Enhanced Hydrophilicity and Biocompatibility of Dental Zirconia Ceramics by Oxygen Plasma Treatment
Abstract
:1. Introduction
2. Results and Discussion
2.1. Morphology
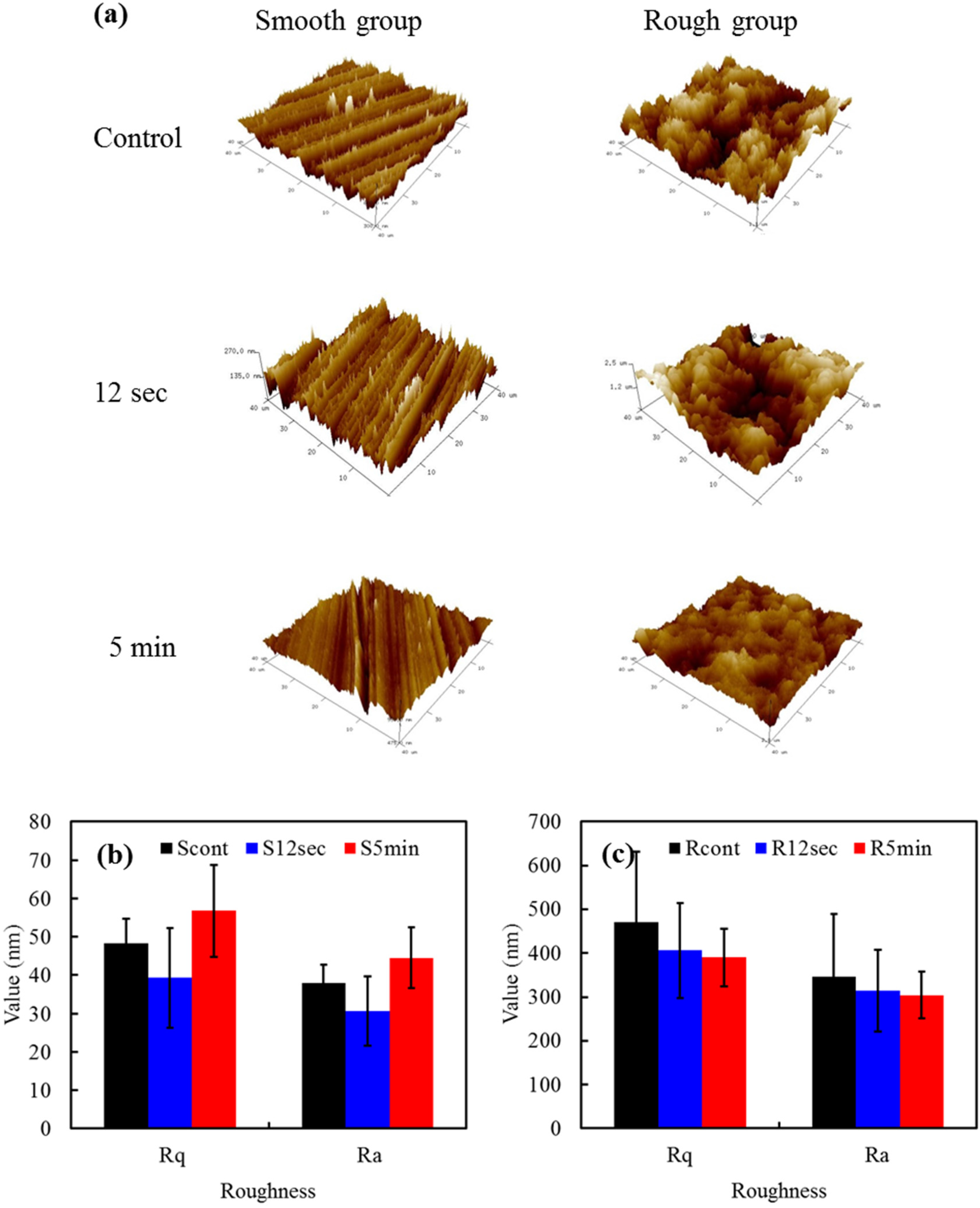
2.2. Phase Composition
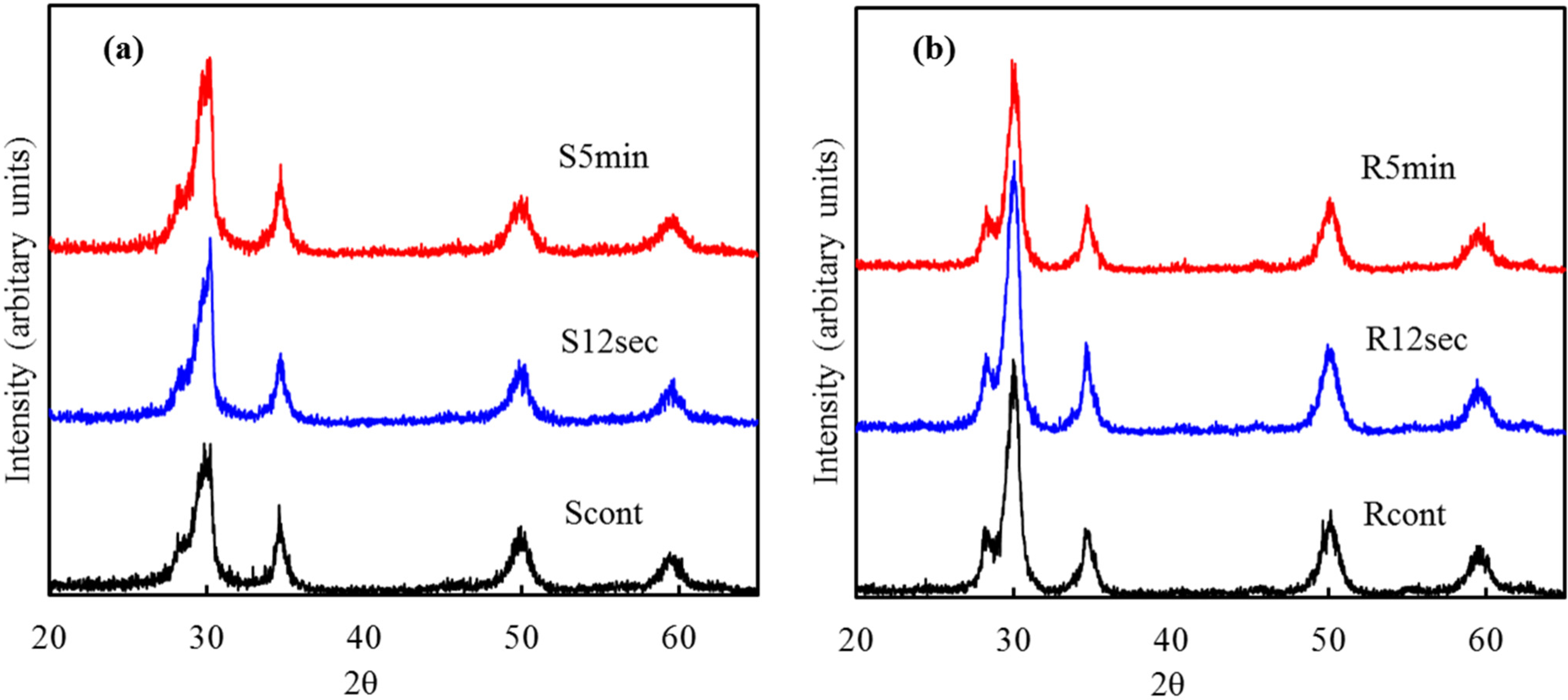
2.3. XPS Analysis
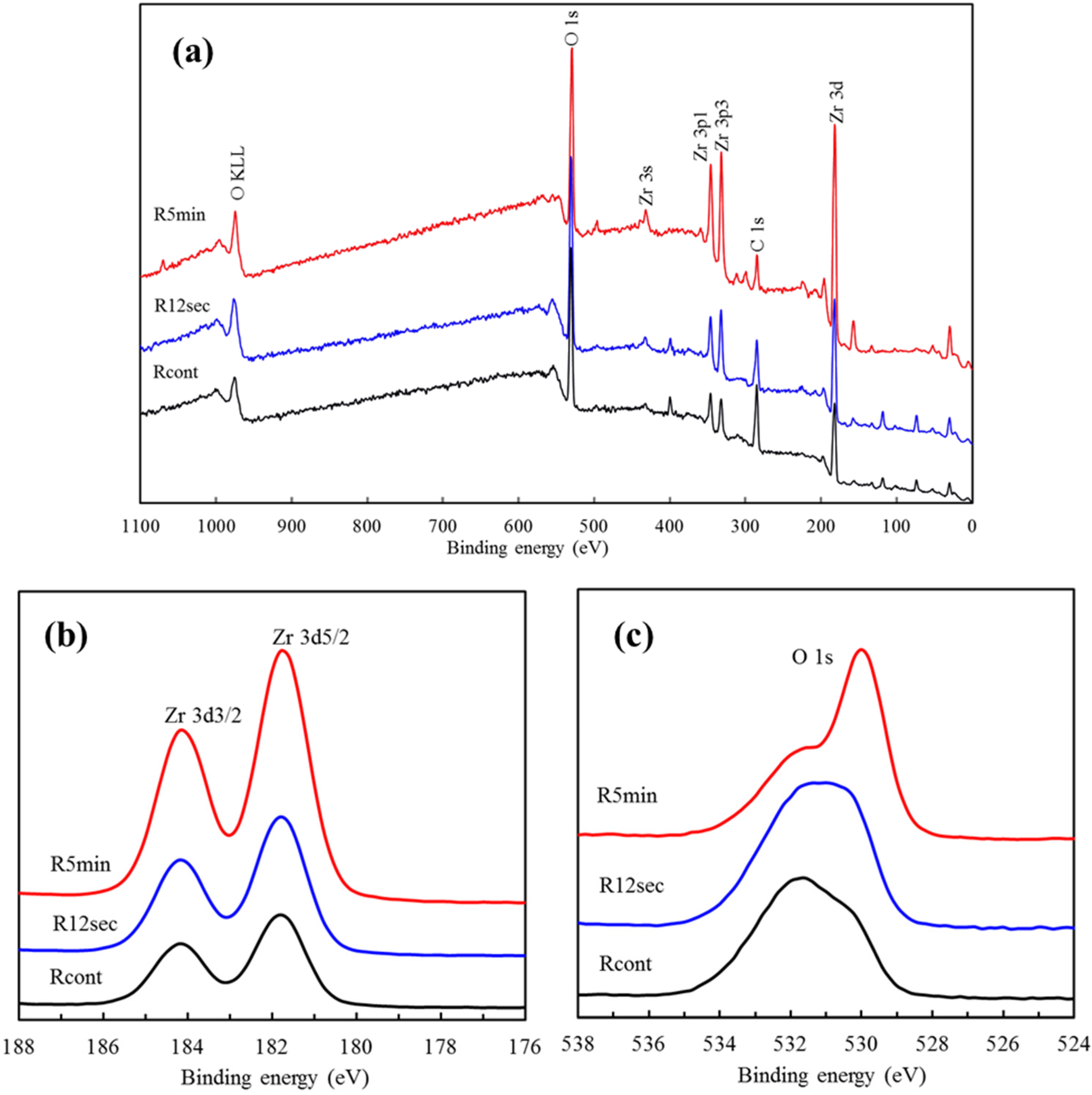
2.4. Contact Angle
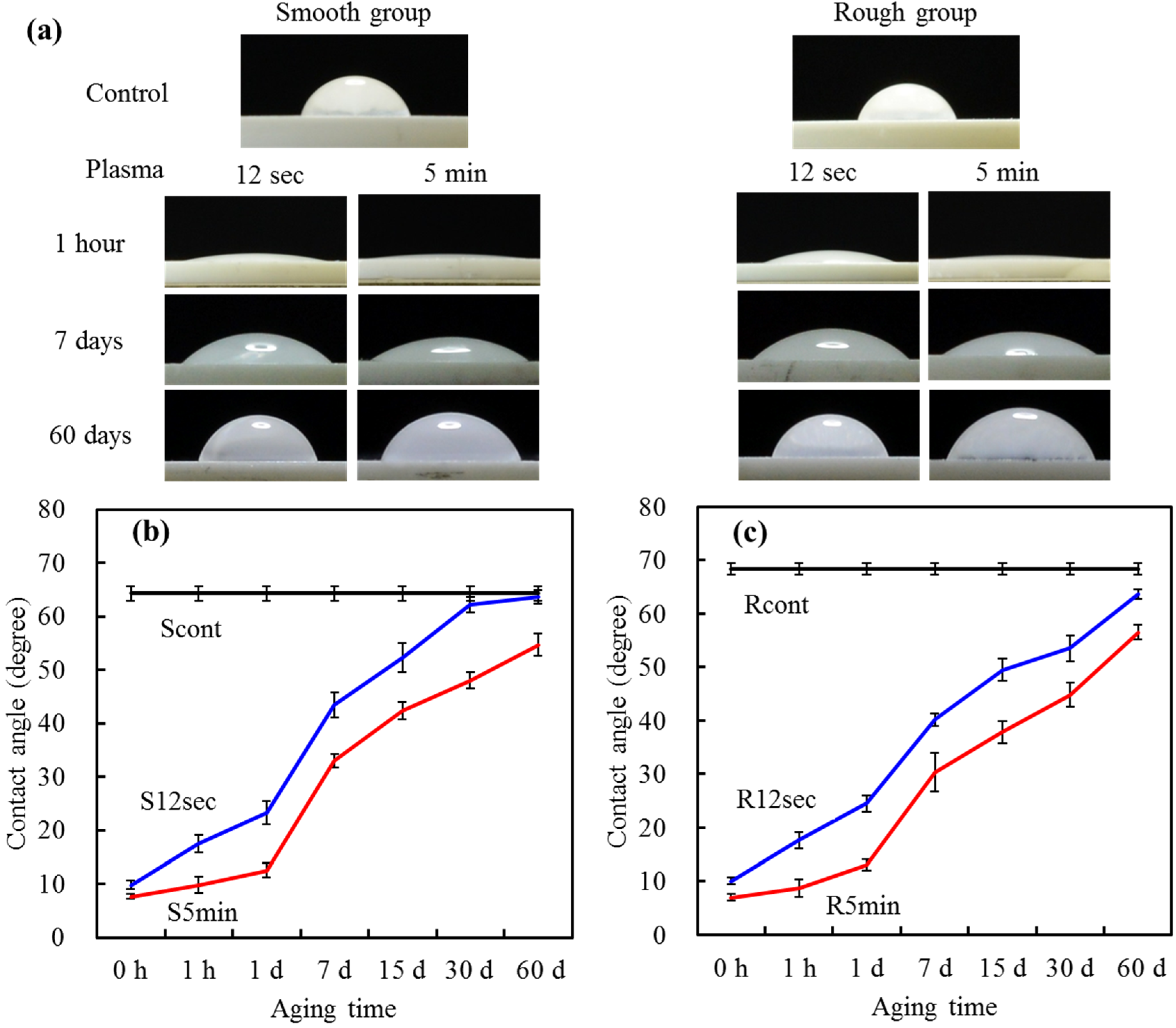
2.5. Cell Attachment
2.6. Cell Proliferation
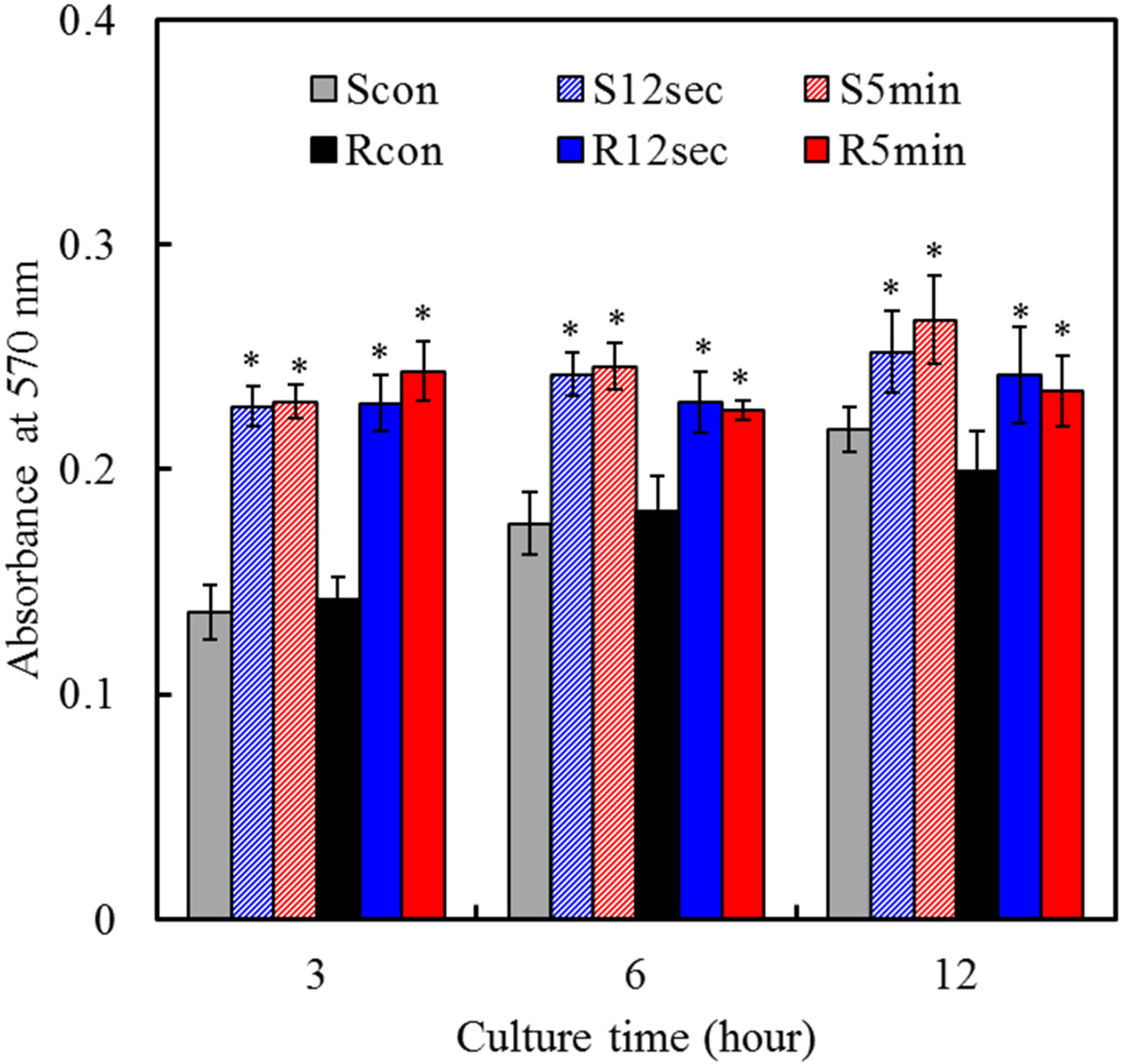
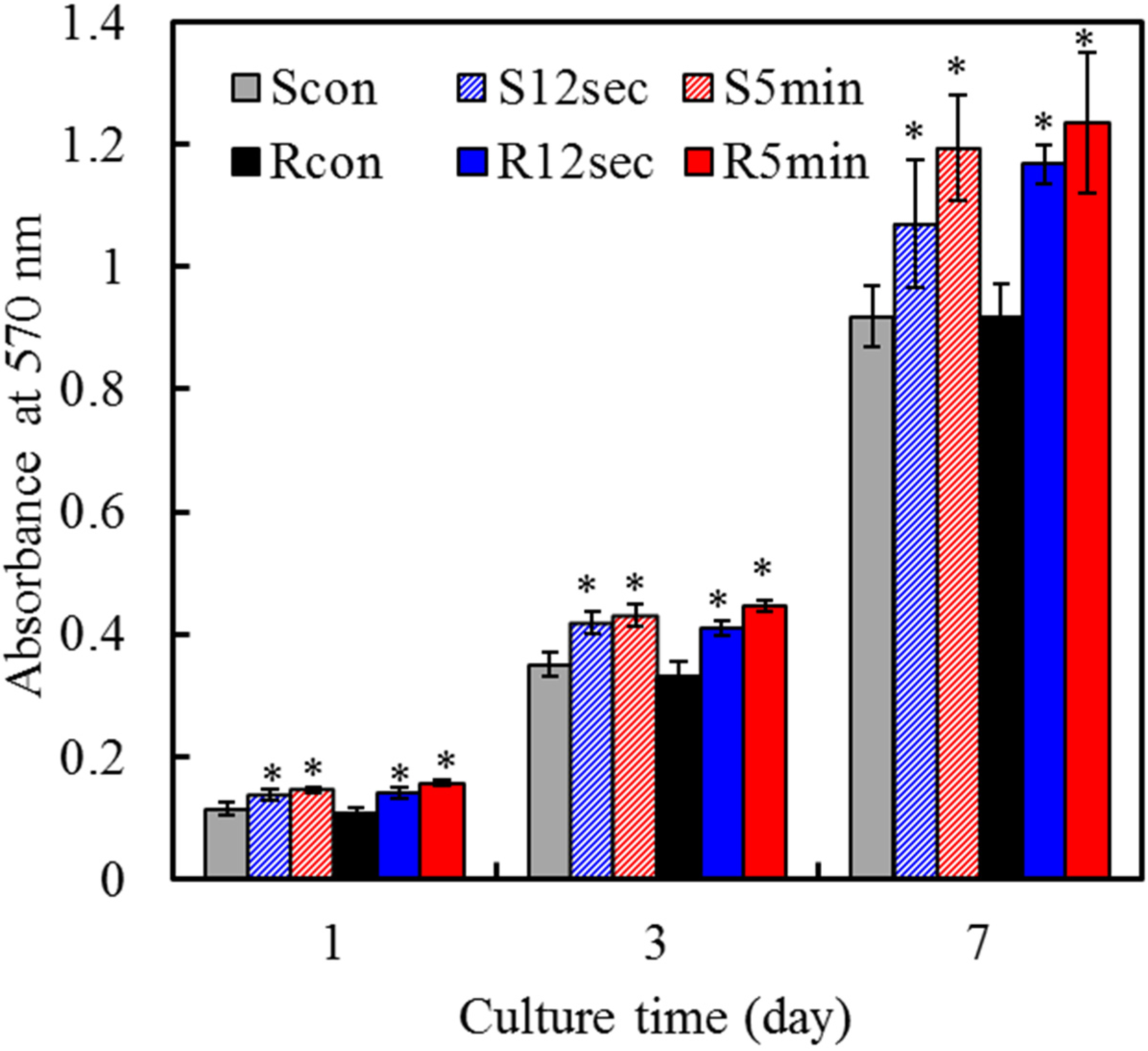
2.7. Cell Differentiation
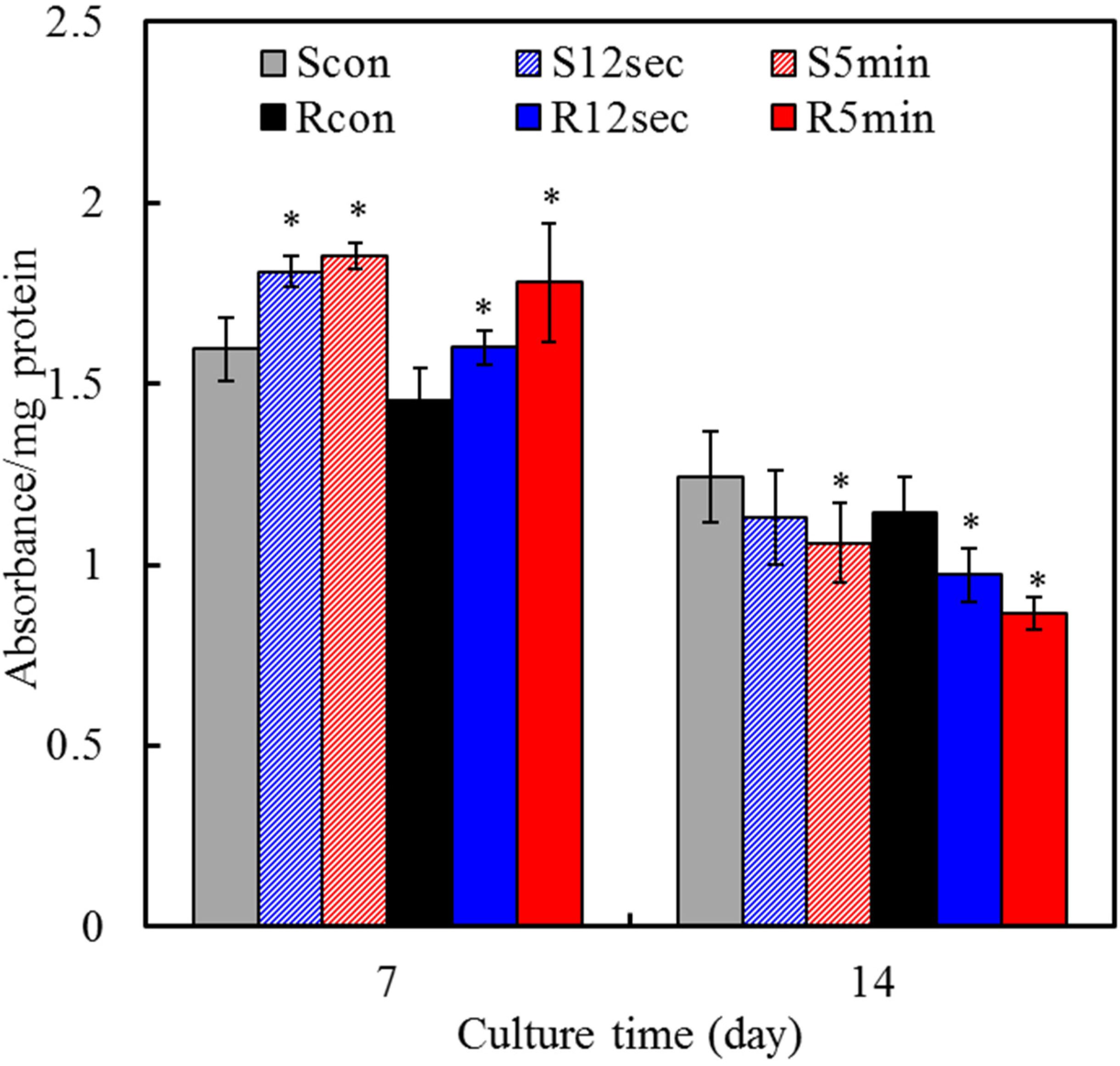
2.8. Mineralization
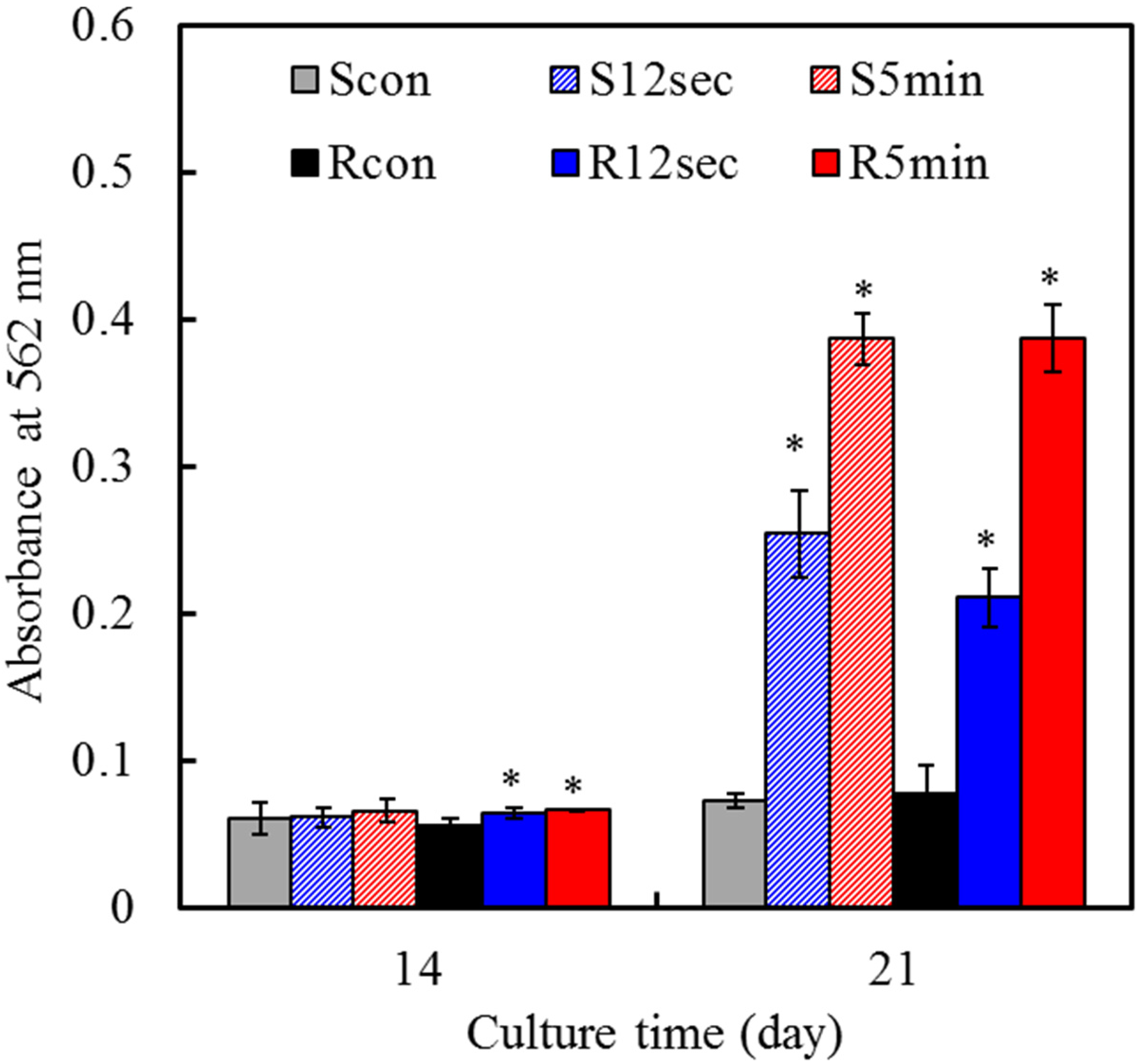
3. Experimental Section
3.1. Oxygen Plasma Treatment
3.2. Topography and Composition
3.3. Estimation of Contact Angle
3.4. Cell Culture
3.5. Cell Attachment and Proliferation
3.6. Cell Differentiation
3.7. Mineralization
3.8. Statistical Analysis
4. Conclusions
Author Contributions
Conflicts of Interest
References
- Chevalier, J. What future for zirconia as a biomaterial. Biomaterials 2006, 27, 535–543. [Google Scholar] [PubMed]
- Hench, L.L. Bioceramics: From concept to clinic. J. Am. Ceram. Soc. 1991, 74, 1487–1510. [Google Scholar] [CrossRef]
- Ferraris, M.; Verne, E.; Appendino, E.P.; Moisescu, C.; Krajewski, A.; Ravaglioli, A.; Piancastelliet, A. Coatings on zirconia for medical applications. Biomaterials 2000, 21, 765–773. [Google Scholar] [CrossRef] [PubMed]
- Watanabe, H.; Saito, K.; Kokubun, K.; Sasaki, H.; Yoshinari, M. Change in surface properties of zirconia and initial attachment of osteoblastlike cells with hydrophilic treatment. Dent. Mater. J. 2012, 31, 806–814. [Google Scholar] [CrossRef] [PubMed]
- Sandhyarani, M.; Rameshbabu, N.; Venkateswarlu, K.; Sreekanth, D.; Subrahmanyam, C. Surface morphology, corrosion resistance and in vitro bioactivity of P containing ZrO2 films formed on Zr by plasma electrolytic oxidation. J. Alloys Compd. 2013, 553, 324–332. [Google Scholar] [CrossRef]
- Han, Y.; Yan, Y.; Lu, C.; Zhang, Y.; Xu, K. Bioactivity and osteoblast response of the micro-arc oxidized zirconia films. J. Biomed. Mater. Res. 2009, 88A, 117–127. [Google Scholar] [CrossRef]
- Kim, H.W.; Georgiou, G.; Knowles, J.C.; Koh, Y.H.; Kim, H.E. Calcium phosphates and glass composite coatings on zirconia for enhanced biocompatibility. Biomaterials 2004, 25, 4203–4213. [Google Scholar] [CrossRef] [PubMed]
- Pelaez-Vargasa, A.; Gallego-Perez, D.; Magallanes-Perdomo, M.; Fernandes, M.H.; Hansford, D.J.; de Aza, A.H.; Penad, P.; Monteiro, F.J. Isotropic micropatterned silica coatings on zirconia induce guided cell growth for dental implants. Dent. Mater. 2011, 27, 581–589. [Google Scholar] [CrossRef] [PubMed]
- Hao, L.; Lawrence, J. On the role of CO2 laser treatment in the human serum albumin and human plasma fibronectin adsorption on zirconia (MGO-PSZ) bioceramic surface. J. Biomed. Mater. Res. 2004, 69A, 748–756. [Google Scholar] [CrossRef]
- Duske, K.; Koban, I.; Kindel, E.; Schröder, K.; Nebe, B.; Holtfreter, B.; Jablonowski, L.; Weltmann, K.D.; Koche, T. Atmospheric plasma enhances wettability and cell spreading on dental implant metals. J. Clin. Periodontol. 2012, 39, 400–407. [Google Scholar] [CrossRef] [PubMed]
- Wei, J.; Yoshinari, M.; Takemoto, S.; Hattori, M.; Kawada, E.; Liu, B.; Oda, Y. Adhesion of mouse fibroblasts on hexamethyldisiloxane surfaces with wide range of wettability. J. Biomed. Mater. Res. 2007, 81B, 66–75. [Google Scholar] [CrossRef]
- Wu, C.C.; Yuan, C.Y.; Ding, S.J. Effect of polydimethylsiloxane surfaces silanized with different nitrogen-containing groups on the adhesion progress of epithelial cells. Surf. Coat. Technol. 2011, 205, 3182–3189. [Google Scholar] [CrossRef]
- Noro, A.; Kaneko, M.; Murata, I.; Yoshinari, M. Influence of surface topography and surface physicochemistry on wettability of zirconia (tetragonal zirconia polycrystal). J. Biomed. Mater. Res. 2013, 101B, 355–363. [Google Scholar] [CrossRef]
- Shon, W.J.; Chung, S.H.; Kim, H.K.; Han, G.J.; Cho, B.H.; Park, Y.S. Peri-implant bone formation of non-thermal atmospheric pressure plasma-treated zirconia implants with different surface roughness in rabbit tibiae. Clin. Oral Implants Res. 2014, 25, 573–579. [Google Scholar] [CrossRef] [PubMed]
- Xu, X.; Wang, X. Fine tuning of the sizes and phases of ZrO2 nanocrystals. Nano Res. 2009, 2, 891–902. [Google Scholar] [CrossRef]
- Kim, M.C.; Song, D.K.; Shin, H.S.; Baeg, S.H.; Kim, G.S.; Boo, J.H.; Han, J.G.; Yang, S.H. Surface modification for hydrophilic property of stainless steel treated by atmospheric-pressure plasma jet. Surf. Coat. Technol. 2003, 171, 312–316. [Google Scholar] [CrossRef]
- Vesel, A.; Mozetic, M.; Drenik, A.; Milosevic, S.; Krstulovic, N.; Balat-Pichelin, M.; Poberaj, I.; Babic, D. Cleaning of porous aluminium titanate by oxygen plasma. Plasma Chem. Plasma Process. 2006, 26, 577–584. [Google Scholar] [CrossRef]
- Smeacetto, F.; Salvo, M.; Ajitdoss, L.C.; Perero, S.; Moskalewicz, T.; Boldrini, S.; Doubova, L.; Ferraris, M. Yttria-stabilized zirconia thin film electrolyte produced by RF sputtering for solid oxide fuel cell applications. Mater. Lett. 2010, 64, 2450–2453. [Google Scholar] [CrossRef]
- Lee, P.R.; Ho, C.C.; Hwang, C.S.; Ding, S.J. Improved physicochemical properties and biocompatibility of stainless steel implants by PVA/ZrO2-based composite coatings. Surf. Coat. Technol. 2014, 258, 374–380. [Google Scholar] [CrossRef]
- Zhao, G.; Schwartz, Z.; Wieland, M.; Rupp, F.; Geis-Gerstorfer, J.; Cochran, D.L.; Boyan, B.D. High surface energy enhances cell response to titanium substrate microstructure. J. Biomed. Mater. Res. 2005, 74A, 49–58. [Google Scholar] [CrossRef]
- Goddard, J.M.; Hotchkiss, J.H. Polymer surface modification for the attachment of bioactive compounds. Prog. Polym. Sci. 2007, 32, 698–725. [Google Scholar] [CrossRef]
- Novotna, K.; Bacakova, M.; Kasalkova, N.S.; Slepicka, P.; Lisa, V.; Svorcik, V.; Bacakova, L. Adhesion and growth of vascular smooth muscle cells on nanostructured and biofunctionalized polyethylene. Materials 2013, 6, 1632–1655. [Google Scholar] [CrossRef]
- Kasemo, B.; Lausmaa, J. Biomaterial and implant surfaces: On the role of cleanliness, contamination, and preparation procedures. J. Biomed. Mater. Res. 1988, 22, 145–158. [Google Scholar] [CrossRef] [PubMed]
- Giljean, S.; Bigerelle, M.; Anselme, K.; Haidara, H. New insights on contact angle/roughness dependence on high surface energy materials. Appl. Surf. Sci. 2011, 257, 9631–9638. [Google Scholar] [CrossRef]
- Huang, S.C.; Wu, B.C.; Ding, S.J. Stem cell differentiation-induced calcium silicate cement with bacteriostatic activity. J. Mater. Chem. B. 2015, 3, 570–580. [Google Scholar] [CrossRef]
- Wu, B.C.; Huang, S.C.; Ding, S.J. Comparative osteogenesis of radiopaque dicalcium silicate cement and white-colored mineral trioxide aggregate in a rabbit femur model. Materials 2013, 6, 5675–5689. [Google Scholar] [CrossRef]
- Ito, H.; Sasaki, H.; Saito, K.; Honma, S.; Yajima, Y.; Yoshinari, M. Response of osteoblast-like cells to zirconia with different surface topography. Dent. Mater. J. 2013, 32, 122–129. [Google Scholar] [CrossRef] [PubMed]
- Yamashita, D.; Machigashira, M.; Miyamoto, M.; Takeuchi, H.; Noguchi, K.; Izumi, Y.; Ban, S. Effect of surface roughness on initial responses of osteoblast-like cells on two types of zirconia. Dent. Mater. J. 2009, 28, 461–470. [Google Scholar] [CrossRef] [PubMed]
- Wang, C.W.; Chiang, T.Y.; Chang, H.C.; Ding, S.J. Physicochemical properties and osteogenic activity of radiopaque calcium silicate-gelatin cements. J. Mater. Sci. Mater. Med. 2014, 25, 2193–2203. [Google Scholar] [CrossRef] [PubMed]
- Ding, S.J.; Shie, M.Y.; Wei, C.K. In vitro physicochemical properties, osteogenic activity, and immunocompatibility of calcium silicate-gelatin bone grafts for load-bearing applications. ACS Appl. Mater. Interfaces 2011, 3, 4142–4153. [Google Scholar] [CrossRef] [PubMed]
- Chen, C.C.; Wang, C.W.; Hsueh, N.S.; Ding, S.J. Improvement of in vitro physicochemical properties and osteogenic activity of calcium sulfate cement for bone repair by dicalcium silicate. J. Alloys Compd. 2014, 585, 25–31. [Google Scholar] [CrossRef]
- Chiang, T.Y.; Wei, C.K.; Ding, S.J. Effects of bismuth oxide on physicochemical properties and osteogenic activity of dicalcium silicate cements. J. Med. Biol. Eng. 2014, 34, 30–35. [Google Scholar] [CrossRef]
- Eriksson, C.; Nygren, H.; Ohlson, K. Implantation of hydrophilic and hydrophobic titanium discs in rat tibia: Cellular reactions on the surfaces during the first 3 weeks in bone. Biomaterials 2004, 25, 4759–4766. [Google Scholar] [CrossRef] [PubMed]
- Shie, M.Y.; Chang, H.C.; Ding, S.J. Composition-dependent protein secretion and integrin level of osteoblastic cell on calcium silicate cements. J. Biomed. Mater. Res. 2014, 102A, 769–780. [Google Scholar] [CrossRef]
- Dulgar-Tulloch, A.J.; Bizios, R.; Siegel, R.W. Human mesenchymal stem cell adhesion and proliferation in response to ceramic chemistry and nanoscale topography. J. Biomed. Mater. Res. 2009, 90A, 586–594. [Google Scholar] [CrossRef]
- Nakamura, M.; Kobayashi, A.; Nozaki, K.; Horiuchi, N.; Nagai, A.; Yamashita, K. Improvement of osteoblast adhesion through polarization of plasma-sprayed hydroxyapatite coatings on metal. J. Med. Biol. Eng. 2014, 34, 44–48. [Google Scholar] [CrossRef]
© 2015 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Wu, C.-C.; Wei, C.-K.; Ho, C.-C.; Ding, S.-J. Enhanced Hydrophilicity and Biocompatibility of Dental Zirconia Ceramics by Oxygen Plasma Treatment. Materials 2015, 8, 684-699. https://doi.org/10.3390/ma8020684
Wu C-C, Wei C-K, Ho C-C, Ding S-J. Enhanced Hydrophilicity and Biocompatibility of Dental Zirconia Ceramics by Oxygen Plasma Treatment. Materials. 2015; 8(2):684-699. https://doi.org/10.3390/ma8020684
Chicago/Turabian StyleWu, Ching-Chou, Chung-Kai Wei, Chia-Che Ho, and Shinn-Jyh Ding. 2015. "Enhanced Hydrophilicity and Biocompatibility of Dental Zirconia Ceramics by Oxygen Plasma Treatment" Materials 8, no. 2: 684-699. https://doi.org/10.3390/ma8020684
APA StyleWu, C.-C., Wei, C.-K., Ho, C.-C., & Ding, S.-J. (2015). Enhanced Hydrophilicity and Biocompatibility of Dental Zirconia Ceramics by Oxygen Plasma Treatment. Materials, 8(2), 684-699. https://doi.org/10.3390/ma8020684







