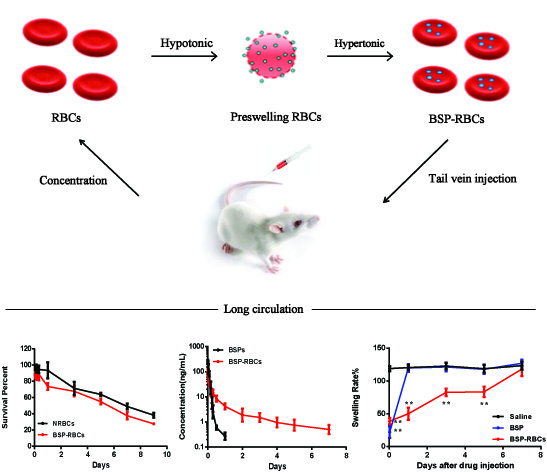
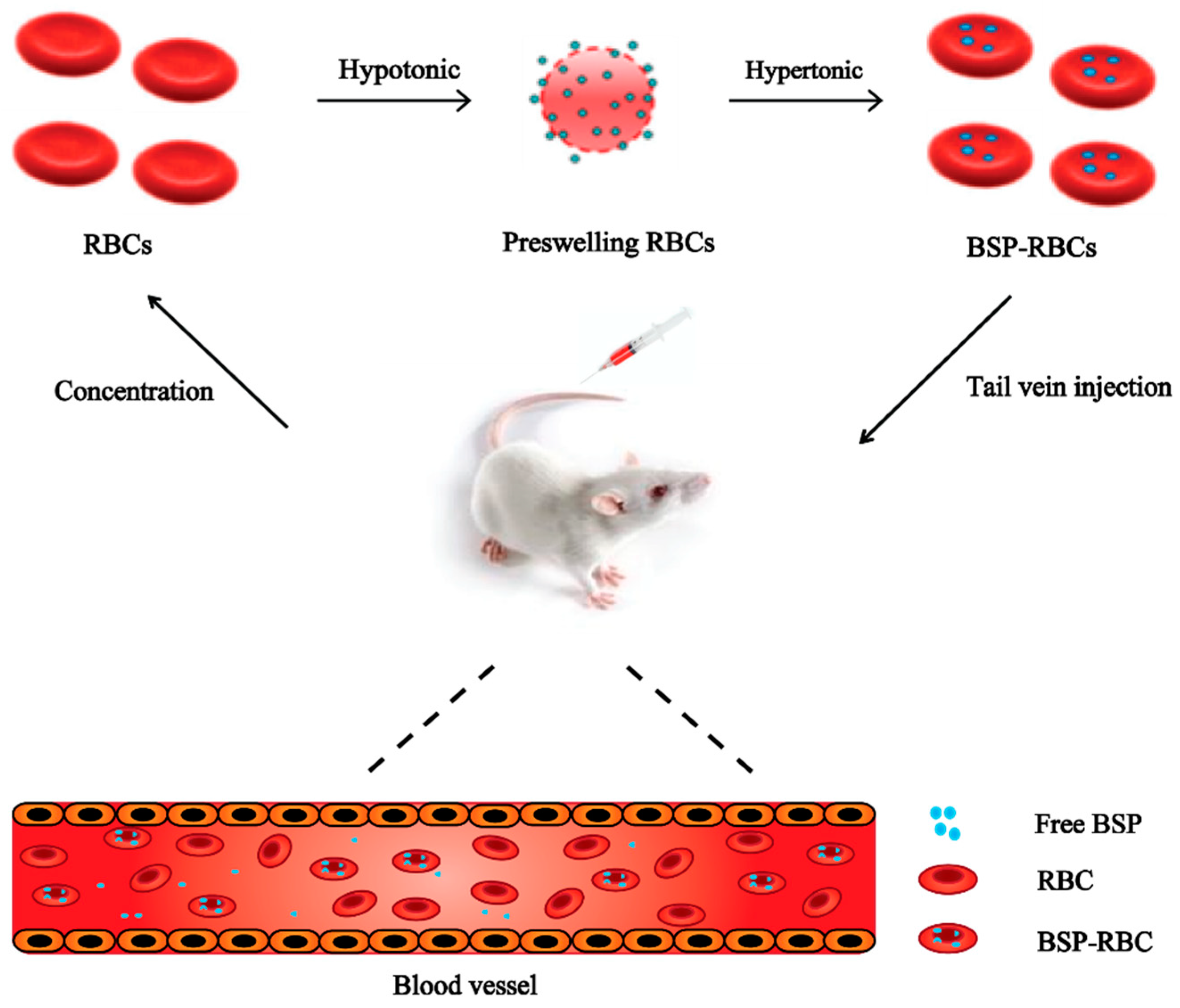
Autologous Red Blood Cell Delivery of Betamethasone Phosphate Sodium for Long Anti-Inflammation
Abstract
1. Introduction
2. Materials and Methods
2.1. Materials
2.2. Animals
2.3. Preparation of BSP-RBCs
2.4. Quantification of Drug
2.5. Scanning Electron Microscopy (SEM)
2.6. Osmotic Fragility
2.7. Activity of Na+/K+-ATPase
2.8. Phosphatidylserine(PS) Exposure
2.9. Survival in Circulation
2.10. Pharmacokinetics (PK)
2.11. In Vivo Anti-Inflammatory Effect
2.12. Statistical and Data Analyses
3. Results and Discussion
3.1. Quantification of Drug
3.2. Scanning Electron Microscopy
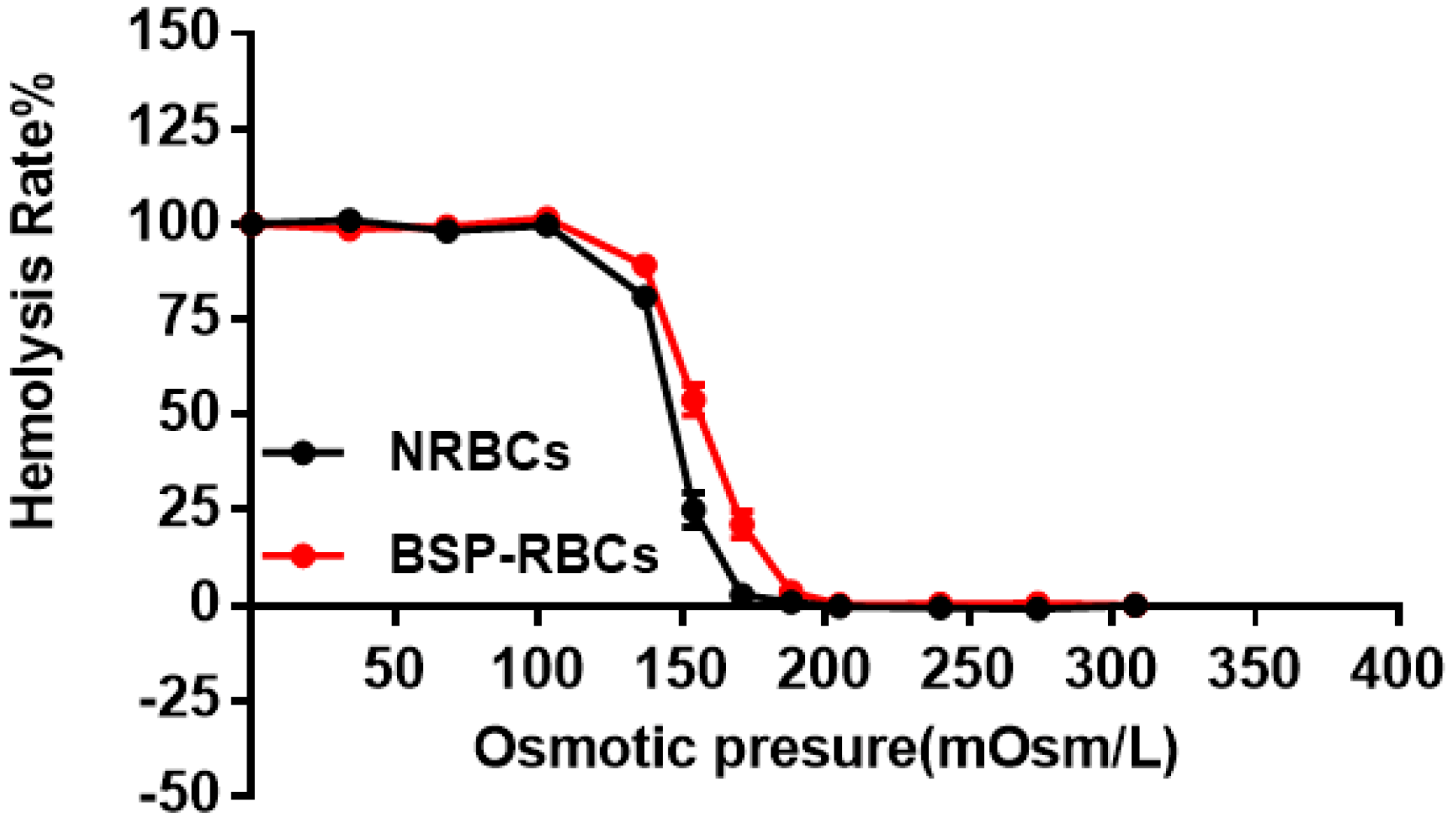
3.3. Osmotic Fragility
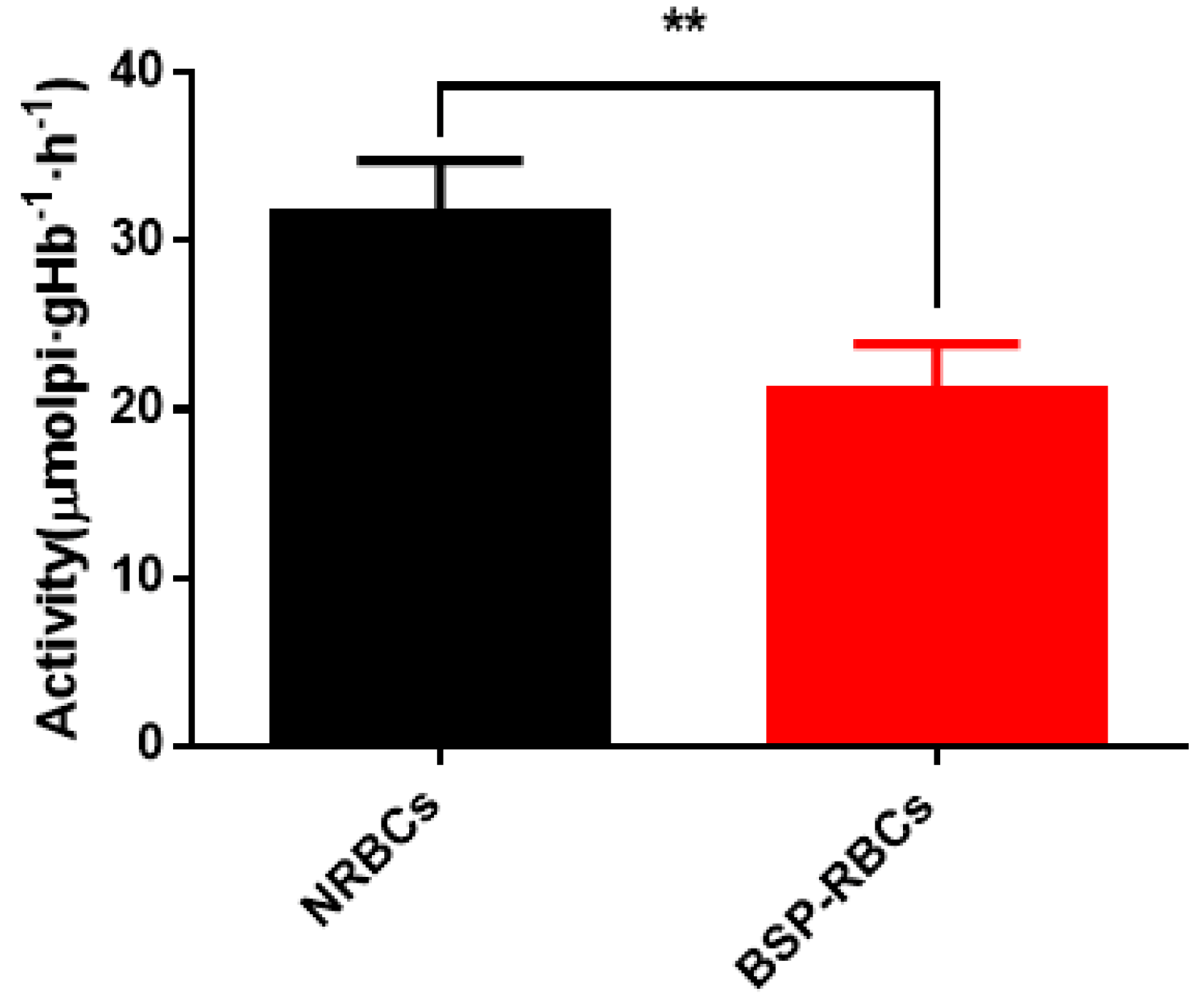
3.4. Activity of Na+/K+-ATPase
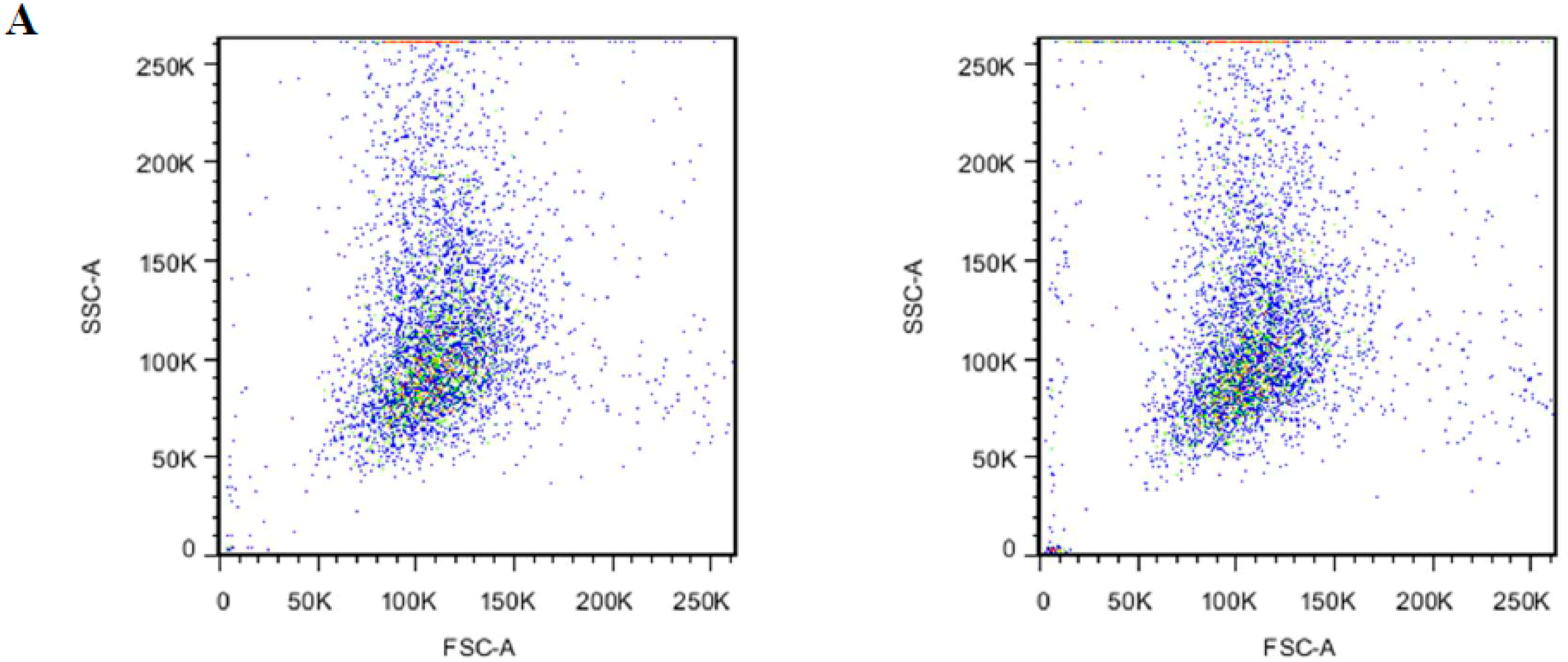
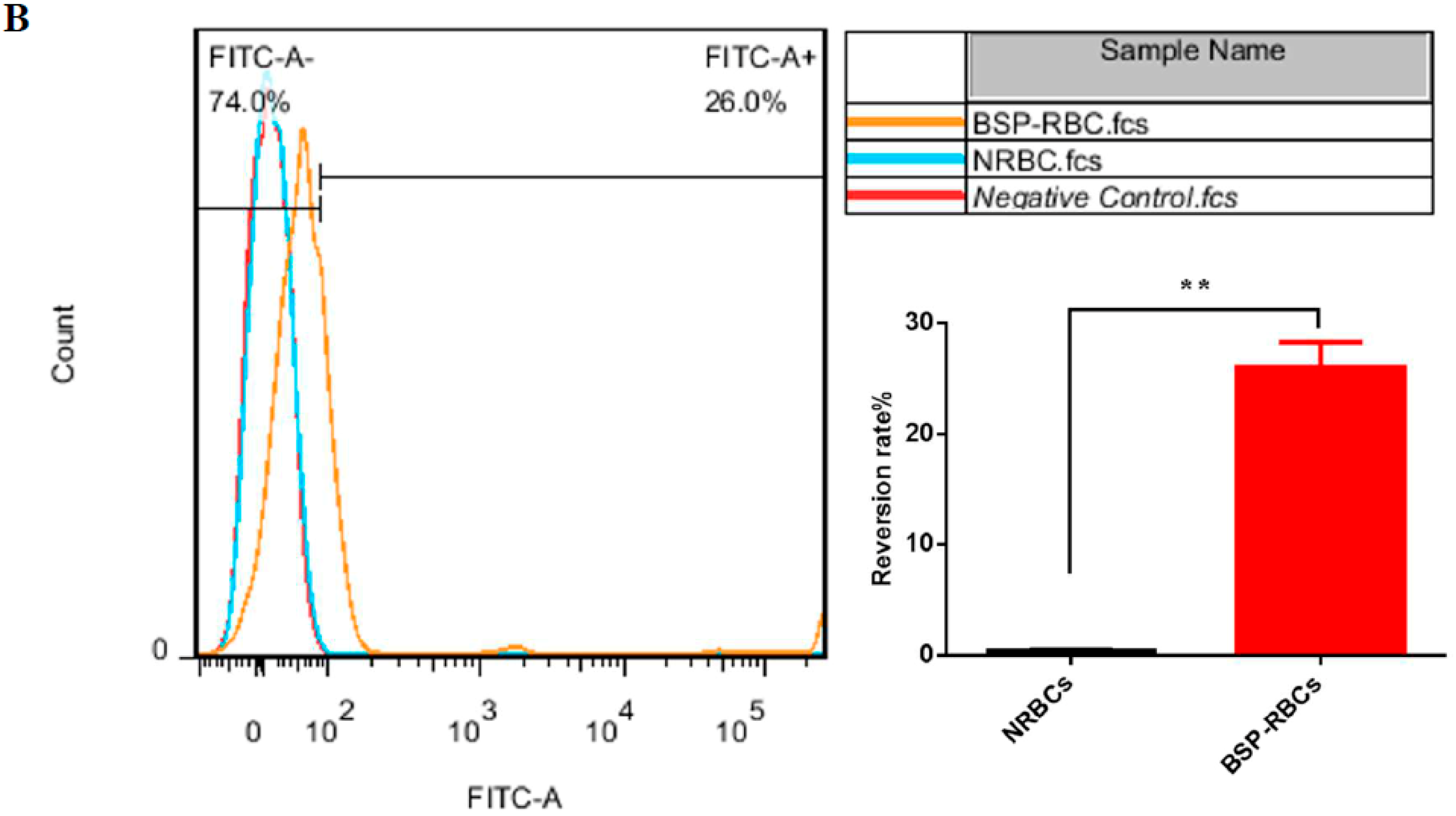
3.5. Phosphatidylserineexposure
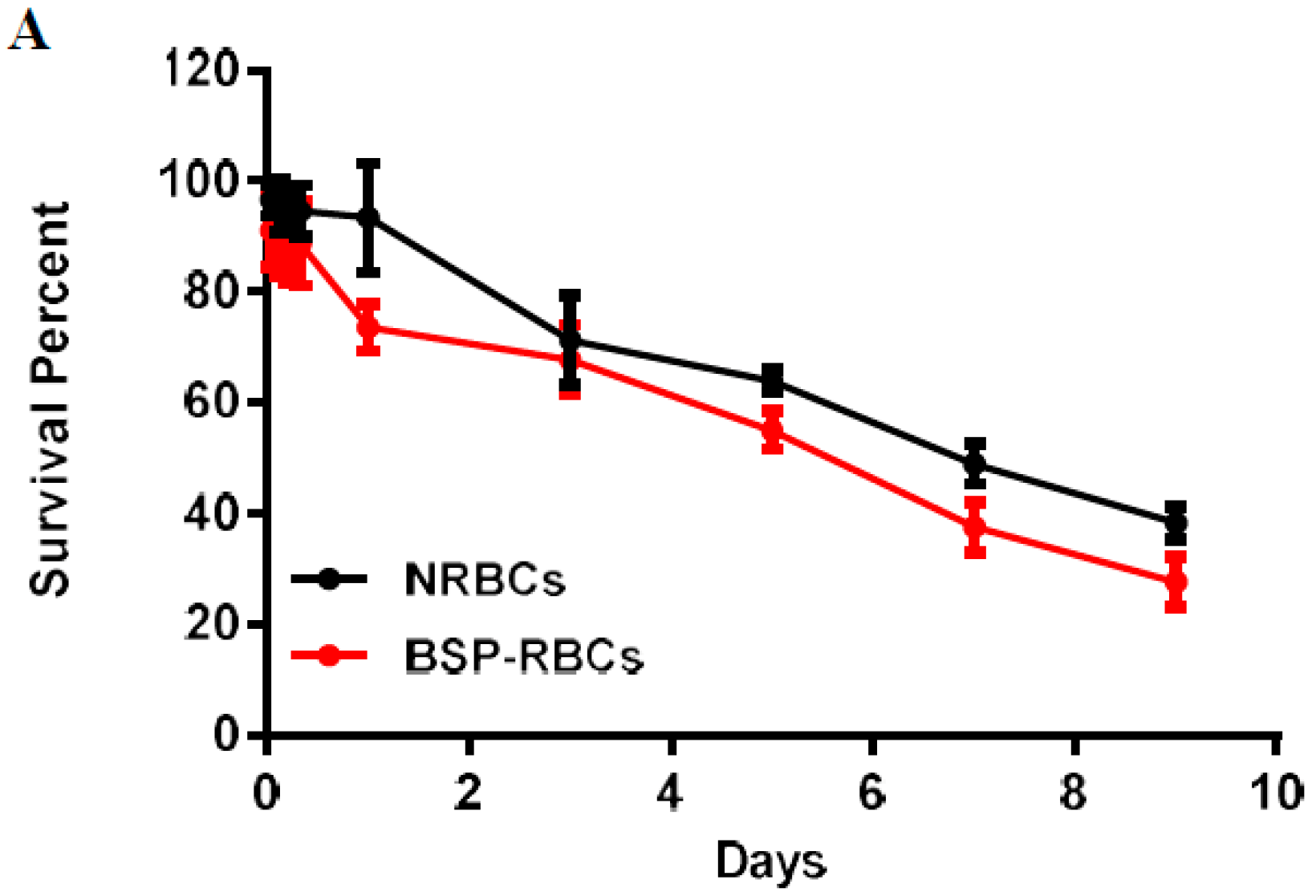
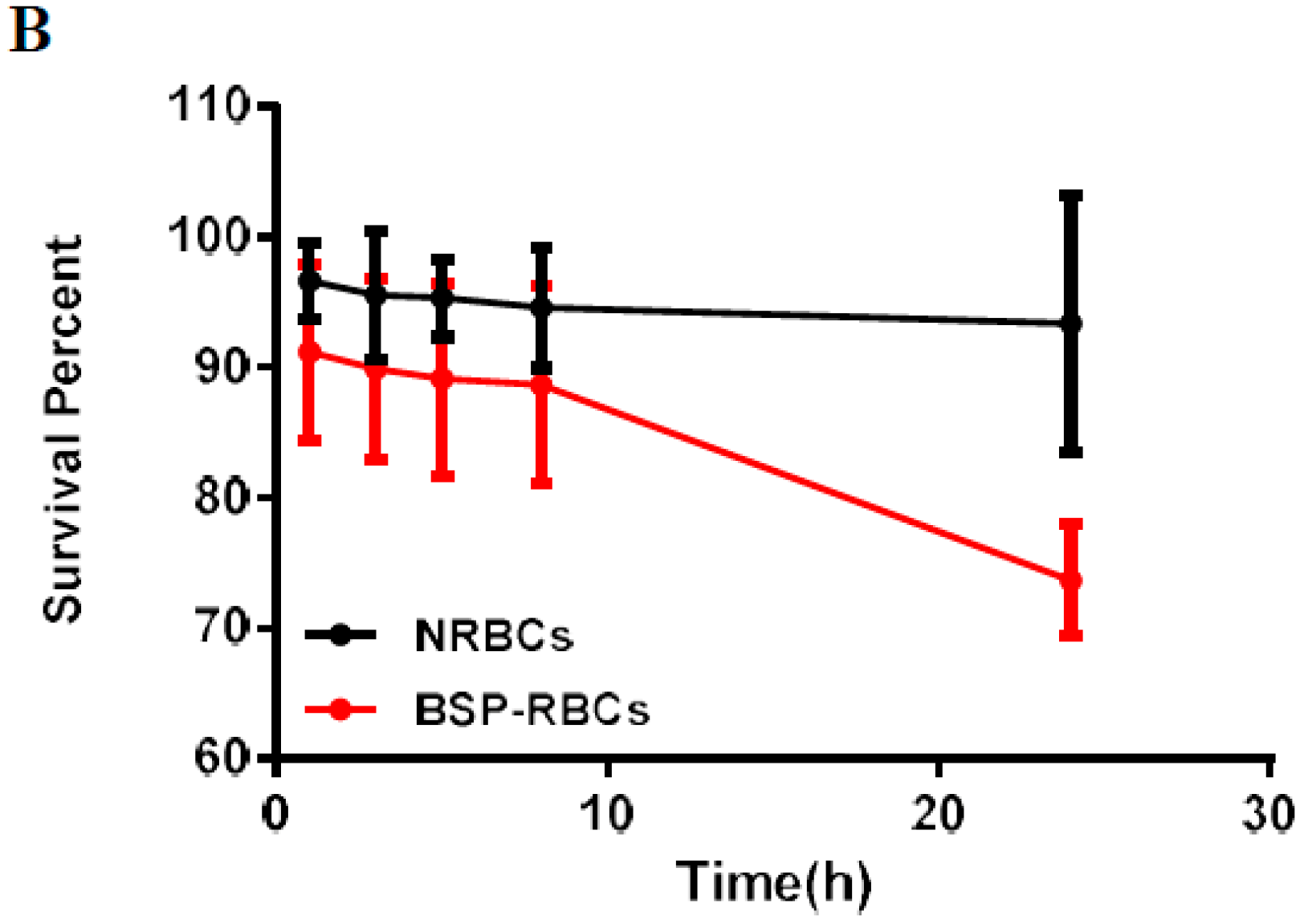
3.6. Survival of BSP-RBC
3.7. Pharmacokinetics
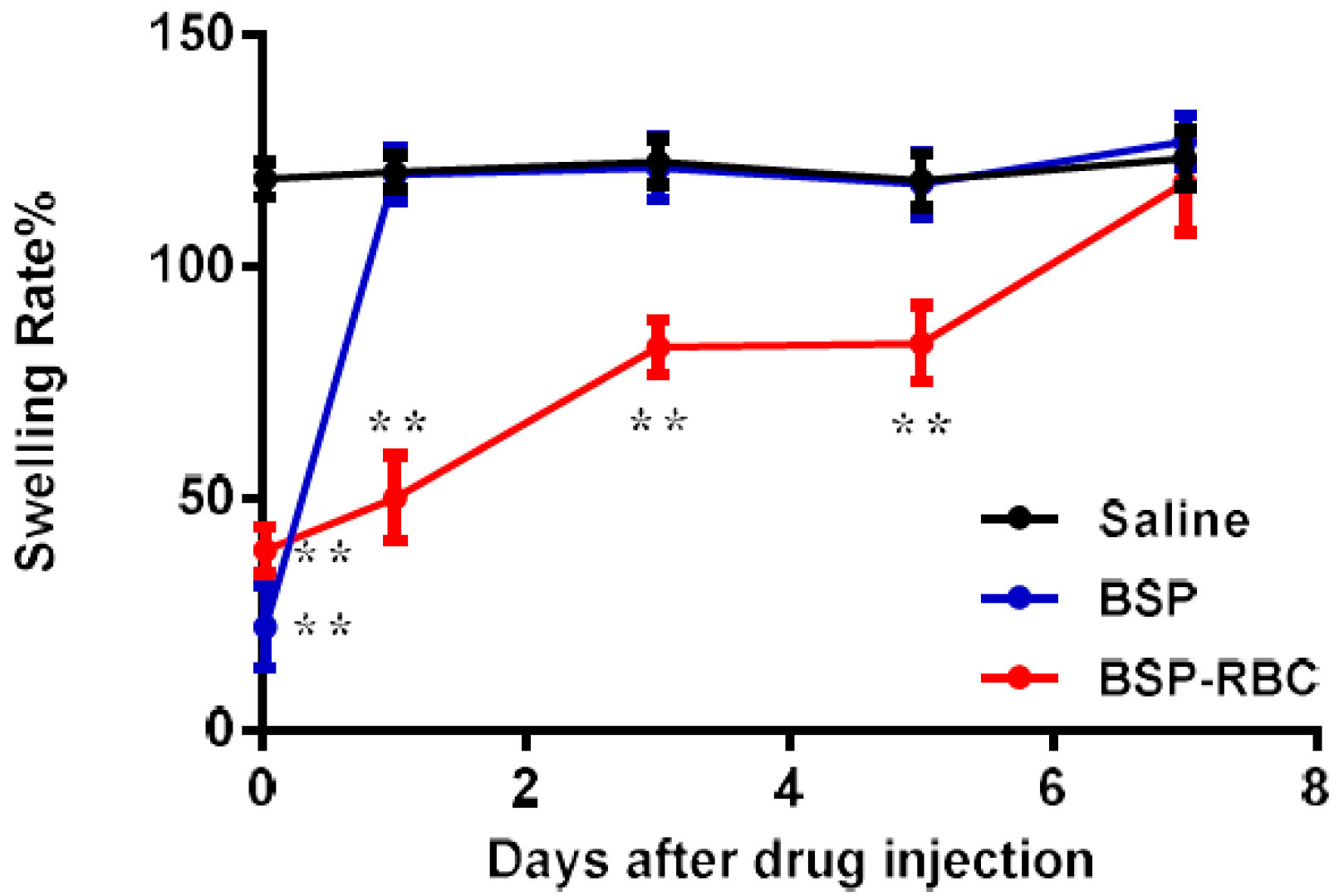
3.8. In Vivo Determination of Anti-Inflammatory Effect
4. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Dahl, R. Systemic side effects of inhaled corticosteroids in patients with asthma. Respir. Med. 2006, 100, 1307–1317. [Google Scholar] [CrossRef] [PubMed]
- Gerber, A.N. Measuring safety of inhaled corticosteroids in asthma. Ann. Allergy Asthma Immunol. 2016, 117, 577–581. [Google Scholar] [CrossRef] [PubMed]
- Rossi, G.A.; Cerasoli, F.; Cazzola, M. Safety of inhaled corticosteroids: Room for improvement. Pulm. Pharmacol. Ther. 2005, 20, 23–25. [Google Scholar] [CrossRef] [PubMed]
- Umland, S.P.; Schleimer, R.P.; Johnston, S.L. Review of the Molecular and Cellular Mechanisms of Action of Glucocorticoids for Use in Asthma. Pulm. Pharmacol. Ther. 2002, 15, 35–50. [Google Scholar] [CrossRef] [PubMed]
- Ishihara, T.; Izumo, N.; Higaki, M.; Shimada, E.; Hagi, T.; Mine, L.; Ogawa, Y.; Mizushima, Y. Role of zinc in formulation of PLGA/PLA nanoparticles encapsulating betamethasone phosphate and its release profile. J. Control. Release 2005, 105, 68–76. [Google Scholar] [CrossRef] [PubMed]
- Ishihara, T.; Takahashi, M.; Higaki, M.; Mizushima, Y. Efficient encapsulation of a water-soluble corticosteroid in biodegradable nanoparticles. Int. J. Pharm. 2008, 365, 200–205. [Google Scholar] [CrossRef]
- Ishihara, T.; Kubota, T.; Choi, T.; Takahashi, M.; Ayano, E.; Kanazawa, H.; Higaki, M. Polymeric nanoparticles encapsulating betamethasone phosphate with different release profiles and stealthiness. Int. J. Pharm. 2009, 375, 148–154. [Google Scholar] [CrossRef]
- Bazile, D.; Prud’homme, C.; Bassoullet, M.T.; Marlard, M.; Spenlehauer, G.; Veillard, M. Stealth Me. PEG-PLA nanoparticles avoid uptake by the mononuclear phagocytes system. J. Pharm. Sci. 1995, 84, 493–498. [Google Scholar] [CrossRef]
- Timin, A.S.; Litvak, M.M.; Gorin, D.A.; Atochina-Vasserman, E.N.; Atochin, D.N.; Sukhorukov, G.B. Cell-Based Drug Delivery and Use of Nano-and Microcarriers for Cell Functionalization. Adv. Healthc. Mater. 2018, 7, 1700818. [Google Scholar] [CrossRef]
- Han, X.; Wang, C.; Liu, Z. Red blood cells as smart delivery systems. Bioconjug. Chem. 2018, 29, 852–860. [Google Scholar] [CrossRef]
- Biagiotti, S.; Paoletti, M.F.; Fraternale, A.; Rossi, L.; Magnani, M. Drug delivery by red blood cells. IUBMB Life 2011, 63, 621–631. [Google Scholar] [CrossRef] [PubMed]
- Pierigè, F.; Serafini, S.; Rossi, L.; Magnani, M. Cell-based drug delivery. Adv. Drug Deliv. Rev. 2008, 60, 286–295. [Google Scholar] [CrossRef] [PubMed]
- Rossi, L.; Serafini, S.; Pierigé, F.; Antonelli, A.; Cerasi, A.; Fraternale, A.; Chiarantini, L.; Magnani, M. Erythrocyte-based drug delivery. Expert Opin. Drug Deliv. 2005, 2, 311–322. [Google Scholar] [CrossRef] [PubMed]
- Sun, Y.; Su, J.; Liu, G.; Chen, J.; Zhang, X.; Zhang, R.; Jiang, M.; Qiu, M. Advances of blood cell-based drug delivery systems. Eur. J. Pharm. Sci. 2017, 96, 115–128. [Google Scholar] [CrossRef] [PubMed]
- Hu, C.M.J.; Fang, R.H.; Zhang, L. Erythrocyte-Inspired Delivery Systems. Adv. Healthc. Mater. 2012, 1, 537–547. [Google Scholar] [CrossRef] [PubMed]
- Tan, S.; Wu, T.; Zhang, D.; Zhang, Z. Cell or cell membrane-based drug delivery systems. Theranostics 2015, 5, 863. [Google Scholar] [CrossRef] [PubMed]
- Hamidi, M.; Zarrin, A.; Foroozesh, M.; Mohammadi-Samani, S. Applications of carrier erythrocytes in delivery of biopharmaceuticals. J. Control. Release 2007, 118, 145–160. [Google Scholar] [CrossRef]
- Matovcik, L.M.; Junga, I.G.; Schrier, S.L. Drug-induced endocytosis of neonatal erythrocytes. Blood 1985, 65, 1056–1063. [Google Scholar]
- Wang, C.; Ye, Y.; Sun, W.; Yu, J.; Wang, J.; Lawrence, D.S.; Buse, J.B.; Gu, Z. Red Blood Cells for Glucose-Responsive Insulin Delivery. Adv. Mater. 2017, 29, 1606617. [Google Scholar] [CrossRef]
- Magnani, M.; Rossi, L. Approaches to erythrocyte-mediated drug delivery. Expert Opin. Drug Deliv. 2014, 11, 677–687. [Google Scholar] [CrossRef]
- Kumari, R.; Panda, P.; Singh, R.; Vishwakarma, D.; Mishra, J.; Verma, N.K. Resealed Erythrocyte: An Approach to Targeted Drug Delivery. Chem. J. 2018, 1, 1–11. [Google Scholar]
- He, H.; Ye, J.; Wang, Y.; Liu, Q.; Chung, H.S.; Kwon, Y.M.; Shin, M.C.; Lee, K.; Yang, V.C. Cell-penetrating peptides meditated encapsulation of protein therapeutics into intact red blood cells and its application. J. Control. Release 2014, 176, 123–132. [Google Scholar] [CrossRef] [PubMed]
- Ge, D.; Zou, L.; Li, C.; Liu, S.; Li, S.; Sun, S.; Ding, W. Simulation of the osmosis-based drug encapsulation in erythrocytes. Eur. Biophys. J. 2018, 47, 261–270. [Google Scholar] [CrossRef] [PubMed]
- Hamidi, M.; Zarei, N.; Zarrin, A.; Mohammadi-Samani, S. Preparation and in vitro characterization of carrier erythrocytes for vaccine delivery. Int. J. Pharm. 2007, 338, 70–78. [Google Scholar] [CrossRef] [PubMed]
- Fadok, V.; Voelker, D.; Campbell, P.; Cohen, J.; Bratton, D.; Henson, P. Exposure of phosphatidylserine on the surface of apoptotic lymphocytes triggers specific recognition and removal by macrophages. J. Immunol. 1992, 148, 2207–2216. [Google Scholar] [PubMed]
- Mambrini, G.; Mandolini, M.; Rossi, L.; Pierigè, F.; Capogrossi, G.; Salvati, P.; Serafini, S.; Benatti, L.; Magnani, M. Ex vivo encapsulation of dexamethasone sodium phosphate into human autologous erythrocytes using fully automated biomedical equipment. Int. J. Pharm. 2017, 517, 175–184. [Google Scholar] [CrossRef] [PubMed]
- Mock, D.M.; Matthews, N.I.; Strauss, R.G.; Burmeister, L.F.; Schmidt, R.; Widness, J.A. Red blood cell volume can be independently determined in vitro using sheep and human red blood cells labeled at different densities of biotin. Transfusion 2009, 49, 1178–1185. [Google Scholar] [CrossRef]
- Zhang, Y.; Huo, M.; Zhou, J.; Xie, S. PKSolver: An add-in program for pharmacokinetic and pharmacodynamic data analysis in Microsoft Excel. Comput. Methods Programs Biomed. 2010, 99, 306–314. [Google Scholar] [CrossRef]
- Wang, Y.; Tu, S.; Steffen, D.; Xiong, M. Iron Complexation to Histone Deacetylase Inhibitors SAHA and LAQ824 in PEGylated Liposomes Can Considerably Improve Pharmacokinetics in Rats. J. Pharm. Pharm. Sci. 2014, 17, 583–602. [Google Scholar] [CrossRef]
- Higaki, M.; Ishihara, T.; Izumo, N.; Takatsu, M.; Mizushima, Y. Treatment of experimental arthritis with poly (D, L-lactic/glycolic acid) nanoparticles encapsulating betamethasone sodium phosphate. Ann. Rheum. Dis. 2005, 64, 1132–1136. [Google Scholar] [CrossRef]
- Briones, E.; Colino, C.I.; Lanao, J.M. Study of the factors influencing the encapsulation of zidovudine in rat erythrocytes. Int. J. Pharm. 2010, 401, 41–46. [Google Scholar] [CrossRef] [PubMed]
- Hamidi, M.; Tajerzadeh, H.; Dehpour, A.-R.; Rouini, M.-R.; Ejtemaee-Mehr, S. In vitro characterization of human intact erythrocytes loaded by enalaprilat. Drug Deliv. 2001, 8, 223–230. [Google Scholar] [CrossRef] [PubMed]
- Alanazi, F.K.; Harisa, G.E.-D.I.; Maqboul, A.; Abdel-Hamid, M.; Neau, S.H.; Alsarra, I.A. Biochemically altered human erythrocytes as a carrier for targeted delivery of primaquine: An in vitro study. Arch. Pharm. Res. 2011, 34, 563–571. [Google Scholar] [CrossRef] [PubMed]
- Harisa, G.I.; Ibrahim, M.F.; Alanazi, F.; Shazly, G.A. Engineering erythrocytes as a novel carrier for the targeted delivery of the anticancer drug paclitaxel. Saudi Pharm. J. 2014, 22, 223–230. [Google Scholar] [CrossRef] [PubMed]
- Hamidi, M.; Zarrin, A.H.; Foroozesh, M.; Zarei, N.; Mohammadi-Samani, S. Preparation and in vitro evaluation of carrier erythrocytes for RES-targeted delivery of interferon-alpha 2b. Int. J. Pharm. 2007, 341, 125–133. [Google Scholar] [CrossRef] [PubMed]
- Kowluru, R.; Bitensky, M.; Kowluru, A.; Dembo, M.; Keaton, P.; Buican, T. Reversible sodium pump defect and swelling in the diabetic rat erythrocyte: Effects on filterability and implications for microangiopathy. Proc. Natl. Acad. Sci. USA 1989, 86, 3327–3331. [Google Scholar] [CrossRef] [PubMed]
- Forst, T.; De La Tour, D.D.; Kunt, T.; Pfützner, A.; Goitom, K.; Pohlmann, T.; Schneider, S.; Johansson, B.; Wahren, J.; Löbig, M. Effects of proinsulin C-peptide on nitric oxide, microvascular blood flow and erythrocyte Na+, K+-ATPase activity in diabetes mellitus type I. Clin. Sci. 2000, 98, 283–290. [Google Scholar] [CrossRef] [PubMed]
- Staedtke, V.; Brähler, M.; Müller, A.; Georgieva, R.; Bauer, S.; Sternberg, N.; Voigt, A.; Lemke, A.; Keck, C.; Möschwitzer, J. In vitro inhibition of fungal activity by macrophage-mediated sequestration and release of encapsulated Amphotericin B nanosupension in red blood cells. Small 2010, 6, 96–103. [Google Scholar] [CrossRef] [PubMed]
- Lizano, C.; Pérez, M.T.; Pinilla, M. Mouse erythrocytes as carriers for coencapsulated alcohol and aldehyde dehydrogenase obtained by electroporation: In vivo survival rate in circulation, organ distribution and ethanol degradation. Life Sci. 2001, 68, 2001–2016. [Google Scholar] [CrossRef]

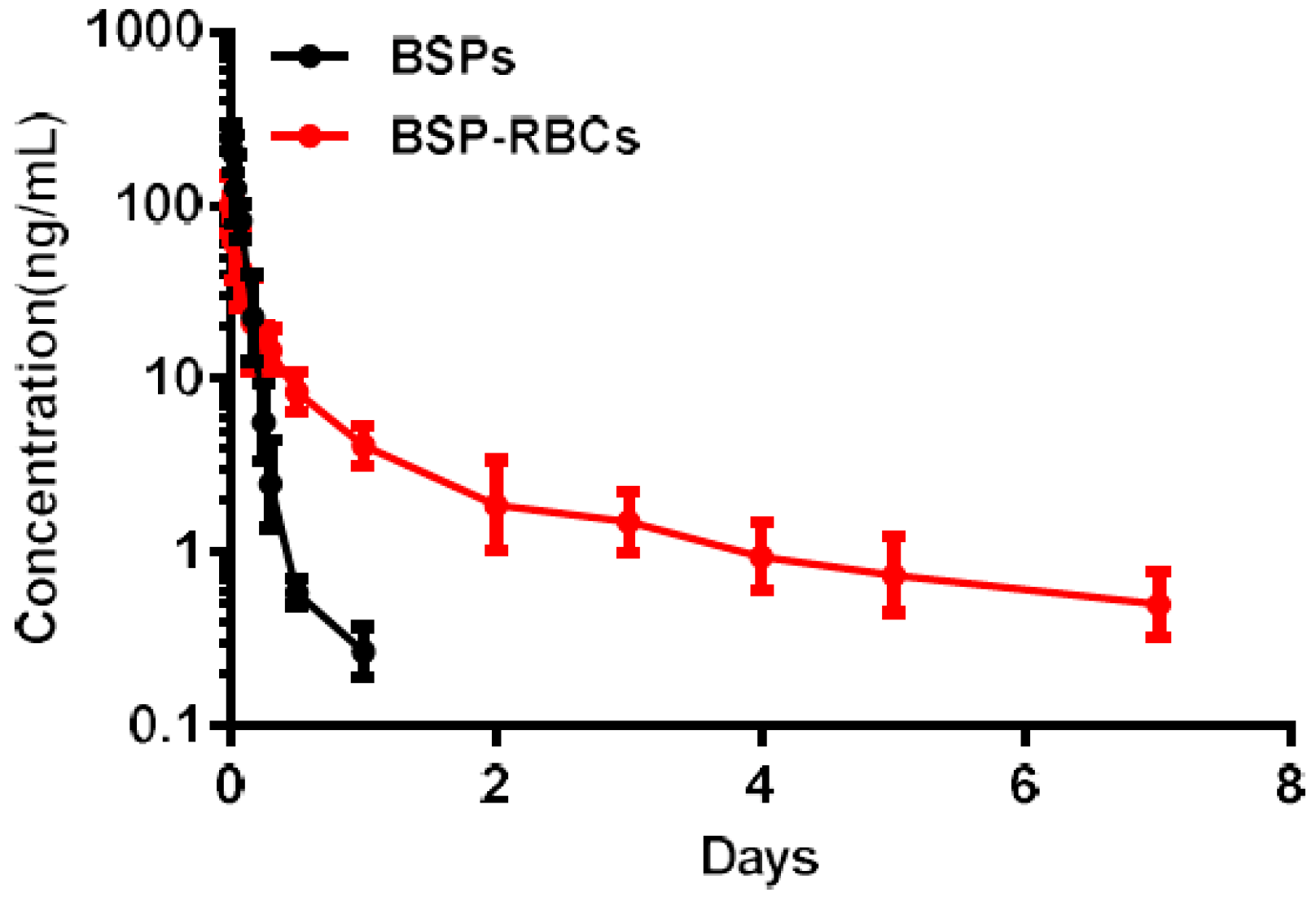
| Preparations | T1/2 (d) | Cmax (ng/mL) | AUC0–t (ng/mL*d) | AUC0–∞ (ng/mL*d) |
|---|---|---|---|---|
| BSP | 0.15 ± 0.03 | 245.77 ± 23.09 | 18.13 ± 4.67 | 18.17 ± 4.67 |
| BSP-RBC | 3.31 ± 0.82 | 101.40 ± 17.83 | 23.81 ± 6.13 | 26.21 ± 6.75 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Zhang, X.; Qiu, M.; Guo, P.; Lian, Y.; Xu, E.; Su, J. Autologous Red Blood Cell Delivery of Betamethasone Phosphate Sodium for Long Anti-Inflammation. Pharmaceutics 2018, 10, 286. https://doi.org/10.3390/pharmaceutics10040286
Zhang X, Qiu M, Guo P, Lian Y, Xu E, Su J. Autologous Red Blood Cell Delivery of Betamethasone Phosphate Sodium for Long Anti-Inflammation. Pharmaceutics. 2018; 10(4):286. https://doi.org/10.3390/pharmaceutics10040286
Chicago/Turabian StyleZhang, Xiumei, Mingfeng Qiu, Pengcheng Guo, Yumei Lian, Enge Xu, and Jing Su. 2018. "Autologous Red Blood Cell Delivery of Betamethasone Phosphate Sodium for Long Anti-Inflammation" Pharmaceutics 10, no. 4: 286. https://doi.org/10.3390/pharmaceutics10040286
APA StyleZhang, X., Qiu, M., Guo, P., Lian, Y., Xu, E., & Su, J. (2018). Autologous Red Blood Cell Delivery of Betamethasone Phosphate Sodium for Long Anti-Inflammation. Pharmaceutics, 10(4), 286. https://doi.org/10.3390/pharmaceutics10040286