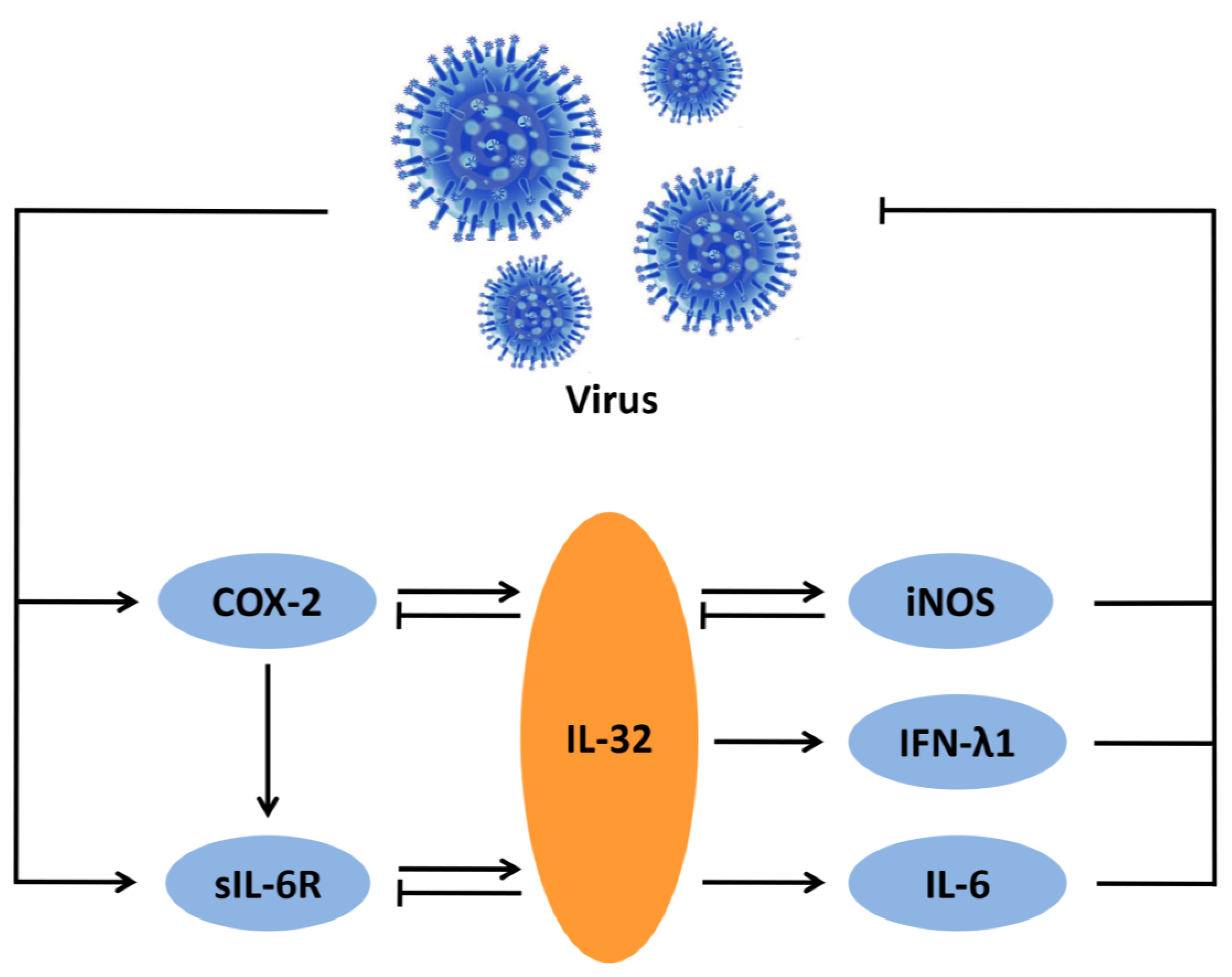
Important Role of the IL-32 Inflammatory Network in the Host Response against Viral Infection
Abstract
:1. Introduction
3. Conclusions
Acknowledgment
Author Contributions
Conflicts of Interest
References
- Li, W.; Liu, Y.; Mukhtar, M.M.; Gong, R.; Pan, Y.; Rasool, S.T.; Gao, Y.; Kang, L.; Hao, Q.; Peng, G.; et al. Activation of interleukin-32 pro-inflammatory pathway in response to influenza A virus infection. PLoS ONE 2008, 3, e1985. [Google Scholar] [CrossRef] [PubMed]
- Dahl, C.A.; Schall, R.P.; He, H.L.; Cairns, J.S. Identification of a novel gene expressed in activated natural killer cells and T cells. J. Immunol. 1992, 148, 597–603. [Google Scholar] [PubMed]
- Kim, S.H.; Han, S.Y.; Azam, T.; Yoon, D.Y.; Dinarello, C.A. Interleukin-32: A cytokine and inducer of TNFalpha. Immunity 2005, 22, 131–142. [Google Scholar] [CrossRef] [PubMed]
- Goda, C.; Kanaji, T.; Kanaji, S.; Tanaka, G.; Arima, K.; Ohno, S.; Izuhara, K. Involvement of IL-32 in activation-induced cell death in T cells. Int. Immunol. 2006, 18, 233–240. [Google Scholar] [CrossRef] [PubMed]
- Chae, J.I.; Shim, J.H.; Lee, K.S.; Cho, Y.S.; Lee, K.S.; Yoon do, Y.; Kim, S.H.; Chung, H.M.; Koo, D.B.; Park, C.S.; et al. Downregulation of immune response by the human cytokines Interleukin-32alpha and beta in cell-mediated rejection. Cell. Immunol. 2010, 264, 47–53. [Google Scholar] [CrossRef] [PubMed]
- Lee, D.H.; Hong, J.E.; Yun, H.M.; Hwang, C.J.; Park, J.H.; Han, S.B.; Yoon do, Y.; Song, M.J.; Hong, J.T. Interleukin-32β ameliorates metabolic disorder and liver damage in mice fed high-fat diet. Obesity 2015, 23, 615–622. [Google Scholar] [CrossRef] [PubMed]
- Kang, J.W.; Park, Y.S.; Lee, D.H.; Kim, M.S.; Bak, Y.; Park, S.H.; Ham, S.Y.; Yang, Y.; Hong, J.T.; Yoon, D.Y. Interleukin-32δ interacts with IL-32β and inhibits IL-32β-mediated IL-10 production. FEBS Lett. 2013, 587, 3776–3781. [Google Scholar] [CrossRef] [PubMed]
- Kim, S.J.; Lee, S.; Kwak, A.; Kim, E.; Jo, S.; Bae, S.; Lee, Y.; Ryoo, S.; Choi, J.; Kim, S. Interleukin-32γ transgenic mice resist LPS-mediated septic shock. J. Microbiol. Biotechnol. 2014, 24, 1133–1142. [Google Scholar] [CrossRef] [PubMed]
- Kang, J.W.; Park, Y.S.; Lee, D.H.; Kim, M.S.; Bak, Y.; Ham, S.Y.; Park, S.H.; Kim, H.; Ahn, J.H.; Hong, J.T.; et al. Interaction network mapping among IL-32 isoforms. Biochimie 2014, 101, 248–251. [Google Scholar] [CrossRef] [PubMed]
- Cho, K.S.; Park, S.H.; Joo, S.H.; Kim, S.H.; Shin, C.Y. The effects of IL-32 on the inflammatory activation of cultured rat primary astrocytes. Biochem. Biophys. Res. Commun. 2010, 402, 48–53. [Google Scholar] [CrossRef] [PubMed]
- Nold, M.F.; Nold-Petry, C.A.; Pott, G.B.; Zepp, J.A.; Saavedra, M.T.; Kim, S.H.; Dinarello, C.A. Endogenous IL-32 controls cytokine and HIV-1 production. J. Immunol. 2008, 181, 557–565. [Google Scholar] [CrossRef] [PubMed]
- Li, W.; Sun, W.; Liu, L.; Yang, F.; Li, Y.; Chen, Y.; Fang, J.; Zhang, W.; Wu, J.; Zhu, Y. IL-32: A host proinflammatory factor against influenza viral replication is upregulated by aberrant epigenetic modifications during influenza A virus infection. J. Immunol. 2010, 185, 5056–5065. [Google Scholar] [CrossRef] [PubMed]
- Rasool, S.T.; Tang, H.; Wu, J.; Li, W.; Mukhtar, M.M.; Zhang, J.; Mu, Y.; Xing, H.X.; Wu, J.; Zhu, Y. Increased level of IL-32 during human immunodeficiency virus infection suppresses HIV replication. Immunol. Lett. 2008, 117, 161–167. [Google Scholar] [CrossRef] [PubMed]
- Zepp, J.A.; Nold-Petry, C.A.; Dinarello, C.A.; Nold, M.F. Protection from RNA and DNA viruses by IL-32. J. Immunol. 2011, 186, 4110–4118. [Google Scholar] [CrossRef] [PubMed]
- Choi, J.D.; Bae, S.Y.; Hong, J.W.; Azam, T.; Dinarello, C.A.; Her, E.; Choi, W.S.; Kim, B.K.; Lee, C.K.; Yoon, D.Y.; et al. Identification of the most active interleukin-32 isoform. Immunology 2009, 126, 535–542. [Google Scholar] [CrossRef] [PubMed]
- Maestrelli, P.; El Messlemani, A.H.; De Fina, O.; Nowicki, Y.; Saetta, M.; Mapp, C.; Fabbri, L.M. Increased expression of heme oxygenase (HO)-1 in alveolar spaces and HO-2 in alveolar walls of smokers. Am. J. Respir. Crit. Care Med. 2001, 164, 1508–1513. [Google Scholar] [CrossRef] [PubMed]
- Netea, M.G.; Azam, T.; Ferwerda, G.; Girardin, S.E.; Walsh, M.; Park, J.S.; Abraham, E.; Kim, J.M.; Yoon, D.Y.; Dinarello, C.A.; et al. IL-32 synergizes with nucleotide oligomerization domain (NOD) 1 and NOD2 ligands for IL-1beta and IL-6 production through a caspase 1-dependent mechanism. Proc. Natl. Acad. Sci. USA 2005, 102, 16309–16314. [Google Scholar] [CrossRef] [PubMed]
- Kim, S. Interleukin-32 in inflammatory autoimmune diseases. Immune Netw. 2014, 14, 123–127. [Google Scholar] [CrossRef] [PubMed]
- Netea, M.G.; Lewis, E.C.; Azam, T.; Joosten, L.A.; Jaekal, J.; Bae, S.Y.; Dinarello, C.A.; Kim, S.H. Interleukin-32 induces the differentiation of monocytes into macrophage-like cells. Proc. Natl. Acad. Sci. USA 2008, 105, 3515–3520. [Google Scholar] [CrossRef] [PubMed]
- Saetta, M.; Baraldo, S.; Corbino, L.; Turato, G.; Braccioni, F.; Rea, F.; Cavallesco, G.; Tropeano, G.; Mapp, C.E.; Maestrelli, P.; et al. CD8+ve cells in the lungs of smokers with chronic obstructive pulmonary disease. Am. J. Respir. Crit. Care Med. 1999, 160, 711–717. [Google Scholar] [CrossRef] [PubMed]
- Netea, M.G.; Azam, T.; Lewis, E.C.; Joosten, L.A.; Wang, M.; Langenberg, D.; Meng, X.; Chan, E.D.; Yoon, D.Y.; Ottenhoff, T.; et al. Mycobacterium tuberculosis induces interleukin-32 production through a caspase-1/IL-18/interferon-gamma-dependent mechanism. PLoS Med. 2006, 3, e277. [Google Scholar] [CrossRef] [PubMed]
- Li, Y.; Xie, J.; Xu, X.; Liu, L.; Wan, Y.; Liu, Y.; Zhu, C.; Zhu, Y. Inducible interleukin 32 (IL-32) exerts extensive antiviral function via selective stimulation of interferon λ1 (IFN-λ1). J. Biol. Chem. 2013, 288, 20927–20941. [Google Scholar] [CrossRef] [PubMed]
- Moschen, A.R.; Fritz, T.; Clouston, A.D.; Rebhan, I.; Bauhofer, O.; Barrie, H.D.; Powell, E.E.; Kim, S.H.; Dinarello, C.A.; Bartenschlager, R.; et al. Interleukin-32: A new proinflammatory cytokine involved in hepatitis C virus-related liver inflammation and fibrosis. Hepatology 2011, 53, 1819–1829. [Google Scholar] [CrossRef] [PubMed]
- Steer, S.A.; Moran, J.M.; Christmann, B.S.; Maggi, L.B., Jr.; Corbett, J.A. Role of MAPK in the regulation of double-stranded RNA- and encephalomyocarditis virus-induced cyclooxygenase-2 expression by macrophages. J. Immunol. 2006, 177, 3413–3420. [Google Scholar] [CrossRef] [PubMed]
- Mizumura, K.; Hashimoto, S.; Maruoka, S.; Gon, Y.; Kitamura, N.; Matsumoto, K.; Hayashi, S.; Shimizu, K.; Horie, T. Role of mitogen-activated protein kinases in influenza virus induction of prostaglandin E2 from arachidonic acid in bronchial epithelial cells. Clin. Exp. Allergy 2003, 33, 1244–1251. [Google Scholar] [CrossRef] [PubMed]
- Steer, S.A.; Moran, J.M.; Maggi, L.B., Jr.; Buller, R.M.; Perlman, H.; Corbett, J.A. Regulation of cyclooxygenase-2 expression by macrophages in response to double-stranded RNA and viral infection. J. Immunol. 2003, 170, 1070–1076. [Google Scholar] [CrossRef] [PubMed]
- Carey, M.A.; Bradbury, J.A.; Seubert, J.M.; Langenbach, R.; Zeldin, D.C.; Germolec, D.R. Contrasting effects of cyclooxygenase-1 (COX-1) and COX-2 deficiency on the host response to influenza A viral infection. J. Immunol. 2005, 175, 6878–6884. [Google Scholar] [CrossRef] [PubMed]
- Gilroy, D.W.; Saunders, M.A.; Wu, K.K. COX-2 expression and cell cycle progression in human fibroblasts. Am. J. Physiol. Cell Physiol. 2001, 281, C188–C194. [Google Scholar] [PubMed]
- Kobayashi, H.; Yazlovitskaya, E.M.; Lin, P.C. Interleukin-32 positively regulates radiation-induced vascular inflammation. Int. J. Radiat. Oncol. Biol. Phys. 2009, 74, 1573–1579. [Google Scholar] [CrossRef] [PubMed]
- Jeong, H.J.; Shin, S.Y.; Oh, H.A.; Kim, M.H.; Cho, J.S.; Kim, H.M. IL-32 up-regulation is associated with inflammatory cytokine production in allergic rhinitis. J. Pathol. 2011, 224, 553–563. [Google Scholar] [CrossRef] [PubMed]
- Jeong, H.J.; Nam, S.Y.; Oh, H.A.; Han, N.R.; Kim, Y.S.; Moon, P.D.; Shin, S.Y.; Kim, M.H.; Kim, H.M. Interleukin-32-induced thymic stromal lymphopoietin plays a critical role in macrophage differentiation through the activation of caspase-1 in vitro. Arthritis Res. Ther. 2012, 14, eR259. [Google Scholar] [CrossRef] [PubMed]
- Cunha, T.M.; Talbot, J.; Pinto, L.G.; Vieira, S.M.; Souza, G.R.; Guerrero, A.T.; Sonego, F.; Verri, W.A., Jr.; Zamboni, D.S.; Ferreira, S.H.; et al. Caspase-1 is involved in the genesis of inflammatory hypernociception by contributing to peripheral IL-1β maturation. Mol. Pain 2010, 6, e63. [Google Scholar] [CrossRef] [PubMed]
- Lara-Pezzi, E.; Gomez-Gaviro, M.V.; Galvez, B.G.; Mira, E.; Iniguez, M.A.; Fresno, M.; Martinez, A.C.; Arroyo, A.G.; Lopez-Cabrera, M. The hepatitis B virus X protein promotes tumor cell invasion by inducing membrane-type matrix metalloproteinase-1 and cyclooxygenase-2 expression. J. Clin. Investig. 2002, 110, 1831–1838. [Google Scholar] [CrossRef] [PubMed]
- Lee, S.; Kim, J.H.; Kim, H.; Kang, J.W.; Kim, S.H.; Yang, Y.; Kim, J.; Park, J.; Park, S.; Hong, J.; et al. Activation of the interleukin-32 pro-inflammatory pathway in response to human papillomavirus infection and over-expression of interleukin-32 controls the expression of the human papillomavirus oncogene. Immunology 2011, 132, 410–420. [Google Scholar] [CrossRef] [PubMed]
- Harris, R.E.; Casto, B.C.; Harris, Z.M. Cyclooxygenase-2 and the inflammogenesis of breast cancer. World J. Clin. Oncol. 2014, 5, 677–692. [Google Scholar] [CrossRef] [PubMed]
- Li, W.; Yang, F.; Liu, Y.; Gong, R.; Liu, L.; Feng, Y.; Hu, P.; Sun, W.; Hao, Q.; Kang, L.; et al. Negative feedback regulation of IL-32 production by iNOS activation in response to dsRNA or influenza virus infection. Eur. J. Immunol. 2009, 39, 1019–1024. [Google Scholar] [CrossRef] [PubMed]
- Murono, S.; Inoue, H.; Tanabe, T.; Joab, I.; Yoshizaki, T.; Furukawa, M.; Pagano, J.S. Induction of cyclooxygenase-2 by Epstein-Barr virus latent membrane protein 1 is involved in vascular endothelial growth factor production in nasopharyngeal carcinoma cells. Proc. Natl. Acad. Sci. USA 2001, 98, 6905–6910. [Google Scholar] [CrossRef] [PubMed]
- Nunez, O.; Fernandez-Martinez, A.; Majano, P.L.; Apolinario, A.; Gomez-Gonzalo, M.; Benedicto, I.; Lopez-Cabrera, M.; Bosca, L.; Clemente, G.; Garcia-Monzon, C.; et al. Increased intrahepatic cyclooxygenase 2, matrix metalloproteinase 2, and matrix metalloproteinase 9 expression is associated with progressive liver disease in chronic hepatitis C virus infection: Role of viral core and NS5A proteins. Gut 2004, 53, 1665–1672. [Google Scholar] [CrossRef] [PubMed]
- Liu, W.; Fan, Z.; Han, Y.; Xu, L.; Wang, M.; Zhang, D.; Mao, Y.; Li, J.; Wang, H. Activation of NF-кB signaling pathway in HSV-1-induced mouse facial palsy: Possible relation to therapeutic effect of glucocorticoids. Neuroscience 2015, 289, 251–261. [Google Scholar] [CrossRef] [PubMed]
- Cheng, C.Y.; Huang, W.R.; Chi, P.I.; Chiu, H.C.; Liu, H.J. Cell entry of bovine ephemeral fever virus requires activation of Src-JNK-AP1 and PI3K-Akt-NF-кB pathways as well as Cox-2-mediated PGE2/EP receptor signalling to enhance clathrin-mediated virus endocytosis. Cell. Microbiol. 2015, 17, 967–987. [Google Scholar]
- He, L.; Zhang, Y.; Fang, Y.; Liang, W.; Lin, J.; Cheng, M. Classical swine fever virus induces oxidative stress in swine umbilical vein endothelial cells. BMC Vet. Res. 2014, 10, e279. [Google Scholar] [CrossRef] [PubMed]
- Imanishi, N.; Andoh, T.; Sakai, S.; Satoh, M.; Katada, Y.; Ueda, K.; Terasawa, K.; Ochiai, H. Induction of inducible nitric oxide (NO) synthase mrna and NO production in macrophages infected with influenza A/PR/8 virus and stimulated with its ether-split product. Microbiol. Immunol. 2005, 49, 41–48. [Google Scholar] [CrossRef] [PubMed]
- Lee, W.J.; Shin, C.Y.; Yoo, B.K.; Ryu, J.R.; Choi, E.Y.; Cheong, J.H.; Ryu, J.H.; Ko, K.H. Induction of matrix metalloproteinase-9 (MMP-9) in lipopolysaccharide-stimulated primary astrocytes is mediated by extracellular signal-regulated protein kinase 1/2 (Erk1/2). Glia 2003, 41, 15–24. [Google Scholar] [CrossRef] [PubMed]
- Bhat, N.R.; Zhang, P.; Lee, J.C.; Hogan, E.L. Extracellular signal-regulated kinase and p38 subgroups of mitogen-activated protein kinases regulate inducible nitric oxide synthase and tumor necrosis factor-alpha gene expression in endotoxin-stimulated primary glial cultures. J. Neurosci. 1998, 18, 1633–1641. [Google Scholar] [PubMed]
- Marcus, J.S.; Karackattu, S.L.; Fleegal, M.A.; Sumners, C. Cytokine-stimulated inducible nitric oxide synthase expression in astroglia: role of Erk mitogen-activated protein kinase and NF-kappaB. Glia 2003, 41, 152–160. [Google Scholar] [CrossRef] [PubMed]
- Mabilleau, G.; Sabokbar, A. Interleukin-32 promotes osteoclast differentiation but not osteoclast activation. PLoS ONE 2009, 4, e4173. [Google Scholar] [CrossRef] [PubMed]
- Bogdan, C. Nitric oxide synthase in innate and adaptive immunity: An update. Trends Immunol. 2015, 36, 161–178. [Google Scholar] [CrossRef] [PubMed]
- Jyoti, A.; Singh, A.K.; Dubey, M.; Kumar, S.; Saluja, R.; Keshari, R.S.; Verma, A.; Chandra, T.; Kumar, A.; Bajpai, V.K.; et al. Interaction of inducible nitric oxide synthase with rac2 regulates reactive oxygen and nitrogen species generation in the human neutrophil phagosomes: Implication in microbial killing. Antioxid. Redox Signal. 2014, 20, 417–431. [Google Scholar] [CrossRef] [PubMed]
- Saini, R.; Patel, S.; Saluja, R.; Sahasrabuddhe, A.A.; Singh, M.P.; Habib, S.; Bajpai, V.K.; Dikshit, M. Nitric oxide synthase localization in the rat neutrophils: immunocytochemical, molecular, and biochemical studies. J. Leukoc. Biol. 2006, 79, 519–528. [Google Scholar] [CrossRef] [PubMed]
- Chakrabarti, S.; Chan, C.K.; Jiang, Y.; Davidge, S.T. Neuronal nitric oxide synthase regulates endothelial inflammation. J. Leukoc. Biol. 2012, 91, 947–956. [Google Scholar] [CrossRef] [PubMed]
- Burrack, K.S.; Morrison, T.E. The role of myeloid cell activation and arginine metabolism in the pathogenesis of virus-induced diseases. Front. Immunol. 2014, 5, e428. [Google Scholar] [CrossRef] [PubMed]
- Bogdan, C.; Rollinghoff, M.; Diefenbach, A. Reactive oxygen and reactive nitrogen intermediates in innate and specific immunity. Curr. Opin. Immunol. 2000, 12, 64–76. [Google Scholar] [CrossRef]
- Fang, F.C. Antimicrobial reactive oxygen and nitrogen species: Concepts and controversies. Nat. Rev. Microbiol. 2004, 2, 820–832. [Google Scholar] [CrossRef] [PubMed]
- Herbst, S.; Schaible, U.E.; Schneider, B.E. Interferon gamma activated macrophages kill mycobacteria by nitric oxide induced apoptosis. PLoS ONE 2011, 6, e19105. [Google Scholar] [CrossRef] [PubMed]
- Monteleone, K.; Selvaggi, C.; Cacciotti, G.; Falasca, F.; Mezzaroma, I.; D’Ettorre, G.; Turriziani, O.; Vullo, V.; Antonelli, G.; Scagnolari, C. Microrna-29 family expression and its relation to antiviral immune response and viro-immunological markers in HIV-1-infected patients. BMC Infect. Dis. 2015, 15, e51. [Google Scholar] [CrossRef] [PubMed]
- Monteleone, K.; Di Maio, P.; Cacciotti, G.; Falasca, F.; Fraulo, M.; Falciano, M.; Mezzaroma, I.; D’Ettorre, G.; Turriziani, O.; Scagnolari, C. Interleukin-32 isoforms: Expression, interaction with interferon-regulated genes and clinical significance in chronically HIV-1-infected patients. Med. Microbiol. Immunol. 2014, 203, 207–216. [Google Scholar] [CrossRef] [PubMed]
- Nold-Petry, C.A.; Rudloff, I.; Baumer, Y.; Ruvo, M.; Marasco, D.; Botti, P.; Farkas, L.; Cho, S.X.; Zepp, J.A.; Azam, T.; et al. IL-32 promotes angiogenesis. J. Immunol. 2014, 192, 589–602. [Google Scholar] [CrossRef] [PubMed]
- Uze, G.; Monneron, D. IL-28 and IL-29: newcomers to the interferon family. Biochimie 2007, 89, 729–734. [Google Scholar] [CrossRef] [PubMed]
- Lopusna, K.; Rezuchova, I.; Betakova, T.; Skovranova, L.; Tomaskova, J.; Lukacikova, L.; Kabat, P. Interferons lambda, new cytokines with antiviral activity. Acta Virol. 2013, 57, 171–179. [Google Scholar] [CrossRef] [PubMed]
- Maher, S.G.; Sheikh, F.; Scarzello, A.J.; Romero-Weaver, A.L.; Baker, D.P.; Donnelly, R.P.; Gamero, A.M. IFNalpha and IFNlambda differ in their antiproliferative effects and duration of JAK/STAT signaling activity. Cancer Biol. Ther. 2008, 7, 1109–1115. [Google Scholar] [CrossRef] [PubMed]
- Robek, M.D.; Boyd, B.S.; Chisari, F.V. Lambda interferon inhibits hepatitis B and C virus replication. J. Virol. 2005, 79, 3851–3854. [Google Scholar] [CrossRef] [PubMed]
- Donnelly, R.P.; Kotenko, S.V. Interferon-lambda: A new addition to an old family. J. Interferon Cytokine Res. 2010, 30, 555–564. [Google Scholar] [CrossRef] [PubMed]
- Sheppard, P.; Kindsvogel, W.; Xu, W.; Henderson, K.; Schlutsmeyer, S.; Whitmore, T.E.; Kuestner, R.; Garrigues, U.; Birks, C.; Roraback, J.; et al. IL-28, IL-29 and their class II cytokine receptor IL-28R. Nat. Immunol. 2003, 4, 63–68. [Google Scholar] [CrossRef] [PubMed]
- Almeida, G.M.; de Oliveira, D.B.; Magalhaes, C.L.; Bonjardim, C.A.; Ferreira, P.C.; Kroon, E.G. Antiviral activity of type I interferons and interleukins 29 and 28a (type III interferons) against apeu virus. Antivir. Res. 2008, 80, 302–308. [Google Scholar] [CrossRef] [PubMed]
- Hong, S.H.; Cho, O.; Kim, K.; Shin, H.J.; Kotenko, S.V.; Park, S. Effect of interferon-lambda on replication of hepatitis B virus in human hepatoma cells. Virus Res. 2007, 126, 245–249. [Google Scholar] [CrossRef] [PubMed]
- Brand, S.; Beigel, F.; Olszak, T.; Zitzmann, K.; Eichhorst, S.T.; Otte, J.M.; Diebold, J.; Diepolder, H.; Adler, B.; Auernhammer, C.J.; et al. IL-28A and IL-29 mediate antiproliferative and antiviral signals in intestinal epithelial cells and murine CMV infection increases colonic IL-28A expression. Am. J. Physiol. Gastrointest. Liver Physiol. 2005, 289, G960–G968. [Google Scholar] [CrossRef] [PubMed]
- Ank, N.; West, H.; Bartholdy, C.; Eriksson, K.; Thomsen, A.R.; Paludan, S.R. Lambda interferon (IFN-lambda), a type III IFN, is induced by viruses and IFNs and displays potent antiviral activity against select virus infections in vivo. J. Virol. 2006, 80, 4501–4509. [Google Scholar] [CrossRef] [PubMed]
- Wang, J.; Wang, Q.; Han, T.; Li, Y.K.; Zhu, S.L.; Ao, F.; Feng, J.; Jing, M.Z.; Wang, L.; Ye, L.B.; et al. Soluble interleukin-6 receptor is elevated during influenza A virus infection and mediates the IL-6 and IL-32 inflammatory cytokine burst. Cell. Mol. Immunol. 2014. [Google Scholar] [CrossRef]
- Wang, Q.; Chen, X.; Feng, J.; Cao, Y.; Song, Y.; Wang, H.; Zhu, C.; Liu, S.; Zhu, Y. Soluble interleukin-6 receptor-mediated innate immune response to DNA and RNA viruses. J. Virol. 2013, 87, 11244–11254. [Google Scholar] [CrossRef] [PubMed]
- Bae, S.; Kang, D.; Hong, J.; Chung, B.; Choi, J.; Jhun, H.; Hong, K.; Kim, E.; Jo, S.; Lee, S.; et al. Characterizing antiviral mechanism of interleukin-32 and a circulating soluble isoform in viral infection. Cytokine 2012, 58, 79–86. [Google Scholar] [CrossRef] [PubMed]
- Kang, J.W.; Park, Y.S.; Lee, D.H.; Kim, J.H.; Kim, M.S.; Bak, Y.; Hong, J.; Yoon, D.Y. Intracellular interaction of interleukin (IL)-32α with protein kinase Cε (PKCε) and STAT3 protein augments IL-6 production in THP-1 promonocytic cells. J. Biol. Chem. 2012, 287, 35556–35564. [Google Scholar] [CrossRef] [PubMed]
- Fima, E.; Shahaf, G.; Hershko, T.; Apte, R.N.; Livneh, E. Expression of PKCeta in NIH-3T3 cells promotes production of the pro-inflammatory cytokine interleukin-6. Eur. Cytokine Netw. 1999, 10, 491–500. [Google Scholar] [PubMed]
- Garcia-Zepeda, E.A.; Rothenberg, M.E.; Ownbey, R.T.; Celestin, J.; Leder, P.; Luster, A.D. Human eotaxin is a specific chemoattractant for eosinophil cells and provides a new mechanism to explain tissue eosinophilia. Nat. Med. 1996, 2, 449–456. [Google Scholar] [CrossRef] [PubMed]
- Garbers, C.; Aparicio-Siegmund, S.; Rose-John, S. The IL-6/gp130/STAT3 signaling axis: recent advances towards specific inhibition. Curr. Opin. Immunol. 2015, 34C, 75–82. [Google Scholar] [CrossRef] [PubMed]
- Scheller, J.; Garbers, C.; Rose-John, S. Interleukin-6: From basic biology to selective blockade of pro-inflammatory activities. Semin. Immunol. 2014, 26, 2–12. [Google Scholar] [CrossRef] [PubMed]
- Chang, Q.; Daly, L.; Bromberg, J. The IL-6 feed-forward loop: A driver of tumorigenesis. Semin. Immunol. 2014, 26, 48–53. [Google Scholar] [CrossRef] [PubMed]
- Bouezzedine, F.; Fardel, O.; Gripon, P. Interleukin 6 inhibits HBV entry through NTCP down regulation. Virology 2015, 481, 34–42. [Google Scholar] [CrossRef] [PubMed]
- Cho, H.J.; Kim, S.S.; Ahn, S.J.; Park, S.Y.; Park, J.H.; Kim, J.K.; Wang, H.J.; Cheong, J.Y.; Cho, S.W. Low serum interleukin-6 levels as a predictive marker of recurrence in patients with hepatitis B virus related hepatocellular carcinoma who underwent curative treatment. Cytokine 2015, 73, 245–252. [Google Scholar] [CrossRef] [PubMed]
- Woods, P.S.; Tazi, M.F.; Chesarino, N.M.; Amer, A.O.; Davis, I.C. TGF-β-induced IL-6 prevents development of acute lung injury in influenza A virus-infected F508del CFTR-heterozygous mice. Am. J. Physiol. Lung Cell. Mol. Physiol. 2015, 308, L1136–L1144. [Google Scholar] [CrossRef] [PubMed]
- Fredeking, T.M.; Zavala-Castro, J.E.; Martinez, P.G.; Rodriguez, W.M.; Sanchez, E.C.; Foster, M.J.; Diaz-Quijano, F.A. Dengue Patients Treated with Doxycycline Showed Lower Mortality Associated to a Reduction in IL-6 and TNF Levels. Recent Pat. Anti-Infect. Drug Discov. 2015, 10, 51–58. [Google Scholar] [CrossRef]
- Karnowski, A.; Chevrier, S.; Belz, G.T.; Mount, A.; Emslie, D.; D’Costa, K.; Tarlinton, D.M.; Kallies, A.; Corcoran, L.M. B and T cells collaborate in antiviral responses via IL-6, IL-21, and transcriptional activator and coactivator, Oct2 and OBF-1. J. Exp. Med. 2012, 209, 2049–2064. [Google Scholar] [CrossRef] [PubMed]
- Heinhuis, B.; Netea, M.G.; van den Berg, W.B.; Dinarello, C.A.; Joosten, L.A. Interleukin-32: A predominantly intracellular proinflammatory mediator that controls cell activation and cell death. Cytokine 2012, 60, 321–327. [Google Scholar] [CrossRef] [PubMed]
© 2015 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Zhou, Y.; Zhu, Y. Important Role of the IL-32 Inflammatory Network in the Host Response against Viral Infection. Viruses 2015, 7, 3116-3129. https://doi.org/10.3390/v7062762
Zhou Y, Zhu Y. Important Role of the IL-32 Inflammatory Network in the Host Response against Viral Infection. Viruses. 2015; 7(6):3116-3129. https://doi.org/10.3390/v7062762
Chicago/Turabian StyleZhou, Yaqin, and Ying Zhu. 2015. "Important Role of the IL-32 Inflammatory Network in the Host Response against Viral Infection" Viruses 7, no. 6: 3116-3129. https://doi.org/10.3390/v7062762
APA StyleZhou, Y., & Zhu, Y. (2015). Important Role of the IL-32 Inflammatory Network in the Host Response against Viral Infection. Viruses, 7(6), 3116-3129. https://doi.org/10.3390/v7062762