A Novel Ebola Virus VP40 Matrix Protein-Based Screening for Identification of Novel Candidate Medical Countermeasures
Abstract
1. Introduction
2. Materials and Methods
2.1. Cells and Cell Culture Conditions
2.2. Fluorescent VP40 Oligomerization Assay
2.3. VLP Isolation and Western Blotting
2.4. Verification of Hits against Infectious Viruses
- Bunyavirales: Arenaviridae: Lassa virus strain Josiah (LASV). LASV (IRF0193; L segment, Genbank #KY425632.1; S segment, Genbank #KY425638.1) was grown in Vero E6 cells with alpha minimum essential media (MEM) (Thermo Fisher Scientific) containing 2% FBS (SAFC Biosciences, Lenexa, KS, USA) for 5 d. This working stock originated from a Centers for Disease Control and Prevention (CDC) isolate (#800789);
- Chitovirales: Poxviridae: recombinant cowpox virus expressing GFP (rCPXV-GFP) (seed stock received from United States Army Medical Research Institute of Infectious Diseases [USAMRIID]) [40] and recombinant vaccinia virus expressing GFP (rVACV-GFP) (seed stock received from Dr. Bernard Moss, National Institutes of Health [NIH] National Institute of Allergy and Infectious Diseases [NIAID]) [41]. Viruses were grown in Vero E6 cells with DMEM (Thermo Fisher Scientific) containing 2% FBS as previously described [42]; and
- Mononegavirales: Filoviridae: Ebola virus/H.sapiens-tc/GIN/2014/Makona-C05 (EBOV) and Marburg virus/H. sapiens-tc/AGO/2005/Angola-1379v (MARV). EBOV (IRF0165, Genbank #KY425645.1) was grown in Vero E6 cells with alpha MEM media containing 5% FBS for 7 d. The seed virus from which it originated was obtained from Public Health Agency of Canada (PHAC). MARV (IRF0202, Biosample #SAMN05916381) was grown in Vero E6 cells with alpha MEM containing 2% FBS for 5 d. The seed virus originated from University of Texas Medical Branch (UTMB).
2.5. Minigenome Assay
3. Results
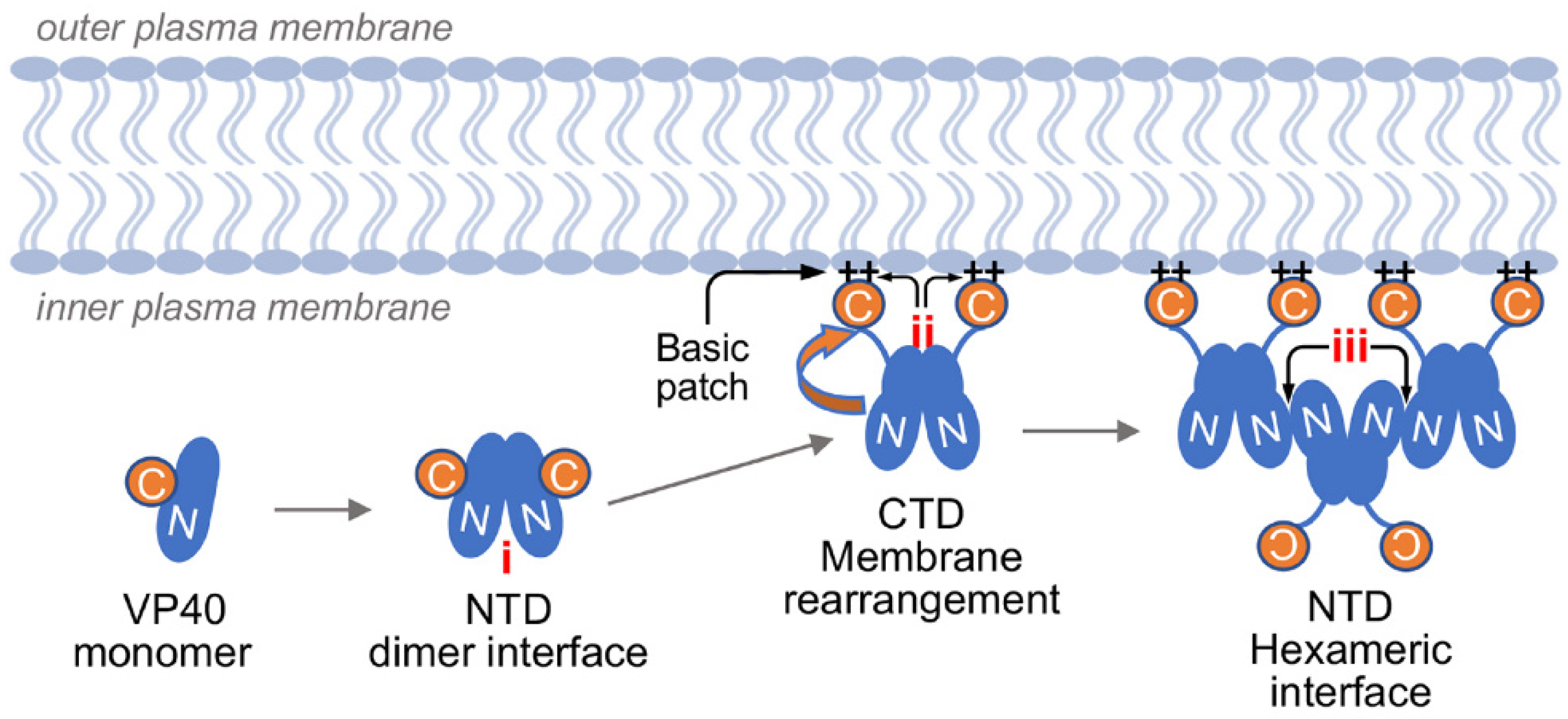
3.1. EBOV VP40 Membrane Localization Is Disrupted by Sangivamycin
3.2. Sangivamycin Decreases VLP Release but Does Not Alter VP40 Abundance or Cellular Transcription/Translation
3.3. Sangivamycin Inhibits the Replication of Multiple Viruses, Including EBOV and MARV
3.4. Sangivamycin Inhibits EBOV RNA Transcription/Replication
3.5. Sangivamycin Inhibits EBOV up to 24 H after Addition Relative to Virus Exposure
4. Discussion
5. Patents
Author Contributions
Funding
Institutional Review Board Statement
Acknowledgments
Conflicts of Interest
Disclaimer
References
- Kuhn, J.H.; Amarasinghe, G.; Perry, D.L. Filoviridae. In Fields Virology, 7th ed.; Howley, P.M., Knipe, D.M., Whelan, S.P.J., Eds.; Wolters Kluwer/Lippincott Williams & Wilkins: Philadelphia, PA, USA, 2020; Volume 1, pp. 449–503. [Google Scholar]
- Kuhn, J.H.; Amarasinghe, G.K.; Basler, C.F.; Bavari, S.; Bukreyev, A.; Chandran, K.; Crozier, I.; Dolnik, O.; Dye, J.M.; Formenty, P.B.H.; et al. ICTV Report Consortium, ICTV virus taxonomy profile: Filoviridae. J. Gen. Virol. 2019, 100, 911–912. [Google Scholar] [CrossRef]
- Kuhn, J.H.; Adachi, T.; Adhikari, N.K.J.; Arribas, J.R.; Bah, I.E.; Bausch, D.G.; Bhadelia, N.; Borchert, M.; Brantsæter, A.B.; Brett-Major, D.M.; et al. New filovirus disease classification and nomenclature. Nat. Rev. Microbiol. 2019, 17, 261–263. [Google Scholar] [CrossRef] [PubMed]
- Bullard, S.G. A Day-by-Day Chronicle of the 2013–2016 Ebola Outbreak; Springer: Cham, Switzerland, 2018. [Google Scholar]
- World Health Organization. Ebola in the Democratic Republic of the Congo, North Kivu, Ituri 2018–2020. 2020. Available online: https://www.who.int/emergencies/diseases/ebola/drc-2019 (accessed on 30 December 2020).
- Martin, B.; Volchkov, V.; Reynard, O. Ebola, des premiers vaccins disponibles. Méd. Sci. 2020, 36, 1027–1033. [Google Scholar] [CrossRef]
- Mulangu, S.; Dodd, L.E.; Davey, R.T., Jr.; Tshiani Mbaya, O.; Proschan, M.; Mukadi, D.; Lusakibanza Manzo, M.; Nzolo, D.; Tshomba Oloma, A.; Ibanda, A.; et al. PALM Writing Group, A randomized, controlled trial of Ebola virus disease therapeutics. N Engl. J. Med. 2019, 381, 2293–2303. [Google Scholar] [CrossRef] [PubMed]
- Warren, T.K.; Jordan, R.; Lo, M.K.; Ray, A.S.; Mackman, R.L.; Soloveva, V.; Siegel, D.; Perron, M.; Bannister, R.; Hui, H.C.; et al. Therapeutic efficacy of the small molecule GS-5734 against Ebola virus in rhesus monkeys. Nature 2016, 531, 381–385. [Google Scholar] [CrossRef] [PubMed]
- Schindell, B.G.; Webb, A.L.; Kindrachuk, J. Persistence and sexual transmission of filoviruses. Viruses 2018, 10, 683. [Google Scholar] [CrossRef] [PubMed]
- Kugelman, J.R.; Kugelman-Tonos, J.; Ladner, J.T.; Pettit, J.; Keeton, C.M.; Nagle, E.R.; Garcia, K.Y.; Froude, J.W.; Kuehne, A.I.; Kuhn, J.H.; et al. Emergence of Ebola virus escape variants in infected nonhuman primates treated with the MB-003 antibody cocktail. Cell Rep. 2015, 12, 2111–2120. [Google Scholar] [CrossRef]
- Iversen, P.L.; Kane, C.D.; Zeng, X.; Panchal, R.G.; Warren, T.K.; Radoshitzky, S.R.; Kuhn, J.H.; Mudhasani, R.R.; Cooper, C.L.; Shurtleff, A.C.; et al. Recent successes in therapeutics for Ebola virus disease: No time for complacency. Lancet Infect. Dis. 2020, 20, e231–e237. [Google Scholar] [CrossRef]
- Hoenen, T.; Groseth, A.; Feldmann, H. Therapeutic strategies to target the Ebola virus life cycle. Nat. Rev. Microbiol. 2019, 17, 593–606. [Google Scholar] [CrossRef]
- Pascal, K.E.; Dudgeon, D.; Trefry, J.C.; Anantpadma, M.; Sakurai, Y.; Murin, C.D.; Turner, H.L.; Fairhurst, J.; Torres, M.; Rafique, A.; et al. Development of clinical-stage human monoclonal antibodies that treat advanced Ebola virus disease in nonhuman primates. J. Infect. Dis. 2018, 218 (Suppl. 5), S612–S626. [Google Scholar] [CrossRef]
- Dyall, J.; Nelson, E.A.; DeWald, L.E.; Guha, R.; Hart, B.J.; Zhou, H.; Postnikova, E.; Logue, J.; Vargas, W.M.; Gross, R.; et al. Identification of combinations of approved drugs with synergistic activity against Ebola virus in cell cultures. J. Infect. Dis. 2018, 218 (Suppl. 5), S672–S678. [Google Scholar] [CrossRef] [PubMed]
- Bai, C.-Q.; Mu, J.-S.; Kargbo, D.; Song, Y.-B.; Niu, W.-K.; Nie, W.-M.; Kanu, A.; Liu, W.-W.; Wang, Y.-P.; Dafae, F.; et al. Clinical and virological characteristics of Ebola virus disease patients treated with favipiravir (T-705)-Sierra Leone, 2014. Clin. Infect. Dis. 2016, 63, 1288–1294. [Google Scholar] [CrossRef] [PubMed]
- Sissoko, D.; Laouenan, C.; Folkesson, E.; M’Lebing, A.-B.; Beavogui, A.H.; Baize, S.; Camara, A.-M.; Maes, P.; Shepherd, S.; Danel, C.; et al. JIKI Study Group, Experimental treatment with favipiravir for Ebola virus disease (the JIKI Trial): A historically controlled, single-arm proof-of-concept trial in Guinea. PLoS Med. 2016, 13, e1001967. [Google Scholar]
- Kerber, R.; Lorenz, E.; Duraffour, S.; Sissoko, D.; Rudolf, M.; Jaeger, A.; Cisse, S.D.; Camara, A.-M.; Miranda, O.; Castro, C.M.; et al. Laboratory findings, compassionate use of favipiravir, and outcome in patients with Ebola virus disease, Guinea, 2015-a retrospective observational study. J. Infect. Dis. 2019, 220, 195–202. [Google Scholar] [CrossRef]
- Furuta, Y.; Komeno, T.; Nakamura, T. Favipiravir (T-705), a broad spectrum inhibitor of viral RNA polymerase. Proc. Jpn. Acad. Ser. B Phys. Biol. Sci. 2017, 93, 449–463. [Google Scholar] [CrossRef]
- Warren, T.K.; Wells, J.; Panchal, R.G.; Stuthman, K.S.; Garza, N.L.; Van Tongeren, S.A.; Dong, L.; Retterer, C.J.; Eaton, B.P.; Pegoraro, G.; et al. Protection against filovirus diseases by a novel broad-spectrum nucleoside analogue BCX4430. Nature 2014, 508, 402–405. [Google Scholar] [CrossRef]
- Bornholdt, Z.A.; Noda, T.; Abelson, D.M.; Halfmann, P.; Wood, M.R.; Kawaoka, Y.; Saphire, E.O. Structural rearrangement of Ebola virus VP40 begets multiple functions in the virus life cycle. Cell 2013, 154, 763–774. [Google Scholar] [CrossRef]
- Radzimanowski, J.; Effantin, G.; Weissenhorn, W. Conformational plasticity of the Ebola virus matrix protein. Protein Sci. 2014, 23, 1519–1527. [Google Scholar] [CrossRef]
- Dessen, A.; Volchkov, V.; Dolnik, O.; Klenk, H.-D.; Weissenhorn, W. Crystal structure of the matrix protein VP40 from Ebola virus. EMBO J. 2000, 19, 4228–4236. [Google Scholar] [CrossRef]
- Timmins, J.; Scianimanico, S.; Schoehn, G.; Weissenhorn, W. Vesicular release of Ebola virus matrix protein VP40. Virology 2001, 283, 1–6. [Google Scholar] [CrossRef]
- Scianimanico, S.; Schoehn, G.; Timmins, J.; Ruigrok, R.H.W.; Klenk, H.-D.; Weissenhorn, W. Membrane association induces a conformational change in the Ebola virus matrix protein. EMBO J. 2000, 19, 6732–6741. [Google Scholar] [CrossRef] [PubMed]
- Hoenen, T.; Biedenkopf, N.; Zielecki, F.; Jung, S.; Groseth, A.; Feldmann, H.; Becker, S. Oligomerization of Ebola virus VP40 is essential for particle morphogenesis and regulation of viral transcription. J. Virol. 2010, 84, 7053–7063. [Google Scholar] [CrossRef] [PubMed]
- Hoenen, T.; Jung, S.; Herwig, A.; Groseth, A.; Becker, S. Both matrix proteins of Ebola virus contribute to the regulation of viral genome replication and transcription. Virology 2010, 403, 56–66. [Google Scholar] [CrossRef]
- Hoenen, T.; Volchkov, V.; Kolesnikova, L.; Mittler, E.; Timmins, J.; Ottmann, M.; Reynard, O.; Becker, S.; Weissenhorn, W. VP40 octamers are essential for Ebola virus replication. J. Virol. 2005, 79, 1898–1905. [Google Scholar] [CrossRef]
- Adu-Gyamfi, E.; Johnson, K.A.; Fraser, M.E.; Scott, J.L.; Soni, S.P.; Jones, K.R.; Digman, M.A.; Gratton, E.; Tessier, C.R.; Stahelin, R.V. Host cell plasma membrane phosphatidylserine regulates the assembly and budding of Ebola virus. J. Virol. 2015, 89, 9440–9453. [Google Scholar] [CrossRef]
- Adu-Gyamfi, E.; Soni, S.P.; Xue, Y.; Digman, M.A.; Gratton, E.; Stahelin, R.V. The Ebola virus matrix protein penetrates into the plasma membrane: A key step in VP40 oligomerization and viral egress. J. Biol. Chem. 2013, 288, 5779–5789. [Google Scholar] [CrossRef] [PubMed]
- Pavadai, E.; Gerstman, B.S.; Chapagain, P.P. A cylindrical assembly model and dynamics of the Ebola virus VP40 structural matrix. Sci. Rep. 2018, 8, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Gomis-Rüth, F.X.; Dessen, A.; Timmins, J.; Bracher, A.; Kolesnikowa, L.; Becker, S.; Klenk, H.-D.; Weissenhorn, W. The matrix protein VP40 from Ebola virus octamerizes into pore-like structures with specific RNA binding properties. Structure 2003, 11, 423–433. [Google Scholar] [CrossRef]
- Silva, L.P.; Vanzile, M.; Bavari, S.; Aman, J.M.; Schriemer, D.C. Assembly of Ebola virus matrix protein VP40 is regulated by latch-like properties of N and C terminal tails. PLoS ONE 2012, 7, e39978. [Google Scholar] [CrossRef]
- Yamayoshi, S.; Kawaoka, Y. Mapping of a region of Ebola virus VP40 that is important in the production of virus-like particles. J. Infect. Dis. 2007, 196 (Suppl. 2), S291–S295. [Google Scholar] [CrossRef]
- Beniac, D.R.; Lamboo, L.L.; Booth, T.F. Filovirus filament proteins. Subcell Biochem. 2018, 88, 73–94. [Google Scholar] [PubMed]
- Noda, T.; Ebihara, H.; Muramoto, Y.; Fujii, K.; Takada, A.; Sagara, H.; Kim, J.H.; Kida, H.; Feldmann, H.; Kawaoka, Y. Assembly and budding of Ebolavirus. PLoS Pathog. 2006, 2, e99. [Google Scholar] [CrossRef] [PubMed]
- Cong, Y.; Dyall, J.; Hart, B.J.; DeWald, L.E.; Johnson, J.C.; Postnikova, E.; Zhou, H.; Gross, R.; Rojas, O.; Alexander, I.; et al. Evaluation of the activity of lamivudine and zidovudine against Ebola virus. PLoS ONE 2016, 11, e0166318. [Google Scholar] [CrossRef] [PubMed]
- Cong, Y.; McArthur, M.A.; Cohen, M.; Jahrling, P.B.; Janosko, K.B.; Josleyn, N.; Kang, K.; Zhang, T.; Holbrook, M.R. Characterization of yellow fever virus infection of human and non-human primate antigen presenting cells and their interaction with CD4+ T cells. PLoS Negl. Trop. Dis. 2016, 10, e0004709. [Google Scholar] [CrossRef] [PubMed]
- Hobbs, S.; Jitrapakdee, S.; Wallace, J.C. Development of a bicistronic vector driven by the human polypeptide chain elongation factor 1α promoter for creation of stable mammalian cell lines that express very high levels of recombinant proteins. Biochem. Biophys. Res. Commun. 1998, 252, 368–372. [Google Scholar] [CrossRef] [PubMed]
- Postnikova, E.; Cong, Y.; DeWald, L.E.; Dyall, J.; Yu, S.; Hart, B.J.; Zhou, H.; Gross, R.; Logue, J.; Cai, Y.; et al. Testing therapeutics in cell-based assays: Factors that influence the apparent potency of drugs. PLoS ONE 2018, 13, e0194880. [Google Scholar] [CrossRef] [PubMed]
- Goff, A.; Twenhafel, N.; Garrison, A.; Mucker, E.; Lawler, J.; Paragas, J. In vivo imaging of cidofovir treatment of cowpox virus infection. Virus Res. 2007, 128, 88–98. [Google Scholar] [CrossRef] [PubMed]
- Norbury, C.C.; Malide, D.; Gibbs, J.S.; Bennink, J.R.; Yewdell, J.W. Visualizing priming of virus-specific CD8+ T cells by infected dendritic cells in vivo. Nat. Immunol. 2002, 3, 265–271. [Google Scholar] [CrossRef]
- Mackett, M.; Smith, G.L.; Moss, B. General method for production and selection of infectious vaccinia virus recombinants expressing foreign genes. J. Virol. 1984, 49, 857–864. [Google Scholar] [CrossRef]
- Johansen, L.M.; Brannan, J.M.; Delos, S.E.; Shoemaker, C.J.; Stossel, A.; Lear, C.; Hoffstrom, B.G.; Dewald, L.E.; Schornberg, K.L.; Scully, C.; et al. FDA-approved selective estrogen receptor modulators inhibit Ebola virus infection. Sci. Transl. Med. 2013, 5, 190ra79. [Google Scholar] [CrossRef]
- Zhao, Y.; Ren, J.; Harlos, K.; Jones, D.M.; Zeltina, A.; Bowden, T.A.; Padilla-Parra, S.; Fry, E.E.; Stuart, D.I. Toremifene interacts with and destabilizes the Ebola virus glycoprotein. Nature 2016, 535, 169–172. [Google Scholar] [CrossRef] [PubMed]
- De Clercq, E.; Luczak, M.; Shugar, D.; Torrence, P.F.; Waters, J.A.; Witkop, B. Effect of cytosine, arabinoside, iododeoxyuridine, ethyldeoxyuridine, thiocyanatodeoxyuridine, and ribavirin on tail lesion formation in mice infected with vaccinia virus. Proc. Soc. Exp. Biol. Med. 1976, 151, 487–490. [Google Scholar] [CrossRef] [PubMed]
- Zhang, P.; Samuel, C.E. Induction of protein kinase PKR-dependent activation of interferon regulatory factor 3 by vaccinia virus occurs through adapter IPS-1 signaling. J. Biol. Chem. 2008, 283, 34580–34587. [Google Scholar] [CrossRef]
- Vogel, P.; Connolly, B.; Abplanalp, D.; Geisbert, T.W.; Kell, W.M.; Jahrling, P.B.; Jaax, N.K. Pathology of experimental Ebola-Zaire (Mayinga) virus infection transmitted to guinea-pigs by oral, conjunctival and tonsillar routes. Cell Vision 1997, 4, 298–307. [Google Scholar]
- Ruo, S.L.; Mitchell, S.W.; Kiley, M.P.; Roumillat, L.F.; Fisher-Hoch, S.P.; McCormick, J.B. Antigenic relatedness between arenaviruses defined at the epitope level by monoclonal antibodies. J. Gen. Virol. 1991, 72, 549–555. [Google Scholar] [CrossRef]
- Bennett, R.P.; Stewart, R.A.; Hogan, P.A.; Ptak, R.G.; Mankowski, M.K.; Hartman, T.L.; Buckheit, R.W., Jr.; Snyder, B.A.; Salter, J.D.; Morales, G.A.; et al. An analog of camptothecin inactive against topoisomerase I is broadly neutralizing of HIV-1 through inhibition of Vif-dependent APOBEC3G degradation. Antivir. Res. 2016, 136, 51–59. [Google Scholar] [CrossRef]
- Platt, E.J.; Wehrly, K.; Kuhmann, S.E.; Chesebro, B.; Kabat, D. Effects of CCR5 and CD4 cell surface concentrations on infections by macrophagetropic isolates of human immunodeficiency virus type 1. J. Virol. 1998, 72, 2855–2864. [Google Scholar] [CrossRef] [PubMed]
- Trunschke, M.; Conrad, D.; Enterlein, S.; Olejnik, J.; Brauburger, K.; Mühlberger, E. The L-VP35 and L-L interaction domains reside in the amino terminus of the Ebola virus L protein and are potential targets for antivirals. Virology 2013, 441, 135–145. [Google Scholar] [CrossRef]
- Hoenen, T.; Groseth, A.; de Kok-Mercado, F.; Kuhn, J.H.; Wahl-Jensen, V. Minigenomes, transcription and replication competent virus-like particles and beyond: Reverse genetics systems for filoviruses and other negative stranded hemorrhagic fever viruses. Antivir. Res. 2011, 91, 195–208. [Google Scholar] [CrossRef] [PubMed]
- Ritch, P.S.; Glazer, R.I.; Cunningham, R.E.; Shackney, S.E. Kinetic effects of sangivamycin in sarcoma 180 in vitro. Cancer Res. 1981, 41, 1784–1788. [Google Scholar]
- Bastea, L.I.; Hollant, L.M.A.; Döppler, H.R.; Reid, E.M.; Storz, P. Sangivamycin and its derivatives inhibit Haspin-Histone H3-survivin signaling and induce pancreatic cancer cell death. Sci. Rep. 2019, 9, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Lee, S.A.; Jung, M. The nucleoside analog sangivamycin induces apoptotic cell death in breast carcinoma MCF7/adriamycin-resistant cells via protein kinase Cδ and JNK activation. J. Biol. Chem. 2007, 282, 15271–15283. [Google Scholar] [CrossRef] [PubMed]
- Wakao, K.; Watanabe, T.; Takadama, T.; Ui, S.; Shigemi, Z.; Kagawa, H.; Higashi, C.; Ohga, R.; Taira, T.; Fujimuro, M. Sangivamycin induces apoptosis by suppressing Erk signaling in primary effusion lymphoma cells. Biochem. Biophys. Res. Commun. 2014, 444, 135–140. [Google Scholar] [CrossRef] [PubMed]
- Tchesnokov, E.P.; Feng, J.Y.; Porter, D.P.; Götte, M. Mechanism of inhibition of Ebola virus RNA-dependent RNA polymerase by remdesivir. Viruses 2019, 11, 326. [Google Scholar] [CrossRef]
- Huang, R.-Y.; Pei, L.; Liu, Q.; Chen, S.; Dou, H.; Shu, G.; Yuan, Z.-X.; Lin, J.; Peng, G.; Zhang, W.; et al. Isobologram analysis: A comprehensive review of methodology and current research. Front. Pharmacol. 2019, 10, 1222. [Google Scholar] [CrossRef]
- Loomis, C.R.; Bell, R.M. Sangivamycin, a nucleoside analogue, is a potent inhibitor of protein kinase C. J. Biol Chem 1988, 263, 1682–1692. [Google Scholar]
- Cavins, J.A.; Hall, T.C.; Olson, K.B.; Khung, C.L.; Horton, J.; Colsky, J.; Shadduck, R.K. Initial toxicity study of sangivamycin (NSC-65346). Cancer Chemother Rep. 1967, 51, 197–200. [Google Scholar]
- Osada, H.; Sonoda, T.; Tsunoda, K.; Isono, K. A new biological role of sangivamycin; inhibition of protein kinases. J. Antibiot. 1989, 42, 102–106. [Google Scholar] [CrossRef]
- Stockwin, L.H.; Yu, S.X.; Stotler, H.; Hollingshead, M.G.; Newton, D.L. ARC (NSC 188491) has identical activity to sangivamycin (NSC 65346) including inhibition of both P-TEFb and PKC. BMC Cancer 2009, 9, 1–13. [Google Scholar] [CrossRef]
- Lin, S.-Y.; Liu, C.-L.; Chang, Y.-M.; Zhao, J.; Perlman, S.; Hou, M.-H. Structural basis for the identification of the N-terminal domain of coronavirus nucleocapsid protein as an antiviral target. J. Med. Chem. 2014, 57, 2247–2257. [Google Scholar] [CrossRef]
- De Clercq, E.; Robins, M.J. Xylotubercidin against herpes simplex virus type 2 in mice. Antimicrob. Agents Chemother. 1986, 30, 719–724. [Google Scholar] [CrossRef] [PubMed][Green Version]
- O’Brien, W.J.; Taylor, J.L.; O’Malley, T.P.; Ritch, P.S. The antiherpesvirus activity and cytotoxicity of sangivamycin. Curr. Eye Res. 1987, 6, 255–257. [Google Scholar] [CrossRef] [PubMed]
- Bergstrom, D.E.; Brattesani, A.J.; Ogawa, M.K.; Reddy, P.A.; Schweickert, M.J.; Balzarini, J.; De Clercq, E. Antiviral activity of C-5 substituted tubercidin analogues. J. Med. Chem. 1984, 27, 285–292. [Google Scholar] [CrossRef]
- De Clercq, E.; Bernaerts, R.; Bergstrom, D.E.; Robins, M.J.; Montgomery, J.A.; Holy, A. Antirhinovirus activity of purine nucleoside analogs. Antimicrob. Agents Chemother. 1986, 29, 482–487. [Google Scholar] [CrossRef][Green Version]
- Glazer, R.I.; Peale, A.L. Comparison between the inhibitory activities of sangivamycin and thiosangivamycin on nuclear ribonucleic acid synthesis in L1210 cells in vitro. Biochem. Pharmacol. 1980, 29, 305–310. [Google Scholar] [CrossRef]
- Uretsky, S.C.; Acs, G.; Reich, E.; Mori, M.; Altwerger, L. Pyrrolopyrimidine nucleotides and protein synthesis. J. Biol. Chem. 1968, 243, 306–312. [Google Scholar]
- García, M.; Cooper, A.; Shi, W.; Bornmann, W.; Carrion, R.; Kalman, D.; Nabel, G.J. Productive replication of Ebola virus is regulated by the c-Abl1 tyrosine kinase. Sci. Transl. Med. 2012, 4, 123ra24. [Google Scholar] [CrossRef]
- Johnson, J.C.; Martinez, O.; Honko, A.N.; Hensley, L.E.; Olinger, G.G.; Basler, C.F. Pyridinyl imidazole inhibitors of p38 MAP kinase impair viral entry and reduce cytokine induction by Zaire ebolavirus in human dendritic cells. Antivir. Res. 2014, 107, 102–109. [Google Scholar] [CrossRef]
- Mohr, E.L.; McMullan, L.K.; Lo, M.K.; Spengler, J.R.; Bergeron, É.; Albariño, C.G.; Shrivastava-Ranjan, P.; Chiang, C.-F.; Nichol, S.T.; Spiropoulou, C.F.; et al. Inhibitors of cellular kinases with broad-spectrum antiviral activity for hemorrhagic fever viruses. Antivir. Res. 2015, 120, 40–47. [Google Scholar] [CrossRef]
- Nelson, E.A.; Dyall, J.; Hoenen, T.; Barnes, A.B.; Zhou, H.; Liang, J.Y.; Michelotti, J.; Dewey, W.H.; DeWald, L.E.; Bennett, R.S.; et al. The phosphatidylinositol-3-phosphate 5-kinase inhibitor apilimod blocks filoviral entry and infection. PLoS Negl. Trop. Dis. 2017, 11, e0005540. [Google Scholar] [CrossRef]
- Stewart, C.M.; Dorion, S.S.; Ottenbrite, M.A.F.; LeBlond, N.D.; Smith, T.K.T.; Qiu, S.; Fullerton, M.D.; Kobasa, D.; Côté, M. A diacylglycerol kinase inhibitor, R-59-022, blocks filovirus internalization in host cells. Viruses 2019, 11, 206. [Google Scholar] [CrossRef] [PubMed]
- Takamatsu, Y.; Krähling, V.; Kolesnikova, L.; Halwe, S.; Lier, C.; Baumeister, S.; Noda, T.; Biedenkopf, N.; Becker, S. Serine-arginine protein kinase 1 regulates Ebola virus transcription. mBio 2020, 11, e02565-19. [Google Scholar] [CrossRef] [PubMed]
- Kang, Y.-L.; Chou, Y.-y.; Rothlauf, P.W.; Liu, Z.; Soh, T.K.; Cureton, D.; Case, J.B.; Chen, R.E.; Diamond, M.S.; Whelan, S.P.J.; et al. Inhibition of PIKfyve kinase prevents infection by Zaire ebolavirus and SARS-CoV-2. Proc. Natl. Acad. Sci. USA 2020, 117, 20803–20813. [Google Scholar] [CrossRef]
- Schein, P.S.; Davis, R.D.; Carter, S.; Newman, J.; Schein, D.R.; Rall, D.P. The evaluation of anticancer drugs in dogs and monkeys for the prediction of qualitative toxicities in man. Clin. Pharmacol. Ther. 1970, 11, 3–40. [Google Scholar] [CrossRef] [PubMed]
- Hardesty, C.T.; Chaney, N.A.; Waravdekar, V.S.; Mead, J.A.R. The disposition of the antitumor agent, sangivamycin, in mice. Cancer Res. 1974, 34, 1005–1009. [Google Scholar] [PubMed]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Bennett, R.P.; Finch, C.L.; Postnikova, E.N.; Stewart, R.A.; Cai, Y.; Yu, S.; Liang, J.; Dyall, J.; Salter, J.D.; Smith, H.C.; et al. A Novel Ebola Virus VP40 Matrix Protein-Based Screening for Identification of Novel Candidate Medical Countermeasures. Viruses 2021, 13, 52. https://doi.org/10.3390/v13010052
Bennett RP, Finch CL, Postnikova EN, Stewart RA, Cai Y, Yu S, Liang J, Dyall J, Salter JD, Smith HC, et al. A Novel Ebola Virus VP40 Matrix Protein-Based Screening for Identification of Novel Candidate Medical Countermeasures. Viruses. 2021; 13(1):52. https://doi.org/10.3390/v13010052
Chicago/Turabian StyleBennett, Ryan P., Courtney L. Finch, Elena N. Postnikova, Ryan A. Stewart, Yingyun Cai, Shuiqing Yu, Janie Liang, Julie Dyall, Jason D. Salter, Harold C. Smith, and et al. 2021. "A Novel Ebola Virus VP40 Matrix Protein-Based Screening for Identification of Novel Candidate Medical Countermeasures" Viruses 13, no. 1: 52. https://doi.org/10.3390/v13010052
APA StyleBennett, R. P., Finch, C. L., Postnikova, E. N., Stewart, R. A., Cai, Y., Yu, S., Liang, J., Dyall, J., Salter, J. D., Smith, H. C., & Kuhn, J. H. (2021). A Novel Ebola Virus VP40 Matrix Protein-Based Screening for Identification of Novel Candidate Medical Countermeasures. Viruses, 13(1), 52. https://doi.org/10.3390/v13010052






