Developments in PDT Sensitizers for Increased Selectivity and Singlet Oxygen Production
Abstract
:1. Introduction
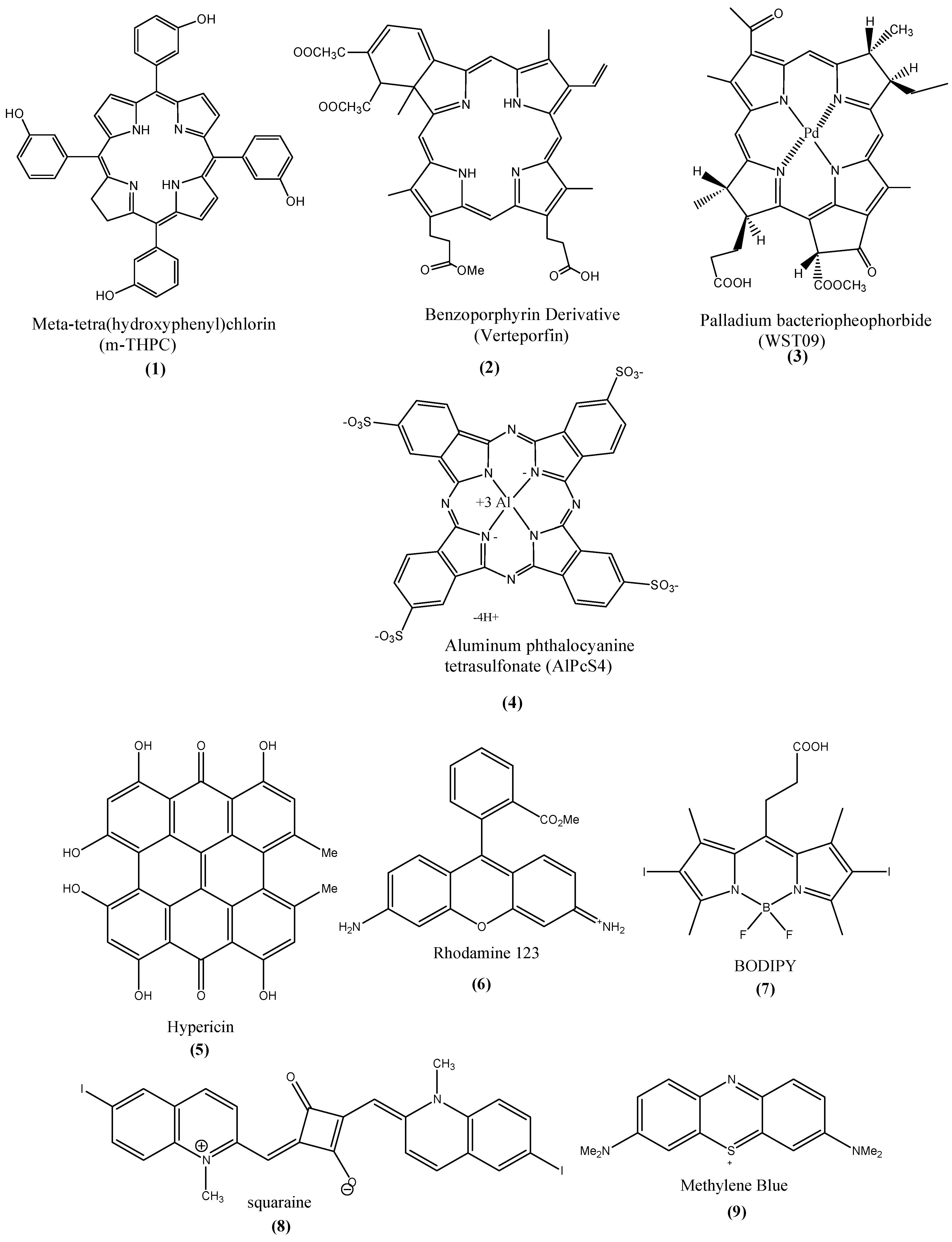
1.1. Photosensitizers (PSs)
- High selectivity toward cancer cells
- Production of toxic reactive oxygen species (e.g., 1O2) or free radicals
- Optimal ADME (absorption, distribution, metabolism, excretion) [10]
- Near IR light absorption
- Absence of dark toxicity
- High molar extinction coefficient
1.2. PDT Mechanism
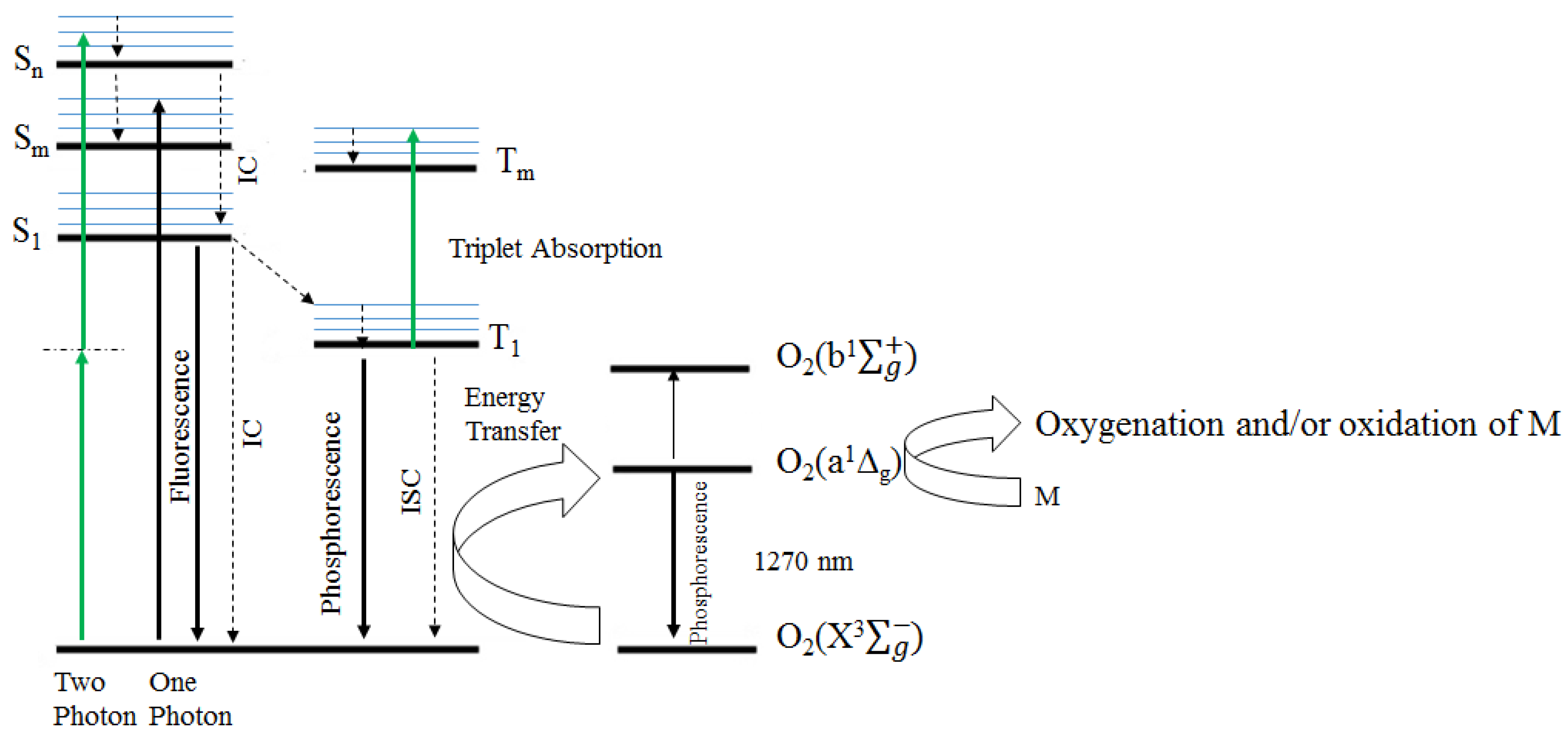
1.3. Singlet Oxygen Formation
1.4. Mechanisms of Cell Death
1.5. Therapeutic Irradiation
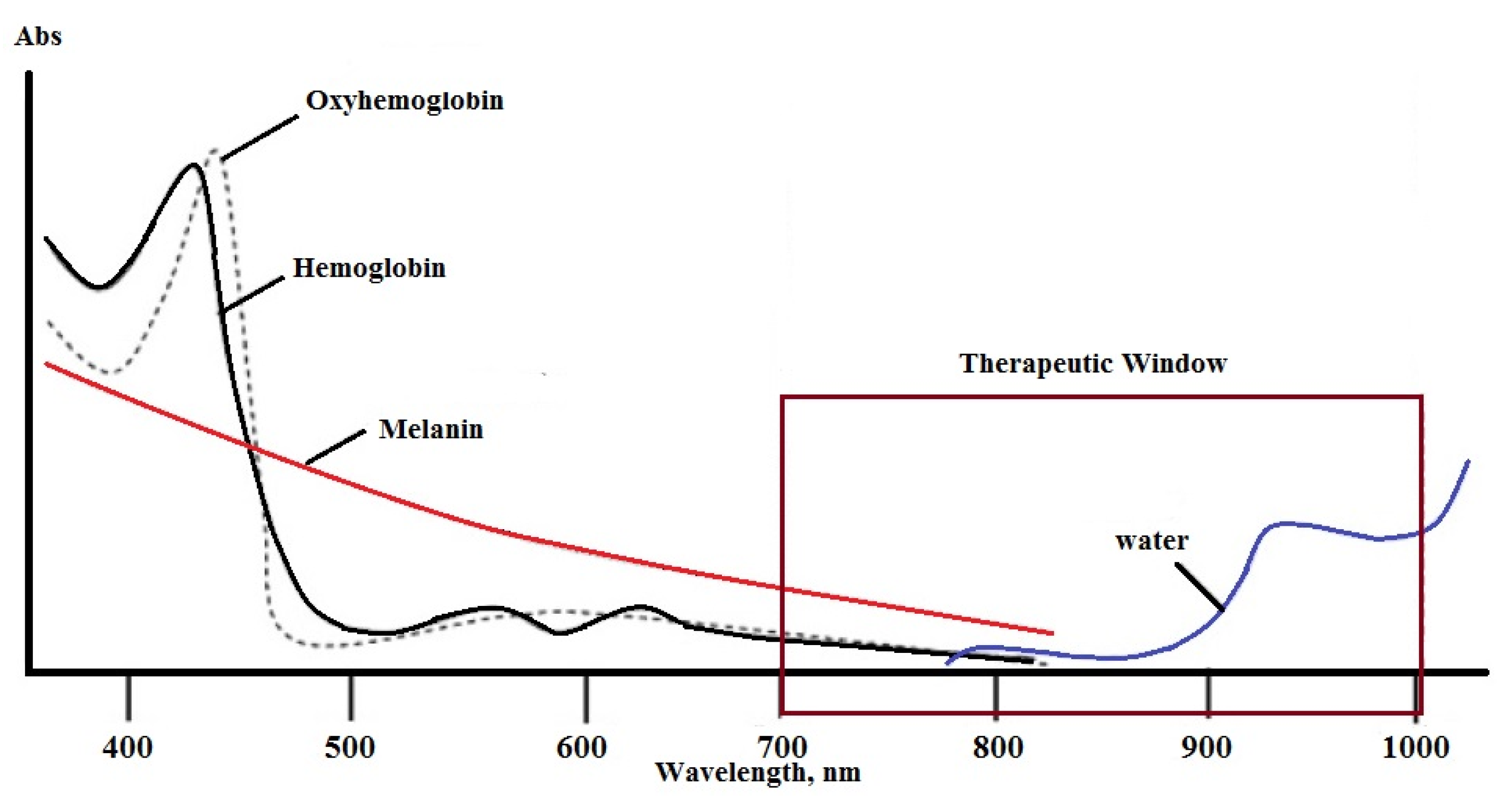
1.6. Importance of Subcellular Localization
| Photosensitizer Type | Sub-Cellular Localization | Reference |
|---|---|---|
| N-aspartyl chlorin E6 (NPe6) | Lysosome | [29] |
| (Benzoporphyrin derivative) (BPD) | Mitochondria | [29] |
| 5-Ethylamino-9-diethylaminobenzo [a]phenothiazinium chloride (EtBNS) | Lysosome | [29] |
| Galactose conjugate of 3-(1-hexyloxyethyl)-3- devinyl pyropeophorbide-a (HPPHgal) | Lysosome | [29] |
| Porphyrin-rhodamine B cation | Mitochondria | [30] |
| Porphyrin-mono-triphenyl phoosphonium cation | Mitochondria | [30] |
| Triphenylphosphonium (TPP) cation | Mitochondria | [31] |
| (E)-N-alkyl-4-[2-(ferrocenyl) vinyl]pyridinium cations | Mitochondria | [31] |
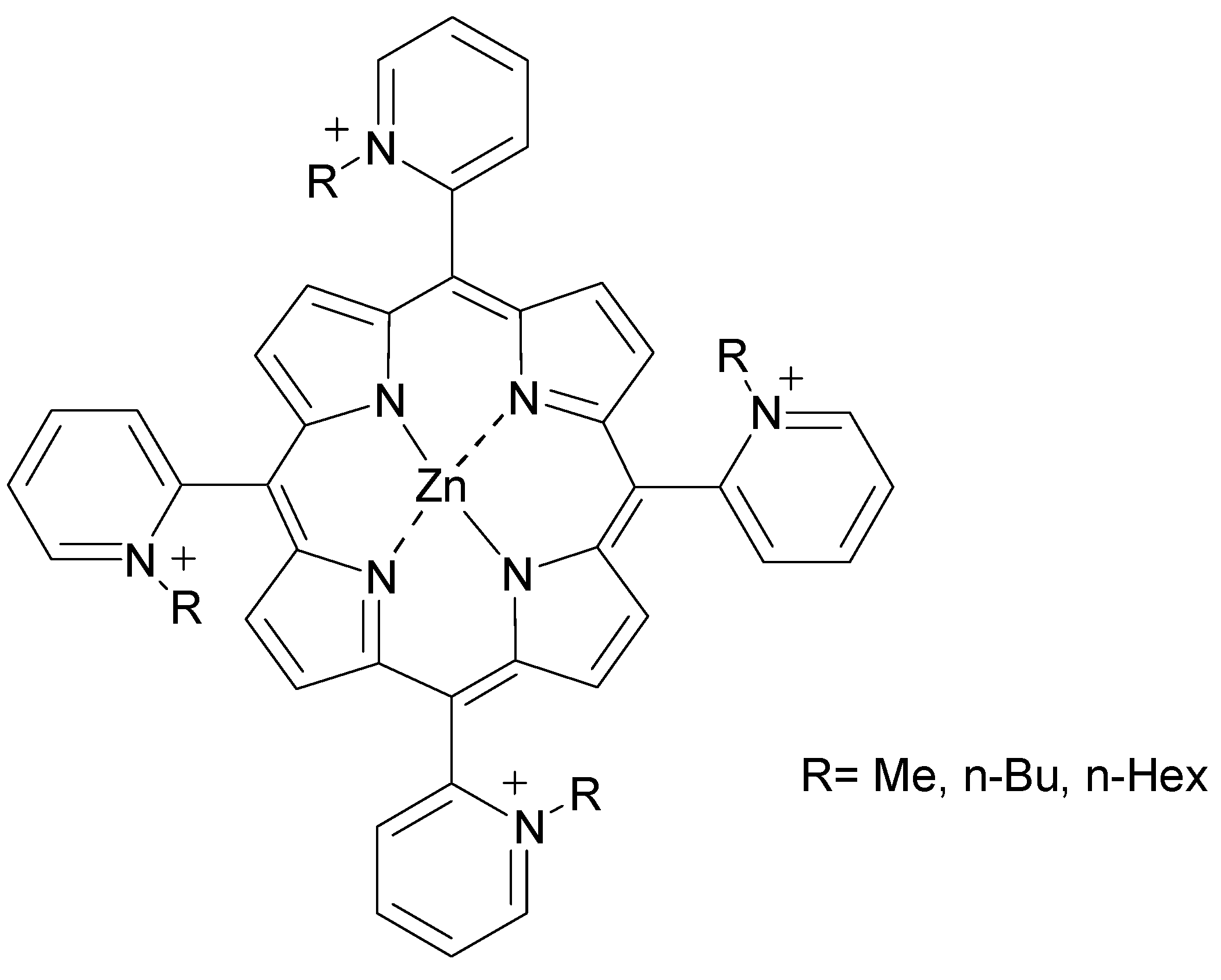
2. PS Uptake and Selectivity
2.1. Effect of Hydrophobicity (Lipophilicity) and Hydrophilicty on Cell Uptake and Selectivity
2.2. Effect of Intracellular pH on PS Uptake
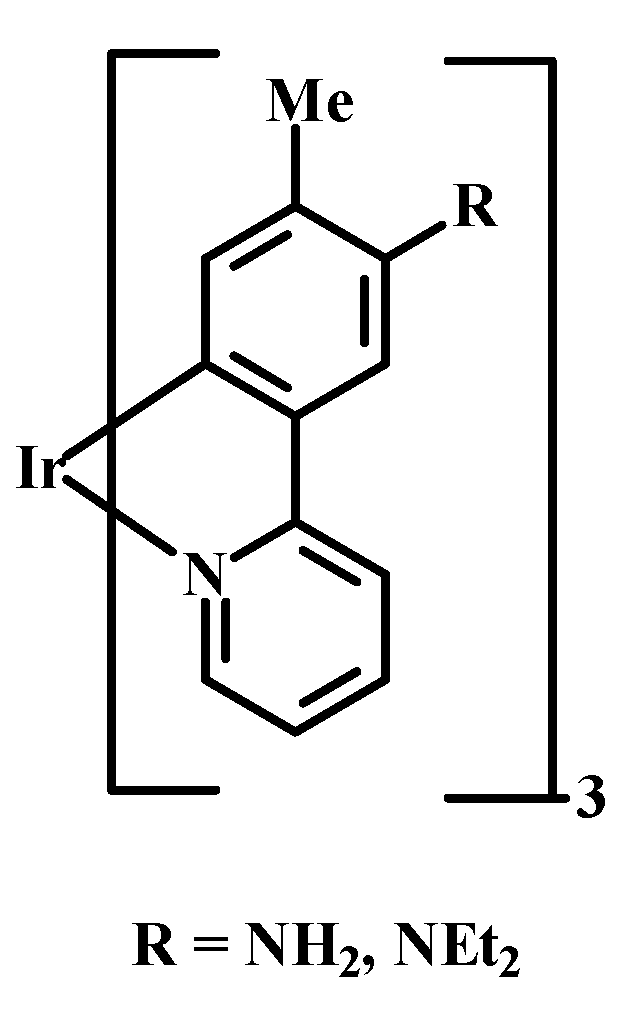
2.3. Use of Nanoparticles
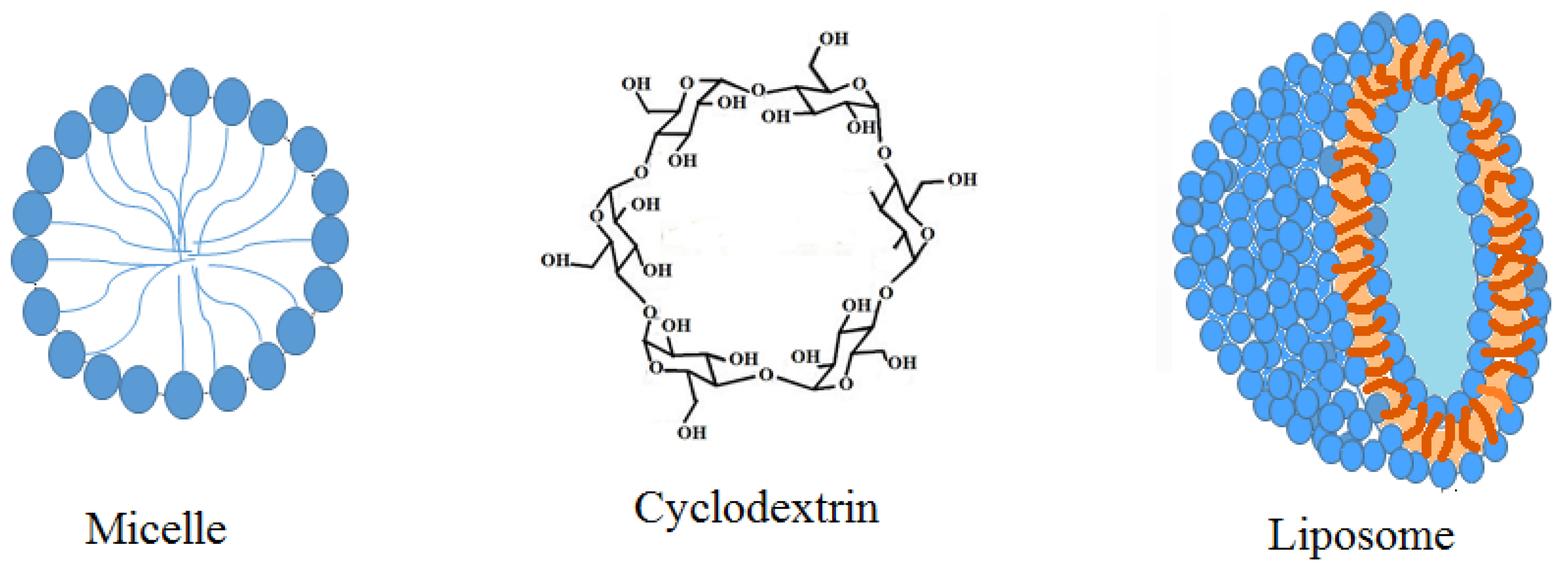
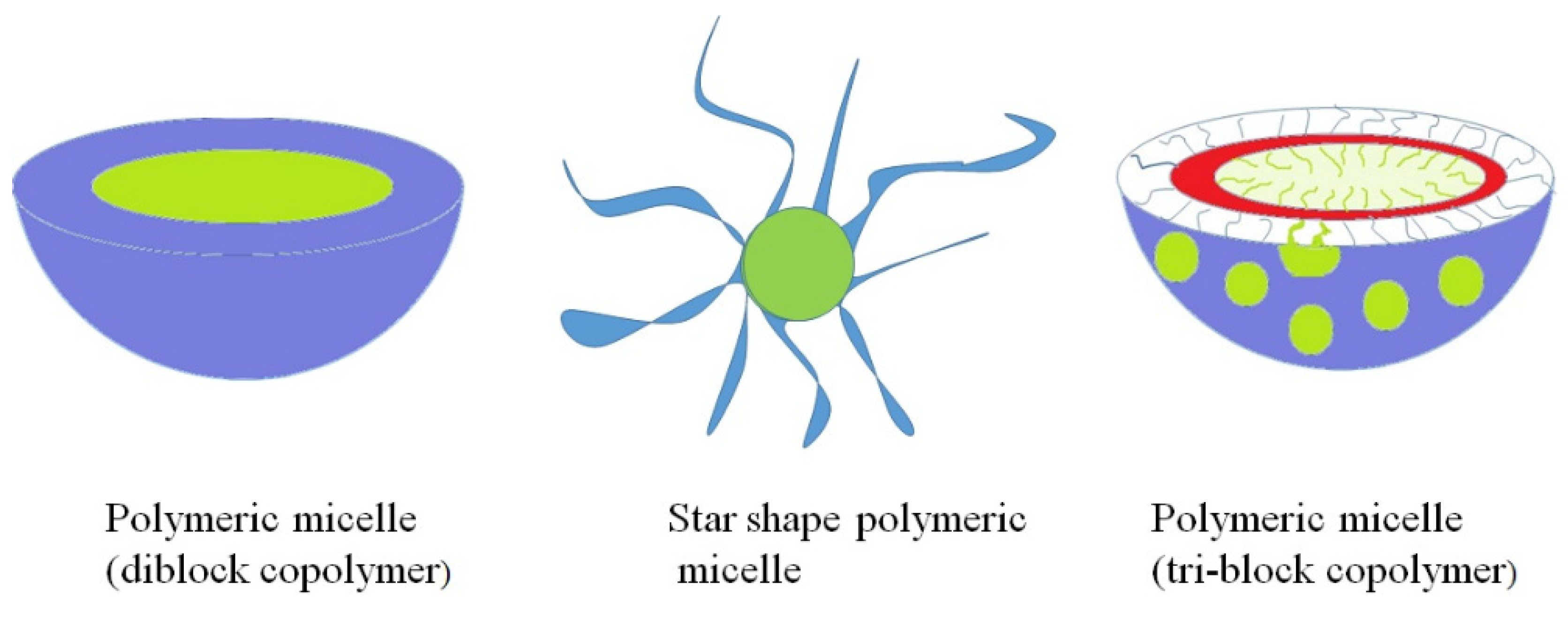
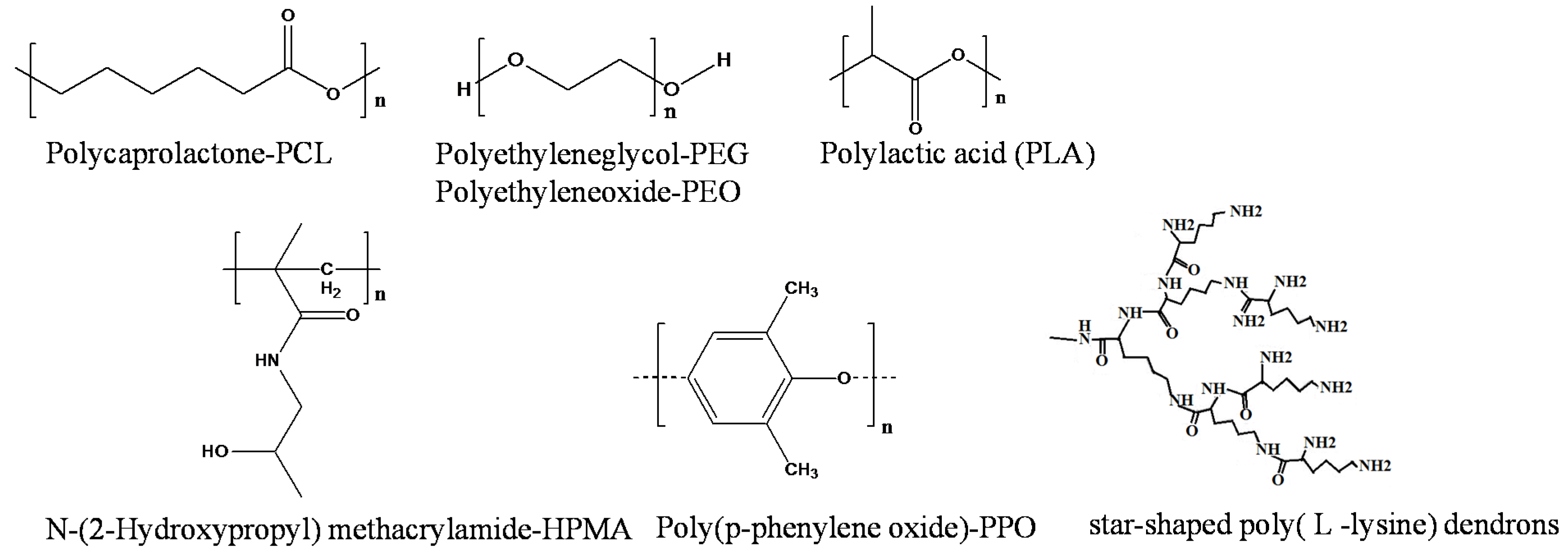
Polymeric Micelle/Micelles
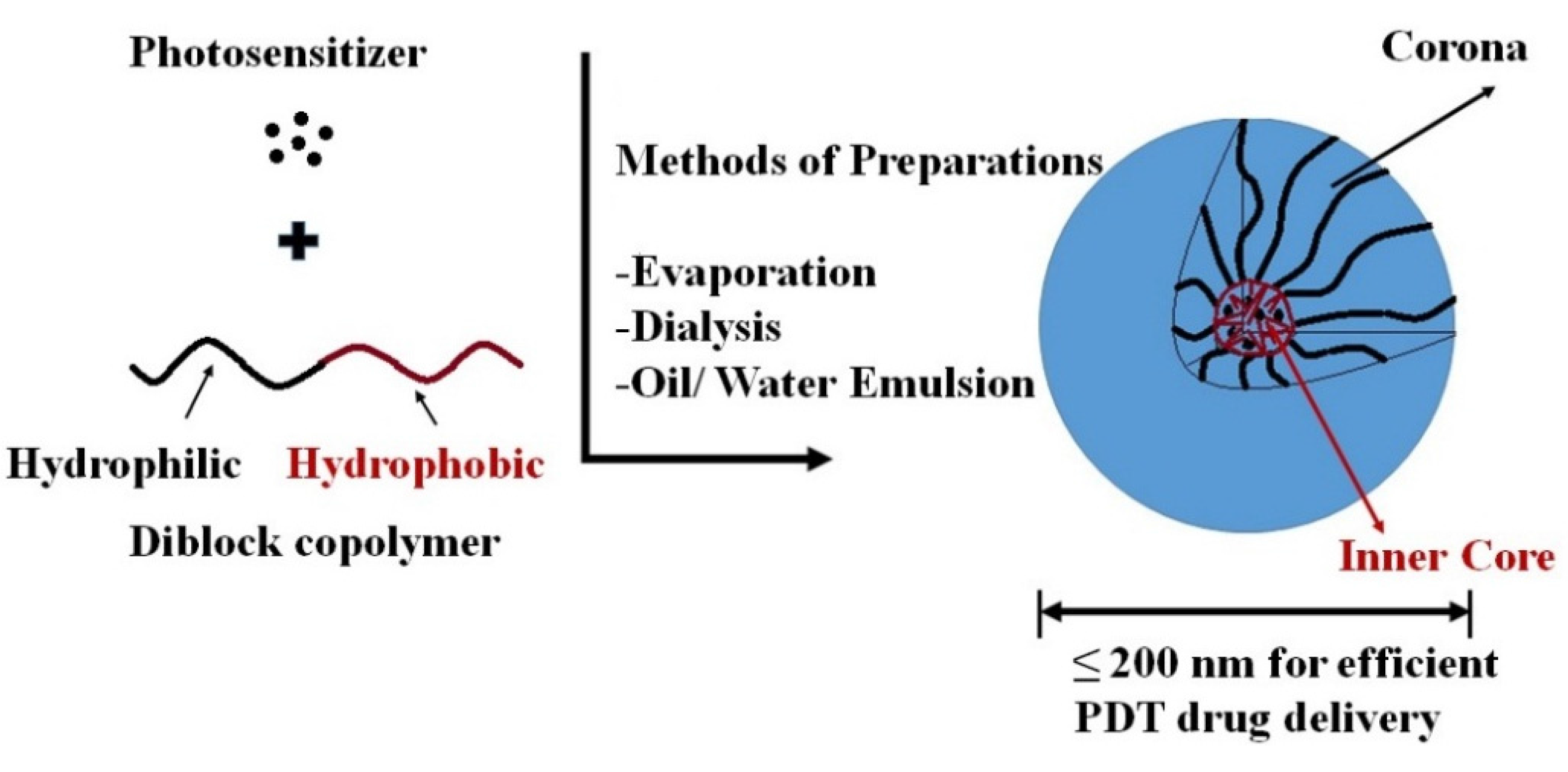
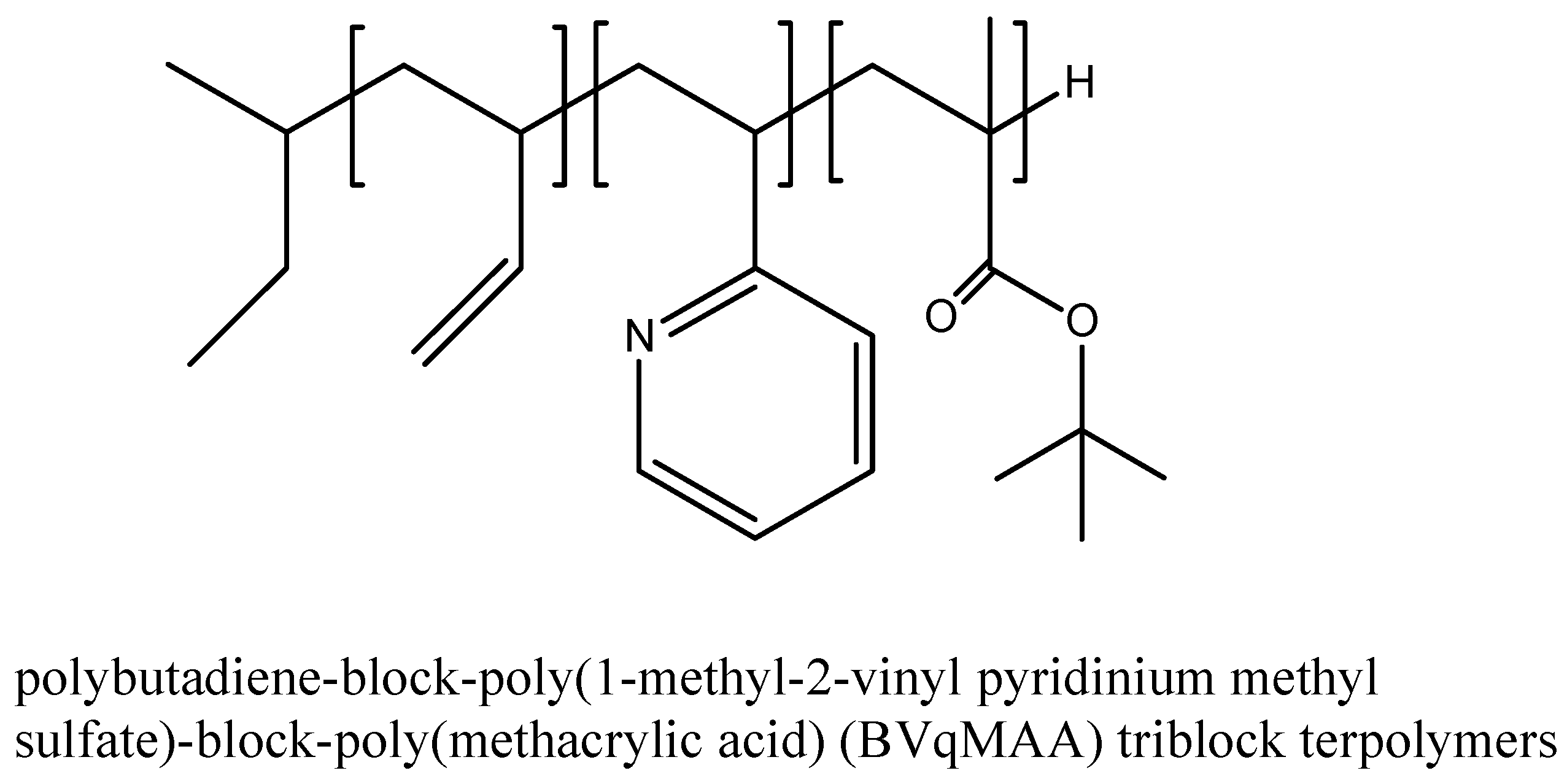
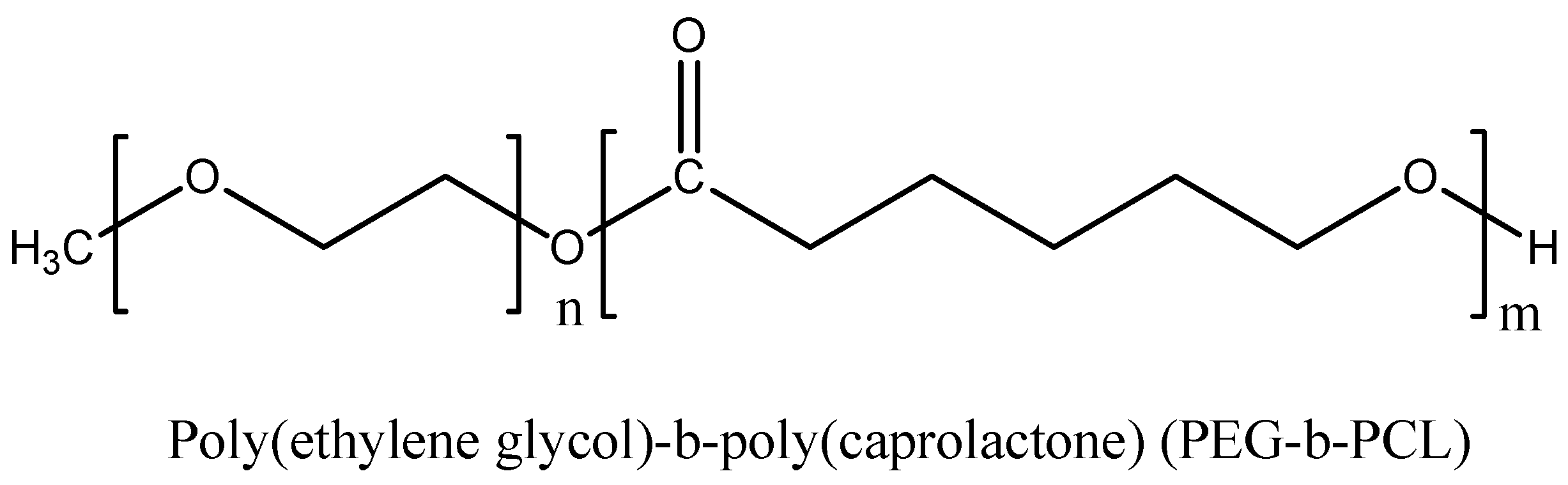
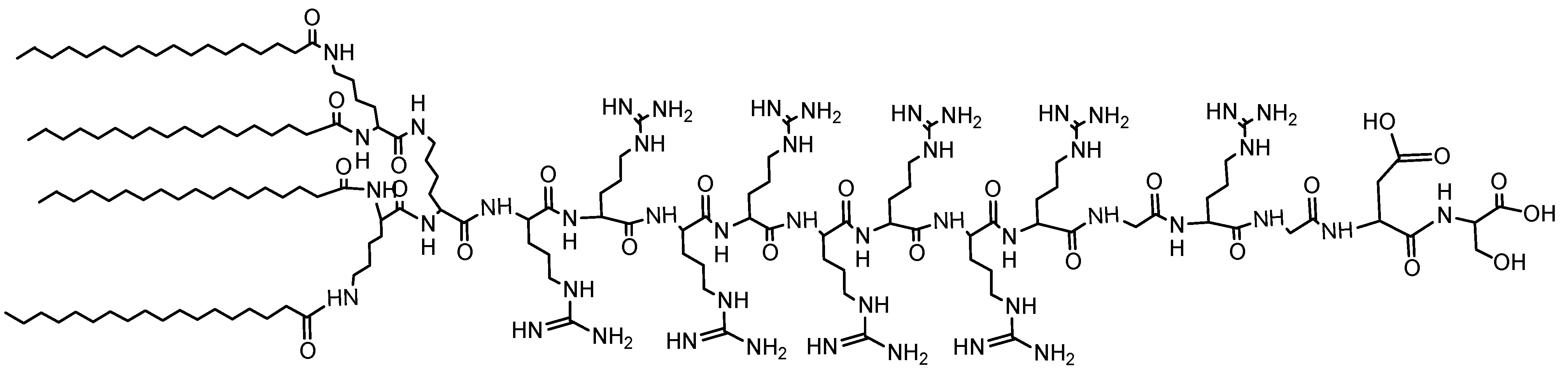
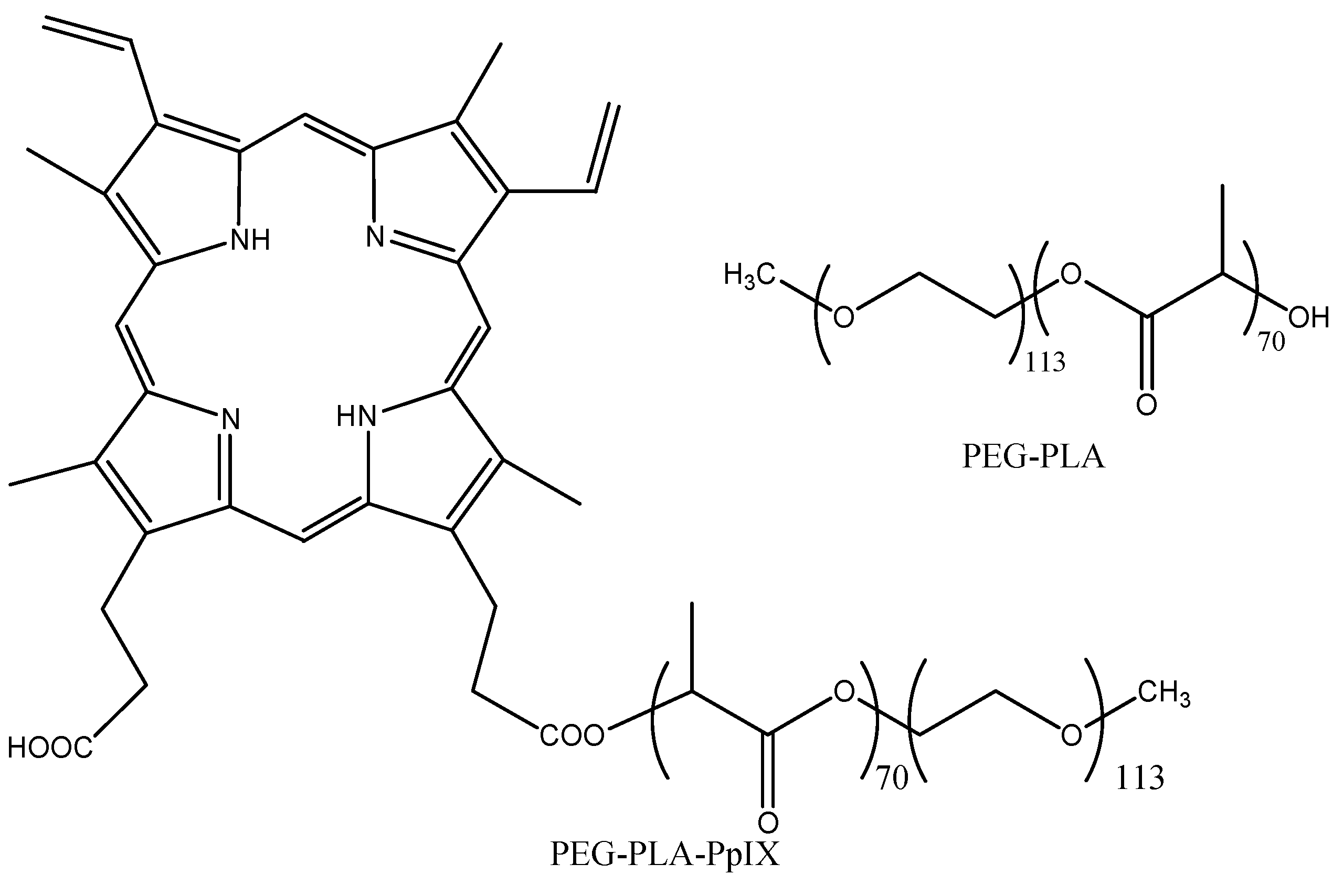
| Strategy for Targeting & Drug Release | Sensitizer | Polymer/Monomer | Loaded Particle Size (nm) | In vitro/In vivo | Ref. |
|---|---|---|---|---|---|
| Active targeting | Silicon phthalocyanine | PEG-PCL-GE11 Peptide (YHWYGYTPQNVI) | Human epidermoid carcinoma and head & neck cancer | [76,81] | |
| Active targeting Folate amino acid and overexpressed folate receptor | THPC | Poly (2-ethyl-2-oxazoline)-b-poly( d, l-lactide) (PEOz-PLA) (m-THPC-PM) (folate-m-THPC-PM) | 103.8 | In vitro on epidermoid cell line (KB); In vivo on KB xenograft mice | [78,92] |
| Active Galactosyl moiety for increased selectivity toward ASGP receptors on HepG2 cells | Porphyrin (conjugated to polymer) | APP-PAEMA_PCL Gal-APP-PAEMA-PCL | 60 | Human laryngeal carcinoma (HEp2); Human hepatocellular liver carcinoma (HepG2) | [69] |
| Passive Cellular endocytosis | Doxorubicin (DOX) | Star shaped poly(L-lysine) dendrons porphyrin polymer (PP-PLLD) | 150–192.5 | Human nasopharyngeal carcinoma (CNE2) | [72] |
| Passive targeting; Dual chemo-photodynamic therapy | Paclitaxel Synthetic chlorin | Star-shaped di-block copolymer (CSBC-58) | 103.2 | Breast cancer (MCF7) | [68] |
| Passive targeting | Pheophorbide a (phA) & β-carotene(CAR) | Poly(ethylene glycol)-b-poly(caprolactone) PEG-b-PCL | 100 | Human breast and cervical cancer cell line | [82] |
| Passive targeting | Chlorin e6 | Poly(ethylene glycol)- b-poly(l-aspartic acid)-b-poly(l-phenylalanine) (PEG-PAsp-PPhe) | 74.6 | In vitro assay on MCF7 | [73] |
| Passive targeting (endocytosis); Dual chemo-PDT | m-THPC SN-38 | Chlorinated core star shape block copolymer (CSBC) | 115.7–163.7 | Human colon cancer (HT-29); In vivo xenograft | [77] |
| Passive targeting Dual photothermal (PTT) and PDT | IR825 Chlorin e6 | C18PMH-PEG-Ce6-Gd | 100–200 | In vitro and in vivo assay on 4T1 Cell line | [93] |
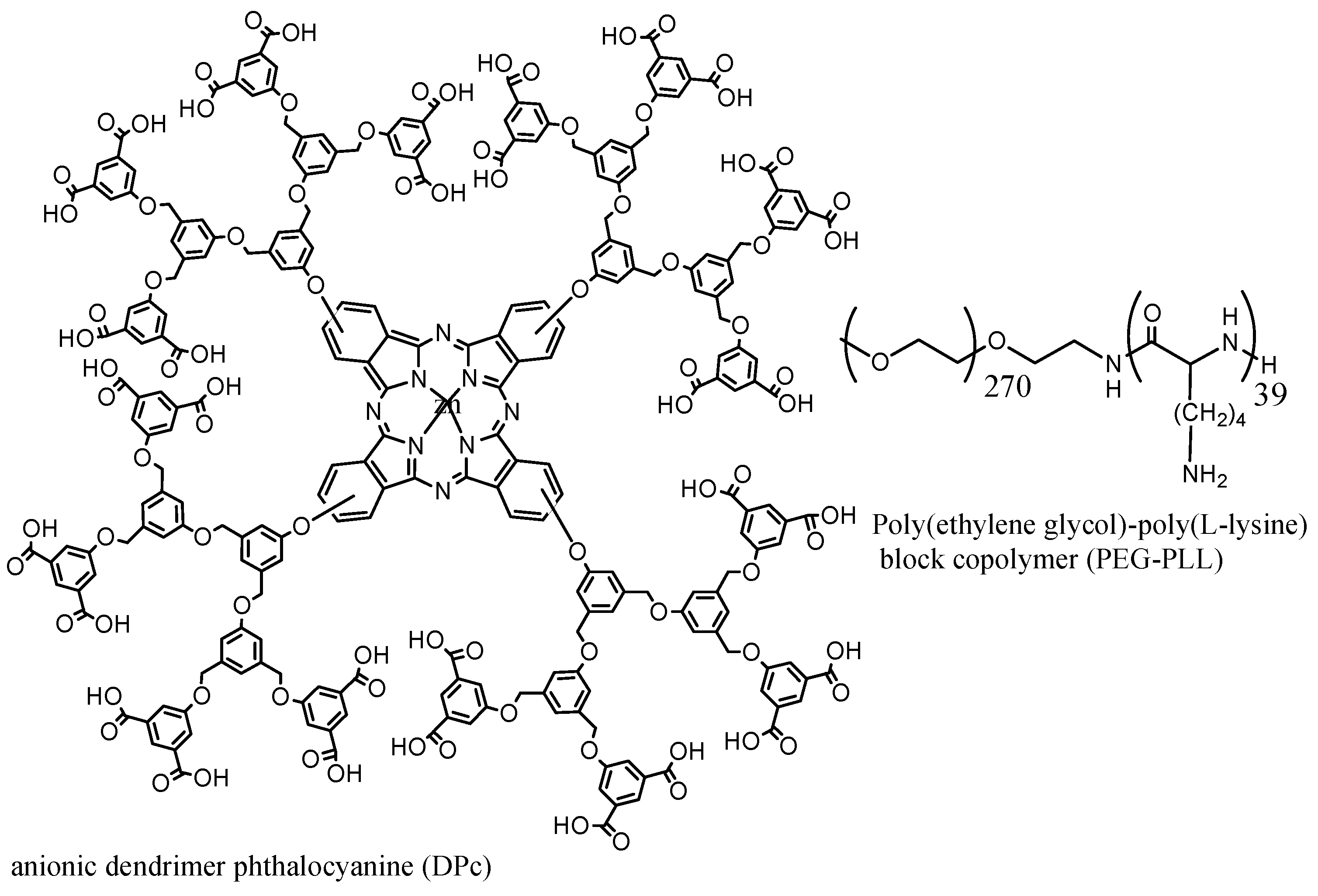
| Passive endocytosis | Dendrimer phthalocyanine DPc | DPc + (PEG-PLL) → (DPc/m) | 50 | A549 cells in mice | [90] |
| Passive targeting Accumulate in mitochondria | Hypericin | DSPE-mPEG2000 micelle | 12 | Malignant brain tumor (MBTs) | [89] |
| Enzyme control release (in presence of l-phenylalanine) | THPP | Ethyl cellulose-graft-poly(ε-Caprolactone) and alpha cyclodextrin → EC-g-PCL and α-CD | 205 | 85% THPP release in 6 h; MCF-7 | [87] |
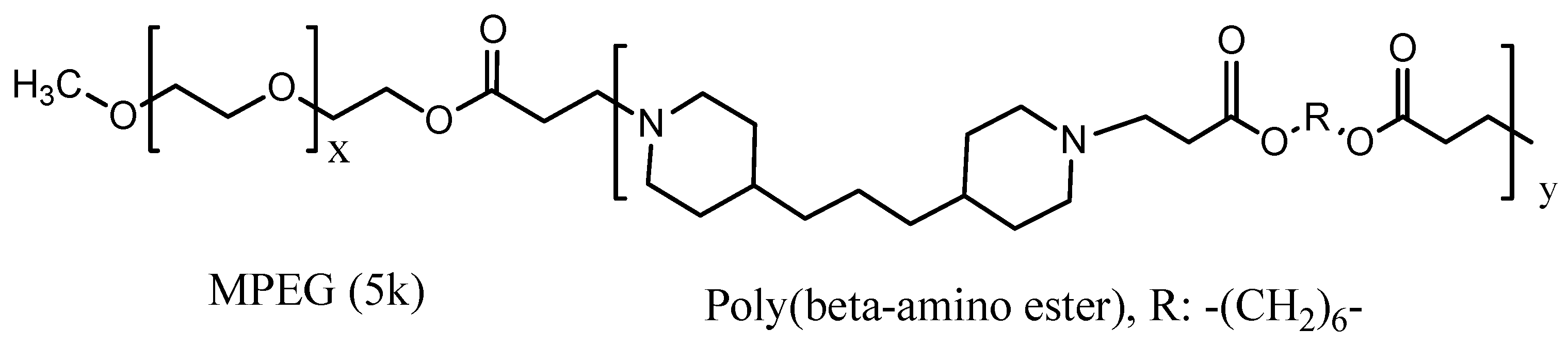
| Passive pH responsive polymeric micelles | PpIX | MPEG-Poly(β-amino ester) block copolymer (PpIx-pH-PMs) | 122 | In vivo on live SCC7 tumor-bearing mice; In vitro on SCC7 cells | [78] |
| Passive targeting | Pheophorbide | PEO750-b-PCL5 polymer | 20 | Human breast cell line (MCF-7) | [70] |
| Passive targeting | Porphyrazine | Polybutadiene-block-poly(1-ethyl-2-vinyl pyridinium methyl sulfate)-block-poly(methacrylic acid) (BVqMAA) triblock terpolymers | 256 | In vitro assay on A549 cells; Diameter size 6%–12% loading; In vivo assay | [71] |
| Passive targeting | Chlorin e6/Fe3O4 | Multimeric grain-marked micelles with Fe3O4 inner core and outer multi grain micelle PLLA-b-PEG-Ma | 98 | KB tumor-bearing nude mice in vivo; KB cells line In vitro | [94] |
| Passive targeting | PpIX | PEG-PLA | 30 | H2009 lung cancer cells | [85] |
| Polymer degrades at site of action due to presence of lipase | m-THPC | mPEG750-b-oligo(ɛ-caprolactone)5 (mPEG750-b-OCL5) with a hydroxyl, benzoyl or naphthoyl end group | In vivo; In vitro on head & neck squamous carcinoma cell line UM-SCC-14C | [83] | |
| Study the effect of the length of hydrophobic units, PPO, on phototoxicity and solubility | ZnPc | Poloxamine polymers: T304 (15-PEO unit, 17.1-PPOunit) T904 (60.9-PEO unit, 69.3-PPO unit) T1107 (238.6-PEO unit, 77.6-PPO unit) T1307 (286.4-PEO unit, 93.1-PPO unit) | 2.7 4.9 13.9 47.6 | KB cells; Increase in phototoxicity and ZnPc solubility by increasing PPO unit | [65] |
| Passive targeting | Xanthene dye erythrosine B (ERY) | CTAB (cationic) micelle SDS (anionic) micelle | logP of 0.46 (hydrophilic dye) | [95] | |
| Tri-block copolymer | Gn-DPcZn | Polyion micelle; Amphiphilic triblock copolymer; PLL-b-PEG-b-PLL | High stability in vivo | [96] | |
| Passive targeting | Pheophorbide | PEO(2000)-b-PCL(2800) PEO(5000)-b-PCL(4000) PEO(2400)-b-PDLLA(2000) PEO(3100)-b-PS(2300) | 20–30 | HCT-116 human colorectal carcinoma | [97] |
3. Increased 1O2 Production
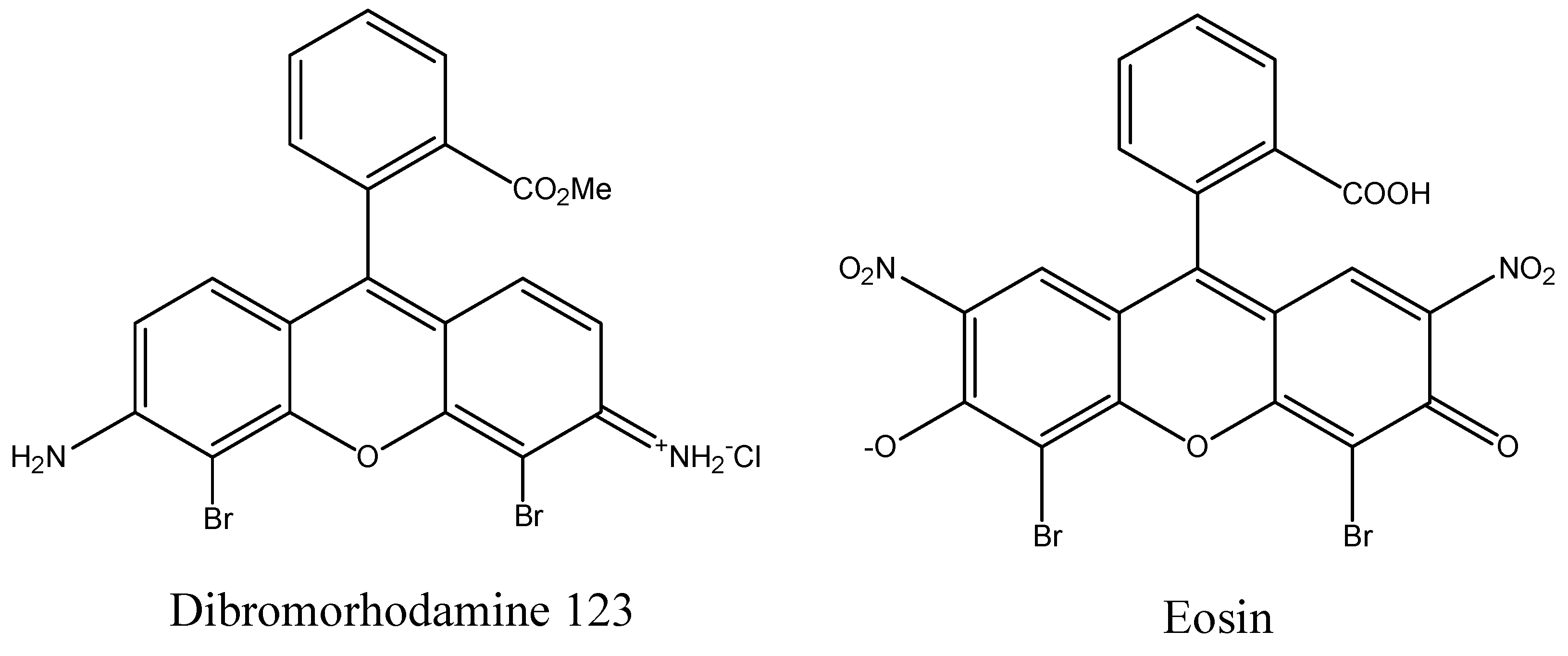
3.1. Incorporation of Heavy Atoms
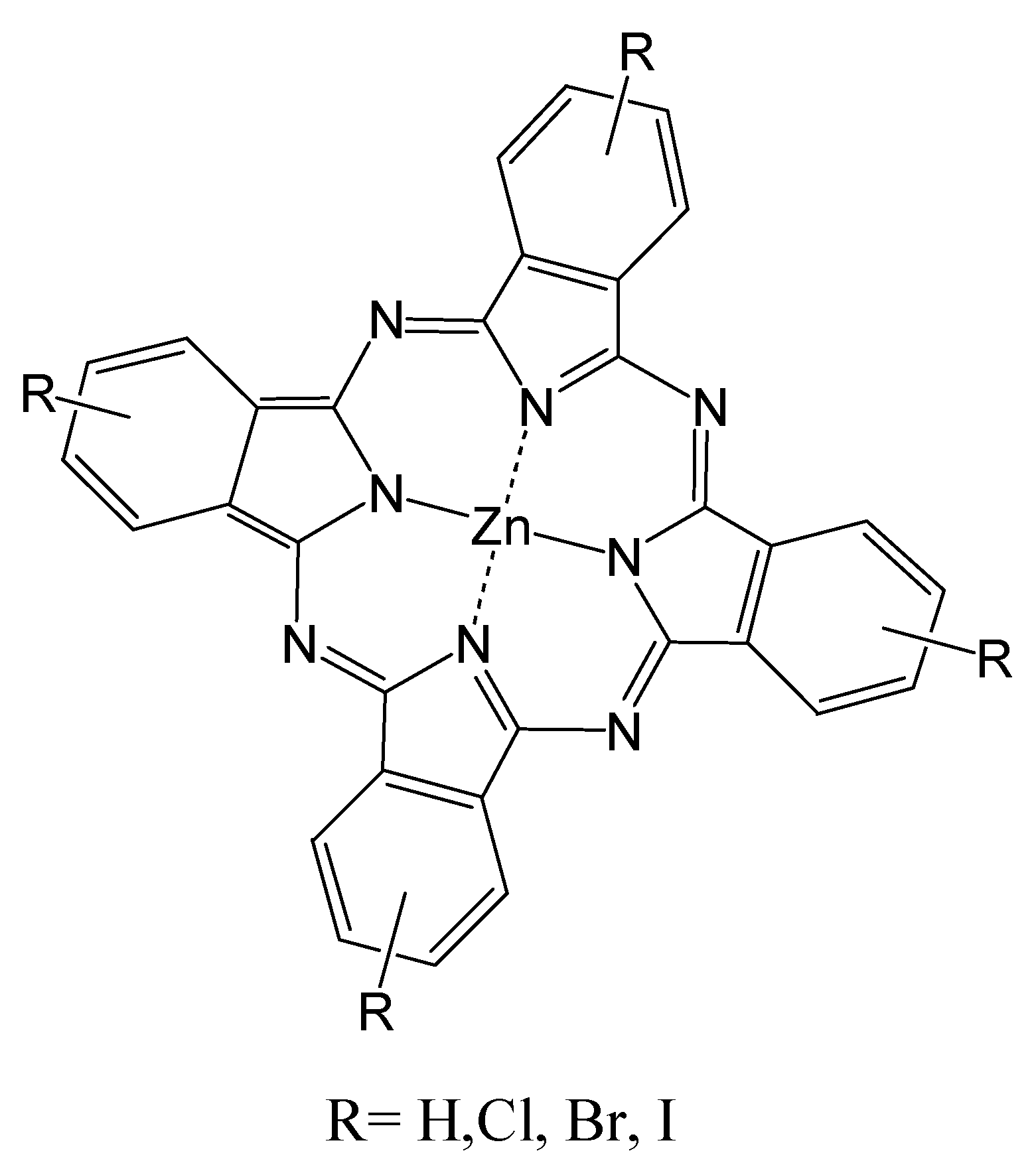
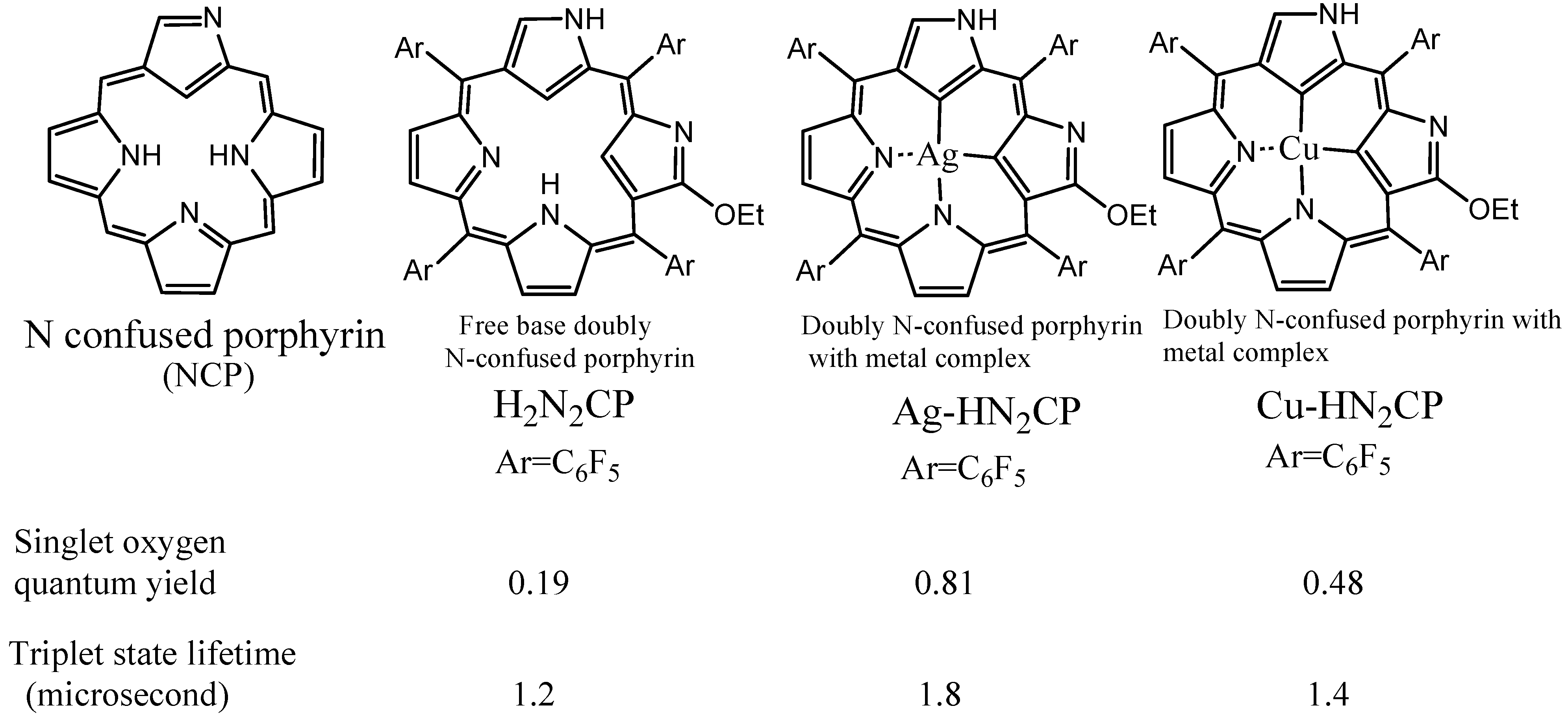
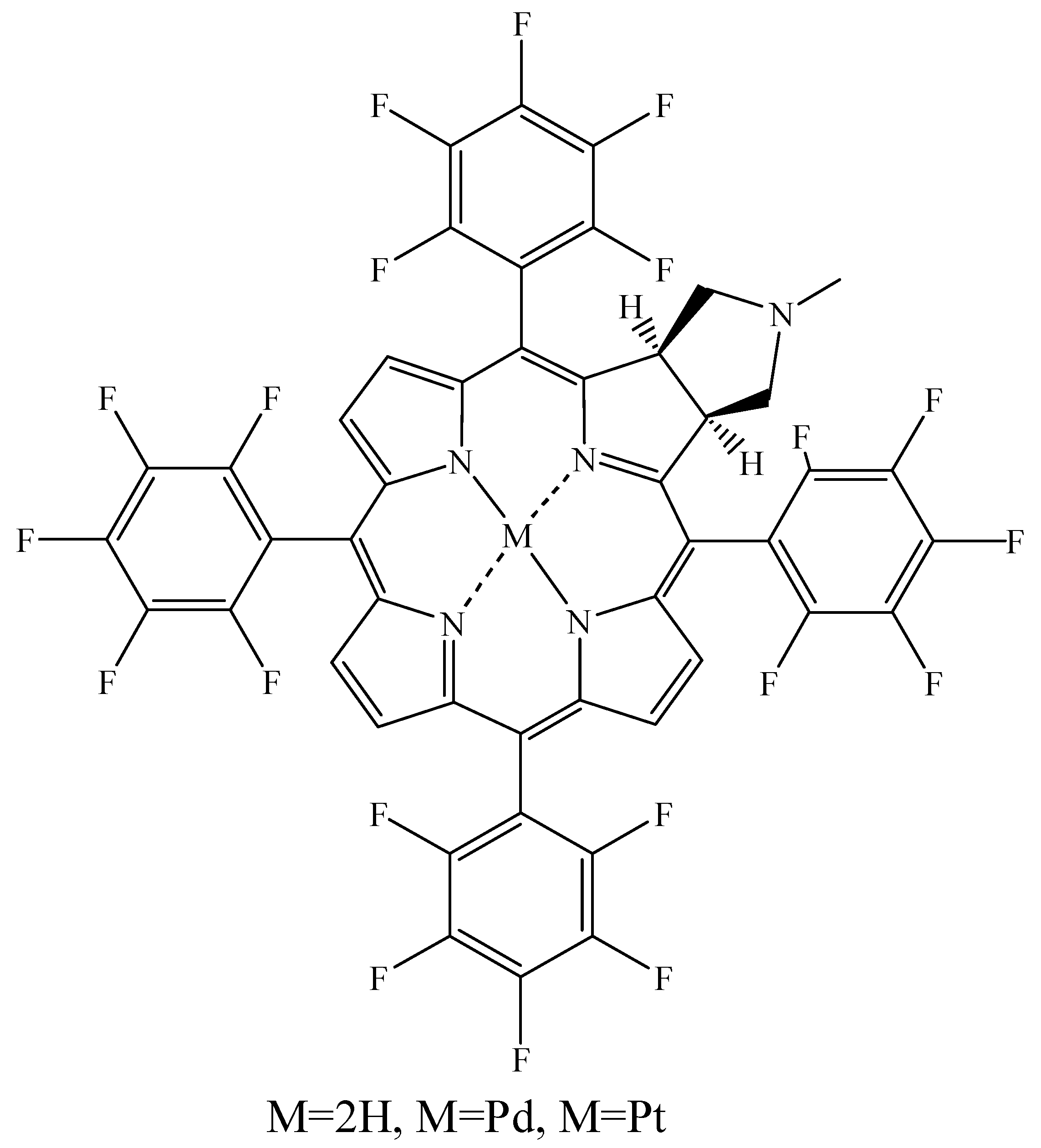
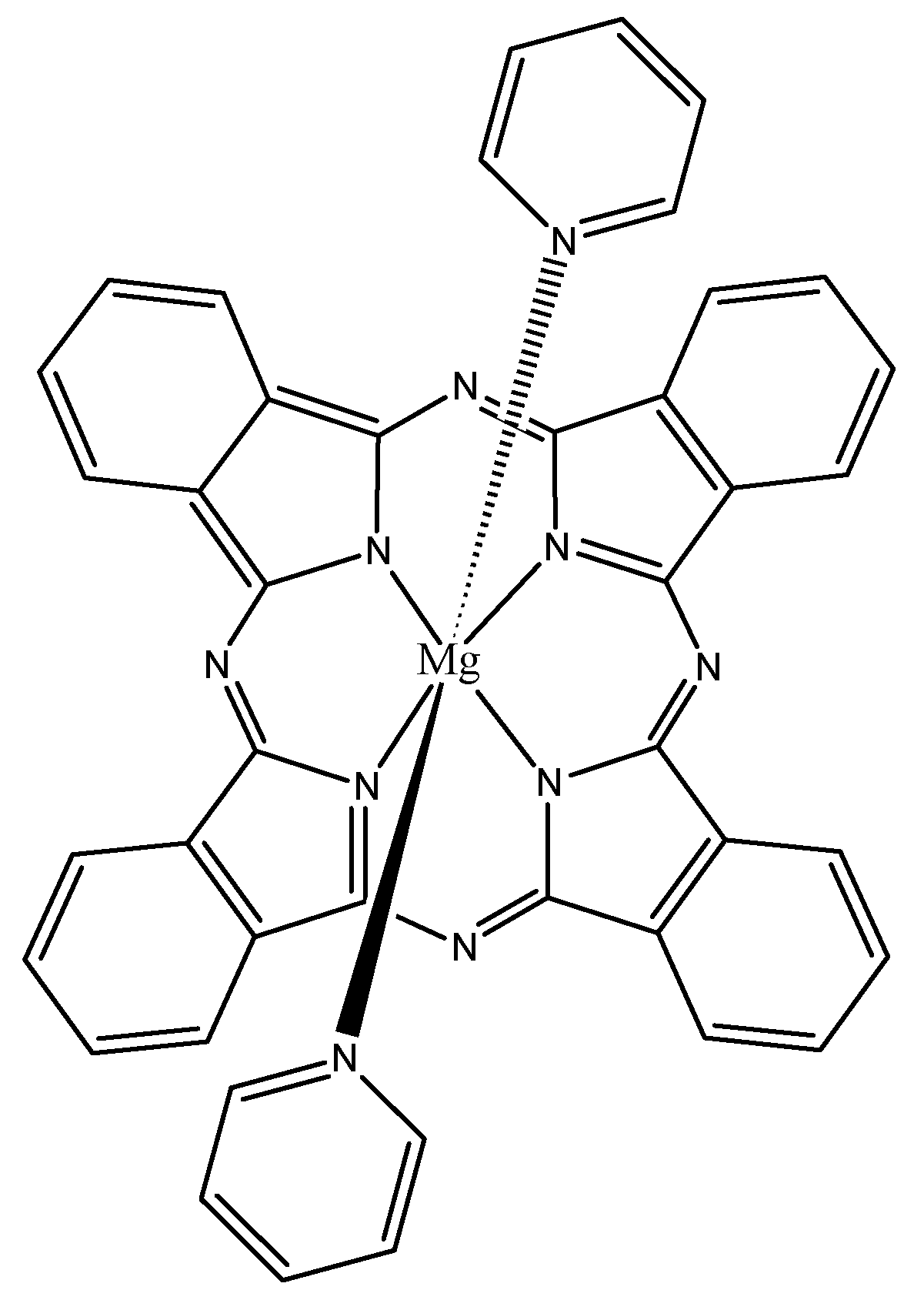
3.2. Isosteric Replacements
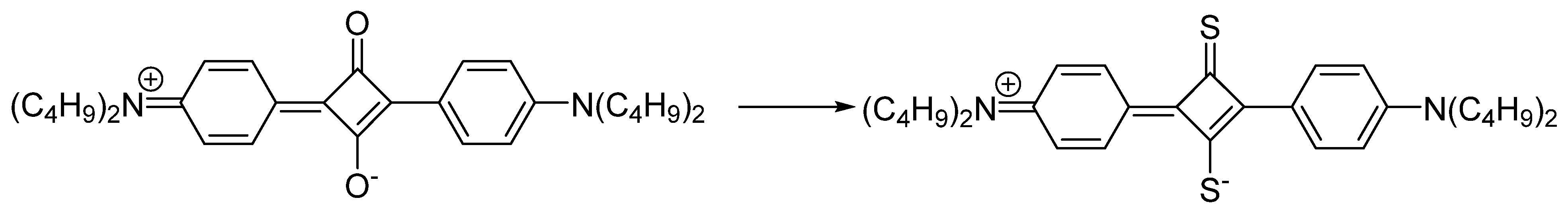
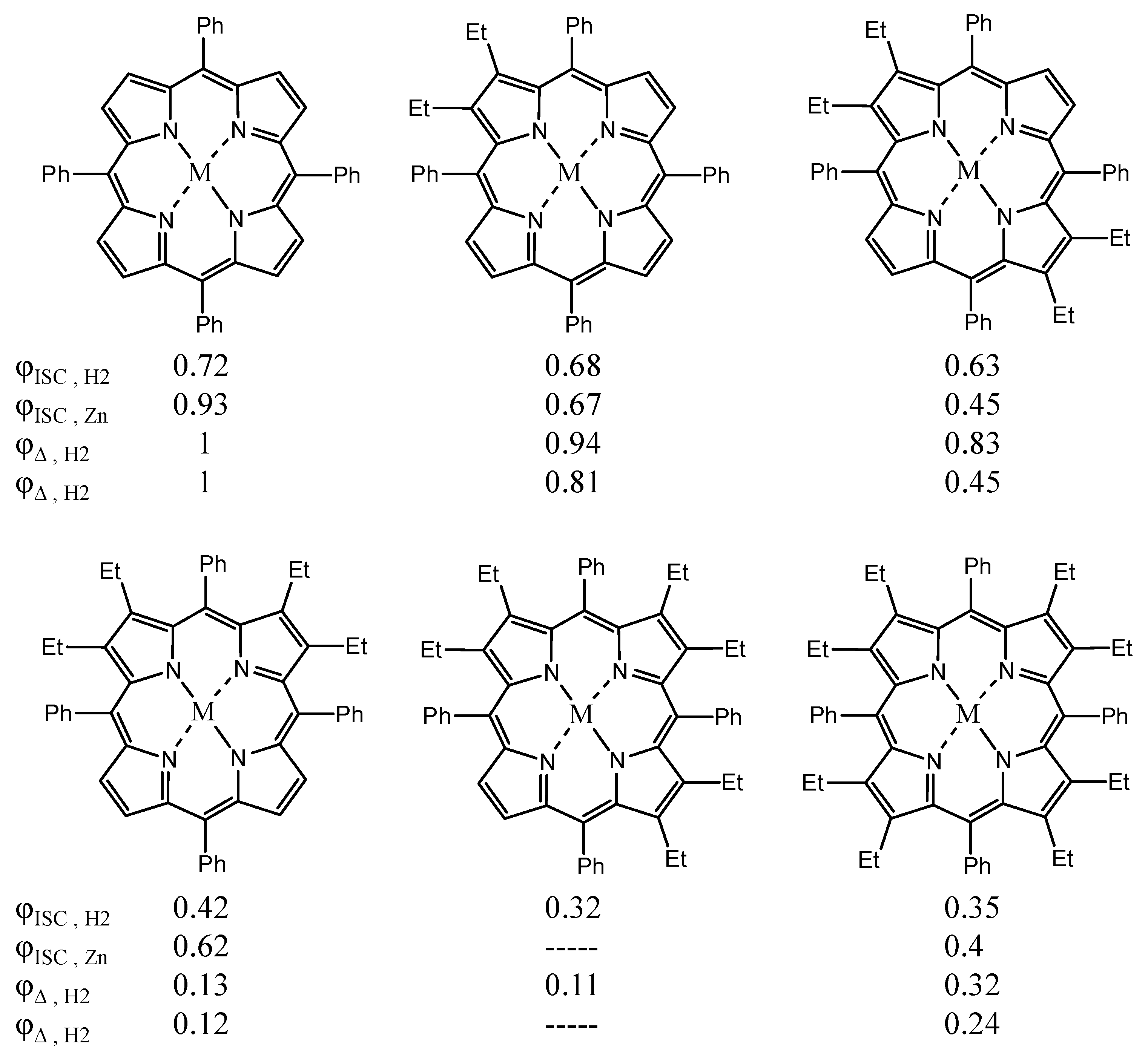
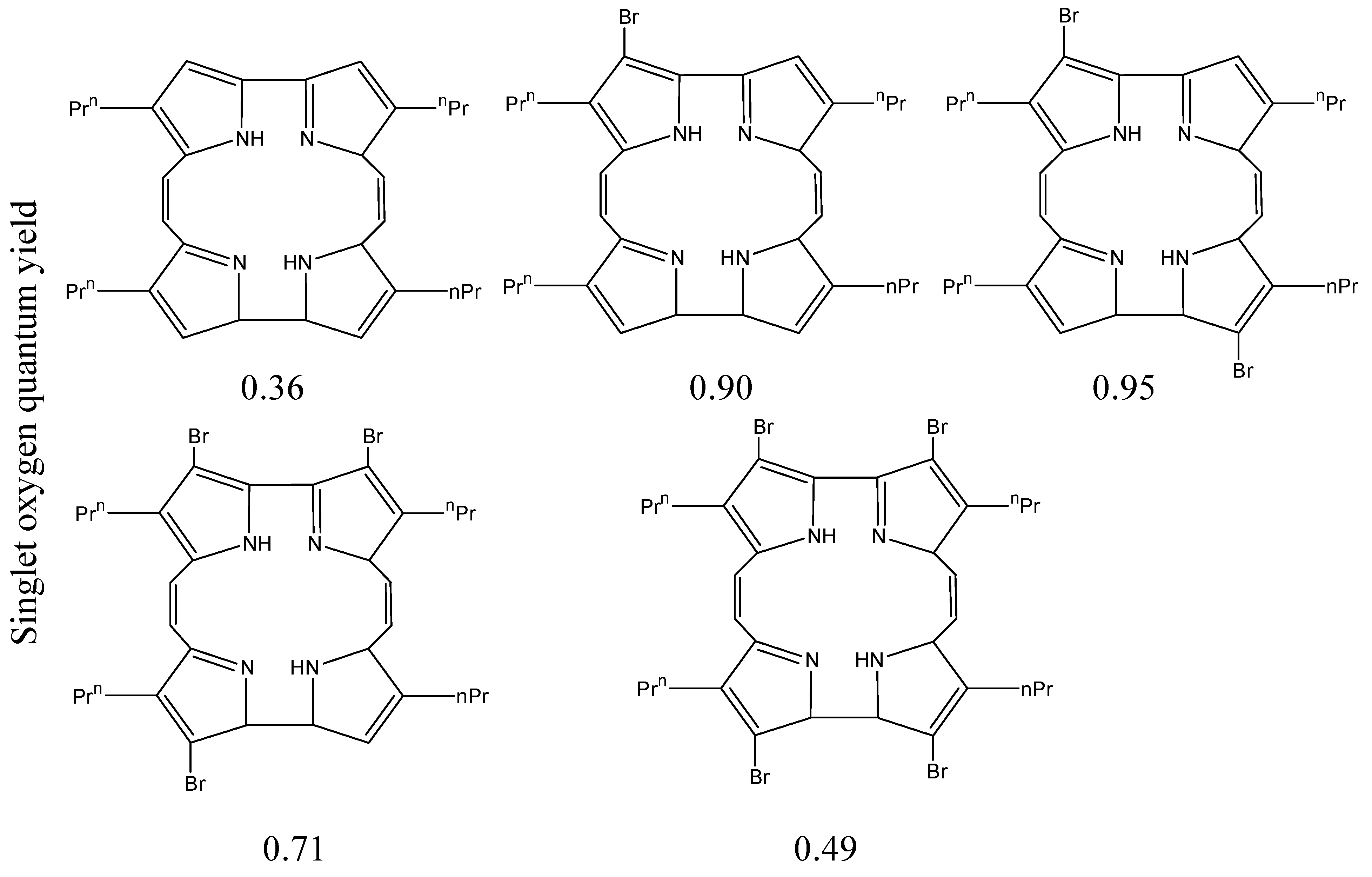
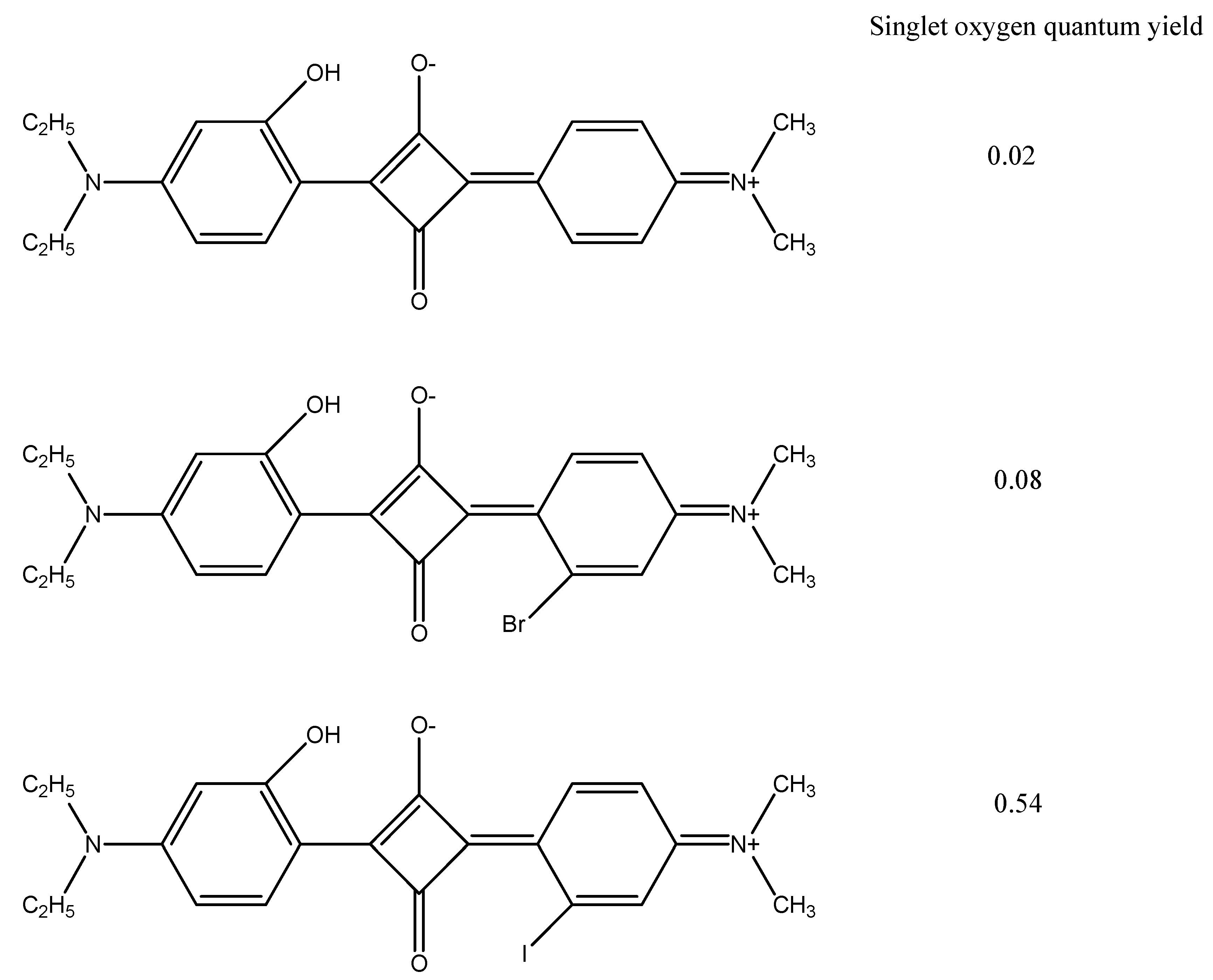
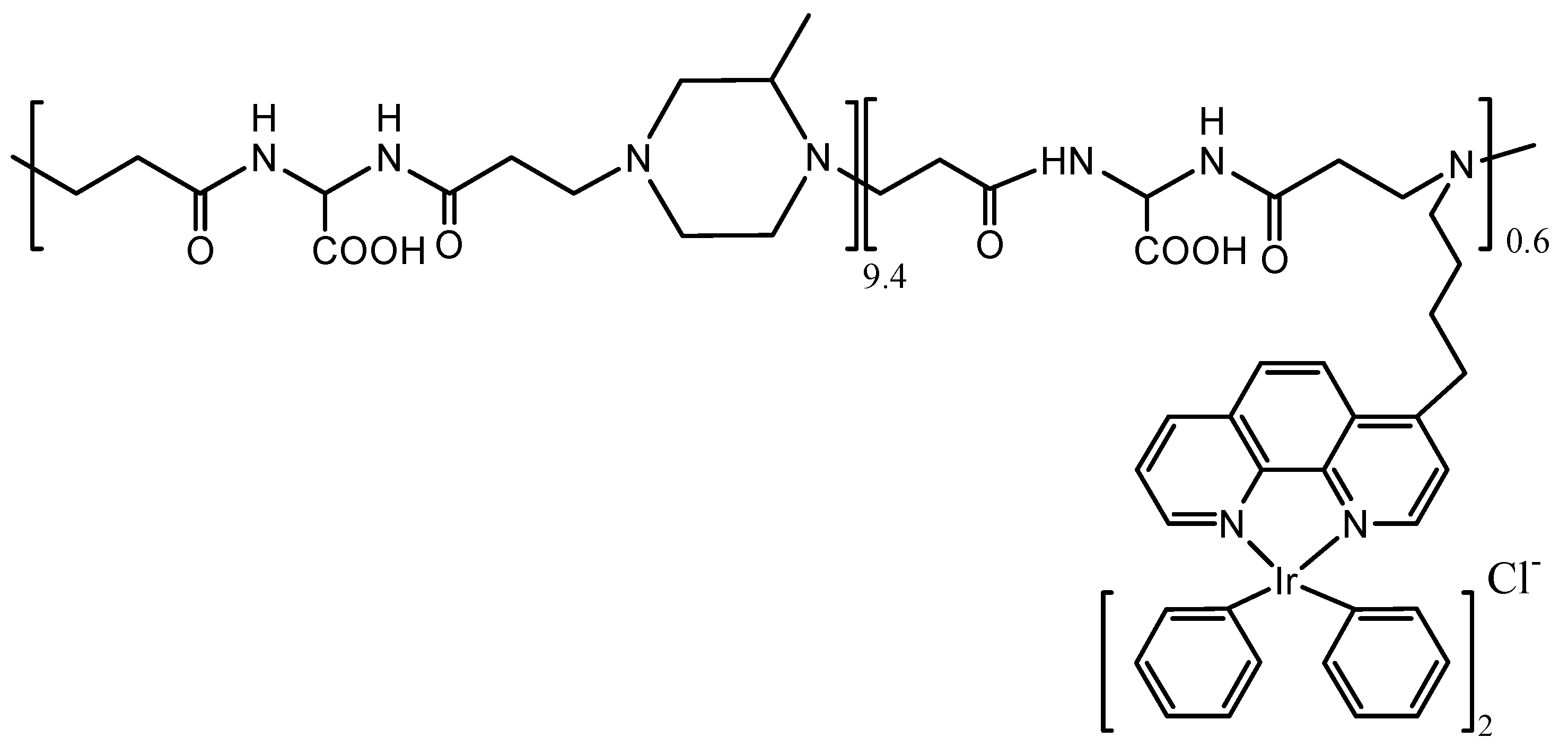
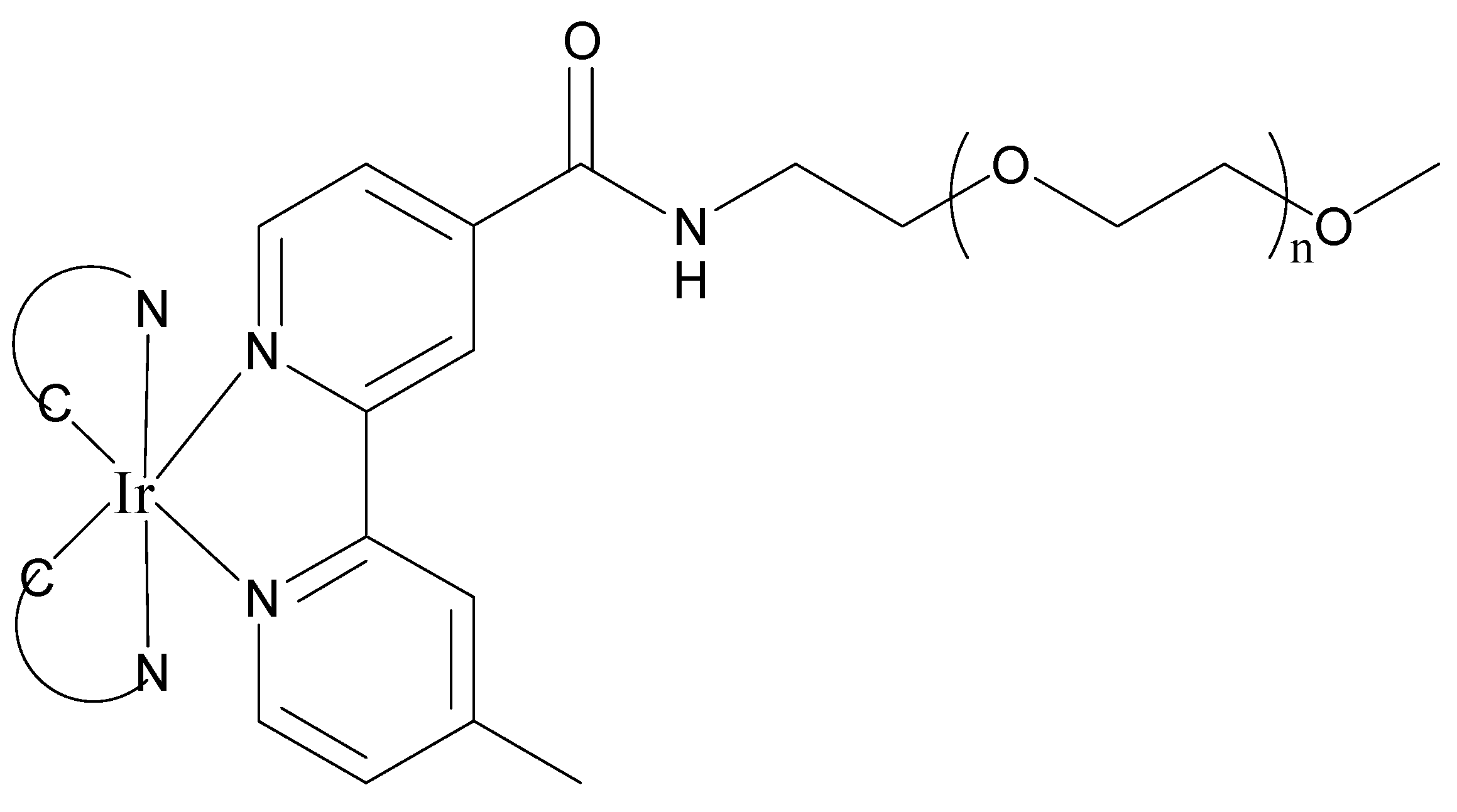
3.3. Two Photon Systems

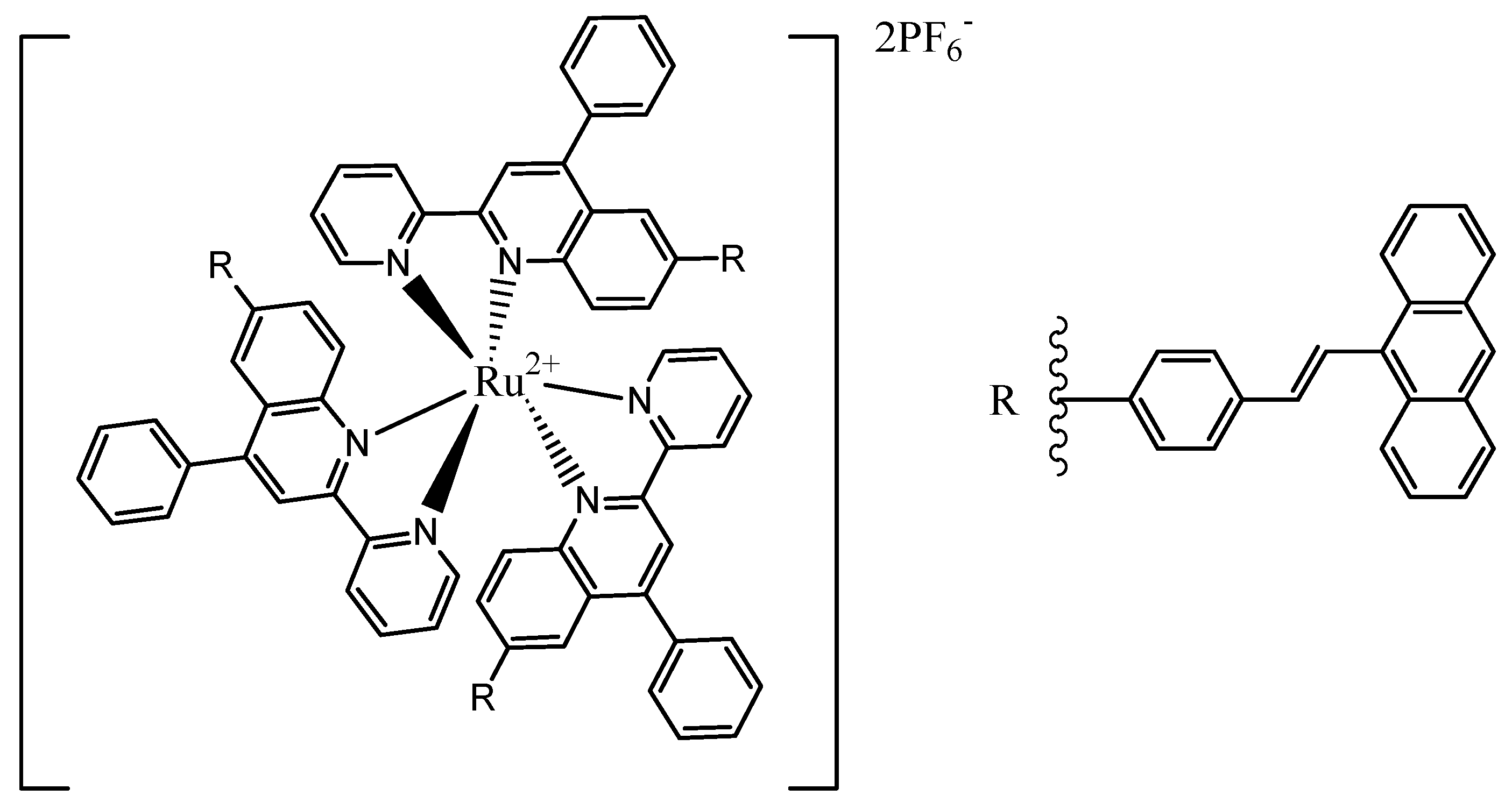
3.4. Triplet PSs
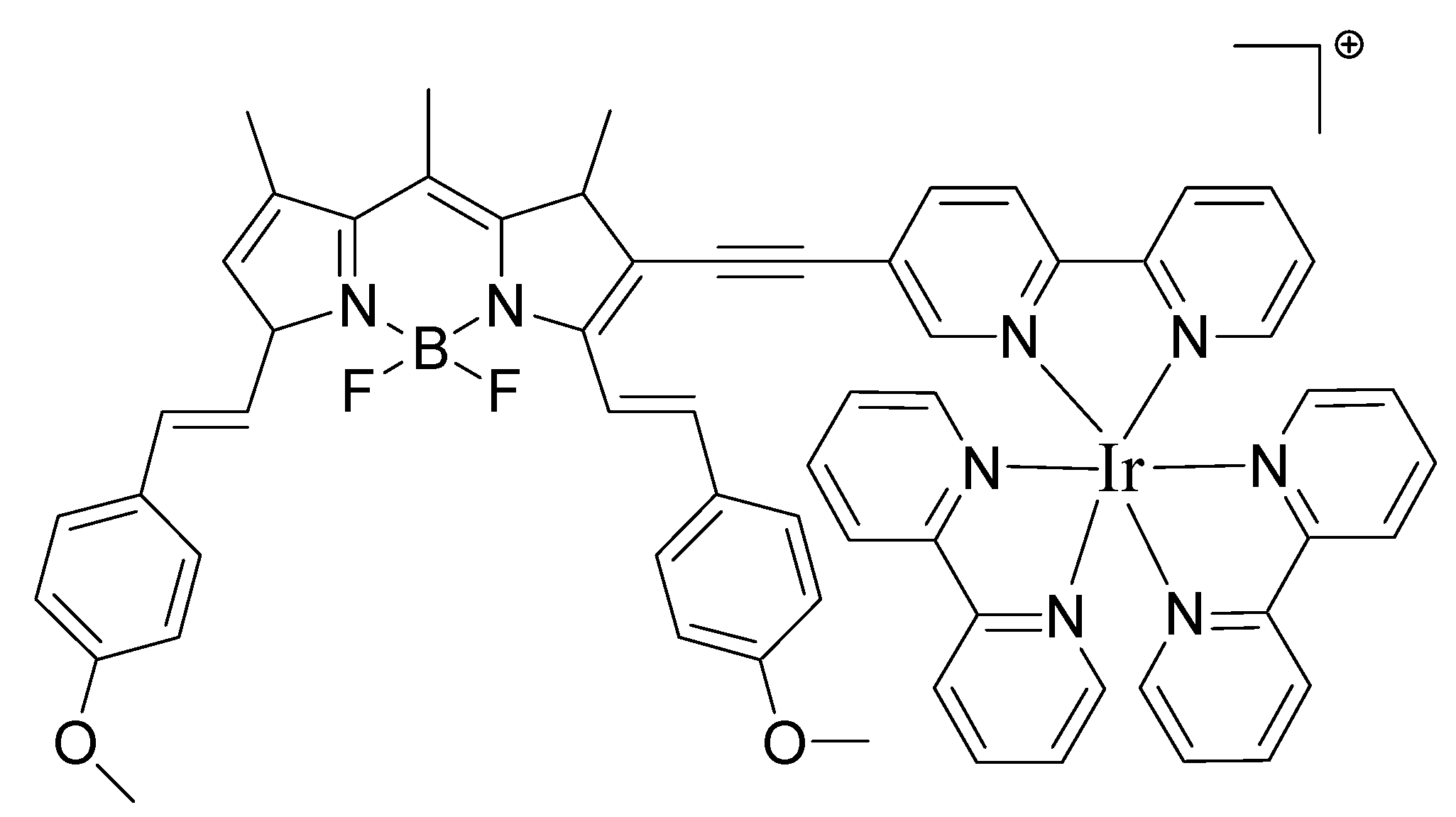
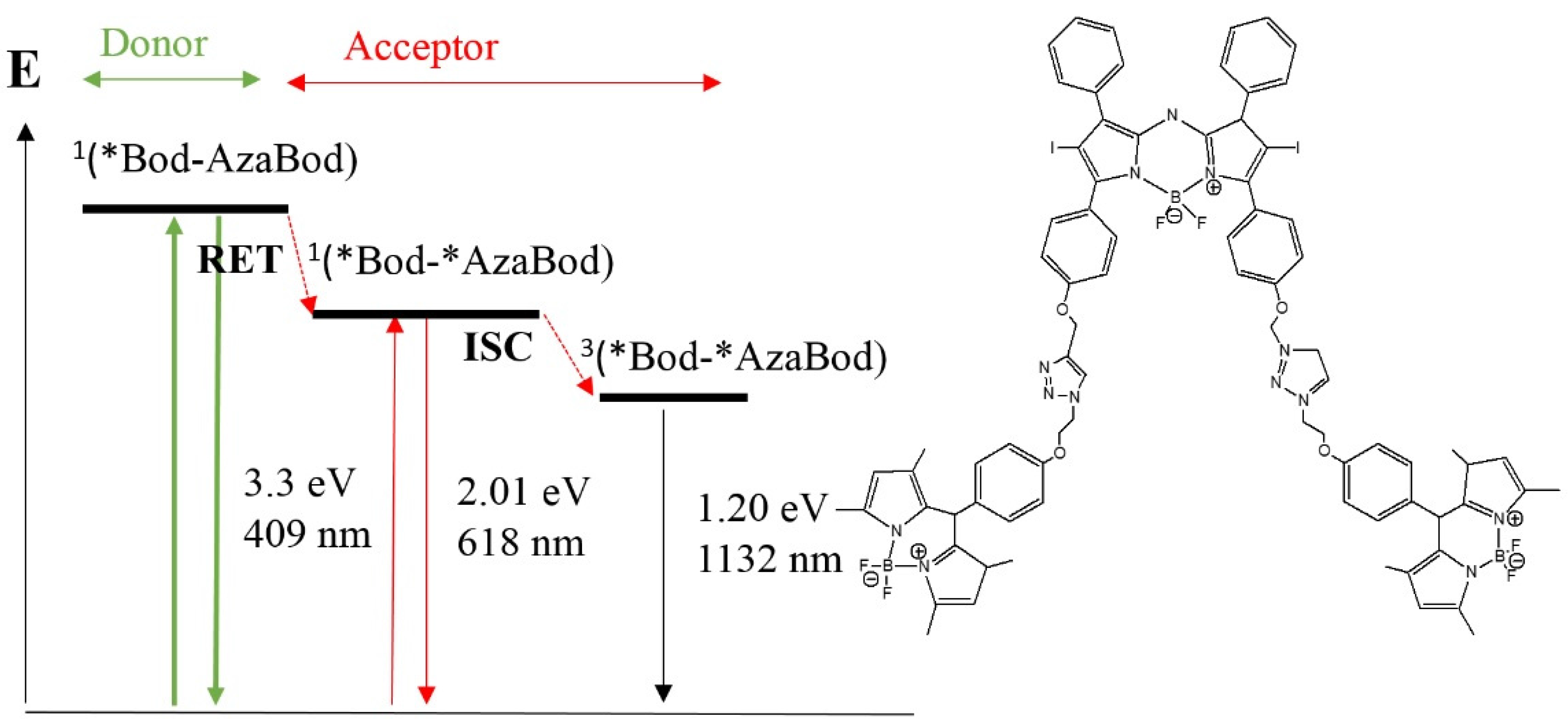
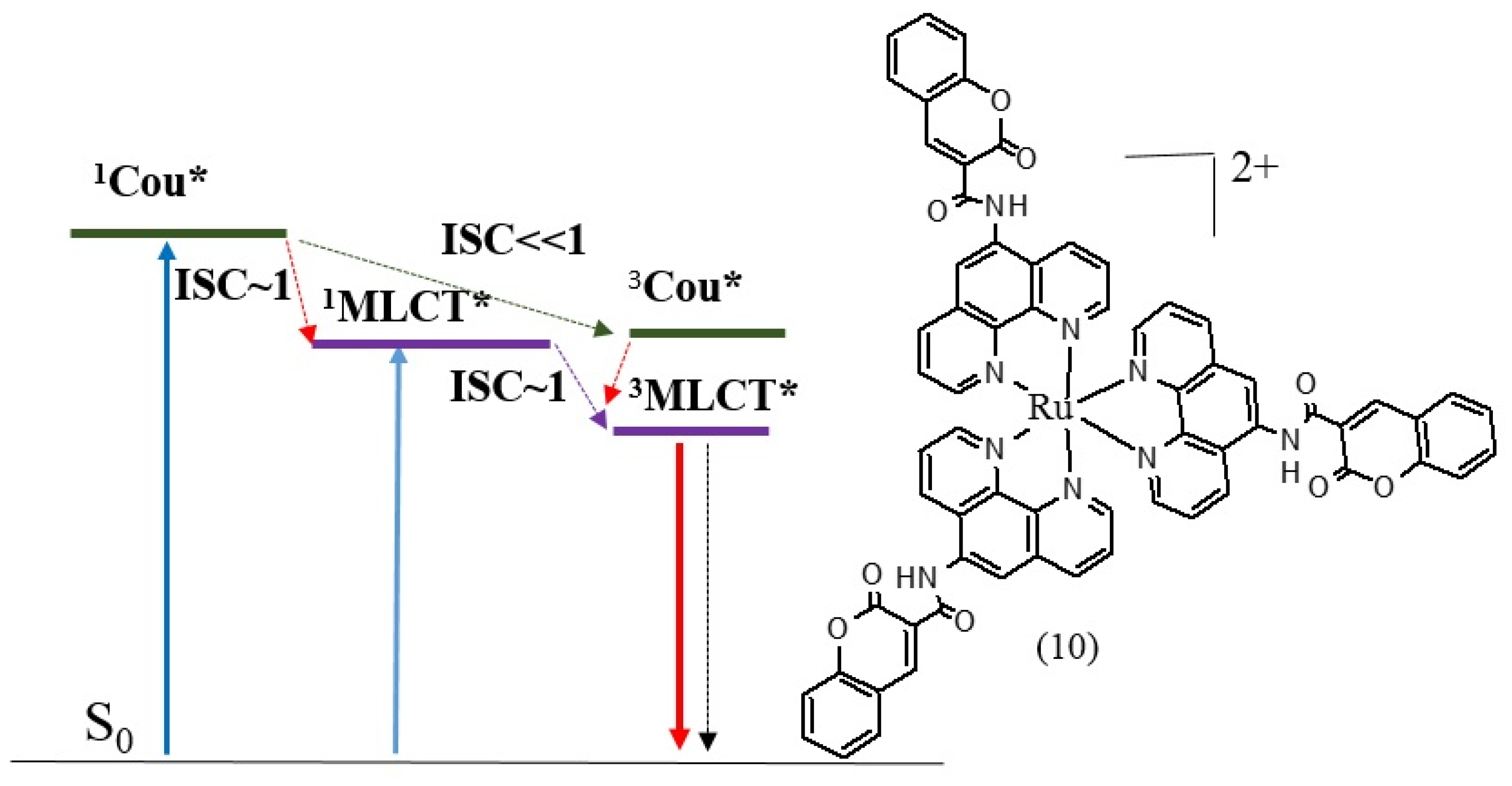
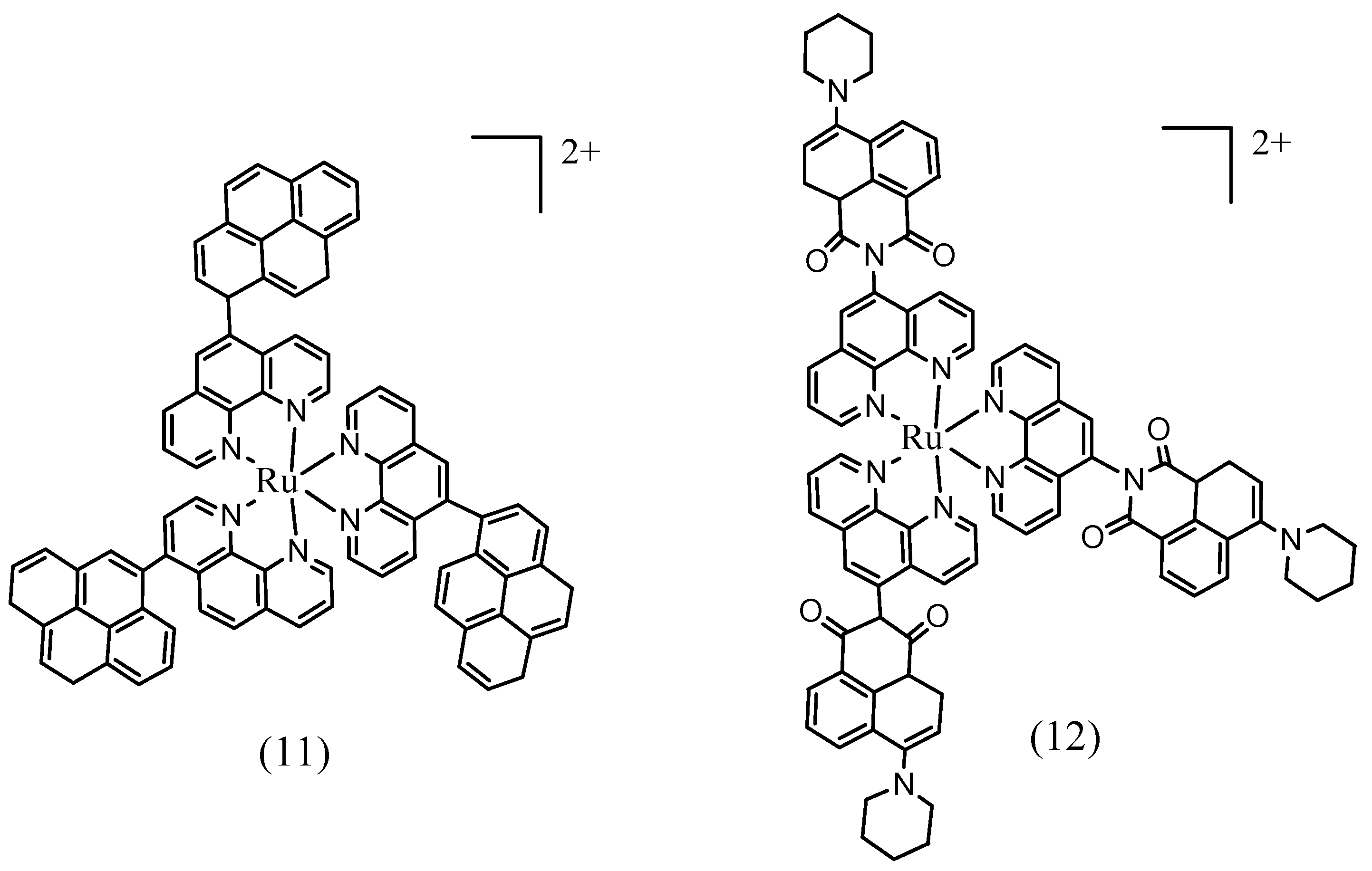
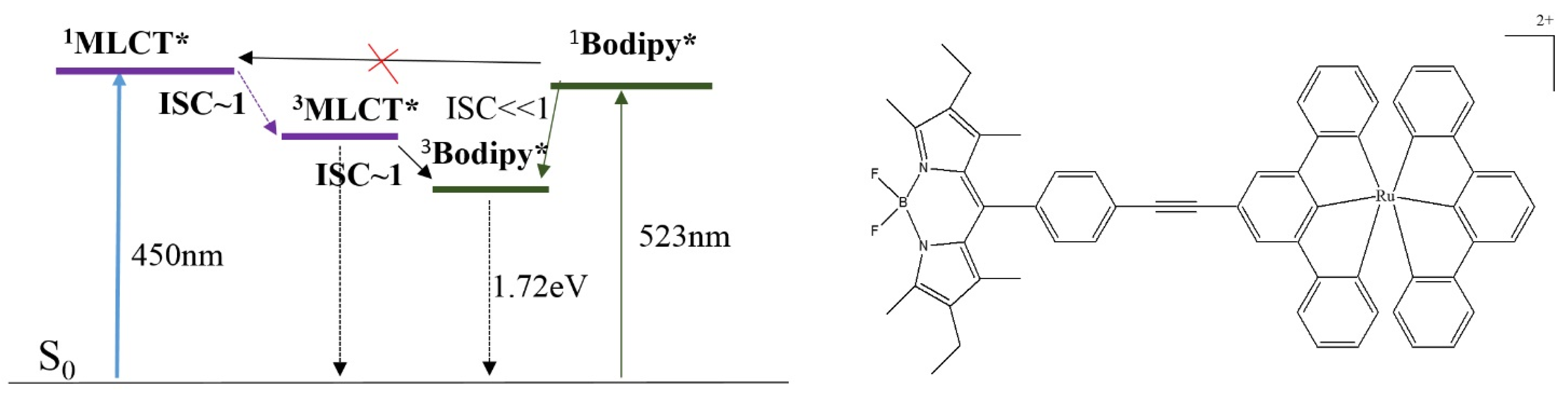
4. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Dougherty, T.J.; Gomer, C.J.; Henderson, B.W.; Jori, G.; Kessel, D.; Korbelik, M.; Moan, J.; Peng, Q. Photodynamic therapy. J. Natl. Cancer Inst. 1998, 90, 889–905. [Google Scholar] [CrossRef] [PubMed]
- Wainwright, M. Non-porphyrin photosensitizers in biomedicine. Chem. Soc. Rev. 1996, 25, 351–359. [Google Scholar] [CrossRef]
- Yoon, I.; Li, J.Z.; Shim, Y.K. Advance in photosensitizers and light delivery for photodynamic therapy. Clin. Endosc. 2013, 46, 7–23. [Google Scholar] [CrossRef] [PubMed]
- Ormond, A.B.; Freeman, H.S. Dye sensitizers for photodynamic therapy. Materials 2013, 6, 817–840. [Google Scholar] [CrossRef]
- Wainwright, M. Photodynamic therapy–from dyestuffs to high–tech clinical practice. Rev. Prog. Colorat. Relat. Top. 2004, 34, 95–109. [Google Scholar] [CrossRef]
- De Melo, L.S.; Gomes, A.S.; Saska, S.; Nigoghossian, K.; Messaddeq, Y.; Ribeiro, S.J.; de Araujo, R.E. Singlet oxygen generation enhanced by silver-pectin nanoparticles. J. Fluoresc. 2012, 22, 1633–1638. [Google Scholar] [CrossRef] [PubMed]
- Zhu, T.C.; Finlay, J.C. The role of photodynamic therapy (PDT) physics. Med. Phys. 2008, 35, 3127–3136. [Google Scholar] [CrossRef] [PubMed]
- Kamkaew, A.; Lim, S.H.; Lee, H.B.; Kiew, L.V.; Chung, L.Y.; Burgess, K. BODIPY dyes in photodynamic therapy. Chem. Soc. Rev. 2013, 42, 77–88. [Google Scholar] [CrossRef] [PubMed]
- Avirah, R.R.; Jayaram, D.T.; Adarsh, N.; Ramaiah, D. Squaraine dyes in PDT: From basic design to in vivo demonstration. Org. Biomol. Chem. 2012, 10, 911–920. [Google Scholar] [CrossRef] [PubMed]
- Dąbrowski, J.M.; Urbanska, K.; Arnaut, L.G.; Pereira, M.M.; Abreu, A.R.; Simões, S.; Stochel, G. Biodistribution and Photodynamic Efficacy of a Water-Soluble, Stable, Halogenated Bacteriochlorin against Melanoma. ChemMedChem 2011, 6, 465–475. [Google Scholar] [CrossRef] [PubMed]
- Maggioni, D.; Galli, M.; D’Alfonso, L.; Inverso, D.; Dozzi, M.V.; Sironi, L.; Iannacone, M.; Collini, M.; Ferruti, P.; Ranucci, E. A Luminescent Poly (amidoamine)–Iridium Complex as a New Singlet-Oxygen Sensitizer for Photodynamic Therapy. Inorg. Chem. 2015, 54, 544–553. [Google Scholar] [CrossRef] [PubMed]
- Ogilby, P.R. Singlet oxygen: There is indeed something new under the sun. Chem. Soc. Rev. 2010, 39, 3181–3209. [Google Scholar] [CrossRef] [PubMed]
- Sharpless, C.M.; Blough, N.V. The importance of charge-transfer interactions in determining chromophoric dissolved organic matter (CDOM) optical and photochemical properties. Environ. Sci. 2014, 16, 654–671. [Google Scholar] [CrossRef] [PubMed]
- Salice, P.; Arnbjerg, J.; Pedersen, B.W.; Toftegaard, R.; Beverina, L.; Pagani, G.A.; Ogilby, P.R. Photophysics of squaraine dyes: Role of charge-transfer in singlet oxygen production and removal. J. Physics. Chem. A 2010, 114, 2518–2525. [Google Scholar] [CrossRef] [PubMed]
- Weyergang, A.; Berg, K.; Kaalhus, O.; Peng, Q.; Selbo, P.K. Photodynamic therapy targets the mTOR signaling network in vitro and in vivo. Mol. Pharm. 2008, 6, 255–264. [Google Scholar] [CrossRef] [PubMed]
- Agostinis, P.; Berg, K.; Cengel, K.A.; Foster, T.H.; Girotti, A.W.; Gollnick, S.O.; Hahn, S.M.; Hamblin, M.R.; Juzeniene, A.; Kessel, D. Photodynamic therapy of cancer: An update. CA Cancer J. Clin. 2011, 61, 250–281. [Google Scholar] [CrossRef] [PubMed]
- Da Silva, E.F.; Pedersen, B.W.; Breitenbach, T.; Toftegaard, R.; Kuimova, M.K.; Arnaut, L.G.; Ogilby, P.R. Irradiation-and sensitizer-dependent changes in the lifetime of intracellular singlet oxygen produced in a photosensitized process. J. Phys. Chem. B 2011, 116, 445–461. [Google Scholar] [CrossRef] [PubMed]
- Wilkinson, F.; Helman, W.P.; Ross, A.B. Rate constants for the decay and reactions of the lowest electronically excited singlet state of molecular oxygen in solution. An expanded and revised compilation. J. Phys. Chem. Ref. Data 1995, 24, 663–677. [Google Scholar] [CrossRef]
- Schweitzer, C.; Schmidt, R. Physical mechanisms of generation and deactivation of singlet oxygen. Chem. Rev. 2003, 103, 1685–1758. [Google Scholar] [CrossRef] [PubMed]
- Robertson, C.; Evans, D.H.; Abrahamse, H. Photodynamic therapy (PDT): A short review on cellular mechanisms and cancer research applications for PDT. J. Photochem. Photobiol. B Biol. 2009, 96, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Wei, M.; Chen, M.; Chen, K.; Lou, P.; Lin, S.Y.; Hung, S.; Hsiao, M.; Yao, C.; Shieh, M. Autophagy promotes resistance to photodynamic therapy-induced apoptosis selectively in colorectal cancer stem-like cells. Autophagy 2014, 10, 1179–1192. [Google Scholar] [CrossRef] [PubMed]
- Dewaele, M.; Maes, H.; Agostinis, P. ROS-mediated mechanisms of Autophagy stimulation and their relevance in cancer therapy. Autophagy 2010, 6, 838–854. [Google Scholar] [CrossRef] [PubMed]
- Xu, J.; Gattacceca, F.; Amiji, M. Biodistribution and Pharmacokinetics of EGFR-Targeted Thiolated Gelatin Nanoparticles Following Systemic Administration in Pancreatic Tumor-Bearing Mice. Mol. Pharm. 2013, 10, 2031–2044. [Google Scholar] [CrossRef] [PubMed]
- Castano, A.P.; Demidova, T.N.; Hamblin, M.R. Mechanisms in photodynamic therapy: Part three—photosensitizer pharmacokinetics, biodistribution, tumor localization and modes of tumor destruction. Photodiagnosis Photodyn. Ther. 2005, 2, 91–106. [Google Scholar] [CrossRef]
- Dumoulin, F. Design and Conception of Photosensitisers. In Photosensitizers in Medicine, Environment, and Security; Springer: Dordrecht, The Netherlands; Heidelberg, Germany; London, UK, New York, NY, USA, 2012. [Google Scholar]
- Silva, E.F.; Serpa, C.; Dąbrowski, J.M.; Monteiro, C.J.; Formosinho, S.J.; Stochel, G.; Urbanska, K.; Simões, S.; Pereira, M.M.; Arnaut, L.G. Mechanisms of Singlet-Oxygen and Superoxide-Ion Generation by Porphyrins and Bacteriochlorins and their Implications in Photodynamic Therapy. Chem. A Eur. J. 2010, 16, 9273–9286. [Google Scholar] [CrossRef] [PubMed]
- Castano, A.P.; Demidova, T.N.; Hamblin, M.R. Mechanisms in photodynamic therapy: Part one—photosensitizers, photochemistry and cellular localization. Photodiagnosis Photodyn. Ther. 2004, 1, 279–293. [Google Scholar] [CrossRef]
- Rubio, N.; Fleury, S.P.; Redmond, R.W. Spatial and temporal dynamics of in vitro photodynamic cell killing: Extracellular hydrogen peroxide mediates neighbouring cell death. Photochem. Photobiol. Sci. 2009, 8, 457–464. [Google Scholar] [CrossRef] [PubMed]
- Kessel, D.; Reiners, J.J. Promotion of Proapoptotic Signals by Lysosomal Photodamage. Photochem. Photobiol. 2015. [Google Scholar] [CrossRef] [PubMed]
- Rajaputra, P.; Nkepang, G.; Watley, R.; You, Y. Synthesis and in vitro biological evaluation of lipophilic cation conjugated photosensitizers for targeting mitochondria. Bioorg. Med. Chem. 2013, 21, 379–387. [Google Scholar] [CrossRef] [PubMed]
- Balaji, B.; Balakrishnan, B.; Perumalla, S.; Karande, A.A.; Chakravarty, A.R. Mitochondria-Targeting Photocytotoxic Ferrocenyl Conjugates of N-Alkylpyridinium Salts. Eur. J. Inorg. Chem. 2015, 2015, 1398–1407. [Google Scholar] [CrossRef]
- Odeh, A.M.; Craik, J.D.; Ezzeddine, R.; Tovmasyan, A.; Batinic-Haberle, I.; Benov, L.T. Targeting mitochondria by Zn (II) N-Alkylpyridylporphyrins: The impact of Compound sub-mitochondrial partition on cell respiration and overall photodynamic efficacy. PLoS ONE 2014, 9, e108238. [Google Scholar] [CrossRef] [PubMed]
- Rancan, F.; Wiehe, A.; Nöbel, M.; Senge, M.O.; Omari, S.A.; Böhm, F.; John, M.; Röder, B. Influence of substitutions on asymmetric dihydroxychlorins with regard to intracellular uptake, subcellular localization and photosensitization of Jurkat cells. J. Photochem. Photobiolo. B Biol. 2005, 78, 17–28. [Google Scholar] [CrossRef] [PubMed]
- Reiners, J.J.; Agostinis, P.; Berg, K.; Oleinick, N.L.; Kessel, D.H. Assessing Autophagy in the context of photodynamic therapy. Autophagy 2010, 6, 7–18. [Google Scholar] [CrossRef] [PubMed]
- Liu, L.; Zhang, Z.; Xing, D. Cell death via mitochondrial apoptotic pathway due to activation of Bax by lysosomal photodamage. Free Radic. Biol. Med. 2011, 51, 53–68. [Google Scholar] [CrossRef] [PubMed]
- Xie, H.; Svenmarker, P.; Axelsson, J.; Gräfe, S.; Kyriazi, M.; Bendsoe, N.; Andersson Engels, S.; Svanberg, K. Pharmacokinetic and biodistribution study following systemic administration of Fospeg®—A Pegylated liposomal mTHPC formulation in a murine model. J. Biophotonics. 2015, 8, 142–152. [Google Scholar] [CrossRef] [PubMed]
- Pandey, R.K. Recent advances in photodynamic therapy. J. Porphyrins Phthalocyanines 2000, 4, 368–373. [Google Scholar] [CrossRef]
- Pavani, C.; Uchoa, A.F.; Oliveira, C.S.; Iamamoto, Y.; Baptista, M.S. Effect of zinc insertion and hydrophobicity on the membrane interactions and PDT activity of porphyrin photosensitizers. Photochem. Photobiol. Sci. 2009, 8, 233–240. [Google Scholar] [CrossRef] [PubMed]
- Zhang, X.; Xu, H. Influence of halogenation and aggregation on photosensitizing properties of zinc phthalocyanine (ZnPC). J. Chem. Soc. Faraday Trans. 1993, 89, 3347–3351. [Google Scholar] [CrossRef]
- Sakamoto, K.; Kato, T.; Kawaguchi, T.; Ohno-Okumura, E.; Urano, T.; Yamaoka, T.; Suzuki, S.; Cook, M.J. Photosensitizer efficacy of non-peripheral substituted alkylbenzopyridoporphyrazines for photodynamic therapy of cancer. J. Photochem. Photobiol. A 2002, 153, 245–253. [Google Scholar] [CrossRef]
- Baek, S.; Na, K. A nano complex of hydrophilic phthalocyanine and polyethylenimine for improved cellular internalization efficiency and phototoxicity. Colloids Surf. B Biointerfaces 2013, 101, 493–500. [Google Scholar] [CrossRef] [PubMed]
- Lee, Y.; Cho, H.; Choi, M.; Park, H.; Bang, J.; Lee, S.; Kwon, I.C.; Kim, S. Directed molecular assembly into a biocompatible photosensitizing nanocomplex for locoregional photodynamic therapy. J. Control Release 2015, 209, 12–19. [Google Scholar] [CrossRef] [PubMed]
- Çakır, D.; Göksel, M.; Çakır, V.; Durmus, M.; Biyiklioglu, Z.; Kantekin, H. Amphiphilic Zinc Phthalocyanine Photosensitizers: Synthesis, Photophysicochemical Properties and in vitro Studies for Photodynamic Therapy. Dalton Trans. 2015. [Google Scholar] [CrossRef]
- Jin, Y.; Zhang, X.; Zhang, B.; Kang, H.; Du, L.; Li, M. Nanostructures of an amphiphilic zinc phthalocyanine polymer conjugate for photodynamic therapy of psoriasis. Colloids Surf. B Biointerfaces 2015, 128, 405–409. [Google Scholar] [CrossRef] [PubMed]
- Doshi, M.; Krienke, M.; Khederzadeh, S.; Sanchez, H.; Copik, A.; Oyer, J.; Gesquiere, A.J. Conducting Polymer Nanoparticles for Targeted Cancer Therapy. RSC Adv. 2015, 5, 37943–37956. [Google Scholar] [CrossRef]
- Lo, P.C.; Huang, J.D.; Cheng, D.Y.Y.; Chan, E.Y.M.; Fong, W.P.; Ko, W.H.; Ng, D.K.P. New amphiphilic silicon (IV) phthalocyanines as efficient photosensitizers for photodynamic therapy: Synthesis, photophysical properties, and in vitro photodynamic activities. Chem. A Eur. J. 2004, 10, 4831–4838. [Google Scholar] [CrossRef] [PubMed]
- Theodossiou, T.A.; Gonçalves, A.R.; Yannakopoulou, K.; Skarpen, E.; Berg, K. Photochemical Internalization of Tamoxifens Transported by a “Trojan-Horse” Nanoconjugate into Breast-Cancer Cell Lines. Angew. Chem. Int. Ed. 2015, 54, 4885–4889. [Google Scholar] [CrossRef] [PubMed]
- Moromizato, S.; Hisamatsu, Y.; Suzuki, T.; Matsuo, Y.; Abe, R.; Aoki, S. Design and synthesis of a luminescent cyclometalated iridium (III) complex having N, N-diethylamino group that stains acidic intracellular organelles and induces cell death by photoirradiation. Inorg. Chem. 2012, 51, 12697–12706. [Google Scholar] [CrossRef] [PubMed]
- Nakagawa, A.; Hisamatsu, Y.; Moromizato, S.; Kohno, M.; Aoki, S. Synthesis and Photochemical Properties of pH Responsive Tris-Cyclometalated Iridium (III) Complexes That Contain a Pyridine Ring on the 2-Phenylpyridine Ligand. Inorg. Chem. 2013, 53, 409–422. [Google Scholar] [CrossRef] [PubMed]
- Huang, P.; Xu, C.; Lin, J.; Wang, C.; Wang, X.; Zhang, C.; Zhou, X.; Guo, S.; Cui, D. Folic Acid-conjugated Graphene Oxide loaded with Photosensitizers for Targeting Photodynamic Therapy. Theranostics 2011, 1, 240–250. [Google Scholar] [CrossRef] [PubMed]
- Schneider, R.; Schmitt, F.; Frochot, C.; Fort, Y.; Lourette, N.; Guillemin, F.; Müller, J.; Barberi-Heyob, M. Design, synthesis, and biological evaluation of folic acid targeted tetraphenylporphyrin as novel photosensitizers for selective photodynamic therapy. Bioorg. Med. Chem. 2005, 13, 2799–2808. [Google Scholar] [CrossRef] [PubMed]
- Van Dongen, G.A.M.S.; Visser, G.W.M.; Vrouenraets, M.B. Photosensitizer-antibody conjugates for detection and therapy of cancer. Adv. Drug Deliv. Rev. 2004, 56, 31–52. [Google Scholar] [CrossRef] [PubMed]
- Josefsen, L.; Boyle, R. Photodynamic therapy: Novel third-generation photosensitizers one step closer? Br. J. Pharmacol. 2008, 154, 1–3. [Google Scholar] [CrossRef] [PubMed]
- Wöhrle, D.; Hirth, A.; Bogdahn-Rai, T.; Schnurpfeil, G.; Shopova, M. Photodynamic therapy of cancer: Second and third generations of photosensitizers. Russ. Chem. Bull. 1998, 47, 807–816. [Google Scholar] [CrossRef]
- Van Nostrum, C.F. Polymeric micelles to deliver photosensitizers for photodynamic therapy. Adv. Drug Deliv. Rev. 2004, 56, 9–16. [Google Scholar] [CrossRef] [PubMed]
- Komeda, C.; Ikeda, A.; Kikuchi, J.; Ishida-Kitagawa, N.; Tatebe, H.; Shiozaki, K.; Akiyama, M. A photo-triggerable drug carrier based on cleavage of PEG lipids by photosensitiser-generated reactive singlet oxygen. Org. Biomol. Chem. 2013, 11, 2567–2570. [Google Scholar] [CrossRef] [PubMed]
- Bovis, M.J.; Woodhams, J.H.; Loizidou, M.; Scheglmann, D.; Bown, S.G.; MacRobert, A.J. Improved in vivo delivery of m-THPC via pegylated liposomes for use in photodynamic therapy. J. Control Release 2012, 157, 196–205. [Google Scholar] [CrossRef] [PubMed]
- Choi, Y.; Kim, S.; Choi, M.; Ryoo, S.; Park, J.; Min, D.; Kim, B. Highly Biocompatible Carbon Nanodots for Simultaneous Bioimaging and Targeted Photodynamic Therapy in Vitro and in Vivo. Adv. Funct. Mater. 2014, 24, 5781–5789. [Google Scholar] [CrossRef]
- Castagnos, P.; Siqueira-Moura, M.; Goto, P.L.; Perez, E.; Franceschi, S.; Rico-Lattes, I.; Tedesco, A.; Blanzat, M. Catanionic vesicles charged with chloroaluminium phthalocyanine for topical photodynamic therapy. In vitro phototoxicity towards human carcinoma and melanoma cell lines. RSC Adv. 2014, 4, 39372–39377. [Google Scholar]
- Wang, N.; Zhao, Z.; Lv, Y.; Fan, H.; Bai, H.; Meng, H.; Long, Y.; Fu, T.; Zhang, X.; Tan, W. Gold nanorod-photosensitizer conjugate with extracellular pH-driven tumor targeting ability for photothermal/photodynamic therapy. Nano Res. 2014, 7, 1291–1301. [Google Scholar]
- Cheng, Y.; Doane, T.L.; Chuang, C.; Ziady, A.; Burda, C. Near Infrared Light-Triggered Drug Generation and Release from Gold Nanoparticle Carriers for Photodynamic Therapy. Small 2014, 10, 1799–1804. [Google Scholar] [CrossRef] [PubMed]
- Fraix, A.; Gref, R.; Sortino, S. A multi-photoresponsive supramolecular hydrogel with dual-color fluorescence and dual-modal photodynamic action. J. Mater. Chem. B 2014, 2, 3443–3449. [Google Scholar] [CrossRef]
- Kesharwani, P.; Jain, K.; Jain, N.K. Dendrimer as nanocarrier for drug delivery. Prog. Polym. Sci. 2014, 39, 268–307. [Google Scholar] [CrossRef]
- Yin, M.; Ju, E.; Chen, Z.; Li, Z.; Ren, J.; Qu, X. Upconverting Nanoparticles with a Mesoporous TiO2 Shell for Near-Infrared-Triggered Drug Delivery and Synergistic Targeted Cancer Therapy. Chem. A Eur. J. 2014, 20, 14012–14017. [Google Scholar] [CrossRef] [PubMed]
- García Vior, M.C.; Marino, J.; Roguin, L.P.; Sosnik, A.; Awruch, J. Photodynamic Effects of Zinc (II) Phthalocyanine-Loaded Polymeric Micelles in Human Nasopharynx KB Carcinoma Cells. Photochem. Photobiol. 2013, 89, 492–500. [Google Scholar] [CrossRef] [PubMed]
- Chen, Y.; Lo, C.; Hsiue, G. Multifunctional nanomicellar systems for delivering anticancer drugs. J. Biomed. Mate Res. Part A 2014, 102, 2024–2038. [Google Scholar] [CrossRef] [PubMed]
- Kataoka, K.; Harada, A.; Nagasaki, Y. Block copolymer micelles for drug delivery: Design, characterization and biological significance. Adv. Drug Deliv. Rev. 2001, 47, 113–131. [Google Scholar] [CrossRef]
- Peng, C.; Shieh, M.; Tsai, M.; Chang, C.; Lai, P. Self-assembled star-shaped chlorin-core poly(ɛ-caprolactone)–poly(ethylene glycol) diblock copolymer micelles for dual chemo-photodynamic therapies. Biomaterials 2008, 29, 3599–3608. [Google Scholar] [CrossRef] [PubMed]
- Wu, D.; Li, Z.; Li, C.; Fan, J.; Lu, B.; Chang, C.; Cheng, S.; Zhang, X.; Zhuo, R. Porphyrin and galactosyl conjugated micelles for targeting photodynamic therapy. Pharm. Res. 2010, 27, 187–199. [Google Scholar] [CrossRef] [PubMed]
- Knop, K.; Mingotaud, A.; El-Akra, N.; Violleau, F.; Souchard, J. Monomeric pheophorbide (a)-containing poly (ethyleneglycol-b-ε-caprolactone) micelles for photodynamic therapy. Photochem. Photobiol. Sci. 2009, 8, 396–404. [Google Scholar] [CrossRef] [PubMed]
- Synatschke, C.V.; Nomoto, T.; Cabral, H.; Förtsch, M.; Toh, K.; Matsumoto, Y.; Miyazaki, K.; Hanisch, A.; Schacher, F.H.; Kishimura, A. Multicompartment Micelles with Adjustable Poly (ethylene glycol) Shell for Efficient in Vivo Photodynamic Therapy. ACS Nano 2014, 8, 1161–1172. [Google Scholar] [CrossRef] [PubMed]
- Ma, D.; Liu, Z.; Zheng, Q.; Zhou, X.; Zhang, Y.; Shi, Y.; Lin, J.; Xue, W. Star-Shaped Polymer Consisting of a Porphyrin Core and Poly (l-lysine) Dendron Arms: Synthesis, Drug Delivery, and In Vitro Chemo/Photodynamic Therapy. Macromol. Rapid Commun. 2013, 34, 548–552. [Google Scholar] [CrossRef] [PubMed]
- Lee, S.U.; Min, K.H.; Jeong, S.Y.; Bae, H.; Lee, S.C. Calcium phosphate-reinforced photosensitizer-loaded polymer nanoparticles for photodynamic therapy. Chem. Asian J. 2013, 8, 3222–3229. [Google Scholar] [CrossRef] [PubMed]
- Li, S.P.; Lau, C.T.; Louie, M.; Lam, Y.; Cheng, S.H.; Lo, K.K. Mitochondria-targeting cyclometalated iridium (III)–PEG complexes with tunable photodynamic activity. Biomaterials 2013, 34, 7519–7532. [Google Scholar] [CrossRef] [PubMed]
- Verma, S.; Watt, G.M.; Mai, Z.; Hasan, T. Strategies for Enhanced Photodynamic Therapy Effects. Photochem. Photobiol. 2007, 83, 996–1005. [Google Scholar] [CrossRef] [PubMed]
- Master, A.; Malamas, A.; Solanki, R.; Clausen, D.M.; Eiseman, J.L.; Sen Gupta, A. A cell-targeted photodynamic nanomedicine strategy for head and neck cancers. Mol. Pharm. 2013, 10, 1988–1997. [Google Scholar] [CrossRef] [PubMed]
- Peng, C.; Lai, P.; Lin, F.; Yueh-Hsiu Wu, S.; Shieh, M. Dual chemotherapy and photodynamic therapy in an HT-29 human colon cancer xenograft model using SN-38-loaded chlorin-core star block copolymer micelles. Biomaterials 2009, 30, 3614–3625. [Google Scholar] [CrossRef] [PubMed]
- Koo, H.; Lee, H.; Lee, S.; Min, K.H.; Kim, M.S.; Lee, D.S.; Choi, Y.; Kwon, I.C.; Kim, K.; Jeong, S.Y. In vivo tumor diagnosis and photodynamic therapy via tumoral pH-responsive polymeric micelles. Chem. Commun. 2010, 46, 5668–5670. [Google Scholar] [CrossRef] [PubMed]
- Lau, J.T.; Lo, P.; Jiang, X.; Wang, Q.; Ng, D.K. A Dual Activatable Photosensitizer toward Targeted Photodynamic Therapy. J. Med. Chem. 2014, 57, 4088–4097. [Google Scholar] [CrossRef] [PubMed]
- Liang, J.; Wu, W.; Xu, X.; Zhuo, R.; Zhang, X. pH Responsive micelle self-assembled from a new amphiphilic peptide as anti-tumor drug carrier. Colloids Surf. B Biointerfaces 2014, 114, 398–403. [Google Scholar] [CrossRef] [PubMed]
- Master, A.M.; Qi, Y.; Oleinick, N.L.; Gupta, A.S. EGFR-mediated intracellular delivery of Pc 4 nanoformulation for targeted photodynamic therapy of cancer: In vitro studies. Nanomedicine 2012, 8, 655–664. [Google Scholar] [CrossRef] [PubMed]
- Li, L.; Cho, H.; Yoon, K.H.; Kang, H.C.; Huh, K.M. Antioxidant-photosensitizer dual-loaded polymeric micelles with controllable production of reactive oxygen species. Int. J. Pharm. 2014, 471, 339–348. [Google Scholar] [CrossRef] [PubMed]
- Hofman, J.; Carstens, M.G.; van Zeeland, F.; Helwig, C.; Flesch, F.M.; Hennink, W.E.; Van Nostrum, C.F. Photocytotoxicity of mTHPC (temoporfin) loaded polymeric micelles mediated by lipase catalyzed degradation. Pharm. Res. 2008, 25, 2065–2073. [Google Scholar] [CrossRef] [PubMed]
- Chen, J.; Wang, H.; Li, C.; Han, K.; Zhang, X.; Zhuo, R. Construction of surfactant-like tetra-tail amphiphilic peptide with RGD ligand for encapsulation of porphyrin for photodynamic therapy. Biomaterials 2011, 32, 1678–1684. [Google Scholar] [CrossRef] [PubMed]
- Ding, H.; Sumer, B.D.; Kessinger, C.W.; Dong, Y.; Huang, G.; Boothman, D.A.; Gao, J. Nanoscopic micelle delivery improves the photophysical properties and efficacy of photodynamic therapy of protoporphyrin IX. J. Control Release 2011, 151, 271–277. [Google Scholar] [CrossRef] [PubMed]
- Yuan, A.; Yang, B.; Wu, J.; Hu, Y.; Ming, X. Dendritic nanoconjugates of photosensitizer for targeted photodynamic therapy. Acta Biomate. 2015, 21, 63–73. [Google Scholar] [CrossRef] [PubMed]
- Dong, H.; Li, Y.; Wen, H.; Xu, M.; Liu, L.; Li, Z.; Guo, F.; Shi, D. Highly Efficient Drug Delivery Nanosystem via l-Phenylalanine Triggering Based on Supramolecular Polymer Micelles. Macromol. Rapid Commun. 2011, 32, 540–545. [Google Scholar] [CrossRef] [PubMed]
- Mojzisova, H.; Bonneau, S.; Vever-Bizet, C.; Brault, D. The pH-dependent distribution of the photosensitizer chlorin e6 among plasma proteins and membranes: A physico-chemical approach. Biochim. Biophys. Acta 2007, 1768, 366–374. [Google Scholar] [CrossRef] [PubMed]
- Chong, K.; Ku, T.; Saw, P.E.; Jon, S.; Park, J.; Choi, C. Enhancement of the photocytotoxic efficiency of sub-12 nm therapeutic polymeric micelles with increased co-localisation in mitochondria. Chem. Commun. 2013, 49, 11476–11478. [Google Scholar] [CrossRef] [PubMed]
- Nishiyama, N.; Nakagishi, Y.; Morimoto, Y.; Lai, P.; Miyazaki, K.; Urano, K.; Horie, S.; Kumagai, M.; Fukushima, S.; Cheng, Y. Enhanced photodynamic cancer treatment by supramolecular nanocarriers charged with dendrimer phthalocyanine. J. Control Release 2009, 133, 245–251. [Google Scholar] [CrossRef] [PubMed]
- Master, A.M.; Livingston, M.; Oleinick, N.L.; Sen Gupta, A. Optimization of a nanomedicine-based silicon Phthalocyanine 4 Photodynamic Therapy (Pc 4-PDT) strategy for targeted treatment of EGFR-overexpressing cancers. Mol. Pharm. 2012, 9, 2331–2338. [Google Scholar] [CrossRef] [PubMed]
- Syu, W.; Yu, H.; Hsu, C.; Rajan, Y.C.; Hsu, Y.; Chang, Y.; Hsieh, W.; Wang, C.; Lai, P. Improved Photodynamic Cancer Treatment by Folate-Conjugated Polymeric Micelles in a KB Xenografted Animal Model. Small 2012, 8, 2060–2069. [Google Scholar] [CrossRef] [PubMed]
- Gong, H.; Dong, Z.; Liu, Y.; Yin, S.; Cheng, L.; Xi, W.; Xiang, J.; Liu, K.; Li, Y.; Liu, Z. Engineering of Multifunctional Nano-Micelles for Combined Photothermal and Photodynamic Therapy under the Guidance of Multimodal Imaging. Adv. Funct. Mater. 2014, 24, 6492–6502. [Google Scholar] [CrossRef]
- Lee, U.Y.; Oh, Y.T.; Kim, D.; Lee, E.S. Multimeric grain-marked micelles for highly efficient photodynamic therapy and magnetic resonance imaging of tumors. Int. J. Pharm. 2014, 471, 166–172. [Google Scholar] [CrossRef] [PubMed]
- Pellosi, D.S.; Estevão, B.M.; Freitas, C.F.; Tsubone, T.M.; Caetano, W.; Hioka, N. Photophysical properties of erythrosin ester derivatives in ionic and non-ionic micelles. Dyes Pigm. 2013, 99, 705–712. [Google Scholar] [CrossRef]
- Chen, K.; Yu, M.; Zhang, H.; Ma, D.; Pang, S.; Huang, W.; Peng, Y. In polyion complex micelles incorporating poly (aryl benzyl ether) dendritic phthalocyanine: Effective photosensitizers for enhanced photodynamic therapy. Proc. SPIE 2012. [Google Scholar] [CrossRef]
- Gibot, L.; Lemelle, A.; Till, U.; Moukarzel, B.; Mingotaud, A.; Pimienta, V.; Saint-Aguet, P.; Rols, M.; Gaucher, M.; Violleau, F. Polymeric micelles encapsulating photosensitizer: Structure/photodynamic therapy efficiency relation. Biomacromolecules 2014, 15, 1443–1455. [Google Scholar] [CrossRef] [PubMed]
- Shao, W.; Wang, H.; He, S.; Shi, L.; Peng, K.; Lin, Y.; Zhang, L.; Ji, L.; Liu, H. Photophysical properties and singlet oxygen generation of three sets of halogenated corroles. J. Phys. Chem. B 2012, 116, 14228–14234. [Google Scholar] [CrossRef] [PubMed]
- Lo, P.; Wang, S.; Zeug, A.; Meyer, M.; Röder, B.; Ng, D.K.P. Preparation and photophysical properties of halogenated silicon(IV) phthalocyanines substituted axially with poly(ethylene glycol) chains. Tetrahedron Lett. 2003, 44, 1967–1970. [Google Scholar] [CrossRef]
- Tanielian, C.; Wolff, C. Determination of the parameters controlling singlet oxygen production via oxygen and heavy-atom enhancement of triplet yields. J. Phys. Chem. 1995, 99, 9831–9837. [Google Scholar] [CrossRef]
- De Melo, J.; Rondão, R.; Burrows, H.D.; Melo, M.J.; Navaratnam, S.; Edge, R.; Voss, G. Spectral and photophysical studies of substituted indigo derivatives in their keto forms. ChemPhysChem. 2006, 7, 2303–2311. [Google Scholar] [CrossRef] [PubMed]
- Gaboury, L.; Giasson, R.; Gupta, A.K.; Li, T.; Villeneuve, L. WO1996007431 A1, 14 March 1996.
- Araki, K.; Engelmann, F.M.; Mayer, I.; Toma, H.E.; Baptista, M.S.; Maeda, H.; Osuka, A.; Furuta, H. Doubly N-Confused Porphyrins as Efficient Sensitizers for Singlet Oxygen Generation. Chem. Lett. 2003, 32, 244–245. [Google Scholar] [CrossRef]
- Obata, M.; Hirohara, S.; Tanaka, R.; Kinoshita, I.; Ohkubo, K.; Fukuzumi, S.; Tanihara, M.; Yano, S. In vitro heavy-atom effect of palladium (II) and platinum (II) complexes of pyrrolidine-fused chlorin in photodynamic therapy. J. Med. Chem. 2009, 52, 2747–2753. [Google Scholar] [CrossRef] [PubMed]
- Weitman, H.; Shatz, S.; Ehrenberg, B. Complexation of Mg-tetrabenzoporphyrin with pyridine enhances singlet oxygen generation and affects its partitioning into apolar microenvironments. J. Photochem. Photobiol. A 2009, 203, 7–12. [Google Scholar] [CrossRef]
- Marydasan, B.; Nair, A.K.; Ramaiah, D. Optimization of Triplet Excited State and Singlet Oxygen Quantum Yields of Picolylamine–Porphyrin Conjugates through Zinc Insertion. J. Phys. Chem. B 2013, 117, 13515–13522. [Google Scholar] [CrossRef] [PubMed]
- Peceli, D.; Hu, H.; Fishman, D.A.; Webster, S.; Przhonska, O.V.; Kurdyukov, V.V.; Slominsky, Y.L.; Tolmachev, A.I.; Kachkovski, A.D.; Gerasov, A.O. Enhanced Intersystem Crossing Rate in Polymethine-Like Molecules: Sulfur-Containing Squaraines versus Oxygen-Containing Analogues. J. Physics. Chem. A 2013, 117, 2333–2346. [Google Scholar] [CrossRef] [PubMed]
- Webster, S.; Peceli, D.; Hu, H.; Padilha, L.A.; Przhonska, O.V.; Masunov, A.E.; Gerasov, A.O.; Kachkovski, A.D.; Slominsky, Y.L.; Tolmachev, A.I. Near-unity quantum yields for intersystem crossing and singlet oxygen generation in polymethine-like molecules: Design and experimental realization. J. Phys. Chem. Lett. 2010, 1, 2354–2360. [Google Scholar] [CrossRef]
- Sagun, E.; Zenkevich, E.; Knyukshto, V.; Panarin, A.Y.; Semeikin, A.; Lyubimova, T. Relaxation processes with participation of excited S 1 and T 1 states of spatially distorted meso-phenyl-substituted octamethylporphyrins. Opt. Spectrosc. 2012, 113, 388–400. [Google Scholar] [CrossRef]
- Röder, B.; Büchner, M.; Rückmann, I.; Senge, M.O. Correlation of photophysical parameters with macrocycle distortion in porphyrins with graded degree of saddle distortion. Photochem. Photobiol. Sci. 2010, 9, 1152–1158. [Google Scholar] [CrossRef] [PubMed]
- Shimakoshi, H.; Baba, T.; Iseki, Y.; Aritome, I.; Endo, A.; Adachi, C.; Hisaeda, Y. Photophysical and photosensitizing properties of brominated porphycenes. Chem. Commun. 2008, 2008, 2882–2884. [Google Scholar] [CrossRef] [PubMed]
- Luo, C.; Zhou, Q.; Jiang, G.; He, L.; Zhang, B.; Wang, X. The synthesis and 1O2 photosensitization of halogenated asymmetric aniline-based squaraines. New J. Chem. 2011, 35, 1128–1132. [Google Scholar] [CrossRef]
- Zhou, L.; Wei, S.; Ge, X.; Zhou, J.; Yu, B.; Shen, J. External heavy-atomic construction of photosensitizer nanoparticles for enhanced in vitro photodynamic therapy of cancer. J. Phys. Chem. B 2012, 116, 12744–12749. [Google Scholar] [CrossRef] [PubMed]
- Maeda, D.; Shimakoshi, H.; Abe, M.; Hisaeda, Y. Syntheses and photophysical behavior of porphyrin isomer Sn (IV) complexes. Inorg. Chem. 2009, 48, 9853–9860. [Google Scholar] [CrossRef] [PubMed]
- Kim, O.; Lee, K.; Woo, H.Y.; Kim, K.; He, G.S.; Swiatkiewicz, J.; Prasad, P.N. New class of two-photon-absorbing chromophores based on dithienothiophene. Chem. Mater. 2000, 12, 284–286. [Google Scholar]
- Das, S.; Nag, A.; Goswami, D.; Bharadwaj, P.K. Zinc (II)-and copper (I)-mediated large two-photon absorption cross sections in a bis-cinnamaldiminato Schiff base. J. Am. Chem. Soc. 2006, 128, 402–403. [Google Scholar] [CrossRef] [PubMed]
- Oar, M.A.; Dichtel, W.R.; Serin, J.M.; Fréchet, J.M.; Rogers, J.E.; Slagle, J.E.; Fleitz, P.A.; Tan, L.; Ohulchanskyy, T.Y.; Prasad, P.N. Light-harvesting chromophores with metalated porphyrin cores for tuned photosensitization of singlet oxygen via two-photon excited FRET. Chem. Mater. 2006, 18, 3682–3692. [Google Scholar] [CrossRef]
- Luo, T.; Wilson, B.C.; Lu, Q. Evaluation of one- and two-photon activated photodynamic therapy with pyropheophorbide-a methyl ester in human cervical, lung and ovarian cancer cells. J. Photochem. Photobiol. B Biol. 2014, 132, 102–110. [Google Scholar] [CrossRef] [PubMed]
- Pefkianakis, E.K.; Christodouleas, D.; Giokas, D.L.; Papadopoulos, K.; Vougioukalakis, G.C. A Family of RuII Photosensitizers with High Singlet Oxygen Quantum Yield: Synthesis, Characterization, and Evaluation. Eur. J. Inorg. Chem. 2013, 2013, 4628–4635. [Google Scholar] [CrossRef]
- Zhao, J.; Wu, W.; Sun, J.; Guo, S. Triplet photosensitizers: From molecular design to applications. Chem. Soc. Rev. 2013, 42, 5323–5351. [Google Scholar] [CrossRef] [PubMed]
- Zhao, Q.; Liu, S.; Shi, M.; Li, F.; Jing, H.; Yi, T.; Huang, C. Tuning photophysical and electrochemical properties of cationic iridium (III) complex salts with imidazolyl substituents by proton and anions. Organometallics 2007, 26, 5922–5930. [Google Scholar] [CrossRef]
- Majumdar, P.; Yuan, X.; Li, S.; Le Guennic, B.; Ma, J.; Zhang, C.; Jacquemin, D.; Zhao, J. Cyclometalated Ir (III) complexes with styryl-BODIPY ligands showing near IR absorption/emission: Preparation, study of photophysical properties and application as photodynamic/luminescence imaging materials. J. Mater. Chem. B 2014, 2, 2838–2854. [Google Scholar] [CrossRef]
- Guo, S.; Ma, L.; Zhao, J.; Küçüköz, B.; Karatay, A.; Hayvali, M.; Yaglioglu, H.G.; Elmali, A. BODIPY triads triplet photosensitizers enhanced with intramolecular resonance energy transfer (RET): Broadband visible light absorption and application in photooxidation. Chem. Sci. 2014, 5, 489–500. [Google Scholar] [CrossRef]
- Armaroli, N. Electronic Excited-State Engineering. ChemPhysChem 2008, 9, 371–373. [Google Scholar] [CrossRef] [PubMed]
- Tyson, D.S.; Luman, C.R.; Zhou, X.; Castellano, F.N. New Ru (II) chromophores with extended excited-state lifetimes. Inorg. Chem. 2001, 40, 4063–4071. [Google Scholar] [CrossRef] [PubMed]
- Vachova, L.; Novakova, V.; Kopecky, K.; Miletin, M.; Zimcik, P. Effect of intramolecular charge transfer on fluorescence and singlet oxygen production of phthalocyanine analogues. Dalton Trans. 2012, 41, 11651–11656. [Google Scholar] [CrossRef] [PubMed]
- Abdel-Shafi, A.A.; Hassanin, H.A.; Al-Shihry, S.S. Partial charge transfer contribution to the solvent isotope effect and photosensitized generation of singlet oxygen, O2 (1Δg), by substituted ruthenium (II) bipyridyl complexes in aqueous media. Photochem. Photobiol. Sci. 2014, 13, 1330–1337. [Google Scholar] [CrossRef] [PubMed]
© 2015 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mehraban, N.; Freeman, H.S. Developments in PDT Sensitizers for Increased Selectivity and Singlet Oxygen Production. Materials 2015, 8, 4421-4456. https://doi.org/10.3390/ma8074421
Mehraban N, Freeman HS. Developments in PDT Sensitizers for Increased Selectivity and Singlet Oxygen Production. Materials. 2015; 8(7):4421-4456. https://doi.org/10.3390/ma8074421
Chicago/Turabian StyleMehraban, Nahid, and Harold S. Freeman. 2015. "Developments in PDT Sensitizers for Increased Selectivity and Singlet Oxygen Production" Materials 8, no. 7: 4421-4456. https://doi.org/10.3390/ma8074421
APA StyleMehraban, N., & Freeman, H. S. (2015). Developments in PDT Sensitizers for Increased Selectivity and Singlet Oxygen Production. Materials, 8(7), 4421-4456. https://doi.org/10.3390/ma8074421






