2. Bioactive Sodium Titanate
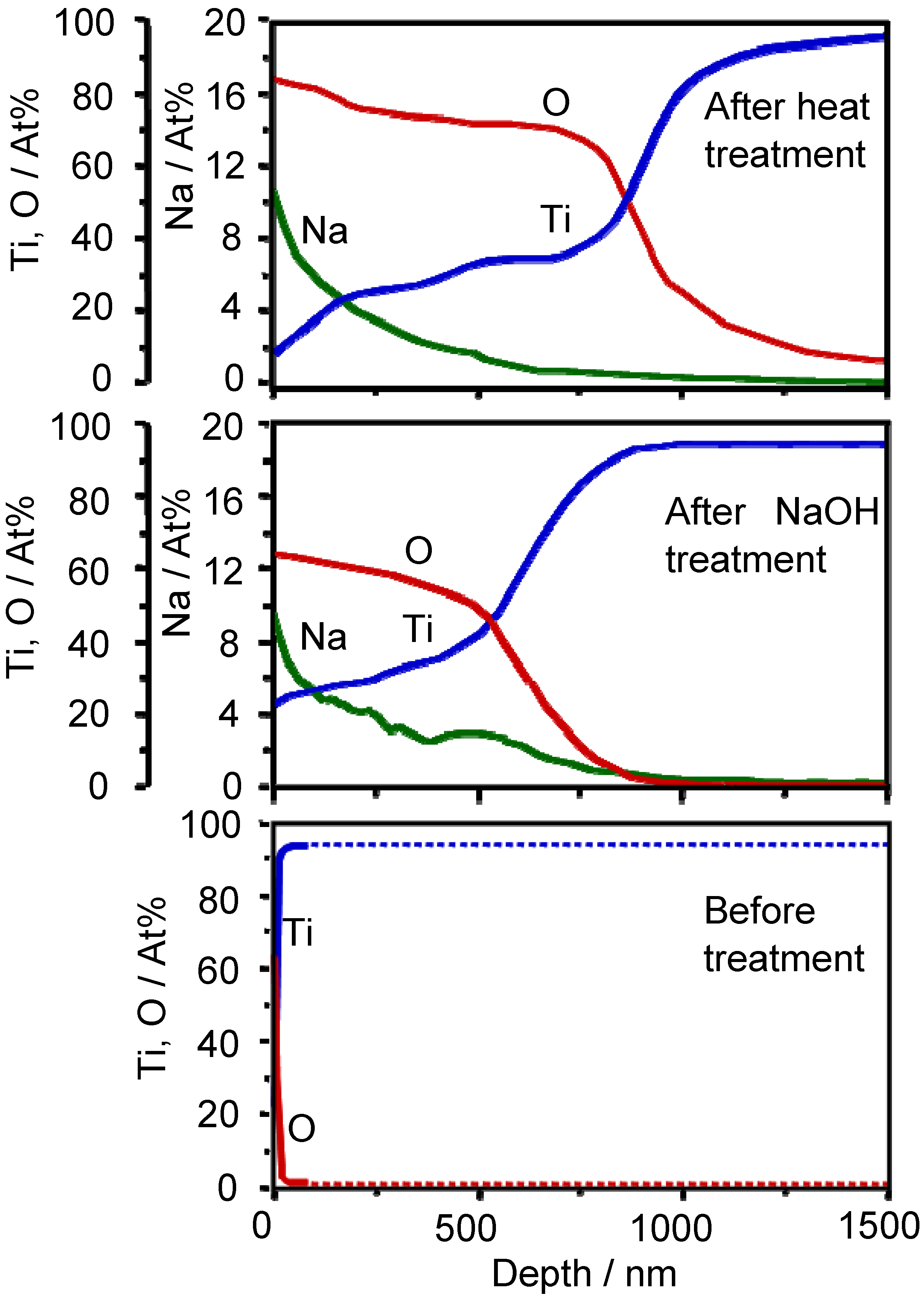
When Ti metal is soaked in a 5 M NaOH aqueous solution at 60 °C for a period of 24 h, sodium and oxygen ions penetrate into the surface of the Ti metal to a depth of 1 μm, and only the oxygen ions penetrate into deeper regions on subsequent heat treatment at 600 °C for a period of 1 h in an ambient atmosphere, as shown by the Auger electron spectra in
Figure 1 [
3].
A fine network structure on the nanometre scale, consisting of feather-like phases, is formed on the surface of Ti metal with a thickness of 1 μm by the NaOH treatment, and this densifies after the subsequent heat treatment, as shown by the SEM photographs in
Figure 2 [
4].
The fine network structure formed by the NaOH treatment is composed of nano-sized sodium hydrogen titanate (Na
xH
2-xTi
yO
2y+1, where 0 <
x < 2 and
y = 2, 3, or 4), and this is converted into sodium titanate (Na
2Ti
yO
2y+1,
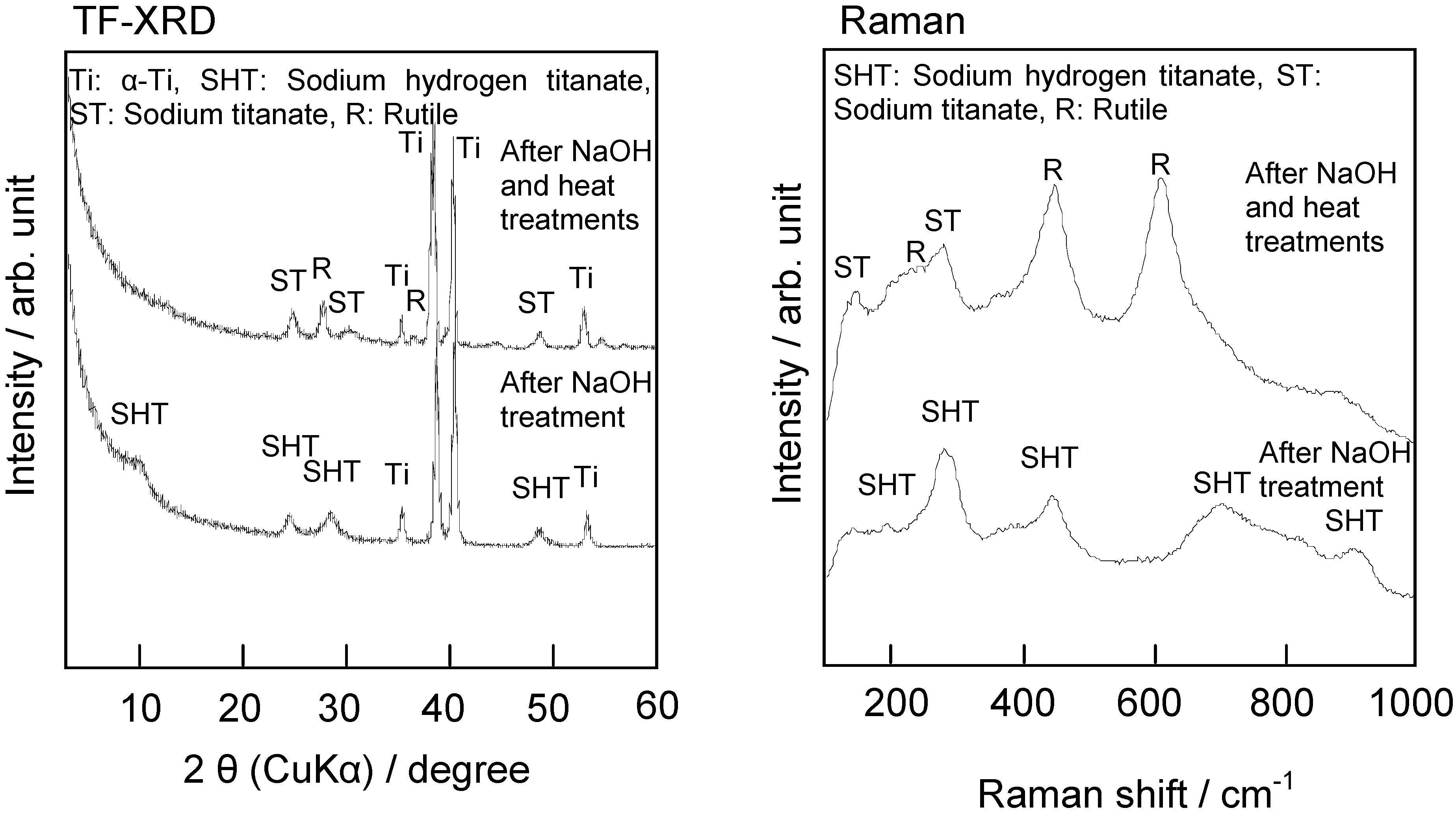
y = 5, 6…) and rutile by the subsequent heat treatment, as shown by thin-film X-ray diffraction pattern and Raman spectra in
Figure 3 [
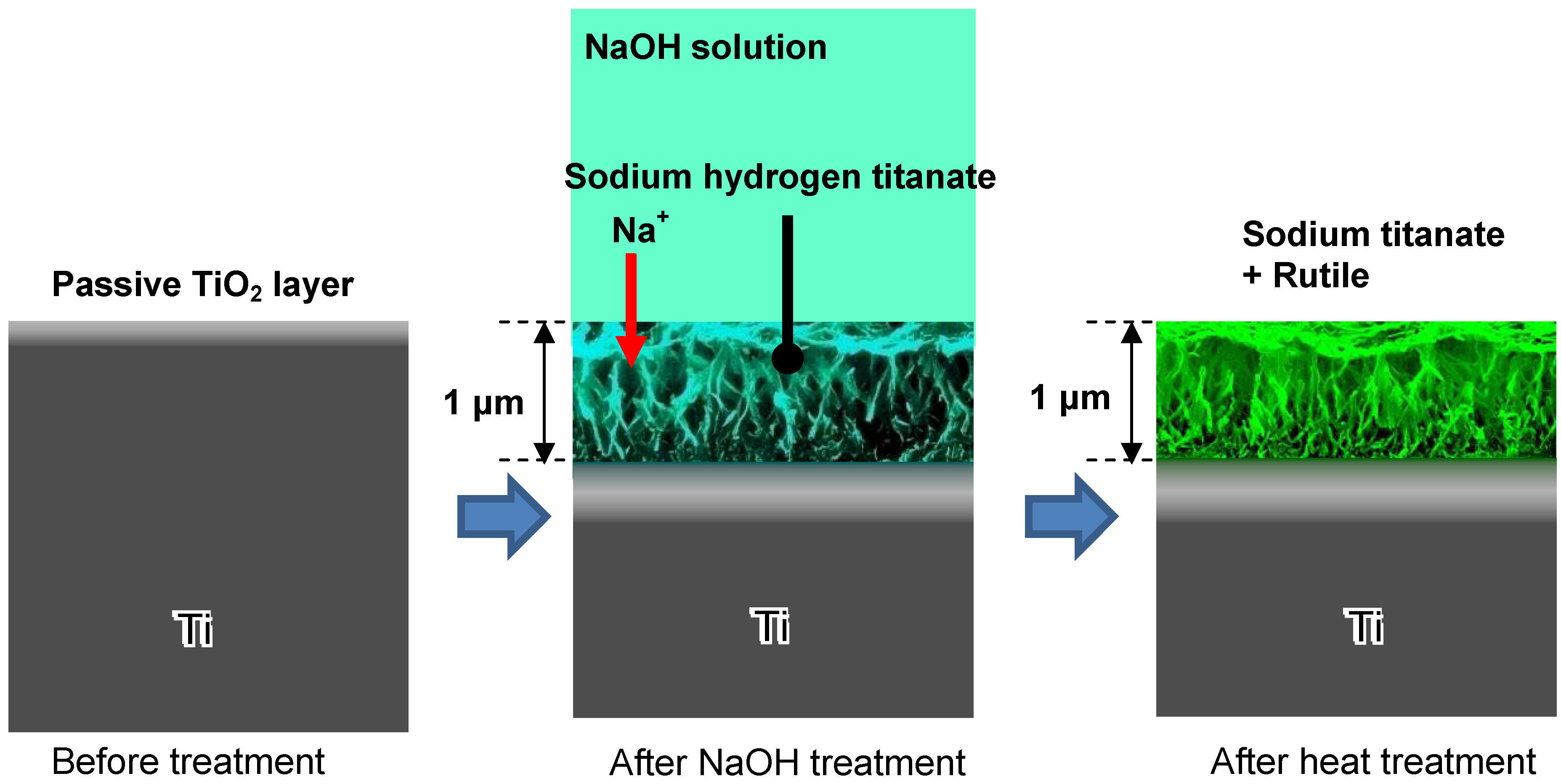
5]. These structural changes due to the NaOH and heat treatments are shown schematically in
Figure 4.
The scratch resistance of this surface layer as formed by the NaOH treatment is poor, but it increases markedly on subsequent heat treatment, from 5 to 50 mN [
5].
When the thus-treated Ti metal is soaked in SBF, bone-like apatite begins to precipitate in the deep regions of the interspaces of the feather-like phases, and grows and fills these interspaces to integrate with the feather-like phases, forming a dense composite of apatite and titanate, which eventually grows over the surface layer, as shown in the SEM photographs in
Figure 5(a) and
Figure 5(b) [
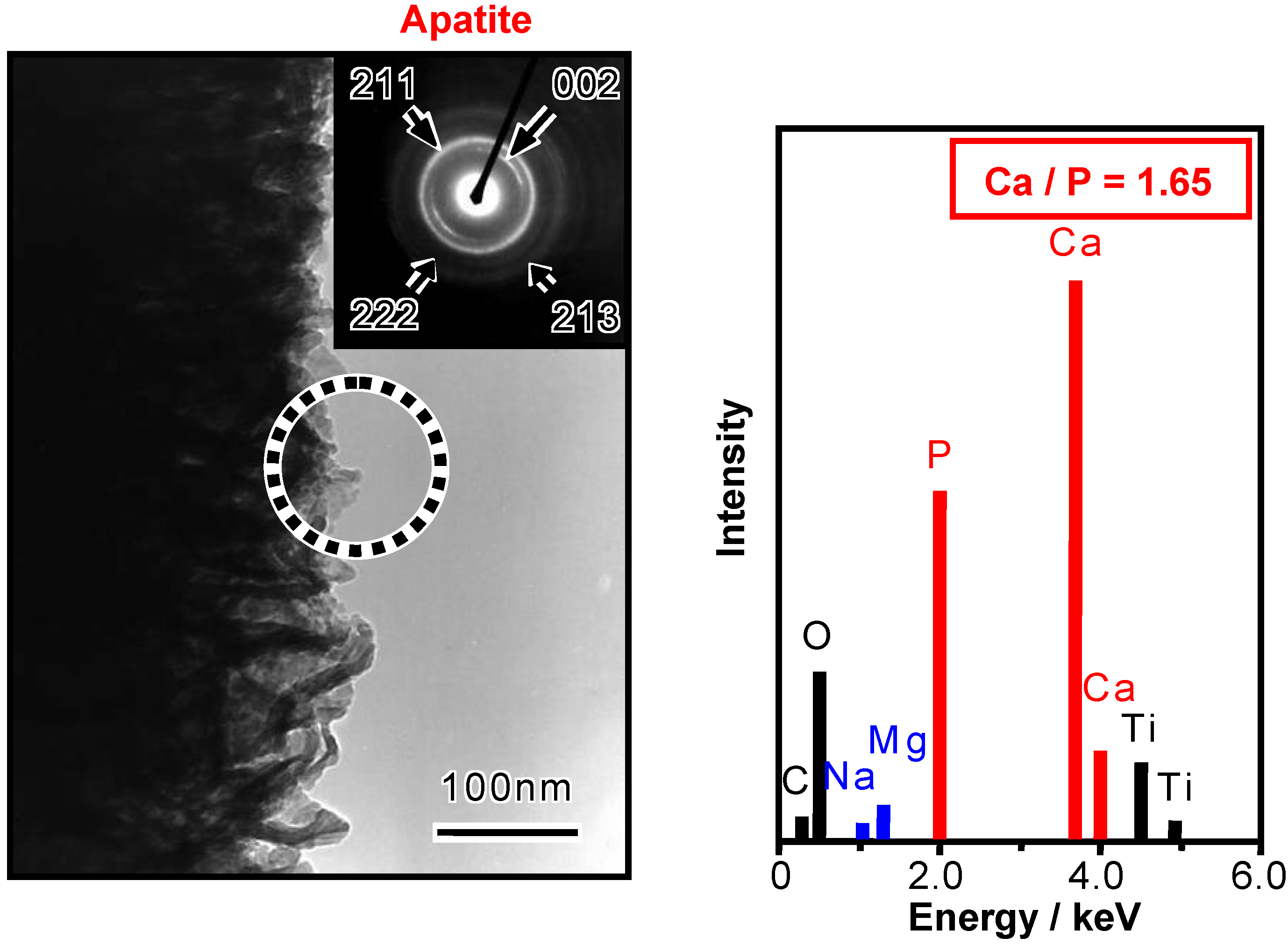
4]. The thus-formed apatite is confirmed to take a needle-like form, and has a composition with a Ca/P ratio = 1.65, accompanied with small amounts of Na and Mg, similar to the bone mineral, from the transmission electron micrograph and energy dispersive X-ray analysis (EDX) shown in
Figure 6 [
6].
Figure 1.
AES depth profiles of the surfaces of Ti metals untreated and those subjected to NaOH and heat treatments.
Figure 1.
AES depth profiles of the surfaces of Ti metals untreated and those subjected to NaOH and heat treatments.
Figure 2.
SEM photographs of cross sections of surfaces of Ti metals subjected to NaOH and heat treatments.
Figure 2.
SEM photographs of cross sections of surfaces of Ti metals subjected to NaOH and heat treatments.
Figure 3.
TF-XRD patterns and Raman spectra of surfaces of Ti metals subjected to NaOH and heat treatments.
Figure 3.
TF-XRD patterns and Raman spectra of surfaces of Ti metals subjected to NaOH and heat treatments.
Figure 4.
Structural change of surface of Ti metal subjected to NaOH and heat treatments.
Figure 4.
Structural change of surface of Ti metal subjected to NaOH and heat treatments.
Figure 5.
SEM photographs of surface (a) and cross-section (b) of NaOH- and heat-treated Ti metal after soaking in SBF for 1 d.
Figure 5.
SEM photographs of surface (a) and cross-section (b) of NaOH- and heat-treated Ti metal after soaking in SBF for 1 d.
Figure 6.
TEM photograph and EDX spectrum of the surface of the NaOH- and heat-treated Ti metal after soaking in SBF for 5 d (dotted circle: area of electron diffraction and EDX analysis).
Figure 6.
TEM photograph and EDX spectrum of the surface of the NaOH- and heat-treated Ti metal after soaking in SBF for 5 d (dotted circle: area of electron diffraction and EDX analysis).
According to X-ray photoemission spectroscopic (XPS) analysis [
7], transmission electron microscopic (TEM) observation [
6] and zeta potential measurement [
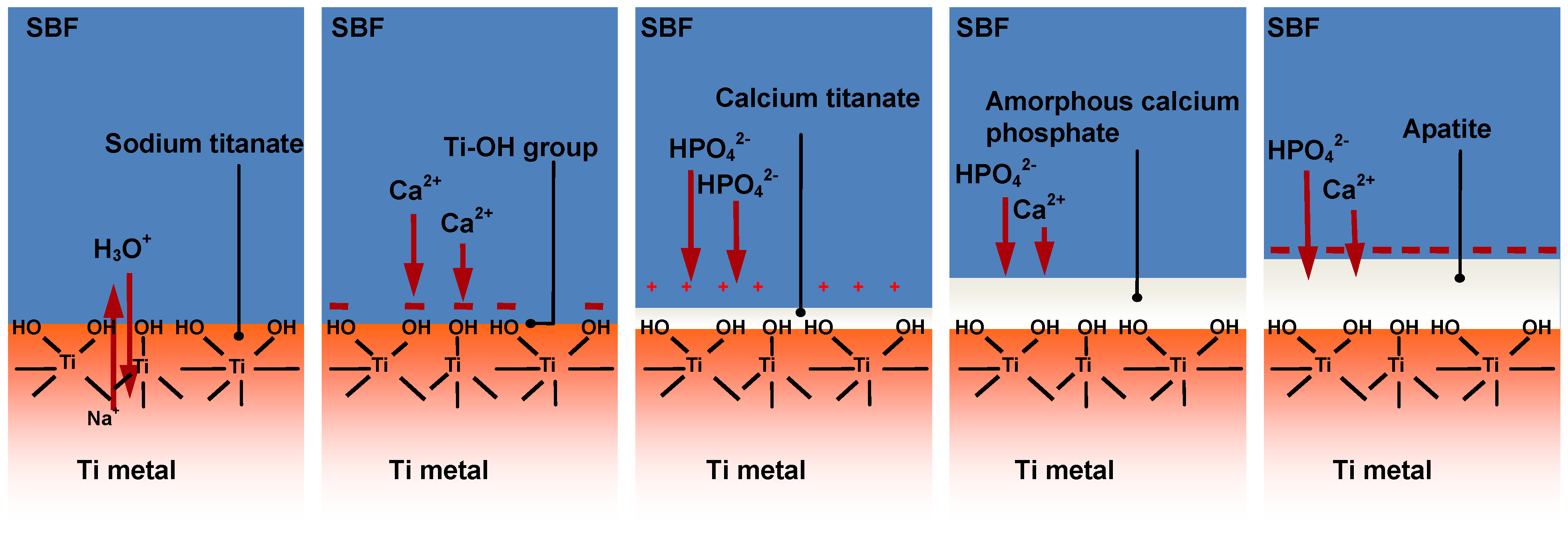
8] of the surfaces of treated Ti metal as a function of soaking time in SBF, bone-like apatite is formed by the following process on the Ti metal in SBF, as shown in
Figure 7. Sodium ions in the sodium titanate at the surface of the Ti metal are exchanged with the H
3O
+ ions in SBF. As a result, Ti–OH groups are formed on the surface of the Ti metal and the pH of the surrounding SBF increases from the released Na
+ ions. In such high a pH environment, the Ti–OH groups are negatively charged [
9] and preferentially combine with the positively charged Ca
2+ ions in SBF. As the calcium ions accumulate, the surface becomes positively charged and combines with negatively charged phosphate ions to form an amorphous calcium phosphate. This calcium phosphate eventually transforms into a stable crystalline bone-like apatite [
8].
Figure 7.
Process of apatite formation on NaOH- and heat-treated Ti metal in SBF.
Figure 7.
Process of apatite formation on NaOH- and heat-treated Ti metal in SBF.
The Na
+ ions in the sodium titanate on the surface of Ti metal are easily released, even when the Ti metal is stored in a humid environment. This is a problem in clinical applications, since any decrease in the sodium concentration of the sodium titanate decreases the apatite-forming ability of the treated Ti metal in a body environment, as shown in
Figure 8 [
5].
This problem can be resolved by the controlled release of Na
+ ions from the top surface of the treated Ti metal before the heat treatment stage. For example, when Ti metal is soaked in water for a period of 3 h after the NaOH treatment, one-third of the sodium ions of the surface sodium hydrogen titanate layer are released from the top surface via exchange with the H
3O
+ ions in the water. The thus-treated Ti metal then forms anatase on the top surface after a heat treatment. The thus-formed anatase is stable in a humid environment and has a high apatite-forming ability in a body environment where the pH is increased by the sodium ions released from the inner layer. As a result, the thus-treated Ti metal exhibits a high apatite-forming ability, and is stable in a humid environment [
5].
Figure 8.
SEM photographs of surfaces of Ti metals soaked in SBF for 1 d, just after NaOH and heat treatments, and after subsequent storage in 95% relative humidity at 80 °C for 1 week.
Figure 8.
SEM photographs of surfaces of Ti metals soaked in SBF for 1 d, just after NaOH and heat treatments, and after subsequent storage in 95% relative humidity at 80 °C for 1 week.
These
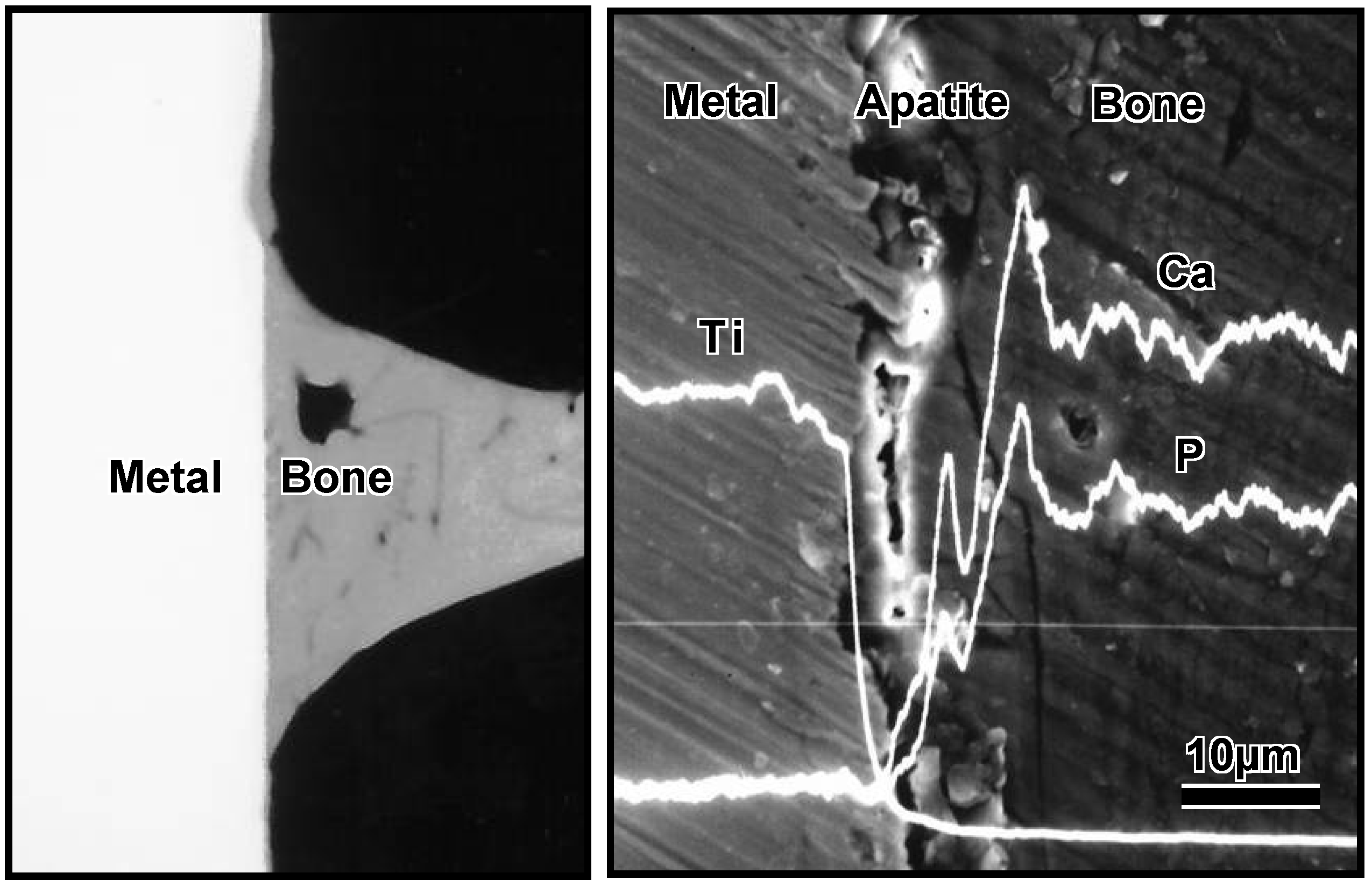
in vitro results indicate that treated Ti metal forms bone-like apatite on its surface in bone defects, and bonds to the surrounding bone through this apatite layer. As expected, it formed apatite on its surface when it was implanted into the tibia of a rabbit and came into direct contact with the surrounding bone through the apatite layer without intervention of the fibrous tissue, as shown in
Figure 9 [
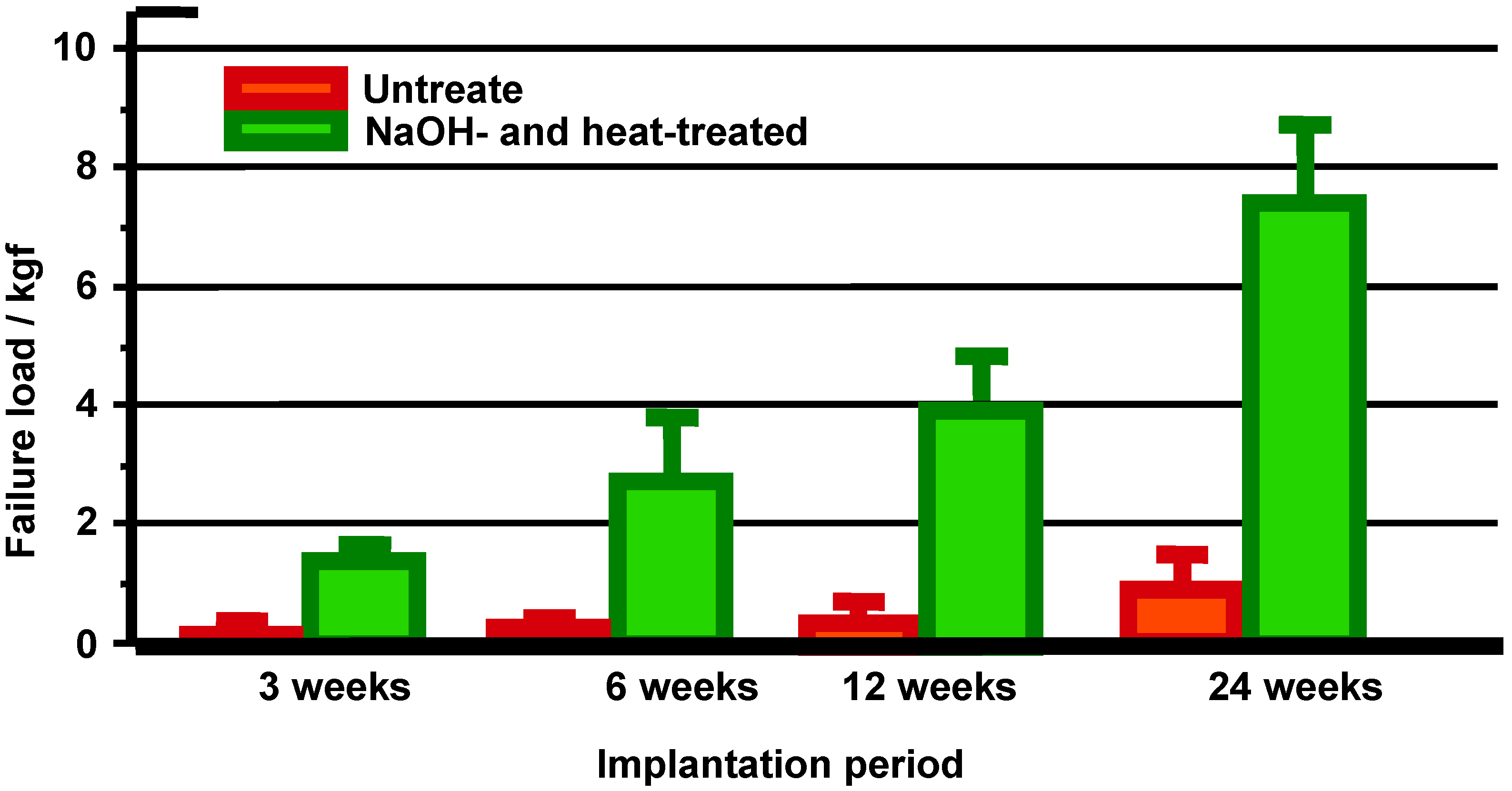
10]. When a tensile stress was applied to the interface, a higher load was required to produce fractures at the interface for the treated Ti metal than for the untreated Ti metal, and the difference between these samples increased with increasing period after implantation, as shown in
Figure 10.
Figure 9.
CMR and SEM-EDX photographs at the interface between Ti metal which was subjected to NaOH and heat treatments, and implanted into rabbit tibial bone for eight weeks.
Figure 9.
CMR and SEM-EDX photographs at the interface between Ti metal which was subjected to NaOH and heat treatments, and implanted into rabbit tibial bone for eight weeks.
Figure 10.
Detaching failure loads of the untreated and the NaOH- and heat-treated Ti metals as a function of implantation period in rabbit tibia.
Figure 10.
Detaching failure loads of the untreated and the NaOH- and heat-treated Ti metals as a function of implantation period in rabbit tibia.
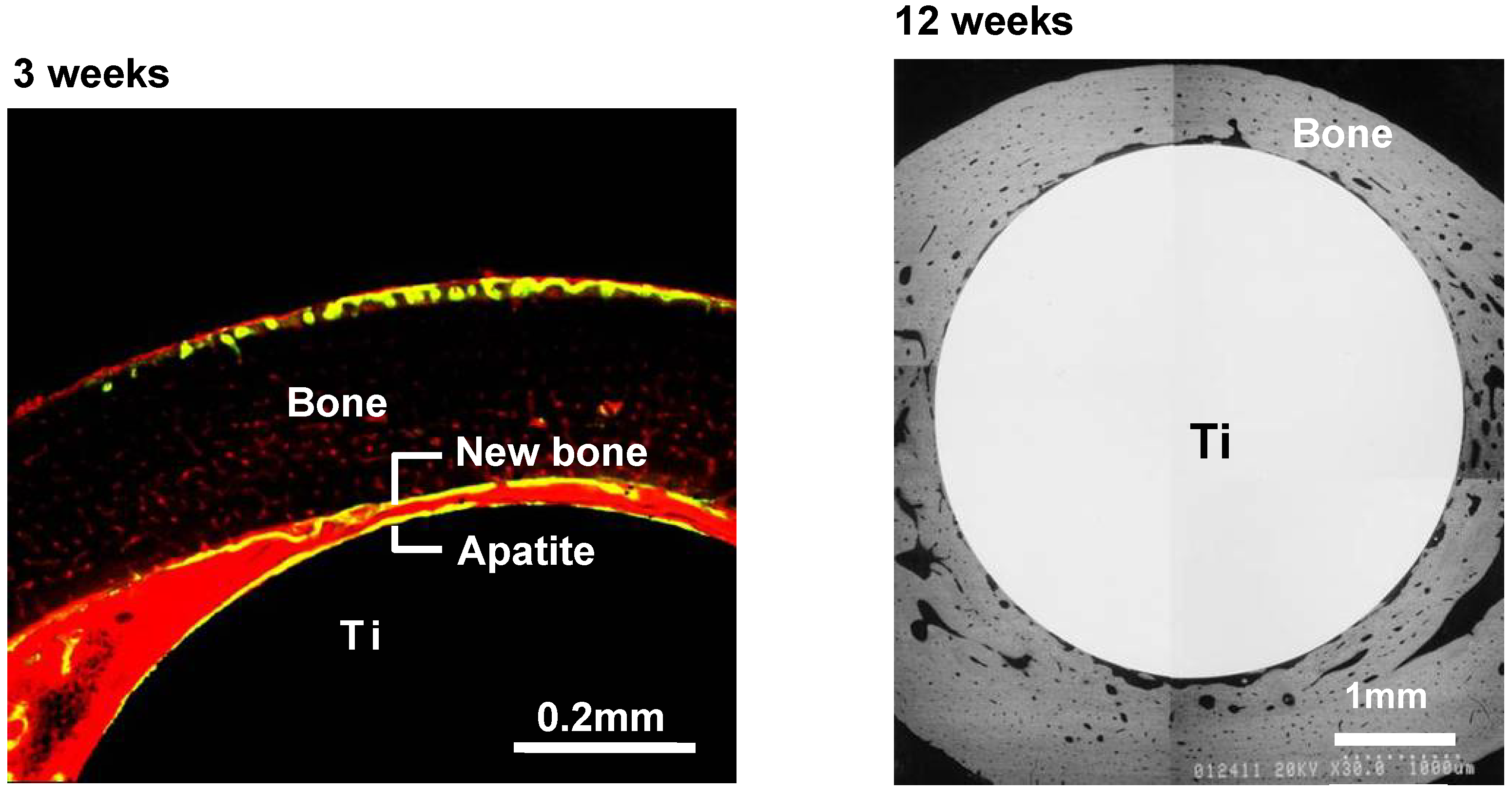
When similarly treated Ti metal rods were implanted into the medullary canal of a rabbit’s femur, they also formed apatite on their surfaces, and were soon fully surrounded by newly grown bone, as shown in
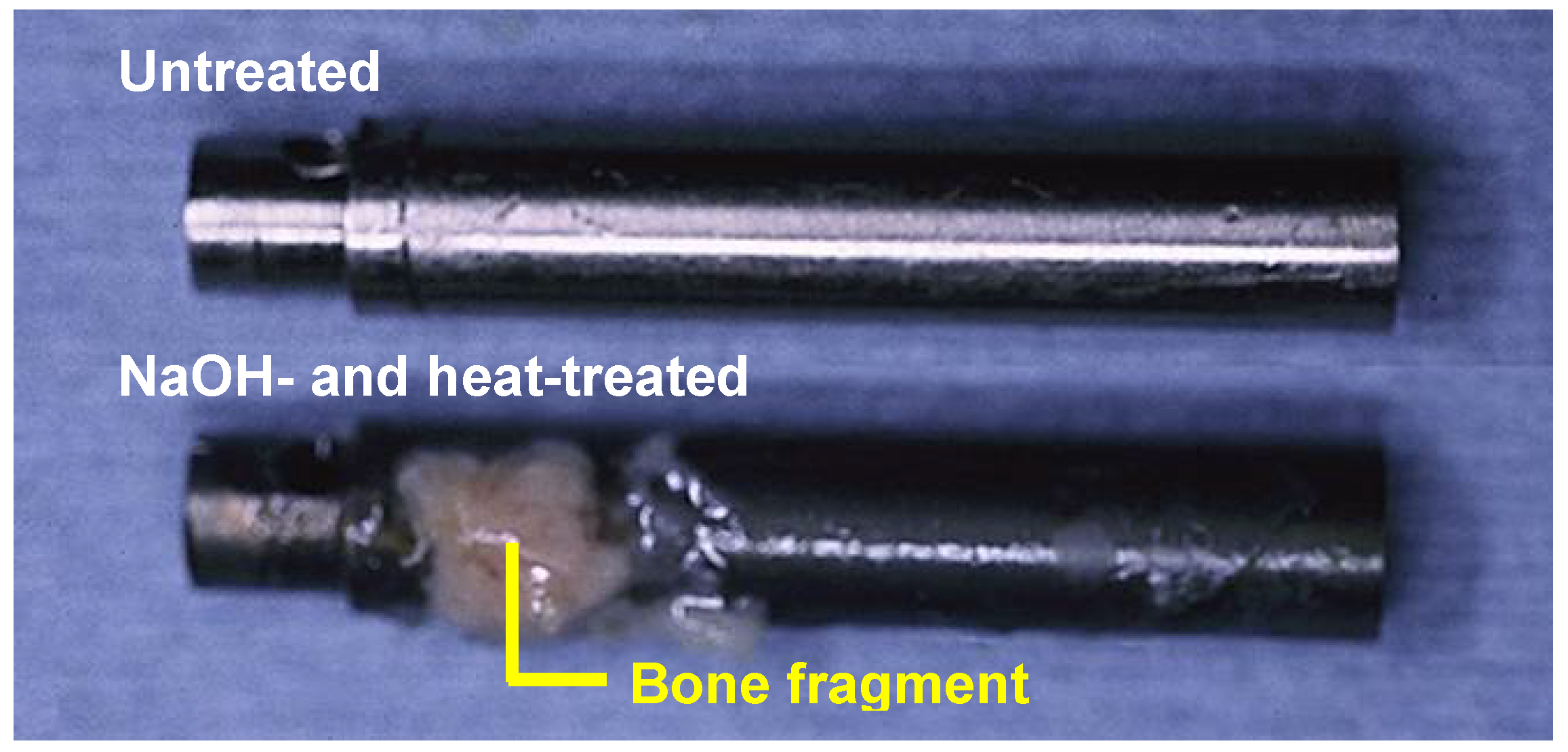
Figure 11. These could not be pulled out from the surrounding bone without being accompanied by bone fragments, as shown in
Figure 12 [
11]. Based on these
in vitro and
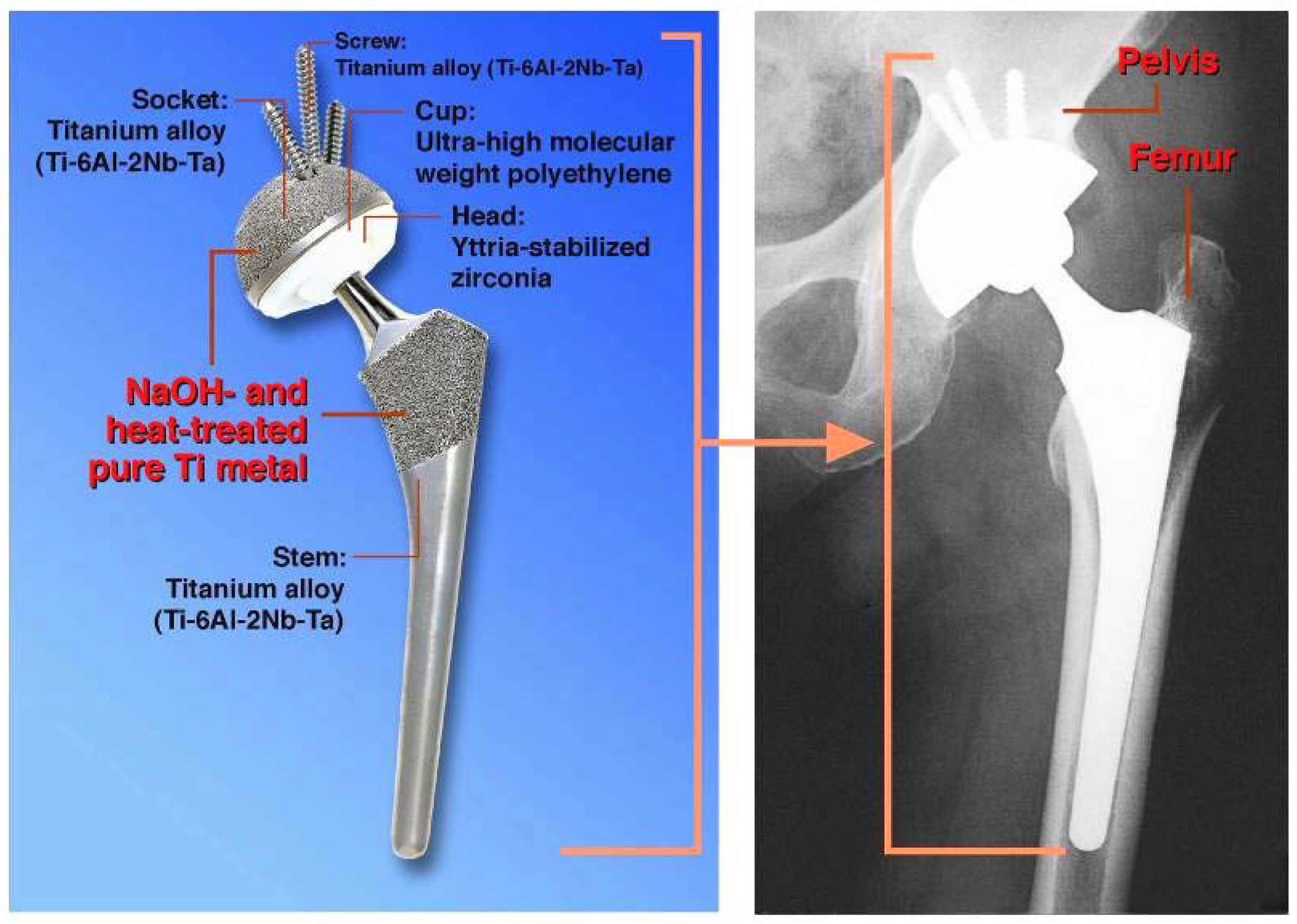
in vivo results, the NaOH and heat treatments were applied to a porous Ti metal layer formed on the Ti-6Al-2Nb-Ta alloy of a total hip joint. The thus-prepared bioactive hip joint has been clinically used in Japan since 2007, as shown
Figure 13 [
12].
Figure 11.
Confocal laser scanning microscopy photograph (left-hand side) and SEM photograph (right-hand side) of the cross-section of the NaOH- and heat-treated Ti metal implanted into rabbit femur for three and 12 weeks, respectively.
Figure 11.
Confocal laser scanning microscopy photograph (left-hand side) and SEM photograph (right-hand side) of the cross-section of the NaOH- and heat-treated Ti metal implanted into rabbit femur for three and 12 weeks, respectively.
Figure 12.
Surfaces of the untreated and the NaOH- and heat-treated Ti implants after the pull-out tests (12 weeks after implantation).
Figure 12.
Surfaces of the untreated and the NaOH- and heat-treated Ti implants after the pull-out tests (12 weeks after implantation).
Figure 13.
Clinical application of NaOH- and heat-treated Ti metal in hip joint system.
Figure 13.
Clinical application of NaOH- and heat-treated Ti metal in hip joint system.
3. Bioactive Calcium Titanate
The NaOH and heat treatments described above are also effective for Ti-based alloys, such as Ti-6Al-4V, Ti-6Al-2Nb-Ta, and Ti-15Mo-5Zr-3Al in inducing bioactivity [
13,
14], but not for new types of Ti-Zr-Nb-Ta alloys that are free from cytotoxic elements.
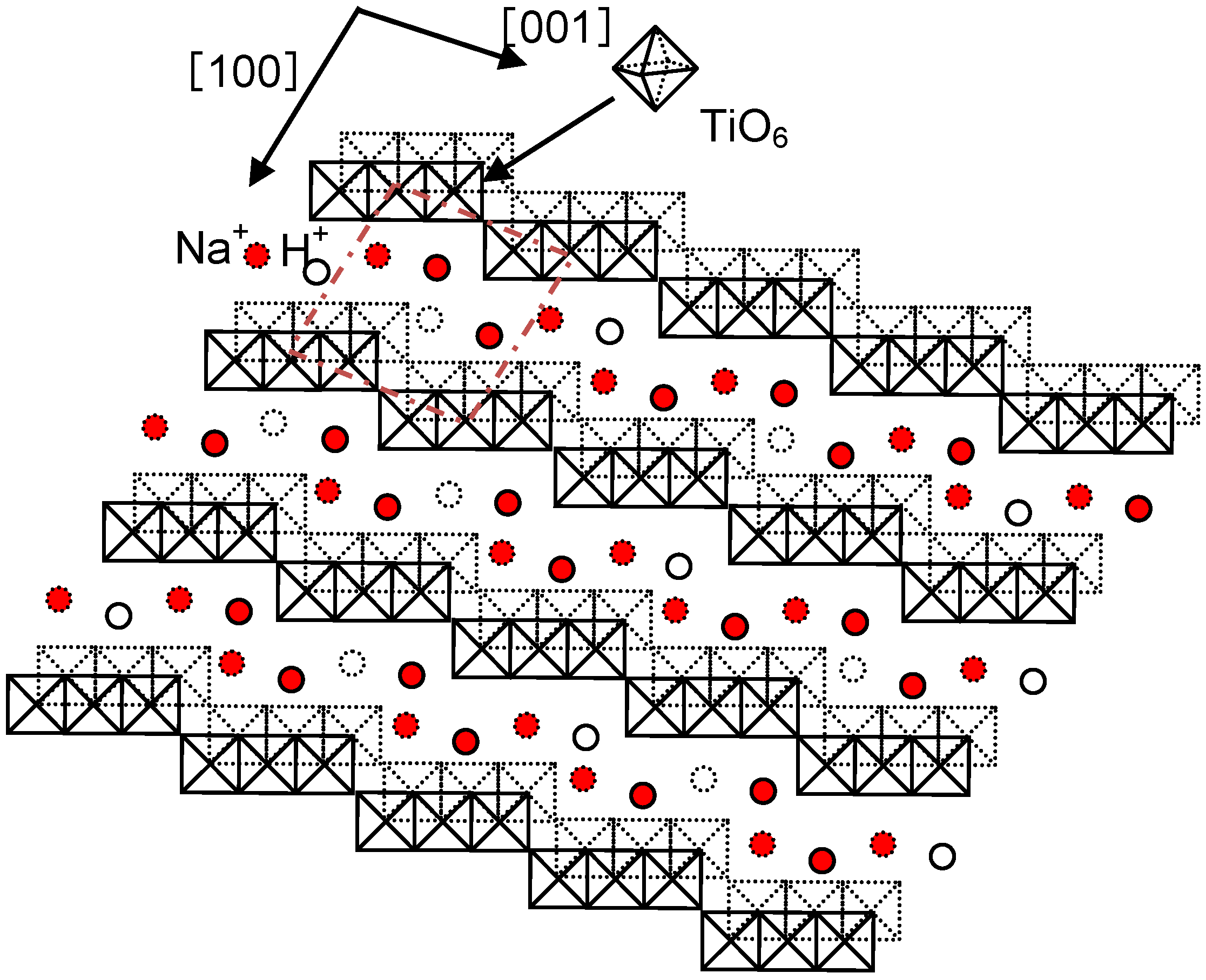
The sodium hydrogen titanate formed on Ti metal and its alloys by the NaOH treatment has a layered structure, as shown in
Figure 14 [
15]. The sodium ions in the interlayers are speculated to be easily replaced by the calcium ions in a calcium solution. Ti metal and its alloys treated using the NaOH solution are expected to form a calcium hydrogen titanate layer after the calcium solution treatment, and to form calcium titanate after a subsequent heat treatment. The resulting product could exhibit a high apatite-forming ability, as well as a higher stability in a humid environment, since the calcium ions released from the surface layer could increase the ionic activity product of the apatite in the surrounding fluid more effectively than sodium ions can, and the diffusion coefficient of the calcium ions in the surface layer would be lower than that of sodium ions.
Figure 14.
Structure of sodium hydrogen titantate [
15].
Figure 14.
Structure of sodium hydrogen titantate [
15].
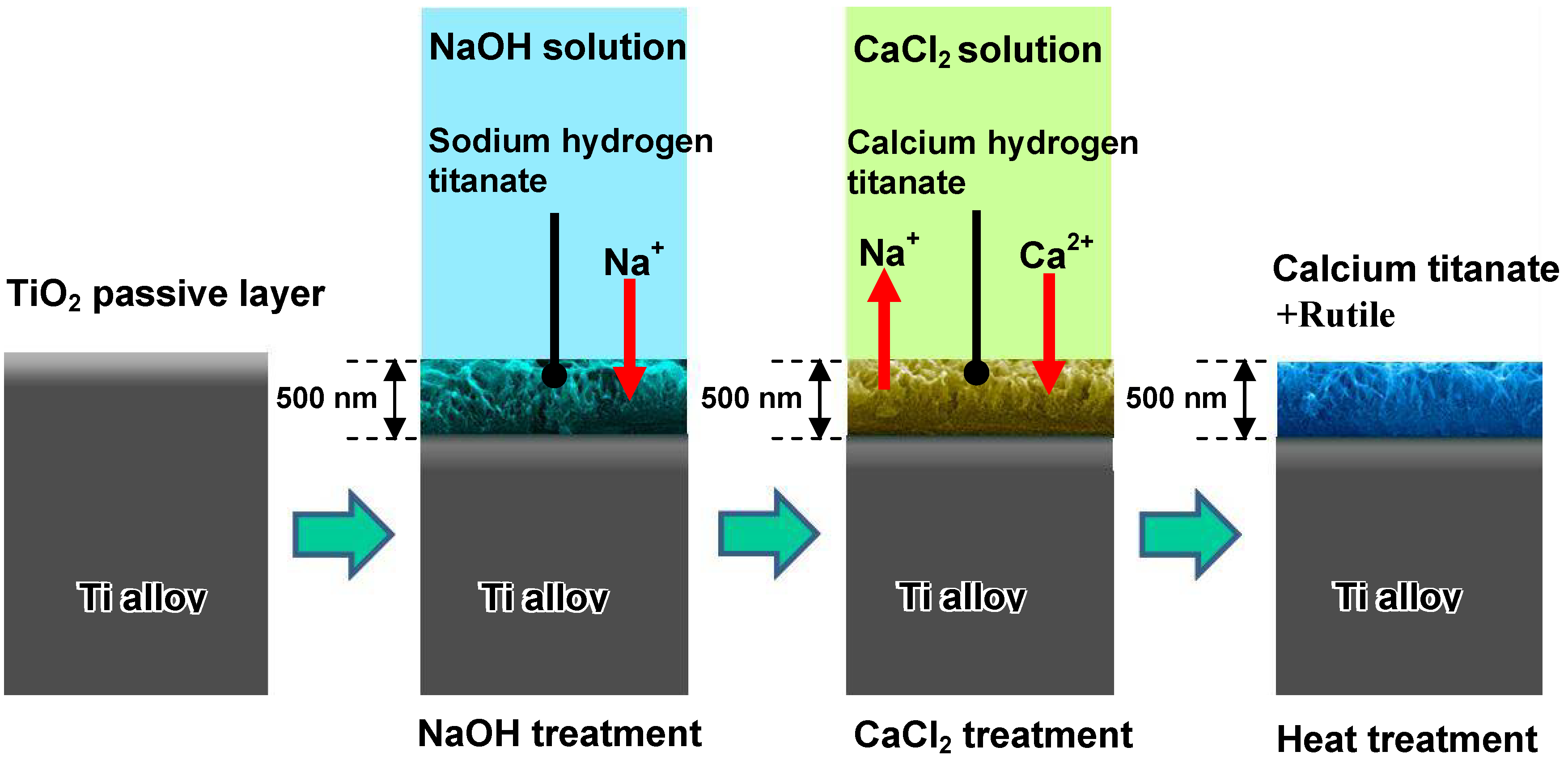
When Ti-15Zr-4Nb-4Ta alloy was soaked in 100 mM of a CaCl
2 solution at 40 °C for a period of 24 h after the NaOH treatment, the sodium hydrogen titanate formed on the alloy surface by the NaOH treatment was isomorphously transformed into calcium hydrogen titanate. This phase was converted into calcium titanate and rutile by a subsequent heat treatment at 600 °C for a period of 1 h, as shown in
Figure 15 [
16]. Unfortunately, the resulting product did not form apatite on its surface in SBF within a period of 3 days. This may be attributable to the extremely low diffusion coefficient of the calcium ions in the calcium titanate.
Figure 15.
Structural changes of surface of Ti-15Zr-4Nb-4Ta alloy subjected by NaOH, CaCl2 and heat treatments.
Figure 15.
Structural changes of surface of Ti-15Zr-4Nb-4Ta alloy subjected by NaOH, CaCl2 and heat treatments.
Such an alloy did form apatite on its surface in SBF within 3 days after it was soaked in water at 80 °C for a period of 24 h, as shown in
Figure 16 [
16]. This is attributed to an increase in diffusion coefficient of the calcium ions in the calcium titanate by the partial replacement of the calcium ions with H
3O
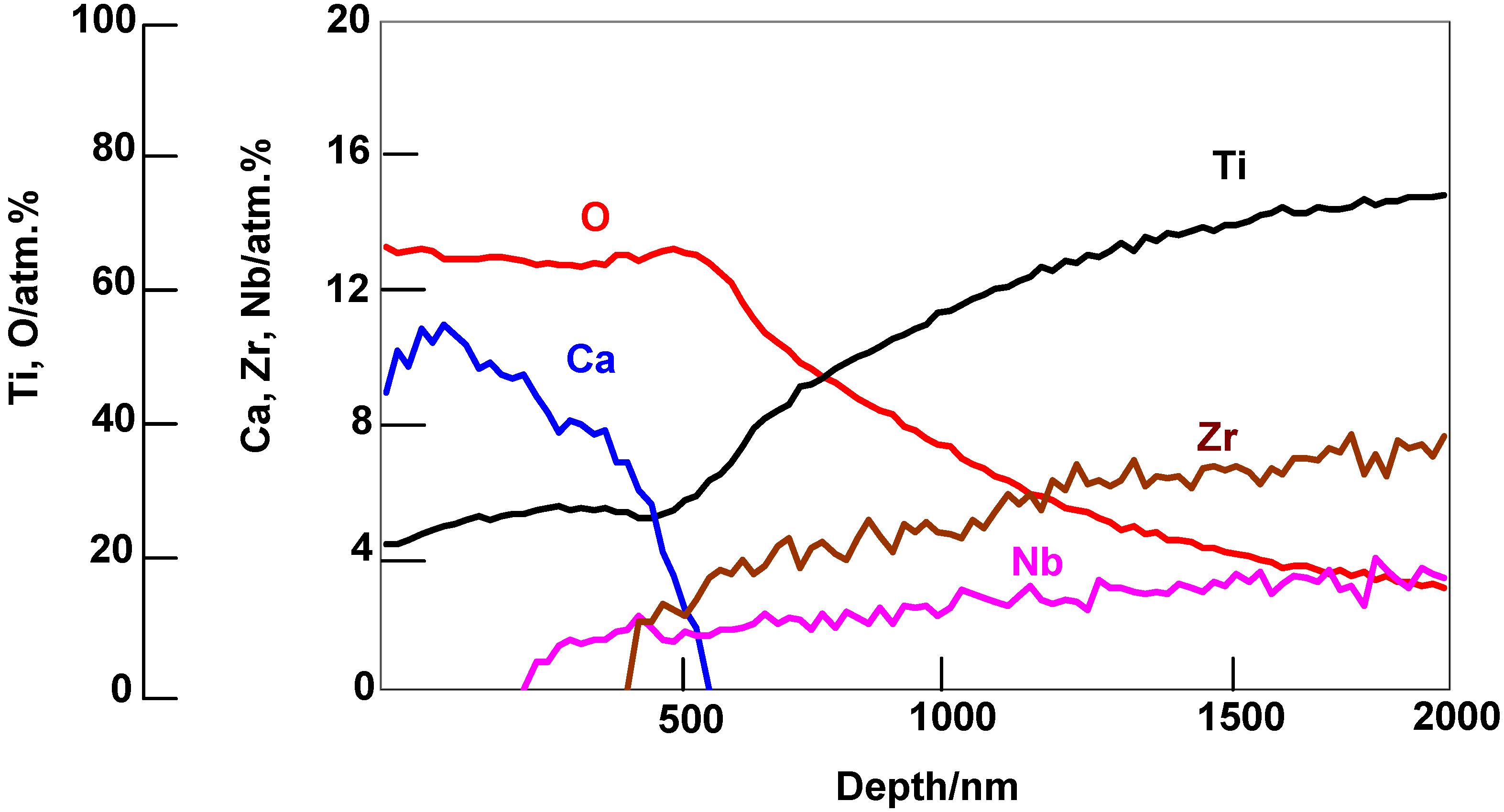
+ ions during the hot-water treatment. This partial replacement was confirmed by the depth profile of the Auger electron spectra of the resulting product shown in
Figure 17 [
16]. A decrease in Ca concentration near to the top surface is due to the ion exchange of Ca
2+ ions with H
3O
+ ions.
Figure 16.
SEM photographs of the surfaces of Ti-15Zr-4Nb-4Ta alloy soaked in SBF for 3 d after NaOH, CaCl2 and heat treatments, and subsequent water treatment.
Figure 16.
SEM photographs of the surfaces of Ti-15Zr-4Nb-4Ta alloy soaked in SBF for 3 d after NaOH, CaCl2 and heat treatments, and subsequent water treatment.
Figure 17.
AES depth profiles of the surface of Ti-15Zr-4Nb-4Ta alloy subjected to NaOH, CaCl2, heat and water treatments.
Figure 17.
AES depth profiles of the surface of Ti-15Zr-4Nb-4Ta alloy subjected to NaOH, CaCl2, heat and water treatments.
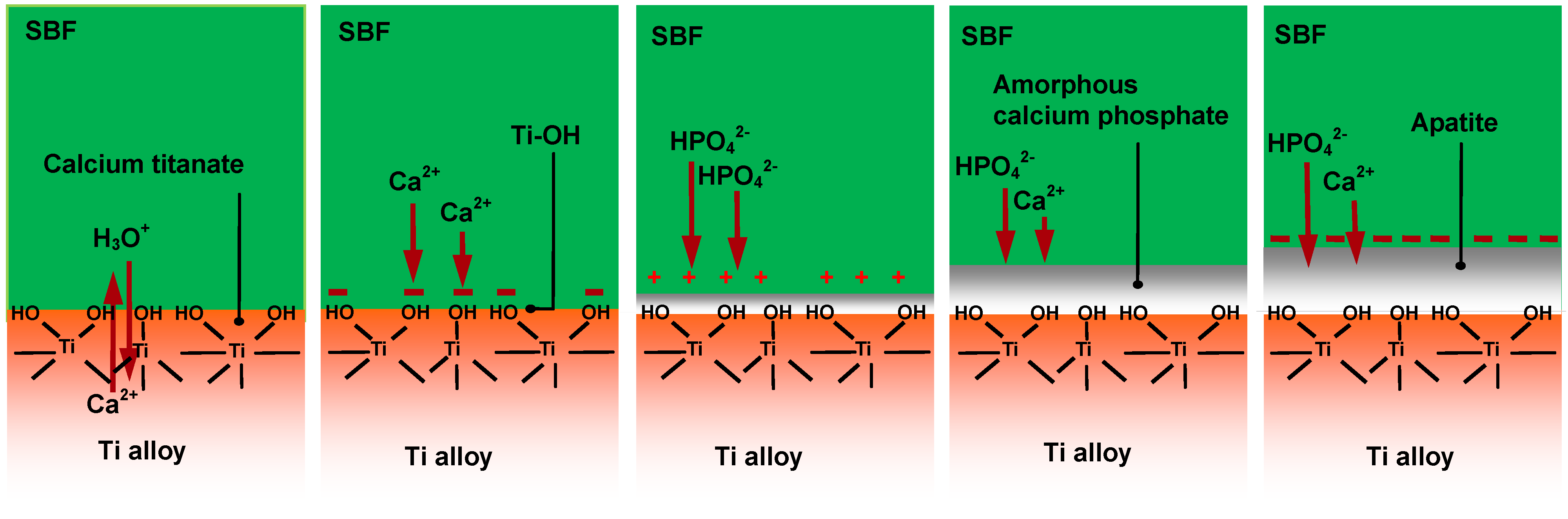
Apatite formation on an alloy enriched with calcium ions on its surface in SBF is considered to proceed by the process shown in
Figure 18. The calcium ions are released from the surface via exchange with H
3O
+ ion in SBF to produce Ti–OH groups on the surface. The thus-formed Ti–OH groups combine with the calcium ions. As the calcium ions accumulate, the surface becomes positively charged and combines with negatively charged phosphate ions forming calcium phosphate, which eventually transforms into apatite.
Figure 18.
Process of apatite formation on Ti-15Zr-4Nb-4Ta alloy subjected to NaOH, CaCl2, heat and water treatments in SBF.
Figure 18.
Process of apatite formation on Ti-15Zr-4Nb-4Ta alloy subjected to NaOH, CaCl2, heat and water treatments in SBF.
The thus-treated alloy does not show any decrease in its apatite-forming ability in SBF, even when it is stored in a 95% relative humidity at 80 °C for a period of 1 week, as expected [
16]. These treatments are also effective in inducing an apatite-forming ability in different types of Ti-Zr-Nb-Ta alloys, such as Ti-29Nb-13Ta-4.6Zr and Ti-36Nb-2Ta-3Zr-0.3O, as well as pure Ti metal.
4. Bioactive Titanium Oxide
The sodium hydrogen titanate formed on Ti metal by the NaOH treatment may substitute its Na
+ ions completely with H
3O
+ ions to form hydrogen titanate when it is exposed to water or an HCl solution, and would form titanium oxide by the subsequent heat treatment. The resulting titanium oxide would be expected to exhibit bioactivity, since even a type of pure titania gel forms bone-like apatite on its surface in SBF [
17]. If bioactive titanium oxide is obtained by such chemical and thermal treatments, then such treatments can be applied to porous titanium metals for forming a uniform bioactive layer on walls of the pores, even in deep regions. The thus-formed bioactive layer does not disturb the biological environment by the released ions, even of the narrow spaces of the pores.
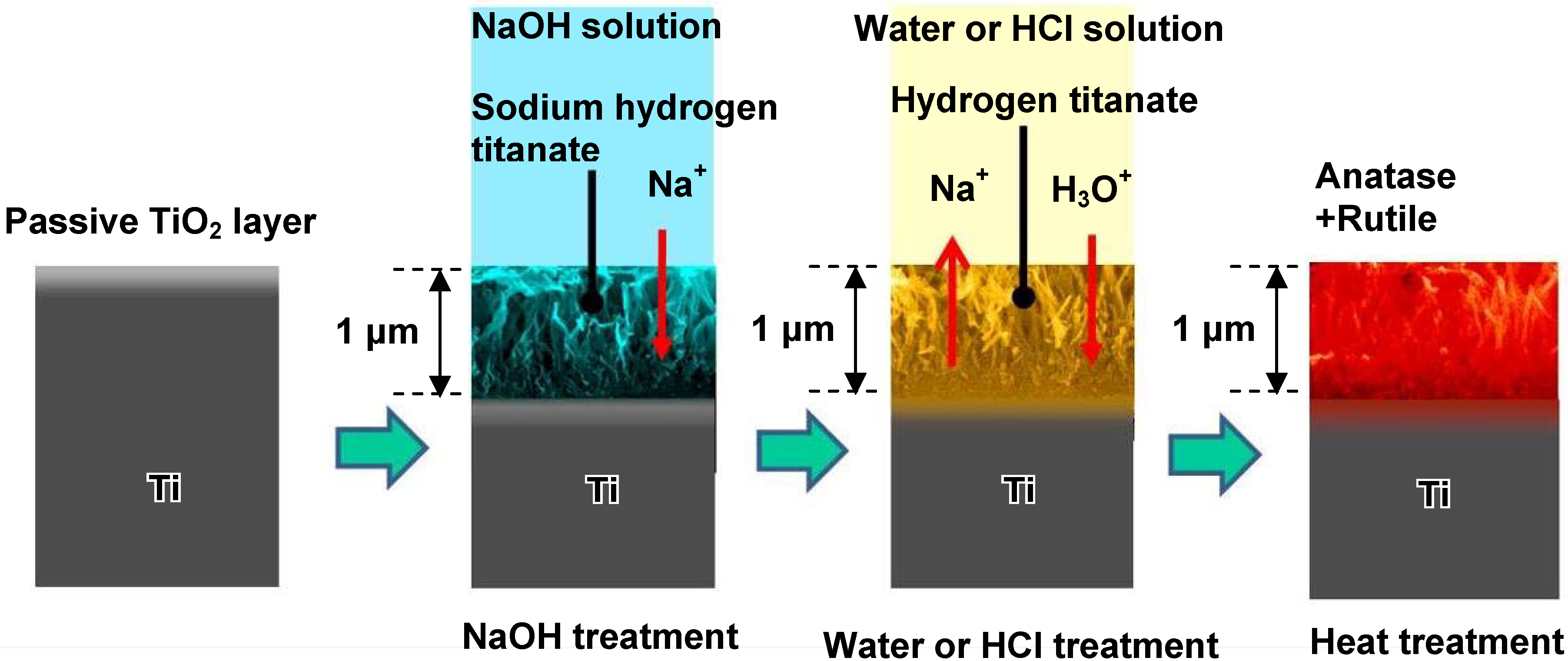
When Ti metal was soaked in pure water or an HCl solution with different concentrations ranging from 0.5 to 100 mM at 40 °C for a period of 24 h after the NaOH treatment, the sodium hydrogen titanate formed on the Ti metal by the NaOH treatment was isomorphously transformed into hydrogen titanate. This phase was converted into anatase and/or rutile TiO
2 by a subsequent heat treatment at 600 °C for a period of 1 h, as shown in
Figure 19 [
18].
Figure 19.
Surface structural change of Ti metal by NaOH, water or HCl and heat treatments.
Figure 19.
Surface structural change of Ti metal by NaOH, water or HCl and heat treatments.
The heat-treated Ti metal formed apatite on its surface in SBF within 1 day, as shown in
Figure 20. Its apatite-forming ability increased with increasing concentration of the HCl solution. Its apatite-forming ability did not depend upon the anatase to rutile ratio. The high apatite-forming ability of Ti metal treated with high concentration HCl solutions can be attributed to the high positive surface charge of the titanium oxide formed on it. Titanium oxide is usually positively charged in acidic solutions [
9]. Positively charged surface can induce apatite deposition by preferential adsorption of negatively charged phosphate ions in SBF, in contrast with the preferential adsorption of the positively charged calcium ions on the negatively charged surface of Ti metal subjected to NaOH and heat treatments.
Figure 20.
SEM photographs of surfaces of Ti metals soaked in SBF for 1 d, after NaOH, water or HCl and heat treatments.
Figure 20.
SEM photographs of surfaces of Ti metals soaked in SBF for 1 d, after NaOH, water or HCl and heat treatments.
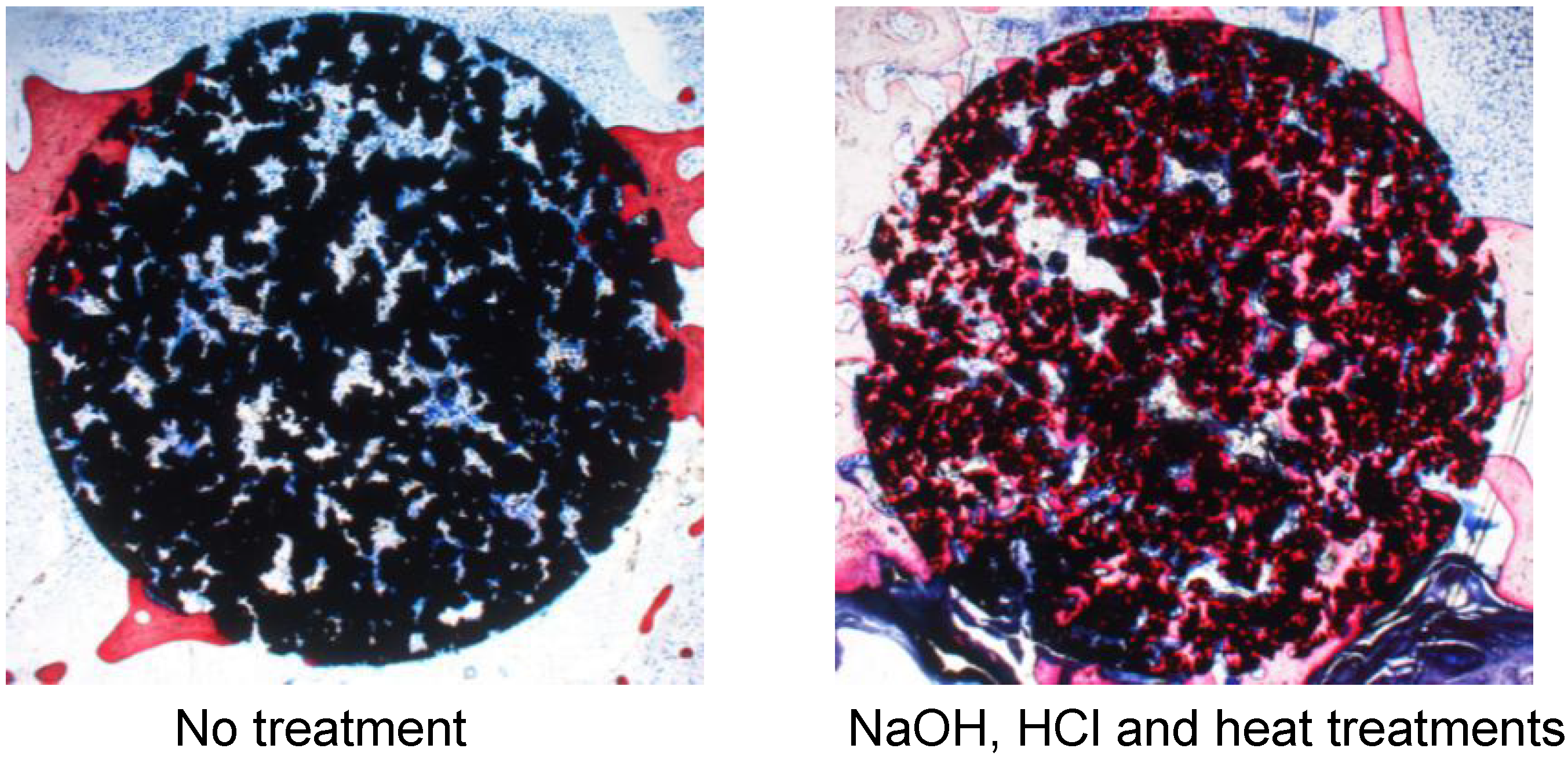
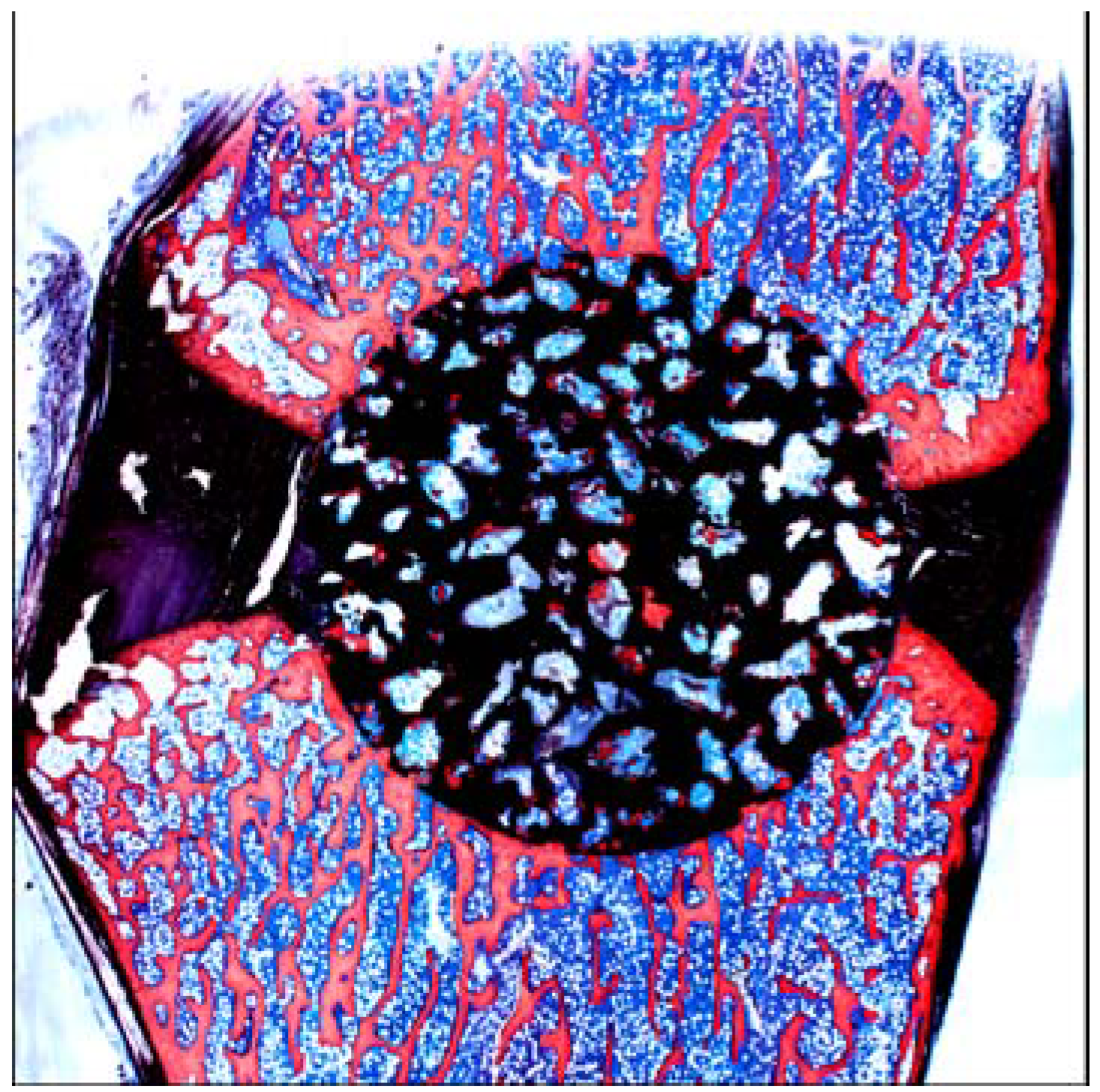
A porous Ti metal sample containing 50 to 70 vol % of interconnected pores 200–500 μm in diameter was subjected to NaOH, 0.5 mM HCl, and heat treatments to form titanium oxide on its pore walls. The thus-treated porous Ti metal was fully penetrated with newly grown bone from its periphery when it was implanted into the femur of a rabbit, as shown in
Figure 21 [
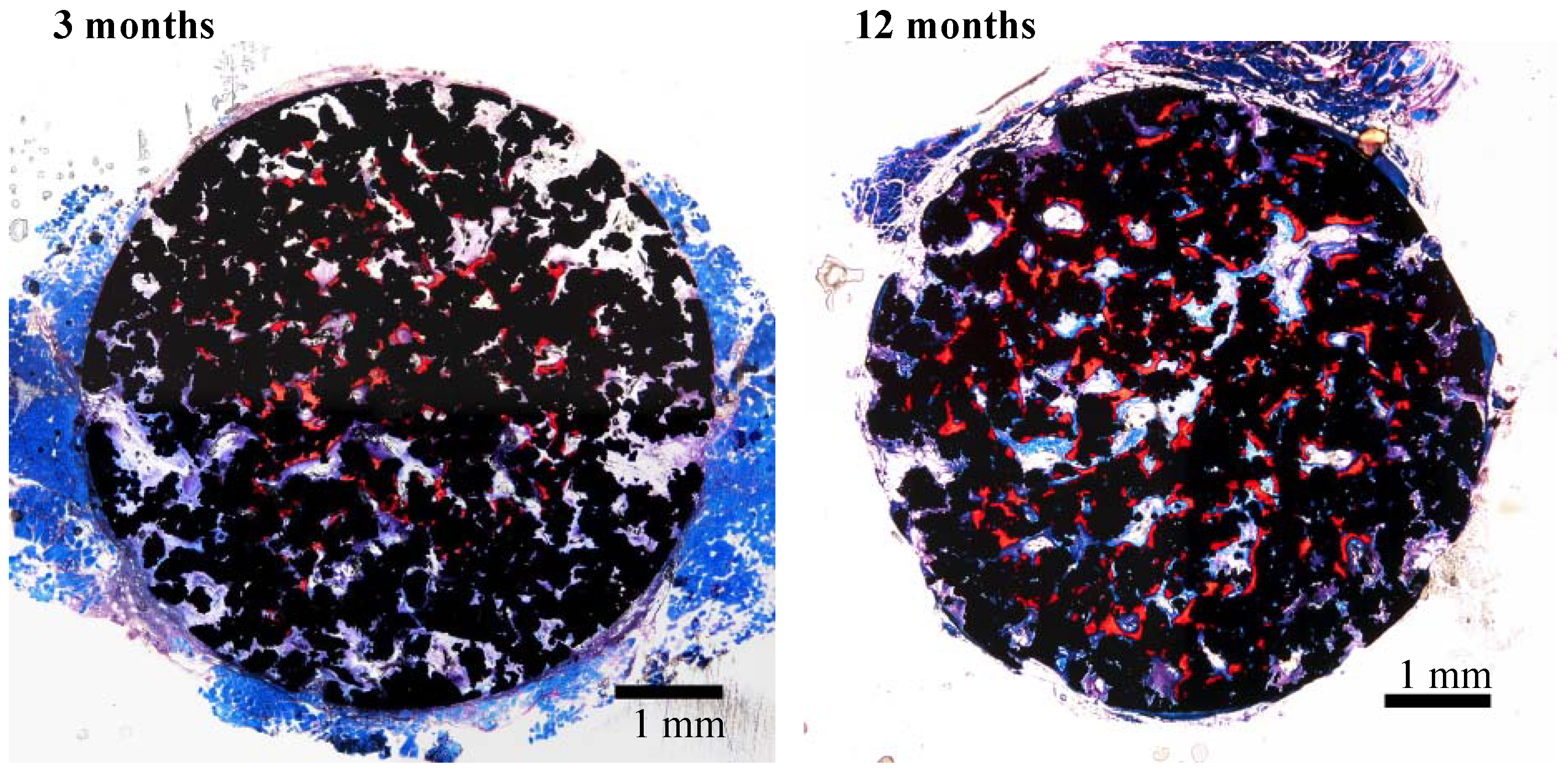
19]. This porous Ti metal formed bone tissue from its centre when it was implanted into the muscle of a dog, as shown in
Figure 22 [
20]. These results indicate that the thus-treated porous Ti metal exhibits osteoinductivity, as well as osteoconductivity. This was successfully applied to a spinal fusion device of a dog, as shown in
Figure 23 [
21], and is subject to clinical tests for a human device.
Figure 21.
Bone formation in porous Ti metals subjected to no treatment and NaOH, HCl and heat treatments, 26 weeks after implantation into rabbit femur.
Figure 21.
Bone formation in porous Ti metals subjected to no treatment and NaOH, HCl and heat treatments, 26 weeks after implantation into rabbit femur.
Figure 22.
Bone formation in porous Ti metal subjected to NaOH, HCl and heat treatments, 3 and 12 months after implantation into muscle of beagle dog. Stain: Stevenel’s blue and Van Gieson’s picrofuchsin. Reprinted from Ref. [
20] with permission from Elsevier.
Figure 22.
Bone formation in porous Ti metal subjected to NaOH, HCl and heat treatments, 3 and 12 months after implantation into muscle of beagle dog. Stain: Stevenel’s blue and Van Gieson’s picrofuchsin. Reprinted from Ref. [
20] with permission from Elsevier.
Figure 23.
Fusion of spine of dog by a bioactive porous Ti metal. Reprinted from Ref. [
21] with permission from American Association of Neurological Surgeons.
Figure 23.
Fusion of spine of dog by a bioactive porous Ti metal. Reprinted from Ref. [
21] with permission from American Association of Neurological Surgeons.