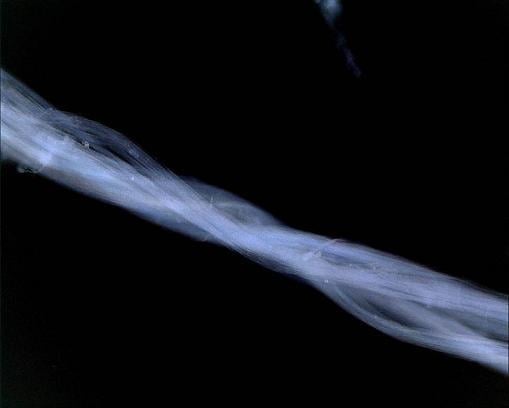
Tissue Response to Subcutaneously Implanted Recombinant Spider Silk: An in Vivo Study
Abstract
:1. Introduction
- Autologous cells are cultured in vitro and transplanted back into the patient as a cell suspension, as a graft, or in a 3D-biodegradable carrier matrix.
- A tissue is stimulated and provided the right prerequisites to regenerate in situ by implantation of specially designed materials, or the application of substances that regulate cell functions. This method is often referred to as guided tissue regeneration.
2. Results and Discussion
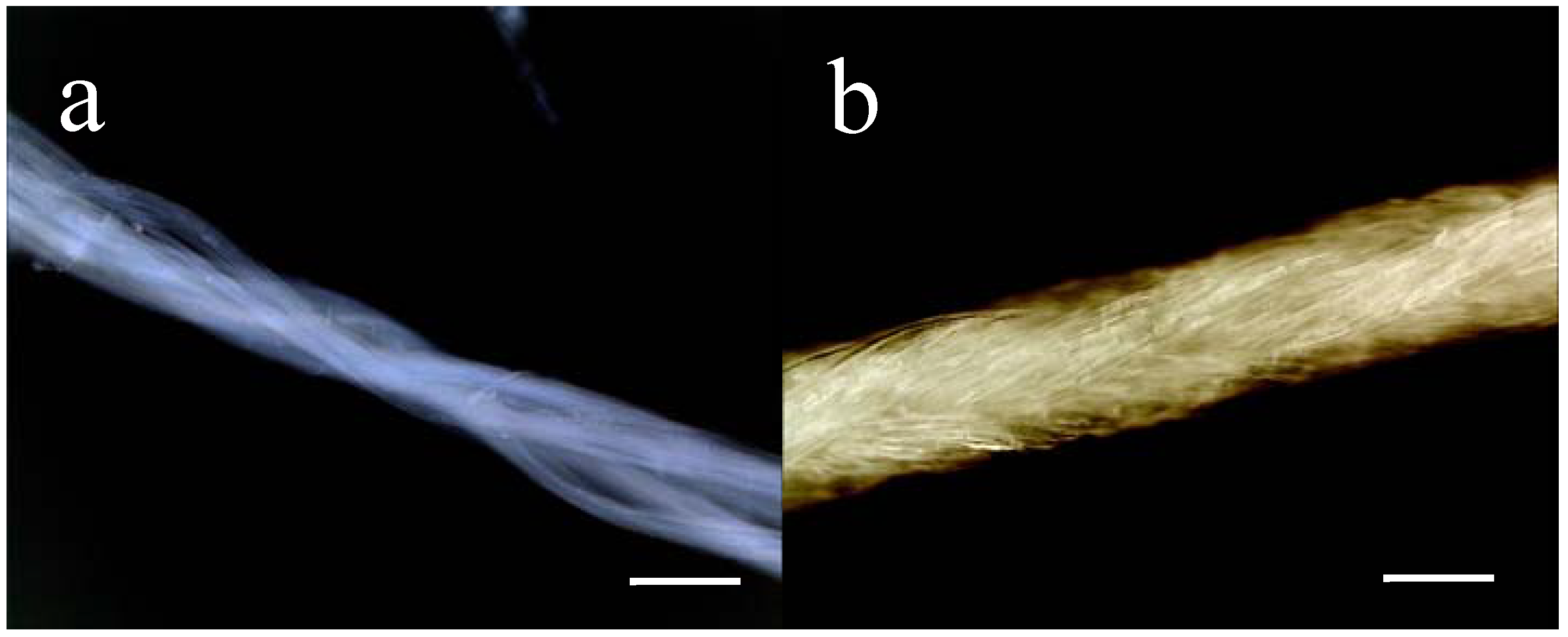
2.1. Materials
| Abbreviation | Treatment |
|---|---|
| C2 | Two EndoTrap columns |
| C3 | Three EndoTrap columns |
| C2M | Two EndoTrap columns, fibres soaked in DMEM |
| C3M | Three EndoTrap columns, fibres soaked in DMEM |
| C2MS | Two EndoTrap columns, fibres soaked in DMEM and FBS |
| C3MS | Three EndoTrap columns, fibres soaked in DMEM and FBS |
2.2. The normal tissue response to implanted materials
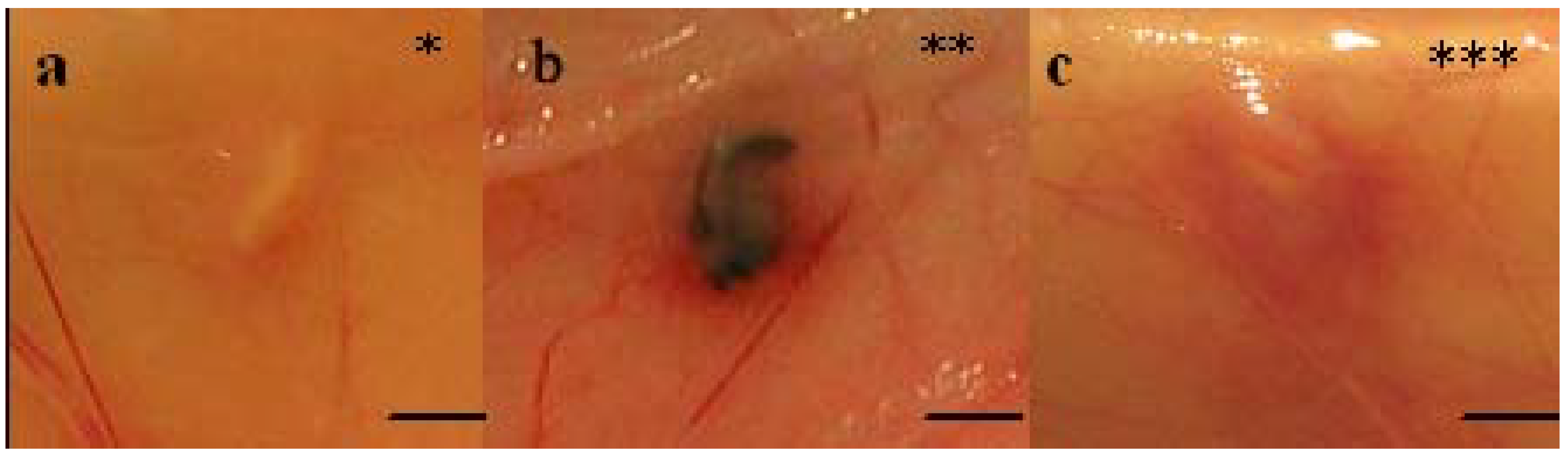
2.3. Macroscopic evaluation
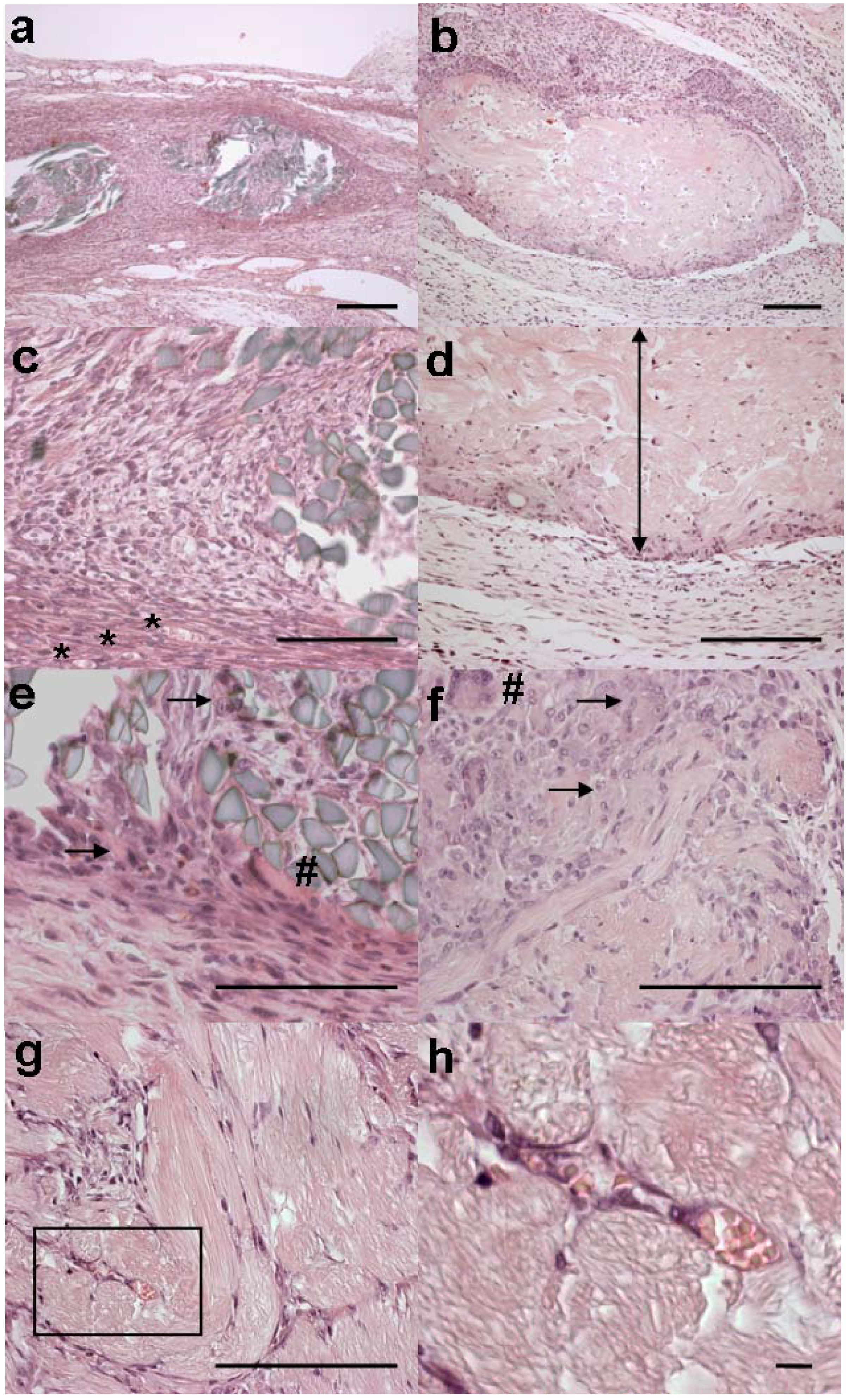
2.4. Histological evaluation
| Implant | 1 | 2 | 3 |
|---|---|---|---|
| C2 | * | ** | ** |
| C3 | * | ** | ** |
| C2M | *** | ** | * |
| C3M | *** | * | * |
| C2MS | *** | ** | *** |
| C3MS | *** | ** | ** |
| MersilkTM | * | * | ** |
| Sham | * | * | * |
| Polymorpho-nuclear cells | Phagocytic cells * | Mono-nuclear leukocytes | Capsule ** | Granulation tissue between fibres | |
|---|---|---|---|---|---|
| Animal 1, implant | |||||
| C2 | + | +++ | ++ | +++ | +++ |
| C3 | + | ++ | + | ++ | ++ |
| C2M | + | ++ | + | +++ | + |
| C3M | + | +++ | ++ | +++ | ++ |
| C2MS | +++ | ++ | ++ | +++ | + |
| C3MS | 0 | +++ | ++ | +++1 | + |
| Sham | - | - | - | - | - |
| MersilkTM | + | +++ | + | ++ | ++ |
| Animal 2, implant | |||||
| C2 | 0 | +++ | 0 | +++ | + |
| C3 | + | +++ | + | +++ | + |
| C2M | nf | nf | nf | nf | nf |
| C3M | 0 | ++ | 0 | ++ | ++ |
| C2MS | 0 | +++ | + | +++ | + |
| C3MS | 0 | +++ | + | +++ | ++ |
| Sham | - | - | - | - | - |
| MersilkTM | + | ++ | 0 | + | + |
| Animal 3, implant | |||||
| C2 | 0 | +++ | ++ | +++ | +++ |
| C3 | 0 | +++ | + | +++ | +++ |
| C2M | 0 | +++ | + | +++ | +++ |
| C3M | 0 | + | ++ | +++ | + |
| C2MS | + | ++ | +++ | +++1 | + |
| C3MS | nf | nf | nf | nf | nf |
| Sham | - | - | - | - | - |
| MersilkTM | 0 | + | + | +++ | +++ |
2.5. Features of 4RepCT for tissue engineering
3. Experimental Section
3.1. Production of 4RepCT
3.2. Protein purification and fibre formation
3.3. Treatments of protein and fibres
- Two Endotrap columns, no additional treatment (C2)
- Three Endotrap columns, no additional treatment (C3)
- Two Endotrap columns, soaked in DMEM (Dulbecco’s Modified Eagle’s Medium, Invitrogen AB, Lidingö , Sweden) for 30 minutes prior to implantation (C2M)
- Three Endotrap columns, soaked in DMEM for 30 minutes prior to implantation (C3M)
- Two Endotrap columns, soaked in DMEM containing 10% fetal bovine serum (FBS, Invitrogen AB, Lidingö, Sweden) for 30 minutes prior to implantation (C2MS)
- Three Endotrap columns, soaked in DMEM containing 10% FBS for 30 minutes prior to implantation (C3MS).
3.4. Pyrogen analysis
3.5. Subcutaneous implantation in rats
3.6. Histological observations
4. Conclusions
Acknowledgements
Supplementary Materials
References and Notes
- Langer, R.; Vacanti, J.P. Tissue engineering. Science 1993, 260, 920–926. [Google Scholar] [CrossRef] [PubMed]
- Huss, F.R.M.; Nyman, E.; Bolin, J.S.C.; Kratz, G. Use of macroporous gelatine spheres as a biodegradable scaffold for guided tissue regeneration of healthy dermis in humans: An in vivo study. J. Plast. Reconstr. Aesthet. Surg. 2009. [Google Scholar] [CrossRef]
- Mano, J.F.; Silva, G.A.; Azevedo, H.S.; Malafaya, P.B.; Sousa, R.A.; Silva, S.S.; Boesel, L.F.; Oliveira, J.M.; Santos, T.C.; Marques, A.P.; Neves, N.M.; Reis, R.L. Natural origin biodegradable systems in tissue engineering and regenerative medicine: present status and some moving trends. J. R. Soc. Interface 2007, 4, 999–1030. [Google Scholar] [CrossRef] [PubMed]
- Livesey, S.A.; Herndon, D.N.; Hollyoak, M.A.; Atkinson, Y.H.; Nag, A. Transplanted acellular allograft dermal matrix. Potential as a template for the reconstruction of viable dermis. Transplantation 1995, 60, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Place, E.S.; George, J.H.; Williams, C.K.; Stevens, M.M. Synthetic polymer scaffolds for tissue engineering. Chem. Soc. Rev. 2009, 38, 1139–1151. [Google Scholar] [CrossRef] [PubMed]
- Brown, R.A.; Phillips, J.B. Cell responses to biomimetic protein scaffolds used in tissue repair and engineering. Int. Rev. Cytol. 2007, 262, 75–150. [Google Scholar] [PubMed]
- Gosline, J.M.; Guerette, P.A.; Ortlepp, C.S.; Savage, K.N. The mechanical design of spider silks: From fibroin sequence to mechanical function. J. Exp. Biol. 1999, 202, 3295–3303. [Google Scholar] [PubMed]
- Altman, G.H.; Diaz, F.; Jakuba, C.; Calabro, T.; Horan, R.L.; Chen, J.; Lu, H.; Richmond, J.; Kaplan, D.L. Silk-based biomaterials. Biomaterials 2003, 24, 401–416. [Google Scholar] [CrossRef] [PubMed]
- Vepari, C.; Kaplan, D.L. Silk as a biomaterial. Prog. Polym. Sci. 2007, 32, 991–1007. [Google Scholar] [CrossRef] [PubMed]
- Vollrath, F.; Barth, P.; Basedow, A.; Engstrom, W.; List, H. Local tolerance to spider silks and protein polymers in vivo. In Vivo 2002, 16, 229–234. [Google Scholar] [PubMed]
- Allmeling, C.; Jokuszies, A.; Reimers, K.; Kall, S.; Choi, C.Y.; Brandes, G.; Kasper, C.; Scheper, T.; Guggenheim, M.; Vogt, P.M. Spider silk fibres in artificial nerve constructs promote peripheral nerve regeneration. Cell Proliferation 2008, 41, 408–420. [Google Scholar] [CrossRef] [PubMed]
- Kluge, J.A.; Rabotyagova, O.; Leisk, G.G.; Kaplan, D.L. Spider silks and their applications. Trends Biotech. 2008, 26, 244–251. [Google Scholar] [CrossRef]
- Menassa, R.; Zhu, H.; Karatzas, C.N.; Lazaris, A.; Richman, A.; Brandle, J. Spider dragline silk proteins in transgenic tobacco leaves: Accumulation and field production. Plant Biotechnol. J. 2004, 2, 431–438. [Google Scholar] [CrossRef] [PubMed]
- Arcidiacono, S.; Mello, C.; Kaplan, D.; Cheley, S.; Bayley, H. Purification and characterization of recombinant spider silk expressed in Escherichia coli. Appl. Microbiol. Biotechnol. 1998, 49, 31–38. [Google Scholar] [CrossRef] [PubMed]
- Arcidiacono, S.; Mello, C.M.; Butler, M.; Welsh, E.; Soares, J.W.; Allen, A.; Ziegler, D.; Laue, T.; Chase, S. Aqueous processing and fiber spinning of recombinant spider silks. Macromolecules 2002, 35, 1262–1266. [Google Scholar] [CrossRef]
- Bini, E.; Foo, C.W.; Huang, J.; Karageorgiou, V.; Kitchel, B.; Kaplan, D.L. RGD-functionalized bioengineered spider dragline silk biomaterial. Biomacromolecules 2006, 7, 3139–3145. [Google Scholar] [CrossRef] [PubMed]
- Fahnestock, S.R.; Bedzyk, L.A. Production of synthetic spider dragline silk protein in Pichia pastoris. Appl. Microbiol. Biotechnol. 1997, 47, 33–39. [Google Scholar] [CrossRef] [PubMed]
- Fahnestock, S.R.; Irwin, S.L. Synthetic spider dragline silk proteins and their production in Escherichia coli. Appl. Microbiol. Biotechnol. 1997, 47, 23–32. [Google Scholar] [CrossRef] [PubMed]
- Huemmerich, D.; Helsen, C.W.; Quedzuweit, S.; Oschmann, J.; Rudolph, R.; Scheibel, T. Primary structure elements of spider dragline silks and their contribution to protein solubility. Biochemistry 2004, 43, 13604–13612. [Google Scholar] [CrossRef] [PubMed]
- Huemmerich, D.; Scheibel, T.; Vollrath, F.; Cohen, S.; Gat, U.; Ittah, S. Novel assembly properties of recombinant spider dragline silk proteins. Curr. Biol. 2004, 14, 2070–2074. [Google Scholar] [CrossRef] [PubMed]
- Lazaris, A.; Arcidiacono, S.; Huang, Y.; Zhou, J.F.; Duguay, F.; Chretien, N.; Welsh, E.A.; Soares, J.W.; Karatzas, C.N. Spider silk fibers spun from soluble recombinant silk produced in mammalian cells. Science 2002, 259, 472–476. [Google Scholar] [CrossRef]
- Lewis, R.V.; Hinman, M.; Kothakota, S.; Fournier, M.J. Expression and purification of a spider silk protein: A new strategy for producing repetitive proteins. Protein Exp. Purif. 1996, 7, 400–406. [Google Scholar] [CrossRef]
- O'Brien, J.P.; Fahnestock, S.R.; Termonia, Y.; Gardner, K.C.H. Nylons from nature: Synthetic analogs to spider silk. Adv. Mater. 1998, 10, 1185–1195. [Google Scholar] [CrossRef]
- Prince, J.; Mcgrath, K.; Digirolamo, C.; Kaplan, D. Construction, cloning, and expression of synthetic genes encoding spider dragline silk. Biochemistry 1995, 34, 10879–10885. [Google Scholar] [CrossRef] [PubMed]
- Scheller, J.; Gührs, K.-H.; Grosse, F.; Conrad, U. Production of spider silk proteins in tobacco and potato. Nat. Biotechnol. 2001, 19, 573–577. [Google Scholar] [CrossRef] [PubMed]
- Teule, F.; Cooper, A.R.; Furin, W.A.; Bittencourt, D.; Rech, E.L.; Brooks, A.; Lewis, R.V. A protocol for the production of recombinant spider silk-like proteins for artificial fiber spinning. Nat. Protoc. 2009, 4, 341–355. [Google Scholar] [CrossRef] [PubMed]
- Stark, M.; Grip, S.; Rising, A.; Hedhammar, M.; Engstrom, W.; Hjalm, G.; Johansson, J. Macroscopic fibers self-assembled from recombinant miniature spider silk proteins. Biomacromolecules 2007, 8, 1695–1701. [Google Scholar] [CrossRef] [PubMed]
- Grip, S.; Johansson, J.; Hedhammar, M. Engineered disulfides improve mechanical properties of recombinant spider silk. Protein Sci. 2009, 18, 1012–1022. [Google Scholar] [CrossRef] [PubMed]
- Gorbet, M.B.; Sefton, M.V. Endotoxin: the uninvited guest. Biomaterials 2005, 26, 6811–6817. [Google Scholar] [CrossRef] [PubMed]
- Hasiwa, M.; Kullmann, K.; von Aulock, S.; Klein, C.; Hartung, T. An in vitro pyrogen safety test for immune-stimulating components on surfaces. Biomaterials 2007, 28, 1367–1375. [Google Scholar] [CrossRef] [PubMed]
- Hartung, T.; Wendel, A. Detection of pyrogens using human whole blood. In Vitro Toxicol. 1996, 9, 353–359. [Google Scholar]
- Williams, K.L. Endotoxins: Pyrogens, LAL Testing and Depyrogenation; 3rd ed.; Informa Healthcare USA, Inc: New York, NY, USA, 2007; Vol. 167. [Google Scholar]
- Setzen, G.; Williams, E.F. 3rd Tissue response to suture materials implanted subcutaneously in a rabbit model. Plast. Reconstr. Surg. 1997, 100, 1788–1795. [Google Scholar] [CrossRef] [PubMed]
- Anderson, J.M.; Rodriguez, A.; Chang, D.T. Foreign body reaction to biomaterials. Sem. Immunol. 2008, 20, 86–100. [Google Scholar] [CrossRef]
- Fernandez-Cossio, S.; Castano-Oreja, M.T. Biocompatibility of two novel dermal fillers: Histological evaluation of implants of a hyaluronic acid filler and a polyacrylamide filler. Plast. Reconstr. Surg. 2006, 117, 1789–1796. [Google Scholar] [CrossRef] [PubMed]
- Foschi, D.; Corsi, F.; Cellerino, P.; Rizzi, A.; Morandi, E.; Trabucchi, E. Angiogenic effects of suture biomaterials. An experimental study in rats. European surgical research. Europaische chirurgische Forschung 2001, 33, 16–20. [Google Scholar] [CrossRef]
- Kasoju, N.; Bhonde, R.R.; Bora, U. Preparation and characterization of Antheraea assama silk fibroin based novel non-woven scaffold for tissue engineering applications. J. Tiss. Eng. Regener. Med. 2009, 3, 539–552. [Google Scholar] [CrossRef]
- Hedhammar, M.; Rising, A.; Grip, S.; Martinez, A.S.; Nordling, K.; Casals, C.; Stark, M.; Johansson, J. Structural properties of recombinant nonrepetitive and repetitive parts of major ampullate spidroin 1 from Euprosthenops australis: implications for fiber formation. Biochemistry 2008, 47, 3407–3417. [Google Scholar] [CrossRef] [PubMed]
© 2009 by the authors; licensee Molecular Diversity Preservation International, Basel, Switzerland. This article is an open-access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Fredriksson, C.; Hedhammar, M.; Feinstein, R.; Nordling, K.; Kratz, G.; Johansson, J.; Huss, F.; Rising, A. Tissue Response to Subcutaneously Implanted Recombinant Spider Silk: An in Vivo Study. Materials 2009, 2, 1908-1922. https://doi.org/10.3390/ma2041908
Fredriksson C, Hedhammar M, Feinstein R, Nordling K, Kratz G, Johansson J, Huss F, Rising A. Tissue Response to Subcutaneously Implanted Recombinant Spider Silk: An in Vivo Study. Materials. 2009; 2(4):1908-1922. https://doi.org/10.3390/ma2041908
Chicago/Turabian StyleFredriksson, Camilla, My Hedhammar, Ricardo Feinstein, Kerstin Nordling, Gunnar Kratz, Jan Johansson, Fredrik Huss, and Anna Rising. 2009. "Tissue Response to Subcutaneously Implanted Recombinant Spider Silk: An in Vivo Study" Materials 2, no. 4: 1908-1922. https://doi.org/10.3390/ma2041908
APA StyleFredriksson, C., Hedhammar, M., Feinstein, R., Nordling, K., Kratz, G., Johansson, J., Huss, F., & Rising, A. (2009). Tissue Response to Subcutaneously Implanted Recombinant Spider Silk: An in Vivo Study. Materials, 2(4), 1908-1922. https://doi.org/10.3390/ma2041908