Advanced Microparticulate/Nanoparticulate Respirable Dry Powders of a Selective RhoA/Rho Kinase (Rock) Inhibitor for Targeted Pulmonary Inhalation Aerosol Delivery
Abstract
1. Background
2. Experimental: Materials and Methods
2.1. Materials
2.2. Methods
2.3. Scanning Electron Microscopy (SEM) and Energy Dispersive X-ray (EDX) Spectrometry
2.4. Particle Sizing and Size Distribution by Image Analysis of SEM Micrographs
2.5. X-ray Powder Diffraction (XRPD)
2.6. Differential Scanning Calorimetry (DSC)
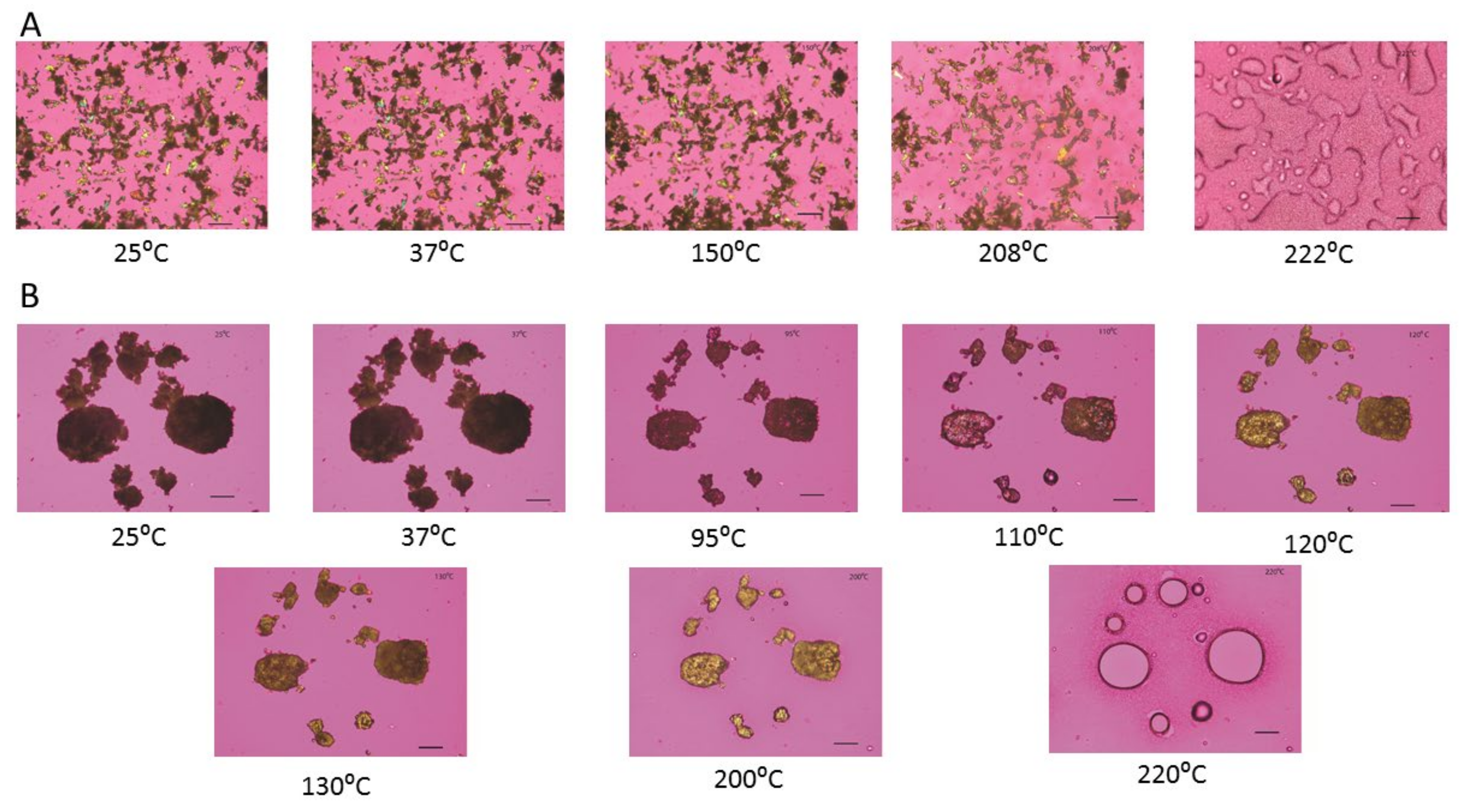
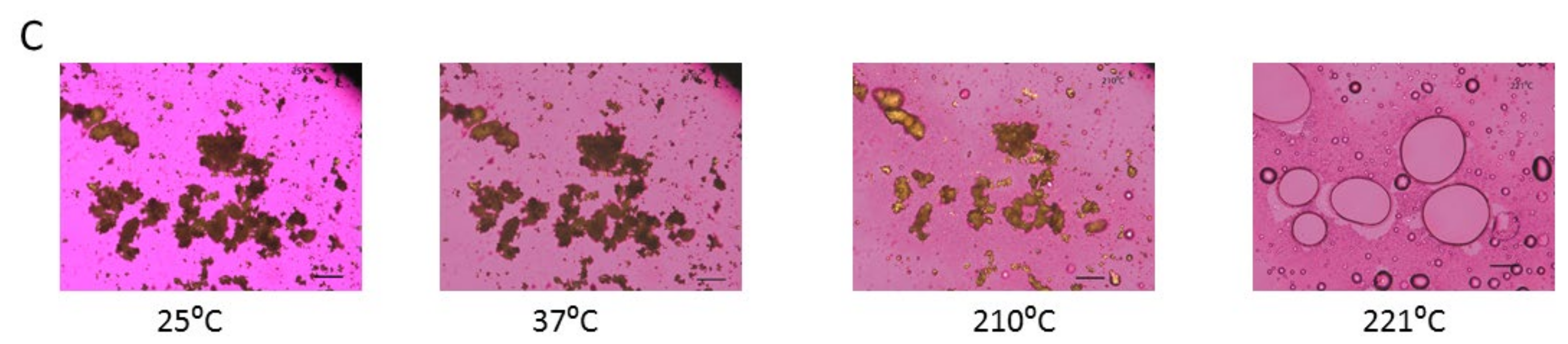
2.7. Hot Stage Microscopy (HSM) under Cross-Polarizers
2.8. Karl Fisher Titration (KFT)
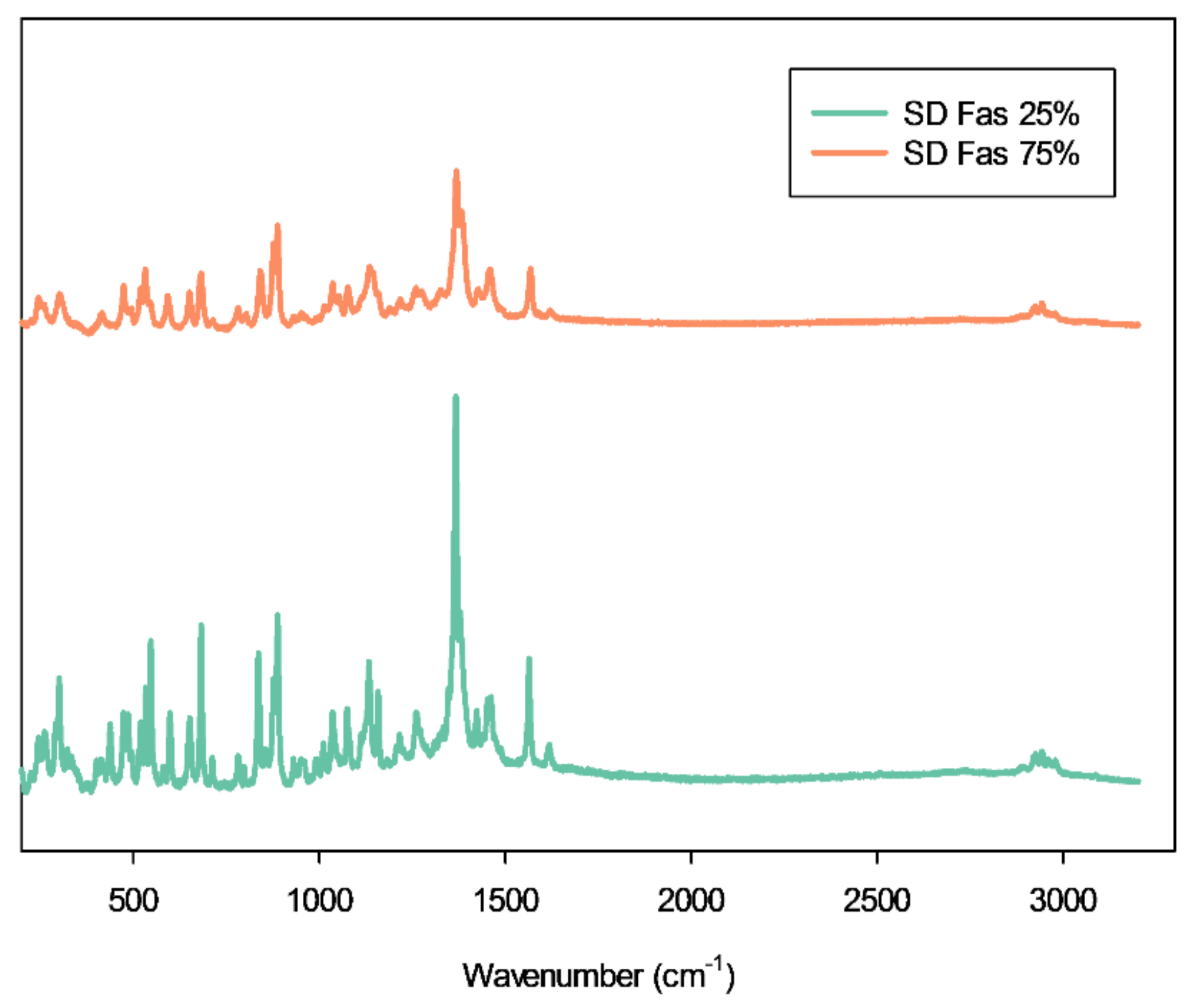
2.9. Confocal Raman Microspectroscopy (CRM), and Chemical Imaging
2.10. Attenuated Total Reflectance (ATR)-Fourier-Transform Infrared (FTIR) Spectroscopy
2.11. In Vitro Aerosol Dispersion Performance
2.12. In Vitro Cell Viability
2.13. In Vitro Transepithelial Electrical Resistance (TEER)
2.14. Statistical Analysis
3. Results
3.1. Scanning Electron Microscopy (SEM) and Energy Dispersive X-ray (EDX)
3.2. Particle Sizing and Size Distribution Using SEM Micrographs
3.3. X-ray Powder Diffraction (XRPD)
3.4. Differential Scanning Calorimetry (DSC)
3.5. Hot-Stage Microscopy (HSM) under Cross-Polarizer Lens
3.6. Karl Fisher Titration (KFT)
3.7. Confocal Raman Microspectroscopy (CRM) and Chemical Imaging
3.8. Attenuated Total Reflectance—Fourier Transform Infrared (ATR-FTIR) Spectroscopy
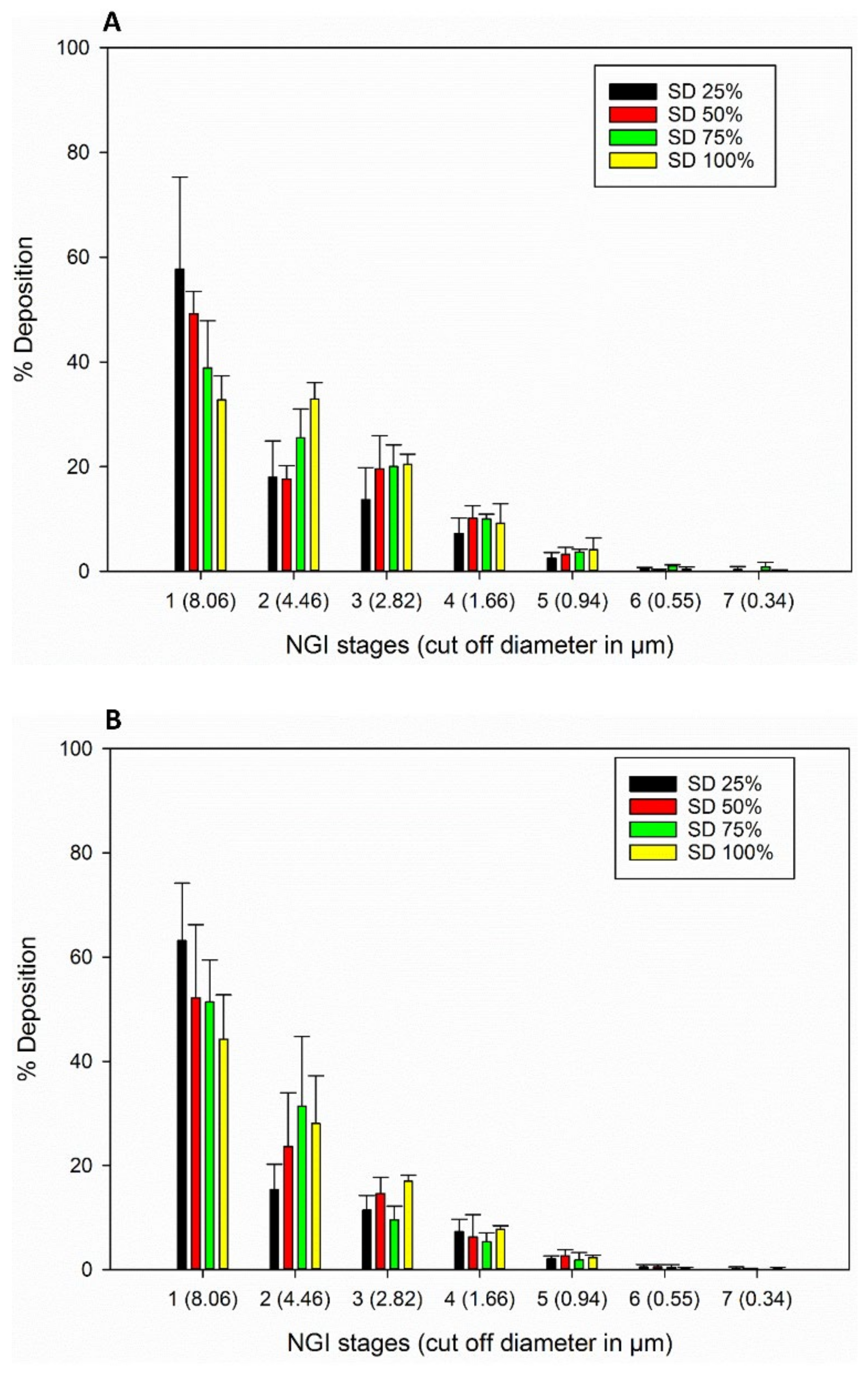
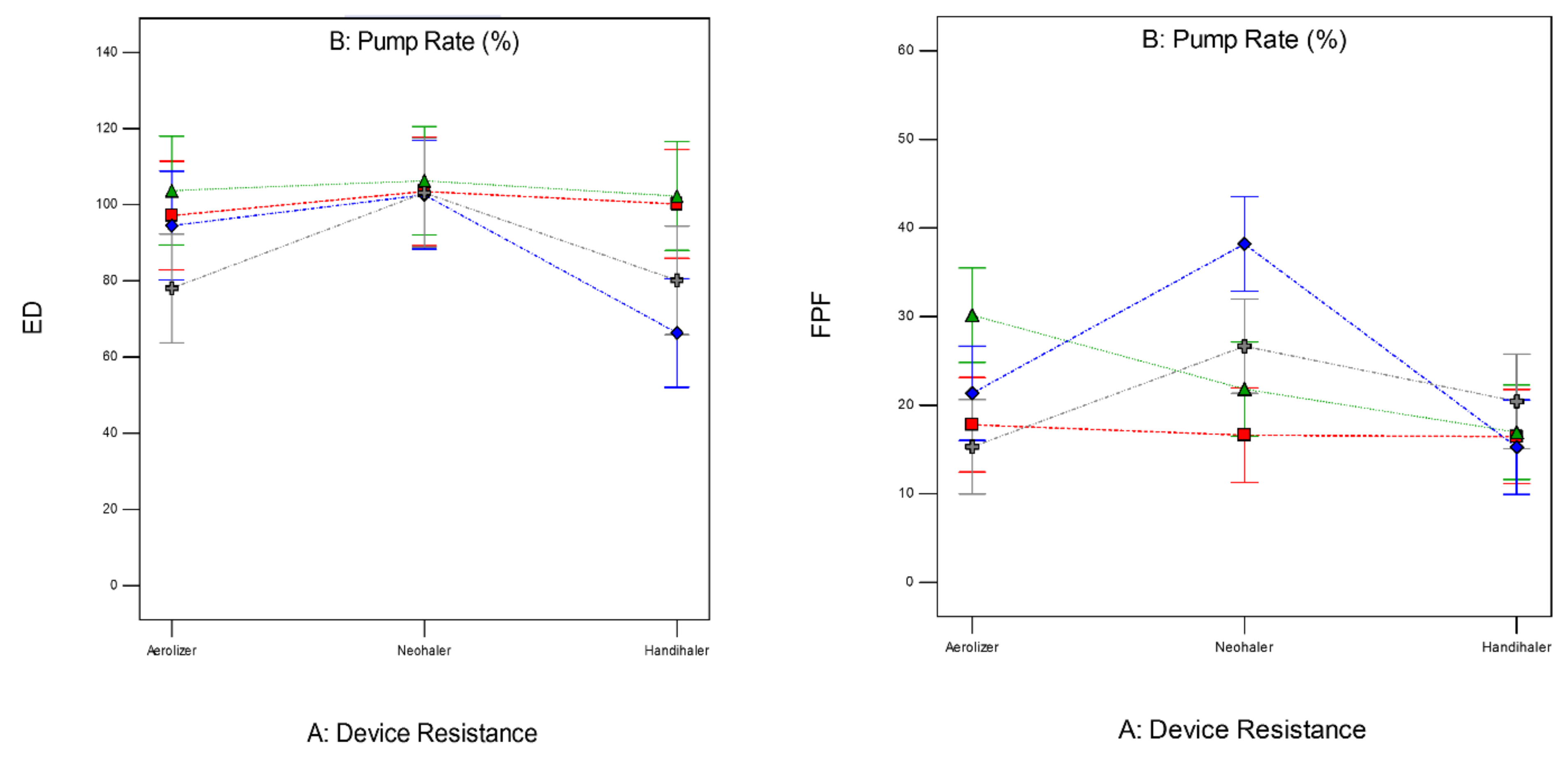
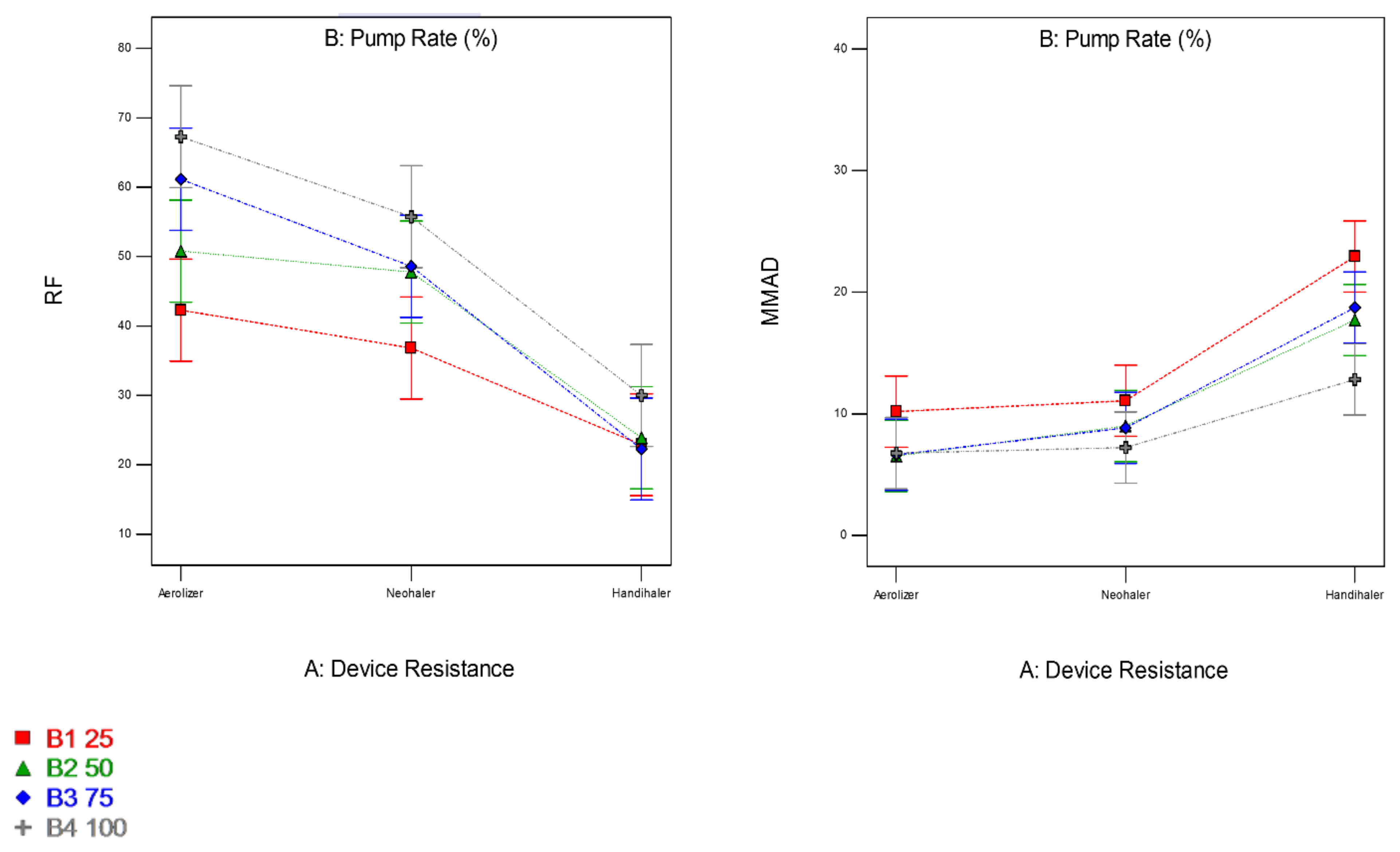
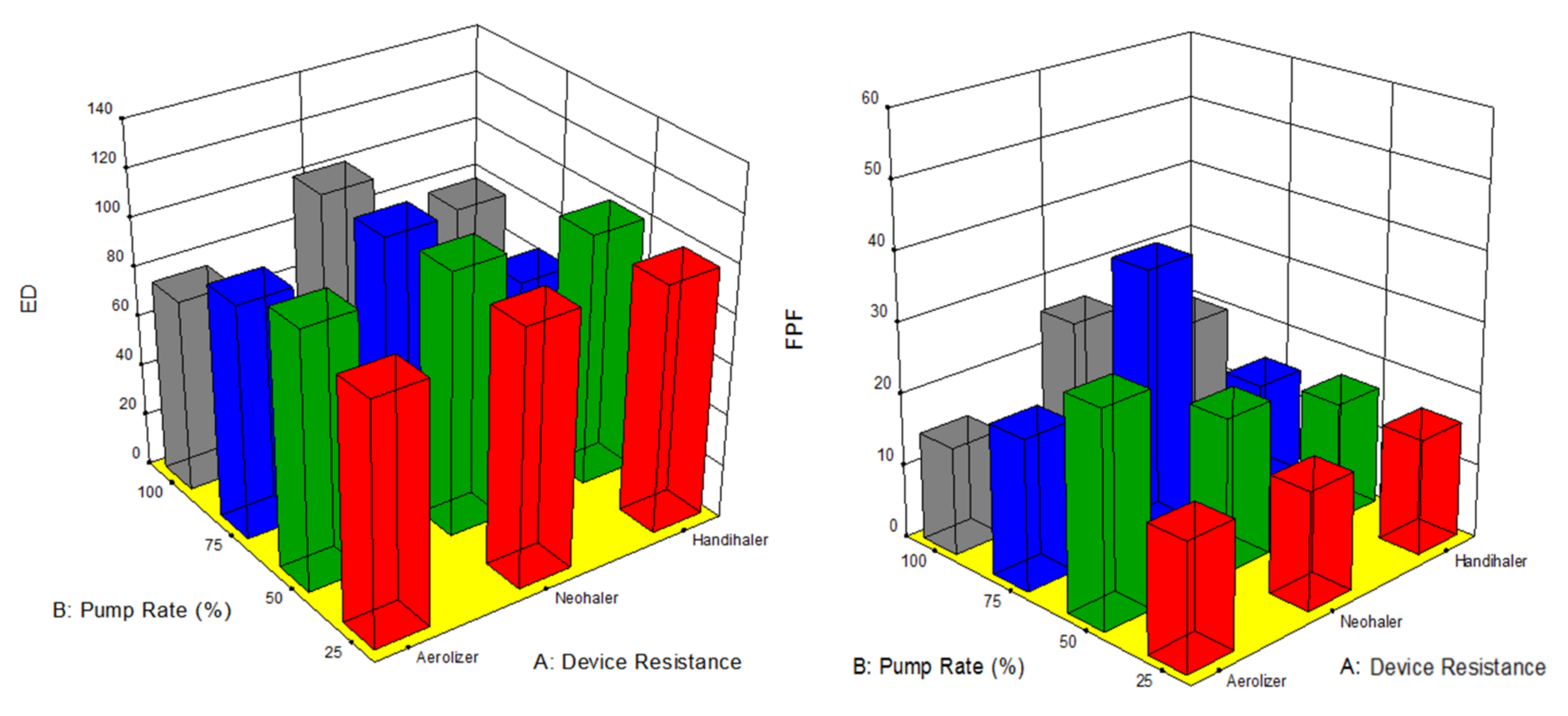
3.9. In Vitro Aerosol Dispersion Performance
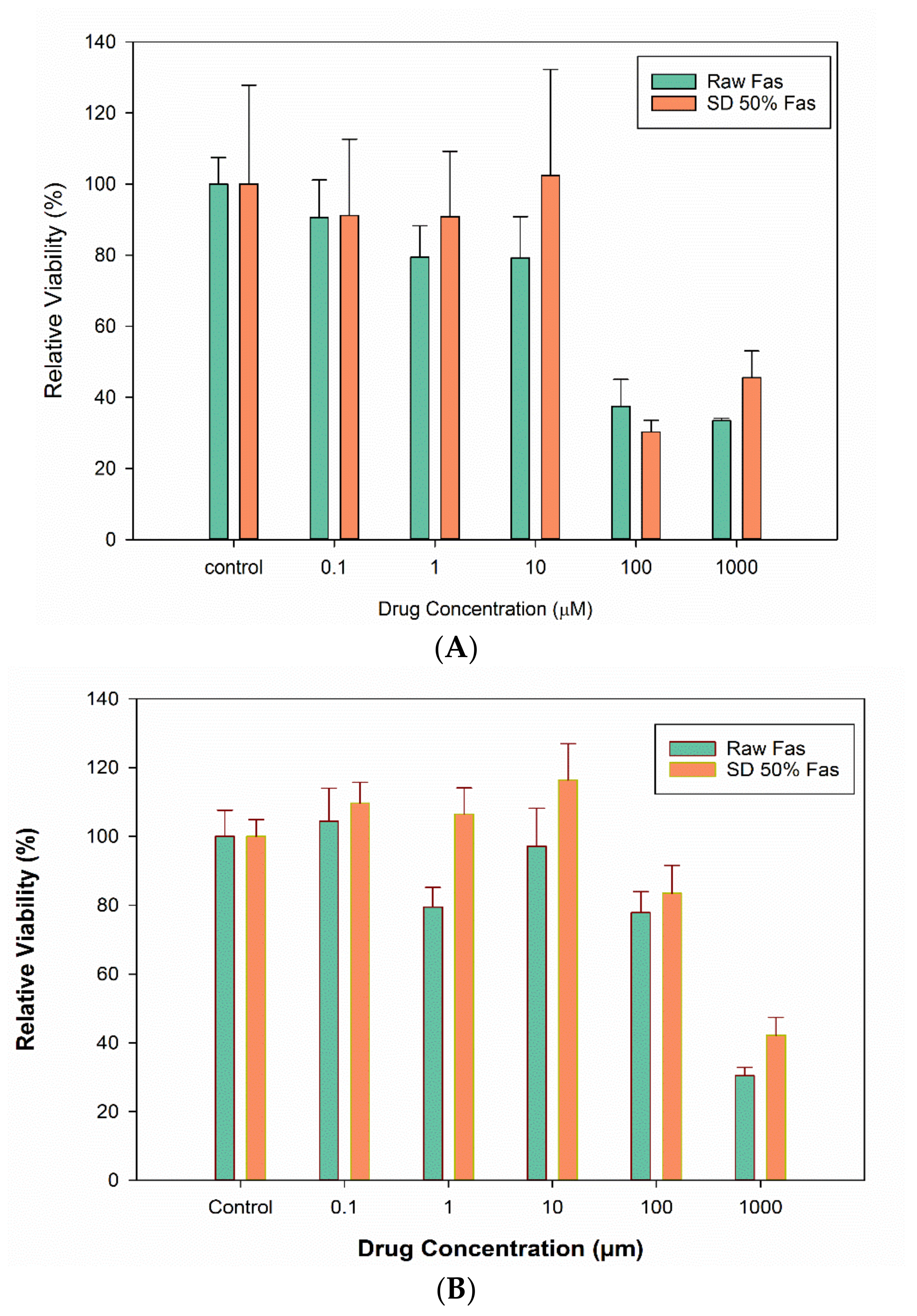
3.10. In Vitro Cell Viability
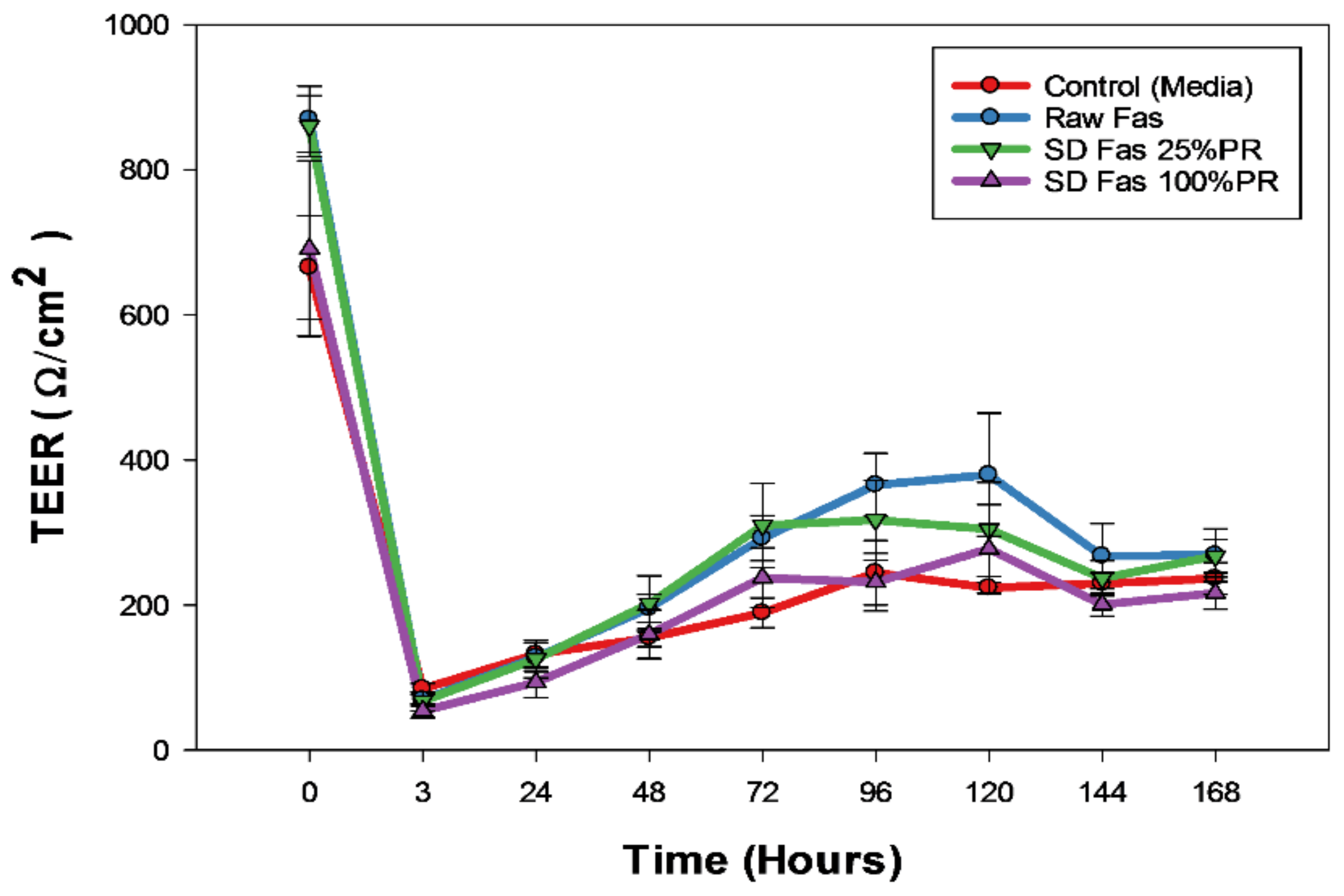
3.11. In Vitro Transepithelial Electrical Resistance Analysis
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Galie, N.; Humbert, M.; Vachiery, J.L.; Gibbs, S.; Lang, I.; Torbicki, A.; Simonneau, G.; Peacock, A.; Vonk Noordegraaf, A.; Beghetti, M.; et al. 2015 ESC/ERS Guidelines for the diagnosis and treatment of pulmonary hypertension: The Joint Task Force for the Diagnosis and Treatment of Pulmonary Hypertension of the European Society of Cardiology (ESC) and the European Respiratory Society (ERS): Endorsed by: Association for European Paediatric and Congenital Cardiology (AEPC), International Society for Heart and Lung Transplantation (ISHLT). Eur. Respir. J. 2015, 46, 903–975. [Google Scholar] [PubMed]
- Odagiri, K.; Watanabe, H. Effects of the Rho-Kinase Inhibitor, Fasudil, on Pulmonary Hypertension. Circ. J. 2015, 79, 1213–1214. [Google Scholar] [CrossRef] [PubMed]
- Sun, X.-Z.; Tian, X.-Y.; Wang, D.-W.; Li, J. Effects of fasudil on hypoxic pulmonary hypertension and pulmonary vascular remodeling in rats. Eur. Rev. Med Pharmacol. Sci. 2014, 18, 959–964. [Google Scholar] [PubMed]
- Acosta, M.F.; Hayes, D.J.; Fineman, J.R.; Yuan, J.X.-J.; Black, S.M.; Mansour, H.M. Book Chapter 19: Therapeutics in Pulmonary Hypertension. In Inhalation Aerosols: Physical and Biological Basis for Therapy: Lung Biology in Health and Diseases Series, 3rd ed.; Hickey, A.J., Mansour, H.M., Eds.; CRC Press/Taylor & Francis: London, UK, 2019; pp. 313–322. [Google Scholar]
- Hayes, D., Jr.; Black, S.M.; Tobias, J.D.; Kirkby, S.; Mansour, H.M.; Whitson, B.A. Influence of Pulmonary Hypertension on Patients with Idiopathic Pulmonary Fibrosis Awaiting Lung Transplantation. Ann. Thorac. Surg. 2016, 101, 246–252. [Google Scholar] [CrossRef]
- Hayes, D., Jr.; Tobias, J.D.; Mansour, H.M.; Kirkby, S.; McCoy, K.S.; Daniels, C.J. Pulmonary hypertension in cystic fibrosis with advanced lung disease. Am. J. Respir. Crit. Care Med. 2014, 190, 898–905. [Google Scholar] [CrossRef]
- Hayes, D., Jr.; Black, S.M.; Tobias, J.D.; Mansour, H.M.; Whitson, B.A. Prevalence of Pulmonary Hypertension and its Influence on Survival in Patients with Advanced Chronic Obstructive Pulmonary Disease Prior to Lung Transplantation. J. Chronic Obstr. Pulm. Dis. 2016, 13, 50–56. [Google Scholar] [CrossRef]
- Amano, M.; Nakayama, M.; Kaibuchi, K. Rho-kinase/ROCK: A key regulator of the cytoskeleton and cell polarity. Cytoskeleton 2010, 67, 545–554. [Google Scholar] [CrossRef]
- Liao, J.K.; Seto, M.; Noma, K. Rho Kinase (ROCK) Inhibitors. J. Cardiovasc. Pharmacol. 2007, 50, 17–24. [Google Scholar] [CrossRef]
- Guan, P.; Liang, Y.; Wang, N. Fasudil alleviates pressure overload-induced heart failure by activating Nrf2-mediated antioxidant responses. J. Cell. Biochem. 2018, 119, 6452–6460. [Google Scholar] [CrossRef]
- Liu, P.; Zhang, H.M.; Tang, Y.J.; Sheng, C.F.; Liu, J.X.; Zeng, Y.J. Influence of Rho kinase inhibitor fasudil on late endothelial progenitor cells in peripheral blood of COPD patients with pulmonary artery hypertension. Bratisl. Lek. List. 2015, 116, 150–153. [Google Scholar] [CrossRef]
- Kasahara, D.I.; Mathews, J.A.; Park, C.Y.; Cho, Y.; Hunt, G.; Wurmbrand, A.P.; Liao, J.K.; Shore, S.A. ROCK insufficiency attenuates ozone-induced airway hyperresponsiveness in mice. Am. J. Physiol. Cell. Mol. Physiol. 2015, 309, L736–L746. [Google Scholar] [CrossRef]
- Lambert, J.A.; Song, W. Ozone-induced airway hyperresponsiveness: Roles of ROCK isoforms. Am. J. Physiol. Cell. Mol. Physiol. 2015, 309, L1394–L1397. [Google Scholar] [CrossRef][Green Version]
- Xie, T.; Luo, G.; Zhang, Y.; Wang, X.; Wang, X.; Wu, M.; Li, G. Rho-kinase inhibitor fasudil reduces allergic airway inflammation and mucus hypersecretion by regulating STAT6 and NFkappaB. Clinical and experimental allergy. J. Br. Soc. Allergy Clin. Immunol. 2015, 45, 1812–1822. [Google Scholar] [CrossRef]
- Qi, X.J.; Ning, W.; Xu, F.; Dang, H.X.; Fang, F.; Li, J. Fasudil, an inhibitor of Rho-associated coiled-coil kinase, attenuates hyperoxia-induced pulmonary fibrosis in neonatal rats. Int. J. Clin. Exp. Pathol. 2015, 8, 12140–12150. [Google Scholar]
- Ding, R.Y.; Zhao, D.M.; Zhang, Z.D.; Guo, R.X.; Ma, X.C. Pretreatment of Rho kinase inhibitor inhibits systemic inflammation and prevents endotoxin-induced acute lung injury in mice. J. Surg. Res. 2011, 171, e209–e214. [Google Scholar] [CrossRef]
- Al-Hilal, T.A.; Hossain, M.A.; Alobaida, A.; Alam, F.; Keshavarz, A.; Nozik-Grayck, E. Design, synthesis and biological evaluations of a long-acting, hypoxia-activated prodrug of fasudil, a ROCK inhibitor, to reduce its systemic side-effects. J. Control. Release 2021, 334, 237–247. [Google Scholar] [CrossRef]
- Mansour, H.M.; Park, C.W.; Bawa, R. Chapter: Design and Development of Approved Nanopharmaceutical Products. In Clinical Nanomedicine: From Bench to Bedside Series of Nanomedicine 1; Bawa, R., Ed.; Pan Stanford Publishing/CRC Press: London, UK, 2011; Volume 1, pp. 1–27. [Google Scholar]
- Mansour, H.M.; Park, C.W.; Hayes, D., Jr. Chapter 3: Nanomedicine lung delivery and inhalation aerosols for targeted pulmonary nanomedicine. In Nanomedicine in Drug Delivery; Kumar, A., Mansour, H.M., Friedman, A., Blough, E.R., Eds.; CRC Press/Taylor & Francis: Boca Raton, FL, USA, 2013; pp. 43–74. [Google Scholar]
- Mansour, H.M.; Rhee, Y.S.; Wu, X. Nanomedicine in Pulmonary Delivery. Int. J. Nanomed. 2009, 4, 299–319. [Google Scholar] [CrossRef]
- Hickey, A.J.; Mansour, H.M. Chapter 5: Delivery of Drugs by the Pulmonary Route. In Modern Pharmaceutics. Drugs and the Pharmaceutical Sciences Series 2, 5th ed.; Florence, A.T., Siepmann, J., Eds.; Taylor and Francis: New York, NY, USA, 2009; pp. 191–219. [Google Scholar]
- Mansour, H.M.; Myrdal, P.B.; Younis, U.; Muralidharan, P.; Hillery, A.M.; Hayes, D.J. Book Chapter 11: Pulmonary Drug Delivery. In Drug Delivery: Fundamentals & Applications; Hillery, A.M., Swarbrick, J., Park, K., Eds.; CRC Press/Taylor & Francis: London, UK, 2016; pp. 249–277. [Google Scholar]
- Hickey, A.J.; Mansour, H.M. Chapter 43: Formulation Challenges of Powders for the Delivery of Small Molecular Weight Molecules as Aerosols. In Modified-Release Drug Delivery Technology. Drugs and the Pharmaceutical Sciences Series 2, 2nd ed.; Rathbone, M.J., Hadgraft, J., Roberts, M.S., Lane, M., Eds.; Informa Healthcare: New York, NY, USA, 2008; pp. 573–602. [Google Scholar]
- Gupta, N.; Al-Saikhan, F.I.; Patel, B.; Rashid, J.; Ahsan, F. Fasudil and SOD packaged in peptide-studded-liposomes: Properties, pharmacokinetics and ex-vivo targeting to isolated perfused rat lungs. Int. J. Pharm. 2015, 488, 33–43. [Google Scholar] [CrossRef]
- Gupta, V.; Gupta, N.; Shaik, I.H.; Mehvar, R.; McMurtry, I.F.; Oka, M. Liposomal fasudil, a rho-kinase inhibitor, for prolonged pulmonary preferential vasodilation in pulmonary arterial hypertension. J. Control. Release 2013, 167, 189–199. [Google Scholar] [CrossRef]
- Gupta, N.; Ibrahim, H.M.; Ahsan, F. Peptide-micelle hybrids containing fasudil for targeted delivery to the pulmonary arteries and arterioles to treat pulmonary arterial hypertension. J. Pharm. Sci. 2014, 103, 3743–3753. [Google Scholar] [CrossRef]
- Nahar, K.; Absar, S.; Gupta, N.; Kotamraju, V.R.; McMurtry, I.F.; Oka, M. Peptide-coated liposomal fasudil enhances site specific vasodilation in pulmonary arterial hypertension. Mol. Pharm. 2014, 11, 4374–4384. [Google Scholar] [CrossRef]
- Nahar, K.; Absar, S.; Patel, B.; Ahsan, F. Starch-coated magnetic liposomes as an inhalable carrier for accumulation of fasudil in the pulmonary vasculature. Int. J. Pharmaceutics. 2014, 464, 185–195. [Google Scholar] [CrossRef]
- Gupta, N.; Patel, B.; Nahar, K.; Ahsan, F. Cell permeable peptide conjugated nanoerythrosomes of fasudil prolong pulmonary arterial vasodilation in PAH rats. Eur. J. Pharm. Biopharm. 2014, 88, 1046–1055. [Google Scholar] [CrossRef]
- Meenach, S.A.; Anderson, K.W.; Zach Hilt, J.; McGarry, R.C.; Mansour, H.M. Characterization and aerosol dispersion performance of advanced spray-dried chemotherapeutic PEGylated phospholipid particles for dry powder inhalation delivery in lung cancer. Eur. J. Pharm. Sci. 2013, 49, 699–711. [Google Scholar] [CrossRef]
- Muralidharan, P.; Hayes, D.; Black, S.M.; Mansour, H.M. Microparticulate/nanoparticulate powders of a novel Nrf2 activator and an aerosol performance enhancer for pulmonary delivery targeting the lung Nrf2/Keap-1 pathway. Mol. Syst. Des. Eng. 2016, 1, 48–65. [Google Scholar] [CrossRef]
- Li, X.; Vogt, F.G.; Hayes, D.; Mansour, H.M. Design, Characterization, and Aerosol Dispersion Performance Modeling of Advanced Spray-Dried Microparticulate/Nanoparticulate Mannitol Powders for Targeted Pulmonary Delivery as Dry Powder Inhalers. J. Aerosol Med. Pulm. Drug Deliv. 2014, 27, 81–93. [Google Scholar] [CrossRef] [PubMed]
- Meenach, S.A.; Vogt, F.G.; Anderson, K.W.; Hilt, J.Z.; McGarry, R.C.; Mansour, H.M. Design, physicochemical characterization, and optimization of organic solution advanced spray-dried inhalable dipalmitoylphosphatidylcholine (DPPC) and dipalmitoylphosphatidylethanolamine poly(ethylene glycol) (DPPE-PEG) microparticles and nanoparticles for targeted respiratory nanomedicine delivery as dry powder inhalation aerosols. Int. J. Nanomed. 2013, 8, 275–293. [Google Scholar]
- Meenach, S.; Anderson, K.W.; Hilt, J.Z.; McGarry, R.C.; Mansour, H.M. High-Performing Dry Powder Inhalers of Paclitaxel DPPC/DPPG Lung Surfactant-Mimic Multifunctional Particles in Lung Cancer: Physicochemical Characterization, In Vitro Aerosol Dispersion, and Cellular Studies. AAPS PharmSciTech 2014, 15, 1574–1587. [Google Scholar] [CrossRef]
- Mansour, H.; Duan, J.; Vogt, F.G.; Li, X.; Hayes, J.D. Design, characterization, and aerosolization of organic solution advanced spray-dried moxifloxacin and ofloxacin dipalmitoylphosphatidylcholine (DPPC) microparticulate/nanoparticulate powders for pulmonary inhalation aerosol delivery. Int. J. Nanomed. 2013, 8, 3489–3505. [Google Scholar] [CrossRef] [PubMed]
- Chapter <601> Aerosols, Nasal Sprays, Metered-Dose Inhalers, and Dry Powder Inhalers Monograph. In USP 29-NF 24 The United States Pharmacopoeia and The National Formulary: The Official Compendia of Standards. 29/24; The United States Pharmacopeial Convention, Inc.: Rockville, MD, USA, 2006; pp. 2617–2636.
- Acosta, M.F.; Muralidharan, P.; Meenach, S.A.; Hayes, D.; Black, S.M.-; Mansour, H.M. In Vitro Pulmonary Cell Culture in Pharmaceutical Inhalation Aerosol Delivery: 2-D, 3-D, and In Situ Bioimpactor Models. Curr. Pharm. Des. 2016, 22, 2522–2531. [Google Scholar] [CrossRef] [PubMed]
- Meenach, S.A.; Tsoras, A.N.; McGarry, R.C.; Mansour, H.M.; Hilt, J.Z.; Anderson, K.W. Development of three-dimensional lung multicellular spheroids in air- and liquid-interface culture for the evaluation of anticancer therapeutics. Int. J. Oncol. 2016, 48, 1701–1709. [Google Scholar] [CrossRef]
- Kawakubo, H.; Ohno, M. 1-(5-Isoquinolinesulfonyl) Homopiperazine Hydrochloride Hydrates. U.S. Patent 5,942,505, 24 August 1999. [Google Scholar]
- Li, X.; Mansour, H.M. Physicochemical characterization and water vapor sorption of organic solution advanced spray-dried inhalable trehalose microparticles and nanoparticles for targeted dry powder pulmonary inhalation delivery. AAPS PharmSciTech 2011, 12, 1420–1430. [Google Scholar] [CrossRef]
- Li, X.; Vogt, F.G.; Hayes, D., Jr.; Mansour, H.M. Physicochemical characterization and aerosol dispersion performance of organic solution advanced spray-dried microparticulate/nanoparticulate antibiotic dry powders of tobramycin and azithromycin for pulmonary inhalation aerosol delivery. Eur. J. Pharm. Sci. 2014, 52, 191–205. [Google Scholar] [CrossRef]
- Park, C.-W.; Li, X.; Vogt, F.G.; Hayes, D.; Zwischenberger, J.B.; Park, E.-S.; Mansour, H.M. Advanced spray-dried design, physicochemical characterization, and aerosol dispersion performance of vancomycin and clarithromycin multifunctional controlled release particles for targeted respiratory delivery as dry powder inhalation aerosols. Int. J. Pharm. 2013, 455, 374–392. [Google Scholar] [CrossRef]
- Muralidharan, P.; Malapit, M.; Mallory, E.; Hayes, D., Jr.; Mansour, H.M. Inhalable nanoparticulate powders for respiratory delivery. Nanomedicine 2015, 11, 1189–1199. [Google Scholar] [CrossRef]
- Xu, Z.; Mansour, H.M.; Hickey, A.J. Particle Interactions in Dry Powder Inhaler Unit Processes: A Review. J. Adhes. Sci. Technol. 2011, 25, 451–482. [Google Scholar] [CrossRef]
- Hickey, A.J.; Mansour, H.M.; Telko, M.J.; Xu, Z.; Smyth, H.D.; Mulder, T. Physical characterization of component particles included in dry powder inhalers. I. Strategy review and static characteristics. J. Pharm. Sci. 2007, 96, 1282–1301. [Google Scholar] [CrossRef]
- Hickey, A.J.; Mansour, H.M.; Telko, M.J.; Xu, Z.; Smyth, H.D.; Mulder, T. Physical characterization of component particles included in dry powder inhalers. II. Dynamic characteristics. J. Pharm. Sci. 2007, 96, 1302–1319. [Google Scholar] [CrossRef]
- Muralidharan, P.; Hayes, D., Jr.; Mansour, H.M. Dry powder inhalers in COPD, lung inflammation and pulmonary infections. Expert Opin. Drug Deliv. 2015, 12, 947–962. [Google Scholar] [CrossRef]
- Xu, Z.; Mansour, H.M.; Mulder, T.; McLean, R.; Langridge, J.; Hickey, A.J. Comparative Dispersion Study of Dry Powder Aerosols of Albuterol Sulfate/Lactose Monohydrate and Cromolyn Sodium/Lactose Monohydrate Delivered by Standardized Entrainment Tubes. In Respiratory Drug Delivery XI. 3; Dalby, R.N., Bryon, P.R., Suman, J.D., Peart, J., Eds.; Davis Healthcare International Publishing, LLC.: Scotsdale, AZ, USA, 2008; pp. 897–900. [Google Scholar]
- Xu, Z.; Mansour, H.M.; Mulder, T.; McLean, R.; Langridge, J.; Hickey, A.J. Heterogeneous particle deaggregation and its implication for therapeutic aerosol performance. J. Pharm. Sci. 2010, 99, 3442–3461. [Google Scholar] [CrossRef][Green Version]
- Xu, Z.; Mansour, H.M.; Mulder, T.; McLean, R.; Langridge, J.; Hickey, A.J. Dry powder aerosols generated by standardized entrainment tubes from drug blends with lactose monohydrate: 2. Ipratropium bromide monohydrate and fluticasone propionate. J. Pharm. Sci. 2010, 99, 3415–3429. [Google Scholar] [CrossRef] [PubMed]
- Xu, Z.; Mansour, H.M.; Mulder, T.; McLean, R.; Langridge, J.; Hickey, A.J. Dry powder aerosols generated by standardized entrainment tubes from drug blends with lactose monohydrate: 1. albuterol sulfate and disodium cromoglycate. J. Pharm. Sci. 2010, 99, 3398–3414. [Google Scholar] [CrossRef] [PubMed]
- Weiler, C.; Egen, M.; Trunk, M.; Langguth, P. Force control and powder dispersibility of spray dried particles for inhalation. J. Pharm. Sci. 2010, 99, 303–316. [Google Scholar] [CrossRef] [PubMed]
- Hassan, M.S.; Lau, R.W. Effect of particle shape on dry particle inhalation: Study of flowability, aerosolization, and deposition properties. AAPS PharmSciTech 2009, 10, 1252–1262. [Google Scholar] [CrossRef]
- Yang, F.F.; Liu, X.B.; Wang, W.; Liu, C.Y.; Quan, L.H.; Liao, Y.H. The effects of surface morphology on the aerosol performance of spray-dried particles within HFA 134a based metered dose formulations. Asian J. Pharm. Sci. 2015, 10, 513–519. [Google Scholar] [CrossRef]

| Feed Pump Rate (PR) % | 25% (7.5 mL/min) | 50% (15 mL/min) | 75% (22.5 mL/min) | 100% (30 mL/min) |
|---|---|---|---|---|
| Inlet Temperature (°C) | 149–152 | 150–151 | 150–151 | 150–152 |
| Outlet Temperature (°C) | 76–88 | 67–68 | 55–65 | 43–56 |
| Aspirator rate (m3/h) | 37.5 | 37.5 | 37.5 | 37.5 |
| Atomization gas flow rate (L/h) | 670 | 670 | 670 | 670 |
| Spray Drying Pump Rate (%) | Size Range (µm) | D50 (Mean) Size (µm) |
|---|---|---|
| 25 | 0.27–1.677 | 0.068 ± 0.023 |
| 50 | 0.343–1.938 | 0.855 ± 0.302 |
| 75 | 0.346–3.199 | 1.075 ± 0.510 |
| 100 | 0.454–2.778 | 1.168 ± 0.507 |
| Powder Identification | Spray Drying Pump Rate (%) | DSC Peaks | Tpeaks (°C) | ΔH (W/g) | Tg (peak) (°C) | ΔCp (J/g °C) |
|---|---|---|---|---|---|---|
| Raw FAS | N/A | Transition 1 Transition 2 Tm (Fas) | 137.19 ± 0.19 159.86 ± 4.94 215.01 ± 0.30 | 55.06 ± 3.29 16.93 ± 3.62 105.5 ± 2.89 | N/A | N/A |
| SD FAS | 25 | Tc Tm (Fas) | 86.10 ± 1.91 209.28 ± 0.71 | 45.35 ± 3.09 88.18 ± 12.69 | 46.91 ± 1.05 | 1.33 ± 0.17 |
| SD FAS | 50 | Tc Tm (Fas) Tm (Fas) | 106.66 ± 0.79 209.47 ± 0.37 215.79± 0.36 | 41.54 ± 11.58 8.54 ± 2.04 44.26 ± 14.19 | 47.07 ± 0.44 | 1.15 ± 0.44 |
| SD FAS | 75 | Tc Tm (Fas) Tm (Fas) | 108.13 ± 0.99 210.52 ± 0.54 216.61 ± 0.42 | 41.50 ± 5.76 45.81 ± 7.8 23.59 ± 1.60 | 49.47 ± 3.42 | 0.49 ± 0.17 |
| SD FAS | 100 | Tc Tm (Fas) Tm (Fas) | 76.25 ± 3.26 186.84 ± 20.81 211.51 ± 2.07 | 39.13 ± 8.46 16.66 ± 0.22 34.48 ± 5.49 | 51.80 ± 1.34 | 0.50 ± 0.22 |
| Powder Identification | Spray Drying Pump Rate (%) | Residual Water Content (% w/w) |
|---|---|---|
| Raw FAS | N/A | 2.97 ± 0.06 |
| SD FAS | 25 | 3.22 ± 0.56 |
| SD FAS | 50 | 2.57 ± 0.36 |
| SD FAS | 75 | 2.45 ± 0.49 |
| SD FAS | 100 | 2.73 ± 0.57 |
| Aerolizer® | Neohaler® | HandiHaler® | |
|---|---|---|---|
| SD FAS 25% | |||
| FPF (%) | 17.79 ± 3.78 | 16.63 ± 4.78 | 16.65 ± 1.76 |
| RF (%) | 42.28 ± 22.14 | 36.82 ± 17.75 | 22.17 ± 2.67 |
| ED (%) | 97.16 ± 2.86 | 103.49 ± 1.26 | 98.56 ± 2.49 |
| MMAD (µm) | 10.18 ± 5.26 | 11.07 ± 5.25 | 22.33 ± 7.06 |
| GSD | 2.38 ± 0.36 | 2.78 ± 0.26 | 3.58 ± 0.57 |
| SD FAS 50% | |||
| FPF (%) | 30.16 ± 3.74 | 21.83 ± 5.94 | 16.53 ± 3.06 |
| RF (%) | 50.79 ± 22.19 | 47.78 ± 22.94 | 23.36 ± 2.15 |
| ED (%) | 103.71 ± 2.76 | 106.29 ± 3.17 | 99.58 ± 0.44 |
| MMAD (µm) | 6.53 ± 2.87 | 9.00 ± 4.49 | 17.83 ± 1.60 |
| GSD | 2.2 ± 0.22 | 2.37 ± 0.38 | 3.27 ± 0.05 |
| SD FAS 75% | |||
| FPF (%) | 21.35 ± 7.05 | 38.21 ± 10.42 | 15.2 ± 0.59 |
| RF (%) | 61.15 ± 27.24 | 48.59 ± 21.79 | 20.07 ± 4.05 |
| ED (%) | 94.52 ± 10.42 | 102.59 ± 1.52 | 92.64 ± 6.62 |
| MMAD (µm) | 6.62 ± 2.98 | 8.84 ± 3.86 | 18.77 ± 0.44 |
| GSD | 2.38 ± 0.31 | 2.12 ± 0.477 | 3.15 ± 0.20 |
| SD FAS 100% | |||
| FPF (%) | 15.32 ± 1.44 | 26.65 ± 7.83 | 21.082 ± 1.40 |
| RF (%) | 67.27 ± 29.31 | 55.74 ± 24.88 | 30.83 ± 2.23 |
| ED (%) | 78.07 ± 1.52 | 103.12 ± 0.98 | 80.57 ± 8.97 |
| MMAD (µm) | 6.77 ± 3.11 | 7.22 ± 3.15 | 12.54 ± 1.11 |
| GSD | 1.86 ± 0.33 | 2.15 ± 0.18 | 3.04 ± 0.41 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Muralidharan, P.; Hayes, D., Jr.; Fineman, J.R.; Black, S.M.; Mansour, H.M. Advanced Microparticulate/Nanoparticulate Respirable Dry Powders of a Selective RhoA/Rho Kinase (Rock) Inhibitor for Targeted Pulmonary Inhalation Aerosol Delivery. Pharmaceutics 2021, 13, 2188. https://doi.org/10.3390/pharmaceutics13122188
Muralidharan P, Hayes D Jr., Fineman JR, Black SM, Mansour HM. Advanced Microparticulate/Nanoparticulate Respirable Dry Powders of a Selective RhoA/Rho Kinase (Rock) Inhibitor for Targeted Pulmonary Inhalation Aerosol Delivery. Pharmaceutics. 2021; 13(12):2188. https://doi.org/10.3390/pharmaceutics13122188
Chicago/Turabian StyleMuralidharan, Priya, Don Hayes, Jr., Jeffrey R. Fineman, Stephen M. Black, and Heidi M. Mansour. 2021. "Advanced Microparticulate/Nanoparticulate Respirable Dry Powders of a Selective RhoA/Rho Kinase (Rock) Inhibitor for Targeted Pulmonary Inhalation Aerosol Delivery" Pharmaceutics 13, no. 12: 2188. https://doi.org/10.3390/pharmaceutics13122188
APA StyleMuralidharan, P., Hayes, D., Jr., Fineman, J. R., Black, S. M., & Mansour, H. M. (2021). Advanced Microparticulate/Nanoparticulate Respirable Dry Powders of a Selective RhoA/Rho Kinase (Rock) Inhibitor for Targeted Pulmonary Inhalation Aerosol Delivery. Pharmaceutics, 13(12), 2188. https://doi.org/10.3390/pharmaceutics13122188








