2.2. Literature Search
2.3. Inclusion and Exclusion Criteria
2.4. Risk of Publication Bias
2.5. Data Extraction
3. Results
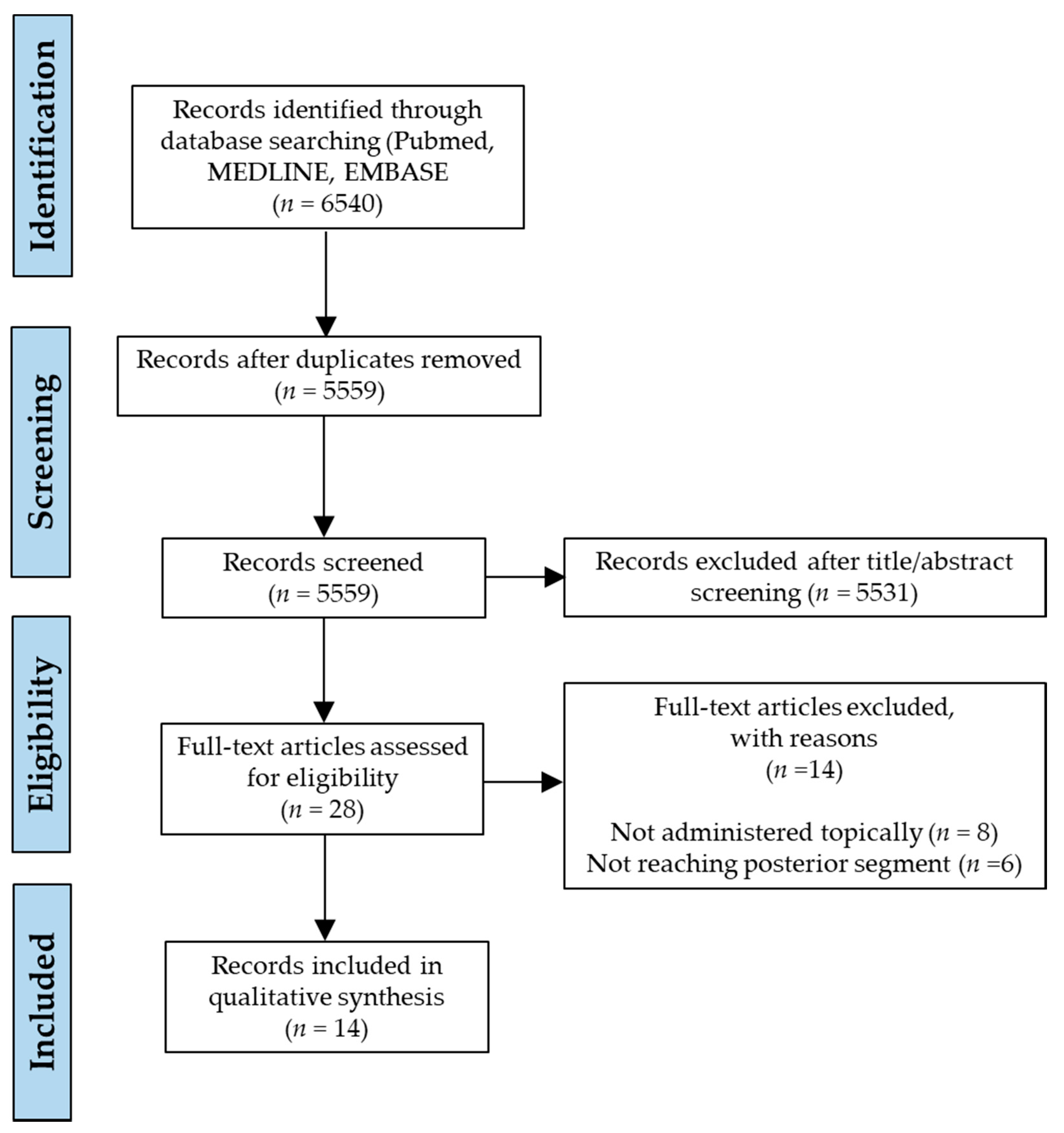
3.1. Study Selection
3.1.1. TAT
3.1.2. Penetratin
3.1.3. Other CPPs
3.2. Chitosan
3.3. Benzalkonium Chloride (BAC)
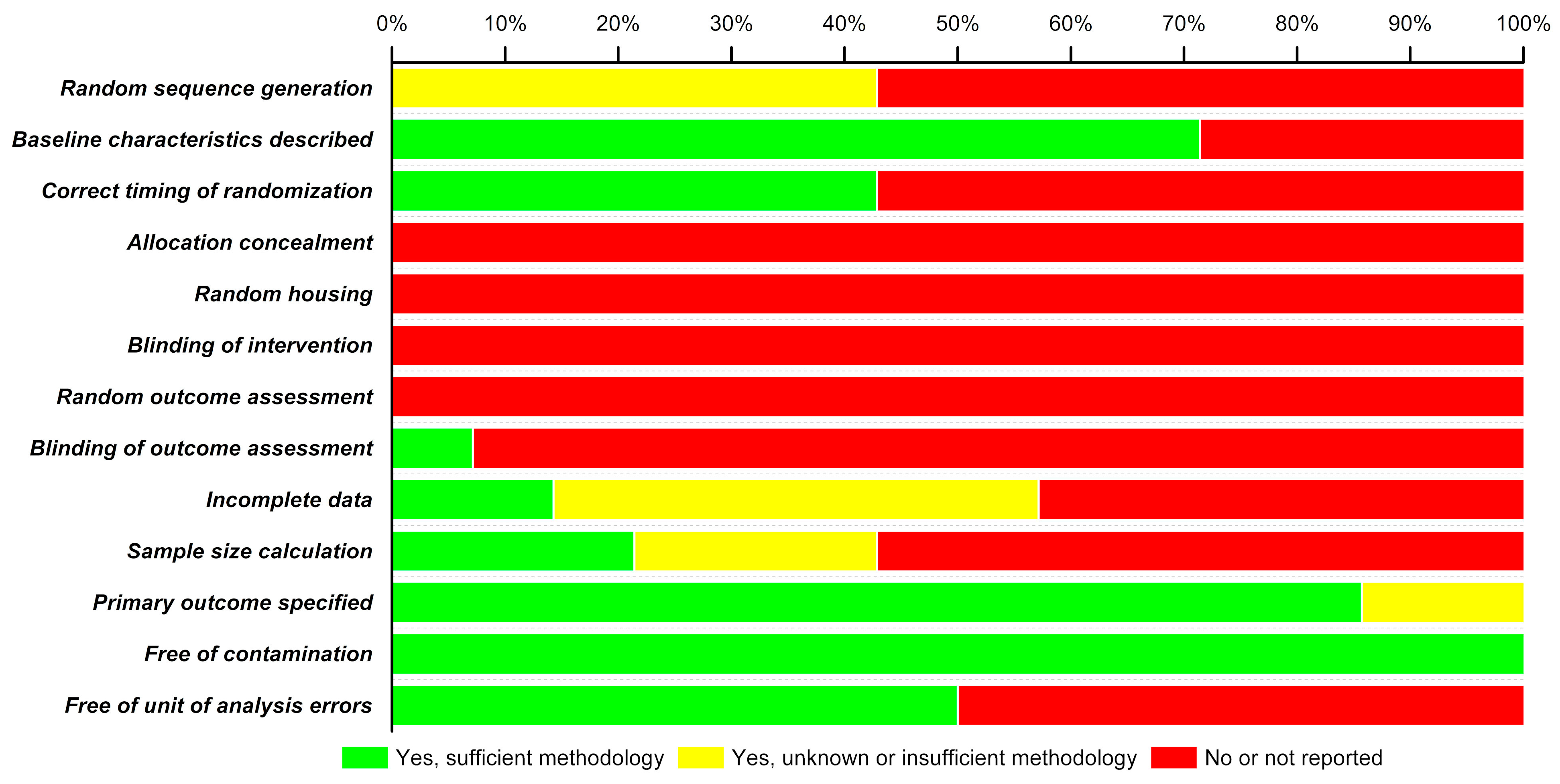
3.4. Risk of Bias (RoB)
4. Discussion
Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
| aFGF | human acidic fibroblast growth factor; |
| AMD | age-related macular degeneration; |
| ARPE-19 | human retinal pigment epithelial cell line; |
| BAB | blood-aqueous barrier; |
| BAC | benzalkonium chloride; |
| BBB | blood-brain barrier; |
| BRB | blood-retina barrier; |
| CD | cyclodextrin; |
| CMCS | carboxymethyl chitosan; |
| CNV | choroidal neovascularization; |
| CPP | cell penetrating peptide; |
| DEX | dexamethasone; |
| DME | diabetic macular edema; |
| DR | diabetic retinopathy; |
| EDTA | Ethylenediaminetetraacetic acid; |
| ELISA | enzyme-linked immunosorbent assay; |
| Es | endostatin; |
| EtE | efficiency for traversing eye to retina; |
| FA | fluorescein angiography; |
| GCL | ganglion cell layer; |
| HA | hyaluronic acid; |
| HCEC | human corneal epithelial cells; |
| HIV | human immunodeficiency virus; |
| HPLC | high performance liquid chromatography; |
| HUVEC | human umbilical vein endothelial cells; |
| IC50 | half maximal inhibitory concentration; |
| IHC | immunohistochemistry; |
| ILM | inner limiting membrane; |
| INL | inner nuclear layer; |
| IPL | inner plexiform layer; |
| IR | ischemia–reperfusion; |
| MTT | 3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyl tetrazolium bromide; |
| HConEpic | human conjunctival epithelial cells; |
| OCT | optical coherence tomography; |
| OIR | oxygen-induced retinopathy; |
| ONL | outer nuclear layer; |
| OPL | outer plexiform layer; |
| PACAP | pituitary adenylate cyclase activating polypeptide; |
| PAMAM | poly(amidoamine); |
| PE | penetration enhancer; |
| PEG | polyethylene glycol; |
| PLGA | poly(lactic-co-glycolic acid); |
| POD | peptide for ocular delivery; |
| PPII | polyproline type II; |
| pRFP | red fluorescent protein plasmid; |
| PRISMA | preferred reporting items for systematic reviews and meta-analyses; |
| PTD | protein transduction domain; |
| RCT | randomized controlled trial; |
| RGC | retinal ganglion cells; |
| RGD | arginine-glycine-aspartic; |
| RNV | retinal neovascularization; |
| RoB | risk of bias; |
| RPE | retinal pigment epithelium; |
| TAT | transactivator of transcription; |
| TUNEL | terminal deoxynucleotidyl transferase dUTP nick end labelling; |
| VEGF | vascular endothelial growth factor; |
| VIP | vasoactive intestinal peptide. |
References
- World Health Organization. World Report on Vision; World Health Organization: Geneva, Switzerland, 2019; Volume 214, ISBN 9789241516570. [Google Scholar]
- Prokofyeva, E.; Zrenner, E. Epidemiology of Major Eye Diseases Leading to Blindness in Europe: A Literature Review. Ophthalmic Res. 2012, 47, 171–188. [Google Scholar] [CrossRef] [PubMed]
- Wong, W.L.; Su, X.; Li, X.; Cheung, C.M.G.; Klein, R.; Cheng, C.Y.; Wong, T.Y. Global Prevalence of Age-Related Macular Degeneration and Disease Burden Projection for 2020 and 2040: A Systematic Review and Meta-Analysis. Lancet Glob. Health 2014, 2, e106–e116. [Google Scholar] [CrossRef]
- Colijn, J.M.; Buitendijk, G.H.S.; Prokofyeva, E.; Alves, D.; Cachulo, M.L.; Khawaja, A.P.; Cougnard-Gregoire, A.; Merle, B.M.J.; Korb, C.; Erke, M.G.; et al. Prevalence of Age-Related Macular Degeneration in Europe: The Past and the Future. Ophthalmology 2017, 124, 1753–1763. [Google Scholar] [CrossRef]
- Yau, J.W.Y.; Rogers, S.L.; Kawasaki, R.; Lamoureux, E.L.; Kowalski, J.W.; Bek, T.; Chen, S.J.; Dekker, J.M.; Fletcher, A.; Grauslund, J.; et al. Global Prevalence and Major Risk Factors of Diabetic Retinopathy. Diabetes Care 2012, 35, 556–564. [Google Scholar] [CrossRef] [PubMed]
- Li, J.Q.; Welchowski, T.; Schmid, M.; Letow, J.; Wolpers, C.; Pascual-Camps, I.; Holz, F.G.; Finger, R.P. Prevalence, Incidence and Future Projection of Diabetic Eye Disease in Europe: A Systematic Review and Meta-Analysis. Eur. J. Epidemiol. 2020, 35, 11–23. [Google Scholar] [CrossRef]
- Urtti, A. Challenges and Obstacles of Ocular Pharmacokinetics and Drug Delivery. Adv. Drug Deliv. Rev. 2006, 58, 1131–1135. [Google Scholar] [CrossRef]
- Loftsson, T.; Sigurdsson, H.H.; Konrádsdóttir, F.; Gísladóttir, S.; Jansook, P.; Stefánsson, E. Topical Drug Delivery to the Posterior Segment of the Eye: Anatomical and Physiological Considerations. Pharmazie 2008, 63, 171–179. [Google Scholar] [CrossRef]
- Smith, S.J.; Smith, B.D.; Mohney, B.G. Ocular Side Effects Following Intravitreal Injection Therapy for Retinoblastoma: A Systematic Review. Br. J. Ophthalmol. 2014, 98, 292–297. [Google Scholar] [CrossRef] [PubMed]
- Sampat, K.M.; Garg, S.J. Complications of Intravitreal Injections. Curr. Opin. Ophthalmol. 2010, 21, 178–183. [Google Scholar] [CrossRef]
- Sen, H.N.; Vitale, S.; Gangaputra, S.S.; Nussenblatt, R.B.; Liesegang, T.L.; Levy-Clarke, G.A.; Rosenbaum, J.T.; Suhler, E.B.; Thorne, J.E.; Foster, C.S.; et al. Periocular Corticosteroid Injections in Uveitis: Effects and Complications. Ophthalmology 2014, 121, 2275–2286. [Google Scholar] [CrossRef]
- Moiseev, R.V.; Morrison, P.W.J.; Steele, F.; Khutoryanskiy, V.V. Penetration Enhancers in Ocular Drug Delivery. Pharmaceutics 2019, 11, 321. [Google Scholar] [CrossRef]
- Kaur, I.P.; Smitha, R. Penetration Enhancers and Ocular Bioadhesives: Two New Avenues for Ophthalmic Drug Delivery. Drug Dev. Ind. Pharm. 2002, 28, 353–369. [Google Scholar] [CrossRef]
- Zambito, Y.; Di Colo, G. Chitosan and Its Derivatives as Intraocular Penetration Enhancers. J. Drug Deliv. Sci. Technol. 2010, 20, 45–52. [Google Scholar] [CrossRef]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G.; Altman, D.; Antes, G.; Atkins, D.; Barbour, V.; Barrowman, N.; Berlin, J.A.; et al. Preferred Reporting Items for Systematic Reviews and Meta-Analyses: The PRISMA Statement. PLoS Med. 2009, 6, e1000097. [Google Scholar] [CrossRef] [PubMed]
- Liberati, A.; Altman, D.G.; Tetzlaff, J.; Mulrow, C.; Gøtzsche, P.C.; Ioannidis, J.P.A.; Clarke, M.; Devereaux, P.J.; Kleijnen, J.; Moher, D. The PRISMA Statement for Reporting Systematic Reviews and Meta-Analyses of Studies That Evaluate Health Care Interventions: Explanation and Elaboration. PLoS Med. 2009, 6, e1000100. [Google Scholar] [CrossRef] [PubMed]
- Fabian-Jessing, B.K.; Vallentin, M.F.; Secher, N.; Hansen, F.B.; Dezfulian, C.; Granfeldt, A.; Andersen, L.W. Animal Models of Cardiac Arrest: A Systematic Review of Bias and Reporting. Resuscitation 2018, 125, 16–21. [Google Scholar] [CrossRef]
- Hooijmans, C.R.; Rovers, M.M.; De Vries, R.B.M.; Leenaars, M.; Ritskes-Hoitinga, M.; Langendam, M.W. SYRCLE’s Risk of Bias Tool for Animal Studies. BMC Med. Res. Methodol. 2014, 14, 43. [Google Scholar] [CrossRef] [PubMed]
- Higgins, J.P.T.; Altman, D.G.; Gøtzsche, P.C.; Jüni, P.; Moher, D.; Oxman, A.D.; Savović, J.; Schulz, K.F.; Weeks, L.; Sterne, J.A.C. The Cochrane Collaboration’s Tool for Assessing Risk of Bias in Randomised Trials. BMJ 2011, 343, d5928. [Google Scholar] [CrossRef]
- Johnson, L.N.; Cashman, S.M.; Kumar-Singh, R. Cell-Penetrating Peptide for Enhanced Delivery of Nucleic Acids and Drugs to Ocular Tissues Including Retina and Cornea. Mol. Ther. 2008, 16, 107–114. [Google Scholar] [CrossRef]
- Wang, Y.; Lin, H.; Lin, S.; Qu, J.; Xiao, J.; Huang, Y.; Xiao, Y.; Fu, X.; Yang, Y.; Li, X. Cell-Penetrating Peptide TAT-Mediated Delivery of Acidic FGF to Retina and Protection against Ischemia-Reperfusion Injury in Rats. J. Cell. Mol. Med. 2010, 14, 1998–2005. [Google Scholar] [CrossRef]
- Liu, C.; Tai, L.; Zhang, W.; Wei, G.; Pan, W.; Lu, W. Penetratin, a Potentially Powerful Absorption Enhancer for Noninvasive Intraocular Drug Delivery. Mol. Pharm. 2014, 11, 1218–1227. [Google Scholar] [CrossRef]
- Zhang, X.; Li, Y.; Cheng, Y.; Tan, H.; Li, Z.; Qu, Y.; Mu, G.; Wang, F. Tat PTD-Endostatin: A Novel Anti-Angiogenesis Protein with Ocular Barrier Permeability via Eye-Drops. Biochim. Biophys. Acta Gen. Subj. 2015, 1850, 1140–1149. [Google Scholar] [CrossRef] [PubMed]
- Mahaling, B.; Katti, D.S. Understanding the Influence of Surface Properties of Nanoparticles and Penetration Enhancers for Improving Bioavailability in Eye Tissues In Vivo. Int. J. Pharm. 2016, 501, 1–9. [Google Scholar] [CrossRef]
- Li, Y.; Li, L.; Li, Z.; Sheng, J.; Zhang, X.; Feng, D.; Zhang, X.; Yin, F.; Wang, A.; Wang, F. Tat PTD-Endostatin-RGD: A Novel Protein with Anti-Angiogenesis Effect in Retina via Eye Drops. Biochim. Biophys. Acta Gen. Subj. 2016, 1860, 2137–2147. [Google Scholar] [CrossRef] [PubMed]
- Liu, C.; Jiang, K.; Tai, L.; Liu, Y.; Wei, G.; Lu, W.; Pan, W. Facile Noninvasive Retinal Gene Delivery Enabled by Penetratin. ACS Appl. Mater. Interfaces 2016, 8, 19256–19267. [Google Scholar] [CrossRef] [PubMed]
- Chu, Y.; Chen, N.; Yu, H.; Mu, H.; He, B.; Hua, H.; Wang, A.; Sun, K. Topical Ocular Delivery to Laser-Induced Choroidal Neovascularization by Dual Internalizing RGD and TAT Peptide-Modified Nanoparticles. Int. J. Nanomed. 2017, 12, 1353–1368. [Google Scholar] [CrossRef]
- de Cogan, F.; Hill, L.J.; Lynch, A.; Morgan-Warren, P.J.; Lechner, J.; Berwick, M.R.; Peacock, A.F.A.; Chen, M.; Scott, R.A.H.; Xu, H.; et al. Topical Delivery of Anti-VEGF Drugs to the Ocular Posterior Segment Using Cell-Penetrating Peptides. Investig. Ophthalmol. Vis. Sci. 2017, 58, 2578–2590. [Google Scholar] [CrossRef]
- Jiang, K.; Gao, X.; Shen, Q.; Zhan, C.; Zhang, Y.; Xie, C.; Wei, G.; Lu, W. Discerning the Composition of Penetratin for Safe Penetration from Cornea to Retina. Acta Biomater. 2017, 63, 123–134. [Google Scholar] [CrossRef]
- Atlasz, T.; Werling, D.; Song, S.; Szabo, E.; Vaczy, A.; Kovari, P.; Tamas, A.; Reglodi, D.; Yu, R. Retinoprotective Effects of TAT-Bound Vasoactive Intestinal Peptide and Pituitary Adenylate Cyclase Activating Polypeptide. J. Mol. Neurosci. 2019, 68, 397–407. [Google Scholar] [CrossRef]
- Li, J.; Cheng, T.; Tian, Q.; Cheng, Y.; Zhao, L.; Zhang, X.; Qu, Y. A More Efficient Ocular Delivery System of Triamcinolone Acetonide as Eye Drop to the Posterior Segment of the Eye. Drug Deliv. 2019, 26, 188–198. [Google Scholar] [CrossRef]
- Yang, X.; Wang, L.; Li, L.; Han, M.; Tang, S.; Wang, T.; Han, J.; He, X.; He, X.; Wang, A.; et al. A Novel Dendrimer-Based Complex Co-Modified with Cyclic RGD Hexapeptide and Penetratin for Noninvasive Targeting and Penetration of the Ocular Posterior Segment. Drug Deliv. 2019, 26, 989–1001. [Google Scholar] [CrossRef]
- Wang, Y.; Zhou, L.; Fang, L.; Cao, F. Multifunctional Carboxymethyl Chitosan Derivatives-Layered Double Hydroxide Hybrid Nanocomposites for Efficient Drug Delivery to the Posterior Segment of the Eye. Acta Biomater. 2020, 104, 104–114. [Google Scholar] [CrossRef]
- Bechara, C.; Sagan, S. Cell-Penetrating Peptides: 20 Years Later, Where Do We Stand? FEBS Lett. 2013, 587, 1693–1702. [Google Scholar] [CrossRef]
- Vivès, E.; Schmidt, J.; Pèlegrin, A. Cell-Penetrating and Cell-Targeting Peptides in Drug Delivery. Biochim. Biophys. Acta Rev. Cancer 2008, 1786, 126–138. [Google Scholar] [CrossRef] [PubMed]
- Felt, O.; Buri, P.; Gurny, R. Chitosan: A Unique Polysaccharide for Drug Delivery. Drug Dev. Ind. Pharm. 1998, 24, 979–993. [Google Scholar] [CrossRef]
- Caramella, C.; Ferrari, F.; Bonferoni, M.C.; Rossi, S.; Sandri, G. Chitosan and Its Derivatives as Drug Penetration Enhancers. J. Drug Deliv. Sci. Technol. 2010, 20, 5–13. [Google Scholar] [CrossRef]
- Richard, J.P.; Melikov, K.; Vives, E.; Ramos, C.; Verbeure, B.; Gait, M.J.; Chernomordik, L.V.; Lebleu, B. Cell-Penetrating Peptides: A Reevaluation of the Mechanism of Cellular Uptake. J. Biol. Chem. 2003, 278, 585–590. [Google Scholar] [CrossRef]
- Duchardt, F.; Fotin-Mleczek, M.; Schwarz, H.; Fischer, R.; Brock, R. A Comprehensive Model for the Cellular Uptake of Cationic Cell-Penetrating Peptides. Traffic 2007, 8, 848–866. [Google Scholar] [CrossRef] [PubMed]
- du Sert, N.P.; Hurst, V.; Ahluwalia, A.; Alam, S.; Avey, M.T.; Baker, M.; Browne, W.J.; Clark, A.; Cuthill, I.C.; Dirnagl, U.; et al. The Arrive Guidelines 2.0: Updated Guidelines for Reporting Animal Research. PLoS Biol. 2020, 18, e3000410. [Google Scholar] [CrossRef]
- du Sert, N.P.; Ahluwalia, A.; Alam, S.; Avey, M.T.; Baker, M.; Browne, W.J.; Clark, A.; Cuthill, I.C.; Dirnagl, U.; Emerson, M.; et al. Reporting Animal Research: Explanation and Elaboration for the Arrive Guidelines 2.0. PLoS Biol. 2020, 18, e3000411. [Google Scholar]
- Schonbrunn, A. Editorial: Antibody Can Get It Right: Confronting Problems of Antibody Specificity and Irreproducibility. Mol. Endocrinol. 2014, 28, 1403–1407. [Google Scholar] [CrossRef] [PubMed]
| Publication | Penetration Enhancers (PE) | Animal Model | In-Vivo Efficacy and Biodistribution |
|---|---|---|---|
| Johnson et al., 2008 [20] | CPP: Peptide for Ocular Delivery (POD)—GGG(ARKKAAKA)4 | C57BL/6J mice | Microscopy—POD conjugates transduced sclera/choroid and dura of the optic nerve 45 min post application and was eliminated within 24 h; no staining in non-POD groups |
| Wang et al., 2010 [21] | TAT—CPP | Sprague–Dawley rats | Immunohistochemistry—TAT conjugates readily detected in retina 30 min post administration, mainly in RGCs in the GCL, peaked around 30 min to 1 h, detectable until up-to 8 h; no detection in non-TAT retinas |
| Liu et al., 2014 [22] | Penetratin—CPP | Sprague–Dawley rats | Fluorescence microscopy—Penetratin reached both anterior and posterior segments of the eye 10 min after application, fluorescence detected in GCL, IPL, OPL, INL, ONL, RPE, and the photoreceptor segments; peaked at 30 min and persisted for 6 h; no fluorescence detected in untreated eyes |
| Zhang et al., 2015 [23] | TAT—CPP | Kunming mice and C57BL/6 mice | Immunohistochemistry—Groups treated with TAT conjugated drug had high drug distribution in the retina after eye drop administration; unconjugated drug groups showed no drug |
| Mahaling and Katti, 2016 [24] | Benzalkonium chloride (BAC) | Pigmented mice | Fluorescence microscopy—Results indicated that presence of BAC led to varying degrees of increase in bioavailability of different nanoparticles to the retina as compared to non-coated nanoparticles |
| Li et al., 2016 [25] | TAT—CPP | C57BL/6 mice | Quantitative analysis (ELISA)—Concentration of drug in the retina groups treated with TAT conjugated drug was approximately 14 times higher than in those with non-conjugated drug; concentration peaked around 1 h, and the half-life was around 11 h |
| Liu et al., 2016 [26] | Penetratin—CPP | Sprague–Dawley rats | Fluorescence microscopy—Penetratin conjugated complexes reached the posterior segment in 10 min post application, fluorescence detected in photoreceptor segments, RPE, GCL, IPL, OPL, choroid, INL, and ONL; no fluorescence detected in eyes treated with unconjugated complexes |
| Chu et al., 2017 [27] | TAT—CPP | Brown Norway rats | Confocal microscopy—Eyes treated with TAT modified complexes exhibited 11 times higher fluorescence in the retina-choroid than those treated with non-modified complexes. |
| de Cogan et al., 2017 [28] | CPP: (5[6]-carboxyfluorescein-RRRRRR-COOH) | Adult Sprague- Dawley rats and Wild-type (WT) C57BL/6J mice | Quantitative analysis (ELISA)—Concentration of drug detected in groups treated with CPP conjugated drug was 10–11 times higher compared to groups treated with non-conjugated drug; drug levels peaked at 40 min post administration and was eliminated by 24 h |
| Jiang et al., 2017 [29] | Penetratin derivatives—CPP | Mice | Fluorescence microscopy—Fluorescence from retinas treated with hydrophobic penetratin derivatives > wild-type penetratin > hydrophilic derivatives; peptides reached the posterior segment within 10 min post instillation and fluorescence peaked around 1 h |
| Atlasz et al., 2019 [30] | TAT—CPP | Rats | Fluorescence microscopy—TAT bound complexes reached the retina with an efficiency of about three-fold higher than that of non-conjugated drugs |
| Li et al., 2019 [31] | Chitosan | C57BL/6 mice | Optical coherence tomography—Eyes treated with chitosan conjugates emitted higher levels of fluorescence from the posterior segment than those eyes treated without chitosan; fluorescence detection started at 10 min, peaked at 6 h, and disappeared 12 h post application |
| Yang et al., 2019 [32] | Penetratin—CPP | ICR mice | Fluorescence microscopy—Retinas treated with penetratin modified complexes demonstrated much higher fluorescence intensities (~3 times greater) as compared to retinas with non-modified complexes; detected in retina 1 h post administration, in RPE within 2 h, peaked at 8 h and still detectable until 12 h |
| Wang et al., 2020 [33] | Carboxymethyl chitosan (CMCS) | New Zealand albino rabbits | Quantitative analysis (HPLC)—Drug concentration in retina-choroid treated with CMCS conjugates were 2.5 times higher than in those with non-conjugated drugs; drug concentration peaked at 1 h and was detectable up-to 3 h post application |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Thareja, A.; Hughes, H.; Alvarez-Lorenzo, C.; Hakkarainen, J.J.; Ahmed, Z. Penetration Enhancers for Topical Drug Delivery to the Ocular Posterior Segment—A Systematic Review. Pharmaceutics 2021, 13, 276. https://doi.org/10.3390/pharmaceutics13020276
Thareja A, Hughes H, Alvarez-Lorenzo C, Hakkarainen JJ, Ahmed Z. Penetration Enhancers for Topical Drug Delivery to the Ocular Posterior Segment—A Systematic Review. Pharmaceutics. 2021; 13(2):276. https://doi.org/10.3390/pharmaceutics13020276
Chicago/Turabian StyleThareja, Abhinav, Helen Hughes, Carmen Alvarez-Lorenzo, Jenni J. Hakkarainen, and Zubair Ahmed. 2021. "Penetration Enhancers for Topical Drug Delivery to the Ocular Posterior Segment—A Systematic Review" Pharmaceutics 13, no. 2: 276. https://doi.org/10.3390/pharmaceutics13020276
APA StyleThareja, A., Hughes, H., Alvarez-Lorenzo, C., Hakkarainen, J. J., & Ahmed, Z. (2021). Penetration Enhancers for Topical Drug Delivery to the Ocular Posterior Segment—A Systematic Review. Pharmaceutics, 13(2), 276. https://doi.org/10.3390/pharmaceutics13020276









